Hemodynamic, Oxygenation and Lymphocyte Parameters Predict COVID-19 Mortality
Abstract
1. Introduction
2. Materials and Methods
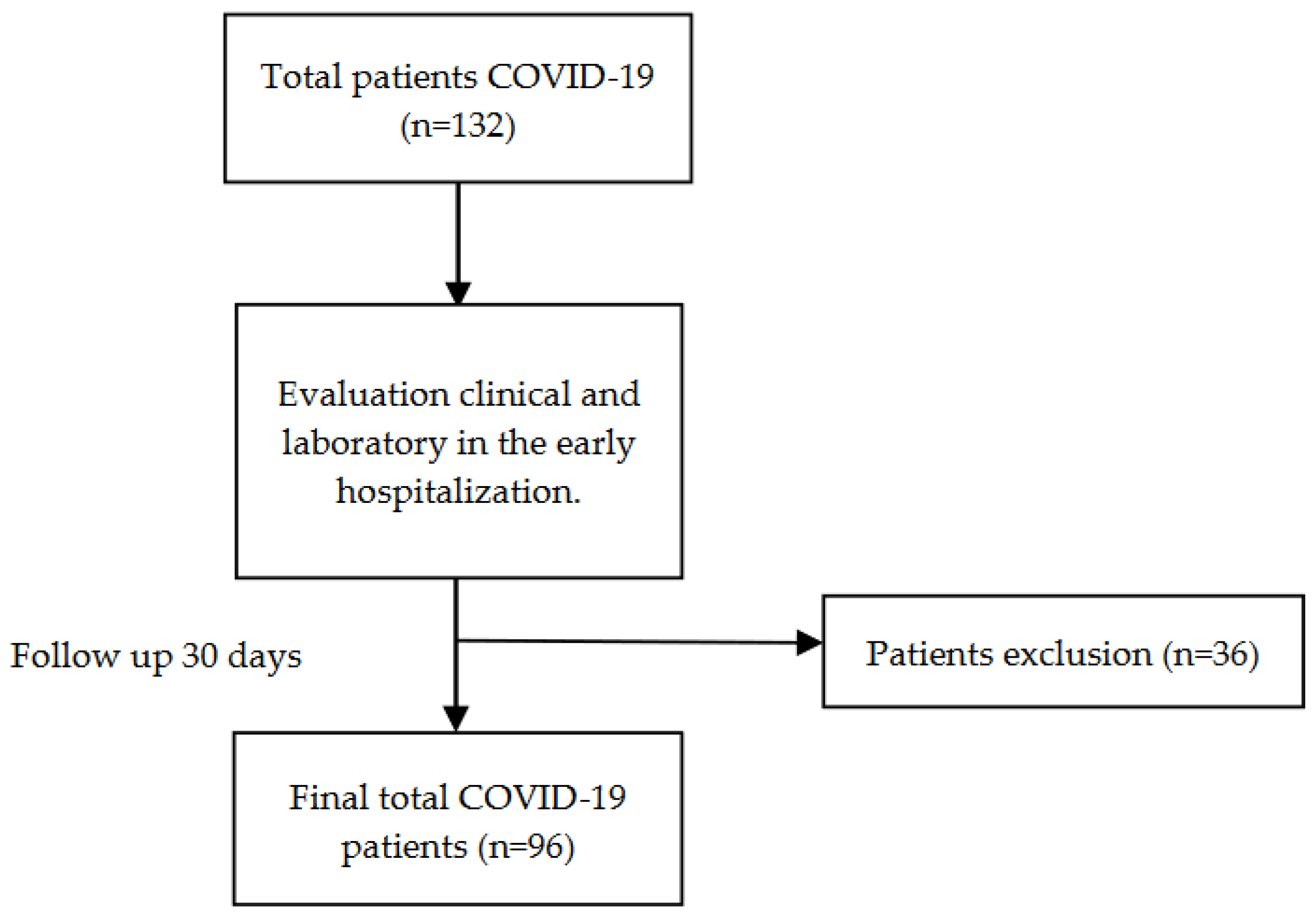
2.1. Study Design, Definition, and Sample Selection
2.2. Statistical Analysis
3. Results
4. Discussion
5. Conclusions
Author Contributions
Funding
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- WHO World Health Organization. Coronavirus Disease (COVID-19) Situation. Available online: https://www.who.int/indonesia/news/novel-coronavirus (accessed on 18 March 2023).
