Improving COVID-19 Vaccine Uptake among Black Populations: A Systematic Review of Strategies
Abstract
1. Introduction
2. Materials and Methods
2.1. Inclusion Criteria
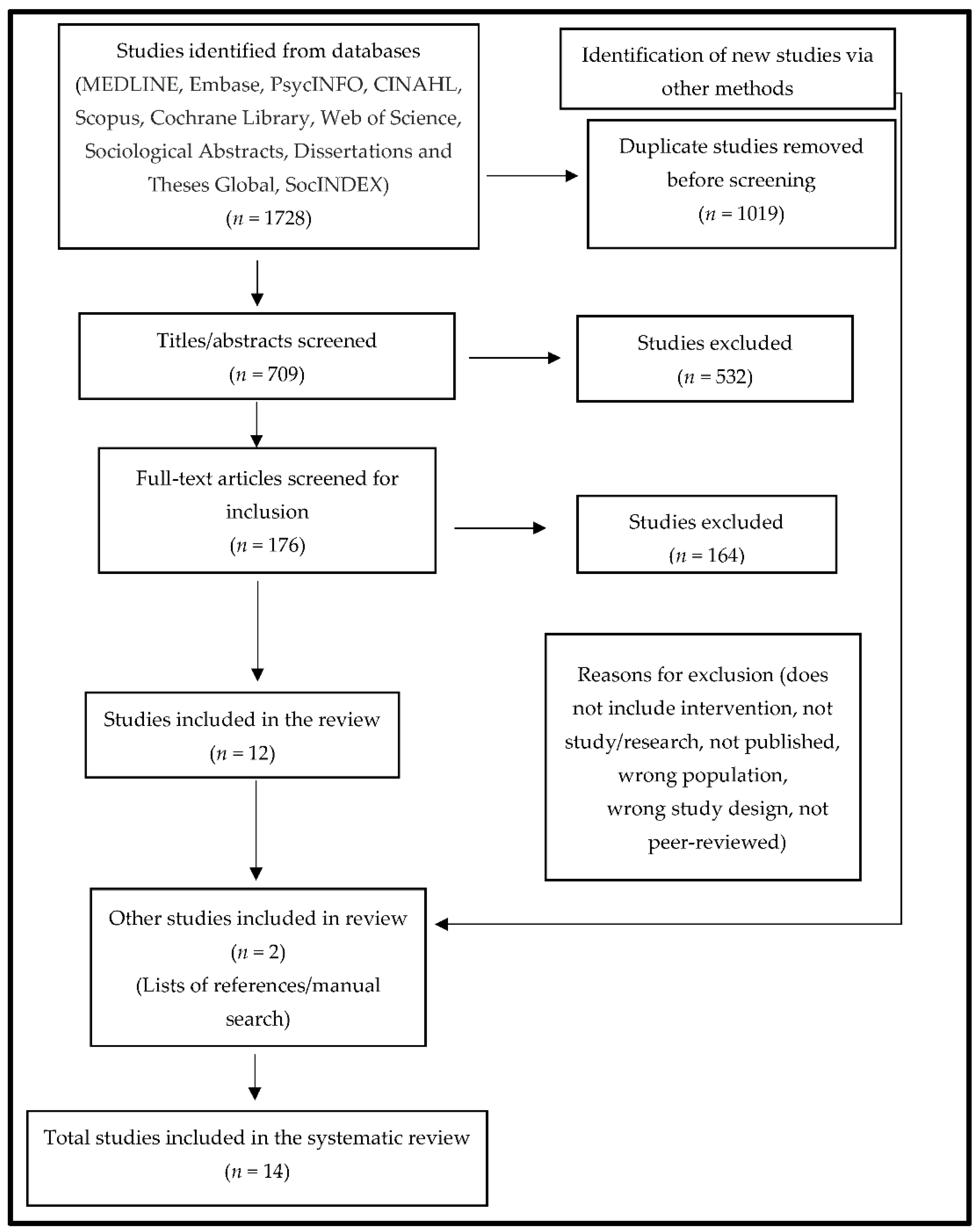
2.2. Search Strategy
2.3. Data Extraction
2.4. Quality Assessment
2.5. Data Synthesis
3. Results
3.1. Quality Appraisal
3.2. Communication- and Information-Based Interventions
3.3. Mandate-Based Interventions
3.4. Incentive-Based Interventions
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- World Health Organization (WHO). WHO Coronavirus (COVID-19) Dashboard. Available online: https://covid19.who.int (accessed on 20 May 2022).
