Management of Pyrexia Associated with the Combination of Dabrafenib and Trametinib: Canadian Consensus Statements
Abstract
:1. Introduction
2. Materials and Methods
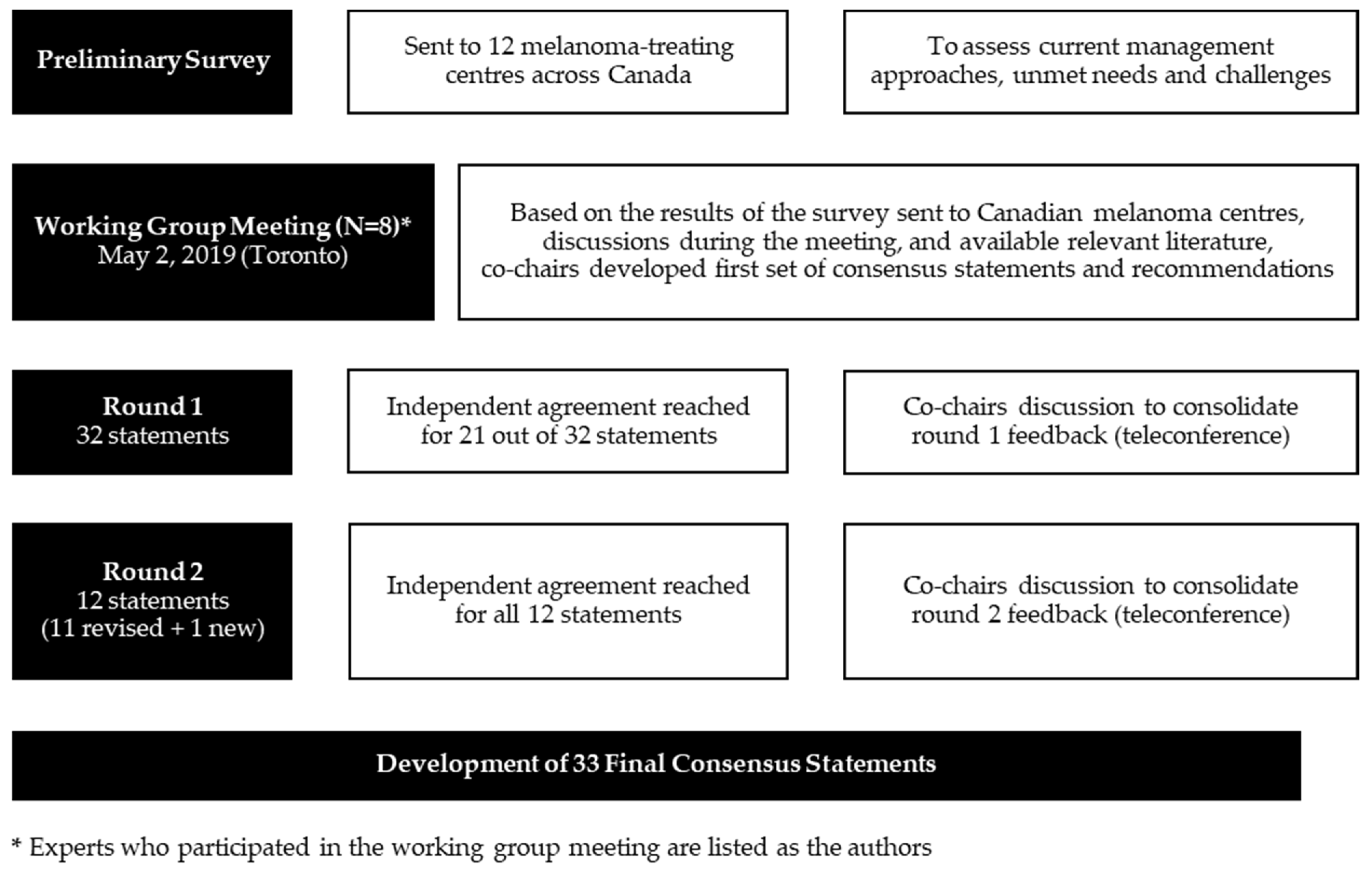
2.1. Preliminary Survey
2.2. Literature Review
2.3. Panel Members
2.4. Consensus Process
3. Results
3.1. Consensus Statements: Definitions
