Efficacy and Cytotoxicity of Binary Mixtures as Root Canal Filling Solvents
Abstract
1. Introduction
2. Materials and Methods
2.1. Solvents and Mixtures
2.2. Sample Preparation, Dissolution and Characterization
2.2.1. Weight Loss
2.2.2. Surface Topography
2.2.3. Mechanical Properties
2.3. The Cytotoxicity of Solvents and Mixtures
2.4. Statistical Analysis
3. Results
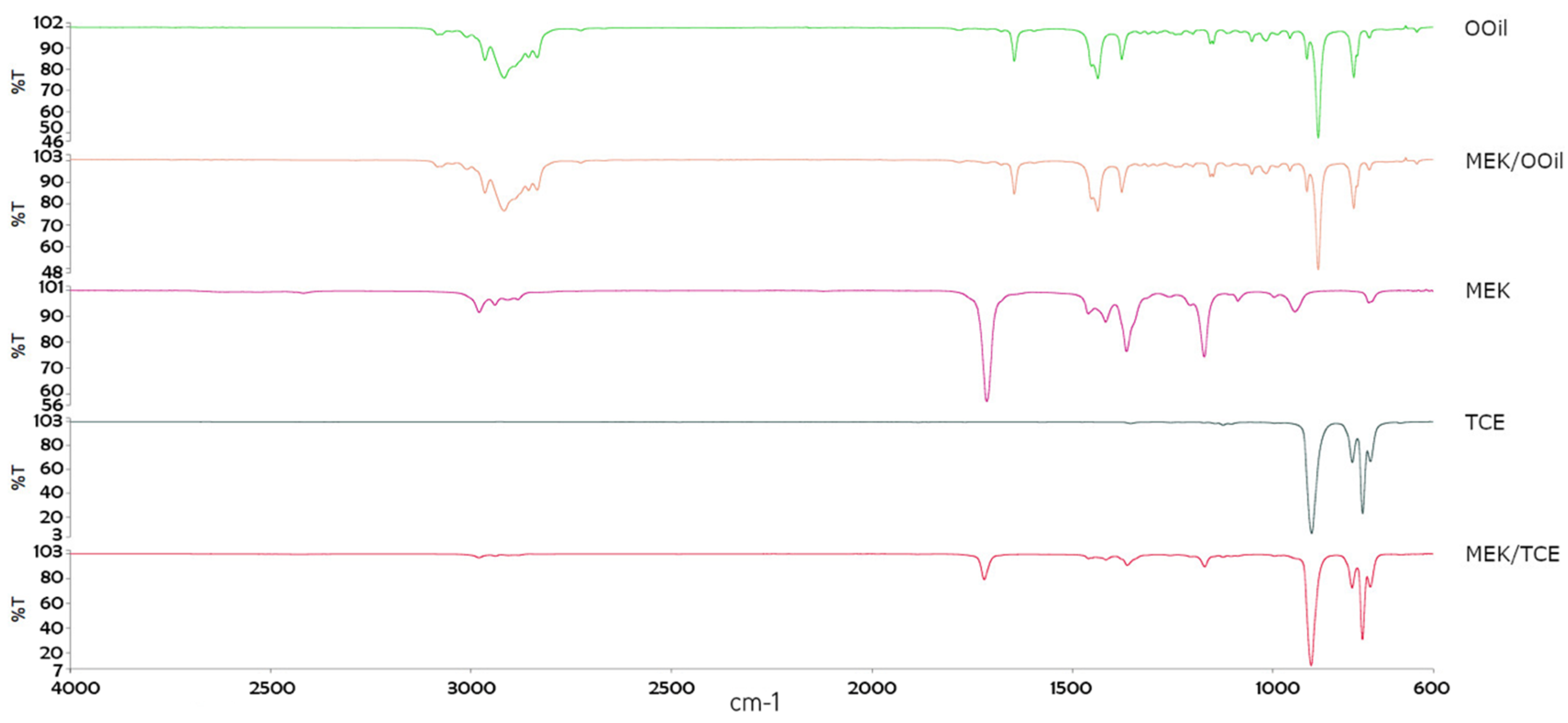
3.1. Elemental Chemical Analysis of the Solvents and Mixtures
3.2. Dissolution of Gutta-Percha and AH Plus Sealer
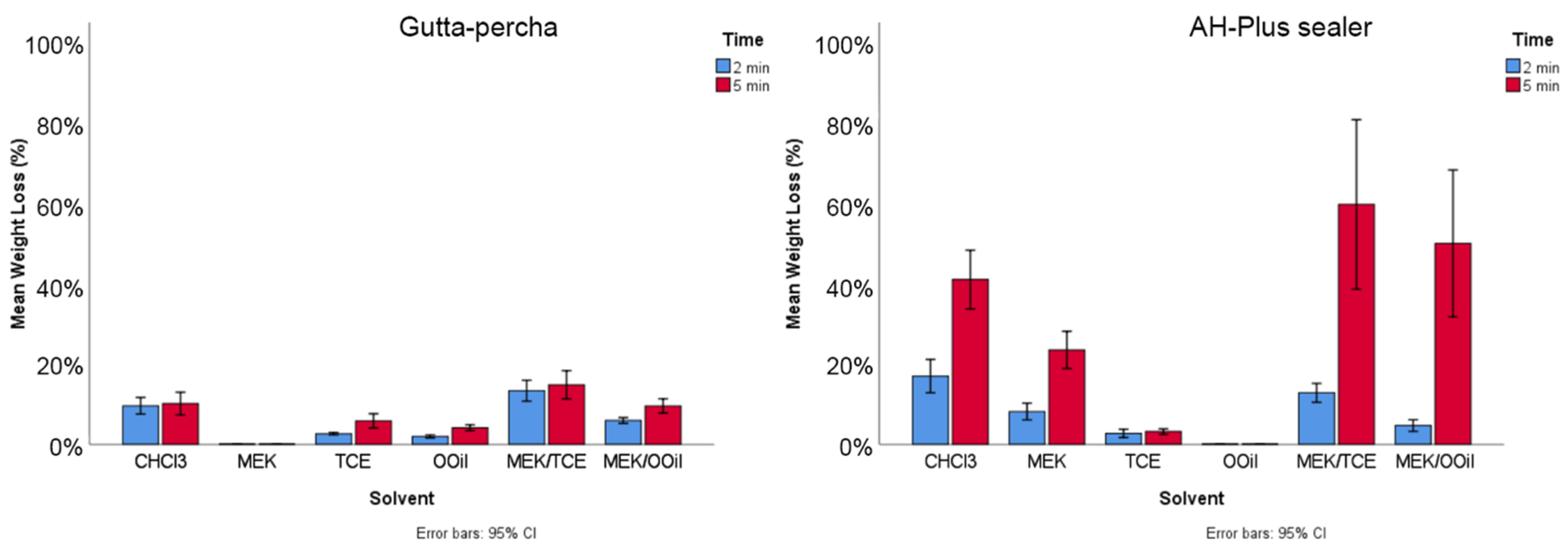
3.2.1. Weight Loss
3.2.2. Surface Topography
3.2.3. Mechanical Properties
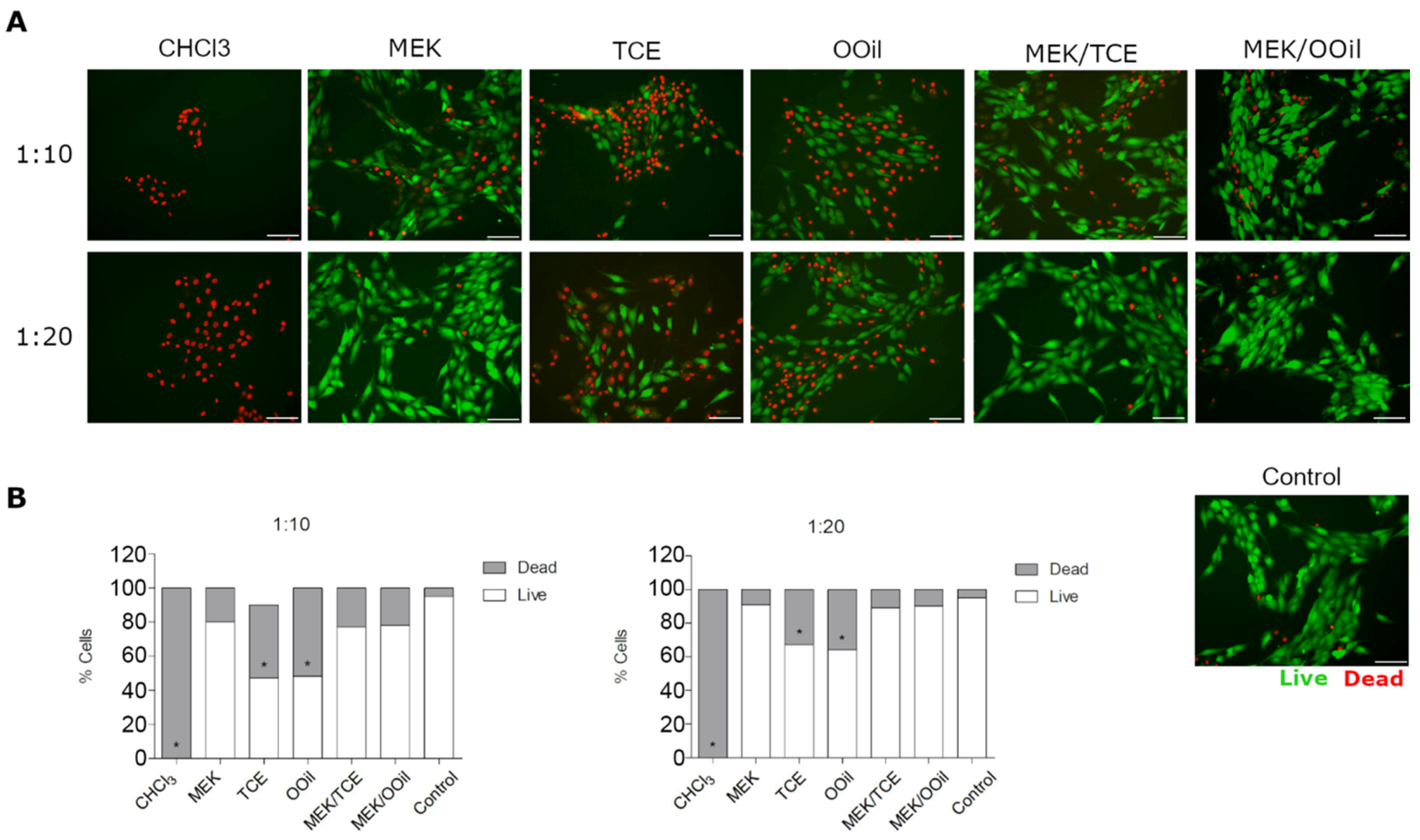
3.3. In Vitro Cytotoxicity
4. Discussion
5. Conclusions
Author Contributions
Funding
Conflicts of Interest
References
- Correia-Sousa, J.; Carvalho, M.F.; Teles, A.M.; Pina-Vaz, I.; Madureira, A.R. Apical periodontitis and related risk factors: Cross-sectional study. Rev. Port. Estomatol. Med. Dentária Cir. Maxilofac. 2015, 56, 226–232. [Google Scholar] [CrossRef]
- Melo, L.; Ferreira, I.; Lacet, G.; Braga, A.C.; Pina-Vaz, I. Apical periodontitis and oral status in patients with different systemic conditions and smoking habits in Portuguese population. Rev. Endod. 2017, 35, 10–22. [Google Scholar]
- Zehnder, M.; Paqué, F. Disinfection of the root canal system during root canal re-treatment. Endod. Top. 2008, 19, 58–73. [Google Scholar] [CrossRef]
- Vieira, A.R.; Siqueira, J.F.; Ricucci, D.; Lopes, W.S.; Siqueira, J.F. Dentinal Tubule Infection as the Cause of Recurrent Disease and Late Endodontic Treatment Failure: A Case Report. J. Endod. 2012, 38, 250–254. [Google Scholar] [CrossRef] [PubMed]
