The North Italian Longitudinal Study Assessing the Mental Health Effects of SARS-CoV-2 Pandemic on Health Care Workers—Part I: Study Design and Psychometric Structural Validity of the HSE Indicator Tool and Work Satisfaction Scale
Abstract
:1. Introduction
2. Materials and Methods
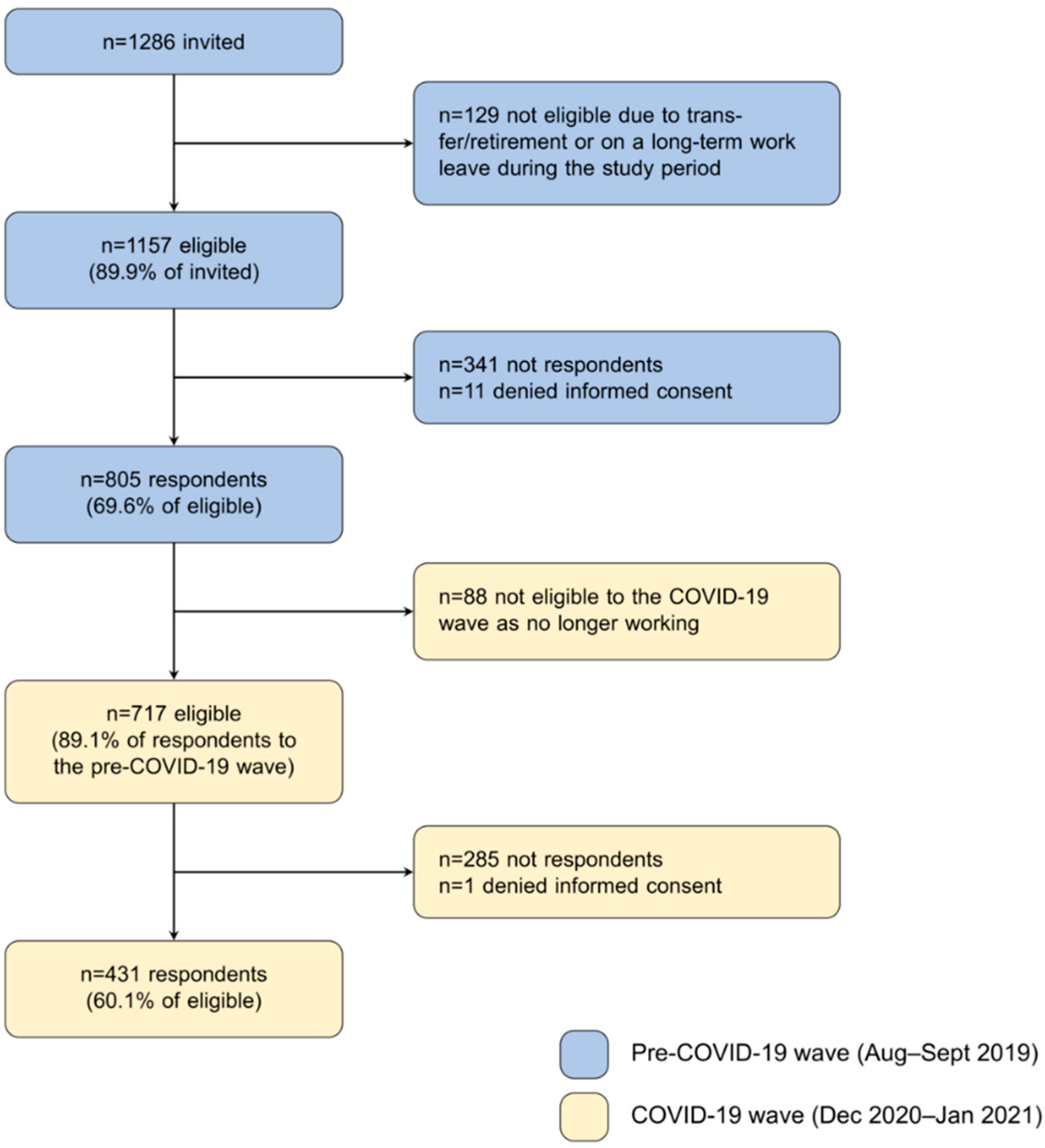
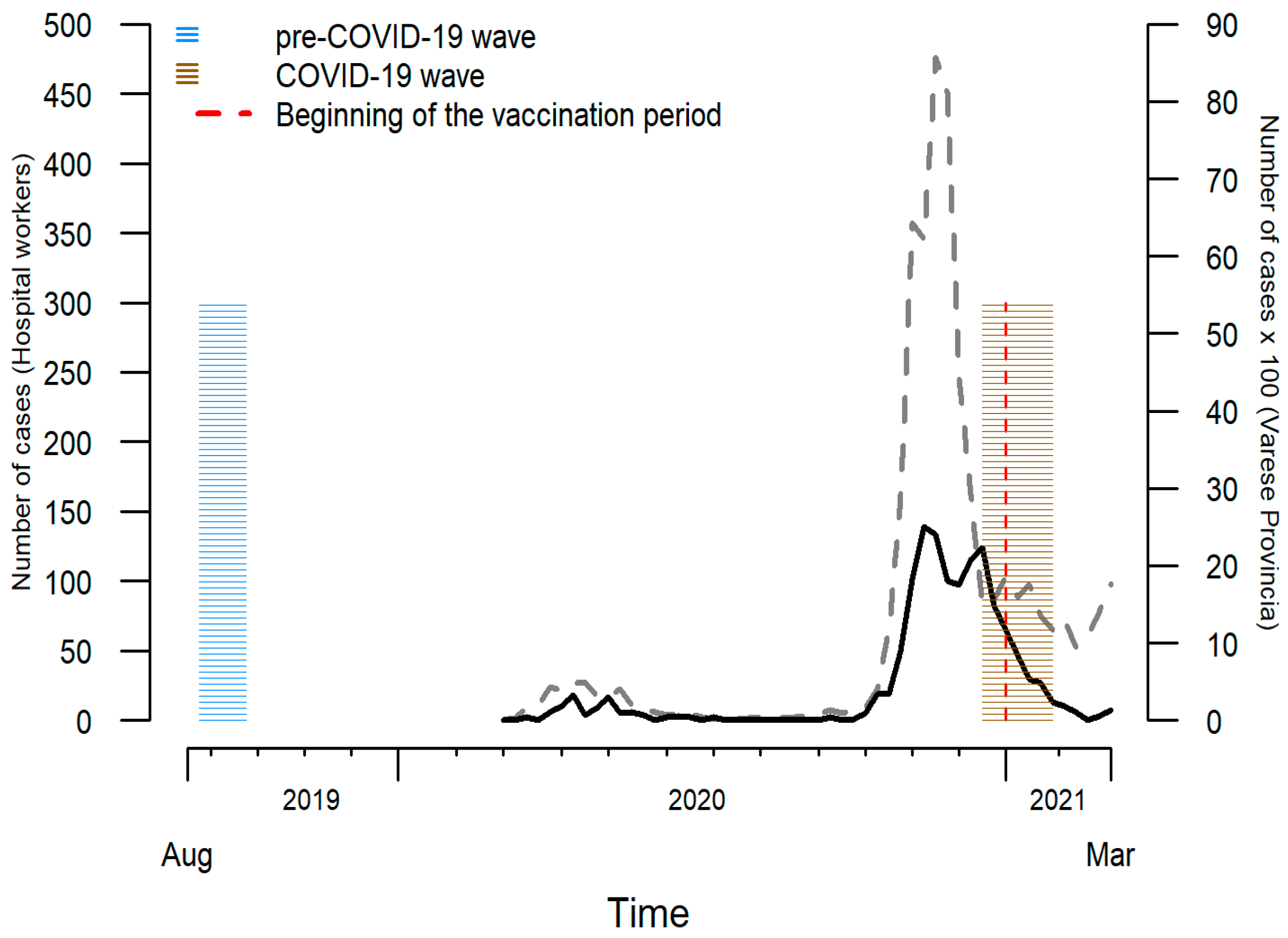
2.1. Study Population, Design and Recruitment
2.2. Assessment of Demographic and Work-Related Characteristics in the Pre-COVID-19 Wave
2.3. Assessment of Work Stress and Work Satisfaction in the Pre-COVID-19 Wave
2.4. Assessment of Burnout and Mental Health
2.5. Statistical Analysis
3. Results
3.1. Sample Representativeness at the Pre-COVID-19 Wave
3.2. Sample Representativeness at the COVID-19 Wave
3.3. Structural Validity of the HSE-IT Questionnaire
3.4. Structural Validity of the Work Satisfaction Scale
4. Discussion
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Sim, M.R. The COVID-19 pandemic: Major risks to healthcare and other workers on the front line. Occup. Environ. Med. 2020, 77, 281–282. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Nafilyan, V.; Pawelek, P.; Ayoubkhani, D.; Rhodes, S.; Pembrey, L.; Matz, M.; Coleman, M.; Allemani, C.; Windsor-Shellard, B.; van Tongeren, M.; et al. Occupation and COVID-19 mortality in England: A national linked data study of 14.3 million adults. Occup. Environ. Med. 2021, 79, 433–441. [Google Scholar] [CrossRef]
- BMA. COVID-19: The Impact of Pandemic on the Medical Profession. May 2022. Available online: https://www.bma.org.uk/advice-and-support/covid-19/what-the-bma-is-doing/covid-19-the-impact-of-the-pandemic-on-the-medical-profession (accessed on 6 June 2022).
- Abbasi, J. Pushed to Their Limits, 1 in 5 Physicians Intends to Leave Practice. JAMA 2022, 327, 1435. [Google Scholar] [CrossRef]
- Kisely, S.; Warren, N.; McMahon, L.; Dalais, C.; Henry, I.; Siskind, D. Occurrence, prevention, and management of the psychological effects of emerging virus outbreaks on healthcare workers: Rapid review and meta-analysis. BMJ 2020, 369, m1642. [Google Scholar] [CrossRef] [PubMed]
- Galanis, P.; Vraka, I.; Fragkou, D.; Bilali, A.; Kaitelidou, D. Nurses’ burnout and associated risk factors during the COVID-19 pandemic: A systematic review and meta-analysis. J. Adv. Nurs. 2021, 77, 3286–3302. [Google Scholar] [CrossRef] [PubMed]
