Menstrual Cycle and Sport Injuries: A Systematic Review
Abstract
1. Introduction
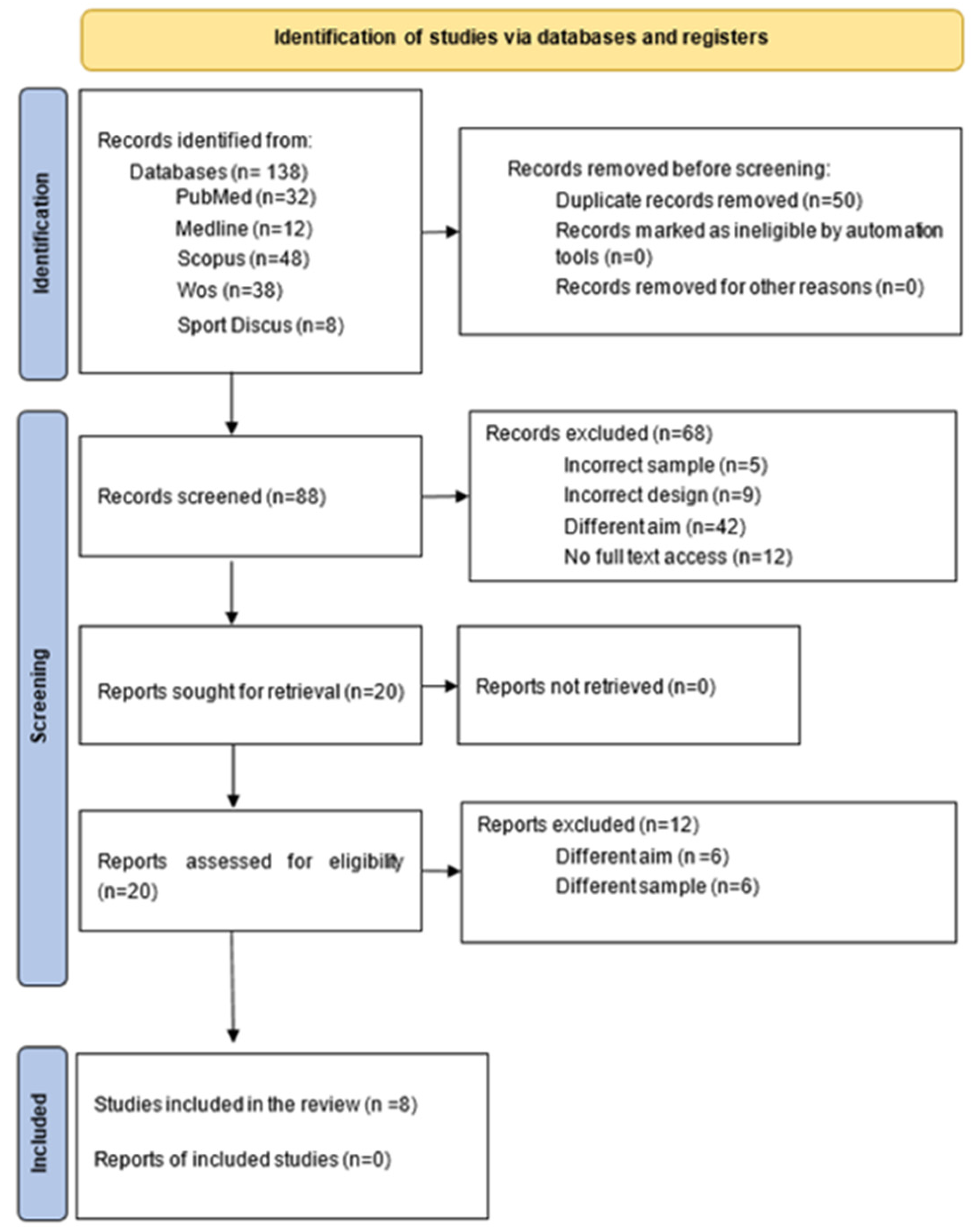
2. Materials and Methods
3. Results
4. Discussion
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Konovalova, E. El ciclo menstrual y el entranmiento deportivo; una mirada al problema. Rev. UDCA Actual. Divulg. Cient. 2013, 16, 293–302. [Google Scholar] [CrossRef]
- Bonen, A.; Keizer, H.A. Athletic Menstrual Cycle Irregularity: Endocrine Response to Exercise and Training. Phys. Sportsmed. 1984, 12, 78–94. [Google Scholar] [CrossRef]
- Wojtys, E.M.; Jannausch, M.L.; Kreinbrink, J.L.; Harlow, S.D.; Sowers, M.R. Athletic activity and hormone concentrations in high school female athletes. J. Athl. Train. 2015, 50, 185–192. [Google Scholar] [CrossRef]
- Moore, K.L.; Persaud, T.V.N. Embriología Clínica, 9th ed.; Elsevier España, S.L.: Barcelona, Spain, 2013; pp. 20–26. [Google Scholar]
- Godoy, R.C.; Pérez, L.F.; Curbelo, S.T.; Bosch, N. Fisiología reproductiva femenina: Hormonas sexuales y sus ciclos. BioCancer Res. J. 2004, 2, 10. [Google Scholar]
- Fisiología de la Reproducción; AEGO: Madrid, España, 2022. Available online: https://aego.es/otra-informacion/fisiologia-de-la-reproduccion (accessed on 23 May 2022).
- Curell Aguilà, N. Normalidad y alteraciones de la menstruación en adolescentes. Pediatr. Integral 2013, XVII, 161–170. [Google Scholar]
- Rodríguez Jiménez, M.J.; Curell Aguilá, N. El ciclo menstrual y sus alteraciones. Pediatr. Integral 2017, XXI, 304–311. [Google Scholar]
- Alanís-Blancas, L.M.; Zamora-Muñoz, P.; Cruz-Miranda, Á. Ruptura de ligamento cruzado anterior en mujeres deportistas. An. Med. 2012, 57, 93–97. [Google Scholar]
- Huston, L.J.; Greenfield, M.L.; Wojtys, E.M. Anterior cruciate ligament injuries in the female athlete. Potential risk factors. Clin. Orthop. Relat. Res. 2000, 372, 50–63. [Google Scholar] [CrossRef] [PubMed]
- Yu, B.; Kirkendall, D.T.; Garrett, W.E.J. Anterior Cruciate Ligament Injuries in Female Athletes: Anatomy, Physiology, and Motor Control. Sport. Med. Arthrosc. Rev. 2002, 10, 58–68. [Google Scholar] [CrossRef]
- Scranton, P.E.; Whitesel, J.P.; Powell, J.W.; Dormer, S.G.; Heidt, R.S.; Losse, G.; Cawley, P.W. A review of selected noncontact anterior cruciate ligament injuries in the National Football League. Foot Ankle Int. 1997, 18, 772–776. [Google Scholar] [CrossRef] [PubMed]
