A Web Survey to Evaluate the Thermal Stress Associated with Personal Protective Equipment among Healthcare Workers during the COVID-19 Pandemic in Italy †
Abstract
1. Introduction
2. Materials and Methods
2.1. Survey Development
- -
- demographic data and characteristics of the worker (question from 1 to 8)
- -
- relevant work information (9–13)
- -
- heat-exposure-related questions and information about PPE’ usage at work (14–20)
- -
- worker’s adaptation to heat stress and behavioral with PPE (21-27)
- -
- worker’s knowledge about thermal stress and attitudes towards the PPE’s use (28–46)
2.2. Survey Administration
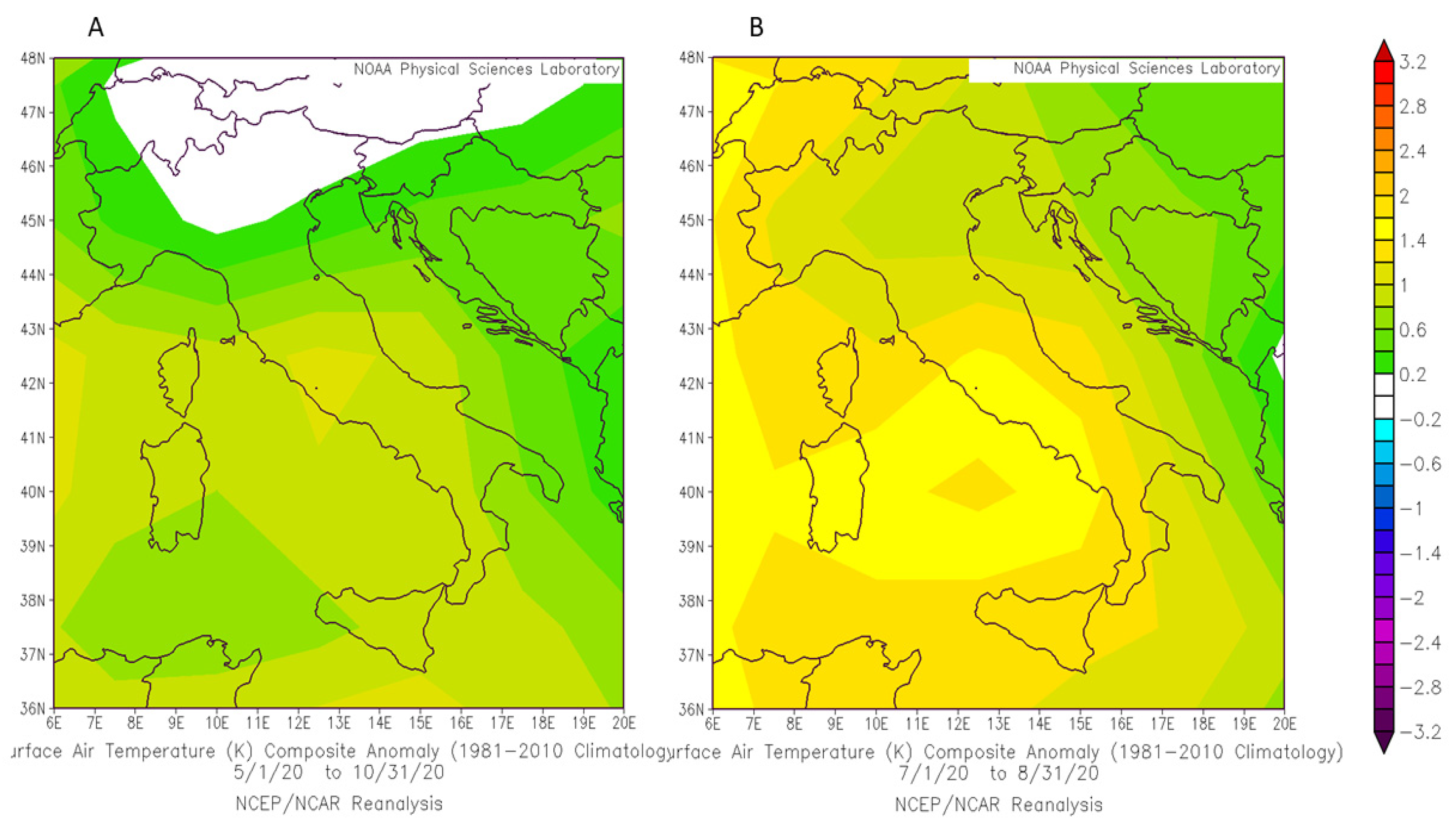
2.3. Study Area and Climatic Characteristics
2.4. Data Analysis
3. Results
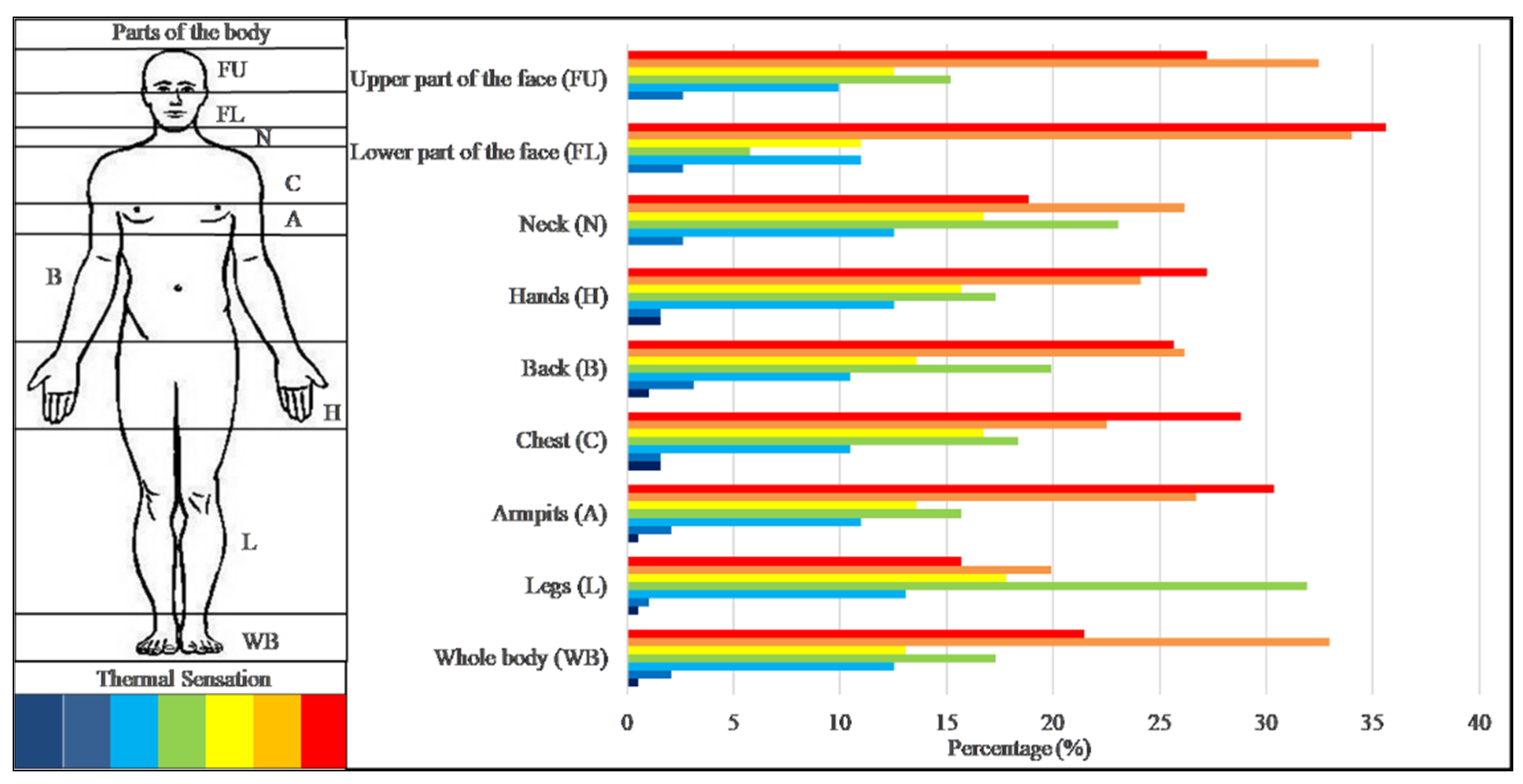
3.1. Descriptive Analysis
3.2. Principal Component Analysis
3.3. Differences between HCW Groups
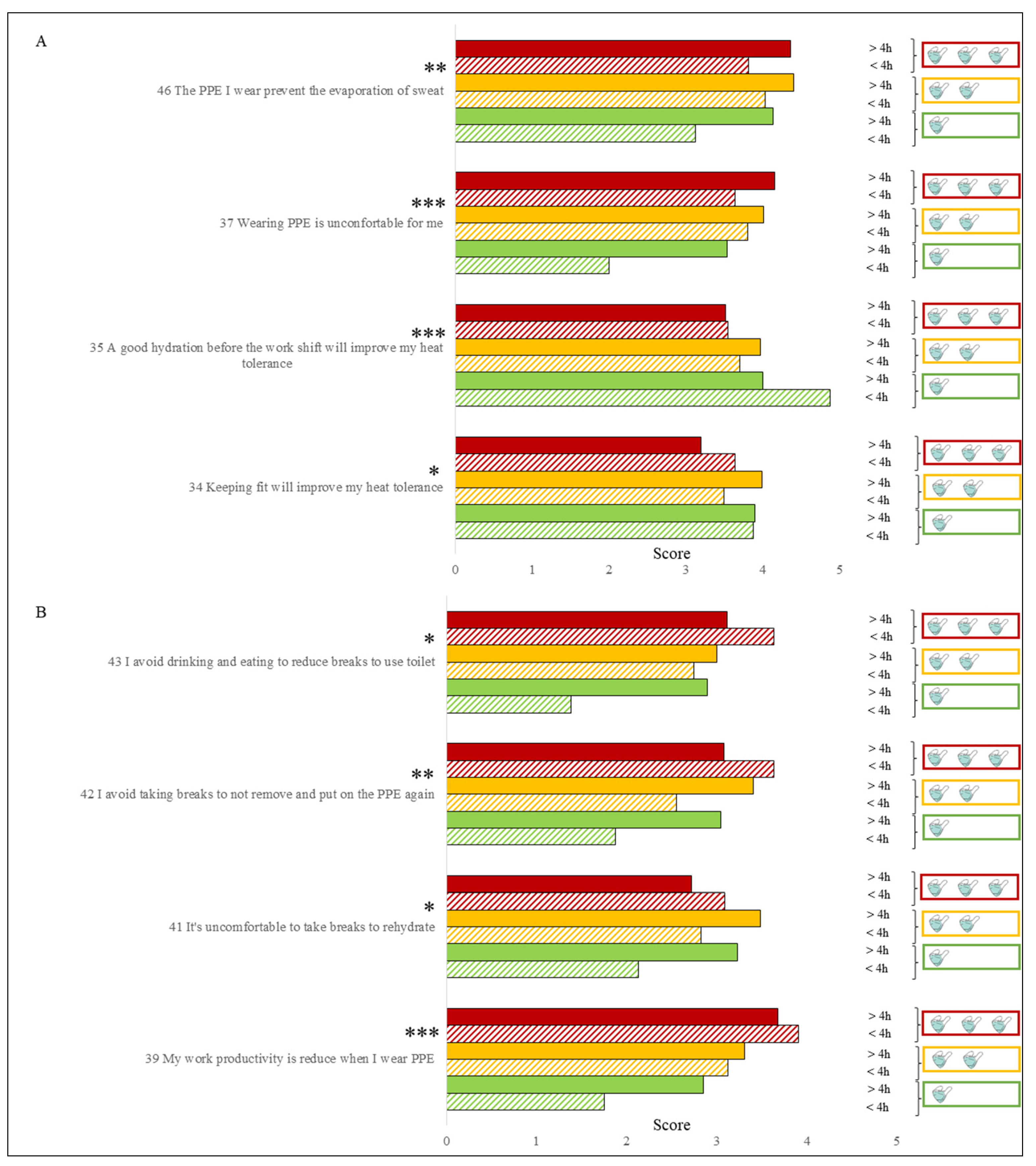
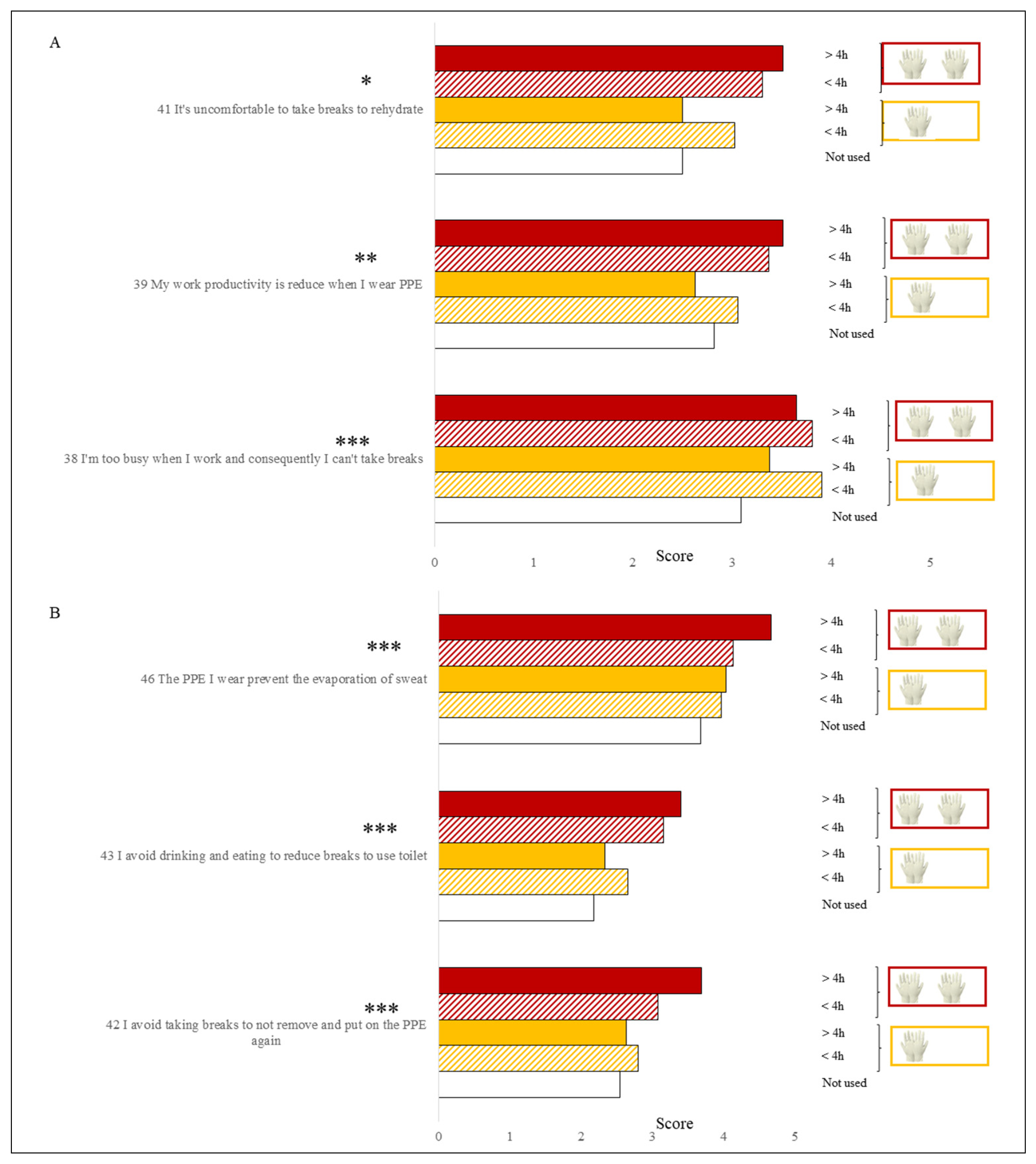
3.4. Masks, Gloves and Other PPE
4. Discussion
- perception of heat stress conditions in the workplace and productivity loss;
- behavior during the working days;
- awareness of good practices.
