Associations between Different Ozone Indicators and Cardiovascular Hospital Admission: A Time-Stratified Case-Crossover Analysis in Guangzhou, China
Abstract
1. Introduction
2. Method and Data Sources
2.1. Hospital Admissions
2.2. Air Pollutants and Meteorological Data
2.3. Statistical Analysis
2.4. Sensitivity Analysis
3. Results
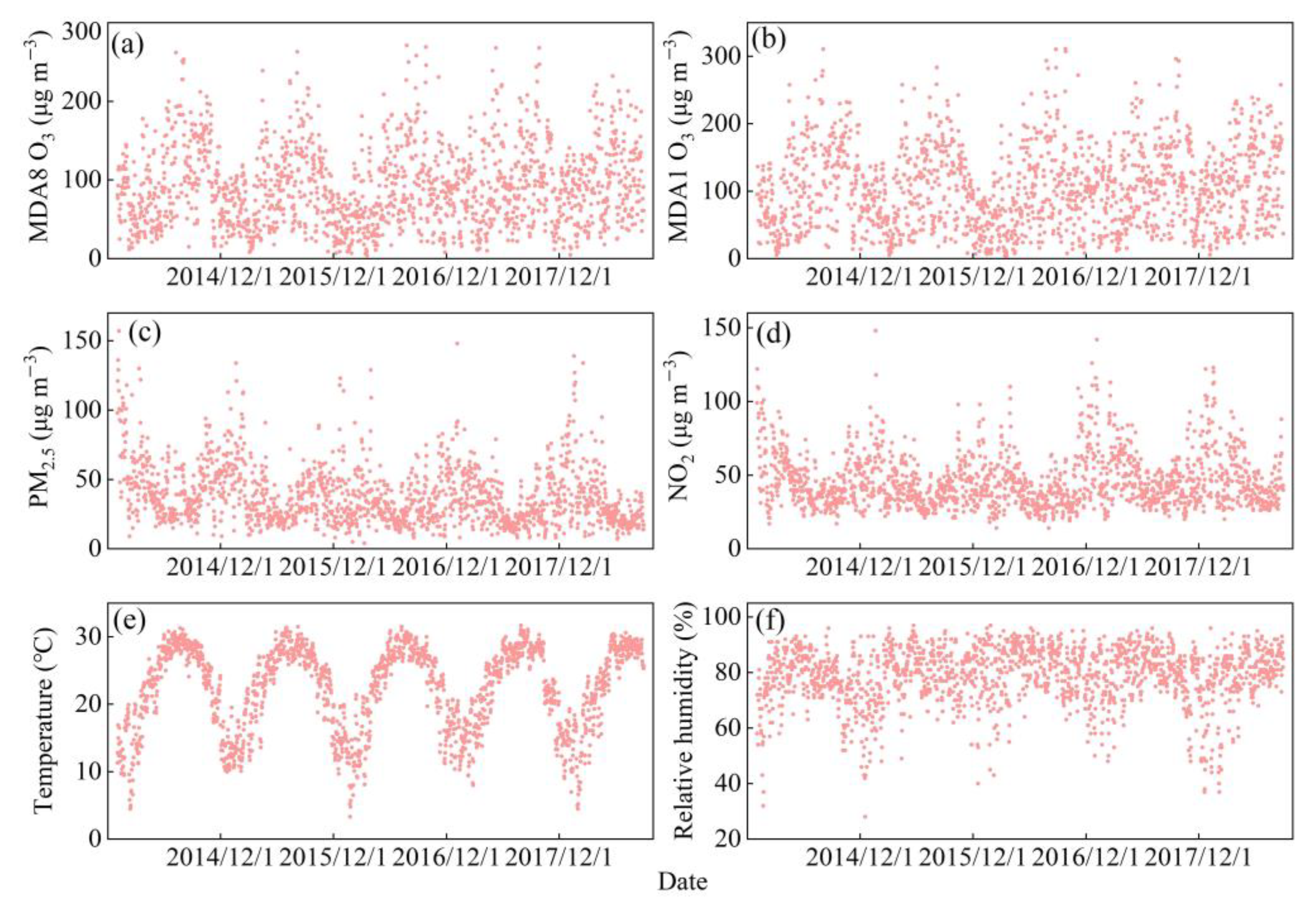
3.1. Basic Information of Data
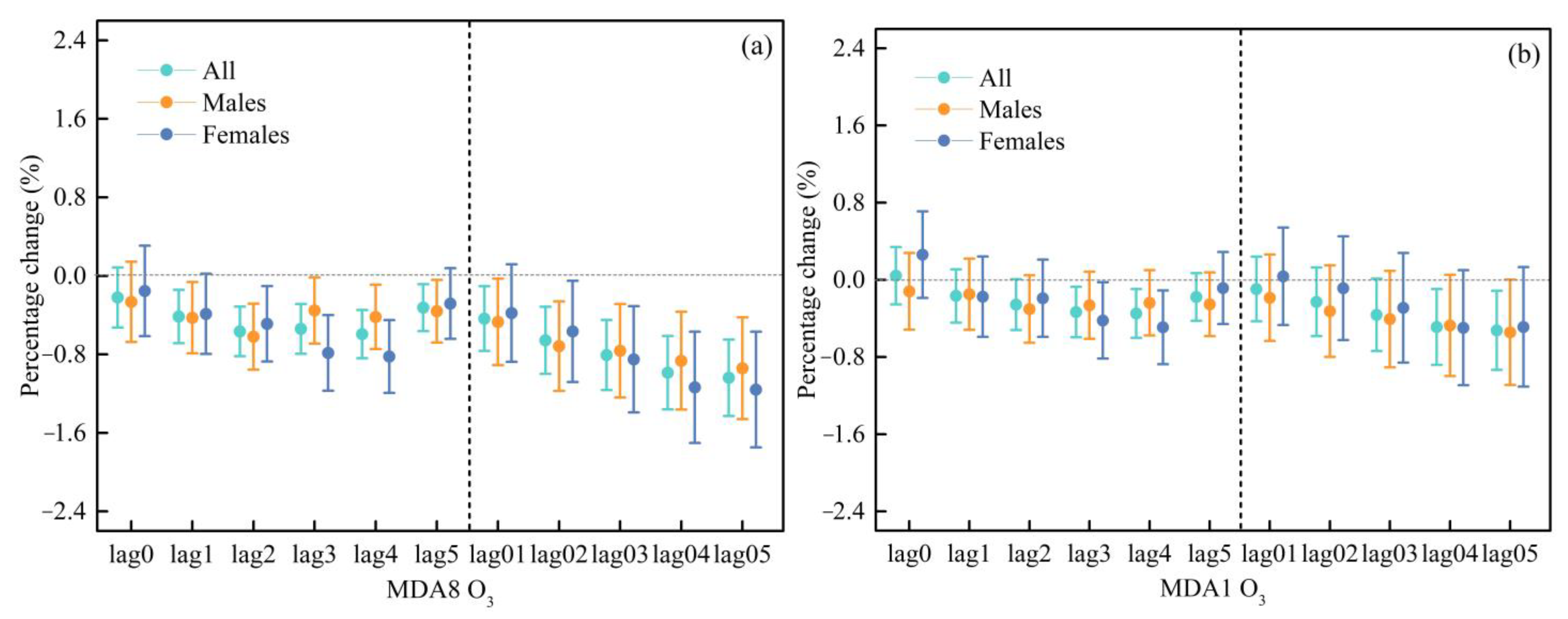
3.2. The Relationship between Ozone and Cardiovascular Hospitalization
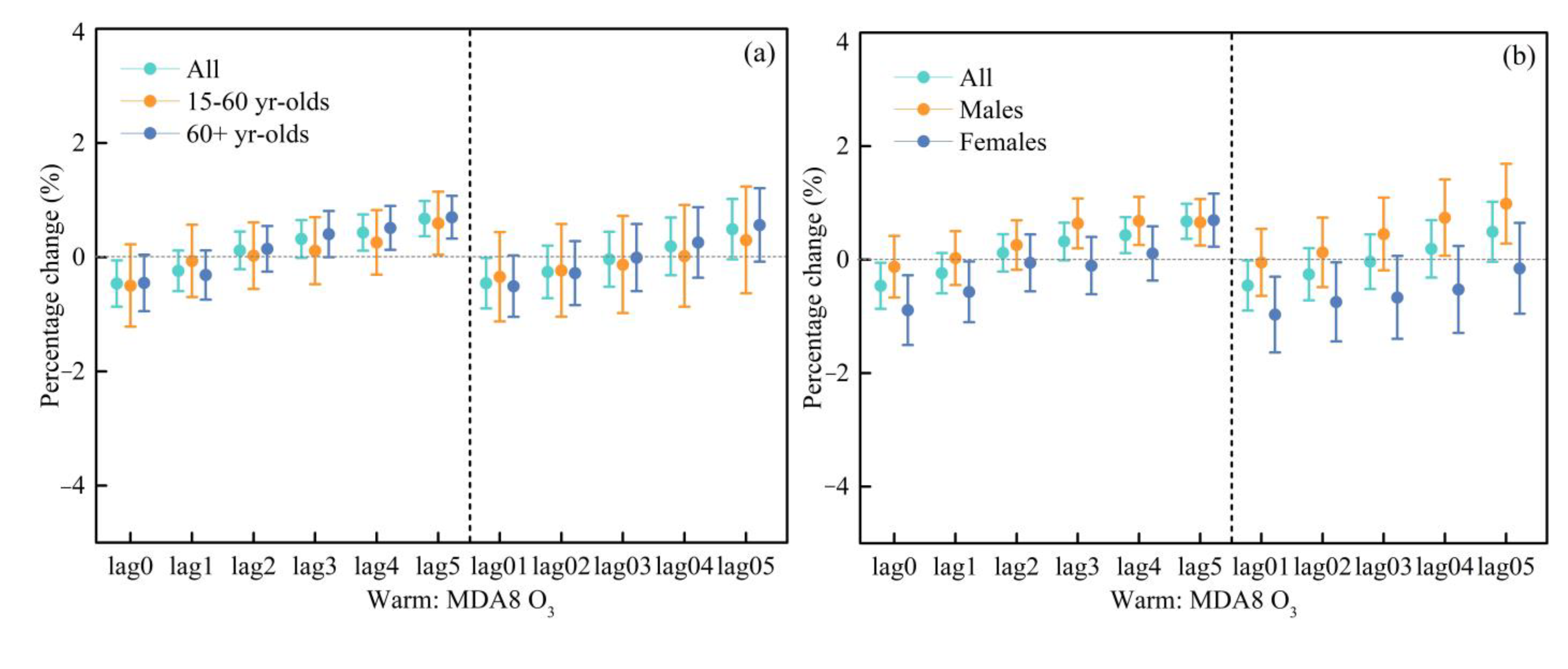
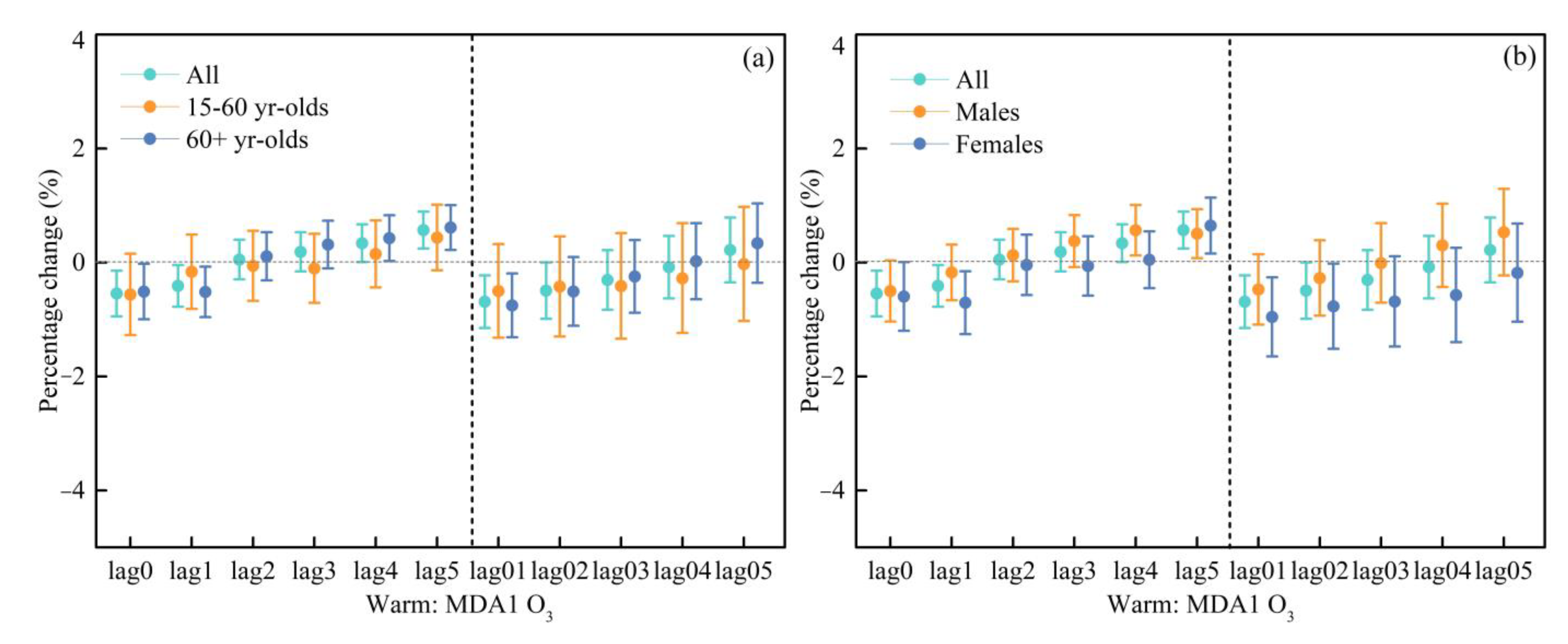
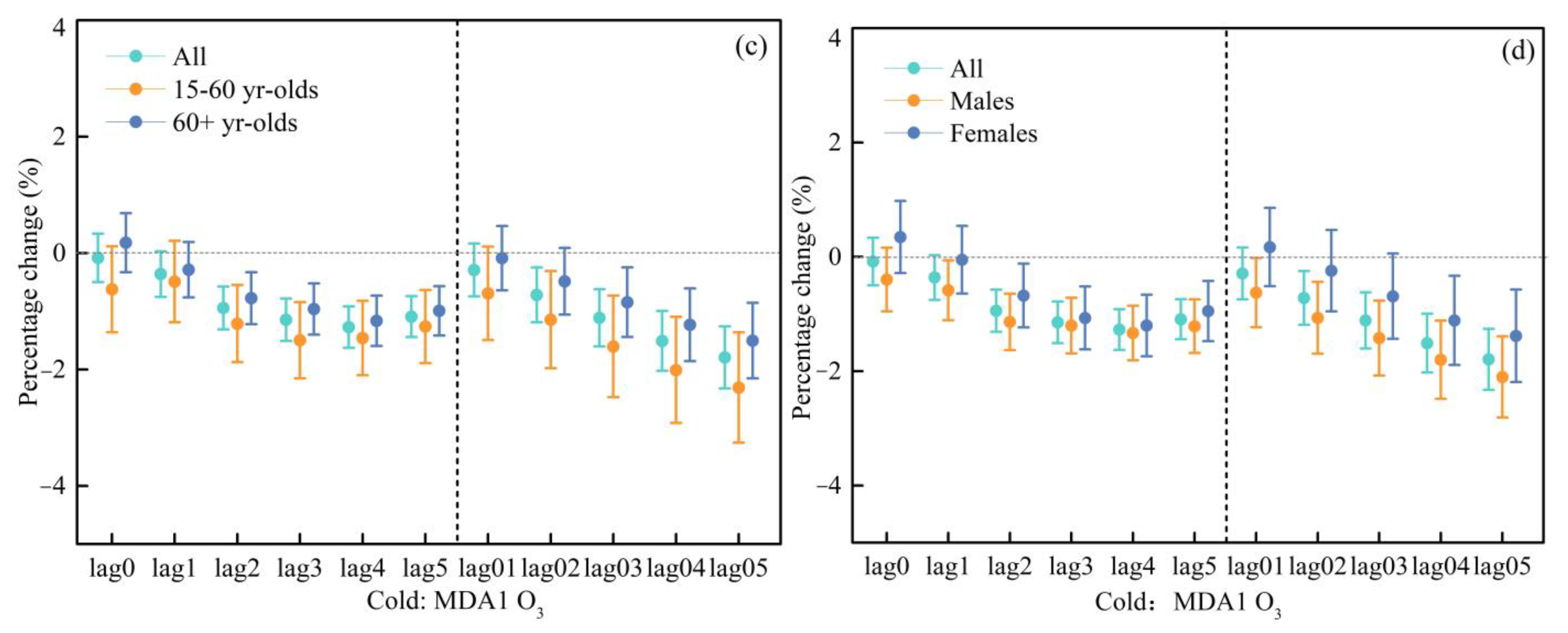
3.3. Seasonal Estimates of the Effects of Different Ozone Indicators on Cardiovascular Hospital Admissions
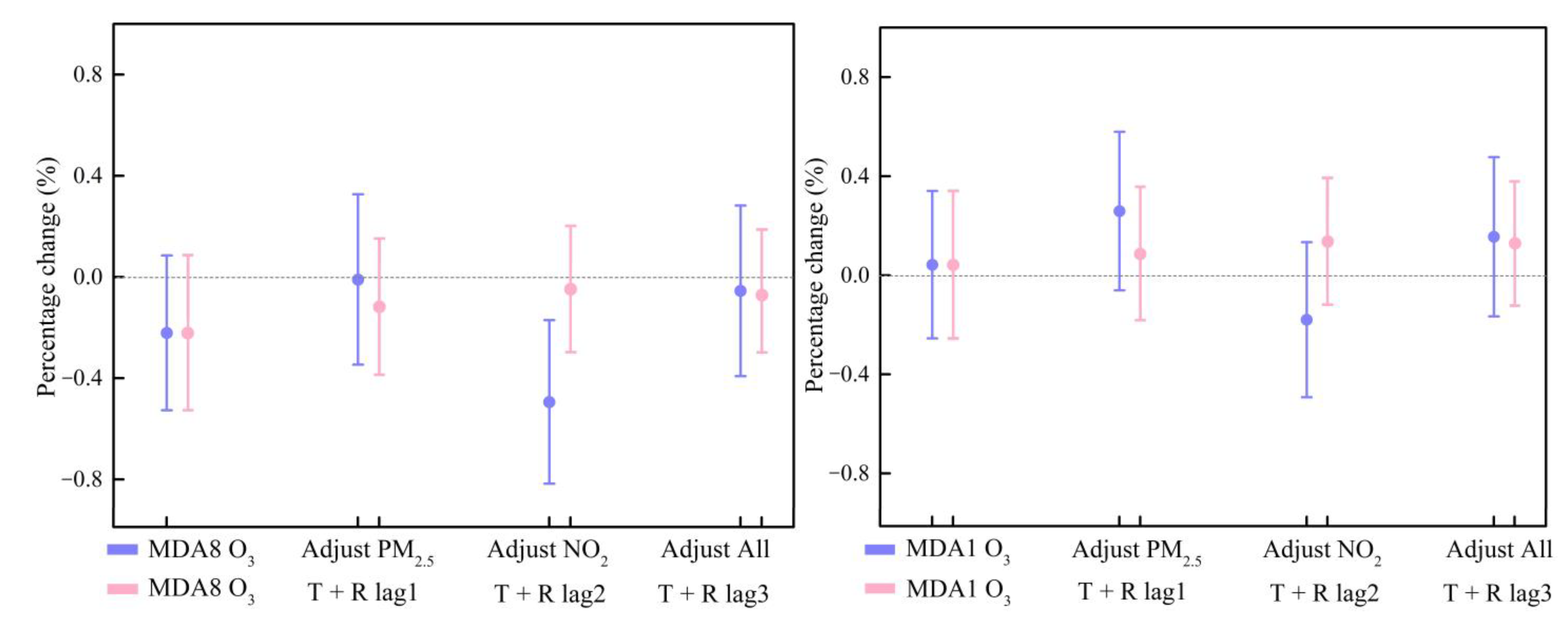
3.4. Sensitivity Analysis
4. Discussion
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
Abbreviations
References
- Jerrett, M.; Burnett, R.T.; Pope III, C.A.; Ito, K.; Thurston, G.; Krewski, D.; Shi, Y.; Calle, E.; Thun, M. Long-term ozone exposure and mortality. N. Engl. J. Med. 2009, 360, 1085–1095. [Google Scholar] [CrossRef] [PubMed]
- Wu, H.; Lu, K.; Fu, J. A time-series study for effects of ozone on respiratory mortality and cardiovascular mortality in Nanchang, Jiangxi Province, China. Front. Public Health 2022, 10, 864537. [Google Scholar] [CrossRef] [PubMed]
- Zhang, X.X.; Yan, B.; Zhou, Y.Y.; Osei, F.; Li, Y.; Zhao, H.; Cheng, C.X.; Stein, A. Short-term health impacts related to ozone in China before and after implementation of policy measures: A systematic review and meta-analysis. Sci. Total Environ. 2022, 847, 157588. [Google Scholar] [CrossRef] [PubMed]
- Zhao, H.; Wang, L.; Zhang, Z.; Qi, Q.; Zhang, H. Quantifying ecological and health risks of ground-level O3 across China during the implementation of the “Three-year Action Plan for Cleaner Air”. Sci. Total Environ. 2022, 817, 153011. [Google Scholar] [CrossRef]
