Prevalence and Determinants of Excessive Screen Viewing Time in Children Aged 3–15 Years and Its Effects on Physical Activity, Sleep, Eye Symptoms and Headache
Abstract
1. Introduction
2. Materials and Methods
2.1. Sample Size Calculation
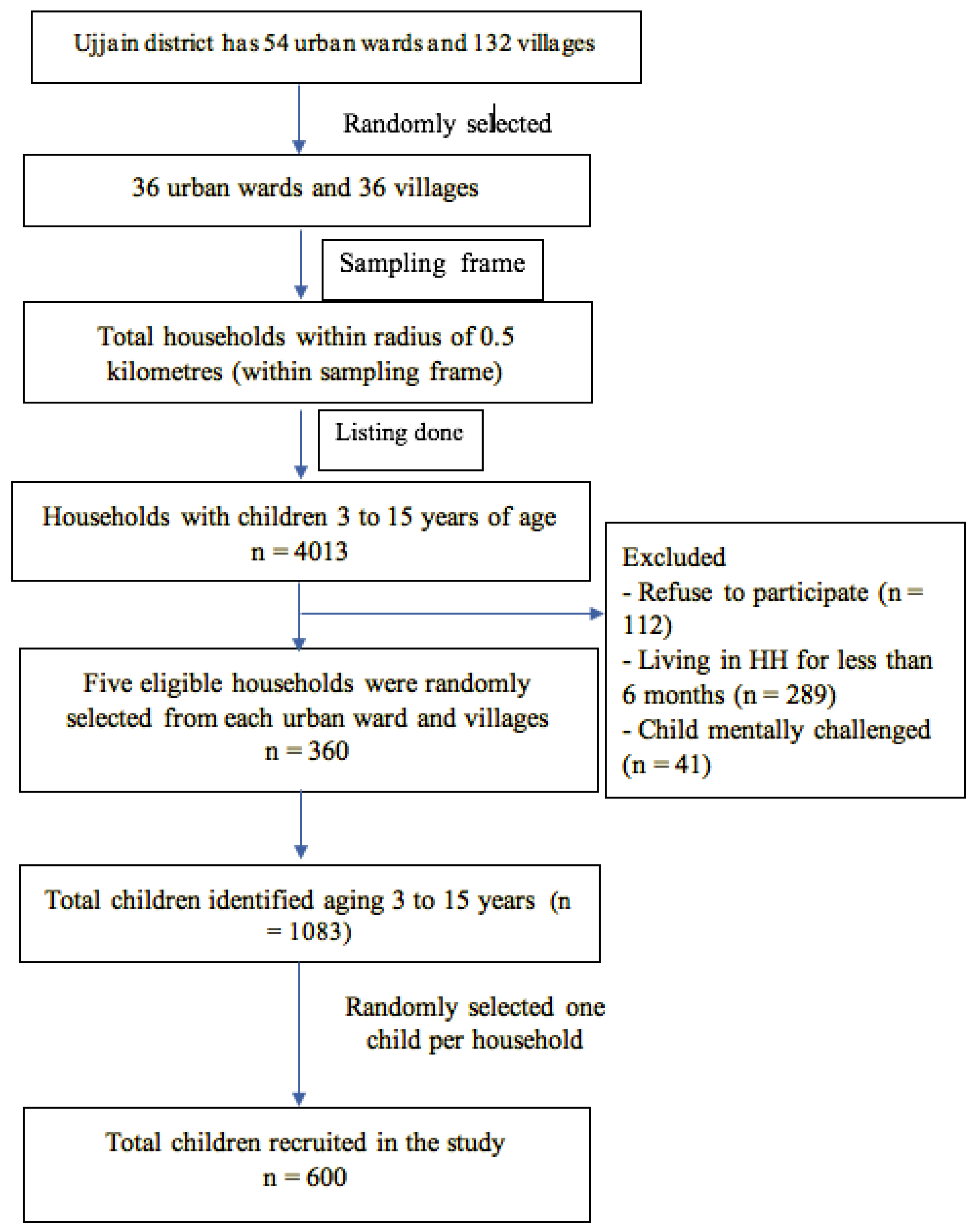
2.2. Sampling Procedure
2.3. Statistical Method
3. Results
4. Discussion
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Barber, S.E.; Kelly, B.; Collings, P.J.; Nagy, L.; Bywater, T.; Wright, J. Prevalence, Trajectories, and Determinants of Television Viewing Time in an Ethnically Diverse Sample of Young Children from the UK. Int. J. Behav. Nutr. Phys. Act. 2016, 14, 88. [Google Scholar] [CrossRef] [PubMed]
- Council on Communications and Media. Media and Young Minds. Pediatrics 2016, 138, e20162591. [Google Scholar] [CrossRef] [PubMed]
- Buchanan, L.R.; Rooks-Peck, C.R.; Finnie, R.K.; Wethington, H.R.; Jacob, V.; Fulton, J.E.; Johnson, D.B.; Kahwati, L.C.; Pratt, C.A.; Ramirez, G.; et al. Reducing Recreational Sedentary Screen Time: A Community Guide Systematic Review. Am. J. Prev. Med. 2016, 50, 402–415. [Google Scholar] [CrossRef] [PubMed]
- Stiglic, N.; Viner, R.M. Effects of Screentime on the Health and Well-Being of Children and Adolescents: A Systematic Review of Reviews. BMJ Open 2019, 9, e023191. [Google Scholar] [CrossRef]
- Torjesen, I. Parents Should Decide When Children’s Screen Time Is Too High, Says First Uk Guidance. BMJ 2019, 364, l60. [Google Scholar] [CrossRef]
- Zhu, R.; Fang, H.; Chen, M.; Hu, X.; Cao, Y.; Yang, F.; Xia, K. Screen Time and Sleep Disorder in Preschool Children: Identifying the Safe Threshold in a Digital World. Public Health 2020, 186, 204–210. [Google Scholar] [CrossRef]
- WHO 2010, Global Recommendations on Physical Activity for Health. WHO Press, World Health Organization, 20 Avenue Appia, 1211 Geneva 27, Switzerland. Available online: https://www.who.int/publications/i/item/9789241599979 (accessed on 14 February 2023).
- Council on Communications and Media. Media Use in School-Aged Children and Adolescents. Pediatrics 2016, 138, e20162592. [Google Scholar] [CrossRef]
