Dieting Behavior Characterized by Caloric Restriction and Relation to Sleep: A Brief Contemporary Review
Abstract
1. Introduction
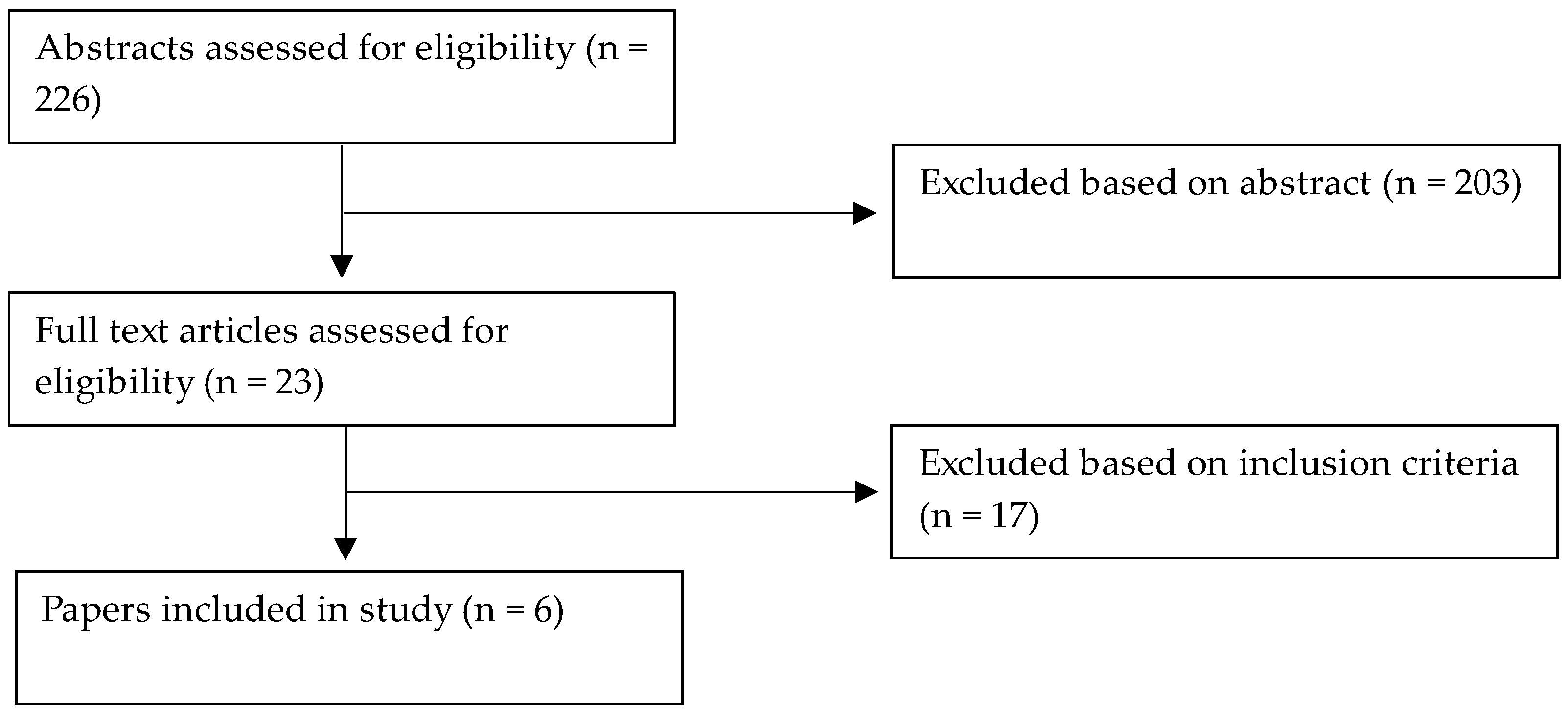
2. Materials and Methods
Sleep Outcome Descriptions
3. Results
3.1. Caloric Restriction and Sleep Outcome
3.2. Caloric Restriction within Specific Diets and Sleep
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Hales, C.M.; Fryar, C.D.; Ogden, C.L. Prevalence of Obesity and Severe Obesity among Adults: United States, 2017–2018; National Center for Health Statistics: Hyattsville, MA, USA, 2020. [Google Scholar]
- Han, L.; You, D.; Zeng, F.; Feng, X.; Astell-Burt, T.; Duan, S.; Qi, L. Trends in Self-perceived Weight Status, Weight Loss Attempts, and Weight Loss Strategies Among Adults in the United States, 1999–2016. JAMA Netw. Open 2019, 2, e1915219. [Google Scholar] [CrossRef]
- Ford, E.S.; Cunningham, T.J.; Croft, J.B. Trends in Self-Reported Sleep Duration among US Adults from 1985 to 2012. Sleep 2015, 38, 829–832. [Google Scholar] [CrossRef] [PubMed]
- Ogilvie, R.P.; Patel, S.R. The epidemiology of sleep and obesity. Sleep Health 2017, 3, 383–388. [Google Scholar] [CrossRef] [PubMed]
- Beccuti, G.; Pannain, S. Sleep and obesity. Curr. Opin. Clin. Nutr. Metab. Care 2011, 14, 402–412. [Google Scholar] [CrossRef] [PubMed]
- Kwok, C.S.; Kontopantelis, E.; Kuligowski, G.; Gray, M.; Muhyaldeen, A.; Gale, C.P.; Peat, G.M.; Cleator, J.; Chew-Graham, C.; Loke, Y.K.; et al. Self-Reported Sleep Duration and Quality and Cardiovascular Disease and Mortality: A Dose-Response Meta-Analysis. J. Am. Heart Assoc. 2018, 7, e008552. [Google Scholar] [CrossRef] [PubMed]
- St-Onge, M.-P.; Grandner, M.A.; Brown, D.; Conroy, M.B.; Jean-Louis, G.; Coons, M.; Bhatt, D.L. Sleep Duration and Quality: Impact on Lifestyle Behaviors and Cardiometabolic Health: A Scientific Statement From the American Heart Association. Circulation 2016, 134, e367–e386. [Google Scholar] [CrossRef]
- Chaput, J.P. Sleep patterns, diet quality and energy balance. Physiol. Behav. 2014, 134, 86–91. [Google Scholar] [CrossRef] [PubMed]
- Lutter, M.; Nestler, E.J. Homeostatic and hedonic signals interact in the regulation of food intake. J. Nutr. 2009, 139, 629–632. [Google Scholar] [CrossRef]
- St-Onge, M.P.; Wolfe, S.; Sy, M.; Shechter, A.; Hirsch, J. Sleep restriction increases the neuronal response to unhealthy food in normal-weight individuals. Int. J. Obes. 2014, 38, 411–416. [Google Scholar] [CrossRef]
- Bales, C.W.; Kraus, W.E. Caloric restriction: Implications for human cardiometabolic health. J. Cardiopulm. Rehabil. Prev. 2013, 33, 201–208. [Google Scholar] [CrossRef]