- Hewett, T.E.; Zazulak, B.T.; Myer, G.D. Effects of the Menstrual Cycle on Anterior Cruciate Ligament Injury Risk: A Systematic Review. Am. J. Sport. Med. 2007, 35, 659–668. [Google Scholar] [CrossRef] [PubMed]
- McFarland, E.G.; Campbell, G.; McDowell, J. Posterior Shoulder Laxity in Asymptomatic Athletes. Am. J. Sport. Med. 1996, 24, 468–471. [Google Scholar] [CrossRef] [PubMed]
- McLean, S.G.; Neal, R.J.; Myers, P.T.; Walters, M.R. Knee joint kinematics during the sidestep cutting maneuver: Potential for injury in women. Med. Sci. Sport. Exerc. 1999, 31, 959–968. [Google Scholar] [CrossRef] [PubMed]
- Wojtys, E.M.; Huston, L.J.; Lindenfeld, T.N.; Hewett, T.E.; Greenfield, M.L. Association between the menstrual cycle and anterior cruciate ligament injuries in female athletes. Am. J. Sport. Med. 1998, 26, 614–619. [Google Scholar] [CrossRef] [PubMed]
- Myklebust, G.; Maehlum, S.; Holm, I.; Bahr, R. A prospective cohort study of anterior cruciate ligament injuries in elite Norwegian team handball. Scand. J. Med. Sci. Sport. 1998, 8, 149–153. [Google Scholar] [CrossRef]
- Slauterbeck, J.R.; Fuzie, S.F.; Smith, M.P.; Clark, R.J.; Xu, K.T.; Starch, D.W.; Hardy, D.M. The Menstrual Cycle, Sex Hormones, and Anterior Cruciate Ligament Injury. J. Athl. Train. 2002, 37, 275–278. [Google Scholar]
- Lefevre, N.; Bohu, Y.; Klouche, S.; Lecocq, J.; Herman, S. Anterior cruciate ligament tear during the menstrual cycle in female recreational skiers. Orthop. Traumatol. Surg. Res. 2013, 99, 571–575. [Google Scholar] [CrossRef]
- Page, M.J.; McKenzie, J.E.; Bossuyt, P.M.; Boutron, I.; Hoffmann, T.C.; Mulrow, C.D.; Shamseer, L.; Tetzlaff, J.M.; Akl, E.A.; Brennan, S.E.; et al. The PRISMA 2020 statement: An updated guideline for reporting systematic reviews. BMJ 2021, 372, n71. [Google Scholar] [CrossRef]
- Guirao Goris, S.J.A. Utilidad y tipos de revisión de literatura. ENE Rev. Enferm. 2015, 9, 14. [Google Scholar] [CrossRef]
- Law, M.; Stewart, D.; Pollock, N.; Letts, L.; Bosch, J.; Westmorland, M. Critical Review Form—Quantitative Studies; McMaster University: Hamilton, ON, Canada, 1998; p. 3. [Google Scholar]
- Lago-Fuentes, C.; Padrón-Cabo, A.; Fernández-Villarino, M.; Mecías-Calvo, M.; Muñoz-Pérez, I.; García-Pinillos, F.; Rey, E. Follicular phase of menstrual cycle is related to higher tendency to suffer from severe injuries among elite female futsal players. Phys. Ther. Sport. 2021, 52, 90–96. [Google Scholar] [CrossRef]
