Functioning Problems Associated with Health Conditions with Greatest Disease Burden in South Africa: A Scoping Review
Abstract
1. Introduction
2. Materials and Methods
2.1. Search Method
2.2. Study Selection
2.3. Charting the Data
| Balance and coordination problems Behaviour problems Bowel and bladder problems Communication problems Fine motor skill problems IADLs problems Joint mobility/stiffness Mental disorders Mobility problems Muscle function/paralysis Pain (acute, chronic, unspecified) | Physical capacity problems Respiratory problems Self-care problems Sensory problems Skin problems Swallowing problems Swelling Vision problems Weight problems Working and schooling problems Sexuality problems |
2.4. Quality Assessment
2.5. Data Analysis
2.5.1. Type of Functioning Problems
2.5.2. Prevalence of the Functioning Problems
3. Results
3.1. Study Characteristics
3.2. Prevalence of the Top 20 Functioning Problems
3.3. Breakdown of the Most Prevalent Problems
3.3.1. Mobility Problems
3.3.2. Pain Problems
3.3.3. Mental Health Problems
3.4. Mapping to the ICF
4. Discussion
4.1. Strengths and Limitations of the Study
4.2. Further Research
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Stucki, G.; Bickenbach, J. Functioning: The Third Health Indicator in the Health System and the Key Indicator for Rehabilitation. Eur. J. Phys. Rehabil. Med. 2017, 53, 134–138. [Google Scholar] [CrossRef] [PubMed]
- World Health Organization. How to Use the ICF: A Practical Manual for Using the International Classification of Functioning, Disability and Health (ICF). Exposure Draft for Comment; World Health Organization: Geneva, Switzerland, 2013. [Google Scholar]
- Barua, A.; Hazarika, J.; Basilio, M.A.; Soans, S.J.; Colin, M.; Kamath, A. Functional Impairments: A Study in Elderly Individuals. J. Int. Med. Sci. Acad. 2011, 24, 61–63. [Google Scholar]
- Duntava, A.; Borisova, L.V.; Mäkinen, I.H. The Structure of Health in Europe: The Relationships between Morbidity, Functional Limitation, and Subjective Health. SSM—Popul. Health 2021, 16, 100911. [Google Scholar] [CrossRef] [PubMed]
- GBD 2019 Diseases and Injuries Collaborators. Global Burden of 369 Diseases and Injuries in 204 Countries and Territories, 1990–2019: A Systematic Analysis for the Global Burden of Disease Study 2019. Lancet 2020, 396, 1204–1222. [Google Scholar] [CrossRef] [PubMed]
- Vos, T.; Flaxman, A.D.; Naghavi, M.; Lozano, R.; Michaud, C.; Ezzati, M.; Shibuya, K.; Salomon, J.A.; Abdalla, S.; Aboyans, V.; et al. Years Lived with Disability (YLDs) for 1160 Sequelae of 289 Diseases and Injuries 1990-2010: A Systematic Analysis for the Global Burden of Disease Study 2010. Lancet 2012, 380, 2163. [Google Scholar] [CrossRef]
- Jesus, T.S.; Landry, M.D.; Hoenig, H. Global Need for Physical Rehabilitation: Systematic Analysis from the Global Burden of Disease Study 2017. Int. J. Environ. Res. Public Health 2019, 16, 980. [Google Scholar] [CrossRef]
- Louw, Q.; Grimmer, K.; Berner, K.; Conradie, T.; Bedada, D.T.; Jesus, T.S. Towards a Needs-Based Design of the Physical Rehabilitation Workforce in South Africa: Trend Analysis [1990–2017] and a 5-Year Forecasting for the Most Impactful Health Conditions Based on Global Burden of Disease Estimates. BMC Public Health 2021, 21, 913. [Google Scholar] [CrossRef]
- Madden, R.; Ferreira, M.; Einfeld, S.; Emerson, E.; Manga, R.; Refshauge, K.; Llewellyn, G. New Directions in Health Care and Disability: The Need for a Shared Understanding of Human Functioning. Aust. N. Z. J. Public Health 2012, 36, 458–461. [Google Scholar] [CrossRef]
- Stucki, G.; Bickenbach, J.; Gutenbrunner, C.; Melvin, J. Rehabilitation: The Health Strategy of the 21st Century. J. Rehabil. Med. 2018, 50, 309–316. [Google Scholar] [CrossRef]
- Rauch, A.; Negrini, S.; Cieza, A. Toward Strengthening Rehabilitation in Health Systems: Methods Used to Develop a WHO Package of Rehabilitation Interventions. Arch. Phys. Med. Rehabil. 2019, 100, 2205–2211. [Google Scholar] [CrossRef]
- Mills, J.A.; Cieza, A.; Short, S.D.; Middleton, J.W. Development and Validation of the WHO Rehabilitation Competency Framework: A Mixed Methods Study. Arch. Phys. Med. Rehabil. 2021, 102, 1113–1123. [Google Scholar] [CrossRef]
- Johnson, L.F.; Meyer-Rath, G.; Dorrington, R.E.; Puren, A.; Seathlodi, T.; Zuma, K.; Feizzadeh, A. The Effect of HIV Programs in South Africa on National HIV Incidence Trends, 2000–2019. J. Acquir. Immune Defic. Syndr. 2022, 90, 115–123. [Google Scholar] [CrossRef]
- Maphumulo, W.T.; Bhengu, B.R. Challenges of Quality Improvement in the Healthcare of South Africa Post-Apartheid: A Critical Review. Curationis 2019, 42, 1901. [Google Scholar] [CrossRef] [PubMed]
- Roomaney, R.A.; van Wyk, B.; Cois, A.; Wyk, V.P. Van One in Five South Africans Are Multimorbid: An Analysis of the 2016 Demographic and Health Survey. PLoS ONE 2022, 17, e0269081. [Google Scholar] [CrossRef] [PubMed]
- Conradie, T.; Berner, K.; Louw, Q. Describing the Rehabilitation Workforce Capacity Data in the Public Sector of Three Rural Provinces in South Africa. Int. J. Environ. Res. Public Health 2022, 19, 12176. [Google Scholar] [CrossRef]
- Achoki, T.; Sartorius, B.; Watkins, D.; Glenn, S.D.; Kengne, A.P.; Oni, T.; Wiysonge, C.S.; Walker, A.; Adetokunboh, O.O.; Babalola, T.K.; et al. Health Trends, Inequalities and Opportunities in South Africa’s Provinces, 1990–2019: Findings from the Global Burden of Disease 2019 Study. J. Epidemiol. Community Health 2022, 76, 471–481. [Google Scholar] [CrossRef] [PubMed]
- South African National Department of Health. National Health Act: National Health Insurance Policy: Towards Universal Health Coverage | South African Government; NDoH: Pretoria, South Africa, 2017.
- Conradie, T.; Charumbira, M.; Bezuidenhout, M.; Leong, T.; Louw, Q. Rehabilitation and Primary Care Treatment Guidelines, South Africa. Bull. World Health Organ. 2022, 100, 689–698. [Google Scholar] [CrossRef]
- Cieza, A.; Oberhauser, C.; Bickenbach, J.; Chatterji, S.; Stucki, G. Towards a Minimal Generic Set of Domains of Functioning and Health. BMC Public Health 2014, 14, 218. [Google Scholar] [CrossRef]
- Prodinger, B.; Cieza, A.; Oberhauser, C.; Bickenbach, J.; Üstün, T.B.; Chatterji, S.; Stucki, G. Toward the International Classification of Functioning, Disability and Health (ICF) Rehabilitation Set: A Minimal Generic Set of Domains for Rehabilitation as a Health Strategy. Arch. Phys. Med. Rehabil. 2016, 97, 875–884. [Google Scholar] [CrossRef]
- Bright, T.; Wallace, S.; Kuper, H. A Systematic Review of Access to Rehabilitation for People with Disabilities in Low-and Middle-Income Countries. Int. J. Environ. Res. Public Health 2018, 15, 2165. [Google Scholar] [CrossRef]
- Mitra, S.; Chen, W.; Hervé, J.; Pirozzi, S.; Yap, J. Invisible or Mainstream? Disability in Surveys and Censuses in Low- and Middle-Income Countries. Soc. Indic. Res. 2022, 163, 219–249. [Google Scholar] [CrossRef]
- Sabariego, C.; Fellinghauer, C.; Lee, L.; Kamenov, K.; Posarac, A.; Bickenbach, J.; Kostanjsek, N.; Chatterji, S.; Cieza, A. Generating Comprehensive Functioning and Disability Data Worldwide: Development Process, Data Analyses Strategy and Reliability of the WHO and World Bank Model Disability Survey. Arch. Public Health 2022, 80, 6. [Google Scholar] [CrossRef]
- Banks, L.M.; Kuper, H.; Polack, S. Poverty and Disability in Low-And Middleincome Countries: A Systematic Review. PLoS ONE 2017, 12, e0189996. [Google Scholar] [CrossRef] [PubMed]
- Gutenbrunner, C.; Bickenbach, J.; Melvin, J.; Lains, J.; Nugraha, B. Strengthening Health-Related Rehabilitation Services at the National Level. J. Rehabil. Med. 2018, 50, 317–325. [Google Scholar] [CrossRef] [PubMed]
- Charumbira, M.Y.; Berner, K.; Louw, Q.A. Functioning Problems Associated with Conditions with Greatest Disease Burden in South Africa and Zimbabwe: A Scoping Review Protocol. F1000Research 2022, 11, 371. [Google Scholar] [CrossRef]
- Arksey, H.; O’Malley, L. Scoping Studies: Towards a Methodological Framework. Int. J. Soc. Res. Methodol. 2005, 8, 19–32. [Google Scholar] [CrossRef]
- Peters, M.D.J.; Godfrey, C.; McInerney, P.; Munn, Z.; Tricco, A.C.; Khalil, H. Chapter 11: Scoping Reviews (2020 Version); Aromataris, E., Munn, Z., Eds. Available online: https://reviewersmanual.joannabriggs.org/ (accessed on 28 May 2020).
- Tricco, A.C.; Lillie, E.; Zarin, W.; O’Brien, K.K.; Colquhoun, H.; Levac, D.; Moher, D.; Peters, M.D.J.; Horsley, T.; Weeks, L.; et al. PRISMA Extension for Scoping Reviews (PRISMA-ScR): Checklist and Explanation. Ann. Intern. Med. 2018, 169, 467–474. [Google Scholar] [CrossRef]
- Groce, N.E. Global Disability: An Emerging Issue. Lancet Glob. Health 2018, 6, e724–e725. [Google Scholar] [CrossRef]
- Karimi, M.; Brazier, J. Health, Health-Related Quality of Life, and Quality of Life: What Is the Difference? PharmacoEconomics 2016, 34, 645–649. [Google Scholar] [CrossRef]
- Ouzzani, M.; Hammady, H.; Fedorowicz, Z.; Elmagarmid, A. Rayyan—A Web and Mobile App for Systematic Reviews. Syst. Rev. 2016, 5, 210. [Google Scholar] [CrossRef] [PubMed]
- Munn, Z.; Tufanaru, C.; Aromataris, E. Data Extraction and Synthesis. Am. J. Nurs. 2014, 114, 49–54. [Google Scholar] [CrossRef] [PubMed]
- Charumbira, M.Y.; Blaauw, D.; Berner, K.; Louw, Q.A. Development of an Innovative Strategy to Determine Functioning Problems Attributed to Health Conditions in Low Resource Settings. Digit. Health 2022. Submitted. [Google Scholar]
- Harrison, J.E.; Weber, S.; Jakob, R.; Chute, C.G. ICD-11: An International Classification of Diseases for the Twenty-First Century. BMC Med. Inform. Decis. Mak. 2021, 21, 206. [Google Scholar] [CrossRef] [PubMed]
- Institute for Health Metrics and Evaluation University of Washington GBD Compare | IHME Viz Hub. Available online: https://vizhub.healthdata.org/gbd-compare/ (accessed on 11 March 2021).
- Vollmar, H.C.; Ostermann, T.; Redaèlli, M. Using the Scenario Method in the Context of Health and Health Care—A Scoping Review Data Collection, Quality, and Reporting. BMC Med. Res. Methodol. 2015, 15, 89. [Google Scholar] [CrossRef]
- Maritz, R.; Baptiste, S.; Darzins, S.W.; Magasi, S.; Weleschuk, C.; Prodinger, B. Linking Occupational Therapy Models and Assessments to the ICF to Enable Standardized Documentation of Functioning. Can. J. Occup. Ther. 2018, 85, 330–341. [Google Scholar] [CrossRef] [PubMed]
- Page, M.J.; McKenzie, J.E.; Bossuyt, P.M.; Boutron, I.; Hoffmann, T.C.; Mulrow, C.D.; Shamseer, L.; Tetzlaff, J.M.; Akl, E.A.; Brennan, S.E.; et al. The PRISMA 2020 Statement: An Updated Guideline for Reporting Systematic Reviews. BMJ 2021, 372, n71. [Google Scholar] [CrossRef]
- Bantjes, J.; Kagee, A. Suicide Prevention in HIV Treatment Centres: Population Attributable Risk Analysis of Treating Common Mental Disorders. AIDS Behav. 2021, 25, 1864–1872. [Google Scholar] [CrossRef]
- Benjamin, N.A.; Jelsma, J. An Innovative Approach to Reducing Pain in Patients with Peripheral Neuropathy Related to HIV: A Single Case Study. Afr. J. Disabil. 2014, 3, 1–4. [Google Scholar] [CrossRef]
- Cholera, R.; Pence, B.W.; Gaynes, B.N.; Bassett, J.; Qangule, N.; Pettifor, A.; Macphail, C.; Miller, W.C. Depression and Engagement in Care Among Newly Diagnosed HIV-Infected Adults in Johannesburg, South Africa. AIDS Behav. 2017, 21, 1632–1640. [Google Scholar] [CrossRef]
- Spies, G.; Fennema-Notestine, C.; Archibald, S.L.; Cherner, M.; Seedat, S. Neurocognitive Deficits in HIV-Infected Women and Victims of Childhood Trauma. AIDS Care 2012, 24, 1126–1135. [Google Scholar] [CrossRef] [PubMed]
