Factors Affecting Mothers’ Adherence to Home Exercise Programs Designed for Their Children with Cerebral Palsy
Abstract
:1. Introduction
2. Materials and Methods
2.1. Design
2.2. Participants
- Inclusion criteria: Mothers with children aged birth to 12 years old who were given an HEP prescription from a physiotherapist.
- Exclusion criteria: Mothers who were unable to read or write in Arabic or who had children with other neurological disorders. In addition, the study rejected incomplete surveys.
2.3. Measures Included in the Questionnaires
- Demographic variables
- 2.
- Questionnaire related to Parents’ Adherence to HEP
2.4. Translation of the Questionnaires
2.5. Pilot Study
2.6. Data Collection
2.7. Data Analysis
3. Results
3.1. Reliability of the Questionnaire
3.2. Outcomes of Descriptive Analysis
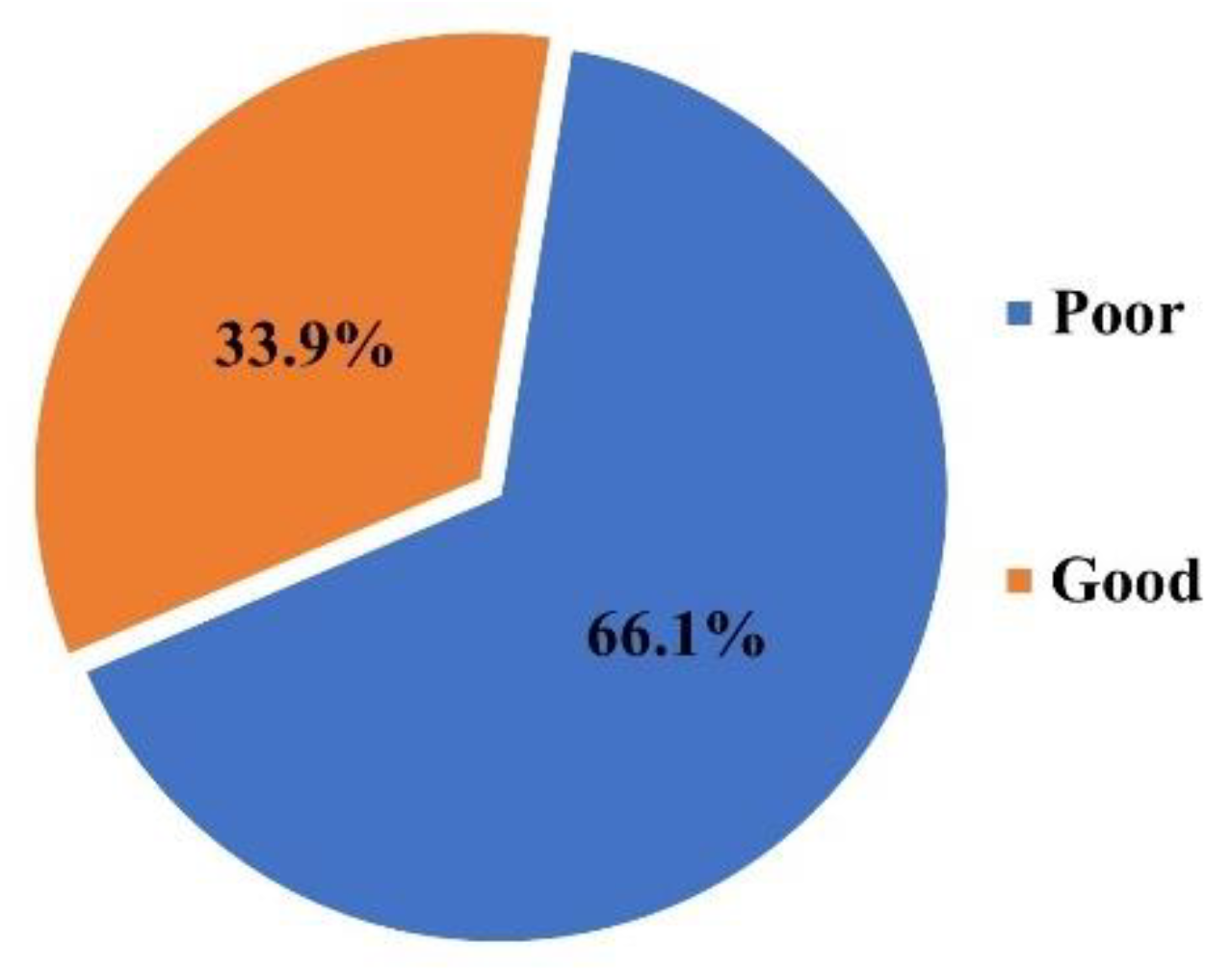
3.3. Analysis of Adherence of Mothers to Recommended HEP
4. Discussion
4.1. HEP Was a Good Fit for Mothers’ Everyday Schedules
4.2. Uncertainty in Mother’s Mind
4.3. Behavior of a Physical Therapist
4.4. Limitations of the Study
4.5. Recommendations
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Morgan, P.; McGinley, J.L. Chapter 20—Cerebral palsy. In Handbook of Clinical Neurology; Day, B.L., Lord, S.R., Eds.; Elsevier: Amsterdam, The Netherlands, 2018; Volume 159, pp. 323–336. [Google Scholar]
- Sadowska, M.; Sarecka-Hujar, B.; Kopyta, I. Cerebral Palsy: Current Opinions on Definition, Epidemiology, Risk Factors, Classification and Treatment Options. Neuropsychiatr. Dis. Treat. 2020, 16, 1505–1518. [Google Scholar] [CrossRef] [PubMed]
- Patel, D.R.; Neelakantan, M.; Pandher, K.; Merrick, J. Cerebral palsy in children: A clinical overview. Transl. Pediatr. 2020, 9 (Suppl. S1), S125–S135. [Google Scholar] [CrossRef] [PubMed]
- Rosenbaum, P.; Paneth, N.; Leviton, A.; Goldstein, M.; Bax, M.; Damiano, D.; Dan, B.; Jacobsson, B. A report: The definition and classification of cerebral palsy April 2006. Dev. Med. Child Neurol. Suppl. 2007, 109, 8–14. [Google Scholar] [PubMed]
- Galea, C.; McIntyre, S.; Smithers-Sheedy, H.; Reid, S.M.; Gibson, C.; Delacy, M.; Watson, L.; Goldsmith, S.; Badawi, N.; Blair, E.; et al. Cerebral palsy trends in Australia (1995–2009): A population-based observational study. Dev. Med. Child Neurol. 2019, 61, 186–193. [Google Scholar] [CrossRef]
- Al Salloum, A.A.; El Mouzan, M.I.; Al Omar, A.A.; Al Herbish, A.S.; Qurashi, M.M. The prevalence of neurological disorders in Saudi children: A community-based study. J. Child Neurol. 2011, 26, 21–24. [Google Scholar] [CrossRef]
- Arora, S.K.; Aggarwal, A.; Mittal, H. Impact of an Educational Film on Parental Knowledge of Children with Cerebral Palsy. Int. J. Pediatr. 2014, 2014, 573698. [Google Scholar] [CrossRef]
