Using Digital Platforms to Promote Blood Donation: Motivational and Preliminary Evidence from Latin America and Spain
Abstract
1. Introduction
2. Theoretical Background and Hypotheses
2.1. Motivations for Blood Donation
2.2. Participation in Collaborative Digital Platforms
2.3. Theory of Planned Behaviour and Participation in Collaborative Platforms
2.4. Hypotheses
3. Materials and Methods
3.1. Study Design
3.2. Participants
3.3. Measures
3.4. Statistical Analysis
4. Results
4.1. Measurement Model
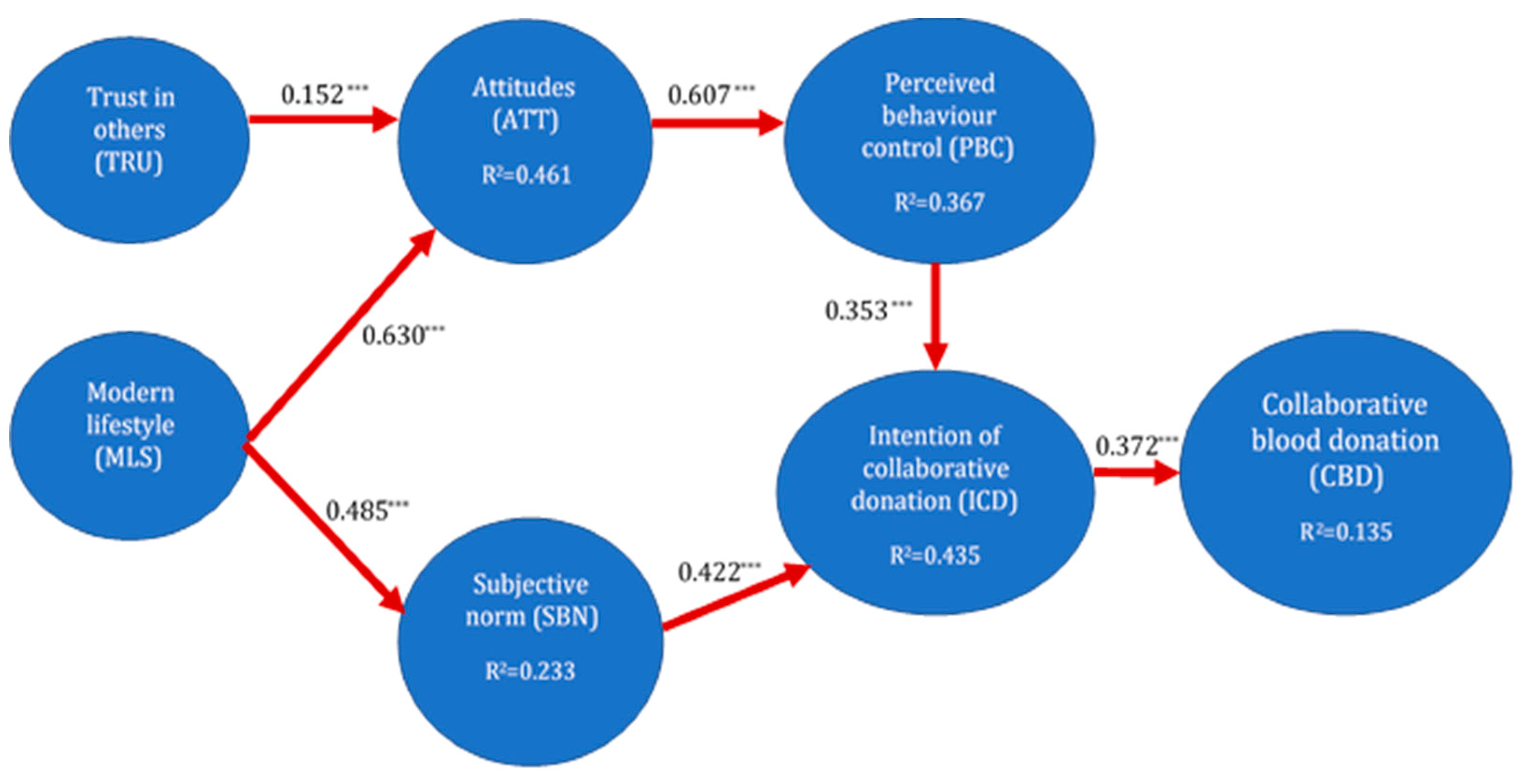
4.2. Structural Model
5. Discussion
5.1. Theoretical Implications
5.2. Management and Social Implications
5.3. Limitations
6. Conclusions
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Sanchez, A.M.; Ameti, I.D.; Schreiber, G.B.; Thomson, R.A.; Lo, A.; Bethel, J.; Williams, A.E. The potential impact of incentives on future blood donation behavior. Transfusion 2001, 41, 172–178. [Google Scholar] [CrossRef] [PubMed]
- Gillespie, T.W.; Hillyer, C.D. Blood donors and factors impacting the blood donation decision. Transfus. Med. Rev. 2002, 16, 115–130. [Google Scholar] [CrossRef] [PubMed]
- Martín-Santana, J.D.; Beerli-Palacio, A. Achieving donor repetition and motivation by block leaders among current blood donors. Transfus. Apher. Sci. 2012, 47, 337–343. [Google Scholar] [CrossRef] [PubMed]
- Grant, D.B. Integration of supply and marketing for a blood service. Manag. Res. Rev. 2010, 33, 123–133. [Google Scholar] [CrossRef]
- Akita, T.; Tanaka, J.; Ohisa, M.; Sugiyama, A.; Nishida, K.; Inoue, S.; Shirasaka, T. Predicting future blood supply and demand in Japan with a Markov model: Application to the sex- and age-specific probability of blood donation. Transfusion 2016, 56, 2750–2759. [Google Scholar] [CrossRef] [PubMed]
- Dhingra, N. International challenges of self-sufficiency in blood products. Transfus. Clin. Biol. 2013, 20, 148–152. [Google Scholar] [CrossRef]
- Shan, H.; Zhang, P. Viral attacks on the blood supply: The impact of severe acute respiratory syndrome in Beijing. Transfusion 2004, 44, 467–469. [Google Scholar] [CrossRef]
- Flavelle, C. Red Cross Warns of a ‘Staggering’ Drop in Blood Supplies. New York Times. 2020. Available online: https://www.nytimes.com/2020/06/02/climate/blood-donations-hospitals-shortage.html (accessed on 15 September 2020).
- Cortez, M.F. How Long Will Coronavirus Last? Pandemic Will Stretch Into 2021. Bloomberg. 2020. Available online: https://www.bloomberg.com/news/features/2020-06-18/we-will-be-living-with-the-coronavirus-pandemic-well-into-2021 (accessed on 15 September 2020).
- World Health Organization. “The Pandemic Is Accelerating”: WHO Warns of Dangerous Coronavirus Phase—Video, World News|Guard. 2020. Available online: https://www.theguardian.com/world/video/2020/jun/20/the-pandemic-is-accelerating-who-warns-of-dangerous-coronavirus-phase-video (accessed on 15 September 2020).
- Masser, B.M.; Hyde, M.K.; Ferguson, E. Exploring predictors of Australian community members’ blood donation intentions and blood donation-related behavior during the COVID-19 pandemic. Transfusion 2020. [Google Scholar] [CrossRef]
