Abstract
Worldwide commitment to disseminate Psychological First Aid (PFA) training to enable frontline workers to support distressed individuals and/or manage their own self-care is increasing, but the evidence base of PFA training is uncertain. Method: a scoping review was undertaken by searching seven databases and hand-searching grey literature to maximise coverage of potential studies. Results: Twenty-three studies met the inclusion criteria. Three PFA training models were commonly used in research studies. A broad selection of PFA training outcomes were observed including learning, behavior, satisfaction and practice in crisis mental and behavior health preparedness. Conclusions: Research evidence of reasonable quality demonstrates that PFA training significantly improves knowledge of appropriate psychosocial response and PFA skills in supporting people in acute distress, thereby enhancing self-efficacy and promoting resilience. However, this review highlights inadequate guidance on how PFA training should be applied and adapted, significant shortcomings of reporting PFA training delivery, limited training evaluation and unclear training outcomes. Whilst behavioral, knowledge and system impact of the PFA training are promising, methodologically stronger evaluations which include systematic training adaptation and selection of sensitive outcome measures is needed to strengthen future implementation of PFA training and thereby enhance population preparedness for future emergencies.
1. Introduction
At time of writing, the mental health crisis posed by the COVID-19 pandemic has reached an epidemic level, threatening the health and economic prosperity of all nations [1]. Early psychosocial response to those affected by such traumatic events is necessary to prevent the onset of mental illness [2]. Frontline healthcare workers are at the forefront of supporting acutely distressed individuals through providing early psychosocial care. Apart from their pivotal role and responsibility for patient care, frontline health workers are also at high-risk themselves of moral injury and mental health problems arising from working in overwhelming stressful situations. This can, in turn, have negative consequences for the quality of patient care and increased attrition rates in the health professions [3,4]. This situation is considered by some as a consequence of an historical underinvestment in mental health prevention, especially in preparing healthcare workers to manage their own self-care [5].
The COVID-19 pandemic is the latest crisis to highlight the importance of Psychological First Aid (PFA) training as being critical to empower frontline workers to mitigate the adverse impact of crises through primarily supporting people in need and promoting self-care [6,7]. However, PFA as a frontline approach to providing immediate psychosocial care is not new. First coined at the end of World War II PFA became increasingly popular in the 1980s and 1990s amongst disaster mental health experts since it offered an integrated continuum of critical incident stress management techniques [8,9]. Despite its long history, PFA has emerged as a mainstay for early psychological intervention only since the post-9/11 era [10,11]. Increasing concern about the unintended consequences of psychological debriefing (e.g., increased risk of PTSD and depression) has accelerated the use of PFA as a “do no harm” alternative and gained a broad professional consensus [11,12]. Since then, numerous PFA frameworks and models have been developed emphasising different components and areas of focus for specific populations and organisations [11]. Whilst here is no universally accepted definition of PFA across different models, the five Hobfoll’s intervention principles established in 2007 has exerted a profound influence on the PFA as an emerging field [13]. For instance, World Health Organization which published its PFA guide in 2011 [14] and the Johns Hopkins PFA Guide published in 2017 [15] both incorporate essential elements of other previous PFA models to assist recovery and both are underpinned by five intervention principles which aim to promote: a sense of safety, calming, a sense of self and community efficacy, connectedness and hope.
While PFA as a therapeutic intervention is still lacking sufficient evidence to support a clinical treatment standard or guideline [16,17,18], this does not, however, detract from the potential utility of PFA training for frontline health professionals. PFA training is an educational intervention that aims to equip workers with the knowledge and skills to deliver PFA as the therapeutic intervention to individuals who require immediate psychological support following a crisis. PFA training as an educational intervention to ensure universal crisis mental health preparedness has several potential advantages. Firstly, PFA as a therapeutic intervention does not involve diagnosis and treatment but provides health workers with a stepwise approach to delivering mental health support which includes approaching the person non-judgmentally, assessing their needs, supporting them with information gathering and linking them with further resources [14,19,20]. Second, as an entry point to more intensive mental health skills, PFA training offers health care professionals with expertise in delivering a low-intensity, step-by-step, therapeutic approach which can be applied in a wide range of humanitarian and disaster situations [10]. Given this, PFA training seems well-suited to delivery within the curriculum for non-specialist frontline workers to prepare them to provide psychosocial care for distressed individuals whilst also ensuring a resilient workforce able to respond effectively to disasters and emergencies [21,22].
The last decade has witnessed a boom in various PFA capacity building and training initiatives for disaster mental health preparedness. Recognizing the significance in mounting psychosocial support following critical events, the dissemination of PFA training has evolved into a frontline psychosocial response skillset that now govern and define how we conceptualize mental health crisis response [23,24]. It is widely accepted that PFA training can be adapted to meet the priorities of the trainees and/or their practice context and delivered on different platforms (live, online and mobile), so creating numerous options for the training programmes [25,26,27]. Furthermore, the increasing availability and promotion of PFA training reflects increasing recognition of the need for mental health crisis mitigation at a population level. For example, PFA was identified as the theme of 2016 World Mental Health Day which aimed to improve mental awareness and called for broad PFA training reach [27]. Advocates of PFA training propose that it should be accessible to all healthcare workers to increase their coping ability, reduce their risk of distress and provide them with skills to better deliver person-centred care [28,29,30]. However, in spite of increasing opportunities for PFA training the current state of PFA training and the outcomes of training for trainees and ultimately for disaster victims are uncertain.
Since the COVID-19 pandemic is likely stimulate increased interest in PFA training to equip healthcare workers to manage the mental health impact of any future pandemics, it is more important than ever to map the existing literature on PFA training The purpose of this review is to examine PFA training evidence to establish the breadth of current training applications, its implementation and outcomes, as well as the barriers and enablers to training in order to guide future PFA training use and support the potential scaling up frontline capacity-building approach.
2. Materials and Methods
Given the broad purpose, a scoping review was considered most appropriate since it provides a systematic methodology for determining the state of the evidence on a topic. Therefore, this review followed the guidelines proposed by Arksey & O’Malley [31], which involves five key steps: developing the research question; identifying relevant studies; selecting studies according to inclusion and exclusion criteria; charting the data; collating, summarising and reporting the results and considering the implications of the study findings for policy, practice and research [32].
2.1. Identifying the Research Question
The research question was identified as: ‘What is the current application of PFA training as an evidence based educational intervention? To address the research question, the following two objectives were developed: (a) To identify and describe the key components of PFA training and its implementation; and (b) To summarise the evidence on the implementation and outcomes of PFA training.
2.2. Identifying Relevant Studies
Considering the broad uncertainties on its use and various terms used to describe PFA, a pilot search was conducted to establish a comprehensive background understanding of PFA. Informed by a previous review of PFA [11], all related search terms including “psychological first aid”, “PFA”, “community-based psychosocial support”, “disaster behavior first aid” and “stress first aid” were included in the pilot search. In this pilot search, no methodological, language or date restrictions were employed. The search results were screened by the first author and discussed with the co-authors.
The pilot search revealed that studies with PFA training as an educational intervention did not always include PFA in the title or abstract, did not always include or included only in part the five key elements—and so a search strategy using the words “Psychological First Aid” and “PFA” would be sensitive and would identify a very high proportion of relevant literature. Given this, the review adopted a two-step approach. The approach taken was to: (1) use a variety of terms searching PFA, and then; (2) hand search the papers identified in step one to identify training intervention studies.
