Increased Prolonged Sitting in Patients with Rheumatoid Arthritis during the COVID-19 Pandemic: A Within-Subjects, Accelerometer-Based Study
Abstract
1. Introduction
2. Materials and Methods
2.1. Participants
2.2. Experimental Design
2.3. Physical Activity Level
2.4. Clinical Assessment
2.5. Statistical Analysis
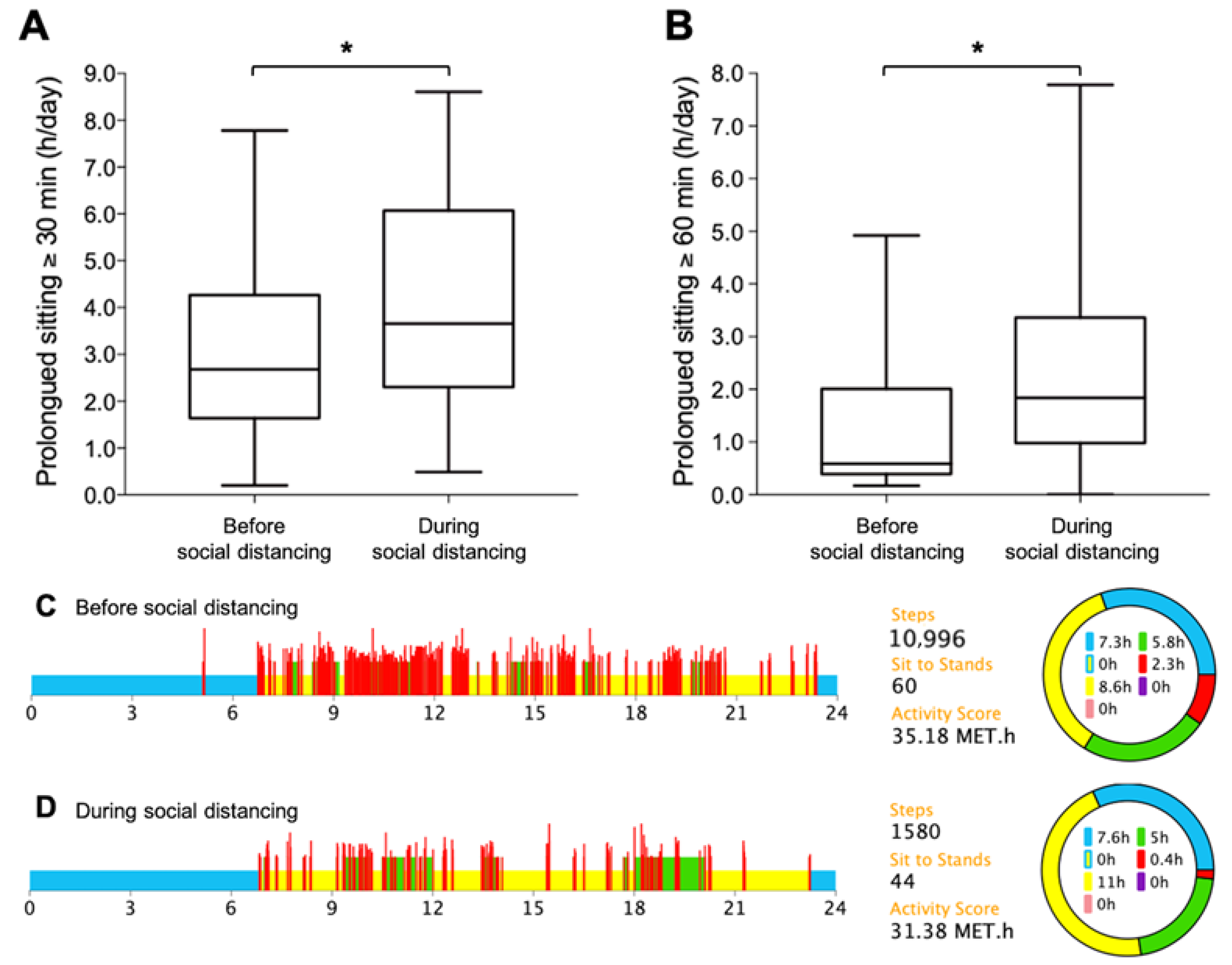
3. Results
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Tison, G.H.; Avram, R.; Kuhar, P.; Abreau, S.; Marcus, G.M.; Pletcher, M.J.; Olgin, J.E. Worldwide Effect of COVID-19 on Physical Activity: A Descriptive Study. Ann. Intern. Med. 2020, 173, 767–770. [Google Scholar] [CrossRef]
- Hall, G.; Laddu, D.R.; Phillips, S.A.; Lavie, C.J.; Arena, R. A tale of two pandemics: How will COVID-19 and global trends in physical inactivity and sedentary behavior affect one another? Prog. Cardiovasc. Dis. 2021, 64, 108–110. [Google Scholar] [CrossRef]
- Ammar, A.; Brach, M.; Trabelsi, K.; Chtourou, H.; Boukhris, O.; Masmoudi, L.; Bouaziz, B.; Bentlage, E.; How, D.; Ahmed, M.; et al. Effects of COVID-19 Home Confinement on Eating Behaviour and Physical Activity: Results of the ECLB-COVID19 International Online Survey. Nutrients 2020, 12, 1583. [Google Scholar] [CrossRef]
- Lee, I.M.; Shiroma, E.J.; Lobelo, F.; Puska, P.; Blair, S.N.; Katzmarzyk, P.T.; Lancet Physical Activity Series Working, G. Effect of physical inactivity on major non-communicable diseases worldwide: An analysis of burden of disease and life expectancy. Lancet 2012, 380, 219–229. [Google Scholar] [CrossRef]
- Chastin, S.; McGregor, D.; Palarea-Albaladejo, J.; Diaz, K.M.; Hagstromer, M.; Hallal, P.C.; van Hees, V.T.; Hooker, S.; Howard, V.J.; Lee, I.M.; et al. Joint association between accelerometry-measured daily combination of time spent in physical activity, sedentary behaviour and sleep and all-cause mortality: A pooled analysis of six prospective cohorts using compositional analysis. Br. J. Sports Med. 2021, 55, 1277–1285. [Google Scholar] [CrossRef]
- Ekelund, U.; Tarp, J.; Fagerland, M.W.; Johannessen, J.S.; Hansen, B.H.; Jefferis, B.J.; Whincup, P.H.; Diaz, K.M.; Hooker, S.; Howard, V.J.; et al. Joint associations of accelero-meter measured physical activity and sedentary time with all-cause mortality: A harmonised meta-analysis in more than 44 000 middle-aged and older individuals. Br. J. Sports Med. 2020, 54, 1499–1506. [Google Scholar] [CrossRef]
- Ekelund, U.; Tarp, J.; Steene-Johannessen, J.; Hansen, B.H.; Jefferis, B.; Fagerland, M.W.; Whincup, P.; Diaz, K.M.; Hooker, S.P.; Chernofsky, A.; et al. Dose-response associations between accelerometry measured physical activity and sedentary time and all cause mortality: Systematic review and harmonised meta-analysis. BMJ 2019, 366, l4570. [Google Scholar] [CrossRef]
