Implementation of a Sense of Home in High-Density Multicultural Singapore Nursing Homes: Challenges and Opportunities
Abstract
:1. Introduction
2. Literature Review
2.1. Environmental Aspects of a Sense of Home in Nursing Homes
2.2. Living Environments in Singapore
3. Materials and Methods
3.1. Five Nursing Homes in Singapore
3.2. Participant Observation
3.3. Focus Group Interviews
3.4. Data Analysis
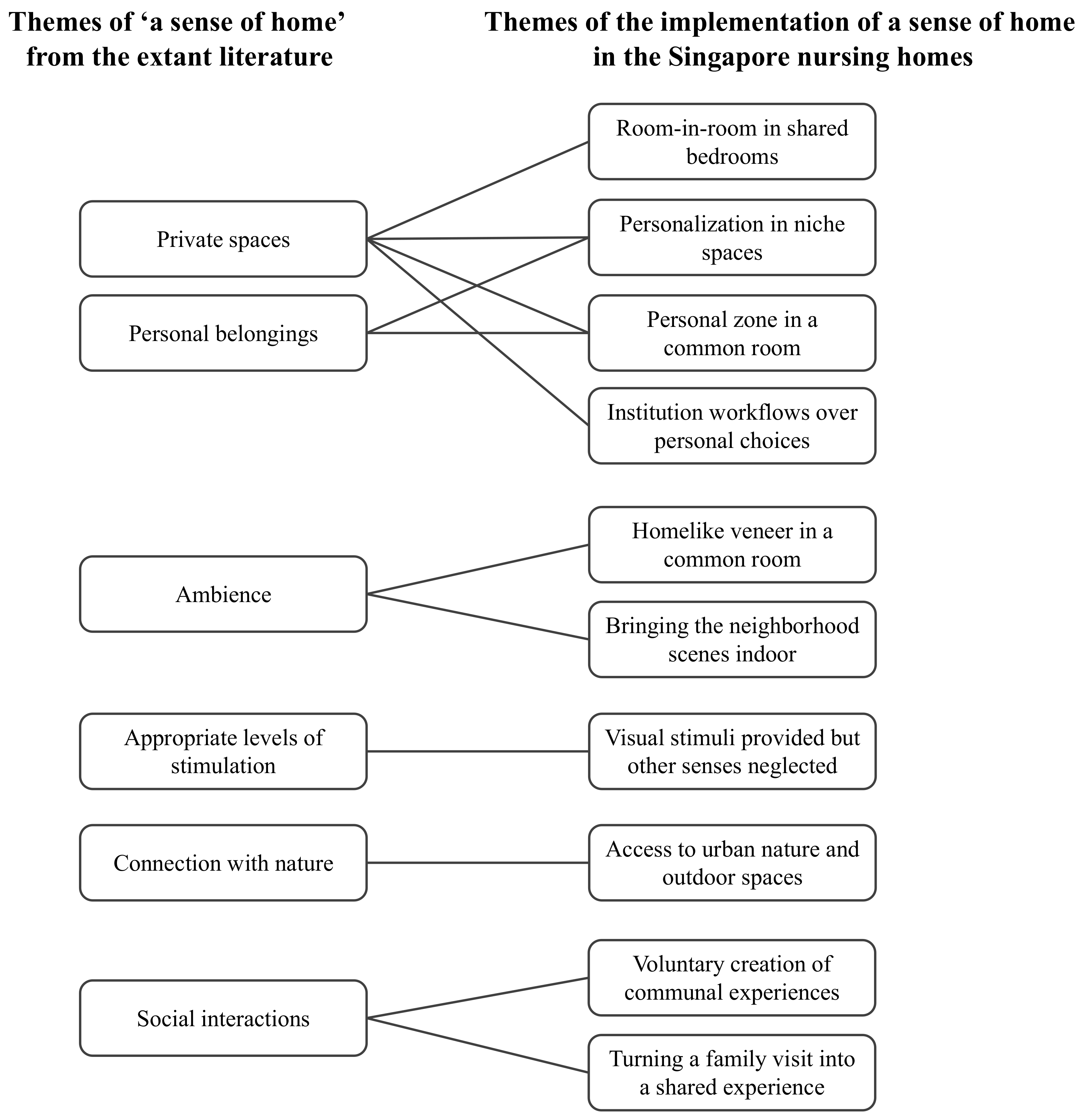
4. Results
4.1. Room-in-Room in Shared Bedrooms
4.2. Personalization in Niche Spaces
4.3. Personal Zone in a Common Room
4.4. Institution Workflows over Personal Choices
“For me, it’s okay. Because I’m not so fussy about that, because they [staff] have to, you know, find a time for me.”—A female resident in NH4.