- Beckers, L.; van der Burg, J.; Janssen-Potten, Y.; Rameckers, E.; Aarts, P.; Smeets, R. Process evaluation of two home-based bimanual training programs in children with unilateral cerebral palsy (the COAD-study): Protocol for a mixed methods study. BMC Pediatr. 2018, 18, 141. [Google Scholar] [CrossRef] [PubMed]
- Argent, R.; Daly, A.; Caulfield, B. Patient Involvement with Home-Based Exercise Programs: Can Connected Health Interventions Influence Adherence? JMIR Mhealth Uhealth 2018, 6, e47. [Google Scholar] [CrossRef]
- Johnson, R.W.; Williams, S.A.; Gucciardi, D.F.; Bear, N.; Gibson, N. Evaluating the effectiveness of home exercise programmes using an online exercise prescription tool in children with cerebral palsy: Protocol for a randomised controlled trial. BMJ Open 2018, 8, e018316. [Google Scholar] [CrossRef]
- Armstrong, E.L.; Boyd, R.N.; Kentish, M.J.; Carty, C.P.; Horan, S.A. Effects of a training programme of functional electrical stimulation (FES) powered cycling, recreational cycling and goal-directed exercise training on children with cerebral palsy: A randomised controlled trial protocol. BMJ Open 2019, 9, e024881. [Google Scholar] [CrossRef]
- Novak, I. Parent experience of implementing effective home programs. Phys. Occup. Ther. Pediatr. 2011, 31, 198–213. [Google Scholar] [CrossRef] [PubMed]
- Beckers, L.W.; Schnackers, M.L.; Janssen-Potten, Y.J.; Kleijnen, J.; Steenbergen, B. Feasibility and effect of home-based therapy programmes for children with cerebral palsy: A protocol for a systematic review. BMJ Open 2017, 7, e013687. [Google Scholar] [CrossRef] [PubMed]
- Beckers, L.; Geijen, M.M.E.; Kleijnen, J.; Rameckers, E.A.A.; Schnackers, M.L.A.P.; Smeets, R.J.E.M.; Janssen-Potten, Y.J.M. Feasibility and effectiveness of home-based therapy programmes for children with cerebral palsy: A systematic review. BMJ Open 2020, 10, e035454. [Google Scholar] [CrossRef] [PubMed]
- Medina-Mirapeix, F.; Lillo-Navarro, C.; Montilla-Herrador, J.; Gacto-Sánchez, M.; Franco-Sierra, M.; Escolar-Reina, P. Predictors of parents’ adherence to home exercise programs for children with developmental disabilities, regarding both exercise frequency and duration: A survey design. Eur. J. Phys. Rehabil. Med. 2017, 53, 545–555. [Google Scholar] [CrossRef]
- Rabino, S.R.; Peretz, S.R.; Kastel-Deutch, T.; Tirosh, E. Factors affecting parental adherence to an intervention program for congenital torticollis. Pediatr. Phys. Ther. 2013, 25, 298–303. [Google Scholar] [CrossRef]
- Rone-Adams, S.A.; Stern, D.F.; Walker, V. Stress and compliance with a home exercise program among caregivers of children with disabilities. Pediatr. Phys. Ther. 2004, 16, 140–148. [Google Scholar] [CrossRef]