The comprehensive search was conducted within seven electronic databases (MEDLINE, PsychINFO, CINAL, Cochrane, Web of Science, PILOTS and CNKI (Chinese) since 1945, which was the year that the term “psychological first aid” was coined in American medical literature by Blain, Hoch and Ryan [8]. The refined search strategy for the literature involved: (i) a traditional search: as an example, the MEDLINE database search for “Psychological First Aid” was (Psychological First Aid *).mp. (mp = title, abstract, original title, name of substance word, subject heading word, keyword heading word, protocol supplementary concept word, rare disease supplementary concept word, unique identifier); (ii) use of internet search engines; and (iii) grey literature by hand-searching reference lists (for example in relevant reviews or journal papers), by using a snowballing process by searching the internet (through Google and Google Scholar search engines, relevant organisational websites and key journals) [33].
2.3. Study Selection
The inclusion and exclusion criteria (see Table 1) were developed based on the PICOS (population, intervention, comparisons, outcomes, study) framework [34,35].

Table 1.
Inclusion and Exclusion criteria.
2.4. Charting of Information and Data within the Included Studies
After removal of duplicates, titles/abstracts were screened in duplicate using Covidence software [36]. Disagreements and uncertainties were resolved by discussion with reference to the title and abstract. Full-text articles were retrieved if inclusion criteria were met or if the abstract did not contain sufficient information; then screened in duplicate with disagreements resolved by discussion.
Data exaction tables were created approved by all authors that included: details of different PFA models comparison (Table 2); general study characteristics -author, year, country of study, aim, design, outcome and key findings (Table 3); summary of current training and outcomes using the Template for Intervention Description and Replication (TIDieR) checklist (Table 4); outcome measures of the training (Table 5).
A formal quality assessment of the articles was not performed as this was not required in line with the scoping review methodology and the paucity of PFA training effectiveness evidence.
2.5. Collating, Summarising and Reporting Results
An analytical descriptive method was used to chart the data on the PFA training intervention and to extract contextual or process-oriented information from included studies [37]. Studies were charted according to the TIDieR checklist items, e.g., underlying theory (why), materials and procedures used (what), the intervention provider (who), the mechanism of delivery (how), the location (where), intervention schedule and intensity (when and how much), whether adaptations were used (tailoring) and the intervention adherence (how well) [38]. A narrative synthesis approach was used to provide a thorough account of the data and to draw comparisons across different PFA training intervention.
3. Result
3.1. Study Selection
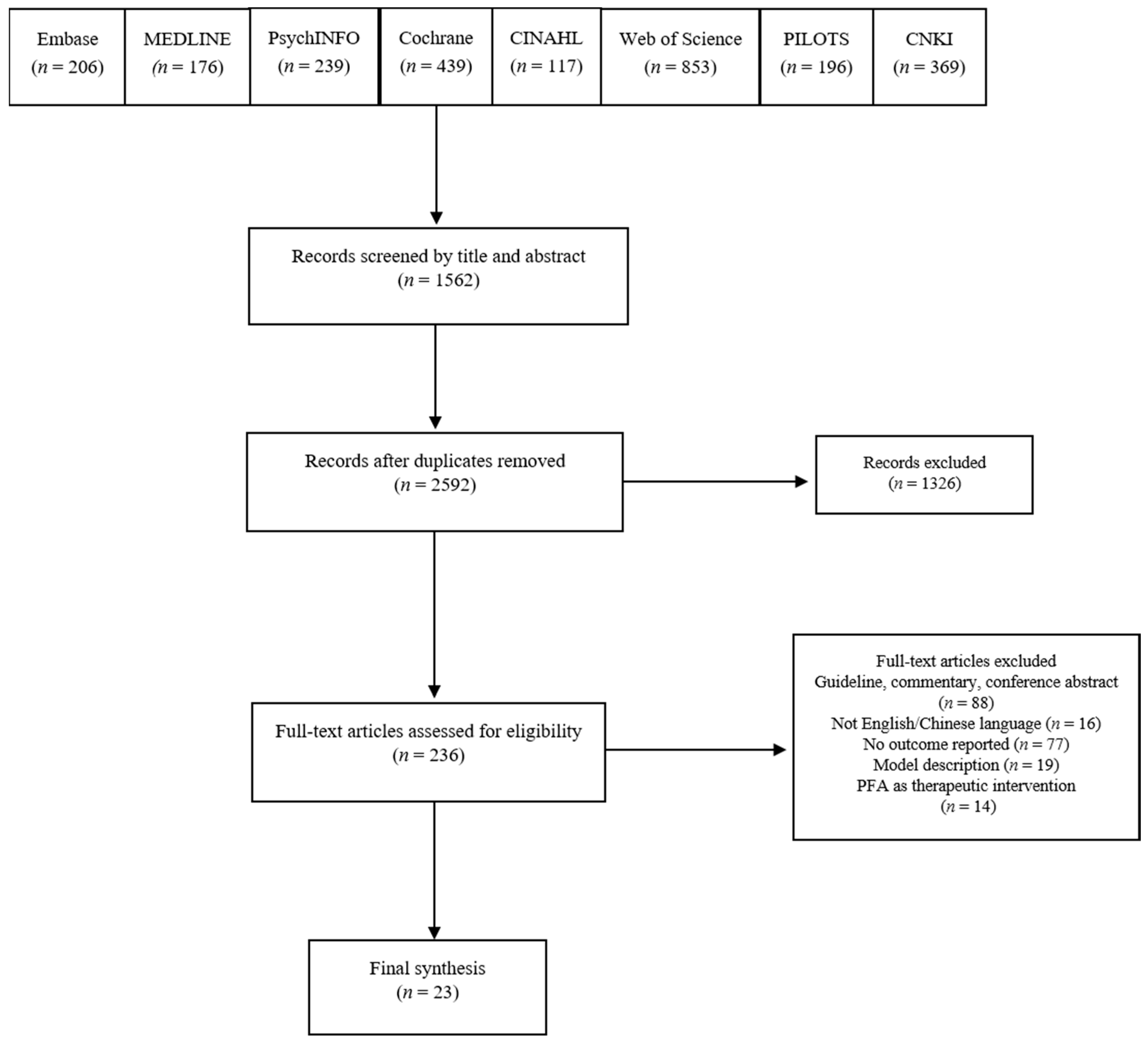
The initial search returned 2592 records (Figure 1). Screening of titles and abstracts excluded 1362 articles, leaving 236 as potentially eligible. Screening of full-text items excluded an additional 213 articles, for the following reasons: lack of model description (n = 19), no outcome reported (n = 77), ineligible publication type (n = 88), not English/Chinese language (n = 16) and not PFA training (n = 14). Of the remaining 23 eligible articles 20 used a quantitative research design and three used a qualitative research design.
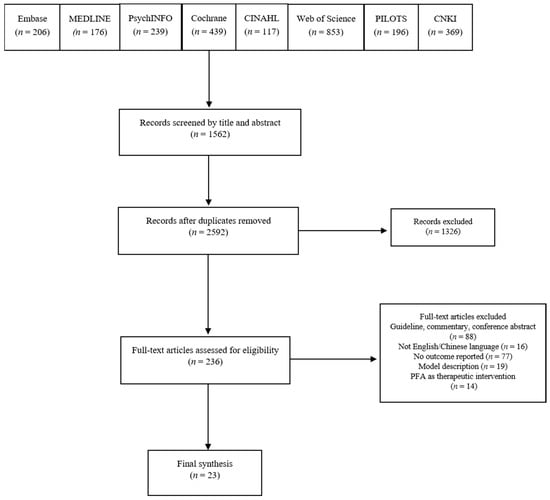
Figure 1.
PRISMA flowchart.