- Spies, G.; Fennema-Notestine, C.; Cherner, M.; Seedat, S. Changes in Cognitive Function in Women with HIV Infection and Early Life Stress. AIDS Care 2017, 29, 14–23. [Google Scholar] [CrossRef] [PubMed]
- Spies, G.; Kader, K.; Kidd, M.; Smit, J.; Myer, L.; Stein, D.J.; Seedat, S. Validity of the K-10 in Detecting DSM-IV-Defined Depression and Anxiety Disorders among HIV-Infected Individuals. AIDS Care 2009, 21, 1163–1168. [Google Scholar] [CrossRef] [PubMed]
- Stanton, A.M.; Lee, J.S.; Wirtz, M.R.; Andersen, L.S.; Joska, J.; Safren, S.A.; Van Zyl, R.; Conall, S. Tobacco Use and Health-Related Quality of Life Among Individuals with Depression Who Are Receiving Treatment for HIV in Cape Town, South Africa. Int. J. Behav. Med. 2021, 28, 417–430. [Google Scholar] [CrossRef] [PubMed]
- Säll, L.; Salamon, E.; Allgulander, C.; Owe-Larssson, B. Psychiatric Symptoms and Disorders in HIV Infected Mine Workers in South Africa. Afr. J. Psychiatry 2009, 12, 206–212. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Troeman, Z.C.E.; Spies, G.; Cherner, M.; Archibald, S.L.; Fennema-notestine, C.; Theilmann, R.J.; Spottiswoode, B.; Stein, D.J.; Seedat, S. Impact of Childhood Trauma on Functionality and Quality of Life in HIV-Infected Women. Health Qual. Life Outcomes 2011, 9, 84. [Google Scholar] [CrossRef] [PubMed]
- Tshifularo, M.; Govender, L.; Monama, G. Otolaryngological, Head and Neck Manifestations in HIV-Infected Patients Seen at Steve Biko Academic Hospital in Pretoria, South Africa. S. Afr. Med. J. 2013, 103, 464. [Google Scholar] [CrossRef]
- Uys, H. Prevalence and Clinical Presentation of HIV Positive Female Psychiatric Inpatients. Afr. J. Psychiatry 2013, 16, 23–28. [Google Scholar] [CrossRef][Green Version]
- Venter, W.D.F.; Moorhouse, M.; Sokhela, S.; Fairlie, L.; Mashabane, N.; Masenya, M.; Serenata, C.; Akpomiemie, G.; Qavi, A.; Chandiwana, N.; et al. Dolutegravir plus Two Different Prodrugs of Tenofovir to Treat HIV. N. Engl. J. Med. 2019, 381, 803–815. [Google Scholar] [CrossRef]
- Venter, W.D.F.; Sokhela, S.; Simmons, B.; Moorhouse, M.; Fairlie, L.; Mashabane, N.; Serenata, C.; Akpomiemie, G. Dolutegravir with Emtricitabine and Tenofovir Alafenamide or Tenofovir Disoproxil Fumarate versus Efavirenz, Emtricitabine, and Tenofovir Disoproxil Fumarate for Initial Treatment of HIV-1 Infection (ADVANCE): Week 96 Results from a Randomised, Phase 3. Lancet HIV 2020, 7, e666–e676. [Google Scholar] [CrossRef]
- Cichowitz, C.; Maraba, N.; Hamilton, R.; Charalambous, S.; Hoffmann, C.J. Depression and Alcohol Use Disorder at Antiretroviral Therapy Initiation Led to Disengagement from Care in South Africa. PLoS ONE 2017, 12, e0189820. [Google Scholar] [CrossRef]
- Vermaak, J.R.; Dave, J.A.; Levitt, N.; Heckmann, J.M. Sensory Neuropathy and Metabolic Risk Factors in Human Immune Deficiency Virus Infected South Africans Receiving Protease Inhibitors. AIDS Res. Ther. 2015, 12, 30. [Google Scholar] [CrossRef] [PubMed]
- Wadley, A.L.; Cherry, C.L.; Price, P.; Kamerman, P.R. HIV Neuropathy Risk Factors and Symptom Characterization in Stavudine-Exposed South Africans. J. Pain Symptom Manag. 2011, 41, 700–706. [Google Scholar] [CrossRef] [PubMed]
- Wadley, A.L.; Mitchell, D.; Kamerman, P.R. Resilience Does Not Explain the Dissociation between Chronic Pain and Physical Activity in South Africans Living with HIV. PeerJ 2016, 4, e2464. [Google Scholar] [CrossRef] [PubMed]
- Williams, M.E.; Ipser, J.C.; Stein, D.J.; Joska, J.A.; Naudé, P.J.W. The Association of Immune Markers with Cognitive Performance in South African HIV-Positive Patients. J. Neuroimmune Pharmacol. 2019, 14, 679–687. [Google Scholar] [CrossRef]
- Witten, J.A.; Thomas, K.G.F.; Westgarth-taylor, J.; Joska, J.A.; Witten, J.A.; Thomas, K.G.F.; Westgarth-taylor, J.; Witten, J.A.; Thomas, K.G.F.; Westgarth-taylor, J.; et al. Executive Dyscontrol of Learning and Memory: Findings from a Clade C HIV-Positive South African Sample. Clin. Neuropsychol. 2015, 29, 956–984. [Google Scholar] [CrossRef]
- Wong, M.; Myer, L.; Zerbe, A.; Phillips, T.; Petro, G.; Claude, A.; Remien, R.H.; Shiau, S.; Brittain, K.; Abrams, E.J. Depression, Alcohol Use, and Stigma in Younger versus Older HIV-Infected Pregnant Women Initiating Antiretroviral Therapy in Cape Town, South Africa. Arch. Womens Ment. Health 2017, 20, 149–159. [Google Scholar] [CrossRef]
- Yemeke, T.T.; Sikkema, K.J.; Watt, M.H.; Ciya, N.; Robertson, C.; Joska, J.A. Screening for Traumatic Experiences and Mental Health Distress Among Women in HIV Care in Cape Town, South Africa. J. Interpers. Violence 2020, 35, 4842–4862. [Google Scholar] [CrossRef]
- Dos Santos, M.; Wolvaardt, G. Integrated Intervention for Mental Health Co-Morbidity in HIV-Positive Individuals: A Public Health Assessment. Afr. J. AIDS Res. 2016, 15, 325–331. [Google Scholar] [CrossRef]
- Van Coppenhagen, B.; Duvenage, H.S. Prevalence of Depression in People Living with HIV and AIDS at the Kalafong Provincial Tertiary Hospital Antiretroviral Clinic. S. Afr. J. Psychiatry 2019, 25, 1–6. [Google Scholar] [CrossRef]
- Van der Watt, J.J.; Benatar, M.G.; Harrison, T.B.; Carrara, H.; Heckmann, J.M. Isoniazid Exposure and Pyridoxine Levels in Human Immunodeficiency Virus Associated Distal Sensory Neuropathy. Int. J. Tuberc. Lung Dis. 2015, 19, 1312–1319. [Google Scholar] [CrossRef] [PubMed]
- Cobbing, S. A Home-Based Rehabilitation Intervention for Adults Living With HIV: A Randomized Controlled Trial. J. Assoc. Nurses AIDS Care 2017, 28, 105–117. [Google Scholar] [CrossRef] [PubMed]
- van der Westhuizen, Y.; Swanepoel, D.W.; Heinze, B.; Hofmeyr, L.M. Auditory and Otological Manifestations in Adults with HIV/AIDS. Int. J. Audiol. 2013, 52, 37–43. [Google Scholar] [CrossRef] [PubMed]
- Woollett, N.; Cluver, L.; Bandeira, M.; Brahmbhatt, H. Identifying Risks for Mental Health Problems in HIV Positive Adolescents Accessing HIV Treatment in Johannesburg. J. Child Adolesc. Ment. Health 2017, 29, 11–26. [Google Scholar] [CrossRef] [PubMed]
- Chiliza, N.; Du Toit, M.; Wasserman, S. Outcomes of HIV-Associated Pneumocystis Pneumonia at a South African Referral Hospital. PLoS ONE 2018, 13, e0201733. [Google Scholar] [CrossRef] [PubMed]
- Cross, H.M.; Combrinck, M.I.; Joska, J.A. HIV-Associated Neurocognitive Disorders: Antiretroviral Regimen, Central Nervous System Penetration Effectiveness, and Cognitive Outcomes. S. Afr. Med. J. 2013, 103, 758. [Google Scholar] [CrossRef]
- Cullen, C.; Bch, M.B.; Sa, F.; Ophth, M. Case Report: Successful Treatment of Bilateral Visual Loss Caused by Idiopathic Optic Neuritis in an HIV-Infected Patient. S. Afr. J. HIV Med. 2011, 12, 29–32. [Google Scholar] [CrossRef]
- Daniels, A.K.; Van Niekerk, R.L. Van The Impact of a Therapeutic Exercise Intervention on Depression and Body Self-Image in HIV-Positive Women in Sub-Saharan Africa. HIV/AIDS—Res. Palliat. Care 2018, 10, 133–144. [Google Scholar] [CrossRef]
- Desmond, K.; Milburn, N.; Richter, L.; Tomlinson, M.; Greco, E.; van Heerden, A.; van Rooyen, H.; Comulada, W.S.; Rotheram-Borus, M.J. Alcohol Consumption among HIV-Positive Pregnant Women in KwaZulu-Natal, South Africa: Prevalence and Correlates. Drug Alcohol Depend. 2012, 120, 113–118. [Google Scholar] [CrossRef]
- Dolan, R.; Maritz, D.; Wallis, L.; Parak, M. Bilateral Lower Motor Neuron Facial Nerve Palsy Due to HIV Seroconversion. S. Afr. J. HIV Med. 2011, 12, 39–40. [Google Scholar] [CrossRef][Green Version]
- Dreyer, A.J.; Nightingale, S.; Heaps-Woodruff, J.M.; Henry, M.; Gouse, H.; Paul, R.H.; Thomas, K.G.F.; Joska, J.A. Rates of Cognitive Impairment in a South African Cohort of People with HIV: Variation by Definitional Criteria and Lack of Association with Neuroimaging Biomarkers. J. Neurovirol. 2021, 27, 579–594. [Google Scholar] [CrossRef] [PubMed]
- Dudley, M.T.; Borkum, M.; Basera, W.; Wearne, N.; Heckmann, J.M. Journal of the Neurological Sciences Peripheral Neuropathy in HIV Patients on Antiretroviral Therapy: Does It Impact Function ? J. Neurol. Sci. 2019, 406, 116451. [Google Scholar] [CrossRef] [PubMed]
- Berner, K.; Strijdom, H.; Essop, M.; Webster, I.; Morris, L.; Louw, Q. Fall History and Associated Factors among Adults Living with HIV-1 in the Cape Winelands, South Africa: An Exploratory Investigation. Open Forum Infect. Dis. 2019, 6, ofz401. [Google Scholar] [CrossRef]
- Edwards, A.; Siedner, M.J.; Nash, S.; Neuman, M.; Danaviah, S.; Smit, T.; Gareta, D.; Kowal, P.; Seeley, J. HIV Serostatus, Inflammatory Biomarkers and the Frailty Phenotype among Older People in Rural KwaZulu-Natal, South Africa. Afr. J. AIDS Res. 2020, 19, 177–185. [Google Scholar] [CrossRef] [PubMed]
- Freeman, M.; Nkomo, N.; Kafaar, Z.; Kelly, K. Factors Associated with Prevalence of Mental Disorder in People Living with HIV/AIDS in South Africa. AIDS Care 2007, 19, 1201–1209. [Google Scholar] [CrossRef] [PubMed]
- Friend-du Preez, N.; Peltzer, K. HIV Symptoms and Health-Related Quality of Life Prior to Initiation of HAART in a Sample of HIV-Positive South Africans. AIDS Behav. 2010, 14, 1437–1447. [Google Scholar] [CrossRef]
- Ganasen, K.A.; Fincham, D.; Smit, J.; Seedat, S.; Stein, D. Utility of the HIV Dementia Scale (HDS) in Identifying HIV Dementia in a South African Sample. J. Neurol. Sci. 2008, 269, 62–64. [Google Scholar] [CrossRef]
- Goodkin, K.; Hardy, D.J.; Singh, D.; Lopez, E. Diagnostic Utility of the International HIV Dementia Scale for HIV-Associated Neurocognitive Impairment and Disorder in South Africa. J. Neuropsychiatry Clin. Neurosci. 2014, 26, 352–358. [Google Scholar] [CrossRef]
- Gouse, H.; Masson, C.; Henry, M.; Thomas, K.G.F.; Robbins, R.; Kew, G.; London, L.; Joska, J.A.; Marcotte, T.D. The Impact of HIV-Associated Neurocognitive Impairment on Driving Performance in Commercial Truck Drivers. AIDS Behav. 2021, 25, 689–698. [Google Scholar] [CrossRef]
- Haas, A.D.; Kunzekwenyika, C.; Hossmann, S.; Manzero, J.; Van Dijk, J.; Manhibi, R.; Verhey, R.; Limacher, A.; Von Groote, P.M.; Manda, E.; et al. Original Research: Symptoms of Common Mental Disorders and Adherence to Antiretroviral Therapy among Adults Living with HIV in Rural Zimbabwe: A Cross-Sectional Study. BMJ Open 2021, 11, 49824. [Google Scholar] [CrossRef]
- Hakkers, C.S.; Beunders, A.J.M.; Ensing, M.H.M.; Barth, R.E.; Boelema, S.; Devillé, W.L.J.; Tempelman, H.A.; Coutinho, R.A.; Hoepelman, A.I.M.; Arends, J.E.; et al. The Montreal Cognitive Assessment–Basic (MoCA-B) Is Not a Reliable Screening Tool for Cognitive Decline in HIV Patients Receiving Combination Antiretroviral Therapy in Rural South Africa. Int. J. Infect. Dis. 2018, 67, 36–40. [Google Scholar] [CrossRef] [PubMed]
- Hansrod, F.; Spies, G.; Seedat, S. Type and Severity of Intimate Partner Violence and Its Relationship with PTSD in HIV-Infected Women. Psychol. Health Med. 2015, 20, 697. [Google Scholar] [CrossRef]
- Hattingh, Z.; Le Roux, M.; Nel, M.; Walsh, C. Assessment of the Physical Activity, Body Mass Index and Energy Intake of HIV-Uninfected and HIV-Infected Women in Mangaung, Free State Province. S. Afr. Fam. Pract. 2014, 56, 196–200. [Google Scholar] [CrossRef][Green Version]
- Bhigjee, A.I.; Moodley, A.A.; Roos, I.; Wells, C.; Ramdial, P.; Esser, M. The Neuromyelitis Optica Presentation and the Aquaporin-4 Antibody in HIV-Seropositive and Seronegative Patients in KwaZulu-Natal, South Africa. S. Afr. J. HIV Med. 2017, 18, 1–7. [Google Scholar] [CrossRef] [PubMed]
