Use of Instant Messaging Software in a German Hospital—An Exploratory Investigation among Physicians
Abstract
1. Introduction
2. Materials and Methods
2.1. Participants and Procedure
2.2. Exploratory Questionnaire
2.3. Data Analysis
3. Results
3.1. Usage of Instant Messaging Software
3.2. Specific Use of Instant Messaging Software in Clinical Practice
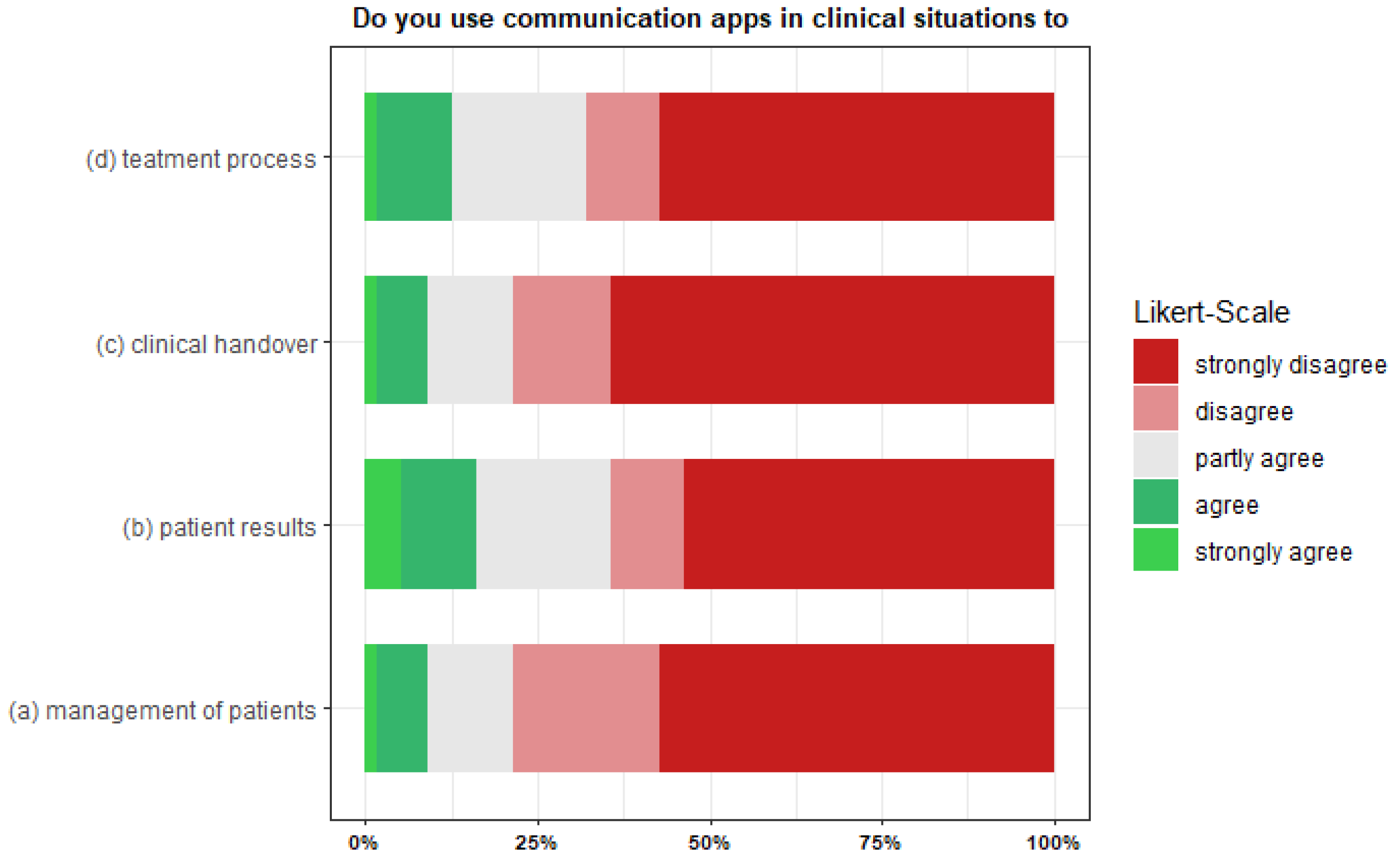
3.2.1. Purpose of Use
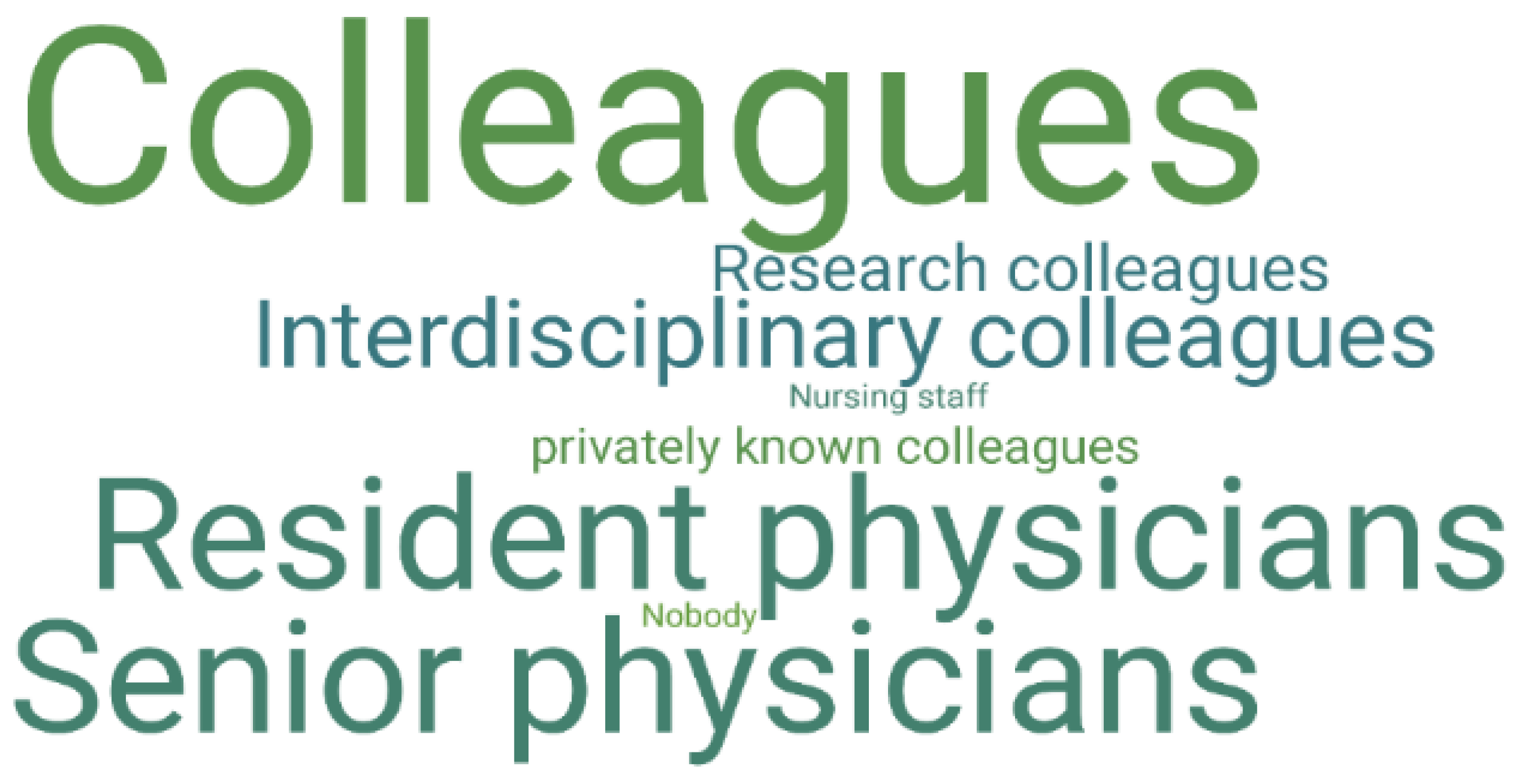
3.2.2. Interlocutors
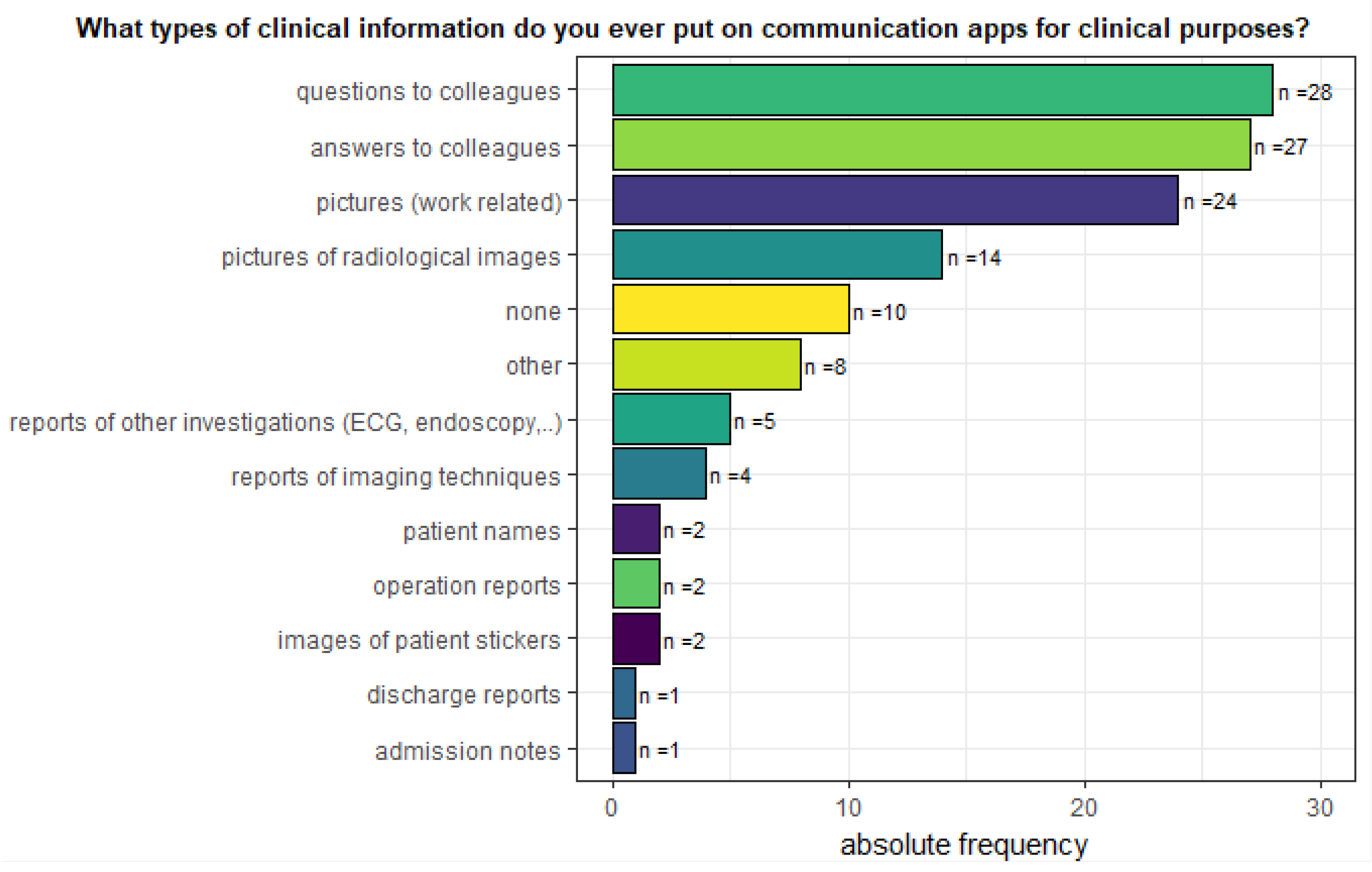
3.2.3. Sent Information
3.2.4. Group Chat Usage
3.2.5. Perceived Advantages and Barriers of Instant Messaging Software in Clinical Practice
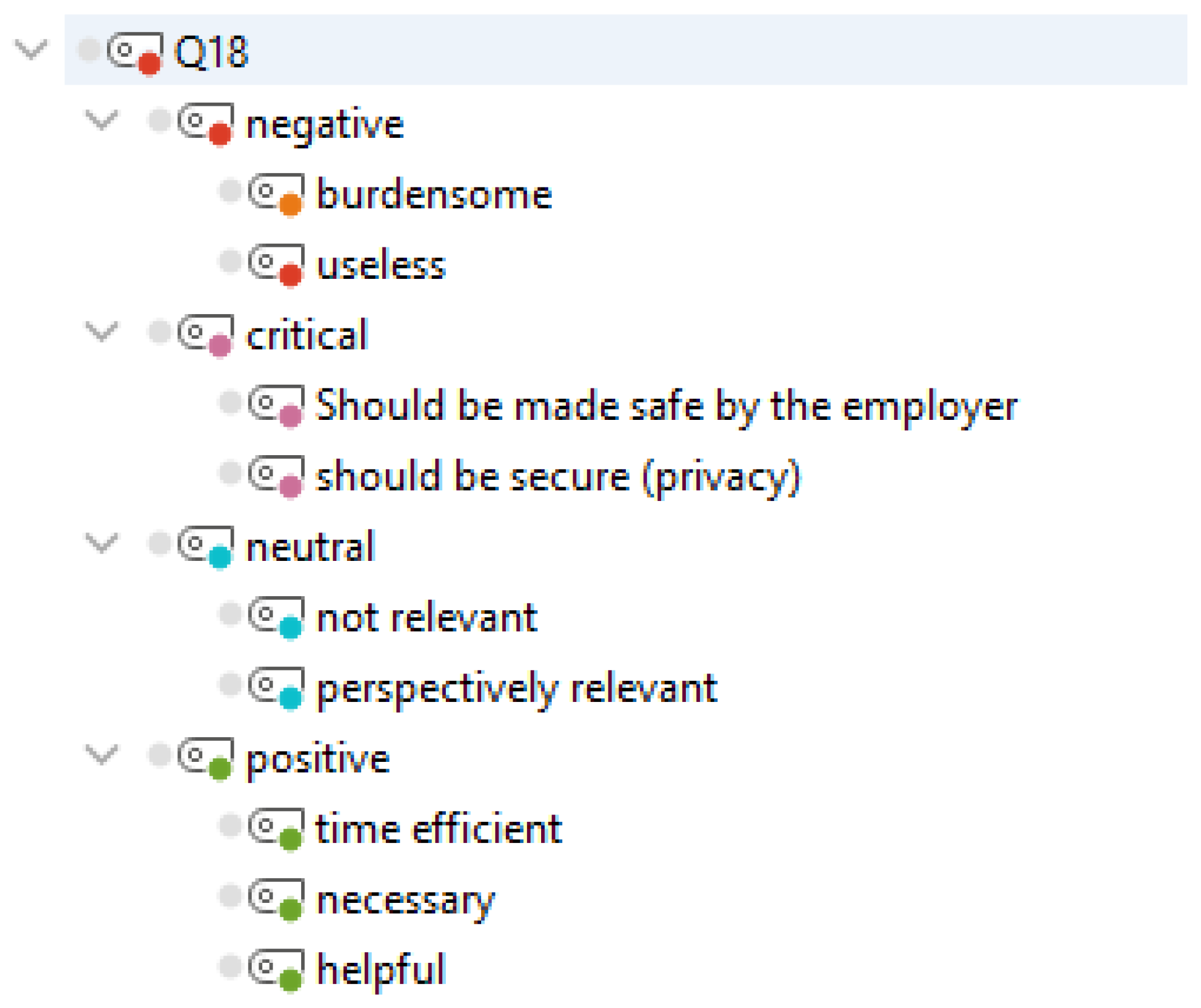
3.2.6. Usage Evaluation
3.3. Self-Reported Need for Media Competence Development
4. Discussion
4.1. General Discussion
4.2. Strengths and Limitations
4.3. Further Implications
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
Appendix A
| No. | Question | Possible Answer |
|---|---|---|