- Domingues-Montanari, S. Clinical and Psychological Effects of Excessive Screen Time on Children. J. Paediatr. Child Health 2017, 53, 333–338. [Google Scholar] [CrossRef]
- Makin, S. Searching for Digital Technology’s Effects on Well-Being. Nature 2018, 563, S138–S140. [Google Scholar] [CrossRef]
- Nguyen, P.; Le, L.K.; Nguyen, D.; Gao, L.; Dunstan, D.W.; Moodie, M. The Effectiveness of Sedentary Behaviour Interventions on Sitting Time and Screen Time in Children and Adults: An Umbrella Review of Systematic Reviews. Int. J. Behav. Nutr. Phys. Act. 2020, 17, 117. [Google Scholar] [CrossRef]
- Tähkämö, L.; Partonen, T.; Pesonen, A.-K. Systematic Review of Light Exposure Impact on Human Circadian Rhythm. Chronobiol. Int. 2019, 36, 151–170. [Google Scholar] [CrossRef] [PubMed]
- Hale, L.; Guan, S. Screen Time and Sleep among School-Aged Children and Adolescents: A Systematic Literature Review. Sleep Med. Rev. 2015, 21, 50–58. [Google Scholar] [CrossRef] [PubMed]
- Caksen, H. Electronic Screen Exposure and Headache in Children. Ann. Indian Acad. Neurol. 2021, 24, 8–10. [Google Scholar] [PubMed]
- Kaka, N.; Madgavkar, A.; Kshirsagar, A.; Gupta, R.; Manyika, J.; Bahl, K.; Gupta, S. Digital India: Technology to Transform a Connected Nation; India McKinsey Global Institute: New Delhi, India, 2019. [Google Scholar]
- WHO 2015. Vaccination Coverage Cluster Surveys: Reference Manual (Version 3, Working Draft, Updated July 2015). Available online: http://www.who.int/immunization/monitoring_surveillance/routine/coverage/en/index2.html (accessed on 14 February 2023).
- Nimbalkar, S.M.; Shah, R.R.; Fahey, N.M.; Soni, A.V.; Phatak, A.G. Screen Time Usage among Preschoolers Aged 2–6 in Rural Western India: A Cross-Sectional Study. J. Fam. Med. Prim. 2019, 8, 1999–2002. [Google Scholar] [CrossRef]
- NHFS-4. National Family Health Survey-4-Ministry of Health and Family Welfare, Government of India, International Institute for Population Sciences, Mumbai. 2015-16. Available online: http://rchiips.org/nfhs/pdf/NFHS4/MP_FactSheet.pdf (accessed on 14 February 2023).
