Associations among Caesarean Section Birth, Post-Traumatic Stress, and Postpartum Depression Symptoms
Abstract
:1. Introduction
2. Theoretical Background and Hypotheses
2.1. Postpartum Depression
2.2. C-Section Births
2.3. C-Section Births and PPD Symptoms
2.4. Birth Experiences and PTSD
2.5. Other Predictors of PPD
2.6. Objectives
3. Materials and Methods
3.1. Study Design and Sample
3.2. Measures
3.2.1. Predictor: C-Section Type
3.2.2. Outcome: PPD Symptoms
3.2.3. Mediator: PTSD Symptoms
3.2.4. Covariates
3.3. Data Analyses
4. Results
4.1. Descriptive Findings
4.2. Association between C-Section Type and PPD
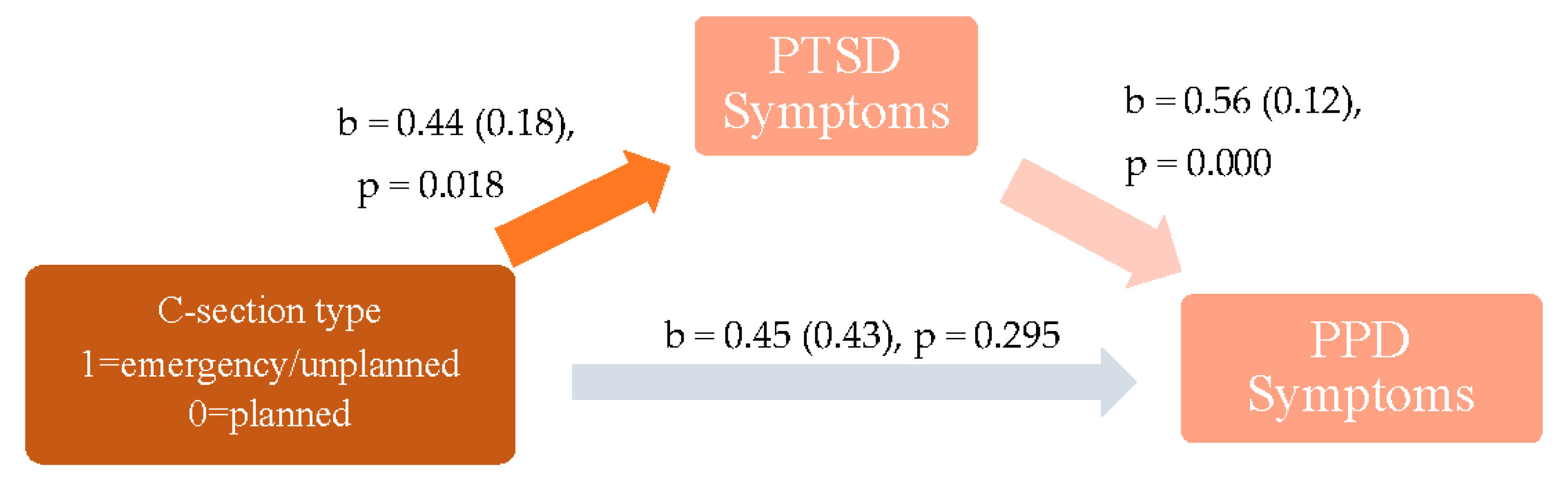
4.3. Mediation by Maternal Postnatal PTSD Symptoms
5. Discussion
6. Strengths and Limitations
7. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Lanes, A.; Kuk, J.L.; Tamim, H. Prevalence and characteristics of postpartum depression symptomatology among Canadian women: A cross-sectional study. BMC Public Health 2011, 11, 302. [Google Scholar] [CrossRef] [Green Version]
- Slomian, J.; Honvo, G.; Emonts, P.; Reginster, J.Y.; Bruyere, O. Consequences of maternal postpartum depression: A systematic review of maternal and infant outcomes. Women’s Health 2019, 15, 1745506519844044. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Bell, A.; Andersson, E. The birth experience and women’s postnatal depression: A systematic review. Midwifery 2016, 39, 112–123. [Google Scholar] [CrossRef] [PubMed]
- Xu, H.; Ding, Y.; Ma, Y.; Xin, X.; Zhang, D. Cesarean section and risk of postpartum depression: A meta-analysis. J. Psychosom. Res. 2017, 97, 118–126. [Google Scholar] [CrossRef] [PubMed]
- World Health Organization. WHO Recommendations Non-Clinic Interventions to Reduce Unnecessary Caesarean Sections. Available online: https://apps.who.int/iris/bitstream/handle/10665/275377/9789241550338-eng.pdf (accessed on 3 January 2022).