- Wang, Y.Y.; Zu, Y.Q.; Huang, L.; Zhang, H.L.; Wang, C.H.; Hu, J.L. Associations between daily outpatient visits for respiratory diseases and ambient fine particulate matter and ozone levels in Shanghai, China. Environ. Pollut. 2018, 240, 754–763. [Google Scholar] [CrossRef]
- Zhang, X.X.; Cheng, C.X.; Zhao, H. A health impact and economic loss assessment of O3 and PM2.5 exposure in China from 2015 to 2020. GeoHealth 2022, 6, e2021GH000531. [Google Scholar] [CrossRef]
- Zhang, X.X.; Osei, F.; Stein, A.; Cheng, C.X.; Maji, J.K. Temporal and spatial evolution of short-term exposure to ozone pollution: Its health impacts in China based on a meta-analysis. J. Clean. Prod. 2022, 373, 133938. [Google Scholar] [CrossRef]
- Zhao, H.; Chen, K.; Liu, Z.; Zhang, Y.; Shao, T.; Zhang, H. Coordinated control of PM2.5 and O3 is urgently needed in China after implementation of the “Air pollution prevention and control action plan”. Chemosphere 2021, 270, 129441. [Google Scholar] [CrossRef]
- Li, K.; Jacob, D.J.; Liao, H.; Shen, L.; Zhang, Q.; Bates, K.H. Anthropogenic drivers of 2013–2017 trends in summer surface ozone in China. Proc. Natl. Acad. Sci. USA 2019, 116, 422–427. [Google Scholar] [CrossRef]
- Shang, Y.; Sun, Z.W.; Cao, J.J.; Wang, X.M.; Zhong, L.J.; Bi, X.H.; Li, H.; Liu, W.X.; Zhu, T.; Huang, W. Systematic review of Chinese studies of short-term exposure to air pollution and daily mortality. Environ. Int. 2013, 54, 100–111. [Google Scholar] [CrossRef]
- Maji, K.J.; Ye, W.F.; Arora, M.; Nagendra, S.M.S. Ozone pollution in Chinese cities: Assessment of seasonal variation, health effects and economic burden. Environ. Pollut. 2019, 247, 792–801. [Google Scholar] [CrossRef] [PubMed]
- Wang, Y.Y.; Hu, J.L.; Zhu, J.; Li, J.; Qin, M.; Liao, H.; Chen, K.; Wang, M. Health Burden and economic impacts attributed to PM2.5 and O3 in China from 2010 to 2050 under different representative concentration pathway scenarios. Resour. Conserv. Recycl. 2021, 173, 105731. [Google Scholar] [CrossRef]