4.5. Homelike Veneer in a Common Room
4.6. Bringing the Neighborhood Scenes Indoors
4.7. Visual Stimuli Provided but Other Senses Neglected
4.8. Access to Urban Nature and Outdoor Spaces
4.9. Voluntary Creation of Communal Experiences
4.10. Turning a Family Visit into a Shared Experience
5. Discussion
5.1. Privacy Management and Territoriality in the Shared Space
5.2. Holistic Implementation of Homelike Environments
5.3. Pivotal Role of Communal Experiences
5.4. Limitations of the Study
6. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Acknowledgments
Conflicts of Interest
References
- Rijnaard, M.D.; van Hoof, J.; Janssen, B.M.; Verbeek, H.; Pocornie, W.; Eijkelenboom, A.; Beerens, H.C.; Molony, S.L.; Wouters, E.J.M. The Factors Influencing the Sense of Home in Nursing Homes: A Systematic Review from the Perspective of Residents. J. Aging Res. 2016, 2016, 6143645. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- van Hoof, J.; Verbeek, H.; Janssen, B.M.; Eijkelenboom, A.; Molony, S.L.; Felix, E.; Nieboer, K.A.; Zwerts-Verhelst, E.L.M.; Sijstermans, J.J.W.M.; Wouters, E.J.M. A Three Perspective Study of the Sense of Home of Nursing Home Residents: The Views of Residents, Care Professionals and Relatives. BMC Geriatr. 2016, 16, 169. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Fung, J.C. Re-Imagining the Nursing Home in Singapore; National Library of Singapore: Singapore, 2014.
- Hauge, S.; Kristin, H. The Nursing Home as a Home: A Field Study of Residents’ Daily Life in the Common Living Rooms. J. Clin. Nurs. 2008, 17, 460–467. [Google Scholar] [CrossRef] [PubMed]
- Nakrem, S.; Vinsnes, A.G.; Harkless, G.E.; Paulsen, B.; Seim, A. Ambiguities: Residents’ Experience of “Nursing Home as My Home”. Int. J. Older People Nurs. 2013, 8, 216–225. [Google Scholar] [CrossRef] [Green Version]
- Sima, L. Are Private Bedrooms Necessary for Residential Facilities for the Elderly in China?: A Study on Resi-dents’ Preferences in Shanghai. AIJ J. Technol. Des. 2017, 23, 219–222. [Google Scholar] [CrossRef] [Green Version]
- Low, L.P.L.; Lee, D.T.F.; Chan, A.W.Y. An Exploratory Study of Chinese Older People’s Perceptions of Privacy in Residential Care Homes. J. Adv. Nurs. 2007, 57, 605–613. [Google Scholar] [CrossRef]
- Lee, D.T.F. The Goal of Culturally Sensitive Gerontological Care. J. Adv. Nurs. 2004, 47, 351. [Google Scholar] [CrossRef]
- Wong, G.H.Z.; Pang, W.S.; Yap, P. A Paradigm Shift in Regulating and Running Nursing Homes in Singapore. J. Am. Med. Dir. Assoc. 2014, 15, 440–444. [Google Scholar] [CrossRef]
- Chaudhury, H. Remembering Home: Rediscovering the Self in Dementia; Johns Hopkins University Press: Baltimore, MD, USA, 2008. [Google Scholar]