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Acknowledgments
Conflicts of Interest
References
- Doumas, M.; Patoulias, D.; Katsimardou, A.; Stavropoulos, K.; Imprialos, K.; Karagiannis, A. COVID19 and increased mortality in African Americans: Socioeconomic differences or does the renin angiotensin system also contribute? J. Hypertens. 2020, 34, 764–767. [Google Scholar] [CrossRef]
- Kramer, A.; Kramer, K.Z. The potential impact of the Covid-19 pandemic on occupational status, work from home, and occupational mobility. J. Vocat. Behav. 2020, 119, 103442. [Google Scholar] [CrossRef] [PubMed]
- Wahed, W.A.Y.; Hefzy, E.M.; Ahmed, M.I.; Hamed, N.S. Assessment of Knowledge, Attitudes, and Perception of Health Care Workers Regarding COVID-19, A Cross-Sectional Study from Egypt. J. Community Health 2020, 7, 1–10. [Google Scholar]
- Shechter, A.; Diaz, F.; Moise, N.; Anstey, D.E.; Agarwal, S.; Birk, J.L.; Brodie, D.; Cannone, D.E.; Chang, B.; Claassen, J.; et al. Psychological distress, coping behaviors, and preferences for support among New York healthcare workers during the COVID-19 pandemic. Gen. Hosp. Psychiatry 2020, 66, 1–8. [Google Scholar] [CrossRef]
- Adams, J.G.; Walls, R.M. Supporting the Health Care Workforce during the COVID-19 Global Epidemic. JAMA 2020, 323, 1439–1440. [Google Scholar] [CrossRef]
- Lee, J.; Venugopal, V.; Latha, P.K.; Ahadad, S.B.; Wei Leow, C.H.; De Goh, N.Y.; Tan, E.; Kjellstrom, T.; Morabito, M.; Lee, W.J.K. Heat Stress and Thermal Perception amongst Healthcare Workers during the COVID-19 Pandemic in India and Singapore. Int. J. Environ. Res. Public Health 2020, 17, 8100. [Google Scholar] [CrossRef] [PubMed]
- World Health Organization (WHO). Rational Use of Personal Protective Equipment for Coronavirus Disease 2019 (COVID-19). Interim Guidance 27 February 2020; WHO: Geneva, Switzerland, 2020. [Google Scholar]
- Komplas, M.; Morris, C.S.; Sinclair, J.; Pearson, M.; Shenoy, E. Universal Masking in Hospitals in the Covid-19 Era. N. Engl. J. Med. 2020, 21, 382. [Google Scholar] [CrossRef]
- Morabito, M.; Messeri, A.; Crisci, A.; Pratali, L.; Bonafede, M.; Marinaccio, A.; on behalf of the WORKLIMATE Collaborative Group. Heat warning and public and workers’ health at the time of COVID-19 pandemic. Sci. Total Environ. 2020, 738, 140347. [Google Scholar] [CrossRef] [PubMed]
- Global Heat Health Information Network. Protecting Health from Hot Weather during the COVID-19 Pandemic. May 2020. Available online: www.ghhin.org (accessed on 5 March 2021).
- Daanen, H.; Bose-O’Reilly, S.; Brearley, M.; Flouris, A.D.; Gerrett, N.M.; Huynen, M.; Jones, H.M.; Lee, J.K.W.; Morris, N.; Norton, I.; et al. COVID-19 and thermoregulation-related problems: Practical recommendations. Temperature 2021, 8. [Google Scholar] [CrossRef]
- Kjellstrom, T.; Homer, I.; Lemke, B. Workplace heat stress, health and productivity-an increase challenge for low and middle-income countries during climate change. Glob. Health Action 2009, 2, 2047. [Google Scholar] [CrossRef] [PubMed]
- Foster, J.; Hodder, S.G.; Goodwin, J.; Havenith, G. Occupational Heat Stress and Practical Cooling Solutions for Healthcare and Industry Workers During the COVID-19 Pandemic. Ann. Work Exp. Health 2020, 64, 915–922. [Google Scholar] [CrossRef] [PubMed]
- Potter, A.W.; Gonzalez, J.A.; Xu, X. Ebola response: Modeling the risk of heat stress from personal protective clothing. PLoS ONE 2015, 10, e0143461. [Google Scholar] [CrossRef]
- Liu, Q.; Luo, D.; Haase, J.E.; Haase, J.E.; Guo, Q.; Wang, X.Q.; Liu, S.; Xia, L.; Liu, Z.; Yang, J. The experiences of healthcare providers during the COVID-19 crisis in China: A qualitative study. Lancet Glob. Health 2020, 8, E790–E798. [Google Scholar] [CrossRef]
- Yuan, N.; Yang, W.X.; Lu, J.L.; Lv, Z.H. Investigation of adverse reactions in healthcare personnel working in Level 3 barrier protection PPE to treat COVID-19. Postgrad. Med. J. 2020, 18. [Google Scholar] [CrossRef] [PubMed]
- Ong, J.J.Y.; Bharatendu, C.; Goh, Y.; Tang, J.Z.Y.; Sooi, K.W.X.; Tan, Y.L.; Tan, B.Y.Q.; Teoh, H.L.; Ong, S.T.; Allen, D.M.; et al. Headaches Associated with Personal Protective Equipment—A Cross-Sectional Study Among Frontline Healthcare Workers During COVID-19. Headache 2020, 60, 864–877. [Google Scholar] [CrossRef] [PubMed]
- Shaukat, N.; Ali, D.M.; Razzak, J. Physical and mental health impacts of COVID-19 on healthcare workers: A scoping review. Int. J. Emerg Med. 2020, 13, 40. [Google Scholar] [CrossRef]
- Muller, A.E.; Hafstad, E.V.; Himmels, J.P.V.; Smedslund, G.; Flottorp, S.; Stensland, S.; Stroobants, S.; Van de Velde, S.; Vist, G.E. The mental health impact of the covid-19 pandemic on healthcare workers, and interventions to help them: A rapid systematic review. Psychiatry Res. 2020, 293, 113441. [Google Scholar] [CrossRef] [PubMed]