- Gupta, P.; Shah, D.; Bedi, N.; Galagali, P.; Dalwai, S.; Agrawal, S.; John, J.J.; Mahajan, V.; Meena, P.; Mittal, H.G.; et al. Indian Academy of Pediatrics Guidelines on Screen Time and Digital Wellness in Infants, Children and Adolescents. Indian Pediatr. 2022, 59, 235–244. [Google Scholar] [CrossRef]
- Caylan, N.; Yalcin, S.S.; Nergiz, M.E.; Yildiz, D.; Oflu, A.; Tezol, O.; Cicek, S.; Foto-Ozdemir, D. Associations between Parenting Styles and Excessive Screen Usage in Preschool Children. Turk. Arch. Pediatr. 2021, 56, 261–266. [Google Scholar]
- Baiden, P.; Tadeo, S.K.; Peters, K.E. The Association between Excessive Screen-Time Behaviors and Insufficient Sleep among Adolescents: Findings from the 2017 Youth Risk Behavior Surveillance System. Psychiatry Res. 2019, 281, 112586. [Google Scholar] [CrossRef]
- Eyimaya, A.O.; Irmak, A.Y. Relationship between Parenting Practices and Children’s Screen Time During the Covid-19 Pandemic in Turkey. J. Pediatr. Nurs. 2021, 56, 24–29. [Google Scholar] [CrossRef]
- McArthur, B.A.; Racine, N.; Browne, D.; McDonald, S.; Tough, S.; Madigan, S. Recreational Screen Time before and During Covid-19 in School-Aged Children. Acta Paediatr. 2021, 110, 2805–2807. [Google Scholar] [CrossRef]
- Bergmann, C.; Dimitrova, N.; Alaslani, K.; Almohammadi, A.; Alroqi, H.; Aussems, S.; Barokova, M.; Davies, C.; Gonzalez-Gomez, N.; Gibson, S.P.; et al. Young Children’s Screen Time During the First Covid-19 Lockdown in 12 Countries. Sci. Rep. 2022, 12, 2015. [Google Scholar] [CrossRef]
- Chwalczynska, A.; Andrzejewski, W. Changes in Body Mass and Composition of the Body as Well as Physical Activity and Time Spent in Front of the Monitor by Students of the Wroclaw University of Health and Sport Sciences During the Period of Covid-19 Restrictions. Int. J. Environ. Res. Public Health 2021, 18, 7801. [Google Scholar] [CrossRef] [PubMed]
- Dubey, M.; Nongkynrih, B.; Gupta, S.K.; Kalaivani, M.; Goswami, A.K.; Salve, H.R. Screen-Based Media Use and Screen Time Assessment among Adolescents Residing in an Urban Resettlement Colony in New Delhi, India. J. Fam. Med. Prim. Care 2018, 7, 1236–1242. [Google Scholar] [CrossRef] [PubMed]
- Ye, S.; Chen, L.; Wang, Q.; Li, Q. Correlates of Screen Time among 8-19-Year-Old Students in China. BMC Public Health 2018, 18, 467. [Google Scholar] [CrossRef] [PubMed]
- Lee, S.T.; Wong, J.E.; Shanita, S.N.; Ismail, M.N.; Deurenberg, P.; Poh, B.K. Daily Physical Activity and Screen Time, but Not Other Sedentary Activities, Are Associated with Measures of Obesity During Childhood. Int. J. Environ. Res. Public Health 2014, 12, 146–161. [Google Scholar] [CrossRef] [PubMed]
- Cerasoli, C.P.; Nicklin, J.M.; Ford, M.T. Intrinsic Motivation and Extrinsic Incentives Jointly Predict Performance: A 40-Year Meta-Analysis. Psychol. Bull. 2014, 140, 980–1008. [Google Scholar] [CrossRef] [PubMed]
- Kaur, N.; Gupta, M.; Malhi, P.; Grover, S. Screen Time in under-Five Children. Indian Pediatr. 2019, 56, 773–788. [Google Scholar] [CrossRef] [PubMed]
- Varadarajan, S.; Venguidesvarane, A.G.; Ramaswamy, K.N.; Rajamohan, M.; Krupa, M.; Christadoss, S.B.W. Prevalence of Excessive Screen Time and Its Association with Developmental Delay in Children Aged <5 Years: A Population-Based Cross-Sectional Study in India. PLoS ONE 2021, 16, e0254102. [Google Scholar]