- Diaz, K.M.; Howard, V.J.; Hutto, B.; Colabianchi, N.; Vena, J.E.; Safford, M.M.; Blair, S.N.; Hooker, S.P. Patterns of Sedentary Behavior and Mortality in U.S. Middle-Aged and Older Adults: A National Cohort Study. Ann. Intern. Med. 2017, 167, 465–475. [Google Scholar] [CrossRef]
- Nicholas, J.A.; Lo Siou, G.; Lynch, B.M.; Robson, P.J.; Friedenreich, C.M.; Csizmadi, I. Leisure-Time Physical Activity Does not Attenuate the Association Between Occupational Sedentary Behavior and Obesity: Results From Alberta’s Tomorrow Project. J. Phys. Act. Health 2015, 12, 1589–1600. [Google Scholar] [CrossRef]
- van der Berg, J.D.; Stehouwer, C.D.; Bosma, H.; van der Velde, J.H.; Willems, P.J.; Savelberg, H.H.; Schram, M.T.; Sep, S.J.; van der Kallen, C.J.; Henry, R.M.; et al. Associations of total amount and patterns of sedentary behaviour with type 2 diabetes and the metabolic syndrome: The Maastricht Study. Diabetologia 2016, 59, 709–718. [Google Scholar] [CrossRef]
- Wilmot, E.G.; Edwardson, C.L.; Achana, F.A.; Davies, M.J.; Gorely, T.; Gray, L.J.; Khunti, K.; Yates, T.; Biddle, S.J. Sedentary time in adults and the association with diabetes, cardiovascular disease and death: Systematic review and meta-analysis. Diabetologia 2012, 55, 2895–2905. [Google Scholar] [CrossRef] [PubMed]
- Patterson, R.; McNamara, E.; Tainio, M.; de Sa, T.H.; Smith, A.D.; Sharp, S.J.; Edwards, P.; Woodcock, J.; Brage, S.; Wijndaele, K. Sedentary behaviour and risk of all-cause, cardiovascular and cancer mortality, and incident type 2 diabetes: A systematic review and dose response meta-analysis. Eur. J. Epidemiol. 2018, 33, 811–829. [Google Scholar] [CrossRef] [PubMed]
- Engelen, L.; Gale, J.; Chau, J.Y.; Hardy, L.L.; Mackey, M.; Johnson, N.; Shirley, D.; Bauman, A. Who is at risk of chronic disease? Associations between risk profiles of physical activity, sitting and cardio-metabolic disease in Australian adults. Aust. N. Z. J. Public Health 2017, 41, 178–183. [Google Scholar] [CrossRef] [PubMed]
- Lynch, B.M. Sedentary behavior and cancer: A systematic review of the literature and proposed biological mechanisms. Cancer Epidemiol. Biomark. Prev. 2010, 19, 2691–2709. [Google Scholar] [CrossRef] [PubMed]
- Matthews, C.E.; George, S.M.; Moore, S.C.; Bowles, H.R.; Blair, A.; Park, Y.; Troiano, R.P.; Hollenbeck, A.; Schatzkin, A. Amount of time spent in sedentary behaviors and cause-specific mortality in US adults. Am. J. Clin. Nutr. 2012, 95, 437–445. [Google Scholar] [CrossRef] [PubMed]