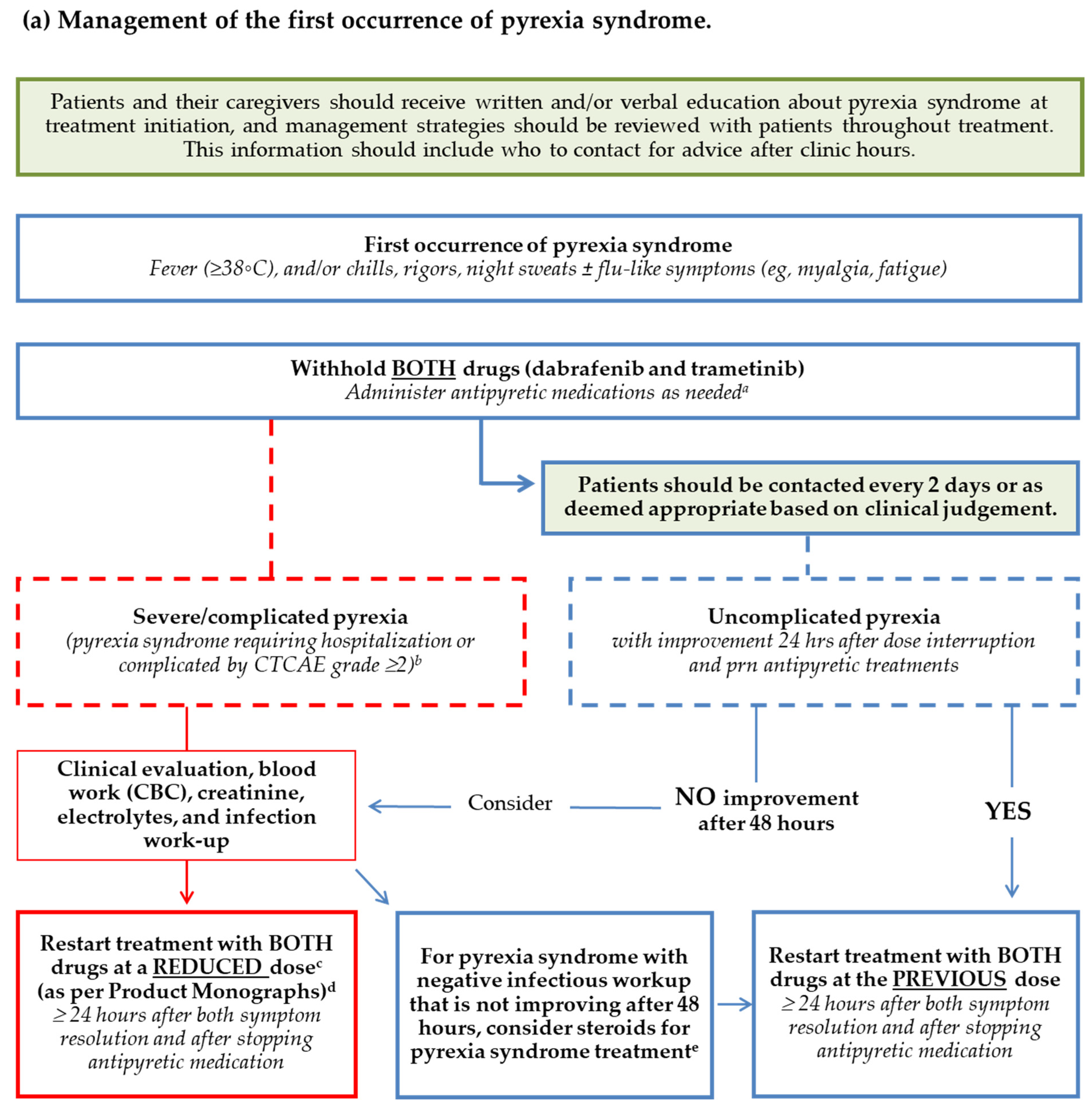
3.2. Consensus Statements: Management of the First Occurrence of Pyrexia Syndrome
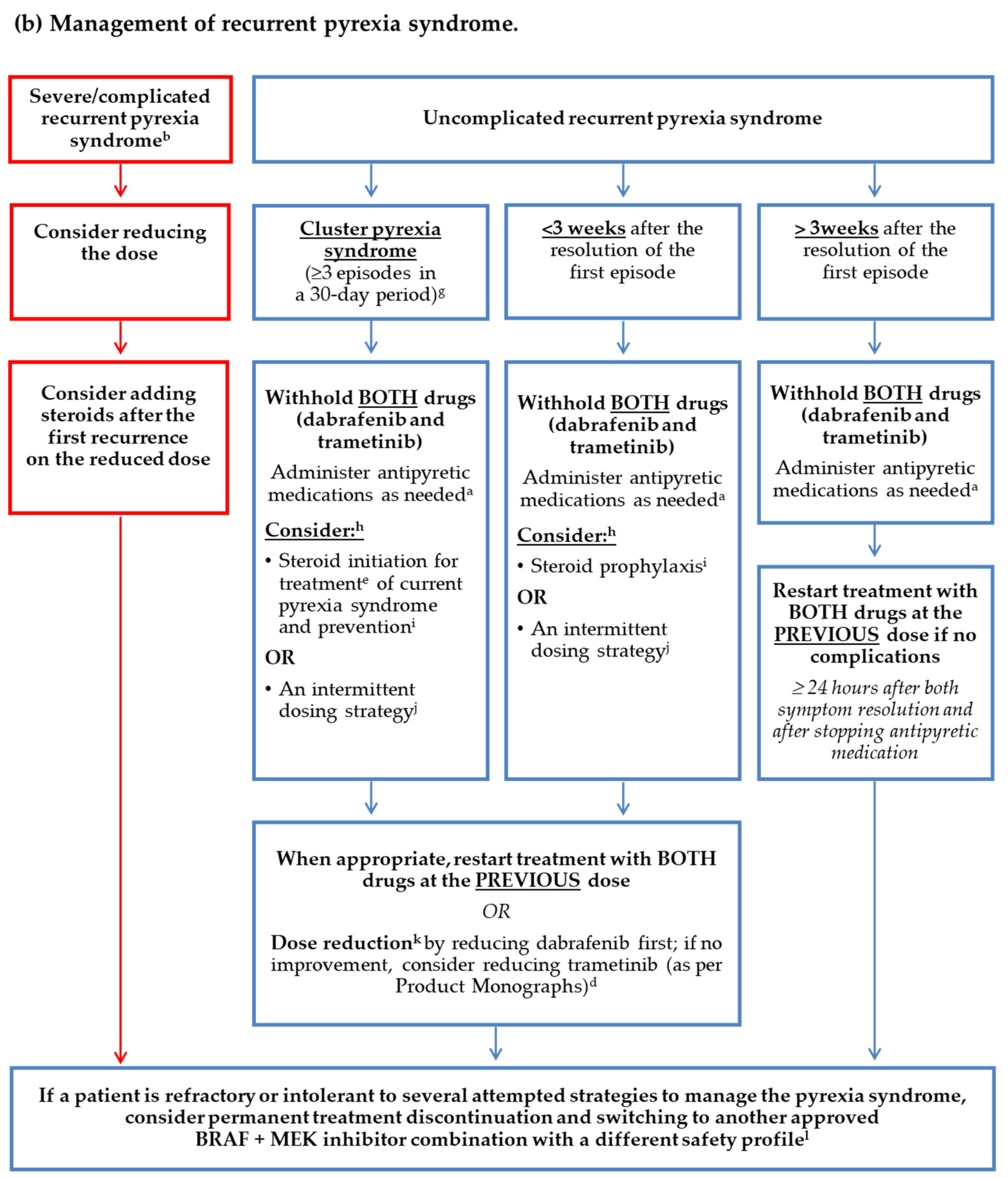
3.3. Consensus Statements: Management of Recurrent Pyrexia Syndrome
3.4. Consensus Statements: When to Consider Steroids/Intermittent Dosing/and Treatment Discontinuation
3.5. Consensus Statements: Dosing Considerations
- First reduction: 100 mg twice daily (2 × 50 mg twice daily);
- Second reduction: 75 mg twice daily (1 × 75 mg twice daily);
- Third reduction: 50 mg twice daily (1 × 50 mg twice daily);
- If unable to tolerate 50 mg twice daily: discontinue dabrafenib.