- Heinze, B.M.; Vinck, B.M.; Hofmeyr, L.M.; Swanepoel, D.W. Auris Nasus Larynx Vestibular Involvement in Adults with HIV/AIDS. Auris Nasus Larynx 2014, 41, 160–168. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Hitchcock, S.; Meyer, H.; Gwyther, E. Neuropathic Pain in AIDS Patients Prior to Antiretroviral Therapy. S. Afr. Med. J. 2008, 98, 889–892. [Google Scholar]
- Hoare, J.; Westgarth-taylor, J.; Fouche, J.-P.; Spottiswoode, B.; Paul, R.; Thomas, K.; Stein, D.; Joska, J. A Diffusion Tensor Imaging and Neuropsychological Study of Prospective Memory Impairment in South African HIV Positive Individuals. Metab. Brain Dis. 2012, 27, 289–297. [Google Scholar] [CrossRef]
- Huis in ‘t Veld, D.; Pengpid, S.; Colebunders, R.; Skaal, L.; Peltzer, K. High-Risk Alcohol Use and Associated Socio-Demographic, Health and Psychosocial Factors in Patients with HIV Infection in Three Primary Health Care Clinics in South Africa. Int. J. STD AIDS 2017, 28, 651–659. [Google Scholar] [CrossRef]
- Joska, J.A.; Fincham, D.S.; Stein, D.J.; Paul, R.H.; Seedat, S. Clinical Correlates of HIV-Associated Neurocognitive Disorders in South Africa. AIDS Behav. 2010, 14, 371–378. [Google Scholar] [CrossRef]
- Joska, J.A.; Sa, F.; Westgarth-Taylor, J.; Hoare, J.; Thomas, K.G.F.; Ph, D.; Paul, R.; Ph, D. Validity of the International HIV Dementia Scale in South Africa. AIDS Patient Care STDS 2011, 25, 95–101. [Google Scholar] [CrossRef]
- Joska, J.A.; Westgarth-Taylor, J.; Hoare, J.; Thomas, K.G.F.; Paul, R.; Myer, L.; Stein, D.J. Neuropsychological Outcomes in Adults Commencing Highly Active Anti-Retroviral Treatment in South Africa: A Prospective Study. BMC Infect. Dis. 2012, 12, 39. [Google Scholar] [CrossRef]
- Joska, J.A.; Witten, J.; Thomas, K.G.; Robertson, C.; Casson-Crook, M.; Roosa, H.; Creighton, J.; Lyons, J.; McArthur, J.; Sacktor, N.C. A Comparison of Five Brief Screening Tools for HIV-Associated Neurocognitive Disorders in the USA and South Africa. AIDS Behav. 2016, 20, 1621–1631. [Google Scholar] [CrossRef] [PubMed]
- Joska, J.A.; Dreyer, A.J.; Nightingale, S.; Combrinck, M.I.; De Jager, C.A. Prevalence of HIV-1 Infection in an Elderly Rural Population and Associations with Neurocognitive Impairment. AIDS 2019, 33, 1765–1771. [Google Scholar] [CrossRef] [PubMed]
- Joska, J.A.; Landon, J.W.; Paul, R.H.; Stein, D.J.; Flisher, A.J. Characterization of HIV-Associated Neurocognitive Disorders Among Individuals Starting Antiretroviral Therapy in South Africa. AIDS Behav. 2011, 15, 1197–1203. [Google Scholar] [CrossRef] [PubMed]
- Bongongo, T.; Tumbo, J.; Govender, I. Depressive Features among Adult Patients Receiving Antiretroviral Therapy for HIV in Rustenburg District, SA. S. Afr. J. Psychiatry 2013, 19, 31. [Google Scholar] [CrossRef][Green Version]
- Kader, R.; Govender, R.; Seedat, S.; Koch, J.R.; Parry, C. Understanding the Impact of Hazardous and Harmful Use of Alcohol and/or Other Drugs on ARV Adherence and Disease Progression. PLoS ONE 2015, 10, e0125088. [Google Scholar] [CrossRef] [PubMed]
- Kagee, A.; Martin, L. Symptoms of Depression and Anxiety among a Sample of South African Patients Living with HIV. AIDS Care 2010, 22, 159–165. [Google Scholar] [CrossRef]
- Kagee, A. Psychological Distress among Persons Living with HIV, Hypertension, and Diabetes. AIDS Care 2010, 22, 1517–1521. [Google Scholar] [CrossRef]
- Kaswa, R.; De Villiers, M. Prevalence of Substance Use amongst People Living with Human Immunodeficiency Virus Who Attend Primary Healthcare Services in Mthatha, South Africa. S. Afr. Fam. Pract. 2020, 62, a5042. [Google Scholar] [CrossRef]
- Kekwaletse, C.T.; Morojele, N.K. Alcohol Use, Antiretroviral Therapy Adherence, and Preferences Regarding an Alcohol-Focused Adherence Intervention in Patients with Human Immunodeficiency Virus. Patient Prefer. Adherence 2014, 8, 401–413. [Google Scholar] [CrossRef]
- Khoza-shangase, K. Vestibular Function in a Group of Adults with HIV/AIDS on HAART. Afr. J. Infect. Dis. 2017, 12, 7–14. [Google Scholar] [CrossRef]
- Khoza-Shangase, K. An Analyisis of Auditory Manifestations in a Group of Adults with AIDS Prior to Antiretroviral Therapy. Afr. J. Infect. Dis. 2011, 5, 11–22. [Google Scholar] [PubMed]
- Khoza-Shangase, K.; Jade Van Rie, K. Pathological Vestibular Symptoms Presenting in a Group of Adults with HIV/AIDS in Johannesburg, South Africa. S. Afr. J. Infect. Dis. 2017, 32, 43–53. [Google Scholar] [CrossRef]
- Kietrys, D.; Myezwa, H.; Galantino, M.L.; Parrott, J.S.; Davis, T.; Levin, T.; O’Brien, K.; Hanass-Hancock, J. Functional Limitations and Disability in Persons Living with HIV in South Africa and United States: Similarities and Differences. J. Int. Assoc. Provid. AIDS Care 2019, 18, 232595821985055. [Google Scholar] [CrossRef]
- Kitshoff, C.; Campbell, L.; Naidoo, S. The Association between Depression and Adherence to Antiretroviral Therapy in HIV-Positive Patients, KwaZulu-Natal, South Africa. S. Afr. Fam. Pract. 2012, 54, 145–150. [Google Scholar] [CrossRef]
- Breuer, E.; Stoloff, K.; Myer, L.; Seedat, S.; Stein, D.J.; Joska, J. Reliability of the Lay Adherence Counsellor Administered Substance Abuse and Mental Illness Symptoms Screener (SAMISS) and the International HIV Dementia Scale (IHDS) in a Primary Care HIV Clinic in Cape Town, South Africa. AIDS Behav. 2012, 16, 1464–1471. [Google Scholar] [CrossRef]
- Mahomed, W.; Audiology, M.A.; Heinze, B.; Vinck, B.; Stoltz, A. Faculty of Humanities Audiovestibular Profile of HIV Positive Adults; upSpace: Ottawa, ON, Canada, 2018; p. 1300. [Google Scholar]
- Martin, L.; Fincham, D.; Kagee, A. Screening for HIV-Related PTSD: Sensitivity and Specificity of the 17-Item Posttraumatic Stress Diagnostic Scale (PDS) in Identifying HIV-Related PTSD among a South African Sample. Afr. J. Psychiatry 2009, 12, 270–274. [Google Scholar] [CrossRef]
- Masenyetse, L.J.; Manda, S.O.; Mwambi, H.G. An Assessment of Adverse Drug Reactions among HIV Positive Patients Receiving Antiretroviral Treatment in South Africa. AIDS Res. Ther. 2015, 12, 6. [Google Scholar] [CrossRef] [PubMed]
- Mashinya, F.; Alberts, M.; Van Geertruyden, J.; Colebunders, R. Tobacco Use among ARV Treated HIV Infected Rural South Africans: Prevalence and Its Determinants. Afr. J. Phys. Health Educ. Recreat. Danc. 2015, 21, 768–776. [Google Scholar]
- Mathebula, S.D.; Makunyane, P.S. Loss of Amplitude of Accommodation in Pre-Presbyopic HIV and AIDS Patients under Treatment with Antiretrovirals. Afr. Vis. Eye Health 2017, 76, 1–6. [Google Scholar] [CrossRef]
- Meel, B.L. HIV/AIDS, Psychiatric Disorder and Sexual Assault in Transkei: A Case Report. Med. Sci. Law 2006, 46, 181–183. [Google Scholar] [CrossRef]
- Menezes, C.N.; Maskew, M.; Sanne, I.; Crowther, N.J.; Raal, F.J. A Longitudinal Study of Stavudine-Associated Toxicities in a Large Cohort of South African HIV Infected Subjects. BMC Infect. Dis. 2011, 11, 244. [Google Scholar] [CrossRef] [PubMed]
- Millar, A.; Joubert, K.; Naude, A. Prevalence of Hearing Loss and Tinnitus in a Group of Adults with Human Immunodeficiency Virus. S. Afr. J. Commun. Disord. 2020, 67, 1–7. [Google Scholar] [CrossRef] [PubMed]
- Millar, A.; Joubert, K.; Naude, A. Prevalence of Peripheral Vestibular Impairment in Adults with Human Immunodeficiency Virus. J. Audiol. Otol. 2021, 25, 36–42. [Google Scholar] [CrossRef]
- Mogambery, J.C.; Dawood, H.; Wilson, D.; Moodley, A. HIV-Associated Neurocognitive Disorder in a KwaZulu-Natal HIV Clinic: A Prospective Study. S. Afr. J. HIV Med. 2017, 18, 1–5. [Google Scholar] [CrossRef]
- Breuer, E.; Stoloff, K.; Myer, L.; Seedat, S.; Stein, D.J.; Joska, J.A. The Validity of the Substance Abuse and Mental Illness Symptom Screener (SAMISS) in People Living with HIV/AIDS in Primary HIV Care in Cape Town, South Africa. AIDS Behav. 2014, 18, 1133–1141. [Google Scholar] [CrossRef] [PubMed]
- Mokhele, I.; Nattey, C.; Jinga, N.; Mongwenyana, C.; Fox, M.P.; Onoya, D. Prevalence and Predictors of Postpartum Depression by HIV Status and Timing of HIV Diagnosis in Gauteng, South Africa. PLoS ONE 2019, 14, e0214849. [Google Scholar] [CrossRef]
- Moodley, K.; Bill, P.L.A.; Bhigjee, A.I.; Patel, V.B. A Comparative Study of Motor Neuron Disease in HIV-Infected and HIV- Uninfected Patients. J. Neurol. Sci. 2019, 397, 96–102. [Google Scholar] [CrossRef]
- Morojele, N.K.; Nkosi, S.; Kekwaletswe, C.T.; Shuper, P.A.; Manda, S.O.; Myers, B.; Parry, C.D. Utility of Brief Versions of the Alcohol Use Disorders Identification Test (AUDIT) to Identify Excessive Drinking Among Patients in HIV Care in South Africa. J. Stud. Alcohol Drugs 2017, 78, 88–96. [Google Scholar] [CrossRef] [PubMed]
- Morris, T.; Naidoo, P.; Cloete, K.J.; Harvey, J.; Seedat, S. No Association Between Cumulative Traumatic Experiences and Sex in Risk for Posttraumatic Stress Disorder Among Human Immunodeficiency Virus–Positive Adults. J. Nerv. Ment. Dis. 2013, 201, 504–509. [Google Scholar] [CrossRef]
- Mphahlele, N.R.; Mitchell, D.; Kamerman, P.R. Pain in Ambulatory HIV-Positive South Africans. Eur. J. Pain 2012, 16, 447–458. [Google Scholar] [CrossRef]
- Mupawose, A.; Broom, Y. Assessing Cognitive-Linguistic Abilities in South African Adults Living with HIV: The Cognitive Linguistic Quick Test. Afr. J. AIDS Res. 2010, 9, 147–152. [Google Scholar] [CrossRef]
- Myer, L.; Smit, J.; Le Roux, L.; Parker, S.; Stein, D.J.; Seedat, S. Common Mental Disorders among HIV-Infected Individuals in South Africa: Prevalence, Predictors, and Validation of Brief Psychiatric Rating Scales. AIDS Patient Care STDS 2008, 22, 147–158. [Google Scholar] [CrossRef]
- Myezwa, H.; Stewart, A.; Musenge, E.; Nesara, P. Assessment of HIV-Positive in-Patients Using the International Classification of Functioning, Disability and Health (ICF) at Chris Hani Baragwanath Hospital, Johannesburg. Afr. J. AIDS Res. 2009, 8, 93–105. [Google Scholar] [CrossRef]
- Naidoo, P.; Premdutt, R. Do Challenges Still Exist amongst HIV/AIDS Patients in Managing Their Condition? A Cross-Sectional Study of 297 Participants in the Ethekwini Metro of Kwazulu-Natal, South Africa. Afr. J. AIDS Res. 2019, 18, 198–204. [Google Scholar] [CrossRef] [PubMed]
- Narasimooloo, C.; Naidoo, S.S.; Gaede, B.M. Adequacy of Pain Management in HIV-Positive Patients. S. Afr. Fam. Pract. 2014, 53, 71–76. [Google Scholar] [CrossRef]
- Brittain, K.; Mellins, C.A.; Phillips, T.; Zerbe, A.; Abrams, E.J.; Myer, L.; Remien, R.H. Social Support, Stigma and Antenatal Depression Among HIV-Infected Pregnant Women in South Africa. AIDS Behav. 2017, 21, 274–282. [Google Scholar] [CrossRef] [PubMed]
- Narsi, K.; Tomita, A.; Ramlall, S. Neuropsychological Functioning and Cognitive Reserve in Newly HIV Diagnosed Antiretroviralnaïve South African Adults from Peri-Urban and Informal Settlements. PLoS ONE 2021, 16, e0260260. [Google Scholar] [CrossRef] [PubMed]
- Nel, A.; Kagee, A. The Relationship between Depression, Anxiety and Medication Adherence among Patients Receiving Antiretroviral Treatment in South Africa. AIDS Care 2013, 25, 948–955. [Google Scholar] [CrossRef]
- Nöthling, J.; Martin, C.L.; Laughton, B.; Cotton, M.F.; Seedat, S. Maternal Post-Traumatic Stress Disorder, Depression and Alcohol Dependence and Child Behaviour Outcomes in Mother–Child Dyads Infected with HIV: A Longitudinal Study. BMJ Open 2013, 3, e003638. [Google Scholar] [CrossRef] [PubMed]
- Olley, B.O. Psychological Distress in the First Year after Diagnosis of HIV Infection among Women in South Africa. Afr. J. AIDS Res. 2006, 5, 207–215. [Google Scholar] [CrossRef] [PubMed]
