Inflammatory Bowel Disease and Irritable Bowel Syndrome: What Differences in Mentalization Abilities? A Scoping Review
Abstract
:1. Introduction
2. Materials and Methods
2.1. Protocol
2.2. Eligibility Criteria
- Studies that did not use validated measures to investigate these constructs or that used ad hoc surveys or qualitative methods.
- Papers that did not contain research data or complete information (i.e., case reports, study protocols, perspective articles, and meeting abstracts).
- Papers published but not peer-reviewed (i.e., gray literature) or under review at the time the search was carried out.
2.3. Information Sources and Search Strategy
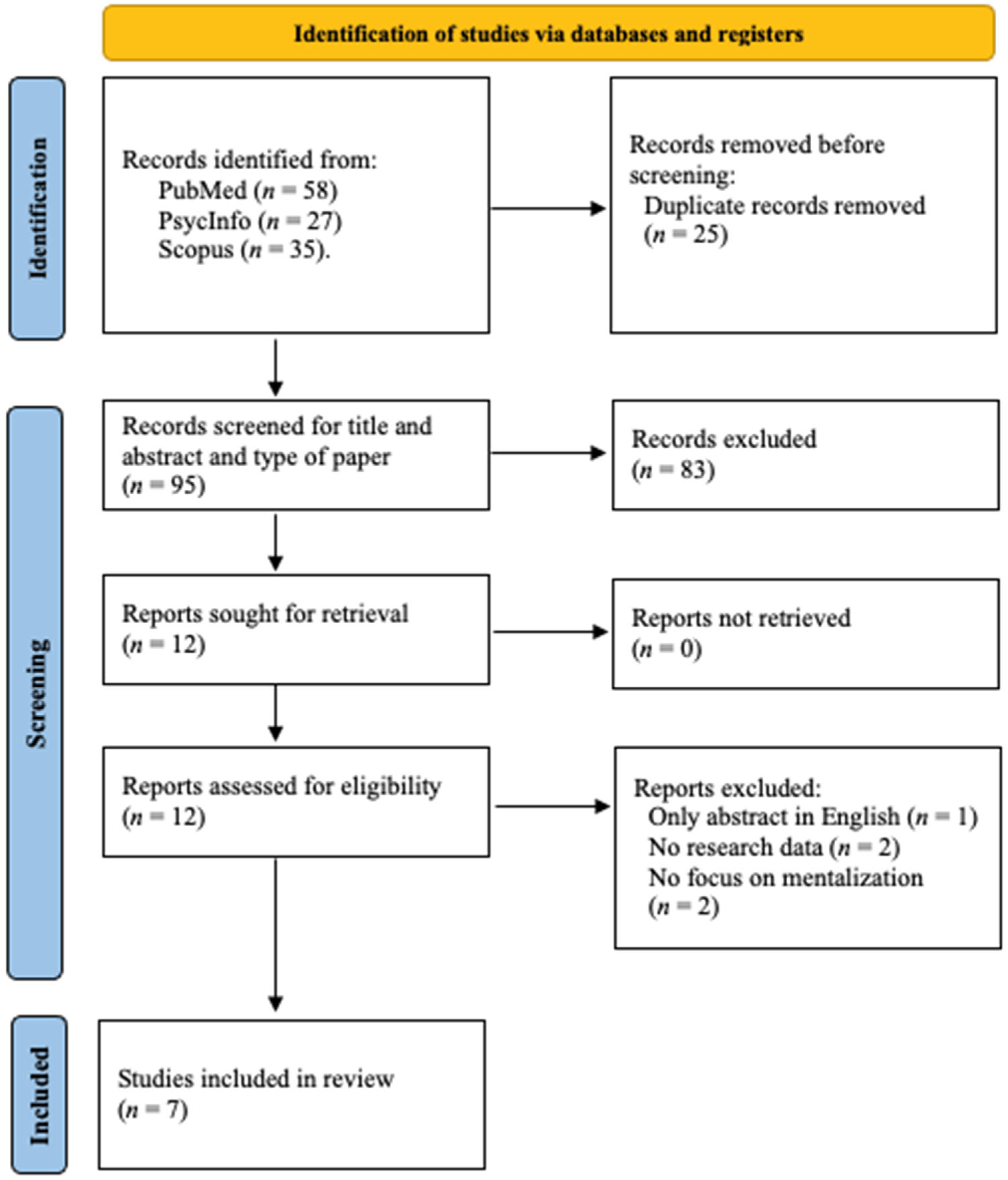
2.4. Studies Selection
2.5. Data Extraction
3. Results
| Authors (Years) | Participants | Mean (SD) Age | Measures of Mentalization | Measures of Other Psychological Variables | Main Results |
|---|---|---|---|---|---|
| Agostini et al. (2019) [29] | 96 IBD; 102 HCs. | IBD = 39.6 (14); HCs = 36.3 (12.3) | RFQ; RMET | ASQ | RMET mean (SD) scores were 22.21 (4.38) for IBD and 24.37 (3.17) for HCs. RFQ-Certainty mean (SD) scores were 1.12 (0.99) for IBD and 0.99 (0.63) for HCs. RFQ-Uncertainty mean (SD) scores were 0.72 (0.62) for IBD and 0.59 (0.49) for HCs. No difference was found between the two groups for RFQ. IBD showed lower scores in the RMET (p < 0.001) than in HCs. |
| Berens et al. (2019) [26] | 127 IBS; 127 IBD (93 with active symptoms, 34 with non-active symptoms); 127 HCs. | IBS = 36.5 (13.4); IBD = 35.3 (12.3); HCs = 35.1 (13.6) | MZQ | ECR-RD12; SSS-8; PHQ-9; GAD-7; WI-7; ACE | MZQ mean (SD) scores were 35.3 (11.4) for IBS, 32.2 (11.0) for IBD, and 29.4 (10.1) for HCs. IBS reported lower scores of MZQ compared to both HCs (p < 0.001) and IBD (p = 0.036). IBD showed lower scores of MZQ compared to HCs ( p = 0.036). IBS showed lower scores of MZQ compared to IBD without active symptoms (p = 0.003,). Whereas, no difference was found between IBS and IBD with active symptoms (p = 0.390). |
| Quattropani et al. (2019) [27] | Study 1: 28 IBS; 33 IBD. | Study 1: IBS = 38.1 (12.2); IBD = 33.9 (11.8) | MCQ-30 | ANPS | Study 1: IBD mean (SD) scores were MCQ-POS, 10.97 (4.57); MCQ-NEG, 15.15 (3.85); MCQ-CC,12.06 (3.98); MCQ-NC, 14.15 (3.87); MCQ-CSC, 17.27 (3.20). IBS mean (SD) scores were MCQ-POS, 11.89 (4.57); MCQ-NEG, 12.57 (3.51); MCQ-CC,12.50 (5.25); MCQ-NC, 13.04 (3.72); MCQ-CSC, 17.29 (2.71). No differences were found between the IBD and IBS on MCQ-30 scores. |
