Preliminary Study on the Effect of an Early Physical Therapy Intervention after Sentinel Lymph Node Biopsy: A Multicenter Non-Randomized Controlled Trial
Abstract
1. Introduction
2. Materials and Methods
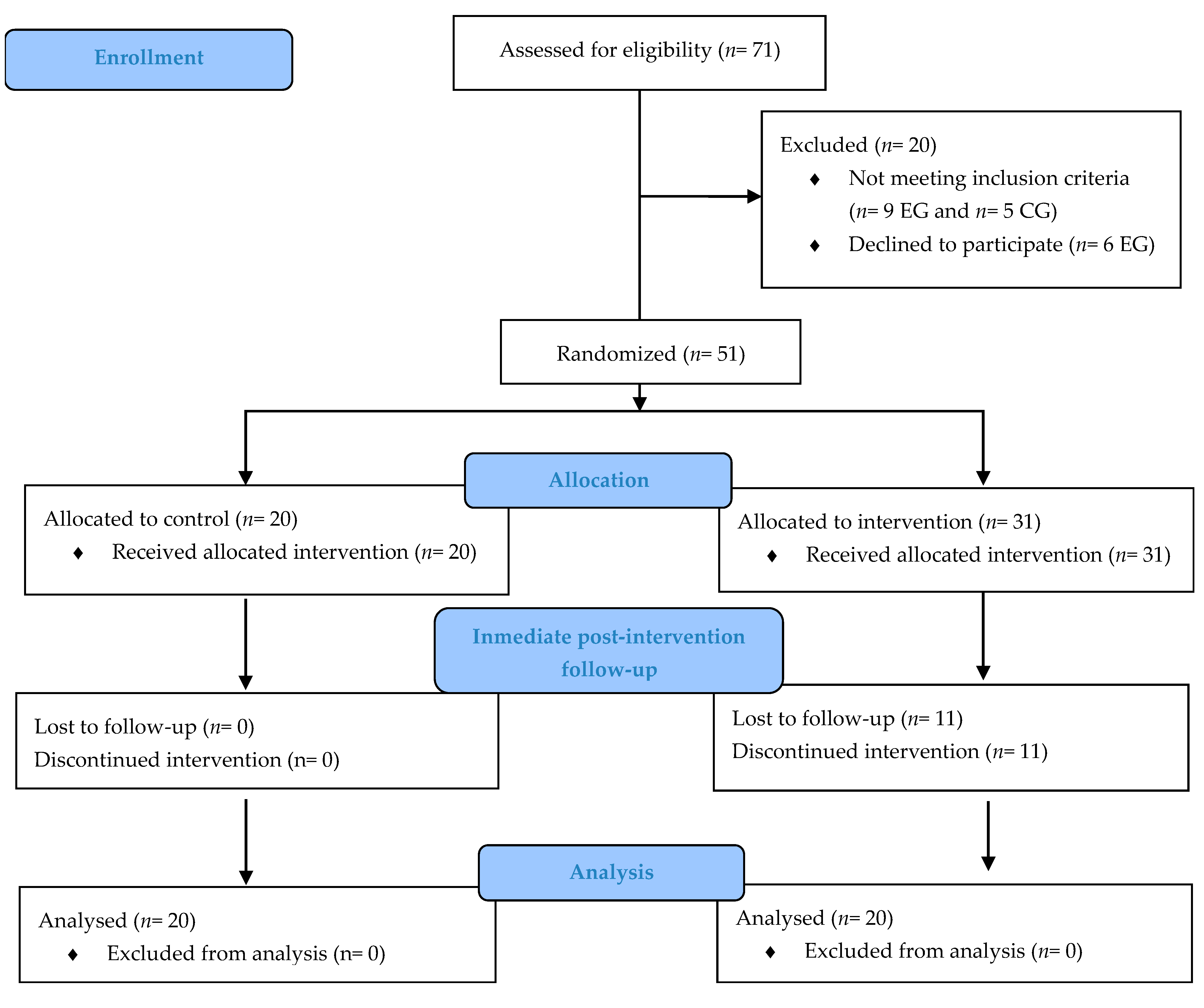
2.1. Study Design
2.2. Participants and Setting
2.3. Outcome Measures
2.3.1. Range of Motion (ROM)
2.3.2. Strength
2.3.3. Pain and Disability
2.3.4. State of Scar
2.3.5. Tissue Adhesions/Myofascial Adhesions
2.3.6. Quality of Life
2.3.7. Axillary Web Syndrome
2.3.8. Lymphoedema
2.4. Interventions
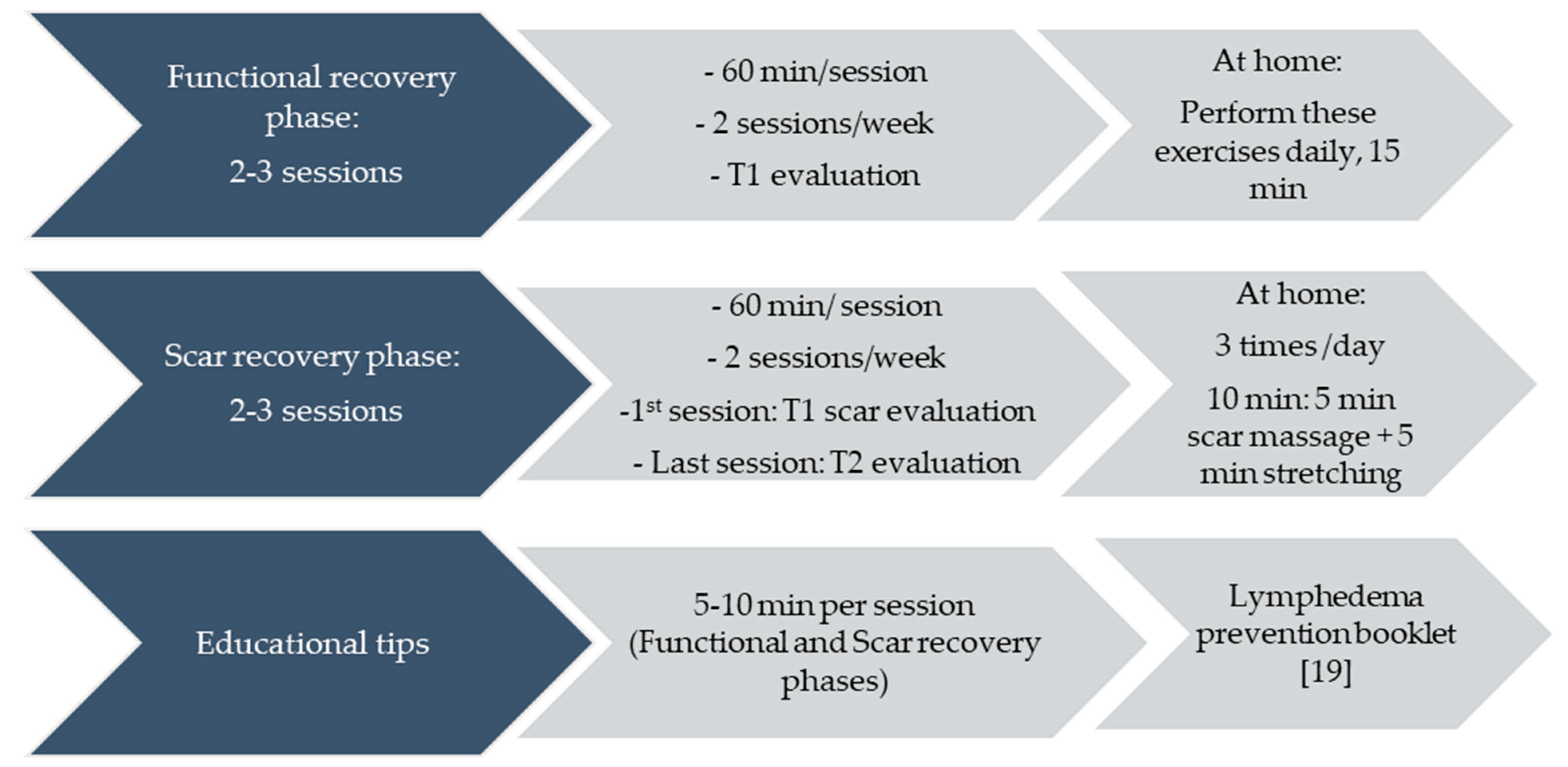
2.4.1. Experimental Group
Functional Recovery
Functional Recovery Exercises
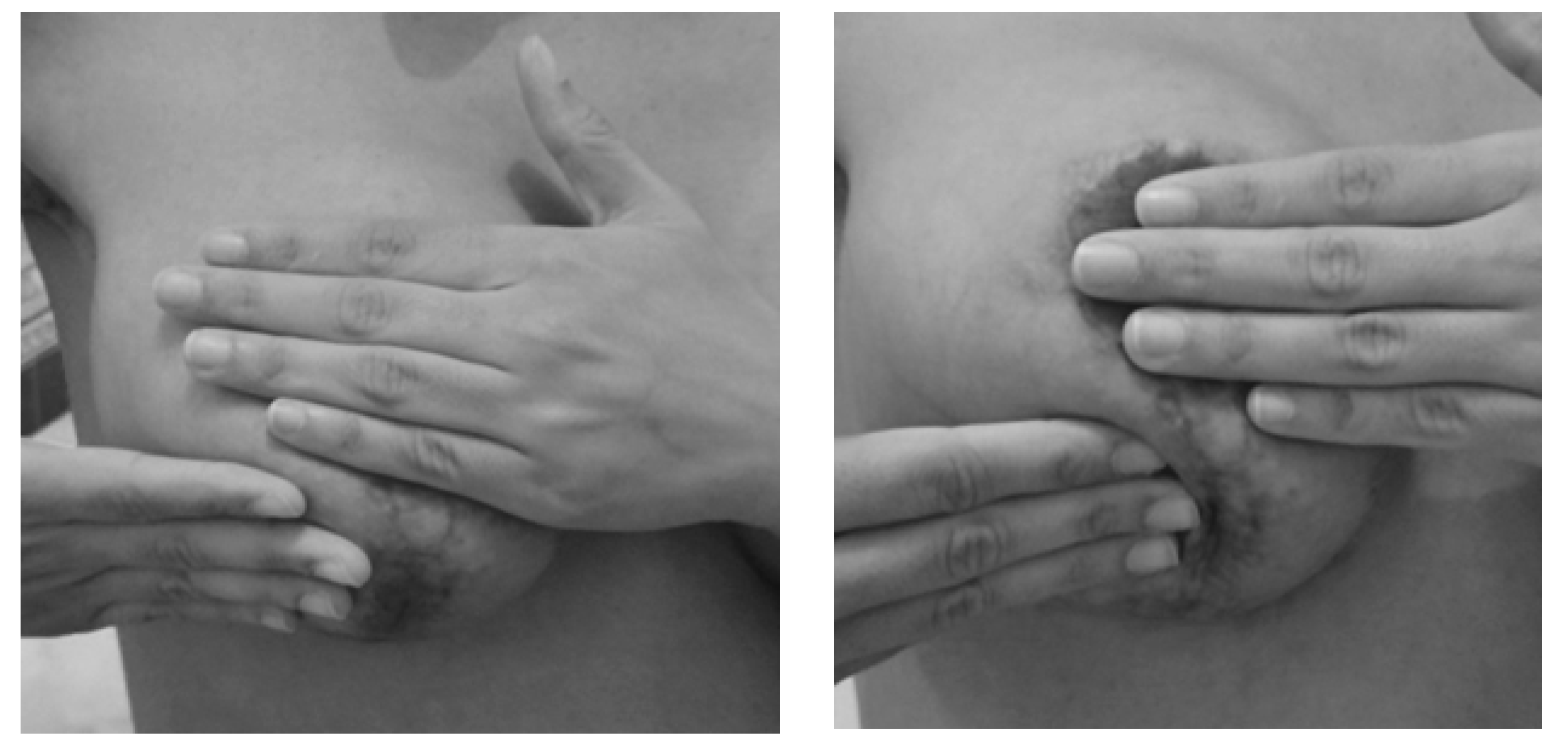
Scar Treatment
Scar Exercises
Educational Tips for Lymphoedema Prevention
2.4.2. Control Group
2.5. Statistical Analysis
3. Results
Preliminary Data of Clinical Outcomes
4. Discussion
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Zeitoun, J.; Babin, G.; Lebrun, J.F. Ganglion sentinelle et cancer du sein: Où en est-on en 2019. Gynécologie Obs. Fertil Sénologie 2019, 47, 522–526. [Google Scholar] [CrossRef]
- Tardieu, A.; Mesnard, C.; Margueritte, F.; Mollard, J.; Lacorre, A.; Aubard, Y.; Deluche, E.; Gauthier, T. Récidive axillaire après prélèvement du ganglion sentinelle avant chimiothérapie néoadjuvante dans le cancer du sein. Gynécologie Obs. Fertil Sénologie 2018, 46, 509–513. [Google Scholar] [CrossRef] [PubMed]
- Qu, L.T.; Peters, S.; Cobb, A.N.; Godellas, C.V.; Perez, C.B.; Vaince, F.T. Considerations for sentinel lymph node biopsy in breast cancer patients with biopsy proven axillary disease prior to neoadjuvant treatment. Am. J. Surg. 2018, 215, 530–533. [Google Scholar] [CrossRef]
- Qiu, S.-Q.; Zhang, G.-J.; Jansen, L.; De Vries, J.; Schröder, C.P.; De Vries, E.G.; Van Dam, G.M. Evolution in sentinel lymph node biopsy in breast cancer. Crit. Rev. Oncol. Hematol. 2018, 123, 83–94. [Google Scholar] [CrossRef] [PubMed]