- Soderquist, J.; Wijma, B.; Wijma, K. The longitudinal course of post-traumatic stress after childbirth. J. Psychosom. Obstet. Gyaecol. 2006, 27, 113–117. [Google Scholar] [CrossRef]
- Dagher, R.K.; McGovern, P.M.; Dowd, B.E.; Gjerdingen, D.K. Postpartum depression and health services expenditures among employed women. J. Occup. Environ. Med. 2012, 54, 210–215. [Google Scholar] [CrossRef] [Green Version]
- Balbierz, A.; Bodnar-Deren, S.; Wang, J.J.; Howell, E.A. Maternal Depressive Symptoms and Parenting Practices 3-Months Postpartum. Matern. Child Health J. 2014, 19, 1212–1219. [Google Scholar] [CrossRef] [Green Version]
- American Psychiatric Association. What Is Postpartum Depression? 2020. Available online: https://www.psychiatry.org/patients-families/postpartum-depression/what-is-postpartum-depression (accessed on 10 September 2021).
- American Psychiatric Association. Diagnostic and Statistical Manual of Mental Disorders: DSM-5, 5th ed.; American Psychiatric Association: Arlington, VA, USA, 2013. [Google Scholar]
- Meltzer-Brody, S.; Maegbaek, M.L.; Medland, S.E.; Miller, W.C.; Sullivan, P.; Munk-Olsen, T. Obstetrical, pregnancy and socio-economic predictors for new-onset severe postpartum psychiatric disorders in primiparous women. Psychol. Med. 2017, 47, 1427–1441. [Google Scholar] [CrossRef] [Green Version]
- Silverman, M.E.; Reichenberg, A.; Savitz, D.A.; Cnattingius, S.; Lichtenstein, P.; Hultman, C.M.; Larsson, H.; Sandin, S. The risk factors for postpartum depression: A population-based study. Depress. Anxiety 2017, 34, 178–187. [Google Scholar] [CrossRef]
- Hahn-Holbrook, J.; Cornwell-Hinrichs, T.; Anaya, I. Economic and Health Predictors of National Postpartum Depression Prevalence: A Systematic Review, Meta-analysis, and Meta-Regression of 291 Studies from 56 Countries. Front. Psychiatry 2017, 8, 248. [Google Scholar] [CrossRef] [Green Version]
- Carter, F.; Frampton, C.; Mulder, R. Cesarean section and postpartum depression: A review of the evidence examining the link. Psychosom. Med. 2006, 68, 321–330. [Google Scholar] [CrossRef] [PubMed]
- Herguner, S.; Cicek, E.; Annagur, A.; Herguner, A.; Ors, R. Association of delivery type with postpartum depression, percieved social support and maternal attachment. J. Psychiatry Neurol. Sci. 2014, 27, 15–20. [Google Scholar] [CrossRef] [Green Version]
- Sword, W.; Landy, C.K.; Thabane, L.; Watt, S.; Krueger, P.; Farine, D.; Foster, G. Is mode of delivery associated with postpartum depression at 6 weeks: A prospective cohort study. BJOG 2011, 118, 966–977. [Google Scholar] [CrossRef] [PubMed]
- Cox, J.; Holden, J.; Sagovsky, R. Detection of postnatal depression. Development of the 10-item Edinburgh Postnatal Depression Scale. Br. J. Psychiatry 1987, 150, 782–786. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Lindahl, V.; Pearson, J.; Colpe, L. Prevalence of suicidality during pregnancy and the postpartum. Arch. Women’s Ment. Health 2005, 8, 77–87. [Google Scholar] [CrossRef] [PubMed]
- Murray, L.; Cooper, P.; Fearon, P. Parenting difficulties and postnatal depression: Implications for primary healthcare assessment and intervention. J. Community Pract. Health Visit. Assoc. 2014, 87, 34–38. [Google Scholar]
- Feild, T. Postpartum depression effects on early interactions, parenting, and safety practices: A review. Infant Behav. Dev. 2009, 33, 1–6. [Google Scholar] [CrossRef] [Green Version]
- Canadian Institue of Health Information. Childbirth Indicators by Place of Residence. Available online: https://apps.cihi.ca/mstrapp/asp/Main.aspx?Server=apmstrextprd_i&project=Quick%20Stats&uid=pce_pub_en&pwd=&evt=2048001&visualizationMode=0&documentID=029DB170438205AEBCC75B8673CCE822&_ga=2.237419200.1918635363.1547572373-2114234065.1530032017 (accessed on 26 November 2021).
