A Cross-Sectional Study of Knowledge, Attitudes, and Practices concerning COVID-19 Outbreaks in the General Population in Malang District, Indonesia
Abstract
1. Introduction
2. Materials and Methods
2.1. Study Setting
2.2. Study Design
2.3. Measures
2.3.1. Knowledge, Attitudes, and Practices regarding COVID-19 Prevention
2.3.2. Sociodemographic and Other Factors
2.4. Statistical Analysis
3. Results
3.1. Sociodemographic Characteristics and Other Factors
3.2. Knowledge, Attitudes and Practices regarding COVID-19
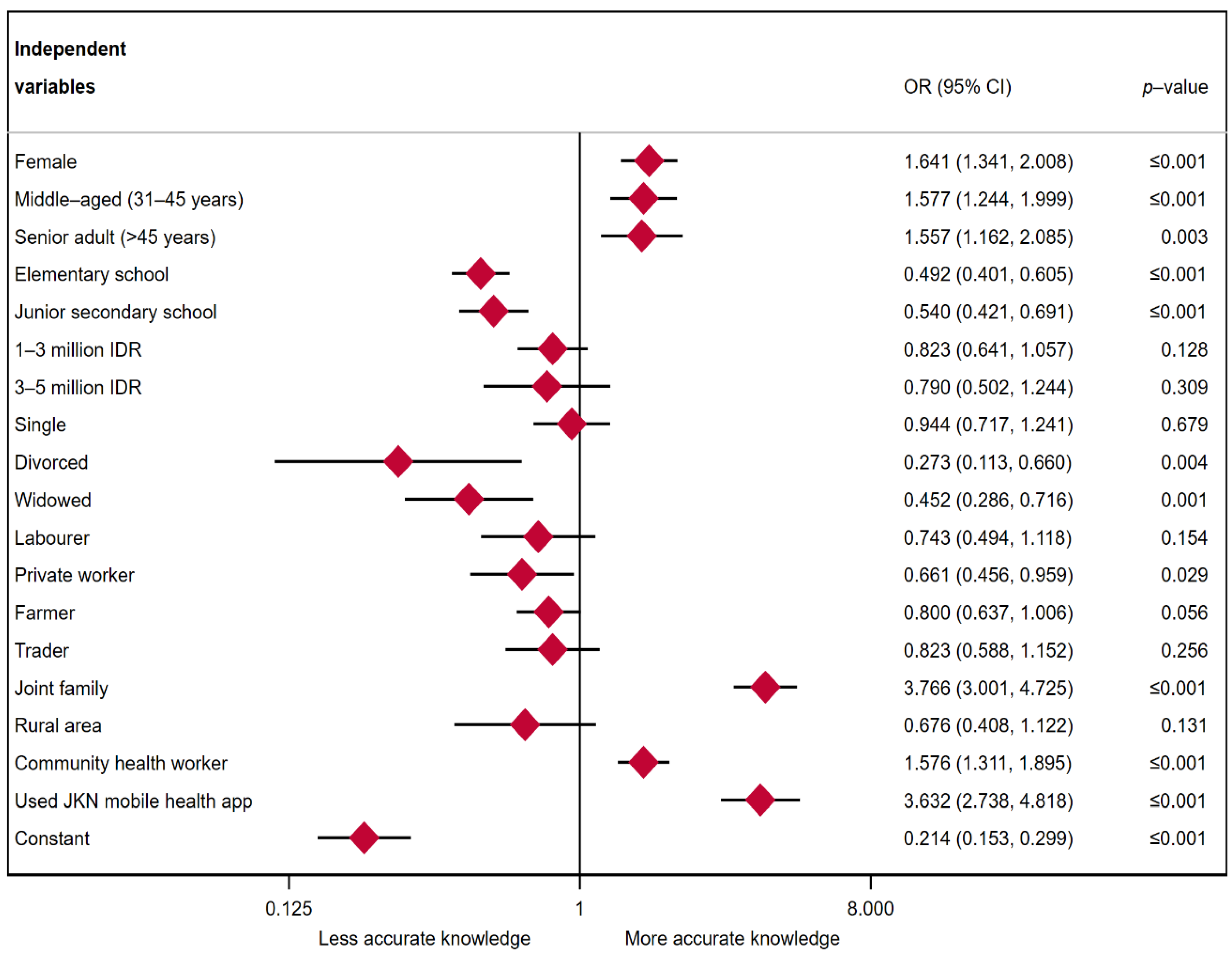
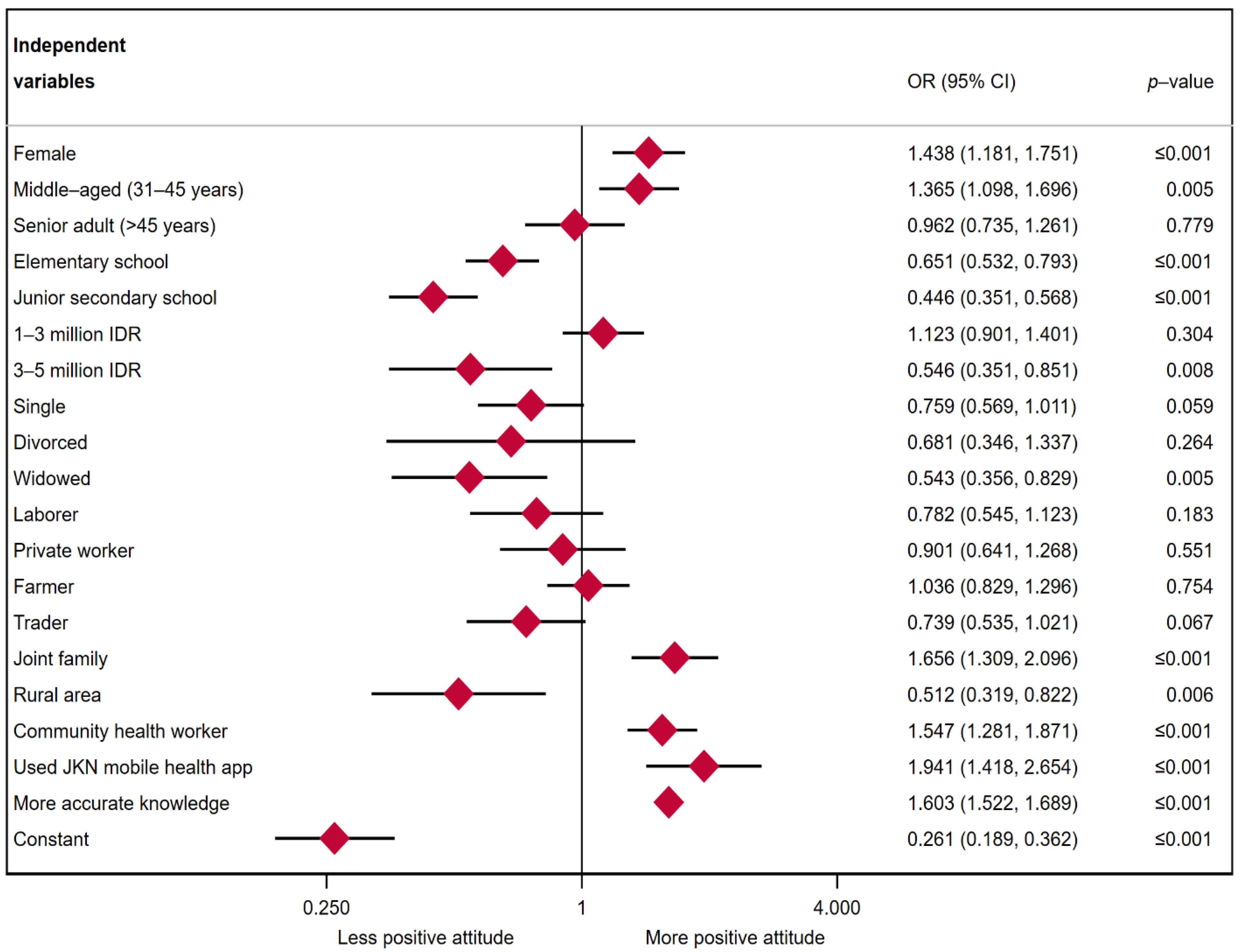
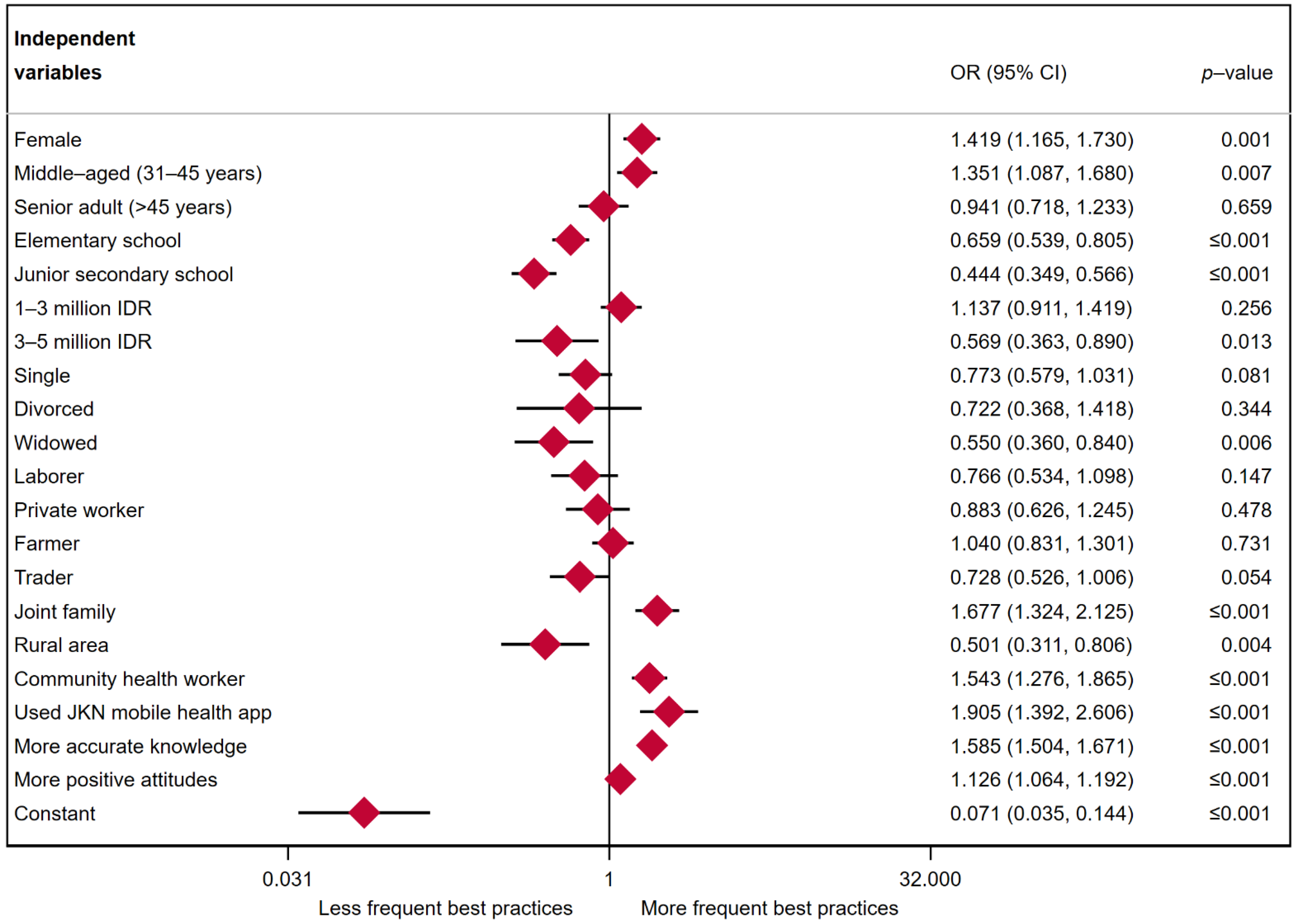
3.3. Multiple Logistic Regression Results
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
Abbreviations
| COVID-19 | Coronavirus disease |
| KAP | Knowledge, attitudes, and practices |
| WHO | World Health Organization |
| MERS-CoV | Middle East respiratory syndrome coronavirus |
| IDR | Indonesian Rupiah |
| CI | Confidence Interval |
| USD | United States Dollar |
| OR | Odds ratio |
References
- Person, B.; Sy, F.; Holton, K.; Govert, B.; Liang, A. Fear and stigma: The epidemic within the SARS outbreak. Emerg. Infect. Dis. 2004, 10, 358. [Google Scholar] [CrossRef] [PubMed]
- Masoud, A.T.; Zaazouee, M.S.; Elsayed, S.M.; Ragab, K.M.; Kamal, E.M.; Alnasser, Y.T.; Assar, A.; Nourelden, A.Z.; Istatiah, L.J.; Abd-Elgawad, M.M. KAP-COVIDGLOBAL: A multinational survey of the levels and determinants of public knowledge, attitudes and practices towards COVID-19. BMJ Open 2021, 11, e043971. [Google Scholar] [CrossRef] [PubMed]
- Ferdous, M.Z.; Islam, M.S.; Sikder, M.T.; Mosaddek, A.S.M.; Zegarra-Valdivia, J.; Gozal, D. Knowledge, attitude, and practice regarding COVID-19 outbreak in Bangladesh: An online-based cross-sectional study. PLoS ONE 2020, 15, e0239254. [Google Scholar] [CrossRef] [PubMed]
- Bates, B.R.; Moncayo, A.L.; Costales, J.A.; Herrera-Cespedes, C.A.; Grijalva, M.J. Knowledge, attitudes, and practices towards COVID-19 among Ecuadorians during the outbreak: An online cross-sectional survey. J. Community Health 2020, 45, 1158–1167. [Google Scholar] [CrossRef] [PubMed]
- Siddiqui, A.A.; Alshammary, F.; Amin, J.; Rathore, H.A.; Hassan, I.; Ilyas, M.; Khursheed Alam, M. Knowledge and practice regarding prevention of COVID-19 among the Saudi Arabian population. Work 2020, 66, 767–775. [Google Scholar] [CrossRef] [PubMed]
- Al-Hanawi, M.K.; Angawi, K.; Alshareef, N.; Qattan, A.; Helmy, H.Z.; Abudawood, Y.; Alqurashi, M.; Kattan, W.M.; Kadasah, N.A.; Chirwa, G.C. Knowledge, attitude and practice toward COVID-19 among the public in the Kingdom of Saudi Arabia: A cross-sectional study. Front. Public Health 2020, 8, 217. [Google Scholar] [CrossRef]
- Zhong, B.-L.; Luo, W.; Li, H.-M.; Zhang, Q.-Q.; Liu, X.-G.; Li, W.-T.; Li, Y. Knowledge, attitudes, and practices towards COVID-19 among Chinese residents during the rapid rise period of the COVID-19 outbreak: A quick online cross-sectional survey. Int. J. Biol. Sci. 2020, 16, 1745. [Google Scholar] [CrossRef]
