Downstream Complications and Healthcare Expenditure after Invasive Procedures for Lung Lesions in Taiwan
Abstract
1. Introduction
2. Methods
2.1. Data Source
2.2. Study Cohort Undergoing Invasive Procedures after Non-Contrast Chest CT
2.3. Matched Cohort Randomly Selected from the General Population
2.4. Downstream Complications and Healthcare Expenditure
2.5. Statistical Analysis
3. Results
3.1. Study and Matched Cohorts
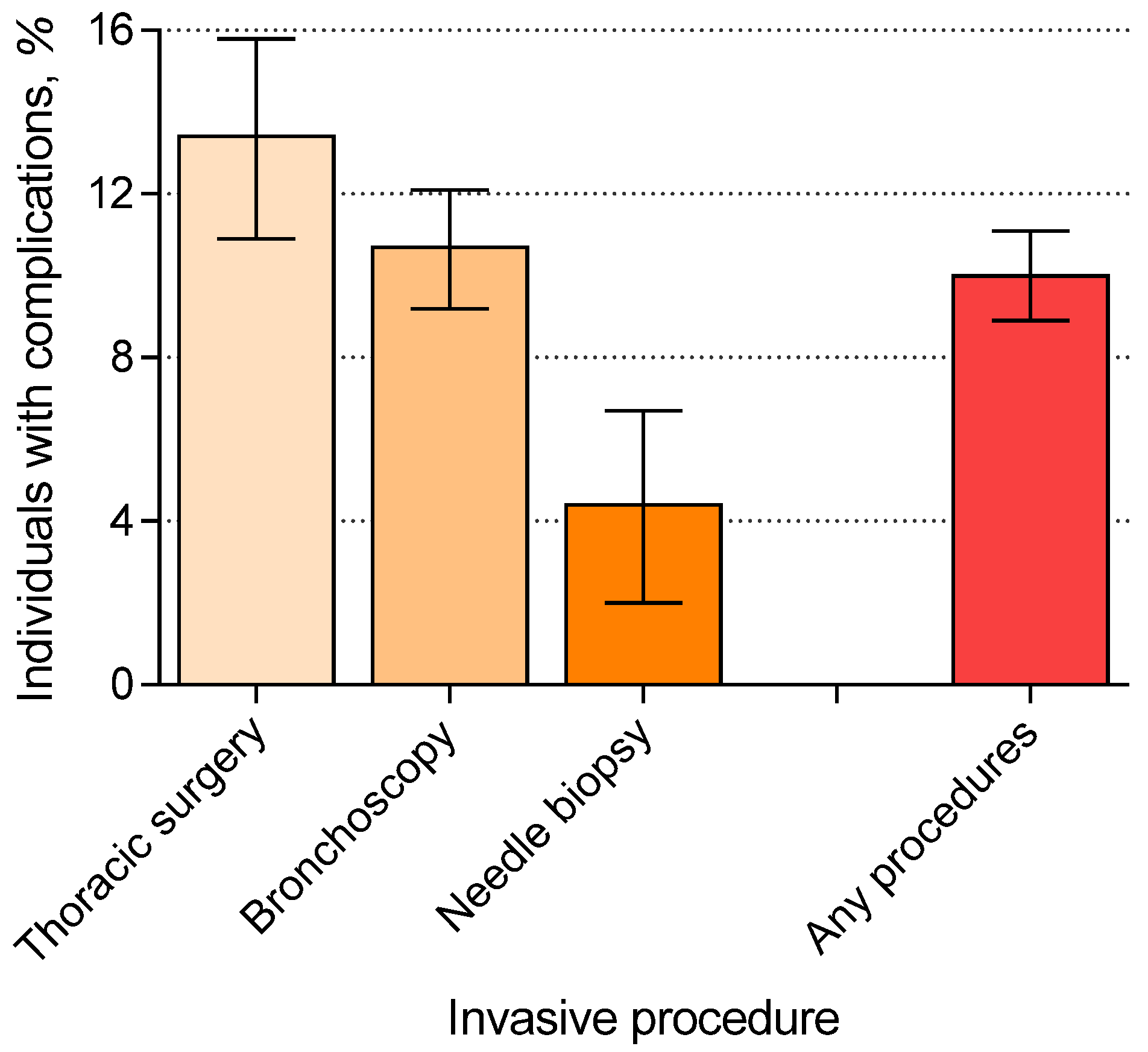
3.2. Incremental Complication Rates
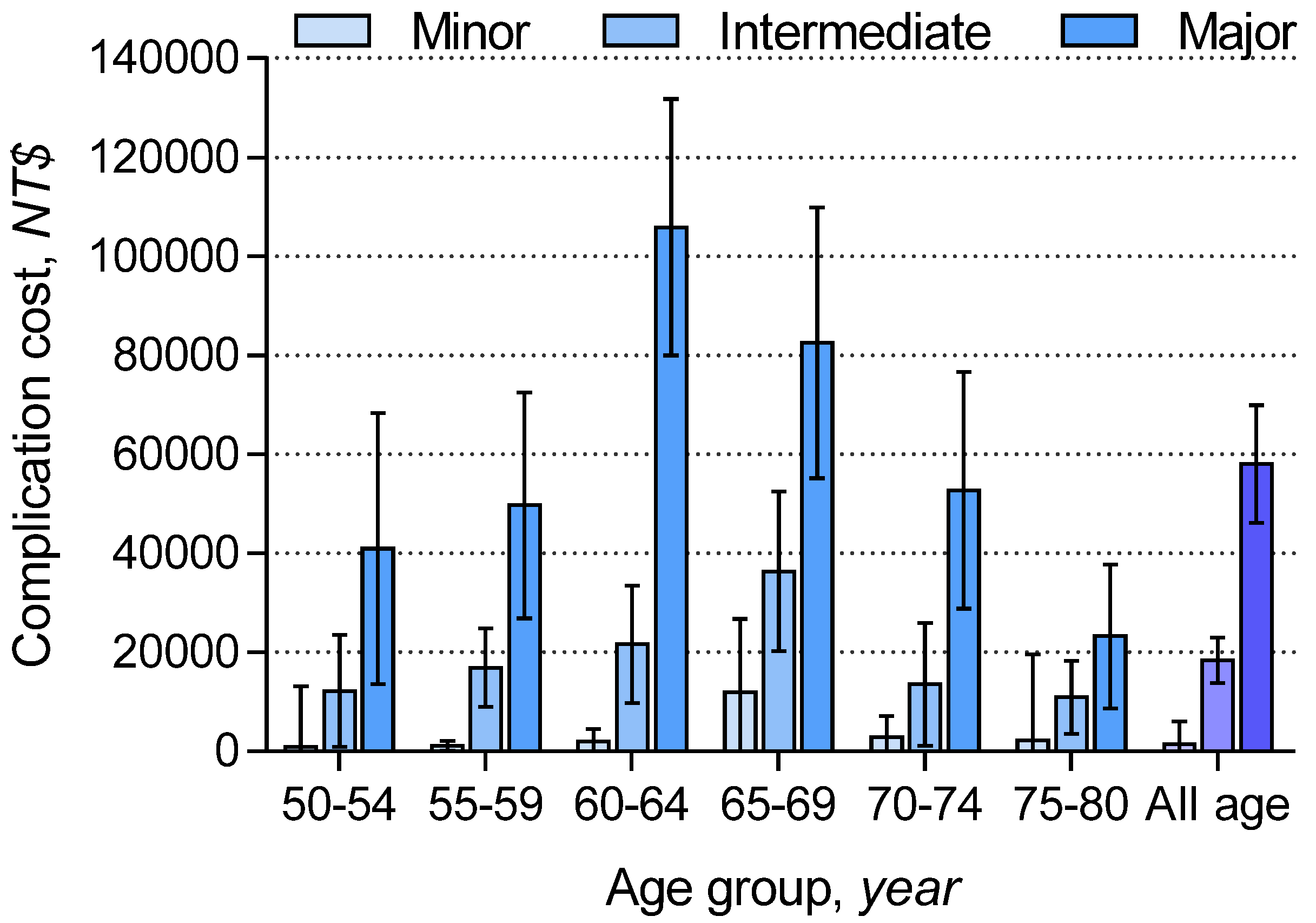
3.3. Incremental Costs Attributable To Complications
4. Discussion
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Aberle, D.R.; Adams, A.M.; Berg, C.D.; Black, W.C.; Clapp, J.D.; Fagerstrom, R.M.; Gareen, I.F.; Gatsonis, C.; Marcus, P.M.; Sicks, J.D. Reduced lung-cancer mortality with low-dose computed tomographic screening. N. Engl. J. Med. 2011, 365, 395–409. [Google Scholar]
- de Koning, H.J.; van der Aalst, C.M.; de Jong, P.A.; Scholten, E.T.; Nackaerts, K.; Heuvelmans, M.A.; Lammers, J.J.; Weenink, C.; Yousaf-Khan, U.; Horeweg, N.; et al. Reduced lung-cancer mortality with volume CT screening in a randomized trial. N. Engl. J. Med. 2020, 382, 503–513. [Google Scholar] [CrossRef] [PubMed]
- Huo, J.; Shen, C.; Volk, R.J.; Shih, Y.T. Use of CT and chest radiography for lung cancer screening before and after publication of screening guidelines: Intended and unintended uptake. JAMA Intern. Med. 2017, 177, 439–441. [Google Scholar] [CrossRef] [PubMed]
- Yang, S.C.; Gross, C.P.; Wang, J.D.; Wang, S.Y. Trend of non-contrast chest computed tomography use in the lung cancer screening era: SEER-Medicare 2008–2016. J. Gen. Intern. Med. 2021, in press. [Google Scholar] [CrossRef]
- Pinsky, P.F.; Gierada, D.S.; Hocking, W.; Patz, E.F., Jr.; Kramer, B.S. National Lung Screening Trial findings by age: Medicare-eligible versus under-65 population. Ann. Intern. Med. 2014, 161, 627–633. [Google Scholar] [CrossRef] [PubMed]
