Sex Education in the Spotlight: What Is Working? Systematic Review
Abstract
1. Introduction
2. Methodology
2.1. Aims
2.2. Methods
2.3. Search Strategy
2.4. Inclusion Criteria
2.5. Exclusion Criteria
- Their primary focus was adult people and adolescents were not included.
- Their primary focus was sexual-health screening, sexual abuse or assault or prevention of sexual abuse or rape.
- The studies targeted specific populations (e.g., pre-pubertal children, children with developmental disorders, migrant and refugee, or sexual minorities).
- The interventions focused on low- and middle-income countries or if high income countries were not included in the study.
- Recipients were professionals, teachers, parents or a combination of the latter.
2.6. Risk of Bias and Assessment of Study Quality
2.7. Data Synthesis
3. Results
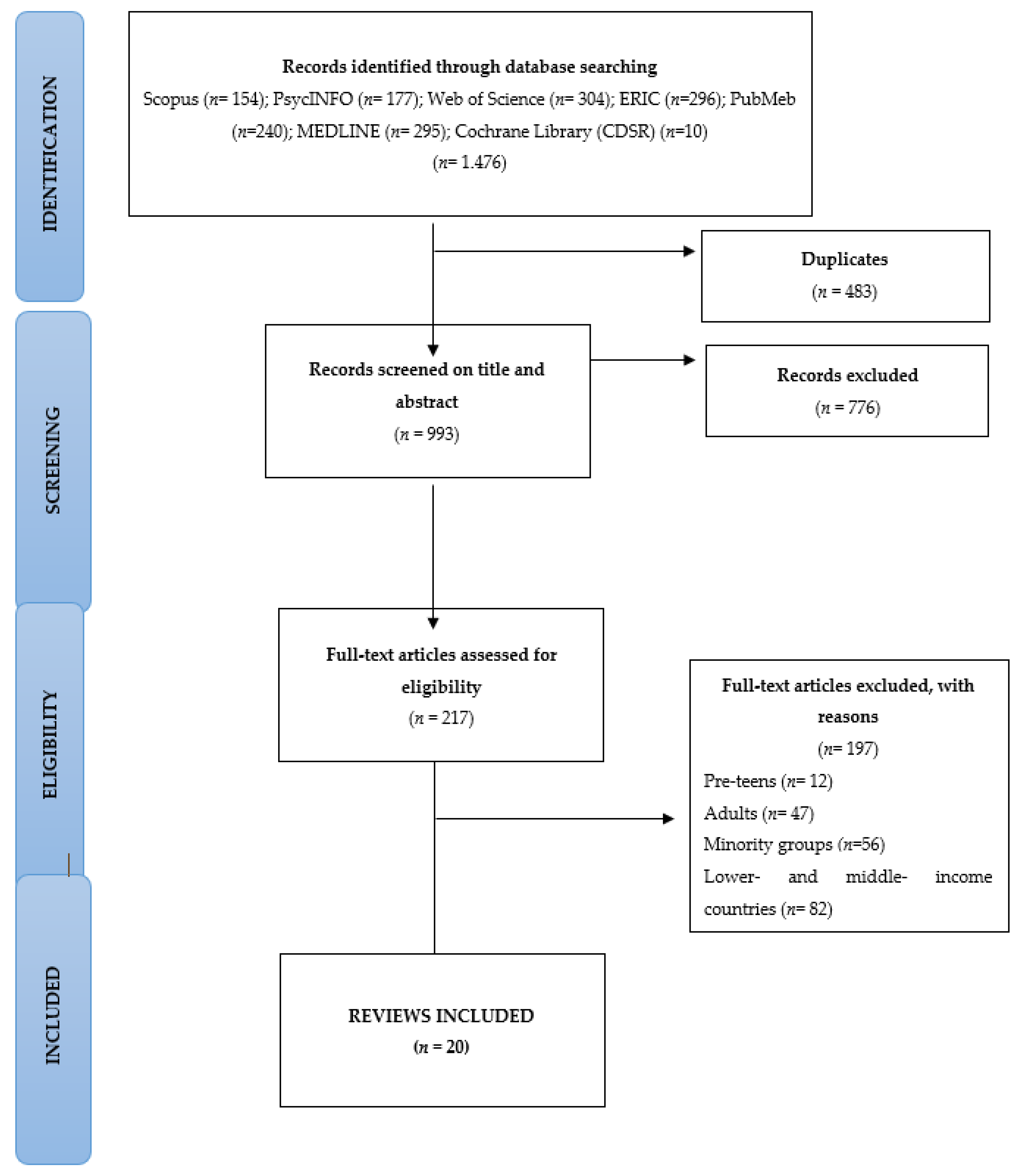
3.1. Results of Search
3.2. Risk of Bias in Included Studies
3.3. Reviews Included
3.3.1. Setting
3.3.2. Population
3.3.3. Interventions/Types of Study
3.3.4. Outcomes
3.3.5. Country of Review
3.3.6. Year of Last Paper Included
3.3.7. Search Tools
3.3.8. Multicenter Studies and Number of Studies Included
3.3.9. Number of Reviews Covered That Include Meta-Analysis
3.4. Effectiveness
3.4.1. School Settings
3.4.2. Online Platforms
3.4.3. Blended Learning
4. Discussion
4.1. Interventions Reviewed
4.2. Effectiveness
4.3. Limitations
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
Appendix A
| Characteristic | Search Terms |
|---|---|
| Sex education | “sex education” OR “sexuality education” OR “sex education program” OR “sexuality education program” OR “reproductive education” OR “Sexual health education” OR “reproductive health education” OR “sexual and reproductive health” OR “sexual health” |
| Study population (adolescents) | “adolescent” OR “adolescents” OR “teenagers” OR “young people” OR “young person” OR “primary students” OR “Secondary Students” OR “student” |
| Setting (school, online, blended learning) | “internet” OR “online” OR “offline” OR “virtual” OR “digital” OR “computer” OR “computer-technology” OR “technology” OR “computerized” OR “internet-based intervention” OR “computer based approach” OR “computer-assisted education” OR “school” OR “school-based” OR “K-12 setting” OR “school based programs” or “school setting” OR “blended learning” |
| Evaluation (review of reviews) | “evaluation” OR “assessment” OR “impact” OR “intervention” OR “impact evaluation” OR “outcome evaluation” OR “process evaluation” OR “comparative effectiveness research” OR “review” OR “review of reviews” OR “systematic reviews” OR “narrative reviews” |
| School | ||||||||
| Authors/Year | Title | Country of the Review | Search Tools | Cover Period | Year of last Paper Included | Last Paper Included | Country of the Studies Included | Synthesis |
| Chokprajakchad et al. (2018) | Sexual Health Interventions Among Early Adolescents: An Integrative Review. | Thailand | PubMed, CINAHL, Scopus, Science Direct, Web of Science, Thaijo and TCI. | 2006–2017 | 2016 | 33 studies | International. | Narrative |
| Goldfarb et al. (2020) | Three Decades of Research: The Case for Comprehensive Sex Education. | USA | ERIC, Psycinfo and MEDLINE. | 1990–2017 | 2017 | 80 studies | USA (n = 55), Israel (n = 1), Canada (n = 6), Australia (n = 3), New Zealand (n = 1), The Netherlands (n = 2) Kenya (n = 1), Mexico (n = 2), South Africa (n = 1), Ireland (n = 2), South Korea (n = 1), China (n = 1), Holland (n = 1) U.K (n = 1), Europe (n = 2). | Narrative |
| Haberland et al. (2016) | The Case for Addressing Gender and Power in Sexuality and HIV Education: A Comprehensive Review of Evaluation Studies. | USA | PubMed, ERIC, Cochrane Central Register of Controlled Trials and Eldis. | 1990–2012 | 2011 | 22 studies | USA (n = 14). High income countries other than the United States (n = 2). Low or middle income country (n = 6). | Meta-analysis (one outcome) and Narrative |
| Kedzior et al. (2020) | A Systematic Review of School-Based Programs to Improve Adolescent Sexual and Reproductive Health: Considering The Role of Social Connectedness. | Australia | PubMed, CINAHL, Embase, Psycinfo, ERIC and SCOPUS. | July 2019 | 2017 | 18 studies | International. | Narrative |
| Lopez et al. (2016) | School-Based Interventions for Improving Contraceptive Use in Adolescents. | USA | PubMed, CENTRAL, ERIC, Web of Science and POPLINE. | 1981–2016 | 2014 | 11 studies | USA (n = 6). U.K (n = 1). Mexico (n = 3). South Africa (n = 1). | Narrative |
| Marseille et al. (2018) | Effectiveness of School-Based Teen Pregnancy Prevention Programs in The USA: A Systematic Review and Meta-Analysis. | USA | Cochrane Central, ERIC, PubMed, Psycinfo, Scopus, Web of Science and The Gray Literature. | 1985–2017 | 2016 | 21 studies | USA (n = 14). Canada (n = 4). | Meta-analysis |
| Mason-Jones et al. (2016) | School-Based Interventions for Preventing HIV, Sexually Transmitted Infections, and Pregnancy in Adolescents. | United Kingdom | MEDLINE, CENTRAL, OMS, AIDS, AEGIS, CDC, and ONUSIDA. | 1990–2016 | 2015 | 8 studies | Sub-Saharan Africa: (South Africa, Tanzania Zimbabwe, Malawi Kenya) n = 5, Europe: (England and Scotland) n = 2, Latin America (n = 1). | Meta-analysis |
| Mirzazadeh et al. (2018) | Do School-Based Programs Prevent HIV and Other Sexually Transmitted Infections in Adolescents? A Systematic Review and Meta-Analysis. | USA | PubMed, Cochrane Central Register of Controlled Trials, ERIC, Psycinfo, Scopus, Web ofScience andThe Gray Literature. | May 2017 | 2017 | 9 studies | USA (n = 9). | Meta-analysis |
| Oringanje et al. (2016) | Interventions for Preventing Unintended Pregnancies Among Adolescents | USA | CENTRAL, The Cochrane Library, MEDLINE, EMBASE, LILACS, Social Science Citation Index and Science Citation Index, Dissertations Abstracts Online, Network, HealthStar, Psycinfo, CINAHL, POPLINE and The Gray Literature | 1994–2015 | 2015 | 53 studies | USA (n = 41), England (n = 2), Scotland (n = 2), Canada (n = 1), Italy (n = 1), Mexico (n = 2), Low and middle income countries (n = 4). | Narrative |
| Peterson et al. (2019) | Effects of Interventions Addressing School Environments or Educational Assets on Adolescent Sexual Health: Systematic Review and Meta-Analysis. | USA | BiblioMap, CINAHL Plus, ERIC, IBSS, Open Grey, ProQuest, Psycinfo, Medline and Web of Science. | 1999–2016 | 2016 | 11 studies | Australia and USA (n = 5), South Africa and Kenya (n = 4), Malawi and Zimbabwe (n = 2). | Meta-analysis and narrative |