- Yapi, R.B.; Houngbedji, C.A.; N’Guessan, D.K.; Dindé, A.O.; Sanhoun, A.R.; Amin, A.; Gboko, K.D.; Heitz-Tokpa, K.; Fokou, G.; Bonfoh, B. Knowledge, Attitudes, and Practices (KAP) Regarding the COVID-19 Outbreak in Côte d’Ivoire: Understanding the Non-Compliance of Populations with Non-Pharmaceutical Interventions. Int. J. Environ. Res. Public Health 2021, 18, 4757. [Google Scholar] [CrossRef]
- Fridman, I.; Lucas, N.; Henke, D.; Zigler, C.K. Association between public knowledge about COVID-19, trust in information sources, and adherence to social distancing: Cross-sectional survey. JMIR Public Health Surveill. 2020, 6, e22060. [Google Scholar] [CrossRef]
- Bassi, A.; Arfin, S.; John, O.; Jha, V. An overview of mobile applications (apps) to support the coronavirus disease 2019 response in India. Indian J. Med. Res. 2020, 151, 468. [Google Scholar]
- Pascawati, N.A.; Satoto, T.B.T. Public knowledge, attitudes and practices towards COVID-19. Int. J. Public Health Sci. 2020, 9, 292–302. [Google Scholar]
- Olivia, S.; Gibson, J.; Nasrudin, R.A. Indonesia in the Time of COVID-19. Bull. Indones. Econ. Stud. 2020, 56, 143–174. [Google Scholar] [CrossRef]
- Firmansyah, M.I.; Rahmanto, F.; Setyawan, D. The preparedness for the COVID-19 pandemic management in Indonesia. J. Adm. Kesehat. Indones. 2020, 8, 188–201. [Google Scholar] [CrossRef]
- Windarwati, H.D.; Ati, N.A.L.; Paraswati, M.D.; Ilmy, S.K.; Supianto, A.A.; Rizzal, A.F.; Sulaksono, A.D.; Lestari, R.; Supriati, L. Stressor, coping mechanism, and motivation among health care workers in dealing with stress due to the COVID-19 pandemic in Indonesia. Asian J. Psychiatry 2021, 56, 102470. [Google Scholar] [CrossRef] [PubMed]
- Papagiannis, D.; Malli, F.; Raptis, D.G.; Papathanasiou, I.V.; Fradelos, E.C.; Daniil, Z.; Rachiotis, G.; Gourgoulianis, K.I. Assessment of knowledge, attitudes, and practices towards new coronavirus (SARS-CoV-2) of health care professionals in Greece before the outbreak period. Int. J. Environ. Res. Public Health 2020, 17, 4925. [Google Scholar] [CrossRef] [PubMed]
- Badan Pusat Statistik. Profil Kependudukan Kabupaten Malang; BPS Kabupaten Malang: Malang, Indonesia, 2021. [Google Scholar]
- Worldometer. (n.d.). COVID live-Coronavirus Statistics. Available online: https://www.worldometers.info/coronavirus/ (accessed on 27 March 2022).
- Indonesia Ministry of Health. Peta Sebaran COVID-19 Indonesia (In Indonesian Language). Available online: https://covid19.go.id/peta-sebaran-covid19 (accessed on 27 March 2022).
- Dinas Kesehatan Kabupaten Malang. Profile Puskesmas Kabupaten Malang (In Indonesian language); Dinkes Kab. Malang: Malang, Indonesia, 2020. [Google Scholar]
- Lakshminarasimhappa, M. Web-Based and Smart Mobile App for Data Collection: Kobo Toolbox/Kobo Collect. J. Indian Libr. Assoc. 2021, 57, 72–79. [Google Scholar]
