Psychological Determinants of Men’s Adherence to Cascade Screening for BRCA1/2
Abstract
1. Introduction
- Higher risk perceptions and outcome expectancies would predict higher intention to undergo genetic test for BRCA germline mutations after three weeks, controlling for socio-demographics and coping self-efficacy (hypothesis 1a–HP1a). Moreover, higher intention and coping self-efficacy would predict higher planning after three weeks, controlling for socio-demographics and the other psychological variables (hypothesis 1b–HP1b).
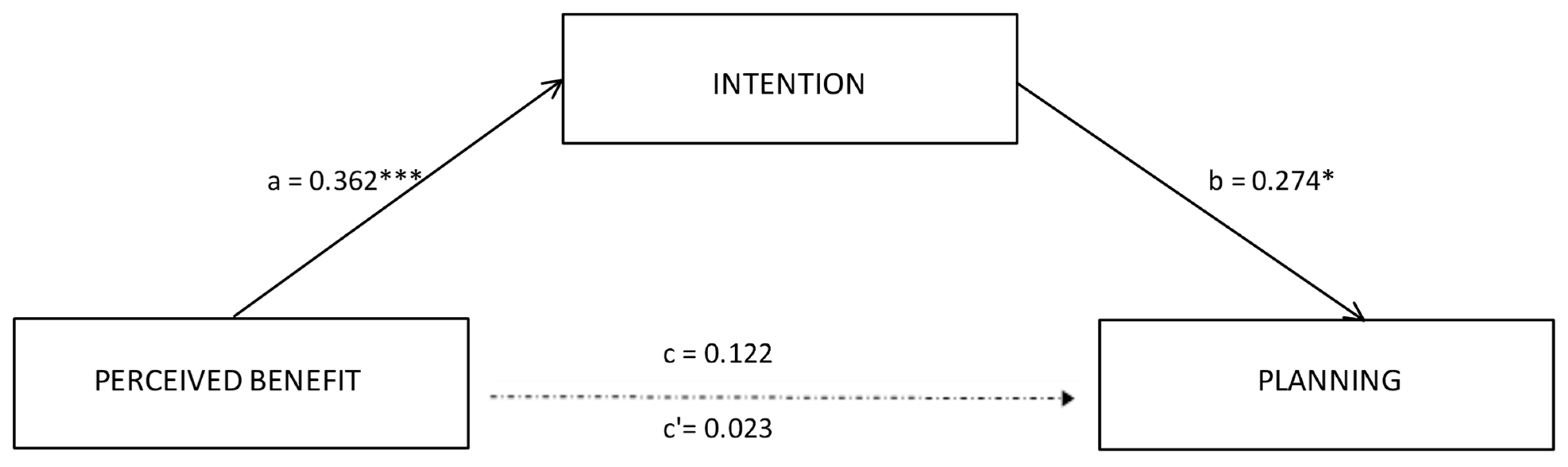
- Intention would serve as a mediator in the relationships between risk perceptions or outcome expectancies, and planning (hypothesis 2–HP2).
2. Materials and Methods
2.1. Procedure
2.2. Participants
2.3. Measures
2.3.1. T1
- Socio-demographic characteristics. Self-reported age, education, employment, parental status (0 = without children; 1 = with children), and degree of kinship with the proband with BRCA1/2 germline mutation were assessed.
- Health Status. Self-reported general health and existing diagnosis for chronic disease were investigated with a single item each [39,40]. Response options for general health conditions were on a 5-point Likert scale, ranging from “very poor health conditions” to “very good health conditions”. Response option for chronic disease item was dichotomous (no–yes, specify).
- Risk perceptions. Relative risk perception regarding the possibility to develop breast, prostatic, and pancreatic cancer was investigated with one item each [41,42], on a 7-point Likert scale ranging from “far below the average” to “far above the average”. An example item is: “Compared to people like you by age and gender, your chances of having breast cancer in the future are…”.
- Outcome Expectancies. The outcome expectancies were assessed through the use of three different measures.