| Online | ||||||||
| Authors/Year | Title | Country of the review | Search tools | Cover period | Year of last paper included | Last paper included | Country of the included studies | Synthesis |
| Bailey et al. (2015) | Sexual Health Promotion for Young People Delivered Via Digital Media: A Scoping Review. | United Kingdom | CENTRAL, DARE, MEDLINE, EMBASE, CINAHL, BNI, Psycinfo and The Gray Literature. | 1989–2013 | 2013 | 19 studies | United Kingdom (n = 19). | Meta-analysis andNarrative |
| Celik et al. (2020) | The Effect of Technology-Based Programmes On Changing Health Behaviours of Adolescents: Systematic Review. | Turkey | PubMeb and Science direct databases. | 2011–2016 | 2016 | 16 studies | Canada (n = 2), New Zealand (n = 1), Australia (n = 3), Norway (n = 1), USA (n = 9). | Narrative |
| Desmet et al. (2015) | A Systematic Review and Meta-Analysis of Interventions for Sexual Health Promotion Involving Serious Digital Games. | Belgium | PubMed, Web of Science, CINAHL and Psycinfo. | July 2013 | 2012 | 7 studies | USA (n = 6), United Kingdom (n = 1). | Meta-analysis |
| Holstrom (2015) | Sexuality Education Goes Viral: What We Know About Online Sexual Health Information. | USA | Medline, EBSCO, ERIC and PubMed. The EBSCO. | 2004–2014 | 2012 | 5 studies | USA (n = 3), Australia (n = 1), Europe (n = 1). | Narrative |
| L’Engle et al. (2016) | Mobile Phone Interventions for Adolescent Sexual and Reproductive Health: A Systematic Review. | USA | PubMed, Embase, Global Health, Psycinfo, Popline, Cochrane Library, Web of Science and The Gray Literature. | 2000–2014 | 2014 | 35 studies | USA (n = 35). | Narrative |
| Martin et al. (2020) | Participatory Interventions for Sexual Health Promotion for Adolescents and Young Adults on The Internet: Systematic Review. | France | PubMeb, Aurore database and The Gray Literature. | 2006–2019 | 2019 | 60 studies | USA (n = 38), Canada (n = 1), United Kingdom (n = 4), Netherlands (n = 1), Europe (n = 2). Australia (n = 3), Uganda (n = 4), Brazil (n = 2), Chile (n = 2), Asia (n = 3), | Narrative |
| Palmer et al. (2020) | Targeted Client Communication Via Mobile Devices for Improving Sexual and Reproductive Health. | United Kingdom | Cochrane Central Register of Controlled Trials, MEDLINE, POPLINE, WHO Global Health Library and The Gray Literature. | July 2019 | 2017 | 33 studies | Colombia (n = 1), China (n = 2), Australia (n = 2), USA (n = 9), U.K. (n = 2), Peru (n = 1), Lower middle income (n = 16). | Meta-analysis AndNarrative |
| Wadham et al. (2019) | New Digital Media Interventions for Sexual Health Promotion Among Young People: A Systematic Review. | Australia | CINAHL, Medline, Psycinfo, Socindex, Informit, PubMed and Scopus. | 2010–2017 | 2016 | 25 studies | USA (n = 16), Canada (n = 1), Netherlands (n = 2), Australia (n = 2), African American communities (n = 1), Chile (n = 1), Uganda (n = 1), Thailand (n = 1). | Narrative |
| Widman et al. (2018) | Technology-Based Interventions to Reduce Sexually Transmitted Infections and Unintended Pregnancy Among Youth. | USA | Medline, Psycinfo and Communication Source. | May 2017 | 2015 | 16 studies | USA (n = 16). | Meta-analysis |
| Blended Learning | ||||||||
| Authors/Year | Title | Country of the Review | Search Tools | Cover Period | Year of last Paper Included | Last Paper Included | Country of the Included Studies | Synthesis |
| Coyle et al. (2019) | Blended Learning for Sexual Health Education: Evidence Base, Promising Practices, and Potential Challenges. | USA | Google Scholar, PubMed and the Cumulative Index of Nursing. | 2000–2017 | 2015 | 9 studies | USA (n = 6), U.K (n = 2), Europe (n = 1). | Narrative |
| School | |||||
| Authors/Year | Objective | Participants | Type of Study | Outcomes | Results |
| Chokprajakchad et al. (2018) | To describe and analyze methodological and substantive features of research on interventions to delay the initiation of sexual intercourse and prevent other sexual risk behaviors among early adolescents. | 10–13 years | 14 studies used randomized controlled trials (RCTs), 16 used quasi-experimental designs and three used a pre-test, post-test design. | PRIMARY (a) Adolescent sexual behavior. (b) Initiation of sexual activity. (c) Condom use and other. Contraceptive use. SECONDARY (a) Adolescents’ attitudes. (b) Self-efficacy. (c) Intentions related to sexual behavior. |
|
| Goldfarb et al. (2020) | To find evidence for the effectiveness of comprehensive sex education in school-based programs. | 3–18 years | Randomized controlled trial (RCTs), quasi-experimental, and pre- and post-test. | PRIMARY (a) Appreciation of sexual diversity: Homophobia, homophobic bullying, understanding of gender/gender norms, recognition of gender equity, rights, and social justice. (b) Dating and intimate partner violence prevention: Knowledge and attitudes about, and reporting of, DV and IPV; DV and IPV perpetration and victimization; bystander, intentions and behaviors. (c) Healthy Relationships. Knowledge, attitudes, and skills and intentions. (d) Child sex abuse prevention: Knowledge, attitudes, skills and social-emotional outcomes related to personal safety and touch. (e) Additional outcomes Social emotional learning. Media literacy. |
|
| Haberland et al. (2016) | Evaluation of behavior-change interventions to prevent HIV, STIs or unintended pregnancy to analyze whether addressing gender and power in sexuality education curricula is associated with better outcomes. | Adolescents under 19 years | Randomized Controlled Trials (RCTs) or quasi-experimental. | PRIMARY (a) STIs. (b) HIV. (c) Pregnancy. (d) Childbearing. |
|
| Kedzior et al. (2020) | Determine the impact of school-based programs that promote social connectedness on adolescent sexual and reproductive health. | 10–19 years | Randomized controlled trials, non-randomized controlled trials (including quasi), controlled before-after (pre-/post-) interrupted time series, and program evaluations. Program evaluation without a control group were eligible if they reported on outcomes pre- and post- program implementation. | PRIMARY (a) Contraception use. (b) Intercourse (frequency or another outcome as defined by authors). (c) Risk of adolescent pregnancy and birth. (d) Rates of sexually transmissible infections (STIs). (e) Attitudes, beliefs and knowledge about sex and reproductive health. (f) Autonomy. (g) Connectedness. |
