Evaluation of the Risk of Birth Defects Related to the Use of Assisted Reproductive Technology: An Updated Systematic Review
Abstract
1. Introduction
1.1. Fertility and Infertility Problem
1.2. Characteristics of Assisted Reproduction Techniques
1.3. Prenatal Diagnostic
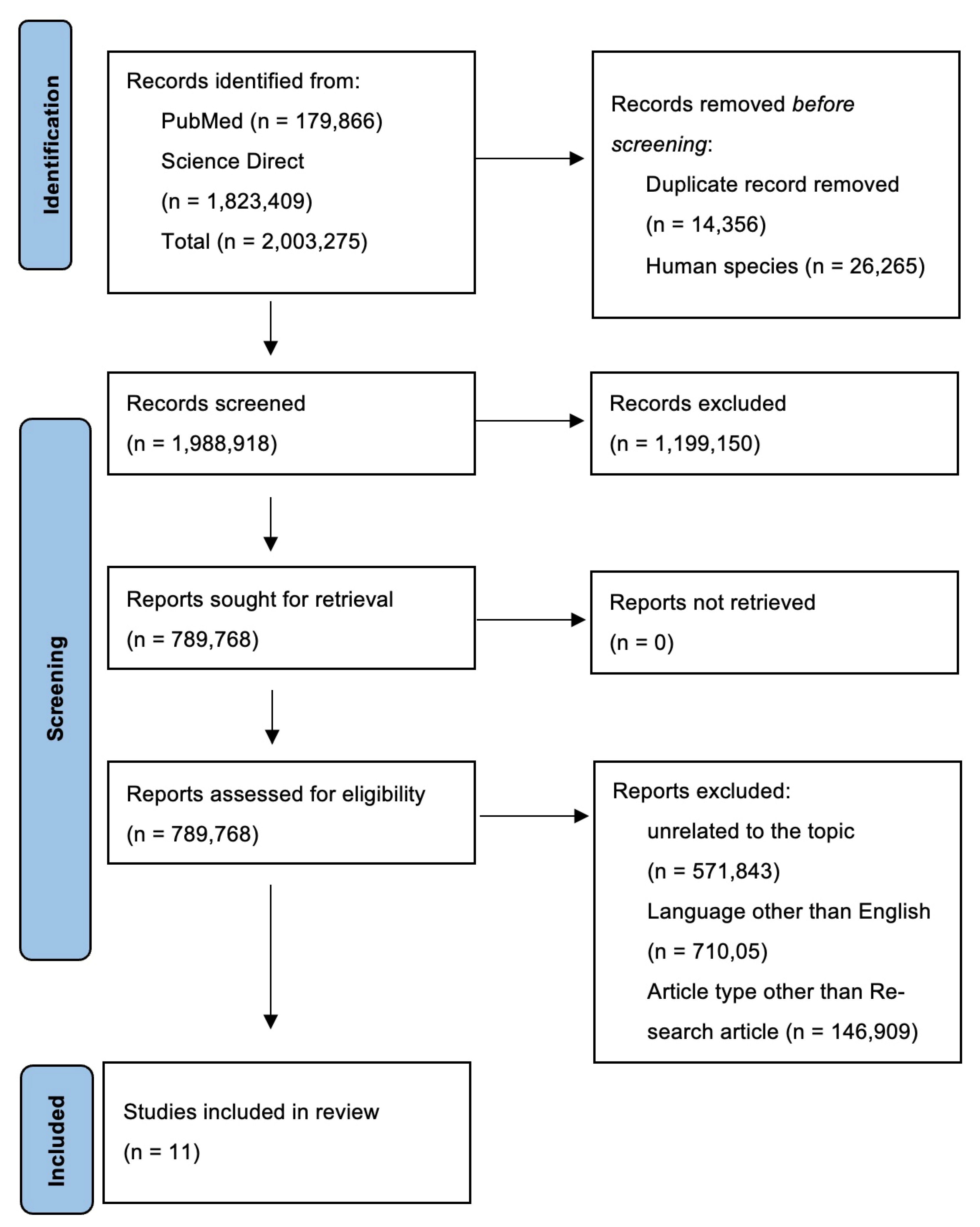
2. Methods
3. Results
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Colleran, H. The Cultural Evolution of Fertility Decline. Philos. Trans. R. Soc. B Biol. Sci. 2016, 371, 20150152. [Google Scholar] [CrossRef] [PubMed]
- Vichinsartvichai, P.; Siriphadung, S.; Traipak, K.; Promrungrueng, P.; Manolertthewan, C.; Ratchanon, S. The Influence of Women Age and Successfulness of Intrauterine Insemination (IUI) Cycles. J. Med. Assoc. Thail. Chotmaihet Thangphaet 2015, 98, 833–838. [Google Scholar]
- Janicka, A.; Spaczyński, R.Z.; Kurzawa, R.; SPiN, P.T.G.; Fertility Clinics; Polish Gynaecological Society. Assisted Reproductive Medicine in Poland—Fertility and Sterility Special Interest Group of the Polish Gynaecological Society (SPiN PTG) 2012 Report. Ginekol. Pol. 2015, 86, 932–939. [Google Scholar] [CrossRef] [PubMed]
- Łepecka-Klusek, C.; Pilewska-Kozak, A.B.; Jakiel, G. Niepłodność w świetle definicji choroby podanej przez WHO. Med. Ogólna Nauk. Zdrowiu 2012, 18, 4. [Google Scholar]
- Koperwas, M.; Głowacka, M. Problem Niepłodności Wśród Kobiet i Mężczyzn-Epidemiologia, Czynniki Ryzyka i Świadomość Społeczna. Asp. Zdrowia Chor. 2017, 2, 31–49. [Google Scholar]
- Łukaszuk, K.; Kozioł, K.; Jakiel, G.; Jakimiuk, A.; Jędrzejczak, P.; Kuczyński, W.; Kurzawa, R.; Pawelczyk, L.; Radwan, M.; Spaczyński, R.; et al. Diagnostyka i leczenie niepłodności—Rekomendacje Polskiego Towarzystwa Medycyny Rozrodu i Embriologii (PTMRiE) oraz Polskiego Towarzystwa Ginekologów i Położników (PTGP). Ginekol. Perinatol. Prakt. 2018, 3, 112–140. [Google Scholar]
- Borowski, D.; Pietryga, M.; Basta, P.; Cnota, W.; Czuba, B.; Dubiel, M.; Fuchs, T.; Huras, H.; Iciek, R.; Jaczyńska, R.; et al. Rekomendacje Sekcji Ultrasonografii Polskiego Towarzystwa Ginekologów i Położników w zakresie przesiewowej diagnostyki ultrasonograficznej w ciąży o przebiegu prawidłowym—2020 rok. Ginekol. Perinatol. Prakt. 2020, 5, 63–75. [Google Scholar]
- Plewka, K.; Dorofeeva, U. przychodni leczenia niepłodności. EJMT 2015, 1, 6. [Google Scholar]
- Polis, C.B.; Cox, C.M.; Tunçalp, Ö.; McLain, A.C.; Thoma, M.E. Estimating Infertility Prevalence in Low-to-Middle-Income Countries: An Application of a Current Duration Approach to Demographic and Health Survey Data. Hum. Reprod. Oxf. Engl. 2017, 32, 1064–1074. [Google Scholar] [CrossRef]