| Quattropani et al. (2019) [27] | Study 2: 20 IBS; 20 UC; 19 CD. | Study 2: IBS = 39.3 (19.8); UC = 37.32 (12.7); CD = 39.8 (14.5) | MCQ-30 | ANPS | Study 2: IBS mean (SD) scores were MCQ-POS, 10.40 (4.90); MCQ-NEG, 13.65 (3.73); MCQ-CC,12.25 (4.61); MCQ-NC, 13.15 (3.15); MCQ-CSC, 18.25 (2.45). UC mean (SD) scores were MCQ-POS, 11.50 (4.50); MCQ-NEG, 14.73 (4.29); MCQ-CC,13.05 (5.33); MCQ-NC, 14.45 (4.68); MCQ-CSC, 17.64 (2.70). CD mean (SD) scores were MCQ-POS, 10.68 (4.87); MCQ-NEG, 15.37 (4.92); MCQ-CC,14.47 (5.35); MCQ-NC, 15.42 (4.55); MCQ-CSC, 17.53 (2.74). No differences among the three groups on MCQ-30 scores. |
| Berens et al. (2021) [28] | 199 patients with IBD, IBS, or other DGBI: 92 with SSD, 107 without SSD. | Overall = 37.5 (14.8); with SSD = 38.3 (14.4); without SSD = 36.7 (15.2) | MZQ | ECR-RD12; SSS-8; PHQ-9); GAD-7; WI-7; ACE; Psy-Ba-Do; OPD-SQ; SSD-12 | MZQ median (IQR) scores were 2.4 (0.8) for overall, 2.2 (0.8) for patients without SSD, and 2.6 (0.8) for those with SSD, on a range of 1–5. Patients with SSD showed lower MZQ scores than patients without SSD (p = 0.001). |
| Dzirlo et al. (2021) [30] | 30 IBS; 32 NAP patients; 28 AD patients. | IBS = 40.8 (11.3); NAP = 38.2 (16.3); AD = 37 (3.8) | RFS (based on BRFI) | RFS mean (SD) scores were 2.7 (1.4) for IBS, 1.4 (1.9) for NAP, and 3.3 (1.7) for AD. Results showed significant differences among the three groups (p < 0.001), particularly between IBS and NAP (p = 0.008). No differences were found between IBS and AD. RFS mean scores were 2.1 for IBS-M, 3.1 for IBS-D, and 4.4 for IBS-C. There were differences between IBS-M and IBS-C (p = 0.023). No significant differences between IBS-M and IBS-D, and between IBS-D and IBS-C. | |
| Engel et al. (2021) [31] | 62 IBD: 31 CD; 31 UC; 31 HCs. | CD = 39.2 (14.7); UC = 38.5 (14.0); HCs = 38.5 (13.3) | MZQ | OPD-SQ; ECR-RD12; GAD-7; PHQ-9 | MZQ median (IQR) scores were 2.07 (1.00) for CD, 2.13 (1.00) for UC, and 1.73 (1.07) for HCs, on a range of 0–4. No differences were found among the three groups in the MZQ score (p = 0.290). |
| Zargar and Kavoosi (2021) [32] | 50 IBS; 50 CHD patients; 50 HCs. | IBS = 35.4 (12.3); CHD = 50.6 (11.6); HCs = 34.5 (11.7) | MCQ-30 | ASI | IBS mean (SD) scores were MCQ-POS, 18.05 (3.85); MCQ-NEG, 14.88 (4.39); MCQ-CC,16.18 (4.14); MCQ-NC, 14.40 (3.74); MCQ-CSC, 15.98 (3.90). CHD mean (SD) scores were MCQ-POS, 16.18 (4.32); MCQ-NEG, 13.39 (4.05); MCQ-CC,17.34 (4.60); MCQ-NC, 12.90 (3.25); MCQ-CSC, 14.47 (4.48). HCs mean (SD) scores were MCQ-POS, 15.96 (4.91); MCQ-NEG, 14.48 (4.24); MCQ-CC,15.25 (4.02); MCQ-NC, 13.48 (3.71); MCQ-CSC, 14.96 (4.31). IBS showed higher scores on MCQ-POS than HCs (p < 0.05). No significant differences were found between IBS and CHD. |
4. Discussion
5. Conclusions
6. Future Directions
