A Realist Evaluation of Case Management Models for People with Complex Health Conditions Using Novel Methods and Tools—What Works, for Whom, and under What Circumstances?
Abstract
1. Introduction
1.1. Study Setting
1.2. Research Aim and Objectives
- Describe the circumstances of the participant (context), the CM actions (mechanism), the CM model and the participant outcomes (outcomes).
- Examine patterns and associations between these components and the participant’s recovery pathway across the 10 years following injury.
- Examine which of the different CM actions (and in turn CM model) are associated with participant outcomes.
2. Methods
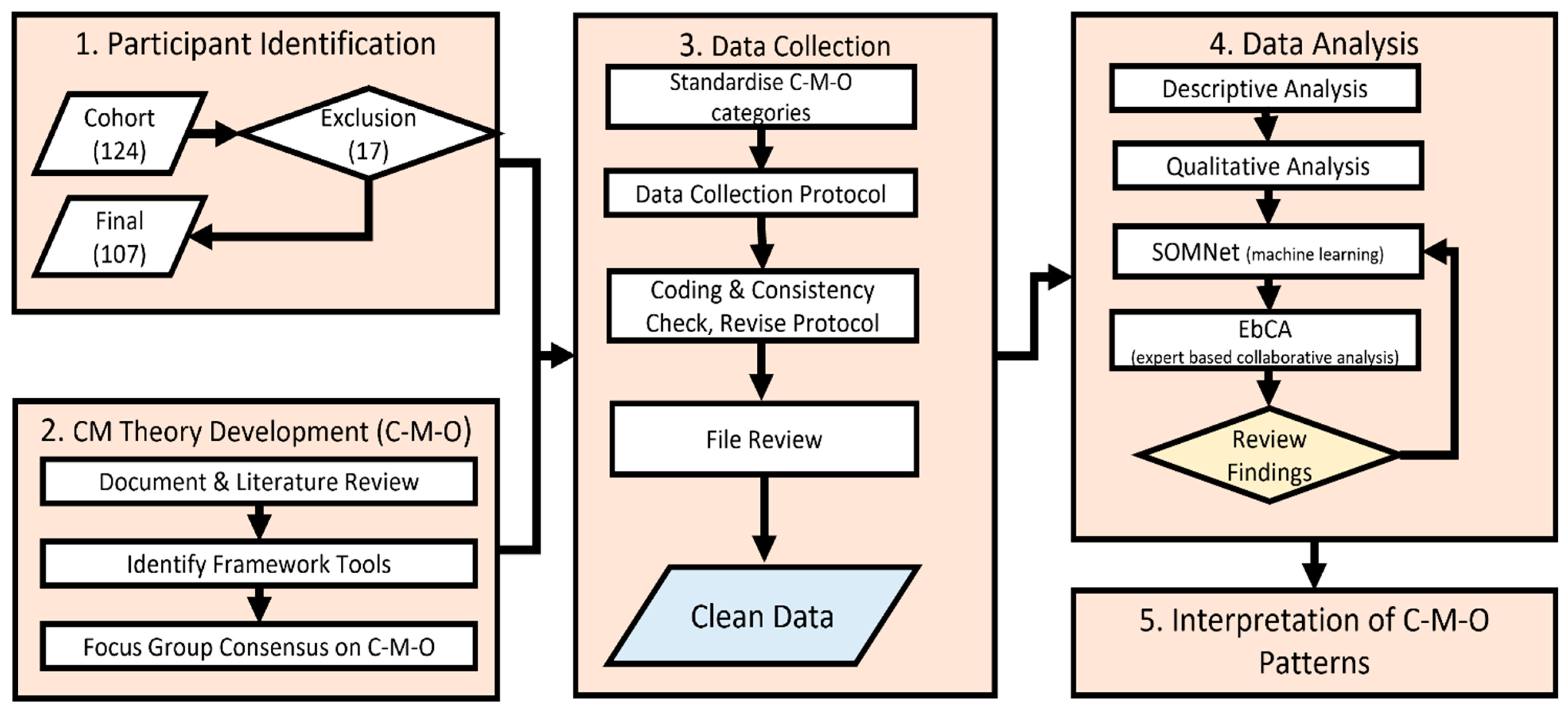
2.1. Research Design
2.2. Time Frames and Ethical Approval
2.3. Participants and Procedures
2.3.1. Participant Identification
2.3.2. CM Theory Development: Realist Context–Mechanism–Outcome (C-M-O)
- Document and literature review: In preparation for the CM theory development, a review of relevant documents and literature was completed, and key elements identified. The documents included:
- b.
- Identify framework tools: There was a large amount of information on the file of each participant from the past 10 years. The following frameworks were identified as tools to code relevant information extracted from the file reviews relevant to the theory of C-M-O:
- Appropriate data collection time points and the phase of the participant’s recovery were guided by the ‘My Plan’ framework of the Scheme’s conceptual model for the pathway following severe injury [27].
- A framework to categorize CM actions (mechanisms) and intensity was needed. The file reviewers mapped case managers’ actions and intensity outlined in reports and file notes, to a CM model at the time of data extraction. In 2016, the Scheme had already published case manager expectations [28,29] framed in terms of the CMTaxonomy [8,9]. In Table 1, the actions performed in the Generalist and Person-centred models of CM are mapped using the validated CMTaxonomy [8,9,30,31,32,33]. Refer to the CMTaxonomy toolkit: the Intervention tree and actions (Mechanisms) in Supplementary File S1, the Service tree (a domain of Context) in Supplementary File S2 and the Glossary in Supplementary File S3.
- c.
- Focus group consensus on the C-M-O: Four subject matter experts and a facilitator developed the program theory for person-centred approaches in CM and specifically in the context of people severely injured. The subject matter experts from LTCS included the Senior Service Development Manager—CM, a regional manager (who also had lived experience), Service Development Officer—CM and a Team Leader of the coordinators (staff who contracted and monitored the CM provided to participants). The first author completed the workshop preparation and facilitated the workshops using the frameworks to focus questions to stimulate and scaffold discussion.