- Chigwedere, O.C.; Sadath, A.; Kabir, Z.; Arensman, E. The Impact of Epidemics and Pandemics on the Mental Health of Healthcare Workers: A Systematic Review. Int. J. Environ. Res. Public Health 2021, 18, 6695. [Google Scholar] [CrossRef] [PubMed]
- Holmes, M.R.; Rentrope, C.R.; Korsch-Williams, A.; King, J.A. Impact of COVID-19 Pandemic on Posttraumatic Stress, Grief, Burnout, and Secondary Trauma of Social Workers in the United States. Clin. Soc. Work J. 2021, 49, 495–504. [Google Scholar] [CrossRef]
- Caldas, M.P.; Ostermeier, K.; Cooper, D. When helping hurts: COVID-19 critical incident involvement and resource depletion in health care workers. J. Appl. Psychol. 2021, 106, 29–47. [Google Scholar] [CrossRef]
- Ghahramani, S.; Lankarani, K.B.; Yousefi, M.; Heydari, K.; Shahabi, S.; Azmand, S. A Systematic Review and Meta-Analysis of Burnout Among Healthcare Workers During COVID-19. Front. Psychiatry 2021, 12, 758849. [Google Scholar] [CrossRef]
- Magnavita, N.; Soave, P.M.; Antonelli, M. A One-Year Prospective Study of Work-Related Mental Health in the Intensivists of a COVID-19 Hub Hospital. Int. J. Environ. Res. Public Health 2021, 18, 9888. [Google Scholar] [CrossRef]
- Brera, A.S.; Arrigoni, C.; Dellafiore, F.; Odone, A.; Magon, A.; Nania, T.; Pittella, F.; Palamenghi, L.; Barello, S.; Caruso, R. Burnout syndrome and its determinants among healthcare workers during the first wave of the COVID-19 outbreak in Italy: A cross-sectional study to identify sex-related differences. Med. Lav. 2021, 112, 306–319. [Google Scholar] [CrossRef]
- Campanini, P. Methodological issues in assessing job stress and burnout in psychosocial research. Med. Lav. 2021, 112, 264–267. [Google Scholar] [CrossRef] [PubMed]
- Hacimusalar, Y.; Misir, E.; Kahve, A.C.; Hacimusalar, G.D.; Guclu, M.A.; Karaaslan, O. The effects of working and living conditions of physicians on burnout level and sleep quality. Med. Lav. 2021, 112, 346–359. [Google Scholar] [CrossRef]
- Olino, T.M.; Case, J.A.C.; Hawes, M.T.; Szenczy, A.; Nelson, B.; Klein, D.N. Testing Invariance of Measures of Internalizing Symptoms Before and After a Major Life Stressor: The Impact of COVID-19 in an Adolescent and Young Adult Sample. Assessment, 2021; online ahead of print. [Google Scholar] [CrossRef]
