Childbirth Care among SARS-CoV-2 Positive Women in Italy
Abstract
1. Introduction
2. Materials and Methods
3. Results
4. Discussion
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- World Health Organization. Clinical Management of COVID-19. Interim Guidance 27 May 2020 WHO/2019-nCoV/Clinical/2020.5; World Health Organization: Geneva, Switzerland, 2020; Available online: https://apps.who.int/iris/bitstream/handle/10665/332196/WHO-2019-nCoV-clinical-2020.5-eng.pdf?sequence=1&isAllowed=y (accessed on 11 April 2021).
- UNICEF UK Baby-Friendly Hospital Initiative. Infant Feeding during the COVID-19 Outbreak. UNICEF UK. Published 2020. Updated 10 July 2020. Available online: https://www.unicef.org.uk/babyfriendly/wp-content/uploads/sites/2/2020/04/Unicef-UK-Baby-Friendly-Initiative-statement-on-infant-feeding-during-the-Covid-19-outbreak.pdf (accessed on 23 March 2021).
- Royal College of Obstetricians and Gynaecologists, Royal College of Midwives, Royal College of Paediatrics and Child Health, Public Health England and Health Protection Scotland. Coronavirus (COVID-19) Infection in Pregnancy. Information for Healthcare Professionals. [Version 13: Published Friday 19 February 2021]. 2020. Available online: https://www.rcog.org.uk/globalassets/documents/guidelines/2021-02-19-coronavirus-covid-19-infection-in-pregnancy-v13.pdf (accessed on 11 April 2021).
- Narang, K.; Ibirogba, E.R.; Elrefaei, A.; Trad, A.T.A.; Theiler, R.; Nomura, R.; Picone, O.; Kilby, M.; Escuriet, R.; Suy, A.; et al. SARS-CoV-2 in Pregnancy: A Comprehensive Summary of Current Guidelines. J. Clin. Med. 2020, 9, 1521. [Google Scholar] [CrossRef] [PubMed]
- Molgora, S.; Accordini, M. Motherhood in the Time of Coronavirus: The Impact of the Pandemic Emergency on Expectant and Postpartum Women’s Psychological Well-Being. Front. Psychol. 2020, 11, 567155. [Google Scholar] [CrossRef] [PubMed]
- Maraschini, A.; Corsi, E.; Salvatore, M.A.; Donati, S.; ItOSS COVID-19 Working Group. Coronavirus and birth in Italy: Results of a national population-based cohort study. Ann. Ist. Super. Sanita. 2020, 56, 378–389. [Google Scholar] [CrossRef] [PubMed]
- Corsi, E.; Maraschini, A.; Perrone, E.; Salvatore, M.A.; D’Aloja, P.; Donati, S.; Gruppo di lavoro ItOSS COVID-19. La preparedness dell’Italian obstetric surveillance system in occasione della pandemia da SARS-CoV-2: Aspetti metodologici di uno studio di popolazione [The preparedness of the Italian obstetric surveillance system in the response to the emergency of the SARS-CoV-2 pandemic: Methodological aspects of a population-based study]. Epidemiol. Prev. 2020, 44, 81–87. [Google Scholar] [CrossRef] [PubMed]
- Donati, S.; Maraschini, A.; Lega, I.; D’Aloja, P.; Buoncristiano, M.; Manno, V.; Regional Maternal Mortality Working Group. Maternal mortality in Italy: Results and perspectives of record-linkage analysis. Acta. Obstet. Gynecol Scand. 2018, 97, 1317–1324. [Google Scholar] [CrossRef] [PubMed]
- Maraschini, A.; Lega, I.; D’Aloja, P.; Buoncristiano, M.; Dell’Oro, S.; Donati, S.; Regional Obstetric Surveillance System Working Group. Women undergoing peripartum hysterectomy due to obstetric hemorrhage: A prospective population-based study. Acta. Obstet. Gynecol. Scand. 2020, 99, 274–282. [Google Scholar] [CrossRef] [PubMed]
- Campi, R.; Cartabia, M.; Miglio, D.; Bonati, M. Certificato di Assistenza al Parto (CedAP)—Regione Lombardia—Analisi dell’evento nascita anno 2017 Laboratorio per la Salute Materno Infantile, Dipartimento di Salute Pubblica, IRCCS—Istituto di Ricerche Farmacologiche Mario Negri Milano: Lombardia Region 2019 [The certificate of delivery care (CeDAP)—Lombardy Region—Year 2017]. Available online: www.dati.lombardia.it/dataset/Rapporto-Cedap/v74r-mqr5 (accessed on 23 March 2021).
