Adverse Effects of the COVID-19 Pandemic on Movement and Play Behaviours of Children and Youth Living with Disabilities: Findings from the National Physical Activity Measurement (NPAM) Study
Abstract
:1. Introduction
2. Materials and Methods
2.1. Study Design and Sample
2.2. Survey Development
2.3. Survey Distribution and Data Collection
2.4. Statistical Analysis
3. Results
3.1. Participants
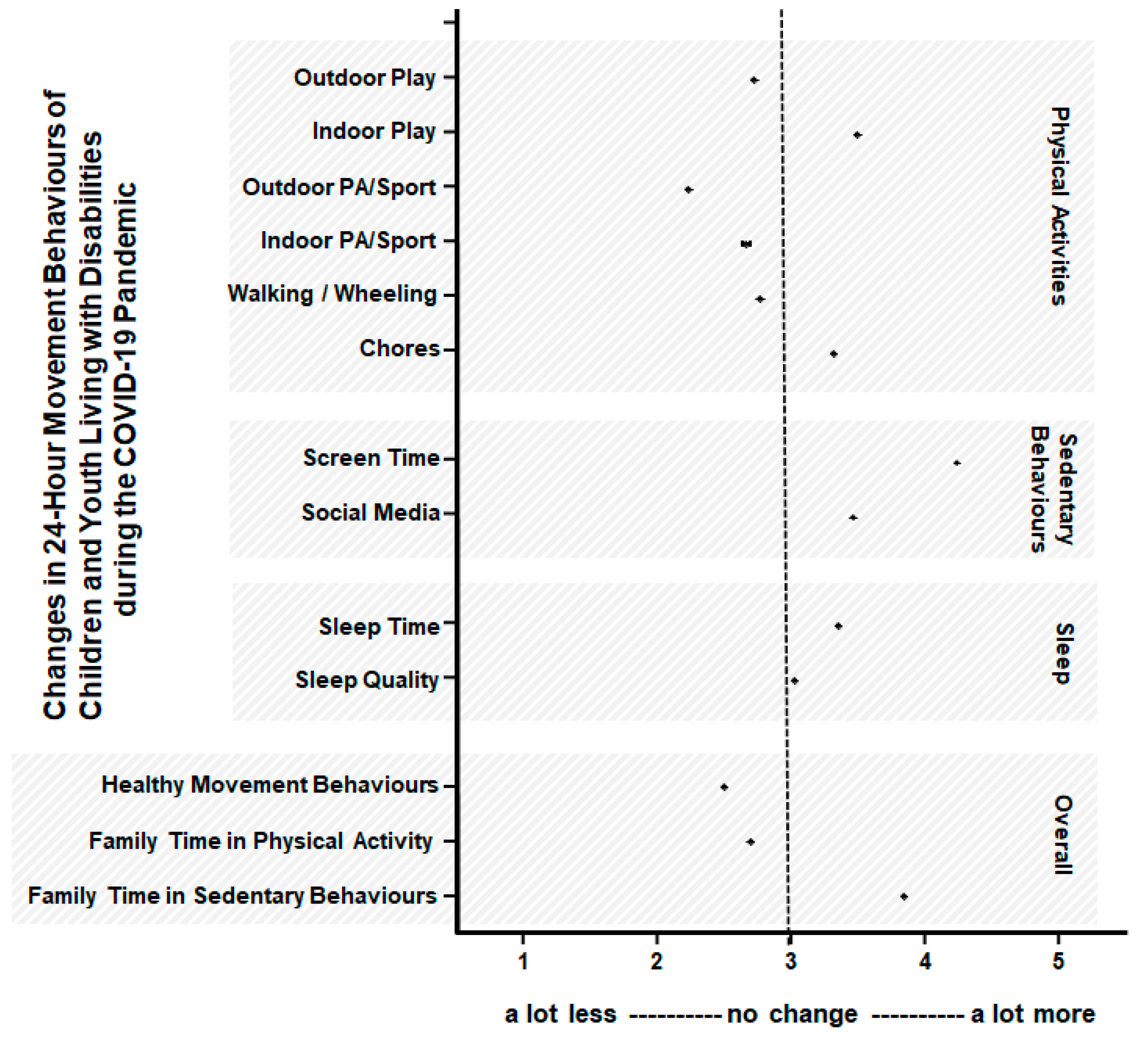
3.2. Movement and Play Behaviours in Children and Youth Living with Disabilities
3.3. Asscoations between Parental Demographics and Child Movement and Play Behaviours
3.4. Changes in Parental Support Variables during COVID-19
3.5. Associations between Parental Support and Child Movement and Play Behaviours
4. Discussion
4.1. Summary of Findings
4.2. COVID-19 and Related Restrictions Exacerbated Barriers to Movement and Play Declined
4.3. Parent Support Contributes to Healthy Movement Behaviours
4.4. Returning to Healthy Movement and Play
4.5. Strengths, Limitations, and Future Directions
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
Appendix A
| Survey Items | Response Options |
|---|---|
| |
| Has anyone in your household been diagnosed with COVID-19? | Yes [thank you, terminate] No [continue] |
| Is your household under a self-isolation or quarantine order? | Yes [thank you, terminate] No [continue] |
| |
| Age | [age rollup] |
| Gender | [gender rollup] |
| Canada regions | [provinces, territories rollup] |
| Ethnicity | [ethnicity rollup] |
| Marital status | [marital status rollup] |
| Employment | [employment status rollup] |
| Education | [education rollup] |
| Household income | [household income rollup] |
| Household make-up (number of adults) | [number of adults rollup] |
| Household make-up (number of children) | [number of children rollup] |
| Type of residence | [type of residence rollup] |
| Residence postal code | Text field |
| |
| Age | [age rollup] |
| Gender | [gender rollup] |
| Ethnicity | [ethnicity rollup] |
| Disability | [disability rollup] |
| |
| In the last week, how many total hours and minutes per day did your child watch TV, use the computer, use social media, or play inactive video games? | Weekdays (per day) _______ Hours AND Minutes Don’t know Weekend (per day)_______ Hours AND Minutes Don’t know |
| In the last week, on how many days was your child physically active, so much that they were out of breath or sweating, for at least 60 min per day? | Drop down <<< 0–7 days >>> |
| In the last week, on how many days did your child engage in light physical activity for 2 or more hours per day? | Drop down <<<0–7 days>>> |
| In the last week, how many hours did your child usually spend sleeping in a 24 h period (including naps but excluding time spent resting)? | Dropdown <<<0–24 h>>> |
| |
| Compared to before the COVID-19 outbreak and related restrictions, my child walks or cycles in the neighbourhood: | A lot less A little less About the same A little more A lot more |
