Physical Fitness Differences, Amenable to Hypoxia-Driven and Sarcopenia Pathophysiology, between Sleep Apnea and COVID-19
Abstract
:1. Introduction
2. Materials and Methods
2.1. Study Population
2.2. Inclusion and Exclusion Criteria
2.3. Study Ethics
2.4. Measurements
2.5. Physical Fitness Tests
2.6. Statistical Analysis
3. Results
4. Discussion
4.1. Hypoxia and Reduced Strength in COVID-19 Survivors and OSAS Patients
4.2. Reduced Handgrip Strength as a Consequence of Loss of Muscle Mass
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Stavrou, V.T.; Astara, K.; Tourlakopoulos, K.N.; Papayianni, E.; Boutlas, S.; Vavougios, G.D.; Daniil, Z.; Gourgoulianis, K.I. Obstructive Sleep Apnea Syndrome: The Effect of Acute and Chronic Responses of Exercise. Front. Med. 2021, 8, 806924. [Google Scholar] [CrossRef]
- Labarca, G.; Gower, J.; Lamperti, L.; Dreyse, J.; Jorquera, J. Chronic intermittent hypoxia in obstructive sleep apnea: A narrative review from pathophysiological pathways to a precision clinical approach. Sleep Breath 2020, 24, 751–760. [Google Scholar] [CrossRef] [PubMed]
- Nitsure, M.; Sarangi, B.; Shankar, G.H.; Reddy, V.S.; Walimbe, A.; Sharma, V.; Prayag, S. Mechanisms of Hypoxia in COVID-19 Patients: A Pathophysiologic Reflection. Indian J. Crit. Care Med. 2020, 24, 967–970. [Google Scholar] [CrossRef] [PubMed]
- Meesters, J.; Conijn, D.; Vermeulen, H.M.; Vliet Vlieland, T. Physical activity during hospitalization: Activities and preferences of adults versus older adults. Physiother. Theory Pract. 2019, 35, 975–985. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Dirks, M.L.; Wall, B.T.; van de Valk, B.; Holloway, T.M.; Holloway, G.P.; Chabowski, A.; Goossens, G.H.; van Loon, L.J. One Week of Bed Rest Leads to Substantial Muscle Atrophy and Induces Whole-Body Insulin Resistance in the Absence of Skeletal Muscle Lipid Accumulation. Diabetes 2016, 65, 2862–2875. