Facilitating Healthier Eating at Restaurants: A Multidisciplinary Scoping Review Comparing Strategies, Barriers, Motivators, and Outcomes by Restaurant Type and Initiator
Abstract
1. Introduction
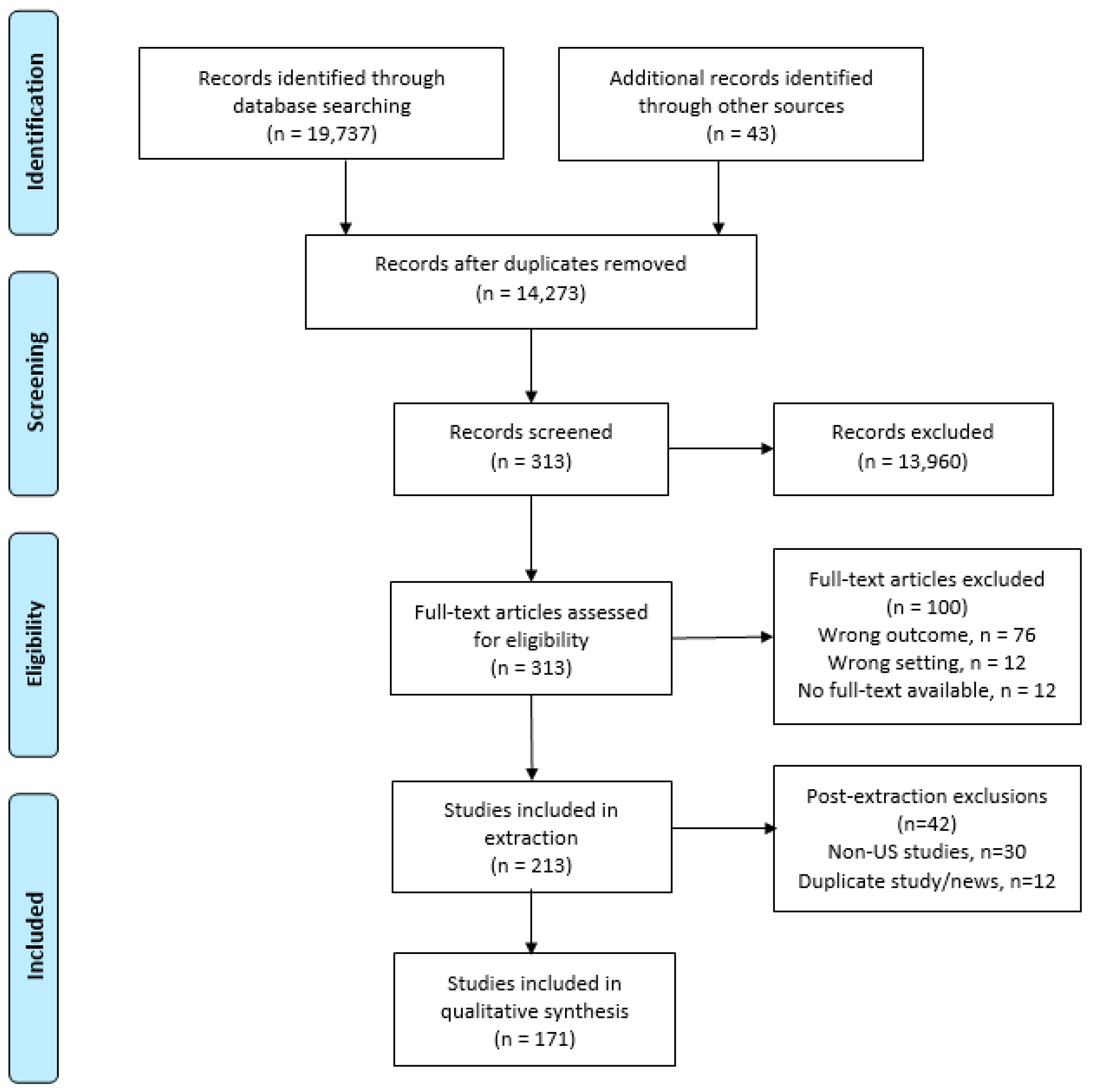
2. Materials and Methods
3. Results
3.1. Sample Description
3.2. Consumer-Facing Strategies for Healthier Eating
3.3. Reported Motivations and Barriers for Strategy Implementation
3.4. Reported Outcomes
4. Discussion
Strengths and Limitations
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Lachat, C.; Nago, E.; Verstraeten, R.; Roberfroid, D.; Van Camp, J.; Kolsteren, P. Eating out of home and its association with dietary intake: A systematic review of the evidence. Obes. Rev. 2012, 13, 329–346. [Google Scholar] [CrossRef]
- Forberger, S.; Reisch, L.; Kampfmann, T.; Zeeb, H. Nudging to move: A scoping review of the use of choice architecture interventions to promote physical activity in the general population. Int. J. Behav. Nutr. Phys. Act. 2019, 16, 1–14. [Google Scholar] [CrossRef]
- VanEpps, E.M.; Roberto, C.A.; Park, S.; Economos, C.D.; Bleich, S.N. Restaurant Menu Labeling Policy: Review of Evidence and Controversies. Curr. Obes. Rep. 2016, 5, 72–80. [Google Scholar] [CrossRef]
- Odoms-Young, A.; Singleton, C.R.; Springfield, S.; McNabb, L.; Thompson, T. Retail Environments as a Venue for Obesity Prevention. Curr. Obes. Rep. 2016, 5, 184–191. [Google Scholar] [CrossRef]
- Rincón-Gallardo, P.S.; Zhou, M.; Da Silva Gomes, F.; Lemaire, R.; Hedrick, V.; Serrano, E.; Kraak, V.I. Effects of Menu Labeling Policies on Transnational Restaurant Chains to Promote a Healthy Diet: A Scoping Review to Inform Policy and Research. Nutrients 2020, 12, 1544. [Google Scholar] [CrossRef] [PubMed]
- Sisnowski, J.; Street, J.M.; Merlin, T. Improving food environments and tackling obesity: A realist systematic review of the policy success of regulatory interventions targeting population nutrition. PLoS ONE 2017, 12, e0182581. [Google Scholar] [CrossRef]
- Hillier-Brown, F.; Summerbell, C.; Moore, H.; Routen, A.; Lake, A.; Adams, J.; White, M.; Araujo-Soares, V.; Abraham, C.; Adamson, A.; et al. The impact of interventions to promote healthier ready-to-eat meals (to eat in, to take away or to be delivered) sold by specific food outlets open to the general public: A systematic review. Obes. Rev. 2017, 18, 227–246. [Google Scholar] [CrossRef]
- Espino, J.N.V.; Guerrero, N.; Rhoads, N.; Simon, N.-J.; Escaron, A.L.; Meinen, A. Community-Based Restaurant Interventions to Promote Healthy Eating: A Systematic Review. Prev. Chronic Dis. 2015, 12, E78. [Google Scholar]
- Penney, T.L.; Brown, H.E.; Maguire, E.R.; Kuhn, I.; Monsivais, P. Local food environment interventions to improve healthy food choice in adults: A systematic review and realist synthesis protocol. BMJ Open 2015, 5, e007161. [Google Scholar] [CrossRef]
- Wright, B.; Bragge, P. Interventions to promote healthy eating choices when dining out: A systematic review of reviews. Br. J. Health Psychol. 2018, 23, 278–295. [Google Scholar] [CrossRef] [PubMed]
- Bleich, S.N.; Economos, C.D.; Spiker, M.L.; Vercammen, K.A.; VanEpps, E.M.; Block, J.P.; Elbel, B.; Story, M.; Roberto, C.A. A Systematic Review of Calorie Labeling and Modified Calorie Labeling Interventions: Impact on Consumer and Restaurant Behavior. Obesity 2017, 25, 2018–2044. [Google Scholar] [CrossRef]
- Beltrán, M.D.P.D.; Romero, Y.M.H. Healthy eating and restaurants. A review of recent evidence in the literature. Cienc. Saude Coletiva 2019, 24, 853–864. [Google Scholar] [CrossRef]
- Fernandes, A.C.; Oliveira, R.C.; Proenca, R.P.; Curioni, C.C.; Rodrigues, V.M.; Fiates, G.M. Influence of menu labeling on food choices in real-life settings: A systematic review. Nutr. Rev. 2016, 74, 534–548. [Google Scholar] [CrossRef] [PubMed]