| Compared to before the COVID-19 outbreak and related restrictions, my child is doing physical activities or sport outdoors: | A lot less A little less About the same A little more A lot more |
| Compared to before the COVID-19 outbreak and related restrictions, my child is doing physical activities or sport inside: | A lot less A little less About the same A little more A lot more |
| Compared to before the COVID-19 outbreak and related restrictions, my child is doing household chores (e.g., cleaning, yard work): | A lot less A little less About the same A little more A lot more |
| Compared to before the COVID-19 outbreak and related restrictions, my child plays outdoors: | A lot less A little less About the same A little more A lot more |
| Compared to before the COVID-19 outbreak and related restrictions, my child plays inside: | A lot less A little less About the same A little more A lot more |
| BEFORE the COVID-19 outbreak and related restrictions, my child’s primary playmate was: | Themselves Sibling(s) Parent Other Caregiver Friend(s) Other [specify] |
| Now, my child’s primary playmate is: | Themselves Sibling(s) Parent Other Caregiver Friend(s) Other [specify] |
| Compared to before the COVID-19 outbreak and related restrictions, my child watches TV, movies, uses the computer for leisure, or plays sedentary video games: | A lot less A little less About the same A little more A lot more |
| Compared to before the COVID-19 outbreak and related restrictions, my child uses social media: | A lot less A little less About the same A little more A lot more |
| Compared to before the COVID-19 outbreak and related restrictions, my child does other sedentary leisure activities not in front of screens (e.g., reading, puzzles, crafts, music, or art): | A lot less A little less About the same A little more A lot more |
| Compared to before the COVID-19 outbreak and related restrictions, my child sleeps: | A lot less A little less About the same A little more A lot more |
| Compared to before the COVID-19 outbreak and related restrictions, my child’s sleep quality is: | A lot worse A little worse About the same A little better A lot better |
| Compared to before the COVID-19 outbreak and related restrictions, our family time spent doing physical activity is: | A lot less A little less About the same A little more A lot more |
| Compared to before the COVID-19 outbreak and related restrictions, our family time spent doing sedentary behaviours (e.g., watching TV, playing board games, doing crafts) is: | A lot less A little less About the same A little more A lot more |
| Compared to before the COVID-19 outbreak and related restrictions, the balance of my child’s overall healthy movement behaviours (i.e., physical activity, sedentary behaviours, and sleep) is: | A lot worse A little worse About the same A little better A lot better |
| As a result of the COVID-19 outbreak and related restrictions, is there an inside leisure activity or hobby that your child is doing a lot more now? | Yes [specify] No |