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Fonagy, P.; Target, M. Playing with reality: I. Theory of mind and the normal development of psychic reality. Int. J. Psychoanal. 1996, 77, 217–233. [Google Scholar] [PubMed]
- Luyten, P.; Campbell, C.; Allison, E.; Fonagy, P. The Mentalizing Approach to Psychopathology: State of the Art and Future Directions. Annu. Rev. Clin. Psychol. 2020, 16, 297–325. [Google Scholar] [CrossRef] [PubMed]
- Choi-Kain, L.W.; Gunderson, J.G. Mentalization: Ontogeny, assessment, and application in the treatment of borderline personality disorder. Am. J. Psychiatry 2008, 165, 1127–1135. [Google Scholar] [CrossRef] [PubMed]
- Fonagy, P.; Steele, H.; Steele, M. Maternal representations of attachment during pregnancy predict the organization of infant-mother attachment at one year of age. Child. Dev. 1991, 62, 891–905. [Google Scholar] [CrossRef] [PubMed]
- Fonagy, P.; Target, M. Attachment and reflective function: Their role in self-organization. Dev. Psychopathol. 1997, 9, 679–700. [Google Scholar] [CrossRef] [PubMed]
- Fischer-Kern, M.; Tmej, A. Mentalization and Depression: Theoretical Concepts, Treatment Approaches and Empirical Studies—An Overview. Z. Psychosom. Med. Psychother. 2019, 65, 162–177. [Google Scholar] [CrossRef]
- Stein, H. Does mentalizing promote resilience? In The Handbook of Mentalization-Based Treatment; Allen, J.G., Fonagy, P., Eds.; Wiley: Chichester, UK, 2006; pp. 305–326. [Google Scholar]
- Premack, D.; Woodruff, G. Does the chimpanzee have a theory of mind? Behav. Brain Sci. 1978, 1, 515–526. [Google Scholar] [CrossRef]
- Baron-Cohen, S.; Leslie, A.M.; Frith, U. Does the autistic child have a “theory of mind”? Cognition 1985, 21, 37–46. [Google Scholar] [CrossRef]
- Hasson-Ohayon, I.; Lysaker, P.H. The role of metacognition and mentalization in the recovery of the self: Introduction and overview. In The Recovery of the Self in Psychosis; Routledge: London, UK, 2021; pp. 1–11. [Google Scholar]
- Lysaker, P.H.; Dimaggio, G.; Hamm, J.A.; Leonhardt, B.L.; Hochheiser, J.; Lysaker, J.T. Disturbances in Self-Experience in Schizophrenia: Metacognition and the Development of an Integrative Recovery-Oriented Individual Psychotherapy. Psychopathology 2019, 52, 135–142. [Google Scholar] [CrossRef]
- Katznelson, H. Reflective functioning: A review. Clin. Psychol. Rev. 2014, 34, 107–117. [Google Scholar] [CrossRef]
- Fonagy, P.; Steele, H.; Steele, M.; Holder, J. Attachment and theory of mind: Overlapping constructs? In Association for Child Psychology and Psychiatry Occasional Papers; Taylor and Francis Group: London, UK, 1997; Volume 14, pp. 31–40. [Google Scholar]
- Luyten, P.; van Houdenhove, B.; Lemma, A.; Target, M.; Fonagy, P. A mentalization-based approach to the understanding and treatment of functional somatic disorders. Psychoanal. Psychother. 2012, 26, 121–140. [Google Scholar] [CrossRef]