|
| Lopez et al. (2016) | To identify school-based interventions that improved contraceptive use among adolescents. | 19 years or younger | Randomized controlled trials (RCTs). (Of 11 trials, 10 were cluster randomized). | PRIMARY (a) Pregnancy (six months or more after the intervention began). (b) Contraceptive use (three months or more after the intervention began). SECONDARY (a) Knowledge of contraceptive effectiveness or effective method use. (b) Attitude about contraception or a specific contraceptive method. |
|
| Marseille et al. (2018) | To evaluate the effectiveness of school-based teen pregnancy prevention programs in the USA. | 10–19 years | Randomized controlled trials (RCTs) (10 studies) and non-RCTs (11 studies) with comparator groups were eligible yielded 30 unique pooled comparisons for pregnancy. | PRIMARY Pregnancy. SECONDARY (a) Sexual Initiation. (b) Condom Use. (c) Oral Contraception Pill Use. |
|
| Mason-Jones et al. (2016) | To evaluate the effects of school-based sexual and reproductive health programs on sexually transmitted infections (such as HIV, herpes simplex virus, and syphilis), and pregnancy among adolescents. | 10–19 years | Randomized Controlled Trials (RCTs) (both individually randomized and cluster-randomized included 8 cluster-RCTs). | PRIMARY Clinical/biological outcomes: (a) HIV prevalence. (b) STI prevalence. (c) Pregnancy prevalence. Behavioral self-reported outcomes: (a) Use of male condoms at first sex. (b) Use of male condoms at most recent (last) sex. (c) Initiation (sexual debut). |
|
| Mirzazadeh et al. (2018) | To evaluate the effectiveness of school-based programs prevent HIV and other sexually Transmitted Infections in adolescents in the USA. | 10–19 years | Three RCTs and six non-RCTs describing seven interventions. | PRIMARY (a) HIV/STI incidence or prevalence. (b) HIV/STI testing. SECONDARY (a) Frequency of intercourse. (b) Number of partners. (c) Initiation of sexual intercourse. (d) Sex without a condom. (e) HIV/STI knowledge, attitude, and behavior. |
|
| Oringanje et al. (2016) | To assess the effects of primary prevention interventions (school-based, community/home-based, clinic-based, and faith-based) on unintended pregnancies among adolescents. | 10–19 years | 53 Randomized Controlled Trials (RCTs) comparing these interventions to various control groups (mostly usual standard sex education offered by schools). | PRIMARY (a) Unintended pregnancy. SECONDARY (a) Reported changes in knowledge and attitudes about the risk of unintended pregnancies. (b) Initiation of sexual intercourse. (c) Use of birth control methods. (d) Abortion. (e) Childbirth. (f) Morbidity related to pregnancy, abortion or child birth. (g) Mortality related to pregnancy, abortion or childbirth. (h) Sexually transmitted infections (including HIV). |
|
| Peterson et al. (2019) | To examine whether interventions, addressing school-level environment or student-level educational assets, can promote young people’s sexual health. | 10–19 years | Randomized trial or quasi experimental design, in which control groups received usual treatment or a comparison intervention, and they must have reported at least one sexual health outcome, such as pregnancy, STDs or sexual behaviors associated with increased risk of pregnancy or STDs. | PRIMARY Interventions designed specifically to improve: (a) Knowledge. (b) Attitudes. (c) Skills. (d) Services related to sexual health. |
|
| Online | |||||
| Authors/Year | Objective | Participants | Type of Study | Outcomes | Results |
| Bailey et al. (2015) | To summarize evidence on effectiveness, cost-effectiveness and mechanism of action of interactive digital interventions (IDIs) for sexual health; optimal practice for intervention development; contexts for successful implementation; research methods for digital intervention evaluation; and the future potential of sexual health promotion via digital media. | 12–19 years | Randomized controlled trials (RCTs). | PRIMARY (a) Sexual health knowledge. (b) Self-efficacy. (c) Intention/motivation. (d) Sexual behavior and biological. |
|
| Celik et al. (2020) | To determine the effect of technology-based programmes in changing adolescent health behaviors. | 10–24 years | Randomized control group. | PRIMARY Adolescents’ health-promoting behaviors: pregnancy, HIV/disease-related knowledge, condom use, condom intentions, condom skills, self-efficacy, and related infectious diseases risk behavior. |
|
| Desmet et al. (2015) | To analyze the effectiveness of interventions for sexual health promotion that use serious digital games. | 13–29 years | Randomized control group, and randomized on an individual. | PRIMARY Behavior, knowledge, behavioral intention, perceived environmental constraints, skills, attitudes, subjective norm, and self-efficacy. SECONDARY Clinical effects (e.g., rates of sexually transmitted infections). |
|
| Holstrom (2015) | To draw a more comprehensive picture of how online sexual health interventions do and do not align with real world habits and interests of adolescents. | 10–24 years | Randomized controlled trials (RCTs), and focus groups participants. | PRIMARY (a) Sexual Health information. (b) What topics they want to know about. (c) Evaluations of Internet-based sexual health interventions. |
|
| L’Engle et al. (2016) | To assess strategies, findings, and quality of evidence on using mobile phones to improve adolescent sexual and reproductive health (ASRH). | 13–24 years | Randomized controlled trials (RCTs), quasi-experimental, observational, or descriptive research. | PRIMARY (a) Promote positive and preventive SRH behaviors. (b) Increase adoption and continuation of contraception. (c) Support medication adherence for HIV-positive young people. (d) Encourage use of health screening and treatment services. |
|
| Martin et al. (2020) | To describe existing published studies on online participatory intervention methods used to promote the sexual health of adolescents and young adults. | 10–24 years | 16 Randomized Controlled Trial (RCT), 15 Control group (NI = 2), 4 Information-only control website, 7 Before-after study (no RCT), 3 Cross-sectional study, 8 other design, 3 Unspecified. | PRIMARY Process outcomes evaluated: Acceptability, Attractiveness, Feasibility, Satisfaction and Implementation. Outcomes evaluation conducted: Behaviors. Condom use, condom use intention, self-efficacy toward condom use, and attitude toward condom use attitudes. Communication. Knowledge. Behavioral skills. Self-efficacy. Contraception use. History of sexually transmitted infections. HIV stigma. HIV test history (date and result of the last test). Incidence of sexually transmitted infections. Intentions related to risky sexual activity. Internalized homophobia. Intimate partner violence. Motivation. Pubertal development. Sexual abstinence. Waiting before having sex. |