- (a)
- Self-referred Outcome Expectancies. Four items on a 5-point Likert scale from “unlikely” to “likely” were created ad hoc to evaluate participant self-referred positive outcome expectancies related to genetic testing (e.g., “The genetic test for BRCA1/2 would increase my sense of safety about my health”). A total score had been calculated as a mean of the scores assigned to each item, with higher scores indicating higher self-referred outcome expectancies. The scale revealed a Cronbach’s alpha coefficient equal to 0.735 (rs > 0.488).
- (b)
- Family-referred Outcome Expectancies. Four items on a 5-point Likert scale from “unlikely” to “likely” were created ad hoc to evaluate participant family-referred positive outcome expectancies related to genetic testing (e.g., “My family members will have important information for their health if I undergo a BRCA1/2 genetic test”). Total scoring is the mean of the points assigned to each item, with higher scores indicating higher family-referred outcome expectancies. The scale has been shown to be internally consistent (α = 0.862; rs > 0.689).
- (c)
- Perceived Benefit. Five-digit semantic differential questions asked where the respondent’s position was on a scale between two bipolar adjectives, with the aim to measure the perceived benefit for the genetic testing. As previously performed in other research [43], the scale was composed of 10 bipolar adjectives with higher scores indicating higher perceived genetic testing benefit. Examples of the proposed adjectives are “not important/important”, “irrelevant/relevant”, “useless/useful”, “unnecessary/necessary”. In this study, this scale has been shown to be internally consistent (α = 0.914, rs > 0.253).
2.3.2. T2
- Intention. The intention to undergo genetic testing was measured through three items on a 5-point Likert scale from “very improbable” to “very probable”, evaluating the urge to engage the behavior [44]. Example of item is: “In the next 6 months, how likely is it that you will undergo BRCA1/2 genetic testing?”. An overall score of intention had been calculated as a mean of the scores assigned to each item with higher scores indicating higher intention. The internal consistency of the scale was moderate (α = 0.694, rs > 0.408).
- Coping Self-efficacy. Three ad hoc items on a 5-point Likert scale, from “not very capable” to “totally capable”, were created to evaluate whether the individual feels to be capable of tackling the possible obstacles and difficulties that could make it difficult to undergo a genetic screening [45]. Total scoring is the mean of the points assigned to each item, with higher scores indicating higher coping self-efficacy. An example item is: “How do you feel you’re capable of tackling the obstacles and difficulties that could make it difficult for you to undergo genetic screening?”. In the present study, the scale revealed acceptable internal consistency (α = 0.773, rs > 0.525).
- Planning. Six ad hoc items were created to assess if participants planned the action to undergo BRCA1/2 genetic testing (action planning—3 items), and if they developed one or more plans to cope with such a challenging situation that they think to encounter in planning the action (coping planning—3 items) [45]. Response options were on a 5-point Likert scale, ranging from “not true at all” to “very true” for the action planning dimension, and from “very improbable” to “very probable” for the coping planning dimension. An example item is: “I made plans about when to do a genetic screening for the BRCA1/BRCA2 mutation (e.g., taking work permits)”. The total score had been calculated as a mean of the scores assigned to each item, with higher scores indicating higher planning. In this study, this scale has been shown to be internally consistent (α = 0.652; rs > 0.168).