| 1 | How do you mainly communicate with your colleagues in your daily clinical routine? | Telephone|E-mail|Communication apps|Direct personal contact|SMS|Other |
| 2 | Do you use one or more of the following communication apps privately? | WhatsApp|Signal|Telegram|Snapchat|Discord|Facebook Messenger|Skype|Slack|Viber|Microsoft Teams|Threema|Ginglo (SIMSme)|Wire|WeChat|Line|Siilo|Zoom|Mattermost|Matrix|Other|I don’t use any communication apps |
| 3 | Do you use one or more of the following communication apps in your daily clinical routine? | WhatsApp|Signal|Telegram|Snapchat|Discord|Facebook Messenger|Skype|Slack|Viber|Microsoft Teams|Threema|Ginglo (SIMSme)|Wire|WeChat|Line|Siilo|Zoom|Mattermost|Matrix|Other|I don’t use any communication apps |
| 4 | Please indicate how many messages you send on average via communication apps in your daily clinical routine. | none|0–10|11–20|21–30|31–40|41–50| > 50 |
| 5 | Please indicate how many messages you receive on average via communication apps in your daily clinical routine. | none|0–10|11–20|21–30|31–40|41–50| > 50 |
| 6 | Do you use communication apps in clinical situations to
| 5-Point scale from “strongly disagree” to “strongly agree” |
| 7 | What do you use communication apps for in your daily clinical routine? | Free text answer |
| 8 | With whom do you communicate via communication apps in the daily clinic routine? | Free text answer |
| 9 | In which situations do you use communication apps in your daily clinical routine? | Free text answer |
| 10 | Are you in one or more communication apps in a “group” that primarily consists of a work team? (e.g., “ENT doctors ward...”; “Stroke Unit Team”;...) | yes/no |
| 11 | In how many clinic-related “groups” are you in the communication app? | Number |
| 12 | I communicate regularly in clinic-related |
|
| 13 | I communicate via communication apps with
| very rarely|rarely|occasionally|often|very often |