- Speakman, J.R.; Mitchell, S.E. Caloric restriction. Mol. Aspects Med. 2011, 32, 159–221. [Google Scholar] [CrossRef] [PubMed]
- Dirks, A.J.; Leeuwenburgh, C. Caloric restriction in humans: Potential pitfalls and health concerns. Mech. Ageing Dev. 2006, 127, 1–7. [Google Scholar] [CrossRef] [PubMed]
- Mann, T.; Tomiyama, A.J.; Westling, E.; Lew, A.M.; Samuels, B.; Chatman, J. Medicare’s search for effective obesity treatments: Diets are not the answer. Am. Psychol. 2007, 62, 220–233. [Google Scholar] [CrossRef] [PubMed]
- Gadde, K.M.; Martin, C.K.; Berthoud, H.R.; Heymsfield, S.B. Obesity: Pathophysiology and Management. J. Am. Coll. Cardiol. 2018, 71, 69–84. [Google Scholar] [CrossRef] [PubMed]
- Weight cycling. National Task Force on the Prevention and Treatment of Obesity. JAMA 1994, 272, 1196–1202. [Google Scholar]
- Cao, V.; Makarem, N.; Maguire, M.; Samayoa, I.; Xi, H.; Liang, C.; Aggarwal, B. History of Weight Cycling Is Prospectively Associated With Shorter and Poorer-Quality Sleep and Higher Sleep Apnea Risk in Diverse US Women. J. Cardiovasc. Nurs. 2021, 36, 573–581. [Google Scholar] [CrossRef]
- Byun, S.S.; Bello, N.A.; Liao, M.; Makarem, N.; Aggarwal, B. Associations of weight cycling with cardiovascular health using American Heart Association’s Life’s Simple 7 in a diverse sample of women. Prev. Med. Rep. 2019, 16, 100991. [Google Scholar] [CrossRef]
- Rajan, T.M.; Menon, V. Psychiatric disorders and obesity: A review of association studies. J. Postgrad. Med. 2017, 63, 182–190. [Google Scholar] [CrossRef]
- Franzen, P.; Buysse, D. Sleep Disorders Medicine: Basic Science, Technical Considerations and Clinical Aspects; Elsevier Health Sciences: Amsterdam, The Netherlands, 2009; Volume 3. [Google Scholar]
- Keel, P.K.; Baxter, M.G.; Heatherton, T.F.; Joiner, T.E. A 20-year longitudinal study of body weight, dieting, and eating disorder symptoms. J. Abnorm. Psychol. 2007, 116, 422–432. [Google Scholar] [CrossRef]
- Ackard, D.M.; Croll, J.K.; Kearney-Cooke, A. Dieting frequency among college females: Association with disordered eating, body image, and related psychological problems. J. Psychosom. Res. 2002, 52, 129–136. [Google Scholar] [CrossRef]
- Barker, E.T.; Bornstein, M.H. Global Self-Esteem, Appearance Satisfaction, and Self-Reported Dieting in Early Adolescence. J. Early Adolesc. 2010, 30, 205–224. [Google Scholar] [CrossRef] [PubMed]
- Lasikiewicz, N.; Myrissa, K.; Hoyland, A.; Lawton, C.L. Psychological benefits of weight loss following behavioural and/or dietary weight loss interventions. A systematic research review. Appetite 2014, 72, 123–137. [Google Scholar] [CrossRef] [PubMed]
