Mental Disorder Symptoms and the Relationship with Resilience among Paramedics in a Single Canadian Site
Abstract
1. Introduction
Objectives
2. Methods
2.1. Overview
2.2. Setting and Participants
2.3. Survey
2.3.1. Demographics
2.3.2. Resilience
2.3.3. Self-Report Symptom Measures
2.4. Analyses
3. Results
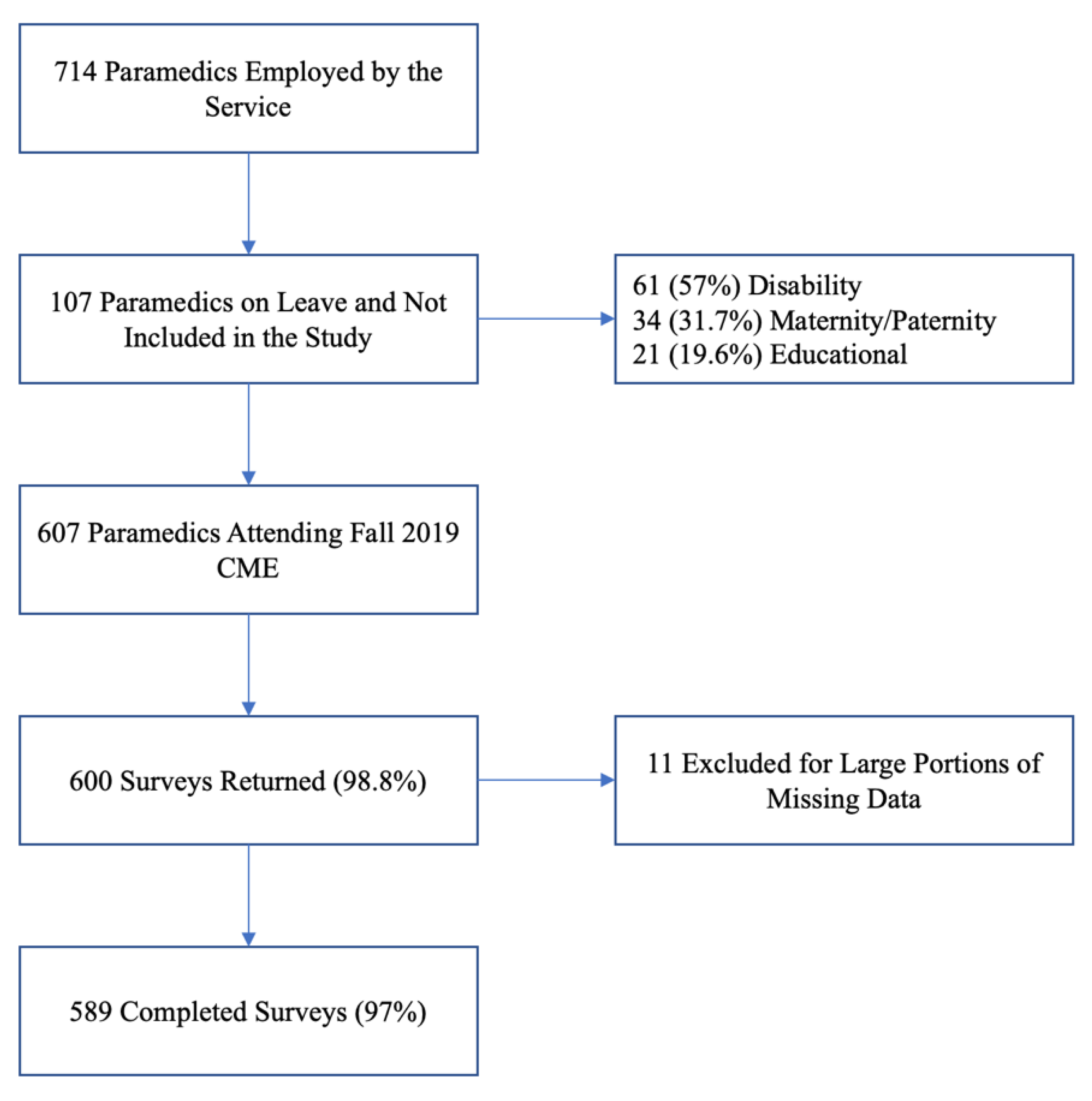
3.1. Participation and Response Rate
3.2. Participant Characteristics
3.3. Resilience
3.4. Mental Disorder Symptom Clusters
3.5. Unadjusted Models
3.6. Adjusted Models
4. Discussion
Limitations
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Berger, W.; Coutinho, E.S.; Figueira, I.; Marques-Portella, C.; Luz, M.P.; Neylan, T.C.; Marmar, C.R.; Mendlowicz, M.V. Rescuers at risk: A systematic review and meta-regression analysis of the worldwide current prevalence and correlates of PTSD in rescue workers. Soc. Psychiatry Psychiatr. Epidemiol. 2012, 47, 1001–1011. [Google Scholar] [CrossRef] [PubMed]
- Renkiewicz, G.K.; Hubble, M.W. Secondary Traumatic Stress in Emergency Services Systems (STRESS) Project: Quantifying and Predicting Compassion Fatigue in Emergency Medical Services Personnel. Prehospital Emerg. 2021, 1–12. [Google Scholar] [CrossRef] [PubMed]
- Bentley, M.A.; Crawford, J.M.; Wilkins, J.R.; Fernandez, A.R.; Studnek, J.R. An assessment of depression, anxiety, and stress among nationally certified EMS professionals. Prehospital Emerg. Care Off. J. Natl. Assoc. EMS Physicians Natl. Assoc. State EMS Dir. 2013, 17, 330–338. [Google Scholar] [CrossRef] [PubMed]
- Renkiewicz, G.K.; Hubble, M.W. Secondary traumatic stress in emergency services systems (STRESS) project: Quantifying personal trauma profiles for secondary stress syndromes in emergency medical services personnel with prior military service. J. Spec. Oper. Med. 2021, 21, 55–64. [Google Scholar]
- Brooks, D.; Brooks, R. A systematic review: What factors predict Post-Traumatic Stress Symptoms in ambulance personnel? Br. Paramed. J. 2021, 5, 18–24. [Google Scholar] [CrossRef]
- Reardon, M.; Abrahams, R.; Thyer, L.; Simpson, P. Review article: Prevalence of burnout in paramedics: A systematic review of prevalence studies. Emerg. Med. Australas. 2020, 32, 182–189. [Google Scholar] [CrossRef]
- Vigil, N.H.; Grant, A.R.; Perez, O.; Blust, R.N.; Chikani, V.; Vadeboncoeur, T.F.; Spaite, D.W.; Bobrow, B.J. Death by Suicide-The EMS Profession Compared to the General Public. Prehospital Emerg. Care Off. J. Natl. Assoc. EMS Physicians Natl. Assoc. State EMS Dir. 2019, 23, 340–345. [Google Scholar] [CrossRef]
- Luftman, K.; Aydelotte, J.; Rix, K.; Ali, S.; Houck, K.; Coopwood, T.B.; Teixeira, P.; Eastman, A.; Eastridge, B.; Brown, C.V.; et al. PTSD in those who care for the injured. Injury 2017, 48, 293–296. [Google Scholar] [CrossRef]
- Carleton, R.N.; Afifi, T.O.; Turner, S.; Taillieu, T.; Duranceau, S.; LeBouthillier, D.M.; Sareen, J.; Ricciardelli, R.; MacPhee, R.; Groll, D.; et al. Mental disorder symptoms among public safety personnel in Canada. Can. J. Psychiatry 2018, 63, 54–64. [Google Scholar] [CrossRef]
