Anxiety, Depression, and Post-Traumatic Stress Disorder (PTSD) Symptomatology According to Gender in Health-Care Workers during the COVID-19 Pandemic in Peru
Abstract
:1. Introduction
2. Methods and Materials
2.1. Study Design and Context
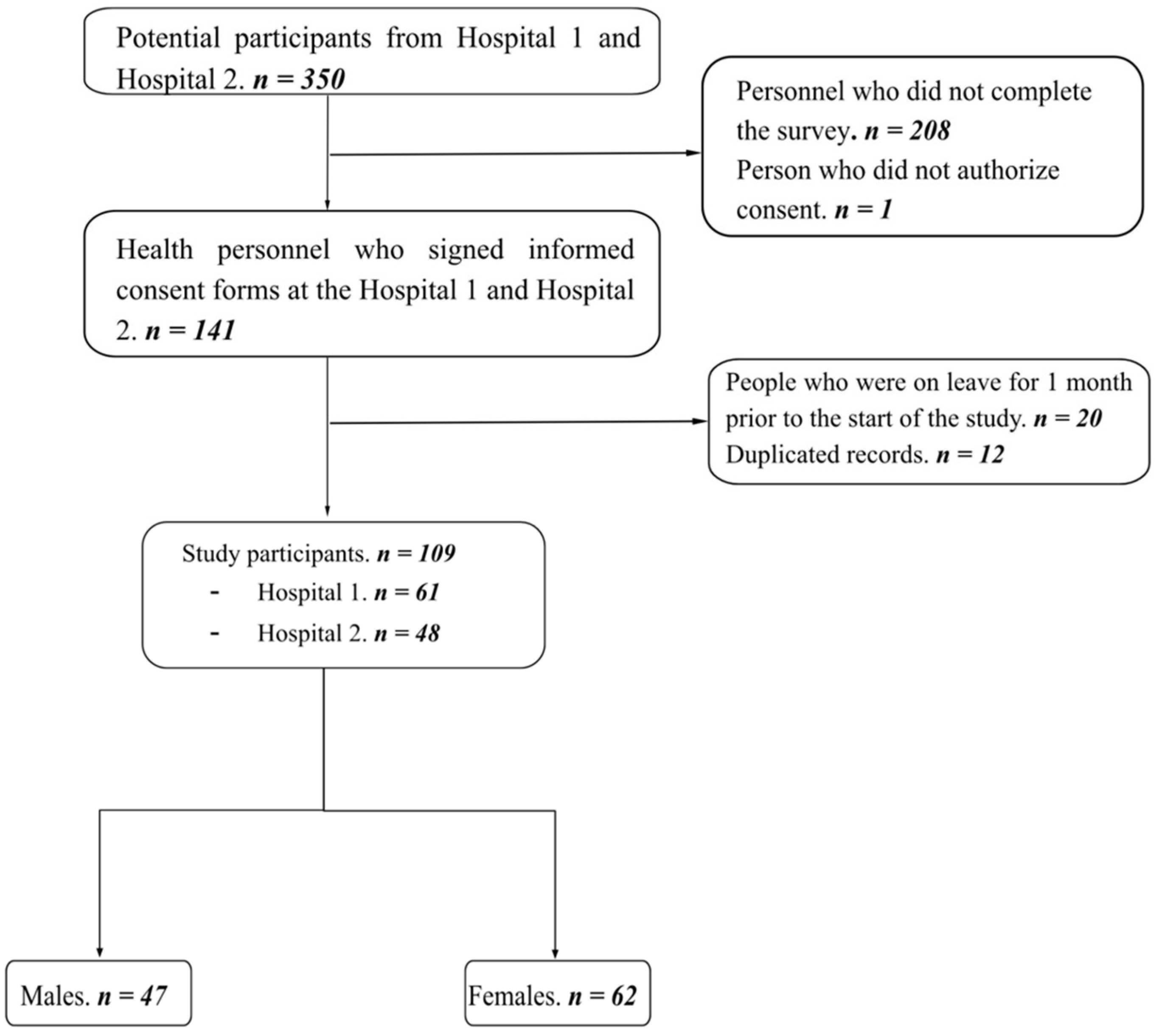
2.2. Population
2.3. Procedures
2.4. Power Estimation
2.5. Analysis Plan
2.6. Ethics
3. Results
3.1. Study Population Characteristics
3.2. Potential Factors Associated to Anxiety, Depression, and PTSD
3.3. Factors Independently Associated with Anxiety, Depression, and PTSD
4. Discussion
4.1. Relevance for the Mental Health of Health-Care Workers
4.2. Limitations and Strengths
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Ruiz-Bravo, A.; Jiménez-Valera, M. SARS-CoV-2 and the pandemic accute respiratory syndrome (COVID-19). Ars Pharm. 2020, 61, 63–79. [Google Scholar]
- Gonzales Castillo, J.R.; Varona Castillo, L.; Dominguez Morante, M.G.; Ocaña Gutierrez, V.R. COVID-19 pandemic and the public heatlh politics in Peru: March-may 2020. Public Health Mag. 2020, 22, 1–9. [Google Scholar]
- Talevi, D.; Socci, V.; Carai, M.; Carnaghi, G.; Faleri, S.; Trebbi, E.; Di Bernardo, A.; Capelli, F.; Pacitti, F. Results of mental health from the COVID-19 pandemic. Riv. Psichiatr. June 2020, 55, 137–144. [Google Scholar]
- Lozano-Vargas, A. Impact from the Coronavirus epidemic (COVID-19) on the mental health of the health personnel and the general population of China. Rev. Neuro-Psiquiatr. 2020, 83, 51–56. [Google Scholar] [CrossRef]
