A Longitudinal Study on the Addictive Behaviors of General Population before and during the COVID-19 Pandemic in China
Abstract
:1. Introduction
2. Materials and Methods
2.1. Data
2.2. Variables
2.3. Statistical Analyses
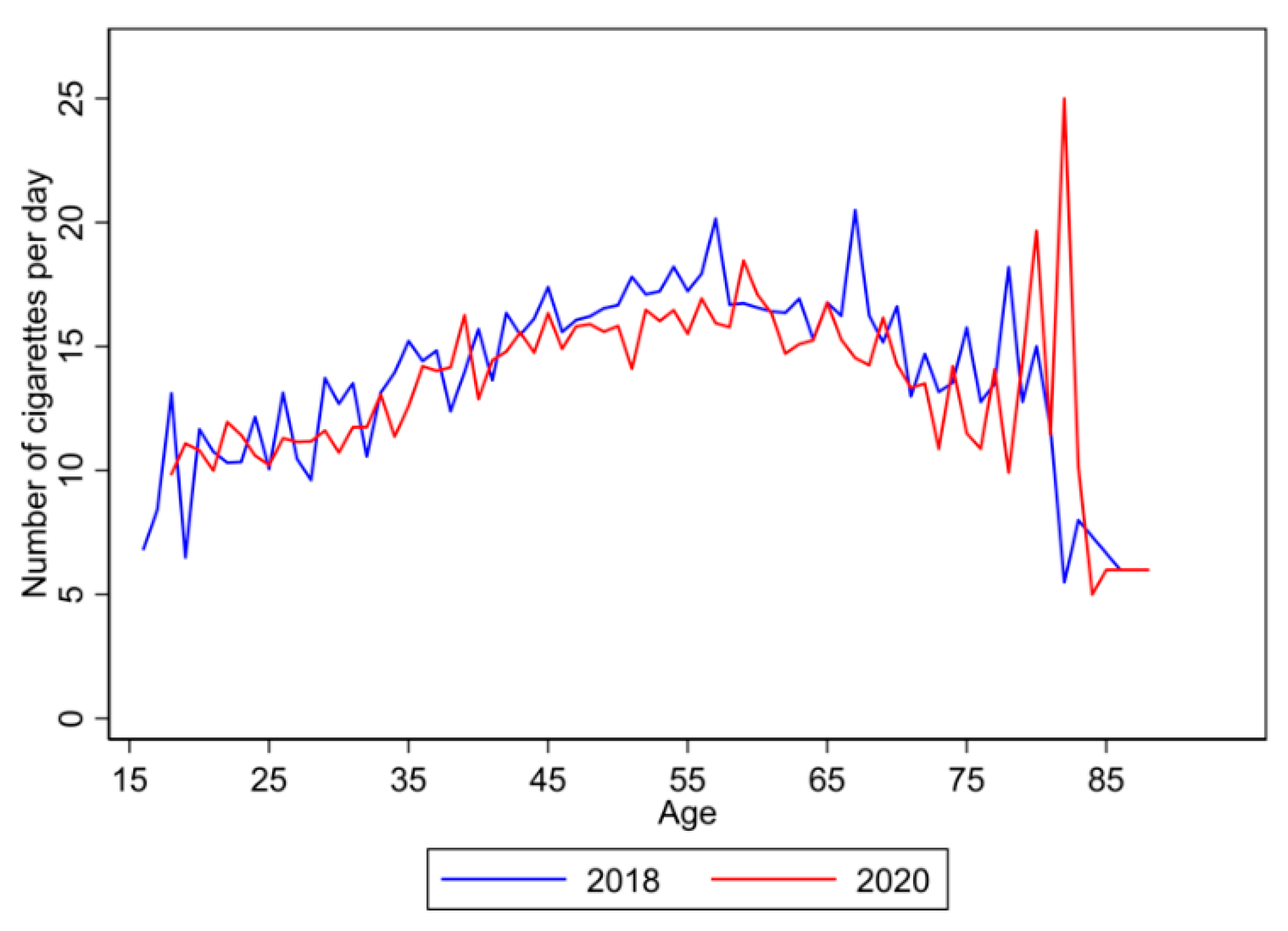
3. Results
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Clay, J.M.; Parker, M.O. Alcohol Use and Misuse during the COVID-19 Pandemic: A Potential Public Health Crisis? Lancet Public Health 2020, 5, e259. [Google Scholar] [CrossRef]
- Rogés, J.; Bosque-Prous, M.; Colom, J.; Folch, C.; Barón-Garcia, T.; González-Casals, H.; Fernández, E.; Espelt, A. Consumption of Alcohol, Cannabis, and Tobacco in a Cohort of Adolescents before and during COVID-19 Confinement. Int. J. Environ. Res. Public Health 2021, 18, 7849. [Google Scholar] [CrossRef] [PubMed]
- Theron, M.; Swart, R.; Londani, M.; Parry, C.; Petersen Williams, P.; Harker, N. Did COVID-19-Related Alcohol Sales Restrictions Reduce Alcohol Consumption? Findings from a National Online Survey in South Africa. Int. J. Environ. Res. Public Health 2022, 19, 2422. [Google Scholar] [CrossRef] [PubMed]
- Nesoff, E.D.; Gutkind, S.; Sirota, S.; McKowen, A.L.; Veldhuis, C.B. Mental Health and Economic Stressors Associated with High-Risk Drinking and Increased Alcohol Consumption Early in the COVID-19 Pandemic in the United States. Prev. Med. 2021, 153, 106854. [Google Scholar] [CrossRef]
- Yingst, J.M.; Krebs, N.M.; Bordner, C.R.; Hobkirk, A.L.; Allen, S.I.; Foulds, J. Tobacco Use Changes and Perceived Health Risks among Current Tobacco Users during the COVID-19 Pandemic. Int. J. Environ. Res. Public Health 2021, 18, 1795. [Google Scholar] [CrossRef]
- Driezen, P.; Kasza, K.A.; Gravely, S.; Thompson, M.E.; Fong, G.T.; Michael Cummings, K.; Hyland, A. Was COVID-19 Associated with Increased Cigarette Purchasing, Consumption, and Smoking at Home among US Smokers in Early 2020? Findings from the US Arm of the International Tobacco Control (ITC) Four Country Smoking and Vaping Survey. Addict. Behav. 2022, 129, 107276. [Google Scholar] [CrossRef]
- Brown, C.R.H. The Relationship between COVID-19-Specific Health Risk Beliefs and the Motivation to Quit Smoking: A UK-Based Survey. Drug Alcohol Depend. 2021, 227, 108981. [Google Scholar] [CrossRef]
- Denlinger-Apte, R.; Suerken, C.K.; Cornacchione Ross, J.; Reboussin, B.A.; Spangler, J.; Wagoner, K.G.; Sutfin, E.L. Decreases in Smoking and Vaping during COVID-19 Stay-at-Home Orders among a Cohort of Young Adults in the United States. Prev. Med. 2022, 156, 106992. [Google Scholar] [CrossRef]
- O’Donnell, R.; Eadie, D.; Stead, M.; Dobson, R.; Semple, S. ‘I Was Smoking a Lot More during Lockdown Because I Can’: A Qualitative Study of How UK Smokers Responded to the COVID-19 Lockdown. Int. J. Environ. Res. Public Health 2021, 18, 5816. [Google Scholar] [CrossRef]
- Gonzalez, M.; Epperson, A.E.; Halpern-Felsher, B.; Halliday, D.M.; Song, A.V. Smokers Are More Likely to Smoke More after the COVID-19 California Lockdown Order. Int. J. Environ. Res. Public Health 2021, 18, 2582. [Google Scholar] [CrossRef]
