Preferences of Canadian Patients and Physicians for Treatment of HR+/HER2− Advanced Breast Cancer
Abstract
1. Introduction
2. Experimental Section
2.1. Overview
2.2. Survey Participants
2.3. Survey Questionnaire
2.4. Survey Pre-Test
2.5. Analyses
3. Results
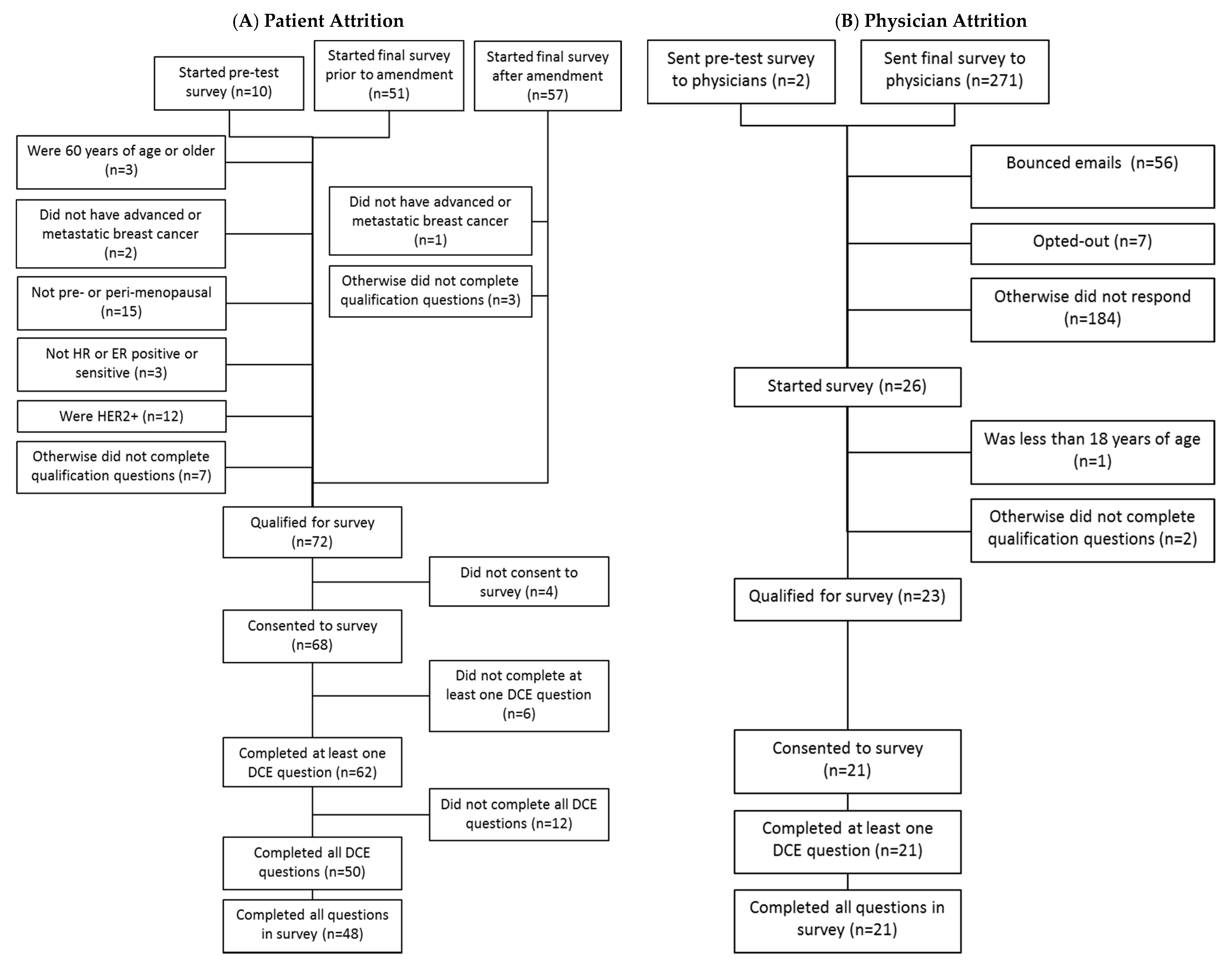
3.1. Study Participants
3.2. Participants Characteristics
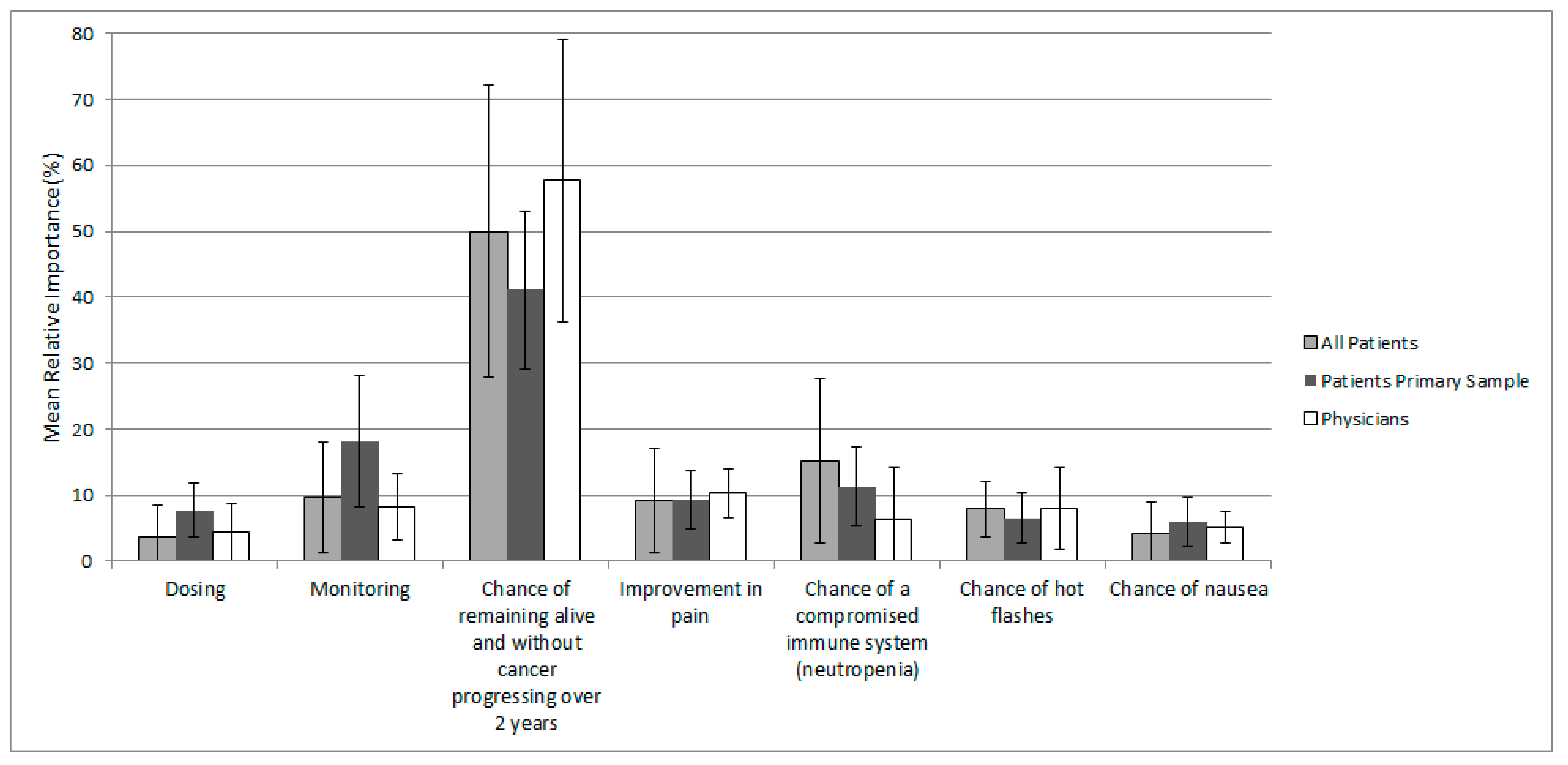
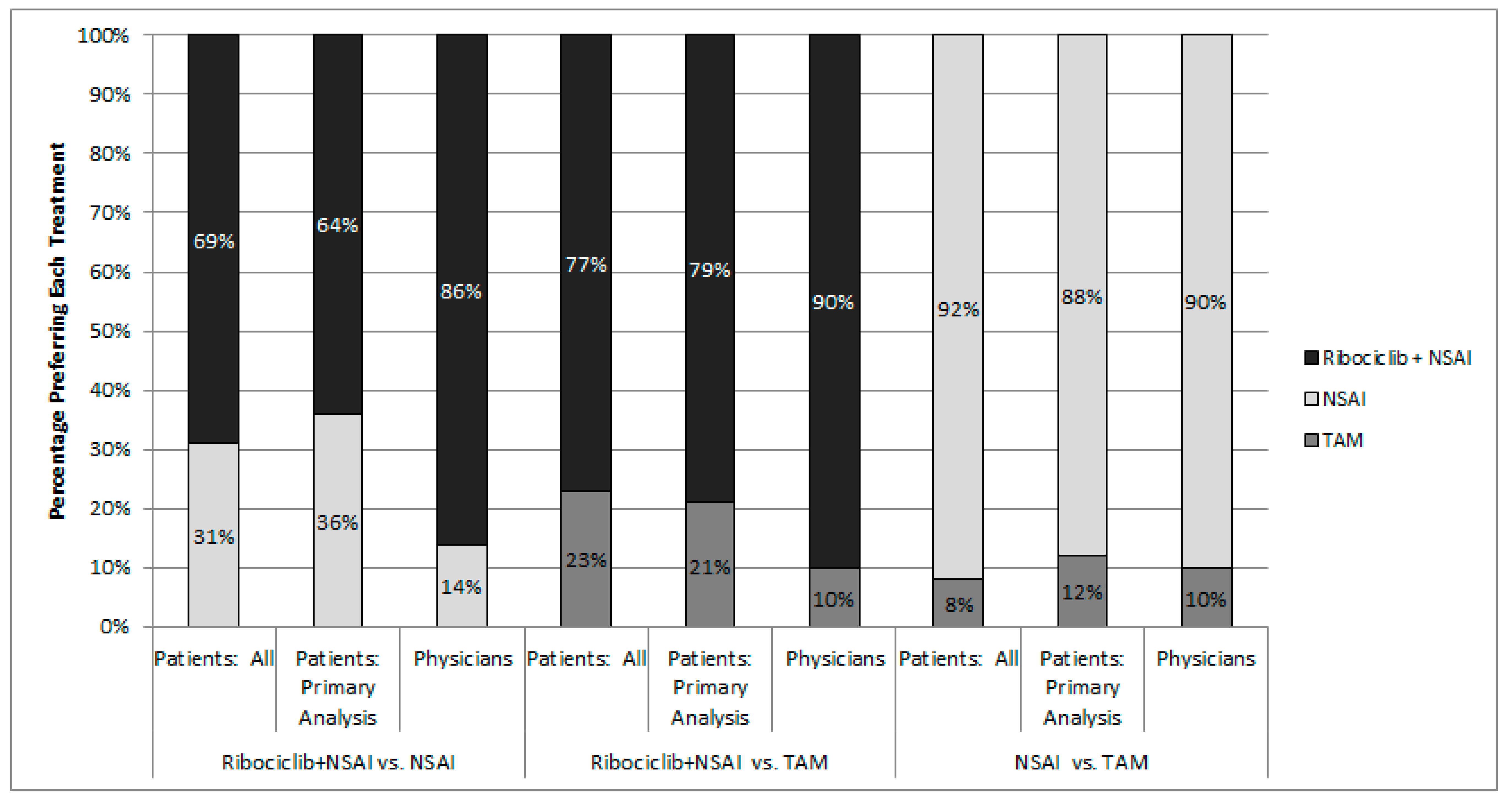
3.3. DCE Findings
3.4. Impact of ABC on Quality of Life and Work and Daily Activities
4. Discussion
4.1. Summary
4.2. Comparison with Prior Studies
4.3. Limitations
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
References
- Center for Disease Control and Prevention. U.S. Cancer Statistics Working Group. United States Cancer Statistics: 1999–2014 Incidence and Mortality Web-based Report; Department of Health and Human Services, Centers for Disease Control and Prevention, and National Cancer Institute: Atlanta, GA, USA, 2017. Available online: http://www.cdc.gov/uscs (accessed on 11 May 2018).
- Surveillance Epidemiology and End Results Program. Cancer Stat Facts: Female Breast Cancer. National Cancer Institute. 2018. Available online: https://seer.cancer.gov/statfacts/html/breast.html (accessed on 11 May 2018).
- Canadian Cancer Society. Breast Cancer Statistics. 2019. Available online: http://www.cancer.ca/en/cancer-information/cancer-type/breast/statistics/?region=on (accessed on 10 February 2019).
- Canadian Cancer Society Advisory Committee. Canadian Cancer Statistics 2015; Canadian Cancer Society: Toronto, ON, Canada, 2015; Available online: http://www.cancer.ca/~/media/cancer.ca/CW/cancer%20information/cancer%20101/Canadian%20cancer%20statistics/Canadian-Cancer-Statistics-2015-EN.pdf?la=en (accessed on 12 December 2018).