- Long, M.W.; Tobias, D.K.; Cradock, A.L.; Batchelder, H.; Gortmaker, S.L. Systematic review and meta-analysis of the impact of restaurant menu calorie labeling. Am. J. Public Health 2015, 105, e11–e24. [Google Scholar] [CrossRef] [PubMed]
- Wilson, A.L.; Buckley, E.; Buckley, J.D.; Bogomolova, S. Nudging healthier food and beverage choices through salience and priming. Evidence from a systematic review. Food Qual. Prefer. 2016, 51, 47–64. [Google Scholar] [CrossRef]
- Kraak, V.I.; Englund, T.; Misyak, S.; Serrano, E.L. A novel marketing mix and choice architecture framework to nudge restaurant customers toward healthy food environments to reduce obesity in the United States. Obes. Rev. 2017, 18, 852–868. [Google Scholar] [CrossRef]
- Blake, M.R.; Backholer, K.; Lancsar, E.; Boelsen-Robinson, T.; Mah, C.; Brimblecombe, J.; Zorbas, C.; Billich, N.; Peeters, A. Investigating business outcomes of healthy food retail strategies: A systematic scoping review. Obes. Rev. 2019, 20, 1384–1399. [Google Scholar] [CrossRef]
- Covidence Systematic Review Software; Veritas Health Innovation: Melbourne, Australia, 2020.
- Peters, M.D.J.; Godfrey, C.M.; Khalil, H.; McInerney, P.; Parker, D.; Soares, C.B. Guidance for conducting systematic scoping reviews. Int. J. Evid.-Based Healthc. 2015, 13, 141–146. [Google Scholar] [CrossRef]
- Glanz, K.; Sallis, J.F.; Saelens, B.E.; Frank, L.D. Healthy nutrition environments: Concepts and measures. Am. J. Health Promot. 2005, 19, 330–333. [Google Scholar] [CrossRef]
- Saelens, B.E.; Glanz, K.; Sallis, J.F.; Frank, L.D. Nutrition Environment Measures Study in Restaurants (NEMS-R): Development and Evaluation. Am. J. Prev. Med. 2001, 32, 273–281. [Google Scholar] [CrossRef]
- Dijikers, M. Duplicate Publications and Systematic Reviews: Problems and Proposals. KT Update, 2 February 2018; 1–12. [Google Scholar]
- Frumkin, P. Menu diversity, healthful foods top talk at DiRoNA confab. Nation’s Restaurant News, 1 November 2004; 8–96. [Google Scholar]
- Hayes, J. Benefits of nutrition info carry more than just cosmetic weight. Nation’s Restaurant News, 5 July 2004; 54. [Google Scholar]
- MaCarthur, K.; Dando, P. Healthier fast-food a reality. Advertising Age, 29 March 2004; S7. [Google Scholar]
- Ruggless, R. Menus’ low-fat, low-carb varieties market to ‘My Own Diet’ trend. Nation’s Restaurant News, 28 June 2004; 210. [Google Scholar]
- Strenk, T. Salads. Restaurant Business, 15 November 2004; 40. [Google Scholar]
- Walkup, C. Sandwich chain roll out low-carb breads, bagels to feed diet craze. Nation’s Restaurant News, 19 April 2004; 4–58. [Google Scholar]
- Operators weigh in on health and diet trends. Nation’s Restaurant News, 2 May 2005; 44–46.
- McDonald’s launches packaging initiative. Food Magazine, 2005; 31.
- A Healthy Start. Nation’s Restaurant News, 8 August 2005; 18–22.
- Barrier, B. The skinny on KnowFat! Lifestyle Grille. Nation’s Restaurant News, 3 January 2005; 16–64. [Google Scholar]
- Barrier, B. Mitchell’s Fish Markets go gluten free. Nation’s Restaurant News, 15 August 2005; 20. [Google Scholar]
- Barrier, B. McD teams up with celebs in outreach programs targeting minorities. Nation’s Restaurant News, 6 June 2005; 20–24. [Google Scholar]
- Cobe, P. Power Eating. Restaurant Business, 1 April 2005; 40–44. [Google Scholar]
- Cobe, P. Keep the Dish, Cut the Calories. Restaurant Business, 11 November 2005; 18–19. [Google Scholar]
- Enis, M. Quick-Service Restaurants Make the Cut. SN: Supermarket News, 26 September 2005; 42–55. [Google Scholar]
- Harper, R. Salad Days. SN: Supermarket News, 28 February 2005; 8. [Google Scholar]
- Parseghan, P.; Ruggless, R.; Thorn, B. Feeding the needs of health-savvy customers. Nation’s Restaurant News, 21 November 2005; 52–56. [Google Scholar]
- Shadx, K. Healthful kids meals don’t have to scrimp on fun, flavor. Nation’s Restaurant News, 25 April 2005; 22. [Google Scholar]
- Wendy’s adds sandwich, yogurt cup to kids’ meals. Nation’s Restaurant News, 1 May 2006; 102.