- Millett, G.A.; Jones, A.T.; Benkeser, D.; Baral, S.; Mercer, L.; Beyrer, C.; Honermann, B.; Lankiewicz, E.; Mena, L.; Crowley, J.S.; et al. Assessing differential impacts of COVID-19 on black communities. Ann. Epidemiol. 2020, 47, 37–44. [Google Scholar] [CrossRef] [PubMed]
- Wadhera, R.K.; Wadhera, P.; Gaba, P.; Figueroa, J.F.; Maddox, K.E.J.; Yeh, R.W.; Shen, C. Variation in COVID-19 Hospitalizations and Deaths Across New York City Boroughs. JAMA 2020, 323, 2192–2195. [Google Scholar] [CrossRef] [PubMed]
- Mude, W.; Oguoma, V.M.; Nyanhanda, T.; Mwanri, L.; Njue, C. Racial disparities in COVID-19 pandemic cases, hospitalisations, and deaths: A systematic review and meta-analysis. J. Glob. Health 2021, 11, 05015. [Google Scholar] [CrossRef] [PubMed]
- Yancy, C.W. COVID-19 and African Americans. JAMA 2020, 323, 1891–1892. [Google Scholar] [CrossRef]
- Bowden, O.; Cain, P. Black Neighbourhoods in Toronto Are Hit Hardest by COVID-19 and It’s ‘Anchored in Racism’: Experts. Global News. 2020. Available online: https://globalnews.ca/news/7015522/Black-neighbourhoods-torontocoronavirusracism/ (accessed on 25 January 2022).
- Denice, P.; Choi, K.H.; Haan, M.; Zajacova, A. Visualizing the Geographic and Demographic Distribution of COVID-19. Socius Sociol. Res. Dyn. World 2020, 6, 2378023120948715. [Google Scholar]
- Guttmann, A.; Gandhi, S.; Wanigaratne, S.; Lu, H.; Ferreira-Legere, L.E.; Paul, J.; Gozdyra, P.; Campbell, T.; Chung, H.; Fung, K.; et al. COVID-19 in Immigrants, Refugees and Other Newcomers in Ontario: Characteristics of Those Tested and Those Confirmed Positive, as of June 13, 2020; ICES: Toronto, ON, Canada, 2020. [Google Scholar]
- City of Toronto, COVID 19: Ethno-Racial Identity & Income. 2022. Available online: https://www.toronto.ca/home/covid-19/covid-19-pandemic-data/covid-19-ethno-racial-group-income-infection-data/ (accessed on 20 May 2022).
- Szilagyi, P.G.; Thomas, K.; Shah, M.D.; Vizueta, N.; Cui, Y.; Vangala, S.; Kapteyn, A. National Trends in the US Public’s Likelihood of Getting a COVID-19 Vaccine—April 1 to December 8, 2020. JAMA 2021, 325, 396–398. [Google Scholar] [CrossRef] [PubMed]
- Nguyen, L.H.; Joshi, A.D.; Drew, D.A.; Merino, J.; Ma, W.; Lo, C.H.; Kwon, S.; Wang, K.; Graham, M.S.; Polidori, L.; et al. Racial and ethnic differences in COVID-19 vaccine hesitancy and uptake. medRxiv 2021. [Google Scholar] [CrossRef]
- Innovative Research Group, African Canadian Civic Engagement Council (ACCEC), and Black Opportunity Fund. COVID-19 Vaccine Confidence: Black Canadian Perspectives. 2021. Available online: https://innovativeresearch.ca/wp-content/uploads/2021/07/Black-Canadian-Vaccine-Confidence-FULL-REPORT-2021-07-07 (accessed on 25 January 2022).