- Pisanti, R.; van der Doef, M.; Maes, S.; Meier, L.L.; Lazzari, D.; Violani, C. How Changes in Psychosocial Job Characteristics Impact Burnout in Nurses: A Longitudinal Analysis. Front. Psychol. 2016, 7, 1082. [Google Scholar] [CrossRef] [Green Version]
- Langballe, E.M.; Innstrand, S.T.; Aasland, O.G.; Falkum, E. The predictive value of individual factors, work-related factors, and work-home interaction on burnout in female and male physicians: A longitudinal study. Stress Health 2010, 27, 73–87. [Google Scholar] [CrossRef]
- Cousins, R.; Mackay, C.J.; Clarke, S.D.; Kelly, C.; Kelly, P.J.; McCaig, R.H. Management Standards and work-related stress in the UK: Practical development. Work Stress 2004, 18, 113–136. [Google Scholar] [CrossRef]
- Iavicoli, S.; Natali, E.; Rondinone, B.M.; Castaldi, T.; Persechino, B. Implementation and validation in the Italian context of the HSE management standards: A contribution to provide a practical model for the assessment of work-related stress. G. Ital. Med. Lav. Ergon. 2011, 32, 130–133. [Google Scholar]
- Magnavita, N. Validation of the Italian version of the HSE Indicator Tool. Occup. Med. Lond. 2012, 62, 288–294. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Edwards, J.A.; Webster, S.; Van Laar, D.; Easton, S. Psychometric analysis of the UK Health and Safety Executive’s Management Standards work-related stress Indicator Tool. Work Stress 2008, 22, 96–107. [Google Scholar] [CrossRef]
- Brookes, K.; Limbert, C.; Deacy, C.; O’Reilly, A.; Scott, S.; Thirlaway, K. Systematic review: Work-related stress and the HSE Management Standards. Occup. Med. 2013, 63, 463–472. [Google Scholar] [CrossRef] [Green Version]
- Giusti, E.M.; Veronesi, G.; Callegari, C.; Calstelnuovo, G.; Iacoviello, L.; Ferrario, M.M. The North Italian Longitudinal Study assessing the Mental Health effects of SARS-CoV-2 pandemic Health Care Workers—Part II: Structural validity of scales assessing mental health paper. Int. J. Environ. Res. Public Health, 2022; accepted. [Google Scholar]
- Dong, E.; Du, H.; Gardner, L. An interactive web-based dashboard to track COVID-19 in real time. Lancet Infect. Dis. 2020, 20, 533–534. [Google Scholar] [CrossRef]