- Forouzandeh Shahraki, S.; Minoonejad, H.; Moghadas Tabrizi, Y. Comparison of some intrinsic risk factors of shoulder injury in three phases of menstrual cycle in collegiate female athletes. Phys. Ther. Sport. 2020, 43, 195–203. [Google Scholar] [CrossRef] [PubMed]
- Sommerfield, L.M.; Harrison, C.B.; Whatman, C.S.; Maulder, P.S. A prospective study of sport injuries in youth females. Phys. Ther. Sport. 2020, 44, 24–32. [Google Scholar] [CrossRef] [PubMed]
- Hohmann, E.; Bryant, A.L.; Livingstone, E.; Reaburn, P.; Tetsworth, K.; Imhoff, A. Tibial acceleration profiles during the menstrual cycle in female athletes. Arch. Orthop. Trauma Surg. 2015, 135, 1419–1427. [Google Scholar] [CrossRef] [PubMed]
- Khowailed, I.A.; Petrofsky, J.; Lohman, E.; Daher, N.; Mohamed, O. 17β-Estradiol Induced Effects on Anterior Cruciate Ligament Laxness and Neuromuscular Activation Patterns in Female Runners. J. Women’s Health 2015, 24, 670–680. [Google Scholar] [CrossRef]
- Stijak, L.; Kadija, M.; Djulejić, V.; Aksić, M.; Petronijević, N.; Marković, B.; Radonjić, V.; Bumbaširević, M.; Filipović, B. The influence of sex hormones on anterior cruciate ligament rupture: Female study. Knee Surg. Sport. Traumatol. Arthrosc. 2015, 23, 2742–2749. [Google Scholar] [CrossRef]
- Bell, D.R.; Blackburn, J.T.; Hackney, A.C.; Marshall, S.W.; Beutler, A.I.; Padua, D.A. Jump-Landing Biomechanics and Knee-Laxity Change across the Menstrual Cycle in Women with Anterior Cruciate Ligament Reconstruction. J. Athl. Train. 2014, 49, 154–162. [Google Scholar] [CrossRef]
- Schmitz, R.J.; Shultz, S.J. Anterior Knee Stiffness Changes in Laxity “Responders” Versus “Nonresponders” across the Menstruai Cycle. J. Athl. Train. 2013, 48, 39–46. [Google Scholar] [CrossRef]
- Shagawa, M.; Maruyama, S.; Sekine, C.; Yokota, H.; Hirabayashi, R.; Hirata, A.; Yokoyama, M.; Edama, M. Comparison of anterior knee laxity, stiffness, genu recurvatum, and general joint laxity in the late follicular phase and the ovulatory phase of the menstrual cycle. BMC Musculoskelet. Disord. 2021, 22, 886. [Google Scholar] [CrossRef]
- Lee, H.; Petrofsky, J.S.; Daher, N.; Berk, L.; Laymon, M.; Khowailed, I.A. Anterior cruciate ligament elasticity and force for flexion during the menstrual cycle. Med. Sci. Monit. 2013, 19, 1080–1088. [Google Scholar] [CrossRef]