- Chen-Sankey, J.C.; Broun, A.; Duarte, D.A.; Ajith, A.; Jewett, B.; Smiley, S.L.; Mead-Morse, E.L.; Guy, M.C.; Choi, K. Exploring Changes in Cigar Smoking Patterns and Motivations to Quit Cigars among Black Young Adults in the Time of COVID-19. Addict. Behav. Rep. 2020, 12, 100317. [Google Scholar] [CrossRef]
- Vogel, E.A.; Henriksen, L.; Schleicher, N.C.; Prochaska, J.J. Perceived Susceptibility to and Seriousness of COVID-19: Associations of Risk Perceptions with Changes in Smoking Behavior. Int. J. Environ. Res. Public Health 2021, 18, 7621. [Google Scholar] [CrossRef] [PubMed]
- Fatollahi, J.J.; Bentley, S.; Doran, N.; Brody, A.L. Changes in Tobacco Use Patterns among Veterans in San Diego during the Recent Peak of the COVID-19 Pandemic. Int. J. Environ. Res. Public Health 2021, 18, 11923. [Google Scholar] [CrossRef] [PubMed]
- Kalkhoran, S.M.; Levy, D.E.; Rigotti, N.A. Smoking and E-Cigarette Use among U.S. Adults during the COVID-19 Pandemic. Am. J. Prev. Med. 2022, 62, 341–349. [Google Scholar] [CrossRef] [PubMed]
- Kale, D.; Perski, O.; Herbec, A.; Beard, E.; Shahab, L. Changes in Cigarette Smoking and Vaping in Response to the COVID-19 Pandemic in the UK: Findings from Baseline and 12-Month Follow up of HEBECO Study. Int. J. Environ. Res. Public Health 2022, 19, 630. [Google Scholar] [CrossRef] [PubMed]
- Mistry, S.K.; Ali, A.M.; Rahman, M.A.; Yadav, U.N.; Gupta, B.; Rahman, M.A.; Huque, R. Changes in Tobacco Use Patterns during COVID-19 and Their Correlates among Older Adults in Bangladesh. Int. J. Environ. Res. Public Health 2021, 18, 1779. [Google Scholar] [CrossRef] [PubMed]
- Tucker, J.S.; Rodriguez, A.; Green, H.D., Jr.; Pollard, M.S. Trajectories of Alcohol Use and Problems during the COVID-19 Pandemic: The Role of Social Stressors and Drinking Motives for Men and Women. Drug Alcohol Depend. 2022, 232, 109285. [Google Scholar] [CrossRef] [PubMed]
- Grossman, E.R.; Benjamin-Neelon, S.E.; Sonnenschein, S. Alcohol Consumption during the COVID-19 Pandemic: A Cross-Sectional Survey of US Adults. Int. J. Environ. Res. Public Health 2020, 17, 9189. [Google Scholar] [CrossRef]
- Alpers, S.E.; Skogen, J.C.; Mæland, S.; Pallesen, S.; Rabben, Å.K.; Lunde, L.-H.; Fadnes, L.T. Alcohol Consumption during a Pandemic Lockdown Period and Change in Alcohol Consumption Related to Worries and Pandemic Measures. Int. J. Environ. Res. Public Health 2021, 18, 1220. [Google Scholar] [CrossRef]
- Killgore, W.D.S.; Cloonan, S.A.; Taylor, E.C.; Lucas, D.A.; Dailey, N.S. Alcohol Dependence during COVID-19 Lockdowns. Psychiatry Res. 2021, 296, 113676. [Google Scholar] [CrossRef]
- Rossow, I.; Bye, E.K.; Moan, I.S.; Kilian, C.; Bramness, J.G. Changes in Alcohol Consumption during the COVID-19 Pandemic—Small Change in Total Consumption, but Increase in Proportion of Heavy Drinkers. Int. J. Environ. Res. Public Health 2021, 18, 4231. [Google Scholar] [CrossRef] [PubMed]