- Möller, U.O.; Beck, I.; Rydén, L.; Malmström, M. A comprehensive approach to rehabilitation interventions following breast cancer treatment-a systematic review of systematic reviews. BMC Cancer 2019, 19, 472. [Google Scholar]
- Sagen, A.; Kaaresen, R.; Sandvik, L.; Thune, I.; Risberg, M.A. Upper limb physical function and adverse effects after breast cancer surgery: A prospective 2.5-year follow-up study and preoperative measures. Arch. Phys. Med. Rehabil. 2014, 95, 875–881. [Google Scholar] [CrossRef]
- Belmonte, R.; Garin, O.; Segura, M.; Pont, A.; Escalada, F.; Ferrer, M. Quality-of-life impact of sentinel lymph node biopsy versus axillary lymph node dissection in breast cancer patients. Value Heal. 2012, 15, 907–915. [Google Scholar] [CrossRef] [PubMed]
- De Groef, A.; Van Kampen, M.; Tieto, E.; Schönweger, P.; Christiaens, M.R.; Neven, P.; Geraerts, I.; Gebruers, N.; Devoogdt, N. Arm lymphoedema and upper limb impairments in sentinel node-negative breast cancer patients: A one year follow-up study. Breast 2016, 29, 102–108. [Google Scholar] [CrossRef]
- Głowacka-Mrotek, I.; Tarkowska, M.; Nowikiewicz, T.; Siedlecki, Z.; Zegarski, W.; Hagner, W. Evaluation of distant sequelae of breast cancer treatment among patients after breast-conserving surgery depending on the type of intervention in the axillary fossa. Wspolczesna Onkol. 2018, 22, 240–246. [Google Scholar] [CrossRef]
- Figueira, P.V.G.; Haddad, C.A.S.; de Almeida Rizzi, S.K.L.; Facina, G.; Nazario, A.C.P. Diagnosis of Axillary Web Syndrome in Patients After Breast Cancer Surgery: Epidemiology, Risk Factors, and Clinical Aspects: A Prospective Study. Am. J. Clin. Oncol. 2018, 41, 992–996. [Google Scholar] [CrossRef] [PubMed]
- Koehler, L.A.; Haddad, T.C.; Hunter, D.W.; Tuttle, T.M. Axillary web syndrome following breast cancer surgery: Symptoms, complications, and management strategies. Breast cancer 2019, 11, 13–19. [Google Scholar] [CrossRef] [PubMed]