2.4. Data Analysis Plan
3. Results
3.1. Preliminary Results
3.2. Regression Analysis
3.3. Mediational Analysis
3.4. Breast Cancer Risk Perception
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Kuchenbaecker, K.B.; Hopper, J.L.; Barnes, D.R.; Phillips, K.A.; Mooij, T.M.; Roos-Blom, M.J.; Jervis, S.; Van Leeuwen, F.E.; Milne, R.L.; Andrieu, N.; et al. Risks of breast, ovarian, and contralateral breast cancer for BRCA1 and BRCA2 mutation carriers. JAMA -J. Am. Med. Assoc. 2017, 317, 2402–2416. [Google Scholar] [CrossRef] [PubMed]
- Corso, G.; Feroce, I.; Intra, M.; Toesca, A.; Magnoni, F.; Sargenti, M.; Naninato, P.; Caldarella, P.; Pagani, G.; Vento, A.; et al. BRCA1/2 germline missense mutations: A systematic review. Eur. J. Cancer Prev. 2018, 27, 279–286. [Google Scholar] [CrossRef] [PubMed]
- Nyberg, T.; Frost, D.; Barrowdale, D.; Evans, D.G.; Bancroft, E.; Adlard, J.; Ahmed, M.; Barwell, J.; Brady, A.F.; Brewer, C.; et al. Prostate Cancer Risks for Male BRCA1 and BRCA2 Mutation Carriers: A Prospective Cohort Study. Eur. Urol. 2020, 77, 24–35. [Google Scholar] [CrossRef] [PubMed]
- Tai, Y.C.; Domchek, S.; Parmigiani, G.; Chen, S. Breast Cancer Risk Among Male BRCA1 and BRCA2 Mutation Carriers. J. Natl. Cancer Inst. 2007, 99, 1811. [Google Scholar] [CrossRef] [PubMed]
- Mahon, S.M. Cancer risks for men with BRCA1/2 mutations. Oncol. Nurs. Forum 2014, 41, 99–101. [Google Scholar] [CrossRef] [PubMed]
- Daly, M.B.; Pal, T.; Berry, M.P.; Buys, S.S.; Dickson, P.; Domchek, S.M.; Elkhanany, A.; Friedman, S.; Goggins, M.; Hutton, M.L.; et al. Genetic/Familial High-Risk Assessment: Breast, Ovarian, and Pancreatic, Version 2.2021, NCCN Clinical Practice Guidelines in Oncology. J. Natl. Compr. Canc. Netw. 2021, 19, 77–102. [Google Scholar] [CrossRef]
- Petrucelli, N.; Daly, M.B.; Pal, T. BRCA1- and BRCA2-Associated Hereditary Breast and Ovarian Cancer; University of Washington: Seattle, WA, USA, 1993. [Google Scholar]
- Shiloh, S.; Dagan, E.; Friedman, I.; Blank, N.; Friedman, E. A follow-up study on men tested for BRCA1/BRCA2 mutations: Impacts and coping processes. Psychooncology 2013, 22, 417–425. [Google Scholar] [CrossRef]
- d’Agincourt-Canning, L.; Baird, P. Genetic testing for hereditary cancers: The impact of gender on interest, uptake and ethical considerations. Crit. Rev. Oncol. Hematol. 2006, 58, 114–123. [Google Scholar] [CrossRef]
- Juan, A.S.; Wakefield, C.; Kasparian, N.A.; Kirk, J.; Tyler, J.; Tucker, K. Development and pilot testing of a decision aid for men considering genetic testing for breast and/or ovarian cancer-related mutations (BRCA1/2). Genet. Test. 2008, 12, 523–532. [Google Scholar] [CrossRef]
- Hesse-Biber, S.; An, C. Within-Gender Differences in Medical Decision Making Among Male Carriers of the BRCA Genetic Mutation for Hereditary Breast Cancer. Am. J. Mens. Health 2017, 11, 1444–1459. [Google Scholar] [CrossRef]
- Graves, K.D.; Gatammah, R.; Peshkin, B.N.; Krieger, A.; Gell, C.; Valdimarsdottir, H.B.; Schwartz, M.D. BRCA1/2 genetic testing uptake and psychosocial outcomes in men. Fam. Cancer 2011, 10, 213–223. [Google Scholar] [CrossRef] [PubMed]