- Villanueva-Blasco, V.J.; Villanueva Silvestre, V.; Vázquez-Martínez, A.; Rial Boubeta, A.; Isorna, M. Age and Living Situation as Key Factors in Understanding Changes in Alcohol Use during COVID-19 Confinement. Int. J. Environ. Res. Public Health 2021, 18, 11471. [Google Scholar] [CrossRef] [PubMed]
- Villanueva-Blasco, V.J.; Villanueva Silvestre, V.; Isorna, M.; Motos, P.; Blay, P.; Vázquez-Martínez, A. Changes in Alcohol Consumption Pattern Based on Gender during COVID-19 Confinement in Spain. Int. J. Environ. Res. Public Health 2021, 18, 8028. [Google Scholar] [CrossRef] [PubMed]
- Lee, S.Y.; Kim, S.; Kim, W.-H.; Heo, J. Employment, Economic, and Sociodemographic Factors Associated with Changes in Smoking and Drinking Behaviors during the COVID-19 Pandemic in South Korea. Int. J. Environ. Res. Public Health 2022, 19, 2802. [Google Scholar] [CrossRef]
- Van Hooijdonk, K.J.M.; Rubio, M.; Simons, S.S.H.; van Noorden, T.H.J.; Luijten, M.; Geurts, S.A.E.; Vink, J.M. Student-, Study- and COVID-19-Related Predictors of Students’ Smoking, Binge Drinking and Cannabis Use before and during the Initial COVID-19 Lockdown in The Netherlands. Int. J. Environ. Res. Public Health 2022, 19, 812. [Google Scholar] [CrossRef]
- Kosendiak, A.; Król, M.; Ściskalska, M.; Kepinska, M. The Changes in Stress Coping, Alcohol Use, Cigarette Smoking and Physical Activity during COVID-19 Related Lockdown in Medical Students in Poland. Int. J. Environ. Res. Public Health 2022, 19, 302. [Google Scholar] [CrossRef]
- Gavurova, B.; Ivankova, V.; Rigelsky, M. Alcohol Use Disorders among Slovak and Czech University Students: A Closer Look at Tobacco Use, Cannabis Use and Socio-Demographic Characteristics. Int. J. Environ. Res. Public Health 2021, 18, 11565. [Google Scholar] [CrossRef]
- Bonar, E.E.; Parks, M.J.; Gunlicks-Stoessel, M.; Lyden, G.R.; Mehus, C.J.; Morrell, N.; Patrick, M.E. Binge Drinking before and after a COVID-19 Campus Closure among First-Year College Students. Addict. Behav. 2021, 118, 106879. [Google Scholar] [CrossRef]
- Jaffe, A.E.; Kumar, S.A.; Hultgren, B.A.; Smith-LeCavalier, K.N.; Garcia, T.A.; Canning, J.R.; Larimer, M.E. Meaning in Life and Stress-Related Drinking: A Multicohort Study of College Students during the COVID-19 Pandemic. Addict. Behav. 2022, 129, 107281. [Google Scholar] [CrossRef]
- Sokolovsky, A.W.; Hertel, A.W.; Micalizzi, L.; White, H.R.; Hayes, K.L.; Jackson, K.M. Preliminary Impact of the COVID-19 Pandemic on Smoking and Vaping in College Students. Addict. Behav. 2021, 115, 106783. [Google Scholar] [CrossRef]
- Vasconcelos, M.; Crego, A.; Rodrigues, R.; Almeida-Antunes, N.; López-Caneda, E. Effects of the COVID-19 Mitigation Measures on Alcohol Consumption and Binge Drinking in College Students: A Longitudinal Survey. Int. J. Environ. Res. Public Health 2021, 18, 9822. [Google Scholar] [CrossRef] [PubMed]
- Tavolacci, M.P.; Wouters, E.; Van de Velde, S.; Buffel, V.; Déchelotte, P.; Van Hal, G.; Ladner, J. The Impact of COVID-19 Lockdown on Health Behaviors among Students of a French University. Int. J. Environ. Res. Public Health 2021, 18, 4346. [Google Scholar] [CrossRef] [PubMed]