- Martinez, G.S.; Linares, C.; de’ Donato, F.; Diaz, J. Protect the vulnerable from extreme heat during the COVID-19 pandemic. Environ. Res. 2020, 187, 109684. [Google Scholar] [CrossRef] [PubMed]
- Daoust, J.F. Elderly people and responses to COVID-19 in 27 Countries. PLoS ONE 2020, 15, e0235590. [Google Scholar] [CrossRef] [PubMed]
- Chindapol, S.; Blair, J.; Osmond, P.; Prasad, D. A suitable thermal stress index for the elderly in summer tropical climates. Procedia Eng. 2017, 180, 932–943. [Google Scholar] [CrossRef]
- BS 7963. Guide to the Assessment of Heat Strain in Workers Wearing Personal Protective Equipment ISO 12894 2002 Ergonomics of the Thermal Environment—Medical Supervision of Individuals Exposed to Extreme Hot or Cold Environments; BSI: London, UK, 2000. [Google Scholar]
- ISO 7933. Ergonomics of the Thermal Environment—Analytical Determination and Interpretation of Heat Stress Using Calculation of the Predicted Heat Strain; BSI: Geneva, Switzerland, 2004. [Google Scholar]
- Morabito, M.; Messeri, A.; Noti, P.; Casanueva, A.; Crisci, A.; Kotlarski, S.; Orlandini, S.; Schwierz, C.; Spirig, C.; Kingma, B.R.M.; et al. An Occupational Heat-Health Warning System for Europe: The HEAT-SHIELD Platform. Int. J. Environ. Res. Public Health 2019, 16, 2890. [Google Scholar] [CrossRef]
- Unoki, T.; Tamoto, M.; Ouchi, A.; Sakuramoto, H.; Nakayama, A.; Katayama, Y.; Miyazaki, S.; Yamada, T.; Fujitani, S.; Nishida, O.; et al. PPe-SAFE in Japan Project, International Exchange Committee, the Japan Society of Intensive Care Medicine. Personal protective equipment use by health-care workers in intensive care units during the COVID-19 pandemic in Japan: Comparative analysis with the PPE-SAFE survey. Acute Med. Surg. 2020, 7, e584. [Google Scholar] [CrossRef]
- Davey, S.L.; Lee, B.J.; Robbins, T.; Randeva, H.; Thake, C.D. Heat stress and PPE during COVID-19: Impact on healthcare workers’ performance, safety and well-being in NHS settings. J. Hosp. Infect. 2021, 108, 185–188. [Google Scholar] [CrossRef] [PubMed]
- Tabah, A.; Ramanan, M.; Laupland, K.B.; Buetti, N.; Cortegiani, A.; Mellinghoff, J.; Morris, A.C.; Comporota, L.; Zappella, N.; Elhadi, M.; et al. Personal protective equipment and intensive care unit healthcareworker safety in the COVID-19 era (PPE-SAFE): An international survey. J. Crit. Care 2020, 59, 70–75. [Google Scholar] [CrossRef] [PubMed]
- Coomber, R. Using the Internet for Survey Research. Available online: www.socresonline.org.uk/2/2/2.html (accessed on 18 February 2021).
- Fricker, R.D.; Schonlau, M. Advantages and Disadvantages of Internet Research Surveys: Evidence from the Literature. Field Methods 2002, 14, 347–367. [Google Scholar] [CrossRef]
- Clarke, S.K.; Kumar, G.; Sutton, J.; Atem, J.; Banerji, A.; Brindamour, M.; Geltman, P.; Zaaeed, N. Potential Impact of COVID-19 on Recently Resettled Refugee Populations in the United States and Canada: Perspectives of Refugee Healthcare Providers. J. Immigr. Minor. Health 2020, 23, 184–189. [Google Scholar] [CrossRef] [PubMed]
- Leso, V.; Fontana, L.; Iavicoli, I. Susceptibility to Coronavirus (COVID-19) in Occupational Settings: The Complex Interplay between Individual and Workplace Factors. Int. J. Environ. Res. Public Health 2021, 18, 1030. [Google Scholar] [CrossRef]
- Jegodka, Y.; Lagally, L.; Mertes, H.; Deering, K.; Schoierer, J.; Buchberger, B.; Bose-O’Reilly, S. Hot days and Covid-19—Unusual heat stress for nursing professions in Germany. MedRxiv 2021. [Google Scholar] [CrossRef]
- Morris, N.B.; Levi, M.; Morabito, M.; Messeri, A.; Ioannous, L.G.; Flouris, A.D.; Samoutis, G.; Pogačar, T.; Bogataj, L.K.; Piil, F.; et al. Health vs. wealth: Employer, employee and policy-maker perspectives on occupational heat stress across multiple European industries. Temperature 2020. [Google Scholar] [CrossRef]
- Gelardi, M.M.; Fiore, V.; Giancaspro, R.; La Gatta, E.; Fortunato, F.; Resta, O.; Carpagnano, G.E.; Santomasi, C.; Dimitri, M.; Foschino Barbaro, M.P.; et al. Surgical Mask and N95 in Healthcare Workers of Covid-19 Departments: Clinical and Social Aspects. Acta Biomed. 2020, 91, e2020171. [Google Scholar] [CrossRef]
- Sprecher, A.G.; Caluwaerts, A.; Draper, M.; Feldmann, H.; Frey, C.P.; Funk, R.H.; Kobinger, G.; Le Duc, J.W.; Spiropoulou, C.; Williams, W.J. Personal Protective Equipment for Filovirus Epidemics: A Call for Better Evidence. J. Infect. Dis. 2015, 212, 2. [Google Scholar] [CrossRef] [PubMed]
- Hersi, M.; Stevens, A.; Quach, P.; Hamel, C.; Thavorn, K.; Garritty, C. Effectiveness of Personal Protective Equipment for Healthcare Workers Caring for Patients with Filovirus Disease: A Rapid Review. PLoS ONE 2015, 10, e0140290. [Google Scholar] [CrossRef]