- Liu, S.H.; Al-Shaikh, R.; Yang, R.-S.; Nelson, S.D.; Soleiman, N.; Finerman, G.A.M.; Lane, J.M. Primary immunolocalization of estrogen and progesterone target cells in the human anterior cruciate ligament. J. Orthop. Res. 1996, 14, 526–533. [Google Scholar] [CrossRef] [PubMed]
- Yu, W.D.; Liu, S.H.; Hatch, J.D.; Panossian, V.; Finerman, G.A.M. Effect of Estrogen on Cellular Metabolism of the Human Anterior Cruciate Ligament. Clin. Orthop. Relat. Res. 1999, 366, 229–238. [Google Scholar] [CrossRef]
- Shafiei, S.E.; Peyvandi, S.; Kariminasab, M.H.; Azar, M.S.; Daneshpoor, S.M.M.; Khalilian, A.; Aghajantabar, Z. Knee Laxity Variations in the Menstrual Cycle in Female Athletes Referred to the Orthopedic Clinic. Asian J. Sport. Med. 2016, 7, e30199. [Google Scholar] [CrossRef]
- Dragoo, J.L.; Castillo, T.N.; Braun, H.J.; Ridley, B.A.; Kennedy, A.C.; Golish, S.R. Prospective Correlation Between Serum Relaxin Concentration and Anterior Cruciate Ligament Tears among Elite Collegiate Female Athletes. Am. J. Sport. Med. 2011, 39, 2175–2180. [Google Scholar] [CrossRef] [PubMed]
- Pearson, S.J.; Burgess, K.E.; Onambélé, G.L. Serum relaxin levels affect the in vivo properties of some but not all tendons in normally menstruating young women: Female tendons and hormone levels. Exp. Physiol. 2011, 96, 681–688. [Google Scholar] [CrossRef]
- Lowe, D.A.; Baltgalvis, K.A.; Greising, S.M. Mechanisms Behind Estrogen’s Beneficial Effect on Muscle Strength in Females. Exerc. Sport Sci. Rev. 2010, 38, 61–67. [Google Scholar] [CrossRef] [PubMed]
- Dedrick, G.S.; Sizer, P.S.; Merkle, J.N.; Hounshell, T.R.; Robert-McComb, J.J.; Sawyer, S.F.; Brismee, J.-M.; James, C.R. Effect of sex hormones on neuromuscular control patterns during landing. J. Electromyogr. Kinesiol. 2008, 18, 68–78. [Google Scholar] [CrossRef]
- Bryant, A.L.; Crossley, K.M.; Bartold, S.; Hohmann, E.; Clark, R.A. Estrogen-induced effects on the neuro-mechanics of hopping in humans. Eur. J. Appl. Physiol. 2011, 111, 245–252. [Google Scholar] [CrossRef]
- Alentorn-Geli, E.; Myer, G.D.; Silvers, H.J.; Samitier, G.; Romero, D.; Lázaro-Haro, C.; Cugat, R. Prevention of non-contact anterior cruciate ligament injuries in soccer players. Part 1: Mechanisms of injury and underlying risk factors. Knee Surg. Sport. Traumatol. Arthrosc. 2009, 17, 705–729. [Google Scholar] [CrossRef] [PubMed]
- dos Santos Andrade, M.; Mascarin, N.C.; Foster, R.; de Jármy di Bella, Z.I.; Vancini, R.L.; Barbosa de Lira, C.A. Is muscular strength balance influenced by menstrual cycle in female soccer players? J. Sport. Med. Phys. Fit. 2017, 57, 1557–1563. [Google Scholar] [CrossRef]