|
| Palmer et al. (2020) | To assess the effects of targeted client communication via delivered via mobile devices on adolescents’ knowledge, and on adolescents’ and adults’ sexual and reproductive health behavior, health service use, and health and well-being. | 10 -24 years | Randomized controlled trials (RCTs). | PRIMARY Health behavior change: • STI/HIV prevention. • STI/HIV treatment. • Contraception/family planning. • Pre-conception care. • Partner violence. Service utilization: • STI/HIV prevention/treatment. • Contraception/family planning. • HPV vaccination. • Cervical screening. • Pre-conception care. Partner violence: • Use of services designed for those who have experienced partner violence. Health status and well-being: • STI/HIV prevention. • STI/HIV treatment. • Contraception/family planning. • Partner violence. • Well-being. Any measure of knowledge or attitudes relating to the following: • STI prevention and/or treatment. • Contraception/family planning. • Cervical cancer screening. • Sexual violence. • HPV vaccination. • Puberty. SECONDARY •Patient/client acceptability and satisfaction with the intervention. •Resource use, including cost to the system and unintended consequences. |
|
| Wadham et al. (2019) | To assess the effectiveness of sexual health interventions delivered via new digital media to young people. | 12–24 years | Randomized to a control group and pre-/post-test evaluation design, uncontrolled longitudinal studies and the remaining studies comprised a mixture of qualitative cohort, observational and mixed methods. | PRIMARY (a) Behavior (number of sexual partners, number of unprotected sexual acts, frequency of condom use, negotiation skills for condom use, sex under the influence of alcohol and other drugs, testing seeking behavior). (b) Self-efficacy (condom use). (c) Skills and Abilities (sexual communication and risk assessment). (d) Intentions (to use condoms). (e) Attitudes. (f) Knowledge (HIV, STI, general sexual health). (g) Efficacy of the Intervention (feasibility, acceptability, usability, satisfaction). (h) Well-being (mental health, sexuality, self-acceptance). |
|
| Widman et al. (2018) | To synthesize the technology-based sexual health interventions among youth people to determine their overall efficacy on two key behavioral outcomes: condom use and abstinence. | 13–24 years | Randomized to a control group and experimental or quasi-experimental design. | PRIMARY (a) Condom use (b) Abstinence. SECONDARY (a) Safer sex attitudes. (b) Social norms for safer sexual activity. (c) self-efficacy. (d) Behavioral intentions to practice safer sex. (e) Sexual health knowledge. |
|
| Blended Learning | |||||
| Authors/Year | Objective | Participants | Type of Study | Outcomes | Results |
| Coyle et al. (2019) | To identify sexual health education studies using blended learning to summarize the best practices and potential challenges. | 13–24 years, and adults of over 25 | Randomized Controlled Trials (RCTs). | PRIMARY (a) Initiation of sexual intercourse (vaginal, oral or anal intercourse). (b) Other sexual risk behaviors (condom use, communication, condom use skills, frequency of sex, unprotected sex, number of partners with whom had sex without protection, frequency of using alcohol and or other substances during sex). (c) Sexual coercion or dating violence (sexual coercion, dating violence). (d) Sexuality-related psychosocial factors (attitudes, beliefs, perceptions regarding abstinence, and protection). (e) Perceived satisfaction and usability (of blended learning). |
|
| School | |||||||||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| Authors | 1 1 | 2 | 3 | 4 | 5 | 6 | 7 | 8 | 9 | 10 | 11 | 12 | 13 | 14 | 15 | 16 | Overall Rating 2 |
| Chokprajakchad et al. (2018) | Y | N | Y | Y | N | N | N | Y | N | N | NM | NM | N | Y | NM | N | CL |
| Goldfarb et al. (2020) | Y | Y | N | Y | Y | Y | Partial Y | Y | N | N | NM | NM | N | Y | NM | Y | CL |
| Haberland et al. (2016) | Y | Y | Y | Y | N | N | N | Partial Y | N | N | NM | NM | N | Y | NM | N | CL |
| Kedzior et al. (2020) | Y | Y | Y | Y | Y | Y | Partial Y | Y | Y | N | NM | NM | Y | Y | NM | Y | M |
| Lopez et al. (2016) | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | NM | NM | Y | Y | NM | Y | H |
| Marseille et al. (2018) | Y | Y | Y | Y | Y | Y | Y | Y | Y | N | Y | Y | Y | Y | Y | Y | H |
| Mason-Jones et al. (2016) | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | H |
| Mirzazadeh et al. (2018) | Y | Y | Y | Y | Y | Y | Y | Y | Y | N | Y | Y | Y | Y | Y | Y | H |
| Oringanje et al. (2016) | Y | Y | Y | Y | Y | Y | Y | Y | Y | N | NM | NM | Y | Y | NM | Y | H |
| Peterson et al. (2019) | Y | Y | Y | Y | Y | Y | N | Y | Y | N | Y | Y | Y | Y | Y | N | L |
| Online | |||||||||||||||||
| Bailey et al. (2015) | Y | Y | Y | Y | Y | Y | N | Y | Y | N | Y | Y | Y | Y | Y | Y | L |
| Celik et al. (2020) | Y | Y | Y | N | N | N | Y | Y | N | N | NM | NM | N | Y | NM | Y | CL |
| DeSmet et al. (2015) | Y | Partial Y | Y | Y | Y | Y | N | Y | Partial Y | N | Y | Y | Y | Y | N | Y | CL |
| Holstrom (2015) | N | N | N | Y | N | N | N | Y | N | N | NM | NM | N | N | NM | N | CL |
| L´Engle et al. (2016) | Y | Y | Y | Y | Y | Y | Partial Y | Partial Y | N | Y | NM | NM | N | Y | NM | Y | CL |
| Martin et al. (2020) | Y | Y | Y | Y | Y | Y | Y | Y | N | N | NM | NM | N | Y | NM | Y | CL |
| Palmer et al. (2020) | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | H |
| Wadham et al. (2019) | N | Y | Y | Y | Partial Y | Partial Y | N | Y | N | N | NM | NM | N | N | NM | Y | CL |
| Widman et al. (2018) | Y | Y | Y | Y | Y | Y | Partial Y | Partial Y | Y | N | Y | Y | N | Y | Y | Y | L |
| Blended Learning | |||||||||||||||||
| Coyle et al. (2019) | Y | N | N | Y | N | N | N | Y | N | N | NM | NM | N | Y | NM | N | CL |
References
- WHO. The Health of Youth. Geneva 1989. Available online: https://www.who.int/maternal_child_adolescent/documents/pdfs/9241591269_op_handout.pdf (accessed on 12 November 2020).
