What Are the Causes of Death among Patients Admitted to a Contemporary Tertiary-Level Cardiology Department? An Analysis of 10 Years of Morbidity and Mortality Meetings
Abstract
1. Introduction
2. Materials and Methods
3. Results
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Derrington, M.C.; Gallimore, S. The effect of the National Confidential Enquiry into Perioperative Deaths on clinical practice. Report of a postal survey of a sample of consultant anaesthetists. Anaesthesia 1997, 52, 3–8. [Google Scholar] [CrossRef] [PubMed]
- Giesbrecht, V.; Au, S. Morbidity and Mortality Conferences: A Narrative Review of Strategies to Prioritize Quality Improvement. Jt. Comm. J. Qual. Patient Saf. 2016, 42, 516–527. [Google Scholar] [CrossRef] [PubMed]
- Higginson, J.; Walters, R.; Fulop, N. Mortality and morbidity meetings: An untapped resource for improving the governance of patient safety? BMJ Qual. Saf. 2012, 21, 576–585. [Google Scholar] [CrossRef] [PubMed]
- Bal, G.; Sellier, E.; Tchouda, S.D.; François, P. Improving quality of care and patient safety through morbidity and mortality conferences. J. Healthc. Qual. 2014, 36, 29–36. [Google Scholar] [CrossRef]
- Ksouri, H.; Balanant, P.Y.; Tadié, J.M.; Heraud, G.; Abboud, I.; Lerolle, N.; Faisy, C. Impact of morbidity and mortality conferences on analysis of mortality and critical events in intensive care practice. Am. J. Crit. Care 2010, 19, 135–145. [Google Scholar] [CrossRef][Green Version]
- Epstein, N.E. Morbidity and mortality conferences: Their educational role and why we should be there. Surg. Neurol. Int. 2012, 3, S377–S388. [Google Scholar] [CrossRef]
- George, J. Medical morbidity and mortality conferences: Past, present and future. Postgrad. Med. J. 2017, 93, 148–152. [Google Scholar] [CrossRef]
- Wakabayashi, K.; Ikeda, N.; Kajimoto, K.; Minami, Y.; Keida, T.; Asai, K.; Sato, N. Trends and predictors of non-cardiovascular death in patients hospitalized for acute heart failure. Int. J. Cardiol. 2018, 250, 164–170. [Google Scholar] [CrossRef]
- Vicent, L.; Bruña, V.; Devesa, C.; Sousa-Casasnovas, I.; Juárez, M.; Fernández-Avilés, F.; Martinez-Sellés, M. Seasonality in Mortality in a Cardiology Department: A Five-Year Analysis in 500 Patients. Cardiology 2019, 142, 67–72. [Google Scholar] [CrossRef]
- Vicent, L.; Bruña, V.; Devesa, C.; García-Carreño, J.; Sousa-Casasnovas, I.; Juárez, M.; Martínez-Sellés, M. An overview of end-of-life issues in a cardiology department. Is the mode of death worse in the cardiac intensive care unit? J. Geriatr. Cardiol. 2019, 16, 482–489. [Google Scholar]
- National Confidential Enquiry into Patient Outcome and Death. Available online: https://www.ncepod.org.uk/grading.html (accessed on 17 August 2020).
- Thiene, G. Sudden cardiac death in the young: A genetic destiny? Clin. Med. 2018, 18 (Suppl. S2), s17–s23. [Google Scholar] [CrossRef] [PubMed]
- Bezzina, C.R.; Lahrouchi, N.; Priori, S.G. Genetics of sudden cardiac death. Circ. Res. 2015, 116, 1919–1936. [Google Scholar] [CrossRef]
- Braunwald, E. The treatment of acute myocardial infarction: The Past, the Present, and the Future. Eur. Heart J. Acute Cardiovasc. Care 2012, 1, 9–12. [Google Scholar] [CrossRef] [PubMed]
- Laforgia, P.L.; Auguadro, C.; Bronzato, S.; Durante, A. The Reduction of Mortality in Acute Myocardial Infarction: From Bed Rest to Future Directions. Int. J. Prev. Med. 2022, 13, 56. [Google Scholar]
- Dani, S.S.; Lone, A.N.; Javed, Z.; Khan, M.S.; Zia Khan, M.; Kaluski, E.; Khan, S.U. Trends in Premature Mortality from Acute Myocardial Infarction in the United States, 1999 to 2019. J. Am. Heart Assoc. 2022, 11, e021682. [Google Scholar] [CrossRef]
- Siddiqi, T.J.; Minhas, A.M.K.; Greene, S.J.; Van Spall, H.G.; Khan, S.S.; Pandey, A.; Mentz, R.J.; Fonarow, G.C.; Butler, J.; Khan, M.S. Trends in Heart Failure-Related Mortality among Older Adults in the United States From 1999–2019. JACC Heart Fail. 2022, 10, 851–859. [Google Scholar] [CrossRef] [PubMed]
- Roger, V.L. Epidemiology of Heart Failure: A Contemporary Perspective. Circ. Res. 2021, 128, 1421–1434. [Google Scholar] [CrossRef]
- Society for Cardiothoracic Surgery in Great Britain and Ireland. Aortic Dissection Kills More People in the UK Than Road Traffic Accidents. Available online: https://scts.org/aortic-dissection-kills-more-people-in-the-uk-than-road-traffic-accidents/ (accessed on 21 September 2020).
