Volume-of-Interest Aware Deep Neural Networks for Rapid Chest CT-Based COVID-19 Patient Risk Assessment
Abstract
1. Introduction
- The publication and use of COVID-19_CHDSET Dataset, a new CT dataset of COVID-19 infected patients from Milan, a region early and intensively involved in the pandemic. The CTs are labeled according the patient hospitalization outcome.
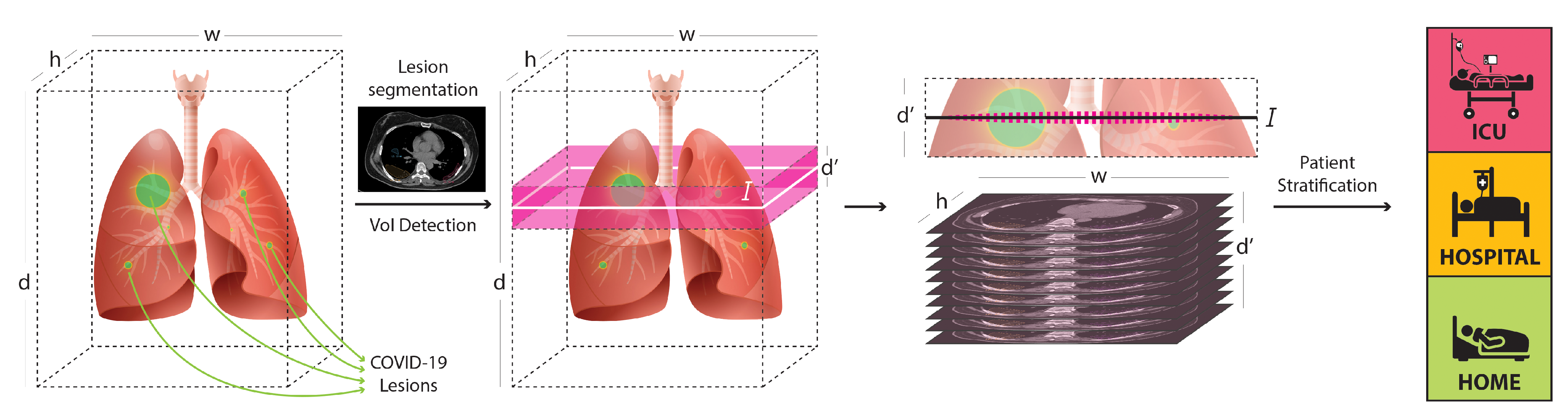
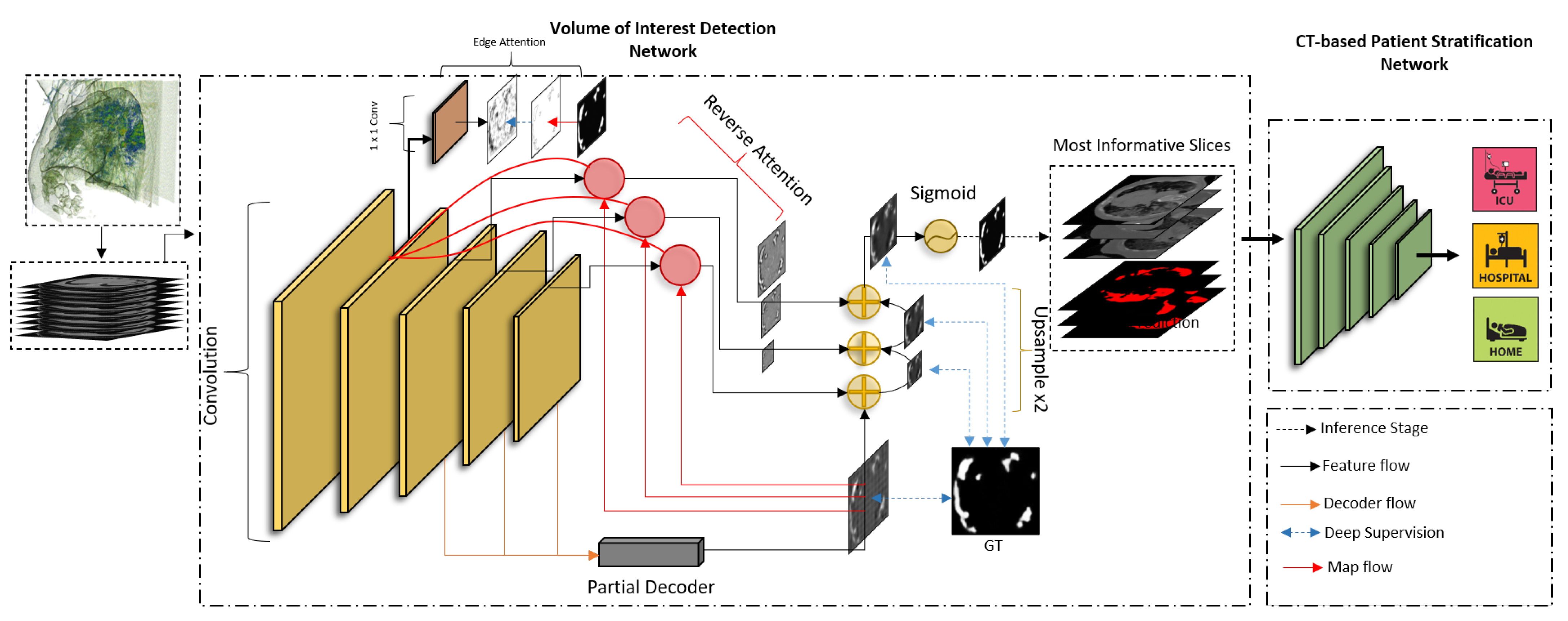
- The introduction of a novel, staged, data-driven technique of spatially coherent sub-sampling of CT volumes by detecting Volumes-of-Interest (VoI). This leads to lightweight but highly informative CT data that allow us to train state-of-the-art 2D and 3D classifiers more effectively than existing techniques.
- The exhaustive experimentation among various CT-based risk-prediction approaches and 2D/3D classifiers for COVID-19 patient stratification, to assess their performance.