- Anderson, R.M. Positive sexuality and its impact on overall well-being. Bundesgesundheitsbl 2013, 56, 208–214. [Google Scholar] [CrossRef]
- WHO. Defining Sexual Health Report of a Technical Consultation on Sexual Health, Geneva 2006. Available online: https://www.who.int/reproductivehealth/topics/gender_rights/defining_sexual_health.pdf (accessed on 15 November 2020).
- UN. Agenda 2030 para el Desarrollo Sostenible. 2015. Available online: https://www.un.org/sustainabledevelopment/es/2015/09/la-asamblea-general-adopta-la-agenda-2030-para-el-desarrollo-sostenible/ (accessed on 9 April 2020).
- Blanc, M.A.; Rojas, T.A. Condom use, number of partners and sexual debut in young people in penile-vaginal intercourse, oral sex and anal sex. Rev. Int. 2018, 16, 8. [Google Scholar]
- Magnusson, B.M.; Crandall, A.; Evans, K. Early sexual debut and risky sex in young adults: The role of low self-control. BMC Public Health 2019, 19, 1483. [Google Scholar] [CrossRef] [PubMed]
- Williams, E.A.; Jensen, R.E. Conflicted identification in the sex education classroom: Balancing professional values with organizational mandates. Qual. Health Res. 2016, 26, 1574–1586. [Google Scholar] [CrossRef]
- Ybarra, M.L.; Thompson, R.E. Predicting the emergence of sexual violence in adolescence. Prev. Sci. 2018, 19, 403–415. [Google Scholar] [CrossRef]
- Rodríguez-Castro, Y.; Alonso, P.; Lameiras, M.; Faílde, J.M. From sexting to cybercontrol among dating teens in Spain: An analysis of their arguments. Rev. Lat. Am. Psicol. 2018, 50, 170–178. [Google Scholar]
- Helmer, J.; Senior, K.; Davison, B.; Vodic, A. Improving sexual health for young people: Making sexuality education a priority. Sex Educ. 2015, 15, 158–171. [Google Scholar] [CrossRef]
- Lindberg, L.D.; Maddow-Zimet, I.; Boonstra, H. Changes in adolescents’ receipt of sex education, 2006–2013. J. Adolesc. Health 2016, 58, 621–627. [Google Scholar] [CrossRef] [PubMed]
- Garcia, L.; Fields, J. Renewed commitments in a time of vigilance: Sexuality education in the USA. Sex Educ. 2017, 17, 471–481. [Google Scholar] [CrossRef][Green Version]
- Kirby, D.B. The Impact of Abstinence and Comprehensive Sex and STD/HIV Education Programs on Adolescent Sexual Behavior. Sex. Res. Soc. Policy 2008, 5, 18–27. [Google Scholar] [CrossRef]
- Heels, S.W. The Impact of Abstinence-Only Sex Education Programs in the United States on Adolescent Sexual Outcomes. Perspectives 2019, 11, 3. [Google Scholar]
- Santelli, J.S.; Kantor, L.M.; Grilo, S.A.; Speizer, I.S.; Lindberg, L.D.; Heitel, J.; Ott, M.A. Abstinence-only-until-marriage: An updated review of US policies and programs and their impact. J. Adolesc. Health 2017, 61, 273–280. [Google Scholar] [CrossRef]
- Gardner, E.A. Abstinence-only sex education: College students’ evaluations and responses. Am. J. Sex. Educ. 2015, 10, 125–139. [Google Scholar] [CrossRef]
- UNESCO. International Technical Guidance on Sexuality Education. 2018. Available online: file:///C:/Users/Profesor/Desktop/260770eng.pdf (accessed on 14 October 2020).
- Bourke, A.; Boduszek, D.; Kelleher, C.; McBride, O.; Morgan, K. Sex education, first sex and sexual health outcomes in adulthood: Findings from a nationally representative sexual health survey. Sex Educ. 2014, 14, 299–309. [Google Scholar] [CrossRef]
- Denford, S.; Abraham, C.; Campbell, R.; Busse, H. A comprehensive review of reviews of school-based interventions to improve sexual-health. Health Psychol. Rev. 2017, 11, 33–52. [Google Scholar] [CrossRef]
- Gray, B.J.; Jones, A.T.; Couzens, Z.; Sagar, T.; Jones, D. University students’ behaviours towards accessing sexual health information and treatment. Int. J. Std Aids 2019, 30, 671–679. [Google Scholar] [CrossRef]
- WHO. Guideline on Digital Interventions for Health System Strengthening. 2019. Available online: file:///C:/Users/Profesor/Desktop/9789241550505-eng.pdf (accessed on 23 September 2020).
- Madden, M.; Lenhart, A.; Duggan, M.; Cortesi, S.; Gasser, U. Teens and Technology. Pew Research Center. 2013. Available online: http://www.pewinternet.org/files/oldmedia//Files/Reports/2013/PIPTeensandTechnology2013.pdf (accessed on 18 November 2020).