- da Silva, T.L. Male breast cancer: Medical and psychological management in comparison to female breast cancer. A review. Cancer Treat. Commun. 2016, 7, 23–34. [Google Scholar] [CrossRef]
- Caswell-Jin, J.L.; Zimmer, A.D.; Stedden, W.; Kingham, K.E.; Zhou, A.Y.; Kurian, A.W. Cascade Genetic Testing of Relatives for Hereditary Cancer Risk: Results of an Online Initiative. JNCI J. Natl. Cancer Inst. 2019, 111, 95–98. [Google Scholar] [CrossRef] [PubMed]
- Daly, M.B. The impact of social roles on the experience of men in BRCA1/2 families: Implications for counseling. J. Genet. Couns. 2009, 18, 42–48. [Google Scholar] [CrossRef]
- Finlay, E.; Stopfer, J.E.; Burlingame, E.; Evans, K.G.; Nathanson, K.L.; Weber, B.L.; Armstrong, K.; Rebbeck, T.R.; Domchek, S.M. Factors Determining Dissemination of Results and Uptake of Genetic Testing in Families with Known BRCA1/2 Mutations. Genet. Test. 2008, 12, 81–91. [Google Scholar] [CrossRef]
- Marabelli, M.; Calvello, M.; Bonanni, B. Test more men for BRCA genes. Nature 2019, 573, 346. [Google Scholar] [CrossRef]
- Roberts, M.C.; Taber, J.M.; Klein, W.M. Engagement with Genetic Information and Uptake of Genetic Testing: The Role of Trust and Personal Cancer History. J. Cancer Educ. 2018, 33, 893–900. [Google Scholar] [CrossRef]
- Daly, P.; Nolan, C.; Green, A.; Ormiston, W.; Cody, N.; McDevitt, T.; O’hIei, B.; Byrne, D.; McDermott, E.; Carney, D.N.; et al. Predictive testing for BRCA1 and 2 mutations: A male contribution. Ann. Oncol. 2003, 14, 549–553. [Google Scholar] [CrossRef]
- McAllister, M.F.; Evans, D.G.R.; Ormiston, W.; Daly, P. Men in breast cancer families: A preliminary qualitative study of awareness and experience. J. Med. Genet. 1998, 35, 739–744. [Google Scholar] [CrossRef]
- Strømsvik, N.; Råheim, M.; Gjengedal, E. Cancer worry among Norwegian male BRCA1/2 mutation carriers. Fam. Cancer 2011, 10, 597–603. [Google Scholar] [CrossRef][Green Version]
- Lodder, L.; Frets, P.G.; Trijsburg, R.W.; Tibben, A.; Meijers-Heijboer, E.J.; Duivenvoorden, H.J.; Wagner, A.; Van Der Meer, C.A.; Devilee, P.; Cornelisse, C.J.; et al. Men at risk of being a mutation carrier for hereditary breast/ovarian cancer: An exploration of attitudes and psychological functioning during genetic testing. Eur. J. Hum. Genet. 2001, 9, 492–500. [Google Scholar] [CrossRef] [PubMed]
- Hallowell, N.; Ardern-Jones, A.; Eeles, R.; Foster, C.; Lucassen, A.; Moynihan, C.; Watson, M. Men’s Decision-Making About Predictive BRCA1/2 Testing: The Role of Family. J. Genet. Couns. 2005, 14, 207–217. [Google Scholar] [CrossRef] [PubMed]
- Strømsvik, N.; Råheim, M.; Yen, N.; Gjengedal, E. Men in the women’s world of hereditary breast and ovarian cancer-a systematic review. Fam. Cancer 2009, 8, 221–229. [Google Scholar] [CrossRef] [PubMed]
- Rauscher, E.A.; Dean, M.; Campbell-Salome, G.; Barbour, J.B. “How do we rally around the one who was positive?” Familial uncertainty management in the context of men managing BRCA-related cancer risks. Soc. Sci. Med. 2019, 242, 112592. [Google Scholar] [CrossRef]