- Santer, M.; Ring, N.; Yardley, L.; Geraghty, A.W.A.; Wyke, S. Treatment non-adherence in pediatric long-term medical conditions: Systematic review and synthesis of qualitative studies of caregivers’ views. BMC Pediatr. 2014, 14, 63. [Google Scholar] [CrossRef]
- Domenech, A.C.P.; Tavares, K.O.; Ruedell, A.M.; Rodrigues da Silva Nobre, J. Cerebral palsy: The meaning of physical therapy for mother caregivers. Fisioter. Mov. 2016, 29, 757–766. [Google Scholar] [CrossRef]
- Madi, S.M.; Mandy, A.; Aranda, K. The Perception of Disability Among Mothers Living with a Child with Cerebral Palsy in Saudi Arabia. Glob. Qual. Nurs. Res. 2019, 6, 2333393619844096. [Google Scholar]
- Alwhaibi, R.M.; Zaidi, U.; Alzeiby, I.; Alhusaini, A. Quality of Life and Socioeconomic Status: A Comparative Study among Mothers of Children with and without Disabilities in Saudi Arabia. Child Care Pract. 2020, 26, 62–80. [Google Scholar] [CrossRef]
- Lillo-Navarro, C.; Medina-Mirapeix, F.; Escolar-Reina, P.; Montilla-Herrador, J.; Gomez-Arnaldos, F.; Oliveira-Sousa, S.L. Parents of children with physical disabilities perceive that characteristics of home exercise programs and physiotherapists’ teaching styles influence adherence: A qualitative study. J. Physiother. 2015, 61, 81–86. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Tavakol, M.; Dennick, R. Making sense of Cronbach’s alpha. Int. J. Med. Educ. 2011, 2, 53–55. [Google Scholar] [CrossRef]
- Basaran, A.; Karadavut, K.I.; Uneri, S.O.; Balbaloglu, O.; Atasoy, N. Adherence to Home Exercise Program among Caregivers of Children with Cerebral Palsy. Turk. J. Phys. Med. Rehab. 2014, 60, 85–91. [Google Scholar] [CrossRef]
- Rahi, J.S.; Manaras, I.; Tuomainen, H.; Hundt, G.L. Meeting the needs of parents around the time of diagnosis of disability among their children: Evaluation of a novel program for information, support, and liaison by key workers. Pediatrics 2004, 114, e477–e482. [Google Scholar] [CrossRef] [PubMed]
- Njelesani, J.; Leckie, K.; Drummond, J.; Cameron, D. Parental perceptions of barriers to physical activity in children with developmental disabilities living in Trinidad and Tobago. Disabil. Rehabil. 2015, 37, 290–295. [Google Scholar] [CrossRef]
- Ekberg, S.; Bradford, N.; Herbert, A.; Danby, S.; Yates, P. Healthcare users’ experiences of communicating with healthcare professionals about children who have life-limiting conditions: A qualitative systematic review protocol. JBI Database Syst. Rev. Implement. Rep. 2015, 13, 33–42. [Google Scholar] [CrossRef]
- Alabri, W. Maternal perspectives: The needs of Saudi families of children with Down’s syndrome. J. Intellect. Disabil. 2022. [Google Scholar] [CrossRef]
- Kelso, T.; French, D.; Fernandez, M. Stress and coping in primary caregivers of children with a disability: A qualitative study using the Lazarus and Folkman Process Model of Coping. J. Res. Spec. Educ. Needs 2005, 5, 3–10. [Google Scholar] [CrossRef]