- Zhou, F.; Yu, T.; Du, R.; Fan, G.; Liu, Y.; Liu, Z.; Xiang, J.; Wang, Y.; Song, B.; Gu, X.; et al. Clinical course and risk factors for mortality of adult inpatients with COVID-19 in Wuhan, China: A retrospective cohort study. Lancet 2020, 395, 1054–1062. [Google Scholar] [CrossRef] [PubMed]
- Hall, M.; Pritchard, M.; Dankwa, E.A.; Baillie, J.K.; Carson, G.; Citarella, B.W.; Docherty, A.; Donnelly, C.A.; Dunning, J.; Fraser, C.; et al. International Severe Acute Respiratory and Emerging Infections Consortium; medRxiv: Oxford, UK, 2020. [Google Scholar]
- Bradley, P.; Frost, F.; Tharmaratnam, K.; Wootton, D.G. Utility of established prognostic scores in COVID-19 hospital admissions: Multicentre prospective evaluation of CURB-65, NEWS2 and qSOFA. BMJ Open Respir. Res. 2020, 7, e000729. [Google Scholar] [CrossRef]
- Berenguer, J.; Borobia, A.M.; Ryan, P.; Rodríguez-Baño, J.; Bellón, J.M.; Jarrín, I.; Carratalà, J.; Pachón, J.; Carcas, A.J.; Yllescas, M.; et al. Development and validation of a prediction model for 30-day mortality in hospitalised patients with COVID-19: The COVID-19 SEIMC score. Thorax 2021, 76, 920–929. [Google Scholar] [CrossRef] [PubMed]
- Berry, D.A.; Ip, A.; Lewis, B.E.; Berry, S.M.; Berry, N.S.; MrKulic, M.; Gadalla, V.; Sat, B.; Wright, K.; Serna, M.; et al. Development and validation of a prognostic 40-day mortality risk model among hospitalized patients with COVID-19. PLoS ONE 2021, 16, e0255228. [Google Scholar] [CrossRef] [PubMed]
- Ferrando-Vivas, P.; Doidge, J.; Thomas, K.; Gould, D.W.; Mouncey, P.; Shankar-Hari, M.; Young, J.D.; Rowan, K.M.; Harrison, D.A. Prognostic Factors for 30-Day Mortality in Critically Ill Patients with Coronavirus Disease 2019: An Observational Cohort Study. Crit. Care Med. 2021, 49, 102–111. [Google Scholar] [CrossRef]
- Sehgal, I.S.; Agarwal, R.; Dhooria, S.; Prasad, K.T.; Muthu, V.; Aggarwal, A.N. Risk stratification of acute respiratory distress syndrome using a PaO2: Fio2 threshold of 150 mmHg: A retrospective analysis from an Indian intensive care unit. Lung India 2020, 37, 473–478. [Google Scholar] [CrossRef]
- Gupta, R.K.; Harrison, E.M.; Ho, A.; Docherty, A.B.; Knight, S.R.; van Smeden, M.; Abubakar, I.; Lipman, M.; Quartagno, M.; Pius, R.; et al. Development and validation of the ISARIC 4C Deterioration model for adults hospitalised with COVID-19: A prospective cohort study. Lancet Respir. Med. 2021, 9, 349–359. [Google Scholar] [CrossRef]
- Incerti, D.; Rizzo, S.; Li, X.; Lindsay, L.; Yau, V.; Keebler, D.; Chia, J.; Tsai, L. Prognostic model to identify and quantify risk factors for mortality among hospitalised patients with COVID-19 in the USA. BMJ Open 2021, 11, e047121. [Google Scholar] [CrossRef]
- Jiwa, N.; Mutneja, R.; Henry, L.; Fiscus, G.; Zu Wallack, R. Development of a brief scoring system to predict any-cause mortality in patients hospitalized with COVID-19 infection. PLoS ONE 2021, 16, e0254580. [Google Scholar] [CrossRef]