- Thomson, C.A.; Morrow, K.L.; Flatt, S.W.; Wertheim, B.C.; Perfect, M.M.; Ravia, J.J.; Sherwood, N.E.; Karanja, N.; Rock, C.L. Relationship between sleep quality and quantity and weight loss in women participating in a weight-loss intervention trial. Obesity 2012, 20, 1419–1425. [Google Scholar] [CrossRef] [PubMed]
- Zuraikat, F.M.; Wood, R.A.; Barragán, R.; St-Onge, M.P. Sleep and Diet: Mounting Evidence of a Cyclical Relationship. Annu. Rev. Nutr. 2021, 41, 309–332. [Google Scholar] [CrossRef]
- McStay, M.; Gabel, K.; Cienfuegos, S.; Ezpeleta, M.; Lin, S.; Varady, K.A. Intermittent Fasting and Sleep: A Review of Human Trials. Nutrients 2021, 13, 3489. [Google Scholar] [CrossRef]
- Krystal, A.D.; Edinger, J.D. Measuring sleep quality. Sleep Med. 2008, 9 (Suppl. 1), S10–S17. [Google Scholar] [CrossRef]
- Nelson, K.L.; Davis, J.E.; Corbett, C.F. Sleep quality: An evolutionary concept analysis. Nurs. Forum 2022, 57, 144–151. [Google Scholar] [CrossRef]
- Crivello, A.; Barsocchi, P.; Girolami, M.; Palumbo, F. The meaning of sleep quality: A survey of available technologies. IEEE Access 2019, 7, 167374–167390. [Google Scholar] [CrossRef]
- Buysse, D.J.; Reynolds, C.F.; Monk, T.H.; Berman, S.R.; Kupfer, D.J. The Pittsburgh Sleep Quality Index: A new instrument for psychiatric practice and research. Psychiatry Res. 1989, 28, 193–213. [Google Scholar] [CrossRef]
- Johns, M.W. A new method for measuring daytime sleepiness: The Epworth sleepiness scale. Sleep 1991, 14, 540–545. [Google Scholar] [CrossRef]
- Hudson, J.L.; Zhou, J.; Campbell, W.W. Adults Who Are Overweight or Obese and Consuming an Energy-Restricted Healthy US-Style Eating Pattern at Either the Recommended or a Higher Protein Quantity Perceive a Shift from “Poor” to “Good” Sleep: A Randomized Controlled Trial. J. Nutr. 2020, 150, 3216–3223. [Google Scholar] [CrossRef] [PubMed]
- Tan, X.; Alén, M.; Wang, K.; Tenhunen, J.; Wiklund, P.; Partinen, M.; Cheng, S. Effect of Six-Month Diet Intervention on Sleep among Overweight and Obese Men with Chronic Insomnia Symptoms: A Randomized Controlled Trial. Nutrients 2016, 176, 751. [Google Scholar] [CrossRef] [PubMed]
- Martin, C.K.; Bhapkar, M.; Pittas, A.G.; Pieper, C.F.; Das, S.K.; Williamson, D.A.; Scott, T.; Redman, L.M.; Stein, R.; Gilhooly, C.H.; et al. Effect of Calorie Restriction on Mood, Quality of Life, Sleep, and Sexual Function in Healthy Nonobese Adults: The CALERIE 2 Randomized Clinical Trial. JAMA Intern. Med. 2016, 176, 743–752. [Google Scholar] [CrossRef] [PubMed]