- Torres-Muñoz, V.; Farias-Cortés, J.D.; Reyes-Vallejo, L.A.; Guillén-Díaz-Barriga, C. Risks and damage on the mental health of the sanitary personnel because of the patients attention against COVID-19. Rev. Mex. Urol. 2020, 80, 1–9. [Google Scholar] [CrossRef]
- Amoafo, E.; Hanbali, N.; Patel, A.; Singh, P. Which are the important factors associated with exhaustion in doctors? Occup. Med. 2015, 65, 117–121. [Google Scholar] [CrossRef]
- Saldaña, I.O.; López, O.V.M. Prevalence of depression in residents of different especialties. Secretaría de Salud del Distrito Federal. Evid. Med. Invest. Salud. 2014, 7, 169–177. [Google Scholar]
- Shigemura, J.; Ursano, R.J.; Morganstein, J.C.; Kurosawa, M.; Benedek, D.M. Public responses to the novel 2019 coronavirus (2019-nCoV) in Japan: Mental health consequences and target populations. Psychiatry Clin. Neurosci. 2020, 74, 281–282. [Google Scholar] [CrossRef]
- Samaniego, A.; Urzúa, A.; Buenahora, M.; Vera, P. Symptomatology associated with mental health disorders in health workers in Paraguay: COVID-19 effect. Rev. Interam. Psicol. Interam. J. Psychol. 2020, 54, e1298. [Google Scholar]
- Blanco-Daza, M.; de la Vieja-Soriano, M.; Macip-Belmonte, S.; Tercero-Cano, M.D.C. Posstraumatic stress disorder in nurses during the COVID-19 pandemic. Enferm. Clin. 2022, 32, 92–102. [Google Scholar] [CrossRef]
- Moreira, W.C.; Sousa, A.R.; de Nóbrega, M.P.S.S. Mental Illness in the General Population and Health Professionals during COVID-19: Scoping Review. SciELO Preprints. 2020. Available online: https://preprints.scielo.org/index.php/scielo/preprint/view/689 (accessed on 29 October 2021).