- Perrone, E.; Formisano, D.; Gargano, G.; Battaglia, S.; Di Mario, S.; Basevi, V. La nascita in Emilia-Romagna—17° Rapporto sui dati del Certificato di Assistenza al Parto (CeDAP)—Anno 2019 [Birth in Emilia-Romagna—Report on the Data of the Certificate of Delivery Care (CeDAP)—Year 2019]. Available online: https://salute.regione.emilia-romagna.it/siseps/sanita/cedap/documentazione/pubblicazioni (accessed on 11 April 2021).
- Betran, A.P.; Torloni, M.R.; Zhang, J.; Ye, J.; Mikolajczyk, R.; Deneux-Tharaux, C.; Oladapo, O.T.; Souza, J.P.; Tunçalp, Ö.; Vogel, J.P.; et al. What is the optimal rate of caesarean section at population level? A systematic review of ecologic studies. Reprod. Health 2015, 12, 57. [Google Scholar] [CrossRef] [PubMed]
- MacFarlane, A.J.; Blondel, B.; Mohangoo, A.D.; Cuttini, M.; Nijhuis, J.; Novak, Z.; Ólafsdóttir, H.S.; Zeitlin, J.; Euro-Peristat Scientific Committee. Wide differences in mode of delivery within Europe: Risk-stratified analyses of aggregated routine data from the Euro-Peristat study. BJOG 2016, 123, 559–568. [Google Scholar] [CrossRef] [PubMed]
- Ministero della Salute-Direzione Generale della digitalizzazione, del sistema informativo sanitario e della Statistica—Ufficio di Statistica. Certificato di assistenza al parto (CeDAP). Analisi dell’evento nascita—2018 [Certificates of delivery care (CeDAP)—Year 2017]. Available online: http://www.salute.gov.it/imgs/C_17_pubblicazioni_3034_allegato.pdf (accessed on 11 April 2021).
- Yan, J.; Guo, J.; Fan, C.; Juan, J.; Yu, X.; Li, J.; Feng, L.; Li, C.; Chen, H.; Qiao, Y.; et al. Coronavirus disease 2019 in pregnant women: A report based on 116 cases. Am. J. Obstet. Gynecol. 2020, 223, 111.e1–111.e14. [Google Scholar] [CrossRef] [PubMed]
- Knight, M.; Bunch, K.; Vousden, N.; Morris, E.; Simpson, N.; Gale, C.; O’Brien, P.; Quigley, M.; Brocklehurst, P.; Kurinczuk, J.J. Characteristics and outcomes of pregnant women admitted to hospital with confirmed SARS-CoV-2 infection in the UK: National population based cohort study. BMJ 2020, 369, m2107. [Google Scholar] [CrossRef]
- Allotey, J.; Stallings, E.; Bonet, M.; Yap, M.; Chatterjee, S.; Kew, T.; Debenham, L.; Llavall, A.C.; Dixit, A.; Zhou, D.; et al. Clinical manifestations, risk factors, and maternal and perinatal outcomes of coronavirus disease 2019 in pregnancy: Living systematic review and meta-analysis. BMJ 2020, 370, m3320. [Google Scholar] [CrossRef]
- NHS—UK Maternity Services Monthly Statistics January 2019, Experimental Statistics. Available online: https://digital.nhs.uk/data-and-information/publications/statistical/maternity-services-monthly-statistics/january-2019 (accessed on 11 April 2021).