- Chahal, R.S.; Chukwu, C.A.; Kalra, P.R.; Kalra, P.A. Heart failure and acute renal dysfunction in the cardiorenal syndrome. Clin. Med. 2020, 20, 146–150. [Google Scholar] [CrossRef]
- Kümler, T.; Gislason, G.H.; Kober, L.; Gustafsson, F.; Schou, M.; Torp-Pedersen, C. Renal function at the time of a myocardial infarction maintains prognostic value for more than 10 years. BMC Cardiovasc. Disord. 2011, 11, 37. [Google Scholar] [CrossRef]
- Rhee, C.; Jones, T.M.; Hamad, Y.; Pande, A.; Varon, J.; O’brien, C.; Anderson, D.J.; Warren, D.K.; Dantes, R.B.; Epstein, L.; et al. Prevalence, Underlying Causes, and Preventability of Sepsis-Associated Mortality in US Acute Care Hospitals. JAMA Netw. Open 2019, 2, e187571. [Google Scholar] [CrossRef]
- Torvik, M.A.; Nymo, S.H.; Nymo, S.H.; Bjørnsen, L.P.; Kvarenes, H.W.; Ofstad, E.H. Patient characteristics in sepsis-related deaths: Prevalence of advanced frailty, comorbidity, and age in a Norwegian hospital trust. Infection 2023, in press. [CrossRef]
- Bagnall, R.D.; Weintraub, R.G.; Ingles, J.; Duflou, J.; Yeates, L.; Lam, L.; Semsarian, C. A Prospective Study of Sudden Cardiac Death among Children and Young Adults. N. Engl. J. Med. 2016, 374, 2441–2452. [Google Scholar] [CrossRef]
- Eckart, R.E.; Shry, E.A.; Burke, A.P.; McNear, J.A.; Appel, D.A.; Castillo-Rojas, L.M.; Avedissian, L.; Pearse, L.A.; Potter, R.N.; Tremaine, L.; et al. Sudden death in young adults: An autopsy-based series of a population undergoing active surveillance. J. Am. Coll. Cardiol. 2011, 58, 1254–1261. [Google Scholar] [CrossRef]
- Díez-Villanueva, P.; Salamanca, J.; Rojas, A.; Alfonso, F. Importance of frailty and comorbidity in elderly patients with severe aortic stenosis. J. Geriatr. Cardiol. 2017, 14, 379–382. [Google Scholar]