- Martínez-Lacalzada, M.; Viteri-Noël, A.; Manzano, L.; Fabregate, M.; Rubio-Rivas, M.; Luis García, S.; Arnalich-Fernández, F.; Beato-Pérez, J.L.; Vargas-Núñez, J.A.; Calvo-Manuel, E.; et al. Predicting critical illness on initial diagnosis of COVID-19 based on easily obtained clinical variables: Development and validation of the PRIORITY model. Clin. Microbiol. Infect. Eur. Soc. Clin. Microbiol. Infect. Dis. 2021, 27, 1838–1844. [Google Scholar] [CrossRef]
- Abkhoo, A.; Shaker, E.; Mehrabinejad, M.M.; Azadbakht, J.; Sadighi, N.; Salahshour, F. Factors Predicting Outcome in Intensive Care Unit-Admitted COVID-19 Patients: Using Clinical, Laboratory, and Radiologic Characteristics. Crit. Care Res. Pract. 2021, 2021, 9941570. [Google Scholar] [CrossRef]
- Wang, K.; Zuo, P.; Liu, Y.; Zhang, M.; Zhao, X.; Xie, S.; Zhang, H.; Chen, X.; Liu, C. Clinical and Laboratory Predictors of In-hospital Mortality in Patients With Coronavirus Disease-2019: A Cohort Study in Wuhan, China. Clin. Infect. Dis. Infect. Dis. Soc. Am. 2020, 71, 2079–2088. [Google Scholar] [CrossRef]
- Knight, S.R.; Ho, A.; Pius, R.; Buchan, I.; Carson, G.; Drake, T.M.; Dunning, J.; Fairfield, C.J.; Gamble, C.; Green, C.A.; et al. Risk stratification of patients admitted to hospital with COVID-19 using the ISARIC WHO Clinical Characterisation Protocol: Development and validation of the 4C Mortality Score. BMJ 2020, 370, m3339. [Google Scholar] [CrossRef]
- Yang, L.; Jin, J.; Luo, W.; Gan, Y.; Chen, B.; Li, W. Risk factors for predicting mortality of COVID-19 patients: A systematic review and meta-analysis. PLoS ONE 2020, 15, e0243124. [Google Scholar] [CrossRef] [PubMed]
- Asmarawati, T.P.; Rosyid, A.N.; Suryantoro, S.D.; Mahdi, B.A.; Windradi, C.; Wulaningrum, P.A.; Arifianto, M.V.; Bramantono, B.; Triyono, E.A.; Rusli, M.; et al. The clinical impact of bacterial co-infection among moderate, severe and critically ill COVID-19 patients in the second referral hospital in Surabaya. F1000Research 2021, 10, 113. [Google Scholar] [CrossRef]
- Asmarawati, T.P.; Suryantoro, S.D.; Rosyid, A.N.; Marfiani, E.; Windradi, C.; Mahdi, B.A. Predictive Value of Sequential Organ Failure Assessment (SOFA), Quick Sequential Organ Failure Assessment (qSOFA), Acute Physiology and Chronic Health Evaluation (APACHE II), and New Early Warning Signs (NEWS-2) Scores Estimate Mortality of COVID-19 Patients Requiring Intensive Care Unit (ICU). Indian J. Crit. Care Med. 2022, 26, 464–471. [Google Scholar]
- Burhan, E.; Susanto, A.D.; Sally, A.N.; Eka, G.; Ceva, W.P.; Susilo, A.; Firdaus, I.; Santoso, A.; Juzar, D.A.; Arif, S.K.; et al. Pedoman Tatalaksana COVID-19 Edisi 3 [Internet], 3rd ed.; PDPI, PERKI, PAPDI, PERDATIN, IDAI: Jakarta, Indonesia, 2020; pp. 36–37. Available online: https://www.papdi.or.id/download/983-pedoman-tatalaksana-covid-19-edisi-3-desember-2020 (accessed on 11 May 2023).
