Changes in Collective Efficacy’s Preventive Effect on Intimate Partner Violence during the COVID-19 Pandemic
Abstract
:1. Introduction
1.1. Association between Collective Efficacy and the Incidence of IPV
1.2. Association between Changes in Collective Efficacy and Changes in IPV
1.3. Purpose of the Study
2. Materials and Methods
2.1. Procedure
2.2. Participants
2.3. Measures
2.4. Analysis
3. Results
3.1. Univariate LGM
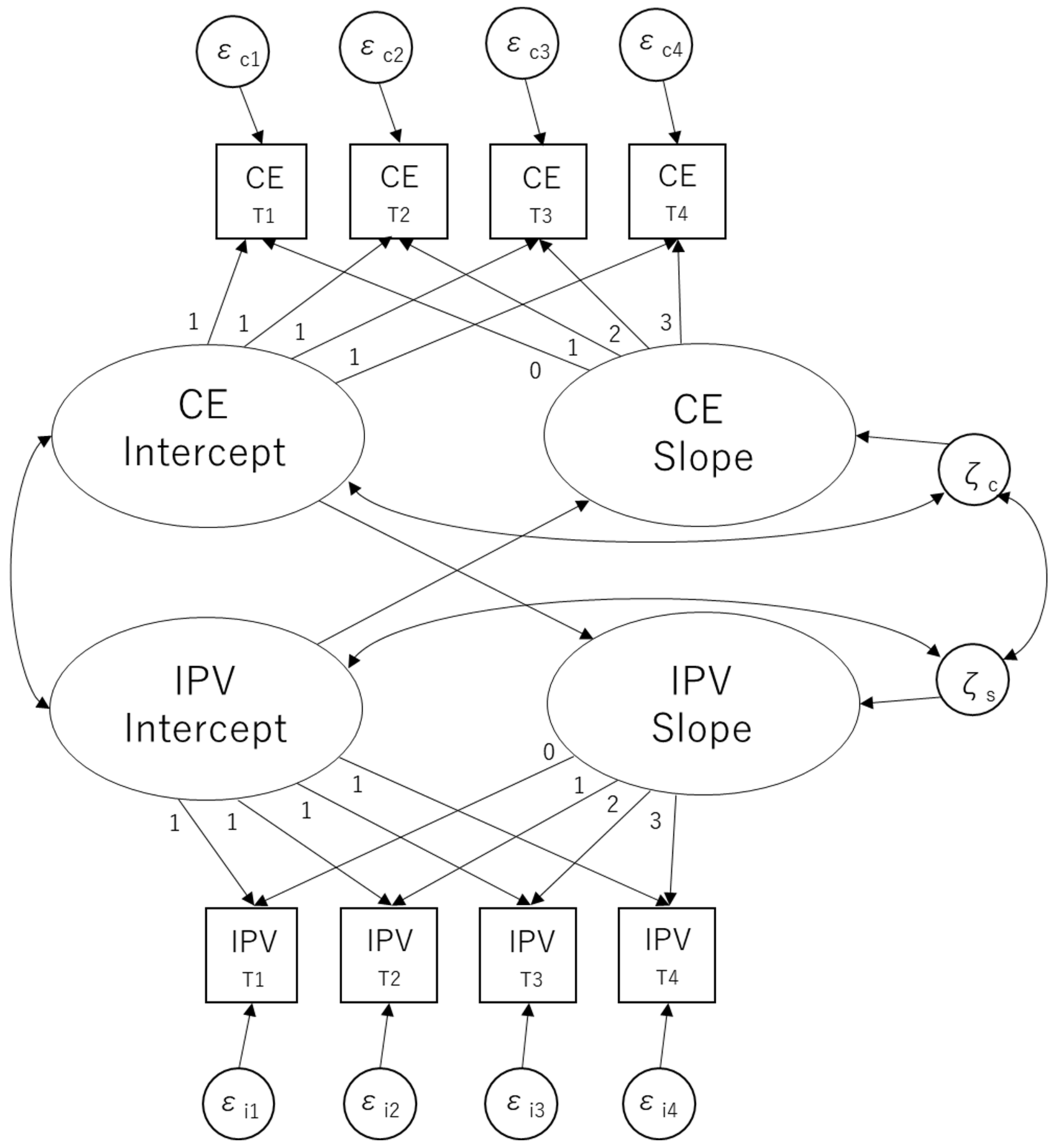
3.2. Parallel LGM
4. Discussion
4.1. Effects of Pre-Pandemic Collective Efficacy on Changes in IPV
4.2. Relationship between Changes in Collective Efficacy and IPV
4.3. Strengths and Limitations
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Van Gelder, N.; Peterman, A.; Potts, A.; O’Donnell, M.; Thompson, K.; Shah, N.; Oertelt-Prigione, S. COVID-19: Reducing the Risk of Infection Might Increase the Risk of Intimate Partner Violence. EClinicalMedicine 2020, 21, 100348. [Google Scholar] [CrossRef] [PubMed]
- Mojahed, A.; Brym, S.; Hense, H.; Grafe, B.; Helfferich, C.; Lindert, J.; Garthus-Niegel, S. Rapid Review on the Associations of Social and Geographical Isolation and Intimate Partner Violence: Implications for the Ongoing COVID-19 Pandemic. Front. Psychiatry 2021, 12, 578150. [Google Scholar] [CrossRef] [PubMed]
- Pattojoshi, A.; Sidana, A.; Garg, S.; Mishra, S.N.; Singh, L.K.; Goyal, N.; Tikka, S.K. Staying Home Is NOT ‘Staying Safe’: A Rapid 8-Day Online Survey on Spousal Violence against Women during the COVID-19 Lockdown in India. Psychiatry Clin. Neurosci. 2021, 75, 64–66. [Google Scholar] [CrossRef]