- Loibner, M.; Hagauer, S.; Schwantzer, G.; Berghold, A.; Zatloukal, K. Limiting factors for wearing personal protective equipment (PPE) in a health care environment evaluated in a randomised study. PLoS ONE 2019, 14, e0210775. [Google Scholar] [CrossRef] [PubMed]
- Alhadad, S.B.; Tan, P.M.S.; Lee, J.K.W. Efficacy of Heat Mitigation Strategies on Core Temperature and Endurance Exercise: A Meta-Analysis. Front. Physiol. 2019, 13. [Google Scholar] [CrossRef]
- McLellan, T.M. The importance of aerobic fitness in determining tolerance to uncompensable heat stress. Comp. Biochem. Physiol. A Mol. Integr. Physiol. 2001, 128, 691–700. [Google Scholar] [CrossRef]
- Mora-Rodriguez, R.; Del Coso, J.; Hamouti, N.; Estevez, E.; Ortega, J.F. Aerobically trained individuals have greater increases in rectal temperature than untrained ones during exercise in the heat at similar relative intensities. Eur. J. Appl. Physiol. 2010, 109, 973–981. [Google Scholar] [CrossRef]
- Kuwahara, T.; Inoue, Y.; Taniguchi, M.; Ogura, Y.; Ueda, H.; Kondo, N. Effects of physical training on heat loss responses of young women to passive heating in relation to menstrual cycle. Eur. J. Appl. Physiol. 2005, 94, 376–385. [Google Scholar] [CrossRef]
- Bach, A.J.E.; Maley, M.J.; Minett, G.M.; Zietek, S.A.; Stewart, K.L.; Stewart, I.B. An Evaluation of Personal Cooling Systems for Reducing Thermal Strain WhilstWorking in Chemical/Biological Protective Clothing. Front. Physiol. 2019, 10, 424. [Google Scholar] [CrossRef]
- Yeo, Z.W.; Fan, P.W.; Nio, A.Q.; Byrne, C.; Lee, J.K. Ice slurry on outdoor running performance in heat. Int. J. Sports Med. 2012, 33, 859–866. [Google Scholar] [CrossRef]
- Tokizawa, K.; Sawada, S.; Tai, T.; Lu, J.; Oka, T.; Yasuda, A.; Takahashi, M. Effects of partial sleep restriction and sub-sequent daytime napping on prolonged exertional heat strain. Occup. Environ. Med. 2015, 72, 521–528. [Google Scholar] [CrossRef] [PubMed]
- Azmoon, H.; Dehghan, H.; Akbari, J.; Souri, S. The relationship between thermal comfort and light intensity with sleep quality and eye tiredness in shift work nurses. J. Environ. Public Health 2013, 639184. [Google Scholar] [CrossRef]
- Piil, J.F.; Lundbye-Jensen, J.; Christiansen, L.; Ioannou, L.; Tsoutsoubi, L.; Dallas, C.N.; Mantzios, K.; Flouris, A.D.; Nybo, L. High prevalence of hypohydration in occupations with heat Stress-Perspectives for performance in combined cognitive and motor tasks. PLoS ONE 2018, 13, e0205321. [Google Scholar] [CrossRef]
| Healthcare Workers | N 1 | % 2 | |
|---|---|---|---|
| Do you avoid eating on fast days for personal reasons? | Never | 167 | 87.4 |
| Sometimes | 7 | 3.7 | |
| Often | 14 | 7.3 | |
| Very often | 1 | 0.5 | |
| Ever | 2 | 1.0 | |
| How do you judge your work effort on average? | At rest | 2 | 1.0 |
| Lightweight | 13 | 6.8 | |
| Moderate | 65 | 34.0 | |
| High | 82 | 42.9 | |
| Very high | 29 | 15.2 | |
| How do you judge the thermal environment in which you generally work? | Very cold | 6 | 3.1 |
| Cold | 11 | 5.8 | |
| Slightly cold | 20 | 10.5 | |
| Neutral | 40 | 20.9 | |
| Slightly hot | 33 | 17.3 | |
| Hot | 53 | 27.7 | |
| Very hot | 28 | 14.7 | |
| For how many hours do you usually wear N95 mask or equivalent (FFP2)? | 0 h | 39 | 20.4 |
| 1 to 3 h | 50 | 26.2 | |
| 4 to 6 h | 65 | 34.0 | |
| over 6 h | 37 | 19.4 | |
| For how many hours do you usually wear FFP3 mask? | 0 h | 146 | 76.4 |
| 1 to 3 h | 28 | 14.7 | |
| 4 to 6 h | 8 | 4.2 | |
| over 6 h | 9 | 4.7 | |
| How many hours do you usually wear a surgical mask? | 0 h | 17 | 8.9 |
| 1 to 3 h | 32 | 16.8 | |
| 4 to 6 h | 69 | 36.1 | |
| over 6 h | 73 | 38.2 | |
| How many hours do you usually wear gloves (one pair)? | 0 h | 40 | 20.9 |
| 1 to 3 h | 66 | 34.6 | |
| 4 to 6 h | 55 | 28.8 | |
| over 6 h | 30 | 15.7 | |
| How many hours do you usually wear gloves (two pairs)? | 0 h | 81 | 42.4 |
| 1 to 3 h | 62 | 32.5 | |
| 4 to 6 h | 29 | 15.2 | |
| over 6 h | 19 | 9.9 | |
| How many hours do you usually wear a disposable gown? | 0 h | 48 | 25.1 |
| 1 to 3 h | 71 | 37.2 | |
| 4 to 6 h | 50 | 26.2 | |
| over 6 h | 22 | 11.5 | |
| How many hours do you usually wear a normal gown? | 0 h | 94 | 49.2 |
| 1 to 3 h | 27 | 14.1 | |
| 4 to 6 h | 43 | 22.5 | |
| over 6 h | 27 | 14.1 | |
| How many hours do you usually wear a disposable apron? | 0 h | 155 | 81.2 |
| 1 to 3 h | 21 | 11.0 | |
| 4 to 6 h | 11 | 5.8 | |
| over 6 h | 4 | 2.1 | |
| How many hours do you usually wear disposable glasses? | 0 h | 77 | 40.3 |
| 1 to 3 h | 41 | 21.5 | |
| 4 to 6 h | 50 | 26.2 | |
| over 6 h | 23 | 12.0 | |
| How many hours do you usually wear a disposable visor? | 0 h | 78 | 40.8 |
| 1 to 3 h | 56 | 29.3 | |
| 4 to 6 h | 38 | 19.9 | |
| over 6 h | 19 | 9.9 | |
| How many hours do you usually wear disposable headgear? | 0 h | 67 | 35.1 |
| 1 to 3 h | 34 | 17.8 | |
| 4 to 6 h | 49 | 25.7 | |
| over 6 h | 41 | 21.5 | |
| How many hours do you usually wear disposable closed boots or work shoes? | 0 h | 119 | 62.3 |