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Savino, E.; Sioulis, F.; Guerra, G.; Cavalieri, M.; Zuliani, G.; Guralnik, J.M.; Volpato, S. Potential Prognostic Value of Handgrip Strength in Older Hospitalized Patients. J. Frailty Aging 2012, 1, 32–38. [Google Scholar] [CrossRef] [PubMed]
- Craig, J.C.; Broxterman, R.M.; Cerbie, J.F.; La Salle, D.T.; Roundy, C.S.; Jarrett, C.L.; Richardson, R.S.; Trinity, J.D. The dynamic adjustment of mean arterial pressure during exercise: A potential tool for discerning cardiovascular health status. J. Appl. Physiol. 2021, 130, 1544–1554. [Google Scholar] [CrossRef] [PubMed]
- Stavrou, V.T.; Tourlakopoulos, K.N.; Vavougios, G.D.; Papayianni, E.; Kiribesi, K.; Maggoutas, S.; Nikolaidis, K.; Fradelos, E.V.; Dimeas, I.; Daniil, Z.; et al. Eight weeks unsupervised pulmonary rehabilitation in previously hospitalized of SARS-CoV-2 infection. J. Pers. Med. 2021, 11, 806. [Google Scholar] [CrossRef] [PubMed]
- Stavrou, V.T.; Vavougios, G.D.; Astara, K.; Siachpazidou, D.I.; Papayianni, E.; Gourgoulianis, K.I. The 6-Minute Walk Test and Anthropometric Characteristics as Assessment Tools in Patients with Obstructive Sleep Apnea Syndrome. A Preliminary Report during the Pandemic. J. Pers. Med. 2021, 11, 563. [Google Scholar] [CrossRef]
- Holland, A.E.; Spruit, M.A.; Troosters, T.; Puhan, M.A.; Pepin, V.; Saey, D.; McCormack, M.C.; Carlin, B.W.; Sciurba, F.C.; Pitta, F.; et al. An official European Respiratory Society/American Thoracic Society technical standard: Field walking tests in chronic respiratory disease. Eur. Respir. J. 2014, 44, 1428–1446. [Google Scholar] [CrossRef] [PubMed]
