Relationships between Physical Activity and Selected Chronic Diseases among Functionally Independent Long-Term Care Residents during the Post-Lockdown Period in Croatia
Abstract
1. Introduction
2. Materials and Methods
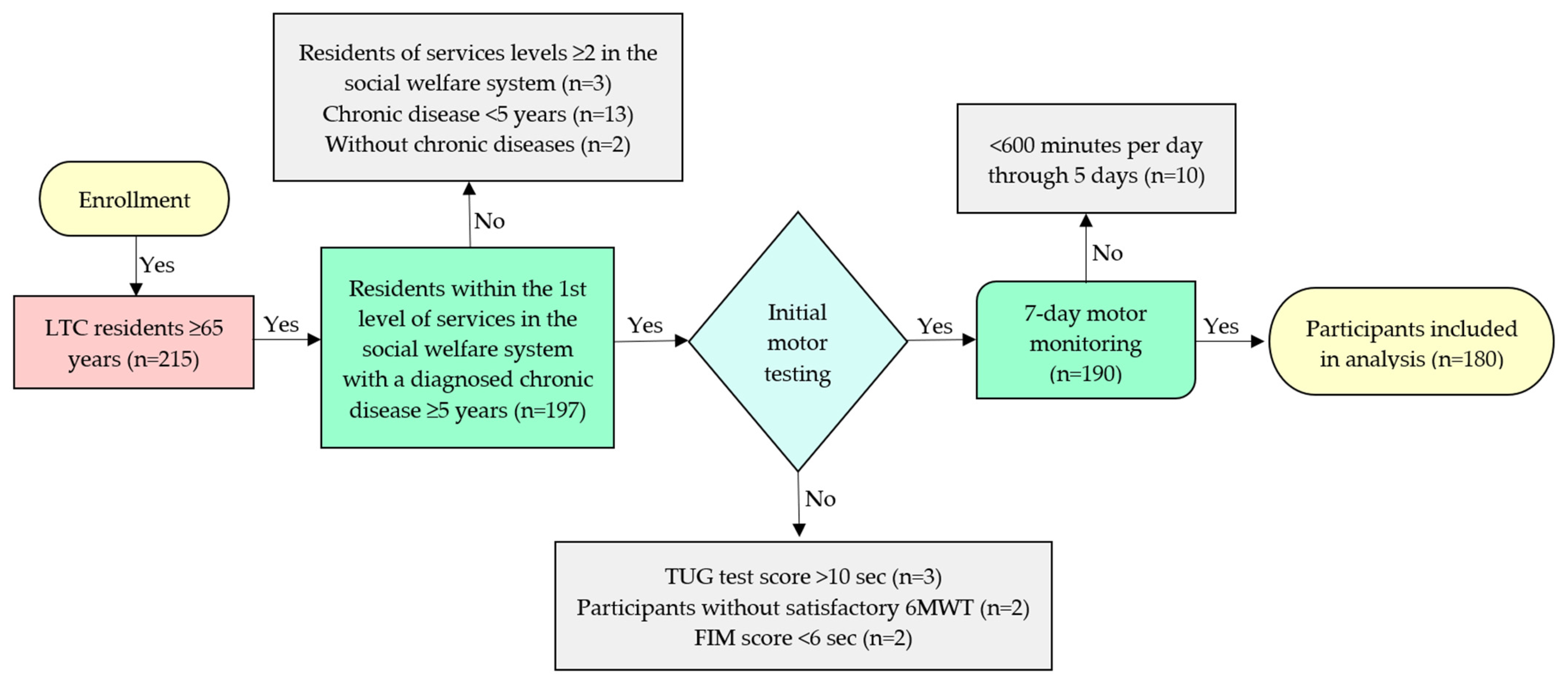
2.1. Study Design, Setting, and Participants
2.2. Measurements
2.3. Procedure
3. Data Analysis
4. Results
5. Multiple Regression
6. Discussion
7. Suggestions for Future Research
8. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Cockerham, W.C.; Hamby, B.W.; Oates, G.R. The Social Determinants of Chronic Disease. Am. J. Prev. Med. 2017, 52, S5–S12. [Google Scholar] [CrossRef] [PubMed]
- OECD/European Union. Health at a Glance: Europe 2022: State of Health in the EU Cycle; OECD Publishing: Paris, France, 2022. [Google Scholar] [CrossRef]
- Börsch-Supan, A. Survey of Health, Ageing and Retirement in Europe (SHARE) Wave 8. 2022, Release Version: 8.0.0. SHARE-ERIC. Data Set. Available online: https://share-eric.eu/data/data-documentation/waves-overview/wave-8 (accessed on 15 June 2023).