- Eijkelenboom, A.; Verbeek, H.; Felix, E.; van Hoof, J. Architectural Factors Influencing the Sense of Home in Nursing Homes: An Operationalization for Practice. Front. Archit. Res. 2017, 6, 111–122. [Google Scholar] [CrossRef]
- Fleming, R.; Purandare, N. Long-Term Care for People with Dementia: Environmental Design Guidelines. Int. Psychogeriatr. 2010, 22, 1084–1096. [Google Scholar] [CrossRef] [Green Version]
- Fleming, R.; Kelly, F.; Stillfried, G. ‘I Want to Feel at Home’: Establishing What Aspects of Environmental Design Are Important to People with Dementia Nearing the End of Life. BMC Palliat. Care 2015, 14, 26. [Google Scholar] [CrossRef] [Green Version]
- Johnson, R.A.; Bibbo, J. Relocation Decisions and Constructing the Meaning of Home: A Phenomenological Study of the Transition into a Nursing Home. J. Aging Stud. 2014, 30, 56–63. [Google Scholar] [CrossRef] [Green Version]
- Weeks, L.; Chamberlain, S.; Keefe, J. What Makes a Nursing Home a Home? Insights from Family Members and Friends. Hous. Care Support 2017, 20, 152–163. [Google Scholar] [CrossRef]
- Robinson, C.A.; Colin Reid, R.; Cooke, H.A. A Home Away from Home: The Meaning of Home According to Families of Residents with Dementia. Dementia 2010, 9, 490–508. [Google Scholar] [CrossRef]
- Saarnio, L.; Boström, A.-M.; Hedman, R.; Gustavsson, P.; Öhlén, J. Enabling At-Homeness for Residents Living in a Nursing Home: Reflected Experience of Nursing Home Staff. J. Aging Stud. 2017, 43, 40–45. [Google Scholar] [CrossRef] [Green Version]
- Van Zadelhoff, E.; Verbeek, H.; Widdershoven, G.; van Rossum, E.; Abma, T. Good Care in Group Home Living for People with Dementia. Experiences of Residents, Family and Nursing Staff. J. Clin. Nurs. 2011, 20, 2490–2500. [Google Scholar] [CrossRef]
- Van Hoof, J.; Janssen, M.L.; Heesakkers, C.M.C.; van Kersbergen, W.; Severijns, L.E.J.; Willems, L.A.G.; Marston, H.R.; Janssen, B.M.; Nieboer, M.E. The Importance of Personal Possessions for the Development of a Sense of Home of Nursing Home Residents. J. Hous. Elder. 2016, 30, 35–51. [Google Scholar] [CrossRef]
- Wohlin, C. Guidelines for Snowballing in Systematic Literature Studies and a Replication in Software Engineering. In Proceedings of the 18th International Conference on Evaluation and Assessment in Software Engineering: EASE ’14, London, UK, 13–14 May 2014; Association for Computing Machinery: New York, NY, USA, 2014; pp. 1–10. [Google Scholar] [CrossRef]
- De Veer, A.J.; Kerkstra, A. Feeling at Home in Nursing Homes. J. Adv. Nurs. 2001, 35, 427–434. [Google Scholar] [CrossRef]
- Falk, H.; Wijk, H.; Persson, L.-O.; Falk, K. A Sense of Home in Residential Care. Scand. J. Caring Sci. 2013, 27, 999–1009. [Google Scholar] [CrossRef]