- Stavrou, V.T.; Astara, K.; Daniil, Z.; Gourgoulianis, K.I.; Kalabakas, K.; Karagiannis, D.; Basdekis, G. The reciprocal association between fitness indicators and sleep quality in the context of recent sport injury. Int. J. Environ. Res. Public Health 2020, 17, 4810. [Google Scholar] [CrossRef] [PubMed]
- Stavrou, V.; Vavougios, G.D.; Bardaka, F.; Karetsi, E.; Daniil, Z.; Gourgoulianis, K.I. The effect of exercise training on the quality of sleep in national-level adolescent finswimmers. Sports Med. Open 2019, 5, 34. [Google Scholar] [CrossRef] [PubMed]
- Jones, M.W. Daytime sleepiness, snoring and obstructive sleep apnea. The Epworth Sleepiness Scale. Chest 1993, 103, 30–36. [Google Scholar]
- European Union Law. Available online: https://europa.eu/european-union/law_en (accessed on 30 August 2021).
- ATS Committee on Proficiency Standards for Clinical Pulmonary Function Laboratories. ATS statement: Guidelines for the six-minute walk test. Am. J. Respir. Crit. Care Med. 2002, 166, 111–117. [Google Scholar] [CrossRef]
- Borg, E.; Borg, G.; Larsson, K.; Letzter, M.; Sundblad, B.M. An index for breathlessness and leg fatigue. Scand. J. Med. Sci. Sports 2010, 20, 644–650. [Google Scholar] [CrossRef] [PubMed]
- Ross, R.M.; Murthy, J.N.; Wollak, I.D.; Jackson, A.S. The six minute walk test accurately estimates mean peak oxygen uptake. BMC Pulm. Med. 2010, 10, 31. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Stavrou, V.; Vavougios, G.; Karetsi, E.; Adam, G.; Daniil, Z.; Gourgoulianis, K.I. Evaluation of respiratory parameters in finswimmers regarding gender, swimming style and distance. Respir. Physiol. Neurobiol. 2018, 254, 30–31. [Google Scholar] [CrossRef]