- Falck, R.S.; Davis, J.C.; Liu-Ambrose, T. What is the association between sedentary behaviour and cognitive function? A systematic review. Br. J. Sports Med. 2016, 51, 800–811. [Google Scholar] [CrossRef]
- Dempsey, P.C.; Strain, T.; Winkler, E.A.H.; Westgate, K.; Rennie, K.L.; Wareham, N.J.; Brage, S.; Wijndaele, K. Association of Accelerometer-Measured Sedentary Accumulation Patterns With Incident Cardiovascular Disease, Cancer, and All-Cause Mortality. J. Am. Heart Assoc. 2022, 11, e023845. [Google Scholar] [CrossRef]
- Biswas, A.; Oh, P.I.; Faulkner, G.E.; Bajaj, R.R.; Silver, M.A.; Mitchell, M.S.; Alter, D.A. Sedentary time and its association with risk for disease incidence, mortality, and hospitalization in adults: A systematic review and meta-analysis. Ann. Intern. Med. 2015, 162, 123–132. [Google Scholar] [CrossRef]
- Katzmarzyk, P.T.; Powell, K.E.; Jakicic, J.M.; Troiano, R.P.; Piercy, K.; Tennant, B.; Physical Activity Guidelines Advisory, C. Sedentary Behavior and Health: Update from the 2018 Physical Activity Guidelines Advisory Committee. Med. Sci. Sports Exerc. 2019, 51, 1227–1241. [Google Scholar] [CrossRef]
- Ekelund, U.; Steene-Johannessen, J.; Brown, W.J.; Fagerland, M.W.; Owen, N.; Powell, K.E.; Bauman, A.; Lee, I.M.; Lancet Physical Activity Series 2 Executive, C.; Lancet Sedentary Behaviour Working, G. Does physical activity attenuate, or even eliminate, the detrimental association of sitting time with mortality? A harmonised meta-analysis of data from more than 1 million men and women. Lancet 2016, 388, 1302–1310. [Google Scholar] [CrossRef]
- Scott, D.L.; Wolfe, F.; Huizinga, T.W. Rheumatoid arthritis. Lancet 2010, 376, 1094–1108. [Google Scholar] [CrossRef]
- Lee, D.M.; Weinblatt, M.E. Rheumatoid arthritis. Lancet 2001, 358, 903–911. [Google Scholar] [CrossRef]
- Pincus, T. Long-term outcomes in rheumatoid arthritis. Br. J. Rheumatol. 1995, 34 (Suppl. S2), 59–73. [Google Scholar] [CrossRef] [PubMed]
- Gabriel, S.E. Cardiovascular morbidity and mortality in rheumatoid arthritis. Am. J. Med. 2008, 121, 9–14. [Google Scholar] [CrossRef] [PubMed]
- Sarzi-Puttini, P.; Atzeni, F.; Gerli, R.; Bartoloni, E.; Doria, A.; Barskova, T.; Matucci-Cerinic, M.; Sitia, S.; Tomasoni, L.; Turiel, M. Cardiac involvement in systemic rheumatic diseases: An update. Autoimmun. Rev. 2010, 9, 849–852. [Google Scholar] [CrossRef] [PubMed]
- Hollan, I.; Meroni, P.L.; Ahearn, J.M.; Cohen Tervaert, J.W.; Curran, S.; Goodyear, C.S.; Hestad, K.A.; Kahaleh, B.; Riggio, M.; Shields, K.; et al. Cardiovascular disease in autoimmune rheumatic diseases. Autoimmun. Rev. 2013, 12, 1004–1015. [Google Scholar] [CrossRef] [PubMed]