2.3.3. Data Collection
Standardise C-M-O Categories
- i.
- The two level classification code from the World Health Organization International Functioning Disability and Health (ICF) classification available on the ICF browser [36].
- ii.
- Established ICF linking rules to map information to the ICF appropriately. Developed in 2016, the refinements to the ICF Linking Rules strengthen the potential for comparability of health information [37]. The file reviewers used the linking rules to map information to the ICF (e.g., target of the goals).
- iii.
- The World Health Organization International Classification of Health Interventions [38].
- iv.
- v.
- The My Plan phases of recovery post injury were incorporated into the C-M-O framework related to time periods [27,39]. The phases post injury refers to the typical pathway for people following a severe traumatic injury, such as brain injury and spinal cord injury. In the My Plan recovery pathway, the first phase (from the time of injury to approximately 2 years post injury) is broadly described as the ‘continued recovery phase’. In the continuing recovery phase, the participant continues to adjust to their injury and changed circumstances. There may be continued treatment and rehabilitation for the participant to settle into living at home (often following extensive acute inpatient hospital care and rehabilitation), and doing activities (often using restorative, adaptive, or learning different approaches to perform activities). In the next phase—occurring approximately in the 3–5 years post injury period—the My Plan pathway refers to this as the Participation phase of resuming participation in life roles. The participant is involved in their chosen activities and major life areas such as education, work, purposeful occupations, domestic