- Filiatrault, M.L.; Chaput, J.P.; Drapeau, V.; Tremblay, A. Eating behavior traits and sleep as determinants of weight loss in overweight and obese adults. Nutr. Diabetes 2014, 4, e140. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Fitzgerald, K.C.; Vizthum, D.; Henry-Barron, B.; Schweitzer, A.; Cassard, S.D.; Kossoff, E.; Hartman, A.L.; Kapogiannis, D.; Sullivan, P.; Baer, D.J.; et al. Effect of intermittent vs. daily calorie restriction on changes in weight and patient-reported outcomes in people with multiple sclerosis. Mult. Scler. Relat. Disord. 2018, 23, 33–39. [Google Scholar] [CrossRef] [PubMed]
- Tremblay, A.; Fogelholm, M.; Jalo, E.; Westerterp-Plantenga, M.S.; Adam, T.C.; Huttunen-Lenz, M.; Stratton, G.; Lam, T.; Handjieva-Darlenska, T.; Handjiev, S.; et al. What Is the Profile of Overweight Individuals Who Are Unsuccessful Responders to a Low-Energy Diet? A PREVIEW Sub-study. Front. Nutr. 2021, 8, 707682. [Google Scholar] [CrossRef]
- Frank, S.; Gonzalez, K.; Lee-Ang, L.; Young, M.C.; Tamez, M.; Mattei, J. Diet and Sleep Physiology: Public Health and Clinical Implications. Front. Neurol. 2017, 8, 393. [Google Scholar] [CrossRef]
- St-Onge, M.P.; Roberts, A.; Shechter, A.; Choudhury, A.R. Fiber and Saturated Fat Are Associated with Sleep Arousals and Slow Wave Sleep. J. Clin. Sleep Med. 2016, 12, 19–24. [Google Scholar] [CrossRef]
- Perron, I.J.; Pack, A.I.; Veasey, S. Diet/Energy Balance Affect Sleep and Wakefulness Independent of Body Weight. Sleep 2015, 38, 1893–1903. [Google Scholar] [CrossRef]
- Grandner, M.A.; Jackson, N.; Gerstner, J.R.; Knutson, K.L. Sleep symptoms associated with intake of specific dietary nutrients. J. Sleep Res. 2014, 23, 22–34. [Google Scholar] [CrossRef]
- Kredlow, M.A.; Capozzoli, M.C.; Hearon, B.A.; Calkins, A.W.; Otto, M.W. The effects of physical activity on sleep: A meta-analytic review. J. Behav. Med. 2015, 38, 427–449. [Google Scholar] [CrossRef] [PubMed]
- Quan, S.F.; O’Connor, G.T.; Quan, J.S.; Redline, S.; Resnick, H.E.; Shahar, E.; Siscovick, D.; Sherrill, D.L. Association of physical activity with sleep-disordered breathing. Sleep Breath 2007, 11, 149–157. [Google Scholar] [CrossRef] [PubMed]
- Kebbe, M.; Sparks, J.R.; Flanagan, E.W.; Redman, L.M. Beyond weight loss: Current perspectives on the impact of calorie restriction on healthspan and lifespan. Expert Rev. Endocrinol. Metab. 2021, 16, 95–108. [Google Scholar] [CrossRef] [PubMed]
- Dorling, J.L.; van Vliet, S.; Huffman, K.M.; Kraus, W.E.; Bhapkar, M.; Pieper, C.F.; Stewart, T.; Das, S.K.; Racette, S.B.; Roberts, S.B.; et al. Effects of caloric restriction on human physiological, psychological, and behavioral outcomes: Highlights from CALERIE phase 2. Nutr. Rev. 2021, 79, 98–113. [Google Scholar] [CrossRef] [PubMed]
- Hargens, T.A.; Kaleth, A.S.; Edwards, E.S.; Butner, K.L. Association between sleep disorders, obesity, and exercise: A review. Nat. Sci. Sleep 2013, 5, 27–35. [Google Scholar] [CrossRef] [PubMed]