- Li, M.; Dong, H.; Wang, B.; Zhao, W.; Sakhvidi, M.J.Z.; Li, L.; Lin, G.; Yang, J. Association between ambient ozone pollution and mortality from a spectrum of causes in Guangzhou, China. Sci. Total Environ. 2021, 754, 142110. [Google Scholar] [CrossRef]
- Tao, Y.; Huang, W.; Huang, X.; Zhong, L.; Lu, S.E.; Li, Y.; Dai, L.; Zhang, Y.; Zhu, T. Estimated acute effects of ambient ozone and nitrogen dioxide on mortality in the Pearl River Delta of southern China. Environ. Health Perspect. 2012, 120, 393–398. [Google Scholar] [CrossRef]
- Day, D.B.; Xiang, J.; Mo, J.; Li, F.; Chung, M.; Gong, J.; Weschler, C.J.; Ohman-Strickland, P.A.; Sundell, J.; Weng, W. Association of ozone exposure with cardiorespiratory pathophysiologic mechanisms in healthy adults. JAMA Intern. Med. 2017, 177, 1344–1353. [Google Scholar] [CrossRef]
- Li, Y.; Shang, Y.; Zheng, C.; Ma, Z. Estimated acute effects of ozone on mortality in a rural district of Beijing, China, 2005–2013: A time-stratified case-crossover study. Int. J. Environ. Res. Public Health 2018, 15, 2460. [Google Scholar] [CrossRef] [PubMed]
- Bell, M.L.; Dominici, F. Effect modification by community characteristics on the short-term effects of ozone exposure and mortality in 98 US communities. Am. J. Epidemiol. 2008, 167, 986–997. [Google Scholar] [CrossRef] [PubMed]
- Ji, M.; Cohan, D.S.; Bell, M. Meta-analysis of the association between short-term exposure to ambient ozone and respiratory hospital admissions. Environ. Res. Lett. 2011, 6, 024006. [Google Scholar] [CrossRef] [PubMed]
- Yang, C.X.; Yang, H.B.; Guo, S.; Wang, Z.S.; Xu, X.H.; Duan, X.L.; Kan, H.D. Alternative ozone metrics and daily mortality in Suzhou: The China Air Pollution and Health Effects Study (CAPES). Sci. Total Environ. 2012, 426, 83–89. [Google Scholar] [CrossRef]
- Bell, M.L.; McDermott, A.; Zeger, S.L.; Samet, J.M.; Dominici, F. Ozone and short-term mortality in 95 US urban communities, 1987–2000. Jama 2004, 292, 2372–2378. [Google Scholar] [CrossRef]