2. Related Work
3. COVID-19_CHDSET Dataset
4. COVID-19 CT-Based Patient Risk Assessment
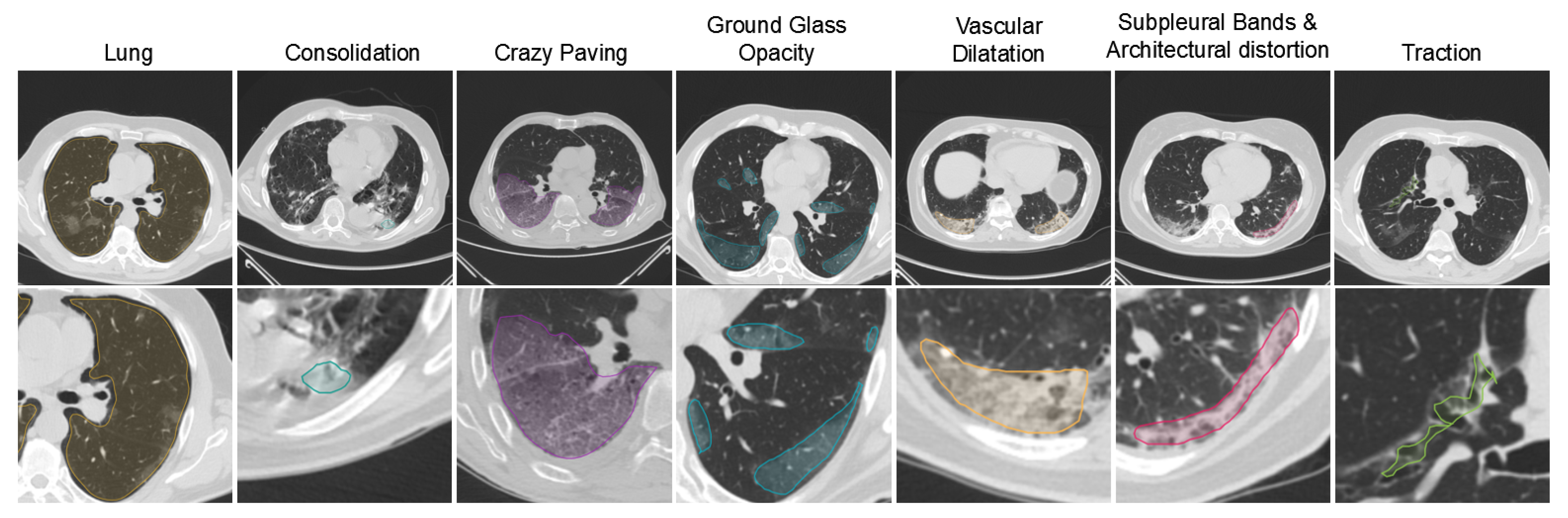
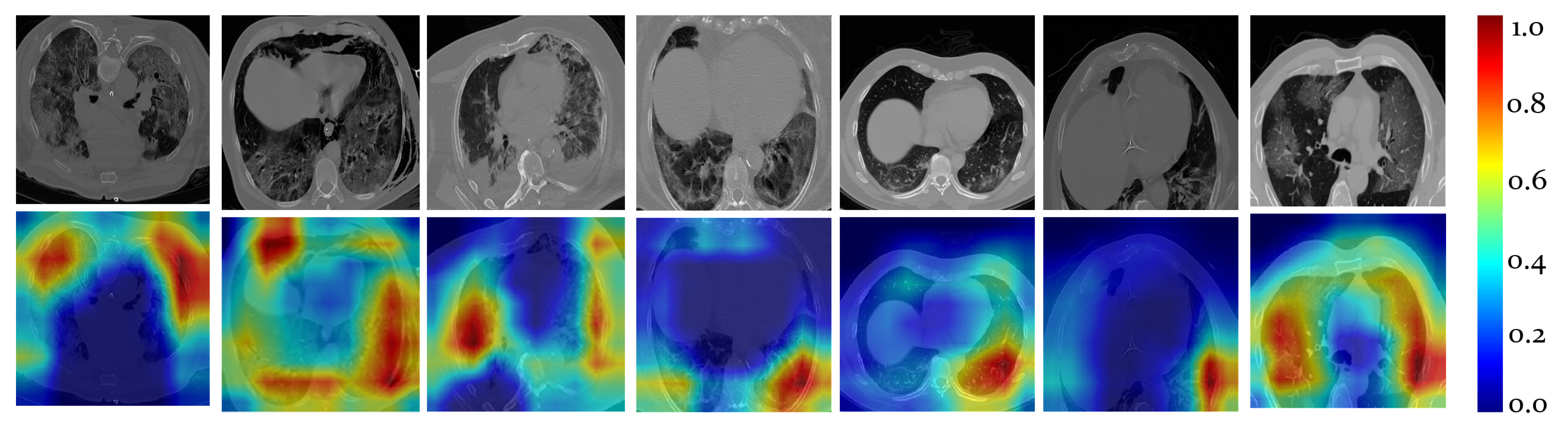
4.1. COVID-19 Quantification for VoI Detection
4.2. VoI Classification for COVID-19 Patient Risk Assessment
5. Evaluation
5.1. Experimental Setup
5.1.1. COVID-19_CHDSET Dataset Splits
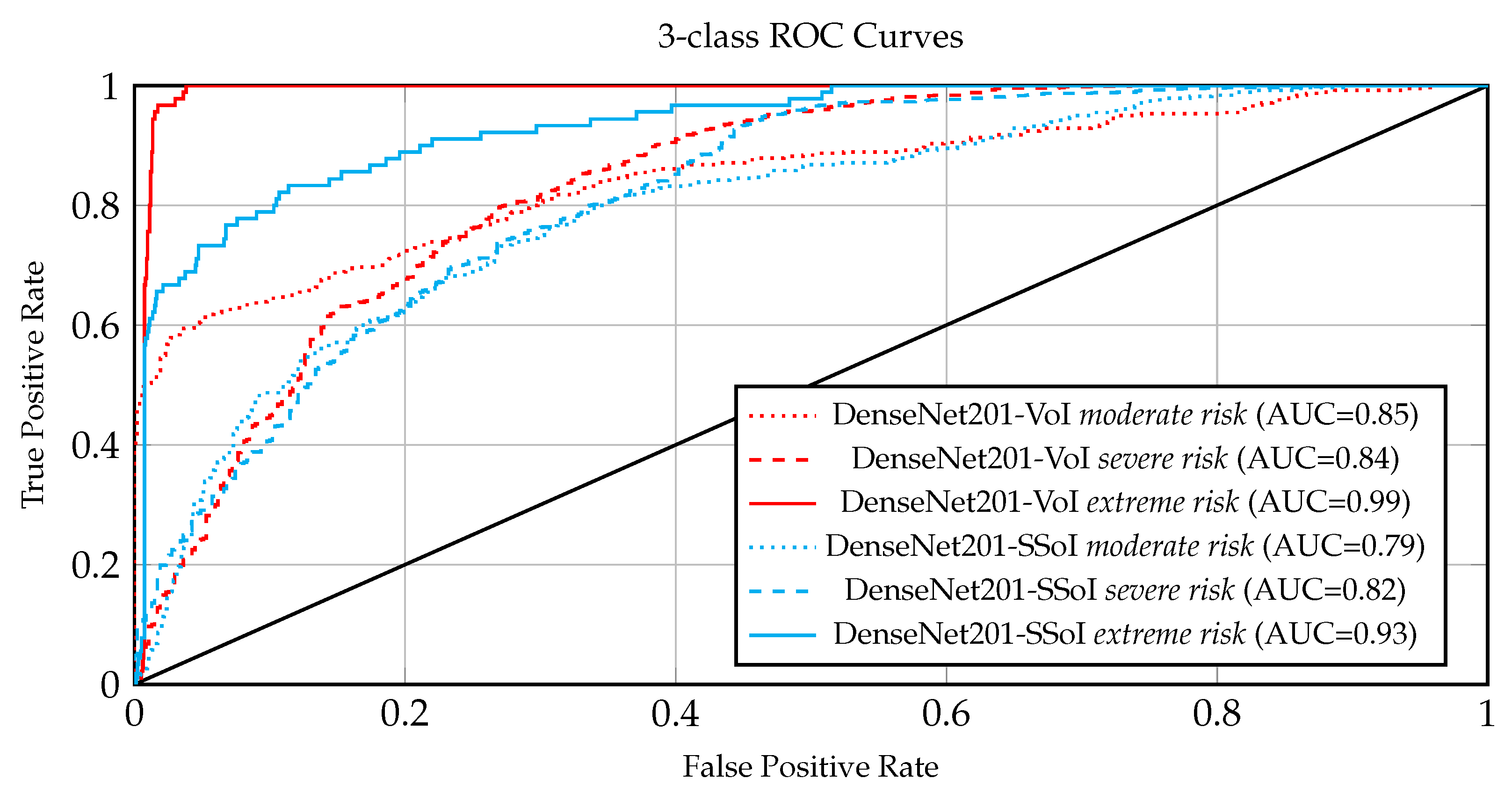
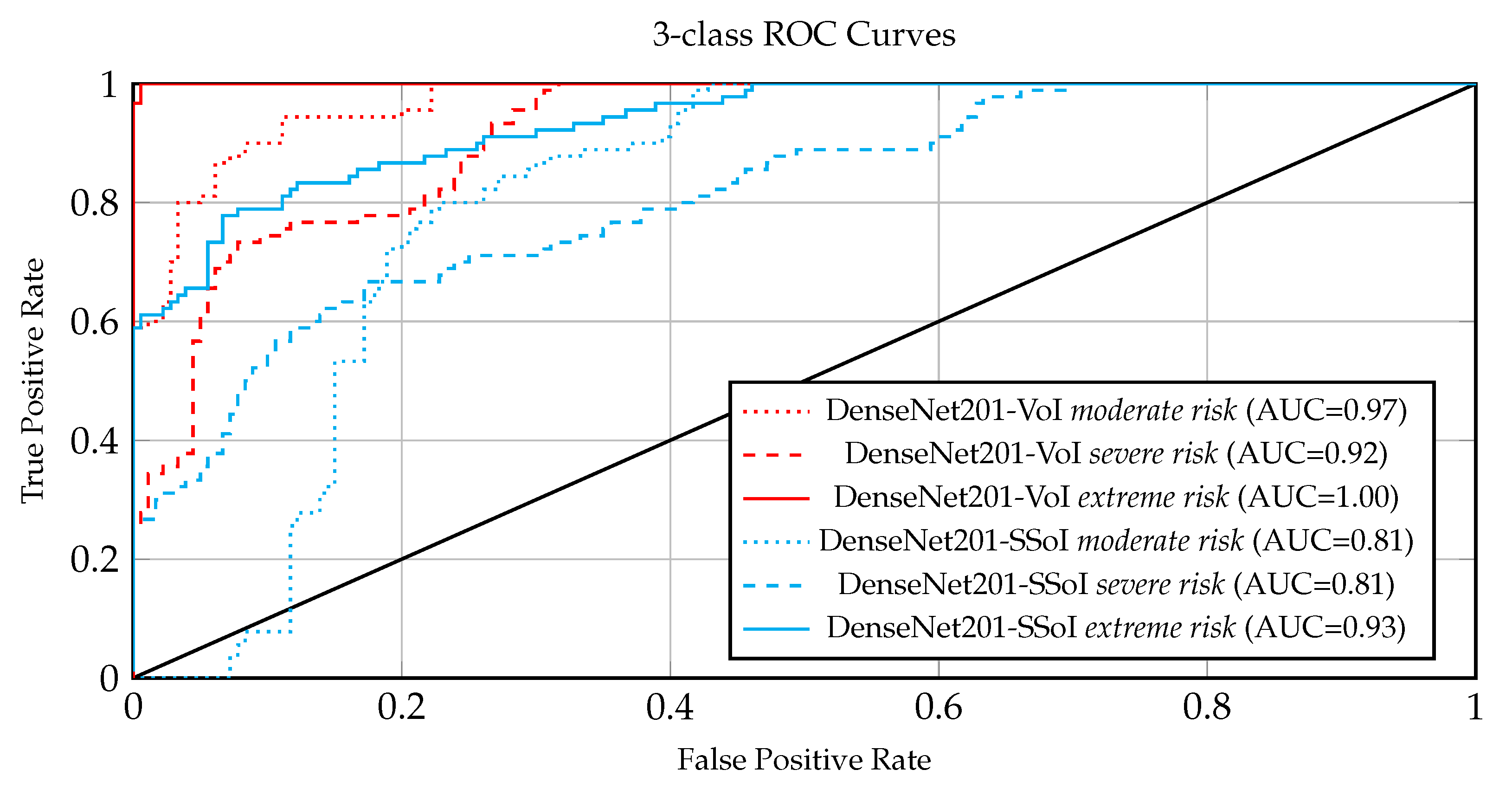
5.1.2. CT-Based Risk Assessment Strategies
- SSoI: is applied in a similar fashion to VoI. Precisely, to avoid any lossy volume down-sampling, by essentially reducing the height of the treated volume, we experimented with an alternative approach based on recent works [16,39]. In detail, CT slices are analyzed to quantify the infection, and the most infected ones (not necessarily consecutive) are considered to compose a stack of slices-of-interest (SSoI); Volume: the second and mostly common approach we experimented with, considers the whole volume and down-scales it to reach manageable data sizes and computational time.