- Olley, B.O.; Seedat, S.; Stein, D.J. Persistence of Psychiatric Disorders in a Cohort of HIV/AIDS Patients in South Africa: A 6-Month Follow-up Study. J. Psychosom. Res. 2006, 61, 479–484. [Google Scholar] [CrossRef] [PubMed]
- Pappin, M.; Wouters, E.; Booysen, F.L.R. Anxiety and Depression amongst Patients Enrolled in a Public Sector Antiretroviral Treatment Programme in South Africa: A Cross-Sectional Study. BMC Public Health 2012, 12, 244. [Google Scholar] [CrossRef]
- Parker, R.; Jelsma, J.; Stein, D.J. Pain in AmaXhosa Women Living With HIV/AIDS: Translation and Validation of the Brief Pain Inventory e Xhosa. J. Pain Symptom Manag. 2016, 51, 126–132.e2. [Google Scholar] [CrossRef] [PubMed]
- Parker, R.; Jelsma, J.; Stein, D.J. Pain in AmaXhosa Women Living with HIV/AIDS: A Cross-Sectional Study of Ambulant Outpatients. BMC Women’s Health 2017, 17, 31. [Google Scholar] [CrossRef]
- Pathai, S.; Lawn, S.D.; Weiss, H.A.; Cook, C.; Sa, F.; Bekker, L.; Gilbert, C.E. Increased Ocular Lens Density in HIV-Infected Individuals With Low Nadir CD4 Counts in South Africa: Evidence of Accelerated Aging. JAIDS J. Acquir. Immune Defic. Syndr. 2013, 63, 307–314. [Google Scholar] [PubMed]
- Pathai, S.; Lawn, S.D.; Weiss, H.A.; Cook, C.; Bekker, L.; Gilbert, C.E. Retinal Nerve Fibre Layer Thickness and Contrast Sensitivity in HIV-Infected Individuals in South Africa: A Case-Control Study. PLoS ONE 2013, 8, e73694. [Google Scholar] [CrossRef] [PubMed]
- Cassimjee, N.; Motswai, P.K. Neuropsychological Profiles of Adults and Older Adults with HIV. S. Afr. J. Psychol. 2017, 47, 35–45. [Google Scholar] [CrossRef]
- Pathai, S.; Gilbert, C.; Weiss, H.A.; Cook, C.; Wood, R.; Bekker, L.; Lawn, S.D. Frailty in HIV-Infected Adults in South Africa. JAIDS J. Acquir. Immune Defic. Syndr. 2013, 62, 43–51. [Google Scholar] [CrossRef]
- Peltzer, K.; Szrek, H.; Ramlagan, S.; Leite, R.; Chao, L.-W. Depression and Social Functioning among HIV-Infected and Uninfected Persons in South Africa. AIDS Care 2015, 27, 41–46. [Google Scholar] [CrossRef]
- Peltzer, K.; Rodriguez, V.J.; Jones, D. Prevalence of Prenatal Depression and Associated Factors among HIV-Positive Women in Primary Care in Mpumalanga Province, South Africa. SAHARA-J J. Soc. Asp. HIV/AIDS 2016, 13, 60–67. [Google Scholar] [CrossRef]
- Peltzer, K. HIV-Related Symptoms and Management in HIV and Antiretroviral Therapy Patients in KwaZulu-Natal, South Africa: A Longitudinal Study. J. Soc. Asp. HIV/AIDS 2013, 10, 96–104. [Google Scholar] [CrossRef] [PubMed]
- Peltzer, K.; Phaswana-Mafuya, N.; Petros, G. Hazardous Alcohol Use among Persons Living with Human Immunodeficiency Virus Infection in the Eastern Cape, South Africa. J. Psychol. Afr. 2009, 19, 247–251. [Google Scholar] [CrossRef]
- Pengpid, S.; Peltzer, K. Mental Morbidity and Its Associations with Socio-Behavioural Factors and Chronic Conditions in Rural Middle- and Older-Aged Adults in South Africa. J. Psychol. Afr. 2020, 30, 257–263. [Google Scholar] [CrossRef]
- Pienaar, M.; Van Rooyen, F.C.; Walsh, C.M. Reported Health, Lifestyle and Clinical Manifestations Associated with HIV Status in People from Rural and Urban Communities in the Free State Province, South Africa. S. Afr. J. HIV Med. 2017, 18, a465. [Google Scholar] [CrossRef]
- Pillay, P.; Wadley, A.L.; Cherry, C.L.; Karstaedt, A.S.; Kamerman, P.R.; Cherry, C.L. Psychological Factors Associated With Painful Versus Non-Painful HIV-Associated Sensory Neuropathy. AIDS Behav. 2018, 22, 1584–1595. [Google Scholar] [CrossRef]
- Pinillos, F.; Dandara, C.; Swart, M.; Strehlau, R.; Kuhn, L.; Patel, F.; Coovadia, A.; Abrams, E. Case Report: Severe Central Nervous System Manifestations Associated with Aberrant Efavirenz Metabolism in Children: The Role of CYP2B6 Genetic Variation. BMC Infect. Dis. 2016, 16, 56. [Google Scholar] [CrossRef]
- Ramirez-Avila, L.; Regan, S.; Giddy, J.; Chetty, S.; Ross, D.; Katz, J.N.; Freedberg, K.A.; Walensky, R.P.; Losina, E.; Bassett, I.V. Depressive Symptoms and Their Impact on Health-Seeking Behaviors in Newly-Diagnosed HIV-Infected Patients in Durban, South Africa. AIDS Behav. 2012, 16, 2226–2235. [Google Scholar] [CrossRef]
- Chetty, S.; Naidu, K. Clinical Presentation of HIV-Infected Patients in a Psychiatric Hospital in South Africa. Afr. J. Infect. Dis. 2018, 12, 29–36. [Google Scholar] [CrossRef]
- Rane, M.S.; Hong, T.; Govere, S.; Thulare, H.; Moosa, M.; Celum, C.; Drain, P.K. Depression and Anxiety as Risk Factors for Delayed Care-Seeking Behavior in Human Immunodeficiency Virus–Infected Individuals in South Africa. Clin. Infect. Dis. 2018, 67, 1411–1418. [Google Scholar] [CrossRef] [PubMed]
- Robbins, R.N.; Remien, R.H.; Mellins, C.A.; Joska, J.A.; Stein, D.J. Screening for HIV-Associated Dementia in South Africa: Potentials and Pitfalls of Task-Shifting. AIDS Patient Care STDS 2011, 25, 587–593. [Google Scholar] [CrossRef] [PubMed]
- Robbins, R.N.; Joska, J.A.; Thomas, K.G.F.; Stein, D.J.; Linda, T.; Mellins, C.A.; Remien, R.H. Exploring the Utility of the Montreal Cognitive Assessment to Detect HIV-Associated Neurocognitive Disorder: The Challenge and Need for Culturally Valid Screening Tests in South Africa. Clin. Neuropsychol. 2013, 27, 437–454. [Google Scholar] [CrossRef] [PubMed]
- Robbins, R.N.; Gouse, H.; Brown, H.G.; Ehlers, A.; Leu, C.; Remien, R.H.; Mellins, C.A.; Joska, J.A. A Mobile App to Screen for Neurocognitive Impairment: Preliminary Validation of NeuroScreen Among HIV-Infected South African Adults. JMIR Mhealth Uhealth 2018, 6, e5. [Google Scholar] [CrossRef] [PubMed]
- Roos, R.; Myezwa, H.; Van Aswegen, H.; Musenge, E. Effects of an Education and Home-Based Pedometer Walking Program on Ischemic Heart Disease Risk Factors in People Infected with HIV: A Randomized Trial. J. Acquir. Immune Defic. Syndr. 2014, 67, 268–276. [Google Scholar] [CrossRef] [PubMed]
- Roos, R.; Myezwa, H.; Van Aswegen, H. Factors Associated with Physical Function Capacity in an Urban Cohort of People Living with the Human Immunodeficiency Virus in South Africa. S. Afr. J. Physiother. 2019, 75, 1–7. [Google Scholar] [CrossRef] [PubMed]
- Schlebusch, L.; Vawda, N. HIV-Infection as a Self-Reported Risk Factor for Attempted Suicide in South Africa. Afr. J. Psychiatry 2010, 13, 280–283. [Google Scholar] [CrossRef]
- Schutte, C.; Ranchhod, N.; Kakaza, M.; Pillay, M. AIDS-Related Progressive Multifocal Leukoencephalopathy (PML): A Retrospective Study from Pretoria, South Africa. S. Afr. Med. J. 2013, 103, 399. [Google Scholar] [CrossRef] [PubMed]
- Sebothoma, B.; Khoza-Shangase, K. Investigation of the Interaction between Hearing Function and Comorbidities in Adults Living with Human Immunodeficiency Virus. Int. J. Environ. Res. Public Health 2021, 18, 12177. [Google Scholar] [CrossRef]
- Shearer, K.; Evans, D.; Xhosa, B.; Hirasen, K.; Bracken, C.; Mahomed, K.; Long, L.; Fox, M.P. Low Prevalence of Depressive Symptoms among Stable Patients on Antiretroviral Therapy in Johannesburg, South Africa. PLoS ONE 2018, 13, e0203797. [Google Scholar] [CrossRef]
- Auld, S.C.; Kornfeld, H.; Maenetje, P.; Mlotshwa, M.; Chase, W.; Vangu, T.; Torigian, D.A.; Wallis, R.S.; Churchyard, G.; Bisson, G.P. Pulmonary Restriction Predicts Long— Term Pulmonary Impairment in People with HIV and Tuberculosis. BMC Pulm. Med. 2021, 21, 19. [Google Scholar] [CrossRef]
- Candy, S.; Chang, G.; Andronikou, S. Acute Myelopathy or Cauda Equina Syndrome in HIV-Positive Adults in a Tuberculosis Endemic Setting: MRI, Clinical, and Pathologic Findings. Am. J. Neuroradiol. 2014, 35, 1634–1641. [Google Scholar] [CrossRef]
- Gounden, S.; Perumal, R.; Magula, N. Extrapulmonary Tuberculosis in the Setting of HIV Hyperendemicity at a Tertiary Hospital in Durban, South Africa. South. Afr. J. Infect. Dis. 2018, 33, 57–64. [Google Scholar] [CrossRef]
- Khan, M.; Pillay, T.; Moodley, J.; Ramjee, A.; Padayatchi, N. Pregnancies Complicated by Multidrug-Resistant Tuberculosis and HIV Co-Infection in Durban, South Africa. Int. J. Tuberc. Lung Dis. 2007, 11, 706–708. [Google Scholar]
- Marais, S.; Roos, I.; Mitha, A.; Patel, V.; Bhigjee, A.I. Posttubercular Syringomyelia in HIV-Infected Patients: A Report of 10 Cases and Literature Review. J. Neurol. Sci. 2018, 395, 54–61. [Google Scholar] [CrossRef] [PubMed]
- Mntonintshi, M.; O’Mahony, D.; Mabunda, S.; Namugenyi, K.A.F. Undiagnosed Tuberculosis in Patients with HIV Infection Who Present with Severe Anaemia at a District Hospital. Afr. J. Prim. Health Care Fam. Med. 2017, 9, 1–6. [Google Scholar] [CrossRef][Green Version]
- Makapi, N.; Morare, T.; Rose, D.M.; Appels, O. Oesophageal Tuberculosis with Concomitant Candidiasis: A Rare Cause of Dysphagia. BMJ Case Rep. 2019, 12, e231435. [Google Scholar] [CrossRef]
- Ramlall, S.; Lessells, R.J.; Naidu, T.; Sandra Mthembu, S.; Padayatchi, N.; Burns, J.K.; Tomita, A. Neurocognitive Functioning in MDR-TB Patients with and without HIV in KwaZulu-Natal, South Africa. Trop. Med. Int. Health 2020, 25, 919–927. [Google Scholar] [CrossRef]
- Stek, C.; Allwood, B.; Du Bruyn, E.; Buyze, J.; Schutz, C.; Thienemann, F.; Lombard, A.; Wilkinson, R.J.; Meintjes, G.; Lynen, L. The Effect of HIV-Associated Tuberculosis, Tuberculosis-IRIS and Prednisone on Lung Function. Eur. Respir. J. 2020, 55, 1901692. [Google Scholar] [CrossRef]
- Wilson, D.; Ch, B.; Hurtado, R.M.; Digumarthy, S. Case 18-2009: A 24-Year-Old Woman with AIDS and Tuberculosis with Progressive Cough, Dyspnea, and Wasting. N. Engl. J. Med. 2009, 360, 2456–2464. [Google Scholar] [CrossRef] [PubMed]
- Patel, N.; Naidoo, P.; Mosiane, P.; Jann-Kruger, C. HIV/AIDS-Associated Kaposi’s Sarcoma of the Gastrointestinal Tract: A Pictorial Spectrum. S. Afr. Med. J. 2016, 106, 986. [Google Scholar] [CrossRef]
- Sebitloane, H.; Moodley, J. Disseminated AIDS-Associated Kaposi’s Sarcoma in Pregnancy. SAMJ 2006, 96, 602–603. [Google Scholar]
- Loyse, A.; Moodley, A.; Rich, P.; Molloy, S.F.; Bicanic, T.; Bishop, L.; Rae, W.I.D.; Bhigjee, A.I.; Loubser, N.D.; Michowicz, A.J.; et al. Neurological, Visual, and MRI Brain Scan Findings in 87 South African Patients with HIV-Associated Cryptococcal. J. Infect. 2015, 70, 668–675. [Google Scholar] [CrossRef]
- Allwood, B.W.; Stolbrink, M.; Baines, N.; Louw, E.; Wademan, D.T.; Lupton-Smith, A.; Nel, S.; Maree, D.; Mpagama, S.; Osman, M.; et al. Persistent Chronic Respiratory Symptoms despite TB Cure Is Poorly Correlated with Lung Function. Int. J. Tuberc. Lung Dis. 2021, 25, 262. [Google Scholar] [CrossRef]
- Peltzer, K.; Louw, J. Prevalence of Suicidal Behaviour & Associated Factors among Tuberculosis Patients in Public Primary Care in South Africa. Indian J. Med. Res. 2013, 138, 194–200. [Google Scholar] [PubMed]
- Peltzer, K.; Naidoo, P.; Matseke, G.; Louw, J.; Mchunu, G.; Tutshana, B. Prevalence of Post-Traumatic Stress Symptoms and Associated Factors in Tuberculosis (TB), TB Retreatment and/or TB–HIV Co-Infected Primary Public Health-Care Patients in Three Districts in South Africa. Psychol. Health Med. 2013, 18, 387–397. [Google Scholar] [CrossRef] [PubMed]
- Wessels, J.; Walsh, C.M.; Nel, M. Smoking Habits and Alcohol Use of Patients with Tuberculosis at Standerton Tuberculosis Specialised Hospital, Mpumalanga, South Africa. Health SA Gesondheid 2019, 24, a1146. [Google Scholar] [CrossRef] [PubMed]
- Zarrabi, A.D.; Heyns, C.F. Clinical Features of Confirmed Versus Suspected Urogenital Tuberculosis in Region With Extremely High Prevalence of Pulmonary Tuberculosis. Urology 2009, 74, 41–45. [Google Scholar] [CrossRef]