- Luyten, P.; Fonagy, P. The neurobiology of mentalizing. Personal. Disord. 2015, 6, 366–379. [Google Scholar] [CrossRef]
- McEwen, B.S. Physiology and neurobiology of stress and adaptation: Central role of the brain. Physiol. Rev. 2007, 87, 873–904. [Google Scholar] [CrossRef] [PubMed]
- Simpson, C.A.; Mu, A.; Haslam, N.; Schwartz, O.S.; Simmons, J.G. Feeling down? A systematic review of the gut microbiota in anxiety/depression and irritable bowel syndrome. J. Affect. Disord. 2020, 266, 429–446. [Google Scholar] [CrossRef] [PubMed]
- Schmulson, M.J.; Drossman, D.A. What Is New in Rome IV. J. Neurogastroenterol. Motil. 2017, 23, 151–163. [Google Scholar] [CrossRef]
- Oka, P.; Parr, H.; Barberio, B.; Black, C.J.; Savarino, E.V.; Ford, A.C. Global prevalence of irritable bowel syndrome according to Rome III or IV criteria: A systematic review and meta-analysis. Lancet Gastroenterol. Hepatol. 2020, 5, 908–917. [Google Scholar] [CrossRef]
- Neuendorf, R.; Harding, A.; Stello, N.; Hanes, D.; Wahbeh, H. Depression and anxiety in patients with Inflammatory Bowel Disease: A systematic review. J. Psychosom. Res. 2016, 87, 70–80. [Google Scholar] [CrossRef]
- Fornaro, R.; Actis, G.C.; Caviglia, G.P.; Pitoni, D.; Ribaldone, D.G. Inflammatory Bowel Disease: Role of Vagus Nerve Stimulation. J. Clin. Med. 2022, 11, 5690. [Google Scholar] [CrossRef]
- Gracie, D.J.; Hamlin, P.J.; Ford, A.C. The influence of the brain-gut axis in inflammatory bowel disease and possible implications for treatment. Lancet Gastroenterol. Hepatol. 2019, 4, 632–642. [Google Scholar] [CrossRef]
- Tricco, A.C.; Lillie, E.; Zarin, W.; O’Brien, K.K.; Colquhoun, H.; Levac, D.; Moher, D.; Peters, M.D.J.; Horsley, T.; Weeks, L.; et al. PRISMA Extension for Scoping Reviews (PRISMA-ScR): Checklist and Explanation. Ann. Intern. Med. 2018, 169, 467–473. [Google Scholar] [CrossRef]
- Page, M.J.; McKenzie, J.E.; Bossuyt, P.M.; Boutron, I.; Hoffmann, T.C.; Mulrow, C.D.; Shamseer, L.; Tetzlaff, J.M.; Akl, E.A.; Brennan, S.E.; et al. The PRISMA 2020 statement: An updated guideline for reporting systematic reviews. BMJ 2021, 372, 71. [Google Scholar] [CrossRef] [PubMed]
- Thomas, J.; Kneale, D.; McKenzie, J.E.; Brennan, S.E.; Bhaumik, S. Chapter 2: Determining the scope of the review and the questions it will address. In Cochrane Handbook for Systematic Reviews of Interventions Version 6.2; Higgins, J.P.T., Thomas, J., Chandler, J., Cumpston, M., Li, T., Page, M.J., Welch, V.A., Eds.; Cochrane: London, UK, 2021; Available online: https://www.training.cochrane.org/handbook (accessed on 16 January 2023).