- Ndugga, N.; Hill, L.; Artiga, S.; Haldar, S. Latest Data on COVID-19 Vaccinations by Race/Ethnicity; Kaiser Family Foundation (KFF): San Francisco, CA, USA, 2022. [Google Scholar]
- Stern, J.A.; Barbarin, O.; Cassidy, J. Working toward anti-racist perspectives in attachment theory, research, and practice. Attach. Hum. Dev. 2022, 24, 392–422. [Google Scholar] [CrossRef]
- Micco, E.; Gurmankin, A.D.; Armstrong, K. Differential willingness to undergo smallpox vaccination among African-American and white individuals. J. Gen. Intern. Med. 2004, 19, 451–455. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Prather, C.; Fuller, T.R.; Jeffries, W.L.; Marshall, K.J.; Howell, A.V.; Belyue-Umole, A.; King, W. Racism, African American Women, and Their Sexual and Reproductive Health: A Review of Historical and Contemporary Evidence and Implications for Health Equity. Health Equity 2018, 2, 249–259. [Google Scholar] [CrossRef] [PubMed]
- Sengupta, S.; Corbie-Smith, G.; Thrasher, A.; Strauss, R.P. African American elders’ perceptions of the influenza vaccine in Durham, North Carolina. N. C. Med. J. 2004, 65, 194–199. [Google Scholar] [CrossRef]
- Okoro, O.; Kennedy, J.; Simmons, G.; Vosen, E.C.; Allen, K.; Singer, D.; Scott, D.; Roberts, R. Exploring the Scope and Dimensions of Vaccine Hesitancy and Resistance to Enhance COVID-19 Vaccination in Black Communities. J. Racial. Ethn. Health Disparities 2021, 1–14. [Google Scholar] [CrossRef]
- Woko, C.; Siegel, L.; Hornik, R. An Investigation of Low COVID-19 Vaccination Intentions among Black Americans: The Role of Behavioral Beliefs and Trust in COVID-19 Information Sources. J. Health Commun. 2020, 25, 819–826. [Google Scholar] [CrossRef]
- Ochieng, C.; Anand, S.; Mutwiri, G.; Szafron, M.; Alphonsus, K. Factors Associated with COVID-19 Vaccine Hesitancy among Visible Minority Groups from a Global Context: A Scoping Review. Vaccines 2021, 9, 1445. [Google Scholar] [CrossRef]
- Ruiz, J.B.; Bell, R.A. Predictors of intention to vaccinate against COVID-19: Results of a nationwide survey. Vaccine 2021, 39, 1080–1086. [Google Scholar] [CrossRef] [PubMed]
- Amoako, J.; MacEachen, E. Understanding the blended impacts of COVID-19 and systemic inequalities on sub-Saharan African immigrants in Canada. Can. J. Public Health 2021, 112, 862–866. [Google Scholar] [CrossRef]
- Chishinga, N.; Gandhi, N.R.; Onwubiko, U.N.; Telford, C.; Prieto, J.; Smith, S.; Chamberlain, A.T.; Khan, S.; Williams, S.; Khan, F.; et al. Characteristics and Risk Factors for Hospitalization and Mortality among Persons with COVID-19 in Atlanta Metropolitan Area. medRxiv 2020. [Google Scholar] [CrossRef]
- Wallis, C. Why Racism, Not Race Is a Risk Factor for Dying of COVID-19. Scientific American. 2020. Available online: https://www.scientificamerican.com/article/why-racism-not-race-is-a-risk-factor-for-dying-of-covid-191/ (accessed on 30 June 2022).
- Fridman, A.; Gershon, R.; Gneezy, A. COVID-19 and vaccine hesitancy: A longitudinal study. PLoS ONE 2021, 16, e0250123. [Google Scholar] [CrossRef]
- Bogart, L.M.; Dong, L.; Gandhi, P.; Klein, D.J.; Smith, T.L.; Ryan, S.; Ojikutu, B.O. COVID-19 Vaccine Intentions and Mistrust in a National Sample of Black Americans. J. Natl. Med. Assoc. 2021, 113, 599–611. [Google Scholar] [CrossRef] [PubMed]
- Kanyanda, S.; Markhof, Y.; Wollburg, P.; Zezza, A. Acceptance of COVID-19 vaccines in sub-Saharan Africa: Evidence from six national phone surveys. BMJ Open 2021, 11, e055159. [Google Scholar] [CrossRef]
- Robertson, E.; Reeve, K.S.; Niedzwiedz, C.L.; Moore, J.; Blake, M.; Green, M.; Katikireddi, S.V.; Benzeval, M.J. Predictors of COVID-19 vaccine hesitancy in the UK household longitudinal study. Brain, Behav. Immun. 2021, 94, 41–50. [Google Scholar] [CrossRef] [PubMed]
- Dula, J.; Mulhanga, A.; Nhanombe, A.; Cumbi, L.; Júnior, A.; Gwatsvaira, J.; Fodjo, J.; Villela, E.F.D.M.; Chicumbe, S.; Colebunders, R. COVID-19 Vaccine Acceptability and Its Determinants in Mozambique: An Online Survey. Vaccines 2021, 9, 828. [Google Scholar] [CrossRef] [PubMed]
- Lamptey, E.; Serwaa, D.; Appiah, A.B. A nationwide survey of the potential acceptance and determinants of COVID-19 vaccines in Ghana. Clin. Exp. Vaccine Res. 2021, 10, 183–190. [Google Scholar] [CrossRef] [PubMed]
- Padamsee, T.J.; Bond, R.M.; Dixon, G.N.; Hovick, S.R.; Na, K.; Nisbet, E.C.; Wegener, D.T.; Garrett, R.K. Changes in COVID-19 Vaccine Hesitancy Among Black and White Individuals in the US. JAMA Netw. Open 2022, 5, e2144470. [Google Scholar] [CrossRef]
- Moher, D.; Liberati, A.; Tetzlaff, J.; Altman, D.G.; PRISMA Group. Preferred reporting items for systematic reviews and meta-analyses: The PRISMA statement. PLoS Med. 2009, 6, e1000097. [Google Scholar] [CrossRef] [PubMed]
- Rethlefsen, M.L.; Kirtley, S.; Waffenschmidt, S.; Ayala, A.P.; Moher, D.; Page, M.J.; Koffel, J.B.; PRISMA-S Group. PRISMA-S: An extension to the PRISMA statement for reporting literature searches in systematic reviews. J. Med. Libr. Assoc. 2021, 109, 174–200. [Google Scholar] [CrossRef]
- Veritas Health Innovation. Covidence Systematic Review Software. 2020. Available online: https://www.covidence.org (accessed on 30 January 2021).