- Mannikko, N.; Ruotsalainen, H.; Miettunen, J.; Marttila-Tornio, K.; Kaariainen, M. Parental Socioeconomic Status, Adolescents’ Screen Time and Sports Participation through Externalizing and Internalizing Characteristics. Heliyon 2020, 6, e03415. [Google Scholar] [CrossRef]
- Mineshita, Y.; Kim, H.K.; Chijiki, H.; Nanba, T.; Shinto, T.; Furuhashi, S.; Oneda, S.; Kuwahara, M.; Suwama, A.; Shibata, S. Screen Time Duration and Timing: Effects on Obesity, Physical Activity, Dry Eyes, and Learning Ability in Elementary School Children. BMC Public Health 2021, 21, 422. [Google Scholar] [CrossRef]
- LeBourgeois, M.K.; Hale, L.; Chang, A.-M.; Akacem, L.D.; Montgomery-Downs, H.E.; Buxton, O.M. Digital Media and Sleep in Childhood and Adolescence. Pediatrics 2017, 140 (Suppl. 2), S92–S96. [Google Scholar] [CrossRef]
- Paruthi, S.; Brooks, L.J.; D’Ambrosio, C.; Hall, W.A.; Kotagal, S.; Lloyd, R.M.; Malow, B.A.; Maski, K.; Nichols, C.; Quan, S.F.; et al. Consensus Statement of the American Academy of Sleep Medicine on the Recommended Amount of Sleep for Healthy Children: Methodology and Discussion. J. Clin. Sleep Med. 2016, 12, 1549–1561. [Google Scholar] [CrossRef] [PubMed]
- Gentile, D.A.; Berch, O.N.; Choo, H.; Khoo, A.; Walsh, D.A. Bedroom Media: One Risk Factor for Development. Dev. Psychol. 2017, 53, 2340–2355. [Google Scholar] [CrossRef] [PubMed]
- Garmy, P.; Nyberg, P.; Jakobsson, U. Sleep and Television and Computer Habits of Swedish School-Age Children. J. Sch. Nurs. 2012, 28, 469–476. [Google Scholar] [CrossRef] [PubMed]
- Johnson, J.G.; Cohen, P.; Kasen, S.; Brook, J.S. Extensive Television Viewing and the Development of Attention and Learning Difficulties During Adolescence. Arch. Pediatr. Adolesc. Med. 2007, 161, 480–486. [Google Scholar] [CrossRef]
- Vandewater, E.A.; Bickham, D.S.; Lee, J.H. Time Well Spent? Relating Television Use to Children’s Free-Time Activities. Pediatrics 2006, 117, e181–e191. [Google Scholar] [CrossRef]
- Fang, K.; Mu, M.; Liu, K.; He, Y. Screen Time and Childhood Overweight/Obesity: A Systematic Review and Meta-Analysis. Child Care Health Dev. 2019, 45, 744–753. [Google Scholar] [CrossRef]
- Redmayne, M.; Smith, E.; Abramson, M.J. The Relationship between Adolescents’ Well-Being and Their Wireless Phone Use: A Cross-Sectional Study. Environ. Health 2013, 12, 90. [Google Scholar] [CrossRef]
- Xavier, M.K.; Pitangui, A.C.; Silva, G.R.; Oliveira, V.M.; Beltrao, N.B.; Araujo, R.C. Prevalence of Headache in Adolescents and Association with Use of Computer and Videogames. Cien. Saude Colet. 2015, 20, 3477–3486. [Google Scholar] [CrossRef]
- Smith, L.; Louw, Q.; Crous, L.; Grimmer, K. Prevalence of Neck Pain and Headaches: Impact of Computer Use and Other Associative Factors. Cephalalgia 2009, 29, 250–257. [Google Scholar] [CrossRef]
- Wahl, S.; Engelhardt, M.; Schaupp, P.; Lappe, C.; Ivanov, I.V. The Inner Clock-Blue Light Sets the Human Rhythm. J. Biophotonics 2019, 12, e201900102. [Google Scholar] [CrossRef]