- First reduction: 1.5 mg once daily;
- Second reduction: 1 mg once daily;
- If unable to tolerate 1 mg once daily: discontinue trametinib.
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
Appendix A
| How do you manage the first occurrence of pyrexia? | |||
| Treatment interruption of both drugs | Treatment interruption of dabrafenib only | Acetaminophen and ibuprofen as needed only | |
| 66% | 25% | 8% | |
| When do you resume treatment? | |||
| 24 h post-resolution of symptoms | 48 h post-resolution of symptoms | ||
| 50% | 50% | ||
| At what point do you consider steroids? | |||
| After 2nd occurrence | After ≥2 occurrences | When refractory to dose reduction | Other a |
| 8% | 42% | 42% | 8% |
| At what point do you consider dose reduction? | |||
| After 2nd occurrence | After ≥2 occurrences | When refractory to steroids | Other b |
| 25% | 42% | 25% | 8% |
| At what point do you consider permanently discontinuing dabrafenib and trametinib? | |||
| ≥2 occurrences | Refractory to dose reduction | Other c | |
| 8% | 42% | 50% | |
References
- Long, G.; Flaherty, K.T.; Stroyakovskiy, D.; Gogas, H.; Levchenko, E.; de Braud, F.; Larkin, J.; Garbe, C.; Jouary, T.; Hauschild, A.; et al. Dabrafenib plus trametinib versus dabrafenib monotherapy in patients with metastatic BRAF V600E/K-mutant melanoma: Long-term survival and safety analysis of a phase 3 study. Ann. Oncol. 2017, 28, 1631–1639. [Google Scholar] [CrossRef]
- Robert, C.; Karaszewska, B.; Schachter, J.; Rutkowski, P.; Mackiewicz, A.; Stroiakovski, D.; Lichinitser, M.; Dummer, R.; Grange, F.; Mortier, L.; et al. Improved Overall Survival in Melanoma with Combined Dabrafenib and Trametinib. N. Engl. J. Med. 2015, 372, 30–39. [Google Scholar] [CrossRef] [Green Version]
- Larkin, J.; Ascierto, P.A.; Dréno, B.; Atkinson, V.; Liszkay, G.; Maio, M.; Mandalà, M.; Demidov, L.; Stroyakovskiy, D.; Thomas, L.; et al. Combined Vemurafenib and Cobimetinib in BRAF-Mutated Melanoma. N. Engl. J. Med. 2014, 371, 1867–1876. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Dummer, R.; Ascierto, P.A.; Gogas, H.J.; Arance, A.; Mandala, M.; Liszkay, G.; Garbe, C.; Schadendorf, D.; Krajsova, I.; Gutzmer, R.; et al. Overall survival in patients with BRAF-mutant melanoma receiving encorafenib plus binimetinib versus vemurafenib or encorafenib (COLUMBUS): A multicentre, open-label, randomised, phase 3 trial. Lancet Oncol. 2018, 19, 1315–1327. [Google Scholar] [CrossRef]
- Dummer, R.; Hauschild, A.; Santinami, M.; Atkinson, V.; Mandalà, M.; Kirkwood, J.M.; Chiarion Sileni, V.; Larkin, J.; Nyakas, M.; Dutriaux, C.; et al. Five-Year Analysis of Adjuvant Dabrafenib plus Trametinib in Stage III Melanoma. N. Engl. J. Med. 2020, 383, 1139–1148. [Google Scholar] [CrossRef] [PubMed]