- George, P.M.; Barratt, S.L.; Condliffe, R.; Desai, S.R.; Devaraj, A.; Forrest, I.; Gibbons, M.A.; Hart, N.; Jenkins, R.G.; McAuley, D.F.; et al. Respiratory follow-up of patients with COVID-19 pneumonia. Thorax 2020, 75, 1009–1016. [Google Scholar] [CrossRef] [PubMed]
- Connors, J.M.; Levy, J.H. COVID-19 and its implications for thrombosis and anticoagulation. Blood 2020, 135, 2033–2040. [Google Scholar] [CrossRef] [PubMed]
- Cui, N.; Zou, X.; Xu, L. Preliminary CT findings of coronavirus disease 2019 (COVID-19). Clin. Imaging 2020, 65, 124–132. [Google Scholar] [CrossRef] [PubMed]
- Zhang, X.; Wang, F.; Shen, Y.; Zhang, X.; Cen, Y.; Wang, B.; Zhao, S.; Zhou, Y.; Hu, B.; Wang, M.; et al. Symptoms and Health Outcomes Among Survivors of COVID-19 Infection 1 Year After Discharge From Hospitals in Wuhan, China. JAMA Netw. Open 2021, 4, e2127403. [Google Scholar] [CrossRef]
- Dewan, N.A.; Nieto, F.J.; Somers, V.K. Intermittent hypoxemia and OSA: Implications for comorbidities. Chest 2015, 147, 266–274. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Vavougios, G.D.; George, D.G.; Pastaka, C.; Zarogiannis, S.G.; Gourgoulianis, K.I. Phenotypes of comorbidity in OSAS patients: Combining categorical principal component analysis with cluster analysis. J. Sleep Res. 2016, 25, 31–38. [Google Scholar] [CrossRef]
- Koren, D.; Chirinos, J.A.; Katz, L.E.; Mohler, E.R.; Gallagher, P.R.; Mitchell, G.F.; Marcus, C.L. Interrelationships between obesity, obstructive sleep apnea syndrome and cardiovascular risk in obese adolescents. Int. J. Obes. 2015, 39, 1086–1093. [Google Scholar] [CrossRef] [Green Version]