- Van Aswegen, H.; Roos, R.; McCree, M.; Quinn, S.; Mer, M. Investigation of Physical and Functional Impairments Experienced by People with Active Tuberculosis Infection: A Feasibility Pilot Study. Afr. J. Disabil. 2019, 8, a515. [Google Scholar] [CrossRef]
- Balkema, C.A.; Irusen, E.M.; Taljaard, J.J.; Koegelenberg, C.F.N. Tuberculosis in the Intensive Care Unit: A Prospective Observational Study. Int. J. Tuberc. Lung Dis. 2014, 18, 824–830. [Google Scholar] [CrossRef]
- Khoza-shangase, K. Hearing Function of Gold Miners with and without a History of Tuberculosis Treatment: A Retrospective Data Review. Braz. J. Otorhinolaryngol. 2020, 86, 294–299. [Google Scholar] [CrossRef]
- Louwagie, G.; Kanaan, M.; Morojele, N.K.; Van Zyl, A.; Moriarty, A.S.; Li, J.; Siddiqi, K.; Turner, A.; Mdege, N.D.; Omole, O.B.; et al. Effect of a Brief Motivational Interview and Text Message Intervention Targeting Tobacco Smoking, Alcohol Use and Medication Adherence to Improve Tuberculosis Treatment Outcomes in Adult Patients with Tuberculosis: A Multicentre, Randomised Controlled Tri. BMJ Open 2022, 12, e056496. [Google Scholar] [CrossRef]
- Myers, B.; Carney, T.; Rooney, J.; Malatesta, S.; White, L.F.; Parry, C.D.H.; Bouton, T.C.; Ragan, E.J.; Horsburgh, C.R.; Warren, R.M.; et al. Alcohol and Tobacco Use in a Tuberculosis Treatment Cohort during South Africa’s COVID-19 Sales Bans: A Case Series. Int. J. Environ. Res. Public Health 2021, 18, 5449. [Google Scholar] [CrossRef] [PubMed]
- Peltzer, K.; Naidoo, P.; Matseke, G.; Louw, J.; Mchunu, G.; Tutshana, B. Prevalence of Psychological Distress and Associated Factors in Tuberculosis Patients in Public Primary Care Clinics in South Africa. BMC Psychiatry 2012, 12, 89. [Google Scholar] [CrossRef]
- Peltzer, K. Longitudinal Analysis of HIV Risk Behaviour Patterns and Their Predictors among Public Primary Care Patients with Tuberculosis in South Africa. SAHARA-J J. Soc. Asp. HIV/AIDS 2018, 15, 1–6. [Google Scholar] [CrossRef] [PubMed]
- Peltzer, K.; Louw, J.; Mchunu, G.; Naidoo, P.; Matseke, G.; Tutshana, B. Hazardous and Harmful Alcohol Use and Associated Factors in Tuberculosis Public Primary Care Patients in South Africa. Int. J. Environ. Res. Public Health 2012, 9, 3245–3257. [Google Scholar] [CrossRef]
- Peltzer, K.; Naidoo, P.; Louw, J.; Matseke, G.; Zuma, K.; Mchunu, G.; Tutshana, B.; Mabaso, M. Screening and Brief Interventions for Hazardous and Harmful Alcohol Use among Patients with Active Tuberculosis Attending Primary Public Care Clinics in South Africa: Results from a Cluster Randomized Controlled Trial. BMC Public Health 2013, 13, 1. [Google Scholar] [CrossRef] [PubMed]
- Appana, D.; Joseph, L.; Paken, J. An Audiological Profile of Patients Infected with Multi-Drug Resistant Tuberculosis at a District Hospital in KwaZulu-Natal. S. Afr. J. Commun. Disord. 2016, 63, 1–12. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Conradie, F.; Mabiletsa, T.; Sefoka, M.; Mabaso, S.; Louw, R.; Evans, D.; Van Rie, A. Prevalence and Incidence of Symmetrical Symptomatic Peripheral Neuropathy in Patients with Multidrug-Resistant TB. S. Afr. Med. J. 2013, 104, 24. [Google Scholar] [CrossRef]
- Harris, T.; Bardien, S.; Schaaf, H.S.; Petersen, L.; De Jong, G.; Fagan, J.J. Aminoglycoside-Induced Hearing Loss in HIV-Positive and HIV-Negative Multidrug-Resistant Tuberculosis Patients. S. Afr. Med. J. 2012, 102, 363. [Google Scholar] [CrossRef]
- Hong, H.; Dowdy, D.W.; Dooley, K.E.; Francis, H.W.; Budhathoki, C.; Han, H.; Farley, J.E. Aminoglycoside-Induced Hearing Loss Among Patients Being Treated for Drug-Resistant Tuberculosis in South Africa: A Prediction Model. Clin. Infect. Dis. 2020, 70, 917–924. [Google Scholar] [CrossRef]
- Hong, H.; Dowdy, D.W.; Dooley, K.E.; Francis, H.W.; Budhathoki, C.; Han, H.-R.; Farley, J.E. Prevalence of Pre-Existing Hearing Loss Among Patients With Drug-Resistant Tuberculosis in South Africa. Am. J. Audiol. 2020, 29, 199–205. [Google Scholar] [CrossRef]
- Jacobs, T.Q.; Lecturer, A.R. Adverse Effects Profile of Multidrug-Resistant Tuberculosis Treatment in a South African Outpatient Clinic Adverse Effects Profile of Multidrug-Resistant Tuberculosis Treatment in a South African Outpatient Clinic. S. Afr. Fam. Pract. 2012, 54, 531–539. [Google Scholar] [CrossRef]
- Khoza-shangase, K.; Prodromos, M. Impact of Drug-Resistant Tuberculosis Treatment on Hearing Function in South African Adults: Bedaquiline versus Kanamycin. Afr. J. Commun. Disord. 2021, 68, a784. [Google Scholar] [CrossRef] [PubMed]
- Padayatchi, N.; Daftary, A.; Moodley, T.; Madansein, R.; Ramjee, A. Case Series of the Long-Term Psychosocial Impact of Drug- Resistant Tuberculosis in HIV-Negative Medical Doctors. Int. J. Tuberc. Lung Dis. 2010, 14, 960–966. [Google Scholar] [PubMed]
- Ramma, L.; Ibekwe, T.S. Cochleo-Vestibular Clinical Findings among Drug Resistant Tuberculosis Patients on Therapy-a Pilot Study. Int. Arch. Med. 2012, 5, 3. [Google Scholar] [CrossRef] [PubMed]
- Tomita, A.; Ramlall, S.; Naidu, T.; Mthembu, S.S.; Padayatchi, N.; Burns, J.K. Neurocognitive Impairment Risk Among Individuals With Multiple Drug–Resistant Tuberculosis and Human Immunodeficiency Virus Coinfection. J. Nerv. Ment. Dis. 2019, 207, 307–310. [Google Scholar] [CrossRef]
- Daniels, K.J.; Irusen, E.; Pharoah, H.; Hanekom, S. Post-Tuberculosis Health-Related Quality of Life, Lung Function and Exercise Capacity in a Cured Pulmonary Tuberculosis Population in the Breede Valley District, South Africa. S. Afr. J. Physiother. 2019, 75, a1319. [Google Scholar] [CrossRef]
- Ehrlich, R.I.; Adams, S.; Baatjies, R.; Jeebhay, M.F. Chronic Airfl Ow Obstruction and Respiratory Symptoms Following Tuberculosis: A Review of South African Studies. Int. J. Tuberc. Lung Dis. 2011, 15, 886–891. [Google Scholar] [CrossRef]
- Louw, J.S.; Mabaso, M.; Peltzer, K. Change in Health-Related Quality of Life among Pulmonary Tuberculosis Patients at Primary Health Care Settings in South Africa: A Prospective Cohort Study. PLoS ONE 2016, 11, e0151892. [Google Scholar] [CrossRef]
- Dunn, R.; Zondagh, I.; Candy, S. Spinal Tuberculosis. Magnetic Resonance Imaging and Neurological Impairment. Spine 2011, 36, 469–473. [Google Scholar] [CrossRef]
- Dunn, R.; Van Der Horst, A.; Lippross, S. Tuberculosis of the Spine—Prospective Neurological and Patient Reported Outcome Study. Clin. Neurol. Neurosurg. 2015, 133, 96–101. [Google Scholar] [CrossRef]
- Marais, S.; Roos, I.; Mitha, A.; Mabusha, S.J.; Patel, V.; Bhigjee, A.I. Spinal Tuberculosis: Clinicoradiological Findings in 274 Patients. Clin. Infect. Dis. 2018, 67, 89–98. [Google Scholar] [CrossRef]
- Marais, S.; Roos, I.; Mitha, A.; Patel, V.; Kalincik, T.; Bhigjee, A.I. Presentation and Outcome of Patients with Intracranial Tuberculoma in a High HIV Prevalence Setting. Int. J. Tuberc. Lung Dis. 2020, 24, 224–232. [Google Scholar] [CrossRef]
- Wait, J.W.; Schoeman, J.F. Behaviour Profiles After Tuberculous Meningitis. J. Trop. Pediatr. 2010, 56, 166–171. [Google Scholar] [CrossRef]
- Arowoiya, A.I.; Elloker, T.; Karachi, F.; Mlenzana, N.; Jacobs-Nzuzi Khuabi, L.-A.; Rhoda, A. Using the World Health Organization’s Disability Assessment Schedule (2) to Assess Disability in Community-Dwelling Stroke Patients. S. Afr. J. Physiother. 2017, 73, 1–7. [Google Scholar] [CrossRef]
- Knox, M.; Stewart, A.; Richards, C.L. Six Hours of Task-Oriented Training Optimizes Walking Competency Post Stroke: A Randomized Controlled Trial in the Public Health-Care System of South Africa. Clin. Rehabil. 2018, 32, 1057–1068. [Google Scholar] [CrossRef]
- Mamabolo, V.; Mudzi, W.; Stewart, A.; Olorunju, S.; Singh, A. A Study to Determine Post Discharge Functional Improvements in Patients with Stroke. S. Afr. J. Occup. Ther. 2009, 39, 15–18. [Google Scholar]
- Ntsiea, M.V.; Van Aswegen, H.; Lord, S.; Olorunju, S.S. The Effect of a Workplace Intervention Programme on Return to Work after Stroke: A Randomised Controlled Trial. Clin. Rehabil. 2015, 29, 663–673. [Google Scholar] [CrossRef]
- Ostrofsky, C.; Seedat, J. The South African Dysphagia Screening Tool (SADS): A Screening Tool for a Developing Context. S. Afr. J. Commun. Disord. 2016, 63, 1–9. [Google Scholar] [CrossRef]
- Penn, C.; Barber, N.; Fridjhon, P. Early Recovery Profiles of Language and Executive Functions after Left Hemisphere Stroke in Bilingualism. Aphasiology 2016, 31, 741–764. [Google Scholar] [CrossRef]
- Puckree, T.; Naidoo, P. Balance and Stability—Focused Exercise Program Improves Stability and Balance in Patients After Acute Stroke in a Resource-Poor Setting. PM&R 2014, 6, 1081–1087. [Google Scholar] [CrossRef]
- Rhoda, A.; Mpofu, R.; De Weerdt, W. Activity Limitations of Patients with Stroke Attending Out-Patient Facilities in the Western Cape, South Africa. S. Afr. J. Physiother. 2011, 67, 16–22. [Google Scholar] [CrossRef]
- Rhoda, A.; Smith, M.; Putman, K.; Mpofu, R.; DeWeerdt, W.; DeWit, L. Motor and Functional Recovery after Stroke: A Comparison between Rehabilitation Settings in a Developed versus a Developing Country. BMC Health Serv. Res. 2014, 14, 82. [Google Scholar] [CrossRef]
- Scheffler, E.; Mash, R. Surviving a Stroke in South Africa: Outcomes of Home-Based Care in a Low-Resource Rural Setting. Top. Stroke Rehabil. 2019, 26, 423–434. [Google Scholar] [CrossRef]
- Titus, A.W.; Hillier, S.; Louw, Q.A.; Inglis-Jassiem, G. An Analysis of Trunk Kinematics and Gait Parameters in People with Stroke. Afr. J. Disabil. 2018, 7, 1–6. [Google Scholar] [CrossRef]
- Blackwell, Z.; Littlejohns, P. A Review of the Management of Dysphagia: A South African Perspective. J. Neurosci. Nurs. 2010, 42, 61–70. [Google Scholar] [CrossRef]
- Wasserman, S.; de Villiers, L.; Bryer, A. Community-based care of stroke patients in a rural African setting. S. Afr. Med. J. 2009, 99, 579–583. [Google Scholar] [PubMed]
- De Villiers, L.; Badri, M.; Ferreira, M.; Bryer, A. Stroke Outcomes in a Socio-Economically Disadvantaged Urban Community. S. Afr. Med. J. 2011, 101, 345–348. [Google Scholar] [CrossRef]
- Van Wyk, A.; Eksteen, C.A.; Rheeder, P. The Effect of Visual Scanning Exercises Integrated Into Physiotherapy in Patients With Unilateral Spatial Neglect Poststroke. Neurorehabil. Neural Repair 2014, 28, 856–873. [Google Scholar] [CrossRef]
- Van Zyl, M.; Pillay, B.; Kritzinger, A.; Lekganyane, M.; Kritzinger, A. Significance of Speech Production Errors on Cross- Linguistic Processing in Sepedi-English Individuals with Bilingual Aphasia: A Case Series Analysis. Top. Stroke Rehabil. 2019, 26, 294–306. [Google Scholar] [CrossRef] [PubMed]
- Comley-White, N.; Mudzi, W.; Musenge, E. Effects of Shoulder Strapping in Patients with Stroke: A Randomised Control Trial. S. Afr. J. Physiother. 2018, 74, 1–11. [Google Scholar] [CrossRef]
- Duff, N.; Ntsiea, M.V.; Mudzi, W. Factors That Influence Return to Work after Stroke. Occup. Health South. Africa 2014, 20, 6–12. [Google Scholar]
- Hartley, T.; Burger, M.; Esterhuizen, T.M.; Inglis-Jassiem, G. Functional Outcome of Stroke Inpatients According to Human Immunodeficiency Virus Status: A Feasibility Study. Afr. J. Disabil. 2020, 9, 1–9. [Google Scholar] [CrossRef] [PubMed]
- Hartley, T.; Burger, M.; Inglis-Jassiem, G. Post Stroke Health-Related Quality of Life, Stroke Severity and Function: A Longitudinal Cohort Study. Afr. J. Disabil. 2022, 11, 1–10. [Google Scholar] [CrossRef] [PubMed]
- Joseph, C.; Rhoda, A. Activity Limitations and Factors Influencing Functional Outcome of Patients with Stroke Following Rehabilitation at a Specialised Facility in the Western Cape. Afr. Health Sci. 2013, 13, 646–654. [Google Scholar] [CrossRef]