- Daud, A.; Tsai, K. Management of Treatment-Related Adverse Events with Agents Targeting the MAPK Pathway in Patients with Metastatic Melanoma. Oncologist 2017, 22, 823–833. [Google Scholar] [CrossRef] [Green Version]
- Menzies, A.M.; Ashworth, M.T.; Swann, S.; Kefford, R.; Flaherty, K.; Weber, J.; Infante, J.R.; Kim, K.B.; Gonzalez, R.; Hamid, O.; et al. Characteristics of pyrexia in BRAFV600E/K metastatic melanoma patients treated with combined dabrafenib and trametinib in a phase I/II clinical trial. Ann. Oncol. 2015, 26, 415–421. [Google Scholar] [CrossRef]
- Lee, C.I.; Menzies, A.M.; Haydu, L.E.; Azer, M.; Clements, A.; Kefford, R.F.; Long, G.V. Features and management of pyrexia with combined dabrafenib and trametinib in metastatic melanoma. Melanoma Res. 2014, 24, 468–474. [Google Scholar] [CrossRef]
- Long, G.V.; Stroyakovskiy, D.; Gogas, H.; Levchenko, E.; De Braud, F.; Larkin, J.; Garbe, C.; Jouary, T.; Hauschild, A.; Grob, J.J.; et al. Combined BRAF and MEK Inhibition versus BRAF Inhibition Alone in Melanoma. N. Engl. J. Med. 2014, 371, 1877–1888. [Google Scholar] [CrossRef] [Green Version]
- Weber, J.; Del Vecchio, M.; Mandala, M.; Gogas, H.; Arance, A.; Dalle, S.; Cowey, C.; Schenker, M.; Grob, J.; Chiarion-Sileni, V.; et al. Analysis of pyrexia in patients (pts) treated with dabrafenib (D) and/or trametinib (T) across clinical trials. Ann. Oncol. 2019, 30, v533–v534. [Google Scholar] [CrossRef]
- Schadendorf, D.; Hauschild, A.; Santinami, M.; Atkinson, V.; Mandalà, M.; Sileni, V.C.; Larkin, J.; Nyakas, M.; Dutriaux, C.; Haydon, A.; et al. Patient-reported outcomes in patients with resected, high-risk melanoma with BRAFV600E or BRAFV600K mutations treated with adjuvant dabrafenib plus trametinib (COMBI-AD): A randomised, placebo-controlled, phase 3 trial. Lancet Oncol. 2019, 20, 701–710. [Google Scholar] [CrossRef]
- Ascierto, P.A.; McArthur, G.A.; Dréno, B.; Atkinson, V.; Liszkay, G.; Di Giacomo, M.; Mandalà, M.; Demidov, L.; Stroyakovskiy, D.; Thomas, P.L.; et al. Cobimetinib combined with vemurafenib in advanced BRAF(V600)-mutant melanoma (coBRIM): Updated efficacy results from a randomised, double-blind, phase 3 trial. Lancet Oncol. 2016, 17, 1248–1260. [Google Scholar] [CrossRef]
- Dummer, R.; Ascierto, P.A.; Gogas, H.J.; Arance, A.; Mandala, M.; Liszkay, G.; Garbe, C.; Schadendorf, D.; Krajsova, I.; Gutzmer, R.; et al. Encorafenib plus binimetinib versus vemurafenib or encorafenib in patients with BRAF -mutant melanoma (COLUMBUS): A multicentre, open-label, randomised phase 3 trial. Lancet Oncol. 2018, 19, 603–615. [Google Scholar] [CrossRef] [Green Version]