- Bergmann, M.; Börsch-Supan, A. SHARE Wave 8 Methodology: Collecting Cross-National Survey Data in Times of COVID-19; MEA, Max Planck Institute for Social Law and Social Policy: Munich, Germany, 2021. [Google Scholar]
- Börsch-Supan, A.; Brandt, M.; Hunkler, C.; Kneip, T.; Korbmacher, J.; Malter, F.; Schaan, B.; Stuck, S.; Zuber, S.; SHARE Central Coordination Team. Data Resource Profile: The Survey of Health, Ageing and Retirement in Europe (SHARE). Int. J. Epidemiol. 2013, 42, 992–1001. [Google Scholar] [CrossRef] [PubMed]
- Fabbri, E.; Zoli, M.; Gonzalez-Freire, M.; Salive, M.E.; Studenski, S.A.; Ferrucci, L. Aging and Multimorbidity: New Tasks, Priorities, and Frontiers for Integrated Gerontological and Clinical Research. J. Am. Med. Dir. Assoc. 2015, 16, 640–647. [Google Scholar] [CrossRef] [PubMed]
- Hudon, C.; Soubhi, H.; Fortin, M. Relationship between multimorbidity and physical activity: Secondary analysis from the Quebec health survey. BMC Public Health 2008, 8, 304. [Google Scholar] [CrossRef]
- Bayliss, E.A.; Bayliss, M.S.; Ware, J.E., Jr.; Steiner, J.F. Predicting declines in physical function in persons with multiple chronic medical conditions: What we can learn from the medical problem list. Health Qual. Life Outcomes 2004, 2, 47. [Google Scholar] [CrossRef]
- World Health Organization. Global Status Report on Noncommunicable Diseases 2014; World Health Organization: Geneva, Switzerland, 2014; Available online: https://apps.who.int/iris/handle/10665/148114 (accessed on 15 June 2023).
- World Health Organization. World Report on Ageing and Health; World Health Organization: Geneva, Switzerland, 2015; Available online: https://apps.who.int/iris/handle/10665/186463 (accessed on 15 June 2023).
- Booth, F.W.; Roberts, C.K.; Laye, M.J. Lack of exercise is a major cause of chronic diseases. Compr. Physiol. 2012, 2, 1143–1211. [Google Scholar] [CrossRef]
- Warburton, D.E.; Nicol, C.W.; Bredin, S.S. Health benefits of physical activity: The evidence. Can. Med. Assoc. J. 2006, 174, 801–809. [Google Scholar] [CrossRef]
- Anderson, E.; Durstine, J.L. Physical activity, exercise, and chronic diseases: A brief review. Sport. Med. Health Sci. 2019, 1, 3–10. [Google Scholar] [CrossRef]
- World Health Organization. Global Recommendations on Physical Activity for Health; World Health Organization: Geneva, Switzerland, 2010; Available online: https://apps.who.int/iris/handle/10665/44399 (accessed on 5 February 2022).
- Ministry of Health. Guidelines on Physical Activity for Older People (Aged 65 Years and Over); Ministry of Health: Wellington, New Zealand, 2013.
- Ashe, M.C.; Miller, W.C.; Eng, J.J.; Noreau, L.; Physical Activity and Chronic Conditions Research Team. Older adults, chronic disease and leisure-time physical activity. Gerontology 2009, 55, 64–72. [Google Scholar] [CrossRef]
- Ruegsegger, G.N.; Booth, F.W. Health Benefits of Exercise. Cold Spring Harb. Perspect. Med. 2018, 8, a029694. [Google Scholar] [CrossRef]
- Leung, K.W.; Sum, K.R.; Yang, Y.J. Patterns of Sedentary Behavior among Older Adults in Care Facilities: A Scoping Review. Int. J. Environ. Res. Public Health 2021, 18, 2710. [Google Scholar] [CrossRef]
- Ramocha, L.M.; Louw, Q.A.; Tshabalala, M.D. Quality of life and physical activity among older adults living in institutions compared to the community. S. Afr. J. Physiother. 2017, 73, 342. [Google Scholar] [CrossRef]
- Dhama, K.; Patel, S.K.; Kumar, R.; Rana, J.; Yatoo, M.I.; Kumar, A.; Tiwari, R.; Dhama, J.; Natesan, S.; Singh, R.; et al. Geriatric Population During the COVID-19 Pandemic: Problems, Considerations, Exigencies, and Beyond. Front. Public Health 2020, 8, 574198. [Google Scholar] [CrossRef]
- Croatia’s National Civil Protection Headquarters. Decision on Necessary Epidemiological Measures Restricting Gatherings and Introducing other Necessary Epidemiological Measures and Recommendations to Prevent the Transmission of COVID-19 Disease. Available online: https://civilna-zastita.gov.hr/odluke-stozera-civilne-zastite-rh-za-sprecavanje-sirenja-zaraze-koronavirusom/2304 (accessed on 18 March 2020).