- Goyal, P.; Ringel, J.B.; Rajan, M.; Choi, J.J.; Pinheiro, L.C.; Li, H.A.; Wehmeyer, G.T.; Alshak, M.N.; Jabri, A.; Schenck, E.J.; et al. Obesity and COVID-19 in New York City: A Retrospective Cohort Study. Ann. Intern. Med. 2020, 173, 855–858. [Google Scholar] [CrossRef] [PubMed]
- Simonnet, A.; Chetboun, M.; Poissy, J.; Raverdy, V.; Noulette, J.; Duhamel, A.; Labreuche, J.; Mathieu, D.; Pattou, F.; Jourdain, M. LICORN and the Lille COVID-19 and Obesity study group. High Prevalence of Obesity in Severe Acute Respiratory Syndrome Coronavirus-2 (SARS-CoV-2) Requiring Invasive Mechanical Ventilation. Obesity 2020, 28, 1195–1199. [Google Scholar] [CrossRef]
- Dixon, A.E.; Peters, U. The effect of obesity on lung function. Expert Rev. Respir. Med. 2018, 12, 755–767. [Google Scholar] [CrossRef] [PubMed]
- Coker, R.H.; Wolfe, R.R. Bedrest and sarcopenia. Curr. Opin. Clin. Nutr. Metab. Care 2012, 15, 7–11. [Google Scholar] [CrossRef] [PubMed]
- Ikezoe, T.; Mori, N.; Nakamura, M.; Ichihashi, N. Effects of age and inactivity due to prolonged bed rest on atrophy of trunk muscles. Eur. J. Appl. Physiol. 2012, 112, 43–48. [Google Scholar] [CrossRef] [PubMed]
- Santilli, V.; Bernetti, A.; Mangone, M.; Paoloni, M. Clinical definition of sarcopenia. Clin. Cases Miner. Bone Metab. 2014, 11, 177–180. [Google Scholar] [CrossRef]
- Welch, C.; Greig, C.; Masud, T.; Wilson, D.; Jackson, T.A. COVID-19 and Acute Sarcopenia. Aging Dis. 2020, 11, 1345–1351. [Google Scholar] [CrossRef] [PubMed]
- Kirwan, R.; McCullough, D.; Butler, T.; Perez de Heredia, F.; Davies, I.G.; Stewart, C. Sarcopenia during COVID-19 lockdown restrictions: Long-term health effects of short-term muscle loss. Geroscience 2020, 42, 1547–1578. [Google Scholar] [CrossRef] [PubMed]
- Piotrowicz, K.; Gąsowski, J.; Michel, J.P.; Veronese, N. Post-COVID-19 acute sarcopenia: Physiopathology and management. Aging Clin. Exp. Res. 2021, 33, 2887–2898. [Google Scholar] [CrossRef] [PubMed]