- Dosil Santamaría, M.; Ozamiz-Etxebarria, N.; Redondo Rodríguez, I.; Jaureguizar Alboniga-Mayor, J.; Picaza Gorrotxategi, M. Psychological impact of COVID-19 in a sample of Spanish health professionals. Rev. Psiquiatr. Salud. Ment. Engl. Ed. 2021, 14, 106–112. [Google Scholar] [CrossRef] [PubMed]
- Bassi, M.; Negri, L.; Delle Fave, A.; Accardi, R. The relationship between post-traumatic stress and positive mental health symptoms among health workers during COVID-19 pandemic in Lombardy, Italy. J. Affect. Disord. 2021, 280, 1–6. [Google Scholar] [CrossRef] [PubMed]
- Heron-Delaney, M.; Kenardy, J.; Charlton, E.; Matsuoka, Y. A systematic review of predictors of posttraumatic stress disorder (PTSD) for adult road traffic crash survivors. Injury 2013, 44, 1413–1422. [Google Scholar] [CrossRef]
- Johnson, S.U.; Ebrahimi, O.V.; Hoffart, A. PTSD symptoms among health workers and public service providers during the COVID-19 outbreak. PLoS ONE 2020, 15, e0241032. [Google Scholar] [CrossRef] [PubMed]
- López-Mato, A.; Illa, G.; Boullosa, O.; Márquez, C.; Vieitez, A. Premenstrual dysphoric disorder. Rev. Chil. Neuro-Psiquiatr. 2000, 38, 187–195. [Google Scholar]
- Dyer, O. COVID-19: Peru’s official death toll triples to become the world’s highest. BMJ 2021, 373, n1442. [Google Scholar] [CrossRef] [PubMed]
- COVID Live Update: 260,900,134 Cases and 5,206,335 Deaths from Coronavirus [Internet]. Worldmeter Information. Available online: https://www.worldometers.info/coronavirus/ (accessed on 27 November 2021).
- Regional Health Management of Arequipa. Virtual Situation Room COVID-19, Arequipa [Internet]. Available online: https://www.saludarequipa.gob.pe/epidemiologia/enlac/Covid19.html (accessed on 29 October 2021).
- Gob.pe. National Vaccination Campaign against COVID-19 [Internet]. Available online: https://www.gob.pe/institucion/pcm/campa%C3%B1as/3451-campana-nacional-de-vacunacion-contra-la-covid-19 (accessed on 29 October 2021).
- Peru Ep by Sesae. COVID-19: Adults Over 80 Years of Age in Arequipa Will Be Vaccinated [Internet]. Available online: https://andina.pe/agencia/noticia-covid19-vacunaran-a-adultos-mayores-80-anos-arequipa-844798.aspx (accessed on 29 October 2021).
- Spitzer, R.L.; Kroenke, K.; Williams, J.B.W.; Löwe, B. A brief measure for assessing generalized anxiety disorder: The GAD-7. Arch. Intern. Med. 2006, 166, 1092–1097. [Google Scholar] [CrossRef]
- Instrument Data Sheet [Internet]. Available online: https://bi.cibersam.es/busqueda-de-instrumentos/ficha?Id=239 (accessed on 29 October 2021).
- Baader, M.T.; Molina, F.J.L.; Venezian, B.S.; Rojas, C.C.; Farías, S.R.; Fierro-Freixenet, C.; Backenstrass, M.; Mundt, C. Validation and usefulness of the survey PHQ-9 (Patient Health Questionnaire) in the diagnosis of depression in patients using primary care in Chile. Rev. Chil. Neuro-Psiquiatr. 2012, 50, 10–22. [Google Scholar] [CrossRef]
- Prins, A.; Bovin, M.J.; Smolenski, D.J.; Marx, B.P.; Kimerling, R.; Jenkins-Guarnieri, M.A.; Kaloupek, D.; Schnurr, P.P.; Kaiser, A.P.; Leyva, Y.E.; et al. The Primary Care PTSD Screen for DSM-5 (PC-PTSD-5): Development and Evaluation within a Veteran Primary Care Sample. J. Gen. Intern. Med. 2016, 31, 1206–1211. [Google Scholar] [CrossRef]
- Bekas, A.; Voitsidis, P.; Athanasiadou, M.; Parlapani, E.; Chatzigeorgiou, A.F.; Skoupra, M.; Syngelakis, M.; Holeva, V.; Diakogiannis, I. COVID-19: PTSD symptoms in Greek health care professionals. Psychol. Trauma. 2020, 12, 812. [Google Scholar] [CrossRef]
- Manzini, J.L. Helsinki declaration: Ethical principles for medical research involving human subjects. Acta Bioeth. 2000, 6. Available online: http://www.scielo.cl/scielo.php?script=sci_arttext&pid=S1726-569X2000000200010&lng=en&nrm=iso&tlng=en (accessed on 27 November 2021).