- Gebruers, N.; Verbelen, H.; De Vrieze, T.; Coeck, D.; Tjalma, W. Incidence and Time Path of Lymphedema in Sentinel Node Negative Breast Cancer Patients: A Systematic Review. Arch. Phys. Med. Rehabil. 2015, 96, 1131–1139. [Google Scholar] [CrossRef] [PubMed]
- Yen, T.W.F.; Fan, X.; Sparapani, R.; Laud, P.W.; Walker, A.P.; Nattinger, A.B. A Contemporary, Population-Based Study of Lymphedema Risk Factors in Older Women with Breast Cancer. Ann. Surg. Oncol. 2009, 16, 979–988. [Google Scholar] [CrossRef]
- Gass, J.; Mitchell, S.; Hanna, M. How do breast cancer surgery scars impact survivorship? Findings from a nationwide survey in the United States. BMC Cancer 2019, 19, 342. [Google Scholar] [CrossRef] [PubMed]
- Delay, E.; Gosset, J.; Toussoun, G.; Delaporte, T.; Delbaere, M. Séquelles thérapeutiques du sein après traitement conservateur du cancer du sein. Ann. Chir. Plast. Esthétique 2008, 53, 135–152. [Google Scholar] [CrossRef]
- De Groef, A.; Van Kampen, M.; Verlvoesem, N.; Dieltjens, E.; Vos, L.; De Vrieze, T.; Christiaens, M.R.; Neven, P.; Geraerts, I.; Devoogdt, N. Effect of myofascial techniques for treatment of upper limb dysfunctions in breast cancer survivors: Randomized controlled trial. Support. Care Cancer 2017, 25, 2119–2127. [Google Scholar] [CrossRef]
- Serra-Añó, P.; Inglés, M.; Bou-Catalá, C.; Iraola-Lliso, A.; Espí-López, G.V. Effectiveness of myofascial release after breast cancer surgery in women undergoing conservative surgery and radiotherapy: A randomized controlled trial. Support. Care Cancer 2019, 27, 2633–2641. [Google Scholar] [CrossRef] [PubMed]
- Scaffidi, M.; Vulpiani, M.C.; Vetrano, M.; Conforti, F.; Marchetti, M.R.; Bonifacino, A.; Marchetti, P.; Saraceni, V.M.F.A. Early rehabilitation reduces the onset of complications in the upper limb following breast cancer surgery. Eur. J. Phys. Rehabil. Med. 2012, 48, 601–611. [Google Scholar]