- Santa-Cruz, D.C.; Agudo, D. Impact of Underlying Stress in Infertility. Curr. Opin. Obstet. Gynecol. 2020, 32, 233–236. [Google Scholar] [CrossRef]
- Hanna, E.; Gough, B. The Social Construction of Male Infertility: A Qualitative Questionnaire Study of Men with a Male Factor Infertility Diagnosis. Sociol. Health Illn. 2020, 42, 465–480. [Google Scholar] [CrossRef] [PubMed]
- Ebrahimzadeh Zagami, S.; Latifnejad Roudsari, R.; Janghorban, R.; Mousavi Bazaz, S.M.; Amirian, M.; Allan, H.T. Infertile Couples’ Needs after Unsuccessful Fertility Treatment: A Qualitative Study. J. Caring Sci. 2019, 8, 95–104. [Google Scholar] [CrossRef] [PubMed]
- Ilioi, E.C.; Golombok, S. Psychological Adjustment in Adolescents Conceived by Assisted Reproduction Techniques: A Systematic Review. Hum. Reprod. Update 2015, 21, 84–96. [Google Scholar] [CrossRef] [PubMed]
- Sinha, P.; Pandey, K.; Srivastava, A. Factors Determining Successful Intrauterine Insemination. Int. J. Reprod. Contracept. Obstet. Gynecol. 2017, 6, 3887. [Google Scholar] [CrossRef]
- Sicchieri, F.; Silva, A.B.; de Sá Rosa e Silva, A.C.J.; de Albuquerque Sales Navarro, P.A.; Ferriani, R.A.; Reis, R.M.D. Prognostic Factors in Intrauterine Insemination Cycles. JBRA Assist. Reprod. 2018, 22, 2–7. [Google Scholar] [CrossRef] [PubMed]
- Honda, T.; Tsutsumi, M.; Komoda, F.; Tatsumi, K. Acceptable Pregnancy Rate of Unstimulated Intrauterine Insemination: A Retrospective Analysis of 17,830 Cycles. Reprod. Med. Biol. 2015, 14, 27–32. [Google Scholar] [CrossRef] [PubMed]
- Liu, J.; Li, T.-C.; Wang, J.; Wang, W.; Hou, Z.; Liu, J. The Impact of Ovarian Stimulation on the Outcome of Intrauterine Insemination Treatment: An Analysis of 8893 Cycles. BJOG Int. J. Obstet. Gynaecol. 2016, 123 (Suppl. 3), 70–75. [Google Scholar] [CrossRef]
- Katz, D.J.; Teloken, P.; Shoshany, O. Male Infertility—The Other Side of the Equation. Aust. Fam. Physician 2017, 46, 641–646. [Google Scholar]
- Dhillon, R.K.; McLernon, D.J.; Smith, P.P.; Fishel, S.; Dowell, K.; Deeks, J.J.; Bhattacharya, S.; Coomarasamy, A. Predicting the Chance of Live Birth for Women Undergoing IVF: A Novel Pretreatment Counselling Tool. Hum. Reprod. Oxf. Engl. 2016, 31, 84–92. [Google Scholar] [CrossRef]
- Teixeira, D.M.; Hadyme Miyague, A.; Barbosa, M.A.; Navarro, P.A.; Raine-Fenning, N.; Nastri, C.O.; Martins, W.P. Regular (ICSI) versus Ultra-High Magnification (IMSI) Sperm Selection for Assisted Reproduction. Cochrane Database Syst. Rev. 2020, 2, CD010167. [Google Scholar] [CrossRef]