responsibilities, community, and social life. The final phase is approximately 8–10 years after their injury. In this phase, the participant has moved on and living their life. The participant has reached a stage and rhythm of maintaining their health and wellbeing [27]. Hereafter, these phases are referred to as Recovery (continued adjustment, treatment/rehabilitation), Participation (in life roles), and Maintaining (life, health and wellbeing) phases respectively. The phase along the My Plan recovery pathway was an outcome variable (Recovery, Participation, Maintaining).
- vi.
- The My Plan goal rating using a three step achievement (not achieved, partially achieved, achieved) [27].
Data Collection Protocol
Coding and Consistency Check, Protocol Revised
File Review
Clean Data
2.3.4. Data Analysis
Descriptive Analysis
Qualitative Analysis
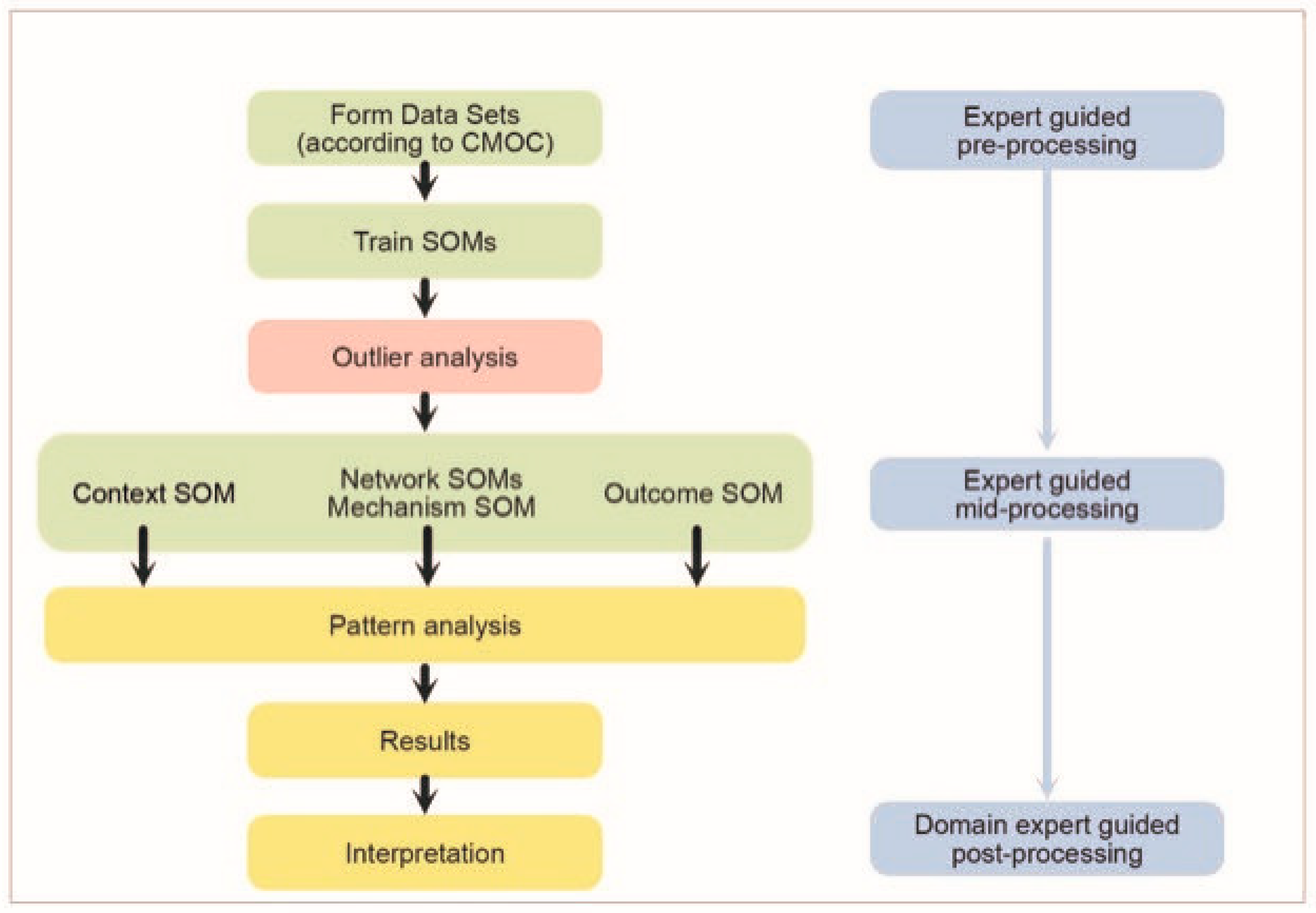
Self-Organising Map Network (SOMNet) with Expert-Based Collaborative Analysis (EbCA) [40,41]
2.3.5. Interpretation of C-M-O Pattens
3. Results
3.1. Description of Context
3.2. Description of Mechanisms
3.2.1. CM Involvement
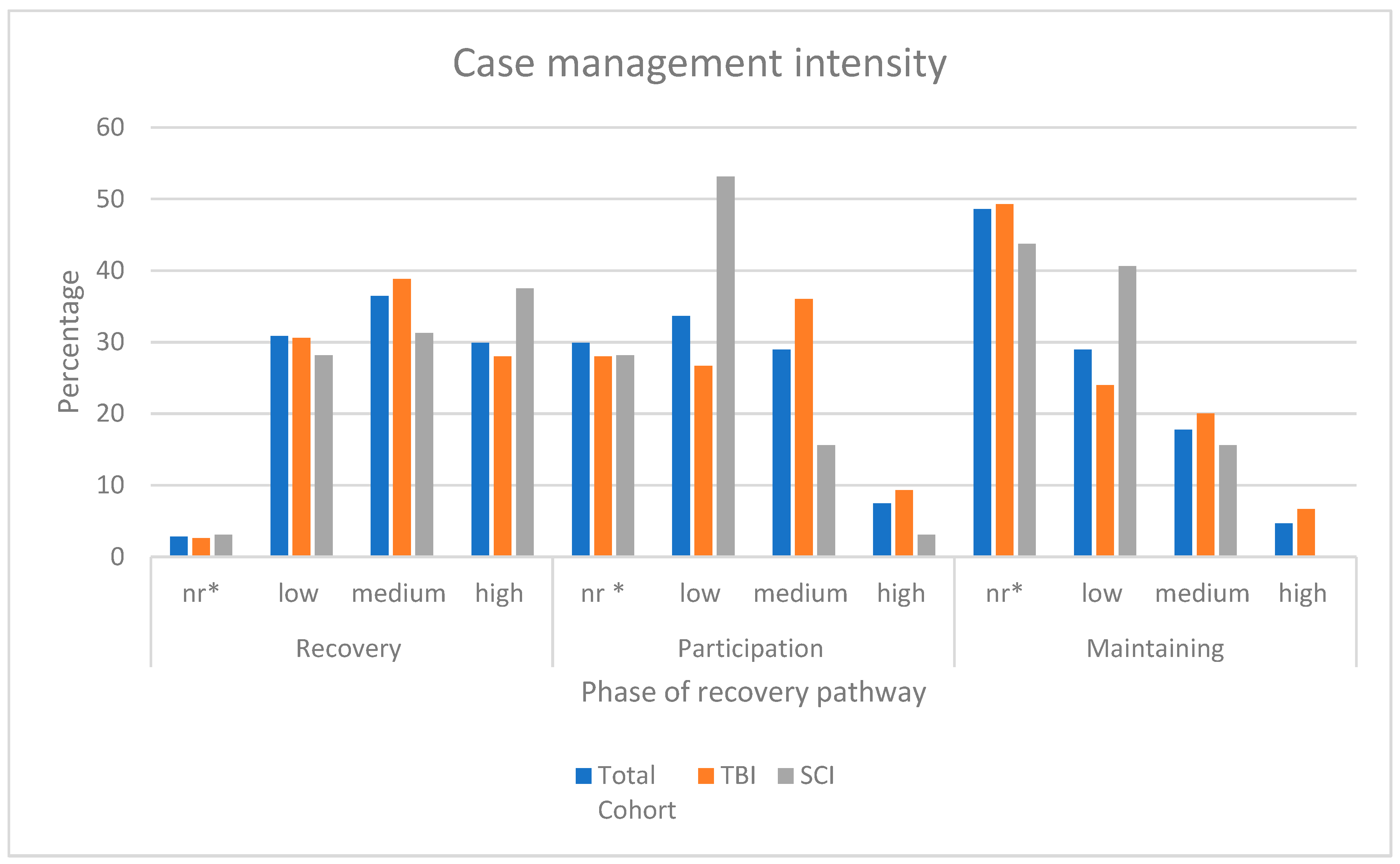
3.2.2. CM Intensity
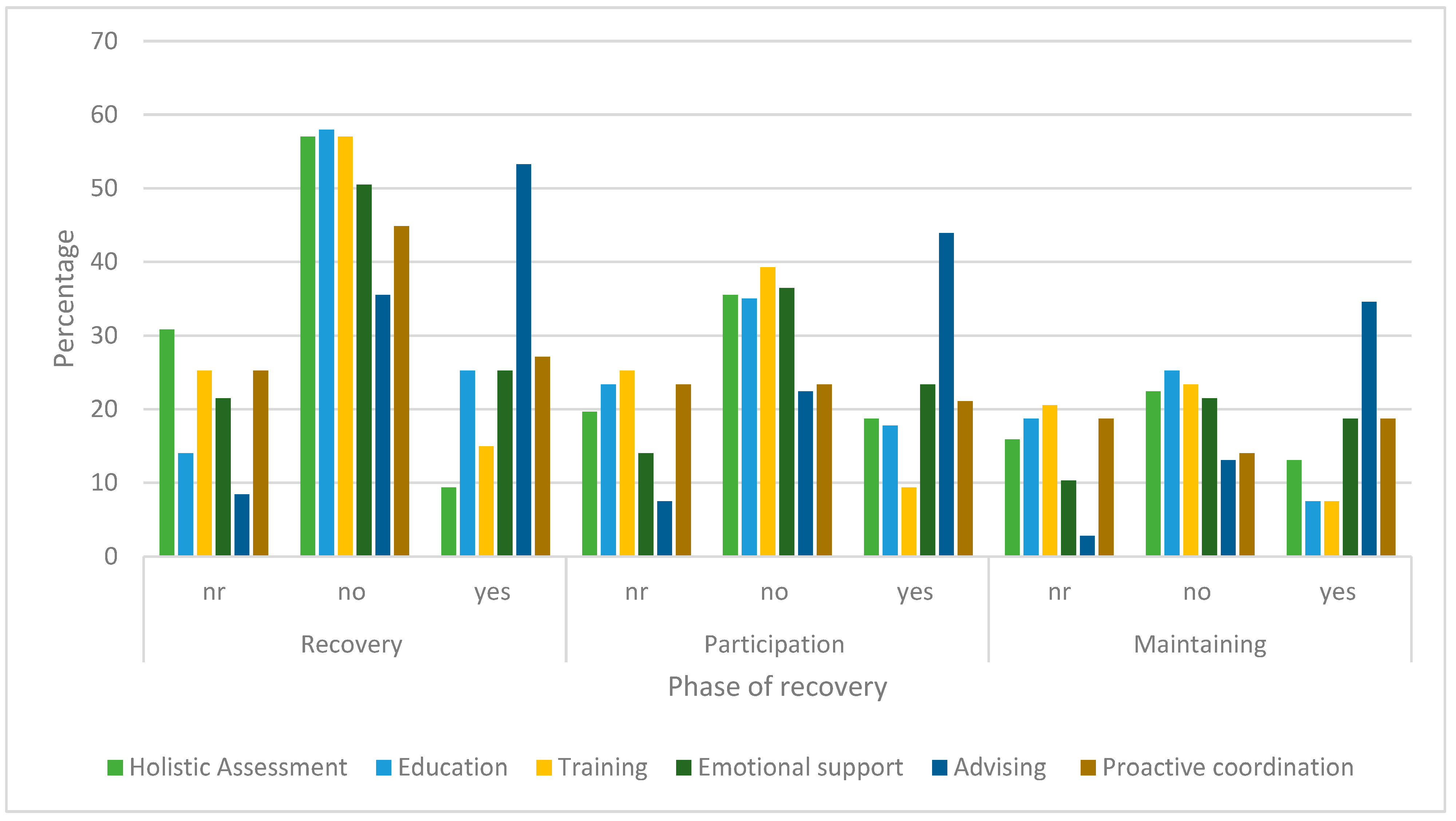
3.2.3. CM Actions Performed
3.3. Description of Outcomes
3.3.1. Goal Target
- Both the Body Function and CM target goals did not significantly decrease in frequency over the 10 years, indicative of the Generalist CM model.
- A high percent of goals targeted Environmental Factor barriers (e.g., home modifications, provision, and testing of equipment) in the Recovery phase, as might be expected for the study cohort.