5.1.3. Evaluation Metrics
5.1.4. Radiologists’ CT-Based Risk Assessment Protocol
5.2. Results
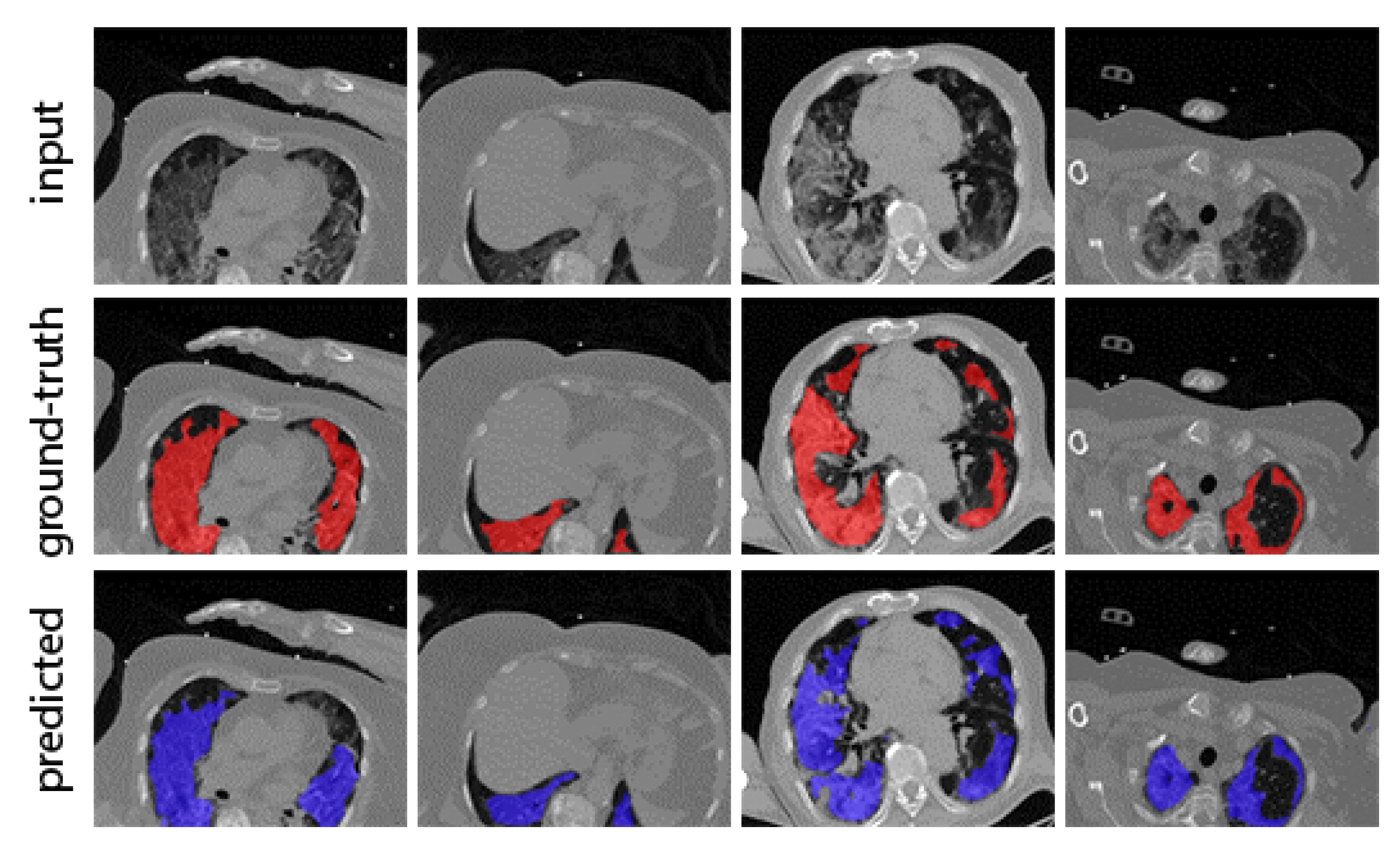
5.2.1. Lesion Segmentation Results
5.2.2. CT-Based Risk Assessment Results
6. Discussion and Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
Appendix A. Implementation Details
References
- Andersen, K.G.; Rambaut, A.; Lipkin, W.I.; Holmes, E.C.; Garry, R.F. The proximal origin of SARS-CoV-2. Nat. Med. 2020, 26, 450–452. [Google Scholar] [CrossRef]
- Mattiuzzi, C.; Lippi, G. Which lessons shall we learn from the 2019 novel coronavirus outbreak? Ann. Transl. Med. 2020, 8, 48. [Google Scholar] [CrossRef]
- Zhu, N.; Zhang, D.; Wang, W.; Li, X.; Yang, B.; Song, J.; Zhao, X.; Huang, B.; Shi, W.; Lu, R.; et al. A novel coronavirus from patients with pneumonia in China, 2019. N. Engl. J. Med. 2020, 382, 727–733. [Google Scholar] [CrossRef]
- Li, Q.; Guan, X.; Wu, P.; Wang, X.; Zhou, L.; Tong, Y.; Ren, R.; Leung, K.S.; Lau, E.H.; Wong, J.Y.; et al. Early transmission dynamics in Wuhan, China, of novel coronavirus—Infected pneumonia. N. Engl. J. Med. 2020, 382, 1199–1207. [Google Scholar] [CrossRef]
- Chung, M.; Bernheim, A.; Mei, X.; Zhang, N.; Huang, M.; Zeng, X.; Cui, J.; Xu, W.; Yang, Y.; Fayad, Z.A.; et al. CT imaging features of 2019 novel coronavirus (2019-nCoV). Radiology 2020, 295, 202–207. [Google Scholar] [CrossRef]
- Xie, X.; Zhong, Z.; Zhao, W.; Zheng, C.; Wang, F.; Liu, J. Chest CT for typical 2019-nCoV pneumonia: Relationship to negative RT-PCR testing. Radiology 2020, 296, E41–E45. [Google Scholar] [CrossRef] [PubMed]
- Giannitto, C.; Sposta, F.M.; Repici, A.; Vatteroni, G.; Casiraghi, E.; Casari, E.; Ferraroli, G.M.; Fugazza, A.; Sandri, M.T.; Chiti, A.; et al. Chest CT in patients with a moderate or high pretest probability of COVID-19 and negative swab. Radiol. Med. 2020, 125, 1260–1270. [Google Scholar] [CrossRef] [PubMed]
- Casiraghi, E.; Malchiodi, D.; Trucco, G.; Frasca, M.; Cappelletti, L.; Fontana, T.; Esposito, A.A.; Avola, E.; Jachetti, A.; Reese, J.; et al. Explainable machine learning for early assessment of COVID-19 risk prediction in emergency departments. IEEE Access 2020, 8, 196299–196325. [Google Scholar] [CrossRef]
- Liu, F.; Zhang, Q.; Huang, C.; Shi, C.; Wang, L.; Shi, N.; Fang, C.; Shan, F.; Mei, X.; Shi, J.; et al. CT quantification of pneumonia lesions in early days predicts progression to severe illness in a cohort of COVID-19 patients. Theranostics 2020, 10, 5613. [Google Scholar] [CrossRef] [PubMed]
- Kim, M.; Yun, J.; Cho, Y.; Shin, K.; Jang, R.; Bae, H.j.; Kim, N. Deep learning in medical imaging. Neurospine 2019, 16, 657. [Google Scholar] [CrossRef] [PubMed]
- Esteva, A.; Robicquet, A.; Ramsundar, B.; Kuleshov, V.; DePristo, M.; Chou, K.; Cui, C.; Corrado, G.; Thrun, S.; Dean, J. A guide to deep learning in healthcare. Nat. Med. 2019, 25, 24–29. [Google Scholar] [CrossRef]
- Barricelli, B.R.; Casiraghi, E.; Gliozzo, J.; Petrini, A.; Valtolina, S. Human Digital Twin for Fitness Management. IEEE Access 2020, 8, 26637–26664. [Google Scholar] [CrossRef]
- Wynants, L.; Van Calster, B.; Collins, G.S.; Riley, R.D.; Heinze, G.; Schuit, E.; Bonten, M.M.J.; Dahly, D.L.; Damen, J.A.A.; Debray, T.P.A.; et al. Prediction models for diagnosis and prognosis of COVID-19: Systematic review and critical appraisal. BMJ 2020, 369, m1328. [Google Scholar] [CrossRef] [PubMed]
- Liu, F.; Zhou, Z.; Samsonov, A.; Blankenbaker, D.; Larison, W.; Kanarek, A.; Lian, K.; Kambhampati, S.; Kijowski, R. Deep learning approach for evaluating knee MR images: Achieving high diagnostic performance for cartilage lesion detection. Radiology 2018, 289, 160–169. [Google Scholar] [CrossRef]