- Taş, A.; Kiraz, E.D.E. Are future doctors ready to donate blood and encourage blood donation? Transfus. Apher. Sci. 2018, 57, 569–572. [Google Scholar] [CrossRef]
- World Health Organization (WHO). Blood Safety and Availability, Fact Sheet. (n.d.). Available online: https://www.who.int/en/news-room/fact-sheets/detail/blood-safety-and-availability (accessed on 15 September 2020).
- Sultan, F.; Mehmood, T.; Mahmood, M.T. Infectious pathogens in volunteer and replacement blood donors in Pakistan: A ten-year experience. Int. J. Infect. Dis. 2007, 11, 407–412. [Google Scholar] [CrossRef][Green Version]
- Bednall, T.C.; Bove, L.L. Donating blood: A meta-analytic review of self-reported motivators and deterrents. Transfus. Med. Rev. 2011, 25, 317–334. [Google Scholar] [CrossRef]
- Appiah, B.; Burdine, J.N.; Aftab, A.; Asamoah-Akuoko, L.; Anum, D.A.; Kretchy, I.A.; Samman, E.W.; Appiah, P.B.; Bates, I. Determinants of intention to use mobile phone caller tunes to promote voluntary blood donation: Cross-sectional study. JMIR MHealth UHealth 2018, 6, e117. [Google Scholar] [CrossRef]
- France, J.L.; France, C.R.; Himawan, L.K. A path analysis of intention to redonate among experienced blood donors: An extension of the theory of planned behavior. Transfusion 2007, 47, 1006–1013. [Google Scholar] [CrossRef]
- France, J.L.; France, C.R.; Himawan, L.K. Re-donation intentions among experienced blood donors: Does gender make a difference? Transfus. Apher. Sci. 2008, 38, 159–166. [Google Scholar] [CrossRef]
- Lemmens, K.P.H.; Abraham, C.; Hoekstra, T.; Ruiter, R.A.C.; de Kort, W.L.A.M.; Brug, J.; Schaalma, H.P. Why don’t young people volunteer to give blood? An investigation of the correlates of donation intentions among young nondonors. Transfusion 2005, 45, 945–955. [Google Scholar] [CrossRef]
- Barboza, S.I.S.; da Costa, F.J. Social marketing of blood donation: An analysis of new donors’ predisposition. Cad. Saude Publica 2014, 30, 1463–1474. [Google Scholar] [CrossRef] [PubMed]
- Gonçalez, T.T.; Oliveira, C.d.; Carneiro-Proietti, A.B.F.; Moreno, E.C.; Miranda, C.; Larsen, N.; Wright, D.; Leão, S.; Loureiro, P.; de Almeida-Neto, C.; et al. Motivation and social capital among prospective blood donors in three large blood centers in Brazil. Transfusion 2013, 53, 1291–1301. [Google Scholar] [CrossRef]
- Ferguson, E. Mechanism of altruism approach to blood donor recruitment and retention: A review and future directions. Transfus. Med. 2015, 25, 211–226. [Google Scholar] [CrossRef] [PubMed]
- Guiddi, P.; Alfieri, S.; Marta, E.; Saturni, V. New donors, loyal donors, and regular donors: Which motivations sustain blood donation? Transfus. Apher. Sci. 2015, 52, 339–344. [Google Scholar] [CrossRef] [PubMed]
- Devine, D.; Goldman, M.; Engelfriet, C.P.; Reesink, H.W.; Hetherington, C.; Hall, S.; Steed, A.; Harding, S.; Westman, P.; Gogarty, G.; et al. Donor recruitment research. Vox Sang. 2007, 93, 250–259. [Google Scholar] [CrossRef] [PubMed]
- Ferguson, E.; Farrell, K.; Lawrence, C. Blood donation is an act of benevolence rather than altruism. Health Psychol. 2008, 27, 327–336. [Google Scholar] [CrossRef]
- Glynn, S.A.; Kleinman, S.H.; Schreiber, G.B.; Zuck, T.; McCombs, S.; Bethel, J.; Garratty, G.; Williams, A.E. Motivations to donate blood: Demographic comparisons. Transfusion 2002, 42, 216–225. [Google Scholar] [CrossRef] [PubMed]