- van Tilborg, M.M.; Murphy, P.J.; Evans, K.S. Impact of Dry Eye Symptoms and Daily Activities in a Modern Office. Optom. Vis. Sci. 2017, 94, 688–693. [Google Scholar] [CrossRef] [PubMed]
| Variable | Total n = 600 | Screen Viewing Time (<2 h/Day) | OR | 95% CI | p Value | |
|---|---|---|---|---|---|---|
| Yes (n = 108) | No (n = 492) | |||||
| Gender | ||||||
| Girls | 314 (52) | 68 (22) | 246 (78) | R | R | - |
| Boys | 286 (48) | 40 (14) | 246 (86) | 1.7 | 1.10–2.60 | 0.015 |
| Place of residence | ||||||
| Urban | 307 (51) | 59 (19) | 248 (81) | R | R | - |
| Rural | 293 (49) | 49 (17) | 244 (83) | 1.18 | 0.77–1.79 | 0.427 |
| Age in years | ||||||
| ≤6 | 245 (41) | 82 (33) | 163 (67) | R | R | - |
| >6 | 355 (59) | 26 (7) | 329 (93) | 0.15 | 0.97–0.25 | <0.001 |
| Type of family | ||||||
| Joint | 196 (33) | 28 (14) | 168 (86) | Ref | Ref | - |
| Nuclear | 404 (67) | 80 (20) | 324 (80) | 0.67 | 0.42–1.07 | 0.1 |
| Number of family members | ||||||
| 3–5 | 452 (75) | 85 (19) | 367 (81) | Ref | Ref | - |
| >5–9 | 116 (19) | 19 (16) | 97 (84) | 1.18 | 0.68–2.03 | 0.547 |
| >10 | 32 (5) | 4 (13) | 28 (87) | 1.62 | 0.55–4.74 | 0.378 |
| Overcrowding | ||||||
| Yes | 226 (38) | 31 (14) | 195 (86) | Ref | Ref | - |
| No | 374 (62) | 77 (21) | 297 (79) | 0.61 | 0.38–0.96 | 0.035 |
| Mother’s level of education | ||||||
| Uneducated/primary | 251 (42) | 53 (21) | 198 (79) | Ref | Ref | - |
| Up to high school | 141 (24) | 21 (15) | 120 (85) | 1.52 | 0.87–2.66 | 0.133 |
| Graduate/PG | 208 (35) | 34 (16) | 174 (84) | 1.36 | 0.85–2.20 | 0.193 |
| Mother’s occupation | ||||||
| Unemployed | 296 (49) | 61 (21) | 235 (79) | Ref | Ref | - |
| Labourer | 169 (28) | 21 (12) | 148 (88) | 1.80 | 1.06–3.12 | 0.027 |
| Salaried job | 135 (23) | 26 (16) | 109 (81) | 1.08 | 0.65–1.81 | 0.746 |
| Father’s level of education | ||||||
| Uneducated/primary | 91 (15) | 15 (16) | 76 (84) | Ref | Ref | - |
| Up to high school | 318 (53) | 65 (20) | 253 (80) | 0.76 | 0.41–1.42 | 0.402 |
| Graduate/PG | 191 (32) | 28 (15) | 163 (85) | 1.14 | 0.57–2.27 | 0.691 |
| Father’s occupation | ||||||
| Unemployed | 27 (5) | 6 (22) | 21 (78) | Ref | Ref | - |
| Self employed | 196 (33) | 36 (18) | 160 (82) | 1.21 | 0.47–3.37 | 0.48 |
| Labourer | 203 (34) | 33 (16) | 170 (84) | 1.47 | 0.55–3.92 | 0.77 |
| Salaried job | 174 (29) | 33 (19) | 141 (81) | 1.22 | 0.45–3.26 | 0.40 |
| Variable | Total n = 600 | Screen Viewing Time (<2 h/Day) | OR | 95% CI | p Value | |
|---|---|---|---|---|---|---|
| Yes (n = 108) | No (n = 492) | |||||
| Night sleep time | ||||||
| ≥6 h | 537 (90) | 104 (19) | 433 (81) | R | R | - |
| <6 h | 63 (10) | 4 (6) | 59 (94) | 3.54 | 1.25–9.97 | 0.017 |
| Mobile phone use at bedtime | ||||||
| No | 218 (36) | 79 (36) | 139 (64) | R | R | - |
| Yes | 382 (64) | 29 (8) | 353 (92) | 6.91 | 4.32–11.05 | <0.001 |
| TV in bedroom | ||||||
| No | 187 (31) | 97 (52) | 90 (48) | R | R | - |
| Yes | 413 (69) | 11 (3) | 402 (97) | 39.38 | 20.27–76.52 | <0.001 |
| Morning mobile screen time | ||||||
| No | 203 (34) | 73 (36) | 130 (64) | R | R | - |
| Yes | 397 (66) | 33 (8) | 364 (92) | 5.80 | 3.70–9.10 | <0.001 |
| Child habituated to screen | ||||||
| No | 293 (49) | 94 (32) | 199 (68) | R | R | - |