- Bohren, M.A.; Hofmeyr, G.J.; Sakala, C.; Fukuzawa, R.K.; Cuthbert, A. Continuous support for women during childbirth. Cochrane Database Syst. Rev. 2017, 7, CD003766. [Google Scholar] [CrossRef]
- Fumagalli, S.; Ornaghi, S.; Borrelli, S.; Vergani, P.; Nespoli, A. The experiences of childbearing women who tested positive to COVID-19 during the pandemic in northern Italy. Women Birth 2021. [Google Scholar] [CrossRef] [PubMed]
- Greene, N.H.; Kilpatrick, S.J.; Wong, M.S.; Ozimek, J.A.; Naqvi, M. Impact of labor and delivery unit policy modifications on maternal and neonatal outcomes during the coronavirus disease 2019 pandemic. Am. J. Obstet. Gynecol. MFM 2020, 2, 100234. [Google Scholar] [CrossRef]
- Young, S.L.; Mbuya, M.N.; Chantry, C.J.; Geubbels, E.P.; Israel-Ballard, K.; Cohan, D.; Vosti, S.A.; Latham, M.C.; Latham, M.C. Current knowledge and future research on infant feeding in the context of HIV: Basic, clinical, behavioral, and programmatic perspectives. Adv. Nutr. 2011, 2, 225–243. [Google Scholar] [CrossRef] [PubMed]