- Liu, F.; Guan, B.; Zhou, Z.; Samsonov, A.; Rosas, H.; Lian, K.; Sharma, R.; Kanarek, A.; Kim, J.; Guermazi, A.; et al. Fully automated diagnosis of anterior cruciate ligament tears on knee MR images by using deep learning. Radiol. Artif. Intell. 2019, 1, 180091. [Google Scholar] [CrossRef] [PubMed]
- Mei, X.; Lee, H.C.; Diao, K.y.; Huang, M.; Lin, B.; Liu, C.; Xie, Z.; Ma, Y.; Robson, P.M.; Chung, M.; et al. Artificial intelligence—Enabled rapid diagnosis of patients with COVID-19. Nat. Med. 2020, 26, 1224–1228. [Google Scholar] [CrossRef] [PubMed]
- Santosh, K.C. AI-Driven Tools for Coronavirus Outbreak: Need of Active Learning and Cross-Population Train/Test Models on Multitudinal/Multimodal Data. J. Med. Syst. 2020, 44, 93. [Google Scholar] [CrossRef] [PubMed]
- Harmon, S.A.; Sanford, T.H.; Xu, S.; Turkbey, E.B.; Roth, H.; Xu, Z.; Yang, D.; Myronenko, A.; Anderson, V.; Amalou, A.; et al. Artificial intelligence for the detection of COVID-19 pneumonia on chest CT using multinational datasets. Nat. Commun. 2020, 11, 4080. [Google Scholar] [CrossRef]
- Ng, M.Y.; Lee, E.Y.; Yang, J.; Yang, F.; Li, X.; Wang, H.; Lui, M.M.s.; Lo, C.S.Y.; Leung, B.; Khong, P.L.; et al. Imaging profile of the COVID-19 infection: Radiologic findings and literature review. Radiol. Cardiothorac. Imaging 2020, 2, e200034. [Google Scholar] [CrossRef]
- Bouguelia, M.R.; Nowaczyk, S.; Santosh, K.C.; Verikas, A. Agreeing to disagree: Active learning with noisy labels without crowdsourcing. Int. J. Mach. Learn. Cybern. 2018, 9, 1307–1319. [Google Scholar] [CrossRef]
- Lenchik, L.; Heacock, L.; Weaver, A.A.; Boutin, R.D.; Cook, T.S.; Itri, J.; Filippi, C.G.; Gullapalli, R.P.; Lee, J.; Zagurovskaya, M.; et al. Automated segmentation of tissues using CT and MRI: A systematic review. Acad. Radiol. 2019, 26, 1695–1706. [Google Scholar] [CrossRef]
- Tilborghs, S.; Dirks, I.; Fidon, L.; Willems, S.; Eelbode, T.; Bertels, J.; Ilsen, B.; Brys, A.; Dubbeldam, A.; Buls, N.; et al. Comparative study of deep learning methods for the automatic segmentation of lung, lesion and lesion type in CT scans of COVID-19 patients. arXiv 2020, arXiv:2007.15546. [Google Scholar]
- Ozsahin, I.; Sekeroglu, B.; Musa, M.S.; Mustapha, M.T.; Uzun Ozsahin, D. Review on Diagnosis of COVID-19 from Chest CT Images Using Artificial Intelligence. Comput. Math. Methods Med. 2020, 2020, 9756518. [Google Scholar] [CrossRef] [PubMed]
- Wang, J.; Bao, Y.; Wen, Y.; Lu, H.; Luo, H.; Xiang, Y.; Li, X.; Liu, C.; Qian, D. Prior-Attention Residual Learning for More Discriminative COVID-19 Screening in CT Images. IEEE Trans. Med. Imaging 2020, 39, 2572–2583. [Google Scholar] [CrossRef]
- Lessmann, N.; Sánchez, C.I.; Beenen, L.; Boulogne, L.H.; Brink, M.; Calli, E.; Charbonnier, J.P.; Dofferhoff, T.; van Everdingen, W.M.; Gerke, P.K.; et al. Automated assessment of CO-RADS and chest CT severity scores in patients with suspected COVID-19 using artificial intelligence. Radiology 2020, 202439. [Google Scholar] [CrossRef] [PubMed]
- Ardila, D.; Kiraly, A.P.; Bharadwaj, S.; Choi, B.; Reicher, J.J.; Peng, L.; Tse, D.; Etemadi, M.; Ye, W.; Corrado, G.; et al. End-to-end lung cancer screening with three-dimensional deep learning on low-dose chest computed tomography. Nat. Med. 2019, 25, 954–961. [Google Scholar] [CrossRef]
- Szegedy, C.; Liu, W.; Jia, Y.; Sermanet, P.; Reed, S.; Anguelov, D.; Erhan, D.; Vanhoucke, V.; Rabinovich, A. Going deeper with convolutions. In Proceedings of the IEEE Conference on Computer Vision and Pattern Recognition, Boston, MA, USA, 7–12 June 2015; pp. 1–9. [Google Scholar]