- Flaherty, K.T.; Robert, C.; Hersey, P.; Nathan, P.; Garbe, C.; Milhem, M.; Demidov, L.V.; Hassel, J.C.; Rutkowski, P.; Mohr, P.; et al. Improved Survival with MEK Inhibition in BRAF-Mutated Melanoma. N. Engl. J. Med. 2012, 367, 107–114. [Google Scholar] [CrossRef] [Green Version]
- Infante, J.R.; Fecher, L.A.; Falchook, G.S.; Nallapareddy, S.; Gordon, M.S.; Becerra, C.; De Marini, D.J.; Cox, D.S.; Xu, Y.; Morris, S.R.; et al. Safety, pharmacokinetic, pharmacodynamic, and efficacy data for the oral MEK inhibitortrametinib: A phase 1 dose-escalation trial. Lancet Oncol. 2012, 13, 773–781. [Google Scholar] [CrossRef]
- Ouellet, D.; Gibiansky, E.; Leonowens, C.; O’Hagan, A.; Haney, P.; Switzky, J.; Goodman, V.L. Population pharmacokinetics of dabrafenib, a BRAF inhibitor: Effect of dose, time, covariates, and relationship with its metabolites. J. Clin. Pharmacol. 2014, 54, 696–706. [Google Scholar] [CrossRef] [PubMed]
- Hajek, E.; Krebs, F.; Bent, R.; Haas, K.; Bast, A.; Steinmetz, I.; Tuettenberg, A.; Grabbe, S.; Bros, M. BRAF inhibitors stimulate inflammasome activation and interleukin 1 beta production in dendritic cells. Oncotarget 2018, 9, 28294–28308. [Google Scholar] [CrossRef] [Green Version]
- Atkinson, V.; Long, G.; Menzies, A.; McArthur, G.; Carlino, M.S.; Millward, M.; Roberts-Thomson, R.; Brady, B.; Kefford, R.; Haydon, A.; et al. Optimizing combination dabrafenib and trametinib therapy in BRAF mutation-positive advanced melanoma patients: Guidelines from Australian melanoma medical oncologists. Asia-Pac. J. Clin. Oncol. 2016, 12, 5–12. [Google Scholar] [CrossRef] [Green Version]
- MEKINIST Product Monograph, Novartis Pharmaceuticals Canada Inc. 19 March 2021. Available online: https://www.ask.novartispharma.ca/download.htm?res=mekinist_scrip_e.pdf&resTitleId=1087 (accessed on 28 April 2021).
- TAFINLAR Product Monograph, Novartis Pharmaceuticals Canada Inc. 19 March 2021. Available online: https://www.ask.novartispharma.ca/download.htm?res=tafinlar_scrip_e.pdf&resTitleId=1095 (accessed on 28 April 2021).
- Long, G.V.; Hauschild, A.; Santinami, M.; Atkinson, V.; Mandalà, M.; Chiarion-Sileni, V.; Larkin, J.; Nyakas, M.; Dutriaux, C.; Haydon, A.; et al. Adjuvant Dabrafenib plus Trametinib in Stage III BRAF-Mutated Melanoma. N. Engl. J. Med. 2017, 377, 1813–1823. [Google Scholar] [CrossRef] [Green Version]
- A Study of the Anti-PD1 Antibody PDR001, in Combination with Dabrafenib and Trametinib in Advanced Melanoma (COMBI-i). Available online: https://clinicaltrials.gov/ct2/show/NCT02967692 (accessed on 7 May 2021).
- Study of Dabrafenib+ Trametinib in the Adjuvant Treatment of Stage III BRAF V600+ Melanoma after Complete Resection to Evaluate the Impact on Pyrexia Related Outcomes (COMBI-APlus). Available online: https://clinicaltrials.gov/ct2/show/NCT03551626 (accessed on 7 May 2021).