- Abdul-Mutakabbir, J.C.; Casey, S.; Jews, V.; King, A.; Simmons, K.; Hogue, M.D.; Belliard, J.C.; Peverini, R.; Veltman, J. A three-tiered approach to address barriers to COVID-19 vaccine delivery in the Black community. Lancet Glob. Health 2021, 9, e749–e750. [Google Scholar] [CrossRef]
- Albarracin, D.; Jung, H.; Song, W.; Tan, A.; Fishman, J. Rather than inducing psychological reactance, requiring vaccination strengthens intentions to vaccinate in US populations. Sci. Rep. 2021, 11, 20796. [Google Scholar] [CrossRef]
- Andrasik, M.P.; Broder, G.B.; Wallace, S.E.; Chaturvedi, R.; Michael, N.L.; Bock, S.; Beyrer, C.; Oseso, L.; Aina, J.; Lucas, J.; et al. Increasing Black, Indigenous and People of Color participation in clinical trials through community engagement and recruitment goal establishment. PLoS ONE 2021, 16, e0258858. [Google Scholar] [CrossRef] [PubMed]
- Feifer, R.A.; Bethea, L.; White, E.M. Racial Disparities in COVID-19 Vaccine Acceptance: Building Trust to Protect Nursing Home Staff & Residents. J. Am. Med. Dir. Assoc. 2021, 22, 1853–1855.e1. [Google Scholar] [PubMed]
- Fox, A.; Choi, Y. Does framing coronavirus in terms of disparities reduce or increase vaccine hesitancy? Health Serv. Res. 2021, 6, 85–86. [Google Scholar] [CrossRef]
- Hirshberg, J.S.; Huysman, B.C.; Oakes, M.C.; Cater, E.B.; Odibo, A.O.; Raghuraman, N.; Kelly, J.C. Offering onsite COVID-19 vaccination to high-risk obstetrical patients: Initial findings. Am. J. Obstet. Gynecol. MFM 2021, 3. [Google Scholar] [CrossRef]
- Reddy, D.L.; Dangor, Z.; Lala, N.; Johnstone, J.; Maswabi, L.; Tsitsi, J.M.L. COVID-19 mass vaccination campaign for healthcare workers in a low-resource setting: A clinician-driven initiative. S. Afr. Med. J. 2021, 111, 610. [Google Scholar] [CrossRef]
- Reddy, K.P.; Fitzmaurice, K.P.; Scott, J.A.; Harling, G.; Lessells, R.J.; Panella, C.; Shebl, F.M.; Freedberg, K.A.; Siedner, M.J. Clinical outcomes and cost-effectiveness of COVID-19 vaccination in South Africa. Nat. Commun. 2021, 12, 6238. [Google Scholar] [CrossRef] [PubMed]
- Serper, M.; Liu, C.; Blumberg, E.A.; Burdzy, A.E.; Veasey, S.; Halpern, S.; Lander, E.; Sigafus, M.R.; Bloom, R.D.; Dunn, T.B.; et al. A pragmatic outreach pilot to understand and overcome barriers to COVID-19 vaccination in abdominal organ transplant. Transpl. Infect. Dis. 2021, 23, e13722. [Google Scholar] [CrossRef]
- Ugwuoke, J.C.; Talabi, F.O.; Adelabu, O.; Sanusi, B.O.; Gever, V.C.; Onuora, C. Expanding the boundaries of vaccine discourse: Impact of visual illustrations communication intervention on intention towards COVID-19 vaccination among victims of insecurity in Nigeria. Hum. Vaccines Immunother. 2021, 17, 3450–3456. [Google Scholar] [CrossRef]
- Wagner, A.L.; Gorin, S.S.; Boulton, M.L.; Glover, B.A.; Morenoff, J.D. Effect of vaccine effectiveness and safety on COVID-19 vaccine acceptance in Detroit, Michigan, July 2020. Hum. Vaccines Immunother. 2021, 17, 2940–2945. [Google Scholar] [CrossRef]
- Williams-Gunpot, D.M. Evaluating “Our COVID-19 Knowledge Test” as a Brief Online E-Health Intervention with African American Adults: Identifying Predictors of High COVID-19 Knowledge and Self-Efficacy for COVID-19 Risk Reduction Behaviors. Ph.D. Thesis, Columbia University, New York, NY, USA, 2021. [Google Scholar]
- Yemer, D.B.; Desta, M.A.; Workie, M.B. Communication Strategies to Combat COVID-19 Vaccines Hesitancy. J. Pharm. Res. Int. 2021, 33, 72–85. [Google Scholar] [CrossRef]
- Wells, G.; Shea, B.; O’Connell, D.; Peterson, J.; Welch, V.; Losos, M.; Tugwell, P. The Newcastle-Ottawa Scale (NOS) for Assessing the Quality of Nonrandomized Studies in Meta-Analyses; The Ottawa Hospital Research Institute: Ottawa, ON, Canada, 2019. [Google Scholar]
- Balasuriya, L.; Santilli, A.; Morone, J.; Ainooson, J.; Roy, B.; Njoku, A.; Mendiola-Iparraguirre, A.; O’Connor Duffany, K.; Macklin, B.; Higginbottom, J.; et al. COVID-19 Vaccine Acceptance and Access Among Black and Latinx Communities. JAMA Netw. Open 2021, 4, e2128575. [Google Scholar] [CrossRef] [PubMed]
- Centers for Disease Control and Prevention (CDC). A Guide for Community Partners-Increasing COVID-19 Vaccine Uptake among Racial and Ethnic Minority Communities; U.S. Department of Health and Human Services/Centers for Disease Control and Prevention National Center for Immunization and Respiratory Diseases: 2021. Available online: https://www.cdc.gov/vaccines/covid-19/downloads/guide-community-partners.pdf (accessed on 25 January 2022).