- Kazdin, A.E.; Holland, L.; Crowley, M.; Breton, S. Barriers to Treatment Participation Scale: Evaluation and validation in the context of child outpatient treatment. J. Child Psychol. Psychiatry 1997, 38, 1051–1062. [Google Scholar] [CrossRef]
- Lau, A.S.; Fung, J.J.; Ho, L.Y.; Liu, L.L.; Gudiño, O.G. Parent training with high-risk immigrant chinese families: A pilot group randomized trial yielding practice-based evidence. Behav. Ther. 2011, 42, 413–426. [Google Scholar] [CrossRef] [Green Version]
| No. of Questions | Cronbach’s Alpha | |
|---|---|---|
| Questionnaire | 17 | 0.814 |
| Categories | N (%) | |
|---|---|---|
| Gender of child | Male | 65 (59.6%) |
| Female | 44 (40.4%) | |
| Age of child | Mean = 69 Month, St. D = 36.50 | |
| The type of hospital in which the child receives rehabilitation | Governmental | 52 (47.7%) |
| Private | 57 (52.3%) | |
| Gender of Physiotherapist responsible for the child | Male | 32 (29.4%) |
| Female | 77 (70.6%) | |
| Mothers’ Adherence | Total | Chi-square = 3.307 p-value = 0.041 * | |||
| Poor | Good | ||||
| Age | 20–25 Years | 1 | 4 | 5 | |
| 26–30 Years | 16 | 9 | 25 | ||
| 31–35 Years | 22 | 7 | 29 | ||
| 36–40 Years | 24 | 12 | 36 | ||
| More than 40 years | 8 | 6 | 14 | ||
| Mothers’ Adherence | Total | Chi-square = 1.051 p-value = 0.591 | |||
| Poor | Good | ||||
| Status | Married | 66 | 35 | 101 | |
| Divorced | 5 | 1 | 6 | ||
| Widow | 1 | 1 | 2 | ||
| Mothers’ Adherence | Total | Chi-square = 3.363 p-value = 0.339 | |||
| Poor | Good | ||||
| Education | Less than Secondary | 10 | 6 | 16 | |
| Secondary | 22 | 16 | 38 | ||
| Universal | 37 | 15 | 52 | ||
| Above Universal | 3 | 0 | 3 | ||
| Mothers’ Adherence | Total | Chi-square = 10.611 p-value = 0.231 | |||
| Poor | Good | ||||
| Children | 0–2 | 24 | 14 | 38 | |
| 3–5 | 41 | 17 | 58 | ||
| 6–10 | 7 | 6 | 13 | ||
| Mothers’ Adherence | Total | Chi-square = 4.164 p-value = 0.384 | |||
| Poor | Good | ||||
| Income | Less than 5000 | 13 | 10 | 23 | |
| 5000–10,000 | 27 | 8 | 35 | ||
| Mothers’ Adherence | Total | Chi-square = 22.320 p-value = 0.000 ** | |||
| Poor | Good | ||||
| 1. Does the home program fit your daily routine? | Rarely | 11 | 0 | 11 | |
| Sometimes | 52 | 18 | 70 | ||
| Often | 6 | 11 | 17 | ||
| Always | 3 | 8 | 11 | ||
| Mothers’ Adherence | Total | Chi-square = 14.347 p-value = 0.006 ** | |||
| Poor | Good | ||||
| 2. I understand my child’s home program | Strongly disagree | 2 | 0 | 2 | |
| Disagree | 12 | 1 | 13 | ||
| Undecided | 10 | 3 | 13 | ||
| Agree | 41 | 20 | 61 | ||
| Strongly agree | 7 | 13 | 20 | ||
| Mothers’ Adherence | Total | Chi-square = 21.136 p-value = 0.000 ** | |||
| Poor | Good | ||||
| 3. I am skillful in carrying out the home program | Strongly disagree | 5 | 0 | 5 | |