- Yang, C.Y.; Chen, Y.S.; Yang, C.H.; Ho, S. Relationship between ambient air pollution and hospital admissions for cardiovascular diseases in Kaohsiung, Taiwan. J. Toxicol. Environ. Health 2004, 67, 483–493. [Google Scholar] [CrossRef]
- Wang, T.; Xue, L.; Brimblecombe, P.; Lam, Y.F.; Li, L.; Zhang, L. Ozone pollution in China: A review of concentrations, meteorological influences, chemical precursors, and effects. Sci. Total Environ. 2017, 575, 1582–1596. [Google Scholar] [CrossRef] [PubMed]
- WHO. Ambient (Outdoor) Air Quality and Health. 2014. Available online: http://www.who.int/mediacentre/factsheets/fs313/en/ (accessed on 11 November 2017).
- Barrero, M.; Orza, J.; Cabello, M.; Cantón, L. Categorisation of air quality monitoring stations by evaluation of PM10 variability. Sci. Total Environ. 2015, 524, 225–236. [Google Scholar] [CrossRef] [PubMed]
- Feng, L.; Ye, B.; Feng, H.; Ren, F.; Huang, S.; Zhang, X.; Zhang, Y.; Du, Q.; Ma, L. Spatiotemporal changes in fine particulate matter pollution and the associated mortality burden in China between 2015 and 2016. Int. J. Environ. Res. Publ. Health 2017, 14, 1321. [Google Scholar] [CrossRef]
- Lumley, T.; Levy, D. Bias in the case–crossover design: Implications for studies of air pollution. Env. Off. J. Int. Env. Soc. 2000, 11, 689–704. [Google Scholar] [CrossRef]
- Maclure, M. The case-crossover design: A method for studying transient effects on the risk of acute events. Am. J. Epidemiol. 1991, 133, 144–153. [Google Scholar] [CrossRef]
- Ding, L.; Zhu, D.; Peng, D.; Zhao, Y. Air pollution and asthma attacks in children: A case–crossover analysis in the city of Chongqing, China. Environ. Pollut. 2017, 220, 348–353. [Google Scholar] [CrossRef]
- Jiao, A.Q.; Xiang, Q.Q.; Ding, Z.; Cao, J.G.; Ho, H.C.; Chen, D.Y.; Cheng, J.; Yang, Z.M.; Zhang, F.X.; Yu, Y.; et al. Short-term impacts of ambient fine particulate matter on emergency department visits: Comparative analysis of three exposure metrics. Chemosphere 2020, 241, 125012. [Google Scholar] [CrossRef]
