Social, Economic and Overall Health Impacts of COVID-19 on People Living with Disabilities in King County, WA
Abstract
:1. Introduction
2. Materials and Methods
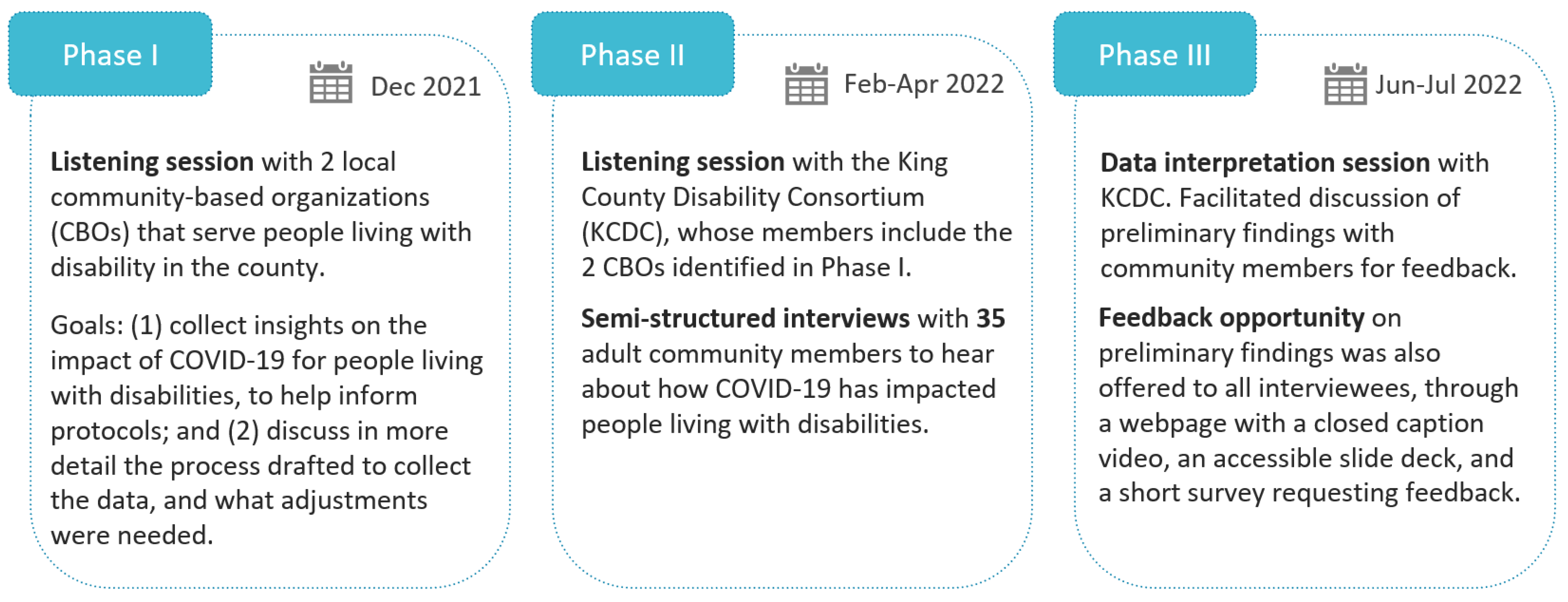
2.1. Study Design
2.2. Qualitative Interviewer Training
2.3. Recruitment and Data Collection
2.3.1. Interviews
2.3.2. Listening Sessions
2.4. Analysis
3. Results
3.1. Demographics of Interviewees
3.2. Findings
3.2.1. Impacts of COVID-19 for People Living with Disabilities
Work/Employment
“Because I’m immunosuppressed, at high risk for COVID, I decided to just work online. And that really impacted the hours that I’m working. I’m working less because of that. They don’t have a lot of the online work for me to do. Not as much as when I was working in-person”.(Interviewee)
“… it’s been pretty hard to maintain employment because of what’s going on with my mental health. At one point during the pandemic, I was working [an] on call job and it was really bad for my mental health, so I actually had to leave the job. So, [for] most of the pandemic, I have not been working”.(Interviewee)
“I will add that some positives that came out of it—that people who have disabilities … would have liked to have seen adapted a lot faster that [the] pandemic made possible—was the push towards remote work. I don’t drive or anything like that. So, going into work I was always very limited … Now that there are so many options out there that are purely remote that gives me a lot more opportunity to be able to find employment”.(KCDC member)
Finances
“… with my lack of job stability because of the pandemic and not having employers that are aligned with my safety standards … I’ve racked up I think almost $10,000 in debt and credit card debt being in between jobs and needing to support my family and pay rent”.(Interviewee)
“I also had like a tragedy, a personal tragedy happened during the pandemic … a suicide in the family and that really deeply impacted me, and I was not able to get treatment for that … To be able to get treatment for that would have also been paying out of pocket … I wasn’t able to get … grief counseling or anything really that I needed for that”.(Interviewee)
“I was already not receiving, not getting any money and it [COVID-19] made it easier for me to get ADB [Aged, Blind or Disabled Cash Assistance]. That was something that was a relief. People were more giving of money than they had been in the past because they knew that everyone was going through something”.(Interviewee)
Food Security
“I’m starving like about a week and a half, two weeks [per month]. …[on] the last week of the month I’m totally broke. I don’t have no food. You know, it’s just crazy … It’s just hard to survive off of what I received from SSI [Supplemental Security Income]”.(Interviewee)
“Food has been so expensive. They increased the food stamp amount to the maximum but that didn’t even last a month. Then the rest of the month, I had to rely on food banks, but food banks aren’t getting the donations that they used to, so they’re short on food and yeah, it’s been a real struggle. There have been times when I lose weight, because I’m forced to eat only one meal a day because I can’t afford to eat more than that”.(Interviewee)
Housing
“Another impact [of COVID-19] … is that I [had] to move. I’m not really going to be living in Seattle that much longer. Just because the cost of living has … They’re raising my rent … And so it’s just not really working for me living here. So, I’m having to uproot my life now, which is really stressful”.(Interviewee)
“It’s made me have a house. I think that one of the things that was sad for so many people. So many people lost a lot. But for the homeless, I think it helped a lot of people get housed”.((Interviewee)
Mental Health