- Klaassens, M.; Meijering, L. Experiences of Home and Institution in a Secured Nursing Home Ward in The Netherlands: A Participatory Intervention Study. J. Aging Stud. 2015, 34, 92–102. [Google Scholar] [CrossRef] [Green Version]
- Board, M.; McCormack, B. Exploring the Meaning of Home and Its Implications for the Care of Older People. J. Clin. Nurs. 2018, 27, 3070–3080. [Google Scholar] [CrossRef] [PubMed]
- Persson, T.; Wästerfors, D. “Such Trivial Matters:” How Staff Account for Restrictions of Residents’ Influence in Nursing Homes. J. Aging Stud. 2009, 23, 1–11. [Google Scholar] [CrossRef]
- Van Dijck-Heinen, C.J.M.L.; Wouters, E.J.M.; Janssen, B.M.; van Hoof, J. A Sense of Home through the Eyes of Nursing Home Residents. Int. J. Innov. Res. Sci. Technol. 2014, 1, 57–69. [Google Scholar]
- Bland, M. The Challenge of Feeling “at Home” in Residential Aged Care in New Zealand. Nurs. Prax. N. Z. Inc 2005, 21, 4–12. [Google Scholar]
- Smith, S.G. The Essential Qualities of a Home. J. Environ. Psychol. 1994, 14, 31–46. [Google Scholar] [CrossRef]
- Carboni, J.T. Homelessness among the Institutionalized Elderly. J. Gerontol. Nurs. 1990, 16, 32–37. [Google Scholar] [CrossRef]
- Lewinson, T. Co-Constructing Home with Photovoice: Older Residents of an Assisted Living Facility Build a Photonarrative. Qual. Soc. Work 2015, 14, 702–720. [Google Scholar] [CrossRef]
- Molony, S.L.; Evans, L.K.; Jeon, S.; Rabig, J.; Straka, L.A. Trajectories of At-Homeness and Health in Usual Care and Small House Nursing Homes. Gerontologist 2011, 51, 504–515. [Google Scholar] [CrossRef] [Green Version]
- Owens, A.; Randhawa, G. “It’s Different from My Culture; They’re Very Different”: Providing Community-Based, “culturally Competent” Palliative Care for South Asian People in the UK. Health Soc. Care Community 2004, 12, 414–421. [Google Scholar] [CrossRef]
- Clegg, A. Older South Asian Patient and Carer Perceptions of Culturally Sensitive Care in a Community Hospital Setting. J. Clin. Nurs. 2003, 12, 283–290. [Google Scholar] [CrossRef]
- Chua, B.-H. Communitarian Ideology and Democracy in Singapore; Routledge: London, UK, 1997. [Google Scholar] [CrossRef]
- Tan, C. “Our Shared Values” in Singapore: A Confucian Perspective. Educ. Theory 2012, 62, 449–463. [Google Scholar] [CrossRef]
- Mahbubani, K.; Yee, T.; Khanna, V.; Tan, E.K.B. Pragmatism Should Be Retained As Singapore’s Governing Philosophy. In Singapore Perspectives 2015; Singapore Perspectives; National University of Singapore: Singapore, 2015; pp. 93–120. [Google Scholar] [CrossRef]
- Wong, A.K.; Yeh, S.H.K. Housing a Nation: 25 Years of Public Housing in Singapore; Maruzen Asia for Housing and Development Board: Singapore, 1985.
- World Population Ageing 2017. Available online: https://www.un.org/en/development/desa/population/theme/ageing/WPA2017.asp (accessed on 9 March 2022).