- Glynn, S.A.; Schreiber, G.B.; Murphy, E.L.; Kessler, D.; Higgins, M.; Wright, D.J.; Mathew, S.; Tu, Y.; King, M.; Smith, J.W. Factors influencing the decision to donate: Racial and ethnic comparisons. Transfusion 2006, 46, 980–990. [Google Scholar] [CrossRef]
- Schreiber, G.B.; Schlumpf, K.S.; Glynn, S.A.; Wright, D.J.; Tu, Y.; King, M.R.; Higgins, M.J.; Kessler, D.; Gilcher, R.; Nass, C.C.; et al. Convenience, the bane of our existence, and other barriers to donating. Transfusion 2006, 46, 545–553. [Google Scholar] [CrossRef] [PubMed]
- Martín-Santana, J.D.; Reinares-Lara, E.; Romero-Domínguez, L. Modelling the role of anticipated emotions in blood donor behaviour: A cross-sectional study. J. Econ. Psychol. 2020, 81. [Google Scholar] [CrossRef]
- Martín-Santana, J.D.; Cabrera-Suárez, M.K.; Déniz-Déniz, M.d. From culture to behaviour: Donor orientation and organisational identification. J. Soc. Mark. 2020. [Google Scholar] [CrossRef]
- Martín-Santana, J.D.; Robaina-Calderín, L.; Reinares-Lara, E.; Romero-Domínguez, L. Knowing the blood nondonor to activate behaviour. Soc. Sci. 2019, 8. [Google Scholar] [CrossRef]
- Romero-Domínguez, L.; Martín-Santana, J.D.; Beerli-Palacio, A. Segmenting active blood donors according to their barriers to develop retention programs. Transfus. Med. Rev. 2019, 33, 176–182. [Google Scholar] [CrossRef]
- Martín-Santana, J.D.; Beerli-Palacio, A.; Romero-Domínguez, L. Recruitment strategies: Non-donor segmentation based on intrinsic and extrinsic stimuli. Vox Sang. 2020, 115, 47–59. [Google Scholar] [CrossRef]
- Ertz, M.; Durif, F.; Arcand, M. Collaborative consumption: Conceptual snapshot at a buzzword. J. Entrep. Educ. 2016, 19, 1–23. [Google Scholar] [CrossRef]
- Hawlitschek, F.; Teubner, T.; Gimpel, H. Consumer motives for peer-to-peer sharing. J. Clean. Prod. 2018, 204, 144–157. [Google Scholar] [CrossRef]
- Barnes, S.J.; Mattsson, J. Understanding collaborative consumption: Test of a theoretical model. Technol. Forecast. Soc. Chang. 2017, 118, 281–292. [Google Scholar] [CrossRef]
- Belk, R. You are what you can access: Sharing and collaborative consumption online. J. Bus. Res. 2014, 67, 1595–1600. [Google Scholar] [CrossRef]
- Hamari, J.; Sjöklint, M.; Ukkonen, A. The sharing economy: Why people participate in collaborative consumption. J. Assoc. Inf. Sci. Technol. 2016, 67, 2047–2059. [Google Scholar] [CrossRef]
- Gazzola, P.; Vătămănescu, E.-M.; Andrei, A.G.; Marrapodi, C. Users’ motivations to participate in the sharing economy: Moving from profits toward sustainable development. Corp. Soc. Responsib. Env. Manag. 2019, 26, 741–751. [Google Scholar] [CrossRef]
- Ertz, M.; Lecompte, A.; Durif, F. Dual roles of consumers: Towards an insight into collaborative consumption motives. Int. J. Mark. Res. 2017, 59, 725–748. [Google Scholar] [CrossRef]
- Belem, B.; Isabel, F. A phenomenological approach to the collaborative consumer. J. Consum. Mark. 2019, 36, 705–714. [Google Scholar] [CrossRef]
- Bucher, E.; Fieseler, C.; Lutz, C. What’s mine is yours (for a nominal fee)—Exploring the spectrum of utilitarian to altruistic motives for Internet-mediated sharing. Comput. Hum. Behav. 2016, 62, 316–326. [Google Scholar] [CrossRef]