“I think the main thing I’ve noticed in the pandemic is particularly around mental health, that’s where I feel it the most. The longer I’ve been in the pandemic I just feel like it really adds to burnout and everything else going on and so they’re just really—there are days where it’s just really hard to get up in the morning …”(Interviewee)
“COVID … has impacted my lifestyle pretty severely. I have virtually no social life … I do deal with anxiety, and it has been getting worse and worse, and I’m trying to manage it. But the restrictions because of COVID has [sic] made my anxiety quite a bit worse and I am sensitive to the anxiety around me, which is everywhere I go. And it’s, you know, so yeah, the atmosphere of mistrust, the atmosphere of anxiety with a lot of people. I think the anxiety over … I mean, a lot of people are very anxious about the economy, and you know, there’s just a lot of that so that impacts me pretty strong”.(Interviewee)
“it’s definitely affected my mental health. … my PTSD has been skyrocketing, my anxiety levels have been skyrocketing. I feel like kind of paralyzed a lot of the time now, like, just in my day-to-day life, I just feel very like paralyzed with anxiety. … because I don’t really have much stability in my life right now. … I don’t really feel like I have a sense of security anymore, which is a pretty bad feeling”.(Interviewee)
“I think the pandemic has really shed a light on the importance of putting an emphasis on taking care of yourself and mental health and we still have a long way to go as a society. I think that companies are getting more to that point that yes you can take a mental health day”.(KCDC member)
Physical Health
Physical and Emotional Safety
“I have felt anxious and depressed more often. I have had less healthy habits, eating less. Less exercise, less hobbies. I lost access to counselors and my support system. I lost access to medications for mental health as well as losing my therapist. I went through a sexual assault from someone that I had known for four years during the pandemic. I had that question from someone else a while ago and I found it interesting that sexual violence increased during the pandemic”.(Interviewee)
Access to Services
“I have gone from going into the hospital at least once a week (often two times a week) to once every couple of months. Honestly, I’m terrified every time I go in. I have gone in and doctors were not wearing masks in the lobby … Waiting rooms are completely packed and no social distancing. I get terrified. Truly terrified”.(KCDC member)
Transportation
“Drive up and go shopping is great, if you have a car. If you don’t have a car, and you are at increased risk of contracting COVID, it may be too risky to take public transit, further increasing isolation”.(KCDC member)
“The domino effect in terms of stay-at-home orders and social distancing orders [is that] a lot of the clients we work directly with on my team are people with specialized transportation needs. People with disabilities, older adults, folks with limited mobility. What we saw and what we continue to see during the pandemic especially early on [is] a reduction in available services, which led to longer wait times, more uncertainty around a service being able to pick you up and drop you off where you needed, more anxiety and worry around safety while on those transportation whether it is a shuttle or individual’s car. Particularly volunteer-based services have been impacted and those are the services that in years previous have come highly recommended and were preferred because they offered a sense of community and connection to a lot of our clients … A lot of volunteers decided to stop driving for their own safety for their own health and wellness …”(KCDC member)
Education