- Hewett, T.E. Neuromuscular and Hormonal Factors Associated with Knee Injuries in Female Athletes: Strategies for Intervention. Sport. Med. 2000, 29, 313–327. [Google Scholar] [CrossRef] [PubMed]
- Bäckström, T.; Baird, D.T.; Bancroft, J.; Bixo, M.; Hammarbäck, S.; Sanders, D.; Smith, S.; Zetterlund, B. Endocrinological aspects of cyclical mood changes during the menstrual cycle or the premenstrual syndrome. J. Psychosom. Obstet. Gynaecol. 1983, 2, 8–20. [Google Scholar] [CrossRef]
- Leguía-Cerna, J.A.; Ronald Puescas-Sanchez, P.; Díaz-Vélez, C. Importace of sample size calculation in research. Rev. Cuerpo Méd. HNAA 2012, 1, 38. [Google Scholar]
- Rondón-Tapía, M.; Reyna-Villasmil, E.; Mejia-Montilla, J.; Reyna-Villasmil, N.; Torres-Cepeda, D.; Fernández-Ramírez, A. Hormonas sexuales pre y posparto en preecampticas y embarazadas normotensas sanas. Rev. Perú. Ginecol. Obstet. 2017, 63, 155–161. [Google Scholar] [CrossRef]
- Sanchez del Moral, R.; Herrera Carranza, J. Conocimiento de los medicamentos anticonceptivos en una población universitaria. Segumiento Farmacoter. 2005, 3, 130–134. [Google Scholar]
- Zurita-Cruz, J.N.; Márquez-González, H.; Miranda-Novales, G.; Villasis-Keever, M.Á. Estudios experimentales: Diseños de investigación para la evaluación de intervenciones en la clínica. RAM 2018, 65, 178–186. [Google Scholar] [CrossRef]
- Gómez-Tomás, C.; Rial Rebullido, T.; Chulvi-Medrano, I. Estrategias de prevención neuromuscular para las lesiones de ligamento cruzado anterior sin contacto en jugadoras de baloncesto. Revisión narrativa. MHSalud 2021, 18, 1–21. [Google Scholar] [CrossRef]
- Jordan, M.; Aagaard, P.; Herzog, W. Anterior cruciate ligament injury/reinjury in alpine ski racing: A narrative review. OAJSM 2017, 8, 71–83. [Google Scholar] [CrossRef]
- Kirkendall, D.T.; Dvorak, J. Effective Injury Prevention in Soccer. Phys. Sportsmed. 2010, 38, 147–157. [Google Scholar] [CrossRef]
- O’Brien, D. Efectos del ejercicio en el ciclo menstrual. Arch. Med. Deporte 1989, 6, 265–268. [Google Scholar]
- Charlton, W.P.H.; Coslett-Charlton, L.M.; Ciccotti, M.G. Correlation of Estradiol in Pregnancy and Anterior Cruciate Ligament Laxity. Clin. Orthop. Relat. Res. 2001, 387, 165–170. [Google Scholar] [CrossRef] [PubMed]