- COVID Collaborative. Coronavirus Vaccine Hesitancy in Black and Latinx Communities; Langer Research Associates, UNIDOS US, NAACP, COVID Collaborative: 2020. Available online: https://www.covidcollaborative.us/assets/uploads/pdf/VaccineHesitancy_BlackLatinx_Final_11.19.pdf (accessed on 25 January 2022).
- Centers for Disease Control and Prevention (CDC). Health Equity Considerations & Racial & Ethnic Minority Groups; National Center for Immunization and Respiratory Diseases (U.S.). Division of Viral Diseases: 2022. Available online: https://www.cdc.gov/coronavirus/2019-ncov/community/health-equity/vaccine-equity.html (accessed on 25 January 2022).
- Hamel, L.; Kirzinger, A.; Muñana, C.; Brodie, M. COVID-19 Vaccine Monitor: December 2020; Kaiser Family Foundation: San Francisco, CA, USA, 2020. [Google Scholar]
- Al Shamsi, H.; Almutairi, A.G.; Al Mashrafi, S.; Al Kalbani, T. Implications of Language Barriers for Healthcare: A Systematic Review. Oman Med. J. 2020, 35, e122. [Google Scholar] [CrossRef] [PubMed]
| Database | Search Terms |
|---|---|
| MEDLINE Embase PsycINFO CINAHL Scopus Cochrane Library Web of Science Sociological Abstracts Dissertations and Theses Global SocINDEX | African Continental Ancestry (black* or African* or Caribbean or afro* or “person of color” or “people of color” or colored or “dark-skin*” or BIPOC or ((racial or ethnic) minority* (Algeria* or Angola* or Benin* or Botswana* or “Burkina Faso” or Burundi or Cameroon or “Cape Verde” or “Central African Republic” or chad or Comoros or Congo* or “cote d’ivoire” or “Ivory Coast” or Djibouti or Egypt* or Guinea* or Eritrea or Ethiopia* or Gabon or Gambia* or Ghana* or Kenya* or Lesotho or Liberia* or Libya* or Madagascar or Malawi* or Mali* or Mauritania* or Mauritius or Morocco or Mozambique or Namibia* or Niger or Nigeria* or Rwanda* or “sao tome and Principe” or Senegal* or Seychelles or “Sierra leone” or Somalia* or “South Africa” or Sudan or Swaziland or Tanzania* or Togo or Tunisia* or Uganda* or Zambia* or Zimbabwe*) (Cuba* or “Dominican Republic” or Haiti* or Hispaniola* or “Puerto Rico” or “Puerto Rican*” or Jamaica* or Barbados or Dominica or Grenad* or “Saint Lucia” or Trinidad* or Bahama* or “Virgin Islands” or Anguilla or “Saint Kitts” or Antigua or “Turks and Caicos” or “West Indies” or “Saint Vincent”) Coronavirus or Coronavirus Infections or (coronavirus* or corona virus* or OC43 or NL63 or 229E or HKU1 or HCoV* or covid* or Sars-coronavirus* or Severe Acute Respiratory Syndrome Coronavirus*) and or Middle East respiratory syndrome or camel* or influenza virus or avian influenza or H1N1 or H5N1 or H5N6 or IBV or murine corona*) or Covid-19 or COVID-19 Vaccines and (confidence* or trust* or faith or accept* or uptake or hesitant* or attitude* or distrust* or mistrust* or reject* or refuse*) (vaccine* or immunize* or immunise*) or Vaccination Refusal |
| Reference | Country | Study Design | Sample/Settings | Intervention | Measurement Scale/Instrument | Results | Quality Assessment |
|---|---|---|---|---|---|---|---|
| Abdul-Mutakabbir et al. (2021) [35] | United States | Not stated | General public—Mass vaccination clinic (n = 24,868); Mobile vaccination clinic (n = 1542); San Bernardino County (n = 2,180,085) | A three-tiered approach intervention: engagement with faith leaders in the academic community; a culturally inclusive and representative group of healthcare professionals from Loma Linda University to deliver the COVID-19 informational webinars; the completion of remote vaccination clinics. | Vaccination counts | Over the course of the intervention (February 1–30 April 2021), 24,808 persons received their vaccination at the routine mass vaccination clinic. 3.7% of these individuals were Black. At the remote clinics, 1542 individuals received a dose of the vaccine, with 44% of these individuals identifying as Black. | 7 |