- Parrott, D.J.; Halmos, M.B.; Stappenbeck, C.A.; Moino, K. Intimate Partner Aggression during the COVID-19 Pandemic: Associations with Stress and Heavy Drinking. Psychol Violence 2021, 12, 95–103. [Google Scholar] [CrossRef] [PubMed]
- Chiaramonte, D.; Simmons, C.; Hamdan, N.; Ayeni, O.O.; López-Zerón, G.; Farero, A.; Sprecher, M.; Sullivan, C.M. The Impact of COVID-19 on the Safety, Housing Stability, and Mental Health of Unstably Housed Domestic Violence Survivors. J. Community Psychol. 2021, 50, 2659–2681. [Google Scholar] [CrossRef] [PubMed]
- Tierolf, B.; Geurts, E.; Steketee, M. Domestic Violence in Families in the Netherlands during the Coronavirus Crisis: A Mixed Method Study. Child Abuse Negl. 2021, 116, 104800. [Google Scholar] [CrossRef]
- Capinha, M.; Guinote, H.; Rijo, D. Intimate Partner Violence Reports During the COVID-19 Pandemic First Year in Portuguese Urban Areas: A Brief Report. J. Fam. Violence 2021, 37, 871–880. [Google Scholar] [CrossRef]
- Gender Equality Bureau Cabinet Office. Survey on Violence between Men and Women. Available online: https://www.gender.go.jp/policy/no_violence/e-vaw/chousa/h11_top.html (accessed on 24 July 2022).
- Japan’s National Police Agency. Stalking, Domestic Violence, etc. Available online: https://www.npa.go.jp/publications/statistics/safetylife/dv.html (accessed on 24 July 2022).