- Teppanyaki Translates Into Healthy Dining. Nation’s Restaurant News, 2006; 10.
- Eden, E. Kids Menus Grow Up. Restaurant Business, September 2006; 14. [Google Scholar]
- Jennings, L. Cheesecake Factory rolls out trans-fat-free menu. Nation’s Restaurant News, 26 June 2006; 3–207. [Google Scholar]
- Katz, F. A healthier foodservice menu. Food Processing (00156523), June 2006; 45–49. [Google Scholar]
- Kramer, L. Park sells healthful takeout meals for kids. Nation’s Restaurant News, 16 October 2006; 34. [Google Scholar]
- Kramer, L. For healthy soul food, Aunt Obie’s owner fools them with flavor. Nation’s Restaurant News, 4 September 2006; 26. [Google Scholar]
- Rowe, M. Better for You, Better for the Planet. Food Management, 2006; 2. [Google Scholar]
- Smaller-portion menu items are more likely to help the restaurant industry than hurt it. Nation’s Restaurant News, 30 April 2007; 17.
- Serving New Tastes. Prepared Foods, November 2007; 69–75.
- Healthy Customers, Healthy Profits. Restaurant Hospitality, January 2007; 38–42.
- Hoffman, E. Efforts to promote healthful dishes must put heavy emphasis on concept’s brand image. Nation’s Restaurant News, 13 August 2007; 50. [Google Scholar]
- Burger King Joins the Ranks with Healthier Options for Kids. Dairy Foods, October 2007; 14.
- 100 Denver McD’s join in Colo. ‘Smart Meal’ promo. Nation’s Restaurant News, 30 April 2007; 19.
- Elan, E. Contractor Bon Appetit rolls trans-fat-free menu. Nation’s Restaurant News, 16 April 2007; 4–8. [Google Scholar]
- Gumpert, D.E. From Fried Chicken to Veggie Burgers. BusinessWeek Online, 26 June 2007; 20. [Google Scholar]
- Prewitt, M. Fast-casual ups the ante with fresh, healthful options. Nation’s Restaurant News, 18 June 2007; 37–40. [Google Scholar]
- Sonic nutrition push for kids adds string cheese. Nation’s Restaurant News, 15 September 2008; 8.
- Cebrzynski, G. Painting the picture of health. Nation’s Restaurant News, 25 February 2008; 43–46. [Google Scholar]
- Korrow, C. Café Gratitude: Eat healthier foods—Think healthier thoughts. LILIPOH, 2008; 31. [Google Scholar]
- Walkup, C. Sandwich players’ latest promotions pitch value, health, loyalty. Nation’s Restaurant News, 28 July 2008; 76. [Google Scholar]
- Caldwell, M. Qdoba’s Smart Meals. Nation’s Restaurant News, 4 May 2009; 54. [Google Scholar]
- Dempsey, M. Spreading the love. Nation’s Restaurant News, 7 September 2009; 17. [Google Scholar]
- Licata, E. Healthy menu options can help eliminate veto votes from guests. Nation’s Restaurant News, 23 March 2009; 29. [Google Scholar]
- Smyth, W. Chick-fil-A’s Chargrilled & Fruit Salad. Nation’s Restaurant News, 4 May 2009; 56. [Google Scholar]
- Brandau, M. A little healthy competition. Nation’s Restaurant News, 8 February 2010; 1–51. [Google Scholar]
- Elan, E. Off to the salt mines. Nation’s Restaurant News, 17 May 2010; 28. [Google Scholar]
- Elan, E. Having Words with Aaron Webster. Nation’s Restaurant News, 23 August 2010; 54. [Google Scholar]
- Parekh, R.; York, E.B. Did Somebody Say...McHealthy? Fast-Food Alums Try New Concept. Advertising Age, 12 July 2010; 1–21. [Google Scholar]
- Target The Calorie Counters. Restaurant Hospitality, October 2011; 16.
- Jack in the Box pulls toys, adds menu items. Nation’s Restaurant News, 27 June 2011; 10.
- Elan, E. Green pastures. Nation’s Restaurant News, 24 January 2011; 18. [Google Scholar]
- Enis, M. Restaurants Make New Strides in Kids’ Nutrition. SN: Supermarket News, 3 October 2011; 10. [Google Scholar]
- Harper, R. PBH Lauds McDonald’s Nutrition Promises. SN: Supermarket News, 1 August 2011; 18–21. [Google Scholar]
- Jennings, L. Meatless menu. Nation’s Restaurant News, 13 June 2011; 3–12. [Google Scholar]
- Ruggless, R. Fit-food nation. Nation’s Restaurant News, 10 January 2011; 3–28. [Google Scholar]
- Wendy’s app puts healthy fast food at your fingertips. Direct Marketing News, October 2012; 44.
- Salad days. Restaurant Business, July 2012; M4.
- Kids LiveWell program gains momentum as industry awareness, participation grow. Nation’s Restaurant News, 19 March 2012; 30.
- Santiago, J. Subway provides healthy nutrition for today’s fast-paced lives. Caribbean Business, 31 May 2012; B34–B35. [Google Scholar]
- Subway Restaurants Healthy food for health-related environments. Caribbean Business, 30 May 2013; B28–B29.
- McDonald’s to offer nutrition-themed books in Happy Meals. Nation’s Restaurant News, 21 October 2013; 4.
- Make it “Craveable”. Prepared Foods, 13 August 2013; 62–63.
- Brandau, M. Low calorie, high buzz. Nation’s Restaurant News, 4 November 2013; 26. [Google Scholar]
- Cobe, P. Sandwich reinvention. Restaurant Business, September 2013; M1–M6. [Google Scholar]
- Cobe, P. Menus: What’s in, what’s out. Restaurant Business, February 2013; 18–20. [Google Scholar]
- Morrison, M. McD’s vow to promote healthful menu options puts pressure on rivals. Advertising Age, 30 September 2013; 6. [Google Scholar]
- Cobe, P. Reconfiguring the Plate. Restaurant Business, October 2015; 57–60. [Google Scholar]
- Glazer, F. Redefining ‘healthful’. Nation’s Restaurant News, 27 April 2015; 60–62. [Google Scholar]
- Jennings, L. Taco Bell cuts sodium in ongoing effort. Nation’s Restaurant News, 27 January 2015; 5. [Google Scholar]
- Jennings, L. Restaurants highlight health, not calories. Nation’s Restaurant News, 9 February 2015; 34. [Google Scholar]
- Mueller, C. Breakfast in a Glass. Restaurant Business, May 2016; 80. [Google Scholar]
- Freier, L.F. Fries Toward the Future: Health, shmealth—consumers want their fries, but not exactly in the same old way. Restaurant Business, July 2017; 39. [Google Scholar]
- Veggie Concepts Go All In. Restaurant Business, May 2017; 54.