- Ostos-Díaz, B.; Casuso-Holgado, M.J.; Muñoz-Fernández, M.J.; Carazo, A.F.; Martín-Valero, R.; Medrano-Sánchez, E.M. Early Physical Rehabilitation after Sentinel Lymph Node Biopsy in Breast Cancer: Is It Feasible and Safe? Int. J. Environ. Res. Public Health 2020, 17, 8382. [Google Scholar] [CrossRef]
- Schulz, K.F.; Altman, D.G.; Moher, D. CONSORT 2010 Statement: Updated guidelines for reporting parallel group randomised trials. BMJ 2010, 340, 698–702. [Google Scholar] [CrossRef] [PubMed]
- Springer, B.A.; Levy, E.; McGarvey, C.; Pfalzer, L.A.; Stout, N.L.; Gerber, L.H.; Soballe, P.W.; Danoff, J. Pre-operative assessment enables early diagnosis and recovery of shoulder function in patients with breast cancer. Breast Cancer Res. Treat. 2010, 120, 135–147. [Google Scholar] [CrossRef] [PubMed]
- Rogers, B.H.; Brown, J.C.; Gater, D.R.; Schmitz, K.H. Association Between Maximal Bench Press Strength and Isometric Handgrip Strength Among Breast Cancer Survivors. Arch. Phys. Med. Rehabil. 2017, 98, 264–269. [Google Scholar] [CrossRef] [PubMed]
- Breckenridge, J.D.; McAuley, J.H. Shoulder Pain and Disability Index (SPADI). J. Physiother. 2011, 57, 197. [Google Scholar] [CrossRef]
- Torres-Lacomba, M.; Sánchez-Sánchez, B.; Prieto-Gómez, V.; Pacheco-da-Costa, S.; Yuste-Sánchez, M.J.; Navarro-Brazález, B.; Gutiérrez-Ortega, C. Spanish cultural adaptation and validation of the shoulder pain and disability index, and the oxford shoulder score after breast cancer surgery. Health Qual. Life Outcomes 2015, 13, 63. [Google Scholar] [CrossRef] [PubMed]
- Membrilla-Mesa, M.D.; Cuesta-Vargas, A.I.; Pozuelo-Calvo, R.; Tejero-Fernández, V.; Martín-Martín, L.; Arroyo-Morales, M. Shoulder pain and disability index: Cross cultural validation and evaluation of psychometric properties of the Spanish version. Health Qual. Life Outcomes 2015, 21, 200. [Google Scholar] [CrossRef] [PubMed]
- Draaijers, L.J.; Tempelman, F.R.H.; Botman, Y.A.M.; Tuinebreijer, W.E.; Middelkoop, E.; Kreis, R.W.; Van Zuijlen, P.P.M. The Patient and Observer Scar Assessment Scale: A Reliable and Feasible Tool for Scar Evaluation. Plast. Reconstr. Surg. 2004, 113, 1960–1965. [Google Scholar] [CrossRef] [PubMed]