| Yes | 307 (51) | 12 (4) | 295 (74) | 9.88 | 5.48–17.82 | <0.001 |
| Child reads books | ||||||
| Yes | 332 (55) | 86 (26) | 246 (74) | R | R | - |
| No | 268 (45) | 20 (7) | 248 (93) | 3.90 | 2.36–6.44 | <0.001 |
| Story telling by parents | ||||||
| Yes | 237 (40) | 69 (29) | 168 (71) | R | R | - |
| No Outdoor play | 363 (60) | 37 (10) | 326 (90) | 3.41 | 2.20–5.26 | <0.001 |
| Yes | 430 (72) | 89 (21) | 343 (79) | R | R | - |
| No | 170 (28) | 19 (11) | 151 (89) | 2.07 | 1.21–3.52 | 0.007 |
| Outdoor play ≥ 2 h | ||||||
| Yes | 244 (41) | 72 (30) | 172 (70) | R | R | - |
| No | 356 (59) | 35 (10) | 321 (90) | 4.12 | 2.63–6.44 | <0.001 |
| Headache | ||||||
| No | 483 (81) | 100 (21) | 383 (79) | R | R | - |
| Yes | 117 (19) | 8 (7) | 109 (93) | 3.31 | 1.67–7.53 | 0.001 |
| Eye pain | ||||||
| No | 478 (80) | 96 (20) | 382 (80) | R | R | - |
| Yes | 122 (20) | 12 (10) | 110 (90) | 2.30 | 1.21–4.53 | 0.010 |
| Eye itching | ||||||
| No | 417 (70) | 102 (29) | 315 (76) | R | R | - |
| Yes | 183 (30) | 6 (3) | 177 (97) | 9.52 | 4.10–22.20 | <0.001 |
| Variable | a OR | 95% CI | p Value |
|---|---|---|---|
| Girls vs. boys | 1.31 | 0.58–2.97 | 0.512 |
| Age (continous variable) | 1.63 | 1.39–1.91 | <0.001 |
| Mobile phone use at bedtime | 3.35 | 1.46–7.69 | 0.004 |
| Child habituated to screen according to parent’s perception | 8.46 | 2.77–25.96 | <0.001 |
| TV in bedroom | 35.91 | 13.30–96.94 | <0.001 |
| Morning mobile screen time | 6.40 | 2.76–14.84 | <0.001 |
| Child not reading books other than textbooks | 6.45 | 2.35–17.73 | <0.001 |
| Less than 2 h/d of outdoor play | 5.17 | 2.24–11.95 | <0.001 |
| Eye pain present | 0.13 | 0.02–0.68 | 0.012 |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2023 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Jain, S.; Shrivastava, S.; Mathur, A.; Pathak, D.; Pathak, A. Prevalence and Determinants of Excessive Screen Viewing Time in Children Aged 3–15 Years and Its Effects on Physical Activity, Sleep, Eye Symptoms and Headache. Int. J. Environ. Res. Public Health 2023, 20, 3449. https://doi.org/10.3390/ijerph20043449
Jain S, Shrivastava S, Mathur A, Pathak D, Pathak A. Prevalence and Determinants of Excessive Screen Viewing Time in Children Aged 3–15 Years and Its Effects on Physical Activity, Sleep, Eye Symptoms and Headache. International Journal of Environmental Research and Public Health. 2023; 20(4):3449. https://doi.org/10.3390/ijerph20043449
Chicago/Turabian StyleJain, Shilpa, Shreya Shrivastava, Aditya Mathur, Deepali Pathak, and Ashish Pathak. 2023. "Prevalence and Determinants of Excessive Screen Viewing Time in Children Aged 3–15 Years and Its Effects on Physical Activity, Sleep, Eye Symptoms and Headache" International Journal of Environmental Research and Public Health 20, no. 4: 3449. https://doi.org/10.3390/ijerph20043449
APA StyleJain, S., Shrivastava, S., Mathur, A., Pathak, D., & Pathak, A. (2023). Prevalence and Determinants of Excessive Screen Viewing Time in Children Aged 3–15 Years and Its Effects on Physical Activity, Sleep, Eye Symptoms and Headache. International Journal of Environmental Research and Public Health, 20(4), 3449. https://doi.org/10.3390/ijerph20043449