- Rausch Osthoff, A.K.; Niedermann, K.; Braun, J.; Adams, J.; Brodin, N.; Dagfinrud, H.; Duruoz, T.; Esbensen, B.A.; Gunther, K.P.; Hurkmans, E.; et al. 2018 EULAR recommendations for physical activity in people with inflammatory arthritis and osteoarthritis. Ann. Rheum. Dis. 2018, 77, 1251–1260. [Google Scholar] [CrossRef] [PubMed]
- Pinto, A.J.; Roschel, H.; de Sa Pinto, A.L.; Lima, F.R.; Pereira, R.M.R.; Silva, C.A.; Bonfa, E.; Gualano, B. Physical inactivity and sedentary behavior: Overlooked risk factors in autoimmune rheumatic diseases? Autoimmun. Rev. 2017, 16, 667–674. [Google Scholar] [CrossRef] [PubMed]
- Pinto, A.J.; Dunstan, D.W.; Owen, N.; Bonfa, E.; Gualano, B. Combating physical inactivity during the COVID-19 pandemic. Nat. Rev. Rheumatol. 2020, 16, 347–348. [Google Scholar] [CrossRef]
- Henchoz, Y.; Bastardot, F.; Guessous, I.; Theler, J.M.; Dudler, J.; Vollenweider, P.; So, A. Physical activity and energy expenditure in rheumatoid arthritis patients and matched controls. Rheumatology 2012, 51, 1500–1507. [Google Scholar] [CrossRef]
- Yu, C.A.; Rouse, P.C.; Veldhuijzen Van Zanten, J.J.; Ntoumanis, N.; Kitas, G.D.; Duda, J.L.; Metsios, G.S. Subjective and objective levels of physical activity and their association with cardiorespiratory fitness in rheumatoid arthritis patients. Arthritis Res. Ther. 2015, 17, 59. [Google Scholar] [CrossRef] [PubMed]
- Huffman, K.M.; Pieper, C.F.; Hall, K.S.; St Clair, E.W.; Kraus, W.E. Self-efficacy for exercise, more than disease-related factors, is associated with objectively assessed exercise time and sedentary behaviour in rheumatoid arthritis. Scand. J. Rheumatol. 2015, 44, 106–110. [Google Scholar] [CrossRef] [PubMed]
- Zhong, J.; Shen, G.; Yang, H.; Huang, A.; Chen, X.; Dong, L.; Wu, B.; Zhang, A.; Su, L.; Hou, X.; et al. COVID-19 in patients with rheumatic disease in Hubei province, China: A multicentre retrospective observational study. Lancet Rheumatol. 2020, 2, e557–e564. [Google Scholar] [CrossRef]
- Aletaha, D.; Neogi, T.; Silman, A.J.; Funovits, J.; Felson, D.T.; Bingham, C.O., 3rd; Birnbaum, N.S.; Burmester, G.R.; Bykerk, V.P.; Cohen, M.D.; et al. 2010 Rheumatoid arthritis classification criteria: An American College of Rheumatology/European League Against Rheumatism collaborative initiative. Arthritis Rheum. 2010, 62, 2569–2581. [Google Scholar] [CrossRef] [PubMed]
- Tudor-Locke, C.; Sisson, S.B.; Collova, T.; Lee, S.M.; Swan, P.D. Pedometer-determined step count guidelines for classifying walking intensity in a young ostensibly healthy population. Can. J. Appl. Physiol. 2005, 30, 666–676. [Google Scholar] [CrossRef] [PubMed]