- Joseph, C.; Rhoda, A.; Conradsson, D.M. Levels and Patterns of Physical Activity in Stroke Survivors with Different Ambulation Status Living in Low-Income Areas of Cape Town, South Africa. Top. Stroke Rehabil. 2020, 27, 494–502. [Google Scholar] [CrossRef]
- Khalema, D.; Goldstein, L.N.; Lucas, S. A Retrospective Analysis of Time Delays in Patients Presenting with Stroke to an Academic Emergency Department. S. Afr. J. Radiol. 2018, 22, 1–6. [Google Scholar] [CrossRef] [PubMed]
- Bongongo, T. An Assessment of Erectile Dysfunction among Male Diabetics Attending Temba Community Health Centre, Pretoria. S. Afr. Fam. Pract. 2019, 61, 229–233. [Google Scholar] [CrossRef]
- Cairncross, J.P.; Steinberg, W.J.; Labuschagne, M.J. Prevalence of Eye Pathology in a Group of Diabetic Patients at National District Hospital Outpatient Department in Bloemfontein, South Africa. Afr. J. Prim. Health Care Fam. Med. 2017, 9, 1–7. [Google Scholar] [CrossRef]
- Hlayisi, V.; Petersen, L.; Ramma, L. High Prevalence of Disabling Hearing Loss in Young to Middle-Aged Adults with Diabetes. Int. J. Diabetes Dev. Ctries. 2019, 39, 148–153. [Google Scholar] [CrossRef]
- Kemp, T.; Rheeder, P. The Prevalence and Associations of Erectile Dysfunction in a South African Male Diabetic Urban Population. J. Endocrinol. Metab. Diabetes S. Afr. 2015, 20, 134–139. [Google Scholar] [CrossRef]
- Mabaso, R.G.; Oduntan, O.A. Risk Factors for Visual Impairment and Blindness amongst Black Adult Diabetics Receiving Treatment at Government Healthcare Facilities in Mopani District, Limpopo Province, South Africa. Afr. J. Prim. Health Care Fam. Med. 2014, 6, 1–8. [Google Scholar] [CrossRef]
- Shukla, A.; Kumar, K.; Singh, A. Association between Obesity and Selected Morbidities: A Study of BRICS Countries. PLoS ONE 2014, 9, e94433. [Google Scholar] [CrossRef]
- Webb, E.M.; Rheeder, P.; Roux, P. Screening in Primary Care for Diabetic Retinopathy, Maculopathy and Visual Loss in South Africa. Ophthalmologica 2016, 235, 141–149. [Google Scholar] [CrossRef]
- Van Vuuren, J.J.; Pillay, S. Major Depressive Disorder in Patients with Diabetes Mellitus in Pietermaritzburg, South Africa. S. Afr. Med. J. 2019, 109, 58–61. [Google Scholar] [CrossRef]
- Mendenhall, E.; Norris, S.A. When HIV Is Ordinary and Diabetes New: Remaking Suffering in a South African Township. Glob. Public Health 2015, 10, 449–462. [Google Scholar] [CrossRef]
- Pillay, S.; Aldous, C.; Mahomed, F. Diabetic Patients Served at a Regional Level Hospital: What Is Their Clinical Picture? J. Endocrinol. Metab. Diabetes S. Afr. 2015, 20, 50–56. [Google Scholar] [CrossRef][Green Version]
- Pillay, S.; Naidoo, K.H.; Msimang, K. The Spectrum of Hearing Abnormalities in Patients Living with Diabetes Mellitus. S. Afr. Med. J. 2021, 111, 1006–1017. [Google Scholar] [CrossRef]
- Ramkisson, S.; Pillay, B.J.; Sartorius, B. Anxiety, Depression and Psychological Well-Being in a Cohort of South African Adults with Type 2 Diabetes Mellitus. S. Afr. J. Psychiatry 2016, 22, 1–9. [Google Scholar] [CrossRef]
- Ramkisson, S.; Pillay, B.J.; Sartorius, B. Psychosocial Stress in South African Patients with Type 2 Diabetes. J. Insul. Resist. 2016, 1, 1–7. [Google Scholar] [CrossRef][Green Version]
- De Wet, H.; Levitt, N.; Tipping, B. Executive Cognitive Impairment Detected by Simple Bedside Testing Is Associated with Poor Glycaemic Control in Type 2 Diabetes. S. Afr. Med. J. 2007, 97, 1074–1076. [Google Scholar]
- Le Roux, M.; Walsh, C.; Reid, M.; Raubenheimer, J. Diabetes-Related Knowledge, Attitude and Practices (KAP) of Adult Patients with Type 2 Diabetes Mellitus in the Free State Province, South Africa. S. Afr. J. Clin. Nutr. 2018, 32, 83–90. [Google Scholar] [CrossRef]
- Kagee, A. Symptoms of Depression and Anxiety among a Sample of South African Patients Living with a Chronic Illness. J. Health Psychol. 2008, 13, 547–555. [Google Scholar] [CrossRef]
- Berkowitz, N.; Okorie, A.; Goliath, R.; Levitt, N.; Wilkinson, R.J.; Oni, T. The Prevalence and Determinants of Active Tuberculosis among Diabetes Patients in Cape Town, South Africa, a High HIV/TB Burden Setting. Diabetes Res. Clin. Pract. 2018, 138, 16–25. [Google Scholar] [CrossRef]
- Basson, C.A.; Stewart, A.; Mudzi, W.; Musenge, E. Effect of Neural Mobilization on Nerve-Related Neck and Arm Pain: A Randomized Controlled Trial. Physiother. Can. 2020, 72, 408–419. [Google Scholar] [CrossRef]
- Cresswell, C.; Galantino, M.L.; Myezwa, H. The Prevalence of Fear Avoidance and Pain Catastrophising amongst Patients with Chronic Neck Pain. S. Afr. J. Physiother. 2020, 76, a1326. [Google Scholar] [CrossRef]
- Demyttenaere, K.; Bruffaerts, R.; Lee, S.; Posada-Villa, J.; Kovess, V.; Angermeyer, M.C.; Levinson, D.; de Girolamo, G.; Nakane, H.; Mneimneh, Z.; et al. Mental Disorders among Persons with Chronic Back or Neck Pain: Results from the World Mental Health Surveys. Pain 2007, 129, 332–342. [Google Scholar] [CrossRef]
- Igumbor, E.; Puoane, T.; Gansky, S.; Plesh, O. Pain as a Reason for Primary Care Visits: Cross-Sectional Survey in a Rural and Periurban Health Clinic in the Eastern Cape, South Africa. S. Afr. Fam. Pract. 2012, 54, 256–263. [Google Scholar] [CrossRef][Green Version]
- Lang, T.; Parker, R.; Burgess, T. Cervico-Mandibular Muscle Activity in Females with Chronic Cervical Pain. S. Afr. J. Physiother. 2013, 69, 3–8. [Google Scholar] [CrossRef][Green Version]
- Rauf, W.; Meyer, H.; Marcus, T.; Becker, P. Prevalence of Chronic Pain in Patients Attending Primary Healthcare Facilities in South-West Tshwane. S. Afr. Fam. Pract. 2013, 55, 85–89. [Google Scholar] [CrossRef][Green Version]
- Soal, L.J.; Bester, C.M.; Shaw, B.S.; Yelverton, C. Changes in Chronic Neck Pain Following the Introduction of a Visco-Elastic Polyurethane Foam Pillow and/or Chiropractic Treatment. Health SA Gesondheid 2019, 24, 1–6. [Google Scholar] [CrossRef]
- Watson, E.D.; Coopoo, Y. Telephone versus Usual Care in Management of Acute Whiplash Associated Disorder: A Pilot Study. S. Afr. J. Res. Sport. Phys. Educ. Recreat. 2016, 38, 259–267. [Google Scholar]
- Kluge, J.; Hall, D.; Louw, Q.; Theron, G.; Grové, D. Specific Exercises to Treat Pregnancy-Related Low Back Pain in a South African Population. Int. J. Gynecol. Obstet. 2011, 113, 187–191. [Google Scholar] [CrossRef]
- Kruger, P.; Billson, J.; Wood, P.S.; Du Toit, P.J. The Effect of Chronic Low Back Pain on Daily Living and Fear-Avoidance Beliefs in Working Adults. Afr. J. Phys. Health Educ. Recreat. Danc. 2015, 21, 300–314. [Google Scholar]
- Major-Helsloot, M.E.; Crous, L.C.; Grimmer-Somers, K.; Louw, Q.A.; Major-Helsloot, M.E.; Grimmer-Somers, K. Management of LBP at Primary Care Level in South Africa: Up to Standards? Afr. Health Sci. 2014, 14, 698–706. [Google Scholar] [CrossRef] [PubMed]
- Mattison, M.C.; Ross, N.A. Comparing Fatigue Responses between Healthy Individuals and Asymptomatic Low Back Pain Sufferers—Implications for Return-to-Work: A Pilot Study. Ergon. SA 2017, 28, 2. [Google Scholar] [CrossRef]
- Kelly, A.; Younus, A.; Lekgwara, P. Minimally Invasive Spinal Surgery in Spinal Tuberculosis—A Case Report Series. Interdiscip. Neurosurg. Adv. Tech. Case Manag. 2021, 23, 101010. [Google Scholar] [CrossRef]
- Younus, A.; Kelly, A. Lumbar Unifacet Dislocation without an Associated Fracture—A Case Report and Literature Review. Interdiscip. Neurosurg. Adv. Tech. Case Manag. 2021, 23, 100973. [Google Scholar] [CrossRef]
- Younus, A.; Kelly, A.; Lekgwara, P. Evaluating Patient Outcome Post Tubular Lumbar Microdiscectomy. Interdiscip. Neurosurg. Adv. Tech. Case Manag. 2021, 23, 100975. [Google Scholar] [CrossRef]
- Adam, S.; Godlwana, L.; Maleka, D. Effect of Pre-Fracture Mobility on the Early Post-Operative Functional Outcome in Elderly Patients with a Hip Fracture. S. Afr. J. Physiother. 2013, 69, 13–18. [Google Scholar] [CrossRef]
- Butler, I.; Tipping, B.; Bhaga, R. Atypical Femoral Fractures. J. Endocrinol. Metab. Diabetes S. Afr. 2013, 18, 125–127. [Google Scholar] [CrossRef]
- Ferreira, N.; Marais, L.C. Bicondylar Tibial Plateau Fractures Treated with Fine-Wire Circular External Fixation. Strateg. Trauma Limb Reconstr. 2014, 9, 25. [Google Scholar] [CrossRef]
- Gdeh, D.; Haffejee, M.; Nel, M. Frequency of Erectile Dysfunction Following Pelvic Fracture Among Patients Admitted to Two Wits Teaching Hospitals, South Africa. Sudan J. Med. Sci. 2018, 13, 144. [Google Scholar] [CrossRef]
- Gross, T.; Huettl, T.; Audigé, L.; Frey, C.; Monesi, M.; Seibert, F.J.; Messmer, P. How Comparable Is So-Called Standard Fracture Fixation with an Identical Implant? A Prospective Experience with the Antegrade Femoral Nail in South Africa and Europe. Injury 2010, 41, 388–395. [Google Scholar] [CrossRef]
- Bhatia, D.N.; de Beer, J.F.; van Rooyen, K.S.; du Toit, D.F. The Reverse Terrible Triad of the Shoulder: Circumferential Glenohumeral Musculoligamentous Disruption and Neurologic Injury Associated with Posterior Shoulder Dislocation. J. Shoulder Elb. Surg. 2007, 16, e13–e17. [Google Scholar] [CrossRef]
- Fleming, M.A.; Dachs, R.; Maqungo, S.; du Plessis, J.P.; Vrettos, B.C.; Roche, S.J. Angular Stable Fixation of Displaced Distal-Third Clavicle Fractures with Superior Precontoured Locking Plates. J. Shoulder Elb. Surg. 2015, 24, 700–704. [Google Scholar] [CrossRef] [PubMed]
- Held, M.; Jordaan, P.; Laubscher, M.; Singer, M.; Solomons, M. Conservative Treatment of Fractures of the Proximal Phalanx: An Option Even for Unstable Fracture Patterns. Hand Surg. 2013, 18, 229–234. [Google Scholar] [CrossRef]
- Leijnen, D.; Med, M.S.; Viljoen, J.T.; Sci, M.E.; Kirby, J.H.; Chb, M.B.; Med, S.; Viviers, P.L.; Chb, M.B.; Sc, M.; et al. Frozen Shoulder or Missed Posterior Dislocation? S. Afr. J. Sport. Med. 2015, 27, 58–59. [Google Scholar] [CrossRef][Green Version]
- Midgley, R. Case Report: The Casting Motion to Mobilize Stiffness Technique for Rehabilitation after a Crush and Degloving Injury of the Hand. J. Hand Ther. 2016, 29, 323–333. [Google Scholar] [CrossRef] [PubMed]
- Arendse, R.; Brink, P.; Beighton, P. Hereditary Bone Dysplasia with Pathological Fractures and Nodal Osteoarthropathy. Skeletal Radiol. 2009, 38, 1197–1203. [Google Scholar] [CrossRef]
- Chetty, M.; Stephen, L.X.G.; Roberts, T. Osteoporosis-Pseudoglioma Syndrome in South Africa. S. Afr. Med. J. 2016, 106, 100. [Google Scholar] [CrossRef] [PubMed]
- Conradie, M.; Conradie, M.M.; Scher, A.T.; Kidd, M.; Hough, S. Vertebral Fracture Prevalence in Black and White South African Women. Arch. Osteoporos. 2015, 10, 1. [Google Scholar] [CrossRef]
- Ramnarain, A.; Govender, S. Fibular Allograft and Anterior Plating for Dislocations/Fractures of the Cervical Spine. Indian J. Orthop. 2008, 42, 83–86. [Google Scholar]
- Oosthuizen, G.V.; De Wet, J.; Bruce, J.L.; Clarke, D.L. Rib Fracture Fixation in a South African Public Trauma Service. S. Afr. J. Surg. 2017, 55, 4–8. [Google Scholar]
- Enicker, B.; Madiba, T.E. Cranial Injuries Secondary to Assault with a Machete. Injury 2014, 45, 1355–1358. [Google Scholar] [CrossRef]
- Awolola, A.M.; Campbell, L.; Ross, A. Pain Management in Patients with Long-Bone Fractures in a District Hospital in KwaZulu-Natal, South Africa. Afr. J. Prim. Health Care Fam. Med. 2015, 7, 1–5. [Google Scholar] [CrossRef]
- Gous, E.; Ally, M.M.T.M.; Meyer, P.W.A.; Suleman, F.E. Simple Erosion Narrowing Score of the Hands as a Predictor of Cervical Spine Subluxation in Rheumatoid Arthritis. S. Afr. J. Radiol. 2020, 24, 1–6. [Google Scholar] [CrossRef]