| 1 to 3 h | 13 | 6.8 | |
| 4 to 6 h | 21 | 11.0 | |
| over 6 h | 38 | 19.9 | |
| How many hours do you usually wear shoes covers? | 0 h | 102 | 53.4 |
| 1 to 3 h | 44 | 23.0 | |
| 4 to 6 h | 32 | 16.8 | |
| over 6 h | 13 | 6.8 | |
| How many hours do you usually wear sanitary clogs? | 0 h | 73 | 38.2 |
| 1 to 3 h | 5 | 2.6 | |
| 4 to 6 h | 42 | 22.0 | |
| over 6 h | 71 | 37.2 | |
| How many days per week do you use PPE at work? | 5.2 | SD 1.0 | |
| How long (minutes) does it take you to wear PPE at the start of the work shift? | 7.1 | SD 5.5 | |
| Do you work mainly in an air-conditioned environment? | Yes | 151 | 79.1 |
| No | 40 | 20.9 | |
| Is there a company procedure that allows you to remove PPE during work breaks? | Yes | 106 | 55.5 |
| No | 85 | 44.5 | |
| If yes, when? More than one answer is possible | In the middle of the day | 39 | 20.4 |
| When i go to the toilet | 31 | 16.2 | |
| After each visit | 31 | 16.2 | |
| Whenever i need to | 42 | 22.0 | |
| Is there a dedicated rest area in your workplace? | Yes | 88 | 46.1 |
| No | 103 | 53.9 | |
| How do you try and reduce heat stress when using PPE? It is possible to select more than one answer for this question. | I often drink water | 108 | 56.5 |
| I drink ice cold drinks | 1 | 0.5 | |
| I take breaks whenever possible | 81 | 42.4 | |
| I try to dress in light clothing | 90 | 47.1 | |
| Breathing techniques | 28 | 14.7 | |
| I prefer ventilated and cool environments | 64 | 33.5 | |
| Heat stress in the areas covered by the PPE | 150 | 78.5 | |
| Symptoms generally perceived when I wear PPE | Thirst | 111 | 58.1 |
| Excessive sweating | 135 | 70.7 | |
| Fatigue | 88 | 46.1 | |
| Headache | 82 | 42.9 | |
| Difficulty concentrating | 56 | 29.3 | |
| Skin reaction | 51 | 26.7 | |
| General discomfort | 99 | 51.8 | |
| What is your thermal sensation when you wear PPE during work activities? | Neutral | 2 | 1.0 |
| Slightly hot | 21 | 11.0 | |
| Hot | 68 | 35.6 | |
| Very hot | 100 | 52.4 | |
| Productivity loss perception caused by heat stress | 155 | 81 | |
| N-Item | Component | ||
|---|---|---|---|
| 1 “Perception of Heat Stress Conditions in the Workplace and of Productivity Loss” | 2 “HCW Behavior during the Working Days” | 3 “Awareness of Good Practices” | |
| 29-Heat stress can impair my reasoning | 0.873 | ||
| 31-Heat Stress can affect my psychological state | 0.829 | ||
| 33-Heat stress can negatively affect my commitment at work | 0.813 | ||
| 28-Heat stress can affect my productivity | 0.790 | ||
| 32-Heat stress can negatively affect my emoticons | 0.788 | ||
| 30-Heat Stress can affect my physical health | 0.765 | ||
| 42-I avoid taking breaks to not remove and put on the PPE again | 0.863 | ||
| 43-I avoid drinking and eating to reduce breaks to use toilet | 0.849 | ||
| 41-It is uncomfortable to take breaks to rehydrate | 0.763 | ||
| 44-I avoid taking breaks to reduce the risk of getting infected | 0.715 | ||
| 35-A good hydration before the work shift will improve my heat tolerance | 0.875 | ||
| 34-Keeping fit will improve my heat tolerance | 0.824 | ||
| 36-Adequate rest between shifts will improve my tolerance | 0.746 | ||
| Item | Kind of Work | Thermal Sensation with PPE | Glasses and Visor | Headgear | ||||||
|---|---|---|---|---|---|---|---|---|---|---|
| N° | G | M(SD) | F/Sig | M(SD) | F/Sig | M(SD) | F/Sig | M(SD) | F/Sig | |
| 29 | Heat stress can impair my reasoning | 1 | 4.2 (0.9) | ns | 4.0 (1.1) | ns | 4.0 (1.1) | ns | 3.9 (1.0) | 4.2 * |
| 2 | 4.2 (1.1) | 4.0 (0.9) | 4.2 (1.0) | 4.1 (1.0) | ||||||
| 3 | 4.2 (1.0) | 4.3 (1.0) | 4.3 (1.0) | 4.4 (1.0) | ||||||
| 30 | Heat Stress can affect my physical health | 1 | 4.0 (1.0) | ns | 4.0 (1.2) | 4.4 ** | 3.9 (1.2) | ns | 3.9 (1.2) | 6.1 ** |
| 2 | 4.3 (0,9) | 4.0 (1.1) | 4.2 (0.9) | 4.2 (0.9) | ||||||
| 3 | 4.2 (0.9) | 4.4 (0.8) | 4.3 (0,8) | 4.4 (0.8) | ||||||
| 31 | Heat Stress can affect my psychological state | 1 | 4.2 (0.9) | ns | 4.1 (1.0) | ns | 4.3 (0.9) | ns | 4.2 (1.0) | Ns |
| 2 | 4.3 (0.9) | 4.2 (1.0) | 3.3 (0.9) | 4.1 (1.0) | ||||||
| 3 | 4.2 (0.9) | 4.4 (0.9) | 4.3 (0.9) | 4.4 (0.8) | ||||||
| 32 | Heat stress can negatively affect my emoticons | 1 | 4.1 (1.1) | ns | 4.0 (1.3) | ns | 4.1 (1.1) | ns | 4.0 (1.2) | Ns |
| 2 | 4.2 (1.0) | 4.0 (1.1) | 4.2 (1.0) | 4.2 (1.1) | ||||||
| 3 | 4.0 (1.2) | 4.2 (1.1) | 4.0 (1.2) | 4.2 (1.1) | ||||||
| 33 | Heat stress can negatively affect my commitment at work | 1 | 4.1 (1.1) | ns | 3.9 (1.4) | ns | 4.0 (1.1) | ns | 3.9 (1.1) | Ns |
| 2 | 4.1 (1.2) | 4.0 (1.1) | 4.2 (1.2) | 4.1 (1.3) | ||||||
| 3 | 4.1 (1.1) | 4.2 (1.1) | 4.1 (1.2) | 4.3 (1.1) | ||||||
| 46 | The PPE I wear prevent the evaporation of sweat | 1 | 4.2(1.0) | ns | 3.5 (1.1) | 7.1 *** | 3.9 (1.0) | 6.9 *** | 3.8 (1.1) | Ns |
| 2 | 4.3 (1.0) | 4.1 (0.8) | 3.9 (1.2) | 4.0 (1.0) | ||||||