- In the Recovery phase only 13.07% of goals or goal steps related to Interpersonal interactions and relationships (d710–d799), with 4.6% of these related to the parent/child relationship. In the Participation phase there were 7.46% of goals or steps related to Interpersonal interactions and relationships, none related to parenting relationship. However, in Year 10 there was a new focus on support and relationships, although only 7.47% were on interpersonal relationships with 2.8% on the parent-child relationship.
3.3.2. The Timelines and Recovery Pathway Phase of the Participant
3.4. Patterns, Associations, and Differences (SOMNet Analysis)
3.4.1. Traumatic Brain Injury Cohort SOMNet Results
3.4.2. Spinal Cord Injury SOMNet Results
4. Discussion
4.1. Case Management Model
4.2. Duration of Case Management
4.3. Case Management Actions and Context
4.4. Case Management and Outcomes
4.5. Limitations
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- World Health Organization—European Regional Office (WHO-Euro). Roadmap: Strengthening People-Centred Health Systems in the WHO European Region. A Framework for Action towards Coordinated/Integrated Health Services Delivery (CIHSD); World Health Organization Copenhagen: Copenhagen, Denmark, 2013. [Google Scholar]
- World Health Organization (WHO). WHO Global Strategy on Integrated People-Centred Health Services 2016–2026; WHO: Geneva, Switzerland, 2015. [Google Scholar]
- World Health Organization (WHO). Framework on Integrated, People-Centred Health Services: Report by the Secretariat to 69th World Health Assembly (Provisional Agenda Item 16.1); WHO: Geneva, Switzerland, 2016. [Google Scholar]
- World Health Organization (WHO). People-Centred and Integrated Health Services: An Overview of the Evidence; WHO: Geneva, Switzerland, 2015. [Google Scholar]
- World Health Organization. Framework on Integrated People-Centred Health Services. Available online: http://apps.who.int/gb/ebwha/pdf_files/WHA69/A69_39-en.pdf?ua=1&ua=1 (accessed on 12 September 2016).