- Sonic intros breakfast ‘lite’. QSRweb.com, 28 September 2018; 1.
- Bloom, B. Fruitful Ideas: Exotic fruit items grow on restaurant menus. Prepared Foods, May 2018; 27. [Google Scholar]
- Fitzpatrick, T. Trendy grain bowls exhibit broad appeal. Nation’s Restaurant News, 23 July 2018; N.PAG. [Google Scholar]
- Pei Wei debuts cauliflower rice, bowl options. FastCasual, 10 January 2019.
- New Uno Pizzeria menu offers 65+ items for 6 different diets. PizzaMarketplace, 24 October.
- Carl’s, Jr. Your Pie intro meat alternative options. PizzaMarketplace, 2 January 2019. [Google Scholar]
- Cobe, P. Dealing with Diet Demands: Operators are ramping up training to meet customers’ current eating preferences. Restaurant Business, April 2019; 29. [Google Scholar]
- Kruse, N. Vegetables move to the center of the plate. Restaurant Hospitality, March 2019; 42–43. [Google Scholar]
- Pepitone, J. Marketing Meatless: Operators are finding ways to draw a wider range of diners to alternate proteins. Restaurant Business, April 2019; 30. [Google Scholar]
- Peters, B. Beyond Meat Rises As KFC Plans Beyond Chicken Test. Investors Business Daily, 26 August 2019. [Google Scholar]
- Uno New Year additions designed to delight despite diet restrictions. PizzaMarketplace, January 2020.
- Boston’s dishes out options to ‘lifestyle’ diners. PizzaMarketplace, January 2020.
- Wendy’s Wows Us With a Winner. Environmental Nutrition, March 2005; 3.
- Update: Battling Trans Fat. Tufts University Health & Nutrition Letter, April 2007; 2.
- Burger King Dethrones Trans Fats. Tufts University Health & Nutrition Letter, September 2007; 3.
- Adams, C. Reframing the Obesity Debate: McDonald’s Role May Surprise You. J. Law Med. Ethics 2007, 35, 154–157. [Google Scholar] [CrossRef]
- Bohm, E.; Quartuccio, N. Healthy Dining Restaurant Nutrition Program—A Winning Recipe for Consumers, Dietitians and Restaurants. J. Am. Dietetic Assoc. 2008, 108, A112. [Google Scholar] [CrossRef]
- Carter, C. Restaurants That Get It Right. Men’s Health, November 2011; 108–113. [Google Scholar]
- Downs, J.S. Does “Healthy” Fast Food Exist? The Gap Between Perceptions and Behavior. J. Adolescent Health 2013, 429–430. [Google Scholar] [CrossRef] [PubMed]
- Hurley, J.; Lim, D. Sandwich, Soup, & Salad Smarts. Nutrition Action Health Letter, November 2010; 12–15. [Google Scholar]
- Jacobson, M.F. Axing Additives: A Good Start. Nutrition Action Health Letter, October 2015; 2. [Google Scholar]
- Jibrin, J. Dine low-carb smart. Natural Health, 20 May 2004; 33–38. [Google Scholar]
- Liebman, B.; Hurley, J.; DeMino, H.J. Beyond Fast Food ‘Fast Casuals’ Come of Age. Nutrition Action Health Letter, April 2003; 10. [Google Scholar]
- McLndoo, H. Kids’ Meals: Work in Fruits and Veggies. Environmental Nutrition, 2012; 5. [Google Scholar]
- Smith, M.D. Chipotle Says No to GMOs. Better Nutrition, 2015; 12. [Google Scholar]
- Stein, K. For your information. Healthful fast foods not part of healthful revenue. J. Am. Dietetic Assoc. 2006, 106, 344–345. [Google Scholar] [CrossRef] [PubMed]
- Walker, T. Soul Food, Vegan-Style. Vegetarian Times, May 2016; 17–19. [Google Scholar]
- Barboza, D. McDonald’s New Recipe Lowers Goo For Arteries. New York Times, September 2002; A16. [Google Scholar]
- Burros, M. In the Temples Of Supersizing, Eating Light Draws Converts. New York Times, 29 October 2003; F1–F5. [Google Scholar]
- Boyle, M. Can You Really Make Fast Food Healthy? Fortune Int. (Europe) 2004, 150, 68–73. [Google Scholar]
- Burros, M. Hold the Fries. Hey, Not All of Them! New York Times, 10 March 2004; F1–F5. [Google Scholar]
- Cooney, J. The Skinny on Subway. License, May 2004; 108. [Google Scholar]
- Gray, S. Fast Fruit? At Wendy’s and McDonald’s, It’s a Main Course. Wall Street J. East. Ed. 2005, 245, B1–B2. [Google Scholar]
- Warner, M. You Want Any Fruit With That Big Mac? New York Times, 20 February 2005; 1–8. [Google Scholar]
- Stein, J. Undersize Me. Time International (Atlantic Edition), 21 May 2007; 45. [Google Scholar]
- Conis, E. Company promises healthful fast food. Los Angeles Times—Southern California Edition (Front. Page), 14 July 2011; E1–E5. [Google Scholar]
- Strom, S. With Tastes Growing Healthier, McDonald’s Aims to Adapt Its Menu. New York Times, 27 September 2013; B1–B6. [Google Scholar]
- Wong, V. Chick-fil-A Changed Its Ingredients and Didn’t Tell Anyone. Bloomberg.com, 11 December 2013; 4. [Google Scholar]
- Chen, A. ReViVer Serves Healthy Food Backed by Science. Wall Street Journal, 4 August 2014; 1. [Google Scholar]
- Moskin, J. Hold the Regret? Fast Food Seeks Virtuous Side. (Cover story). New York Times, 25 July 2014; A1–A3. [Google Scholar]
- Jargon, J. McDonald’s to Remove High-Fructose Corn Syrup From Sandwich Buns. Wall Street Journal (Online), 1 August 2016. [Google Scholar]
- Maloney, J.; Jargon, J. McDonald’s Is Trying to Make the Happy Meal Healthier—Again. Wall Street Journal—Online Ed. 15 September 2017. [Google Scholar]