- Berens, S.; Schaefert, R.; Baumeister, D.; Gauss, A.; Eich, W.; Tesarz, J. Does symptom activity explain psychological differences in patients with irritable bowel syndrome and inflammatory bowel disease? Results from a multi-center cross-sectional study. J. Psychosom. Res. 2019, 126, 109836. [Google Scholar] [CrossRef] [PubMed]
- Quattropani, M.C.; Lenzo, V.; Filastro, A.; Fries, W. Metacognitions and basic emotions in patients with irritable bowel syndrome and inflammatory bowel disease. Psicoter. Cogn. Comport. 2019, 25, 35–51. [Google Scholar]
- Berens, S.M.-P.; Schaefert, R.; Ehrenthal, J.C.; Baumeister, D.; Gauss, A.; Eich, W.; Tesarz, J. The Validity of Somatic Symptom Disorder in Patients with Gastrointestinal Complaints. J. Clin. Gastroenterol. 2021, 55, e66–e76. [Google Scholar] [CrossRef] [PubMed]
- Agostini, A.; Scaioli, E.; Belluzzi, A.; Campieri, M. Attachment and Mentalizing Abilities in Patients with Inflammatory Bowel Disease. Gastroenterol. Res. Pract. 2019, 2019, 7847123. [Google Scholar] [CrossRef]
- Dzirlo, L.; Richter, F.; Steinmair, D.; Löffler-Stastka, H. Reflective Functioning in Patients with Irritable Bowel Syndrome, Non-Affective Psychosis and Affective Disorders-Differences and Similarities. Int. J. Environ. Res. Public Health 2021, 18, 2780. [Google Scholar] [CrossRef] [PubMed]
- Engel, F.; Berens, S.; Gauss, A.; Schaefert, R.; Eich, W.; Tesarz, J. Higher Levels of Psychological Burden and Alterations in Personality Functioning in Crohn’s Disease and Ulcerative Colitis. Front. Psychol. 2021, 12, 671493. [Google Scholar] [CrossRef]
- Zargar, F.; Kavoosi, M. Comparing anxiety sensitivity and metacognition beliefs in patients with irritable bowel syndrome and coronary heart diseases: A case-control study. Arch. Psychiatry Psychother. 2021, 23, 53–60. [Google Scholar] [CrossRef]
- Rief, W.; Martin, A. How to use the new DSM-5 somatic symptom disorder diagnosis in research and practice: A critical evaluation and a proposal for modifications. Annu. Rev. Clin. Psychol. 2014, 10, 339–367. [Google Scholar] [CrossRef]
- Zamani, M.; Alizadeh-Tabari, S.; Zamani, V. Systematic review with meta-analysis: The prevalence of anxiety and depression in patients with irritable bowel syndrome. Aliment. Pharmacol. Ther. 2019, 50, 132–143. [Google Scholar] [CrossRef]
- Alsubaie, M.A.; Alkhalifah, H.A.; Ali, A.H.; Bahabri, M.A.; Alharbi, B.A.; Alfakeh, S.A. Adverse Childhood Experiences and Their Effect on Irritable Bowel Syndrome Among Saudi Arabian Adults. Cureus 2022, 14, e25791. [Google Scholar] [CrossRef] [PubMed]
- Bowlby, J. A Secure Base: Parent-Child Attachment and Healthy Human Development; Basic Books: New York, NY, USA, 1988. [Google Scholar]
- Abdel-Hamid, M.; Lehmkämper, C.; Sonntag, C.; Juckel, G.; Daum, I.; Brüne, M. Theory of mind in schizophrenia: The role of clinical symptomatology and neurocognition in understanding other people’s thoughts and intentions. Psychiatry Res. 2009, 165, 19–26. [Google Scholar] [CrossRef] [PubMed]
- Fischer-Kern, M.; Fonagy, P.; Kapusta, N.D.; Luyten, P.; Boss, S.; Naderer, A.; Blüml, V.; Leithner, K. Mentalizing in female inpatients with major depressive disorder. J. Nerv. Ment. Dis. 2013, 201, 202–207. [Google Scholar] [CrossRef] [PubMed]
- Debbané, M.; Salaminios, G.; Luyten, P.; Badoud, D.; Armando, M.; Tozzi, A.S.; Fonagy, P.; Brent, B.K. Attachment, Neurobiology, and Mentalizing along the Psychosis Continuum. Front. Hum. Neurosci. 2016, 10, 406. [Google Scholar] [CrossRef]