- Schwarzer, R.; Luszczynska, A. The Health Action Process Approach. Eur. Psychol. 2008, 13, 141–151. [Google Scholar] [CrossRef]
- van Hooft, E.A.J.; Born, M.P.; Taris, T.W.; van der Flier, H.; Blonk, R.W.B. Bridging the gap between intentions and behavior: Implementation intentions, action control, and procrastination. J. Vocat. Behav. 2005, 66, 238–256. [Google Scholar] [CrossRef]
- Sheeran, P.; Webb, T.L. The Intention–Behavior Gap. Soc. Personal. Psychol. Compass 2016, 10, 503–518. [Google Scholar] [CrossRef]
- Oliveri, S.; Cincidda, C.; Ongaro, G.; Cutica, I.; Gorini, A.; Spinella, F.; Fiorentino, F.; Baldi, M.; Pravettoni, G. What people really change after genetic testing (GT) performed in private labs: Results from an Italian study. Eur. J. Hum. Genet. 2022, 30, 62–72. [Google Scholar] [CrossRef]
- Scholz, U.; Nagy, G.; Göhner, W.; Luszczynska, A.; Kliegel, M. Changes in self-regulatory cognitions as predictors of changes in smoking and nutrition behaviour. Psychol. Health 2009, 24, 545–561. [Google Scholar] [CrossRef]
- Parschau, L.; Barz, M.; Richert, J.; Knoll, N.; Lippke, S.; Schwarzer, R. Physical activity among adults with obesity: Testing the health action process approach. Rehabil. Psychol. 2014, 59, 42–49. [Google Scholar] [CrossRef]
- Zhang, C.Q.; Zhang, R.; Schwarzer, R.; Hagger, M.S. A Meta-Analysis of the Health Action Process Approach. Health Psychol. 2019, 38, 623. [Google Scholar] [CrossRef] [PubMed]
- Hattar, A.; Pal, S.; Hagger, M.S. Predicting Physical Activity-Related Outcomes in Overweight and Obese Adults: A Health Action Process Approach. Appl. Psychol. Health Well. Being. 2016, 8, 127–151. [Google Scholar] [CrossRef] [PubMed]
- Daniel, A.O.; Omorogieva Enoma, I.; Omobude-Idiado, S.N. Application of Protection Motivation Theory (PMT) and Health Action Process Approach (HAPA) in promoting women’s adaptive engagement towards breast self examination. Acad. Res. Int. 2014, 5, 291. [Google Scholar]
- Annoni, A.M.; Longhini, C. Investigating men’s motivations to engage in genetic screening for BRCA1 and BRCA2 mutations. PLoS ONE 2022, 17, e0265387. [Google Scholar] [CrossRef] [PubMed]
- Petrocchi, S.; Ongaro, G.; Calvello, M.; Feroce, I.; Bonanni, B.; Pravettoni, G.; Pravettoni, G. A randomized controlled trial comparing self-referred message to family-referred message promoting men’s adherence to evidence based guidelines on BRCA1/2 germline genetic testing: A registered study protocol. PLoS ONE 2022. [Google Scholar] [CrossRef]
- Faul, F.; Erdfelder, E.; Lang, A.G.; Buchner, A. G*Power 3: A flexible statistical power analysis program for the social, behavioral, and biomedical sciences. Behav. Res. Methods 2007, 39, 175–191. [Google Scholar] [CrossRef]
- Luszczynska, A.; Schwarzer, R.; Lippke, S.; Mazurkiewicz, M. Self-efficacy as a moderator of the planning-behaviour relationship in interventions designed to promote physical activity. Psychol. Health 2011, 26, 151–166. [Google Scholar] [CrossRef]