- Wilhelms, M.-P.; Henkel, S.; Falk, T. To earn is not enough: A means-end analysis to uncover peer-providers’ participation motives in peer-to-peer carsharing. Technol. Forecast. Soc. Chang. 2017, 125, 38–47. [Google Scholar] [CrossRef]
- Li, H.; Wen, H. How is motivation generated in collaborative consumption: mediation effect in extrinsic and intrinsic motivation. Sustainability 2019, 11, 640. [Google Scholar] [CrossRef]
- Park, H.; Armstrong, C.M.J. Is money the biggest driver? Uncovering motives for engaging in online collaborative consumption retail models for apparel. J. Retail. Consum. Serv. 2019, 51, 42–50. [Google Scholar] [CrossRef]
- Edbring, E.G.; Lehner, M.; Mont, O. Exploring consumer attitudes to alternative models of consumption: Motivations and barriers. J. Clean. Prod. 2016, 123, 5–15. [Google Scholar] [CrossRef]
- Ter Huurne, M.; Ronteltap, A.; Corten, R.; Buskens, V. Antecedents of trust in the sharing economy: A systematic review. J. Consum. Behav. 2017, 16, 485–498. [Google Scholar] [CrossRef]
- Davis, F.D.; Bagozzi, R.P.; Warshaw, P.R. User acceptance of computer technology: A comparison of two theoretical models. Manag. Sci. 1989, 35, 982–1003. [Google Scholar] [CrossRef]
- Venkatesh, V.; Davis, F.D. Theoretical extension of the Technology Acceptance Model: Four longitudinal field studies. Manag. Sci. 2000, 46, 186–204. [Google Scholar] [CrossRef]
- Venkatesh, V.; Morris, M.G.; Davis, G.B.; Davis, F.D. User acceptance of information technology: Toward a unified view. MIS Q. 2003, 27, 425–478. Available online: http://www.jstor.org/stable/30036540 (accessed on 15 September 2020). [CrossRef]
- Benbasat, I.; Barki, H. Quo vadis TAM? J. Assoc. Inf. Syst. 2007, 8, 16. [Google Scholar] [CrossRef]
- Lee, Y.; Kozar, K.A.; Larsen, K.R.T. The technology acceptance model: Past, present, and future. Commun. Assoc. 2003, 12, 50. Available online: http://aisel.aisnet.org/cgi/viewcontent.cgi?article=3217%7B&%7Dcontext=cais (accessed on 15 September 2020). [CrossRef]
- Junghwa, S.; Byoungho, J.; Bobby, G. Consumers’ purchase intention toward foreign brand goods. Manag. Decis. 2013, 51, 434–450. [Google Scholar] [CrossRef]
- Schilke, O.; Wirtz, B.W. Consumer acceptance of service bundles: An empirical investigation in the context of broadband triple play. Inf. Manag. 2012, 49, 81–88. [Google Scholar] [CrossRef]
- Ajzen, I. The theory of planned behavior. Organ Behav. Hum. Decis. Process. 1991, 50, 179–211. [Google Scholar] [CrossRef]
- Ajzen, I. Attitudes, Personality, and Behavior; McGraw-Hill Education: London, UK, 2005. [Google Scholar]
- Ajzen, I. Constructing a TpB Questionnaire: Conceptual and Methodological Considerations. 2002. Available online: http://www.people.umass.edu/aizen/pdf/tpb.measurement.pdf (accessed on 15 September 2020).
- Ortbach, K.; Köffer, S.; Bode, M.; Niehaves, B. Individualization of Information Systems—Analyzing Antecedents of IT Consumerization Behavior. In Proceedings of the International Conference on Information Systems (ICIS 2013), Milano, Italy, 15–18 December 2013; Available online: https://www.wi.uni-muenster.de/research/publications/88668 (accessed on 15 September 2020).