- Vincent, J.L.; Nielsen, N.D.; Shapiro, N.I.; Gerbasi, M.E.; Grossman, A.; Doroff, R.; Zeng, F.; Young, P.J.; Russell, J.A. Mean arterial pressure and mortality in patients with distributive shock: A retrospective analysis of the MIMIC-III database. Ann Intensive Care 2018, 8, 107. [Google Scholar] [CrossRef]
- Prediletto, I.; D’Antoni, L.; Carbonara, P.; Daniele, F.; Dongilli, R.; Flore, R.; Pacilli, A.M.G.; Pisani, L.; Tomsa, C.; Vega, M.L.; et al. Standardizing PaO2 for PaCO2 in P/F ratio predicts in-hospital mortality in acute respiratory failure due to COVID-19: A pilot prospective study. Eur. J. Intern. Med. 2021, 92, 48–54. [Google Scholar] [CrossRef] [PubMed]
- Patel, S.; Singh, G.; Zarbiv, S.; Ghiassi, K.; Rachoin, J.S. Mortality Prediction Using SaO(2)/FiO(2) Ratio Based on eICU Database Analysis. Crit. Care Res. Pract. 2021, 2021, 6672603. [Google Scholar] [PubMed]
- Zidar, D.A.; Al-Kindi, S.G.; Liu, Y.; Krieger, N.I.; Perzynski, A.T.; Osnard, M.; Nmai, C.; Anthony, D.D.; Lederman, M.M.; Freeman, M.L.; et al. Association of Lymphopenia with Risk of Mortality among Adults in the US General Population. JAMA Netw. Open 2019, 2, e1916526. [Google Scholar] [CrossRef]
- Garrido, D.; Assioun, J.J.; Keshishyan, A.; Sanchez-Gonzalez, M.A.; Goubran, B. Respiratory Rate Variability as a Prognostic Factor in Hospitalized Patients Transferred to the Intensive Care Unit. Cureus 2018, 10, e2100. [Google Scholar] [CrossRef] [PubMed]
- Vittorio, G.; Anna, D.S.; Francesco, G.; Michele, S.; Daniela, P. National Early Warning Score 2 (NEWS2) better predicts critical Coronavirus Disease 2019 (COVID-19) illness than COVID-GRAM, a multi-centre study. Infection 2021, 2, 3–8. [Google Scholar] [CrossRef]
- Fei, Y. Understanding the association between mean arterial pressure and mortality in young adults. Postgrad. Med. J. 2010, 96, 453–454. [Google Scholar] [CrossRef] [PubMed]
- Bansal, S.; Do, R.K.; Tietjen, P.A. Early Mean Arterial Blood Pressure: A Predictor of Mortality in Critically Ill Patients. Chest 2007, 132, 551A. [Google Scholar] [CrossRef]
- Burstein, B.; Tabi, M.; Barsness, G.W.; Bell, M.R.; Kashani, K.; Jentzer, J.C. Association between mean arterial pressure during the first 24 hours and hospital mortality in patients with cardiogenic shock. Crit. Care 2020, 20, 513. [Google Scholar] [CrossRef]
- Altschul, D.J.; Unda, S.R.; Benton, J.; de la Garza, R.R.; Cezayirli, P.; Mehler, M.; Eskandar, E.N. A novel severity score to predict inpatient mortality in COVID-19 patients. Sci. Rep. 2020, 10, 16726. [Google Scholar] [CrossRef] [PubMed]
- Imanieh, M.H.; Amirzadehfard, F.; Zoghi, S.; Sehatpour, F.; Jafari, P.; Hassanipour, H.; Feili, M.; Mollaie, M.; Bostanian, P.; Mehrabi, S.; et al. A novel scoring system for early assessment of the risk of the COVID-19-associated mortality in hospitalized patients: COVID-19 BURDEN. Eur. J. Med. Res. 2023, 28, 4. [Google Scholar] [CrossRef]
- Hayes, G.M.; Mathews, K.; Boston, S.; Dewey, C.; Medicine, C.C. Low central venous oxygen saturation in critically ill dogs. J. Vet. Emerg. Crit. Care 2011, 52, 154–161. [Google Scholar] [CrossRef]
- Id, J.Q.; Ding, L.; Bao, L.; Id, D.C. The ratio of shock index to pulse oxygen saturation predicting mortality of emergency trauma patients. PLoS ONE 2020, 15, e0236094. [Google Scholar] [CrossRef]