- Kristensen, T.S.; Hannerz, H.; Høgh, A.; Borg, V. The Copenhagen Psychosocial Questionnaire—A tool for the assessment and improvement of the psychosocial work environment. Scand. J. Work Environ. Health 2005, 31, 438–449. [Google Scholar] [CrossRef] [Green Version]
- Maslach, C.; Jackson, S.E. The measurement of experienced burnout. J. Organ. Behav. 1981, 2, 99–113. [Google Scholar] [CrossRef]
- Goldberg, D.P.; Hillier, V.F. A scaled version of the General Health Questionnaire. Psychol. Med. 1979, 9, 139–145. [Google Scholar] [CrossRef]
- Blevins, C.A.; Weathers, F.W.; Davis, M.T.; Witte, T.K.; Domino, J.L. The Posttraumatic Stress Disorder Checklist for DSM-5 (PCL-5): Development and Initial Psychometric Evaluation. J. Trauma. Stress 2015, 28, 489–498. [Google Scholar] [CrossRef] [PubMed]
- Connor, K.M.; Davidson, J.R.T. Development of a new resilience scale: The Connor-Davidson Resilience Scale (CD-RISC). Depress. Anxiety 2003, 18, 76–82. [Google Scholar] [CrossRef] [PubMed]
- Tedeschi, R.G.; Calhoun, L.G. The Posttraumatic Growth Inventory: Measuring the positive legacy of trauma. J. Trauma. Stress. 1996, 9, 455–471. [Google Scholar] [CrossRef] [PubMed]
- Ferrario, M.M.; Bertù, L.; Cimmino, L.; Conti, M.; Borsani, A.; Veronesi, G. A multi-dimensional evaluation of job stress integrating organizational and subjective risk indicators: One application to health care workers in Northern Italy. G. Ital. Med. Lav. Ergon. 2013, 33, 315–318. [Google Scholar]
- Little, R.J.A. A Test of Missing Completely at Random for Multivariate Data with Missing Values. J. Am. Stat. Assoc. 1988, 83, 1198. [Google Scholar] [CrossRef]
- Bollen, K.A.; Diamantopoulos, A. In defense of causal-formative indicators: A minority report. Psychol. Methods 2017, 22, 581–596. [Google Scholar] [CrossRef] [PubMed]
- Diamantopoulos, A.; Siguaw, J.A. Formative Versus Reflective Indicators in Organizational Measure Development: A Comparison and Empirical Illustration. Br. J. Manag. 2006, 17, 263–282. [Google Scholar] [CrossRef]
- Hu, L.; Bentler, P.M. Cutoff criteria for fit indexes in covariance structure analysis: Conventional criteria versus new alternatives. Struct. Equ. Model. Multidiscip. J. 1999, 6, 1–55. [Google Scholar] [CrossRef]