- Howlader, N.; Altekruse, S.F.; Li, C.I.; Chen, V.W.; Clarke, C.A.; Ries, L.A.; Cronin, K.A. US incidence of breast cancer subtypes defined by joint hormone receptor and HER2 status. JNCI J. Natl. Cancer Inst. 2014, 106, dju055. [Google Scholar] [CrossRef]
- Canadian Cancer Statistics Advisory Committee. Canadian Cancer Statistics 2018; Canadian Cancer Society: Toronto, ON, Canada, 2018; Available online: https://www.cancer.ca/~/media/cancer.ca/CW/cancer%20information/cancer%20101/Canadian%20cancer%20statistics/Canadian-Cancer-Statistics-2018-EN.pdf?la=en (accessed on 12 December 2018).
- Partridge, A.H.; Rumble, R.B.; Carey, L.A.; Come, S.E.; Davidson, N.E.; Di Leo, A.; Gralow, J.; Hortobagyi, G.N.; Moy, B.; Yee, D.; et al. Chemotherapy and targeted therapy for women with human epidermal growth factor receptor 2-negative (or unknown) advanced breast cancer: American Society of Clinical Oncology Clinical Practice Guideline. J. Clin. Oncol. 2014, 32, 3307–3329. [Google Scholar] [CrossRef] [PubMed]
- Cardoso, F.; Spence, D.; Mertz, S.; Corneliussen-James, D.; Sabelko, K.; Gralow, J.; Cardoso, M.J.; Peccatori, F.; Paonessa, D.; Benares, A.; et al. Global analysis of advanced/metastatic breast cancer: Decade report (2005–2015). Breast 2018, 39, 131–138. [Google Scholar] [CrossRef] [PubMed]
- Cardoso, F.; Senkus, E.; Costa, A.; Papadopoulos, E.; Aapro, M.; Andre, F.; Harbeck, N.; Aguilar Lopez, B.; Barrios, C.H.; Bergh, J.; et al. 4th ESO-ESMO International Consensus Guidelines for Advanced Breast Cancer (ABC 4). Ann. Oncol. 2018, 29, 1634–1657. [Google Scholar] [CrossRef] [PubMed]
- National Comprehensive Cancer Network. NCCN Clinical Practice Guidelines in Oncology (NCCN Guidelines). Breast Cancer. 2019. Available online: https://www.nccn.org/professionals/physician_gls/pdf/breast.pdf (accessed on 18 July 2019).
- Matutino, A.; Joy, A.A.; Brezden-Masley, C.; Chia, S.; Verma, S. Hormone receptor-positive, HER2-negative metastatic breast cancer: Redrawing the lines. Curr. Oncol. 2018, 25 (Suppl. 1), S131–S141. [Google Scholar] [CrossRef]
- Higgins, M.J.; Baselga, J. Targeted therapies for breast cancer. J. Clin. Investig. 2011, 121, 3797–3803. [Google Scholar] [CrossRef]
- Cardoso, F.; Costa, A.; Senkus, E.; Aapro, M.; Andre, F.; Barrios, C.H.; Bergh, J.; Bhattacharyya, G.; Biganzoli, L.; Cardoso, M.J.; et al. 3rd ESO-ESMO International Consensus Guidelines for Advanced Breast Cancer (ABC 3). Ann. Oncol. 2017, 28, 3111. [Google Scholar] [CrossRef]
- Rugo, H.S.; Rumble, R.B.; Macrae, E.; Barton, D.L.; Connolly, H.K.; Dickler, M.N.; Fallowfield, L.; Fowble, B.; Ingle, J.N.; Jahanzeb, M.; et al. Endocrine Therapy for Hormone Receptor-Positive Metastatic Breast Cancer: American Society of Clinical Oncology Guideline. J. Clin. Oncol. 2016, 34, 3069–3103. [Google Scholar] [CrossRef] [PubMed]
- Tripathy, D.; Sohn, J.; Im, S.-A.; Colleoni, M.; Franke, F.; Bardia, A.; Harbeck, N.; Hurvitz, S.; Chow, L.; Lee, K.S.; et al. First-line ribociclib vs placebo with goserelin and tamoxifen or a non-steroidal inhibitorin premenopausal women with hormone receptor-positive, HER2-negative advaced breast cancer: Results from the randomized phase III MONALEESA-7 trial. In Proceedings of the San Antonio Breast Cancer Conference, Abstract GS2-05, San Antonio, TX, USA, 5–9 December 2017. [Google Scholar]
- Tripathy, D.; Im, S.A.; Colleoni, M.; Franke, F.; Bardia, A.; Harbeck, N.; Hurvitz, S.A.; Chow, L.; Sohn, J.; Lee, K.S.; et al. Ribociclib plus endocrine therapy for premenopausal women with hormone-receptor-positive, advanced breast cancer (MONALEESA-7): A randomised phase 3 trial. Lancet Oncol. 2018, 19, 904–915. [Google Scholar] [CrossRef]