| As a result of the COVID-19 outbreak and related restrictions, is there an outdoor leisure activity or hobby that your child is doing a lot more now? | Yes [specify] No |
| As a result of the COVID-19 outbreak and related restrictions, has your family begun any new or novel activities not previously practiced? | Yes [specify] No |
| As a result of the COVID-19 outbreak and related restrictions, has your family used any online resources or apps to support healthy movement behaviours? | Yes [specify] No |
| As a result of the COVID-19 outbreak and related restrictions, has there been a decrease in your child’s health (e.g., existing condition worsened or new condition developed)? | Yes [specify] No |
| Using the scale below, please select the number that best describes how much distress your family has been experiencing over the past week. | 0 (No Distress) 1 2 3 4 5 6 7 8 9 10 (Extreme Distress) |
| |
| Compared to before the COVID-19 outbreak and related restrictions, I have encouraged my child to participate in physical activity or sport: | A lot less A little less About the same A little more A lot more |
| Compared to before the COVID-19 outbreak and related restrictions, I play outdoors with my child or do physical activity with my child: | A lot less A little less About the same A little more A lot more |
| Compared to before the COVID-19 outbreak and related restrictions, I drive or provide transportation for my child to do physical activity or sport: | A lot less A little less About the same A little more A lot more |
| Compared to before the COVID-19 outbreak and related restrictions, I have encouraged my child to do household chores (e.g., cleaning, yard work): | A lot less A little less About the same A little more A lot more |
| Compared to before the COVID-19 outbreak and related restrictions, I have encouraged my child to stop sitting and watching screens (e.g., screen breaks): | A lot less A little less About the same A little more A lot more |
| Compared to before the COVID-19 outbreak and related restrictions, I encouraged my child to sleep between 9 and 11 h per night: | A lot less A little less About the same A little more A lot more |
| Throughout the COVID-19 outbreak and related restrictions, and assuming I am fully motivated, I am capable of supporting my child’s physical activity over the next two weeks. | Strongly disagree Disagree Neutral Agree Strongly agree |
| Throughout the COVID-19 outbreak and related restrictions, and assuming I am fully motivated, I will have an opportunity to support my child’s physical activity over the next two weeks. | Strongly disagree Disagree Neutral Agree Strongly agree |
| Throughout the COVID-19 outbreak and related restrictions, and assuming I am fully motivated, I am capable of restricting my child’s screen time to no more than 2 h per day over the next two weeks. | Strongly disagree Disagree Neutral Agree Strongly agree |