- Lombard, L.A.; du Plessis, L.M.; Visser, J. Body Composition of Rheumatoid Arthritis Patients in the City of Cape Town, South Africa. Clin. Rheumatol. 2014, 33, 467–476. [Google Scholar] [CrossRef]
- Nolte, K. Land- and Water-Based Exercises in Rheumatoid Arthritis Patients: A Series of Case Reports. S. Afr. J. Sport. Med. 2011, 23, 69–70. [Google Scholar] [CrossRef][Green Version]
- Prioreschi, A.; Makda, M.A.; Tikly, M.; McVeigh, J.A. In Patients with Established RA, Positive Effects of a Randomised Three Month WBV Therapy Intervention on Functional Ability, Bone Mineral Density and Fatigue Are Sustained for up to Six Months. PLoS ONE 2016, 11, e0153470. [Google Scholar] [CrossRef]
- Solomon, A.; Christian, B.F.; Woodiwiss, A.J.; Norton, G.R.; Dessein, P.H. Burden of Depressive Symptoms in South African Public Healthcare Patients with Established Rheumatoid Arthritis: A Case-Control Study. Clin. Exp. Rheumatol. 2011, 29, 506–512. [Google Scholar]
- Younus, A.; Kelly, A. Hip Spine Syndrome—A Case Series and Literature Review. Interdiscip. Neurosurg. Adv. Tech. Case Manag. 2021, 23, 100960. [Google Scholar] [CrossRef]
- Frimpong, E.; Mcveigh, J.A.; Van Der Jagt, D.; Mokete, L.; Kaoje, Y.S. Light Intensity Physical Activity Increases and Sedentary Behavior Decreases Following Total Knee Arthroplasty in Patients with Osteoarthritis. Knee Surg. Sport. Traumatol. Arthrosc. 2019, 27, 2196–2205. [Google Scholar] [CrossRef]
- Cloake, T.; Haigh, T.; Cheshire, J.; Walker, D. ScienceDirect The Impact of Patient Demographics and Comorbidities upon Burns Admitted to Tygerberg Hospital Burns Unit, Western Cape, South Africa. Burns 2016, 43, 411–416. [Google Scholar] [CrossRef]
- Eyal, A.S.; Kemp, M.; Luvhengo, T. A 10-Year Audit of Burns at Kalafong Hospital. Burns 2007, 33, 393–395. [Google Scholar] [CrossRef][Green Version]
- Kinoo, S.M.; Singh, B. Complex Regional Pain Syndrome in Burn Pathological Scarring: A Case Report and Review of the Literature. Burns 2017, 43, e47–e52. [Google Scholar] [CrossRef]
- Morris, L.L. Pain and Anxiety Experiences of South African Adult Burn Injury Patients. S. Afr. J. Physiother. 2010, 66, 6–9. [Google Scholar] [CrossRef]
- Den Hollander, D.; Albert, M.; Strand, A.; Hardcastle, T.C. Epidemiology and Referral Patterns of Burns Admitted to the Burns Centre at Inkosi Albert Luthuli Central Hospital, Durban. Burns 2014, 40, 1201–1208. [Google Scholar] [CrossRef]
- Ablort-morgan, C.; Allorto, N.L.; Rode, H. ScienceDirect Rehabilitation of a Bilateral Upper Limb Amputee in a Resource Restricted Burn Service. Burns 2016, 42, e81–e85. [Google Scholar] [CrossRef]
- Govender, S.M.; de Jongh, M. Identifying Hearing Impairment and the Associated Impact on the Quality of Life among the Elderly Residing in Retirement Homes in Pretoria, South Africa. S. Afr. J. Commun. Disord. 2021, 68, 1–9. [Google Scholar] [CrossRef]
- Louw, C.; Swanepoel, D.W.; Eikelboom, R.H.; Hugo, J. Prevalence of Hearing Loss at Primary Health Care Clinics in South Africa. Afr. Health Sci. 2018, 18, 313–320. [Google Scholar] [CrossRef]
- Olivier, B.; Pramod, A.; Maleka, D. Trigger Point Sensitivity Is a Differentiating Factor between Cervicogenic and Non-Cervicogenic Headaches: A Cross-Sectional, Descriptive Study. Physiother. Can. 2018, 70, 323–329. [Google Scholar] [CrossRef] [PubMed]
- Rouillard, S.; De Weerdt, W.; De Wit, L.; Jelsma, J. Functioning at 6 Months Post Stroke Following Discharge from Inpatient Rehabilitation. S. Afr. Med. J. 2012, 102, 545–548. [Google Scholar] [CrossRef]
- Parker, R.; Stein, D.J.; Jelsma, J. Pain in People Living with HIV/AIDS: A Systematic Review. J. Int. AIDS Soc. 2014, 17, 18719. [Google Scholar] [CrossRef] [PubMed]
- Maritz, J.; Benatar, M.; Dave, J.A.; Harrison, T.B.; Badri, M.; Levitt, N.S.; Heckmann, J.M. HIV Neuropathy in South Africans: Frequency, Characteristics, and Risk Factors. Muscle Nerve 2010, 41, 599–606. [Google Scholar] [CrossRef]
- Naude, J.J.; Manjra, M.A.; Birkholtz, F.; Barnard, A.; Tetsworth, K.; Glatt, V.; Hohmann, E. Functional Outcomes and Quality of Life Following Complex Tibial Fractures Treated with Circular External Fixation: A Comparison between Proximal, Midshaft, and Distal Tibial Fractures. Strateg. Trauma Limb Reconstr. 2021, 16, 32–40. [Google Scholar] [CrossRef]
- Wasserman, S.; de Villiers, L.; Bryer, A.; de Villiers, L.; Bryer, A.; de Villiers, L.; Bryer, A. Stroke Care in a Rural African Setting. Int. J. Stroke 2009, 4, 151. [Google Scholar] [CrossRef]
- Spies, G.; Ahmed-Leitao, F.; Fennema-Notestine, C.; Cherner, M.; Seedat, S. Effects of HIV and Childhood Trauma on Brain Morphometry and Neurocognitive Function. J. Neurovirol. 2016, 22, 149–158. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Penn, C.; Commerford, A.; Ogilvy, D. Spatial and Facial Processing in the Signed Discourse of Two Groups of Deaf Signers with Clinical Language Impairment. Clin. Linguist. Phon. 2007, 21, 369–391. [Google Scholar] [CrossRef]
- Nicholas, P.K.; Voss, J.; Wantland, D.; Lindgren, T.; Huang, E.; Holzemer, W.L.; Cuca, Y.; Moezzi, S.; Portillo, C.; Willard, S.; et al. Prevalence, Self-Care Behaviors, and Self-Care Activities for Peripheral Neuropathy Symptoms of HIV/AIDS. Nurs. Health Sci. 2010, 12, 119–126. [Google Scholar] [CrossRef]
- Matter, R.A.; Eide, A.H. Access to Assistive Technology in Two Southern African Countries. BMC Health Serv. Res. 2018, 18, 792. [Google Scholar] [CrossRef]
- Maart, S. Disability in Under-Resourced Areas in the Western Cape, South Africa: A Descriptive Analytical Study. Ph.D. Thesis, University of Cape Town, Cape Town, South Africa, 2015. [Google Scholar]
- Jesus, T.S.; Bright, F.; Kayes, N.; Cott, C.A. Person-Centred Rehabilitation: What Exactly Does It Mean? Protocol for a Scoping Review with Thematic Analysis towards Framing the Concept and Practice of Person-Centred Rehabilitation. BMJ Open 2016, 6, e011959. [Google Scholar] [CrossRef] [PubMed]
- Üstün, T.B.; Chatterji, S.; Bickenbach, J.; Kostanjsek, N.; Schneider, M. The International Classification of Functioning, Disability and Health: A New Tool for Understanding Disability and Health. Disabil. Rehabil. 2003, 25, 565–571. [Google Scholar] [CrossRef] [PubMed]
- Zondi, T.; Day, C. Measuring National Health Insurance: Towards Universal Health Coverage in South Africa. S. Afr. Health Rev. 2019, 2019, 55–68. [Google Scholar]
- Ned, L.; Cloete, L.; Mji, G. The Experiences and Challenges Faced by Rehabilitation Community Service Therapists within the South African Primary Healthcare Health System. Afr. J. Disabil. 2017, 6, 1–11. [Google Scholar] [CrossRef]
- World Health Organization. Rehabilitation Competency Framework; Electronic Version; World Health Organization: Geneva, Switzerland, 2020; ISBN 9789240008281. [Google Scholar]
- Kredo, T.; Abrams, A.; Young, T.; Louw, Q.; Volmink, J.; Daniels, K. Primary Care Clinical Practice Guidelines in South Africa: Qualitative Study Exploring Perspectives of National Stakeholders. BMC Health Serv. Res. 2017, 17, 608. [Google Scholar] [CrossRef]
- Stander, J.; Grimmer, K.; Brink, Y. Factors Influencing Clinical Practice Guideline Uptake by South African Physiotherapists: A Qualitative Investigation of Barriers and Facilitators. J. Eval. Clin. Pract. 2020, 26, 728–737. [Google Scholar] [CrossRef]
- WHO. Task Shifting: Global Recommendations and Guidelines; WHO: Geneva, Switzerland, 2008. [Google Scholar]
- WHO. Rehabilitation in Health Systems; World Health Organization: Geneva, Switzerland, 2017; ISBN 9789241549974. [Google Scholar]
- Hone, T.; Macinko, J.; Millett, C. Revisiting Alma-Ata: What Is the Role of Primary Health Care in Achieving the Sustainable Development Goals? Lancet 2018, 392, 1461–1472. [Google Scholar] [CrossRef]
- Singh, R.; Küçükdeveci, A.A.; Grabljevec, K.; Gray, A. The Role of Interdisciplinary Teams in Physical and Rehabilitation Medicine. J. Rehabil. Med. 2018, 50, 673–678. [Google Scholar] [CrossRef]
- Kuper, H.; Smythe, T.; Kujinga, T.; Chivandire, G.; Rusakaniko, S. Should Disability-Inclusive Health Be a Priority in Low-Income Countries? A Case-Study from Zimbabwe. Glob. Health Action 2022, 15, 2032929. [Google Scholar] [CrossRef]
- Mapanga, W.; Casteleijn, D.; Ramiah, C.; Odendaal, W.; Metu, Z.; Robertson, L.; Goudge, J. Strategies to Strengthen the Provision of Mental Health Care at the Primary Care Setting: An Evidence Map. PLoS ONE 2019, 14, e0222162. [Google Scholar] [CrossRef]
- Petersen, I.; Fairall, L.; Bhana, A.; Kathree, T.; Selohilwe, O.; Brooke-Sumner, C.; Faris, G.; Breuer, E.; Sibanyoni, N.; Lund, C.; et al. Integrating Mental Health into Chronic Care in South Africa: The Development of a District Mental Healthcare Plan. Br. J. Psychiatry 2016, 208, s29. [Google Scholar] [CrossRef] [PubMed]
- Hoosain, M.; Plastow, N.A. Protocol: Workplace-Based Occupational Therapy for Mental Health in Africa: A Scoping Review Protocol. BMJ Open 2022, 12, e054821. [Google Scholar] [CrossRef] [PubMed]
- Plastow, N.A.; van Niekerk, L.; Cloete, L.; Leibbrandt, D. The Effect of Interventions to Support Mental Health Post-Stroke in Africa: A Systematic Review. In Collaborative Capacity Development to Complement Stroke Rehabilitation in Africa [Internet]; AOSIS: Cape Town, South Africa, 2021; pp. 133–169. [Google Scholar]
- Barnabé, M.A.; Gordon, R.; Ramjee, G.; Loots, G.; Blackburn, J.M. National Expenditure on Health Research in South Africa: How Has the Landscape Changed in the Past Decade? S. Afr. Med. J. 2020, 110, 274–283. [Google Scholar] [CrossRef] [PubMed]
- Lekoubou, A.; Echouffo-Tcheugui, J.B.; Kengne, A.P. Epidemiology of Neurodegenerative Diseases in Sub-Saharan Africa: A Systematic Review. BMC Public Health 2014, 14, 653. [Google Scholar] [CrossRef] [PubMed]
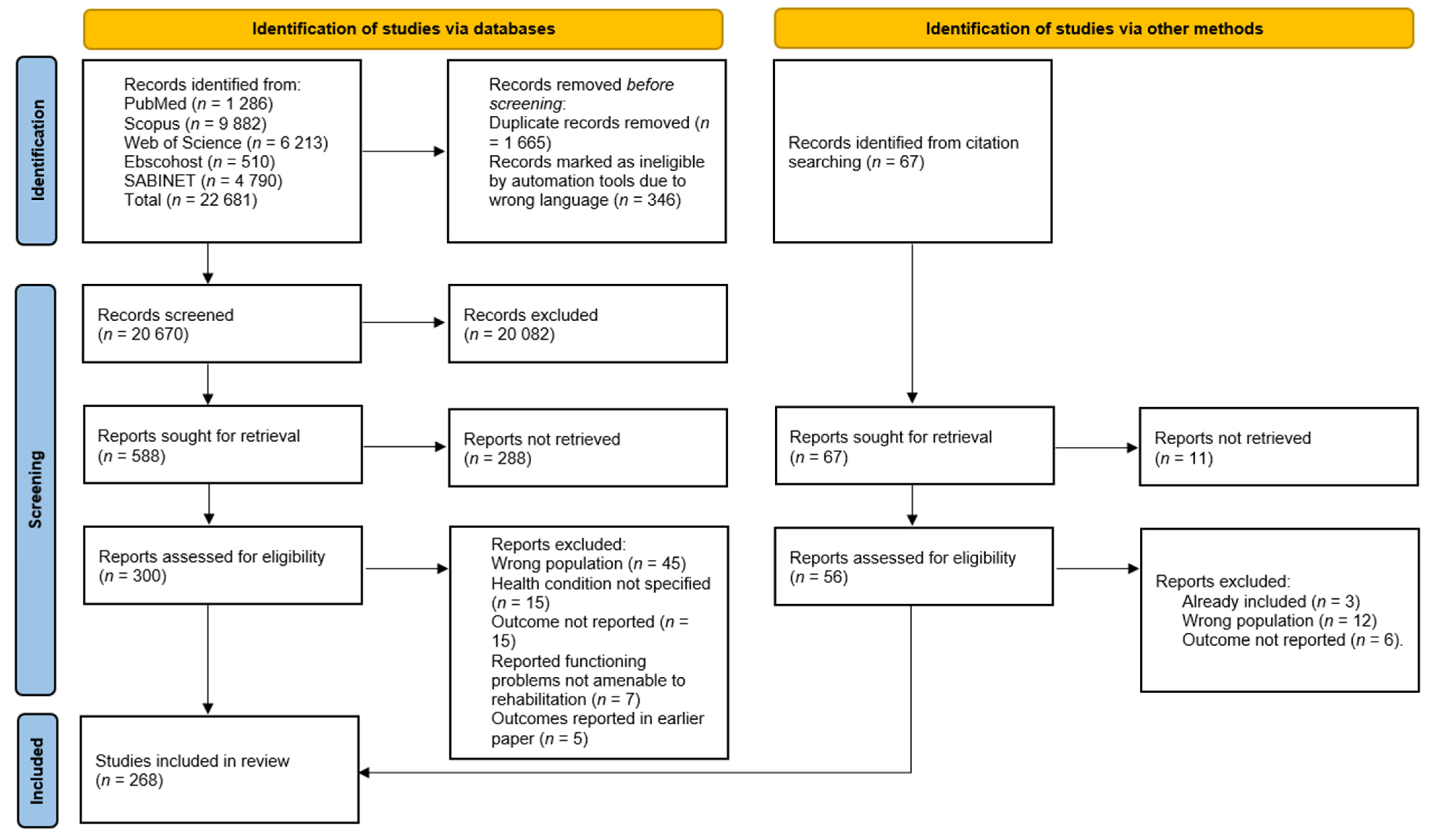
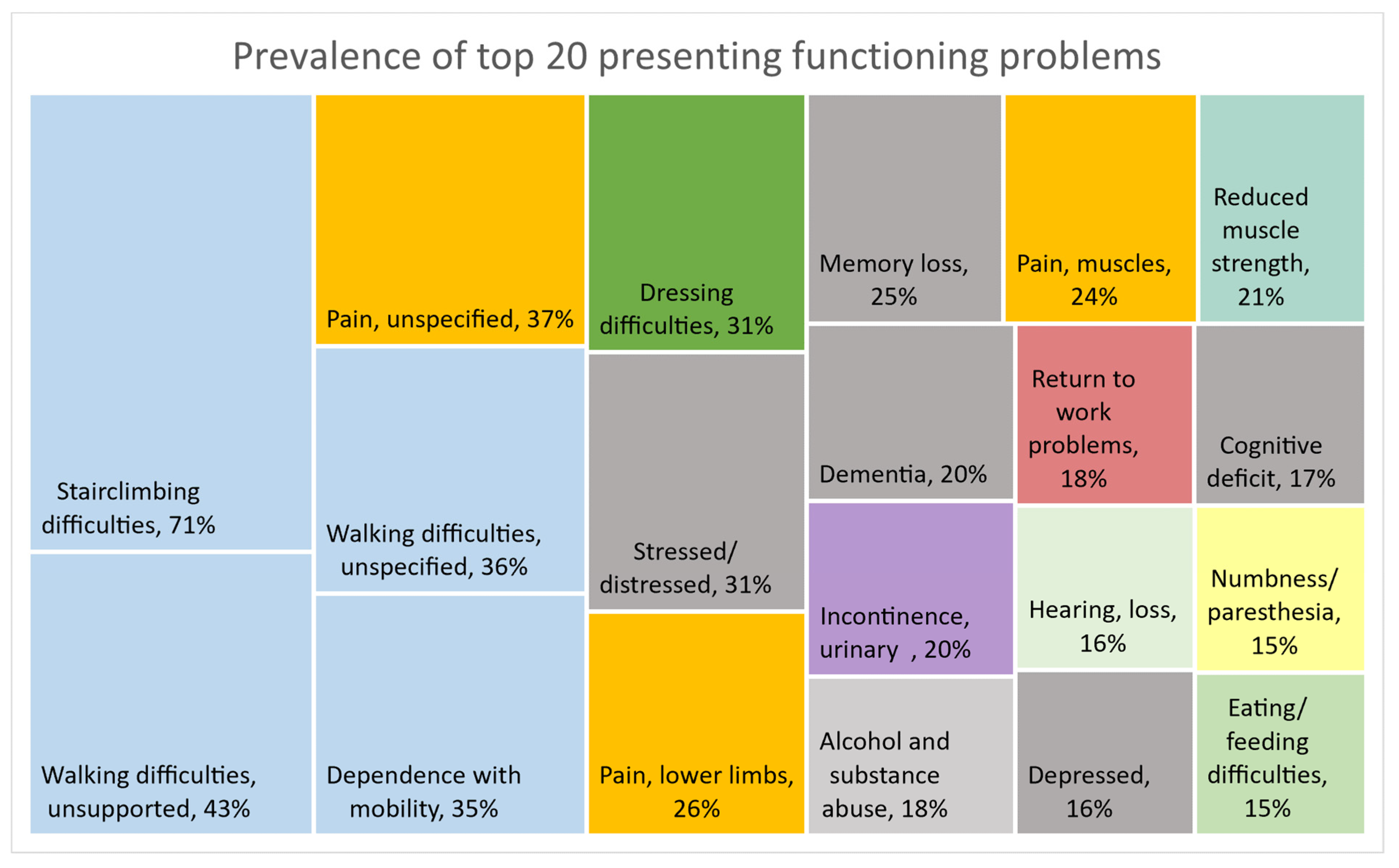
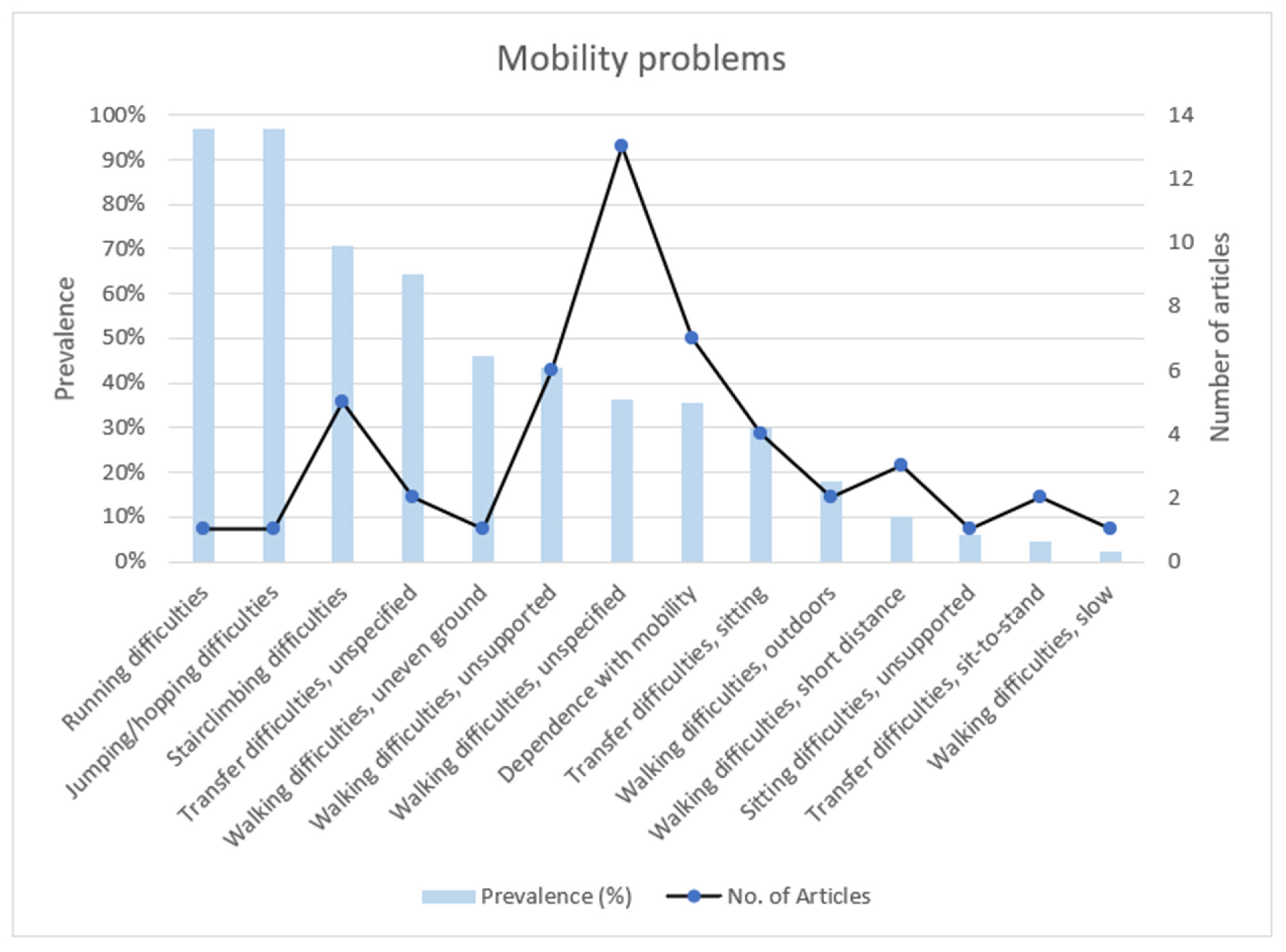
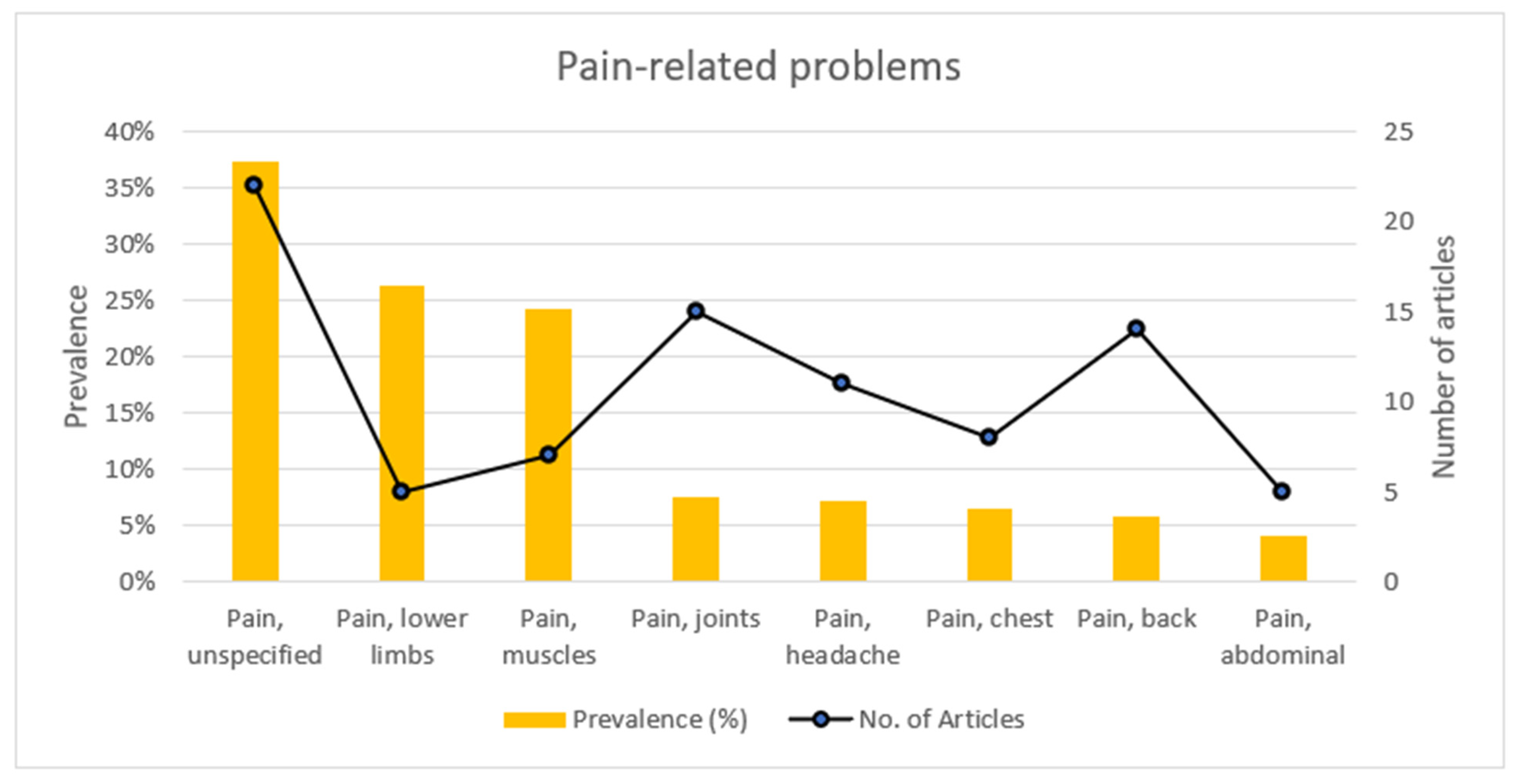
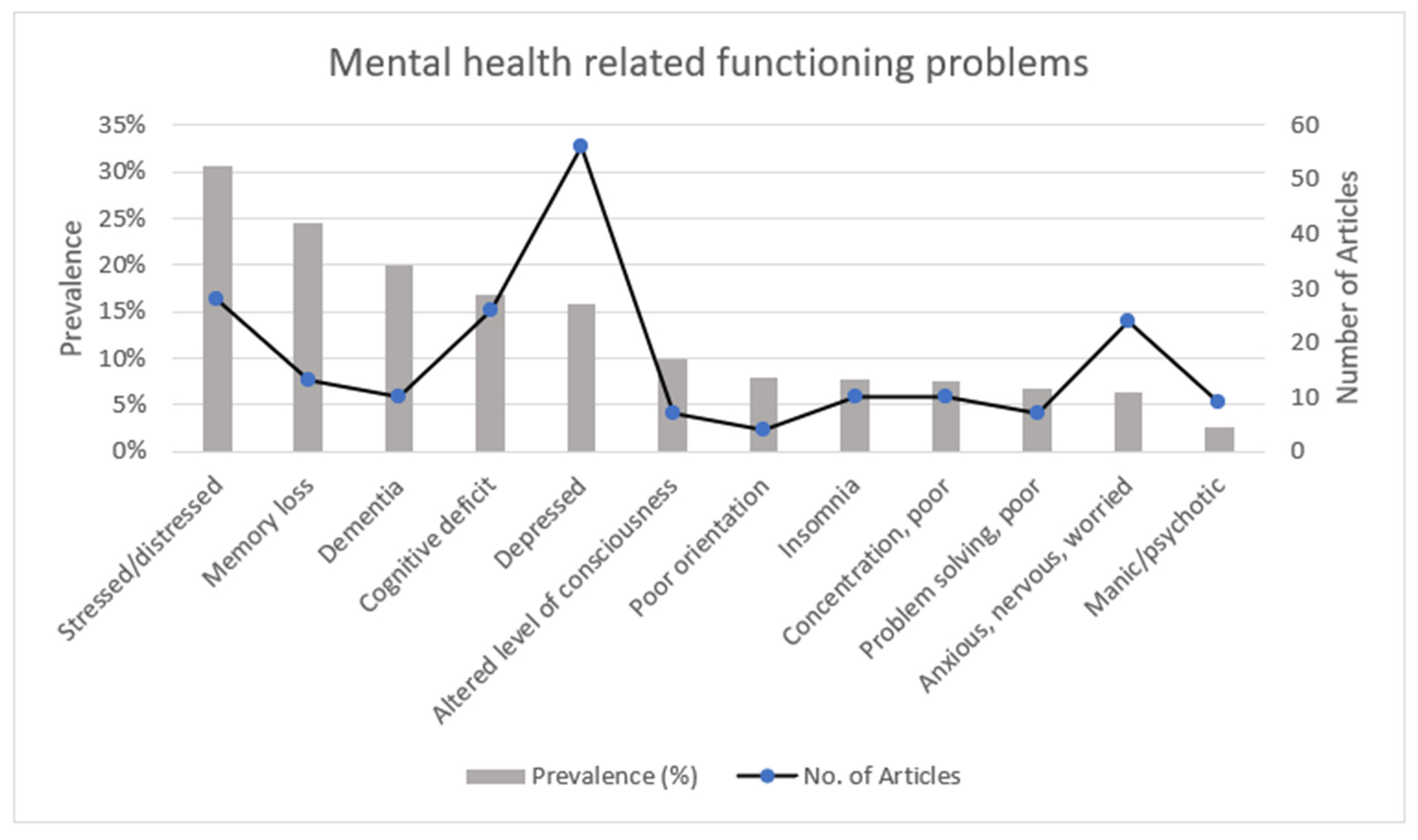
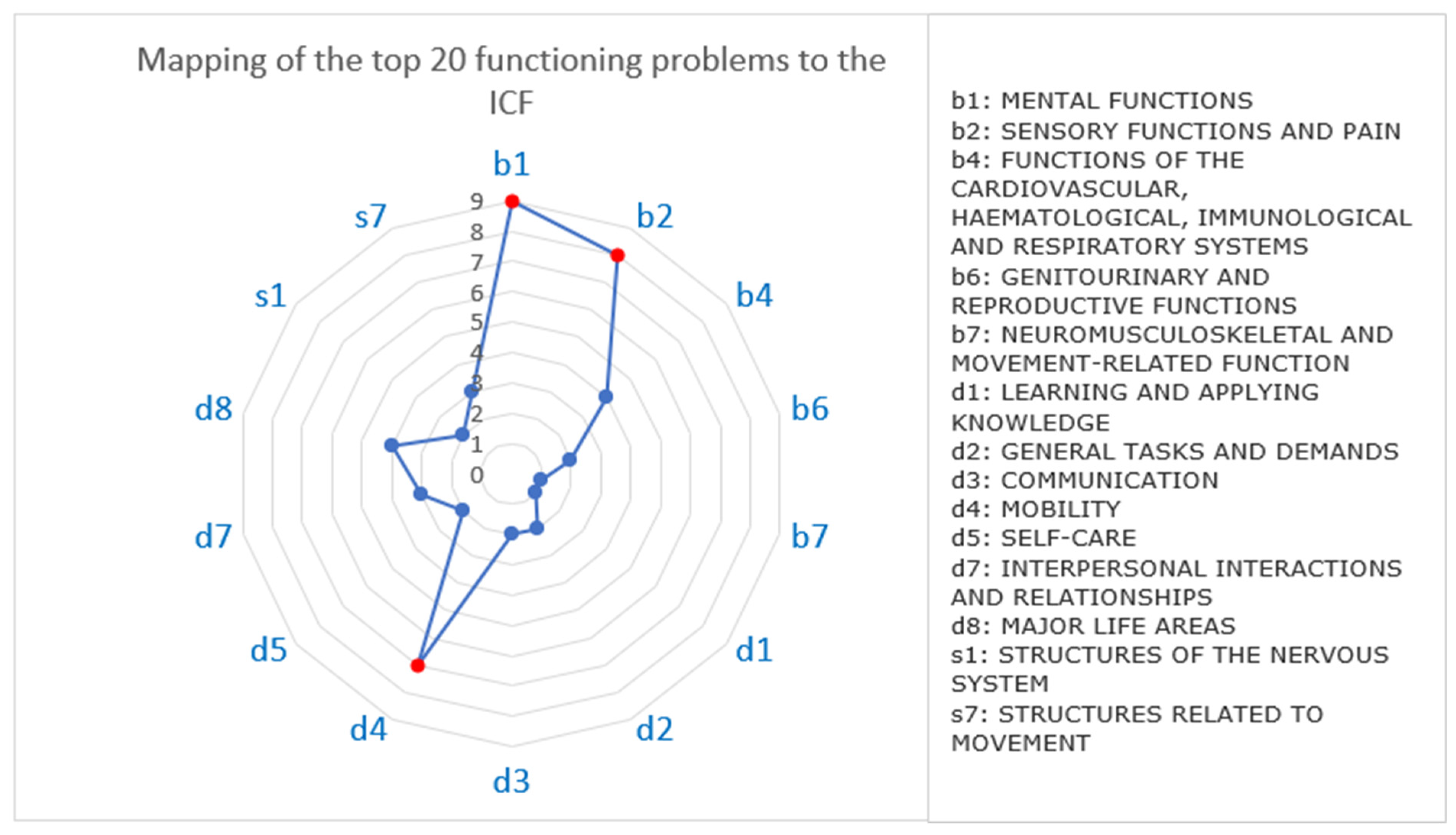
| Condition | Sub-Category | No of Articles (n) | Subtotals |
|---|---|---|---|
| HIV | HIV only [41,42,43,44,45,46,47,48,49,50,51,52,53,54,55,56,57,58,59,60,61,62,63,64,65,66,67,68,69,70,71,72,73,74,75,76,77,78,79,80,81,82,83,84,85,86,87,88,89,90,91,92,93,94,95,96,97,98,99,100,101,102,103,104,105,106,107,108,109,110,111,112,113,114,115,116,117,118,119,120,121,122,123,124,125,126,127,128,129,130,131,132,133,134,135,136,137,138,139,140,141,142,143,144,145,146,147,148,149,150,151,152,153,154,155,156,157,158,159,160,161,162,163] | 126 | |
| HIV with TB [164,165,166,167,168,169,170,171,172,173] | 10 | ||
| HIV with Kaposi’s sarcoma [174,175] | 2 | ||
| HIV with Cryptococcal Meningocele [176] | 1 | 139 | |
| Tuberculosis | TB, unspecified [148,177,178,179,180,181,182,183,184,185,186,187,188,189,190] | 15 | |
| TB, MDR [191,192,193,194,195,196,197,198,199,200] | 10 | ||
| TB, pulmonary [201,202,203] | 3 | ||
| TB, spinal [204,205,206] | 3 | ||
| TB, tuberculoma [207] | 1 | ||
| TB, meningitis [208] | 1 | 33 | |
| Stroke | Stroke, unspecified [148,209,210,211,212,213,214,215,216,217,218,219,220,221,222,223,224,225,226,227,228,229,230,231] | 24 | 24 |
| Diabetes Mellitus | DM, Type unspecified [232,233,234,235,236,237,238,239] | 8 | |
| DM, Type II [240,241,242,243,244,245,246] | 7 | ||
| DM, Type I [241,242] | 2 | ||
| DM with hypertension [247] | 1 | ||
| DM with HIV [248] | 1 | 19 | |
| Spinal pain | Neck pain [249,250,251,252,253,254,255,256] | 8 | |