- Carleton, R.N.; Afifi, T.O.; Taillieu, T.; Turner, S.; Krakauer, R.; Anderson, G.S.; MacPhee, R.S.; Ricciardelli, R.; Cramm, H.A.; Groll, D.; et al. Exposures to potentially traumatic events among public safety personnel in Canada. Can. J. Behav. Sci./Rev. Can. Sci. Du Comport. 2019, 51, 37–52. [Google Scholar] [CrossRef]
- Sommer, J.L.; El-Gabalawy, R.; Taillieu, T.; Afifi, T.O.; Carleton, R.N. Associations between Trauma Exposure and Physical Conditions among Public Safety Personnel: Associations entre l’exposition a un traumatisme et les problemes physiques chez le personnel de la sante publique. Can. J. Psychiatry 2020, 65, 548–558. [Google Scholar] [CrossRef] [PubMed]
- Ricciardelli, R.; Czarnuch, S.; Afifi, T.O.; Taillieu, T.; Carleton, R.N. Public Safety Personnel’s interpretations of potentially traumatic events. Occup. Med. (Lond.) 2020, 70, 155–161. [Google Scholar] [CrossRef] [PubMed]
- Carleton, R.N.; Afifi, T.O.; Taillieu, T.; Turner, S.; Mason, J.E.; Ricciardelli, R.; McCreary, D.R.; Vaughan, A.D.; Anderson, G.S.; Krakauer, R.L.; et al. Assessing the Relative Impact of Diverse Stressors among Public Safety Personnel. Int. J. Environ. Res. Public Health 2020, 17, 1234. [Google Scholar] [CrossRef] [PubMed]
- Ricciardelli, R.; Carleton, R.N.; Groll, D.; Cramm, H. Qualitatively Unpacking Canadian Public Safety Personnel Experiences of Trauma and Their Well-Being. Can. J. Criminol. Crim. Justice 2018, 60, 566–577. [Google Scholar] [CrossRef]
- Regehr, C.; Hill, J.; Goldberg, G.; Hughes, J. Postmortem Inquiries and Trauma Responses in Paramedics and Firefighters. J. Interpers. Violence 2016, 18, 607–622. [Google Scholar] [CrossRef]
- Harenberg, S.; McCarron, M.C.; Carleton, R.N.; O’Malley, T.; Ross, T. Experiences of trauma, depression, anxiety, and stress in Western-Canadian HEMS personnnel. J. Community Saf. Well-Being 2018, 3, 18–21. [Google Scholar] [CrossRef]
- Carleton, R.N.; Afifi, T.O.; Turner, S.; Taillieu, T.; El-Gabalawy, R.; Sareen, J.; Asmundson, G.J.G. Chronic pain among public safety personnel in Canada. Can. J. Pain 2017, 1, 237–246. [Google Scholar] [CrossRef]
- Angehrn, A.; Teale Sapach, M.J.N.; Ricciardelli, R.; MacPhee, R.S.; Anderson, G.S.; Carleton, R.N. Sleep Quality and Mental Disorder Symptoms among Canadian Public Safety Personnel. Int. J. Environ. Res. Public Health 2020, 17, 2708. [Google Scholar] [CrossRef]
- Carleton, R.N.; Afifi, T.O.; Turner, S.; Taillieu, T.; LeBouthillier, D.M.; Duranceau, S.; Sareen, J.; Ricciardelli, R.; MacPhee, R.S.; Groll, D.; et al. Suicidal ideation, plans, and attempts among public safety personnel in Canada. Can. Psychol./Psychol. Can. 2018, 59, 220–231. [Google Scholar] [CrossRef]