- Gomez, S.; Anderson, B.J.; Yu, H.; Gutsche, J.; Jablonski, J.; Martin, N.; Kerlin, M.P.; Mikkelsen, M.E. Benchmarking Critical Care Well-Being: Before and After the Coronavirus Disease 2019 Pandemic. Crit. Care Explor. 2020, 2, e0233. [Google Scholar] [CrossRef]
- Kok, N.; van Gurp, J.; Teerenstra, S.; van der Hoeven, H.; Fuchs, M.; Hoedemaekers, C.; Zegers, M. Coronavirus Disease 2019 Immediately Increases Burnout Symptoms in ICU Professionals: A Longitudinal Cohort Study. Crit. Care Med. 2021, 49, 419–427. [Google Scholar] [CrossRef] [PubMed]
- Jiang, Y.; He, X.; Zhu, Y.; Wu, G.; Gao, X. The Economic Effects of Direct and Indirect Employee Involvement: Evidence From Corporate Social Responsibility Reports of Chinese Listed Companies. Front. Psychol. 2021, 12, 762608. [Google Scholar] [CrossRef]
| Metric | Unit of Measurement | Recruited Hospital Wards/Offices (n = 67) | Other Hospital Wards/Offices (n = 297) | p-Value ^ |
|---|---|---|---|---|
| Turn-over | number per 100 HCWs | 38.9 (15.8; 68.3) | 28.9 (0.0; 63.6) | 0.11 |
| Up/down sizing | number per 100 HCWs | 0.0 (−8.9; 4.8) | 0.0 (−9.3; 0.0) | 0.44 |
| Overload | hours/week per HCW | 1.5 (0.6; 2.4) | 1.1 (0.4; 2.2) | 0.11 |
| Spell of short-term * sick leave | number per 100 HCWs | 124.5 (62.6; 175.2) | 119.7 (42.0; 205.1) | 0.75 |
| Night shifts | number per HCW | 58.5 (20.5; 75.9) | 47.9 (14.4; 79.2) | 0.56 |
| Regular night shifts | percent | 85.3 (41.4; 96.6) | 65.5 (32.9; 97.5) | 0.54 |
| Respondents (n = 431) | Not Respondents (n = 286) | p-Value ^ | |
|---|---|---|---|
| Age, years | 46.5 ± 9.5 | 46.5 ± 10.0 | 0.94 |
| Men, n (%) | 83 (19.3%) | 70 (24.1%) | 0.12 |
| Educational attainment, n (%) | |||
| Less than high school | 50 (11.6%) | 42 (14.7%) | 0.16 |
| High school | 185 (43.0%) | 104 (36.4%) | |
| University degree | 195 (45.4%) | 140 (49.0%) | |
| Work seniority, years | 16.2 ± 10.9 | 15.1 ± 11.4 | 0.21 |
| Type of employment, n (%) | |||
| Full-time | 364 (85.7%) | 250 (87.7%) | 0.25 |
| Part-time | 66 (15.3%) | 35 (12.3%) | |
| Work schedule, n (%) | |||
| Day-time work | 69 (16.1%) | 60 (21.1%) | 0.18 |
| Shift work w/o night shift | 83 (19.3%) | 46 (16.1%) | |
| Shift work with night shift | 278 (64.6%) | 179 (62.8%) | |
| Hospital ward/office, n (%) | |||