- Im, S.A.; Lu, Y.S.; Bardia, A.; Harbeck, N.; Colleoni, M.; Franke, F.; Chow, L.; Sohn, J.; Lee, K.S.; Campos-Gomez, S.; et al. Overall Survival with Ribociclib plus Endocrine Therapy in Breast Cancer. N. Engl. J. Med. 2019, 381, 307–316. [Google Scholar] [CrossRef]
- Ngorsuraches, S.; Thongkeaw, K. Patients’ preferences and willingness-to-pay for postmenopausal hormone receptor-positive, HER2-negative advanced breast cancer treatments after failure of standard treatments. Springerplus 2015, 4, 674. [Google Scholar] [CrossRef]
- Johnson, F.R.; Lancsar, E.; Marshall, D.; Kilambi, V.; Muhlbacher, A.; Regier, D.A.; Bresnahan, B.W.; Kanninen, B.; Bridges, J.F. Constructing experimental designs for discrete-choice experiments: Report of the ISPOR Conjoint Analysis Experimental Design Good Research Practices Task Force. Value Health J. Int. Soc. Pharm. Outcomes Res. 2013, 16, 3–13. [Google Scholar] [CrossRef] [PubMed]
- Sawtooth Software, Inc. Lighthouse Studio v9.6: Software for Web Interviewing and Conjoint Analysis; Sawtooth Software, Inc.: Orem, UT, USA, 2018. [Google Scholar]
- Bridges, J.F.; Hauber, A.B.; Marshall, D.; Lloyd, A.; Prosser, L.A.; Regier, D.A.; Johnson, F.R.; Mauskopf, J. Conjoint analysis applications in health—A checklist: A report of the ISPOR Good Research Practices for Conjoint Analysis Task Force. Value Health J. Int. Soc. Pharm. Outcomes Res. 2011, 14, 403–413. [Google Scholar] [CrossRef]
- Hauber, A.B.; Gonzalez, J.M.; Groothuis-Oudshoorn, C.G.; Prior, T.; Marshall, D.A.; Cunningham, C.; IJzerman, M.J.; Bridges, J.F. Statistical Methods for the Analysis of Discrete Choice Experiments: A Report of the ISPOR Conjoint Analysis Good Research Practices Task Force. Value Health J. Int. Soc. Pharm. Outcomes Res. 2016, 19, 300–315. [Google Scholar] [CrossRef]
- Sawtooth Software. Conjoint Choice Analysis. 2017. Available online: https://www.sawtoothsoftware.com/products/conjoint-choice-analysis (accessed on 13 September 2017).
- Davis, C.; Naci, H.; Gurpinar, E.; Poplavska, E.; Pinto, A.; Aggarwal, A. Availability of evidence of benefits on overall survival and quality of life of cancer drugs approved by European Medicines Agency: Retrospective cohort study of drug approvals 2009–2013. BMJ 2017, 359, j4530. [Google Scholar] [CrossRef]
- Forsythe, A.; Chandiwana, D.; Barth, J.; Thabane, M.; Baeck, J.; Tremblay, G. Progression-free survival/time to progression as a potential surrogate for overall survival in HR+, HER2- metastatic breast cancer. Breast Cancer 2018, 10, 69–78. [Google Scholar] [CrossRef] [PubMed]
- Piccart, M.; Hortobagyi, G.N.; Campone, M.; Pritchard, K.; Lebrun, F.; Ito, Y.; Noguchi, S.; Perez, A.; Rugo, H.S.; Deleu, I.; et al. Everolimus plus exemestane for hormone-receptor-positive, human epidermal growth factor receptor-2-negative advanced breast cancer: Overall survival results from BOLERO-2. Ann. Oncol. 2014, 25, 2357–2362. [Google Scholar] [CrossRef]
- Kisqali(R) [Package Insert]; Novartis Pharmaceuticals Corporation: East Hanover, NJ, USA, 2018.
- Hortobagyi, G.N.; Stemmer, S.M.; Burris, H.A.; Yap, Y.S.; Sonke, G.S.; Paluch-Shimon, S.; Campone, M.; Blackwell, K.L.; André, F.; Winer, E.P.; et al. Ribociclib as First-Line Therapy for HR-Positive, Advanced Breast Cancer. N. Engl. J. Med. 2016, 375, 1738–1748. [Google Scholar] [CrossRef] [PubMed]
- Mouridsen, H.; Giobbie-Hurder, A.; Goldhirsch, A.; Thurlimann, B.; Paridaens, R.; Smith, I.; Mauriac, L.; Forbes, J.; Price, K.N.; Regan, M.M.; et al. Letrozole therapy alone or in sequence with tamoxifen in women with breast cancer. N. Engl. J. Med. 2009, 361, 766–776. [Google Scholar]
- KISQALI[TM] Product Monograph; Novartis Pharmaceuticals Canada Inc.: Dorval, QC, Canada, 2018.