- Du, R.-H.; Liang, L.-R.; Yang, C.-Q.; Wang, W.; Cao, T.-Z.; Li, M.; Guo, G.-Y.; Du, J.; Zheng, C.-L.; Zhu, Q.; et al. Predictors of mortality for patients with COVID-19 pneumonia caused by SARS-CoV-2: A prospective cohort study. Eur. Respir. J. 2020, 55, 2000524. [Google Scholar] [CrossRef]
- Berlin, D.A.; Gulick, R.M.; Martinez, F.J. Severe COVID-19. N. Engl. J. Med. 2020, 383, 2451–2460. [Google Scholar] [CrossRef]
- Nlandu, Y.; Mafuta, D.; Sakaji, J.; Brecknell, M.; Engole, Y.; Abatha, J.; Nkumu, J.-R.; Nkodila, A.; Mboliassa, M.-F.; Tuyinama, O.; et al. Predictors of mortality in COVID-19 patients at Kinshasa Medical Center and a survival analysis: A retrospective cohort study. BMC Infect. Dis. 2021, 21, 1272. [Google Scholar] [CrossRef]
- Kaydu, A.; Akar, N. Relationship between arterial oxygen tension and mortality of patients in intensive care unit on mechanical ventilation support. Ulus Travma Acil Cerrahi Derg. 2019, 25, 331–337. [Google Scholar] [CrossRef]
- Eastwood, G.; Bellomo, R.; Bailey, M.; Taori, G.; Pilcher, D.; Young, P.; Beasley, R. Arterial oxygen tension and mortality in mechanically ventilated patients. Intensive Care Med. 2012, 38, 91–98. [Google Scholar] [CrossRef]
- de Jonge, E.; Peelen, L.; Keijzers, P.J.; Joore, H.; de Lange, D.; van der Voort, P.H.; Bosman, R.J.; de Waal, R.A.; Wesselink, R.; de Keizer, N.F. Association between administered oxygen, arterial partial oxygen pressure and mortality in mechanically ventilated intensive care unit patients. Crit. Care 2008, 12, R156. [Google Scholar] [CrossRef]
- Gu, Y.; Wang, D.; Chen, C.; Lu, W.; Liu, H.; Lv, T. PaO2/FiO2 and IL-6 are risk factors of mortality for intensive care COVID-19 patients. Sci. Rep. 2021, 11, 7334. [Google Scholar] [CrossRef]
- Chen, W.; Janz, D.R.; Shaver, C.M.; Bernard, G.R.; Bastarache, J.A.; Ware, L.B. Clinical Characteristics and Outcomes Are Similar in ARDS Diagnosed by Oxygen Saturation/FiO2 Ratio Compared with PaO2/FiO2 Ratio. Chest 2015, 148, 1477–1483. [Google Scholar] [CrossRef]
- Basheer, M.; Saad, E.; Hagai, R. Clinical Predictors of Mortality and Critical Illness in Patients with COVID-19 Pneumonia. Metabolites 2021, 11, 679. [Google Scholar] [CrossRef]
- Lee, J.; Park, S.; Kim, T.Y.; Lee, D.; Kim, D. Lymphopenia as a Biological Predictor of Outcomes in COVID-19 Patients: A Nationwide Cohort Study. Cancers 2021, 13, 471. [Google Scholar] [CrossRef]
- Satici, C.; Asim, M.; Sargin, E.; Gursoy, B.; Alkan, M.; Kamat, S.; Demirok, B.; Dilsah, C.; Calik, M.; Cavus, Z.; et al. Performance of pneumonia severity index and CURB-65 in predicting 30-day mortality in patients with COVID-19. Int. J. Infect. Dis. 2020, 98, 84–89. [Google Scholar] [CrossRef]

| Demographic Characteristics | n (%) or Mean ± SD |
|---|---|
| Male | 49 (51) |
| Female | 47 (49) |
| Age (years, Mean ± SD) | 52.77 ± 12.28 |
| COVID-19 Severity, n (%) | |
| Non-critical | 23 (24) |
| Critical | 73 (76) |
| Duration of hospitalization (days, Mean ± SD) | 13.72 ± 7.73 |
| Comorbidities, n (%) | |
| DM | 39 (40.6) |
| HT | 32 (33.3) |
| Heart disease | 6 (6.3) |
| Stroke | 2 (2.1) |
| Outcomes, n (%) | |
| Death | 43 (44.8) |
| Survive | 53 (55.2) |
| Vital signs, mean ± SD | |
| Systolic blood pressure (mmHg) | 128.2 ± 27.38 |