- Jackson, S.E.; Garnett, C.; Shahab, L.; Oldham, M.; Brown, J. Association of the COVID-19 Lockdown with Smoking, Drinking and Attempts to Quit in England: An Analysis of 2019–20 Data. Addiction 2021, 116, 1233–1244. [Google Scholar] [CrossRef] [PubMed]
- Garnett, C.; Jackson, S.; Oldham, M.; Brown, J.; Steptoe, A.; Fancourt, D. Factors Associated with Drinking Behaviour during COVID-19 Social Distancing and Lockdown among Adults in the UK. Drug Alcohol Depend. 2021, 219, 108461. [Google Scholar] [CrossRef] [PubMed]
- Tobaiqy, M.; MacLure, A.; Thomas, D.; MacLure, K. The Impact of COVID-19 on Smoking Behaviours and Support for Smoke-Free Zones in Saudi Arabia. Int. J. Environ. Res. Public Health 2021, 18, 6927. [Google Scholar] [CrossRef] [PubMed]
- Loud, E.E.; Gallegos-Carrillo, K.; Barrientos-Gutiérrez, I.; Arillo-Santillán, E.; Lambert, V.C.; Zavala-Arciniega, L.; Thrasher, J.F. Smoking Behaviors, Mental Health, and Risk Perceptions during the Beginning of the COVID-19 Pandemic among Mexican Adult Smokers. Int. J. Environ. Res. Public Health 2021, 18, 10905. [Google Scholar] [CrossRef]
- Rossow, I.; Bartak, M.; Bloomfield, K.; Braddick, F.; Bye, E.K.; Kilian, C.; López-Pelayo, H.; Mäkelä, P.; Moan, I.S.; Moskalewicz, J.; et al. Changes in Alcohol Consumption during the COVID-19 Pandemic Are Dependent on Initial Consumption Level: Findings from Eight European Countries. Int. J. Environ. Res. Public Health 2021, 18, 10547. [Google Scholar] [CrossRef]
- Valente, J.Y.; Sohi, I.; Garcia-Cerde, R.; Monteiro, M.G.; Sanchez, Z.M. What is Associated with the Increased Frequency of Heavy Episodic Drinking during the COVID-19 Pandemic? Data from the PAHO Regional Web-Based Survey. Drug Alcohol Depend. 2021, 221, 108621. [Google Scholar] [CrossRef]
- Wang, C.; Pan, R.; Wan, X.; Tan, Y.; Xu, L.; McIntyre, R.S.; Choo, F.N.; Tran, B.; Ho, R.; Sharma, V.K.; et al. A Longitudinal Study on the Mental Health of General Population during the COVID-19 Epidemic in China. Brain Behav. Immun. 2020, 87, 40–48. [Google Scholar] [CrossRef]
- Li, Y.; Luan, S.; Li, Y.; Hertwig, R. Changing Emotions in the COVID-19 Pandemic: A Four-Wave Longitudinal Study in the United States and China. Soc. Sci. Med. 2021, 285, 114222. [Google Scholar] [CrossRef]
- Li, Y.; Zhao, J.; Ma, Z.; McReynolds, L.S.; Lin, D.; Chen, Z.; Wang, T.; Wang, D.; Zhang, Y.; Zhang, J.; et al. Mental Health among College Students during the COVID-19 Pandemic in China: A 2-Wave Longitudinal Survey. J. Affect. Disord. 2021, 281, 597–604. [Google Scholar] [CrossRef] [PubMed]
- Zhang, Y.; Zhang, H.; Ma, X.; Di, Q. Mental Health Problems during the COVID-19 Pandemics and the Mitigation Effects of Exercise: A Longitudinal Study of College Students in China. Int. J. Environ. Res. Public Health 2020, 17, 3722. [Google Scholar] [CrossRef] [PubMed]
- Li, H.Y.; Cao, H.; Leung, D.Y.P.; Mak, Y.W. The Psychological Impacts of a COVID-19 Outbreak on College Students in China: A Longitudinal Study. Int. J. Environ. Res. Public Health 2020, 17, 3933. [Google Scholar] [CrossRef] [PubMed]