- Horgen, K.B.; Brownell, K.D. Comparison of price change and health message interventions in promoting healthy food choices. Health Psychol. 2002, 21, 505–512. [Google Scholar] [CrossRef]
- Fitzgerald, C.M.; Kannan, S.; Sheldon, S.; Eagle, K.A. Effect of a promotional campaign on heart-healthy menu choices in community restaurants. J. Am. Diet. Assoc. 2004, 104, 429–432. [Google Scholar] [CrossRef]
- Acharya, R.N.; Patterson, P.M.; Hill, E.P.; Schmitz, T.G.; Bohm, E. An evaluation of the “TrEAT Yourself Well” restaurant nutrition campaign. Health Educ. Behav. 2006, 33, 309–324. [Google Scholar] [CrossRef]
- Economos, C.D.; Folta, S.C.; Goldberg, J.; Hudson, D.; Collins, J.; Baker, Z.; Lawson, E.; Nelson, M. A community-based restaurant initiative to increase availability of healthy menu options in Somerville, Massachusetts: Shape Up Somerville. Prev. Chronic Dis. 2009, 6, A102. [Google Scholar] [PubMed]
- Hanni, K.D.; Garcia, E.; Ellemberg, C.; Winkleby, M. Steps to a Healthier Salinas: Targeting the taqueria: Implementing healthy food options at Mexican American restaurants. Health Promot. Pract. 2009, 10, 91S–99S. [Google Scholar] [CrossRef]
- Pulos, E.; Leng, K. Evaluation of a Voluntary Menu-Labeling Program in Full-Service Restaurants. Am. J. Public Health 2010, 100, 1035–1039. [Google Scholar] [CrossRef] [PubMed]
- Blair, A.M.; Drass, J.A.; Stone, M.; Rhoades, D.; Baldwin, S.A.; Russ, K.M. Restaurant challenge offers healthful meal options and builds diabetes awareness. Diabetes Educ. 2011, 37, 581–588. [Google Scholar] [CrossRef] [PubMed]
- Britt, J.W.; Frandsen, K.; Leng, K.; Evans, D.; Pulos, E. Feasibility of voluntary menu labeling among locally owned restaurants. Health Promot. Pract. 2011, 12, 18–24. [Google Scholar] [CrossRef]
- Chen, R.; Carrillo, M.; Kapp, J.; Cheadle, A.; Angulo, A.; Chrisman, N.; Rubio, R. Partnering with REACH to create a “diabetes-friendly” restaurant: A restaurant owner’s experience. Prog. Commun. Health Partnersh. Res. Educ. Act. 2011, 5, 307–312. [Google Scholar] [CrossRef]
- Schwartz, J.; Riis, J.; Elbel, B.; Ariely, D. Inviting consumers to downsize fast-food portions significantly reduces calorie consumption. Health Aff. Proj. Hope 2012, 31, 399–407. [Google Scholar] [CrossRef]
- Lee-Kwan, S.H.; Goedkoop, S.; Yong, R.; Batorsky, B.; Hoffman, V.; Jeffries, J.; Hamouda, M.; Gittelsohn, J. Development and implementation of the Baltimore healthy carry-outs feasibility trial: Process evaluation results. BMC Public Health 2013, 13, 638. [Google Scholar] [CrossRef] [PubMed]
- Nevarez, C.R.; Lafleur, M.S.; Schwarte, L.U.; Rodin, B.; de Silva, P.; Samuels, S.E. Salud Tiene Sabor: A model for healthier restaurants in a Latino community. Am. J. Prev. Med. 2013, 44, S186–S192. [Google Scholar] [CrossRef]
- Nothwehr, F.K.; Snetselaar, L.; Dawson, J.; Schultz, U. Promoting healthy choices in non-chain restaurants: Effects of a simple cue to customers. Health Promot. Pract. 2013, 14, 132–138. [Google Scholar] [CrossRef]
- Biediger-Friedman, L.; Sosa, E.T.; Shields, K.; Shutt, A. A Voluntary Approach to Improve Menu Options in Restaurants Through a Local Collaborative Partnership. Tex. Public Health J. 2014, 66, 11–14. [Google Scholar]
- Crixell, S.H.; Friedman, B.; Fisher, D.T.; Biediger-Friedman, L. Improving children’s menus in community restaurants: Best food for families, infants, and toddlers (Best Food FITS) intervention, South Central Texas, 2010–2014. Prev. Chronic Dis. 2014, 11, E223. [Google Scholar] [CrossRef]
- Schuster, M.J.; Carlson, J.R.; Mackenzie, J.A.; Roche, J.D.; Brooks, T.L.; Painter, J.E. Do Pre-Meal To-Go Boxes Affect the Amount of Food Consumed in a Restaurant Setting? J. Acad. Nutr. Diet. 2014, 114, A62. [Google Scholar] [CrossRef]
- Anzman-Frasca, S.; Mueller, M.P.; Sliwa, S.; Dolan, P.R.; Harelick, L.; Roberts, S.B.; Washburn, K.; Economos, C.D. Changes in children’s meal orders following healthy menu modifications at a regional U.S. restaurant chain. Obesity 2015, 23, 1055–1062. [Google Scholar] [CrossRef]
- Bedard, K.; Kuhn, P. Micro-marketing healthier choices: Effects of personalized ordering suggestions on restaurant purchases. J. Health Econ. 2015, 39, 106–122. [Google Scholar] [CrossRef] [PubMed]
- Gase, L.N.; Kaur, M.; Dunning, L.; Montes, C.; Kuo, T. What menu changes do restaurants make after joining a voluntary restaurant recognition program? Appetite 2015, 89, 131–135. [Google Scholar] [CrossRef]
- Tritt, A.; Reicks, M.; Marquart, L. Reformulation of pizza crust in restaurants may increase whole-grain intake among children. Public Health Nutr. 2015, 18, 1407–1411. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Berkowitz, S.; Marquart, L.; Mykerezi, E.; Degeneffe, D.; Reicks, M. Reduced-portion entrées in a worksite and restaurant setting: Impact on food consumption and waste. Public Health Nutr. 2016, 19, 3048–3054. [Google Scholar] [CrossRef] [PubMed]