- Chen, C.K.; Chang, H.T.; Chen, Y.C.; Chiang, S.C.; Chou, H.P.; Chen, T.J. Utilization and safety of percutaneous lung biopsy: A 10-year nationwide population-based study. Int. J. Environ. Res. Public Health 2019, 16, 1316. [Google Scholar] [CrossRef] [PubMed]
- Yang, P. MS16.04 National Lung Screening Program in Taiwan. J. Thorac. Oncol. 2018, 13, S274–S275. [Google Scholar] [CrossRef]
- Huo, J.; Xu, Y.; Sheu, T.; Volk, R.J.; Shih, Y.T. Complication rates and downstream medical costs associated with invasive diagnostic procedures for lung abnormalities in the community setting. JAMA Intern. Med. 2019, 179, 324–332. [Google Scholar] [CrossRef] [PubMed]
- Wu, T.Y.; Majeed, A.; Kuo, K.N. An overview of the healthcare system in Taiwan. London J. Prim. Care 2010, 3, 115–119. [Google Scholar] [CrossRef]
- Moyer, V.A. Screening for lung cancer: U.S. Preventive Services Task Force recommendation statement. Ann. Intern. Med. 2014, 160, 330–338. [Google Scholar] [CrossRef] [PubMed]
- Li, C.H.; Li, C.C.; Lu, C.L.; Wu, J.S.; Ku, L.E.; Li, C.Y. Urban-rural disparity in lower extremities amputation in patients with diabetes after nearly two decades of universal health insurance in Taiwan. BMC Public Health 2020, 20, 212. [Google Scholar] [CrossRef]
- Charlson, M.E.; Pompei, P.; Ales, K.L.; MacKenzie, C.R. A new method of classifying prognostic comorbidity in longitudinal studies: Development and validation. J. Chronic. Dis. 1987, 40, 373–383. [Google Scholar] [CrossRef]
- Chu, Y.T.; Ng, Y.Y.; Wu, S.C. Comparison of different comorbidity measures for use with administrative data in predicting short- and long-term mortality. BMC Health Serv. Res. 2010, 10, 140. [Google Scholar] [CrossRef] [PubMed]
- Yabroff, K.R.; Lamont, E.B.; Mariotto, A.; Warren, J.L.; Topor, M.; Meekins, A.; Brown, M.L. Cost of care for elderly cancer patients in the United States. J. Natl. Cancer Inst. 2008, 100, 630–641. [Google Scholar] [CrossRef] [PubMed]