- Park, E.; Kwon, M. Health-related internet use by children and adolescents: Systematic review. J. Med Internet Res. 2018, 20, e120. [Google Scholar] [CrossRef]
- Eleuteri, S.; Rossi, R.; Tripodi, F.; Fabrizi, A.; Simonelli, C. Sexual health in your hands: How the smartphone apps can improve your sexual wellbeing? Sexologies 2018, 27, e57–e60. [Google Scholar] [CrossRef]
- Lim, M.S.; Vella, A.; Sacks-Davis, R.; Hellard, M.E. Young people’s comfort receiving sexual health information via social media and other sources. Int. J. Std. Aids 2014, 25, 1003–1008. [Google Scholar] [CrossRef]
- Widman, L.; Kamke, K.; Evans, R.; Stewart, J.L.; Choukas-Bradley, S.; Golin, C.E. Feasibility, acceptability, and preliminary efficacy of a brief online sexual health program for adolescents. J. Sex Res. 2020, 57, 145–154. [Google Scholar] [CrossRef]
- Garzón-Orjuela, N.; Samacá-Samacá, D.; Moreno-Chaparro, J.; Ballesteros-Cabrera, M.D.P.; Eslava-Schmalbach, J. Effectiveness of sex education interventions in adolescents: An overview. Compr. Child Adolesc. Nurs. 2020, 1–34. [Google Scholar] [CrossRef]
- Lindberg, L.D.; Bell, D.L.; Kantor, L.M. The Sexual and Reproductive Health of Adolescents and Young Adults During the COVID-19 Pandemic. Perspect. Sex. Reprod. Health 2020. [Google Scholar] [CrossRef]
- Johns Hopkins Coronavirus Resource Center. COVID-19 Map. 2021. Available online: https://coronavirus.jhu.edu/map.html (accessed on 14 January 2021).
- Decker, M.J.; Gutmann-Gonzalez, A.; Price, M.; Romero, J.; Sheoran, B.; Yarger, J. Evaluating the effectiveness of an intervention integrating technology and in-person sexual health education for adolescents (In the Know): Protocol for a cluster randomized controlled trial. JMIR Res. Protoc. 2020, 9, e18060. [Google Scholar] [CrossRef]
- Doubova, S.V.; Martinez-Vega, I.P.; Infante-Castañeda, C.; Pérez-Cuevas, R. Effects of an internet-based educational intervention to prevent high-risk sexual behavior in Mexican adolescents. Health Educ. Res. 2017, 32, 487–498. [Google Scholar] [CrossRef]
- Bowring, A.L.; Wright, C.J.; Douglass, C.; Gold, J.; Lim, M.S. Features of successful sexual health promotion programs for young people: Findings from a review of systematic reviews. Health Promot. J. Aust. 2018, 29, 46–57. [Google Scholar] [CrossRef]
- Bowring, A.L.; Veronese, V.; Doyle, J.S.; Stoove, M.; Hellard, M. HIV and sexual risk among men who have sex with men and women in Asia: A systematic review and meta-analysis. Aids Behav. 2016, 20, 2243–2265. [Google Scholar] [CrossRef] [PubMed]
- Kirby, D.B.; Laris, B.A.; Rolleri, L.A. Sex and HIV education programs: Their impact on sexual behaviors of young people throughout the world. J. Adolesc. Health 2007, 40, 206–217. [Google Scholar] [CrossRef]
- Shackleton, N.; Jamal, F.; Viner, R.M.; Dickson, K.; Patton, G.; Bonell, C. School-based interventions going beyond health education to promote adolescent health: Systematic review of reviews. J. Adolesc. Health 2016, 58, 382–396. [Google Scholar] [CrossRef]
- Collins, R.L.; Martino, S.C.; Shaw, R. Influence of New Media on Adolescent Sexual Health: Evidence and Opportunities (Working Paper). Rand Health. 2011. Available online: http://aspe.hhs.gov/hsp/11/AdolescentSexualActivity/NewMediaLitRev/index.pdf (accessed on 26 November 2020).
- Döring, N.M. The Internet’s impact on sexuality: A critical review of 15 years of research. Comput. Hum. Behav. 2009, 25, 1089–1101. [Google Scholar] [CrossRef]
- Simon, L.; Daneback, K. Adolescents’ use of the internet for sex education: A thematic and critical review of the literature. Int. J. Sex. Health 2013, 25, 305–319. [Google Scholar] [CrossRef]
- Talukdar, J. The prospects of a virtual sex education: A review. Am. J. Sex. Educ. 2013, 8, 104–115. [Google Scholar] [CrossRef]
- Hartmann, M.; Khosla, R.; Krishnan, S.; George, A.; Gruskin, S.; Amin, A. How are gender equality and human rights interventions included in sexual and reproductive health programmes and policies: A systematic review of existing research foci and gaps. PLoS ONE 2016, 11, e0167542. [Google Scholar] [CrossRef]
- Schardt, C.; Adams, M.B.; Owens, T.; Keitz, S.; Fontelo, P. Utilization of the PICO framework to improve searching PubMed for clinical questions. BMC Med Inf. Decis. Mak. 2007, 7, 16. [Google Scholar] [CrossRef]
- Shea, B.J.; Reeves, B.C.; Wells, G.; Thuku, M.; Hamel, C.; Moran, J.; Moher, D.; Tugwell, P.; Welch, G.; Thuku, M.; et al. AMSTAR 2: A critical appraisal tool for systematic reviews that include randomised or non-randomised studies of healthcare interventions, or both. BMJ 2017, 358, j4008. [Google Scholar] [CrossRef]
- Shea, B.J.; Grimshaw, J.M.; Wells, G.A.; Boers, M.; Andersson, N.; Hamel, C.; Porter, A.C.; Tugwell, P.; Moher, D.; Bouter, L.M. Development of AMSTAR: A measurement tool to assess the methodological quality of systematic reviews. BMC Med. Res. Methodol. 2007, 7, 10. [Google Scholar] [CrossRef]
- Shea, B.J.; Bouter, L.M.; Peterson, J.; Boers, M.; Andersson, N.; Ortiz, Z.; Ramsay, T.; Bai, A.; Shukla, V.K.; Grimshaw, J.M. External validation of a measurement tool to assess systematic reviews (AMSTAR). PLoS ONE 2007, 2, e1350. [Google Scholar] [CrossRef] [PubMed]
- Mason-Jones, A.J.; Sinclair, D.; Mathews, C.; Kagee, A.; Hillman, A.; Lombard, C. School-based interventions for preventing HIV, sexually transmitted infections, and pregnancy in adolescents. Cochrane Database Syst. Rev. 2016, 11, 1–72. [Google Scholar] [CrossRef]
- Palmer, M.J.; Henschke, N.; Villanueva, G.; Maayan, N.; Bergman, H.; Glenton, C.; Free, C. Targeted client communication via mobile devices for improving sexual and reproductive health. Cochrane Database Syst. Rev. 2020, 8, 1–84. [Google Scholar]
- Lopez, L.M.; Bernholc, A.; Chen, M.; Tolley, E.E. School-based interventions for improving contraceptive use in adolescents. Cochrane Database Syst. Rev. 2016, 6, 1–66. [Google Scholar] [CrossRef]
- Marseille, E.; Mirzazadeh, A.; Biggs, M.A.; Miller, A.P.; Horvath, H.; Lightfoot, M.; Kahn, J.G. Effectiveness of school-based teen pregnancy prevention programs in the USA: A systematic review and meta-analysis. Prev. Sci. 2018, 19, 468–489. [Google Scholar] [CrossRef] [PubMed]