- Wahed, W.Y.A.; Hefzy, E.M.; Ahmed, M.I.; Hamed, N.S. Assessment of knowledge, attitudes, and perception of health care workers regarding COVID-19, a cross-sectional study from Egypt. J. Community Health 2020, 45, 1242–1251. [Google Scholar] [CrossRef]
- Taber, K.S. The use of Cronbach’s alpha when developing and reporting research instruments in science education. Res. Sci. Educ. 2018, 48, 1273–1296. [Google Scholar] [CrossRef]
- Sulistyawati, S.; Hidayat, M.S.; Wijayanti, S.P.M.; Sukesi, T.W.; Hastuti, S.K.W.; Mulasari, S.A.; Tentama, F.; Rokhmayanti, R.; Putra, U.Y.; Djannah, S.N. Knowledge, attitude, and practice towards COVID-19 among university students in Indonesia: A cross-sectional study. Int. J. Public Health 2021, 10, 735–743. [Google Scholar] [CrossRef]
- Azlan, A.A.; Hamzah, M.R.; Sern, T.J.; Ayub, S.H.; Mohamad, E. Public knowledge, attitudes and practices towards COVID-19: A cross-sectional study in Malaysia. PLoS ONE 2020, 15, e0233668. [Google Scholar] [CrossRef]
- Yue, S.; Zhang, J.; Cao, M.; Chen, B. Knowledge, attitudes and practices of COVID-19 among urban and rural residents in China: A cross-sectional study. J. Community Health 2021, 46, 286–291. [Google Scholar] [CrossRef] [PubMed]
- Reuben, R.C.; Danladi, M.M.; Saleh, D.A.; Ejembi, P.E. Knowledge, attitudes and practices towards COVID-19: An epidemiological survey in North-Central Nigeria. J. Community Health 2021, 46, 457–470. [Google Scholar] [CrossRef] [PubMed]
- Yousaf, M.A.; Noreen, M.; Saleem, T.; Yousaf, I. A cross-sectional survey of knowledge, attitude, and practices (KAP) toward pandemic COVID-19 among the general population of Jammu and Kashmir, India. Soc. Work Public Health 2020, 35, 569–578. [Google Scholar] [CrossRef] [PubMed]
- Lee, M.; Kang, B.-A.; You, M. Knowledge, attitudes, and practices (KAP) toward COVID-19: A cross-sectional study in South Korea. BMC Public Health 2021, 21, 295. [Google Scholar] [CrossRef]
- Rivera-Lozada, O.; Galvez, C.A.; Castro-Alzate, E.; Bonilla-Asalde, C.A. Factors associated with knowledge, attitudes and preventive practices towards COVID-19 in health care professionals in Lima, Peru. F1000Research 2021, 10, 1–31. [Google Scholar] [CrossRef]
- Hossain, M.A.; Jahid, M.I.K.; Hossain, K.M.A.; Walton, L.M.; Uddin, Z.; Haque, M.O.; Kabir, M.F.; Arafat, S.Y.; Sakel, M.; Faruqui, R. Knowledge, attitudes, and fear of COVID-19 during the Rapid Rise Period in Bangladesh. PLoS ONE 2020, 15, e0239646. [Google Scholar] [CrossRef]
- Honarvar, B.; Lankarani, K.B.; Kharmandar, A.; Shaygani, F.; Zahedroozgar, M.; Haghighi, M.R.R.; Ghahramani, S.; Honarvar, H.; Daryabadi, M.M.; Salavati, Z. Knowledge, attitudes, risk perceptions, and practices of adults toward COVID-19: A population and field-based study from Iran. Int. J. Public Health 2020, 65, 731–739. [Google Scholar] [CrossRef]
- Rahman, A.; Sathi, N.J. Knowledge, Attitude, and Preventive Practices toward COVID-19 among Bangladeshi Internet Users. Electron. J. Gen. Med. 2020, 17, em245. [Google Scholar] [CrossRef]