| Throughout the COVID-19 outbreak and related restrictions, and assuming I am fully motivated, I will have an opportunity to restrict my child’s screen time to no more than 2 h per day over the next two weeks. | Strongly disagree Disagree Neutral Agree Strongly agree |
| Throughout the COVID-19 outbreak and related restrictions, and assuming I am fully motivated, I am capable of supporting my child’s sleep over the next two weeks. | Strongly disagree Disagree Neutral Agree Strongly agree |
| Throughout the COVID-19 outbreak and related restrictions, and assuming I am fully motivated, I will have an opportunity to support my child’s sleep over the next two weeks. | Strongly disagree Disagree Neutral Agree Strongly agree |
References
- Carson, V.; Chaput, J.P.; Janssen, I.; Tremblay, M.S. Health associations with meeting new 24-hour movement guidelines for Canadian children and youth. Prev. Med. 2017, 95, 7–13. [Google Scholar] [CrossRef]
- Dale, L.P.; Vanderloo, L.; Moore, S.A.; Faulkner, G. Physical activity and depression, anxiety, and self-esteem in children and youth: An umbrella systematic review. Ment. Health Phys. Act. 2019, 16, 66–79. [Google Scholar] [CrossRef]
- Pearson, N.; Braithwaite, R.E.; Biddle, S.J.; van Sluijs, E.M.; Atkin, A.J. Associations between sedentary behaviour and physical activity in children and adolescents: A meta-analysis. Obes. Rev. 2014, 15, 666–675. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Lin, Y.; Tremblay, M.S.; Katzmarzyk, P.T.; Fogelholm, M.; Hu, G.; Lambert, E.V.; Maher, C.; Maia, J.; Olds, T.; Sarmiento, O.L.; et al. Temporal and bi-directional associations between sleep duration and physical activity/sedentary time in children: An international comparison. Prev. Med. 2018, 111, 436–441. [Google Scholar] [CrossRef]
- Tremblay, M.S.; Carson, V.; Chaput, J.P.; Connor Gorber, S.; Dinh, T.; Duggan, M.; Faulkner, G.; Gray, C.E.; Gruber, R.; Janson, K.; et al. Canadian 24-hour Movement Guidelines for Children and Youth: An integration of physical activity, sedentary behaviour, and sleep. Appl. Physiol. Nutr. Metab. 2016, 41, S311–S327. [Google Scholar] [CrossRef]
- Bull, F.C.; Al-Ansari, S.S.; Biddle, S.; Borodulin, K.; Buman, M.P.; Cardon, G.; Carty, C.; Chaput, J.P.; Chastin, S.; Chou, R.; et al. World Health Organization 2020 guidelines on physical activity and sedentary behaviour. Br. J. Sports Med. 2020, 54, 1451–1462. [Google Scholar] [CrossRef] [PubMed]
- Rhodes, R.E.; Spence, J.C.; Berry, T.; Faulkner, G.; Latimer-Cheung, A.E.; O’Reilly, N.; Tremblay, M.S.; Vanderloo, L. Parental support of the Canadian 24-hour movement guidelines for children and youth: Prevalence and correlates. BMC Public Health 2019, 19, 1385. [Google Scholar] [CrossRef] [Green Version]
- Human Resources and Skills Development Canada. Disability in Canada: A 2006 Profile. 2006. Available online: https://www.canada.ca/en/employment-social-development/programs/disability/arc/disability-2006.html (accessed on 1 September 2021).
- Statistics Canada. Canadian Survey on Disability, 2017. 2018. Available online: https://www150.statcan.gc.ca/n1/en/catalogue/89-654-X (accessed on 1 September 2021).