- Mirzazadeh, A.; Biggs, M.A.; Viitanen, A.; Horvath, H.; Wang, L.Y.; Dunville, R.; Marseille, E. Do school-based programs prevent HIV and other sexually transmitted infections in adolescents? A systematic review and meta-analysis. Prev. Sci. 2018, 19, 490–506. [Google Scholar] [CrossRef] [PubMed]
- Oringanje, C.; Meremikwu, M.; Eko, H.; Esu, E.; Meremikwu, A.; Ehiri, J.E. Interventions for preventing unintended pregnancies among adolescents. Cochrane Database Syst. Rev. 2016, 2, 1–105. [Google Scholar] [CrossRef]
- Kedzior, S.G.; Lassi, Z.S.; Oswald, T.K.; Moore, V.M.; Marino, J.L.; Rumbold, A.R. A Systematic Review of School-based Programs to Improve Adolescent Sexual and Reproductive Health: Considering the Role of Social Connectedness. Adolesc. Res. Rev. 2020, 1–29. [Google Scholar] [CrossRef]
- Chokprajakchad, M.; Phuphaibul, R.; Sieving, R.E. Sexual health interventions among early adolescents: An integrative review. J. Health Res. 2018, 32, 467–477. [Google Scholar] [CrossRef]
- Goldfarb, E.S.; Lieberman, L.D. Three Decades of Research: The Case for Comprehensive Sex Education. J. Adolesc. Health 2020, 68, 7–8. [Google Scholar] [CrossRef]
- Haberland, N.A. The case for addressing gender and power in sexuality and HIV education: A comprehensive review of evaluation studies. Int. Perspect. Sex. Reprod. Health 2015, 41, 31–42. [Google Scholar] [CrossRef] [PubMed]
- Peterson, A.J.; Donze, M.; Allen, E.; Bonell, C. Effects of Interventions Addressing School Environments or Educational Assets on Adolescent Sexual Health: Systematic Review and Meta-analysis. Perspect. Sex. Reprod. Health 2019, 51, 91–107. [Google Scholar] [CrossRef]
- Bailey, J.; Mann, S.; Wayal, S.; Hunter, R.; Free, C.; Abraham, C.; Murray, E. Sexual health promotion for young people delivered via digital media: A scoping review. Public Health Res. 2015, 3, 1–119. [Google Scholar] [CrossRef]
- Celik, R.; Toruner, E.K. The Effect of Technology-Based Programmes on Changing Health Behaviours of Adolescents: Systematic Review. Compr. Child Adolesc. Nurs. 2020, 43, 92–110. [Google Scholar] [CrossRef]
- DeSmet, A.; Shegog, R.; Van Ryckeghem, D.; Crombez, G.; De Bourdeaudhuij, I. A systematic review and meta-analysis of interventions for sexual health promotion involving serious digital games. Games Health J. 2015, 4, 78–90. [Google Scholar] [CrossRef]
- Holstrom, A.M. Sexuality education goes viral: What we know about online sexual health information. Am. J. Sex. Educ. 2015, 10, 277–294. [Google Scholar] [CrossRef]
- L’Engle, K.L.; Mangone, E.R.; Parcesepe, A.M.; Agarwal, S.; Ippoliti, N.B. Mobile phone interventions for adolescent sexual and reproductive health: A systematic review. Pediatrics 2016, 138. [Google Scholar] [CrossRef]
- Martin, P.; Cousin, L.; Gottot, S.; Bourmaud, A.; Rochebrochard, E.; Alberti, C. Participatory interventions for sexual health promotion for adolescents and young adults on the internet: Systematic review. J. Med Internet Res. 2020, 22, e15378. [Google Scholar] [CrossRef]
- Wadham, E.; Green, C.; Debattista, J.; Somerset, S.; Sav, A. New digital media interventions for sexual health promotion among young people: A systematic review. Sex. Health 2019, 16, 101–123. [Google Scholar] [CrossRef]
- Widman, L.; Nesi, J.; Kamke, K.; Choukas-Bradley, S.; Stewart, J.L. Technology-based interventions to reduce sexually transmitted infections and unintended pregnancy among youth. J. Adolesc. Health 2018, 62, 651–660. [Google Scholar] [CrossRef]
- Coyle, K.K.; Chambers, B.D.; Anderson, P.M.; Firpo-Triplett, R.; Waterman, E.A. Blended Learning for Sexual Health Education: Evidence Base, Promising Practices, and Potential Challenges. J. Sch. Health 2019, 89, 847–859. [Google Scholar] [CrossRef] [PubMed]
- The World Bank. 2020. Available online: https://datatopics.worldbank.org/world-development-indicators/stories/the-classification-of-countries-by-income.html (accessed on 23 December 2020).
- Marsch, L.A.; Grabinski, M.J.; Bickel, W.K.; Desrosiers, A.; Guarino, H.; Muehlbach, B.; Acosta, M. Computer-assisted HIV prevention for youth with substance use disorders. Subst. Use Misuse 2011, 46, 46–56. [Google Scholar] [CrossRef]
- Janssens, A.; Blake, S.; Allwood, M.; Ewing, J.; Barlow, A. Exploring the content and delivery of relationship skills education programmes for adolescents: A systematic review. Sex Educ. 2020, 20, 494–516. [Google Scholar] [CrossRef]
- Todaro, E.; Silvaggi, M.; Aversa, F.; Rossi, V.; Nimbi, F.M.; Rossi, R.; Simonelli, C. Are Social Media a problem or a tool? New strategies for sexual education. Sexologies 2018, 27, e67–e70. [Google Scholar] [CrossRef]
- Preston, M. Very Very Risky: Sexuality Education Teachers’ Definition of Sexuality and Teaching and Learning Responsibilities. Am. J. Sex. Educ. 2013, 8, 18–35. [Google Scholar] [CrossRef]
- Layzer, C.J.; Rosapep, L.; Barr, S. A Peer education program: Delivering highly reliable sexual health promotion messages in schools. J. Adolesc. Health 2014, 54, 70–77. [Google Scholar] [CrossRef] [PubMed]
- Ketting, E.; Brockschmidt, L.; Ivanova, O. Investigating the C’in CSE: Implementation and effectiveness of comprehensive sexuality education in the WHO European region. Sex Educ. 2020, 1–15. [Google Scholar] [CrossRef]
- Lamb, S.; Lustig, K.; Graling, K. The use and misuse of pleasure in sex education curricula. Sex Educ. 2013, 13, 305–318. [Google Scholar] [CrossRef]
- Fine, M. Sexuality, schooling, and adolescent females: The missing discourse of desire. Harv. Educ. Rev. 1988, 58, 29–54. [Google Scholar] [CrossRef]
- Fine, M.; McClelland, S. Sexuality education and desire: Still missing after all these years. Harv. Educ. Rev. 2006, 76, 297–338. [Google Scholar] [CrossRef]
- Gill, R. The sexualisation of culture? Soc. Personal. Psychol. Compass 2012, 6, 483–498. [Google Scholar] [CrossRef]
- Liss, M.; Erchull, M.J.; Ramsey, L.R. Empowering or oppressing? Development and exploration of the Enjoyment of Sexualization Scale. Personal. Soc. Psychol. Bull. 2011, 37, 55–68. [Google Scholar] [CrossRef]