- Oltra, E.; Cox, T.C.; LaCourse, M.R.; Johnson, J.D.; Paranjpe, A. Retreatability of two endodontic sealers, EndoSequence BC Sealer and AH Plus: A micro-computed tomographic comparison. Restor. Dent. Endod. 2017, 42, 19–26. [Google Scholar] [CrossRef] [PubMed]
- Alves, F.R.; Alves, F.R.F.; Sousa, J.C.N.; Silveira, S.B.; Provenzano, J.C.; Siqueira, J.F. Removal of Root Canal Fillings in Curved Canals Using Either Reciprocating Single- or Rotary Multi-instrument Systems and a Supplementary Step with the XP-Endo Finisher. J. Endod. 2016, 42, 1114–1119. [Google Scholar] [CrossRef]
- Çanakçi, B.C.; Er, O.; Dincer, A. Do the Sealer Solvents Used Affect Apically Extruded Debris in Retreatment? J. Endod. 2015, 41, 1507–1509. [Google Scholar] [CrossRef]
- Kfir, A.; Tsesis, I.; Yakirevich, E.; Matalon, S.; Abramovitz, I. The efficacy of five techniques for removing root filling material: Microscopic versus radiographic evaluation. Int. Endod. J. 2011, 45, 35–41. [Google Scholar] [CrossRef] [PubMed]
- Rossi-Fedele, G.; Ahmed, H.M.A.; Dent, M.C. Assessment of Root Canal Filling Removal Effectiveness Using Micro–computed Tomography: A Systematic Review. J. Endod. 2017, 43, 520–526. [Google Scholar] [CrossRef] [PubMed]
- Duncan, H.F.; Chong, B.S. Removal of root filling materials. Endod. Top. 2008, 19, 33–57. [Google Scholar] [CrossRef]
- De Faria-Júnior, N.B.; De Loiola, L.E.; Guerreiro-Tanomaru, J.M.; Berbert, F.L.C.V.; Tanomaru-Filho, M. Effectiveness of three solvents and two associations of solvents on gutta-percha and resilon. Braz. Dent. J. 2011, 22, 41–44. [Google Scholar] [CrossRef] [PubMed]
- Ferreira, I.; Braga, A.C.; Lopes, M.A.; Pina-Vaz, I. Improvement of the efficacy of endodontic solvents by ultrasonic agitation. Saudi Dent. J. 2019, in press. [Google Scholar] [CrossRef]