- Chen, L. Applying the extended theory of planned behaviour to predict Chinese people’s non-remunerated blood donation intention and behaviour: The roles of perceived risk and trust in blood collection agencies. Asian J. Soc. Psychol. 2017, 20, 221–231. [Google Scholar] [CrossRef]
- Hawlitschek, F.; Teubner, T.; Weinhardt, C. Trust in the sharing economy. Die Unternehmung 2016, 70, 26–44. [Google Scholar] [CrossRef]
- Pavlou, P.A. Consumer acceptance of electronic commerce: Integrating trust and risk with the technology acceptance model. Int. J. Electron. Commer. 2003, 7, 101–134. [Google Scholar] [CrossRef]
- Pavlou, P.A.; Fygenson, M. Understanding and predicting electronic commerce adoption: An extension of the theory of planned behavior. MIS Q. 2006, 30, 115–143. [Google Scholar] [CrossRef]
- Gefen, D.; Benbasat, I.; Pavlou, P. A research agenda for trust in online environments. J. Manag. Inf. Syst. 2008, 24, 275–286. [Google Scholar] [CrossRef]
- Mittendorf, C. The implications of trust in the sharing economy—An empirical analysis of uber. In HICSS; HICSS Conference Office: Maui, Hawaii, USA, 2017; pp. 5837–5843. [Google Scholar] [CrossRef]
- Tussyadiah, I.P.; Pesonen, J. Drivers and barriers of peer-to-peer accommodation stay—An exploratory study with American and Finnish travellers. Curr. Issues Tour. 2018, 21, 703–720. [Google Scholar] [CrossRef]
- Möhlmann, M. Collaborative consumption: Determinants of satisfaction and the likelihood of using a sharing economy option again. J. Consum. Behav. 2015, 14, 193–207. [Google Scholar] [CrossRef]
- Teubner, T.; Hawlitschek, F. The economics of peer-to-peer online sharing. In The Rise of the Sharing Economy: Exploring the Challenges and Opportunities of Collaborative Consumption; Albinsson, P., Perera, Y.B., Eds.; Praege: Santa Barbara, CA, USA, 2018; pp. 129–156. [Google Scholar]
- Evans, R.; Ferguson, E. Defining and measuring blood donor altruism: A theoretical approach from biology, economics and psychology. Vox Sang. 2014, 106, 118–126. [Google Scholar] [CrossRef]
- Ferguson, E.; Atsma, F.; de Kort, W.; Veldhuizen, I. Exploring the pattern of blood donor beliefs in first-time, novice, and experienced donors: Differentiating reluctant altruism, pure altruism, impure altruism, and warm glow. Transfusion 2012, 52, 343–355. [Google Scholar] [CrossRef]
- Torrent-Sellens, J. Collaborative behavior and the sharing economy: Pan-European evidence for a new economic approach. In Strategy and Behaviors in the Digital Economy; IntechOpen: London, UK, 2020. [Google Scholar]
- Universitat Oberta de Catalunya, The UOC’s Code of Good Practice in Research and Innovation (CBPRI) UOC Doctoral School, Barcelona. 2014. Available online: https://research.uoc.edu/portal/_resources/CA/documents/recerca/kit_etica/Juliol_2016/kit_angles_20160712/1_Code_Good_Practices_2014_EN.pdf (accessed on 15 December 2020).
- Torrent-Sellens, J.; Díaz-Chao, Á.; Soler-Ramos, I.; Saigí-Rubió, F. Modelling and predicting ehealth usage in Europe: A multidimensional approach from an online survey of 13,000 European Union internet users. J. Med. Internet Res. 2016, 18, e188. [Google Scholar] [CrossRef]
- Torrent-Sellens, J.; Díaz-Chao, Á.; Soler-Ramos, I.; Saigí-Rubió, F. Modeling and predicting outcomes of ehealth usage by european physicians: Multidimensional approach from a survey of 9196 general practitioners. J. Med. Internet Res. 2018, 20, e279. [Google Scholar] [CrossRef]
- Eysenbach, G. Improving the quality of Web surveys: The Checklist for Reporting Results of Internet E-Surveys (CHERRIES). J. Med. Internet Res. 2004, 6, e34. [Google Scholar] [CrossRef]
- Kerlinger, F. Research of Behavior: Research Methods in Social Sciences; McGraw-Hill: New York, NY, USA, 2001. [Google Scholar]
- Muñiz, J.; Elosua, P.; Hambleton, R.K. International test commission guidelines for test translation and adaptation: Second edition, Background. Psicothema 2013, 25, 151–157. [Google Scholar] [CrossRef] [PubMed]