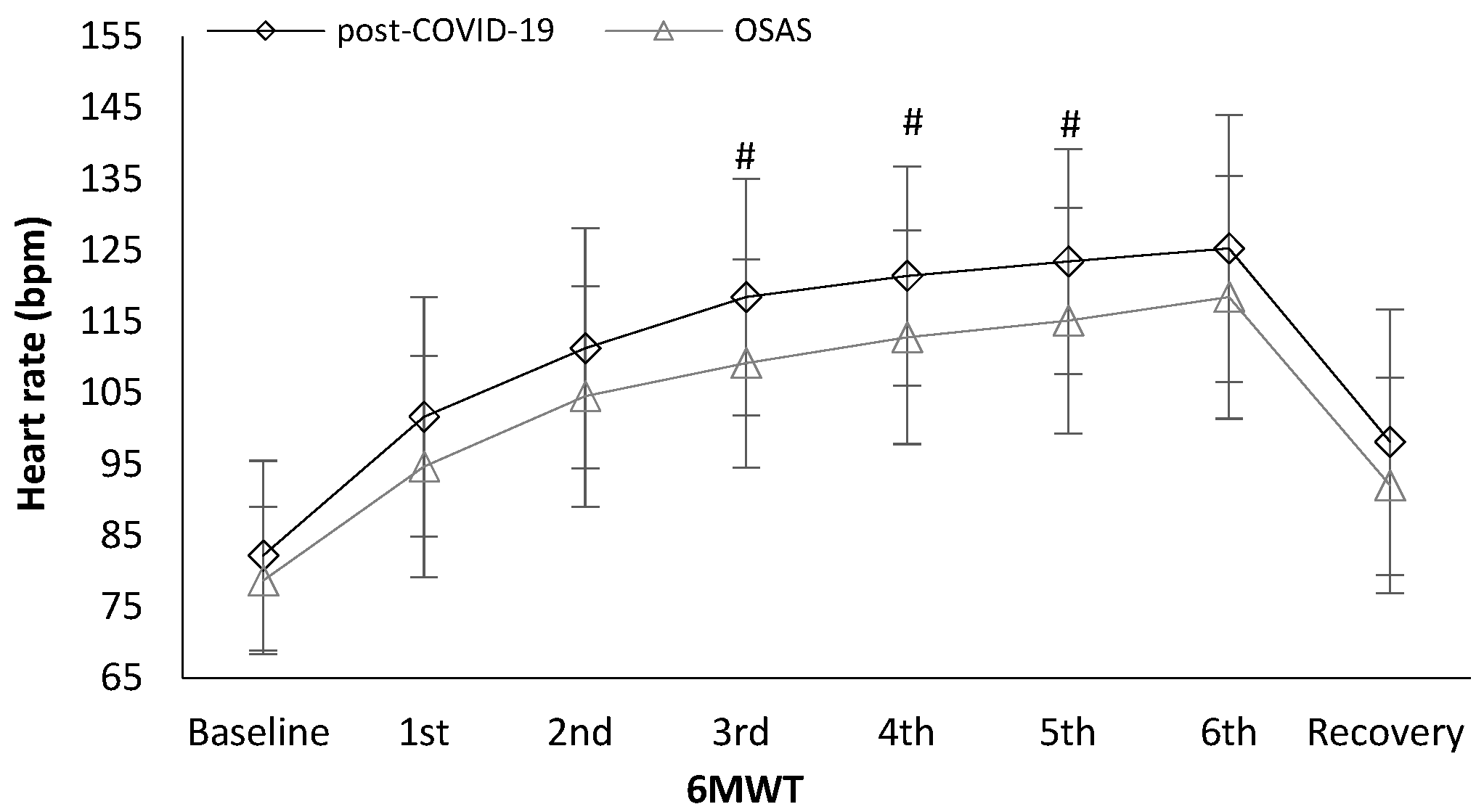
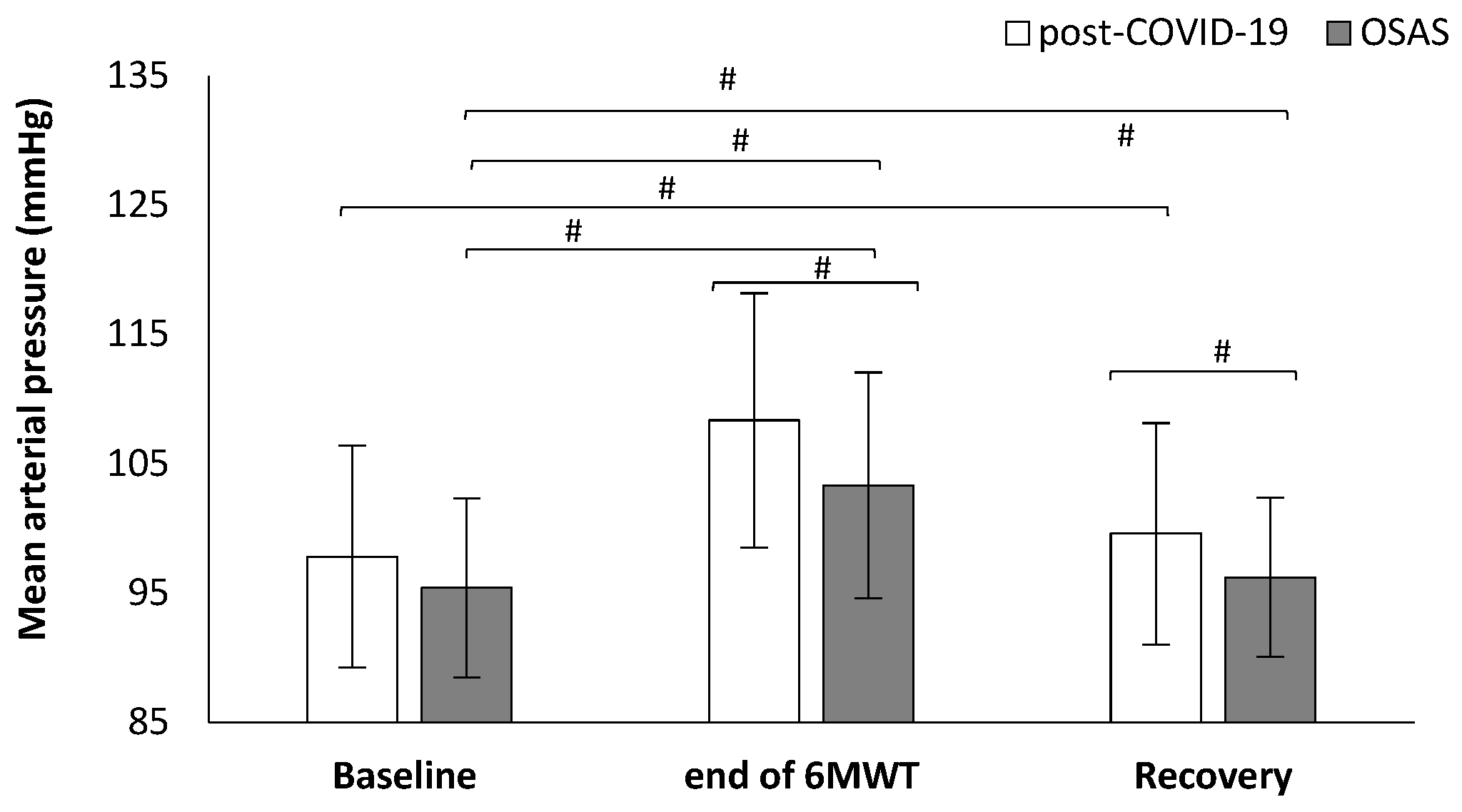



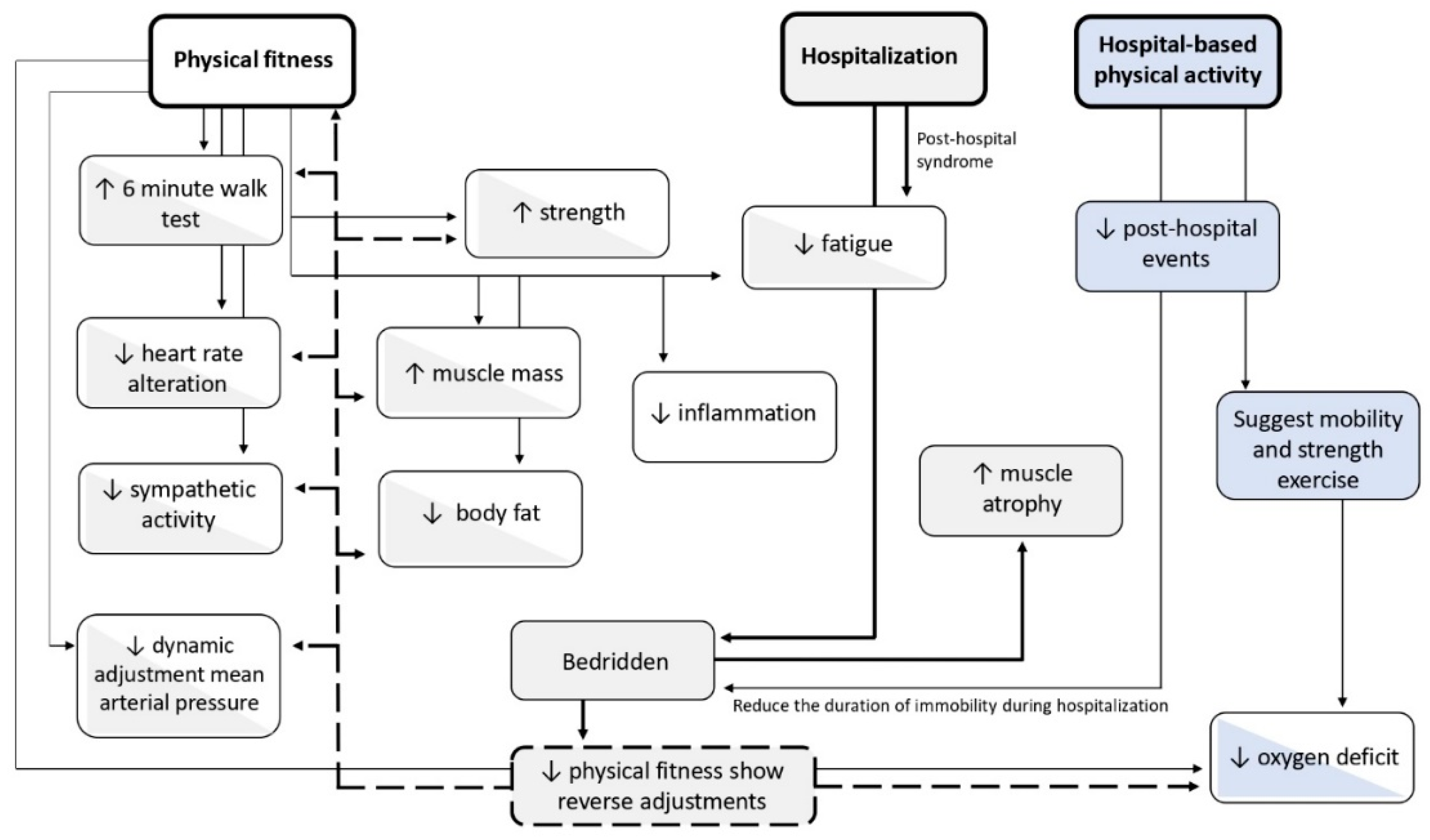
| Post-COVID-19 | OSAS | p-Value | |
|---|---|---|---|
| Age, yrs | 51.7 ± 6.5 | 48.3 ± 9.5 | 0.072 |
| Gender, F/M | 7/33 | 7/33 | - |
| Body mass, kg | 90.2 ± 13.0 | 101.9 ± 19.9 | 0.002 |
| Body mass index, kg/m2 | 29.7 ± 4.3 | 33.2 ± 6.3 | 0.005 |
| Body surface area, m2 | 2.2 ± 0.4 | 2.5 ± 0.5 | 0.004 |
| Body fat, % | 30.3 ± 9.0 | 34.0 ± 9.1 | 0.069 |
| Muscle mass, kg | 31.5 ± 4.6 | 30.1 ± 4.7 | 0.155 |
| Visceral fat, score | 12.5 ± 3.7 | 15.0 ± 5.6 | 0.024 |
| Lean body mass, kg | 64.1 ± 6.5 | 69.1 ± 9.1 | 0.006 |
| Total body water, % | 48.2 ± 9.1 | 46.9 ± 8.8 | 0.529 |
| Neck circumference, cm | 40.9 ± 9.3 | 41.1 ± 4.2 | 0.914 |
| Waist–hip ratio | 1.0 ± 0.1 | 1.0 ± 0.1 | 0.416 |
| Δchest | 6.6 ± 3.0 | 6.3 ± 1.7 | 0.676 |
| Post-COVID-19 | OSAS | p-Value | |
|---|---|---|---|
| Distance, m | 525.6 ± 120.6 | 449.7 ± 61.0 | 0.001 |
| Distance, % of predicted | 88.0 ± 18.6 | 76.5 ± 12.9 | 0.002 |
| Estimated VO2peak, ml/min/kg | 17.0 ± 2.8 | 15.3 ± 1.4 | 0.001 |
| Metabolic equivalent | 4.9 ± 0.8 | 4.4 ± 0.4 | 0.001 |
| Leg Fatigue, Borg scale | |||
| Baseline | 0.4 ± 0.8 | 0.8 ± 0.9 | 0.085 |
| End of 6MWT | 1.3 ± 1.3 | 1.3 ± 1.2 | 0.928 |
| Dyspnea, Borg scale | |||
| Baseline | 0.5 ± 0.9 | 0.9 ± 1.1 | 0.108 |
| End of 6MWT | 1.6 ± 1.7 | 1.4 ± 1.3 | 0.607 |
| 95% C.I.for EXP(B) | ||||||||
|---|---|---|---|---|---|---|---|---|
| B | S.E. | Wald | df | Sig. | Exp(B) | Lower | Upper | |
| Handgrip, kg | −0.135 | 0.039 | 12.114 | 1 | 0.001 | 0.874 | 0.810 | 0.943 |
| Body fat, % | −0.077 | 0.034 | 5.001 | 1 | 0.025 | 0.926 | 0.866 | 0.991 |