| 14 | What types of clinical information do you ever put on communication apps for clinical purposes? (You can choose more than 1 response) |
|
| 15 | I have sent the following other clinical information via a communication app | Free text answer |
| 16 | What do you see as the benefits of using communication apps in your daily clinical practice? | Free text answer |
| 17 | What challenges do you see in using communication apps in everyday clinical practice? | Free text answer |
| 18 | How do you evaluate the use of communication apps in everyday clinical practice? | Free text answer |
| 19 | What support requirements do you see for yourself personally with regard to your own digital media competence? | Free text answer |
References
- Blumenfeld, O.; Brand, R. Real Time Medical Learning Using the WhatsApp Cellular Network: A Cross Sectional Study Following the Experience of a Division’s Medical Officers in the Israel Defense Forces. Disaster Mil. Med. 2016, 2, 12. [Google Scholar] [CrossRef] [PubMed]
- Woods, J.; Moorhouse, M.; Knight, L. A Descriptive Analysis of the Role of a WhatsApp Clinical Discussion Group as a Forum for Continuing Medical Education in the Management of Complicated HIV and TB Clinical Cases in a Group of Doctors in the Eastern Cape, South Africa. S. Afr. J. HIV Med. 2019, 20, 982. [Google Scholar] [CrossRef] [PubMed]
- Borges do Nascimento, I.J.; de Queiroz Oliveira, J.A.; Souza Wolff, I.; Defensor Ribeiro, L.; Souza e Silva, M.V.R.; Silva Cardoso, C.; Mars, M.; Ribeiro, A.L.; Soriano Marcolino, M. Use of smartphone-based instant messaging services in medical practice: A cross-sectional study. Sao Paulo Med. J. 2020, 138, 86–92. [Google Scholar] [CrossRef] [PubMed]
- von Lutterotti, N. Wenn der Arzt am Smartphone klebt. Frankfurter Allgemeine Zeitung, 9 May 2018; 107. [Google Scholar]
- Albert, F. Sicher Chatten im Krankenhaus. Available online: https://www.bibliomedmanager.de/fw/artikel/37598-sicher-chatten-im-krankenhaus (accessed on 26 August 2022).