- Arbour-Nicitopoulos, K.P.; Bassett-Gunter, R.L.; Leo, J.; Sharma, R.; Olds, T.; Latimer-Cheung, A.E.; Martin Ginis, K.A. A cross-sectional examination of the 24-hour movement behaviours in Canadian youth with physical and sensory disabilities. Disabil. Health J. 2021, 14, 100980. [Google Scholar] [CrossRef]
- Bedell, G.; Coster, W.; Law, M.; Liljenquist, K.; Kao, Y.C.; Teplicky, R.; Anaby, D.; Khetani, M.A. Community participation, supports, and barriers of school-age children with and without disabilities. Arch. Phys. Med. Rehabil. 2013, 94, 315–323. [Google Scholar] [CrossRef] [PubMed]
- Engel-Yeger, B.; Jarus, T.; Anaby, D.; Law, M. Differences in patterns of participation between youths with cerebral palsy and typically developing peers. Am. J. Occup. Ther. 2009, 63, 96–104. [Google Scholar] [CrossRef] [Green Version]
- Aishworiya, R.; Kiing, J.S.; Chan, Y.H.; Tung, S.S.; Law, E. Screen time exposure and sleep among children with developmental disabilities. J. Paediatr. Child. Health 2018, 54, 889–894. [Google Scholar] [CrossRef]
- Rimmer, J.A.; Rowland, J.L. Physical activity for youth with disabilities: A critical need in an underserved population. Dev. Neurorehabil. 2008, 11, 141–148. [Google Scholar] [CrossRef] [PubMed]
- Law, M.; King, G.; King, S.; Kertoy, M.; Hurley, P.; Rosenbaum, P.; Young, N.; Hanna, S. Patterns of participation in recreational and leisure activities among children with complex physical disabilities. Dev. Med. Child. Neurol. 2006, 48, 337–342. [Google Scholar] [CrossRef] [Green Version]
- MacDuffie, K.E.; Munson, J.; Greenson, J.; Ward, T.M.; Rogers, S.J.; Dawson, G.; Estes, A. Sleep problems and trajectories of restricted and repetitive behaviors in children with neurodevelopmental disabilities. J. Autism. Dev. Disord. 2020, 50, 3844–3856. [Google Scholar] [CrossRef] [PubMed]
- Köse, S.; Yılmaz, H.; Ocakoğlu, F.T.; Özbaran, N.B. Sleep problems in children with autism spectrum disorder and intellectual disability without autism spectrum disorder. Sleep Med. 2017, 40, 69–77. [Google Scholar] [CrossRef] [PubMed]
- Hemmingsson, H.; Stenhammar, A.M.; Paulsson, K. Sleep problems and the need for parental night-time attention in children with physical disabilities. Child. Care Health Dev. 2009, 35, 89–95. [Google Scholar] [CrossRef]
- Dumuid, D.; Olds, T.; Sawyer, S.M. Moving beyond more: Towards a healthy balance of daily behaviours. Lancet 2021, 398, 373–374. [Google Scholar] [CrossRef]
- Handler, L.; Tennant, E.M.; Faulkner, G.; Latimer-Cheung, A.E. Perceptions of inclusivity: The Canadian 24-Hour Movement Guidelines for Children and Youth. Adapt. Phys. Activ. Q. 2019, 36, 1–18. [Google Scholar] [CrossRef] [PubMed]
- Canadian Disability Participation Project: Research Update: A First Look at the Preliminary Findings from the National Physical Activity Measurement Study. 2018. Available online: https://cdpp.ca/sites/default/files/Ability%20Insights%20-%20CDPP%20Sport%20%26%20Exercise%20Family%20Newsletter%20-%20Fall%202018.pdf (accessed on 1 September 2021).
- World Health Organization. Coronavirus Disease (COVID-19) Pandemic: WHO Characterizes COVID-19 as a Pandemic. 2020. Available online: https://www.who.int/emergencies/diseases/novel-coronavirus-2019/events-as-they-happen (accessed on 1 September 2021).
- de Lannoy, L.; Rhodes, R.E.; Moore, S.A.; Faulkner, G.; Tremblay, M.S. Regional differences in access to the outdoors and outdoor play of Canadian children and youth during the COVID-19 outbreak. Can. J. Public Health 2020, 111, 988–994. [Google Scholar] [CrossRef]
- de Araújo, L.A.; Veloso, C.F.; Souza, M.C.; Azevedo, J.M.C.; Tarro, G. The potential impact of the COVID-19 pandemic on child growth and development: A systematic review. J. Pediatr. Rio. J. 2021, 97, 369–377. [Google Scholar] [CrossRef] [PubMed]