| Disagree | 29 | 3 | 32 | ||
| Undecided | 9 | 7 | 16 | ||
| Agree | 27 | 20 | 47 | ||
| Strongly agree | 2 | 7 | 9 | ||
| Mothers’ Adherence | Total | Chi-square = 15.869 p-value = 0.103 | |||
| Poor | Good | ||||
| 4. How confident are you about performing the home program | <5 | 33 | 7 | 40 | |
| 5 and above | 49 | 30 | 69 | ||
| Mothers’ Adherence | Total | Chi-square = 5.484 p-value = 0.241 | |||
| Poor | Good | ||||
| 5. My partner supports me at home | Never | 16 | 5 | 21 | |
| Rarely | 16 | 5 | 21 | ||
| Sometimes | 26 | 17 | 43 | ||
| Often | 11 | 5 | 16 | ||
| Always | 3 | 5 | 8 | ||
| Mothers’ Adherence | Total | Chi-square = 2.808 p-value = 0.104 | |||
| Poor | Good | ||||
| 6. I have the equipment required to do the exercises at home | No | 47 | 18 | 65 | |
| Yes | 25 | 19 | 44 | ||
| Model | R | R2 | Adjusted R2 | Std. Error of the Estimate | Durbin-Datson Test |
|---|---|---|---|---|---|
| 1 | 0.354 a | 0.125 | 0.100 | 1.62340 | 1.871 |
| Model | Sum of Squares | df | Mean Square | F | Sig. | |
|---|---|---|---|---|---|---|
| 1 | Regression | 39.564 | 3 | 13.188 | 5.004 | 0.003 b |
| Residual | 276.721 | 105 | 2.635 | |||
| Total | 316.284 | 108 | ||||
| Model | Unstandardized Coefficients | Standardized Coefficients | t | Sig. | ||
|---|---|---|---|---|---|---|
| B | Std. Error | Beta | ||||
| 1 | (Constant) | 2.759 | 0.648 | 4.255 | 0.000 | |
| Social support | 0.302 | 0.242 | 0.156 | 1.249 | 0.041 | |
| Health professionals’ behavior | 0.430 | 0.190 | 0.268 | 2.265 | 0.026 | |
| Mother’s sense of unsureness | −0.537 | 0.179 | −0.306 | −3.003 | 0.003 | |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Alwhaibi, R.M.; Omer, A.B.; Khan, R. Factors Affecting Mothers’ Adherence to Home Exercise Programs Designed for Their Children with Cerebral Palsy. Int. J. Environ. Res. Public Health 2022, 19, 10792. https://doi.org/10.3390/ijerph191710792
Alwhaibi RM, Omer AB, Khan R. Factors Affecting Mothers’ Adherence to Home Exercise Programs Designed for Their Children with Cerebral Palsy. International Journal of Environmental Research and Public Health. 2022; 19(17):10792. https://doi.org/10.3390/ijerph191710792
Chicago/Turabian StyleAlwhaibi, Reem M., Asma B. Omer, and Ruqaiyah Khan. 2022. "Factors Affecting Mothers’ Adherence to Home Exercise Programs Designed for Their Children with Cerebral Palsy" International Journal of Environmental Research and Public Health 19, no. 17: 10792. https://doi.org/10.3390/ijerph191710792
APA StyleAlwhaibi, R. M., Omer, A. B., & Khan, R. (2022). Factors Affecting Mothers’ Adherence to Home Exercise Programs Designed for Their Children with Cerebral Palsy. International Journal of Environmental Research and Public Health, 19(17), 10792. https://doi.org/10.3390/ijerph191710792