- Mushtaq, M.; Masoodi, A.; Farooq, R.; Khan, F.Y. The Dissolving Ability of Different Organic Solvents on Three Different Root Canal Sealers: In Vitro Study. Iran. Endod. J. 2012, 7, 198–202. [Google Scholar] [PubMed]
- Ferreira, I.; Soares, S.; Sousa, J.; Barros, J.; Braga, A.C.; Lopes, M.A.; Pina-Vaz, I. New Insight into the Dissolution of Epoxy Resin–based Sealers. J. Endod. 2017, 43, 1505–1510. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Martos, J.; Bassotto, A.P.S.; González-Rodríguez, M.P.; Ferrer-Luque, C.M. Dissolving efficacy of eucalyptus and orange oil, xylol and chloroform solvents on different root canal sealers. Int. Endod. J. 2011, 44, 1024–1028. [Google Scholar] [CrossRef]
- ISO: International Organization for Standardization. ISO 6876-Dentistry: Dental Root Sealing Materials; ISO: Geneva, Switzerland, 2012. [Google Scholar]
- Magalhães, B.S.; Johann, J.E.; Lund, R.G.; Martos, J.; Del Pino, F.A.B. Dissolving efficacy of some organic solvents on gutta-percha. Braz. Oral Res. 2007, 21, 303–307. [Google Scholar] [CrossRef]
- Haypek, E.; Silva, L.; Batista, E.; Marques, D.S.; Meireles, M.; Meirelles, A. Recovery of aroma compounds from orange essential oil. Braz. J. Chem. Eng. 2000, 17, 705–712. [Google Scholar] [CrossRef]
- Vajrabhaya, L.-O.; Suwannawong, S.K.; Kamolroongwarakul, R.; Pewklieng, L. Cytotoxicity evaluation of gutta-percha solvents: Chloroform and GP-Solvent (limonene). Oral Surg. Oral Med. Oral Pathol. Oral Radiol. Endodontol. 2004, 98, 756–759. [Google Scholar] [CrossRef]
- Ribeiro, D.A.; Matsumoto, M.A.; Marques, M.E.A.; Salvadori, D.M. Biocompatibility of gutta-percha solvents using in vitro mammalian test-system. Oral Surg. Oral Med. Oral Pathol. Oral Radiol. Endodontol. 2007, 103, e106–e109. [Google Scholar] [CrossRef]