- Ministry of Social Policy and Youth. Ordinance on Minimum Conditions for the Provision of Social Services. Official Gazette No. 40. 2014. Available online: https://narodne-novine.nn.hr/clanci/sluzbeni/2014_03_40_712.html (accessed on 1 March 2020).
- Kolarić, B.; Vranešić Bender, D.; Pavić, E. Nutrition-Gerontological Norms/Menus in Homes for the Elderly and Gerontological Centers; Ministry of Health of the Republic of Croatia: Zagreb, Croatia, 2020.
- Croatian Bureau of Statistics. Available online: https://www.dzs.hr/Hrv_Eng/publication/2019/07-01-03_01_2019.htm (accessed on 5 June 2020).
- City Office for the Strategic Planning and Development of the City. Statistical Yearbook of the City of Zagreb. 2019. Available online: https://www.zagreb.hr/UserDocsImages/arhiva/statistika/statisticki%20ljetopis%202019_digital.pdf (accessed on 5 June 2020).
- World Health Organization. International Statistical Classification of Diseases and Related Health Problems, 10th Revision, 5th ed.; World Health Organization: Geneva, Switzerland, 2016; Available online: https://apps.who.int/iris/handle/10665/246208 (accessed on 1 March 2020).
- ATS Committee on Proficiency Standards for Clinical Pulmonary Function Laboratories. ATS statement: Guidelines for the six-minute walk test. Am. J. Respir. Crit. Care Med. 2002, 166, 111–117, Erratum in: Am. J. Respir. Crit. Care Med. 2016, 193, 1185. [Google Scholar] [CrossRef]
- Podsiadlo, D.; Richardson, S. The timed “Up & Go”: A test of basic functional mobility for frail elderly persons. J. Am. Geriatr. Soc. 1991, 39, 142–148. [Google Scholar] [CrossRef]
- Keith, R.A.; Granger, C.V.; Hamilton, B.B.; Sherwin, F.S. The functional independence measure: A new tool for rehabilitation. Adv. Clin. Rehabil. 1987, 1, 6–18. [Google Scholar]
- Health Care Act of the Republic of Croatia. NN 158/08, 71/10, 139/10, 22/11, 84/11, 12/12, 35/12, 70/12 i 82/13. Available online: https://www.zakon.hr/z/190/Zakon-o-zdravstvenoj-za%C5%A1titi (accessed on 3 January 2020).
- Patients’ Rights Act of the Republic of Croatia. NN 169/04, 37/08. Available online: https://www.zakon.hr/z/255/Zakon-o-za%C5%A1titi-prava-pacijenata (accessed on 3 January 2020).
- Croatian Institute of Public Health. Recommendations for Preserving the Health of People over 60 Years of Age and Suffering from Chronic Diseases. 2021. Available online: https://www.hzjz.hr/ (accessed on 10 May 2021).
- Croatian Institute of Public Health. Protection Measures against Respiratory Infections, Including SARS-CoV-2, for People with Chronic Diseases and the Elderly. 2021. Available online: https://www.hzjz.hr/ (accessed on 10 May 2021).
- Teaching Institute of Public Health, Andrija Štampar“. Recommendations for Preserving the Health of Persons over 65 Years of Age and Chronically Ill Patients (COVID-19). 2021. Available online: https://www.stampar.hr/hr (accessed on 10 May 2021).