- Mamun, K.; Lim, J. Role of Nasogastric Tube in Preventing Aspiration Pneumonia in Patients with Dysphagia. Singap. Med. J. 2005, 46, 627–631. [Google Scholar]
- Yap, L.K.P.; Au, S.Y.L.; Ang, Y.H.; Kwan, K.Y.; Ng, S.C.; Ee, C.H. Who Are the Residents of a Nursing Home in Singapore? Singap. Med. J. 2003, 44, 65–73. [Google Scholar]
- Tew, C.W.; Ong, S.P.; Yap, L.K.P.; Lim, A.Y.C.; Luo, N.; Koh, G.C.H.; Ng, T.P.; Wee, S.L. Quality of Life, Person-Centred Care and Lived Experiences of Nursing Home Residents in a Developed Urban Asian Country: A Cross-Sectional Study. J. Nurs. Home Res. Sci. 2021, 7, 1–8. [Google Scholar] [CrossRef]
- Christensen, R.D. Transinstitutionalization: A Case Study of Two Residential Care Facilities in Rural Midwest North America. Ph.D. Thesis, University of Missouri, Columbia, MO, USA, 2015. [Google Scholar] [CrossRef]
- Lincoln, Y.S.; Guba, E.G. Naturalistic Inquiry; SAGE: Thousand Oaks, CA, USA, 1985. [Google Scholar]
- Geertz, C. Thick Description: Toward an Interpretive Theory of Culture. In The Interpretations of Cultures; Basic Books: New York, NY, USA, 1973; pp. 3–30. [Google Scholar]
- Braun, V.; Clarke, V. Using Thematic Analysis in Psychology. Qual. Res. Psychol. 2006, 3, 77–101. [Google Scholar] [CrossRef] [Green Version]
- Raghunath, N. Technological Adoption as a Social Process in Food Centres in Singapore. Sci. Technol. Soc. 2021, 26, 375–391. [Google Scholar] [CrossRef]
- Starfield, B. Is Patient-Centered Care the Same As Person-Focused Care? Perm. J. 2011, 15, 63–69. [Google Scholar] [CrossRef]
- Schwarz, B.; Chaudhury, H.; Tofle, R.B. Effect of Design Interventions on a Dementia Care Setting. Am. J. Alzheimers Dis. Dement. 2004, 19, 172–176. [Google Scholar] [CrossRef]
- Morgan, D.G.; Stewart, N.J. Multiple Occupancy Versus Private Rooms on Dementia Care Units. Environ. Behav. 1998, 30, 487–503. [Google Scholar] [CrossRef]
- Zeisel, J.; Silverstein, N.M.; Hyde, J.; Levkoff, S.; Lawton, M.P.; Holmes, W. Environmental Correlates to Behavioral Health Outcomes in Alzheimer’s Special Care Units. Gerontologist 2003, 43, 697–711. [Google Scholar] [CrossRef] [Green Version]
- McParland, J.; Scott, P.A.; Arndt, M.; Dassen, T.; Gasull, M.; Lemonidou, C.; Valimaki, M.; Leino-Kilpi, H. Autonomy and Clinical Practice. 2: Patient Privacy and Nursing Practice. Br. J. Nurs. Mark Allen Publ. 2000, 9, 566–569. [Google Scholar] [CrossRef]
- Davies, S.; Brown, J.; Wilson, F.; Nolan, M. Dignity on the Ward: Promoting Excellence in Care. Nurs. Times 2000, 96, 37–39. [Google Scholar]
- Laurence, G.A.; Fried, Y.; Slowik, L.H. “My Space”: A Moderated Mediation Model of the Effect of Architectural and Experienced Privacy and Workspace Personalization on Emotional Exhaustion at Work. J. Environ. Psychol. 2013, 36, 144–152. [Google Scholar] [CrossRef]
- Baig, M.M.; Afifi, S.; GholamHosseini, H.; Mirza, F. A Systematic Review of Wearable Sensors and IoT-Based Monitoring Applications for Older Adults—A Focus on Ageing Population and Independent Living. J. Med. Syst. 2019, 43, 233. [Google Scholar] [CrossRef] [PubMed]
- Daniel, K.M.; Cason, C.L.; Ferrell, S. Emerging Technologies to Enhance the Safety of Older People in Their Homes. Geriatr. Nur. 2009, 30, 384–389. [Google Scholar] [CrossRef] [PubMed]