- Geng, Y.; Xun, Y.; Hu, S.; Lai, Q.; Jin, L. GnRH Antagonist versus Follicular-Phase Single-Dose GnRH Agonist Protocol in Patients of Normal Ovarian Responses during Controlled Ovarian Stimulation. Gynecol. Endocrinol. Off. J. Int. Soc. Gynecol. Endocrinol. 2019, 35, 309–313. [Google Scholar] [CrossRef] [PubMed]
- Alper, M.M.; Fauser, B.C. Ovarian Stimulation Protocols for IVF: Is More Better than Less? Reprod. Biomed. Online 2017, 34, 345–353. [Google Scholar] [CrossRef] [PubMed]
- Cohlen, B.; Bijkerk, A.; Van der Poel, S.; Ombelet, W. IUI: Review and Systematic Assessment of the Evidence That Supports Global Recommendations. Hum. Reprod. Update 2018, 24, 300–319. [Google Scholar] [CrossRef] [PubMed]
- Gardner, D.K.; Weissman, A.; Howles, C.M.; Shoham, Z. Textbook of Assisted Reproductive Techniques|Volume 2: Clinical Pers; CRC Press: Boca Raton, FL, USA, 2018. [Google Scholar] [CrossRef]
- Elzeiny, H.; Garrett, C.; Toledo, M.; Stern, K.; McBain, J.; Baker, H.W.G. A Randomised Controlled Trial of Intra-Uterine Insemination versus in Vitro Fertilisation in Patients with Idiopathic or Mild Male Infertility. Aust. N. Z. J. Obstet. Gynaecol. 2014, 54, 156–161. [Google Scholar] [CrossRef]
- Farquhar, C.M.; Bhattacharya, S.; Repping, S.; Mastenbroek, S.; Kamath, M.S.; Marjoribanks, J.; Boivin, J. Female Subfertility. Nat. Rev. Dis. Primer 2019, 5, 7. [Google Scholar] [CrossRef]
- Wołoszyn, F.; Kwiatkowski, O. Ethical problems associated with prenatal diagnosis. Nurs. Public Health 2020, 10, 133–137. [Google Scholar] [CrossRef]
- Carlson, L.M.; Vora, N.L. Prenatal Diagnosis: Screening and Diagnostic Tools. Obstet. Gynecol. Clin. N. Am. 2017, 44, 245–256. [Google Scholar] [CrossRef]
- Farhud, D.; Pourkalhor, H. Prenatal Diagnostic Methods. Lab. Diagn. 2019, 11, 25–35. [Google Scholar]
- Abramowicz, J.S. Benefits and Risks of Ultrasound in Pregnancy. Semin. Perinatol. 2013, 37, 295–300. [Google Scholar] [CrossRef]
- Syngelaki, A.; Hammami, A.; Bower, S.; Zidere, V.; Akolekar, R.; Nicolaides, K.H. Diagnosis of Fetal Non-Chromosomal Abnormalities on Routine Ultrasound Examination at 11-13 Weeks’ Gestation. Ultrasound Obstet. Gynecol. Off. J. Int. Soc. Ultrasound Obstet. Gynecol. 2019, 54, 468–476. [Google Scholar] [CrossRef]
- Gil, M.M.; Galeva, S.; Jani, J.; Konstantinidou, L.; Akolekar, R.; Plana, M.N.; Nicolaides, K.H. Screening for Trisomies by CfDNA Testing of Maternal Blood in Twin Pregnancy: Update of The Fetal Medicine Foundation Results and Meta-Analysis. Ultrasound Obstet. Gynecol. Off. J. Int. Soc. Ultrasound Obstet. Gynecol. 2019, 53, 734–742. [Google Scholar] [CrossRef]