- Esme, M.; Topeli, A.; Yavuz, B.B.; Akova, M. Infections in the Elderly Critically-Ill Patients. Front. Med. 2019, 6, 118. [Google Scholar] [CrossRef]

| CAUSE OF DEATH | 2010 (%) | 2011 (%) | 2012 (%) | 2013 (%) | 2014 (%) | 2015 (%) | 2016 (%) | 2017 (%) | 2018 (%) | 2019 (%) |
|---|---|---|---|---|---|---|---|---|---|---|
| Acute myocardial infarction | 61.9 | 69.5 | 59.8 | 61.8 | 52.3 | 50.0 | 58.3 | 51.0 | 52.2 | 46.7 |
| Heart failure | 11.1 | 15.3 | 13.7 | 15.1 | 21.1 | 23.3 | 12.5 | 19.5 | 17.9 | 25.9 |
| Aortic stenosis | 1.6 | 1.7 | 2.6 | 2.6 | 0.0 | 3.3 | 0.0 | 4.7 | 2.2 | 1.5 |
| Isolated cardiac arrest | 1.6 | 5.1 | 6.0 | 6.6 | 10.1 | 6.7 | 7.6 | 6.7 | 6.7 | 5.9 |
| Infective endocarditis | 1.6 | 0.0 | 0.9 | 2.0 | 1.8 | 2.5 | 1.4 | 0.7 | 4.5 | 1.5 |
| Arrhythmia | 0.0 | 3.4 | 3.4 | 3.9 | 5.5 | 0.8 | 2.1 | 3.4 | 3.7 | 3.0 |
| Cardiac tamponade | 0.0 | 0.0 | 0.9 | 0.0 | 0.0 | 1.7 | 0.7 | 1.3 | 0.7 | 1.5 |
| Other cardiac causes | 0.0 | 0.0 | 0.0 | 0.0 | 0.9 | 0.8 | 2.1 | 0.0 | 2.2 | 2.2 |
| Total cardiac (%) | 77.8 | 94.9 | 87.2 | 92.1 | 91.7 | 89.2 | 84.7 | 87.2 | 90.3 | 88.1 |
| Pathologies of aorta | 6.3 | 0.0 | 0.0 | 2.0 | 2.8 | 3.3 | 3.5 | 0.7 | 0.0 | 4.4 |
| Sepsis | 4.8 | 3.4 | 7.7 | 2.0 | 0.9 | 4.2 | 4.9 | 4.7 | 6.7 | 4.4 |
| Pulmonary embolism | 3.2 | 1.7 | 0.0 | 0.0 | 0.9 | 1.7 | 1.4 | 0.7 | 0.0 | 0.0 |
| Malignancy | 1.6 | 0.0 | 1.7 | 0.0 | 1.8 | 0.0 | 3.5 | 0.0 | 2.2 | 0.0 |
| Stroke | 1.6 | 0.0 | 0.9 | 0.0 | 0.0 | 0.0 | 0.0 | 2.7 | 0.7 | 0.0 |
| Other non-cardiac | 4.8 | 0.0 | 2.6 | 3.9 | 1.8 | 1.7 | 2.1 | 4.0 | 0.0 | 3.0 |