- Tsamakis, K.; Tsiptsios, D.; Ouranidis, A.; Mueller, C.; Schizas, D.; Terniotis, C.; Nikolakakis, N.; Tyros, G.; Kympouropoulos, S.; Lazaris, A.; et al. COVID-19 and its consequences on mental health (Review). Exp. Ther. Med. 2021, 21, 1. [Google Scholar] [CrossRef] [PubMed]
- Wang, C.; Pan, R.; Wan, X.; Tan, Y.; Xu, L.; McIntyre, R.S.; Choo, F.N.; Tran, B.; Ho, R.; Sharma, V.K.; et al. A longitudinal study on the mental health of general population during the COVID-19 epidemic in China. Brain Behav. Immun. 2020, 87, 40–48. [Google Scholar] [CrossRef] [PubMed]
- Dutta, A.; Sharma, A.; Torres-Castro, R.; Pachori, H.; Mishra, S. Mental health outcomes among health-care workers dealing with COVID-19/severe acute respiratory syndrome coronavirus 2 pandemic: A systematic review and meta-analysis. Indian J. Psychiatry 2021, 63, 335–347. [Google Scholar] [CrossRef]
- Luo, M.; Guo, L.; Yu, M.; Jiang, W.; Wang, H. The psychological and mental impact of coronavirus disease 2019 (COVID-19) on medical staff and the general public—A systematic review and meta-analysis. Psychiatry Res. 2020, 291, 113190. [Google Scholar] [CrossRef]
- Danet, A. Psychological impact of COVID-19 pandemic in Western frontline healthcare professionals. A systematic review. Med. Clínica. Barc. 2021, 156, 449–458. [Google Scholar] [CrossRef]
- Vizheh, M.; Qorbani, M.; Arzaghi, S.M.; Muhidin, S.; Javanmard, Z.; Esmaeili, M. The mental health of healthcare workers in the COVID-19 pandemic: A systematic review. J. Diabetes Metab. Disord. 2020, 19, 1967–1978. [Google Scholar] [CrossRef]
- Kunz, M.; Strasser, M.; Hasan, A. Impact of the coronavirus disease 2019 pandemic on healthcare workers: Systematic comparison between nurses and medical doctors. Curr. Opin. Psychiatry 2021, 34, 413–419. [Google Scholar] [CrossRef]
- García-Iglesias, J.J.; Gómez-Salgado, J.; Martín-Pereira, J.; Fagundo-Rivera, J.; Ayuso-Murillo, D.; Martínez-Riera, J.R. SARS-COV-2 (COVID-19) impact on the mental health of the sanitary professional: A sistematic. Rev. Esp. Salud Pública 2020, 94, e1–e20. [Google Scholar]
- Huarcaya-Victoria, J.; Huarcaya-Victoria, J. Mental health considerations in the COVID-19 pandemic. Rev. Peru. Med. Exp. Salud Publica 2020, 37, 327–334. [Google Scholar] [CrossRef]
- Van Hassel, D.; van der Velden, L.; de Bakker, D.; Batenburg, R. Age-related differences in working hours among male and female GPs: An SMS-based time use study. Hum. Resour. Health 2017, 15, 84. [Google Scholar] [CrossRef] [PubMed]
- Song, J.; Cheng, T.C. How do gender differences in family responsibilities affect doctors’ labor supply? Evidence from Australian panel data. Soc. Sci. Med. 2020, 265, 113475. [Google Scholar] [CrossRef] [PubMed]
- Miller, L. Doctors, their mental health and capacity for work. Occup. Med. 2009, 59, 53–55. [Google Scholar] [CrossRef] [PubMed]
- Husky, M.M.; Pietrzak, R.H.; Marx, B.P.; Mazure, C.M. Research on Post-traumatic Stress Disorder in the Context of the COVID-19 Pandemic: A Review of Methods and Implications in General Population Samples. Chronic Stress 2021, 5, 24705470211051327. [Google Scholar] [CrossRef]
- National Institute of Mental Health (NIMH). Post-Traumatic Stress Disorder. Available online: https://www.nimh.nih.gov/health/topics/post-traumatic-stress-disorder-ptsd (accessed on 25 August 2022).