3.2. PFA Models
The most commonly used PFA models in training evaluations studies were the Psychological First Aid Guide for Field Workers [14], the Psychological First Aid: Field Operations Guide [20], the Johns Hopkins Guide to Psychological First Aid [15]. A comparison table of these PFA models and the Immediate Cognitive-Functional Psychological First Aid (ICF-PFA) model (which is used less frequently), is provided below (see Table 2). This table compares models using Hobfoll’s five principle goals of PFA: (i) how to approach and listen, (ii) assess the needs, (iii) provide support with information, (iv) referral and (v) self-care. The available resources and settings in which evaluations have been undertaken are also compared.

Table 2.
Comparison of different PFA model.
3.2.1. Psychological First Aid: Guide for Field Workers
This model was jointly developed by the World Health Organisation, World Vision International and War Trauma Foundation based on the contributions of 60 international peer reviewers and has been endorsed by 24 humanitarian organisations. The guide’s authors deliberately used simple language to make it easily adaptable for diverse socio-cultural settings within in low-and middle-income countries (LMICs). As PFA was part of a broader response to crises which was recommended by the Inter-Agency Standing Committee guidelines on Mental Health and Psychosocial Support (MHPSS), it fueled the dissemination of the WHO PFA guide in humanitarian aid settings. The PFA guide for field workers was subsequently developed and accompanied by a facilitator’s manual and tailored for specific fields, for example, Ebola Virus Disease, and has been translated into more than 20 languages. In order to drive the humanitarian aid capacity-building initiatives mostly in LMICs, WHO, in collaboration with international organisations and local institutions offered various resources and networks to facilitate the spread of PFA training courses worldwide [39,40,41,42].
3.2.2. Psychological First Aid: Field Operations Guide
This model was created collaboratively between the National Child Traumatic Stress Network (NCTSN) and the National Center for Posttraumatic Stress Disorder in America. The National Center for PTSD, the International Federation of the Red Cross (IFRC) and the American Red Cross (ARC), had all advocated that PFA training should be a mandatory, priority skills-based training for first responders, in order to equip them with the skills and knowledge to address the mental health consequences of responding to disasters and public health emergencies. Since the second and most current edition of the guide, published in 2006, several translations and system-specific adaptations of the PFA guide along with the training approaches had been developed and are available as open access resources [20]. The distribution of operation manuals for related groups (such as homeless, nursing home staff, medical reserve corps volunteers) had explicitly contributed to wide-spread application of PFA as a disaster intervention tool [43,44,45,46,47].
3.2.3. The Johns Hopkins Guide to Psychological First Aid
This model was developed by George Everly and Jeffery Lating. It was based upon their accumulated field experience, whereas the guide was produced in collaboration with the Johns Hopkins University’s, United States Centers for Disease Control and Prevention, who provided organisational support. As one of the most disaster-prone countries aiming to enhance surge capacity, a large initiative representing 14 preparedness and emergency response learning centres were established to equip the public health workforce with PFA competencies which further shaped the present model through expert consensus. In contrast to the first two models, the Johns Hopkins Guide, (also known and referred to as the RAPID PFA model), purports to be a theory-driven, evidence-informed and empirically validated model [48,49]. A therapeutic intervention, based on the Johns Hopkins Guide to PFA has been evaluated in a randomised controlled trial [50,51].
3.2.4. Mixed Models
A blend of the elements of the three commonly used models described above was also identified. These modified PFA training programmes were tailored for delivery to college students and school counsellors [52,53,54]. Amongst these mixed PFA models was the SIX Cs model (also known as immediate cognitive-functional PFA ICF-PFA), which contained six basic elements: cognitive communication, challenge and control, commitment and continuity [55].
3.3. Characteristics of Included Studies
PFA training evaluations (Table 3) have been undertaken in 10 countries: Haiti, Israel, Turkey, Korea, Japan, China, Sierra Leone, Lebanon, Australia and the USA. Of these, 15 studies were conducted in upper-and-middle income countries (n = 15, 68%), most notably in the USA (n = 11, 52%). The majority (n = 19, 83%) of the PFA training courses were applied by humanitarian aid and disaster response sectors and mostly delivered to non-specialists first responders such as Non-Government Organisation (NGO) staff, health workers, lay community citizens, faith leaders and police. The sample sizes ranged from 76 to 1500 (Mean = 82). Most PFA trainees were female (i.e., 65% to 99%). Of six studies reporting the length of trainees work experience, half of the school counsellors and medical reserve corps had less than 5 years in employment [46,53], however, nursing home staff and police trainees had more than 14 years’ work experience [45,56]. More than 50% of trainees were educated to degree level in a related discipline (e.g., psychology, social work, nursing, education) [44,46,57], and among primary healthcare workers responding to Ebola outbreak less than 10% were educated to diploma level [40]. More than 50% trainees (community leaders and nursing students) had no prior disaster or emergency experience [52,56].

Table 3.
Characteristics of included studies (n = 23).
Most studies used a pre-and-post intervention research design (n = 14, see Table 3), whereas four studies only collected a post-intervention data. Even though four studies conducted a randomised controlled trial (RCT) [42,47,52,54], their randomisation methods were not described in detail. In the seven studies that conducted follow-up evaluations, these ranged from two weeks to six months follow up periods [42,44,47,52,55,56,57]. Six studies reported using a mixed-method evaluation design and three studies only collected qualitative data. Few studies collected views of third parties within their evaluations (e.g., course facilitator’s field notes, subjected trainees to observation by ward mangers or collected data from service users) [56,57,58]. The selection and type of outcomes measures varied enormously across studies (Table 5).

Table 5.
Outcome measures of PFA training.
3.4. The Characteristics of PFA Training Delivery
Table 4 presents results using the TIDieR [38] reporting checklist to describe the content and delivery of PFA training interventions, such as “why”, “who”, “how”, “when” and “how much”, “tailoring” and “how well” for the 20 quantitative studies. The table does not include the three qualitative studies as they failed to report any details of the PFA training.

Table 4.
Summary of PFA trainings and outcomes according to the TIDieR checklist (n = 20).
3.4.1. Theory (Why?)
All studies reported either a rationale, a goal, or an underpinning theory of the PFA training intervention with regard to training design and/or delivery. Most studies provided a rationale statement for the training, whereas two studies also incorporated theoretical concepts. Everly et al. justified the theoretical foundations for the Johns Hopkins PFA model, indicating the need to address determinants of environmental stressors via cognitive and subsequent affective change to establish the eight learning objectives in the training intervention [48]. Farchi stated four theoretical concepts of the ICF-PFA model: hardiness; sense of coherence; self-efficacy; and neuropsychology of the stress response [55].
3.4.2. Material and Procedures (What?)
Most studies reported their training intervention procedures or blended materials (n = 19, see Table 4). A few studies provided a full description of the training content covering theoretical knowledge (disaster mental health, resilience, common stress reactions) and subsequently PFA knowledge (basic principles, core actions of PFA, self-care). An educational package as a disaster toolkit was occasionally assembled for the trainees which incorporated PowerPoint slides and educational material about disaster mental health (e.g., literature references, videos, posters and brochures) [58,62]. Given the subsequent adaptations of the training in each study, no studies provided details of where their new materials could be accessed (e.g., online appendix, URL).
3.4.3. Training Provider (Who?)
PFA training courses were provided by mental health professionals, namely three psychiatrists [48,49,62], four psychologists [47,53,54,63] and five mental health researchers or practitioners [41,42,43,52,61]. Non-mental health professionals also provided the PFA training such as trained facilitators [44,58] and trained health workers [45,56].