- Spielberger, C.D.; Hambleton, R.K.; Merenda, P.F. Adapting Educational and Psychological Tests for Cross-Cultural Assessment; Erlbaum Lawrence: London, UK, 2001. [Google Scholar]
- Roldán, J.L.; Sánchez-Franco, M.J. Variance-based structural equation modeling: Guidelines for using partial least squares in information systems research. In Research Methodologies, Innovations and Philosophies in Software Systems Engineering and Information Systems; Mora, M., Gelman, O., Steenkamp, A., Raisinghani, M., Eds.; IGI Global: Hershey, PA, USA, 2012; pp. 193–221. [Google Scholar] [CrossRef]
- Hair, J.F.; Hult, G.T.M.; Ringle, C.M.; Sarstedt, M. A Primer on Partial Least Squares Structural Equation Modeling (PLS-SEM), 2nd ed.; Sage Publications, Inc.: Thousand Oaks, CA, USA, 2017. [Google Scholar]
- Chin, W.W. The partial least squares approach to structural equation modelling. In Modern Methods for Business Research; Marcoulides, G.A., Ed.; Lawrence Erlbaum Associates: Mahwah, NJ, USA, 1998; pp. 295–358. [Google Scholar]
- Sarstedt, M.; Ringle, C.M.; Hair, J.F. Partial Least Squares Structural Equation Modeling. In Handbook of Market Research; Homburg, C., Klarmann, M., Vomberg, A., Eds.; Springer International Publishing: Cham, Switzerland, 2017; pp. 1–40. [Google Scholar]
- Wen-Lung, S.; Sarstedt, M.; Hair, J.F. Internet research using partial least squares structural equation modeling (PLS-SEM). Internet Res. 2019, 29, 398–406. [Google Scholar] [CrossRef]
- Awang, Z.; Afthanorhan, A.; Mohamad, M.; Asri, M. An evaluation of measurement model for medical tourism research: The confirmatory factor analysis approach. Int. J. Tour. Policy. 2015, 6, 29–45. [Google Scholar] [CrossRef]
- Jana, R.; Rosnita, I.I.; Marc, R.C. The agony of choice for medical tourists: A patient satisfaction index model. J. Hosp. Tour. Technol. 2018, 9, 267–279. [Google Scholar] [CrossRef]
- Hair, J.; Matthews, L.; Matthews, R.L.; Sarstedt, M. PLS-SEM or CB-SEM: Updated guidelines on which method to use. Int. J. Multivar. Data Anal. 2017, 1, 107–123. [Google Scholar] [CrossRef]
- Giles, M.; Cairns, E. Blood donation and Ajzen’s theory of planned behaviour: An examination of perceived behavioural control. Br. J. Soc. Psychol. 1995, 34, 173–188. [Google Scholar] [CrossRef]
- Giles, M.; McClenahan, C.; Cairns, E.; Mallet, J. An application of the Theory of Planned Behaviour to blood donation: The importance of self-efficacy. Health Educ. Res. 2004, 19, 380–391. [Google Scholar] [CrossRef]
- Robinson, N.G.; Masser, B.M.; White, K.M.; Hyde, M.K.; Terry, D.J. Predicting intentions to donate blood among nondonors in Australia: An extended theory of planned behavior. Transfusion 2008, 48, 2559–2567. [Google Scholar] [CrossRef] [PubMed]
- Veldhuizen, I.; Ferguson, E.; de Kort, W.; Donders, R.; Atsma, F. Exploring the dynamics of the theory of planned behavior in the context of blood donation: Does donation experience make a difference? Transfusion 2011, 51, 2425–2437. [Google Scholar] [CrossRef] [PubMed]
- McMahon, R.; Byrne, M. Predicting donation among an Irish sample of donors and nondonors: Extending the theory of planned behavior. Transfusion 2008, 48, 321–331. [Google Scholar] [CrossRef]
- France, C.R.; France, J.L.; Wissel, M.E.; Kowalsky, J.M.; Bolinger, E.M.; Huckins, J.L. Enhancing blood donation intentions using multimedia donor education materials. Transfusion 2011, 51, 1796–1801. [Google Scholar] [CrossRef] [PubMed]
- Masser, B.M.; White, K.M.; Hyde, M.K.; Terry, D.J.; Robinson, N.G. Predicting blood donation intentions and behavior among Australian blood donors: Testing an extended theory of planned behavior model. Transfusion 2009, 49, 320–329. [Google Scholar] [CrossRef] [PubMed]
- Masser, B.M.; White, K.M.; Hamilton, K.; McKimmie, B.M. Beliefs underlying blood donors’ intentions to donate during two phases of an avian influenza outbreak. Transfus. Apher. Sci. 2012, 46, 47–52. [Google Scholar] [CrossRef][Green Version]