- Bodnar, A.; Rybakowski, J.K. Mentalization deficit in bipolar patients during an acute depressive and manic episode: Association with cognitive functions. Int. J. Bipolar Disord. 2017, 5, 38. [Google Scholar] [CrossRef] [PubMed]
- Fonagy, P.; Luyten, P. A developmental, mentalization-based approach to the understanding and treatment of borderline personality disorder. Dev. Psychopathol. 2009, 21, 1355–1381. [Google Scholar] [CrossRef] [PubMed]
- Fonagy, P.; Luyten, P.; Strathearn, L. Borderline personality disorder, mentalization, and the neurobiology of attachment. Infant. Ment. Health J. 2011, 32, 47–69. [Google Scholar] [CrossRef] [PubMed]
- Petersen, R.; Brakoulias, V.; Langdon, R. An experimental investigation of mentalization ability in borderline personality disorder. Compr. Psychiatry 2016, 64, 12–21. [Google Scholar] [CrossRef]
- Kuipers, G.S.; van Loenhout, Z.; van der Ark, L.A.; Bekker, M.H. Attachment insecurity, mentalization and their relation to symptoms in eating disorder patients. Attach. Hum. Dev. 2016, 18, 250–272. [Google Scholar] [CrossRef]
- Rothschild-Yakar, L.; Peled, M.; Enoch-Levy, A.; Gur, E.; Stein, D. “Eating Me Up from Inside”: A Pilot Study of Mentalization of Self and Others and Emotion Regulation Strategies among Young Women with Eating Disorders. Isr. J. Psychiatry 2018, 55, 35–43. [Google Scholar]
- Bizzi, F.; Ensink, K.; Borelli, J.L.; Mora, S.C.; Cavanna, D. Attachment and reflective functioning in children with somatic symptom disorders and disruptive behavior disorders. Eur. Child. Adolesc. Psychiatry 2019, 28, 705–717. [Google Scholar] [CrossRef] [PubMed]
- Cieślak, M.; Kozaka, J.; Golińska, P.B.; Bidzan, M. Mentalization and Its Relation to Life Satisfaction and the Level of Mental Adjustment to Illness in Women with Breast Cancer-A Pilot Study. Int. J. Environ. Res. Public Health 2022, 19, 10323. [Google Scholar] [CrossRef] [PubMed]
- Porcelli, P. Medicina Psicosomatica e Psicologia Clinica; Modelli Teorici, Diagnosi, Trattamento. Nuova Edizione; Raffaello Cortina: Milan, Italy, 2022. [Google Scholar]
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2023 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Benfante, A.; Cisarò, F.; Ribaldone, D.G.; Castelli, L.; Sandroni, N.; Romeo, A. Inflammatory Bowel Disease and Irritable Bowel Syndrome: What Differences in Mentalization Abilities? A Scoping Review. Int. J. Environ. Res. Public Health 2023, 20, 7125. https://doi.org/10.3390/ijerph20237125
Benfante A, Cisarò F, Ribaldone DG, Castelli L, Sandroni N, Romeo A. Inflammatory Bowel Disease and Irritable Bowel Syndrome: What Differences in Mentalization Abilities? A Scoping Review. International Journal of Environmental Research and Public Health. 2023; 20(23):7125. https://doi.org/10.3390/ijerph20237125
Chicago/Turabian StyleBenfante, Agata, Fabio Cisarò, Davide Giuseppe Ribaldone, Lorys Castelli, Nikolas Sandroni, and Annunziata Romeo. 2023. "Inflammatory Bowel Disease and Irritable Bowel Syndrome: What Differences in Mentalization Abilities? A Scoping Review" International Journal of Environmental Research and Public Health 20, no. 23: 7125. https://doi.org/10.3390/ijerph20237125
APA StyleBenfante, A., Cisarò, F., Ribaldone, D. G., Castelli, L., Sandroni, N., & Romeo, A. (2023). Inflammatory Bowel Disease and Irritable Bowel Syndrome: What Differences in Mentalization Abilities? A Scoping Review. International Journal of Environmental Research and Public Health, 20(23), 7125. https://doi.org/10.3390/ijerph20237125