3.4.4. Mechanism of Delivery and Location (How and Where?)
Current training evaluation studies had been done all using face-to-face sessions delivered in the workplace. These included interactive didactic presentations (n = 17) and role-play or simulation practice (n = 9) [42,44,46,47,49,52,53,57,63]. A few studies reported providing a train-the-trainer workshop (n = 4) [42,45,46,61]. The PFA training was administered for groups but only three studies stated the group size: 15–20 Non-Government Organisation (NGO) workers [41], 9–10 students in Kilic study [52] and three public health workers in role-playing reflective listening [49]. Of note, only Sijbrandij et al. reported providing supervision after the training course [42].
3.4.5. Training Schedule and Intensity (When and How Much?)
The length of PFA training courses varied considerably, ranging from a minimum of 90 min to a maximum of 6 days. Most PFA training was given in regular sequential sessions (e.g., spread between 1–2.5 days), with the majority in a one-day course (7–8 h) (n = 11, 55%). For example, the RAPID-PFA training programme was delivered in a 6-h/session in a one-day format. Some training interventions were provided in a very short format due to time constraints in real settings [42,45,61]. Most studies did not report full details of training intensity. Of those that did eight training courses were of a short-to-medium duration ranging from 4 session to 20 sessions and five studies reported that the training was delivered over three or four sessions [56,58,61,62,64].
3.4.6. Adaptations (Tailoring)
Most of the training courses incorporated some adaptation, although few elaborated upon the procedure for these adaptations. None of the studies incorporated systematic approaches to adaptation for example, stakeholder involvement to programme design, or testing and refinement of the training intervention. The PFA training content was tailored to the specific population or contexts, for instance, a health assistant-oriented version included problem solving, relaxation, breathing and mindfulness techniques, sleep hygiene education, stress management, social mobilisations, behavioral activation and self-care strategies [57].
3.4.7. Adherence and Fidelity (How Well)
The fidelity check of the training was only supported by three studies [42,53,58]. Only Sijbrandij et al. reported 72% to 95% adherence to key features of PFA training [42].
3.5. Outcomes of PFA Training
We have used Kirkpatrick’s levels of training evaluation to classify the outcomes into four subthemes: change in practice (evaluation of behaviour), change in knowledge, skills, attitude (evaluation of learning), satisfaction with training (programme evaluation) and change in participant outcomes (evaluation of trainee practice from recipients or observers) [65] (see Table 5).
3.5.1. Effect on Learning
Of the 14 studies reporting successful learning outcomes, there was an overall improvement in some or all aspects of knowledge and all trainees endorsed PFA training as helpful for increasing their preparedness. PFA training increased trainee’s knowledge and understanding of the appropriate psychosocial responses to traumatic events, how to provide support to individuals facing adversity and the need for self-care in stressful contexts. Improved knowledge acquisition and retention was reported to be sustained at 3-month and 6-month follow-up in a cluster randomised controlled trial compared with the baseline assessment [42].
An improvement in PFA skills (i.e., through application of PFA skills in real-world situations or simulated scenarios) was demonstrated in 12 studies. These skills included early detection of mental health distress, approach communication, relaxation techniques and stress management. Everly et al. assessed the trainees’ skills for early detection in a recognition task (via a videotape recognition exercise) indicating that trainees were able to recognise key clinical markers of acute distress with greater accuracy than the mental health-trained respondents in the comparison condition [48].
Twelve studies measured substantial improvements in attitude and awareness about disaster mental health, post-traumatic stress and mental illness. Trainees in all studies showed an improved attitude towards emergency response engagement, renewed awareness of nonverbal communication, readiness to deliver PFA and a clear focus on safety.
3.5.2. Effect on Behaviour
Seventeen studies reported a positive effect on behavioural outcomes including improving self-efficacy, resilience and capability in terms of being able to manage and respond to stress. The behavioural indexes in a one-year follow-up survey indicated that 83.5% trainees provided PFA to someone experiencing an emotional crisis in a non-disaster context (e.g., trauma caused by violence, serious illness or the death of a loved one) and reported an increased ability to cope [56]. One study using the professional’s quality of life scale evaluated at 3-month and 6-month follow-up did not show a significant difference compared with baseline [42].
3.5.3. Effect on Practice
Real world practice changes were evaluated in three studies, where post-training evaluation was conducted at follow-up with patients (or any individuals who suffered acute distress). These studies purported a positive effect on actual practice [43,56,57]. The only evidence available on how PFA training influenced practice from their recipients assessed the trainees’ clinical practice change at 4–6 weeks follow-up using both quantitative and qualitative data [57]. This study using the therapeutic engagement questionnaire investigated the service users who received the healthcare assistants’ services prior to their PFA training and followed up at two weeks later, indicating a statistical improvement in therapeutic engagement (59.6 in mean scores). In addition, when interviewed, their ward managers, reported having observed their staff using their new PFA skills and noticed a renewed enthusiasm and confidence in delivering therapeutic care practice [57].
Two self-report studies using a follow-up survey found trainees were better at responding in simulations of traumatic situations, for example, expressing empathy, differentiating psychological distress and dysfunction and making referrals or advocating for those in need [43,56].
3.5.4. Effect on Satisfaction
Of six studies reporting on PFA trainee satisfaction, findings suggested that the trainees were considerably satisfied (ranged from 68–80%) with the appropriateness of PFA training for preparing them for their role as aid workers, and with the materials, content and delivery of the course [41,43,45,47,57,62].
3.5.5. Effect on System Changes
In addition to training outcomes, changes at system level were reported. In an effort to assess the scalable PFA capacity-building initiatives in America, system impact was also evaluated at local and state government levels, including: (1) translational impact—improved organisation preparedness, increased awareness of emergency response facilities utilisation and strengthened emergency response network by partner engagement; and (2) policy change—acceptance of lay members into professional volunteer corps and investment support for continuous training [56,63,64]. PFA training delivered in response to an Ebola outbreak showed that it was well accepted by non-specialists, addressed significant gaps of mental health professionals and was considered cost-effective in low-resources settings, and therefore a way to strengthen in-country capacity of emergency response [60].
3.6. PFA Training Implementation Barriers and Enablers
Three qualitative studies [39,59,60] and three mixed-method studies [41,46,56] reported PFA training implementation barriers and enablers.
3.6.1. Potential Risks
Potential risks from inappropriately delivering PFA training was revealed from PFA trainees’ practice, such as confusion about role boundaries, inadequate skills development and inconsistent use of PFA guidance, which could potentially harm a person in distress [46,60]. Shortened PFA training led to insufficient understanding of the challenges in applying PFA [39]. PFA providers helping hurricane survivors reported that they often hesitated or over-estimated their roles in responding to survivors’ needs and felt they were unprepared to understand cultural differences [46]. Findings from a 1-day PFA training programme tailored to dealing with an outbreak of Ebola described potential risky practices in relation to the application of Hobfoll’s essential principles [60]. For example, giving a false reassurance to calm a distressed person by promising that everything would be fine which undermined their credibility and was counterproductive. Meanwhile, they also found trainees’ attempt to solve the problem for a distressed person rather than promoting the person’s own coping abilities, which could decrease self-efficacy and ultimately hinder recovery.
The major strengths of PFA is that it is regarded as a low-cost intervention and is sufficiently simple that non-mental health workers can easily acquire PFA knowledge and skills, however, the limited training time, absence of post training supervision and lack opportunity for putting PFA skills into practice could all potentially reduce its efficacy. Horn et al. reported findings from large PFA training initiatives delivered during an Ebola outbreak which suggested that PFA knowledge and skills were not easily acquired for these reasons and should be treated with caution [60].