- Sampson, R.J.; Raudenbush, S.W.; Earls, F.; Taylor, D.J. Neighborhoods and Violent Crime: A Multilevel Study of Collective Efficacy. Science 1997, 277, 918–924. [Google Scholar] [CrossRef]
- Yoshizawa, H.; Yoshida, T.; Harada, C.; Unagami, T.; Park, H.; Nakajima, M.; Ozeki, M. Effects of Neighborhood Collective Efficacy and Violence on Antisocial Behavior: Dual Mediation of Socialization and Routine Activities. Jpn. J. Psychol. 2009, 80, 33–41. [Google Scholar] [CrossRef] [Green Version]
- Yoshizawa, H.; Ozeki, M. Cross-Cultural Protective Effects of Neighborhood Collective Efficacy on Antisocial Behaviors: Mediating Role of Social Information Processing. Jpn. Psychol. Res. 2020, 62, 116–130. [Google Scholar] [CrossRef]
- Browning, C.R. The Span of Collective Efficacy: Extending Social Disorganization Theory to Partner Violence. J. Marriage Fam. 2002, 64, 833–850. [Google Scholar] [CrossRef]
- Jackson, A.L. The Combined Effect of Women’s Neighborhood Resources and Collective Efficacy on IPV. J. Marriage Fam. 2016, 78, 890–907. [Google Scholar] [CrossRef]
- Jain, S.; Buka, S.L.; Subramanian, S.V.; Molnar, B.E. Neighborhood Predictors of Dating Violence Victimization and Perpetration in Young Adulthood: A Multilevel Study. Am. J. Public Health 2010, 100, 1737–1744. [Google Scholar] [CrossRef] [PubMed]
- Edwards, K.M.; Mattingly, M.J.; Dixon, K.J.; Banyard, V.L. Community Matters: Intimate Partner Violence among Rural Young Adults. Am. J. Community Psychol. 2014, 53, 198–207. [Google Scholar] [CrossRef] [PubMed]
- Wright, E.M.; Benson, M.L. Clarifying the Effects of Neighborhood Context on Violence “Behind Closed Doors. Justice Q. 2011, 28, 775–798. [Google Scholar] [CrossRef]
- Alderton, A.; Henry, N.; Foster, S.; Badland, H. Examining the Relationship between Urban Liveability and Gender-Based Violence: A Systematic Review. Health Place 2020, 64, 102365. [Google Scholar] [CrossRef]
- Fay-Ramirez, S.; Antrobus, E.; Piquero, A.R. Assessing the Effect of the Queensland “Summer of Disasters” on Perceptions of Collective Efficacy. Soc. Sci. Res. 2015, 54, 21–35. [Google Scholar] [CrossRef] [Green Version]
- Davidson Arad, B.; Mcleigh, J.D.; Katz, C. Perceived Collective Efficacy and Parenting Competence: The Roles of Quality of Life and Hope. Fam. Process 2020, 59, 273–287. [Google Scholar] [CrossRef]
- Dekeseredy, W.S.; Schwartz, M.D.; Alvi, S.; Tomaszewski, E.A. Perceived Collective Efficacy and Women’s Victimization in Public Housing. Crim. Justice 2003, 3, 5–27. [Google Scholar] [CrossRef] [Green Version]
- Paat, Y.F.; Hope, T.L.; Mangadu, T.; Núñez-Mchiri, G.G.; Chavez-Baray, S.M. Family- and Community-Related Determinants of Intimate Partner Violence among Mexican and Puerto Rican Origin Mothers in Fragile Families. Womens Stud. Int. Forum. 2017, 62, 136–147. [Google Scholar] [CrossRef]
- Banyard, V.L.; Cross, C.; Modecki, K.L. Interpersonal Violence in Adolescence: Ecological Correlates of Self-Reported Perpetration. J. Interpers. Violence 2006, 21, 1314–1332. [Google Scholar] [CrossRef] [PubMed]
- Banyard, V.L.; Rizzo, A.J.; Edwards, K.M. Community Actionists: Understanding Adult Bystanders to Sexual and Domestic Violence Prevention in Communities. Psychol. Violence 2020, 10, 531–541. [Google Scholar] [CrossRef] [PubMed]
- Burrmann, U.; Mutz, M.; Sielschott, S.; Braun, S. Social Capital Trends in Germany in the Face of the Covid-19 Pandemic: A Research Note. Front. Polit. Sci. 2022, 4, 1–7. [Google Scholar] [CrossRef]