- Antiel, R.M. Oedipus and the Coronavirus Pandemic. JAMA 2020, 323, 2231–2232. [Google Scholar] [CrossRef] [PubMed]
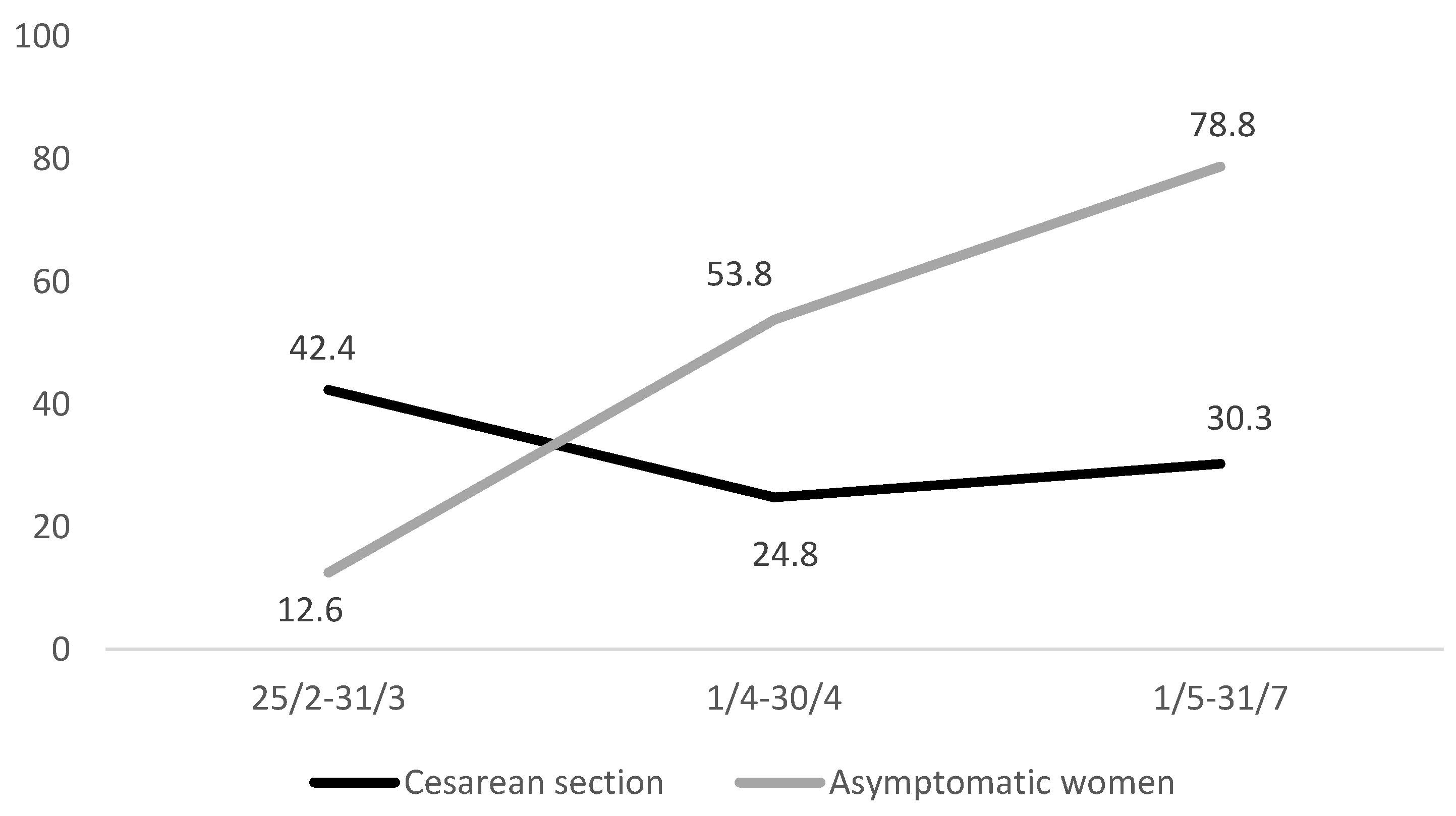
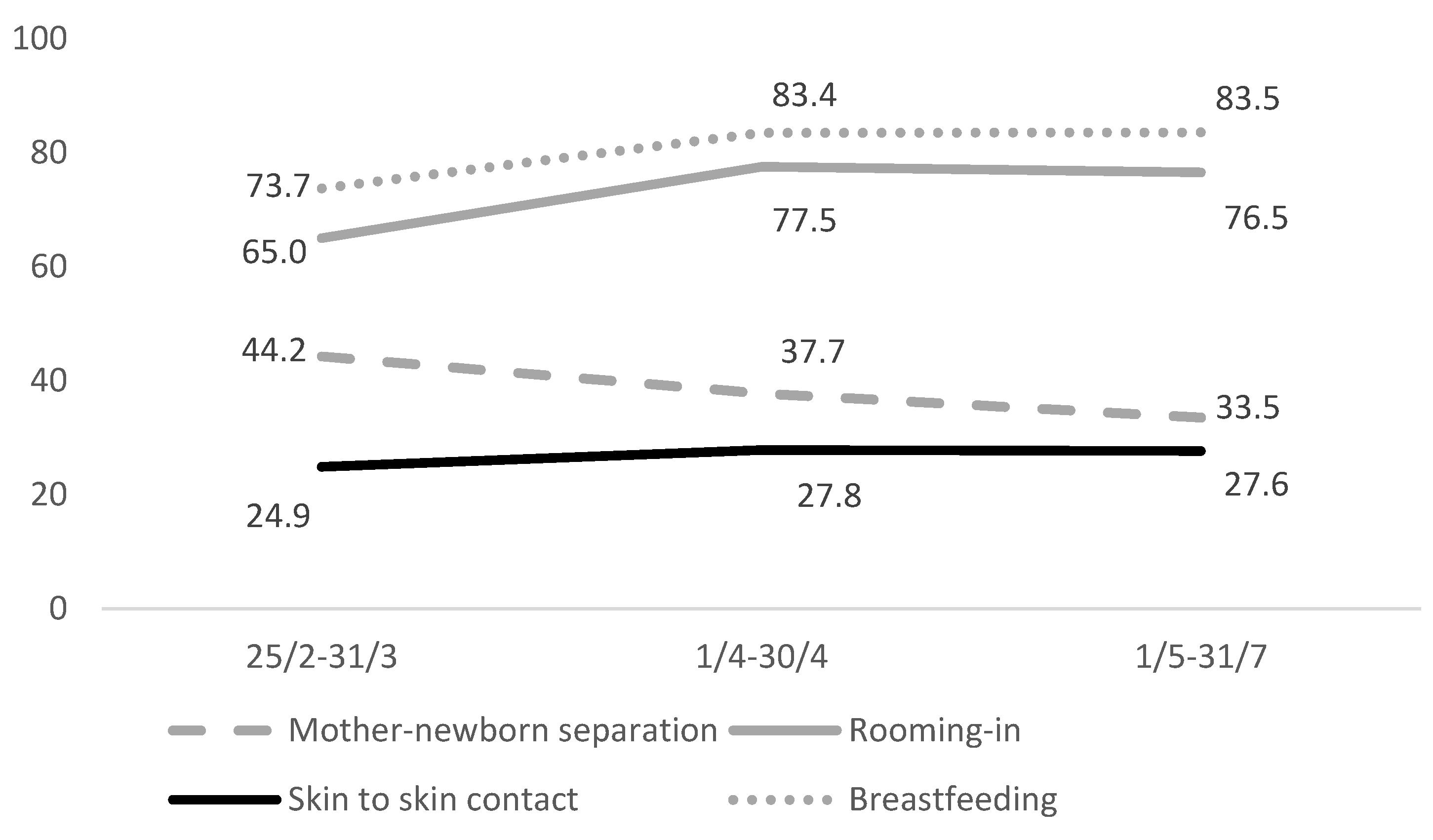
| Characteristics | n | % |
|---|---|---|
| Maternal age (3 missing) | ||
| <30 | 169 | 32.4 |
| 30–34 | 180 | 34.5 |
| ≥35 | 173 | 33.1 |
| Citizenship | ||
| Not Italian | 125 | 23.8 |
| Italian | 400 | 76.2 |
| Country of birth | ||
| Italy and Western Europe | 368 | 70.1 |
| Eastern Europe | 34 | 6.5 |
| Africa | 49 | 9.3 |
| South/Central America | 37 | 7 |
| Asia | 37 | 7 |
| Parity (11 missing) | ||
| Nulliparae | 187 | 36.4 |
| Multiparae | 327 | 63.6 |
| Multiple pregnancies | ||
| No | 508 | 96.8 |
| Yes | 17 | 3.2 |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Donati, S.; Corsi, E.; Salvatore, M.A.; Maraschini, A.; Bonassisa, S.; Casucci, P.; Cataneo, I.; Cetin, I.; D’Aloja, P.; Dardanoni, G.; et al. Childbirth Care among SARS-CoV-2 Positive Women in Italy. Int. J. Environ. Res. Public Health 2021, 18, 4244. https://doi.org/10.3390/ijerph18084244