- Geller, A.D.; Zheng, H.; Mathisen, D.J.; Wright, C.D.; Lanuti, M. Relative incremental costs of complications of lobectomy for stage I non-small cell lung cancer. J. Thorac. Cardiovasc. Surg. 2018, 155, 1804–1811. [Google Scholar] [CrossRef]
- Yang, S.C.; Lai, W.W.; Lin, C.C.; Su, W.C.; Ku, L.J.; Hwang, J.S.; Wang, J.D. Cost-effectiveness of implementing computed tomography screening for lung cancer in Taiwan. Lung Cancer 2017, 108, 183–191. [Google Scholar] [CrossRef]
- Yang, S.C.; Lai, W.W.; Su, W.C.; Wu, S.Y.; Chen, H.H.; Wu, Y.L.; Hung, M.C.; Wang, J.D. Estimating the lifelong health impact and financial burdens of different types of lung cancer. BMC Cancer 2013, 13, 579. [Google Scholar] [CrossRef] [PubMed]
- Iaccarino, J.M.; Silvestri, G.A.; Wiener, R.S. Patient-level trajectories and outcomes after low-dose CT screening in the National Lung Screening Trial. Chest 2019, 156, 965–971. [Google Scholar] [CrossRef]
- Wiener, R.S.; Schwartz, L.M.; Woloshin, S.; Welch, H.G. Population-based risk for complications after transthoracic needle lung biopsy of a pulmonary nodule: An analysis of discharge records. Ann. Intern. Med. 2011, 155, 137–144. [Google Scholar] [CrossRef]
- Yu, C.J. Letter from Taiwan. Respirology 2018, 23, 535–537. [Google Scholar] [CrossRef]
- Yang, S.C.; Kuo, C.W.; Lai, W.W.; Lin, C.C.; Su, W.C.; Chang, S.M.; Wang, J.D. Dynamic changes of health utility in lung cancer patients receiving different treatments: A 7-year follow-up. J. Thorac. Oncol. 2019, 14, 1892–1900. [Google Scholar] [CrossRef] [PubMed]
| Study Cohort (n = 5805) | Without Procedures a (n = 7,849,430) | |||||||
|---|---|---|---|---|---|---|---|---|
| Surgery (n = 1263) | Bronchoscopy (n = 3417) | Needle Biopsy (n = 1125) | ||||||
| n | % | n | % | n | % | n | % | |
| Calendar year | ||||||||
| 2014 | 380 | 30.1 | 1072 | 31.4 | 357 | 31.7 | 7,051,719 | 89.8 |
| 2015 | 444 | 35.2 | 1129 | 33.0 | 346 | 30.8 | 406,912 | 5.2 |
| 2016 | 439 | 34.8 | 1216 | 35.6 | 422 | 37.5 | 390,799 | 5.0 |
| Age, years | ||||||||