3.6.2. Barriers and Enablers Factors to the PFA Training
This review identified limited implementation barriers which made it difficult to ensure proactive preparedness and capacity building. Firstly, difficulties of delivering high quality PFA training in emergency situations which had frequently led to delivering just-in time PFA training out of necessity [60].
Secondly, there were other obstacles to delivering high quality PFA training delivery, such as time constraints (e.g., workload made attending training difficult), lack of site-specific training content, limited organisational support due to the misinterpretation of PFA training by funders and confused conception of PFA [59]. Finally, Semlitz also found that lack of qualified PFA trainers and an underestimation of cultural differences in Japan might hinder the sustainability of the training [41].
Conversely, some studies reporting qualitative findings highlighted enabling factors which might improve the PFA training spread. Firstly, contextualisation/adaptation of the PFA training materials to the target trainees for which they were intended would be beneficial [60]. Clarification of the learning objectives with context-tailored content could sustain interest and promote uptake both at individual and organisational levels. In particular, Horn suggested that government standardisation of PFA training and integration in national emergency response structures/systems were important to strengthen organisational capacity [60]. Additionally, short yet ongoing training, using an existing training platform at prescheduled training time, and certain incentives (free training, credits) could be a feasible method of sustaining the training. A mixture of approaches (e.g., online, face-to-face, interactive, role play, real-world application) supplemented with materials in a short-term ongoing training (e.g., conferences, agency meetings, in-service days) was preferred by trainees [59]. Chandra pointed out that online back-up information system with referral resources, mobile PFA tips, lecture slides and evaluation tool with community were welcomed by disaster volunteers [46].
4. Discussion
This scoping review of Psychological First Aid training has mapped out the current PFA training application, outcomes and its implementation by reviewing available empirical evidence. The inadequate guidance on how PFA training should be applied and adapted, significant shortcomings of reporting PFA training delivery, limited training evaluation and unclear training outcomes have been highlighted.
4.1. Lack Guidance on PFA Training Application and Adaptation
Even though various models existed, three PFA models (WHO-PFA, NCTSN-PFA, RAPID-PFA) were most influential and each targeted different priorities and were developed for use in different populations and settings. For example, the WHO-PFA training manual introduced “Look, Listen, Link” action steps into 20 languages for use in various international settings, whereas training in the Johns Hopkins RAPID PFA model represented proactive preparedness efforts to enhance surge capacity during disaster scenarios in America [25]. As a general observation, there is currently insufficient clear guidance on how to adapt and implement these models for use in different populations and settings.
Firstly, the multitude of different PFA training resources brings complexities in interpretation which may lead to confusion for implementors [10,59]. Given this, it is increasingly common for trainers to integrate different PFA models when attempting to adapt PFA for their specific populations or settings [52,54], and in doing so, the fidelity to the core components of the PFA models remain unclear.
Secondly, PFA is predominately used in Western counties and humanitarian settings. PFA tends to be seen as only as a disaster frontline approach for first responders [10], which could further deter the use by other types of health workers, i.e., non-first responders’ groups.
Thus, despite an emerging consensus for making PFA a mandatory, pre-requisite training for all health workers to ensure frontline support [23], guidance on how to adapt PFA materials and deliver training for use in different settings and populations has not yet been developed. We would recommend that this work is urgent.
4.2. Significant Shortcomings in Reporting PFA Training Intervention
This review is the first to provide a detailed profile of current PFA training delivery using the TIDieR checklist and has revealed a striking variability. The significant shortcomings of reporting this educational intervention include a lack of clarification around the theoretical basis of the training, differences in training intensity and limited or no fidelity checks. This in turn leads to challenges for implementors, for example, no ideal length/duration for PFA training leads to varied interpretations, so training intensity can range from 90 min to 6 days. Additionally, in reporting their findings, many authors of the included studies do not provide adequate training content description or, information about how to access this information, which is likely to hamper the replicability of PFA training.
As a consequence of vague descriptions of PFA training content and delivery, it further highlights the difficulties of evaluating fidelity to the original PFA model. Thus, better reporting of PFA training interventions is essential to enable replication, implementation and also facilitate understanding the effectiveness, as there is still a lack of evidence on the use of PFA as a therapeutic intervention [66].
4.3. Unintended Potential Harms from Inappropriate Training Delivery
The unintended potential harms from inappropriate PFA training delivery identified by this review need to be considered by all stakeholders in order to support future uptake. These potential harms arise from trainees’ confusion about role boundaries in practicing PFA (e.g., how to assess and decide whether to refer to mental health services?). It is conceivable that inconsistences in PFA guidance could damage the widely held perception of PFA being a “good thing”. Similarly, a lack of training evaluations, and shortened and non-observable PFA training courses have reinforced the perception of PFA as easy to learn and cheap to deliver [60], and diluted versions of PFA training courses are increasingly common.
Baron argues that psychosocial training courses need to provide trainees with adequate opportunity to rehearse and practice [67], for instance, providing trainees with the opportunities to receive post training PFA supervision might be necessary. This review raises questions for future research, on whether insufficient PFA training without supervision leads to adequate skill development. Our review suggest action is needed to address these challenges in order to retain PFA as a humane, do no harm approach to support distressed ones, which is similar to the conclusions of a previous five-year retrospective report [10].
4.4. Limited Efforts in Evaluation of PFA Training
There is reasonable evidence in the effectiveness of the PFA training that it significantly improves both trainees’ knowledge of what an appropriate psychosocial response is and PFA skills to provide support to individuals exposed to acute adversity, thereby enhancing self-efficacy and promoting resilience. However, despite the popularity of the term “psychological first aid” in published literature, a limited number of robust evaluations have been taken. As our broad search returned near 3000 articles, only 23 studies met the inclusion criteria of having the training course having been empirically evaluated. Among these, over two third of PFA training evaluations were conducted in the high-income countries and mostly among the official disaster first responders such as NGO workers. This is due to their advanced systems receiving long-term funding, and a comprehensive capacity-building initiative through guidelines and strategic policy mechanisms [68]. Few evaluations have been undertaken in regions that experience frequent emergencies, such as Asian countries or in populations of healthcare sector workers who are the backbone workforce that are called out to respond to a range of public health emergencies and disaster situations.
We also found that there was a huge variability of research designs and outcome measures used to evaluate PFA training courses. Unfortunately, studies with larger samples and a longitudinal design or randomised trial designs were scarce. In particular, given that numerous online learning platform offering PFA training now exist, little is known about the feasibility, effects and costs of these online learning platforms comparing to other types of training delivery formats. This may explain why such preparedness and prevention efforts are not always prioritised in health care approaches by funders and policymaking [69]. Given the lack of formal consideration for evaluation, it may be helpful to develop evaluation protocols to inform local stakeholders, identify PFA training focal points and encourage collaboration through joint planning, monitoring and evaluating.
4.5. Less Defined Clear Outcomes for Evaluating the PFA Training
This review has classified the outcome measures for PFA training evaluation which include not only domains of wellbeing such as quality of life, resilience, but the broader range of knowledge, attitudinal and behavioral outcomes. This could serve as a basis for future more targeted selection of outcome measures to identify the anticipated and desired benefits. Secondly, this review shows that evaluators favored measures of knowledge acquisition and preparedness over skill development of the trainees. Importantly, researchers have evaluated less real-world application of PFA skills and knowledge via the measurement of service users’ outcomes. There is a need for future robust research studies to evaluate the application of PFA knowledge and skills in real world settings as part of achieving population-level crisis mental health preparedness.
4.6. Implications for Research and Policy
The following inter-linked future research questions arise from this review:
- What are the ‘core’ and ‘adaptable periphery’ components of PFA?