“I don’t think that the schools were equipped to help children with disabilities succeed; and with their IEP plans [Individualized Educational Plan] and putting that on the back burner and not giving kids their hours that are needed, and having that put on the parents even more to make sure their child is getting what they are owed while also even working or not having access to internet or a computer. So, I think there was a huge educational impact when it came to [mitigation stay-at-home orders]—and stay-at-home orders are great, and we should definitely stay home and be safe … I’m not sure if the schools could have done more to help families”.(KCDC member)
How COVID-19 Impacts Differed for People Living with Disabilities
“COVID-19 impacts people with disabilities significantly differently because they are already at high risk for contracting, getting sick from, and dying from COVID-19. We all have different forms of care that we need and seek from the medical system, and when the system is overburdened and at capacity, people with disabilities lose their essential support and critical care that they need to survive, to live, to thrive”.(Interviewee)
3.2.2. Supports to Deal with Impacts of COVID-19
Helpful Supports for COVID-19 Impacts
Barriers to Accessing Resources
“… fighting with insurance to get [medication]… yeah, that was not fun, and then fighting with the people for unemployment. And I’m sick during this period, I mean, it’s like insane, I should not have been dealing with all of that at once”.(Interviewee)
Potential Improvements for COVID-19-Related Supports
3.2.3. Other Themes
Disenfranchisement
“… we are not collecting statistics on people with disabilities. When I got testing, never once did anyone ask if I had a disability. That is huge … You can’t recognize us as a community until you look at our data and collect data on us especially in this data-driven world. We are making funding decisions based on data. If we are not collecting information about us, then we are not included in those decisions or disproportionately unequally included”.(KCDC member)
Reactions about Government Policies
“At the very least, please be transparent and actually tell the public the truth, that the mask mandate is not going away because it’s actually safer. … lots of people trust you [the WA state DOH] and follow the mask mandates, and they believe that the mask mandates will only be lifted when it’s safe, so therefore the mask mandates being lifted means it’s safe. People really believe that. But it’s not true. It’s not any safer. It’s just that the hospitals are less overwhelmed. Over and over again, cases start to go down, mask mandate gets lifted, then they climb back up, then the mask mandates go into effect again. People see it as inconsistency, and they lose belief and are less likely to follow mandates when they are in effect. At least tell people that they are not actually safer, it’s just that the healthcare system is ready/equipped for the next spike”.(KCDC member)
Concerns about the near Future
“I’m very concerned about communities not bouncing back from this in the same way they were before. Like HIV/AIDS epidemic, when it first started, like where people were dying and the government wasn’t doing anything … they just didn’t care because they were considered like a disposable population”.(Interviewee)
4. Discussion and Lessons Learned
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Wong, E.Y.; Schachter, A.; Collins, H.N.; Song, L.; Ta, M.T.; Dawadi, S.; Neal, S.; Pajimula, F.F.; Colombara, D.V.; Johnson, K.; et al. Cross-sector monitoring and evaluation framework: Social, economic, and health conditions impacted during the COVID-19 Pandemic. Am. J. Public Health 2021, 111, S215–S223. [Google Scholar] [CrossRef]
- An Approach for Monitoring and Evaluating Community Mitigation Strategies for COVID-19. Available online: https://www.cdc.gov/coronavirus/2019-ncov/php/monitoring-evaluating-community-mitigation-strategies.html (accessed on 21 July 2022).