- Sheeran, P.; Maki, A.; Montanaro, E.; Avishai-Yitshak, A.; Bryan, A.; Klein, W.M.; Miles, E.; Rothman, A.J. The impact of changing attitudes, norms, and self-efficacy on health-related intentions and behavior: A meta-analysis. Health Psychol. 2016, 35, 1178. [Google Scholar] [CrossRef]
- McEachan, R.; Taylor, N.; Harrison, R.; Lawton, R.; Gardner, P.; Conner, M. Meta-analysis of the reasoned action approach (RAA) to understanding health behaviors. Ann. Behav. Med. 2016, 50, 592–612. [Google Scholar] [CrossRef]
- Godin, G.; Kok, G. The theory of planned behavior: A review of its applications to health-related behaviors. Am. J. Health Promot. 1996, 11, 87–98. [Google Scholar] [CrossRef] [PubMed]
- Chang, C.T.; Lee, M.; Lee, J.C.Y.; Lee, N.C.T.; Ng, T.Y.; Shafie, A.A.; Thong, K.S. Public KAP towards COVID-19 and antibiotics resistance: A Malaysian survey of knowledge and awareness. Int. J. Environ. Res. Public Health 2021, 18, 3964. [Google Scholar] [CrossRef] [PubMed]
- Alqahtani, A.H.; Alqahtani, S.A.; Alhodaib, A.S.; Al-Wathinani, A.M.; Daoulah, A.; Alhamid, S.; Al-Otaibi, S.N.; Abufayyah, M.; Wazzan, A.M.; Alshahrani, S.S. Knowledge, Attitude, and Practice (KAP) toward the Novel Coronavirus (COVID-19) Pandemic in a Saudi Population-Based Survey. Int. J. Environ. Res. Public Health 2021, 18, 5286. [Google Scholar] [CrossRef] [PubMed]
- Alnasser, A.H.A.; Al-Tawfiq, J.A.; Al-Kalif, M.S.H.; Shahadah, R.F.B.; Almuqati, K.S.A.; Al-Sulaiman, B.S.A.; Alharbi, K.K.S.; Alabbad, F.Y.M.; Alabbad, J.Y.M.; Alquwaiz, I.A.I. Public knowledge, attitudes, and practice towards COVID-19 pandemic in Saudi Arabia: A web-based cross-sectional survey. Med. Sci. 2021, 9, 11. [Google Scholar] [CrossRef]
- Inad, N. Knowledge, Attitude and Practices (KAP) during the COVID-19 pandemic among Palestinians in the Hebron governorate, Palestine. Indian J. Posit. Psychol. 2021, 12, 35–39. [Google Scholar]
- Warner, D.; Procaccino, J.D. Women seeking health information: Distinguishing the web user. J. Health Commun. 2007, 12, 787–814. [Google Scholar] [CrossRef]
- Saah, F.I.; Amu, H.; Seidu, A.-A.; Bain, L.E. Health knowledge and care seeking behaviour in resource-limited settings amidst the COVID-19 pandemic: A qualitative study in Ghana. PLoS ONE 2021, 16, e0250940. [Google Scholar] [CrossRef]
- Muslih, M.; Susanti, H.D.; Rias, Y.A.; Chung, M.-H. Knowledge, attitude and practice of Indonesian residents toward COVID-19: A cross-sectional survey. Int. J. Environ. Res. Public Health 2021, 18, 4473. [Google Scholar] [CrossRef]
- Cotten, S.R.; Gupta, S.S. Characteristics of online and offline health information seekers and factors that discriminate between them. Soc. Sci. Med. 2004, 59, 1795–1806. [Google Scholar] [CrossRef]
- Mistry, S.K.; Ali, A.M.; Yadav, U.N.; Ghimire, S.; Hossain, M.B.; Das Shuvo, S.; Saha, M.; Sarwar, S.; Nirob, M.M.H.; Sekaran, V.C. Older adults with non-communicable chronic conditions and their health care access amid COVID-19 pandemic in Bangladesh: Findings from a cross-sectional study. PLoS ONE 2021, 16, e0255534. [Google Scholar] [CrossRef]