- Walter, E.J.; Hanna-Jumma, S.; Carraretto, M.; Forni, L. The pathophysiological basis and consequences of fever. Crit. Care 2016, 20, 1–10. [Google Scholar] [CrossRef] [Green Version]
- Loblaw, D.A.; Prestrud, A.A.; Somerfield, M.R.; Oliver, T.K.; Brouwers, M.C.; Nam, R.K.; Lyman, G.H.; Basch, E. American Society of Clinical Oncology Clinical Practice Guidelines: Formal Systematic Review–Based Consensus Methodology. J. Clin. Oncol. 2012, 30, 3136–3140. [Google Scholar] [CrossRef] [PubMed]
- Falkson, C.; Bezjak, A.; Darling, G.; Gregg, R.; Malthaner, R.; Maziak, D.E.; Yu, E.; Smith, C.A.; McNair, S.; Ung, Y.C.; et al. The Management of Thymoma: A Systematic Review and Practice Guideline. J. Thorac. Oncol. 2009, 4, 911–919. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Algazi, A. Continuous dosing of BRAF and MEK inhibitors improves PFS in melanoma subset Abstract CT02-01. In Proceedings of the AACR Annual Meeting, Virtual Meeting, 27–28 April 2020. [Google Scholar]
- Tkinson, V.; Robert, C.; Grob, J.J.; Gogas, H.; Dutriaux, C.; Demidov, L.V.; Gupta, A.; Menzies, A.M.; Ryll, B.; Miranda, F.; et al. Improved pyrexia-related outcomes associated with an adapted pyrexia adverse event (AE) management algorithm in patients (pts) treated with adjuvant dabrafenib + trametinib (dab + tram): Primary results of COMBI-APlus. ASCO 2021, 9525. [Google Scholar] [CrossRef]
- Ascierto, P.A.; Robert, C.; Nathan, P.D.; Dummer, R.; Tawbi, H.A.-H.; Flaherty, K.T.; Ribas, A.; Schadendorf, D.; Green, S.; Sandalic, L.; et al. Pyrexia-related outcomes upon application of an adapted pyrexia management algorithm in patients (pts) with BRAF V600: Mutant unresectable or metastatic melanoma treated with dabrafenib plus trametinib (DabTram) in the COMBI-i trial. J. Clin. Oncol. 2021, 39, 9560. [Google Scholar] [CrossRef]
| Sources | PrTAFINLAR® (dabrafenib) Product Monograph [20] | COMBI AD [5,21] | COMBI I [22] | COMBI-APlus [23] | Australian Guidelines [18] |
|---|---|---|---|---|---|
| Definition of pyrexia/pyrexia syndrome | Pyrexia definition is not explicitly stated. Guidance for fever ≥ 38.5 °C | Pyrexia defined as body temperature ≥ 38 °C | Pyrexia syndrome:
| Pyrexia:
| Pyrexia syndrome: Presence of any of the following symptoms:
|
| Definition of severe pyrexia | Fever > 40 °C or any fever with complications:
| Fever >40 °C or associated with rigors, severe chills, dehydration or hypotension, serum creatinine and other evidence of renal dysfunction |
| ||
| Infectious Workup | Any fever occurrence | Laboratory work-up and clinical evaluation for infection for patients with pyrexia not resolving within 24 h |
| ||
| Management of first occurrence of pyrexia syndrome | |||||
| Treatment interruption | Interrupt dabrafenib if uncomplicated fever 38.5–40 °C; Continue trametinib | Interrupt dabrafenib if uncomplicated fever ≥38 °C; Continue trametinib | Interrupt both drugs for pyrexia syndrome | Interrupt both drugs if uncomplicated fever ≥38 °C. | Interrupt both drugs for pyrexia syndrome |
| Restart | Restart dabrafenib at same or reduced dose once fever resolves | Restart dabrafenib at resolution of fever at same dose | Restart both drugs at same dose once symptom free for at least 24 h | Restart both drugs at same dose once symptom free for at least 24 h | Restart both drugs at same dose once symptom free for at least 24 h |
| Management of subsequent occurrence of pyrexia syndrome | |||||