Donati S, Corsi E, Salvatore MA, Maraschini A, Bonassisa S, Casucci P, Cataneo I, Cetin I, D’Aloja P, Dardanoni G, et al. Childbirth Care among SARS-CoV-2 Positive Women in Italy. International Journal of Environmental Research and Public Health. 2021; 18(8):4244. https://doi.org/10.3390/ijerph18084244
Chicago/Turabian StyleDonati, Serena, Edoardo Corsi, Michele Antonio Salvatore, Alice Maraschini, Silvia Bonassisa, Paola Casucci, Ilaria Cataneo, Irene Cetin, Paola D’Aloja, Gabriella Dardanoni, and et al. 2021. "Childbirth Care among SARS-CoV-2 Positive Women in Italy" International Journal of Environmental Research and Public Health 18, no. 8: 4244. https://doi.org/10.3390/ijerph18084244
APA StyleDonati, S., Corsi, E., Salvatore, M. A., Maraschini, A., Bonassisa, S., Casucci, P., Cataneo, I., Cetin, I., D’Aloja, P., Dardanoni, G., De Ambrosi, E., Ferrazzi, E., Fieni, S., Franchi, M. P., Gargantini, G., Iurlaro, E., Leo, L., Liberati, M., Livio, S., ... Zullino, S. (2021). Childbirth Care among SARS-CoV-2 Positive Women in Italy. International Journal of Environmental Research and Public Health, 18(8), 4244. https://doi.org/10.3390/ijerph18084244