- Suryadarma, D.; Jones, G.W. Education in Indonesia; Institute of Southeast Asian Studies: Pasar Panjang, Singapore, 2013. [Google Scholar]
- Peretti-Watel, P.; Seror, V.; Cortaredona, S.; Launay, O.; Raude, J.; Verger, P.; Beck, F.; Legleye, S.; L’haridon, O.; Ward, J. Attitudes about COVID-19 lockdown among general population, France, March 2020. Emerg. Infect. Dis. 2021, 27, 301. [Google Scholar] [CrossRef] [PubMed]
- Puspitasari, I.M.; Yusuf, L.; Sinuraya, R.K.; Abdulah, R.; Koyama, H. Knowledge, attitude, and practice during the COVID-19 pandemic: A review. J. Multidiscip. Healthc. 2020, 13, 727. [Google Scholar] [CrossRef] [PubMed]
- Nobles, J.; Buttenheim, A. Marriage and socioeconomic change in contemporary Indonesia. J. Marriage Fam. 2008, 70, 904–918. [Google Scholar] [CrossRef] [PubMed]
- Goldman, N.; Korenman, S.; Weinstein, R. Marital status and health among the elderly. Soc. Sci. Med. 1995, 40, 1717–1730. [Google Scholar] [CrossRef]
- Mohammed, M.; Sha’aban, A.; Jatau, A.I.; Yunusa, I.; Isa, A.M.; Wada, A.S.; Obamiro, K.; Zainal, H.; Ibrahim, B. Assessment of COVID-19 information overload among the general public. J. Racial Ethn. Health Disparities 2021, 9, 184–192. [Google Scholar] [CrossRef]
- Chua, A.Q.; Tan, M.M.J.; Verma, M.; Han, E.K.L.; Hsu, L.Y.; Cook, A.R.; Teo, Y.Y.; Lee, V.J.; Legido-Quigley, H. Health system resilience in managing the COVID-19 pandemic: Lessons from Singapore. BMJ Glob. Health 2020, 5, e003317. [Google Scholar] [CrossRef]
- Roy, D.; Tripathy, S.; Kar, S.K.; Sharma, N.; Verma, S.K.; Kaushal, V. Study of knowledge, attitude, anxiety & perceived mental healthcare need in Indian population during COVID-19 pandemic. Asian J. Psychiatry 2020, 51, 102083. [Google Scholar]
- Peña-Longobardo, L.; Rodríguez-Sánchez, B.; Oliva-Moreno, J. The impact of widowhood on wellbeing, health, and care use: A longitudinal analysis across Europe. Econ. Hum. Biol. 2021, 43, 101049. [Google Scholar] [CrossRef]
- Zehra, S.S.; Khalil, M.A.; Shoukat, L. When the Big Shots Deviate: On the KAP of Religious Clerics Regarding Prevention of COVID-19. Risk Manag. Healthc. Policy 2020, 13, 2801. [Google Scholar] [CrossRef]
- Marmot, M. The influence of income on health: Views of an epidemiologist. Health Aff. 2002, 21, 31–46. [Google Scholar] [CrossRef]
- Lau, L.L.; Hung, N.; Go, D.J.; Ferma, J.; Choi, M.; Dodd, W.; Wei, X. Knowledge, attitudes and practices of COVID-19 among income-poor households in the Philippines: A cross-sectional study. J. Glob. Health 2020, 10, 011007. [Google Scholar] [CrossRef] [PubMed]
- Weech-Maldonado, R.; Miller, M.J.; Lord, J.C. The relationships among socio-demographics, perceived health, and happiness. Appl. Res. Qual. Life 2017, 12, 289–302. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Mirowsky, J.; Ross, C.E. Education, Social Status, and Health; Routledge: Abingdon, UK, 2017. [Google Scholar]