- Prokop, M.; van Everdingen, W.; van Rees Vellinga, T.; Quarles van Ufford, J.; Stöger, L.; Beenen, L.; Geurts, B.; Gietema, H.; Krdzalic, J.; Schaefer-Prokop, C.; et al. CO-RADS–A categorical CT assessment scheme for patients with suspected COVID-19: Definition and evaluation. Radiology 2020, 296, E97–E104. [Google Scholar] [CrossRef] [PubMed]
- Xu, X.; Jiang, X.; Ma, C.; Du, P.; Li, X.; Lv, S.; Yu, L.; Ni, Q.; Chen, Y.; Su, J.; et al. A Deep Learning System to Screen Novel Coronavirus Disease 2019 Pneumonia. Engineering 2020, 6, 1122–1129. [Google Scholar] [CrossRef]
- Li, L.; Qin, L.; Xu, Z.; Yin, Y.; Wang, X.; Kong, B.; Bai, J.; Lu, Y.; Fang, Z.; Song, Q.; et al. Artificial intelligence distinguishes COVID-19 from community acquired pneumonia on chest CT. Radiology 2020. [Google Scholar] [CrossRef]
- Chassagnon, G.; Vakalopoulou, M.; Battistella, E.; Christodoulidis, S.; Hoang-Thi, T.N.; Dangeard, S.; Deutsch, E.; Andre, F.; Guillo, E.; Halm, N.; et al. AI-Driven quantification, staging and outcome prediction of COVID-19 pneumonia. Med. Image Anal. 2020, 67, 101860. [Google Scholar] [CrossRef]
- Hearst, M.A.; Dumais, S.T.; Osuna, E.; Platt, J.; Scholkopf, B. Support vector machines. IEEE Intell. Syst. Appl. 1998, 13, 18–28. [Google Scholar] [CrossRef]
- Dey, L.; Chakraborty, S.; Mukhopadhyay, A. Machine learning techniques for sequence-based prediction of viral–host interactions between SARS-CoV-2 and human proteins. Biomed. J. 2020, 43, 438–450. [Google Scholar] [CrossRef]
- Breiman, L. Random Forests. Mach. Learn. 2001, 45, 5–32. [Google Scholar] [CrossRef]
- Mostafiz, R.; Uddin, M.S.; Alam, N.A.; Reza, M.M.; Rahman, M.M. COVID-19 Detection in Chest X-ray Through Random Forest Classifier using a Hybridization of Deep CNN and DWT Optimized Features. J. King Saud Univ. Comput. Inf. Sci. 2020. [Google Scholar] [CrossRef]
- Sahlol, A.T.; Yousri, D.; Ewees, A.A.; Al-Qaness, M.A.; Damasevicius, R.; Abd Elaziz, M. COVID-19 image classification using deep features and fractional-order marine predators algorithm. Sci. Rep. 2020, 10, 15364. [Google Scholar] [CrossRef]
- Akram, T.; Attique, M.; Gul, S.; Shahzad, A.; Altaf, M.; Naqvi, S.S.R.; Damaševičius, R.; Maskeliūnas, R. A novel framework for rapid diagnosis of COVID-19 on computed tomography scans. Pattern Anal. Appl. 2021, 1–14. [Google Scholar] [CrossRef]
- Chao, H.; Fang, X.; Zhang, J.; Homayounieh, F.; Arru, C.D.; Digumarthy, S.R.; Babaei, R.; Mobin, H.K.; Mohseni, I.; Saba, L.; et al. Integrative analysis for COVID-19 patient outcome prediction. Med. Image Anal. 2021, 67, 101844. [Google Scholar] [CrossRef]
- Fan, D.P.; Zhou, T.; Ji, G.P.; Zhou, Y.; Chen, G.; Fu, H.; Shen, J.; Shao, L. Inf-Net: Automatic COVID-19 Lung Infection Segmentation from CT Images. IEEE Trans. Med. Imaging 2020, 39, 2626–2637. [Google Scholar] [CrossRef]
- Selvaraju, R.R.; Cogswell, M.; Das, A.; Vedantam, R.; Parikh, D.; Batra, D. Grad-CAM: Visual Explanations From Deep Networks via Gradient-Based Localization. In Proceedings of the IEEE International Conference on Computer Vision, Venice, Italy, 22–29 October 2017; pp. 618–626. [Google Scholar]
- Wang, X.; Han, S.; Chen, Y.; Gao, D.; Vasconcelos, N. Volumetric attention for 3D medical image segmentation and detection. In Proceedings of the International Conference on Medical Image Computing and Computer-Assisted Intervention, Shenzhen, China, 13–17 October 2019; pp. 175–184. [Google Scholar]
- Khan, A.; Sohail, A.; Zahoora, U.; Qureshi, A.S. A survey of the recent architectures of deep convolutional neural networks. Artif. Intell. Rev. 2020, 53, 5455–5516. [Google Scholar] [CrossRef]
- He, K.; Zhang, X.; Ren, S.; Sun, J. Deep Residual Learning for Image Recognition. In Proceedings of the IEEE Conference on Computer Vision and Pattern Recognition, Las Vegas, NV, USA, 27–30 June 2016; pp. 770–778. [Google Scholar]