- Turner, S.; Taillieu, T.; Carleton, R.N.; Sareen, J.; Afifi, T.O. Association between a history of child abuse and suicidal ideation, plans and attempts among Canadian public safety personnel: A cross-sectional survey. CMAJ Open 2018, 6, E463–E470. [Google Scholar] [CrossRef][Green Version]
- Regehr, C.; Goldberg, G.; Glancy, G.D.; Knott, T. Posttraumatic symptoms and disability in paramedics. Can. J. Psychiatry 2002, 47, 953–958. [Google Scholar] [CrossRef] [PubMed]
- Regehr, C. Bringing the Trauma Home: Spouses of Paramedics. J. Loss Trauma 2005, 10, 97–114. [Google Scholar] [CrossRef]
- Berger, W.; Figueira, I.; Maurat, A.M.; Bucassio, E.P.; Vieira, I.; Jardim, S.R.; Coutinho, E.S.; Mari, J.J.; Mendlowicz, M.V. Partial and full PTSD in Brazilian ambulance workers: Prevalence and impact on health and on quality of life. J. Trauma. Stress 2007, 20, 637–642. [Google Scholar] [CrossRef] [PubMed]
- Studnek, J.R.; Crawford, J.M.; Wilkins, J.R., 3rd; Pennell, M.L. Back problems among emergency medical services professionals: The LEADS health and wellness follow-up study. Am. J. Ind. Med. 2010, 53, 12–22. [Google Scholar] [CrossRef]
- Rahimi, A.; Vazini, H.; Alhani, F.; Anoosheh, M. Relationship between Low Back Pain with Quality of Life, Depression, Anxiety and Stress among Emergency Medical Technicians. Trauma Mon. 2015, 20, e18686. [Google Scholar] [CrossRef]
- Bracken-Scally, M.; McGilloway, S.; Gallagher, S.; Mitchell, J.T. Life after the emergency services: An exploratory study of well being and quality of life in emergency services retirees. J. Emerg. Ment. Health Hum. Resil. 2014, 16, 44–51. [Google Scholar]
- Sterud, T.; Hem, E.; Lau, B.; Ekeberg, Ø. Suicidal ideation and suicide attempts in a nationwide sample of operational Norwegian ambulance personnel. J. Occup. Health 2008, 50, 406–414. [Google Scholar] [CrossRef]
- Crowe, R.P.; Fernandez, A.R.; Pepe, P.E.; Cash, R.E.; Rivard, M.K.; Wronski, R.; Anderson, S.E.; Hogan, T.H.; Andridge, R.R.; Panchal, A.R.; et al. The association of job demands and resources with burnout among emergency medical services professionals. J. Am. Coll. Emerg. Physicians Open 2020, 1, 6–16. [Google Scholar] [CrossRef]
- Cash, R.E.; White-Mills, K.; Crowe, R.P.; Rivard, M.K.; Panchal, A.R. Workplace Incivility among Nationally Certified EMS Professionals and Associations with Workforce-Reducing Factors and Organizational Culture. Prehospital Emerg. Care Off. J. Natl. Assoc. EMS Physicians Natl. Assoc. State EMS Dir. 2019, 23, 346–355. [Google Scholar] [CrossRef]
- Fullerton, L.; Oglesbee, S.; Weiss, S.J.; Ernst, A.A.; Mesic, V. Assessing the Prevalence and Predictors of Bullying among Emergency Medical Service Providers. Prehospital Emerg. Care Off. J. Natl. Assoc. EMS Physicians Natl. Assoc. State EMS Dir. 2019, 23, 9–14. [Google Scholar] [CrossRef]
- Dopelt, K.; Wacht, O.; Strugo, R.; Miller, R.; Kushnir, T. Factors that affect Israeli paramedics’ decision to quit the profession: A mixed methods study. Isr. J. Health Policy Res. 2019, 8, 78. [Google Scholar] [CrossRef] [PubMed]