- SAS Institute Inc. SAS® 9.4 and SAS® Viya® 3.4 Programming Documentation; SAS Institute Inc.: Cary, NC, USA, 2019. [Google Scholar]
- Oliveira, M.R.; Sudati, I.P.; Konzen, V.M.; de Campos, A.C.; Wibelinger, L.M.; Correa, C.; Miguel, F.M.; Silva, R.N.; Borghi-Silva, A. COVID-19 and the impact on the physical activity level of elderly people: A systematic review. Exp. Gerontol. 2022, 159, 111675. [Google Scholar] [CrossRef]
- Sasaki, S.; Sato, A.; Tanabe, Y.; Matsuoka, S.; Adachi, A.; Kayano, T.; Yamazaki, H.; Matsuno, Y.; Miyake, A.; Watanabe, T. Associations between Socioeconomic Status, Social Participation, and Physical Activity in Older People during the COVID-19 Pandemic: A Cross-Sectional Study in a Northern Japanese City. Int. J. Environ. Res. Public Health 2021, 18, 1477. [Google Scholar] [CrossRef]
- Sweeney, M.R.; Boilson, A.; White, C.; Nevin, M.; Casey, B.; Boylan, P.; Staines, A. Experiences of residents, family members and staff in residential care settings for older people during COVID-19: A mixed methods study. J. Nurs. Manag. 2022, 30, 872–882. [Google Scholar] [CrossRef]
- Yamada, M.; Kimura, Y.; Ishiyama, D.; Otobe, Y.; Suzuki, M.; Koyama, S.; Kikuchi, T.; Kusumi, H.; Arai, H. The Influence of the COVID-19 Pandemic on Physical Activity and New Incidence of Frailty among Initially Non-Frail Older Adults in Japan: A Follow-Up Online Survey. J. Nutr. Health Aging. 2021, 25, 751–756. [Google Scholar] [CrossRef]
- Nygård, A.J.; Taraldsen, K.; Granbo, R.; Selbæk, G.; Helbostad, J.L. Impacts of COVID-19 restrictions on level of physical activity and health in home-dwelling older adults in Norway. Eur. Rev. Aging Phys. Act. 2022, 19, 30. [Google Scholar] [CrossRef] [PubMed]
- Shinohara, T.; Saida, K.; Tanaka, S.; Murayama, A. Association between frailty and changes in lifestyle and physical or psychological conditions among older adults affected by the coronavirus disease 2019 countermeasures in Japan. Geriatr. Gerontol. Int. 2021, 21, 39–42. [Google Scholar] [CrossRef] [PubMed]
- Douma, J.G.; Volkers, K.M.; Engels, G.; Sonneveld, M.H.; Goossens, R.H.M.; Scherder, E.J.A. Setting-related influences on physical inactivity of older adults in residential care settings: A review. BMC Geriatr. 2017, 17, 97. [Google Scholar] [CrossRef] [PubMed]
- Auerswald, T.; Meyer, J.; von Holdt, K.; Voelcker-Rehage, C. Application of Activity Trackers among Nursing Home Residents-A Pilot and Feasibility Study on Physical Activity Behavior, Usage Behavior, Acceptance, Usability and Motivational Impact. Int. J. Environ. Res. Public Health 2020, 17, 6683. [Google Scholar] [CrossRef]
- Bains, N.; Abdijadid, S. Major Depressive Disorder. In StatPearls [Internet]; StatPearls Publishing: Treasure Island, FL, USA, 2023. [Google Scholar]
- Proudman, D.; Greenberg, P.; Nellesen, D. The Growing Burden of Major Depressive Disorders (MDD): Implications for Researchers and Policy Makers. Pharmacoeconomics 2021, 39, 619–625. [Google Scholar] [CrossRef]
- Lebrasseur, A.; Fortin-Bédard, N.; Lettre, J.; Raymond, E.; Bussières, E.L.; Lapierre, N.; Faieta, J.; Vincent, C.; Duchesne, L.; Ouellet, M.C.; et al. Impact of the COVID-19 Pandemic on Older Adults: Rapid Review. JMIR Aging 2021, 4, e26474. [Google Scholar] [CrossRef]