| Albarracin et al. (2021) [36] | United States | Multicomponent study: 1 survey & 3 experiments (3-cell, within-subjects experimental design; 3 × 2 within-subjects factorial design; between-subjects design) | Total sample, randomly sampled US population including White, Black, & Hispanic American respondents (n = 1621); Survey (n = 299); Experiment 1 (n = 359); Experiment 2 (n = 357); Experiment 3 (n = 606). Randomly sampled US population | Survey: participants were asked two questions; Experiment 1: participants were randomly rotated through 3 different conditions; Experiment 2: participants were randomly rotated through 3 different conditions; Experiment 3: participants were randomized to either condition 1 or condition 3. | Yes/No scale, Likert scales | Survey: for Black participants, there was an increased likelihood of vaccination with the requirement questions than with the control question (p = 0.001); 80% of Black respondents reported the intent to vaccinate within the required condition; 56% of Black respondents reported the intent to vaccinate within the control condition. Experiments 2, 3, 4: data not disaggregated | 9 |
| Andrasik et al. (2021) [37] | United States | Community-based participatory research | Scientists and community leaders from four BIPOC communities (n = 40–60). Clinical trial sample size: variable throughout the course of study. | Meaningful involvement of the community; Stakeholder engagement and trust-building; Faith initiative: faith-based advisory; Communications & community influence | Pre-screening survey, enrollment counts | Across all 4 clinical trials, 47% of the enrolled participants were BIPOC, 15% of whom identified as Black or African American. The enrollment rates of various BIPOC communities aligned with their proportions within the broader US population. BIPOC enrollment was slow initially, but steadily grew and eventually overtook White enrollment. COVID-19 Prevention Network (CoVPN) sites that actively engaged with BIPOC communities had more success in recruiting BIPOC participants compared to non-CoVPN sites. | 7 |
| Feifer et al. (2021) [38] | United States | Not stated | Black and Hispanic healthcare workers/employees (n = 27,000) | Facts and informational sessions provided by experts; social media educational campaign; resources on the COVID-19 vaccine in Spanish and English; provision of culturally sensitive information through small group discussions and one-on-one conversations | Not stated | At the first time point, rates of vaccination were lowest among Black employees (45.5%) and highest among Asian employees (74.5%). The greatest increase in vaccination rates were among Alaskan Native employees (8.2%), Hispanic employees (6.1%), and Black employees (5.4%). There was a statistically significant increase in the likelihood of Black employees receiving the COVID-19 vaccination compared to White employees (p = 0.004). | 6 |
| Fox A. & Choi, Y. (2021) [39] | United States | Survey experiment | New York residents (n = 1353 (443 non-Hispanic Blacks, 429 non-Hispanic Whites, 481 Hispanics). | A messaging campaign that acknowledged historical racism through a newspaper prime that prioritizes minorities | Questionnaire | Participants’ intention to get vaccinated against COVID-19 was not influenced by the messaging campaign. | 5 |
| Hirshberg et al. (2021) [40] | United States | Not stated | High-risk obstetrical patients (n = 87) | Counseling on COVID-19 vaccination for pregnant and breastfeeding patients; onsite vaccine availability | Standardized COVID-19 vaccination discussion tool, state database | Patients seen before onsite vaccination was available: 1/32 (3%) patients received the vaccination offsite post-counselling. Patients who were seen after onsite vaccination: 2/55 (3%) received the vaccination onsite; 4/55 (7%) received the vaccination offsite. The availability of onsite vaccination was not significantly associated with an increase in vaccination (p = 0.22). Among the 55 patients who received counseling during the availability of onsite vaccination, 25 were counseled during the pilot program but did not receive a vaccination onsite or offsite. | 7 |
| Reddy et al. (2021) [41] | South Africa | Not stated | Healthcare workers (n = 7400) | Creation of staff database for appointment management; Vaccinators completed an online training program for healthcare workers; Vaccines were distributed by pharmacy teams and occupational health nurses. Reconciliation of doses was undertaken after every 24 doses dispensed. Staff arriving to be vaccinated had to display identification of booking confirmation, screened for symptoms, provided consent, then were observed for 15 min in a separate area after vaccination. | Dose counts | There was an upward trend in the number of vaccine doses administered in the week after the roll-out was initiated. Number of vaccines administered each subsequent day of the vaccination campaign (from 17 February 2021 to 26 February 2021, excluding 20 &21 February) = 32, 240, 460, 788, 823, 1018, 1138, 1160. | 5 |