- Paterson, D.C.; Ramage, K.; Moore, S.A.; Riazi, N.; Tremblay, M.S.; Faulkner, G. Exploring the impact of COVID-19 on the movement behaviors of children and youth: A scoping review of evidence after the first year. J. Sport Health Sci. 2021, 11. [Google Scholar] [CrossRef]
- Moore, S.A.; Faulkner, G.; Rhodes, R.E.; Brussoni, M.; Chulak-Bozzer, T.; Ferguson, L.J.; Mitra, R.; O’Reilly, N.; Spence, J.C.; Vanderloo, L.M.; et al. Impact of the COVID-19 virus outbreak on movement and play behaviours of Canadian children and youth: A national survey. Int. J. Behav. Nutr. Phys. Act. 2020, 17, 85. [Google Scholar] [CrossRef] [PubMed]
- Cacioppo, M.; Bouvier, S.; Bailly, R.; Houx, L.; Lempereur, M.; Mensah-Gourmel, J.; Kandalaft, C.; Varengue, R.; Chatelin, A.; Vagnoni, J.; et al. Emerging health challenges for children with physical disabilities and their parents during the COVID-19 pandemic: The ECHO French survey. Ann. Phys. Rehabil. Med. 2021, 64, 101429. [Google Scholar] [CrossRef]
- Esentürk, O.K. Parents’ perceptions on physical activity for their children with autism spectrum disorders during the novel Coronavirus outbreak. Int. J. Dev. Disabil. 2020. [Google Scholar] [CrossRef]
- Garcia, J.M.; Lawrence, S.; Brazendale, K.; Leahy, N.; Fukuda, D. Brief report: The impact of the COVID-19 pandemic on health behaviors in adolescents with Autism Spectrum Disorder. Disabil. Health J. 2021, 14, 101021. [Google Scholar] [CrossRef] [PubMed]
- Masi, A.; Mendoza Diaz, A.; Tully, L.; Azim, S.I.; Woolfenden, S.; Efron, D.; Eapen, V. Impact of the COVID-19 pandemic on the well-being of children with neurodevelopmental disabilities and their parents. J. Paediatr. Child. Health 2021, 57, 631–636. [Google Scholar] [CrossRef] [PubMed]
- Manganello, J.A. Media use for children with disabilities in the United States during COVID-19. J. Child. Media 2021, 15, 29–32. [Google Scholar] [CrossRef]
- Yarimkaya, E.; Esentürk, O.K. Promoting physical activity for children with autism spectrum disorders during Coronavirus outbreak: Benefits, strategies, and examples. Int. J. Dev. Disabil. 2020. [Google Scholar] [CrossRef]
- Loades, M.E.; Chatburn, E.; Higson-Sweeney, N.; Reynolds, S.; Shafran, R.; Brigden, A.; Linney, C.; McManus, M.N.; Borwick, C.; Crawley, E. Rapid systematic review: The impact of social isolation and loneliness on the mental health of children and adolescents in the context of COVID-19. J. Am. Acad. Child. Adolesc. Psychiatry 2020, 59, 1218–1239.e3. [Google Scholar] [CrossRef]
- Moore, S.A.; Faulkner, G.; Rhodes, R.E.; Vanderloo, L.M.; Ferguson, L.J.; Guerrero, M.D.; Brussoni, M.; Mitra, R.; O’Reilly, N.; Spence, J.C.; et al. Few Canadian children and youth were meeting the 24-hour movement behaviour guidelines 6-months into the COVID-19 pandemic: Follow-up from a national study. Appl. Physiol. Nutr. Metab. 2021, 46, 1225–1240. [Google Scholar] [CrossRef]
- Bridgland, V.M.E.; Moeck, E.K.; Green, D.M.; Swain, T.L.; Nayda, D.M.; Matson, L.A.; Hutchison, N.P.; Takarangi, M.K.T. Why the COVID-19 pandemic is a traumatic stressor. PLoS ONE 2021, 16, e0240146. [Google Scholar] [CrossRef]
- Singh, S.; Roy, D.; Sinha, K.; Parveen, S.; Sharma, G.; Joshi, G. Impact of COVID-19 and lockdown on mental health of children and adolescents: A narrative review with recommendations. Psychiatry Res. 2020, 293, 113429. [Google Scholar] [CrossRef] [PubMed]
- Schiariti, V. The human rights of children with disabilities during health emergencies: The challenge of COVID-19. Dev. Med. Child. Neurol. 2020, 62, 661. [Google Scholar] [CrossRef] [Green Version]
- Statistics Canada. The Impact of the COVID-19 Pandemic on Canadian Families of Children with Disabilities. 2020. Available online: https://www150.statcan.gc.ca/n1/pub/45-28-0001/2020001/article/00066-eng.htm (accessed on 1 September 2021).