- Zanobetti, A.; Schwartz, J. Is there adaptation in the ozone mortality relationship: A multi-city case-crossover analysis. Environ. Health 2008, 7, 22. [Google Scholar] [CrossRef]
- Qin, L.; Gu, J.; Liang, S.; Fang, F.; Bai, W.; Liu, X.; Zhao, T.; Walline, J.; Zhang, S.; Cui, Y. Seasonal association between ambient ozone and mortality in Zhengzhou, China. Int. J. Biometeorol. 2017, 61, 1003–1010. [Google Scholar] [CrossRef]
- Gryparis, A.; Forsberg, B.; Katsouyanni, K.; Analitis, A.; Touloumi, G.; Schwartz, J.; Samoli, E.; Medina, S.; Anderson, H.R.; Niciu, E.M. Acute effects of ozone on mortality from the “air pollution and health: A European approach” project. Am. J. Respir. Crit. Care Med. 2004, 170, 1080–1087. [Google Scholar] [CrossRef] [PubMed]
- Lin, Y.K.; Chang, S.C.; Lin, C.; Chen, Y.C.; Wang, Y.C. Comparing ozone metrics on associations with outpatient visits for respiratory diseases in Taipei Metropolitan area. Environ. Pollut. 2013, 177, 177–184. [Google Scholar] [CrossRef] [PubMed]
- Sun, Q.; Wang, W.; Chen, C.; Ban, J.; Xu, D.; Zhu, P.; He, M.Z.; Li, T. Acute effect of multiple ozone metrics on mortality by season in 34 Chinese counties in 2013–2015. J. Intern. Med. 2018, 283, 481–488. [Google Scholar] [CrossRef]
- Shi, W.; Sun, Q.; Du, P.; Tang, S.; Chen, C.; Sun, Z.; Wang, J.; Li, T.; Shi, X. Modification effects of temperature on the ozone–mortality relationship: A nationwide multicounty study in China. Environ. Sci. Technol. 2020, 54, 2859–2868. [Google Scholar] [CrossRef] [PubMed]
- Kazemiparkouhi, F.; Eum, K.D.; Wang, B.Y.; Manjourides, J.; Suh, H.H. Long-term ozone exposures and cause-specific mortality in a US Medicare cohort. J. Expo. Sci. Environ. Epidemiol. 2020, 30, 650–658. [Google Scholar] [CrossRef]
- Chen, K.; Yang, H.B.; Ma, Z.W.; Bi, J.; Huang, L. Influence of temperature to the short-term effects of various ozone metrics on daily mortality in Suzhou, China. Atmos. Environ. 2013, 79, 119–128. [Google Scholar] [CrossRef]