- Yu, B.; Luo, M.; Liu, M.; Zhou, J.; Yang, S.; Jia, P. Social Capital Changes After COVID-19 Lockdown Among Youths in China: COVID-19 Impact on Lifestyle Change Survey (COINLICS). Front. Public Health 2021, 9, 1–8. [Google Scholar] [CrossRef] [PubMed]
- Luo, M.; Zhang, D.; Shen, P.; Yin, Y.; Yang, S.; Jia, P. COVID-19 Lockdown and Social Capital Changes Among Youths in China. Int. J. Health Policy Manag. 2021, 1–6. [Google Scholar] [CrossRef] [PubMed]
- Lochner, K.; Kawachi, I.; Kennedy, B.P. Social Capital: A Guide to Its Measurement. Health Place 1999, 5, 259–270. [Google Scholar] [CrossRef] [Green Version]
- Drakulich, K.M. Social Capital and Collective Efficacy. In Encyclopedia of Criminology and Criminal Justice; Bruinsma, G., Weisburd, D., Eds.; Springer: New York, NY, USA, 2014; pp. 4891–4899. ISBN 978-1-4614-5690-2. [Google Scholar]
- Tunçgenç, B.; El Zein, M.; Sulik, J.; Newson, M.; Zhao, Y.; Dezecache, G.; Deroy, O. Social Influence Matters: We Follow Pandemic Guidelines Most When Our Close Circle Does. Br. J. Psychol. 2021, 112, 763–780. [Google Scholar] [CrossRef]
- Tabernero, C.; Castillo-Mayén, R.; Luque, B.; Cuadrado, E. Social Values, Self- and Collective Efficacy Explaining Behaviours in Coping with COVID-19: Self-Interested Consumption and Physical Distancing in the First 10 Days of Confinement in Spain. PLoS ONE 2020, 15, e0238682. [Google Scholar] [CrossRef]
- Muniz-Terrera, G.; Robitaille, A.; Kelly, A.; Johansson, B.; Hofer, S.; Piccinin, A. Latent Growth Models Matched to Research Questions to Answer Questions about Dynamics of Change in Multiple Processes. J. Clin. Epidemiol. 2017, 82, 158–166. [Google Scholar] [CrossRef] [Green Version]
- Maniaci, M.R.; Rogge, R.D. Caring about Carelessness: Participant Inattention and Its Effects on Research. J. Res. Pers. 2014, 48, 61–83. [Google Scholar] [CrossRef]
- Krosnick, J.A. Response Strategies for Coping with the Cognitive Demands of Attitude Measures in Surveys. Appl. Cogn. Psychol. 1991, 5, 213–236. [Google Scholar] [CrossRef]
- Miura, A.; Kobayashi, T. Exploring Tips to Detect” Satisficing” in an Online Survey: A Study Using University Student Samples. Res. Soc. Psychol. 2016, 32, 123–132. [Google Scholar] [CrossRef]
- Gau, J.M. Unpacking Collective Efficacy: The Relationship between Social Cohesion and Informal Social Control. Crim. Justice Stud. 2014, 27, 210–225. [Google Scholar] [CrossRef]
- Heid, A.R.; Pruchno, R.; Cartwright, F.P.; Wilson-Genderson, M. Exposure to Hurricane Sandy, Neighborhood Collective Efficacy, and Post-Traumatic Stress Symptoms in Older Adults. Aging Ment. Health 2017, 21, 742–750. [Google Scholar] [CrossRef] [PubMed]
- Morgan, G.B.; Hodge, K.J.; Wells, K.E.; Watkins, M.W. Are Fit Indices Biased in Favor of Bi-Factor Models in Cognitive Ability Research?: A Comparison of Fit in Correlated Factors, Higher-Order, and Bi-Factor Models via Monte Carlo Simulations. J. Intell. 2015, 3, 2–20. [Google Scholar] [CrossRef] [Green Version]
- Grunst, M.L.; Grunst, A.S.; Pinxten, R.; Eens, G.; Eens, M. An Experimental Approach to Investigating Effects of Artificial Light at Night on Free-Ranging Animals: Implementation, Results, and Directions for Future Research. J. Vis. Exp. 2022, 2022, 53–60. [Google Scholar] [CrossRef]
- Kenny, D.A. Measuring Model Fit. Available online: http://www.davidakenny.net/cm/fit.htm (accessed on 23 September 2022).