- Escaron, A.L.; Martinez-Donate, A.P.; Riggall, A.J.; Meinen, A.; Hall, B.; Nieto, F.J.; Nitzke, S. Developing and implementing ‘Waupaca Eating Smart’: A restaurant and supermarket intervention to promote healthy eating through changes in the food environment. Health Promot. Pract. 2016, 17, 265–277. [Google Scholar] [CrossRef]
- Ayala, G.X.; Castro, I.A.; Pickrel, J.L.; Lin, S.-F.; Williams, C.B.; Madanat, H.; Jun, H.-J.; Zive, M. A Cluster Randomized Trial to Promote Healthy Menu Items for Children: The Kids’ Choice Restaurant Program. Int. J. Environ. Res. Public Health 2017, 14, 1494. [Google Scholar] [CrossRef]
- Lopez, N.V.; Folta, S.C.; Glenn, M.E.; Lynskey, V.M.; Patel, A.A.; Anzman-Frasca, S. Promoting healthier children’s meals at quick-service and full-service restaurants: Results from a pilot and feasibility study. Appetite 2017, 117, 91–97. [Google Scholar] [CrossRef]
- Thayer, L.M.; Pimentel, D.C.; Smith, J.C.; Garcia, B.A.; Lee Sylvester, L.; Kelly, T.; Johnston, L.F.; Ammerman, A.S.; Keyserling, T.C. Eating Well While Dining Out: Collaborating with Local Restaurants to Promote Heart Healthy Menu Items. Am. J. Health Educ. 2017, 48, 11–21. [Google Scholar] [CrossRef] [PubMed]
- Lindberg, R.; Sidebottom, A.C.; McCool, B.; Pereira, R.F.; Sillah, A.; Boucher, J.L. Changing the restaurant food environment to improve cardiovascular health in a rural community: Implementation and evaluation of the Heart of New Ulm restaurant programme. Public Health Nutr. 2018, 21, 992–1001. [Google Scholar] [CrossRef] [PubMed]
- Ma, G.X.; Shive, S.E.; Guo, Z.; Aquilante, J. Evaluation of a Healthy Chinese Take-Out Sodium-Reduction Initiative in Philadelphia Low-Income Communities and Neighborhoods. Public Health Rep. 2018, 133, 472–480. [Google Scholar] [CrossRef]
- Fuster, M.; Guerrero, K.; Elbel, B.; Ray, K.; Huang, T.T.K. Engaging Ethnic Restaurants to Improve Community Nutrition Environments: A Qualitative Study with Hispanic Caribbean Restaurants in New York City. Ecol. Food Nutr. 2020, 59, 1–17. [Google Scholar] [CrossRef]
- Sharma, S.; Wagle, A.; Sucher, K.; Bugwadia, N. Impact of Point of Selection Nutrition Information on Meal Choices at a Table-Service Restaurant. J. Foodserv. Bus. Res. 2011, 14, 146–161. [Google Scholar] [CrossRef]
- Shuo, L.; McCluskey, J.J.; Mittelhammer, R.C. Effects of Healthier Choices on Kid’s Menu: A Difference-in-Differences Analysis. J. Food Distrib. Res. 2012, 43, 1–14. [Google Scholar]
- Shah, A.M.; Bettman, J.R.; Ubel, P.A.; Keller, P.A.; Edell, J.A. Surcharges Plus Unhealthy Labels Reduce Demand for Unhealthy Menu Items. J. Mark. Res. JMR 2014, 51, 773–789. [Google Scholar] [CrossRef]
- Crimarco, A.; Turner-McGrievy, G.M.; Botchway, M.; Macauda, M.; Adams, S.A.; Blake, C.E.; Younginer, N. “We’re Not Meat Shamers. We’re Plant Pushers.”: How Owners of Local Vegan Soul Food Restaurants Promote Healthy Eating in the African American Community. J. Black Stud. 2020, 51, 168–193. [Google Scholar] [CrossRef]
- Wienerschnitzel rolls out low-fat hot-dog option. Nation’s Restaurant News, 30 June 2003; 38.
- Wendy’s Promotes Nutrition Info. Restaurant Business, 1 October 2003; 12.
- Wendy’s Offers Kids Reduced-Fat Options. Restaurant Business, 15 October 2003; 12.
- New Atlanta casual concept ‘balances’ nutrition and taste. Nation’s Restaurant News, 23 May 2003; 8.
- Garber, A. Sandwich chains get in shape to meet consumer preference for upscale settings, healthful fare. Nation’s Restaurant News, 30 June 2003; 88. [Google Scholar]
- Garber, A. Pizza Magia unveils leaner, ‘more nutritious’ menu items. Nation’s Restaurant News, 28 July 2003; 128. [Google Scholar]
- Garber, A. It’s not easy not being green. Nation’s Restaurant News, 11 August 2003; 61. [Google Scholar]
- Lohmeyer, L. ‘Healthful’ QSR brands slow to win broad acceptance. Nation’s Restaurant News, 7 April 2003; 4. [Google Scholar]
- Lohmeyer, L. Fast feeders seek to raise bar, toss around salad ideas. (cover story). Nation’s Restaurant News, 21 April 2003; 1. [Google Scholar]
- Zuber, A. Skinny on QSR: Chains get wise, wealthy on good health. (cover story). Nation’s Restaurant News, 17 February 2003; 1. [Google Scholar]
- Subway: Healthy eating is child’s play. MarketWatch: Food, 30 May 2004; 8–9.
- Subway: Healthier options. MarketWatch: Global Round-up, March 2004; 53.
- Slim Choices. Restaurant Business, 15 December 2004; 36–37.
- Ruby Tuesday: Smart Eating. MarketWatch: Global Round-up, April 2004; 53.
- Refining the Family Focus. Nation’s Restaurant News, 23 August 2004; 16–18.
- McDonalds Trims Supersized Portions. PT: Magazine of Physical Therapy, March 2004; 11.
- The Low Carb Craze--Fad or Lifestyle? Nation’s Restaurant News, 2004; 30.
- McDonald’s Groups Offer Dieting Tips. Restaurant Business, 1 February 2004; 14.
- It’s OK to appease carb-conscious customers but don’t go hog-wild crazy just to earn dough. Nation’s Restaurant News, 19 April 2004; 19.
- Fast foods: Adding health to the menu. Consumer Reports, September 2004; 28–31.
- The Best Kids Menu In America Contest Winners. Restaurant Hospitality, 20 July 2004; 51–60.