- Li, T.; Yan, M.; Ma, W.; Ban, J.; Liu, T.; Lin, H.; Liu, Z. Short-term effects of multiple ozone metrics on daily mortality in a megacity of China. Environ. Sci. Pollut. Res. 2015, 22, 8738–8746. [Google Scholar] [CrossRef]
- Cheng, L.; Wang, S.; Gong, Z.; Li, H.; Yang, Q.; Wang, Y. Regionalization based on spatial and seasonal variation in ground-level ozone concentrations across China. J. Environ. Sci. 2018, 67, 179–190. [Google Scholar] [CrossRef]
- Pothirat, C.; Chaiwong, W.; Liwsrisakun, C.; Bumroongkit, C.; Deesomchok, A.; Theerakittikul, T.; Limsukon, A.; Tajarernmuang, P.; Phetsuk, N. Acute effects of air pollutants on daily mortality and hospitalizations due to cardiovascular and respiratory diseases. J. Thorac. Dis. 2019, 11, 3070–3083. [Google Scholar] [CrossRef]
- Lu, K.; Kang, J.; Wang, G. The Impact of Air Quality on Cardiovascular Disease in Shanghai. J. Healthc. Eng. 2022, 2022, 4421686. [Google Scholar] [CrossRef]
- Ren, C.; Williams, G.M.; Mengersen, K.; Morawska, L.; Tong, S. Does temperature modify short-term effects of ozone on total mortality in 60 large eastern US communities?—An assessment using the NMMAPS data. Environ. Int. 2008, 34, 451–458. [Google Scholar] [CrossRef] [PubMed]
- Chen, K.; Wolf, K.; Hampel, R.; Stafoggia, M.; Breitner, S.; Cyrys, J.; Samoli, E.; Andersen, Z.J.; Bero-Bedada, G.; Bellander, T.; et al. Does temperature-confounding control influence the modifying effect of air temperature in ozone–mortality associations? Environ. Epidemiol. 2018, 2, e008. [Google Scholar] [CrossRef]
- Pascal, M.; Wagner, V.; Chatignoux, E.; Falq, G.; Corso, M.; Blanchard, M.; Host, S.; Larrieu, S.; Pascal, L.; Declercq, C. Ozone and short-term mortality in nine French cities: Influence of temperature and season. Atmos. Environ. 2012, 62, 566–572. [Google Scholar] [CrossRef]
- Chen, R.; Cai, J.; Meng, X.; Kim, H.; Honda, Y.; Guo, Y.L.; Samoli, E.; Yang, X.; Kan, H. Ozone and daily mortality rate in 21 cities of East Asia: How does season modify the association? Am. J. Epidemiol. 2014, 7, 729–736. [Google Scholar] [CrossRef]