- Quinn, B.A. Sexual harassment and masculinity: The power and meaning of “girl watching”. Gend. Soc. 2002, 16, 386–402. [Google Scholar] [CrossRef]
- Fredrickson, B.L.; Roberts, T.A. Objectification theory: Toward understanding women’s lived experience and mental health risks. Psychol. Women Q. 1997, 21, 173–206. [Google Scholar] [CrossRef]
- Calogero, R.M.; Herbozo, S.; Thompson, J.K. Complimentary weightism: The potential costs of appearancerelated commentary for women’s self-objectification. Psychol. Women Q. 2009, 33, 120–132. [Google Scholar] [CrossRef]
- Renold, E.; Ringrose, J. Schizoid subjectivities? Re-theorizing teen girls sexual cultures in an era of sexualization. J. Sociol. 2011, 47, 389–409. [Google Scholar] [CrossRef]
- Gill, R.C. Critical Respect: The difficulties and dilemmas of agency and ‘choice’ for feminism: A reply to Duits and van Zoonen. Eur. J. Womens Stud. 2007, 14, 69–80. [Google Scholar] [CrossRef]
- Gill, R. Empowerment/sexism Figuring female sexual agency in contemporary advertising. Fem. Psychol. 2008, 18, 35–60. [Google Scholar] [CrossRef]
- Thompson, L. Desiring to be Desired: A Discursive Analysis of Women’s Responses to the ‘Raunch Culture’ Debates. Ph.D. Thesis, Murdoch University, Murdoch, Australia, 2012. [Google Scholar]
- Koepsel, E.R. The power in pleasure: Practical implementation of pleasure in sex education classrooms. Am. J. Sex. Educ. 2016, 11, 205–265. [Google Scholar] [CrossRef]
- Ketting, E.; Friele, M.; Micielsen, K. European Expert Group on Sexuality Education. Evaluation of Holistic Sexuality Education: A European Expert Group Consensus Agreement. Eur. J. Contracept. Reprod. Health Care 2015, 21, 68–80. [Google Scholar] [CrossRef]
- Patterson, S.; Hilton, P.; Flowers, S.; McDaid, L. What are the Barriers and Challenges Faced by Adolescents When Searching for Sexual Health Information on the Internet? Implications for Policy and Practice from a Qualitative Study. Sex. Transm. Infect. 2019, 95, 462–467. [Google Scholar] [CrossRef]
- King, B.M.; Burke, S.R.; Gates, T.M. Is there a gender difference in US college students’ desire for school-based sexuality education? Sex Educ. 2020, 20, 350–359. [Google Scholar] [CrossRef]
- Ruane-McAteer, E.; Gillespie, K.; Amin, A.; Aventin, A.; Robinson, M.; Hanratty, J.; Lohan, M. Gender-transformative programming with men and boys to improve sexual and reproductive health and rights: A systematic review of intervention studies. BMJ Glob. Health 2020, 5, e002997. [Google Scholar] [CrossRef] [PubMed]
- Schmidt, S.C.; Wandersman, A.; Hills, K.J. Evidence-Based Sexuality Education Programs in Schools: Do They Align with the National Sexuality Education Standards? Am. J. Sex. Educ. 2015, 10, 177–195. [Google Scholar] [CrossRef]
- European Expert Group on Sexuality Education. Sexuality education—What is it? Sex Educ. 2016, 16, 427–431. [Google Scholar] [CrossRef]
- McCarty-Caplan, D. Sex education and support of LGB families: A family impact analysis of the personal responsibility education program. Sex. Res. Soc. Policy 2015, 12, 213–223. [Google Scholar] [CrossRef]
- Jarpe-Ratner, E. How can we make LGBTQ+-inclusive sex education programmes truly inclusive? A case study of Chicago Public Schools’ policy and curriculum. Sex Educ. 2020, 20, 283–299. [Google Scholar] [CrossRef]
- Mustanski, B.; Greene, G.J.; Ryan, D.; Whitton, S.W. Feasibility, acceptability, and initial efficacy of an online sexual health promotion program for LGBT youth: The Queer Sex Ed intervention. J. Sex Res. 2015, 52, 220–230. [Google Scholar] [CrossRef]
- Haley, S.G.; Tordoff, D.M.; Kantor, A.Z.; Crouch, J.M.; Ahrens, K.R. Sex Education for Transgender and Non-Binary Youth: Previous Experiences and Recommended Content. J. Sex. Med. 2019, 16, 1834–1848. [Google Scholar] [CrossRef] [PubMed]
- Shannon, B. Comprehensive for who? Neoliberal directives in Australian ‘comprehensive’sexuality education and the erasure of GLBTIQ identity. Sex Educ. 2016, 16, 573–585. [Google Scholar] [CrossRef]
- Kirana, P.S.; Gudeloglu, A.; Sansone, A.; Fode, M.; Reisman, Y.; Corona, G.; Burri, A. E-Sexual Health: A Position Statement of the European Society for Sexual Medicine. J. Sex. Med. 2020, 17, 1246–1253. [Google Scholar] [CrossRef] [PubMed]
- Brayboy, L.M.; McCoy, K.; Thamotharan, S.; Zhu, E.; Gil, G.; Houck, C. The use of technology in the sexual health education especially among minority adolescent girls in the United States. Curr. Opin. Obstet. Gynecol. 2018, 30, 305. [Google Scholar] [CrossRef]
- Cushman, N.; Kantor, L.M.; Schroeder, E.; Eicher, L.; Gambone, G. Sexuality education: Findings and recommendations from an analysis of 10 United States programmes. Sex Educ. 2014, 14, 481–496. [Google Scholar] [CrossRef]
- Butler, R.S.; Sorace, D.; Beach, K.H. Institutionalizing sex education in diverse US school districts. J. Adolesc. Health 2018, 62, 149–156. [Google Scholar] [CrossRef] [PubMed]
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Lameiras-Fernández, M.; Martínez-Román, R.; Carrera-Fernández, M.V.; Rodríguez-Castro, Y. Sex Education in the Spotlight: What Is Working? Systematic Review. Int. J. Environ. Res. Public Health 2021, 18, 2555. https://doi.org/10.3390/ijerph18052555
Lameiras-Fernández M, Martínez-Román R, Carrera-Fernández MV, Rodríguez-Castro Y. Sex Education in the Spotlight: What Is Working? Systematic Review. International Journal of Environmental Research and Public Health. 2021; 18(5):2555. https://doi.org/10.3390/ijerph18052555
Chicago/Turabian StyleLameiras-Fernández, María, Rosana Martínez-Román, María Victoria Carrera-Fernández, and Yolanda Rodríguez-Castro. 2021. "Sex Education in the Spotlight: What Is Working? Systematic Review" International Journal of Environmental Research and Public Health 18, no. 5: 2555. https://doi.org/10.3390/ijerph18052555
APA StyleLameiras-Fernández, M., Martínez-Román, R., Carrera-Fernández, M. V., & Rodríguez-Castro, Y. (2021). Sex Education in the Spotlight: What Is Working? Systematic Review. International Journal of Environmental Research and Public Health, 18(5), 2555. https://doi.org/10.3390/ijerph18052555