- Lukersmith, S.; Millington, M.; Salvador-Carulla, L. What is Case Management? A Scoping and Mapping Review. Int. J. Integr. Care 2016, 16, 2. [Google Scholar] [CrossRef] [PubMed]
- Ross, S.; Curry, N.; Goodwin, N. Case management. In What It is and How It can Best be Implemented; The King’s Fund London: London, UK, 2011. [Google Scholar]
- Lukersmith, S.; Fernandez, A.; Millington, M.; Salvador-Carulla, L. The brain injury case management taxonomy (BICM-T); a classification of community-based case management interventions for a common language. Disabil. Health J. 2015, 9, 272–280. [Google Scholar] [CrossRef]
- Lukersmith, S. A Taxonomy of Case Management: Development, Dissemination and Impact. Ph.D. Thesis, University of Sydney, Sydney, Australia, 2017. [Google Scholar]
- Lowry, J.; Wakeham, T.; Norman, A.; Dean, J.; Holloway, M.; Needham-Holmes, B.; Clark-Wilson, V.; Feltham-White, P. Whose Outcome is it Anyway? Outcome and Brain Injury Case Management. J. Long-Term Care 2022. [Google Scholar] [CrossRef]
- Lannin, N.A.; Laver, K.; Henry, K.; Turnbull, M.; Elder, M.; Campisi, J.; Schmidt, J.; Schneider, E. Effects of case management after brain injury: A systematic review. NeuroRehabilitation 2014, 35, 635–641. [Google Scholar] [CrossRef] [PubMed]
- Chan, V.; Toccalino, D.; Omar, S.; Shah, R.; Colantonio, A. A systematic review on integrated care for traumatic brain injury, mental health, and substance use. PLoS ONE 2022, 17, e0264116. [Google Scholar] [CrossRef]
- Struckmann, V.; Leijten, F.R.M.; van Ginneken, E.; Kraus, M.; Reiss, M.; Spranger, A.; Boland, M.R.S.; Czypionka, T.; Busse, R.; Rutten-van Molken, M.; et al. Relevant models and elements of integrated care for multi-morbidity: Results of a scoping review. Health Policy 2018, 122, 23–35. [Google Scholar] [CrossRef]
- Braaf, S.; Ameratunga, S.; Christie, N.; Teague, W.; Ponsford, J.; Cameron, P.A.; Gabbe, B.J. Care coordination experiences of people with traumatic brain injury and their family members in the 4-years after injury: A qualitative analysis. Brain Inj. 2019, 33, 574–583. [Google Scholar] [CrossRef]
- Eliacin, J.; Fortney, S.K.; Rattray, N.A.; Kean, J. Patients’ and caregivers’ perspectives on healthcare navigation in Central Indiana, USA after brain injury. Health Soc. Care Community 2022, 30, 988–997. [Google Scholar] [CrossRef]
- Fernandez-Miranda, J.J.; Diaz-Fernandez, S.; Lopez-Munoz, F. Effectiveness of More Personalized, Case-Managed, and Multicomponent Treatment for Patients with Severe Schizophrenia Compared to the Standard Treatment: A Ten-Year Follow-Up. J. Pers. Med. 2022, 12, 1101. [Google Scholar] [CrossRef]
- Croker, D. Overview of the Costs of Case Management in LTCS; Coopers, P.W., Ed.; University of Sydney: Sydney, Australia, 2015. [Google Scholar]
- Gilmore, B.; McAuliffe, E.; Power, J.; Vallières, F. Data Analysis and Synthesis Within a Realist Evaluation: Toward More Transparent Methodological Approaches. Int. J. Qual. Methods 2019, 18, 1609406919859754. [Google Scholar] [CrossRef]
- Rameses Projects. The Rameses II Projects. Available online: https://www.ramesesproject.org/ (accessed on 10 January 2022).
- Lukersmith, S.; Salvador-Carulla, L.; Chung, Y.; Du, W.; Sarkissian, A. Mapping Case Management Provided to People with Severe Injuries; Lukersmith & Associates, Australian National University: Sydney, Australia, 2021. [Google Scholar]
- Salvador-Carulla, L.; Lukersmith, S.; Sullivan, W. From the EBM pyramid to the Greek temple: A new conceptual approach to guidelines as implementation tools in mental health. Epidemiol. Psychiatr. Sci. 2017, 26, 105–114. [Google Scholar] [CrossRef] [PubMed]
- Fernandez, A.; Sturmberg, J.; Lukersmith, S.; Madden, R.; Torkfar, G.; Colagiuri, R.; Salvador-Carulla, L. Evidence-based medicine: Is it a bridge too far? Health Res. Policy Syst. 2015, 13, 66. [Google Scholar] [CrossRef] [PubMed]
- Pozzato, I.; Higgins, K. Lifetime Care and Support Scheme Five and Two Year Participants Project: Predictive and Comparative analyses; John Walsh Centre for Rehabilitation Research, University of Sydney: Sydney, Australia, 2015. [Google Scholar]
- Cameron, I.; Higgins, K.; Monaghan, N.; Pozzato, I.; Ramakrishnan, K. Lifetime Care and Support Scheme Five Year Participant Outcome Evaluation; John Walsh Centre for Rehabilitation Research: Sydney, Australia, 2015. [Google Scholar]
- Collie, A.; Simpson, P.M.; Cameron, P.A.; Ameratunga, S.; Ponsford, J.; Lyons, R.A.; Braaf, S.; Nunn, A.; Harrison, J.E.; Gabbe, B.J. Patterns and Predictors of Return to Work After Major Trauma: A Prospective, Population-based Registry Study. Ann. Surg. 2019, 269, 972–978. [Google Scholar] [CrossRef] [PubMed]
- Lau, G.; Gabbe, B.J.; Collie, A.; Ponsford, J.; Ameratunga, S.; Cameron, P.A.; Harrison, J.E.; Giummarra, M.J. The Association Between Fault Attribution and Work Participation After Road Traffic Injury: A Registry-Based Observational Study. J. Occup. Rehabil. 2020, 30, 235–254. [Google Scholar] [CrossRef] [PubMed]
- Lifetime Care and Support Authority; Lukersmith, S. My Plan—Person-Centred Planning Approach. Available online: https://www.icare.nsw.gov.au/-/media/icare/unique-media/practitioners-and-providers/healthcare-and-service-providers/planning-with-an-injured-person/my-plan-2022/mpf001_my-plan.docx (accessed on 10 January 2022).
- Icare NSW, L.C. Case management expectations—Private Providers. Available online: https://www.icare.nsw.gov.au/practitioners-and-providers/healthcare-and-service-providers/case-managers#gref (accessed on 10 January 2021).
- icare NSW. Case Manager Expectations. Available online: https://www.icare.nsw.gov.au/-/media/icare/unique-media/practitioners-and-providers/healthcare-and-service-providers/case-management/case-management-expectations---private-providers.pdf (accessed on 10 January 2022).