- Murray, C.J.; Aravkin, A.Y.; Zheng, P.; Abbafati, C.; Abbas, K.M.; Abbasi-Kangevari, M.; Abd-Allah, F.; Abdelalim, A.; Abdollahi, M.; Abdollahpour, I. Global burden of 87 risk factors in 204 countries and territories, 1990–2019: A systematic analysis for the Global Burden of Disease Study 2019. Lancet 2020, 396, 1223–1249. [Google Scholar] [CrossRef]


| Factors | IQR | 25% | 50% | 75% | Min | Mean | Max |
|---|---|---|---|---|---|---|---|
| COV hospital admission (number) | 12 | 5 | 12 | 17 | 0 | 12 | 46 |
| MDA1 O3 (μg/m3) | 87 | 57 | 100 | 144 | 4.3 | 105 | 311 |
| Warm period | 90 | 77 | 125 | 167 | 8 | 125 | 311 |
| Cold period | 75 | 42 | 78 | 117 | 4 | 84 | 272 |
| MDA8 O3 (μg/m3) | 71 | 51 | 86 | 122 | 4 | 91 | 271 |
| Warm period | 73 | 70 | 103 | 143 | 15 | 111 | 271 |
| Cold period | 53 | 43 | 69 | 96 | 5 | 70 | 180 |
| NO2 (μg/m3) | 22 | 33 | 42 | 55 | 14 | 46 | 148 |
| PM2.5 (μg/m3) | 26 | 23 | 33 | 49 | 4 | 38 | 157 |
| Temperature (℃) | 10.6 | 17.1 | 23.9 | 27.7 | 3.3 | 22.2 | 31.7 |
| Relative humidity (%) | 13 | 73 | 80 | 86 | 28 | 79 | 97 |
| References | Study Year | Study Area | Model | O3 Indicator | Relative Risks (RR) |
|---|---|---|---|---|---|
| Kazemiparkouhi et al., 2020 | 2000–2008 | USA | LLRM | MDA8 O3 | 0.9985 (0.9975, 0.9995) |
| MDA1 O3 | 1.0025 (1.0015, 1.0035) | ||||
| 24 h average | 0.9864 (0.9849, 0.9874) | ||||
| Gryparis et al., 2004 | 1990–1996 | 23 cities, Europe | GAM | MDA8 O3 | 1.0046 (1.0022, 1.0073) |
| MDA1 O3 | 1.0045 (1.0022, 1.0069) | ||||
| Moshammer et al., 2013 | 1991–2009 | Vienna, Austria | GAM | MDA8 O3 | 1.0051 (1.0026, 1.0076) |
| MDA1 O3 | 1.0047 (1.0026, 1.0069) | ||||
| 24 h average | 1.0062 (1.0030, 1.0093) | ||||
| Sun et al., 2018 | 2013–2015 | 34 counties, China | DLNM | MDA8 O3 | 1.0039 (1.0016, 1.0062) |
| MDA1 O3 | 1.0031 (1.0011, 1.0051) | ||||
| 24 h average | 1.0066 (1.0028, 1.0104) | ||||
| Yang et al., 2012 | 2006–2008 | Suzhou, China | GAM | MDA8 O3 | 1.0074 (1.0024, 1.0122) |