- Van Overmeire, R. The Methodological Problem of Identifying Criterion A Traumatic Events During the COVID-19 Era: A Commentary on Karatzias et al. J. Trauma. Stress 2020, 33, 864–865. [Google Scholar] [CrossRef]
- Tyson, G.; Wild, J. Post-Traumatic Stress Disorder Symptoms among Journalists Repeatedly Covering COVID-19 News. Int. Environ. Res. Public Health 2021, 18, 8536. [Google Scholar] [CrossRef] [PubMed]
- Pfefferbaum, B.; North, C.S. Mental Health and the Covid-19 Pandemic. N. Engl. J. Med. 2020, 383, 510–512. [Google Scholar] [CrossRef]
- MINSA. Guia Tecnica para el Cuidado de la Salud Mental del Personal de Salud en el Contexto del COVID-19. Ministerio de Salud. 2020. Available online: http://bvs.minsa.gob.pe/local/MINSA/5000.pdf (accessed on 25 August 2022).
- Liu, N.; Zhang, F.; Wei, C.; Jia, Y.; Shang, Z.; Sun, L.; Wu, L.; Sun, Z.; Zhou, Y.; Wang, Y.; et al. Prevalence and Predictors of PTSD during COVID-19 Outbreak in China Hardest-Hit Areas: Gender Differences Matter. Psychiatry Res. 2020, 287, 112921. Available online: https://pubmed.ncbi.nlm.nih.gov/32489190/ (accessed on 25 September 2021). [CrossRef] [PubMed]
| Variable | N = 109 | |
|---|---|---|
| Age (years) n (%) | ||
| ≤45 | 54 | 49.5% |
| >45 | 55 | 50.5% |
| Sex, n (%) | ||
| Female | 62 | 56.9% |
| Male | 47 | 43.1% |
| Marital Status, n (%) | ||
| Single | 31 | 28.4% |
| Married/cohabitant | 66 | 60.6% |
| Divorced | 12 | 11.0% |
| Number of Children, n (%) | ||
| No children | 26 | 24.1% |
| 1–2 children | 62 | 57.4% |
| 3–4 children | 20 | 18.5% |
| Profession, n (%) | ||
| Nurse | 35 | 32.4% |
| Technical staff | 29 | 26.9% |
| Physician | 44 | 40.7% |
| Labor hospital, n (%) | ||
| Hospital 1 | 61 | 56.0% |
| Hospital 2 | 48 | 44.0% |
| Occupation, n (%) | ||
| COVID-19 area | 32 | 29.6% |
| Non-COVID-19 area | 20 | 18.5% |
| Both | 56 | 51.9% |
| Service where you work, n (%) | ||
| Emergency | 10 | 9.4% |
| Triage COVID-19 | 6 | 5.6% |
| Non-COVID-19 Hospitalization | 37 | 35.0% |
| COVID-19 Hospitalization | 36 | 34.0% |
| Consultation | 17 | 16.0% |
| Working hours, n (%) | ||
| <150 h | 64 | 63.4% |
| ≥150 h | 37 | 36.6% |
| Pathological history, n (%) | ||
| Yes | 16 | 14.7% |
| No | 93 | 85.3% |
| Loss of family member/close friend, n (%) | ||
| Yes | 61 | 56.0% |