- Young, J.; Lukersmith, S.; Salvador-Carulla, L.; Stancliffe, R. Case Management for Children and Adolescents with Acquired Brain Injury in Community Settings: A Scoping Review. Brain Impair. 2017, 18, 226–239. [Google Scholar] [CrossRef]
- Lukersmith, S.; Taylor, J.; Salvador-Carulla, L. Vagueness and Ambiguity in Communication of Case Management: A Content Analysis in the Australian National Disability Insurance Scheme. Int. J. Integr. Care 2021, 21, 17. [Google Scholar] [CrossRef]
- McRae, P.; Kobel, C.; Lukersmith, S.; Simpson, G. What Does It Take to Get Somebody Back to Work after Severe Acquired Brain Injury? Service Actions within the Vocational Intervention Program (VIP 2.0). Int. J. Environ. Res. Public. Health 2022, 19, 9548. [Google Scholar] [CrossRef]
- Stiekema, A.; Resch, C.; Donkervoort, M.; Jansen, N.; Jurrius, K.H.M.; Zadoks, J.M.; Heugten, C.M.v. Case management after acquired brain injury compared to care as usual: Study protocol for a two-year pragmatic randomized controlled trial. Res. Sq. 2020. [Google Scholar] [CrossRef]
- World Health Organisation (WHO). International Classification of Functioning, Disability and Health; WHO: Geneva, Switzerland, 2001. [Google Scholar]
- Lifetime Care and Support Scheme (icare NSW). My Plan Manual. Available online: https://www.icare.nsw.gov.au/practitioners-and-providers/healthcare-and-service-providers/planning-with-an-injured-person (accessed on 15 January 2016).
- World Health Organization (WHO). International Classification of Functioning, Disability and Health. Available online: https://apps.who.int/classifications/icfbrowser/ (accessed on 10 January 2022).
- Cieza, A.; Fayed, N.; Bickenbach, J.; Prodringer, B. Refinements of the ICF Linking Rules to strengthen their potential for establishing comparability of health information. Disabil. Rehabil. 2016, 41, 574–583. [Google Scholar] [CrossRef]
- World Health Organization (WHO). Interntional Classification of Health Interventions—ICHI Beta-2. Available online: https://mitel.dimi.uniud.it/ichi/ (accessed on 10 November 2018).
- Lukersmith, S.; Croker, D.; Maclean, L.; Gleeson, R. My Plan—a new meso to micro level building block to promote person-centred care planning. Int. J. Integr. Care 2017, 17, A60. [Google Scholar] [CrossRef]
- Chung, Y.; Salvador-Carulla, L.; Salinas-Pérez, J.A.; Uriarte-Uriarte, J.J.; Iruin-Sanz, A.; García-Alonso, C.R. Use of the self-organising map network (SOMNet) as a decision support system for regional mental health planning. Health Res. Policy Syst. 2018, 16, 35. [Google Scholar] [CrossRef]
- Gibert, K.; García-Alonso, C.; Salvador-Carulla, L. Integrating clinicians, knowledge and data: Expert-based cooperative analysis in healthcare decision support. Health Res. Policy Syst. 2010, 30, 28. [Google Scholar] [CrossRef] [PubMed]
- Galderisi, S.; Rucci, P.; Kirkpatrick, B.; Mucci, A.; Gibertoni, D.; Rocca, P.; Rossi, A.; Bertolino, A.; Strauss, G.P.; Aguglia, E.; et al. Interplay Among Psychopathologic Variables, Personal Resources, Context-Related Factors, and Real-life Functioning in Individuals With Schizophrenia: A Network Analysis. JAMA Psychiatry 2018, 75, 396–404. [Google Scholar] [CrossRef]
- Luke, D.A.; Harris, J.K. Network analysis in public health: History, methods, and applications. Annu. Rev. Public Health 2007, 28, 69–93. [Google Scholar] [CrossRef] [PubMed]
- Chung, Y.J. The Self-Organising Map Network: An Interactive Visual Data Mining Framework for Exploratory Causal Analysis. Ph.D. Thesis, The University of Sydney, Camperdown, Australia, 2017. [Google Scholar]
- Hankins, R.; Peng, Y.; Yin, H. Somnet: Unsupervised feature learning networks for image classification. In Proceedings of International Joint Conference on Neural Networks, Rio de Janeiro, Brazil, 8–13 July 2018. [Google Scholar]
- Khan, F.; Baguley, I.; Cameron, I. Rehabilitation after traumatic brain injury Med. J. Aust. 2003, 178, 290–295. [Google Scholar] [CrossRef]
- Lannin, N.; Oates, J.; Cameron, I.; Goodall, S.; McCluskey, A.; Lukersmith, S. The Economic Cost of Attendant Care for Adults with Traumatic Brain and Spinal Cord Injury in NSW; University of Sydney: Sydney, Australia, 2012. [Google Scholar]
- Patrick, K. How can I help the student who is returning to school after a brain injury. NASN Sch. Nurse 2011, 26, 15–17. [Google Scholar] [CrossRef]
- McIntyre, M.; Ehrlich, C.; Kendall, E. Informal care management after traumatic brain injury: Perspectives on informal carer workload and capacity. Disabil. Rehabil. 2020, 42, 754–762. [Google Scholar] [CrossRef] [PubMed]
- WHO ICHI Development Project. International Classification of Health Interventions (ICHI) Alpha 2 Version 2013. Available online: http://sydney.edu.au/health-sciences/ncch/about.shtml (accessed on 10 November 2018).