- Allen, R.L.; Gould, A.; Koteff, E.; Garber, A.; Liddle, A.; Franklin, P.; Ruggless, R. Act responsibly: Corporate good deeds help communities and build long-term business. Nation’s Restaurant News, 6 September 2004; 22. [Google Scholar]
- Barrier, B. McDonald’s, Greene go distance to strike healthful balance. Nation’s Restaurant News, 14 June 2004; 40. [Google Scholar]
- Cebrzynski, G. Fresh City starts ‘eat-healthy’ program but keeps emphasis on ‘fresh’. Nation’s Restaurant News, 5 April 2004; 14. [Google Scholar]
- Cobe, P. Green Goddesses. Restaurant Business, 15 October 2004; 56–59. [Google Scholar]
- NRA. 2020 State of the Restaurant Industry; National Restaurant Association: Washington, DC, USA, 2020. [Google Scholar]
- Glanz, K.; Resnicow, K.; Seymour, J.; Hoy, K.; Stewart, H.; Lyons, M.; Goldberg, J. How Major Restaurant Chains Plan Their Menus. Am. J. Prev. Med. 2007, 32, 383–388. [Google Scholar] [CrossRef]
- Khawandanah, J.; Twefik, I. Fad Diets: Lifestyle Promises and Health Challenges. J. Food Res. 2016, 5, 80–94. [Google Scholar] [CrossRef]
- Steenson, S.; Buttriss, J.L. The challenges of defining a healthy and ‘sustainable’ diet. Nutr. Bull. 2020, 45, 206–222. [Google Scholar] [CrossRef]
- Watson, E. Consumers and ‘Clean’ Food: Where Is the Clean Label Going Next? Food Navigator USA. 2017. Available online: http://www.foodnavigator-usa.com/content/view/print/139773 (accessed on 1 December 2020).
- Leone, L.A.; Fleischhacker, S.; Anderson-Steeves, B.; Harper, K.; Winkler, M.; Racine, E.; Baquero, B.; Gittelsohn, J. Healthy Food Retail during the COVID-19 Pandemic: Challenges and Future Directions. Int. J. Environ. Res. Public Health 2020, 17, 7397. [Google Scholar] [CrossRef] [PubMed]
| Strategies | Overall (n = 171) | Type of Restaurant(s) Addressed in Source | Initiator of Change | |||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|
| Corporate-Owned (n = 132) | Independently Owned (n = 27) | Both (n = 12) | Restaurant-Initiated (n = 141) | Investigator-Initiated (n = 30) | ||||||||
| n | % | n | % | n | % | n | % | n | % | n | % | |
| Changes in food availability | ||||||||||||
| General increase in healthy offerings | 98 | 57% | 77 | 58% | 13 | 48% | 8 | 67% | 86 | 61% | 12 | 40% |
| Fruit | 29 | 17% | 26 | 20% | 2 | 7% | 1 | 8% | 27 | 19% | 2 | 7% |
| Salads | 24 | 14% | 23 | 17% | 1 | 4% | 0 | 0% | 24 | 17% | 0 | 0% |
| Vegetables | 29 | 17% | 19 | 14% | 5 | 19% | 5 | 42% | 27 | 19% | 2 | 7% |
| Whole grains | 12 | 7% | 11 | 8% | 1 | 4% | 0 | 0% | 11 | 8% | 1 | 3% |
| Healthier beverages | 15 | 9% | 9 | 7% | 2 | 7% | 4 | 33% | 9 | 6% | 6 | 20% |
| Sustainable/clean offerings | 38 | 22% | 29 | 22% | 5 | 19% | 4 | 33% | 38 | 27% | 0 | 0% |
| Diet “fad” offerings | 19 | 11% | 15 | 11% | 2 | 7% | 2 | 17% | 19 | 13% | 0 | 0% |
| Environmental facilitators | ||||||||||||
| Provision of nutrition information | 43 | 25% | 30 | 23% | 10 | 37% | 3 | 25% | 29 | 21% | 14 | 47% |
| Changes in portion size offerings | 29 | 17% | 20 | 15% | 5 | 19% | 4 | 33% | 21 | 15% | 8 | 27% |
| Pricing schemes to favor healthy options | 19 | 11% | 12 | 9% | 5 | 19% | 2 | 17% | 9 | 6% | 10 | 33% |
| Promotion of healthy options | 52 | 30% | 34 | 26% | 12 | 44% | 6 | 50% | 35 | 25% | 17 | 57% |
| Encouraging healthy substitutions | 20 | 12% | 19 | 14% | 0 | 0% | 1 | 8% | 18 | 13% | 2 | 7% |
| Motivation | Type of Restaurant(s) Addressed in Source | Initiator of Change | ||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|
| Overall (n = 171) | Corporate-Owned (n = 132) | Independently Owned (n = 27) | Both (n = 12) | Restaurant-Initiated (n = 141) | Investigator-Initiated (n = 30) | |||||||
| Motivation not reported | 40 | 23% | 25 | 19% | 11 | 41% | 4 | 33% | 19 | 13% | 21 | 70% |
| Profit-driven | ||||||||||||
| Perceived customer demand | 74 | 56% 1 | 64 | 60% | 5 | 31% | 5 | 63% | 73 | 60% | 1 | 11% |
| Want to increase profit | 9 | 7% | 8 | 7% | 1 | 6% | 0 | 0% | 8 | 7% | 1 | 11% |
| Recognizing health as business opportunity | 12 | 9% | 8 | 7% | 4 | 25% | 0 | 0% | 12 | 10% | 0 | 0% |
| Following food trends | 4 | 3% | 3 | 3% | 0 | 0% | 1 | 13% | 4 | 3% | 0 | 0% |
| Business promotion opportunity | 9 | 7% | 6 | 6% | 2 | 13% | 1 | 13% | 5 | 4% | 4 | 44% |
| Intrinsic motivations/factors | ||||||||||||
| Want to improve community health | 35 | 27% | 20 | 19% | 13 | 81% | 2 | 25% | 30 | 25% | 5 | 56% |
| Desire to innovate | 3 | 2% | 1 | 1% | 0 | 0% | 2 | 25% | 3 | 2% | 0 | 0% |
| Top-down pressure | ||||||||||||
| Public health criticism | 29 | 22% | 27 | 25% | 1 | 6% | 1 | 13% | 28 | 23% | 1 | 11% |
| Mandates/guidelines | 5 | 4% | 4 | 4% | 1 | 6% | 0 | 0% | 4 | 3% | 1 | 11% |
| External factors | ||||||||||||
| Food sourcing/availability | 2 | 2% | 2 | 2% | 0 | 0% | 0 | 0% | 2 | 2% | 0 | 0% |
| Barriers | Overall (n = 171) | Type of Restaurant(s) Addressed in Source | Initiator of Change | |||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|