- Shih, S.F.; Wagner, A.L.; Masters, N.B.; Prosser, L.A.; Lu, Y.; Zikmund-Fisher, B.J. Vaccine hesitancy and rejection of a vaccine for the novel coronavirus in the United States. Front. Immunol. 2021, 12, 2275. [Google Scholar] [CrossRef] [PubMed]
- Saqlain, M.; Ahmed, A.; Gulzar, A.; Naz, S.; Munir, M.M.; Ahmed, Z.; Kamran, S. Public Knowledge and Practices regarding COVID-19: A cross-sectional survey from Pakistan. Front. Public Health 2021, 9, 377. [Google Scholar]
- Bhaumik, S.; Moola, S.; Tyagi, J.; Nambiar, D.; Kakoti, M. Community health workers for pandemic response: A rapid evidence synthesis. BMJ Glob. Health 2020, 5, e002769. [Google Scholar] [CrossRef]
- Mane Abhay, B.; Khandekar Sanjay, V. Strengthening primary health care through Asha Workers: A novel approach in India. Prim. Health Care 2014, 4, 2167-1079. [Google Scholar]
- Gilson, L.; Walt, G.; Heggenhougen, K.; Owuor-Omondi, L.; Perera, M.; Ross, D.; Salazar, L. National community health worker programs: How can they be strengthened? J. Public Health Policy 1989, 10, 518–532. [Google Scholar] [CrossRef]
- Johnson, C.D.; Noyes, J.; Haines, A.; Thomas, K.; Stockport, C.; Ribas, A.N.; Harris, M. Learning from the Brazilian community health worker model in North Wales. Glob. Health 2013, 9, 25. [Google Scholar] [CrossRef]
- Sujarwoto, S.; Maharani, A. Participation in community-based health care interventions (CBHIs) and its association with hypertension awareness, control and treatment in Indonesia. PLoS ONE 2020, 15, e0244333. [Google Scholar] [CrossRef]
- Hassounah, M.; Raheel, H.; Alhefzi, M. Digital response during the COVID-19 pandemic in Saudi Arabia. J. Med. Internet Res. 2020, 22, e19338. [Google Scholar] [CrossRef]
- Huang, Z.; Guo, H.; Lee, Y.-M.; Ho, E.C.; Ang, H.; Chow, A. Performance of digital contact tracing tools for COVID-19 response in Singapore: Cross-sectional study. JMIR Mhealth Uhealth 2020, 8, e23148. [Google Scholar] [CrossRef] [PubMed]
- Whitelaw, S.; Mamas, M.A.; Topol, E.; Van Spall, H.G. Applications of digital technology in COVID-19 pandemic planning and response. Lancet Digit. Health 2020, 2, e435–e440. [Google Scholar] [CrossRef]
| No | Knowledge about COVID-19 | Coding and Cut-Off Levels |
|---|---|---|
| 1 | Is COVID-19 a dangerous disease? | Correct answer = 1, wrong answer or don’t know = 0. A cut-off level of ≥4 was chosen to indicate a respondent with a precise understanding of COVID-19 [4]. |
| 2 | Does it affect only humans? | |
| 3 | Does it transmit from humans to animals? | |
| 4 | Does it transmit from animals to humans? | |
| 5 | Is it transmitted by animal products (e.g., milk, meat)? | |
| 6 | Is it transmitted in well-cooked products? | |
| Attitudes toward COVID-19 | ||
| 1 | It is crucial to report a suspected case to health authorities | Disagree = 0, undecided = 1, agree = 2. A cut-off level of ≥11 was set to indicate a respondent with positive attitudes towards the prevention of COVID-19 [4]. |