- Prevoo, M.L.; van′t Hof, M.A.; Kuper, H.H.; van Leeuwen, M.A.; van de Putte, L.B.; van Riel, P.L. Modified disease activity scores that include twenty-eight-joint counts. Development and validation in a prospective longitudinal study of patients with rheumatoid arthritis. Arthritis Rheum. 1995, 38, 44–48. [Google Scholar] [CrossRef]
- Aletaha, D.; Smolen, J. The Simplified Disease Activity Index (SDAI) and the Clinical Disease Activity Index (CDAI): A review of their usefulness and validity in rheumatoid arthritis. Clin. Exp. Rheumatol. 2005, 23, S100–S108. [Google Scholar]
- Ferraz, M.B.; Oliveira, L.M.; Araujo, P.M.; Atra, E.; Tugwell, P. Crosscultural reliability of the physical ability dimension of the health assessment questionnaire. J. Rheumatol. 1990, 17, 813–817. [Google Scholar]
- Price, D.D.; Bush, F.M.; Long, S.; Harkins, S.W. A comparison of pain measurement characteristics of mechanical visual analogue and simple numerical rating scales. Pain 1994, 56, 217–226. [Google Scholar] [CrossRef]
- Pouchot, J.; Kherani, R.B.; Brant, R.; Lacaille, D.; Lehman, A.J.; Ensworth, S.; Kopec, J.; Esdaile, J.M.; Liang, M.H. Determination of the minimal clinically important difference for seven fatigue measures in rheumatoid arthritis. J. Clin. Epidemiol. 2008, 61, 705–713. [Google Scholar] [CrossRef]
- Ciconelli, R.M.; Ferraz, M.B.; Santos, W.; Meinão, I.; Quaresma, M.R. Brazilian-Portuguese version of the SF-36. A reliable and valid quality of life outcome measure. Rev. Bras. Rheumatol. 1999, 39, 8. [Google Scholar]
- Freiberg, A.; Schubert, M.; Romero Starke, K.; Hegewald, J.; Seidler, A. A Rapid Review on the Influence of COVID-19 Lockdown and Quarantine Measures on Modifiable Cardiovascular Risk Factors in the General Population. Int. J. Environ. Res. Public Health 2021, 18, 8567. [Google Scholar] [CrossRef]
- Silva, D.R.; Werneck, A.O.; Malta, D.C.; Souza-Junior, P.R.B.; Azevedo, L.O.; Barros, M.B.A.; Szwarcwald, C.L. Incidence of physical inactivity and excessive screen time during the first wave of the COVID-19 pandemic in Brazil: What are the most affected population groups? Ann. Epidemiol. 2021, 62, 30–35. [Google Scholar] [CrossRef]
- Silva, D.; Werneck, A.O.; Malta, D.C.; Souza Junior, P.R.B.; Azevedo, L.O.; Barros, M.B.A.; Szwarcwald, C.L. Changes in the prevalence of physical inactivity and sedentary behavior during COVID-19 pandemic: A survey with 39,693 Brazilian adults. Cad. Saude Publica 2021, 37, e00221920. [Google Scholar] [CrossRef]