- FEMARA[R] Product Monograph; Novartis Pharmaceuticals Canada Inc.: Dorval, QC, Canada, 2017.
- NOLVADEX[R] -D Product Monograph; Astrazeneca Canada Inc.: Mississauga, ON, Canada, 2015.
- Spitzer, R.L.; Kroenke, K.; Williams, J.B.; Löwe, B. A brief measure for assessing generalized anxiety disorder: The GAD-7. Arch. Intern. Med. 2006, 166, 1092–1097. [Google Scholar] [CrossRef]
- Kroenke, K.; Spitzer, R.L.; Williams, J.B. The PHQ-9: Validity of a brief depression severity measure. J. Gen. Intern. Med. 2001, 16, 606–613. [Google Scholar] [CrossRef] [PubMed]
- Henderson, J.W.; Donatelle, R.J. The relationship between cancer locus of control and complementary and alternative medicine use by women diagnosed with breast cancer. Psycho-Oncology 2003, 12, 59–67. [Google Scholar] [CrossRef] [PubMed]
- Hinz, A.; Mehnert, A.; Ernst, J.; Herschbach, P.; Schulte, T. Fear of progression in patients 6 months after cancer rehabilitation—A validation study of the fear of progression questionnaire FoP-Q-12. Support. Care Cancer 2015, 23, 1579–1587. [Google Scholar] [CrossRef] [PubMed]
- Gorman, J.R.; Su, H.I.; Pierce, J.P.; Roberts, S.C.; Dominick, S.A.; Malcarne, V.L. A multidimensional scale to measure the reproductive concerns of young adult female cancer survivors. J. Cancer Surviv. 2014, 8, 218–228. [Google Scholar] [CrossRef] [PubMed]
- Reilly, M.C.; Zbrozek, A.S.; Dukes, E.M. The validity and reproducibility of a work productivity and activity impairment instrument. Pharmacoeconomics 1993, 4, 353–365. [Google Scholar] [CrossRef] [PubMed]
- Robertson, J.F.; Llombart-Cussac, A.; Rolski, J.; Feltl, D.; Dewar, J.; Macpherson, E.; Lindemann, J.; Ellis, M.J. Activity of fulvestrant 500 mg versus anastrozole 1 mg as first-line treatment for advanced breast cancer: Results from the FIRST study. J. Clin. Oncol. 2009, 27, 4530–4535. [Google Scholar] [CrossRef]
- MacEwan, J.P.; Doctor, J.; Mulligan, K.; May, S.G.; Batt, K.; Zacker, C.; Lakdawalla, D.; Goldman, D. The Value of Progression-Free Survival in Metastatic Breast Cancer: Results from a Survey of Patients and Providers. MDM Policy Pract. 2019, 4. [Google Scholar] [CrossRef]
- Spaich, S.; Kinder, J.; Hetjens, S.; Fuxius, S.; Gerhardt, A.; Sutterlin, M. Patient Preferences Regarding Chemotherapy in Metastatic Breast Cancer-A Conjoint Analysis for Common Taxanes. Front. Oncol. 2018, 8, 535. [Google Scholar] [CrossRef] [PubMed]
- Beusterien, K.; Grinspan, J.; Kuchuk, I.; Mazzarello, S.; Dent, S.; Gertler, S.; Bouganim, N.; Vandermeer, L.; Clemons, M. Use of conjoint analysis to assess breast cancer patient preferences for chemotherapy side effects. Oncologist 2014, 19, 127–134. [Google Scholar] [CrossRef] [PubMed]
| Attribute | Level 1 | Level 2 | Level 3 |
|---|---|---|---|
| Dosing regimen | One tablet daily | Two medications: For first medication, three tablets daily for 21 consecutive days followed by 7 days off treatment; For second medication, one tablet daily | -- |
| Monitoring | No electrocardiograms or bone mineral density tests; and blood tests every 1 to 3 months | Bone mineral density tests every 3 months; and blood tests every 1 to 3 months | Electrocardiograms every 2 weeks for 6 months, then every 3 months; bone mineral density tests every 3 months; and blood tests every 2 weeks for the first 2 months, then once every month for 4 months, and every 1 to 3 months thereafter |
| Chance of remaining alive and progression-free over 24 months | 25% | 35% | 53% |