- Yang, H.; Ma, J. How the COVID-19 Pandemic Impacts Tobacco Addiction: Changes in Smoking Behavior and Associations with Well-Being. Addict. Behav. 2021, 119, 106917. [Google Scholar] [CrossRef] [PubMed]
- Jodczyk, A.M.; Kasiak, P.S.; Adamczyk, N.; Gębarowska, J.; Sikora, Z.; Gruba, G.; Mamcarz, A.; Śliż, D. PaLS Study: Tobacco, Alcohol and Drugs Usage among Polish University Students in the Context of Stress Caused by the COVID-19 Pandemic. Int. J. Environ. Res. Public Health 2022, 19, 1261. [Google Scholar] [CrossRef]
- Zhang, X.; Oluyomi, A.; Woodard, L.; Raza, S.A.; Adel Fahmideh, M.; El-Mubasher, O.; Byun, J.; Han, Y.; Amos, C.I.; Badr, H. Individual-Level Determinants of Lifestyle Behavioral Changes during COVID-19 Lockdown in the United States: Results of an Online Survey. Int. J. Environ. Res. Public Health 2021, 18, 4364. [Google Scholar] [CrossRef]
- Ettman, C.K.; Abdalla, S.M.; Cohen, G.H.; Sampson, L.; Vivier, P.M.; Galea, S. Prevalence of Depression Symptoms in US Adults Before and During the COVID-19 Pandemic. JAMA Netw. Open 2020, 3, e2019686. [Google Scholar] [CrossRef]
- Naser, A.Y.; Dahmash, E.Z.; Al-Rousan, R.; Alwafi, H.; Alrawashdeh, H.M.; Ghoul, I.; Abidine, A.; Bokhary, M.A.; Al-Hadithi, H.T.; Ali, D.; et al. Mental Health Status of the General Population, Healthcare Professionals, and University Students during 2019 Coronavirus Disease Outbreak in Jordan: A Cross-Sectional Study. Brain Behav. 2020, 10, e01730. [Google Scholar] [CrossRef]
- Holmes, E.A.; O’Connor, R.C.; Perry, V.H.; Tracey, I.; Wessely, S.; Arseneault, L.; Ballard, C.; Christensen, H.; Silver, R.C.; Everall, I.; et al. Multidisciplinary Research Priorities for the COVID-19 Pandemic: A Call for Action for Mental Health Science. Lancet Psychiatry 2020, 7, 547–560. [Google Scholar] [CrossRef]
- Bu, F.; Steptoe, A.; Fancourt, D. Loneliness during a Strict Lockdown: Trajectories and Predictors during the COVID-19 Pandemic in 38,217 United Kingdom Adults. Soc. Sci. Med. 2020, 265, 113521. [Google Scholar] [CrossRef]
- Buecker, S.; Horstmann, K.T.; Krasko, J.; Kritzler, S.; Terwiel, S.; Kaiser, T.; Luhmann, M. Changes in Daily Loneliness for German Residents during the First Four Weeks of the COVID-19 Pandemic. Soc. Sci. Med. 2020, 265, 113541. [Google Scholar] [CrossRef] [PubMed]
- Devaraj, S.; Patel, P.C. Change in Psychological Distress in Response to Changes in Reduced Mobility during the Early 2020 COVID-19 Pandemic: Evidence of Modest Effects from the U.S. Soc. Sci. Med. 2021, 270, 113615. [Google Scholar] [CrossRef] [PubMed]
- El-Zoghby, S.M.; Soltan, E.M.; Salama, H.M. Impact of the COVID-19 Pandemic on Mental Health and Social Support among Adult Egyptians. J. Community Health 2020, 45, 689–695. [Google Scholar] [CrossRef] [PubMed]
- Pierce, M.; McManus, S.; Hope, H.; Hotopf, M.; Ford, T.; Hatch, S.L.; John, A.; Kontopantelis, E.; Webb, R.T.; Wessely, S.; et al. Mental Health Responses to the COVID-19 Pandemic: A Latent Class Trajectory Analysis Using Longitudinal UK Data. Lancet Psychiatry 2021, 8, 610–619. [Google Scholar] [CrossRef]