- Docherty, S.; Haskell-Ramsay, C.F.; McInnes, L.; Wetherell, M.A. The Effects of COVID-19 Lockdown on Health and Psychosocial Functioning in Older Adults Aged 70 and over. Gerontol. Geriatr. Med. 2021, 7, 23337214211039974. [Google Scholar] [CrossRef]
- Briggs, R.; McDowell, C.P.; De Looze, C.; Kenny, R.A.; Ward, M. Depressive Symptoms Among Older Adults Pre- and Post-COVID-19 Pandemic. J. Am. Med. Dir. Assoc. 2021, 22, 2251–2257. [Google Scholar] [CrossRef]
- Sepúlveda-Loyola, W.; Rodríguez-Sánchez, I.; Pérez-Rodríguez, P.; Ganz, F.; Torralba, R.; Oliveira, D.V.; Rodríguez-Mañas, L. Impact of Social Isolation Due to COVID-19 on Health in Older People: Mental and Physical Effects and Recommendations. J. Nutr. Health Aging 2020, 24, 938–947. [Google Scholar] [CrossRef]
- Cortés Zamora, E.B.; Mas Romero, M.; Tabernero Sahuquillo, M.T.; Avendaño Céspedes, A.; Andrés-Petrel, F.; Gómez Ballesteros, C.; Sánchez-Flor Alfaro, V.; López-Bru, R.; López-Utiel, M.; Celaya Cifuentes, S.; et al. Psychological and Functional Impact of COVID-19 in Long-Term Care Facilities: The COVID-A Study. Am. J. Geriatr. Psychiatry 2022, 30, 431–443. [Google Scholar] [CrossRef]
- Cai, H.; Jin, Y.; Liu, R.; Zhang, Q.; Su, Z.; Ungvari, G.S.; Tang, Y.L.; Ng, C.H.; Li, X.H.; Xiang, Y.T. Global prevalence of depression in older adults: A systematic review and meta-analysis of epidemiological surveys. Asian J. Psychiatr. 2023, 80, 103417. [Google Scholar] [CrossRef]
- Harvey, J.A.; Chastin, S.F.; Skelton, D.A. Prevalence of sedentary behavior in older adults: A systematic review. Int. J. Environ. Res. Public Health 2013, 10, 6645–6661. [Google Scholar] [CrossRef]
- Moreno-Martin, P.; Jerez-Roig, J.; Rierola-Fochs, S.; Oliveira, V.R.; Farrés-Godayol, P.; Bezerra de Souza, D.L.; Giné-Garriga, M.; Booth, J.; Skelton, D.A.; Minobes-Molina, E. Incidence and Predictive Factors of Functional Decline in Older People Living in Nursing Homes: A Systematic Review. J. Am. Med. Dir. Assoc. 2022, 23, 1815–1825.e9. [Google Scholar] [CrossRef]
- Snowdon, J. Depression in nursing homes. Int. Psychogeriatr. 2010, 22, 1143–1148. [Google Scholar] [CrossRef]
- Liubicich, M.; Magistro, D.; Candela, F.; Rabaglietti, E.; Ciairano, S. Physical Activity and Mobility Function in Elderly People Living in Residential Care Facilities. “Act on Aging”: A Pilot Study. Adv. Phys. Educ. 2012, 2, 54–60. [Google Scholar] [CrossRef]
- Cacioppo, J.T.; Hawkley, L.C. Perceived social isolation and cognition. Trends Cogn. Sci. 2009, 13, 447–454. [Google Scholar] [CrossRef]
- Gujral, S.; Aizenstein, H.; Reynolds, C.F., 3rd; Butters, M.A.; Erickson, K.I. Exercise effects on depression: Possible neural mechanisms. Gen. Hosp. Psychiatry 2017, 49, 2–10. [Google Scholar] [CrossRef]
- Huang, Y.; Li, L.; Gan, Y.; Wang, C.; Jiang, H.; Cao, S.; Lu, Z. Sedentary behaviors and risk of depression: A meta-analysis of prospective studies. Transl. Psychiatry 2020, 10, 26. [Google Scholar] [CrossRef]
- Zhang, K.; Kim, K.; Silverstein, N.M.; Song, Q.; Burr, J.A. Social Media Communication and Loneliness Among Older Adults: The Mediating Roles of Social Support and Social Contact. Gerontologist 2021, 61, 888–896. [Google Scholar] [CrossRef]
- Hawker, G.A. Osteoarthritis is a serious disease. Clin. Exp. Rheumatol. 2019, 37 (Suppl. S120), 3–6. [Google Scholar]