| Dose reduction | Dabrafenib only | Dabrafenib in patients experiencing pyrexia not controlled by antipyretics or associated with rigors, severe chills, dehydration, hypotension or renal insufficiency | Can be considered if interruptions unmanageable * | Can be considered if recurrent pyrexia cannot be managed with interruption or prophylactic steroids, dose reduction is required * | If intermittent dosing and corticosteroid prophylaxis fail, consider dose reduction (only as a last resort) |
| Steroids | If antipyreticsineffective in treating fever | Recommended for treatment of pyrexia not controlled by antipyretics or associated with rigors, severe chills, dehydration, hypotension or renal insufficiency AND any second or subsequent occurrence | For fever treatment where antipyretics insufficient As clinically indicated for recalcitrant pyrexia | Recommended as treatment for recurrent pyrexia that cannot be managed with dose interruptions and antipyretic treatments and for pyrexia associated with complications. Consider as prophylaxis to prevent further episodes of pyrexia in those with recurrent pyrexia events | Recurrent or severe pyrexia syndrome as prophylaxis |
| Intermittent dosing | Not mentioned | Not mentioned | Not allowed | Not allowed | Recurrent or severe pyrexia syndrome |
| Pyrexia Syndrome Severity | Treatment Restart |
|---|---|
| Uncomplicated pyrexia with improvement 24 h after dose interruption and antipyretic treatments (as needed) | Restart treatment with BOTH drugs at the PREVIOUS dose ≥24 h after both symptom resolution and after stopping antipyretic medication |
| Uncomplicated pyrexia not improving after 48 h and negative infectious workup | Consider steroids for pyrexia syndrome treatment Restart treatment with BOTH drugs at the PREVIOUS dose |
| Severe/complicated pyrexia (pyrexia syndrome requiring hospitalization or complicated by CTCAE grade ≥2) | Restart treatment with BOTH drugs at a REDUCED dose (as per product monographs) ≥24 h after both symptom resolution and after stopping antipyretic medication |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Thawer, A.; Miller, W.H., Jr.; Gregorio, N.; Claveau, J.; Rajagopal, S.; Savage, K.J.; Song, X.; Petrella, T.M.; on behalf of the Canadian Working Group. Management of Pyrexia Associated with the Combination of Dabrafenib and Trametinib: Canadian Consensus Statements. Curr. Oncol. 2021, 28, 3537-3553. https://doi.org/10.3390/curroncol28050304
Thawer A, Miller WH Jr., Gregorio N, Claveau J, Rajagopal S, Savage KJ, Song X, Petrella TM, on behalf of the Canadian Working Group. Management of Pyrexia Associated with the Combination of Dabrafenib and Trametinib: Canadian Consensus Statements. Current Oncology. 2021; 28(5):3537-3553. https://doi.org/10.3390/curroncol28050304
Chicago/Turabian StyleThawer, Alia, Wilson H. Miller, Jr., Nancy Gregorio, Joël Claveau, Sudha Rajagopal, Kerry J. Savage, Xinni Song, Teresa M. Petrella, and on behalf of the Canadian Working Group. 2021. "Management of Pyrexia Associated with the Combination of Dabrafenib and Trametinib: Canadian Consensus Statements" Current Oncology 28, no. 5: 3537-3553. https://doi.org/10.3390/curroncol28050304
APA StyleThawer, A., Miller, W. H., Jr., Gregorio, N., Claveau, J., Rajagopal, S., Savage, K. J., Song, X., Petrella, T. M., & on behalf of the Canadian Working Group. (2021). Management of Pyrexia Associated with the Combination of Dabrafenib and Trametinib: Canadian Consensus Statements. Current Oncology, 28(5), 3537-3553. https://doi.org/10.3390/curroncol28050304