- Pierce, M.; Hope, H.; Ford, T.; Hatch, S.; Hotopf, M.; John, A.; Kontopantelis, E.; Webb, R.; Wessely, S.; McManus, S.; et al. Mental Health before and during the COVID-19 Pandemic: A Longitudinal Probability Sample Survey of the UK Population. Lancet Psychiatry 2020, 7, 883–892. [Google Scholar] [CrossRef]
- Yu, H.; Li, M.; Li, Z.; Xiang, W.; Yuan, Y.; Liu, Y.; Li, Z.; Xiong, Z. Coping Style, Social Support and Psychological Distress in the General Chinese Population in the Early Stages of the COVID-19 Epidemic. BMC Psychiatry 2020, 20, 426. [Google Scholar] [CrossRef]
- Latikka, R.; Koivula, A.; Oksa, R.; Savela, N.; Oksanen, A. Loneliness and Psychological Distress before and during the COVID-19 Pandemic: Relationships with Social Media Identity Bubbles. Soc. Sci. Med. 2022, 293, 114674. [Google Scholar] [CrossRef]
- Brooks, S.K.; Webster, R.K.; Smith, L.E.; Woodland, L.; Wessely, S.; Greenberg, N.; Rubin, G.J. The Psychological Impact of Quarantine and How to Reduce It: Rapid Review of the Evidence. Lancet 2020, 395, 912–920. [Google Scholar] [CrossRef] [Green Version]
- Mata, J.; Wenz, A.; Rettig, T.; Reifenscheid, M.; Möhring, K.; Krieger, U.; Friedel, S.; Fikel, M.; Cornesse, C.; Blom, A.G.; et al. Health Behaviors and Mental Health during the COVID-19 Pandemic: A Longitudinal Population-Based Survey in Germany. Soc. Sci. Med. 2021, 287, 114333. [Google Scholar] [CrossRef]
| Age Groups | Age 16–39 | Age 40–59 | Age 60+ | |||
|---|---|---|---|---|---|---|
| Variables | N | Percentage or Mean (SD) | N | Percentage or Mean (SD) | N | Percentage or Mean (SD) |
| Age | 9051 | 30.76 (5.18) | 12,814 | 49.87 (5.32) | 7071 | 67.10 (5.24) |
| Smoking | ||||||
| Yes | 2497 | 27.59 | 3754 | 29.3 | 2169 | 30.67 |
| No | 6554 | 72.41 | 9060 | 70.7 | 4902 | 69.33 |
| Drinking | ||||||
| Yes | 982 | 10.85 | 2029 | 15.83 | 1256 | 17.76 |
| No | 8069 | 89.15 | 10,785 | 84.17 | 5815 | 82.24 |
| COVID-19 | ||||||
| Yes | 4295 | 47.45 | 6436 | 50.23 | 3737 | 52.85 |
| No | 4756 | 52.55 | 6378 | 49.77 | 3334 | 47.15 |
| Gender | ||||||
| Male | 4357 | 48.14 | 6212 | 48.48 | 3893 | 55.06 |
| Female | 4694 | 51.86 | 6602 | 51.52 | 3178 | 44.94 |
| Married | ||||||
| Yes | 6522 | 72.06 | 12631 | 98.57 | 7009 | 99.12 |
| No | 2529 | 27.94 | 183 | 1.43 | 62 | 0.88 |
| Hukou | ||||||
| Urban | 2346 | 25.92 | 3311 | 25.84 | 2241 | 31.69 |
| Rural | 6705 | 74.08 | 9503 | 74.16 | 4830 | 68.31 |
| Education | ||||||
| Illiteracy | 287 | 3.17 | 1838 | 14.34 | 2095 | 29.63 |
| Primary school | 599 | 6.62 | 2950 | 23.02 | 1878 | 26.56 |
| Junior high school | 3349 | 37 | 5170 | 40.35 | 1886 | 26.67 |
| Senior high school | 1771 | 19.57 | 1898 | 14.81 | 992 | 14.03 |
| University or above | 3045 | 33.64 | 958 | 7.48 | 220 | 3.11 |
| Self-reported health (SRH) | ||||||
| Poor | 537 | 5.93 | 2164 | 16.89 | 1818 | 25.71 |
| Fair | 631 | 6.97 | 1757 | 13.71 | 1198 | 16.94 |
| Good | 4428 | 48.92 | 5599 | 43.69 | 2659 | 37.6 |
| Very good | 1911 | 21.11 | 1592 | 12.42 | 694 | 9.81 |