- Donnelly, E.; Bradford, P.; Davis, M.; Hedges, C.; Socha, D.; Morassutti, P.; Pichika, S.C. What influences safety in paramedicine? Understanding the impact of stress and fatigue on safety outcomes. J. Am. Coll. Emerg. Physicians 2020, 1, 460–473. [Google Scholar] [CrossRef] [PubMed]
- Koopmans, E.; Wagner, S.L.; Schmidt, G.; Harder, H. Emergency Response Services Suicide: A Crisis in Canada? J. Loss Trauma 2017, 22, 527–539. [Google Scholar] [CrossRef]
- Public Safety Canada. Supporting Canada’s Public Safety Personnel: An Action Plan on Post-Traumatic Stress Injuries; Public Safety Canada: Ottawa, ON, Canada, 2019.
- Joyce, S.; Shand, F.; Tighe, J.; Laurent, S.J.; Bryant, R.A.; Harvey, S.B. Road to resilience: A systematic review and meta-analysis of resilience training programmes and interventions. BMJ Open 2018, 8, e017858. [Google Scholar] [CrossRef]
- Clompus, S.R.; Albarran, J.W. Exploring the nature of resilience in paramedic practice: A psycho-social study. Int. Emerg. Nurs. 2016, 28, 1–7. [Google Scholar] [CrossRef]
- Grant, L.; Kinman, G. Emotional Resilience in the Helping Professions and how it can be Enhanced. Health Soc. Care Educ. 2014, 3, 23–34. [Google Scholar] [CrossRef]
- Jackson, D.; Firtko, A.; Edenborough, M. Personal resilience as a strategy for surviving and thriving in the face of workplace adversity: A literature review. J. Adv. Nurs. 2007, 60, 1–9. [Google Scholar] [CrossRef]
- Gayton, S.D.; Lovell, G.P. Resilience in ambulance service paramedics and its relationships with well-being and general health. Traumatology 2012, 18, 58–64. [Google Scholar] [CrossRef]
- Stelnicki, A.M.; Jamshidi, L.; Fletcher, A.J.; Carleton, R.N. Evaluation of before Operational Stress: A Program to Support Mental Health and Proactive Psychological Protection in Public Safety Personnel. Front. Psychol. 2021, 12, 511755. [Google Scholar] [CrossRef]
- Szeto, A.; Dobson, K.S.; Knaak, S. The Road to Mental Readiness for First Responders: A Meta-Analysis of Program Outcomes. Can. J. Psychiatry 2019, 64, 18S–29S. [Google Scholar] [CrossRef]
- Dobson, K.S.; Szeto, A.; Knaak, S. The Working Mind: A Meta-Analysis of a Workplace Mental Health and Stigma Reduction Program. Can. J. Psychiatry 2019, 64, 39S–47S. [Google Scholar] [CrossRef] [PubMed]
- van der Meulen, E.; van der Velden, P.G.; Setti, I.; van Veldhoven, M. Predictive value of psychological resilience for mental health disturbances: A three-wave prospective study among police officers. Psychiatry Res. 2018, 260, 486–494. [Google Scholar] [CrossRef] [PubMed]
- Joyce, S.; Shand, F.; Bryant, R.A.; Lal, T.J.; Harvey, S.B. Mindfulness-Based Resilience Training in the Workplace: Pilot Study of the Internet-Based Resilience@Work (RAW) Mindfulness Program. J. Med. Internet. Res. 2018, 20, e10326. [Google Scholar] [CrossRef] [PubMed]