- Is PFA training sufficient to avoid unintended harms and should trainees be given supervision whilst they learn to put training into practice?
- Is PFA training effective and at what levels and which population?
The discussion of this review on solutions is in line with global discussions about the need to task-shift at least a portion of mental health care to non-specialists [70,71], and the integration of Mental Health and Psychosocial Support (MHPSS) into disaster risk reduction efforts [72]. Especially as mental health preparedness plays a crucial role in responding to public health emergencies across countries, better dissemination and advocacy to policy makers about evidence based PFA training intervention are essential pillars of prevention efforts.
4.7. Strengths and Limitations
There are several strengths to this review. Firstly, the review has identified the range of settings and populations in which PFA has been applied. Secondly, the use of TIDieR checklist enabled us to compare and contrast how PFA training for mental health preparedness has been designed and delivered. Thirdly, the review has classified and summarised the outcome measures used to evaluate PFA. Lastly, the review has identified barriers and enablers to implementing PFA, including potential unintended harms.
Several limitations are also apparent. Firstly, the TIDieR checklist highlighted poor adherence to CONSORT guidelines for accurately reporting PFA training intervention in some studies and attempts to contact several authors for more information went unanswered. Secondly, only standard indexed sources of published literature were searched, so the search strategy may not have identified all relevant studies and other “unevaluated” PFA training programmes may have been omitted.
5. Conclusions
Research evidence of reasonable quality demonstrates that PFA training significantly improves knowledge of appropriate psychosocial response and PFA skills in supporting people in acute distress, thereby enhancing self-efficacy and promoting resilience. The lack of guidance on how PFA training is applied and adapted, significant shortcoming of reporting PFA training delivery, lack of robust PFA training evaluation and clarity around outcomes has been highlighted. Whilst behavioral, knowledge and system impact of the PFA training are promising, methodologically stronger evaluations which include systematic training adaptation and selection of sensitive outcome measures is needed to strengthen future implementation of PFA training and thereby enhance population preparedness for future emergencies.
Author Contributions
Conceptualisation: M.L., I.N., L.W., Y.L., T.X.; screening/extraction: L.W.; discussion: M.L., I.N., L.W.; original draft preparation: L.W.; writing and editing: M.L., I.N., L.W. All authors have read and agreed to the published version of the manuscript.
Funding
This work was partially supported by the health research project of Hunan Provincial Health Commission (20190365) and the innovative education project of Central South University (2018CXKZ06).
Institutional Review Board Statement
Not applicable.
Informed Consent Statement
Not applicable.
Data Availability Statement
The data that support the findings of this study are available from the corresponding author, upon reasonable request.
Conflicts of Interest
The authors declare no conflict of interest.
References
- Holmes, E.A.; O’Connor, R.C.; Perry, V.H.; Tracey, I.; Wessely, S.; Arseneault, L.; Ballard, C.; Christensen, H.; Silver, R.C.; Everall, I.; et al. Multidisciplinary research priorities for the COVID-19 pandemic: A call for action for mental health science. Lancet Psychiatry 2020, 7, 547–560. [Google Scholar] [CrossRef]
- Bryant, R.A.; Litz, B. Mental Health Treatments in the Wake of Disaster. Ment. Health Disasters 2010, 321–335. [Google Scholar] [CrossRef]
- Greenberg, N.; Docherty, M.; Gnanapragasam, S.; Wessely, S. Managing mental health challenges faced by healthcare workers during covid-19 pandemic. BMJ 2020, 368, m1211. [Google Scholar] [CrossRef]
- Čartolovni, A.; Stolt, M.; Scott, P.A.; Suhonen, R. Moral injury in healthcare professionals: A scoping review and discussion. Nurs. Ethics 2021. [Google Scholar] [CrossRef]
- Policy Brief: COVID-19 and the Need for Action on Mental Health. Available online: https://unsdg.un.org/sites/default/files/2020-05/UN-Policy-Brief-COVID-19-and-mental-health.pdf (accessed on 12 December 2020).
- Psychological First Aid in Emergencies Training for Frontline Staff and Volunteers. Available online: https://www.gov.uk/government/news/psychological-first-aid-in-emergencies-training-for-frontline-staff-and-volunteers (accessed on 12 December 2020).
- Choong, T.C.; Chai, Y.C.; Huri, S.Z.; Nawawi, W.Z.W.; Ibrahim, N. Innovative psychological first aid (PFA) in the new normal for frontliners. Perspect. Psychiatr. Care 2020. [Google Scholar] [CrossRef]
- Daniel, B.; Hoch, P.; Ryan, V.G. A course in psychological first aid and prevention: A preliminary report. Am. J. Psychiatry 1945, 101, 629–634. [Google Scholar]
- Raphael, B. When Disaster Strikes; Basic Books: New York, NY, USA, 1986; p. 257. [Google Scholar]
- Church of Sweden. Psychological First Aid: Five Year Retrospective (2011–2016) Uppsala: Church of Sweden. 2018. Available online: https://www.svenskakyrkan.se/internationelltarbete/reports-policy-documents–and-positions-on-church-of-swedens-international-work (accessed on 12 December 2020).
- Shultz, J.M.; Forbes, D. Psychological first aid: Rapid proliferation and the search for evidence. Disaster Health 2014, 2, 3–12. [Google Scholar] [CrossRef]
- Rose, S.C.; Bisson, J.; Churchill, R.; Wessely, S. Psychological debriefing for preventing post traumatic stress disorder (PTSD). Cochrane Database Syst. Rev. 2002. [Google Scholar] [CrossRef]
- Hobfoll, S.E.; Watson, P.; Bell, C.C.; Bryant, R.A.; Brymer, M.J.; Friedman, M.J.; Friedman, M.; Gersons, B.P.; De Jong, J.T.; Layne, C.M.; et al. Five Essential Elements of Immediate and Mid–Term Mass Trauma Intervention: Empirical Evidence. Psychiatry 2007, 70, 283–315. [Google Scholar] [CrossRef]
- World Health Organization. War Trauma Foundation and World Vision International. Psychological First Aid: Guide for Fieldworkers; WHO: Geneva, Switzerland, 2011; Available online: https://www.who.int/publications/i/item/9789241548205 (accessed on 12 December 2020).
- Everly, G.S.; Lating, J.M. The Johns Hopkins Guide to Psychological First Aid; JHU Press: Baltimore, MD, USA, 2017. [Google Scholar]
- Dieltjens, T.; Moonens, I.; Van Praet, K.; De Buck, E.; Vandekerckhove, P. A Systematic Literature Search on Psychological First Aid: Lack of Evidence to Develop Guidelines. PLoS ONE 2014, 9, e114714. [Google Scholar] [CrossRef] [PubMed]
- North, C.S.; Pfefferbaum, B. Mental health response to community disasters: A systematic review. JAMA 2013, 310, 507–518. [Google Scholar] [CrossRef]
- Fox, J.H.; Burkle, F.M.; Bass, J.; Pia, F.A.; Epstein, J.L.; Markenson, D. The effectiveness of psychological first aid as a disaster intervention tool: Eesearch analysis of peer-reviewed literature from 1990–2010. Disaster Med. Public Health Prep. 2012, 6, 247–252. [Google Scholar] [CrossRef]
- Ruzek, J.I.; Brymer, M.J.; Jacobs, A.K.; Layne, C.M.; Vernberg, E.M.; Watson, P.J. Psychological first aid. J. Ment. Health Couns. 2007, 29, 17–49. [Google Scholar] [CrossRef]
- Brymer, M.; Jacobs, A.; Layne, C.; Pynoos, R.; Ruzek, J.; Steinberg, A.; Vernberg, E.; Watson, P. Psychological First Aid: Field Operations Guide, 2nd ed.; 2006. Available online: https://www.nctsn.org/resources/psychological-first-aid-pfa-field-operations-guide-2nd-edition. (accessed on 12 December 2020).