- Booth, F.W.; Roberts, C.K.; Thyfault, J.P.; Ruegsegger, G.N.; Toedebusch, R.G. Role of Inactivity in Chronic Diseases: Evolutionary Insight and Pathophysiological Mechanisms. Physiol. Rev. 2017, 97, 1351–1402. [Google Scholar] [CrossRef]
- Bellettiere, J.; Winkler, E.A.H.; Chastin, S.F.M.; Kerr, J.; Owen, N.; Dunstan, D.W.; Healy, G.N. Associations of sitting accumulation patterns with cardio-metabolic risk biomarkers in Australian adults. PLoS ONE 2017, 12, e0180119. [Google Scholar] [CrossRef]
- van Dijk, S.B.; Takken, T.; Prinsen, E.C.; Wittink, H. Different anthropometric adiposity measures and their association with cardiovascular disease risk factors: A meta-analysis. Neth Heart J 2012, 20, 208–218. [Google Scholar] [CrossRef]
- Pedersen, B.K.; Saltin, B. Exercise as medicine—Evidence for prescribing exercise as therapy in 26 different chronic diseases. Scand. J. Med. Sci. Sports 2015, 25 (Suppl. S3), 1–72. [Google Scholar] [CrossRef] [PubMed]
- Benatti, F.B.; Pedersen, B.K. Exercise as an anti-inflammatory therapy for rheumatic diseases-myokine regulation. Nat. Rev. Rheumatol. 2015, 11, 86–97. [Google Scholar] [CrossRef] [PubMed]
- Saunders, T.J.; Atkinson, H.F.; Burr, J.; MacEwen, B.; Skeaff, C.M.; Peddie, M.C. The Acute Metabolic and Vascular Impact of Interrupting Prolonged Sitting: A Systematic Review and Meta-Analysis. Sports Med. 2018, 48, 2347–2366. [Google Scholar] [CrossRef] [PubMed]
- Fenton, S.A.M.; Veldhuijzen van Zanten, J.; Kitas, G.D.; Duda, J.L.; Rouse, P.C.; Yu, C.A.; Metsios, G.S. Sedentary behaviour is associated with increased long-term cardiovascular risk in patients with rheumatoid arthritis independently of moderate-to-vigorous physical activity. BMC Musculoskelet. Disord. 2017, 18, 131. [Google Scholar] [CrossRef] [PubMed]
- Pinto, A.J.; Meireles, K.; Pecanha, T.; Mazzolani, B.C.; Smaira, F.I.; Rezende, D.; Benatti, F.B.; Ribeiro, A.C.M.; Pinto, A.L.S.; Lima, F.R.; et al. Acute cardiometabolic effects of brief active breaks in sitting for patients with rheumatoid arthritis. Am. J. Physiol. Endocrinol. Metab. 2021, 321, E782–E794. [Google Scholar] [CrossRef] [PubMed]
- Ryan, S.; Campbell, P.; Paskins, Z.; Hider, S.; Manning, F.; Rule, K.; Brooks, M.; Hassell, A. Exploring the physical, psychological and social well-being of people with rheumatoid arthritis during the coronavirus pandemic: A single-centre, longitudinal, qualitative interview study in the UK. BMJ Open 2022, 12, e056555. [Google Scholar] [CrossRef] [PubMed]
| Variable | n = 35 |
|---|---|
| Age, years | 60.9 (58.0 to 63.7) |
| BMI, kg/m² | 29.5 (27.2 to 31.9) |
| Disease Activity Score (DAS28 PCR) | 3.4 (2.9 to 3.8) |
| Clinical Disease Activity Index (CDAI) | 10.1 (6.7 to 13.4) |
| Health Assessment Questionnaire (HAQ) | 1.2 (0.9 to 1.4) |