- Carleton, R.N.; Korol, S.; Mason, J.E.; Hozempa, K.; Anderson, G.S.; Jones, N.A.; Dobson, K.S.; Szeto, A.; Bailey, S. A longitudinal assessment of the road to mental readiness training among municipal police. Cogn. Behav. Ther. 2018, 46, 508–528. [Google Scholar] [CrossRef]
- Canadian Institute for Publish Safety Research and Treatment (CIPSRT). Glossary of Terms: A Shared Understanding of the Common Terms Used to Describe Psychological Trauma (Version 2.1); CIPSRT: Regina, SK, Canada, 2019. [Google Scholar]
- Bigham, B.L.; Jensen, J.L.; Tavares, W.; Drennan, I.R.; Saleem, H.; Dainty, K.N.; Munro, G. Paramedic self-reported exposure to violence in the emergency medical services (EMS) workplace: A mixed-methods cross-sectional survey. Prehospital Emerg. Care Off. J. Natl. Assoc. EMS Physicians Natl. Assoc. State EMS Dir. 2014, 18, 489–494. [Google Scholar] [CrossRef]
- Thoits, P.A. Mechanisms linking social ties and support to physical and mental health. J. Health Soc. Behav. 2011, 52, 145–161. [Google Scholar] [CrossRef]
- Thoits, P.A. Stress and health: Major findings and policy implications. J. Health Soc. Behav. 2010, 51, S41–S53. [Google Scholar] [CrossRef]
- Donnelly, E.A.; Chonody, J.; Campbell, D. Measuring Chronic Stress in the Emergency Medical Services. J. Workplace Behav. Health 2014, 29, 333–353. [Google Scholar] [CrossRef]
- Donnelly, E. Work-related stress and posttraumatic stress in emergency medical services. Prehospital Emerg. Care Off. J. Natl. Assoc. EMS Physicians Natl. Assoc. State EMS Dir. 2012, 16, 76–85. [Google Scholar] [CrossRef]
- Rivard, M.K.; Cash, R.E.; Mercer, C.B.; Chrzan, K.; Panchal, A.R. Demography of the National Emergency Medical Services Workforce: A Description of Those Providing Patient Care in the Prehospital Setting. Prehospital Emerg. Care Off. J. Natl. Assoc. EMS Physicians Natl. Assoc. State EMS Dir. 2021, 25, 213–220. [Google Scholar] [CrossRef]
- Smith, B.W.; Dalen, J.; Wiggins, K.; Tooley, E.; Christopher, P.; Bernard, J. The brief resilience scale: Assessing the ability to bounce back. Int. J. Behav. Med. 2008, 15, 194–200. [Google Scholar] [CrossRef] [PubMed]
- Blevins, C.A.; Weathers, F.W.; Davis, M.; Witte, T.K.; Domino, J.L. The posttraumatic stress disorder checklist for DSM-5 (PCL-5): Development and initial psychometric evaluation. J. Trauma. Stress 2015, 28, 489–498. [Google Scholar] [CrossRef] [PubMed]
- Wortmann, J.H.; Jordan, A.H.; Weathers, F.W.; Resick, P.A.; Dondanville, K.A.; Hall-Clark, B.; Foa, E.B.; Young-McCaughan, S.; Yarvis, J.S.; Hembree, E.A.; et al. Psychometric analysis of the PTSD Checklist-5 (PCL-5) among treatment-seeking military service members. Psychol. Assess 2016, 28, 1392–1403. [Google Scholar] [CrossRef] [PubMed]
- United Starts Department of Veterans Affairs National Centre for PTSD. PTSD Checklist for DSM-5 (PCL-5). Available online: https://www.ptsd.va.gov/professional/assessment/adult-sr/ptsd-checklist.asp (accessed on 15 January 2022).