| Amount of pain experienced | No noticeable improvement | Noticeable improvement | -- |
| Chance of neutropenia | 7% | 78% | -- |
| Chance of hot flashes | 21% | 24% | 29% |
| Chance of nausea | 20% | 31% | -- |
| Attribute | Ribociclib + NSAI | NSAI | Tamoxifen |
|---|---|---|---|
| Dosing schedule | Two medications: For first medication, three tablets daily for 21 consecutive days followed by 7 days off treatment; For second medication, one tablet daily | One tablet daily | One tablet daily |
| Monitoring | Electrocardiograms every 2 weeks for 6 months, then every 3 months; bone mineral density tests every 3 months; and blood tests every 2 weeks for the first 2 months, then once every month for 4 months, and every 1 to 3 months thereafter | Bone mineral density tests every 3 months; and blood tests every 1 to 3 months | No electrocardiograms or bone mineral density tests; and blood tests every 1 to 3 months |
| Chance of remaining alive and progression-free over 24 months | 53% | 35% | 25% |
| Amount of pain experienced | Noticeable improvement | No noticeable improvement | No noticeable improvement |
| Chance of neutropenia | 78% | 7% | 7% |
| Chance of hot flashes | 21% | 24% | 29% |
| Chance of nausea | 31% | 20% | 20% |
| Characteristic | Primary Analysis (n = 27) | All Patients (n = 118) | Physicians (n = 21) |
|---|---|---|---|
| Age, years, Mean (SD) * | 46.1 (9.3) | 50.0 (8.6) | 46.6 (7.8) |
| Gender, n (%) | |||
| Female | 27 (100) | 115 (100) | 13 (61.9) |
| Province of Residence, n (%) | |||
| Alberta | 2 (11.8) | 9 (18.4) | 2 (9.5) |
| British Columbia | 1 (5.9) | 7 (14.3) | 4 (19.0) |
| New Brunswick | 0 | 3 (6.1) | 0 |
| Newfoundland and Labrador | 0 | 2 (4.1) | 1 (4.8) |
| Nova Scotia | 0 | 0 | 1 (4.8) |
| Ontario | 13 (76.5) | 23 (46.9) | 11 (52.4) |
| Prince Edward Island | 0 | 1 (2.0) | 0 |
| Quebec | 0 | 0 | 2 (9.5) |
| Saskatchewan | 1 (5.9) | 4 (8.2) | 0 |
| Highest education level attained, n (%) | |||
| High school | 2 (11.8) | 9 (18.4) | --- |
| Associates degree | 5 (29.4) | 14 (28.6) | --- |
| Bachelor’s degree | 4 (23.5) | 14 (28.6) | --- |
| Postgraduate degree | 6 (35.3) | 12 (24.5) | --- |
| Employment (work for pay), n (%) | |||
| Full-time | 2 (11.8) | 9 (18.4) | --- |
| Part-time | 6 (35.3) | 9 (18.4) | --- |
| Unemployed | 9 (52.9) | 31 (63.3) | --- |
| HR status | |||
| HR+ | 27 (100) | 79 (89.8) | --- |
| HR- | 0 | 9 (10.2) | --- |
| HER2 status | |||
| HER2+ | 0 | 30 (35.7) | --- |
| HER2− | 27 (100) | 54 (64.3) | --- |
| Pre-menopausal | |||
| Yes | 27 (100) | 57 (54.3) | --- |
| No | 0 | 48 (45.7) | --- |
| Stage of ABC when diagnosed | |||
| Stage I or II | 5 (29.4) | 14 (28.6) | --- |
| Stage III | 5 (29.4) | 17 (34.7) | --- |
| Stage IV | 7 (41.2) | 18 (33.7) | --- |
| Taking medication for ABC, n (%) | |||
| Currently | 15 (88.2) | 42 (85.7) | --- |
| Not currently but did previously | 1 (5.9) | 2 (4.1) | --- |
| Never | 1 (5.9) | 5 (10.2) | --- |
| Medications currently or previously taken/received, n (%) | |||
| Ribociclib (Kisqali) | 3 (4.5) | 4 (2.1) | --- |
| Palbociclib (Ibrance) | 7 (10.6) | 18 (9.6) | --- |
| Tamoxifen | 12 (18.2) | 25 (13.4) | --- |
| Letrozole (Femara) | 11 (16.7) | 30 (16.0) | --- |
| Anastrozole (Arimidex) | 2 (3.0) | 8 (4.3) | --- |
| Fulvestrant (Faslodex) | 5 (7.6) | 12 (6.4) | --- |
| Exemestane (Aromasin) | 3 (4.5) | 11 (5.9) | --- |
| Unknown (e.g., due to trial participation) | 0 | 2 (1.1) | --- |