| Corporate-Owned (n = 132) | Independently Owned (n = 27) | Both (n = 12) | Restaurant-Initiated (n = 141) | Investigator-Initiated (n = 30) | ||||||||
| Barrier not reported | 119 | 70% | 98 | 74% | 14 | 52% | 7 | 58% | 103 | 73% | 16 | 53% |
| Profit-related | ||||||||||||
| Worry about revenue decrease | 22 | 42% 1 | 11 | 32% | 7 | 54% | 4 | 80% | 13 | 34% | 9 | 64% |
| Worry about customer acceptance | 25 | 48% | 21 | 62% | 3 | 23% | 1 | 20% | 24 | 63% | 1 | 7% |
| Customer demand for unhealthy options | 3 | 6% | 2 | 6% | 1 | 8% | 0% | 2 | 5% | 1 | 7% | |
| Personal/intrinsic barriers | ||||||||||||
| Lack of interest or recognition regarding the role of restaurants in health promotion | 9 | 17% | 1 | 3% | 5 | 38% | 3 | 60% | 2 | 5% | 7 | 50% |
| Time constraints | 11 | 21% | 3 | 9% | 5 | 38% | 3 | 60% | 5 | 13% | 6 | 43% |
| Physical environment barriers | ||||||||||||
| Food sourcing constraints (cost, access) | 12 | 23% | 10 | 29% | 1 | 8% | 1 | 20% | 10 | 26% | 2 | 14% |
| Spatial limitations (kitchen or restaurant space) | 3 | 6% | 1 | 3% | 2 | 15% | 0% | 1 | 3% | 2 | 14% | |
| Staff-related constraints issues (i.e., Staff turnover, knowledge and culinary skills.) | 2 | 4% | 0% | 1 | 8% | 1 | 20% | 1 | 3% | 1 | 7% | |
| Food/recipe limitations | 4 | 8% | 2 | 6% | 2 | 15% | 0% | 2 | 5% | 2 | 14% | |
| Outcomes | Overall (n = 171) | Type of Restaurant(s) Addressed in Source | Initiator of Change | |||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|
| Corporate-Owned (n = 132) | Independently Owned (n = 27) | Both (n = 12) | Restaurant-Initiated (n = 141) | Investigator-Initiated (n = 30) | ||||||||
| n | % | n | % | n | % | n | % | n | % | n | % | |
| Outcomes not reported | 109 | 64% | 98 | 74% | 6 | 22% | 5 | 42% | 108 | 77% | 1 | 3% |
| Revenue positive | ||||||||||||
| Revenue increased | 16 | 26% 1 | 10 | 29% | 4 | 19% | 2 | 29% | 12 | 36% | 4 | 14% |
| Customer accepted change | 17 | 27% | 7 | 21% | 7 | 33% | 3 | 43% | 8 | 24% | 9 | 31% |
| Restaurant promotion/visibility | 6 | 10% | 5 | 15% | 0 | 0% | 1 | 14% | 4 | 12% | 2 | 7% |
| Revenue negative | ||||||||||||
| Revenue decreased | 2 | 3% | 1 | 3% | 1 | 5% | 0 | 0% | 1 | 3% | 1 | 3% |
| Customer did not like change | 2 | 3% | 2 | 6% | 0 | 0% | 0 | 0% | 2 | 6% | 0 | 0% |
| Revenue neutral | ||||||||||||
| Mixed (customer acceptance) | 2 | 3% | 2 | 6% | 0 | 0% | 0 | 0% | 2 | 6% | 0 | 0% |
| Revenue not affected | 2 | 3% | 1 | 3% | 1 | 5% | 0 | 0% | 0 | 0% | 2 | 7% |
| Health-improving outcomes | ||||||||||||
| Customer improved eating behaviors | 15 | 24% | 4 | 12% | 10 | 48% | 1 | 14% | 1 | 3% | 14 | 48% |
| Restaurant accepted intervention (investigator-initiated only) | 6 | 10% | 0 | 0% | 5 | 24% | 1 | 14% | 0% | 6 | 21% | |
| Restaurant nutrition environment improved | 15 | 24% | 5 | 15% | 6 | 29% | 4 | 57% | 5 | 15% | 10 | 34% |
| Restaurant staff increased nutrition knowledge | 4 | 6% | 0 | 0% | 3 | 14% | 1 | 14% | 0 | 0% | 4 | 14% |
| Other | ||||||||||||
| Mixed (restaurant acceptability) | 1 | 2% | 1 | 3% | 0 | 0% | 0 | 0% | 1 | 3% | 0 | 0% |
| No change in eating behaviors | 2 | 3% | 2 | 6% | 0 | 0% | 0 | 0% | 0 | 0% | 2 | 7% |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Fuster, M.; Handley, M.A.; Alam, T.; Fullington, L.A.; Elbel, B.; Ray, K.; Huang, T.T.-K. Facilitating Healthier Eating at Restaurants: A Multidisciplinary Scoping Review Comparing Strategies, Barriers, Motivators, and Outcomes by Restaurant Type and Initiator. Int. J. Environ. Res. Public Health 2021, 18, 1479. https://doi.org/10.3390/ijerph18041479
Fuster M, Handley MA, Alam T, Fullington LA, Elbel B, Ray K, Huang TT-K. Facilitating Healthier Eating at Restaurants: A Multidisciplinary Scoping Review Comparing Strategies, Barriers, Motivators, and Outcomes by Restaurant Type and Initiator. International Journal of Environmental Research and Public Health. 2021; 18(4):1479. https://doi.org/10.3390/ijerph18041479
Chicago/Turabian StyleFuster, Melissa, Margaret A. Handley, Tamara Alam, Lee Ann Fullington, Brian Elbel, Krishnendu Ray, and Terry T-K Huang. 2021. "Facilitating Healthier Eating at Restaurants: A Multidisciplinary Scoping Review Comparing Strategies, Barriers, Motivators, and Outcomes by Restaurant Type and Initiator" International Journal of Environmental Research and Public Health 18, no. 4: 1479. https://doi.org/10.3390/ijerph18041479
APA StyleFuster, M., Handley, M. A., Alam, T., Fullington, L. A., Elbel, B., Ray, K., & Huang, T. T.-K. (2021). Facilitating Healthier Eating at Restaurants: A Multidisciplinary Scoping Review Comparing Strategies, Barriers, Motivators, and Outcomes by Restaurant Type and Initiator. International Journal of Environmental Research and Public Health, 18(4), 1479. https://doi.org/10.3390/ijerph18041479