| 2 | It is important to use a face mask in crowded places | |
| 3 | It is important to wash hands and face after being outside | |
| 4 | COVID-19 is a preventable disease | |
| 5 | It can be treated at home | |
| 6 | Health education can play an important role in COVID-19 prevention | |
| Practice toward COVID-19 | ||
| 1 | Do you use tissues or handkerchiefs when you cough/sneeze? | Yes = 1, no = 0, sometimes = 0 for questions 1–6. For question 7, yes = 0, sometimes = 0, no = 1. A cut-off level of ≥6 was set to indicate frequent best practices [4]. |
| 2 | Do you wash hands frequently using water and soap? | |
| 3 | Do you avoid touching face and eyes? | |
| 4 | Do you maintain social distance (or quarantine at home)? | |
| 5 | Do you eat healthy food focusing on the outbreak? | |
| 6 | Do you maintain a healthy lifestyle focusing on the outbreak? | |
| 7 | Do you obey all government rules related to COVID? |
| Variables | n (%) |
|---|---|
| Sex | |
| Male | 1286 (37.6) |
| Female | 2139 (62.4) |
| Age | |
| Young adult (17–30 years) | 1146 (33.5) |
| Middle-aged adult (30–45 years) | 1565 (45.7) |
| Older adult (>45 years) | 714 (20.8) |
| Education | |
| Elementary or less | 1763 (51.5) |
| Junior secondary | 699 (20.4) |
| High school or more | 963 (28.1) |
| Monthly family income (in IDR) | |
| <1 million | 2818 (82.3) |
| 1–3 million | 485 (14.1) |
| >3 million | 122 (3.6) |
| Marital status | |
| Single | 736 (21.5) |
| Married | 2508 (73.2) |
| Divorced | 41 (1.2) |
| Widowed | 140 (4.1) |
| Type of employment | |
| Student | 948 (27.7) |
| Laborer (i.e., construction, factory workers) | 205 (6.0) |
| Civil servant | 62 (1.8) |
| Privately employed (i.e., bank, supermarket, restaurant, hotel) | 230 (6.7) |
| Farmer | 1763 (51.5) |
| Trader (merchant, dealer, salesperson) | 217 (6.3) |
| Family type | |
| Nuclear | 2185 (63.8) |
| Joint | 1240 (36.2) |
| Used JKN COVID-19 screening app | |
| No | 3179 (92.8) |
| Yes | 246 (7.2) |
| Informed by community health workers about COVID-19 prevention | |
| No | 2596 (75.8) |
| Yes | 829 (24.2) |
| Residential area | |
| Rural | 3325 (97.1) |
| Urban | 100 (2.9) |
| Knowledge about COVID-19 | |
| More accurate | 914 (25.3%) |
| Less accurate | 2661 (74.7%) |
| Attitudes towards COVID-19 | |
| More positive attitude | 784 (36.6%) |
| Less positive attitude | 2641 (62.4%) |
| Practices regarding COVID-19 | |
| More frequent best practices | 1670 (48.8%) |
| Less frequent best practices | 1755 (51.2%) |
| Knowledge about COVID-19 | Yes | No | Don’t Know |
|---|---|---|---|
| Is COVID-19 a dangerous disease? | 3251 (94.9%) | 84 (2.5%) | 90 (2.6%) |
| Does it affect only humans? | 2484 (72.5%) | 586 (17.1%) | 355 (10.4%) |
| Does it transmit from humans to animals? | 1133 (33.1%) | 1063 (31.0%) | 1229 (35.9%) |
| Does it transmit from animals to humans? | 1608 (46.9%) | 640 (18.7%) | 1177 (34.4%) |