| METs | 2.496 | 0.640 | 15.205 | 1 | 0.000 | 12.135 | 3.461 | 45.552 |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Stavrou, V.T.; Vavougios, G.D.; Boutlas, S.; Tourlakopoulos, K.N.; Papayianni, E.; Astara, K.; Stavrou, I.T.; Daniil, Z.; Gourgoulianis, K.I. Physical Fitness Differences, Amenable to Hypoxia-Driven and Sarcopenia Pathophysiology, between Sleep Apnea and COVID-19. Int. J. Environ. Res. Public Health 2022, 19, 669. https://doi.org/10.3390/ijerph19020669
Stavrou VT, Vavougios GD, Boutlas S, Tourlakopoulos KN, Papayianni E, Astara K, Stavrou IT, Daniil Z, Gourgoulianis KI. Physical Fitness Differences, Amenable to Hypoxia-Driven and Sarcopenia Pathophysiology, between Sleep Apnea and COVID-19. International Journal of Environmental Research and Public Health. 2022; 19(2):669. https://doi.org/10.3390/ijerph19020669
Chicago/Turabian StyleStavrou, Vasileios T., George D. Vavougios, Stylianos Boutlas, Konstantinos N. Tourlakopoulos, Eirini Papayianni, Kyriaki Astara, Ilias T. Stavrou, Zoe Daniil, and Konstantinos I. Gourgoulianis. 2022. "Physical Fitness Differences, Amenable to Hypoxia-Driven and Sarcopenia Pathophysiology, between Sleep Apnea and COVID-19" International Journal of Environmental Research and Public Health 19, no. 2: 669. https://doi.org/10.3390/ijerph19020669
APA StyleStavrou, V. T., Vavougios, G. D., Boutlas, S., Tourlakopoulos, K. N., Papayianni, E., Astara, K., Stavrou, I. T., Daniil, Z., & Gourgoulianis, K. I. (2022). Physical Fitness Differences, Amenable to Hypoxia-Driven and Sarcopenia Pathophysiology, between Sleep Apnea and COVID-19. International Journal of Environmental Research and Public Health, 19(2), 669. https://doi.org/10.3390/ijerph19020669