- Truong, P.T.; Lee, J.C.; Soer, B.; Gaul, C.A.; Olivotto, I.A. Reliability and Validity Testing of the Patient and Observer Scar Assessment Scale in Evaluating Linear Scars after Breast Cancer Surgery. Plast. Reconstr. Surg. 2007, 119, 487–494. [Google Scholar] [CrossRef]
- De Groef, A.; Van Kampen, M.; Vervloesem, N.; De Geyter, S.; Dieltjens, E.; Christiaens, M.R.; Neven, P.; Geraerts, I.; Devoogdt, N. An evaluation tool for myofascial adhesions in patients after breast cancer (MAP-BC evaluation tool): Development and interrater reliability. PLoS ONE 2017, 12, 1–10. [Google Scholar] [CrossRef]
- De Groef, A.; Van Kampen, M.; Moortgat, P.; Anthonissen, M.; Van den Kerckhove, E.; Christiaens, M.R.; Neven, P.; Geraerts, I.; Devoogdt, N. An evaluation tool for Myofascial Adhesions in Patients after Breast Cancer (MAP-BC evaluation tool): Concurrent, face and content validity. PLoS ONE 2018, 13, 1–12. [Google Scholar] [CrossRef]
- Irarrázaval, M.E.; Rodriguez, P.F.; Fasce, G.; Silva, F.W.; Waintrub, H.; Torres, C.; Barriga, C.; Fritis, M.; Marin, L. Validation of BR23 questionnaire for the assessment of quality of life of breast cancer patients in Chile. Artículos Investig. 2013, 141, 723–734. [Google Scholar]
- Lancaster, G.; Dodd, S.; Williamson, P.R. Design and analysis of pilot studies: Recommendations for good practice. J. Eval. Clin. Pract. 2001, 10, 307–312. [Google Scholar] [CrossRef] [PubMed]
- Peintinger, F.; Reitsamer, R.; Stranzl, H.; Ralph, G. Comparison of quality of life and arm complaints after axillary lymph node dissection vs sentinel lymph node biopsy in breast cancer patients. Br. J. Cancer 2003, 89, 648–652. [Google Scholar] [CrossRef] [PubMed]