- Siegel, C.; Hochgatterer, A.; Dorner, T.E. Contributions of Ambient Assisted Living for Health and Quality of Life in the Elderly and Care Services—A Qualitative Analysis from the Experts’ Perspective of Care Service Professionals. BMC Geriatr. 2014, 14, 112. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Lee, H.-T.S.; Cheng, S.-C.; Dai, Y.-T.; Chang, M.; Hu, W.-Y. Cultural Perspectives of Older Nursing Home Residents Regarding Signing Their Own DNR Directives in Eastern Taiwan: A Qualitative Pilot Study. BMC Palliat. Care 2016, 15, 45. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Tsai, H.-H.; Tsai, Y.-F. Family Members’ Perceived Meaning of Visiting Nursing Home Residents in Taiwan. J. Adv. Nurs. 2012, 68, 302–311. [Google Scholar] [CrossRef]
- Robinson, S. Nested Bodies. In Mind in Architecture: Neuroscience, Embodiment, and the Future of Design; Robinson, S., Pallasmaa, J., Eds.; The MIT Press: Cambridge, MA, USA, 2015. [Google Scholar]
- Chaudhury, H.; Oswald, F. Advancing Understanding of Person-Environment Interaction in Later Life: One Step Further. J. Aging Stud. 2019, 51, 100821. [Google Scholar] [CrossRef]
- Porteous, J.D. Environment and Behavior: Planning and Everyday Urban Life; Addison-Wesley: Reading, MA, USA, 1977. [Google Scholar]
- Sedgwick, P.; Greenwood, N. Understanding the Hawthorne Effect. BMJ 2015, 351, h4672. [Google Scholar] [CrossRef] [Green Version]
- Monahan, T.; Fisher, J.A. Benefits of ‘Observer Effects’: Lessons from the Field. Qual. Res. 2010, 10, 357–376. [Google Scholar] [CrossRef] [Green Version]












| Themes | Recommendations | Key References |
|---|---|---|
| Private spaces | Private rooms allow residents an opportunity to withdraw and be on their own and to create their own environment by having control over space. | Van Hoof et al. [2], Hauge and Heggen [4], Nakrem et al. [5], Eijkelenboom et al. [11], de Veer and Kerkstra [21], van Hoof et al. [19], Falk et al. [22] |
| Private rooms allow residents to be able to receive visitors. | Van Hoof et al. [2] | |
| Access to a private bathroom offers residents a sense of control and privacy during personal care activities. | Fleming et al. [13], van Hoof et al. [19], Klaassens and Meijering [23] | |
| Furniture in private spaces, meant to accommodate residents’ visitors. | Eijkelenboom et al. [11] | |
| Personal belongings | Residents’ personal belongings such as cherished items and furniture create a semblance of familiarity. | Fleming et al. [13], van Hoof et al. [19], Board and McCormack [24] |
| Sufficient space to store and display personal items. | Van Hoof et al. [2] | |
| Storage space for personal items. | Eijkelenboom et al. [11] | |
| Ambience | Evoke a sense of warmth and coziness through strategies such as having access to daylight, with homelike furniture, decorations and homelike smells. | Van Hoof et al. [2], Eijkelenboom et al. [11], Fleming and Purandare [12], Board and McCormack [24] |
| Reserved spaces in communal spaces, such as having their own spot at the dining table, or a private chair in a preferred spot. | Van Hoof et al. [2], Eijkelenboom et al. [11], van Hoof et al. [19] | |