- Krishnapillai, A.; Omar, M.A.; Ariaratnam, S.; Awaluddin, S.; Sooryanarayana, R.; Kiau, H.B.; Tauhid, N.M.; Ghazali, S.S. The Prevalence of Anemia and Its Associated Factors among Older Persons: Findings from the National Health and Morbidity Survey (NHMS) 2015. Int. J. Environ. Res. Public Health 2022, 19, 4983. [Google Scholar] [CrossRef]
- Cegla, T.H.; Magner, A. Einfluss der Coronapandemie auf Schmerzpatienten: Welche Auswirkungen der Pandemie auf ihre Versorgung nehmen Patienten mit chronischen Schmerzen wahr? [Influence of the corona pandemic on pain patients: Which impacts of the pandemic on their care do patients with chronic pain experience?]. Schmerz 2021, 35, 188–194. [Google Scholar] [CrossRef]
- Endstrasser, F.; Braito, M.; Linser, M.; Spicher, A.; Wagner, M.; Brunner, A. The negative impact of the COVID-19 lockdown on pain and physical function in patients with end-stage hip or knee osteoarthritis. Knee Surg. Sports Traumatol. Arthrosc. 2020, 28, 2435–2443. [Google Scholar] [CrossRef] [PubMed]
- Román Belmonte, J.M.; Muñoz de la Torre, E.; Vázquez Sasot, A.; Sánchez Polo, M.T.; Rodríguez Damiani, B.A.; Resino Luís, C. Impacto del confinamiento en el ejercicio físico de los pacientes con artrosis durante la pandemia COVID-19 [Impact of lockdown on physical activity of patients with osteoarthritis during the COVID-19 pandemic]. Rehabilitacion 2023, 57, 100732. [Google Scholar] [CrossRef] [PubMed]
- O’Neill, T.W.; Felson, D.T. Mechanisms of Osteoarthritis (OA) Pain. Curr. Osteoporos. Rep. 2018, 16, 611–616. [Google Scholar] [CrossRef] [PubMed]
- Fawole, H.O.; Idowu, O.A.; Abaraogu, U.O.; Dell’Isola, A.; Riskowski, J.L.; Oke, K.I.; Adeniyi, A.F.; Mbada, C.E.; Steultjens, M.P.; Chastin, S.F.M. Factors associated with fatigue in hip and/or knee osteoarthritis: A systematic review and best evidence synthesis. Rheumatol. Adv. Pract. 2021, 5, rkab013. [Google Scholar] [CrossRef]
- Penninx, B.W.; Pahor, M.; Cesari, M.; Corsi, A.M.; Woodman, R.C.; Bandinelli, S.; Guralnik, J.M.; Ferrucci, L. Anemia is associated with disability and decreased physical performance and muscle strength in the elderly. J. Am. Geriatr. Soc. 2004, 52, 719–724. [Google Scholar] [CrossRef]
- Marzban, M.; Nabipour, I.; Farhadi, A.; Ostovar, A.; Larijani, B.; Darabi, A.H.; Shabankari, E.; Gholizade, M. Association between anemia, physical performance and cognitive function in Iranian elderly people: Evidence from Bushehr Elderly Health (BEH) program. BMC Geriatr. 2021, 21, 329. [Google Scholar] [CrossRef]
- Lima, L.V.; Abner, T.S.S.; Sluka, K.A. Does exercise increase or decrease pain? Central mechanisms underlying these two phenomena. J. Physiol. 2017, 595, 4141–4150. [Google Scholar] [CrossRef]
- Peterson, J.A.; Staud, R.; Thomas, P.A.; Goodin, B.R.; Fillingim, R.B.; Cruz-Almeida, Y. Self-reported pain and fatigue are associated with physical and cognitive function in middle to older-aged adults. Geriatr. Nurs. 2023, 50, 7–14. [Google Scholar] [CrossRef]
- Elliott, J.; Munford, L.; Ahmed, S.; Littlewood, A.; Todd, C. The impact of COVID-19 lockdowns on physical activity amongst older adults: Evidence from longitudinal data in the UK. BMC Public Health 2022, 22, 1802. [Google Scholar] [CrossRef]
- Valderas, J.M.; Starfield, B.; Sibbald, B.; Salisbury, C.; Roland, M. Defining comorbidity: Implications for understanding health and health services. Ann. Fam. Med. 2009, 7, 357–363. [Google Scholar] [CrossRef]