- Equity and Social Justice. Available online: https://kingcounty.gov/elected/executive/equity-social-justice.aspx (accessed on 21 July 2022).
- Disability Empowerment Center. Available online: https://www.disabilityempowerment.org/ (accessed on 21 July 2022).
- Lifelong. Available online: https://www.lifelong.org/ (accessed on 21 July 2022).
- Disability and Health Data System, Centers for Disease Control and Prevention. Available online: https://www.cdc.gov/ncbddd/disabilityandhealth/dhds/index.html (accessed on 21 July 2022).
- King County Community Health Indicators, Adults Living with Disabilities. Available online: https://kingcounty.gov/depts/health/data/community-health-indicators/behavioral-risk-factor-surveillance-system.aspx?shortname=Disability (accessed on 21 July 2022).
- Disability and Health Data System (DHDS) Data Guide Status and Types. Available online: https://www.cdc.gov/ncbddd/disabilityandhealth/dhds/data-guide/status-and-types.html (accessed on 12 August 2022).
- Dixon-Ibarra, A.; Horner-Johnson, W. Disability status as an antecedent to chronic conditions: National Health Interview Survey, 2006–2012. Prev. Chronic. Dis. 2014, 11, 130251. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Okoro, C.A.; Hollis, N.D.; Cyrus, A.C.; Griffin-Blake, S. Prevalence of disabilities and health care access by disability status and type among adults—United States. 2016. Morb. Mortal. Wkly. Rep. 2018, 67, 882–887. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Preliminary estimates of the prevalence of selected underlying health conditions among patients with coronavirus disease—United States, February 12–March 28, 2020. Morb. Mortal. Wkly. Rep. 2020, 69, 382–386. [CrossRef] [PubMed]
- Navas, P.; Amor, A.M.; Crespo, M.; Wolowiec, Z.; Verdugo, M.Á. Supports for people with intellectual and developmental disabilities during the COVID-19 pandemic from their own perspective. Res. Dev. Disabil. 2021, 108, 103813. [Google Scholar] [CrossRef] [PubMed]
- Chicoine, C.; Hickey, E.E.; Kirschner, K.L.; Chicoine, B.A. Ableism at the bedside: People with intellectual disabilities and COVID-19. J. Am. Board Fam. Med. 2022, 35, 390–393. [Google Scholar] [CrossRef]
- Gleason, H.; Ross, W.; Fossi, A.; Blonsky, H.; Tobias, J.; Stephens, M. The devastating impact of COVID-19 on individuals with intellectual disabilities in the United States. N. Engl. J. Med. 2021. [Google Scholar] [CrossRef]
- Mirouse, A.; Darmon, M.; Zafrani, L.; Lengliné, E.; Azoulay, E. Impact of immunosuppression on mortality in critically ill COVID-19 patients. Br. J. Haematol. 2020, 191, 394–395. [Google Scholar] [CrossRef]
- Feng, Y.; Ling, Y.; Bai, T.; Xie, Y.; Huang, J.; Li, J.; Xiong, W.; Yang, D.; Chen, R.; Lu, F.; et al. COVID-19 with different severities: A multicenter study of clinical features. Am. J. Respir. Crit. Care Med. 2020, 201, 1380–1388. [Google Scholar] [CrossRef]
- Goldman, J.D.; Robinson, P.C.; Uldrick, T.S.; Ljungman, P. COVID-19 in immunocompromised populations: Implications for prognosis and repurposing of immunotherapies. J. Immunother. Cancer. 2021, 9, e002630. [Google Scholar] [CrossRef]