- Shim, M.; Kelly, B.; Hornik, R. Cancer information scanning and seeking behavior is associated with knowledge, lifestyle choices, and screening. J. Health Commun. 2006, 11, 157–172. [Google Scholar] [CrossRef]
- Mauri, A.; Tomas, M.; Ongaro, G.; Riccato, O. Perceived well-being and mindfulness practices in hospital patients. Psicol. Della Salut. 2018, 1, 146–159. [Google Scholar] [CrossRef]
- Renner, B. Hindsight bias after receiving self-relevant health risk information: A motivational perspective. Memory 2003, 11, 455–472. [Google Scholar] [CrossRef]
- Renner, B. Biased Reasoning: Adaptive Responses to Health Risk Feedback. Personal. Soc. Psychol. Bull. 2004, 30, 384–396. [Google Scholar] [CrossRef] [PubMed]
- Petrocchi, S.; Ludolph, R.; Labrie, N.H.M.; Schulz, P. Application of the theory of regulatory fit to promote adherence to evidence-based breast cancer screening recommendations: Experimental versus longitudinal evidence. BMJ Open 2020, 10, e037748. [Google Scholar] [CrossRef] [PubMed]
- Kim, H.K.; Lee, T.K. Conditional Effects of Gain–Loss-Framed Narratives among Current Smokers at Different Stages of Change. J. Health Commun. 2017, 22, 990–998. [Google Scholar] [CrossRef] [PubMed]
- Schwarzer, R. Modeling health behavior change: How to predict and modify the adoption and maintenance of health behaviors. Appl. Psychol. 2008, 57, 1–29. [Google Scholar] [CrossRef]
- Hallowell, N.; Arden-Jones, A.; Eeles, R.; Foster, C.; Lucassen, A.; Moynihan, C.; Watson, M. Guilt, blame and responsibility: Men’s understanding of their role in the transmission of BRCA1/2 mutations within their family. Sociol. Health Illn. 2006, 28, 969–988. [Google Scholar] [CrossRef] [PubMed]
- Ongaro, G.; Brivio, E.; Cincidda, C.; Oliveri, S.; Spinella, F.; Steinberger, D.; Cutica, I.; Gorini, A.; Pravettoni, G. Genetic testing users in Italy and Germany: Health orientation, health-related habits, and psychological profile. Mol. Genet. Genom. Med. 2022, 10, e1851. [Google Scholar] [CrossRef]
- Henneman, L.; Vermeulen, E.; Van El, C.G.; Claassen, L.; Timmermans, D.R.M.; Cornel, M.C. Public attitudes towards genetic testing revisited: Comparing opinions between 2002 and 2010. Eur. J. Hum. Genet. 2012, 21, 793–799. [Google Scholar] [CrossRef]
- Cherkas, L.F.; Harris, J.M.; Levinson, E.; Spector, T.D.; Prainsack, B. A survey of UK public interest in internet-based personal genome testing. PLoS ONE 2010, 5, e13473. [Google Scholar] [CrossRef]
- Liede, A.; Metcalfe, K.; Hanna, D.; Hoodfar, E.; Snyder, C.; Durham, C.; Lynch, H.T.; Narod, S.A. Evaluation of the Needs of Male Carriers of Mutations in BRCA1 or BRCA2 Who Have Undergone Genetic Counseling. Am. J. Hum. Genet. 2000, 67, 1494–1504. [Google Scholar] [CrossRef]
- Shiloh, S.; Drori, E.; Orr-Urtreger, A.; Friedman, E. Being “at-risk” for developing cancer: Cognitive representations and psychological outcomes. J. Behav. Med. 2009, 32, 197–208. [Google Scholar] [CrossRef]
- Bjorvatn, C.; Eide, G.E.; Hanestad, B.R.; Øyen, N.; Havik, O.E.; Carlsson, A.; Berglund, G. Risk perception, worry and satisfaction related to genetic counseling for hereditary cancer. J. Genet. Couns. 2007, 16, 211–222. [Google Scholar] [CrossRef] [PubMed]