- Herzberg, S.D.; Motu’apuaka, M.L.; Lambert, W.; Fu, R.; Brady, J.; Guise, J.M. The Effect of Menstrual Cycle and Contraceptives on ACL Injuries and Laxity: A Systematic Review and Meta-analysis. Orthop. J. Sport. Med. 2017, 5, 232596711771878. [Google Scholar] [CrossRef] [PubMed]
- Yanguas Leyes, J.; Til Pérez, L.; Cortés de Olano, C. Lesión del ligamento cruzado anterior en fútbol femenino. Estudio epidemiológico de tres temporadas. Apunts. Med. l’Esport 2011, 46, 137–143. [Google Scholar] [CrossRef]
- Murcia-Lora, J.M.; Esparza-Encina, M.L. La ventana de la fertilidad y marcadores biológicos: Revisión y análisis en ciclos ovulatorios normales. Pers. Bioét. 2011, 15, 17. [Google Scholar] [CrossRef]
- Duane, M.; Contreras, A.; Jensen, E.T.; White, A. The Performance of Fertility Awareness-based Method Apps Marketed to Avoid Pregnancy. J. Am. Junta Fam. Med. 2016, 29, 508–511. [Google Scholar] [CrossRef] [PubMed]
- McLean, S.G.; Oh, Y.K.; Palmer, M.L.; Lucey, S.M.; Lucarelli, D.G.; Ashton-Miller, J.A.; Wojtys, E.M. The Relationship between Anterior Tibial Acceleration, Tibial Slope, and ACL Strain during a Simulated Jump Landing Task. J. Bone Jt. Surg. 2011, 93, 1310–1317. [Google Scholar] [CrossRef] [PubMed]
- Makino, A.; Garces, E.; Costa Paz, M.; Aponte Tinao, L.; Muscolo, D.L. Evaluación artrométrica de rodilla con KT 1000 en pacientes con ruptura del L.C.A. sin y con anestesia. Rev. Argent. Artrosc. 1998, 5, 40–43. [Google Scholar]
- Shultz, S.J.; Wideman, L.; Montgomery, M.M.; Levine, B.J. Some sex hormone profiles are consistent over time in normal menstruating women: Implications for sports injury epidemiology. Br. J. Sport. Med. 2011, 45, 735–742. [Google Scholar] [CrossRef]
- Beynnon, B.D.; Johnson, R.J.; Braun, S.; Sargent, M.; Bernstein, I.M.; Skelly, J.M.; Vacek, P.M. The Relationship between Menstrual Cycle Phase and Anterior Cruciate Ligament Injury: A Case-Control Study of Recreational Alpine Skiers. Am. J. Sport. Med. 2006, 34, 757–764. [Google Scholar] [CrossRef]
- Park, S.K.; Stefanyshyn, D.J.; Ramage, B.; Hart, D.A.; Ronsky, J.L. Alterations in Knee Joint Laxity During the Menstrual Cycle in Healthy Women Leads to Increases in Joint Loads during Selected Athletic Movements. Am. J. Sport. Med. 2009, 37, 1169–1177. [Google Scholar] [CrossRef] [PubMed]
- Rodríguez Rozalén, M.A. Guía Los Consejos de tu Matrona. AEM. 2021. Available online: https://aesmatronas.com/wp-content/uploads/2021/04/GuiaMatronas_21_150RGB-DEFINITIVO-PUBLI1.pdf (accessed on 23 May 2022).