| Case Management Actions and Definitions (Refer to the CMTaxonomy Intervention Tree) | Generalist Model | Person-Centred Model |
|---|---|---|
| Engagement^: Establish, develop, and maintain a relationship with the client. | X | X |
| Assessment: through listening and gathering information from other sources (e.g., reports from therapists, doctors, teachers, vocational professionals) | X | X |
| Holistic assessment: Assessment conducted by the case manager through observation of functioning, testing, and measurement of outcomes | X | |
| Person-centred planning: Supporting the person to develop their individualised plan including setting goals and identify support needs as well, as therapy and rehabilitation related goals | X | |
| Advising: Recommending a course to be followed, encourage change in functioning, environment, and attitude or behaviour to meet health needs and goals, and reduce risk | X | |
| Coordination: Case consultation, maintaining feedback, managing documentation | X | X |
| Proactive coordination: Including navigation, facilitation, advocacy for services, and extensive collaboration | X | |
| Education: Providing structured information to the person, and/or their family, other stakeholders in a manner conducive to improve knowledge about the persons’ condition, treatment, functioning, or strategies | X | |
| Training and skill development: Teaching, enhancing, or developing skills through context-specific practice to stakeholders | X | |
| Emotional(and Motivational) support: Providing the person (and others as appropriate) with comfort, empathy, or motivational support | X | |
| Monitoring: Continuous acquisition of information to evaluate the person’s situation to determine their progress, anticipate problems | X | X |
| Related actions: Actions that are less frequently performed to facilitate coordination (practical support and performing tasks—e.g., making a medical appointment). | X | X |
| Variable | N | % | Mean | Range | SD |
|---|---|---|---|---|---|
| Health Condition | |||||
| TBI | 75 | 70 | n/a * | n/a | n/a |
| SCI | 32 | 30 | n/a | n/a | n/a |
| Gender | |||||
| Male | 77 | 72 | n/a | n/a | n/a |
| Female | 39 | 28 | n/a | n/a | n/a |
| Age at injury | 107 | n/a | 32.2 | 8–96 years | 20.16 |
| Age at time of study | 107 | n/a | 45.8 | 19–106 years | 20.16 |
| Personal relationship | |||||
| Pre-injury | 58 | 54 | n/a | n/a | n/a |
| Year 2 | 53 | 49.4 | n/a | n/a | n/a |
| Year 5 | 49 | 45.9 | n/a | n/a | n/a |
| Year 10 | 39 | 36.4 | n/a | n/a | n/a |
| Phase Post Injury | Recovery Phase | Participation Phase | Maintenance Phase | |||
|---|---|---|---|---|---|---|
| ICF Domain | Number | % | Number | % | Number | % |
| Body functions and structures | 69 | 16 | 30 | 14.4 | 25 | 15.7 |
| Most frequent sub-domain | Neuro-musculoskeletal movement related, mental functions, sensory functions, and pain | Structures of the nervous system (e.g., parasympathetic nervous system) | No frequency pattern observed | |||
| Activities and participation | 206 | 48 | 135 | 65 | 104 | 66 |
| Most frequent sub-domain | Major life areas (i.e., education, work, managing money), self-care (looking after one’s health), mobility, general tasks and demands (e.g., undertaking multiple tasks, carrying out daily routine and handling stress) | Self-care (with a high frequency of maintaining one’s health 1), major life areas (education and employment), mobility, general tasks, and demands | Major life areas (acquiring, keeping and maintaining paid employment), self-care (changed focus to—diet and fitness and managing one’s health), community, social and civic life (recreation and leisure) | |||
| Environment | 114 | 26 | 18 | 8.6 | 19 | 12 |
| Most frequent sub-domain | Products and technology (specifically equipment activities of daily living) | Products and technology (for personal use) | Products and technology (for personal use) | |||
| Case management | 42 | 10 | 24 | 12 | 10 | 6.3 |
| Context Variable | Association with Mechanism (CM Actions and Intensity) |
|---|---|
| Age | In the first 5 years following injury, a person’s age at the time of the injury was associated with CM actions. In this cohort, the mean age of participants was 25 years old when injured in motor vehicle crashes. All Person-centred CM actions included in the analysis were used more frequently (holistic assessment, emotional and motivational support, education, training and skill development, advising, and proactive coordination). |
| Functioning impairment | The level of functioning and impairment and accident-related chronic pain were not associated with CM actions until year 10, when chronic pain and mental health were associated with the actions of the case manager. |
| Level of education | By year 5, there was an association of CM actions for those people who had completed secondary and tertiary education preinjury with all Person-centred CM actions, but not for those who completed vocational education. The reason could be due to the participant resuming life roles as most participants were in the Participation phase by year 5. Continuing up to the phase of maintaining health and wellbeing, being married and/or vocationally or tertiary educated at the time of accident were associated with CM actions of person-centred coordination and assessment. |
| Participant attitude | The participant’s faciliatory/positive attitude towards their own recovery had an association with the CM advising and coordination (but did not increase the costs). The association was not there for participants if they had a negative attitude towards their recovery. |
| Living with spouse/partner | Up to year 5, there was a strong association with CM action proactive coordination (navigating, facilitating, advocating, and collaboration) and the CM intensity was strongly associated when the participant was living with their spouse. The data showed that proactive coordination actions were less frequently performed when the participant lived with their spouse/partner rather than more. When the participant had a spouse/partner involved, the intensity was higher. Quite possibly the higher intensity is because of the complexity and dynamics of working with a couple in a household, and CM related to two people (there may also be children in the household). |
| Living alone | Intensity was also associated with people who were single and living alone at any phase in the recovery pathway. |
| Outcome Variable | Association with Mechanism (CM Actions and Intensity) |
|---|---|
| Progress on the pathway (progress along the recovery pathway from Recovery to Participation to Maintaining) | At all three phases in the recovery pathway (Recovery, Participation, and Maintaining), there were strong associations with all Person-centred CM actions. In particular, the Person-centred CM actions contributed to the participant reaching the Participation phase by the 2 years post injury period (78% of participants). This was reinforced by the association of CM intensity for participants who had reached either the Participation or Maintaining phases, in particular the CM action of advising. |
| Participation phase | In the Participation phase, there were associations with CM intensity and, CM actions of education, emotional support, proactive coordination (but not advising). The results consistently show that Person-centred CM model supports participants to progress along the recovery pathway particularly if the CM is involved in the early stages following their injury. |