| Is it transmitted by animal products (e.g., milk, meat)? | 1039 (30.3%) | 1116 (32.6%) | 1270 (37.1%) |
| Is it transmitted in well-cooked products? | 730 (21.3%) | 1696 (49.5%) | 999 (29.2%) |
| Attitudes toward COVID-19 | Agree | Undecided | Disagree |
| It is crucial to report a suspected case to health authorities | 3209 (93.7%) | 159 (4.6%) | 57 (1.7%) |
| It is important to use a face mask in crowded places | 3328 (97.2%) | 62 (1.8%) | 35 (1.0%) |
| It is important to wash hands and face after being outside | 3305 (96.5%) | 63 (1.8%) | 57 (1.7%) |
| COVID-19 is a preventable disease | 3151 (92.0%) | 211 (6.2%) | 63 (1.8%) |
| It can be treated at home | 2388 (69.7%) | 532 (15.5%) | 505 (14.7%) |
| Health education can play an important role in COVID-19 prevention | 3198 (93.4%) | 140 (4.1%) | 87 (2.5%) |
| Practices regarding COVID-19 | Yes | No | Sometimes |
| Do you use tissues or handkerchiefs when you cough/sneeze? | 1983 (57.9%) | 231 (6.7%) | 1211 (35.4%) |
| Do you wash your hands frequently using water and soap? | 2470 (72.1%) | 66 (1.9%) | 889 (26.0%) |
| Do you avoid touching face and eyes? | 1774 (51.8%) | 340 (9.9%) | 1311 (38.3%) |
| Do you maintain social distance (or quarantine at home)? | 1961 (57.3%) | 371 (10.8%) | 1093 (31.9%) |
| Do you eat healthy food focusing on the outbreak? | 2123 (62.0%) | 207 (6.0%) | 1095 (32.0%) |
| Do you maintain a healthy lifestyle focusing on the outbreak? | 2374 (69.3%) | 112 (3.3%) | 939 (27.4%) |
| Do you obey all government rules related to COVID-19? | 1984 (57.9%) | 590 (17.2%) | 851 (24.8%) |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Sujarwoto, S.; Holipah, H.; Maharani, A. A Cross-Sectional Study of Knowledge, Attitudes, and Practices concerning COVID-19 Outbreaks in the General Population in Malang District, Indonesia. Int. J. Environ. Res. Public Health 2022, 19, 4287. https://doi.org/10.3390/ijerph19074287
Sujarwoto S, Holipah H, Maharani A. A Cross-Sectional Study of Knowledge, Attitudes, and Practices concerning COVID-19 Outbreaks in the General Population in Malang District, Indonesia. International Journal of Environmental Research and Public Health. 2022; 19(7):4287. https://doi.org/10.3390/ijerph19074287
Chicago/Turabian StyleSujarwoto, Sujarwoto, Holipah Holipah, and Asri Maharani. 2022. "A Cross-Sectional Study of Knowledge, Attitudes, and Practices concerning COVID-19 Outbreaks in the General Population in Malang District, Indonesia" International Journal of Environmental Research and Public Health 19, no. 7: 4287. https://doi.org/10.3390/ijerph19074287
APA StyleSujarwoto, S., Holipah, H., & Maharani, A. (2022). A Cross-Sectional Study of Knowledge, Attitudes, and Practices concerning COVID-19 Outbreaks in the General Population in Malang District, Indonesia. International Journal of Environmental Research and Public Health, 19(7), 4287. https://doi.org/10.3390/ijerph19074287