| Emergency Department | 182 (42.2%) | 120 (42.0%) | 0.003 |
| Medical wards | 80 (18.6%) | 60 (21.0%) | |
| Surgical wards | 132 (30.6%) | 61 (21.3%) | |
| Administration offices | 37 (8.6%) | 45 (15.7%) |
| Item | Demands | Control | Peer Support | Manager’s Support | Role | Participation in Work Organization | Relationships |
|---|---|---|---|---|---|---|---|
| Item 3 | 0.64 | −0.06 | 0.06 | 0.03 | 0.22 | 0 | −0.06 |
| Item 6 | 0.69 | −0.03 | 0.07 | 0.04 | 0.19 | −0.11 | 0.05 |
| Item 9 | 0.62 | 0.14 | −0.04 | −0.04 | −0.28 | 0.07 | 0.11 |
| Item 12 | 0.69 | −0.07 | 0 | −0.08 | 0.05 | 0.20 | 0.07 |
| Item 16 | 0.42 | 0.21 | −0.12 | 0.16 | −0.16 | 0.01 | 0.15 |
| Item 18 | 0.34 | −0.03 | −0.03 | 0.28 | −0.03 | 0.02 | 0.23 |
| Item 20 | 0.57 | 0.20 | −0.03 | −0.01 | −0.28 | 0.06 | 0.12 |
| Item 22 | 0.73 | 0.03 | 0.11 | 0.02 | 0.09 | −0.04 | 0.01 |
| Item 2 | 0.24 | 0.60 | 0 | 0.04 | −0.14 | −0.03 | −0.06 |
| Item 10 | 0.06 | 0.80 | 0.04 | −0.05 | 0.09 | 0.03 | −0.02 |
| Item 15 | −0.08 | 0.80 | −0.02 | 0.07 | 0.14 | −0.02 | 0.03 |
| Item 19 | −0.13 | 0.77 | 0.10 | 0.05 | 0.03 | 0.08 | −0.05 |
| Item 25 | −0.09 | 0.59 | 0.13 | 0.03 | 0.19 | 0.18 | 0.20 |
| Item 7 | 0.14 | 0.07 | 0.73 | 0.19 | −0.07 | −0.21 | −0.09 |
| Item 24 | 0.03 | 0.10 | 0.78 | 0.08 | −0.07 | −0.02 | 0.10 |
| Item 27 | −0.11 | 0.13 | 0.62 | −0.02 | 0.13 | 0.01 | 0.28 |
| Item 31 | 0 | 0.02 | 0.80 | −0.06 | −0.07 | 0.16 | 0.04 |
| Item 8 | 0.15 | 0.10 | 0.35 | 0.41 | 0.03 | 0.03 | −0.22 |
| Item 23 | 0 | 0.04 | 0 | 0.87 | 0.03 | −0.01 | 0.03 |
| Item 29 | −0.09 | 0.04 | 0.02 | 0.79 | −0.01 | 0.05 | 0.17 |
| Item 35 | −0.04 | 0.02 | 0.02 | 0.83 | 0.03 | 0.10 | −0.03 |
| Item 1 | 0.17 | 0.07 | 0.17 | −0.04 | 0.62 | 0.13 | −0.08 |
| Item 4 | −0.03 | 0.12 | −0.11 | −0.07 | 0.60 | −0.10 | 0.12 |
| Item 11 | 0 | 0.08 | −0.02 | 0.12 | 0.63 | −0.11 | 0.18 |
| Item 13 | 0.07 | −0.04 | 0.03 | 0.24 | 0.61 | 0.24 | −0.07 |
| Item 17 | 0.16 | −0.06 | 0 | 0.09 | 0.56 | 0.37 | −0.13 |
| Item 26 | −0.03 | 0.12 | 0.05 | 0.3 | 0.01 | 0.53 | 0.09 |
| Item 28 | −0.04 | 0.01 | 0.10 | 0.22 | −0.02 | 0.64 | 0.10 |
| Item 30 | 0.05 | 0.15 | −0.10 | 0 | −0.15 | 0.59 | 0.01 |
| Item 32 | 0.05 | −0.03 | 0.05 | −0.01 | 0.23 | 0.68 | −0.03 |
| Item 33 | 0.06 | 0.13 | 0.35 | 0.15 | 0.01 | 0.39 | −0.09 |