| Total non-cardiac (%) | 22.2 | 5.1 | 12.8 | 7.9 | 8.3 | 10.8 | 15.3 | 12.8 | 9.7 | 11.9 |
| Absolute number of deaths | 63 | 59 | 117 | 152 | 109 | 120 | 144 | 149 | 134 | 135 |
| MAIN GROUP | SUBGROUP | Total (n = 1182) | % | Age < 65 (n = 236) | % | Age ≥ 65 (n = 946) | % | p-Value | Men (n = 717) | % | Women (n = 426) | % | p-Value |
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
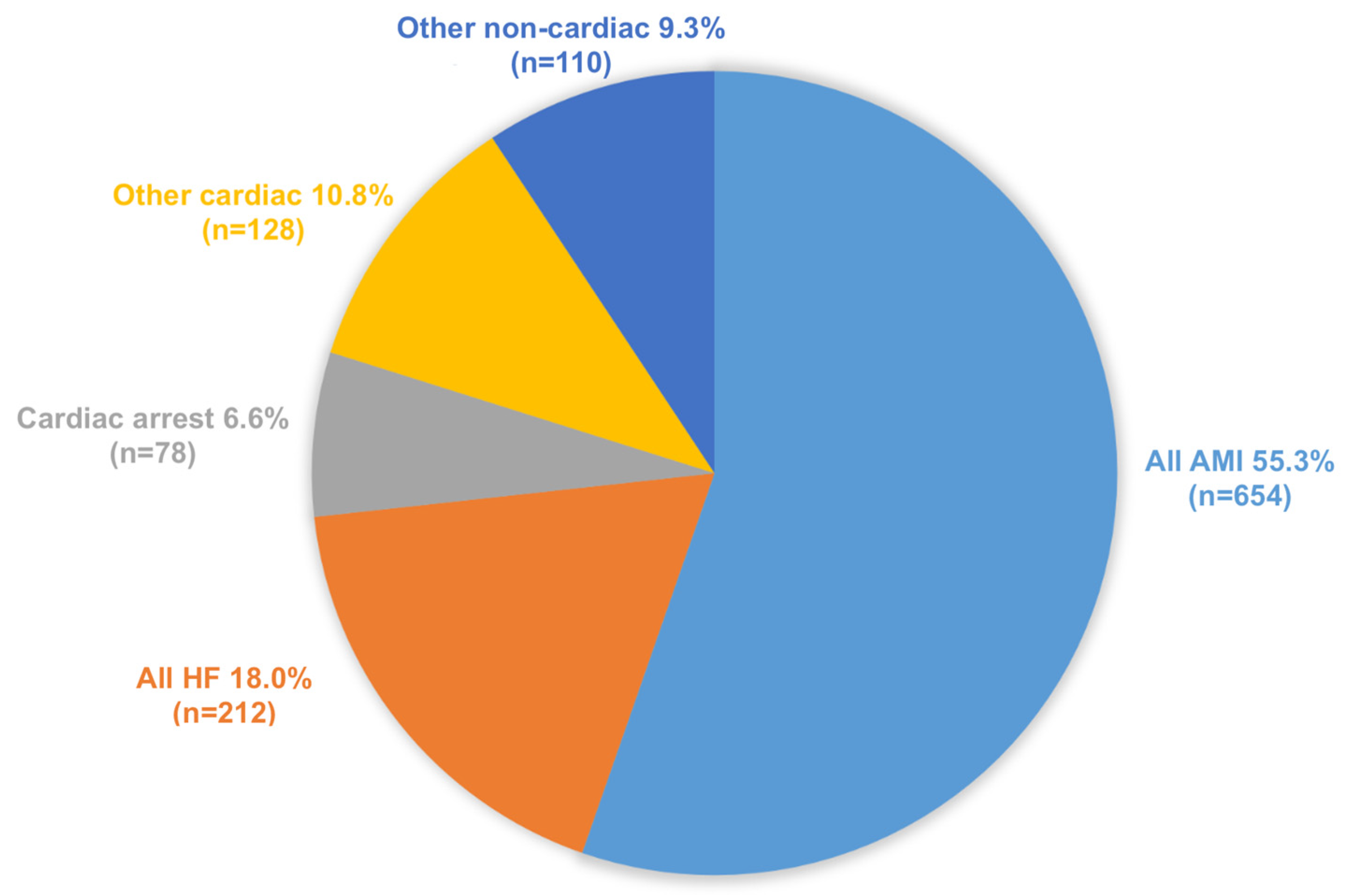
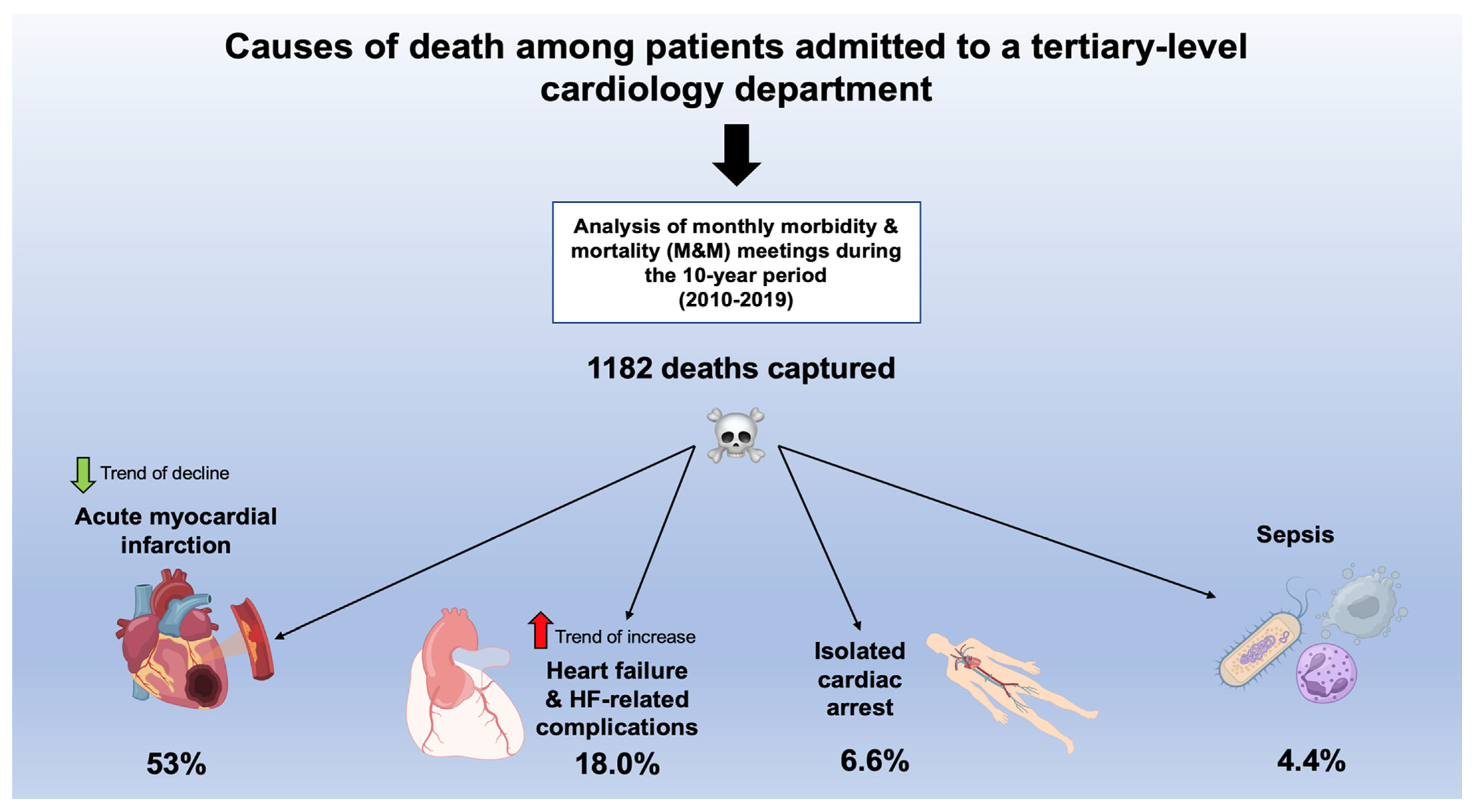
| Acute myocardial infarction (N = 654) | AMI | 626 | 53.0 | 118 | 50.0 | 508 | 53.7 | 0.31 | 367 | 51.2 | 232 | 54.5 | 0.28 |
| AMI/non-HF complication | 28 | 2.4 | 4 | 1.7 | 24 | 2.5 | 0.45 | 19 | 2.6 | 7 | 1.6 | 0.27 | |
| Heart failure (N = 212) | Heart failure (HF) | 138 | 11.7 | 24 | 10.2 | 114 | 12.1 | 0.42 | 94 | 13.1 | 41 | 9.6 | 0.08 |
| HF/complication | 74 | 6.3 | 9 | 3.8 | 65 | 6.9 | 0.083 | 42 | 5.9 | 31 | 7.3 | 0.34 | |
| Isolated cardiac arrest (N = 78) | Cardiac arrest | 78 | 6.6 | 37 | 15.7 | 41 | 4.3 | <0.001 | 51 | 7.1 | 26 | 6.1 | 0.51 |
| Other cardiac causes (N = 102) | Aortic stenosis (AS) | 17 | 1.4 | 2 | 0.9 | 15 | 1.6 | 0.39 | 6 | 0.8 | 11 | 2.6 | 0.02 |
| AS & complication | 8 | 0.7 | 0 | 0 | 8 | 0.9 | 0.16 | 5 | 0.7 | 3 | 0.7 | 0.99 | |
| Infective endocarditis | 21 | 1.8 | 3 | 1.3 | 18 | 1.9 | 0.51 | 17 | 2.4 | 4 | 0.9 | 0.08 | |
| Arrhythmia | 36 | 3.0 | 3 | 1.3 | 33 | 3.5 | 0.076 | 18 | 2.5 | 16 | 3.8 | 0.23 | |
| Cardiac tamponade | 9 | 0.8 | 3 | 1.3 | 6 | 0.6 | 0.31 | 7 | 1.0 | 2 | 0.48 | 0.35 | |
| Other cardiac cause | 11 | 0.9 | 7 | 3.0 | 4 | 0.4 | <0.001 | 8 | 1.1 | 3 | 0.7 | 0.49 | |
| Other non-cardiac causes (N = 136) | Pathology of aorta | 26 | 2.2 | 4 | 1.7 | 22 | 2.3 | 0.56 | 14 | 2.0 | 11 | 2.6 | 0.48 |