| Item | Studies | |||||||
|---|---|---|---|---|---|---|---|---|
| Lago-Fuentes et al. [23] | Forouzandeh et al. [24] | Sommerfield et al. [25] | Hohmann et al. [26] | Khowailed et al. [27] | Stijak et al. [28] | Bell et al. [29] | Schmitz, Shultz. [30] | |
| Is the purpose clearly established? | Yes | Yes | Yes | Yes | Yes | Yes | Yes | Yes |
| Was relevant background literature reviewed? | Yes | Yes | Yes | Yes | Yes | Yes | Yes | Yes |
| Study design | PCS | TS | PCS | CS | NR | CCS | CS | DS |
| Sample size | 179 W | 15 W | 103 W | 11 W/6 M | 12 W | 24 W | 20 W | 38 W |
| Is the sample described in detail? | Yes | Yes | No | Yes | Yes | Yes | Yes | Yes |
| Is the sample size justified? | Yes | Yes | No | Yes | Yes | Yes | Yes | Yes |
| Are the results confident? | No | Yes | No | Yes | Yes | Yes | Yes | Yes |
| Are the results valid measurements? | Yes | Yes | Yes | Yes | Yes | Yes | Yes | Yes |
| Is the intervention described in detail? | Yes | Yes | Yes | Yes | Yes | Yes | Yes | Yes |
| Contamination was avoided? | NR | NR | NR | Yes | NR | NR | NR | NR |
| Cointervention was avoided? | NR | NR | NR | NR | NR | NR | NR | NR |
| Are the results meaningful in terms of statistical significance? | Yes | Yes | Yes | Yes | Yes | Yes | Yes | Yes |
| Were the analyses appropriate? | Yes | Yes | Yes | Yes | Yes | Yes | Yes | Yes |
| Was the clinical relevance reported? | Yes | Yes | Yes | Yes | Yes | Yes | Yes | Yes |
| Were the losts reported? | Yes | No | No | No | No | No | Yes | No |
| Are the conclusions appropriate considering the methods and results? | Yes | Yes | Yes | Yes | Yes | Yes | Yes | Yes |
| Authors | Characteristics of the Sample | Characteristics of Sports Practice | |||||||
|---|---|---|---|---|---|---|---|---|---|
| Sample Size | Group | Age (Years) | Weight (Kg) | Height (cm) | BMI (Kg/m2) | Type of Sport | Level of Professionality | Exercise Frequency per Week | |
| Lago-Fuentes et al. [23] | 179 | - | - | 59.9 ± 7.8 | 164.2 ± 5.6 | 22.2 ± 2.3 | Futsal | professional | 5–8 h + 1 competition |
| Forouzandeh et al. [24] | 15 | - | 23.27 ± 1.66 | 57.60 ± 6.75 | 167 ± 0.05 | - | Overhead athletics | recreational | 3 sessions |
| Sommerfield et al. [25] | 103 | - | 14.0 ± 0.6 | 57.4 ± 9.8 | 162.6 ± 5.8 | - | Netball, soccer, hockey, lacrosse, swimming, badminton, athletics, and kayak | recreational | 3.4 h training + 1 competition + 2.2 h physical training |
| Hohman et al. [26] | 17 | EG = 11 W CG = 6 M | 16.3 ± 0.7 | 60.7 ± 6.3 | 164 ± 6.2 | - | EG = netball CG = Rugby | recreational | - |
| Khowailed et at. [27] | 12 | - | 25.6 ± 3.7 | 56.8 ± 8.2 | 160.2 ± 8.6 | 22 ± 2.2 | Athletics | - | No more than 20 Km or 7 h |
| Stijak et al. [28] | 24 | EG = 12 W ACL injury CG = 12 W no ACL injury | EG = 24.2 CG = 24.8 | - | - | - | Volleyball, athletics, handball, and soccer | 18 professional 6 recreational | CG = 4.2 sessions EG = 4 sessions |
| Bell et al. [29] | 20 | - | 19.6 ±1.3 | 66.2 ± 9.1 | 168.6 ± 5.3 | - | Soccer | - | - |
| Schmitz, Shultz. [30] | 38 | - | G1: 21.4 ± 2.6 G2: 22.5 ± 3.5 | G1: 64.4 ± 9.7 G2: 60.2 ± 7.5 | G1: 164 ±0.06 G2: 166 ± 0.06 | - | - | recreational | 2.5–10 h |
| Authors | Variables | Tools | Intervention Time | Measurements | Results |
|---|---|---|---|---|---|
| Lago-Fuentes et al. [23] | Injuries and exposure time MC phases | Excel and calendar | Two sport seasons in soccer | - | 191 injuries (104 in training and 87 in matches) 22% in quadriceps 40.8% distension More risk found during the follicular phase. |