| Reddy et al. (2021) [42] | South Africa | Not stated | South Africa’s population (specific sample size not stated) | COVID-19 vaccination program simulations over 360 days under various scenarios | Incremental cost-effectiveness ratio (ICER) = difference in healthcare costs divided by difference in years-of-life saved (YLS) | There were varying economic and clinical benefits to various vaccination strategies in the two scenarios—lack of vaccination program led to greatest amount of infections, deaths, costs; a 40% vaccination rate led to the lowest healthcare costs on both scenarios and decrease in deaths in both scenarios; a 67% vaccination rate also decreased deaths, however healthcare costs increased; an 80% vaccine supply and 80% vaccine acceptance decreased deaths and increased healthcare costs in both scenarios. Highest pace of vaccination at 300,000 daily led to optimal clinical outcomes and lowest costs when compared with lower paces in both scenarios. In the scenarios where the effective reproductive number = 1.4, 67% vaccine supply was less efficient (in terms of incremental cost-effectiveness ratio: the difference between healthcare costs divided by the difference between years-of-life saved, compared with other approaches to supply and pace) than the 80% vaccine supply. In the scenarios a two-wave epidemic, 67% vaccine supply was more efficient than the 80% vaccine supply; 20% vaccine supply was less efficient that higher levels of vaccine supply, yet decreased deaths by 72–76% and decreased healthcare costs by 15–32% when compared with no vaccination. | 4 |
| Robertson et al. (2021) [28] | United States | Randomized survey experiment (between-subjects design) | American adults (n = 1000) | Participants were assigned to four conditions for financial incentives ($1000, $1500, $2000, or no incentive). | Online survey form | Large financial incentives were found to be counterproductive in Black populations. 53% of Black Americans in the group receiving no incentives reported that they would most likely take the vaccine. The $1500 incentive resulted in an increase to 68% in the proportion of Black participants who reported that they would most likely take the vaccine. At the $2000 incentive, only 39% of Black respondents reported willingness to take the vaccine (a value 13.6% below the acceptance rate in the control group receiving no financial incentive). | 7 |
| Serper et al. (2021) [43] | United States | Not stated | Solid organ transplant recipients (n = 103) | Outreach & motivational interviewing by transplant center staff. Follow-up calls were scheduled to evaluate if participants proceeded to receive the vaccine. | Vaccination counts | People who identified as Black were more likely to schedule a vaccination appointment during the call with transplant center staff or to schedule a vaccine appointment on their own time compared to all other races (odd ratio = 1.6, 95%CI 1.02–2. 6; p = 0.042) after they received information from staff. | 7 |
| Ugwuoke et al. (2021) [44] | Nigeria | Quasi-experimental design | Victims of conflict in Nigeria (n = 470) | Artistic illustration communication intervention delivered concurrently with counseling on the acceptance of COVID-19 vaccination after it was available. This included experts from various disciplines: fine and applied arts, guidance and counseling, mass communication. It took place over the course of 10 days, with each session lasting 1 h. The control group did not receive this intervention. There was collaboration between the research team and the officials at the camp to ensure that the two groups did not interact over the course of the study. | Questionnaire | Participants who engaged with visual communication and counseling had greater average reports of self-efficacy than those who did not on the post-test questionnaire (3.3 vs. 1.4); they also had greater average reports of task efficacy on the post-test questionnaire (3.6 vs. 1.4). There were greater positive reports in terms of intent to vaccine in those who had exposure to visual arts on COVID-19 vaccination on the post-test questionnaire (3.8 vs. 1.3). Participants who had exposure to visual messages about COVID-19 vaccination reported higher levels of intention to vaccinate compared to the control group (self-efficacy 1.4 vs. 3.3, task efficacy 1.6 vs. 3.6, vaccination intention 1.1 vs. 3.8). | 8 |