| 50–54 | 277 | 21.9 | 482 | 14.1 | 140 | 12.4 | 2,581,833 | 32.9 |
| 55–59 | 264 | 20.9 | 528 | 15.4 | 174 | 15.5 | 1,688,033 | 21.5 |
| 60–64 | 257 | 20.4 | 625 | 18.3 | 191 | 17.0 | 1,423,362 | 18.1 |
| 65–69 | 200 | 15.8 | 518 | 15.2 | 212 | 18.8 | 850,932 | 10.8 |
| 70–74 | 143 | 11.3 | 584 | 17.1 | 207 | 18.4 | 684,706 | 8.7 |
| 75–80 | 122 | 9.7 | 680 | 19.9 | 201 | 17.9 | 620,564 | 7.9 |
| Gender | ||||||||
| Male | 791 | 62.6 | 2059 | 60.3 | 665 | 59.1 | 3,787,622 | 48.3 |
| Female | 472 | 37.4 | 1358 | 39.7 | 460 | 40.9 | 4,061,808 | 51.8 |
| Residence | ||||||||
| Urban | 778 | 61.6 | 1998 | 58.5 | 669 | 59.5 | 4,825,156 | 61.5 |
| Sub-urban | 370 | 29.3 | 961 | 28.1 | 310 | 27.5 | 2,293,026 | 29.2 |
| Rural | 115 | 9.1 | 458 | 13.4 | 146 | 13.0 | 731,239 | 9.3 |
| Unknown | 0 | 0 | 0 | 0 | 0 | 0 | 9 | 0.0 |
| CCI score | ||||||||
| 0 | 405 | 32.1 | 928 | 27.2 | 252 | 22.4 | 5,100,874 | 65.0 |
| 1 | 295 | 23.3 | 828 | 24.2 | 208 | 18.5 | 1,472,067 | 18.8 |
| 2 | 202 | 16.0 | 596 | 17.4 | 204 | 18.1 | 683,080 | 8.7 |
| ≥3 | 361 | 28.6 | 1065 | 31.2 | 461 | 41.0 | 593,409 | 7.6 |
| Past one-year healthcare expenditure b | ||||||||
| 1st quintile | 89 | 7.0 | 189 | 5.5 | 43 | 3.8 | 1,584,424 | 20.2 |
| 2nd quintile | 92 | 7.3 | 222 | 6.5 | 66 | 5.9 | 1,583,674 | 20.2 |
| 3rd quintile | 145 | 11.5 | 401 | 11.7 | 88 | 7.8 | 1,581,260 | 20.1 |
| 4th quintile | 269 | 21.3 | 683 | 20.0 | 188 | 16.7 | 1,575,448 | 20.1 |
| 5th quintile | 668 | 52.9 | 1922 | 56.3 | 740 | 65.8 | 1,524,624 | 19.4 |
| Study Cohort (n = 5805) | Matched Cohort (n = 58,050) | |||
|---|---|---|---|---|
| n | % | n | % | |
| Calendar year | ||||
| 2014 | 1809 | 31.2 | 18,090 | 31.2 |
| 2015 | 1919 | 33.1 | 19,190 | 33.1 |
| 2016 | 2077 | 35.8 | 20,770 | 35.8 |
| Age, years | ||||
| 50–54 | 899 | 15.5 | 8990 | 15.5 |
| 55–59 | 966 | 16.6 | 9660 | 16.6 |
| 60–64 | 1073 | 18.5 | 10,730 | 18.5 |
| 65–69 | 930 | 16.0 | 9300 | 16.0 |
| 70–74 | 934 | 16.1 | 9340 | 16.1 |