- Vernberg, E.M.; Steinberg, A.M.; Jacobs, A.K.; Brymer, M.J.; Watson, P.J.; Osofsky, J.D.; Layne, C.M.; Pynoos, R.S.; Ruzek, J.I. Innovations in disaster mental health: Psychological first aid. Prof. Psychol. Res. Pr. 2008, 39, 381–388. [Google Scholar] [CrossRef]
- Jacobs, G.A.; Gray, B.L.; Erickson, S.E.; Gonzalez, E.D.; Quevillon, R.P. Disaster Mental Health and Community-Based Psychological First Aid: Concepts and Education/Training. J. Clin. Psychol. 2016, 72, 1307–1317. [Google Scholar] [CrossRef] [PubMed]
- Roudini, J.; Khankeh, H.R.; Witruk, E. Disaster mental health preparedness in the community: A systematic review study. Health Psychol. Open 2017, 4, 2055102917711307. [Google Scholar] [CrossRef]
- McCabe, O.L.; Everly, G.S.; Brown, L.M.; Wendelboe, A.M.; Hamid, N.H.A.; Tallchief, V.L.; Links, J.M. Psychological First Aid: A Consensus-Derived, Empirically Supported, Competency-Based Training Model. Am. J. Public Health 2014, 104, 621–628. [Google Scholar] [CrossRef]
- COVID-19: Psychological First Aid. Available online: https://www.futurelearn.com/courses/psychological-first-aid-covid-19. (accessed on 12 December 2020).
- Psychological First Aid. Available online: https://www.coursera.org/learn/psychological-first-aid (accessed on 12 December 2020).
- Dignity in Mental Health. Psychological & Mental Health First Aid for All. Available online: https://www.who.int/mental_health/world-mental-health-day/paper_wfmh_2016.pdf (accessed on 12 December 2020).
- Gispen, F.; Wu, A.W. Psychological first aid: CPR for mental health crises in healthcare. J. Patient Saf. Risk Manag. 2018, 23, 51–53. [Google Scholar] [CrossRef]
- Everly, G.S., Jr. Psychological first aid to support healthcare professionals. J. Patient Saf. Risk Manag. 2020, 25, 159–162. [Google Scholar] [CrossRef]
- Shah, K.; Bedi, S.; Onyeaka, H.; Singh, R.; Chaudhari, G. The Role of Psychological First Aid to Support Public Mental Health in the COVID-19 Pandemic. Cureus 2020, 12, e8821. [Google Scholar] [CrossRef]
- Arksey, H.; O’Malley, L. Scoping studies: Towards a methodological framework. Int. J. Soc. Res. Methodol. 2005, 8, 19–32. [Google Scholar] [CrossRef]
- Levac, D.; Colquhoun, H.; O’Brien, K.K.; Levac, D.; Colquhoun, H.; O’Brien, K.K. Scoping studies: Advancing the methodology. Implement. Sci. 2010, 5, 69. [Google Scholar] [CrossRef] [PubMed]
- Franks, H.; Hardiker, N.; McGrath, M.; McQuarrie, C. Public health interventions and behaviour change: Reviewing the grey literature. Public Health 2012, 126, 12–17. [Google Scholar] [CrossRef]
- Helmer, D.; Savoie, I.; Green, C.; Kazanjian, A. Evidence-based practice: Extending the search to find material for the systematic review. Bull. Med. Libr. Assoc. 2001, 89, 346–352. [Google Scholar]
- Amir-Behghadami, M.; Janati, A. Population, Intervention, Comparison, Outcomes and Study (PICOS) design as a framework to formulate eligibility criteria in systematic reviews. Emerg. Med. J. 2020, 37, 387. [Google Scholar] [CrossRef]
- Babineau, J. Product Review: Covidence (Systematic Review Software). J. Can. Health Libr. Assoc. J. l’Association bibliothèques de la santé du Can. 2014, 35, 68–71. [Google Scholar]
- Grant, M.J.; Booth, A. A typology of reviews: An analysis of 14 review types and associated methodologies. Health Inf. Libr. J. 2009, 26, 91–108. [Google Scholar] [CrossRef]
- Hoffmann, T.C.; Glasziou, P.P.; Boutron, I.; Milne, R.; Perera, R.; Moher, D.; Altman, D.G.; Barbour, V.; Macdonald, H.; Johnston, M.; et al. Better reporting of interventions: Template for intervention description and replication (TIDieR) checklist and guide. BMJ 2014, 348, g1687. [Google Scholar] [CrossRef]
- Schafer, A.; Snider, L.; Van Ommeren, M. Psychological first aid pilot: Haiti emergency response. Intervention 2010, 8, 245–254. [Google Scholar] [CrossRef]
- Schafer, A.; Snider, L.; Sammour, R. A reflective learning report about the implementation and impacts of Psychological First Aid (PFA) in Gaza. Disaster Health 2015, 3, 1–10. [Google Scholar] [CrossRef]
- Semlitz, L.; Ogiwara, K.; Weissbecker, I.; Gilbert, E.; Sato, M.; Taniguchi, M.; Ishii, C.; Sawa, C. Psychological first aid training after Japan’s triple disaster: Changes in perceived self competency. Int. J. Emerg. Ment. Health Hum. Resil. 2013, 15, 181–196. [Google Scholar]
- Sijbrandij, M.; Horn, R.; Esliker, R.; O’May, F.; Reiffers, R.; Ruttenberg, L.; Stam, K.; de Jong, J.; Ager, A. The effect of psychological first Aid training on knowledge and understanding about psychosocial support principles: A cluster-randomized controlled trial. Int. J. Environ. Res. Public Health 2020, 17, 484. [Google Scholar] [CrossRef]
- Allen, B.; Brymer, M.J.; Steinberg, A.M.; Vernberg, E.M.; Jacobs, A.; Speier, A.H.; Pynoos, R.S. Perceptions of psychological first aid among providers responding to Hurricanes Gustav and Ike. J. Trauma. Stress 2010, 23, 509–513. [Google Scholar] [CrossRef]
- Akoury-Dirani, L.; Sahakian, T.S.; Hassan, F.Y.; Hajjar, R.V.; El Asmar, K. Psychological First Aid Training for Lebanese Field Workers in the Emergency Context of the Syrian Refugees in Lebanon. Psychol. Trauma Theory Res. Pr. Policy 2015, 7, 533–538. [Google Scholar] [CrossRef]
- Brown, L.M.; Bruce, M.L.; Hyer, K.; Mills, W.L.; Vongxaiburana, E.; Polivka-West, L. A Pilot Study Evaluating the Feasibility of Psychological First Aid for Nursing Home Residents. Clin. Gerontol. 2009, 32, 293–308. [Google Scholar] [CrossRef]
- Chandra, A.; Kim, J.; Pieters, H.C.; Tang, J.; McCreary, M.; Schreiber, M.; Wells, K. Implementing psychological first-aid training for medical reserve corps volunteers. Disaster Med. Public Health Prep. 2014, 8, 95–100. [Google Scholar] [CrossRef] [PubMed]
- Cheung, Y.L. Psychological First Aid as a Public Health Disaster Response Preparedness Strategy for Responders in Critical Incidents and Disasters. Ph.D. Thesis, The Chinese University of Hong Kong, Hong Kong, China, 2014. [Google Scholar]
- Everly, G.S., Jr.; Barnett, D.J.; Links, J.M. The Johns Hopkins model of psychological first aid (RAPID—PFA): Curriculum development and content validation. Int. J. Emerg. Ment. Health 2012, 14, 95–103. [Google Scholar] [PubMed]