- Martin, J.; Hamilton, B.; Osterman, M.; Driscoll, A. Births: Final data for 2018. Natl. Vital Stat. Rep. 2019, 68, 1–47. [Google Scholar]
- NHS Digital. NHS Maternity Statistics, England 2017–2018. Available online: https://digital.nhs.uk/data-and-information/publications/statistical/nhs-maternity-statistics/2017-18#key-facts (accessed on 26 November 2021).
- Curran, E.A.; Dalman, C.; Kearney, P.M.; Kenny, L.C.; Cryan, J.F.; Dinan, T.G.; Khashan, A.S. Association between obstetric mode of delivery and autism spectrum disorder: A population-based sibling design study. JAMA Psychiatry 2015, 72, 935–942. [Google Scholar] [CrossRef] [Green Version]
- Rutayisire, E.; Wu, X.; Huang, K.; Tao, S.; Chen, Y.; Tao, F. Childhood emotional and behavior problems and their associations with cesarean delivery. Rev. Bras. Psiquiatr. 2017, 40, 145–153. [Google Scholar] [CrossRef] [Green Version]
- Canadian Institue of Health Information. Inpatient Hospitalization, Surgery, Newborn, Alternate Level of Care and Childbirth Statistics, 2017–2018. Available online: https://www.cihi.ca/sites/default/files/document/dad-hmdb-childbirth-quick-stats-2017-2018-snapshot-en-web.pdf (accessed on 11 October 2021).
- Youn, H.; Lee, S.; Han, S.W.; Kim, L.Y.; Lee, T.S.; Oh, M.J.; Jeong, H.G.; Cho, G.J. Obstetric risk factors for depression during the postpartum period in South Korea: A nationwide study. J. Psychosom. Res. 2017, 102, 15–20. [Google Scholar] [CrossRef] [PubMed]
- Chang, S.-R.; Chen, K.-H.; Ho, H.-N.; Lai, Y.-H.; Lin, M.-I.; Lee, C.-N.; Lin, W.-A. Depressive symptoms, pain, and sexual dysfunction over the first year following vaginal or cesarean delivery: A prospective longitudinal study. Int. J. Nurs. Stud. 2015, 52, 1433–1444. [Google Scholar] [CrossRef] [PubMed]
- Clout, D.; Brown, R. Sociodemographic, pregnancy, obstetric, and postnatal predictors of postpartum stress, anxiety and depression in new mothers. J. Affect. Disord. 2015, 188, 60–67. [Google Scholar] [CrossRef] [PubMed]
- Rauh, C.; Beetz, A.; Burger, P.; Engel, A.; Haberle, L.; Fasching, P.A.; Kornhuber, J.; Beckmann, M.W.; Goecke, T.W.; Faschingbauer, F. Delivery mode and the course of pre- and postpartum depression. Arch. Gynecol. Obstet. 2012, 286, 1407–1412. [Google Scholar] [CrossRef]
- Rowlands, I.J.; Redshaw, M. Mode of birth and women’s psychological and physical wellbeing in the postnatal period. BMC Pregnancy Childbirth 2012, 12, 138. [Google Scholar] [CrossRef] [Green Version]
- Hanlon, A.; Beckmann, M. Mode of birth and early postnatal psychological morbidity. Aust. N. Z. J. Obstet. Gynaecol. 2015, 55, 578–583. [Google Scholar] [CrossRef]
- Waldenstrom, U.; Schytt, E. A longitudinal study of women’s memory of labour pain--from 2 months to 5 years after the birth. BJOG 2009, 116, 577–583. [Google Scholar] [CrossRef]
- Sandall, J.; Tribe, R.M.; Avery, L.; Mola, G.; Visser, G.H.; Homer, C.S.; Gibbons, D.; Kelly, N.M.; Kennedy, H.P.; Kidanto, H.; et al. Short-term and long-term effects of caesarean section on the health of women and children. Lancet 2018, 392, 1349–1357. [Google Scholar] [CrossRef]