- Huang, G.; Liu, Z.; Van Der Maaten, L.; Weinberger, K.Q. Densely connected convolutional networks. In Proceedings of the IEEE Conference on Computer Vision and Pattern Recognition, Honolulu, HI, USA, 21–26 July 2017; pp. 4700–4708. [Google Scholar]
- Hara, K.; Kataoka, H.; Satoh, Y. Can Spatiotemporal 3D CNNs Retrace the History of 2D CNNs and ImageNet? In Proceedings of the 2018 IEEE/CVF Conference on Computer Vision and Pattern Recognition, Salt Lake City, UT, USA, 18–22 June 2018; pp. 6546–6555. [Google Scholar]
- Tran, D.; Wang, H.; Torresani, L.; Ray, J.; LeCun, Y.; Paluri, M. A Closer Look at Spatiotemporal Convolutions for Action Recognition. In Proceedings of the 2018 IEEE/CVF Conference on Computer Vision and Pattern Recognition, Salt Lake City, UT, USA, 18–22 June 2018; pp. 6450–6459. [Google Scholar]
- Fernández, A.; García, S.; Galar, M.; Prati, R.C.; Krawczyk, B.; Herrera, F. Learning from Imbalanced Data Sets; Springer: Cham, Switzerland, 2018; Volume 11. [Google Scholar]
- Devore, J. Probability and Statistics for Engineering and the Sciences; Nelson Education: Boston, MA, USA, 2011. [Google Scholar]
- Singh, B.K. Determining relevant biomarkers for prediction of breast cancer using anthropometric and clinical features: A comparative investigation in machine learning paradigm. Biocybern. Biomed. Eng. 2019, 39, 393–409. [Google Scholar] [CrossRef]
- Deng, J.; Dong, W.; Socher, R.; Li, L.J.; Li, K.; Fei-Fei, L. Imagenet: A large-scale hierarchical image database. In Proceedings of the 2009 IEEE Conference on Computer Vision and Pattern Recognition, Miami, FL, USA, 20–25 June 2009; pp. 248–255. [Google Scholar]
- Bottou, L. Large-scale machine learning with stochastic gradient descent. In Proceedings of the COMPSTAT’2010, Paris, France, 22–27 August 2010; Springer: Paris, France, 2010; pp. 177–186. [Google Scholar]
- Lin, T.Y.; Goyal, P.; Girshick, R.; He, K.; Dollár, P. Focal loss for dense object detection. In Proceedings of the IEEE International Conference on Computer Vision, Venice, Italy, 22–29 October 2017; pp. 2980–2988. [Google Scholar]
- Kingma, D.P.; Ba, J. Adam: A method for stochastic optimization. arXiv 2014, arXiv:1412.6980. [Google Scholar]
- Paszke, A.; Gross, S.; Massa, F.; Lerer, A.; Bradbury, J.; Chanan, G.; Killeen, T.; Lin, Z.; Gimelshein, N.; Antiga, L.; et al. Pytorch: An imperative style, high-performance deep learning library. arXiv 2019, arXiv:1912.01703. [Google Scholar]
- Lanza, E.; Muglia, R.; Bolengo, I.; Santonocito, O.G.; Lisi, C.; Angelotti, G.; Morandini, P.; Savevski, V.; Politi, L.S.; Balzarini, L. Quantitative Chest CT analysis in COVID-19 to predict the need for oxygenation support and intubation. Eur. Radiol. 2020, 30, 6770–6778. [Google Scholar] [CrossRef] [PubMed]
| COVID-19_CHDSET | Training Set | Testing Set | Total |
|---|---|---|---|
| moderate risk | 94 | 24 | 118 |
| severe risk | 374 | 94 | 468 |
| extreme risk | 31 | 9 | 40 |
| Total | 499 | 127 | 626 |
| COVID-19_CHDSETOS | Training Set | Testing Set | Total |
| moderate risk | 332 | 24 | 356 |
| severe risk | 374 | 94 | 468 |
| extreme risk | 341 | 9 | 350 |
| COVID-19_CHDSETUS | Training Set | Testing Set | Total |
| moderate risk | 31 | 9 | 40 |
| severe risk | 31 | 9 | 40 |
| extreme risk | 31 | 9 | 40 |
| mDice (%) | mIoU (%) | |
|---|---|---|
| Lesion Seg. | 97.8 (+1.1–7.9%) | 95.6 (+1.5–8.7%) |
| Acc (%) ↑ | Sens (%) ↑ | Spec (%) ↑ | F1 (%) ↑ | ||
|---|---|---|---|---|---|
| 3D | ResNet2Plus1D-VoI | 79.58 | 70.29 | 83.67 | 70.02 |
| ResNet2Plus1D-SSoI | 74.01 | 33.33 | 66.67 | 28.35 | |