| Chemotherapy | 10 (15.2) | 31 (16.6) | |
| Other | 8 (12.1) | 19 (10.2) | --- |
| Time since most recent physician visit for management of ABC, n (%) | |||
| Less than one month | 13 (76.5) | 38 (77.6) | --- |
| One to three months | 2 (11.8) | 6 (12.2) | --- |
| Three to six months | 0 | 3 (6.1) | --- |
| Six to 12 months | 2 (11.8) | 2 (4.1) | --- |
| Specialty of physician seen most regularly for management of ABC, n (%) | |||
| Medical Oncologist | 16 (94.1) | 45 (91.8) | --- |
| Primary Care | 0 | 1 (2.0) | --- |
| Other | 1 (5.9) | 3 (6.1) | --- |
| Work setting | |||
| Community-based health center | --- | --- | 8 (38.1) |
| Academic health center | --- | --- | 13 (61.9) |
| Attribute Level | Primary Analysis Patients (n = 23) Mean (SD) | All Patients (n = 62) Mean (SD) | Physicians (n = 21) Mean (SD) |
|---|---|---|---|
| Dosing regimen | |||
| Two medications: For first medication, three tablets daily for 21 consecutive days followed by 7 days off treatment; for second medication, one tablet daily | −17.2 (26) | −1.3 (21) | −1.1 (22) |
| One tablet daily | 17.2 (26) | 1.3 (21) | 1.1 (22) |
| Monitoring | |||
| Electrocardiograms every 2 weeks for 6 months, then every 3 months; bone mineral density tests every 3 months; and blood tests every 2 weeks for the first 2 months, then once every month for 4 months, and every 1 to 3 months thereafter | −74.8 (42) | −29.4 (40) | −19.0 (26) |
| Bone mineral density tests every 3 months; and blood tests every 1 to 3 months | 29.7 (26) | 16.5 (18) | 28.2 (18) |
| Blood tests every 1 to 3 months | 45.1 (32) | 12.9 (34) | −9.2 (18) |
| Chance of remaining alive and without cancer progressing over 2 years | |||
| 53% | 134.4 (65) | 172.1 (101) | 206.3 (80) |
| 35% | 8.2 (38) | −9.9 (32) | −26.4 (30) |
| 25% | −142.6 (37) | −162.2 (85) | −179.9 (107) |
| Improvement in pain | |||
| Noticeable improvement | 31.8 (16) | 30.4 (29) | 28.0 (27) |
| No noticeable improvement | −31.8 (16) | −30.4 (29) | −28.0 (27) |
| Chance of a compromised immune system (neutropenia) | |||
| 7% | 39.0 (22) | 50.5 (47) | 15.3 (32) |
| 78% | −39.0 (22) | −50.5 (47) | −15.3 (32) |
| Chance of hot flashes | |||
| 21% | −1.3 (16) | −7.3 (27) | −21.4 (31) |
| 24% | −0.3 (25) | −7.8 (16) | 7.3 (30) |
| 29% | 1.6 (26) | 15.1 (29) | 14.1 (10) |
| Chance of nausea | |||
| 31% | −10.1 (22) | −9.3 (20) | −4.3 (20) |
| 20% | 10.1 (22) | 9.3 (20) | 4.3 (20) |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Stellato, D.; Thabane, M.; Eichten, C.; Delea, T.E. Preferences of Canadian Patients and Physicians for Treatment of HR+/HER2− Advanced Breast Cancer. Curr. Oncol. 2021, 28, 491-508. https://doi.org/10.3390/curroncol28010051
Stellato D, Thabane M, Eichten C, Delea TE. Preferences of Canadian Patients and Physicians for Treatment of HR+/HER2− Advanced Breast Cancer. Current Oncology. 2021; 28(1):491-508. https://doi.org/10.3390/curroncol28010051
Chicago/Turabian StyleStellato, Daniel, Marroon Thabane, Caitlin Eichten, and Thomas E. Delea. 2021. "Preferences of Canadian Patients and Physicians for Treatment of HR+/HER2− Advanced Breast Cancer" Current Oncology 28, no. 1: 491-508. https://doi.org/10.3390/curroncol28010051
APA StyleStellato, D., Thabane, M., Eichten, C., & Delea, T. E. (2021). Preferences of Canadian Patients and Physicians for Treatment of HR+/HER2− Advanced Breast Cancer. Current Oncology, 28(1), 491-508. https://doi.org/10.3390/curroncol28010051