- Kroenke, K.; Spitzer, R.L.; Williams, J. The PHQ-9: Validity of a brief depression severity measure. J. Gen. Intern. Med. 2001, 16, 606–613. [Google Scholar] [CrossRef]
- Kroenke, K.; Spitzer, R.L.; Williams, J.B.; Lowe, B. The Patient Health Questionnaire Somatic, Anxiety, and Depressive Symptom Scales: A systematic review. Gen. Hosp. Psychiatry 2010, 32, 345–359. [Google Scholar] [CrossRef]
- Spitzer, R.L.; Kroenke, K.; Williams, J.B.; Löwe, B. A brief measure for assessing generalized anxiety disorder. Arch. Intern. Med. 2006, 1666, 1092–1097. [Google Scholar] [CrossRef]
- Mat Salleh, M.N.; Ismail, H.; Mohd Yusoff, H. Reliability and validity of a post-traumatic checklist-5 (PCL-5) among fire and rescue officers in Selangor, Malaysia. J. Health Res. 2020, 35, 379–387. [Google Scholar] [CrossRef]
- Beard, C.; Hsu, K.J.; Rifkin, L.S.; Busch, A.B.; Bjorgvinsson, T. Validation of the PHQ-9 in a psychiatric sample. J. Affect. Disord. 2016, 193, 267–273. [Google Scholar] [CrossRef]
- Beard, C.; Bjorgvinsson, T. Beyond generalized anxiety disorder: Psychometric properties of the GAD-7 in a heterogeneous psychiatric sample. J. Anxiety Disord. 2014, 28, 547–552. [Google Scholar] [CrossRef]
- Carleton, R.N.; Afifi, T.O.; Taillieu, T.; Turner, S.; El-Gabalawy, R.; Sareen, J.; Asmundson, G.J.G. Anxiety-related psychopathology and chronic pain comorbidity among public safety personnel. J. Anxiety Disord. 2018, 55, 48–55. [Google Scholar] [CrossRef]
- Ricciardelli, R.; Andres, E.; Kaur, N.; Czarnuch, S.; Carleton, R.N. Fit for public safety: Informing attitudes and practices tied to the hiring of public safety personnel. J. Workplace Behav. Health 2019, 35, 14–36. [Google Scholar] [CrossRef]
- Ricciardelli, R.; Carleton, R.N.; Mooney, T.; Cramm, H. “Playing the system”: Structural factors potentiating mental health stigma, challenging awareness, and creating barriers to care for Canadian public safety personnel. Health 2020, 24, 259–278. [Google Scholar] [CrossRef] [PubMed]
- Carleton, R.N.; Afifi, T.O.; Turner, S.; Taillieu, T.; Vaughan, A.D.; Anderson, G.S.; Ricciardelli, R.; MacPhee, R.S.; Cramm, H.A.; Czarnuch, S.; et al. Mental health training, attitudes toward support, and screening positive for mental disorders. Cogn. Behav. Ther. 2019, 49, 55–73. [Google Scholar] [CrossRef] [PubMed]
- Donnelly, E.A.; Bradford, P.; Davis, M.; Hedges, C.; Klingel, M. Predictors of posttraumatic stress and preferred sources of social support among Canadian paramedics. CJEM 2016, 18, 205–212. [Google Scholar] [CrossRef]
- Mental Health Commission of Canada. Overview of Mental Health Data in Canada: Background, Needs, and Gaps; Mental Health Commission of Canada: Toronto, ON, Canada, 2014. [Google Scholar]
- Affleck, W.; Carmichael, V.; Whitley, R. Men’s Mental Health: Social Determinants and Implications for Services. Can. J. Psychiatry 2018, 63, 581–589. [Google Scholar] [CrossRef]
- Whitley, R. Men’s Mental Health: Beyond Victim-Blaming. Can. J. Psychiatry 2018, 63, 577–580. [Google Scholar] [CrossRef]
- Hartmann, S.; Weiss, M.; Newman, A.; Hoegl, M. Resilience in the Workplace: A Multilevel Review and Synthesis. Appl. Psychol. 2019, 69, 913–959. [Google Scholar] [CrossRef]
- Leppin, A.L.; Bora, P.R.; Tilburt, J.C.; Gionfriddo, M.R.; Zeballos-Palacios, C.; Dulohery, M.M.; Sood, A.; Erwin, P.J.; Brito, J.P.; Boehmer, K.R.; et al. The efficacy of resiliency training programs: A systematic review and meta-analysis of randomized trials. PLoS ONE 2014, 9, e111420. [Google Scholar] [CrossRef]