| Sepsis | 52 | 4.4 | 9 | 3.8 | 43 | 4.6 | 0.62 | 39 | 5.4 | 12 | 2.8 | 0.04 | |
| Pulmonary embolism | 9 | 0.8 | 4 | 1.7 | 5 | 0.5 | 0.065 | 2 | 0.3 | 7 | 1.6 | 0.01 | |
| Malignancy | 13 | 1.1 | 5 | 2.1 | 8 | 0.9 | 0.093 | 11 | 1.5 | 2 | 0.5 | 0.10 | |
| Stroke | 7 | 0.6 | 1 | 0.4 | 6 | 0.6 | 0.71 | 2 | 0.3 | 4 | 0.9 | 0.14 | |
| Other non-cardiac | 29 | 2.5 | 3 | 1.3 | 26 | 2.8 | 0.19 | 15 | 2.1 | 14 | 3.3 | 0.21 |
| Acute Myocardial Infarction | Aortic Stenosis | Pathologies of Aorta | Arrhythmia | ||||
|---|---|---|---|---|---|---|---|
| Valvular heart disease Arrhythmia Bleeding Peripheral vascular disease Bowel complication Sepsis Other organ dysfunction | 4 1 3 1 6 6 7 | Bowel complication Arrhythmia Sepsis | 2 2 4 | AAA rupture Thoracic aorta occlusion Thoracic acute aorta syndrome Thoracic aorta infection | 3 1 19 3 | Tachycardia Bradycardia | 13 23 |
| Total | 28 | Total | 8 | Total | 26 | Total | 36 |
| Heart failure | Sepsis | Other cardiac causes | Other non-cardiac causes | ||||
| Valvular heart disease Defined cardiomyopathy or adult congenital heart disease Sepsis Other organ dysfunction Thrombosis/bleeding/hematological problem Complete heart block | 20 5 31 11 5 2 | Gastrointestinal disease Skin and limb Pneumonia Device-related Unclear source Urosepsis | 3 3 19 1 23 3 | Adult congenital heart disease Constriction Device-related Other | 2 1 3 5 | Other organ dysfunction Peripheral vascular disease Infection Abdomino-pelvic bleeding or ischemia Cerebral bleed Vascular disease Other | 6 2 3 5 8 1 4 |