- Fernández-González, L.; Wekerle, C.; Goldstein, A.L. Measuring Adolescent Dating Violence: Development of’conflict in Adolescent Dating Relationships Inventory(CADRI) Short Form. Adv. Adolesc. Mental Health 2012, 11, 35–54. [Google Scholar] [CrossRef]
- Enders, C.K. Analyzing Structural Equation Models with Missing Data. In Structural Equation Modeling: A Second Course, 2nd ed.; Quantitative methods in education and the behavioral sciences: Issues, research, and teaching; Hancock, G.R., Mueller, R.O., Eds.; IAP Information Age Publishing: Charlotte, NC, USA, 2013; pp. 493–519. ISBN 978-1-62396-244-9. [Google Scholar]
| Mean | SD | α | 1 | 2 | 3 | 4 | 5 | 6 | 7 | 8 | 9 | 10 | 11 | ||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| 1 | IPV-T1 | 1.25 | 0.45 | 0.90 | |||||||||||
| 2 | IPV-T2 | 1.32 | 0.60 | 0.95 | 0.45 ** | ||||||||||
| 3 | IPV-T3 | 1.26 | 0.48 | 0.92 | 0.38 ** | 0.42 ** | |||||||||
| 4 | IPV-T4 | 1.22 | 0.47 | 0.94 | 0.32 ** | 0.33 ** | 0.33 ** | ||||||||
| 5 | Informal social control-T1 | 2.78 | 0.88 | 0.88 | 0.07 | −0.08 | −0.14 * | −0.14 | |||||||
| 6 | Informal social control-T2 | 2.62 | 0.92 | 0.92 | 0.09 | 0.15 * | 0.16 * | 0.14 * | 0.43 ** | ||||||
| 7 | Informal social control-T3 | 2.49 | 0.98 | 0.91 | 0.01 | −0.01 | 0.07 | −0.08 | 0.33 ** | 0.43 ** | |||||
| 8 | Informal social control-T4 | 2.53 | 0.94 | 0.89 | −0.02 | 0.04 | 0.11 | 0.07 | 0.33 ** | 0.48 ** | 0.43 ** | ||||
| 9 | Social cohesion and trust-T1 | 2.56 | 0.91 | 0.94 | 0.12 * | 0.02 | −0.08 | −0.04 | 0.45 ** | 0.35 ** | 0.38 ** | 0.33 ** | |||
| 10 | Social cohesion and trust-T2 | 2.64 | 0.91 | 0.95 | 0.11 | 0.16 ** | 0.15 * | 0.14 * | 0.36 ** | 0.61 ** | 0.32 ** | 0.38 ** | 0.56 ** | ||
| 11 | Social cohesion and trust-T3 | 2.47 | 0.96 | 0.95 | 0.08 | −0.04 | 0.05 | −0.05 | 0.24 ** | 0.34 ** | 0.58 ** | 0.35 ** | 0.47 ** | 0.52 ** | |
| 12 | Social cohesion and trust-T4 | 2.50 | 0.89 | 0.94 | 0.02 | 0.09 | 0.03 | 0.07 | 0.35 ** | 0.45 ** | 0.35 ** | 0.48 ** | 0.53 ** | 0.64 ** | 0.63 ** |
| Intercept | SE | p | Slope | SE | p | Correlation between intercept and slope | p | χ2 | df | p | CFI | TLI | RMSEA | SRMR | |
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| IPV | 1.28 | 0.03 | 0.00 | 0.00 | 0.01 | 0.87 | −0.38 | 0.02 | 11.74 | 5.00 | 0.04 | 0.96 | 0.95 | 0.07 | 0.04 |
| Informal social control | 2.75 | 0.05 | 0.00 | −0.08 | 0.02 | 0.00 | −0.25 | 0.22 | 8.12 | 5.00 | 0.15 | 0.98 | 0.98 | 0.04 | 0.05 |