| Excellent | 1544 | 17.06 | 1702 | 13.28 | 702 | 9.93 |
| Work | ||||||
| Yes | 7340 | 81.1 | 10,344 | 80.72 | 3515 | 49.71 |
| No | 1711 | 18.9 | 2470 | 19.28 | 3556 | 50.29 |
| N | 9051 | 12,814 | 7071 | |||
| Panel A | (2018, 2020) | ||||||
|---|---|---|---|---|---|---|---|
| (No, No) | (No, Yes) | (Yes, Yes) | (Yes, No) | ||||
| Smoking | N | 9844 | 313 | 3796 | 515 | ||
| Percentage | 68.04 | 2.16 | 26.24 | 3.56 | |||
| Drinking | N | 11,491 | 698 | 1290 | 989 | ||
| Percentage | 79.42 | 4.82 | 8.92 | 6.84 | |||
| Panel B | 2018 | 2020 | |||||
| Mean | SD | Mean | SD | Mean Difference | 95% Bootstrap CI | p-Value | |
| Smoking | 0.2980 | 0.4574 | 0.2840 | 0.4510 | 0.0140 | (0.0031, 0.0248) | 0.011 |
| Drinking | 0.1575 | 0.3643 | 0.1374 | 0.3443 | 0.0201 | (0.0122, 0.0280) | <0.001 |
| Age 16–39 | Age 40–59 | Age 60+ | ||||
|---|---|---|---|---|---|---|
| OR | 95% CI | OR | 95% CI | OR | 95% CI | |
| COVID-19 | ||||||
| No | (ref) | (ref) | (ref) | |||
| Yes | 1.068 * | 0.993–1.148 | 0.880 *** | 0.835–0.927 | 0.898 *** | 0.842–0.959 |
| Age | 1.150 * | 0.995–1.329 | 0.794 ** | 0.641–0.983 | 1.004 | 0.758–1.332 |
| Age2 | 0.998 ** | 0.995–1.000 | 1.002 ** | 1.000–1.005 | 1.000 | 0.998–1.002 |
| Gender | ||||||
| Female | (ref) | (ref) | (ref) | |||
| Male | 117.803 *** | 82.382–168.453 | 63.763 *** | 50.412–80.650 | 21.055 *** | 16.495–26.875 |
| Married | ||||||
| No | (ref) | (ref) | (ref) | |||
| Yes | 1.083 | 0.872–1.345 | 0.987 | 0.635–1.533 | 1.211 | 0.642–2.283 |
| Hukou | ||||||
| Rural | (ref) | (ref) | (ref) | |||
| Urban | 1.257 ** | 1.035–1.526 | 1.052 | 0.892–1.239 | 0.871 | 0.723–1.051 |
| Education | ||||||
| Illiteracy | (ref) | (ref) | (ref) | |||
| Primary school | 0.709 | 0.376–1.339 | 0.952 | 0.732–1.237 | 0.820 * | 0.649–1.037 |
| Junior high school | 0.741 | 0.420–1.307 | 0.645 *** | 0.505–0.823 | 0.762 ** | 0.606–0.958 |
| Senior high school | 0.687 | 0.384–1.227 | 0.619 *** | 0.467–0.820 | 0.570 *** | 0.430–0.754 |
| University or above | 0.273 *** | 0.152–0.490 | 0.463 *** | 0.329–0.653 | 0.524 *** | 0.321–0.854 |
| Self-reported health (SRH) | ||||||
| Poor | (ref) | (ref) | (ref) | |||
| Fair | 1.266 | 0.855–1.874 | 1.036 | 0.837–1.282 | 1.074 | 0.870–1.325 |
| Good | 1.256 | 0.910–1.734 | 1.201 ** | 1.004–1.437 | 1.164 | 0.967–1.401 |
| Very good | 1.406 ** | 1.000–1.975 | 1.152 | 0.926–1.433 | 1.039 | 0.799–1.351 |
| Excellent | 1.425 ** | 1.006–2.017 | 1.004 | 0.810–1.244 | 1.291 * | 0.999–1.668 |
| Work | ||||||
| No | (ref) | (ref) | (ref) | |||
| Yes | 1.101 | 0.856–1.416 | 0.962 | 0.806–1.149 | 1.190 ** | 1.017–1.391 |
| Drinking | ||||||
| No | (ref) | (ref) | (ref) | |||
| Yes | 2.070 *** | 1.714–2.500 | 1.532 *** | 1.337–1.756 | 1.402 *** | 1.184–1.660 |
| Constant | 0.002 *** | 0.000–0.015 | 7.091 | 0.037–1353.468 | 0.151 | 0.000–2515.675 |
| N | 9051 | 12,814 | 7071 | |||
| Age 16–39 | Age 40–59 | Age 60+ | ||||
|---|---|---|---|---|---|---|
| OR | 95% CI | OR | 95% CI | OR | 95% CI | |
| COVID-19 | ||||||
| No | (ref) | (ref) | (ref) | |||