- Ryding, E.L.; Wijma, K.; Wijma, B. Psychological impact of emergency cesarean section in comparison with elective cesarean section, instrumental and normal vaginal delivery. J. Psychosom. Obstet. Gynecol. 1998, 19, 135–144. [Google Scholar] [CrossRef]
- Verreault, N.; Da Costa, D.; Marchand, A.; Ireland, K.; Banack, H.; Dritsa, M.; Khalife, S. PTSD following childbirth: A prospective study of incidence and risk factors in Canadian women. J. Psychosom. Res. 2012, 73, 257–263. [Google Scholar] [CrossRef]
- Cook, N.; Ayers, S.; Horsch, A. Maternal posttraumatic stress disorder during the perinatal period and child outcomes: A systematic review. J. Affect. Disord. 2018, 225, 18–31. [Google Scholar] [CrossRef] [PubMed]
- Garthus-Niegel, S.; Ayers, S.; Martini, J.; von Soest, T.; Eberhard-Gran, M. The impact of postpartum post-traumatic stress disorder symptoms on child development: A population-based, 2-year follow-up study. Psychol. Med. 2017, 47, 161–170. [Google Scholar] [CrossRef] [PubMed]
- Tomsis, Y.; Perez, E.; Sharabi, L.; Shaked, M.; Haze, S.; Hadid, S. Postpartum Post-Traumatic Stress Symptoms Following Cesarean Section—The Mediating Effect of Sense of Control. Psychiatr. Q. 2021, 92, 1839–1853. [Google Scholar] [CrossRef] [PubMed]
- Kaplan, B.J.; Giesbrecht, G.F.; Leung, B.M.; Field, C.J.; Dewey, D.; Bell, R.C.; Manca, D.P.; O’Beirne, M.; Johnston, D.W.; Pop, V.J.; et al. The Alberta Pregnancy Outcomes and Nutrition (APrON) cohort study: Rationale and methods. Matern. Child Nutr. 2012, 10, 44–60. [Google Scholar] [CrossRef]
- Letourneau, N.; Aghajafari, F.; Bell, R.C.; Deane, A.J.; Dewey, D.; Field, C.; Giesbrecht, G.; Kaplan, B.; Leung, B.; Ntanda, H. The Alberta Pregnancy Outcomes and Nutrition (APrON) longitudinal study: Cohort profile and key findings from the first three years. BMJ Open 2022, 12, e047503. [Google Scholar] [CrossRef] [PubMed]
- Cox, J. Use and misuse of the Edinburgh Postnatal Depression Scale (EPDS): A ten point ‘survival analysis’. Arch. Women’s Ment. Health 2017, 20, 789–790. [Google Scholar] [CrossRef] [Green Version]
- Zimmerman, M.; Mattia, J. The Psychiatric Diagnostic Screening Questionnaire: Development, reliability and validity. Compr. Psychiatry 2001, 42, 175–189. [Google Scholar] [CrossRef]
- Leung, B.; Letourneau, N.; Bright, K.; Giesbrecht, G.; Ntanda, H.; Gagnon, L. Appraisal of the psychiatric diagnostic screening questionnaire in a perinatal cohort: The APrON study. Scand. J. Public Health 2017, 45, 658–665. [Google Scholar] [CrossRef]
- Gibson, J.; McKenzie-McHarg, K.; Shakespeare, J.; Price, J.; Gray, R. A systematic review of studies validating the Edinburgh Postnatal Depression Scale in antepartum and postpartum women. Acta Psychiatr. Scand. 2009, 119, 350–364. [Google Scholar] [CrossRef]
- Statistics Canada. National Population Health Survey: Household Component. Available online: https://www23.statcan.gc.ca/imdb-bmdi/pub/document/3225_D10_T9_V3-eng.pdf (accessed on 11 October 2021).