| Forouzandeh et al. [24] | MC phases Strength Proprioception Laxity Stability | Ovulation kit Lafayette hand-held dynamometer Inclinometer ACL test | Complete MC (four weeks) | 3: Menstruation, ovulation, and medium luteal phase | Shoulder strength increased significantly during ovulation. Proprioception decreased significantly during the luteal phase. No significant changes were reported in stability or laxity. |
| Sommerfield et al. [25] | Injuries and exposure time MC phases | OSTRC physical training assistance FITrWoman or My Calendar App | 1 year | - | 595 injuries in 74 participants 51% in the knee 35% in the ankle No significant relationship was found between the phase of the MC and the risk of injury. A slightly greater tendency to be injured was observed in the luteal phase. |
| Hohmann et al. [26] | LH, FSH, E2, and P4 Tibial acceleration | Blood sample Acceleration during a jump | Complete MC (four weeks) | 3: Menstruation, ovulation, follicular, and medium luteal phase | Higher levels of E2 and AKL were found during ovulation. Lower levels of E2 and AKL were found in CG compared to EG. LH and tibial acceleration were similar in both groups. |
| Khowailed et al. [27] | MC phases E2 and AKL levels Neuromuscular control | Ovulation kit Blood sample Arthrometer KT-2000 Run 6 min Electromyography | Complete MC (four weeks) | 2: follicular and ovulation | Higher levels of E2 and AKL were found during ovulation. In the follicular phase, a higher recruitment in quadriceps was found compared to a lower recruitment in hamstrings when running. |
| Stijak et al. [28] | E2, P4, AKL, and testosterone | Saliva samples Beighton test | Complete MC (four weeks) | 2: luteal and ovulation phases | Women with an ACL injury had significantly lower levels of testosterone and higher levels of E2 and P4. |
| Bell et al. [29] | E2, P4, AKL, and testosterone Cinematic evaluation of knee and hip | Blood sample Arthrometer KT-2000 Electromyography | Complete MC (four weeks) | 2: menstruation and ovulation | Levels of E2, AKL, and P4 were significantly higher during ovulation. No significant changes were found in testosterone levels. |
| Schmitz and Shultz [30] | MC phases AKL levels | Ovulation kit Arthrometer KT-2000 | 2 complete MCs (8 weeks) | 2: menstruation and ovulation (two times) | Women with higher AKL levels during the ovulation phase also had a significantly higher tolerance to changes. |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2023 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Martínez-Fortuny, N.; Alonso-Calvete, A.; Da Cuña-Carrera, I.; Abalo-Núñez, R. Menstrual Cycle and Sport Injuries: A Systematic Review. Int. J. Environ. Res. Public Health 2023, 20, 3264. https://doi.org/10.3390/ijerph20043264
Martínez-Fortuny N, Alonso-Calvete A, Da Cuña-Carrera I, Abalo-Núñez R. Menstrual Cycle and Sport Injuries: A Systematic Review. International Journal of Environmental Research and Public Health. 2023; 20(4):3264. https://doi.org/10.3390/ijerph20043264
Chicago/Turabian StyleMartínez-Fortuny, Núria, Alejandra Alonso-Calvete, Iria Da Cuña-Carrera, and Rocío Abalo-Núñez. 2023. "Menstrual Cycle and Sport Injuries: A Systematic Review" International Journal of Environmental Research and Public Health 20, no. 4: 3264. https://doi.org/10.3390/ijerph20043264
APA StyleMartínez-Fortuny, N., Alonso-Calvete, A., Da Cuña-Carrera, I., & Abalo-Núñez, R. (2023). Menstrual Cycle and Sport Injuries: A Systematic Review. International Journal of Environmental Research and Public Health, 20(4), 3264. https://doi.org/10.3390/ijerph20043264