| Yes | 0.710 *** | 0.626–0.804 | 0.852 *** | 0.788–0.920 | 0.868 *** | 0.789–0.955 |
| Age | 0.968 | 0.824–1.136 | 0.921 | 0.748–1.134 | 1.009 | 0.747–1.363 |
| Age2 | 1.001 | 0.998–1.004 | 1.001 | 0.999–1.003 | 1.000 | 0.998–1.002 |
| Gender | ||||||
| Female | (ref) | (ref) | (ref) | |||
| Male | 9.516 *** | 7.002–12.933 | 10.398 *** | 8.474–12.759 | 9.656 *** | 7.457–12.505 |
| Married | ||||||
| No | (ref) | (ref) | (ref) | |||
| Yes | 1.409 *** | 1.103–1.801 | 1.637 * | 0.997–2.686 | 0.797 | 0.393–1.617 |
| Hukou | ||||||
| Rural | (ref) | (ref) | (ref) | |||
| Urban | 0.832 | 0.668–1.036 | 1.168 * | 0.996–1.370 | 0.888 | 0.726–1.086 |
| Education | ||||||
| Illiteracy | (ref) | (ref) | (ref) | |||
| Primary school | 2.166 ** | 1.102–4.260 | 0.892 | 0.695–1.144 | 0.913 | 0.726–1.149 |
| Junior high school | 2.412 *** | 1.299–4.477 | 1.090 | 0.866–1.374 | 0.902 | 0.715–1.139 |
| Senior high school | 1.976 ** | 1.046–3.735 | 0.961 | 0.732–1.263 | 0.690 ** | 0.512–0.930 |
| University or above | 1.619 | 0.850–3.086 | 0.622 *** | 0.441–0.878 | 1.096 | 0.679–1.769 |
| Self-reported health (SRH) | ||||||
| Poor | (ref) | (ref) | (ref) | |||
| Fair | 1.116 | 0.744–1.676 | 1.698 *** | 1.345–2.143 | 1.951 *** | 1.532–2.485 |
| Good | 0.849 | 0.606–1.191 | 1.642 *** | 1.344–2.006 | 1.967 *** | 1.588–2.438 |
| Very good | 0.811 | 0.566–1.162 | 1.925 *** | 1.522–2.433 | 2.109 *** | 1.596–2.786 |
| Excellent | 1.146 | 0.800–1.640 | 2.126 *** | 1.687–2.680 | 2.116 *** | 1.615–2.773 |
| Work | ||||||
| No | (ref) | (ref) | (ref) | |||
| Yes | 1.161 | 0.885–1.521 | 1.223 ** | 1.022–1.464 | 1.230 ** | 1.034–1.462 |
| Smoking | ||||||
| No | (ref) | (ref) | (ref) | |||
| Yes | 2.084 *** | 1.726–2.516 | 1.519 *** | 1.325–1.740 | 1.399 *** | 1.182–1.657 |
| Constant | 0.008 *** | 0.001–0.096 | 0.055 | 0.000–9.435 | 0.025 | 0.000–815.180 |
| N | 9051 | 12,814 | 7071 | |||
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Wang, X.; Ma, Z.; Wang, C. A Longitudinal Study on the Addictive Behaviors of General Population before and during the COVID-19 Pandemic in China. Int. J. Environ. Res. Public Health 2022, 19, 5979. https://doi.org/10.3390/ijerph19105979
Wang X, Ma Z, Wang C. A Longitudinal Study on the Addictive Behaviors of General Population before and during the COVID-19 Pandemic in China. International Journal of Environmental Research and Public Health. 2022; 19(10):5979. https://doi.org/10.3390/ijerph19105979
Chicago/Turabian StyleWang, Xiaoyu, Zaifei Ma, and Chunan Wang. 2022. "A Longitudinal Study on the Addictive Behaviors of General Population before and during the COVID-19 Pandemic in China" International Journal of Environmental Research and Public Health 19, no. 10: 5979. https://doi.org/10.3390/ijerph19105979
APA StyleWang, X., Ma, Z., & Wang, C. (2022). A Longitudinal Study on the Addictive Behaviors of General Population before and during the COVID-19 Pandemic in China. International Journal of Environmental Research and Public Health, 19(10), 5979. https://doi.org/10.3390/ijerph19105979