- Parham, L.; Michie, M.; Allyse, M. Expanding Use of CfDNA Screening in Pregnancy: Current and Emerging Ethical, Legal, and Social Issues. Curr. Genet. Med. Rep. 2017, 1, 44–53. [Google Scholar] [CrossRef]
- The PRISMA 2020 Statement: An Updated Guideline for Reporting Systematic Reviews|The BMJ. Available online: https://www.bmj.com/content/372/bmj.n71 (accessed on 3 April 2022).
- Davies, M.J.; Moore, V.M.; Willson, K.J.; Van Essen, P.; Priest, K.; Scott, H.; Haan, E.A.; Chan, A. Reproductive Technologies and the Risk of Birth Defects. N. Engl. J. Med. 2012, 366, 1803–1813. [Google Scholar] [CrossRef] [PubMed]
- Luke, B.; Gopal, D.; Cabral, H.; Stern, J.E.; Diop, H. Pregnancy, Birth, and Infant Outcomes by Maternal Fertility Status: The Massachusetts Outcomes Study of Assisted Reproductive Technology. Am. J. Obstet. Gynecol. 2017, 217, 327.e1–327.e14. [Google Scholar] [CrossRef] [PubMed]
- Boulet, S.L.; Kirby, R.S.; Reefhuis, J.; Zhang, Y.; Sunderam, S.; Cohen, B.; Bernson, D.; Copeland, G.; Bailey, M.A.; Jamieson, D.J.; et al. Assisted Reproductive Technology and Birth Defects Among Liveborn Infants in Florida, Massachusetts, and Michigan, 2000–2010. JAMA Pediatr. 2016, 170, e154934. [Google Scholar] [CrossRef]
- Iwashima, S.; Ishikawa, T.; Itoh, H. Reproductive Technologies and the Risk of Congenital Heart Defects. Hum. Fertil. 2017, 20, 14–21. [Google Scholar] [CrossRef]
- Tatsumi, T.; Jwa, S.C.; Kuwahara, A.; Irahara, M.; Kubota, T.; Saito, H. No Increased Risk of Major Congenital Anomalies or Adverse Pregnancy or Neonatal Outcomes Following Letrozole Use in Assisted Reproductive Technology. Hum. Reprod. Oxf. Engl. 2017, 32, 125–132. [Google Scholar] [CrossRef][Green Version]
- Liberman, R.F.; Getz, K.D.; Heinke, D.; Luke, B.; Stern, J.E.; Declercq, E.R.; Chen, X.; Lin, A.E.; Anderka, M. Assisted Reproductive Technology and Birth Defects: Effects of Subfertility and Multiple Births. Birth Defects Res. 2017, 109, 1144–1153. [Google Scholar] [CrossRef]
- Mussa, A.; Molinatto, C.; Cerrato, F.; Palumbo, O.; Carella, M.; Baldassarre, G.; Carli, D.; Peris, C.; Riccio, A.; Ferrero, G.B. Assisted Reproductive Techniques and Risk of Beckwith-Wiedemann Syndrome. Pediatrics 2017, 140, e20164311. [Google Scholar] [CrossRef]