| MDA1 O3 | 1.0060 (1.0019, 1.0100) | ||||
| 24 h average | 1.0099 (1.0015, 1.0181) | ||||
| Chen et al., 2013 | 2008–2009 | Suzhou, China | GAM | MDA8 O3 | 1.0177 (1.0069, 1.0287) |
| MDA1 O3 | 1.0116 (1.0025, 1.0209) | ||||
| 24 h average | 1.0317 (1.0124, 1.0514) | ||||
| Shi et al., 2020 | 2013–2018 | 128 counties, China | GLM | MDA8 O3 | 1.0042 (1.0032, 1.0051) |
| MDA1 O3 | 1.0034 (1.0027, 1.0042) | ||||
| 24 h average | 1.0060 (1.0046, 1.0075) |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2023 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Zhang, X.; Maji, K.J.; Wang, Z.; Yang, F.F.; Wang, G.; Cheng, C. Associations between Different Ozone Indicators and Cardiovascular Hospital Admission: A Time-Stratified Case-Crossover Analysis in Guangzhou, China. Int. J. Environ. Res. Public Health 2023, 20, 2056. https://doi.org/10.3390/ijerph20032056
Zhang X, Maji KJ, Wang Z, Yang FF, Wang G, Cheng C. Associations between Different Ozone Indicators and Cardiovascular Hospital Admission: A Time-Stratified Case-Crossover Analysis in Guangzhou, China. International Journal of Environmental Research and Public Health. 2023; 20(3):2056. https://doi.org/10.3390/ijerph20032056
Chicago/Turabian StyleZhang, Xiangxue, Kamal Jyoti Maji, Zhuoqing Wang, Fiona Fan Yang, Guobin Wang, and Changxiu Cheng. 2023. "Associations between Different Ozone Indicators and Cardiovascular Hospital Admission: A Time-Stratified Case-Crossover Analysis in Guangzhou, China" International Journal of Environmental Research and Public Health 20, no. 3: 2056. https://doi.org/10.3390/ijerph20032056
APA StyleZhang, X., Maji, K. J., Wang, Z., Yang, F. F., Wang, G., & Cheng, C. (2023). Associations between Different Ozone Indicators and Cardiovascular Hospital Admission: A Time-Stratified Case-Crossover Analysis in Guangzhou, China. International Journal of Environmental Research and Public Health, 20(3), 2056. https://doi.org/10.3390/ijerph20032056