- Friedman, C.M.; Sandrik, J.L.; Heuer, M.A.; Rapp, G.W. Composition and Mechanical Properties of Gutta-Percha Endodontic Points. J. Dent. Res. 1975, 54, 921–925. [Google Scholar] [CrossRef]
- Maniglia-Ferreira, C.; Silva, J.B., Jr.; Paula, R.C.; Feitosa, J.P.; Cortez, D.G.; Zaia, A.A.; Souza-Filho, F.J. Brazilian gutta-percha points: Part I: Chemical composition and X-ray diffraction analysis. Braz. Oral Res. 2005, 19, 193–197. [Google Scholar] [CrossRef] [PubMed]
- Marín-Bauza, G.A.; Silva-Sousa, Y.T.C.; Da Cunha, S.A.; Rached-Junior, F.J.A.; Bonetti-Filho, I.; Sousa-Neto, M.D.; Miranda, C.E.S. Physicochemical properties of endodontic sealers of different bases. J. Appl. Oral Sci. 2012, 20, 455–461. [Google Scholar] [CrossRef]
- Goodman, A.; Schilder, H.; Aldrich, W. The thermomechanical properties of gutta-percha. Oral Surg. Oral Med. Oral Pathol. 1974, 37, 954–961. [Google Scholar] [CrossRef]
- Zehnder, M. Root Canal Irrigants. J. Endod. 2006, 32, 389–398. [Google Scholar] [CrossRef]
- Topçuoğlu, H.S.; Demirbuga, S.; Tuncay, O.; Arslan, H.; Kesim, B.; Yasa, B. The bond strength of endodontic sealers to root dentine exposed to different gutta-percha solvents. Int. Endod. J. 2014, 47, 1100–1106. [Google Scholar] [CrossRef]
- Palhais, M.; Sousa-Neto, M.D.; Rached-Junior, F.J.A.; Amaral, M.C.D.A.; Alfredo, E.; Miranda, C.E.S.; Silva-Sousa, Y.T.C. Influence of solvents on the bond strength of resin sealer to intraradicular dentin after retreatment. Braz. Oral Res. 2017, 31. [Google Scholar] [CrossRef]
- Nasim, I.; Neelakantan, P.; Subbarao, C.V. Effect of gutta-percha solvents on the bond strength of two resin-based sealers to root canal dentin. Acta Odontol. Scand. 2013, 72, 376–379. [Google Scholar] [CrossRef] [PubMed]