- Sene, A.A.; Ghorbani, S.; Ashrafi, M. Comparison of the Pregnancy Outcomes and the Incidence of Fetal Congenital Abnormalities in Infertile Women Treated with Letrozole and Clomiphene Citrate. J. Obstet. Gynaecol. Res. 2018, 44, 1036–1041. [Google Scholar] [CrossRef]
- Wen, S.W.; Miao, Q.; Taljaard, M.; Lougheed, J.; Gaudet, L.; Davies, M.; Lanes, A.; Leader, A.; Corsi, D.J.; Sprague, A.E.; et al. Associations of Assisted Reproductive Technology and Twin Pregnancy With Risk of Congenital Heart Defects. JAMA Pediatr. 2020, 174, 446–454. [Google Scholar] [CrossRef]
- Luke, B.; Brown, M.B.; Wantman, E.; Forestieri, N.E.; Browne, M.L.; Fisher, S.C.; Yazdy, M.M.; Ethen, M.K.; Canfield, M.A.; Watkins, S.; et al. The Risk of Birth Defects with Conception by ART. Hum. Reprod. Oxf. Engl. 2021, 36, 116–129. [Google Scholar] [CrossRef] [PubMed]
- Serafin, D.; Grabarek, B.O.; Boroń, D.; Madej, A.; Czuba, B. Risk Assessment of the Increased Occurrence of Congenital Cardiac and Non-Cardiac Defects in Fetuses with a Normal Karyotype after Assisted Fertilization in Comparison to Natural Fertilization Based on Ultrasound Diagnostics. J. Clin. Med. 2021, 10, 5630. [Google Scholar] [CrossRef] [PubMed]
- Carneiro, M.M.; França Ferreira, M.C. Infertility Awareness: Why Should We Care? Women Health 2021, 61, 501–502. [Google Scholar] [CrossRef] [PubMed]
- Deshpande, P.S.; Gupta, A.S. Causes and Prevalence of Factors Causing Infertility in a Public Health Facility. J. Hum. Reprod. Sci. 2019, 12, 287–293. [Google Scholar] [CrossRef]
- Department of Internal diseases Nursing, Chair of Nursing and Midwifery, Ludwig Rydygier Collegium Medicum in Bydgoszcz, Poland; Dowbór-Dzwonka, A.; Cegła, B.; Filanowicz, M.; Szymkiewicz, E. Assisted Reproductive Techniques and NaProTechnology. Zdrow. Publiczne 2012, 122, 322–328. [Google Scholar] [CrossRef]
- Oliveira, B.L.; Ataman, L.M.; Rodrigues, J.K.; Birchal, T.S.; Reis, F.M. Restricted Access to Assisted Reproductive Technology and Fertility Preservation: Legal and Ethical Issues. Reprod. Biomed. Online 2021, 43, 571–576. [Google Scholar] [CrossRef]
- Kooli, C. Review of Assisted Reproduction Techniques, Laws, and Regulations in Muslim Countries. Middle East Fertil. Soc. J. 2020, 24, 8. [Google Scholar] [CrossRef]
- Chaudhary, B.L. Assisted Reproductive Techniques Ethical and Legal Issues. J. Indian Acad. Forensic Med. 2012, 34, 350–354. [Google Scholar]
- Jak to Się Wszystko Zaczęło, Czyli Krótko o Historii In Vitro. Available online: https://www.gyncentrum.pl/blog/pl/jak-to-sie-wszystko-zaczelo-czyli-krotko-o-historii-in-vitro (accessed on 5 April 2022).