- Everly, G.S., Jr.; McCabe, O.L.; Semon, N.L.; Thompson, C.B.; Links, J.M. The development of a model of psychological first aid for non–mental health trained public health personnel: The Johns Hopkins RAPID-PFA. J. Public Health Manag. Pract. 2014, 20, S24–S29. [Google Scholar] [CrossRef] [PubMed]
- Despeaux, K.E.; Lating, J.M.; Everly, G.S.; Sherman, M.F.; Kirkhart, M.W. A Randomized Controlled Trial Assessing the Efficacy of Group Psychological First Aid. J. Nerv. Ment. Dis. 2019, 207, 626–632. [Google Scholar] [CrossRef]
- Everly, G.S., Jr.; Lating, J.M.; Sherman, M.F.; Goncher, I. The potential efficacy of psychological first aid on self-reported anxiety and mood: A pilot study. J. Nerv. Ment. Dis. 2016, 204, 233–235. [Google Scholar] [CrossRef] [PubMed]
- Kılıç, N.; Şimşek, N. The effects of psychological first aid training on disaster preparedness perception and self-efficacy. Nurse Educ. Today 2019, 83, 104203. [Google Scholar] [CrossRef] [PubMed]
- Lee, J.-S.; You, S.; Choi, Y.-K.; Youn, H.-Y.; Shin, H.S. A preliminary evaluation of the training effects of a didactic and simulation-based psychological first aid program in students and school counselors in South Korea. PLoS ONE 2017, 12, e0181271. [Google Scholar] [CrossRef]
- Zhang, J.; Liu, J.; Xue, Z.; Xue, Y. Effect of psychological first aid training on medical students’ cognitive appraisal about sudden events. Chin. J. Behav. Med. Brain Sci. 2016, 25, 838–841. [Google Scholar]
- Farchi, M.; Ben Hirsch-Gornemann, M.; Whiteson, A.; Gidron, Y. The SIX Cs model for Immediate Cognitive Psychological First Aid: From Helplessness to Active Efficient Coping. Int. J. Emerg. Ment. Health Hum. Resil. 2018, 20, 1–12. [Google Scholar] [CrossRef]
- McCabe, O.L.; Semon, N.L.; Thompson, C.B.; Lating, J.M.; Everly, G.S.; Perry, C.J.; Moore, S.S.; Mosley, A.M.; Links, J.M. Building a National Model of Public Mental Health Preparedness and Community Resilience: Validation of a Dual-Intervention, Systems-Based Approach. Disaster Med. Public Health Prep. 2014, 8, 511–526. [Google Scholar] [CrossRef]
- Kantaris, X.; Radcliffe, M.; Acott, K.; Hughes, P.; Chambers, M. Training healthcare assistants working in adult acute inpatient wards in Psychological First Aid: An implementation and evaluation study. J. Psychiatr. Ment. Health Nurs. 2020, 27, 742–751. [Google Scholar] [CrossRef] [PubMed]
- Mosley, A.; Marum, F.; Gwon, H.S.; McCabe, O.L.; Kaminsky, M.J.; George, S.; Links, E.J.M., Jr.; Langlieb, A. Community capacity-building in disaster mental health resilience: A pilot study of an academic/faith partnership model. Int. J. Emerg. Ment. Health 2012, 14, 112–122. [Google Scholar]
- Hambrick, E.P.; Rubens, S.L.; Vernberg, E.M.; Jacobs, A.K.; Kanine, R.M. Towards successful dissemination of psychological first aid: A study of provider training preferences. J. Behav. Health Serv. Res. 2014, 41, 203–215. [Google Scholar] [CrossRef]
- Horn, R.; O’May, F.; Esliker, R.; Gwaikolo, W.; Woensdregt, L.; Ruttenberg, L.; Ager, A. The myth of the 1-day training: The effectiveness of psychosocial support capacity-building during the Ebola outbreak in West Africa. Glob. Ment. Health 2019, 6. [Google Scholar] [CrossRef]
- Lewis, V.; Varker, T.; Phelps, A.; Gavel, E.; Forbes, D. Organizational implementation of psychological first aid (PFA): Training for managers and peers. Psychol. Trauma Theory Res. Pract. Policy 2014, 6, 619. [Google Scholar] [CrossRef]
- McCabe, O.L.; Mosley, A.M.; Gwon, H.S.; Everly, G.S.; Lating, J.M.; Links, J.M.; Kaminsky, M.J. The tower of ivory meets the house of worship: Psychological first aid training for the faith community. Int. J. Emerg. Ment. Health Hum. Resil. 2007, 9, 171–180. [Google Scholar]
- McCabe, O.L.; Perry, C.; Azur, M.; Taylor, H.G.; Bailey, M.; Links, J.M. Psychological First-Aid Training for Paraprofessionals: A Systems-Based Model for Enhancing Capacity of Rural Emergency Responses. Prehosp. Disaster Med. 2011, 26, 251–258. [Google Scholar] [CrossRef] [PubMed]
- McCabe, O.L.; Semon, N.L.; Lating, J.M.; Everly, J.G.S.; Perry, C.J.; Moore, S.S.; Mosley, A.M.; Thompson, C.B.; Links, J.M. An Academic-Government-Faith Partnership to Build Disaster Mental Health Preparedness and Community Resilience. Public Health Rep. 2014, 129, 96–106. [Google Scholar] [CrossRef] [PubMed]
- Wilkes, M.; Bligh, J. Evaluating educational interventions. BMJ 1999, 318, 1269–1272. [Google Scholar] [CrossRef] [PubMed]
- Bisson, J.I.; Lewis, C. Systematic Review of Psychological First Aid; World Health Organization: Geneva, Switzerland, 2009. [Google Scholar]
- Baron, N. The’TOT’: A Global Approach for the Training of Trainers for Psychosocial and Mental Health Interventions in Countries Affected by War, Violence and Natural Disasters; National Emergency Training Center: Emmitsburg, MD, USA, 2006.
- Simmons, R.; Fajans, P.; Ghiron, L. (Eds.) Scaling up Health Service Delivery: From Pilot Innovations to Policies and Programmes; World Health Organization: Geneva, Switzerland, 2007. [Google Scholar]
- Généreux, M.; Schluter, P.J.; Takahashi, S.; Usami, S.; Mashino, S.; Kayano, R.; Kim, Y. Psychosocial Management Before, During, and After Emergencies and Disasters—Results from the Kobe Expert Meeting. Int. J. Environ. Res. Public Health 2019, 16, 1309. [Google Scholar] [CrossRef]
- Javadi, D.; Feldhaus, I.; Mancuso, A.; Ghaffar, A. Applying systems thinking to task shifting for mental health using lay providers: A review of the evidence. Glob. Ment. Health 2017, 4, e14. [Google Scholar] [CrossRef]
- Caulfield, A.; Vatansever, D.; Lambert, G.; Van Bortel, T. WHO guidance on mental health training: A systematic review of the progress for non-specialist health workers. BMJ Open 2019, 9, e024059. [Google Scholar] [CrossRef]
- Gray, B.; Hanna, F.; Reifels, L. The Integration of Mental Health and Psychosocial Support and Disaster Risk Reduction: A Mapping and Review. Int. J. Environ. Res. Public Health 2020, 17, 1900. [Google Scholar] [CrossRef]
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).