- Rantala, J.; Platten, U.; Lindgren, G.; Nilsson, B.; Arver, B.; Lindblom, A.; Brandberg, Y. Risk perception after genetic counseling in patients with increased risk of cancer. Hered. Cancer Clin. Pract. 2009, 7, 15. [Google Scholar] [CrossRef] [PubMed]
- Kim, S.E.; Pérez-Stable, E.J.; Wong, S.; Gregorich, S.; Sawaya, G.F.; Walsh, J.M.E.; Kaplan, C.P. Association Between Cancer Risk Perception and Screening Behavior Among Diverse Women. Arch. Intern. Med. 2008, 7, 728–734. [Google Scholar] [CrossRef] [PubMed]
- Oliveri, S.; Ongaro, G.; Durosini, I.; Curigliano, G.; Pravettoni, G. Breast implant-associated anaplastic large cell lymphoma: Emotional impact and guidelines for psychological support. Breast Cancer Res. Treat. 2020, 181, 221–224. [Google Scholar] [CrossRef] [PubMed]
- Young, A.L.; Butow, P.N.; Vetsch, J.; Quinn, V.F.; Patenaude, A.F.; Tucker, K.M.; Wakefield, C.E. Family Communication, Risk Perception and Cancer Knowledge of Young Adults from BRCA1/2 Families: A Systematic Review. J. Genet. Couns. 2017, 26, 1179–1196. [Google Scholar] [CrossRef] [PubMed]
- Bradbury, A.R.; Patrick-Miller, L.; Pawlowski, K.; Ibe, C.N.; Cummings, S.A.; Hlubocky, F.; Olopade, O.I.; Daugherty, C.K. Learning of your parent’s BRCA mutation during adolescence or early adulthood: A study of offspring experiences. Psychooncology 2009, 18, 200–208. [Google Scholar] [CrossRef]
- Oliveri, S.; Scotto, L.; Ongaro, G.; Triberti, S.; Guiddi, P.; Pravettoni, G. “You do not get cancer by chance”: Communicating the role of environmental causes in cancer diseases and the risk of a “guilt rhetoric. ” Psychooncology 2019, 28, 2422. [Google Scholar] [CrossRef]
- Hopwood, P. Breast cancer risk perception: What do we know and understand? Breast Cancer Res. 2000, 2, 387. [Google Scholar] [CrossRef]
- Schulz, P.J.; Pessina, A.; Hartung, U.; Petrocchi, S. Effects of Objective and Subjective Health Literacy on Patients’ Accurate Judgment of Health Information and Decision-Making Ability: Survey Study. J. Med. Internet Res. 2021, 23, e20457. [Google Scholar] [CrossRef]
- Oliveri, S.; Pravettoni, G.; Fioretti, C.; Hansson, M.G. Let the Individuals Directly Concerned Decide: A Solution to Tragic Choices in Genetic Risk Information. Public Health Genom. 2016, 19, 307–313. [Google Scholar] [CrossRef]
| Variables | M (SD) | 1 | 2 | 3 | 4 | 5 | 6 | 7 | 8 | 9 | 10 | 11 |
|---|---|---|---|---|---|---|---|---|---|---|---|---|
| 1. Age | 41.93 (17.28) | − | 0.717 ** | −0.220 * | 0.216 * | −0.043 | 0.002 | 0.231 * | 0.171 | −0.237 * | −0.006 | −0.082 |
| 2. Parental Status ^ | - | - | −0.235 * | 0.137 | 0.034 | 0.074 | 0.246 ** | 0.144 | −0.223 * | −0.039 | −0.076 | |
| 3. Breast Cancer Risk Perception | 3.07 (1.59) | - | 0.413 ** | 0.519 ** | −0.044 | −0.070 | 0.020 | 0.227 * | 0.149 | 0.129 | ||
| 4. Prostate Cancer Risk Perception | 3.88 (1.11) | - | 0.680 ** | 0.155 | 0.164 | 0.095 | −0.072 | −0.024 | 0.003 | |||
| 5. Pancreatic Cancer Risk Perception | 3.52 (1.20) | - | 0.138 | 0.056 | 0.090 | 0.037 | −.016 | 0.189 | ||||