- Datenschutzgrundverordnung: Ärzte Sollten Sichere WhatsApp-Alternativen Nutzen. Available online: https://www.aerzteblatt.de/nachrichten/95118/Datenschutzgrundverordnung-Aerzte-sollten-sichere-WhatsApp-Alternativen-nutzen (accessed on 28 August 2022).
- Datenschutzkonferenz. “Whitepaper” der Konferenz der Unabhängigen Datenschutzaufsichtsbehörden des Bundes und der Länder—07.11.2019. Available online: https://www.datenschutzkonferenz-online.de/media/oh/20191106_whitepaper_messenger_krankenhaus_dsk.pdf (accessed on 26 August 2022).
- Rose, M.; Hofhues, S.; Sayegh-Jodehl, S.; Müller-Birn, C. DocTalk Dialog trifft Chatbot: Kollaborierendes Lernen & Lehren für Ärzt*innen im Prozess der Arbeit. Available online: https://www.qualifizierungdigital.de/qualifizierungdigital/shareddocs/projekte/de/projektdatenbank/01pg20002.html (accessed on 26 August 2022).
- Mattermost Inc. Mattermost; Mattermost Inc.: Palo Alto, CA, USA, 2022. [Google Scholar]
- Microsoft Teams. Available online: https://www.microsoft.com/de-de/microsoft-teams/free?market=de (accessed on 20 September 2022).
- Slack Technologies. Available online: https://slack.com/intl/de-de (accessed on 20 September 2022).
- Harris, P.A.; Taylor, R.; Thielke, R.; Payne, J.; Gonzalez, N.; Conde, J.G. Research Electronic Data Capture (REDCap): A Metadata-Driven Methodology and Workflow Process for Providing Translational Research Informatics Support. J. Biomed. Inform. 2009, 42, 377–381. [Google Scholar] [CrossRef] [PubMed]
- Harris, P.A.; Taylor, R.; Minor, B.L.; Elliott, V.; Fernandez, M.; O’Neal, L.; McLeod, L.; Delacqua, G.; Delacqua, F.; Kirby, J.; et al. The REDCap Consortium: Building an International Community of Software Platform Partners. J. Biomed. Inform. 2019, 95, 103208. [Google Scholar] [CrossRef] [PubMed]
- Nikolic, A.; Wickramasinghe, N.; Claydon-Platt, D.; Balakrishnan, V.; Smart, P. The Use of Communication Apps by Medical Staff in the Australian Health Care System: Survey Study on Prevalence and Use. JMIR Med. Inform. 2018, 6, e9526. [Google Scholar] [CrossRef] [PubMed]
- R Core Team. R: A Language and Environment for Statistical Computing. Available online: https://www.R-project.org (accessed on 25 August 2022).
- Wickham, H. Ggplot2: Elegant Graphics for Data Analysis; Springer: New York, NY, USA, 2009; ISBN 978-0-387-98141-3. [Google Scholar]
- Verbi Software. MAXQDA 2022. Available online: https://www.maxqda.com (accessed on 25 August 2022).
- Silver, C.; Lewins, A. Computer Assisted Qualitative Data Analysis. In International Encyclopedia of Education, 3rd ed.; Peterson, P., Baker, E., McGaw, B., Eds.; Elsevier: Oxford, UK, 2010; pp. 326–334. ISBN 978-0-08-044894-7. [Google Scholar]
- Microsoft Excel. Available online: https://www.microsoft.com (accessed on 30 August 2022).