- Graber, K.M.; Byrne, E.M.; Goodacre, E.J.; Kirby, N.; Kulkarni, K.; O’Farrelly, C.; Ramchandani, P.G. A rapid review of the impact of quarantine and restricted environments on children’s play and the role of play in children’s health. Child. Care Health Dev. 2021, 47, 143–153. [Google Scholar] [CrossRef] [PubMed]
- Faulkner, G.; Rhodes, R.E.; Vanderloo, L.M.; Chulak-Bozzer, T.; O’Reilly, N.; Ferguson, L.; Spence, J.C. Physical activity as a coping strategy for mental health due to the COVID-19 rirus: A potential disconnect among Canadian adults? Front. Commun. 2020, 5, 74. [Google Scholar] [CrossRef]
- Nijhof, S.L.; Vinkers, C.H.; van Geelen, S.M.; Duijff, S.N.; Achterberg, E.J.M.; van der Net, J.; Veltkamp, R.C.; Grootenhuis, M.A.; van de Putte, E.M.; Hillegers, M.H.J.; et al. Healthy play, better coping: The importance of play for the development of children in health and disease. Neurosci. Biobehav. Rev. 2018, 95, 421–429. [Google Scholar] [CrossRef] [PubMed]
- Shields, N.; Synnot, A.J.; Barr, M. Perceived barriers and facilitators to physical activity for children with disability: A systematic review. Br. J. Sports Med. 2012, 46, 989–997. [Google Scholar] [CrossRef] [PubMed]
- Sterdt, E.; Liersch, S.; Walter, U. Correlates of physical activity of children and adolescents: A systematic review of reviews. Health Educ. J. 2014, 73, 72–89. [Google Scholar] [CrossRef]
- Martin Ginis, K.A.; van der Ploeg, H.P.; Foster, C.; Lai, B.; McBride, C.B.; Ng, K.; Pratt, M.; Shirazipour, C.H.; Smith, B.; Vásquez, P.M.; et al. Participation of people living with disabilities in physical activity: A global perspective. Lancet 2021, 398, 443–455. [Google Scholar] [CrossRef]
- Beets, M.W.; Cardinal, B.J.; Alderman, B.L. Parental social support and the physical activity-related behaviors of youth: A review. Health Educ. Behav. 2010, 37, 621–644. [Google Scholar] [CrossRef]
- Bassett-Gunter, R.; Rhodes, R.; Sweet, S.; Tristani, L.; Soltani, Y. Parent support for children’s physical activity: A qualitative investigation of barriers and strategies. Res. Q. Exerc. Sport 2017, 88, 282–292. [Google Scholar] [CrossRef] [PubMed]
- Bassett-Gunter, R.; Tanna, S.; Arbour-Nicitopoulos, K.P.; Rhodes, R.; Leo, J. Understanding parent support for physical activity among parents of children and youth with disabilities: A behaviour change theory perspective. Eur. J. Adapt. Phys. Act. 2020, 13, 1–16. [Google Scholar] [CrossRef]
- Brown, D.M.; Arbour-Nicitopoulos, K.P.; Martin Ginis, K.A.; Latimer-Cheung, A.E.; Bassett-Gunter, R.L. Examining the relationship between parent physical activity support behaviour and physical activity among children and youth with Autism Spectrum Disorder. Autism 2020, 24, 1783–1794. [Google Scholar] [CrossRef]
- Spence, J.C.; Lee, R.E. Toward a comprehensive model of physical activity. Psychol. Sport Exerc. 2003, 4, 7–24. [Google Scholar] [CrossRef]
- Tremblay, M.S.; Connor Gorber, S. Canadian health measures survey: Brief overview. Can. J. Public Health 2007, 98, 453–456. [Google Scholar] [CrossRef]
- Cohen, J. Statistical Power Analysis for the Behavioral Sciences; Routledge Academic: New York, NY, USA, 1998. [Google Scholar]
- Holland, J.C.; Andersen, B.; Breitbart, W.S.; Buchmann, L.O.; Compas, B.; Deshields, T.L.; Dudley, M.M.; Fleishman, S.; Fulcher, C.D.; Greenberg, D.B.; et al. Distress management. J. Natl. Compr. Canc. Netw. 2013, 11, 190–209. [Google Scholar] [CrossRef] [Green Version]
- Mohamed, S.; Elgohary, G.; ElHaffez, A.; Kamel, E.; El-Aziz, N. Does distress thermometer have a utility in the era of COVID-19 pandemic? Open Access Libr. J. 2020, 7, 6643. [Google Scholar] [CrossRef]
- Embregts, P.; Heerkens, L.; Frielink, N.; Giesbers, S.; Vromans, L.; Jahoda, A. Experiences of mothers caring for a child with an intellectual disability during the COVID-19 pandemic in the Netherlands. J. Intellect. Disabil. Res. 2021, 65, 760–771. [Google Scholar] [CrossRef]
- Canadian Institute for Health Information. COVID-19 Intervention Timeline in Canada. 2021. Available online: http://www.cihi.ca/en/covid-19-intervention-timeline-in-canada (accessed on 1 September 2021).