| C-reactive protein, mg/L | 10.8 (5.5 to 16.2) |
| Erythrocyte sedimentation rate, mm/H | 28.4 (15.7 to 41.1) |
| Disease duration, years | 18.5 (14.7 to 22.3) |
| Comorbidities, n (%) | |
| Hypertension | 18 (51.4%) |
| Dyslipidemias | 17 (48.6%) |
| Type 2 diabetes | 12 (34.3%) |
| Fibromyalgia | 11 (31.4%) |
| Other rheumatic diseases | 18 (51.4%) |
| Depression | 7 (20.0%) |
| Medication, n (%) | |
| DMARDs | 30 (85.7%) |
| Leflunomide | 19 (54.3%) |
| Methotrexate | 16 (45.7%) |
| Prednisone | 26 (74.3%) |
| Biological agents | 12 (34.3%) |
| Anti-inflammatory drugs | 11 (31.4%) |
| Pain killers | 20 (57.1%) |
| Antihypertensive drugs | 18 (51.4%) |
| Antihyperlipidemic drugs | 17 (48.6%) |
| Antidiabetic drugs | 12 (34.3%) |
| Anti-depressants | 14 (40.0%) |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2023 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Pinto, A.J.; Rezende, D.; Sieczkowska, S.M.; Meireles, K.; Bonfiglioli, K.; Ribeiro, A.C.d.M.; Bonfá, E.; Owen, N.; Dunstan, D.W.; Roschel, H.; et al. Increased Prolonged Sitting in Patients with Rheumatoid Arthritis during the COVID-19 Pandemic: A Within-Subjects, Accelerometer-Based Study. Int. J. Environ. Res. Public Health 2023, 20, 3944. https://doi.org/10.3390/ijerph20053944
Pinto AJ, Rezende D, Sieczkowska SM, Meireles K, Bonfiglioli K, Ribeiro ACdM, Bonfá E, Owen N, Dunstan DW, Roschel H, et al. Increased Prolonged Sitting in Patients with Rheumatoid Arthritis during the COVID-19 Pandemic: A Within-Subjects, Accelerometer-Based Study. International Journal of Environmental Research and Public Health. 2023; 20(5):3944. https://doi.org/10.3390/ijerph20053944
Chicago/Turabian StylePinto, Ana Jessica, Diego Rezende, Sofia Mendes Sieczkowska, Kamila Meireles, Karina Bonfiglioli, Ana Cristina de Medeiros Ribeiro, Eloisa Bonfá, Neville Owen, David W. Dunstan, Hamilton Roschel, and et al. 2023. "Increased Prolonged Sitting in Patients with Rheumatoid Arthritis during the COVID-19 Pandemic: A Within-Subjects, Accelerometer-Based Study" International Journal of Environmental Research and Public Health 20, no. 5: 3944. https://doi.org/10.3390/ijerph20053944
APA StylePinto, A. J., Rezende, D., Sieczkowska, S. M., Meireles, K., Bonfiglioli, K., Ribeiro, A. C. d. M., Bonfá, E., Owen, N., Dunstan, D. W., Roschel, H., & Gualano, B. (2023). Increased Prolonged Sitting in Patients with Rheumatoid Arthritis during the COVID-19 Pandemic: A Within-Subjects, Accelerometer-Based Study. International Journal of Environmental Research and Public Health, 20(5), 3944. https://doi.org/10.3390/ijerph20053944