| Diastolic blood pressure (mmHg) | 77.52 ± 15.41 |
| MAP (mmHg) | 94.42 ± 18.27 |
| Heart rate (times per minute) | 105.5 ± 18.15 |
| Respiration rate (times per minute) | 25.59 ± 6.2 |
| Temperature (°C) | 36.6 ± 0.6 |
| Oxygen saturation (%) | 94.98 ± 4.94 |
| Laboratory parameter, mean ± SD | |
| Hb (g/dL) | 13.1 ± 2.3 |
| Hct (%) | 38.5 ± 5.35 |
| Leukocyte (103/μL) | 8.88 ± 5.79 |
| Nuetrophill (%) | 78.7 ± 15.3 |
| Lymphocyte (%) | 12.45 ±11.08 |
| Absolute lymphocyte count (/μL) | 1163.8 ± 1498.97 |
| Thrombocyte (103/μL) | 263.5 ± 138.86 |
| NLR | 6.55 ± 10.99 |
| CRP (mg/L) | 20.33 ± 86.11 |
| Procalcitonin (ng/mL) | 2.499 ± 10.83 |
| BUN (mg/dL) | 14.15 ± 26.37 |
| Creatinine serum (mg./dL) | 0.97 ± 2.23 |
| pCO2 level (mmHg) | 32.07 ± 13.39 |
| HCO3 level (mEq/L) | 20.4 ± 5.06 |
| PF ratio | 147.41 ± 92.41 |
| SF ratio | 158.83 ± 84.93 |
| Scoring Category | Death | p-Value † | p-Value ‡ | B | SE | B/SE | (B/SE/Cof) | Score |
|---|---|---|---|---|---|---|---|---|
| MPL | ||||||||
| MAP < 75 mmHg | 15 | 0.012 | 0.039 | 1.19 | 0.58 | 2.06 * | 1.00 | 1 |
| PF Ratio < 200 | 37 | 0.000 | 0.003 | 1.61 | 0.55 | 2.92 | 1.42 | 1 |
| Lymphocyte absolute < 1500 | 34 | 0.001 | 0.011 | 1.30 | 0.51 | 2.56 | 1.24 | 1 |
| MSLR | ||||||||
| MAP < 75 mmHg | 15 | 0.012 | 0.151 | 0.84 | 0.58 | 1.43 * | 1.00 | 1 |
| SF Ratio < 200 | 36 | 0.000 | 0.129 | 0.88 | 0.58 | 1.52 | 1.06 | 1 |
| Lymphocyte absolute < 1500 | 34 | 0.001 | 0.009 | 1.34 | 0.52 | 2.60 | 1.82 | 2 |
| RR ≥ 24/min | 35 | 0.000 | 0.03 | 1.20 | 0.55 | 2.17 | 1.52 | 2 |
| Scoring Category | Point |
|---|---|
| MPL | |
| MAP < 75 mmHg | 1 |
| MAP ≥ 75 mmHg | 0 |
| PF ratio < 200 | 1 |
| PF ratio ≥ 200 | 0 |
| ALC < 1500/μL | 1 |
| ALC ≥ 1500/μL | 0 |
| MSLR | |
| MAP < 75 mmHg | 1 |
| MAP ≥ 75 mmHg | 0 |
| SF ratio < 200 | 1 |
| SF ratio ≥ 200 | 0 |
| ALC < 1500/μL | 2 |
| ALC ≥ 1500/μL | 0 |
| RR ≥ 24/min | 2 |
| RR < 24/min | 0 |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2023 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Windradi, C.; Asmarawati, T.P.; Rosyid, A.N.; Marfiani, E.; Mahdi, B.A.; Martani, O.S.; Giarena, G.; Agustin, E.D.; Rosandy, M.G. Hemodynamic, Oxygenation and Lymphocyte Parameters Predict COVID-19 Mortality. Pathophysiology 2023, 30, 314-326. https://doi.org/10.3390/pathophysiology30030025
Windradi C, Asmarawati TP, Rosyid AN, Marfiani E, Mahdi BA, Martani OS, Giarena G, Agustin ED, Rosandy MG. Hemodynamic, Oxygenation and Lymphocyte Parameters Predict COVID-19 Mortality. Pathophysiology. 2023; 30(3):314-326. https://doi.org/10.3390/pathophysiology30030025
Chicago/Turabian StyleWindradi, Choirina, Tri Pudy Asmarawati, Alfian Nur Rosyid, Erika Marfiani, Bagus Aulia Mahdi, Okla Sekar Martani, Giarena Giarena, Esthiningrum Dewi Agustin, and Milanitalia Gadys Rosandy. 2023. "Hemodynamic, Oxygenation and Lymphocyte Parameters Predict COVID-19 Mortality" Pathophysiology 30, no. 3: 314-326. https://doi.org/10.3390/pathophysiology30030025
APA StyleWindradi, C., Asmarawati, T. P., Rosyid, A. N., Marfiani, E., Mahdi, B. A., Martani, O. S., Giarena, G., Agustin, E. D., & Rosandy, M. G. (2023). Hemodynamic, Oxygenation and Lymphocyte Parameters Predict COVID-19 Mortality. Pathophysiology, 30(3), 314-326. https://doi.org/10.3390/pathophysiology30030025