| 2D | DenseNet201-VoI | 81.42 | 84.45 | 87.32 | 78.82 |
| DenseNet201-SSoI | 82.85 | 81.37 | 87.54 | 79.15 |
| Model | Acc (%) ↑ | Sens (%) ↑ | Spec (%) ↑ | F1 (%) ↑ | |
|---|---|---|---|---|---|
| 3D | ResNet2Plus1D-VoI | 62.90 | 62.90 | 81.4 | 63.06 |
| ResNet2Plus1D-SSoI | 33.33 | 33.33 | 66.66 | 16.66 | |
| 2D | DenseNet201-VoI | 88.88 | 89.77 | 94.73 | 88.88 |
| DenseNet201-SSoI | 82.33 | 82.57 | 90.89 | 82.33 | |
| Radiologists | 40.74 | 39.19 | 70.37 | 39.05 |
| Model | Acc (%) ↑ | Sens (%) ↑ | Spec (%) ↑ | F1 (%) ↑ | |
|---|---|---|---|---|---|
| 3D | ResNet3D-VoI | 66.67 | 66.67 | 83.31 | 65.85 |
| ResNet3D-RVoI | 72.54 | 51.97 | 77.58 | 52.32 | |
| MixedConv-VoI | 51.85 | 51.85 | 75.92 | 45.71 | |
| MixedConv-RVoI | 66.2 | 46.35 | 73.10 | 45.78 | |
| ResNet2Plus1D-VoI | 62.90 | 62.90 | 81.4 | 63.06 | |
| ResNet2Plus1D-RVoI | 42.85 | 33.33 | 66.66 | 20.00 | |
| ResNet2Plus1D-Volume | 33.33 | 33.33 | 66.66 | 16.66 | |
| 2D | ResNet101-RVoI | 76.42 | 83.80 | 86.35 | 76.42 |
| ResNet101-VoI | 85.18 | 85.60 | 92.32 | 85.60 | |
| DenseNet201-RVoI | 77.77 | 80.68 | 89.47 | 78.88 | |
| DenseNet201-VoI | 88.88 | 89.77 | 94.73 | 88.88 | |
| DenseNet201-Volume | 72.14 | 72.68 | 79.58 | 61.33 |
| Acc (%) ↑ | Sens (%) ↑ | Spec (%) ↑ | F1 (%) ↑ | ||
|---|---|---|---|---|---|
| 3D | ResNet3D-VoI | 80.99 | 71.14 | 82.93 | 71.11 |
| ResNet3D-RVoI | 68.31 | 52.32 | 73.69 | 52.32 | |
| MixedConv-VoI | 76.76 | 67.31 | 82.07 | 65.85 | |
| MixedConv-RVoI | 67.61 | 57.47 | 75.64 | 55.55 | |
| ResNet2Plus1D-VoI | 79.58 | 70.29 | 83.67 | 70.02 | |
| ResNet2Plus1D-RVoI | 71.83 | 42.11 | 73.71 | 41.82 | |
| ResNet2Plus1D-Volume | 68.84 | 33.33 | 66.67 | 27.18 | |
| 2D | ResNet101-RVoI | 76.00 | 66.30 | 77.44 | 69.86 |
| ResNet101-VoI | 76.42 | 83.80 | 86.35 | 77.27 | |
| DenseNet201-RVoI | 74.29 | 74.27 | 81.80 | 74.29 | |
| DenseNet201-VoI | 81.42 | 84.45 | 87.32 | 78.82 | |
| DenseNet201-Volume | 68.10 | 53.07 | 69.98 | 46.45 |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Chatzitofis, A.; Cancian, P.; Gkitsas, V.; Carlucci, A.; Stalidis, P.; Albanis, G.; Karakottas, A.; Semertzidis, T.; Daras, P.; Giannitto, C.; et al. Volume-of-Interest Aware Deep Neural Networks for Rapid Chest CT-Based COVID-19 Patient Risk Assessment. Int. J. Environ. Res. Public Health 2021, 18, 2842. https://doi.org/10.3390/ijerph18062842
Chatzitofis A, Cancian P, Gkitsas V, Carlucci A, Stalidis P, Albanis G, Karakottas A, Semertzidis T, Daras P, Giannitto C, et al. Volume-of-Interest Aware Deep Neural Networks for Rapid Chest CT-Based COVID-19 Patient Risk Assessment. International Journal of Environmental Research and Public Health. 2021; 18(6):2842. https://doi.org/10.3390/ijerph18062842
Chicago/Turabian StyleChatzitofis, Anargyros, Pierandrea Cancian, Vasileios Gkitsas, Alessandro Carlucci, Panagiotis Stalidis, Georgios Albanis, Antonis Karakottas, Theodoros Semertzidis, Petros Daras, Caterina Giannitto, and et al. 2021. "Volume-of-Interest Aware Deep Neural Networks for Rapid Chest CT-Based COVID-19 Patient Risk Assessment" International Journal of Environmental Research and Public Health 18, no. 6: 2842. https://doi.org/10.3390/ijerph18062842
APA StyleChatzitofis, A., Cancian, P., Gkitsas, V., Carlucci, A., Stalidis, P., Albanis, G., Karakottas, A., Semertzidis, T., Daras, P., Giannitto, C., Casiraghi, E., Sposta, F. M., Vatteroni, G., Ammirabile, A., Lofino, L., Ragucci, P., Laino, M. E., Voza, A., Desai, A., ... Savevski, V. (2021). Volume-of-Interest Aware Deep Neural Networks for Rapid Chest CT-Based COVID-19 Patient Risk Assessment. International Journal of Environmental Research and Public Health, 18(6), 2842. https://doi.org/10.3390/ijerph18062842