- Vgontzas, A.N.; Lin, H.M.; Papaliaga, M.; Calhoun, S.; Vela-Bueno, A.; Chrousos, G.P.; Bixler, E.O. Short sleep duration and obesity: The role of emotional stress and sleep disturbances. Int. J. Obes. 2008, 32, 801–809. [Google Scholar] [CrossRef]
- Anandam, A.; Akinnusi, M.; Kufel, T.; Porhomayon, J.; El-Solh, A.A. Effects of dietary weight loss on obstructive sleep apnea: A meta-analysis. Sleep Breath 2013, 17, 227–234. [Google Scholar] [CrossRef]
- Tuomilehto, H.; Seppä, J.; Uusitupa, M. Obesity and obstructive sleep apnea--clinical significance of weight loss. Sleep Med. Rev. 2013, 17, 321–329. [Google Scholar] [CrossRef]
- Chan, W.S.; Levsen, M.P.; McCrae, C.S. A meta-analysis of associations between obesity and insomnia diagnosis and symptoms. Sleep Med. Rev. 2018, 40, 170–182. [Google Scholar] [CrossRef]
- Taheri, S.; Lin, L.; Austin, D.; Young, T.; Mignot, E. Short sleep duration is associated with reduced leptin, elevated ghrelin, and increased body mass index. PLoS Med. 2004, 1, e62. [Google Scholar] [CrossRef]
- Pagliai, G.; Dinu, M.; Casini, A.; Sofi, F. Relationship between sleep pattern and efficacy of calorie-restricted Mediterranean diet in overweight/obese subjects. Int. J. Food Sci. Nutr. 2018, 69, 93–99. [Google Scholar] [CrossRef] [PubMed]
- Moreno-Frías, C.; Figueroa-Vega, N.; Malacara, J.M. Sleep Extension Increases the Effect of Caloric Restriction Over Body Weight and Improves the Chronic Low-Grade Inflammation in Adolescents With Obesity. J. Adolesc. Health 2020, 66, 575–581. [Google Scholar] [CrossRef] [PubMed]
- Chaput, J.P.; Tremblay, A. Sleeping habits predict the magnitude of fat loss in adults exposed to moderate caloric restriction. Obes. Facts 2012, 5, 561–566. [Google Scholar] [CrossRef] [PubMed]
- Williamson, D.A.; Martin, C.K.; Anton, S.D.; York-Crowe, E.; Han, H.; Redman, L.; Ravussin, E.; Team, P.C. Is caloric restriction associated with development of eating-disorder symptoms? Results from the CALERIE trial. Health Psychol. 2008, 27, S32–S42. [Google Scholar] [CrossRef] [PubMed]
- Ford, E.S.; Cunningham, T.J.; Giles, W.H.; Croft, J.B. Trends in insomnia and excessive daytime sleepiness among U.S. adults from 2002 to 2012. Sleep Med. 2015, 16, 372–378. [Google Scholar] [CrossRef] [PubMed]
- Sabanayagam, C.; Shankar, A. Sleep duration and cardiovascular disease: Results from the National Health Interview Survey. Sleep 2010, 33, 1037–1042. [Google Scholar] [CrossRef]
| Reference | Study Design | Sample Size and Baseline Characteristics | Intervention/ Control | Diet Duration | Dietary Intake Intervention | Sleep Outcome Measurement Method | Sleep Outcome Results | Limitations |
|---|---|---|---|---|---|---|---|---|