| Accommodate lower-density spaces within the larger units | Van Hoof et al. [2], Eijkelenboom et al. [11] | |
| Location in a familiar neighborhood or hometown. | Eijkelenboom et al. [11], Board and McCormack [24] | |
| Appropriate levels of stimulation | Provide activities that promote pleasure and appropriate levels of stimulation, according to the resident’s needs and abilities. | Van Hoof et al. [2], Fleming et al. [13], Fleming and Purandare [12] |
| Provide a variety of spaces to suit different functions and preferences (e.g., having quiet spaces to retreat to when someone else is watching TV). | Fleming and Purandare [12] | |
| Connection with nature | Physical and visual access to outdoor and green spaces with fresh air and sun enables connection to the outside world. | Van Hoof et al. [2], Nakrem et al. [5], van Hoof et al. [19] |
| Animal life (e.g., birds or fish) provides a welcomed distraction for residents. | Van Hoof et al. [2], van Hoof et al. [19] | |
| Social interactions | Supporting engagement in everyday homelike activities invites residents and their families to be involved in everyday life. | Robinson et al. [16], van Zadelhoff et al. [18] |
| Comfortable spaces conducive to engagement and interaction with other residents, family and visitors. | Van Hoof et al. [2], Falk et al. [22] |
| NH1 | NH2 | NH3 | NH4 | NH5 | |
|---|---|---|---|---|---|
| Site area (sqm)/Number of stories | 4830/ 11 stories | 2800/ 12 stories | 3000/ 9 stories | 2991/ 6 stories | 9056/ 3 buildings: (1), (2) and (3), each 3 stories high |
| Bedroom type | 4 beds | 9 beds and 4 beds | 8 beds | 6 beds | (1) 8 beds (2) 5 beds (3) 2 beds |
| Typical bedroom size (sqm) | 36 | 85 | 64 | 90 | (1) 54 (2) 50 (3) 20 |
| Beds occupied/ Total capacity | 343/392 | 560/600 | 203/225 | 218/230 | 190/190 |
| Types of residents * | Cat I: 0 Cat II: 27 Cat III: 198 Cat IV: 118 | Cat I: 0 Cat II: 14 Cat III: 318 Cat IV: 228 | Cat I: 0 Cat II: 5 Cat III: 103 Cat IV: 95 | Cat I: 1 Cat II: 6 Cat III: 83 Cat IV: 128 | Cat I: 0 Cat II: 0 Cat III: 128 Cat IV: 162 |
| Ethnicity of residents | Chinese: 87.1% Malay: 8.9% Indian: 4% Others: 0% | Chinese:96% Malay: 0% Indian: 4% Others: 0% | Chinese: 61.3% Malay: 24.7% Indian: 12.9% Others: 1.1% | Chinese: 88% Malay: 4% Indian: 8% Others: 0% | Chinese: 60% Malay: 10% Indian: 24% Others: 6% |
| Unit type | Household: 4 rooms × 4 beds | Ward-wing: 4 rooms × 8 beds (plus 1 room × 4 beds (haze room)) | Ward-floor: 6 rooms × 8 beds | Ward-floor: 9 rooms × 6 beds | Ward-floor cluster: (1) 8 rooms × 8 beds (2) 6 rooms × 5 beds (3) 8 rooms × 2 beds |
| Residents per unit | 16 | 36 | 48 | 54 | (1) 64 (2) 30 (3) 16 |
| Staff per unit | 5 (plus 1 shared staff member between units) | 15 to 17 | 10 | 18 to 20 | 60 |
| NH1 | NH2 | NH3 | NH4 | NH5 | |||||||
|---|---|---|---|---|---|---|---|---|---|---|---|
| Total Residents Recruited | 101 | 29.5% | 99 | 17.7% | 95 | 46.8% | 100 | 45.9% | 100 | 52.6% | |
| Participant’s age group | <40 | 0 | 0% | 0 | 0% | 1 | 1.1% | 0 | 0% | 0 | 0% |
| 40–50 | 3 | 3% | 1 | 1% | 3 | 3.2% | 1 | 1% | 3 | 3% | |
| 51–60 | 7 | 6.9% | 2 | % | 12 | 12.6% | 2 | 2% | 13 | 13% | |