| Total | 74 | Total | 52 | Total | 26 | Total | 36 |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2023 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Kwok, C.S.; Tafuro, J.; Wong, C.W.; Bennett, S.; Zachariah, D.; Barker, D.; Morley-Davies, A.; Satchithananda, D.; Gunning, M.; Borovac, J.A. What Are the Causes of Death among Patients Admitted to a Contemporary Tertiary-Level Cardiology Department? An Analysis of 10 Years of Morbidity and Mortality Meetings. Pathophysiology 2023, 30, 467-479. https://doi.org/10.3390/pathophysiology30040034
Kwok CS, Tafuro J, Wong CW, Bennett S, Zachariah D, Barker D, Morley-Davies A, Satchithananda D, Gunning M, Borovac JA. What Are the Causes of Death among Patients Admitted to a Contemporary Tertiary-Level Cardiology Department? An Analysis of 10 Years of Morbidity and Mortality Meetings. Pathophysiology. 2023; 30(4):467-479. https://doi.org/10.3390/pathophysiology30040034
Chicago/Turabian StyleKwok, Chun Shing, Jacopo Tafuro, Chun Wai Wong, Sadie Bennett, Donah Zachariah, Diane Barker, Adrian Morley-Davies, Duwarakan Satchithananda, Mark Gunning, and Josip A. Borovac. 2023. "What Are the Causes of Death among Patients Admitted to a Contemporary Tertiary-Level Cardiology Department? An Analysis of 10 Years of Morbidity and Mortality Meetings" Pathophysiology 30, no. 4: 467-479. https://doi.org/10.3390/pathophysiology30040034
APA StyleKwok, C. S., Tafuro, J., Wong, C. W., Bennett, S., Zachariah, D., Barker, D., Morley-Davies, A., Satchithananda, D., Gunning, M., & Borovac, J. A. (2023). What Are the Causes of Death among Patients Admitted to a Contemporary Tertiary-Level Cardiology Department? An Analysis of 10 Years of Morbidity and Mortality Meetings. Pathophysiology, 30(4), 467-479. https://doi.org/10.3390/pathophysiology30040034