- Russell, C.D.; Lone, N.I.; Baillie, J.K. Comorbidities, multimorbidity and COVID-19. Nat. Med. 2023, 29, 334–343. [Google Scholar] [CrossRef]
- Ismail, H.; Marshall, V.D.; Patel, M.; Tariq, M.; Mohammad, R.A. The impact of the COVID-19 pandemic on medical conditions and medication adherence in people with chronic diseases. J. Am. Pharm. Assoc. 2022, 62, 834–839.e1. [Google Scholar] [CrossRef]
- Delpino, F.M.; Caputo, E.L.; da Silva, M.C.; Reichert, F.F.; Nunes, B.P.; Feter, N.; Leite, J.S.; Cassuriaga, J.; Huckembeck, C.M.; Alt, R.; et al. Incidence of multimorbidity and associated factors during the COVID-19 pandemic in Brazil: A cohort study. Sao Paulo Med. J. 2022, 140, 447–453. [Google Scholar] [CrossRef]
- Ruzafa-Martinez, M.; García-González, J.; Morales-Asencio, J.M.; Leal-Costa, C.; Hernández-Méndez, S.; Hernández-López, M.J.; Albarracín-Olmedo, J.; Ramos-Morcillo, A.J. Consequences of the COVID-19 pandemic on complex multimorbid elderly: Follow-up of a community-based cohort. SAMAC3 Study. J. Nurs. Scholarsh. 2022, 1–13. [Google Scholar] [CrossRef]
- Pérez-Gisbert, L.; Torres-Sánchez, I.; Ortiz-Rubio, A.; Calvache-Mateo, A.; López-López, L.; Cabrera-Martos, I.; Valenza, M.C. Effects of the COVID-19 Pandemic on Physical Activity in Chronic Diseases: A Systematic Review and Meta-Analysis. Int. J. Environ. Res. Public Health 2021, 18, 12278. [Google Scholar] [CrossRef]
- Esain, I.; Gil, S.M.; Duñabeitia, I.; Rodriguez-Larrad, A.; Bidaurrazaga-Letona, I. Effects of COVID-19 Lockdown on Physical Activity and Health-Related Quality of Life in Older Adults Who Regularly Exercise. Sustainability 2021, 13, 3771. [Google Scholar] [CrossRef]
| Demographic Characteristics | |||
|---|---|---|---|
| Age ( = 81.18, SD = 4.54) | |||
| N | % | ||
| Gender | M | 48 | 26.7 |
| F | 132 | 73.3 | |
| Marital status | Unmarried | 12 | 6.7 |
| Lives in a marital or extramarital union | 39 | 21.7 | |
| Divorced | 21 | 11.7 | |
| Widowed | 108 | 60.0 | |
| Educational level | No education | 6 | 3.3 |
| Primary school | 16 | 8.9 | |
| High school | 133 | 73.9 | |
| Bachelor’s degree | 11 | 6.1 | |
| Master’s degree | 14 | 7.8 | |
| Anthropometric characteristic | |||
| Height ( = 166.2, SD = 9.23) | |||
| Weight ( = 71.36, SD = 9.59) | |||
| Health characteristics | |||
| N | % | ||
| Number of chronic diseases | 1 | 37 | 20.6 |
| 2 | 86 | 47.8 | |
| ≥3 | 57 | 31.7 | |
| Comorbidities | Angina pectoris | 7 | 3.9 |
| Asthma | 6 | 3.3 | |
| Cerebrovascular accident | 27 | 15.0 | |
| Type 2 Diabetes Mellitus | 28 | 15.6 | |
| Hypertension | 115 | 63.9 | |
| Chronic Obstructive Pulmonary Disease (COPD) | 7 | 3.9 | |
| Chronic bronchitis | 9 | 5.0 | |
| Osteoarthritis | 42 | 23.3 | |
| Osteoporosis | 25 | 13.9 | |
| Major depressive disorder, recurrent | 6 | 3.3 | |
| Suffered from heart attack | 17 | 9.4 | |
| Rheumatoid arthritis | 56 | 31.1 | |
| Iron deficiency anemia | 18 | 10.0 | |
| Cardiac arrhythmia | 20 | 11.1 | |
| SD | Minimum | Maximum | Median | ||
|---|---|---|---|---|---|
| Steps | 5058.74 | 3237.66 | 482 | 17,567 | 4441.00 |
| Distance (km) | 3.22 | 2.08 | 0.33 | 10.71 | 2.67 |
| Energy Expenditure (kcal) | 114.36 | 85.04 | 8.00 | 442.00 | 93.50 |
| SD | Minimum | Maximum | Median | ||