- Sayegh-Jodehl, S.; Mukowski-Kickhöfel, R.; Gocke, P. Digitalisierung: Messengerdienste Im Klinikalltag. Dtsch. Arztebl. 2022, 119, 371–372. [Google Scholar]
- Schütze, D.; Engler, F.; Nohl-Deryk, P.; Müller, B.; Müller, A. Implementierung einer Secure Instant Messaging-App in der COVID-19 Pandemie: Nutzungserfahrungen von Hausärzt*innen und Mitarbeiter*innen von Gesundheitsämtern. Z. Evidenz Fortbild. Qual. Gesundh. 2022, 2013, 40–48. [Google Scholar] [CrossRef]
- Krefting, D. Digitale Transformation: Neues Tempo Nutzen. Dtsch. Arztebl. Int. 2021, 118, 2437–2438. [Google Scholar]
- Ebert, H. Medienkompetenz. In Praxishandbuch Berufliche Schlüsselkompetenzen; Becker, J.H., Ebert, H., Pastoors, S., Eds.; Springer: Berlin/Heidelberg, Germany, 2018; pp. 125–132. ISBN 978-3-662-54925-4. [Google Scholar]
- Bauer, R.; Hafer, J.; Hofhues, S.; Schiefner-Rohs, S.; Thillosen, A.; Volk, B.; Wannemacher, K. Mythen, Realitäten und Perspektiven rund um Digitalisierung. In Vom E-Learning zur Digitalisierung. Mythen, Realitäten, Perspektiven; Bauer, R., Hafer, J., Hofhues, S., Schiefner-Rohs, M., Thillosen, A., Volk, B., Wannemacher, K., Eds.; Waxmann: Münster, Germany, 2020; pp. 12–22. ISBN 978-3-8309-4109-5. [Google Scholar]
- Gematik GmbH. Über uns. Available online: https://www.gematik.de/ueber-uns (accessed on 20 September 2022).
- Hodgson, M. Germany’s National Healthcare System Adopts Matrix! Available online: https://matrix.org/blog/2021/07/21/germanys-national-healthcare-system-adopts-matrix (accessed on 26 August 2022).
- TI-Messenger—Ihr Einstieg in die Anwendung für das interoperable Instant Messaging im Gesundheitswesen. Available online: https://fachportal.gematik.de/anwendungen/ti-messenger (accessed on 25 August 2022).
- Kumar, R.; Tripathi, R. Secure Healthcare Framework Using Blockchain and Public Key Cryptography. In Blockchain Cybersecurity, Trust and Privacy; Choo, K.R., Dehghantanha, A., Parizi, R.M., Eds.; Springer: Cham, Switzerland, 2020; pp. 185–202. ISBN 978-3-030-38181-3. [Google Scholar]
- Morris, C.; Scott, R.E.; Mars, M. WhatsApp in Clinical Practice—The Challenges of Record Keeping and Storage. A Scoping Review. Int. J. Environ. Res. Public Health 2021, 18, 13426. [Google Scholar] [CrossRef] [PubMed]
- Yu, Z.; Liu, Y.; Yu, Y.; Han, H.; Li, Y. The Study on Public-Interest Short Message Service (SMS) in China during the COVID-19 Pandemic: Mobile User Survey and Content Analysis. Int. J. Environ. Res. Public Health 2021, 18, 7915. [Google Scholar] [CrossRef] [PubMed]


| Item | Possible Answers |
|---|---|
| How do you mainly communicate with your colleagues in your daily clinical routine? | Telephone|E-mail|Communication apps|Direct personal contact|SMS|Other |
| Do you use one or more of the following communication apps privately|in your daily clinical routine? | WhatsApp|Signal|Telegram|Snapchat|Discord|Facebook Messenger|Skype|Slack|Viber|Microsoft Teams|Threema|Ginglo (SIMSme)|Wire|WeChat|Line|Siilo|Zoom|Mattermost|Matrix|Other|I don’t use any communication apps |
| Please indicate how many messages you send|receive on average via communication apps in your daily clinic routine. | none|0–10|11–20|21–30|31–40|41–50| > 50 |
Do you use communication apps in clinical situations to
| 5-Point scale from “strongly disagree” to “strongly agree” |
| What do you see as the benefits|challenges of using communication apps in your daily clinical practice? | free text answer |
| No. | Question | Possible Answer | N = x/70 |
|---|---|---|---|
| Q7. | What do you use communication apps for in your daily clinical routine? | Free text answer | 45 |
| Q8. | With whom do you communicate via communication apps in the daily clinic routine? | Free text answer | 42 |
| Q9. | In which situations do you use communication apps in your daily clinical routine? | Free text answer | 33 |