- Jones, N.; Whelan, C.; Harden, L.; Macfarlane, A.; Burdett, H.; Greenberg, N. Resilience-based intervention for UK military recruits: A randomised controlled trial. Occup. Environ. Med. 2019, 76, 90–96. [Google Scholar] [CrossRef]
- Robertson, I.T.; Cooper, C.L.; Sarkar, M.; Curran, T. Resilience training in the workplace from 2003 to 2014: A systematic review. J. Occup. Organ. Psychol. 2015, 88, 533–562. [Google Scholar] [CrossRef]
- Everly, G.S.; Flannery, R.B.; Mitchell, J.T. Critical incident stress management (CISM): A review of the literature. Aggress. Violent Behav. 2000, 5, 23–40. [Google Scholar] [CrossRef]
- Cyr, C.; McKee, H.; O’Hagan, M.; Robyn, P. Making the Case for Peer Support: Report to the Peer Support Project Committee of the Mental Health Comission of Canada; Mental Health Commission of Canada: Toronto, ON, Canada, 2010. [Google Scholar]
- Feuer, B.S. First Responder Peer Support: An Evidence-Informed Approach. J. Police Crim. Psychol. 2021, 36, 365–371. [Google Scholar] [CrossRef]
- Anderson, G.S.; Di Nota, P.M.; Groll, D.; Carleton, R.N. Peer Support and Crisis-Focused Psychological Interventions Designed to Mitigate Post-Traumatic Stress Injuries among Public Safety and Frontline Healthcare Personnel: A Systematic Review. Int. J. Environ. Res. Public Health 2020, 17, 7645. [Google Scholar] [CrossRef] [PubMed]
- Gillard, S. Peer support in mental health services: Where is the research taking us, and do we want to go there? J. Ment. Health 2019, 28, 341–344. [Google Scholar] [CrossRef] [PubMed]
- Vittinghoff, E.; McCulloch, C.E. Relaxing the rule of ten events per variable in logistic and Cox regression. Am. J. Epidemiol. 2007, 165, 710–718. [Google Scholar] [CrossRef]
| Demographic Category | N (%) | BRS | PCL-5 | PHQ-9 | GAD-7 | |
|---|---|---|---|---|---|---|
| Range 1–5 | Range 0–80 | Range 0–27 | Range 0–21 | |||
| Mean (SD) | Mean (SD) | Mean (SD) | Mean (SD) | |||
| All Participants | 589 | 3.73 (0.67) | 13.98 (4.16) | 4.73 (4.74) | 4.46 (4.76) | |
| Gender | Men | 354 (60%) | 3.77 (0.65) | 13.69 (0.72) | 4.34 (4.28) | 3.87 (4.23) |
| Women | 232 (39%) | 3.67 (0.69) | 14.50 (0.99) | 5.34 (5.34) * | 5.38 (5.38) *** | |
| Relationship status | Single | 143 (24%) | 3.62 (0.61) | 14.17 (14.28) | 5.25 (4.79) | 4.71 (4.75) |
| Relationship | 446 (76%) | 3.77 (0.68) * | 13.92 (14.14) | 4.57 (4.72) | 4.37 (4.70) | |
| Employment | Part-time | 194 (33%) | 3.74 (0.66) | 10.85 (11.90) | 3.70 (4.32) | 3.29 (4.08) |
| Full-time | 394 67%) | 3.73 (0.67) | 15.56 (14.92) *** | 5.24 (4.86) *** | 5.04 (4.97) *** | |
| Education | College | 330 (56%) | 3.71 (0.67) | 14.77 (14.33) | 4.97 (4.97) | 4.75 (4.84) |
| University | 259 (44%) | 3.76 (0.65) | 12.98 (13.91) | 4.42 (4.60) | 4.09 (4.64) | |
| Provider classification | PCP | 398 (67%) | 3.69 (0.67) | 13.30 (13.62) | 4.77 (4.82) | 4.45 (4.82) |
| ACP | 188 (32%) | 3.82 (0.65) * | 15.42 (15.16) | 4.64 (4.57) | 4.48 (4.64) | |
| Peer support team | Member | 29 (45%) | 3.54 (0.82) | 23.41 (22.59) *** | 7.76 (6.42) *** | 7.38 (6.50) ** |
| Nonmember | 560 (95%) | 3.74 (0.66) | 13.53 (13.46) | 4.58 (4.60) | 4.31 (4.62) | |
| All Participants (N (%)) | BRS < 3.00 | PCL-5 > 32 | PHQ-9 > 9 | GAD-7 > 9 | Any | |||||
|---|---|---|---|---|---|---|---|---|---|---|
| 63 (10.7%) | 66 (11.2%) | 91 (15.4%) | 87 (14.7%) | 145 (24.6%) | ||||||
| Covariate | OR | 95% CI | OR | 95% CI | OR | 95% CI | OR | 95% CI | OR | 95% CI |
| Age | 0.99 | 0.96–1.02 | 1.06 *** | 1.02–1.09 | 1.04 *** | 1.02–1.07 | 1.03 * | 1.00–1.06 | 1.04 *** | 1.01–1.06 |
| Experience | 0.99 | 0.95–1.02 | 1.05 *** | 1.02–1.09 | 1.04 ** | 1.01–1.07 | 1.03 ** | 1.00–1.06 | 1.05 *** | 1.02–1.07 |