| 6. Self-referred Outcome Expectancies | 4.11 (0.72) | - | 0.573 ** | 0.521 ** | 0.237 * | 0.104 | 0.065 | |||||
| 7. Family-referred Outcome Expectancies | 4.17 (0.84) | - | 0.377 ** | 0.052 | 0.126 | −0.003 | ||||||
| 8. Perceived Benefit | 4.05 (0.84) | - | 0.320 ** | 0.173 | 0.199 | |||||||
| 9. Intention | 3.34 (0.87) | - | 0.370 ** | 0.272 ** | ||||||||
| 10. Planning | 3.07 (0.57) | - | 0.406 ** | |||||||||
| 11. Coping Self-Efficacy | 3.56 (0.74) | - |
| Dependent Variables | ||||||
|---|---|---|---|---|---|---|
| Intention | Planning | |||||
| β | p | β | p | |||
| Step 1: Sociodemographic | ||||||
| Age | −0.231 | 0.102 | −0.009 | 0.949 | ||
| Parental Status | −0.102 | 0.468 | −0.041 | 0.789 | ||
| = 4.51 *; R2 = 9.6% | = 0.09; R2 = 0.2% | |||||
| Step 2: Psychological variables | ||||||
| Age | −0.243 | 0.071 | 0.022 | 0.881 | ||
| Parental Status | −0.088 | 0.500 | −0.025 | 0.860 | ||
| Breast Cancer Risk Perception | 0.127 | 0.205 | 0.103 | 0.342 | ||
| Self-referred Outcome Expectancies | 0.116 | 0.297 | 0.059 | 0.620 | ||
| Perceived Benefit | 0.305 | 0.008 ** | 0.094 | 0.446 | ||
| Coping Self-Efficacy | 0.126 | 0.198 | 0.334 | 0.002 ** | ||
| = 5.35 ***; R2 = 28.4% | = 2.585 *; R2 = 16.1% | |||||
| Step 3 Intention | ||||||
| Age | - | - | 0.085 | 0.555 | ||
| Parental Status | - | - | −0.002 | 0.989 | ||
| Breast Cancer Risk Perception | - | - | 0.070 | 0.513 | ||
| Self-referred Outcome Expectancies | - | - | 0.029 | 0.804 | ||
| Perceived Benefit | - | - | 0.014 | 0.911 | ||
| Coping Self-Efficacy | - | - | 0.301 | 0.005 ** | ||
| Intention | - | - | 0.261 | 0.029 * | ||
| = 3.03 **; R2 = 21% | ||||||
| Independent Variable: Perceived Benefit Mediator: Intention | |||
|---|---|---|---|
| Dependent Variable | Direct Effect | Indirect Effect | Total Effect |
| Planning | β = 0.02 | β = 0.10 | β = 0.12 |
| SE = 0.07 | SE = 0.06 | SE = 0.07 | |
| [95% CI] = −0.137, 0.169 | [95% CI] = 0.009, 0.229 | [95% CI] = −0.061, 0.231 | |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Ongaro, G.; Petrocchi, S.; Calvello, M.; Bonanni, B.; Feroce, I.; Pravettoni, G. Psychological Determinants of Men’s Adherence to Cascade Screening for BRCA1/2. Curr. Oncol. 2022, 29, 2490-2503. https://doi.org/10.3390/curroncol29040203
Ongaro G, Petrocchi S, Calvello M, Bonanni B, Feroce I, Pravettoni G. Psychological Determinants of Men’s Adherence to Cascade Screening for BRCA1/2. Current Oncology. 2022; 29(4):2490-2503. https://doi.org/10.3390/curroncol29040203
Chicago/Turabian StyleOngaro, Giulia, Serena Petrocchi, Mariarosaria Calvello, Bernardo Bonanni, Irene Feroce, and Gabriella Pravettoni. 2022. "Psychological Determinants of Men’s Adherence to Cascade Screening for BRCA1/2" Current Oncology 29, no. 4: 2490-2503. https://doi.org/10.3390/curroncol29040203
APA StyleOngaro, G., Petrocchi, S., Calvello, M., Bonanni, B., Feroce, I., & Pravettoni, G. (2022). Psychological Determinants of Men’s Adherence to Cascade Screening for BRCA1/2. Current Oncology, 29(4), 2490-2503. https://doi.org/10.3390/curroncol29040203