|---|---|---|---|---|---|
| Steps | 5940.73 | 3527.10 | 1361.00 | 16,631.00 | 5661.00 |
| Distance (km) | 3.82 | 2.26 | 0.96 | 9.64 | 3.37 |
| Energy Expenditure (kcal) | 139.97 | 94.23 | 24.00 | 382.00 | 110.00 |
| SD | Minimum | Maximum | Median | ||
|---|---|---|---|---|---|
| Steps | 5660.28 | 3412.77 | 482.00 | 17,567.00 | 4921.50 |
| Distance (km) | 3.59 | 2.18 | 0.33 | 10.71 | 2.97 |
| Energy Expenditure (kcal) | 128.17 | 89.35 | 9.00 | 442.00 | 101.00 |
| SD | Minimum | Maximum | Median | ||
|---|---|---|---|---|---|
| Steps | 3578.63 | 2128.58 | 484.00 | 9945.00 | 3173.00 |
| Distance (km) | 2.29 | 1.41 | 0.34 | 6.99 | 2.00 |
| Energy Expenditure (kcal) | 76.89 | 55.98 | 8.00 | 269.00 | 66.00 |
| Log (Steps) | Log (Distance) | Log (Energy Expenditure) | |||||||
|---|---|---|---|---|---|---|---|---|---|
| Par. Estimate | Pr > F | exp(Par. Estimate) | Par. Estimate | Pr > F | exp(Par. Estimate) | Par. Estimate | Pr > F | exp(Par. Estimate) | |
| Major depressive disorder | −0.86 | 0.0001 | 0.42 | −0.80 | 0.0002 | 0.45 | −0.83 | 0.0008 | 0.44 |
| Osteoarthritis | −0.36 | 0.0001 | 0.70 | −0.33 | 0.0004 | 0.72 | −0.42 | 0.0001 | 0.66 |
| Iron deficiency anemia | −0.44 | 0.0010 | 0.64 | −0.41 | 0.0024 | 0.66 | −0.43 | 0.0073 | 0.65 |
| Comorbidities | - | - | - | −0.08 | 0.1360 | 0.92 | −0.10 | 0.1270 | 0.91 |
| Age | −0.05 | <.0001 | 0.95 | −0.05 | <.0001 | 0.95 | −0.07 | <.0001 | 0.94 |
| Educational level | 0.15 | 0.0038 | 1.16 | 0.15 | 0.0050 | 1.16 | 0.16 | 0.0105 | 1.17 |
| Male participants | 0.28 | 0.0020 | 1.32 | 0.28 | 0.0018 | 1.32 | 0.35 | 0.0007 | 1.43 |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2023 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Crnković, I.; Lončarek, K.; Železnik, D.; Ledinski Fičko, S.; Vlahović, T.; Režan, R.; Knežević, G. Relationships between Physical Activity and Selected Chronic Diseases among Functionally Independent Long-Term Care Residents during the Post-Lockdown Period in Croatia. Int. J. Environ. Res. Public Health 2023, 20, 6301. https://doi.org/10.3390/ijerph20136301
Crnković I, Lončarek K, Železnik D, Ledinski Fičko S, Vlahović T, Režan R, Knežević G. Relationships between Physical Activity and Selected Chronic Diseases among Functionally Independent Long-Term Care Residents during the Post-Lockdown Period in Croatia. International Journal of Environmental Research and Public Health. 2023; 20(13):6301. https://doi.org/10.3390/ijerph20136301
Chicago/Turabian StyleCrnković, Ivana, Karmen Lončarek, Danica Železnik, Sanja Ledinski Fičko, Tomislav Vlahović, Robert Režan, and Goran Knežević. 2023. "Relationships between Physical Activity and Selected Chronic Diseases among Functionally Independent Long-Term Care Residents during the Post-Lockdown Period in Croatia" International Journal of Environmental Research and Public Health 20, no. 13: 6301. https://doi.org/10.3390/ijerph20136301
APA StyleCrnković, I., Lončarek, K., Železnik, D., Ledinski Fičko, S., Vlahović, T., Režan, R., & Knežević, G. (2023). Relationships between Physical Activity and Selected Chronic Diseases among Functionally Independent Long-Term Care Residents during the Post-Lockdown Period in Croatia. International Journal of Environmental Research and Public Health, 20(13), 6301. https://doi.org/10.3390/ijerph20136301