- Beurskens, C.H.G.; van Uden, C.J.T.; Strobbe, L.J.A.; Oostendorp, R.A.B.; Wobbes, T. The efficacy of physiotherapy upon shoulder function following axillary dissection in breast cancer, a randomized controlled study. BMC Cancer 2007, 7, 1–6. [Google Scholar] [CrossRef] [PubMed]
- Testa, A.; Iannace, C.; Di Libero, L. Strengths of early physical rehabilitation programs in surgical breast cancer patients: Results of a randomized controlled study. Eur. J. Phys. Rehabil. Med. 2014, 50, 275–284. [Google Scholar] [CrossRef] [PubMed]
- Hsiao, P.-C.; Hong, R.-B.; Chou, W.; Lu, S.-R. Role of physiotherapy and patient education in lymphedema control following breast cancer surgery. Ther. Clin. Risk Manag. 2015, 11, 319–327. [Google Scholar] [CrossRef][Green Version]
- Lacomba, M.T.; Sánchez, M.J.Y.; Goñi, Á.Z.; Merino, D.P.; del Moral, O.M.; Téllez, E.C.; Mogollón, E.M. Effectiveness of early physiotherapy to prevent lymphoedema after surgery for breast cancer: Randomised, single blinded, clinical trial. BMJ 2010, 340, 140. [Google Scholar]
- Sato, F.; Ishida, T.; Ohuchi, N. The Perioperative Educational Program for Improving Upper Arm Dysfunction in Patients with Breast Cancer: A Controlled Trial. Tohoku J. Exp. Med. 2014, 232, 115–122. [Google Scholar] [CrossRef]
- Koehler, L.A.; Hunter, D.W.; Blaes, A.H.; Haddad, T.C. Function, shoulder motion, pain, and lymphedema in breast cancer with and without axillary web syndrome: An 18-month follow-up. Phys. Ther. 2018, 98, 518–527. [Google Scholar] [CrossRef]

| T0 Evaluation | T1 Evaluation | T2 Evaluation | 6 Months Follow-Up |
|---|---|---|---|
| Upper limb function: Shoulder ROM Grip strength Upper limb pain and disability (SPADI) Quality of life (EORTCQLQ- BR-23) | Upper limb function: Shoulder ROM Grip strength Upper limb pain and disability (SPADI) Scar-recovery outcomes:State of scar (POSAS) Tissue adhesions (MAP-BC) Quality of life (EORTCQLQ- BR-23) | T1 measurements plus: Axillary web syndrome exploration Lymphoedema exploration | Lymphoedema surveillance |
| EG (N = 20) Mean (SD) Median (Range) | CG (N = 20) Mean (SD) Median (Range) | p Values | |