| Wagner et al. (2021) [45] | United States | Randomized survey experiment | Detroit residents (n = 1117; 76.5% Black) | Hypothetical vaccine profile experiment | Questionnaire | More participants (77.1%) presented with a higher (95%) hypothetical effective vaccine had more acceptance rate compared to participants presented with vaccine that has lower (50%) effectiveness. Vaccine safety and some vaccine profiles had no significant impact on participants’ vaccine acceptance. | 9 |
| Williams-Gunpot (2021) [46] | United States | Cross-sectional survey | African American adults (n = 188) | E-health educational intervention that consisted of a pre and post knowledge test. The educational intervention (Our COVID-19 Knowledge Test) is a true-false tool programmed to have all true answers. The test consisted of 44 questions. | ‘Our COVID-19 Knowledge’ Test (OCKT-44); COVID-19 Knowledge Scale; COVID-19 Prevention Self-Efficacy Scale; Intention to Vaccinate for COVID-19 (IVC-1) tool; Diffusion of Innovation of Our COVID-19 Knowledge Test (DOI-OCKT-1) Tool; COVID-19 Knowledge and Self-Efficacy for Risk Reduction Behaviors | Knowledge of COVID-19 was increased in the post-test (mean score 4.57 vs. 4.85, p = 0.000); knowledge of COVID-19 self-efficacy related to risk reduction (including vaccination) was also higher in the post-test (mean score 5.17 vs. 5.33, p = 0.000). 127 participants reported being vaccinated or having the intent to vaccinate. For the open-ended question, participants had feelings of hope about vaccination, noting that while there is still a chance of contracting COVID-19 with the vaccine, only a small percentage of vaccinated individuals get COVID-19. | 8 |
| (C-K-SE-FRRB-4) tool | |||||||
| Yemer et al. (2021) [47] | Ethiopia | Not stated | Leaders disseminating messages; sample size not stated | Various communication strategies and messages were analyzed. Messages such as health information about COVID-19 vaccination, vaccination campaigns, advocacy, and vaccine hesitancy. SMS messages were sent, religious leaders were involved to increase the spread of positive COVID-19 vaccine messages, workshops were developed to increase awareness of COVID-19 vaccines. | Not stated | Messages (TV, radio, newspaper, social media) about COVID-19 vaccine hesitancy reported on side effects (4/4), accuracy/low quality (2/4), safety testing (3/4), doubts about vaccines (4/4), and others (1/4). The use of various communication strategies contributed to greater vaccine advocacy and vaccine campaigns contributed to increased vaccine acceptance. | 3 |
| Study | Selection | Comparability | Outcome/Exposure | Total |
|---|---|---|---|---|
| [35] | **** | * | ** | 7 |
| [36] | ***** | * | *** | 9 |
| [37] | **** | * | ** | 7 |
| [38] | ** | * | *** | 6 |
| [39] | *** | * | * | 5 |
| [40] | *** | * | *** | 7 |
| [41] | ** | * | ** | 5 |
| [42] | * | * | ** | 4 |
| [28] | ***** | * | * | 7 |
| [43] | *** | * | *** | 7 |
| [44] | ***** | * | ** | 8 |
| [45] | ***** | * | *** | 9 |
| [46] | ***** | * | ** | 8 |
| [47] | * | ** | 3 |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Adeagbo, M.; Olukotun, M.; Musa, S.; Alaazi, D.; Allen, U.; Renzaho, A.M.N.; Sekyi-Otu, A.; Salami, B. Improving COVID-19 Vaccine Uptake among Black Populations: A Systematic Review of Strategies. Int. J. Environ. Res. Public Health 2022, 19, 11971. https://doi.org/10.3390/ijerph191911971
Adeagbo M, Olukotun M, Musa S, Alaazi D, Allen U, Renzaho AMN, Sekyi-Otu A, Salami B. Improving COVID-19 Vaccine Uptake among Black Populations: A Systematic Review of Strategies. International Journal of Environmental Research and Public Health. 2022; 19(19):11971. https://doi.org/10.3390/ijerph191911971
Chicago/Turabian StyleAdeagbo, Morolake, Mary Olukotun, Salwa Musa, Dominic Alaazi, Upton Allen, Andre M. N. Renzaho, Ato Sekyi-Otu, and Bukola Salami. 2022. "Improving COVID-19 Vaccine Uptake among Black Populations: A Systematic Review of Strategies" International Journal of Environmental Research and Public Health 19, no. 19: 11971. https://doi.org/10.3390/ijerph191911971
APA StyleAdeagbo, M., Olukotun, M., Musa, S., Alaazi, D., Allen, U., Renzaho, A. M. N., Sekyi-Otu, A., & Salami, B. (2022). Improving COVID-19 Vaccine Uptake among Black Populations: A Systematic Review of Strategies. International Journal of Environmental Research and Public Health, 19(19), 11971. https://doi.org/10.3390/ijerph191911971