| Maintaining health and wellbeing phase | When a participant continued to have CM involvement in year 10, all participants were in either the Participation or Maintaining phases. CM intensity was high for those in Participation and less intensity if in Maintaining. In the Maintaining phase, there was no association with continuous CM (versus intermittent CM) on other outcome variables measured in the study. The result suggests that by year 10 continuous CM (compared to intermittent CM) is not associated with other measured outcomes (e.g., further education). |
| There was an association between holistic assessment, stable accommodation (> 2 years) and intermittent CM. In these circumstances, the participant reached the Maintaining health and wellbeing phase. | |
| The intensity of case management, the length of time living in the current home, and intermittent CM were associated with the phase post injury (Participation and Maintaining). |
| Context Variable | Association with Mechanism (CM Actions and Intensity) |
|---|---|
| Level of spinal cord injury | In the first 2 years, following injury the CM actions of holistic assessment, advising, proactive coordination was associated with participants who had sustained a cervical SCI. Whereas with thoracic SCI there was a different configuration with holistic assessment, emotional support, and advising. There were no CM action associations with the lumbar SCI in this period. Over the next 2–5-year period, there was still an association with CM actions of holistic assessment and proactive coordination for people with cervical SCI, with thoracic SCI, American Spinal Cord Association Impairment Scale (ASIA) ASIA B and ASIA C participants having an additional association with CM action of education. Participants with lumbar SCI was associated with all six Person-centred CM actions. In the Participation phase for ASIA A there was only an association with proactive coordination, whereas ASIA D had an association with all six CM actions. |
| Motor and sensory function | In the first 2 years after injury, there was no association with the severity of motor and sensory spinal injury ASIA A 1 (complete no motor and sensory function below the level of injury), although there was an association with ASIA B (incomplete some sensory but no motor function) but only for CM education. For ASIA C (some limited motor function) the actions of assessment, emotional support, advising, and coordination were all significantly associated. However, there was no association with ASIA D (some motor weakness). |
| Functioning | For the first 5 years post injury, accident related-pain was associated with all Person-centred CM actions, and where there were accident-related mental health issues, the CM actions of assessment and proactive coordination. |
| Level of education | If the participant had vocational or tertiary education prior to their injury, there was an association with most Person-centred CM actions in the Participation phase. |
| Participant attitude | Participants with a positive attitude towards their recovery were associated with all Person-centred CM actions up until the Participation phase. At the 5-year period, if the participants’ attitude towards their recovery was negative, there was an association with CM actions of education and proactive coordination. |
| Living with spouse/partner | Holistic assessment action was associated with participants who were married living with their spouse. There was an even stronger association with holistic assessment for participants who were divorced. Case management costs were associated with who the participants lived with (their spouse, single, divorced, or living with their family of origin). CM proactive coordination was associated with Participation phase, but strongly associated with people who were divorced in the Recovery phase and less so people married and living with their spouse. |
| Living alone | Being single at the time of the accident was associated with all the Person-centred CM actions in the Participation phase. Participants who were single post injury were also associated CM actions of education, training, and skill development, advising in the first Recovery phase. |
| Outcome Variable | Association with Mechanism (CM Actions and Intensity) |
|---|---|
| Progress on the Pathway (progress along the recovery pathway from Recovery to Participation to Maintaining) | All participants considered to be in the Maintaining phase in Year 10 had a case manager involved, be it ongoing or intermittent. The most frequent CM action was proactive coordination (notably not coordination). This suggests a dependency of the participant on the CM. |
| Recovery phase | CM education, training, and skill development, advising in Recovery phase were associated with the target of the participant’s goals |
| Participation phase | CM intensity in year 5 was associated with the Participation phase. In the Participation phase there was high frequency of all CM actions with the most common CM action was proactive coordination. Holistic assessment action was associated with the participant being in the Participation phase. Proactive coordination was associated with goal rating in the Participation phase. |
| Maintaining health and wellbeing phase | There was an association with CM costs and goal rating, if the participant had reached the Maintaining life phase by year 5. This suggests that the involvement of the case manager is associated with the participant moving further along the recovery pathway within 5 years post injury. |
| For participants with SCI, most were in Maintaining phase by Year 5, with associations of all Person-centred CM actions and the plan period. However, only 6 of the 18 participants in the Maintaining phase were working, none were studying (including work preparation and voluntary work). Less than half had therefore established their occupational focus. By Year 10, there were no additional participants employed and only one additional participant had retired, and one was studying. | |
| CM action advising and coordination were associated with the Maintaining phase |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2023 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Lukersmith, S.; Salvador-Carulla, L.; Chung, Y.; Du, W.; Sarkissian, A.; Millington, M. A Realist Evaluation of Case Management Models for People with Complex Health Conditions Using Novel Methods and Tools—What Works, for Whom, and under What Circumstances? Int. J. Environ. Res. Public Health 2023, 20, 4362. https://doi.org/10.3390/ijerph20054362
Lukersmith S, Salvador-Carulla L, Chung Y, Du W, Sarkissian A, Millington M. A Realist Evaluation of Case Management Models for People with Complex Health Conditions Using Novel Methods and Tools—What Works, for Whom, and under What Circumstances? International Journal of Environmental Research and Public Health. 2023; 20(5):4362. https://doi.org/10.3390/ijerph20054362
Chicago/Turabian StyleLukersmith, Sue, Luis Salvador-Carulla, Younjin Chung, Wei Du, Anoush Sarkissian, and Michael Millington. 2023. "A Realist Evaluation of Case Management Models for People with Complex Health Conditions Using Novel Methods and Tools—What Works, for Whom, and under What Circumstances?" International Journal of Environmental Research and Public Health 20, no. 5: 4362. https://doi.org/10.3390/ijerph20054362
APA StyleLukersmith, S., Salvador-Carulla, L., Chung, Y., Du, W., Sarkissian, A., & Millington, M. (2023). A Realist Evaluation of Case Management Models for People with Complex Health Conditions Using Novel Methods and Tools—What Works, for Whom, and under What Circumstances? International Journal of Environmental Research and Public Health, 20(5), 4362. https://doi.org/10.3390/ijerph20054362