| Sample 1 | Sample 2 | Pa |
|---|---|---|
| Orange Oil | Tetrachloroethylene | 0.143 |
| Orange Oil | MEK | 0.002 |
| Orange Oil | MEK/Orange Oil | <0.001 |
| Orange Oil | Chloroform | <0.001 |
| Orange Oil | MEK/Tetrachloroethylene | <0.001 |
| Tetrachloroethylene | MEK | 1.000 |
| Tetrachloroethylene | MEK/Orange Oil | <0.001 |
| Tetrachloroethylene | Chloroform | <0.001 |
| Tetrachloroethylene | MEK/Tetrachloroethylene | <0.001 |
| MEK | MEK/Orange Oil | 0.003 |
| MEK | Chloroform | <0.001 |
| MEK | MEK/Tetrachloroethylene | <0.001 |
| MEK/Orange Oil | Chloroform | 0.141 |
| MEK/Orange Oil | MEK/Tetrachloroethylene | 0.014 |
| Chloroform | MEK/Tetrachloroethylene | 1.000 |
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Ferreira, I.; Grenho, L.; Gomes, P.; Braga, A.C.; Fernandes, M.H.; Lopes, M.A.; Pina-Vaz, I. Efficacy and Cytotoxicity of Binary Mixtures as Root Canal Filling Solvents. Materials 2020, 13, 3237. https://doi.org/10.3390/ma13143237
Ferreira I, Grenho L, Gomes P, Braga AC, Fernandes MH, Lopes MA, Pina-Vaz I. Efficacy and Cytotoxicity of Binary Mixtures as Root Canal Filling Solvents. Materials. 2020; 13(14):3237. https://doi.org/10.3390/ma13143237
Chicago/Turabian StyleFerreira, Inês, Liliana Grenho, Pedro Gomes, Ana Cristina Braga, Maria Helena Fernandes, Maria Ascensão Lopes, and Irene Pina-Vaz. 2020. "Efficacy and Cytotoxicity of Binary Mixtures as Root Canal Filling Solvents" Materials 13, no. 14: 3237. https://doi.org/10.3390/ma13143237
APA StyleFerreira, I., Grenho, L., Gomes, P., Braga, A. C., Fernandes, M. H., Lopes, M. A., & Pina-Vaz, I. (2020). Efficacy and Cytotoxicity of Binary Mixtures as Root Canal Filling Solvents. Materials, 13(14), 3237. https://doi.org/10.3390/ma13143237