| Filiatrault et al. [36] | Cross over, pooled data from 4 weight-reducing interventions | n = 150, adults (men, women), BMI (average ± SD): 33.3 ± 3.5 kg/m2, age (mean ± SD): 38.8 ± 8.6 yr | Intervention: personalized diet plan targeting CR ** in most cases, some participants were on a control diet based on Canada’s food guide to promote a negative energy balance | 12–16 weeks | Average 500–700 kcal/day reduction in diet period | PSQI * (measured at baseline and end of intervention) | Sleep quality was significantly improved in response to weight-loss program (p < 0.01) | Small sample size, personalized weight loss plans with variable amounts of CR ** |
| Fitzgerald et al. [37] | RCT † | n = 36, adults with MS, BMI > 23 | Participants randomized to 1 of 3 diets: (1) daily CR **, (2) intermittent CR **, or (3) weight-stable diet | 8 weeks | (1) 78% of calorie needs 7 days/week (2) 25% of calorie needs 2 consecutive days/week, 100% of dietary needs 5 days/week (3) 100% of caloric needs 7 days/week | PSQI *, (measured at baseline and 8 weeks), FAMS * (measured at baseline, 4 weeks, and 8 weeks) | CR ** was not significantly associated with changes in fatigue or sleep quality (p > 0.05) | Short duration, reduced generalizability, reliance on self-reports of dietary adherence |
| Hudson et al. [33] | Randomized, parallel study design | n = 51, adults (mean ± SEM age: 47 ± 1 y, BMI: 32.6 ± 0.5 kg/m2) | Controlled USDA Healthy US-Style Eating Pattern and randomly assigned either 5 or 12.5 oz-equivalent (eq)/d of protein foods | 12 weeks | 750 kcal/day CR ** | PSQI *, ESS *, GSS * (measured at baseline, week 6, and week 12) | No change in time spent in bed, time spent sleeping, sleep onset latency, and time awake after sleep onset. Significant improvement in sleep efficiency (1 ± 1%, p < 0.027), subjective measures of GSS (−3.8 ± 0.4 au, p < 0.001) and daytime sleepiness score (−3.8 ± 0.4 au, p < 0.001) | CR ** is not the only dietary intervention, no causal claim made, more females than males, higher attrition rate in high protein group, dietary adherence unknown |
| Martin et al. [35] | Multisite RCT † | n = 220, Adults (men, women), BMI: 22–28 kg/m2 | Intervention: CR ** Control: AL ‡ | 2 years | 25% CR ** | PSQI * (measured at baseline, 12 months, and 24 months) | Intervention: Subjective sleep quality: mean (SE) = 0.11 (0.05), p = 0.07 Sleep duration: mean (SE) = 0.06 (0.07), p = 0.75 PSQI total score: mean (SE) = 0.24 (0.20), p = 0.47 Control: Subjective sleep quality: mean (SE) = 0.12 (0.07), p = 0.14 Sleep duration change: mean (SE) = 1.19 (0.09), p = 0.08 PSQI total score: mean (SE) = 0.60 (0.26), p = 0.04 | Composed of mostly white and female, healthy sample. Possible influence on health-related quality of life on sleep due to more study visits in intervention group. |