- Park, J.; Sung, C.; Fisher, M.H.; Okyere, C.; Kammes, R.R. Psychosocial and vocational impacts of COVID-19 on people with and without disabilities. Rehabil. Psychol. 2022, 67, 381–390. [Google Scholar] [CrossRef] [PubMed]
- Pfeiffer, B.; Brusilovskiy, E.; Hallock, T. Impact of COVID-19 on Community Participation and Mobility in Young Adults with Autism Spectrum Disorders. J. Autism. Dev. Disord. 2022, 52, 1553–1567. [Google Scholar] [CrossRef] [PubMed]
- Koon, L.M.; Greiman, L.; Schulz, J.A.; Goddard, K.S.; Nzuki, I.M.; Hall, J.P. Examining the effects of the COVID-19 pandemic on community engagement for people with mobility disabilities. Disabil. Health J. 2022, 15, 1936–6574. [Google Scholar] [CrossRef]
- Jonikas, J.A.; Cook, J.A.; Swarbrick, M.; Nemec, P.; Steigman, P.J.; Boss, K.A.; Brice, G.H. The impact of the COVID-19 pandemic on the mental health and daily life of adults with behavioral health disorders. Transl. Behav. Med. 2021, 11, 1162–1171. [Google Scholar] [CrossRef] [PubMed]
- Amuedo-Dorantes, C.; Kaushal, N.; Muchow, A.N. Is the Cure Worse than the Disease? County-Level Evidence from the COVID-19 Pandemic in the United States. IZA Discussion Paper 13695. 2020. Available online: https://ssrn.com/abstract=3695396 (accessed on 12 August 2022).
- Ebrahim, S.; Ashworth, H.; Noah, C.; Kadambi, A.; Toumi, A.; Chhatwal, J. Reduction of COVID-19 Incidence and Nonpharmacologic Interventions: Analysis Using a US County–Level Policy Data Set. J. Med. Internet Res. 2020, 22, e24614. [Google Scholar] [CrossRef]
- Economic, Social, and Overall Health Impacts Dashboard. Available online: https://kingcounty.gov/depts/health/covid-19/data/impacts.aspx (accessed on 21 July 2022).
- Phonic AI Software. Available online: https://www.phonic.ai/ (accessed on 18 July 2022).
- Braun, V.; Clarke, V. Thematic analysis. Am. Psychol. 2012, 2, 57–71. [Google Scholar] [CrossRef]
- Dedoose, Version 9.0.54, Web Application for Managing, Analyzing, and Presenting Qualitative and Mixed Method Research data; SocioCultural Research Consultants, LLC.: Los Angeles, CA, USA, 2022. Available online: https://dedoose.com (accessed on 12 August 2022).
- Fleiss, J.L. Measuring nominal scale agreement among many raters. Psychol. Bull. 1991, 76, 378–382. [Google Scholar] [CrossRef]
- Cicchetti, D.V. Guidelines, criteria, and rules of thumb for evaluating normed and standardized assessment instruments in psychology. Psychol. Assess. 1994, 6, 284–290. [Google Scholar] [CrossRef]
- Santini, K.; Disability Empowerment Center, Washington, USA. Personal communication, 2022.
- King County COVID-19 Vaccination Dashboard. Available online: https://kingcounty.gov/depts/health/covid-19/data/vaccination.aspx (accessed on 12 August 2022).
- Goddard, K.S.; Schulz, J.; Nzuki, I.; Hall, J.P. Examining the Impacts of the Coronavirus Pandemic and Social Distancing on the Health of People with Mobility Disabilities. Front. Public Health. 2022. [Google Scholar] [CrossRef]
- Washington State 2020 CORONA Survey: King County Results. Available online: https://kingcounty.gov/depts/health/covid-19/data/impacts/corona.aspx (accessed on 12 August 2022).
- Behavioral Health Needs and Services; Economic, Social, and Overall Impacts. Available online: https://kingcounty.gov/depts/health/covid-19/data/impacts/behavioral-health.aspx (accessed on 12 August 2022).