| Intrauterine inseminations | In vitro fertilization |
| Semen liquefaction dysfunctions | Irreversible fallopian tube damage |
| Ejaculation dysfunctions (including retrograde ejaculation) | Lack of fallopian tubes |
| Problems with intercourse | Endometriosis of the III or IV stages with a severity level of moderate to serious |
| Cervical factor | Abnormal semen in the form of severe oligoasthenoteratozoospermia or azoospermia with normal spermatogenesis |
| Using donor semen due to male factor infertility | Ineffective pharmacological or surgical treatment in couples with moderate male factor, idiopathic infertility, fallopian tube factor, or ovulatory dysfunctions |
| Fertile couples diagnosed with recessive genetic changes for both partners, which are connected with the incidence of irreversible defects or disease in the offspring, or were diagnosed with a viral disease or encouraged to postpone fertility due to medical recommendations |
| Author, Year | Country, Period of Study | Type of Study | Sample Size | Main Conclusion |
|---|---|---|---|---|
| Davies et al., 2012 [35] | Australia (period unknown) | Original article | 308,974 births (6163 after using ART; 302,811 after spontaneous conception) | High risk of birth defects after using ART |
| Luke et al., 2016 [36] | USA, 2004–2010 | Cohort study | 459,623 women (441,420 fertile, 8054 subfertile, and 10,149 IVF) | High risk of birth defects after using ART |
| Boulet et al., 2016 [37] | USA, 2000–2010 | Original article | 4,618,076 women (64,861 after using ART; 4,553,215 without the use of ART) | Increased incidence of certain birth defects in ART neonates |
| Iwashima et al., 2017 [38] | Japan (period unknown) | Original article | 2716 pregnant women (2317 in a(SC) group and 399 (AC) group) | No link between ART and CHD |
| Tatsumi et al., 2017 [39] | Japan, 2011–2013 | Original article | 2951 women (2267 natural cycles; 684 letrozole-induced cycles resulting in pregnancy after fresh-embryo transfer) | No link between offspring after OI with letrozole and CHD |
| Liberman et al., 2017 [40] | USA, 2004–2010 | Cohort study | 472,340 live births (17,829 births after using ART; 9432 births to subfertile mothers; 445,080 births to fertile mothers) | Risk of birth defects after using ART is low |
| Mussa et al., 2017 [41] | Italy, 2005–2014 | Original study | 379,872 live births (7884 after using ATR; 371,988 without the use of ART) | ART entails a 10-fold increased risk of Beckwith–Wiedemann syndrome |
| Sene et al., 2018 [42] | Iran, 2007–2014 | Cohort study | 2009 women (1237 clomiphene citrate cycles; 772 letrozole cycles) | No link between offspring after OI and letrozole and CHD |
| Wen et al., 2020 [43] | Canada, 2012–2015 | Original study | 507,390 singleton or twin pregnancies (10,149 pregnancies assisted by ISI or IVF and 497,241 unassisted pregnancies) | No link between ART and CHD |
| Luke et al., 2021 [44] | USA, 2004–2013 | Original study | 1,236,016 children (135,051 after the use ART, 23,647 ART siblings, 9396 OI/IUI-conceived, and 1,067,922 naturally conceived) | ART is associated with increased risks of major non-chromosomal birth defects, cardiovascular defects, and any defect in singleton children and chromosomal defects in twins |
| Serafin et al., 2021 [45] | Poland, 2011–2016 | Original study | 1581 women (1298 pregnancies without the use of ART; 178 patients induced ovulation with clomiphene citrate; 137 women had intercourse naturally, 41 women AIH, 13 AID) | No link between ART and CHD and non-CHD |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Serafin, D.; Grabarek, B.O.; Boroń, D.; Madej, A.; Cnota, W.; Czuba, B. Evaluation of the Risk of Birth Defects Related to the Use of Assisted Reproductive Technology: An Updated Systematic Review. Int. J. Environ. Res. Public Health 2022, 19, 4914. https://doi.org/10.3390/ijerph19084914
Serafin D, Grabarek BO, Boroń D, Madej A, Cnota W, Czuba B. Evaluation of the Risk of Birth Defects Related to the Use of Assisted Reproductive Technology: An Updated Systematic Review. International Journal of Environmental Research and Public Health. 2022; 19(8):4914. https://doi.org/10.3390/ijerph19084914
Chicago/Turabian StyleSerafin, Dawid, Beniamin Oskar Grabarek, Dariusz Boroń, Andrzej Madej, Wojciech Cnota, and Bartosz Czuba. 2022. "Evaluation of the Risk of Birth Defects Related to the Use of Assisted Reproductive Technology: An Updated Systematic Review" International Journal of Environmental Research and Public Health 19, no. 8: 4914. https://doi.org/10.3390/ijerph19084914
APA StyleSerafin, D., Grabarek, B. O., Boroń, D., Madej, A., Cnota, W., & Czuba, B. (2022). Evaluation of the Risk of Birth Defects Related to the Use of Assisted Reproductive Technology: An Updated Systematic Review. International Journal of Environmental Research and Public Health, 19(8), 4914. https://doi.org/10.3390/ijerph19084914