| No | 48 | 44.0% |
| Anxiety score, median (p25–p75) | 6 | (2–11) |
| Depression score, median (p25–p75) | 6 | (2–10) |
| PTSD score, median (p25–p75) | 1 | (0–3) |
| C. Anxiety | p | C. Depression | p | C. PTSD | p | |
|---|---|---|---|---|---|---|
| Age (**), median (DE) | ||||||
| ≤45 | 6.5 (4.4) | 0.923 | 7.0 (6.0) | 0.446 | 1.7 (1.7) | 0.307 |
| >45 | 6.6 (4.5) | 6.2 (4.8) | 1.4 (1.3) | |||
| Sex (**), median (DE) | ||||||
| Female | 8.7 (3.5) | <0.001 | 8.7 (4.8) | <0.001 | 2.0 (1.5) | <0.001 |
| Male | 3.7 (4.0) | 3.8 (5.0) | 1.0 (1.4) | |||
| Marital Status (***), median (DE) | ||||||
| Single | 5.7 (4.3) | 0.002 | 6.7 (6.0) | 0.030 | 1.8 (1.8) | 0.088 |
| Married/cohabitant | 7.5 (4.4) | 7.2 (5.2) | 1.6 (1.4) | |||
| Divorced | 3 (2.8) | 2.7 (4.0) | 0.6 (1.2) | |||
| Number of Children (***), median (DE) | ||||||
| No children | 5.4 (4.6) | 0.059 | 6.5 (6.2) | 0.116 | 1.8 (1.8) | 0.742 |
| 1–2 children | 6.4 (4.2) | 5.9 (5.1) | 1.5 (1.5) | |||
| 3–4 children | 8.5 (4.6) | 8.8 (5.3) | 1.5 (1.1) | |||
| Profession (***), median (DE) | ||||||
| Nurse | 7.7 (4.5) | 0.100 | 8.1 (6.1) | 0.125 | 2.1 (1.4) | 0.051 |
| Technical staff | 6.7 (5.0) | 5.6 (4.4) | 1.3 (1.3) | |||
| Physician | 5.5 (4.0) | 6.0 (5.4) | 1.3 (1.6) | |||
| Labor hospital (**), median (DE) | ||||||
| 1 | 7.7 (4.3) | 0.002 | 7.0 (4.6) | 0.361 | 1.5 (1.2) | 0.467 |
| 2 | 5.1 (4.2) | 6.0 (6.3) | 1.7 (1.8) | |||
| Occupation (***), median (DE) | ||||||
| COVID-19 area | 4.8 (3.9) | 0.020 | 5.4 (5.7) | 0.330 | 1.7 (1.6) | 0.837 |
| Non-COVID-19 area | 6.4 (4.5) | 7.6 (6.2) | 1.7 (1.8) | |||
| Both | 7.6 (4.5) | 6.9 (5.0) | 1.5 (1.4) | |||
| Service where you work (***), median (DE) | ||||||
| Emergency | 6.9 (4.7) | 0.150 | 5.7 (4.0) | 0.570 | 0.8 (1.0) | 0.121 |
| Triage COVID-19 | 4.7 (4.4) | 4.7 (6.4) | 1.5 (1.0) | |||
| Non-COVID-19 Hospitalization | 7.9 (4.3) | 7.8 (5.6) | 1.9 (1.6) | |||
| COVID-19 Hospitalization | 5.5 (4.4) | 6.3 (6.0) | 1.7 (1.7) | |||
| Consultation | 6.9 (4.0) | 6.1 (4.7) | 0.9 (1.0) | |||
| Working hours (**), median (DE) | ||||||
| <150 h | 7.9 (4.5) | <0.001 | 8.1 (5.5) | <0.001 | 2.0 (1.5) | 0.004 |
| ≥150 h | 4.6 (3.4) | 4.2 (4.3) | 1.0 (1.4) | |||
| Pathological history (+), median (p25–p75) | ||||||
| Yes | 8 (2.5–11) | 0.454 | 9 (4.5–13.5) | 0.056 | 3 (0–4) | 0.097 |