| Tan et al. [34] | RCT † | n = 49, adult males with overweight and obesity and chronic complaints of insomnia, average age ± SD (51.8 ± 8.4 yr), average BMI ± SD (30.9 ± 4.8) | Intervention: 300–500 kcal/day less energy intake. Control: AL ‡ | 6 months | 300–500 kcal/day CR | BNSQ *, ESS * (measured at baseline and 6 months) | Between group: Diet group has a shorter objective sleep onset latency (p < 0.001). Within diet group: prolonged total time asleep (p = 0.004), shorter sleep onset latency (p < 0.001), increased sleep efficiency (p = 0.004), fewer subjective nocturnal awakenings (p = 0.035), and decreased number of nocturia (p = 0.029) | Sleep onset latency was the only time-by-treatment sleep parameter difference, dietary intervention was not strictly adhered to, limited dietary records, included patients with mild sleep apnea |
| Tremblay et al. [38] | Multisite clinical trial | n = 2020 (138 unsuccessful responder women, 1214 successful responder women, 53 unsuccessful responder men, 615 successful responder men); age 25–70 years; BMI > 25 kg/m2; pre-diabetic | Low energy diet | 8 weeks | 800 kcal/day with macronutrient composition of 15–20, 35–40, 45–50% energy as fat, protein, and carbohydrate, respectively | PSQI * (measured at baseline and 8 weeks) | Between group differences: significant for sleep duration (p = 0.0385), sleep quality (p = 0.0508) | More women participants than men, no racial data provided, multi-site study may cause between-site differences |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Cao, V.; Clark, A.; Aggarwal, B. Dieting Behavior Characterized by Caloric Restriction and Relation to Sleep: A Brief Contemporary Review. Int. J. Environ. Res. Public Health 2023, 20, 276. https://doi.org/10.3390/ijerph20010276
Cao V, Clark A, Aggarwal B. Dieting Behavior Characterized by Caloric Restriction and Relation to Sleep: A Brief Contemporary Review. International Journal of Environmental Research and Public Health. 2023; 20(1):276. https://doi.org/10.3390/ijerph20010276
Chicago/Turabian StyleCao, Vivian, Alisha Clark, and Brooke Aggarwal. 2023. "Dieting Behavior Characterized by Caloric Restriction and Relation to Sleep: A Brief Contemporary Review" International Journal of Environmental Research and Public Health 20, no. 1: 276. https://doi.org/10.3390/ijerph20010276
APA StyleCao, V., Clark, A., & Aggarwal, B. (2023). Dieting Behavior Characterized by Caloric Restriction and Relation to Sleep: A Brief Contemporary Review. International Journal of Environmental Research and Public Health, 20(1), 276. https://doi.org/10.3390/ijerph20010276