- Preacher, K.J.; Rucker, D.D.; Hayes, A.F. Addressing Moderated Mediation Hypotheses: Theory, Methods, and Prescriptions. Multivar. Behav. Res. 2007, 42, 185–227. [Google Scholar] [CrossRef]
- Faul, F.; Erdfelder, E.; Lang, A.G.; Buchner, A. G*Power 3: A flexible statistical power analysis program for the social, behavioral, and biomedical sciences. Behav. Res. Methods 2007, 39, 175–191. [Google Scholar] [CrossRef] [PubMed]
- Ayers, S.; Eagle, A.; Waring, H. The effects of childbirth-related post-traumatic stress disorder on women and their relationships: A qualitative study. Psychol. Health Med. 2006, 11, 389–398. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Dekel, S.; Ein-Dor, T.; Berman, Z.; Barsoumian, I.S.; Agarwal, S.; Pitman, R.K. Delivery mode is associated with maternal mental health following childbirth. Arch. Women’s Ment. Health 2019, 22, 817–824. [Google Scholar] [CrossRef] [PubMed]
- Modarres, M.; Afrasiabi, S.; Rahnama, P.; Montazeri, A. Prevalence and risk factors of childbirth-related post-traumatic stress symptoms. BMC Pregnancy Childbirth 2012, 12, 88. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Patterson, J.; Hollins Martin, C.; Karatzias, T. PTSD post-childbirth: A systematic review of women’s and midwives’ subjective experiences of care provider interaction. J. Reprod. Infant Psychol. 2018, 37, 56–83. [Google Scholar] [CrossRef]
- Beck, C.; Gable, R.; Sakala, C.; Declercq, E. Posttraumatic stress disorder in new mothers: Results from a two-stage U.S. national survey. Birth 2011, 38, 216–227. [Google Scholar] [CrossRef]
- Dikmen-Yildiz, P.; Ayers, S.; Phillips, L. Longitudinal trajectories of post-traumatic stress disorder (PTSD) after birth and associated risk factors. J. Affect. Disord. 2018, 229, 377–385. [Google Scholar] [CrossRef]
- Shahar, G.; Herishanu-Gilutz, S.; Holcberg, G.; Kofman, O. In first-time mothers, post-partum depressive symptom prospectively predict symptoms of post-traumatic stress. J. Affect. Disord. 2015, 186, 168–170. [Google Scholar] [CrossRef]
- Parfitt, Y.; Ayers, S. The effect of postnatal symptoms of post-traumatic stress and depression on the couple’s relationship and parent-baby bond. J. Reprod. Infant Psychol. 2009, 27, 127–142. [Google Scholar] [CrossRef] [Green Version]
- Grisbrook, M.A.; Letourneau, N. Improving maternal postpartum mental health screening guidelines requires assessment of post-traumatic stress disorder. Can. J. Public Health 2020, 112, 240–243. [Google Scholar] [CrossRef]
- Orovou, E.; Dagla, M.; Iatrakis, G.; Lykeridou, A.; Tzavara, C.; Antoniou, E. Correlation between Kind of Cesarean Section and Posttraumatic Stress Disorder in Greek Women. Int. J. Environ. Res. Public Health 2020, 17, 1592. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- White, T.; Matthey, S.; Boyd, K.; Barnett, B. Postnatal depression and post-traumatic stress after childbirth: Prevalence, course and co-occurrence. J. Reprod. Infant Psychol. 2006, 24, 107–120. [Google Scholar] [CrossRef]
- Patel, R.R.; Murphy, D.J.; Peters, T.J. Operative delivery and postnatal depression: A cohort study. BMJ 2005, 330, 879. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- O’Connor, E.; Rossom, R.C.; Henninger, M.; Groom, H.C.; Burda, B.U. Primary Care Screening for and Treatment of Depression in Pregnant and Postpartum Women: Evidence Report and Systematic Review for the US Preventive Services Task Force. JAMA 2016, 315, 388–406. [Google Scholar] [CrossRef] [Green Version]
- Rafferty, J.; Mattson, G.; Earls, M.F.; Yogman, M.W. Incorporating Recognition and Management of Perinatal Depression Into Pediatric Practice. Pediatrics 2019, 143, e20183260. [Google Scholar] [CrossRef]