| Item 5 | 0.18 | 0.07 | −0.03 | 0.10 | 0.02 | −0.03 | 0.67 |
| Item 14 | −0.04 | −0.1 | 0.46 | −0.05 | 0.07 | 0.18 | 0.53 |
| Item 21 | 0.14 | 0.06 | −0.01 | 0.17 | 0.02 | 0.04 | 0.68 |
| Item 34 | 0.07 | 0 | 0.23 | 0 | 0.11 | −0.02 | 0.48 |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Veronesi, G.; Giusti, E.M.; D’Amato, A.; Gianfagna, F.; Borchini, R.; Castelnuovo, G.; Iacoviello, L.; Ferrario, M.M. The North Italian Longitudinal Study Assessing the Mental Health Effects of SARS-CoV-2 Pandemic on Health Care Workers—Part I: Study Design and Psychometric Structural Validity of the HSE Indicator Tool and Work Satisfaction Scale. Int. J. Environ. Res. Public Health 2022, 19, 9514. https://doi.org/10.3390/ijerph19159514
Veronesi G, Giusti EM, D’Amato A, Gianfagna F, Borchini R, Castelnuovo G, Iacoviello L, Ferrario MM. The North Italian Longitudinal Study Assessing the Mental Health Effects of SARS-CoV-2 Pandemic on Health Care Workers—Part I: Study Design and Psychometric Structural Validity of the HSE Indicator Tool and Work Satisfaction Scale. International Journal of Environmental Research and Public Health. 2022; 19(15):9514. https://doi.org/10.3390/ijerph19159514
Chicago/Turabian StyleVeronesi, Giovanni, Emanuele Maria Giusti, Alessia D’Amato, Francesco Gianfagna, Rossana Borchini, Gianluca Castelnuovo, Licia Iacoviello, and Marco Mario Ferrario. 2022. "The North Italian Longitudinal Study Assessing the Mental Health Effects of SARS-CoV-2 Pandemic on Health Care Workers—Part I: Study Design and Psychometric Structural Validity of the HSE Indicator Tool and Work Satisfaction Scale" International Journal of Environmental Research and Public Health 19, no. 15: 9514. https://doi.org/10.3390/ijerph19159514
APA StyleVeronesi, G., Giusti, E. M., D’Amato, A., Gianfagna, F., Borchini, R., Castelnuovo, G., Iacoviello, L., & Ferrario, M. M. (2022). The North Italian Longitudinal Study Assessing the Mental Health Effects of SARS-CoV-2 Pandemic on Health Care Workers—Part I: Study Design and Psychometric Structural Validity of the HSE Indicator Tool and Work Satisfaction Scale. International Journal of Environmental Research and Public Health, 19(15), 9514. https://doi.org/10.3390/ijerph19159514