| Social cohesion and trust | 2.59 | 0.05 | 0.00 | −0.02 | 0.02 | 0.24 | −0.17 | 0.27 | 7.00 | 5.00 | 0.22 | 0.99 | 0.99 | 0.04 | 0.02 |
| Estimates | SE | p | |||||
|---|---|---|---|---|---|---|---|
| Model 1. Model for informal social control and IPV | |||||||
| Intercept | IPV | → | Slope | Informal social control | −0.07 | 0.07 | 0.30 |
| Informal social control | → | IPV | −0.05 | 0.02 | 0.03 | ||
| Intercept | IPV | ↔ | Intercept | Informal social control | 0.04 | 0.02 | 0.10 |
| Intercept | IPV | ↔ | Slope | IPV | −0.01 | 0.01 | 0.24 |
| Informal social control | ↔ | Informal social control | −0.03 | 0.03 | 0.30 | ||
| Slope | IPV | ↔ | Slope | Informal social control | 0.01 | 0.00 | 0.00 |
| Model 2. Model for Social cohesion and trust and IPV | |||||||
| Intercept | IPV | → | Slope | Social cohesion and trust | −0.13 | 0.06 | 0.04 |
| Social cohesion and trust | → | IPV | −0.05 | 0.02 | 0.01 | ||
| Intercept | IPV | ↔ | Intercept | Social cohesion and trust | 0.06 | 0.02 | 0.01 |
| Intercept | IPV | ↔ | Slope | IPV | −0.01 | 0.01 | 0.29 |
| Social cohesion and trust | ↔ | Social cohesion and trust | −0.01 | 0.02 | 0.52 | ||
| Slope | IPV | ↔ | Slope | Social cohesion and trust | 0.01 | 0.00 | 0.01 |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Souma, T.; Komura, K.; Arai, T.; Shimada, T.; Kanemasa, Y. Changes in Collective Efficacy’s Preventive Effect on Intimate Partner Violence during the COVID-19 Pandemic. Int. J. Environ. Res. Public Health 2022, 19, 12849. https://doi.org/10.3390/ijerph191912849
Souma T, Komura K, Arai T, Shimada T, Kanemasa Y. Changes in Collective Efficacy’s Preventive Effect on Intimate Partner Violence during the COVID-19 Pandemic. International Journal of Environmental Research and Public Health. 2022; 19(19):12849. https://doi.org/10.3390/ijerph191912849
Chicago/Turabian StyleSouma, Toshihiko, Kentaro Komura, Takashi Arai, Takahito Shimada, and Yuji Kanemasa. 2022. "Changes in Collective Efficacy’s Preventive Effect on Intimate Partner Violence during the COVID-19 Pandemic" International Journal of Environmental Research and Public Health 19, no. 19: 12849. https://doi.org/10.3390/ijerph191912849
APA StyleSouma, T., Komura, K., Arai, T., Shimada, T., & Kanemasa, Y. (2022). Changes in Collective Efficacy’s Preventive Effect on Intimate Partner Violence during the COVID-19 Pandemic. International Journal of Environmental Research and Public Health, 19(19), 12849. https://doi.org/10.3390/ijerph191912849