| No | 6 (2–11) | 5 (2–10) | 1 (0–2) | |||
| Loss of family member/close friend (**), median (DE) | ||||||
| Yes | 6.5 (4.8) | 0.900 | 6.7 (6.0) | 0.836 | 1.7 (1.7) | 0.403 |
| No | 6.6 (4.0) | 6.4 (4.7) | 1.4 (1.3) |
| C. Anxiety | C. Depression | C. PTSD | ||||
|---|---|---|---|---|---|---|
| Variable | Crude | Adjusted * | Crude | Adjusted * | Crude | Adjusted * |
| Coef (CI 95%) | Coef (CI 95%) | Coef (CI 95%) | Coef (CI 95%) | Coef CI 95% | Coef CI 95% | |
| Age | ||||||
| ≤45 | Ref | Ref | Ref | Ref | Ref | Ref |
| >45 | 0.08 (−1.60–1.77) | −1.23 (−2.77–0.31) | −0.80 (−2.87–1.27) | −1.54 (−3.68–0.60) | −0.31 (−0.91–0.29) | −0.40 (−1.05–0.25) |
| Sex | ||||||
| Female | Ref | Ref | Ref | Ref | Ref | Ref |
| Male | 4.96 (3.54–6.38) | 4.48 (2.95–6.00) | 4.87 (3.0–6.75) | 4.50 (2.39–6.62) | 1.04 (0.46–1.61) | 1.13 (0.50–1.76) |
| Marital Status | ||||||
| Single | Ref | Ref | Ref | Ref | Ref | Ref |
| Married/cohabitant | 1.84 (0.02–3.66) | 1.35 (−0.93–3.63) | 0.53 (−1.76–2.83) | 1.11 (−2.06–4.27) | −0.14 (−0.82–0.54) | 0.33 (−0.61–1.27) |
| Divorced | −2.71 (−5.55–0.13) | −0.56 (−3.24–2.12) | −4.01 (−7.59–−0.43) | −1.58 (−5.30–2.14) | −1.15 (−2.21–−0.09) | −0.63 (−1.74–0.48) |
| Number of Children | ||||||
| No children | Ref | Ref | Ref | Ref | Ref | Ref |
| 1 to 2 children | 0.98 (−1.04–3.00) | 0.27 (−2.05–2.59) | −0.65 (−3.15–1.85) | −0.16 (−3.38–3.05) | −0.28 (−1.02–0.46) | −0.07 (−1.03–0.88) |
| 3 to 4 children | 3.08 (0.50–5.65) | 1.41 (−1.65–4.48) | 2.26 (−0.92–5.45) | 2.30 (−1.96–6.55) | −0.26 (−1.23–0.71) | −0.27 (−1.58–1.04) |
| Profession | ||||||
| Nurse | Ref | Ref | Ref | Ref | Ref | Ref |
| Technical staff | −1.03 (−3.22–1.16) | 0.40 (−1.76–2.56) | −2.50 (−5.18–0.20) | −0.65 (−3.65–2.35) | −0.78 (−1.58–0.02) | 0.13 (−0.78–1.05) |
| Physician | −2.16 (−4.14–−0.19) | −0.26 (−2.05–1.54) | −2.11 (−4.54–0.31) | −0.79 (−3.28–1.70) | −0.78 (−1.46–−0.09) | −0.42 (−1.16–0.32) |
| Labor hospital | ||||||
| Hospital 1 | Ref | Ref | Ref | Ref | Ref | Ref |
| Hospital 2 | −2.57 (−4.20–−0.94) | −0.27 (−2.66–2.11) | −0.96 (−3.04–1.12) | 1.18 (−2.12–4.49) | 0.22 (−0.38–0.83) | 0.68 (−0.30–1.66) |
| Occupation | ||||||
| COVID-19 area | Ref | Ref | Ref | Ref | Ref | Ref |