- Wang, K.; Manning, R.B.; Bogart, K.R.; Adler, J.M.; Nario-Redmond, M.R.; Ostrove, J.M.; Lowe, S.R. Predicting depression and anxiety among adults with disabilities during the COVID-19 pandemic. Rehabil. Psychol. 2022, 67, 179–188. [Google Scholar] [CrossRef]
- Lund, E.M.; Forber-Pratt, A.J.; Wilson, C.; Mona, L.R. The COVID-19 pandemic, stress, and trauma in the disability community: A call to action. Rehabil. Psychol. 2020, 65, 313–322. [Google Scholar] [CrossRef] [PubMed]
- Bowleg, L. Evolving Intersectionality Within Public Health: From Analysis to Action. Am. J. Public Health. 2021, 111, 88–90. [Google Scholar] [CrossRef] [PubMed]
| Topic Area | Indicator |
|---|---|
| Economic | Unemployment claims |
| Social service needs | |
| Traffic, transportation | |
| Social | Food insecurity |
| Family violence | |
| Access to internet and technology | |
| Social impacts on childcare, work, ability to stay at home | |
| Health | Access to care |
| Mental and behavioral health | |
| Changes to death patterns | |
| Policy | Federal, state, county, city policies pertaining to COVID-19 |
| Demographics | % | n = 35 |
|---|---|---|
| Age group | ||
| 18–24 | 9% | 3 |
| 25–34 | 40% | 14 |
| 35–44 | 6% | 2 |
| 45–54 | 14% | 5 |
| 55–64 | 11% | 4 |
| 65+ | 20% | 7 |
| Gender * | ||
| Female | 63% | 22 |
| Non-binary/genderqueer | 23% | 8 |
| Male | 11% | 4 |
| Transgender/other | 11% | 4 |
| Disability type * | ||
| Mental health condition (depression, anxiety, bipolar, schizophrenia, etc.) | 91% | 32 |
| Other disability or chronic condition (dyslexia, HIV/AIDS, cancer, diabetes, etc.) | 83% | 29 |
| Developmental or intellectual disability (Down syndrome, Autism, ADHD, etc.) | 54% | 19 |
| Mobility disability (use a wheelchair, walker, cane, prosthetic, etc.) | 43% | 15 |
| Sensory disability (blindness, low-vision, d/Deaf, hard-of-hearing, Deaf, Blind, etc.) | 8% | 8 |
| Race/ethnicity * | ||
| American Indian/Alaska Native | 9% | 3 |
| Asian | 14% | 5 |
| Black | 23% | 3 |
| Hispanic | 3% | 1 |
| Native Hawaiian/Pacific Islander | 6% | 2 |
| White | 66% | 23 |
| Another race/ethnicity | 6% | 2 |
| Prefer not to answer | 6% | 2 |
| Previously tested positive for COVID | ||
| Yes | 20% | 7 |
| No | 80% | 28 |
| Vaccination status | ||
| Fully vaccinated and boosted | 69% | 24 |
| 2 shots only | 23% | 8 |
| Not vaccinated | 9% | 3 |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Turcheti, N.; Laurent, A.A.; Delgado, C.; Sainati, K.; Johnson, K.; Wong, E.Y. Social, Economic and Overall Health Impacts of COVID-19 on People Living with Disabilities in King County, WA. Int. J. Environ. Res. Public Health 2022, 19, 10520. https://doi.org/10.3390/ijerph191710520
Turcheti N, Laurent AA, Delgado C, Sainati K, Johnson K, Wong EY. Social, Economic and Overall Health Impacts of COVID-19 on People Living with Disabilities in King County, WA. International Journal of Environmental Research and Public Health. 2022; 19(17):10520. https://doi.org/10.3390/ijerph191710520
Chicago/Turabian StyleTurcheti, Nicole, Amy A. Laurent, Christina Delgado, Kayla Sainati, Kris Johnson, and Eva Y. Wong. 2022. "Social, Economic and Overall Health Impacts of COVID-19 on People Living with Disabilities in King County, WA" International Journal of Environmental Research and Public Health 19, no. 17: 10520. https://doi.org/10.3390/ijerph191710520
APA StyleTurcheti, N., Laurent, A. A., Delgado, C., Sainati, K., Johnson, K., & Wong, E. Y. (2022). Social, Economic and Overall Health Impacts of COVID-19 on People Living with Disabilities in King County, WA. International Journal of Environmental Research and Public Health, 19(17), 10520. https://doi.org/10.3390/ijerph191710520