- Charseatd, P. Role of religious beliefs in blood donation behavior among the youngster in Iran: A theory of planned behavior perspective. J. Islam. Mark. 2016, 7, 250–263. [Google Scholar] [CrossRef]
- Masser, B.M.; White, K.M.; Hyde, M.K.; Terry, D.J. The psychology of blood donation: Current research and future directions. Transfus. Med. Rev. 2008, 22, 215–233. [Google Scholar] [CrossRef]
- Rivis, A.; Sheeran, P. Descriptive norms as an additional predictor in the theory of planned behaviour: A meta-analysis. Curr. Psychol. 2003, 22, 218–233. [Google Scholar] [CrossRef]
- Armitage, C.J.; Conner, M. Social cognitive determinants of blood donation. J. Appl. Soc. Psychol. 2001, 31, 1431–1457. [Google Scholar] [CrossRef]
- Holdershaw, J.; Gendall, P.; Wright, M. Predicting blood donation behaviour: Further application of the theory of planned behaviour. J. Soc. Mark. 2011, 1, 120–132. [Google Scholar] [CrossRef]
- Centola, D.; van de Rijt, A. Choosing your network: Social preferences in an online health community. Soc. Sci. Med. 2015, 125, 19–31. [Google Scholar] [CrossRef] [PubMed]
- Masser, B.M.; White, K.M.; Hamilton, K.; McKimmie, B.M. An examination of the predictors of blood donors’ intentions to donate during two phases of an avian influenza outbreak. Transfusion 2011, 51, 548–557. [Google Scholar] [CrossRef] [PubMed]
- Renner, S.; Lindenmeier, J.; Tscheulin, D.K.; Drevs, F. Guilt appeals and prosocial behavior: An experimental analysis of the effects of anticipatory versus reactive guilt appeals on the effectiveness of blood donor appeals. J. Nonprofit Public Sect. Mark. 2013, 25, 237–255. [Google Scholar] [CrossRef]
- Kowalsky, J.M.; France, C.R.; France, J.L.; Whitehouse, E.A.; Himawan, L.K. Blood donation fears inventory: Development and validation of a measure of fear specific to the blood donation setting. Transfus. Apher. Sci. 2014, 51, 146–151. [Google Scholar] [CrossRef]
- Faqah, A.; Moiz, B.; Shahid, F.; Ibrahim, M.; Raheem, A. Assessment of blood donation intention among medical students in Pakistan—An application of theory of planned behavior. Transfus. Apher. Sci. 2015, 53, 353–359. [Google Scholar] [CrossRef] [PubMed]
- Zeelenberg, M.; van Dijk, W.W.; Manstead, A.S.R.; van der Pligt, J. On bad decisions and disconfirmed expectancies: The psychology of regret and disappointment. Cogn. Emot. 2000, 14, 521–541. [Google Scholar] [CrossRef]
- Fong, C.P.S.; Wyer, R.S. Cultural, social, and emotional determinants of decisions under uncertainty. Organ. Behav. Hum. Decis. Process. 2003, 90, 304–322. [Google Scholar] [CrossRef]
- Masser, B.; Ferguson, E.; Merz, E.M.; Williams, L. Beyond description: The predictive role of affect, memory, and context in the decision to donate or not donate blood. Transfus. Med. Hemotherapy 2020, 47, 175–185. [Google Scholar] [CrossRef]
- Ferguson, E.; France, C.R.; Abraham, C.; Ditto, B.; Sheeran, P. Improving blood donor recruitment and retention: Integrating theoretical advances from social and behavioral science research agendas. Transfusion 2007, 47, 1999–2010. [Google Scholar] [CrossRef]
| Latent Variable | Indicators | Internal Consistency Reliability | Convergent Validity | Discriminant Validity | |
|---|---|---|---|---|---|
| Composite Reliability >0.7 | Loadings >0.7 | AVE >0.5 | HTMT Confidence Interval Does Not Include 1 | ||
| TRU | TRU1 | 0.946 | 0.958 | 0.897 | Yes |
| TRU3 | 0.936 | ||||
| MLS | MLS1 | 0.917 | 0.920 | 0.847 | Yes |
| MLS3 | 0.921 | ||||
| ATT | ATT1 | 0.913 | 0.915 | 0.778 | Yes |
| ATT2 | 0.921 | ||||
| ATT3 | 0.806 | ||||
| SBN | SBN1 | 0.935 | 0.940 | 0.877 | Yes |
| SBN3 | 0.934 | ||||
| PBC | PBC1 | 0.904 | 0.908 | 0.825 | Yes |
| PBC2 | 0.909 | ||||
| ICD | ICD1 | 0.909 | 0.896 | 0.833 | Yes |
| ICD2 | 0.930 | ||||
| CBD | CBD1 | 0.945 | 0.950 | 0.896 | Yes |
| CBD2 | 0.943 | ||||
| Fornell-Larcker Criterion | |||||||
| ATT | CBD | ICD | MLS | PBC | SBN | TRU | |