- Beck, C. Birth Trauma: In the Eye of the Beholder. Nurs. Res. 2004, 53, 28–35. [Google Scholar] [CrossRef]
- Caughey, A.B.; Cahill, A.G.; Guise, J.M.; Rouse, D.J. Safe prevention of the primary cesarean delivery. Am. J. Obstet. Gynecol. 2014, 210, 179–193. [Google Scholar] [CrossRef]
- Haerskjold, A.; Hegaard, H.K.; Kjaergaard, H. Emergency caesarean section in low risk nulliparous women. J. Obstet. Gynaecol. 2012, 32, 543–547. [Google Scholar] [CrossRef]
- Spong, C.Y.; Berghella, V.; Wenstrom, K.D.; Mercer, B.M.; Saade, G.R. Preventing the first cesarean delivery: Summary of a joint Eunice Kennedy Shriver National Institute of Child Health and Human Development, Society for Maternal-Fetal Medicine, and American College of Obstetricians and Gynecologists Workshop. Obstet. Gynecol. 2012, 120, 1181–1193. [Google Scholar] [CrossRef]

| Variable | Frequency (n) | Percentage |
|---|---|---|
| Sociodemographic Maternal education | ||
| Below university degree | 89 | 25.80 |
| University degree or more | 256 | 74.20 |
| Marital status | ||
| Single | 7 | 1.98 |
| Married | 347 | 98.02 |
| Household Income | ||
| Less than 70 k | 47 | 13.54 |
| 70 k or more | 300 | 86.46 |
| Mean (SD) | Range | |
| Maternal age | 32.80 (4.36) | 23–44 |
| Medical Characteristics | ||
| Parity | ||
| 0 | 220 | 62.15 |
| 1 | 103 | 29.10 |
| 2 | 31 | 8.76 |
| C-section Type | ||
| Emergency/unplanned | 198 | 55.93 |
| Planned | 156 | 44.07 |
| Gestational age at birth | ||
| <37 weeks | 31 | 8.76 |
| 37 and more weeks | 323 | 91.24 |
| Child sex | ||
| Male | 192 | 54.24 |
| Female | 162 | 45.76 |
| Psychological Measurements PTSD score | ||
| 5 or more (cutoff) | 14 | 3.96 |
| EPDS score (postpartum) | 48 | 13.6 |
| 10 or more (cutoff) | Mean (SD) | Range |
| Prenatal depression symptoms | 7.03 (4.13) | 0–22 |
| PPD symptoms | 4.92 (4.12) | 0–30 |
| Prenatal social support | 14.80 (2.22) | 4–16 |
| PTSD symptoms | 0.64 (1.73) | 0–13 |
| Variables | 1 | 2 | 3 | 4 | 5 | 6 |
|---|---|---|---|---|---|---|
| Socio-economic status (1) | - | −0.07 * | −0.21 ** | 0.11 ** | −0.11 ** | −0.08 * |
| Parity (2) | - | 0.01 | −0.13 ** | −0.00 | −0.01 | |
| Prenatal depression symptoms (3) | - | −0.28 ** | 0.22 ** | 0.54 ** | ||
| Prenatal social support (4) | - | −0.16 ** | −0.20 ** | |||
| PTSD symptoms (5) | - | 0.27 ** | ||||
| PPD symptoms (6) | - |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Grisbrook, M.-A.; Dewey, D.; Cuthbert, C.; McDonald, S.; Ntanda, H.; Giesbrecht, G.F.; Letourneau, N. Associations among Caesarean Section Birth, Post-Traumatic Stress, and Postpartum Depression Symptoms. Int. J. Environ. Res. Public Health 2022, 19, 4900. https://doi.org/10.3390/ijerph19084900
Grisbrook M-A, Dewey D, Cuthbert C, McDonald S, Ntanda H, Giesbrecht GF, Letourneau N. Associations among Caesarean Section Birth, Post-Traumatic Stress, and Postpartum Depression Symptoms. International Journal of Environmental Research and Public Health. 2022; 19(8):4900. https://doi.org/10.3390/ijerph19084900
Chicago/Turabian StyleGrisbrook, Marie-Andrée, Deborah Dewey, Colleen Cuthbert, Sheila McDonald, Henry Ntanda, Gerald F. Giesbrecht, and Nicole Letourneau. 2022. "Associations among Caesarean Section Birth, Post-Traumatic Stress, and Postpartum Depression Symptoms" International Journal of Environmental Research and Public Health 19, no. 8: 4900. https://doi.org/10.3390/ijerph19084900
APA StyleGrisbrook, M.-A., Dewey, D., Cuthbert, C., McDonald, S., Ntanda, H., Giesbrecht, G. F., & Letourneau, N. (2022). Associations among Caesarean Section Birth, Post-Traumatic Stress, and Postpartum Depression Symptoms. International Journal of Environmental Research and Public Health, 19(8), 4900. https://doi.org/10.3390/ijerph19084900