| 3 | 4.0(1.1) | 4.4 (1.1) | 4.5 (0.9) | 4.5 (0.9) | ||||||
| 37 | Wearing PPE is uncomfortable for me | 1 | 4.1 (1.0) | 5.7 ** | 2.9 (1.4) | 10.6 *** | 3.7 (1.2) | ns | 3.7 (1.2) | Ns |
| 2 | 3.7 (1.2) | 3.6 (1.1) | 3.6 (1.4) | 3.6 (1.3) | ||||||
| 3 | 3.4 (1.3) | 4.1 (1.1) | 4.0 (1.1) | 3.9 (1.1) | ||||||
| 39 | My work productivity is reduced when I wear PPE | 1 | 3.2 (1.2) | ns | 2.6 (1.3) | 7.7 *** | 3.0 (1.0) | ns | 3.1 (1.2) | Ns |
| 2 | 3.2 (1.2) | 2.9 (1.1) | 3.2 (1.4) | 3.2 (1.2) | ||||||
| 3 | 3.1 (1.2) | 3.5 (1.2) | 3.3 (1.3) | 3.3 (1.2) | ||||||
| 28 | Heat stress can affect my productivity | 1 | 4.3 (0.8) | ns | 4.1 (1.1) | 5.3 ** | 4.4 (1.0) | ns | 4.0 (1.0) | 4.6 ** |
| 2 | 4.4 (0.9) | 4.1 (0.9) | 4.3 (0.8) | 4.3 (0.8) | ||||||
| 3 | 4.2 (1.0) | 4.5 (0.8) | 4.4 (0.8) | 4.5 (0.9) | ||||||
| Item | Work Effort | Company Procedure to Dress PPE | Rest Area | Parts of the Body | ||||||
|---|---|---|---|---|---|---|---|---|---|---|
| N° | G | M(SD) | F/Sig | M(SD) | F/Sig | M(SD) | F/Sig | M(SD) | F/Sig | |
| 29 | Heat stress can impair my reasoning | 1 | 4.1 (1.0) | ns | 4.0 (1.1) | 4.8 * | 4.2 (1.0) | ns | 4.2 (1.0) | ns |
| 2 | 4.2 (1.0) | 4.4 (0.8) | 4.1 (1.0) | 4.3 (1.0) | ||||||
| 30 | Heat Stress can affect my physical health | 1 | 4.0 (1.0) | ns | 4.1 (1.0) | ns | 4.2 (0.9) | ns | 4.2 (0.9) | ns |
| 2 | 4.3 (0.9) | 4.3 (0.9) | 4.2 (1.0) | 4.1 (1.1) | ||||||
| 31 | Heat Stress can affect my psychological state | 1 | 4.2 (1.0) | ns | 4.1 (1.0) | 6.1 ** | 4.3 (0.9) | ns | 4.2 (1.0) | ns |
| 2 | 4.3 (0.9) | 4.5 (0.8) | 4.2 (1.0) | 4.4 (0.7) | ||||||
| 32 | Heat stress can negatively affect my emoticons | 1 | 4.0 (1.2) | ns | 3.9 (1.2) | ns | 4.0 (1.1) | ns | 4.1 (1.1) | ns |
| 2 | 4.1 (1.1) | 4.3 (0.9) | 4.2 (1.1) | 3.9 (1.2) | ||||||
| 33 | Heat stress can negatively affect my commitment at work | 1 | 4.2 (1.1) | ns | 3.9 (1.2) | 4.4 * | 4.1 (1.2) | ns | 4.1 (1.2) | ns |
| 2 | 4.0 (1.2) | 4.3 (1.0) | 4.1 (1.1) | 4.1 (1.2) | ||||||
| 46 | The PPE I wear prevent the evaporation of sweat | 1 | 4.1 (1.0) | ns | 4.1 (1.1) | ns | 4.2 (1.0) | ns | 4.2 (1.1) | ns |
| 2 | 4.2 (1.0) | 4.3 (0.9) | 4.1 (1.1) | 4.2 (0.9) | ||||||
| 37 | Wearing PPE is unconfortable for me | 1 | 3.6 (1.3) | 4.4 * | 3.5 (1.3) | ns | 3.7 (1.1) | ns | 3.7 (1.2) | ns |
| 2 | 3.9 (1.1) | 4.1 (1.0) | 3.8 (1.3) | 3.9 (1.2) | ||||||
| 39 | My work productivity is reduced when I wear PPE | 1 | 3.0 (1.2) | ns | 3.0 (1.2) | 4.9 * | 3.2 (1.3) | ns | 3.1 (1.2) | 6.2 ** |
| 2 | 3.3 (1.3) | 3.4 (1.2) | 3.2 (1.2) | 3.6 (1.2) | ||||||
| 28 | Heat stress can affect my productivity | 1 | 4.2 (0.8) | ns | 4.1 (1.0) | 7.9 *** | 4.3 (0.9) | ns | 4.3 (0.9) | ns |
| 2 | 4.3 (0.9) | 4.5 (0.7) | 4.3 (0.9) | 4.3 (1.0) | ||||||
| Item | Kind of Work | Thermal Sensation with PPE | Glasses and Visor | Headgear | ||||||
|---|---|---|---|---|---|---|---|---|---|---|
| N° | G | M (SD) | F/Sig | M(SD) | F/Sig | M(SD) | F/Sig | M(SD) | F/Sig | |
| 38 | I’m too busy when I work and consequently I can’t take breaks | 1 | 3.7 (1.1) | ns | 3.5 (1.1) | ns | 3.6 (1.1) | ns | 3.5 (1.1) | ns |
| 2 | 3.7 (1.1) | 3.7 (1.1) | 3.6 (1.2) | 3.8 (1.0) | ||||||
| 3 | 3.5 (1.2) | 3.6 (1.1) | 3.7 (1.1) | 3.7 (1.1) | ||||||
| 41 | It is uncomfortable to take breaks to rehydrate | 1 | 3.1 (1.4) | ns | 2.8 (1.2) | ns | 2.9 (1.1) | 5.7 ** | 2.8 (1.2) | 8.0 *** |
| 2 | 3.4 (1.4) | 3.1 (1.3) | 2.7 (1.4) | 2.6 (1.5) | ||||||
| 3 | 2.8 (1.4) | 3.2 (1.4) | 3.5 (1.4) | 3.5 (1.4) | ||||||
| 42 | I avoid taking breaks to not remove and put on the PPE again | 1 | 3.2 (1.4) | ns | 2.4 (1.3) | ns | 2.7 (1.2) | 5.5 ** | 2.7 (1.4) | 6.5 *** |
| 2 | 3.2 (1.5) | 3.0 (1.3) | 2.8 (1.5) | 2.6 (1.4) | ||||||
| 3 | 2.7 (1.5) | 3.2 (1.5) | 3.4 (1.5) | 3.5 (1.5) | ||||||
| 43 | I avoid drinking and eating to reduce breaks to use toilet | 1 | 3.1 (1.5) | 7.9 *** | 2.6 (1.6) | ns | 2.6 (1.5) | ns | 2.6 (1.5) | 3.3 * |
| 2 | 3.2 (1.4) | 2.9 (1.4) | 2.8 (1.5) | 2.9 (1.6) | ||||||
| 3 | 2.2 (1.3) | 3.0 (1.5) | 3.2 (1.4) | 3.2 (1.4) | ||||||
| 44 | I avoid taking breaks to reduce the risk of getting infected | 1 | 2.7 (1.4) | ns | 2.9 (1.5) | 3.1 * | 2.5 (1.4) | ns | 2.5 (1.4) | ns |
| 2 | 2.9 (1.5) | 2.9 (1.4) | 3.0 (1.4) | 3.0 (1.4) | ||||||
| 3 | 2.7 (1.5) | 2.7 (1.5) | 2.8 (1.5) | 2.9 (1.5) | ||||||
| 40 | It is important to keep hydrated during the work shift | 1 | 4.4 (0.9) | ns | 4.6 (0.7) | ns | 4.4 (0.7) | ns | 4.5 (0.7) | ns |
| 2 | 4.5 (0.8) | 4.3 (0.9) | 4.6 (0.6) | 4.4 (0.8) | ||||||
| 3 | 4.6 (0.7) | 4.6 (0.8) | 4.6 (0.8) | 4.5 (0.9) | ||||||
| 45 | Slush drinks improve my tolerance to heat | 1 | 2.1 (1.2) | ns | 2.0 (1.5) | ns | 2.2 (1.2) | ns | 2.3 (1.3) | 9.8 *** |
| 2 | 2.1 (1.3) | 2.0 (1.1) | 2.2 (1.3) | 2.1 (1.1) | ||||||
| 3 | 2.0 (1.2) | 2.1 (1.2) | 1.8 (1.1) | 1.8 (1.1) | ||||||