| ATT | 0.882 | ||||||
| CBD | 0.320 | 0.947 | |||||
| ICD | 0.641 | 0.372 | 0.913 | ||||
| MLS | 0.665 | 0.213 | 0.576 | 0.920 | |||
| PBC | 0.607 | 0.258 | 0.545 | 0.604 | 0.908 | ||
| SBN | 0.522 | 0.371 | 0.583 | 0.485 | 0.454 | 0.937 | |
| TRU | 0.298 | 0.209 | 0.220 | 0.232 | 0.255 | 0.267 | 0.947 |
| Heterotrait-Monotrait Ratio (HTMT) | |||||||
| ATT | CBD | ICD | MLS | PBC | SBN | TRU | |
| ATT | |||||||
| CBD | 0.370 [0.265;0.481] | ||||||
| ICD | 0.779 [0.681;0.893] | 0.435 [0.338;0.529] | |||||
| MLS | 0.793 [0.701;0.913] | 0.250 [0.147;0.361] | 0.715 [0.602;0.821] | ||||
| PBC | 0.742 [0.634;0.853] | 0.308 [0.203;0.413] | 0.685 [0.581;0.792] | 0.752 [0.646;0.864] | |||
| SBN | 0.611 [0.504;0.722] | 0.425 [0.312;0.524] | 0.694 [0.578;0.802] | 0.578 [0.470;0.682] | 0.552 [0.451;0.670] | ||
| TRU | 0.342 [0.255;0.421] | 0.231 [0.128;0.314] | 0.250 [0.143;0.261] | 0.268 [0.152;0.370] | 0.302 [0.112;0.405] | 0.302 [0.100;0.407] | |
| Endogenous Variable Structural Path | Direct Effect | t-Value | Bootstrap 95% CI 1 | Cohen’s f2 |
|---|---|---|---|---|
| Attitudes (ATT) TRU ➔ ATT MLS ➔ ATT (R2 = 0.461; Q2 = 0.453) | 0.152 0.630 | 2.691 *** 12.343 *** | [0.065;0.254 [0.536;0.704] | 0.041 0.701 |
| Subjective norm (SBN) MLS ➔ SBN (R2 = 0.233; Q2 = 0.227) | 0.485 | 7.302 *** | [0.375; 0.590] | 0.308 |
| Perceived behavioural control (PBC) ATT➔ PBC (R2 = 0.367; Q2 = 0.332) | 0.607 | 13.124 *** | [0.529; 0.681] | 0.585 |
| Intention of collaborative donation (ICD) PBC ➔ ICD SBN ➔ ICD (R2 = 0.435; Q2 = 0.276) | 0.353 0.422 | 5.590 *** 7.053 *** | [0.254;0.461] [0.319;0.517] | 0.176 0.252 |
| Collaborative blood donation (CBD) ICD ➔ CBD (R2 = 0.135; Q2 = 0.039) | 0.372 | 7.561 *** | [0.289; 0.448] | 0.160 |
| Latent Variable | Indirect Effect | t-Value | Bootstrap 95% CI 1 | |
|---|---|---|---|---|
| 5% | 95% | |||
| MLS -> ATT -> PBC -> ICD -> CBD | 0.050 *** | 3.039 | 0.028 | 0.080 |
| PBC -> ICD -> CBD | 0.131 *** | 4.178 | 0.085 | 0.184 |
| ATT -> PBC -> ICD -> CBD | 0.080 *** | 3.556 | 0.048 | 0.118 |
| TRU -> ATT -> PBC -> ICD -> CBD | 0.012 ** | 2.196 | 0.005 | 0.022 |
| SBN -> ICD -> CBD | 0.157 *** | 4.763 | 0.103 | 0.212 |
| MLS -> SBN -> ICD -> CBD | 0.076 *** | 3.293 | 0.043 | 0.102 |
| MLS -> ATT -> PBC -> ICD | 0.135 *** | 4.009 | 0.084 | 0.195 |
| ATT -> PBC -> ICD | 0.214 *** | 4.820 | 0.145 | 0.287 |
| TRU -> ATT -> PBC -> ICD | 0.033 ** | 2.221 | 0.012 | 0.059 |
| MLS -> SBN -> ICD | 0.205 *** | 4.237 | 0.131 | 0.289 |
| MLS -> ATT -> PBC | 0.383 *** | 6.510 | 0.281 | 0.480 |
| TRU -> ATT -> PBC | 0.092 ** | 2.629 | 0.035 | 0.150 |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Torrent-Sellens, J.; Salazar-Concha, C.; Ficapal-Cusí, P.; Saigí-Rubió, F. Using Digital Platforms to Promote Blood Donation: Motivational and Preliminary Evidence from Latin America and Spain. Int. J. Environ. Res. Public Health 2021, 18, 4270. https://doi.org/10.3390/ijerph18084270
Torrent-Sellens J, Salazar-Concha C, Ficapal-Cusí P, Saigí-Rubió F. Using Digital Platforms to Promote Blood Donation: Motivational and Preliminary Evidence from Latin America and Spain. International Journal of Environmental Research and Public Health. 2021; 18(8):4270. https://doi.org/10.3390/ijerph18084270
Chicago/Turabian StyleTorrent-Sellens, Joan, Cristian Salazar-Concha, Pilar Ficapal-Cusí, and Francesc Saigí-Rubió. 2021. "Using Digital Platforms to Promote Blood Donation: Motivational and Preliminary Evidence from Latin America and Spain" International Journal of Environmental Research and Public Health 18, no. 8: 4270. https://doi.org/10.3390/ijerph18084270
APA StyleTorrent-Sellens, J., Salazar-Concha, C., Ficapal-Cusí, P., & Saigí-Rubió, F. (2021). Using Digital Platforms to Promote Blood Donation: Motivational and Preliminary Evidence from Latin America and Spain. International Journal of Environmental Research and Public Health, 18(8), 4270. https://doi.org/10.3390/ijerph18084270