| Non-COVID-19 area | 1.56 (−0.89–4.00) | 0.86 (−1.70–3.41) | 2.16 (−0.92–5.24) | 1.45 (−2.08–4.99) | 0.07 (−0.90–1.03) | −0.22 (−1.27–0.82) |
| Both | 2.73 (0.83–4.63) | 1.35 (−0.42–3.12) | 1.44 (−0.96–3.83) | 0.31 (−2.15–2.77) | −0.16 (−0.85–0.54) | −0.37 (−1.10–0.36) |
| Service where you work | ||||||
| Emergency | Ref | - | Ref | - | Ref | - |
| Triage COVID-19 | −2.23 (−6.70–2.23) | - | −1.03 (−6.69–4.62) | - | 0.72 (−0.85–2.29) | - |
| Non-COVID-19 Hospitalization | 1.02 (−2.06–4.10) | - | 2.08 (−1.82–5.99) | - | 1.14 (0.02–2.25) | - |
| COVID-19 Hospitalization | −1.4 (−4.49–1.69) | - | 0.58 (−3.34–4.49) | - | 0.96 (−0.16–2.07) | - |
| Consultation | −0.02 (−3.46–3.43) | - | 0.42 (−3.95–4.78) | - | 0.16 (−1.10–1.41) | - |
| Working hours | ||||||
| ≥150 h | Ref | Ref | Ref | Ref | Ref | Ref |
| <150 h | 3.29 (1.62–4.97) | 1.60 (−0.09–3.29) | 3.93 (1.83–6.03) | 2.14 (−0.20–4.48) | 0.92 (0.30–1.54) | 0.80 (0.10–1.49) |
| Pathological history | ||||||
| Yes | Ref | Ref | Ref | Ref | Ref | Ref |
| No | −0.77 (−3.16–1.60) | −0.37 (−2.43–1.69) | −3.08 (−5.95–−0.21) | −2.73 (−5.59–0.13) | −0.81 (−1.65–0.02) | −0.96 (−1.82–−0.10) |
| Loss of family member/close friend | ||||||
| No | Ref | Ref | Ref | Ref | Ref | Ref |
| Yes | −0.11 (−1.81–1.60) | 0.24 (−1.29–1.77) | 0.22 (−1.87–2.31) | −0.24 (−2.36–1.89) | 0.26 (−0.35–0.86) | 0.19 (−0.44–0.83) |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Martínez Pajuelo, A.R.; Irrazabal Ramos, J.E.; Lazo-Porras, M.
Anxiety, Depression, and Post-Traumatic Stress Disorder (PTSD) Symptomatology According to Gender in Health-Care Workers during the COVID-19 Pandemic in Peru
Martínez Pajuelo AR, Irrazabal Ramos JE, Lazo-Porras M.
Anxiety, Depression, and Post-Traumatic Stress Disorder (PTSD) Symptomatology According to Gender in Health-Care Workers during the COVID-19 Pandemic in Peru
Martínez Pajuelo, Alex Ricardo, José Eduardo Irrazabal Ramos, and Maria Lazo-Porras.
2022. "Anxiety, Depression, and Post-Traumatic Stress Disorder (PTSD) Symptomatology According to Gender in Health-Care Workers during the COVID-19 Pandemic in Peru
Martínez Pajuelo, A. R., Irrazabal Ramos, J. E., & Lazo-Porras, M.
(2022). Anxiety, Depression, and Post-Traumatic Stress Disorder (PTSD) Symptomatology According to Gender in Health-Care Workers during the COVID-19 Pandemic in Peru