| 34 | Keeping fit will improve my heat tolerance | 1 | 3.9 (1.1) | 4.3 (0.8) | 4.7 ** | 3.9 (1.1) | ns | 3.7 (1.1) | ns | |
| 2 | 3.6 (1.2) | ns | 3.9 (1.1) | 3.7 (1.1) | 3.5 (1.2) | |||||
| 3 | 3.7 (1.2) | 3.5 (1.2) | 3.6 (1.2) | 3.8 (1.2) | ||||||
| 35 | A good hydration before the work shift will improve my heat tolerance | 1 | 3.9 (1.1) | 3.4 * | 4.6 (0.7) | 6.6 *** | 4.0 (1.1) | ns | 4.0 (1.0) | ns |
| 2 | 3.6 (1.1) | 3.9 (1.2) | 4.0 (1.1) | 3.7 (1.2) | ||||||
| 3 | 4.2 (1.0) | 3.7 (1.1) | 3.8 (1.1) | 3.9 (1.1) | ||||||
| 36 | Adequate rest between shifts will improve my tolerance | 1 | 4.3 (1.0) | 3.3 * | 4.4 (0.9) | ns | 4.2 (0.9) | ns | 4.3 (0.9) | ns |
| 2 | 3.9 (1.2) | 4.3 (0.9) | 4.1 (1.2) | 3.9 (1.3) | ||||||
| 3 | 4.4 (0.9) | 4.0 (1.2) | 4.2 (1.1) | 4.2 (1.0) | ||||||
| Item | Work Effort | Company Procedure to Dress PPE | Rest Area | Parts of the Body | ||||||
|---|---|---|---|---|---|---|---|---|---|---|
| N° | G | M(SD) | F/Sig | M(SD) | F/Sig | M(SD) | F/Sig | M(SD) | F/Sig | |
| 38 | I’m too busy when I work and consequently I can’t take breaks | 1 | 3.5 (1.1) | 4.5 * | 3.5 (1.1) | ns | 3.5 (1.1) | 4.5 * | 3.6 (1.1) | 4.6 * |
| 2 | 3.8 (1.1) | 3.8 (1.1) | 3.8 (1.1) | 4.0 (1.0) | ||||||
| 41 | It’s uncomfortable to take breaks to rehydrate | 1 | 2.8 (1.3) | 5.6 ** | 3.1 (1.3) | ns | 2.9 (1.3) | 4.1 * | 2.9 (1.4) | 13.8 *** |
| 2 | 3.3 (1.4) | 3.3 (1.4) | 3.3 (1.5) | 3.8 (1.2) | ||||||
| 42 | I avoid taking breaks to not remove and put on the PPE again | 1 | 2.8 (1.5) | ns | 2.9 (1.4) | ns | 3.0 (1.4) | ns | 2.9 (1.4) | 5.0 * |
| 2 | 3.2 (1.4) | 3.3 (1.5) | 3.1 (1.5) | 3.5 (1.5) | ||||||
| 43 | I avoid drinking and eating to reduce breaks to use toilet | 1 | 2.8 (1.5) | ns | 2.8 (1.4) | ns | 2.9 (1.5) | ns | 2.8 (1.4) | ns |
| 2 | 3.0 (1.5) | 3.1 (1.5) | 2.9 (1.5) | 3.2 (1.6) | ||||||
| 44 | I avoid taking breaks to reduce the risk of getting infected | 1 | 2.7 (1.4) | ns | 2.6 (1.4) | ns | 2.8 (1.4) | ns | 2.7 (1.4) | ns |
| 2 | 2.8 (1.5) | 2.9 (1.4) | 2.7 (1.5) | 3.1 (1.5) | ||||||
| 40 | It is important to keep hydrated during the work shift | 1 | 4.4 (0.9) | ns | 4.4 (0.9) | ns | 4.5 (0.7) | ns | 4.5 (0.8) | ns |
| 2 | 4.6 (0.8) | 4.6 (0.6) | 4.5 (0.9) | 4.4 (0.8) | ||||||
| 45 | Slush drinks improve my tolerance to heat | 1 | 2.1 (1.1) | ns | 1.8 (1.1) | 7.3 *** | 2.2 (1.3) | ns | 2.1 (1.2) | ns |
| 2 | 2.0 (1.3) | 2.3 (1.2) | 1.9 (1.1) | 1.9 (1.2) | ||||||
| 34 | Keeping fit will improve my heat tolerance | 1 | 3.6 (1.1) | ns | 3.9 (1.1) | 5.3 * | 3.7 (1.2) | ns | 3.8 (1.1) | ns |
| 2 | 3.8 (1.2) | 3.5 (1.2) | 3.8 (1.1) | 3.6 (1.1) | ||||||
| 35 | A good hydration before the work shift will improve my heat tolerance | 1 | 3.7 (1.2) | ns | 4.0 (1.1) | ns | 3.8 (1.1) | ns | 3.9 (1.1) | ns |
| 2 | 4.0 (1.0) | 3.7 (1.1) | 3.9 (1.1) | 3.7 (1.2) | ||||||
| 36 | Adequate rest between shifts will improve my tolerance | 1 | 4.0 (1.2) | 5.2 * | 4.3 (0.9) | Ns | 4.0 (1.1) | 4.7 * | 4.2 (1.0) | ns |
| 2 | 4.3 (0.9) | 4.0 (1.2) | 4.3 (1.0) | 3.9 (1.2) | ||||||
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Messeri, A.; Bonafede, M.; Pietrafesa, E.; Pinto, I.; de’Donato, F.; Crisci, A.; Lee, J.K.W.; Marinaccio, A.; Levi, M.; Morabito, M.; et al. A Web Survey to Evaluate the Thermal Stress Associated with Personal Protective Equipment among Healthcare Workers during the COVID-19 Pandemic in Italy. Int. J. Environ. Res. Public Health 2021, 18, 3861. https://doi.org/10.3390/ijerph18083861
Messeri A, Bonafede M, Pietrafesa E, Pinto I, de’Donato F, Crisci A, Lee JKW, Marinaccio A, Levi M, Morabito M, et al. A Web Survey to Evaluate the Thermal Stress Associated with Personal Protective Equipment among Healthcare Workers during the COVID-19 Pandemic in Italy. International Journal of Environmental Research and Public Health. 2021; 18(8):3861. https://doi.org/10.3390/ijerph18083861
Chicago/Turabian StyleMesseri, Alessandro, Michela Bonafede, Emma Pietrafesa, Iole Pinto, Francesca de’Donato, Alfonso Crisci, Jason Kai Wei Lee, Alessandro Marinaccio, Miriam Levi, Marco Morabito, and et al. 2021. "A Web Survey to Evaluate the Thermal Stress Associated with Personal Protective Equipment among Healthcare Workers during the COVID-19 Pandemic in Italy" International Journal of Environmental Research and Public Health 18, no. 8: 3861. https://doi.org/10.3390/ijerph18083861
APA StyleMesseri, A., Bonafede, M., Pietrafesa, E., Pinto, I., de’Donato, F., Crisci, A., Lee, J. K. W., Marinaccio, A., Levi, M., Morabito, M., & on behalf of the WORKLIMATE Collaborative Group. (2021). A Web Survey to Evaluate the Thermal Stress Associated with Personal Protective Equipment among Healthcare Workers during the COVID-19 Pandemic in Italy. International Journal of Environmental Research and Public Health, 18(8), 3861. https://doi.org/10.3390/ijerph18083861