| Q15. | I have sent the following other clinical information via a communication app | Free text answer | 7 |
| Q16. | What do you see as the benefits of using communication apps in your daily clinical practice? | Free text answer | 50 |
| Q17. | What challenges do you see in using communication apps in everyday clinical practice? | Free text answer | 51 |
| Q18. | How do you evaluate the use of communication apps in everyday clinical practice? | Free text answer | 49 |
| Q19. | What support requirements do you see for yourself personally with regard to your own digital media competence? | Free text answer | 34 |
| Functionality | Functions | No Benefits | |||
|---|---|---|---|---|---|
| Code | x/50 | Code | x/50 | Code | x/50 |
| fast | 27 | exchange with colleagues | 8 | unnecessary/none | 10 |
| uncomplicated/simple | 12 | accessibility of a group | 7 | distracting | 3 |
| asynchronous response option | 9 | Video telephony | 7 | ||
| with high availability | 7 | sending pictures | 6 | ||
| Bridging of spatial distance | 4 | Share screen | 5 | ||
| effective | 4 | memory for information | 4 | ||
| reliable | 3 | Sending text | 3 | ||
| less disturbing | 3 | Transmission of findings | 3 | ||
| interdisciplinary exchange | 2 | ||||
| accessibility of the background service | 2 | ||||
| Document Number | Segment | Code/Sub Code |
|---|---|---|
| 131 | “Good should be made more” | positive |
| 44 | “Practical and labor saving when used professionally” | positive/helpful |
| oa_132 | “Helpful and time efficient” | positive/time efficient |
| oa_37 | “Meanwhile indispensable” | positive/necessary |
| 27 | “not very relevant at the moment” | neutral |
| 86 | “neutral” | neutral |
| 31 | “Great potential, but currently critical due to lack of software adapted to legal framework conditions and lack of implementation by management level --> Frequently either (data protection) legally critical use or corresponding restraint and non-use.” | neutral/not yet relevant critical/should make employer safe critical/should be safe (data protection) |
| 119 | “If there was a secure app established at Charité, I would like to use the path more and see great potential here.” | neutral/perspective relevant critical/should be safe (data protection) |
| oa_75 | “Critical, it is essential that patient rights and data protection are preserved.” | critical/should be safe (data protection), |
| 99 | “additional channel that needs to be “checked”” | negative |
| “bad” | negative |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Sayegh-Jodehl, S.; Mukowski-Kickhöfel, R.; Linke, D.; Müller-Birn, C.; Rose, M. Use of Instant Messaging Software in a German Hospital—An Exploratory Investigation among Physicians. Int. J. Environ. Res. Public Health 2022, 19, 12618. https://doi.org/10.3390/ijerph191912618
Sayegh-Jodehl S, Mukowski-Kickhöfel R, Linke D, Müller-Birn C, Rose M. Use of Instant Messaging Software in a German Hospital—An Exploratory Investigation among Physicians. International Journal of Environmental Research and Public Health. 2022; 19(19):12618. https://doi.org/10.3390/ijerph191912618
Chicago/Turabian StyleSayegh-Jodehl, Sabine, Rebecca Mukowski-Kickhöfel, Diane Linke, Claudia Müller-Birn, and Matthias Rose. 2022. "Use of Instant Messaging Software in a German Hospital—An Exploratory Investigation among Physicians" International Journal of Environmental Research and Public Health 19, no. 19: 12618. https://doi.org/10.3390/ijerph191912618
APA StyleSayegh-Jodehl, S., Mukowski-Kickhöfel, R., Linke, D., Müller-Birn, C., & Rose, M. (2022). Use of Instant Messaging Software in a German Hospital—An Exploratory Investigation among Physicians. International Journal of Environmental Research and Public Health, 19(19), 12618. https://doi.org/10.3390/ijerph191912618