| LBP, mechanical [252,254,257,258,259,260] | 6 | ||
| LBP, pathological [261,262,263] | 3 | 17 | |
| Fracture/dislocation | Lower limb fracture/dislocation [264,265,266,267,268] | 5 | |
| Upper limb fracture/dislocation [269,270,271,272,273] | 5 | ||
| Pathological fracture(s) [274,275] | 2 | ||
| Spinal fracture(s) [276,277] | 2 | ||
| Rib fracture(s) [278] | 1 | ||
| Skull/cranial fracture(s) [279] | 1 | ||
| Fracture, unspecified [280] | 1 | 17 | |
| Arthritis | Rheumatoid arthritis [281,282,283,284,285] | 5 | |
| OA, hip [286] | 1 | ||
| OA, knee [287] | 1 | ||
| OA, other [237] | 1 | 8 | |
| Burns | Burns only [288,289,290,291,292] | 5 | |
| Burns with amputation [293] | 1 | 6 | |
| Hearing loss | Hearing loss [293,294,295] | 3 | 3 |
| Headaches | Headache, cervicogenic [296] | 1 | |
| Headache, unspecified [254] | 1 | 2 |
| Problem | ICF Domain | ICF Code/Category | Outcome Measures |
|---|---|---|---|
| Stairclimbing difficulties | d4 MOBILITY | d455 moving around | Barthel Index (BI); [211,216,217] Rivermead Motor Assessment scores of Gross function (RMA-G); Nottingham extended activities of daily living (NEADL) scale [297] |
| Walking difficulties, unsupported | d4 MOBILITY | d450 Walking d465 Moving around using equipment | Rivermead Mobility Index (RMI); [215] Berg Balance Scale (BBS); [215] Postural Assessment Scale for Stroke Patients (PASS); [215] self-report; [76] Use of assistive devices [227] |
| Pain, unspecified | b1 MENTAL FUNCTIONS | b134 Sleep functions b152 Emotional functions | Wisconsin Brief Pain Questionnaire (WBPQ); [125] Beck Depression Inventory (BDI); [139] Pain Catastrophizing Scale (PCS); [150,249] Hopkins Symptoms Checklist-25 (HSCL-25); [150] Neuropathic Diagnostic Questionnaire (DN4) [249] |
| b2 SENSORY FUNCTIONS AND PAIN | b270 Sensory functions related to temperature and other stimuli b280 Sensation of pain | Brief Pain Inventory (Xhosa) (BPI-Xhosa); [298] WBPQ; [125,150] Brief Neuropathy Screening Tool (BNST); [150,299] Visual Analogue Scale (VAS), [280] Numeric Pain Rating Scale (NPRS); [249] Brief Peripheral Neuropathy Screen (BPNS) [75] | |
| s7 STRUCTURES RELATED TO MOVEMENT | s750 Structure of lower extremity | ASAMI score, the Foot Function Index (FFI), radiographic outcomes; [300] The Lower Extremity Functional Scale (LEFS) [75] | |
| d2 GENERAL TASKS AND DEMANDS | d240 Handling stress and other psychological demands | HSCL-25 [150] | |
| d4 MOBILITY | d450 Walking | (BPI [130]; Karnofsky Performance Scale (KPS) [125] | |
| d7 INTERPERSONAL INTERACTIONS AND RELATIONSHIPS | d710 Basic interpersonal interactions | BPI [130] | |
| d8 MAJOR LIFE AREAS | d820 School education d845 Acquiring, keeping, and terminating a job | BPI [130] | |
| Walking difficulties, unspecified | b2 SENSORY FUNCTIONS AND PAIN | b235 Vestibular functions | Self-report [76] |
| d4 MOBILITY | d450 Walking | Self-report [76] | |
| Dependence with mobility | d4 MOBILITY | d450 Walking d465 Moving around using equipment | Rankin scores; [301] BI; [211] Timed-up-and-go-test; [182] BBS; [215] Nurick classification [205] |
| Dressing difficulties | d5 SELF-CARE | d540 Dressing | BI; [211] World Health Organization’s Disability Assessment Schedule 2.0 (WHODAS 2.0) [209] |
| Stressed/distressed | b1 MENTAL FUNCTIONS | b126 Temperament and personality functions | Questionnaire on Stress in Diabetes—Revised (QSD-R); [244] Breslau PTSD screener [61] |
| d2 GENERAL TASKS AND DEMANDS | d240 Handling stress and other psychological demand | Primary Care PTSD Screen (PC-PTSD); [179] The Kessler Psychological Distress Scale (K-10); [179] Mini-International Neuropsychiatric Interview (MINI); [135] Hopkins Symptom Checklist (HSCL); [101] Composite International Diagnostic Interview (CIDI); [78] CIDI [111] | |
| d7 INTERPERSONAL INTERACTIONS AND RELATIONSHIPS | d750 Informal social relationships | Questionnaire on Stress in Diabetes—Revised (QSD-R) [244] | |
| Pain, lower limbs | b2 SENSORY FUNCTIONS AND PAIN | b280 Sensation of pain | BPI-Xhosa; [138] NPRS; [291] BPNS; [64] Visual Analogue Scale (VAS) [280] |
| s7 STRUCTURES RELATED TO MOVEMENT | s750 Structure of lower extremity | BPI-Xhosa; [57,138] Burn Specific Pain and Anxiety scale (BSPAS) [291] | |
| Memory loss | b1 MENTAL FUNCTIONS | b117 Intellectual functions b144 Memory functions b164 Higher-level cognitive functions | WHODAS 2.0; [209] International HIV Dementia Scale (IHDS); [93] Neuropsychological (NP) test battery; [132] The revised signs and symptoms checklist for persons with HIV disease (SSC-HIVrev); [146] The International Classification of Functioning, Disability and Health (ICF) [128] |
| Pain, muscles | b2 SENSORY FUNCTIONS AND PAIN | b280 Sensation of pain | ICF; [128] WHODAS 2.0; [107] self-report; [265] SSC-HIVrev [79] |
| Reduced muscle strength | b4 FUNCTIONS OF THE CARDIOVASCULAR, HAEMATOLOGICAL, IMMUNOLOGICAL AND RESPIRATORY SYSTEMS | b455 Exercise tolerance functions | ICF; [128] |
| b7 NEUROMUSCULOSKELETAL AND MOVEMENT-RELATED FUNCTION | b710 Mobility of joint functions b730 Muscle power functions | ICF; [128] Oxford Scale of muscle strength; [42] isokinetic dynamometry; [269,283] sphygmomanometer [283] | |
| s7 STRUCTURES RELATED TO MOVEMENT | s750 Structure of lower extremity s720 Structure of shoulder region | ICF; [128] isokinetic dynamometry [269,283] | |
| Dementia | b1 MENTAL FUNCTIONS | b117 Intellectual functions b144 Memory functions b147 Psychomotor functions b152 Emotional functions | NP test battery; [132] IHDS; [80,155,200] mini-mental state examination (MMSE), Montreal cognitive assessment (MOCA), Simioni symptom questionnaire (SSQ) and cognitive assessment tool-rapid version (CAT-rapid) [95] |
| Incontinence, urinary | b6 GENITOURINARY AND REPRODUCTIVE FUNCTIONS | b620 Urination functions | Self-report [198] BI; [211,217] Survey of Autonomic Symptoms (SAS) [75] |
| Alcohol and substance abuse | b1 MENTAL FUNCTIONS | b117 Intellectual functions b130 Energy and drive functions b152 Emotional functions | MINI; [155] Alcohol Use Disorder Identification Test (AUDIT); [91,147,189] CAGE questionnaire; [54] Alcohol, Smoking and Substance Involvement Screening Test questionnaire (ASSIST) [102] |
| Return to work problems | b1 MENTAL FUNCTIONS | b117 Intellectual functions b130 Energy and drive functions b144 Memory functions b152 Emotional functions b167 Mental functions of language | Return to work questionnaire [212,226] |
| b2 SENSORY FUNCTIONS AND PAIN | b210 Seeing functions b280 Sensation of pain | Return to work questionnaire; [212,226] BPI [212,226] | |
| b4 FUNCTIONS OF THE CARDIOVASCULAR, HAEMATOLOGICAL, IMMUNOLOGICAL AND RESPIRATORY SYSTEMS | b455 Exercise tolerance functions | Return to work questionnaire [212,226] | |
| b6 GENITOURINARY AND REPRODUCTIVE FUNCTIONS | b620 Urination functions | Return to work questionnaire [212,226] | |
| d3 COMMUNICATION | d330 Speaking | Return to work questionnaire [212,226] | |
| d4 MOBILITY | d445 Hand and arm use d450 Walking d470 Using transportation | Return to work questionnaire [212,226] | |
| d8 MAJOR LIFE AREAS | d845 Acquiring, keeping, and terminating a job | Return to work questionnaire [212,226,250] | |
| Cognitive deficit | b1 MENTAL FUNCTIONS | b117 Intellectual functions b140 Attention functions b144 Memory functions b147 Psychomotor functions b156 Perceptual functions b160 Thought functions b164 Higher-level cognitive functions | NP test battery; [157] MoCA; [156] Tampa Scale for Kinesiophobia-11 (TSK-11); PCS; [250] NeuroScreen Performance [157]; IHDS; [80,155,200] MMSE, SSQ and cognitive assessment tool-rapid version (CAT-rapid); [95] Bedside Executive Screening Test (BEST) [245] |
| b3 VOICE AND SPEECH FUNCTIONS | b330 Fluency and rhythm of speech functions | NP test battery; [45,157,171] | |
| b4 FUNCTIONS OF THE CARDIOVASCULAR, HAEMATOLOGICAL, IMMUNOLOGICAL AND RESPIRATORY SYSTEMS | b435 Immunological system functions | Laboratory assessments for immune markers TYMP and NGAL [58] | |
| d4 MOBILITY | d475 Driving | NP test battery and driving simulations [82] | |
| d8 MAJOR LIFE AREAS | d820 School education | NP test battery; [157] | |
| s1 STRUCTURES OF THE NERVOUS SYSTEM | s110 Structure of brain | Brain imaging [302] | |
| Hearing, loss | b2 SENSORY FUNCTIONS AND PAIN | b167 Mental functions of language b230 Hearing functions | Otoscopy, tympanometry, pure-tone audiometry, and distortion product otoacoustic emissions [66,105,184,191,197] |
| d1 LEARNING AND APPLYING KNOWLEDGE | d166 Reading | South African Sign Language (SASL) [303] | |
| d3 COMMUNICATION | d330 Speaking | SASL [303] | |
| Depressed | b1 MENTAL FUNCTIONS | b126 Temperament and personality functions b130 Energy and drive functions b134 Sleep functions b147 Psychomotor functions b152 Emotional functions | NP test battery; Patient Health Questionnaire (PHQ-9); [154] Centers for Epidemiologic Studies Depression Scale (CES-D) [108,144] Hospital Anxiety and Depression Scale (HADS) [243] Beck Depression Inventory—Second Edition (BDI II) [133] |
| b2 SENSORY FUNCTIONS AND PAIN | b280 Sensation of pain | PHQ-9; [154] | |
| b4 FUNCTIONS OF THE CARDIOVASCULAR, HAEMATOLOGICAL | b455 Exercise tolerance functions | PHQ-9; [154] | |
| d7 INTERPERSONAL INTERACTIONS AND RELATIONSHIPS | d710 Basic interpersonal interactions d770 Intimate relationships | Edinburgh Postnatal Depression Scale (EPDS) [60,131] | |
| d8 MAJOR LIFE AREAS | d845 Acquiring, keeping, and terminating a job d850 Remunerative employment | BPI [57] | |
| Numbness/paraesthesia | b2 SENSORY FUNCTIONS AND PAIN | b265 Touch function b270 Sensory functions related to temperature and stimuli b280 Sensation of pain b840 Sensation related to the skin | Total Neuropathy Score (TNSr) [64] SCC- HIVrev; [304] Assessment of fine touch, pin-prick and vibration sense for neuropathy symptom score (NSS) and neuropathy disability score (NDS); [192] AIDS Clinical Trials Group BPNS [56] |
| s1 STRUCTURES OF THE NERVOUS SYSTEM | s120 Spinal cord and related structures | Radiological imaging | |
| Eating/feeding difficulties | d5 SELF-CARE | d550 Eating | National Institute of Health Stroke Scale, (NIHSS); [217] WHODAS 2.0; [209] South African dysphagia screening tool (SADS); [213] Self-report [215] |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Charumbira, M.Y.; Berner, K.; Louw, Q.A. Functioning Problems Associated with Health Conditions with Greatest Disease Burden in South Africa: A Scoping Review. Int. J. Environ. Res. Public Health 2022, 19, 15636. https://doi.org/10.3390/ijerph192315636
Charumbira MY, Berner K, Louw QA. Functioning Problems Associated with Health Conditions with Greatest Disease Burden in South Africa: A Scoping Review. International Journal of Environmental Research and Public Health. 2022; 19(23):15636. https://doi.org/10.3390/ijerph192315636
Chicago/Turabian StyleCharumbira, Maria Y., Karina Berner, and Quinette A. Louw. 2022. "Functioning Problems Associated with Health Conditions with Greatest Disease Burden in South Africa: A Scoping Review" International Journal of Environmental Research and Public Health 19, no. 23: 15636. https://doi.org/10.3390/ijerph192315636
APA StyleCharumbira, M. Y., Berner, K., & Louw, Q. A. (2022). Functioning Problems Associated with Health Conditions with Greatest Disease Burden in South Africa: A Scoping Review. International Journal of Environmental Research and Public Health, 19(23), 15636. https://doi.org/10.3390/ijerph192315636