| 61–70 | 17 | 16.8% | 22 | 22.2% | 18 | 19% | 17 | 17% | 18 | 18% | |
| 71–80 | 31 | 32.7% | 26 | 42.4% | 29 | 28.4% | 33 | 31% | 27 | 32% | |
| 81–90 | 33 | 32.7% | 42 | 42.4% | 27 | 28.4% | 31 | 31% | 32 | 32% | |
| 91–100 | 9 | 8.9% | 6 | 6.1% | 5 | 5.3% | 12 | 12% | 7 | 7% | |
| >100 | 1 | 1% | 0 | 0% | 0 | 0% | 2 | 2% | 0 | 0% | |
| Unknown | 0 | 0% | 0 | 0% | 0 | 0% | 2 | 2% | 0 | 0% | |
| Participant’s length of stay(years) | 0 | 19 | 18.8% | 35 | 35.4% | 65 | 68.4% | 20 | 20% | 40 | 40% |
| 1–3 | 50 | 49.5% | 37 | 37.4% | 29 | 30.5% | 37 | 37% | 27 | 27% | |
| 4–6 | 23 | 22.8% | 18 | 18.2% | 0 | 0% | 18 | 18% | 15 | 15% | |
| 7–10 | 5 | 5% | 8 | 8.1% | 0 | 0% | 11 | 11% | 9 | 9% | |
| >10 | 4 | 4% | 1 | 1% | 0 | 0% | 11 | 11% | 9 | 9% | |
| No data | 0 | 0% | 0 | 0% | 1 | 1.1% | 3 | 3% | 0 | 0% | |
| Participant’s RAF category | Cat II | 7 | 6.9% | 2 | 2% | 5 | 5.3% | 0 | 0% | 0 | 0% |
| Cat III | 62 | 61.4% | 80 | 80.8% | 66 | 69.5% | 41 | 41% | 29 | 29% | |
| Cat IV | 32 | 31.7% | 14 | 14.1% | 24 | 25.3% | 59 | 59% | 71 | 71% | |
| Participants ethnicity | Chinese | 88 | 87.1% | 95 | 96% | 59 | 62.1% | 88 | 88% | 60 | 60% |
| Malay | 9 | 8.9% | 0 | 0% | 23 | 24.2% | 4 | 4% | 24 | 24% | |
| Indian | 4 | 4% | 4 | 4% | 12 | 12.6% | 8 | 8% | 10 | 10% | |
| Others | 0 | 0% | 0 | 0% | 1 | 1.1% | 0 | 0% | 6 | 6% | |
| Participants gender | Male | 61 | 60.4% | 44 | 44.4% | 53 | 55.8% | 48 | 48% | 54 | 54% |
| Female | 40 | 39.6% | 55 | 55.6% | 42 | 44.2% | 52 | 52% | 46 | 46% | |
| Diagnosed with dementia | Yes | 42 | 41.6% | 61 | 61.6% | 28 | 29.5% | 56 | 56% | 59 | 59% |
| No | 59 | 58.4% | 38 | 38.4% | 67 | 70.5% | 44 | 44% | 41 | 41% | |
| Ability to communicate | Yes | 93 | 92.1% | 95 | 96% | 93 | 97.9% | 86 | 86% | 100 | 100% |
| No | 8 | 7.9% | 4 | 4% | 2 | 2.1% | 14 | 14% | 0 | 0% | |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Lee, J.-J.; Ng, T.P.; Nasution, I.K.; Eng, J.Y.; Christensen, R.D.; Fung, J.C. Implementation of a Sense of Home in High-Density Multicultural Singapore Nursing Homes: Challenges and Opportunities. Int. J. Environ. Res. Public Health 2022, 19, 6557. https://doi.org/10.3390/ijerph19116557
Lee J-J, Ng TP, Nasution IK, Eng JY, Christensen RD, Fung JC. Implementation of a Sense of Home in High-Density Multicultural Singapore Nursing Homes: Challenges and Opportunities. International Journal of Environmental Research and Public Health. 2022; 19(11):6557. https://doi.org/10.3390/ijerph19116557
Chicago/Turabian StyleLee, Jung-Joo, Tse Pei Ng, Ivan Kurniawan Nasution, Jia Yen Eng, Renee Desneige Christensen, and John Chye Fung. 2022. "Implementation of a Sense of Home in High-Density Multicultural Singapore Nursing Homes: Challenges and Opportunities" International Journal of Environmental Research and Public Health 19, no. 11: 6557. https://doi.org/10.3390/ijerph19116557
APA StyleLee, J.-J., Ng, T. P., Nasution, I. K., Eng, J. Y., Christensen, R. D., & Fung, J. C. (2022). Implementation of a Sense of Home in High-Density Multicultural Singapore Nursing Homes: Challenges and Opportunities. International Journal of Environmental Research and Public Health, 19(11), 6557. https://doi.org/10.3390/ijerph19116557