|---|---|---|---|
| Age (years) | 59.25 (7.52) | 64.15 (11.78) | 0.125 |
| BodyMassIndex | 25.73 (4.31) | 26.76 (3.17) | 0.401 |
| Ethinicity (C/L) | 19/1 | 20/0 | 0.311 |
| Type of BreastCancer DCIS IDC LCIS Others | 4 15 1 0 | 1 14 1 4 | 0.098 |
| Stage of BreastCancer IA IB IIA IIB IIIA Missing | 11 1 3 1 1 3 | 15 1 2 2 - - | 0.751 |
| Type of breastsurgery (SUM/BCS) | 2/18 | 5/15 | 0.215 |
| Numbers of lymphnodesremoved a | 2 (0.75) | 2 (1.75) | 0.760 |
| Positive LymphNodes a | 0.00 (0.00) | 0.00 (0.00) | 0.553 |
| Side Involved Right Left | 9 11 | 9 11 | - |
| Involvedsidetohanddominance (Yes/No) | 11/9 | 8/12 | 0.342 |
| AdjuvantTherapy: chemotherapy (Yes/No) | 4/16 | 5/15 | 0.705 |
| Numbers of sessions of adjuvanttherapy a | 7.50 (5.50) | 15.00 (8.00) | 0.079 |
| ROM a | 100.00 (8.55) | 100.00 (0.00) | 0.309 |
| Gripstrength | 10.35 (4.45) | 18.85 (6.01) | 0.000 |
| Global SPADI a | 5.50 (17.50) | 6.00 (15.25) | 0.806 |
| QoLFunction | 54.17 (12.83) | 54.90 (19.37) | 0.889 |
| QoLSymptoms a | 7.80 (13.89) | 11.18 (25.80) | 0.588 |
| Outcomes | Experimental Group (n = 20) | Control Group (n = 20) | EG/CG p-Values | Effect Sizes | ||||
|---|---|---|---|---|---|---|---|---|
| Pre-Intervention T1 | Post-Intervention T2 | p-Values | Pre-Intervention T1 | Post-Intervention T2 | p-Values | |||
| ROM a | 94.87 (26.92) | 100.00 (0.00) | 0.003 | 90.60 (29.49) | 100.00 (29.91) | 0.498 | 0.006 | 0.43 |
| GripStrength a | 14.85 (9.18) | 15.15 (6.67) | 0.113 | 18.88 (6.45) | 18.62 (6.54) | 0.380 | 0.041 | 0.32 |
| Global SPADI | 32.30 (26.84) | 14.55(14.95) | 0.001 | 27.90 (28.84) | 24.15 (25.88) | 0.466 | 0.046 | 0.45 |
| POSAS | 25.90 (9.57) | 9.00 (5.60) | 0.000 | 21.30 (11.32) | 20.70 (11.67) | 0.709 | 0.000 | 1.28 |
| MAP-BC | 28.15 (9.66) | 5.70 (5.33) | 0.000 | 19.10 (11.04) | 24.70 (13.79) | 0.002 | 0.004 | 1.82 |
| QoLFunction | 47.71 (11.29) | 53.72 (12.55) | 0.013 | 44.59 (15.69) | 58.78 (14.54) | 0.000 | 0.011 | 0.37 |