| 75–80 | 1003 | 17.3 | 10,030 | 17.3 |
| Gender | ||||
| Male | 3515 | 60.6 | 35,150 | 60.6 |
| Female | 2290 | 39.4 | 22,900 | 39.4 |
| Residence | ||||
| Urban | 3445 | 59.3 | 34,450 | 59.3 |
| Sub-urban | 1641 | 28.3 | 16,410 | 28.3 |
| Rural | 719 | 12.4 | 7190 | 12.4 |
| CCI score | ||||
| 0 | 1585 | 27.3 | 15,850 | 27.3 |
| 1 | 1331 | 22.9 | 13,310 | 22.9 |
| 2 | 1002 | 17.3 | 10,020 | 17.3 |
| ≥3 | 1887 | 32.5 | 18,870 | 32.5 |
| Past one-year healthcare expenditure a | ||||
| 1st quintile | 321 | 5.5 | 3210 | 5.5 |
| 2nd quintile | 380 | 6.5 | 3800 | 6.5 |
| 3rd quintile | 634 | 10.9 | 6340 | 10.9 |
| 4th quintile | 1140 | 19.6 | 11,400 | 19.6 |
| 5th quintile | 3330 | 57.4 | 33,300 | 57.4 |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Yang, S.-C.; Lai, C.-H.; Kuo, C.-W.; Lin, C.-C.; Lai, W.-W.; Wang, J.-D. Downstream Complications and Healthcare Expenditure after Invasive Procedures for Lung Lesions in Taiwan. Int. J. Environ. Res. Public Health 2021, 18, 4040. https://doi.org/10.3390/ijerph18084040
Yang S-C, Lai C-H, Kuo C-W, Lin C-C, Lai W-W, Wang J-D. Downstream Complications and Healthcare Expenditure after Invasive Procedures for Lung Lesions in Taiwan. International Journal of Environmental Research and Public Health. 2021; 18(8):4040. https://doi.org/10.3390/ijerph18084040
Chicago/Turabian StyleYang, Szu-Chun, Ching-Han Lai, Chin-Wei Kuo, Chien-Chung Lin, Wu-Wei Lai, and Jung-Der Wang. 2021. "Downstream Complications and Healthcare Expenditure after Invasive Procedures for Lung Lesions in Taiwan" International Journal of Environmental Research and Public Health 18, no. 8: 4040. https://doi.org/10.3390/ijerph18084040
APA StyleYang, S.-C., Lai, C.-H., Kuo, C.-W., Lin, C.-C., Lai, W.-W., & Wang, J.-D. (2021). Downstream Complications and Healthcare Expenditure after Invasive Procedures for Lung Lesions in Taiwan. International Journal of Environmental Research and Public Health, 18(8), 4040. https://doi.org/10.3390/ijerph18084040