| Women | 1.35 | 0.79–2.27 | 0.73 | 0.43–1.26 | 1.61 * | 1.02–2.52 | 1.88 ** | 1.19–2.98 | 1.38 | 0.94–2.02 |
| Single | 1.38 | 0.78–2.46 | 0.81 | 0.43–1.52 | 1.21 | 0.73–2.00 | 1.13 | 0.67–1.90 | 1.25 | 0.81–1.91 |
| Full-time | 0.78 | 0.45–1.34 | 2.72 ** | 1.39–5.33 | 2.87 *** | 1.60–5.16 | 2.63 *** | 1.50–4.83 | 2.82 *** | 1.77–4.50 |
| College | 0.97 | 0.57–1.64 | 1.53 | 0.89–2.61 | 1.32 | 0.78–1.94 | 1.78 * | 1.10–2.89 | 1.43 | 0.97–2.11 |
| ACP | 0.76 | 0.42–1.36 | 1.54 | 0.91–2.60 | 0.98 | 0.61–1.59 | 1.00 | 0.61–1.63 | 1.06 | 0.71–1.58 |
| Peer supporter | 1.35 | 0.45–4.01 | 4.70 *** | 2.08–10.62 | 4.72 *** | 1.96–9.28 | 2.76 * | 1.21–6.28 | 3.03 ** | 1.42–6.45 |
| “Low” resilience (BRS < 3.00) | 9.30 *** | 5.12–16.89 | 6.34 *** | 3.61–11.12 | 6.29 *** | 3.57–11.08 | 8.15 *** | 4.62–14.36 | ||
| Model ((χ2 (p)) | PCL-5 > 32 | PHQ-9 > 9 | GAD-7 > 9 | Any Positive Screen | ||||||
| 82.19 (p < 0.001) | 78.30 (p < 0.001) | 72.14 (p < 0.001) | 101.3 (p < 0.001) | |||||||
| Covariate | OR | 95% CI | OR | 95% CI | OR | 95% CI | OR | 95% CI | ||
| Age | 1.07 * | 1.00–1.13 | 1.06 * | 1.00–1.11 | 1.02 | 0.96–1.08 | 1.02 | 0.97–1.07 | ||
| Experience | 0.96 | 0.90–1.03 | 0.97 | 0.91–1.03 | 0.99 | 0.93–1.05 | 1.00 | 0.95–1.06 | ||
| Women | 0.73 | 0.39–1.37 | 1.78 * | 1.07–2.95 | 2.20 ** | 1.32–3.67 | 1.52 | 0.98–2.34 | ||
| Single | 0.95 | 0.46–1.96 | 1.35 | 0.76–2.40 | 1.22 | 0.68–2.19 | 1.45 | 0.88–2.34 | ||
| Full-time | 2.15 | 0.93–4.96 | 2.85 ** | 1.41–5.77 | 2.85 ** | 1.41–5.77 | 3.06 *** | 1.70–5.50 | ||
| University | 0.70 | 0.37–1.32 | 0.82 | 0.48–1.39 | 0.50 * | 0.29–0.86 | 0.70 | 0.45–1.10 | ||
| Advanced care | 1.19 | 0.62–2.28 | 0.77 | 0.40–1.29 | 0.82 | 0.45–1.46 | 0.76 | 0.46–1.24 | ||
| Peer supporter | 4.05 ** | 1.57–10.43 | 3.31 ** | 1.40–7.84 | 2.07 | 0.83–5.14 | 2.13 | 0.92–4.89 | ||
| “Low” resilience (BRS < 3.00) | 13.09 *** | 6.70–25.54 | 7.65 *** | 4.14–14.10 | 7.33 *** | 3.96–13.55 | 10.41 *** | 5.59–19.40 | ||
| Model (χ2 (p)) | 0.41 (p = 0.81) | 0.911 (p = 0.63) | 0.75 (p = 0.68) | 1.06 (p = 0.58) | ||||||
| Interaction Term | OR | 95% CI | OR | 95% CI | OR | 95% CI | OR | 95% CI | ||
| Gender × university | 1.48 | 0.42–5.32 | 0.62 | 0.22–1.75 | 0.97 | 0.33–2.85 | 0.68 | 0.28–1.66 | ||
| Full-time × gender | 0.90 | 0.19–4.19 | 0.77 | 0.22–2.72 | 0.56 | 0.15–2.07 | 0.70 | 0.24–1.97 | ||
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Mausz, J.; Donnelly, E.A.; Moll, S.; Harms, S.; McConnell, M. Mental Disorder Symptoms and the Relationship with Resilience among Paramedics in a Single Canadian Site. Int. J. Environ. Res. Public Health 2022, 19, 4879. https://doi.org/10.3390/ijerph19084879
Mausz J, Donnelly EA, Moll S, Harms S, McConnell M. Mental Disorder Symptoms and the Relationship with Resilience among Paramedics in a Single Canadian Site. International Journal of Environmental Research and Public Health. 2022; 19(8):4879. https://doi.org/10.3390/ijerph19084879
Chicago/Turabian StyleMausz, Justin, Elizabeth Anne Donnelly, Sandra Moll, Sheila Harms, and Meghan McConnell. 2022. "Mental Disorder Symptoms and the Relationship with Resilience among Paramedics in a Single Canadian Site" International Journal of Environmental Research and Public Health 19, no. 8: 4879. https://doi.org/10.3390/ijerph19084879
APA StyleMausz, J., Donnelly, E. A., Moll, S., Harms, S., & McConnell, M. (2022). Mental Disorder Symptoms and the Relationship with Resilience among Paramedics in a Single Canadian Site. International Journal of Environmental Research and Public Health, 19(8), 4879. https://doi.org/10.3390/ijerph19084879