| QoLSymptoms | 20.31 (14.40) | 17.09 (10.89) | 0.072 | 17.54 (10.42) | 17.54 (12.32) | 0.999 | 0.296 | 0.038 |
| Axillary web syndrome | - | 2 (10%) | - | - | 0 (0%) | - | 0.244 | |
| Lymphedema | - | 0 (0%) | - | - | 0 (0%) | - | - |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Muñoz-Fernández, M.J.; Medrano-Sánchez, E.M.; Ostos-Díaz, B.; Martín-Valero, R.; Suárez-Serrano, C.; Casuso-Holgado, M.J. Preliminary Study on the Effect of an Early Physical Therapy Intervention after Sentinel Lymph Node Biopsy: A Multicenter Non-Randomized Controlled Trial. Int. J. Environ. Res. Public Health 2021, 18, 1275. https://doi.org/10.3390/ijerph18031275
Muñoz-Fernández MJ, Medrano-Sánchez EM, Ostos-Díaz B, Martín-Valero R, Suárez-Serrano C, Casuso-Holgado MJ. Preliminary Study on the Effect of an Early Physical Therapy Intervention after Sentinel Lymph Node Biopsy: A Multicenter Non-Randomized Controlled Trial. International Journal of Environmental Research and Public Health. 2021; 18(3):1275. https://doi.org/10.3390/ijerph18031275
Chicago/Turabian StyleMuñoz-Fernández, María Jesús, Esther M. Medrano-Sánchez, Beatriz Ostos-Díaz, Rocío Martín-Valero, Carmen Suárez-Serrano, and María Jesús Casuso-Holgado. 2021. "Preliminary Study on the Effect of an Early Physical Therapy Intervention after Sentinel Lymph Node Biopsy: A Multicenter Non-Randomized Controlled Trial" International Journal of Environmental Research and Public Health 18, no. 3: 1275. https://doi.org/10.3390/ijerph18031275
APA StyleMuñoz-Fernández, M. J., Medrano-Sánchez, E. M., Ostos-Díaz, B., Martín-Valero, R., Suárez-Serrano, C., & Casuso-Holgado, M. J. (2021). Preliminary Study on the Effect of an Early Physical Therapy Intervention after Sentinel Lymph Node Biopsy: A Multicenter Non-Randomized Controlled Trial. International Journal of Environmental Research and Public Health, 18(3), 1275. https://doi.org/10.3390/ijerph18031275