- Leo, J.A.; Faulkner, G.; Volfson, Z.; Bassett-Gunter, R.; Arbour, K.P. Physical activity preferences, attitudes, and behaviour of children and youth with physical disabilities. Ther. Recreat. J. 2018, 52, 140–153. [Google Scholar] [CrossRef]
- Groulx, M.; Lemieux, C.; Freeman, S.; Cameron, J.; Wright, P.A.; Healy, T. Participatory planning for the future of accessible nature. Local Environ. 2021, 26, 808–824. [Google Scholar] [CrossRef]
- Prvu Bettger, J.; Thoumi, A.; Marquevich, V.; De Groote, W.; Rizzo Battistella, L.; Imamura, M.; Delgado Ramos, V.; Wang, N.; Dreinhoefer, K.E.; Mangar, A.; et al. COVID-19: Maintaining essential rehabilitation services across the care continuum. BMJ Glob. Health 2020, 5, e002670. [Google Scholar] [CrossRef] [PubMed]
- Lee, J. Maternal stress, well-being, and impaired sleep in mothers of children with developmental disabilities: A literature review. Res. Dev. Disabil. 2013, 34, 4255–4273. [Google Scholar] [CrossRef] [PubMed]
- Iacob, C.I.; Avram, E.; Cojocaru, D.; Podina, I.R. Resilience in familial caregivers of children with developmental disabilities: A meta-analysis. J. Autism. Dev. Disord. 2020, 50, 4053–4068. [Google Scholar] [CrossRef] [PubMed]
- Bekhet, A.K.; Johnson, N.L.; Zauszniewski, J.A. Resilience in family members of persons with autism spectrum disorder: A review of the literature. Issues Ment. Health Nurs. 2012, 33, 650–656. [Google Scholar] [CrossRef] [PubMed]
- Rhodes, R.E.; Guerrero, M.D.; Vanderloo, L.M.; Barbeau, K.; Birken, C.S.; Chaput, J.P.; Faulkner, G.; Janssen, I.; Madigan, S.; Mâsse, L.C.; et al. Development of a consensus statement on the role of the family in the physical activity, sedentary, and sleep behaviours of children and youth. Int. J. Behav. Nutr. Phys. Act. 2020, 17, 74. [Google Scholar] [CrossRef]
- Taylor, W.C.; Baranowski, T.; Sallis, J.F. Family Determinants of Childhood Physical Activity: A Social Cognitive Model; Dishman, R.K., Ed.; Human Kinetics: Champaign, IL, USA, 1994; pp. 319–342. [Google Scholar]
- Rhodes, R.E.; Lim, C. Promoting parent and child physical activity together: Elicitation of potential intervention targets and preferences. Health Educ. Behav. 2018, 45, 112–123. [Google Scholar] [CrossRef]
- Diaz, K.M. Physical inactivity among parents of children with and without Down syndrome: The National Health Interview Survey. J. Intellect. Disabil. Res. 2020, 64, 38–44. [Google Scholar] [CrossRef] [PubMed]
- Ku, B.; Rhodes, R.E. Physical activity behaviors in parents of children with disabilities: A systematic review. Res. Dev. Disabil. 2020, 107, 103787. [Google Scholar] [CrossRef] [PubMed]
- Pan, C.Y.; Frey, G.C.; Bar-Or, O.; Longmuir, P. Concordance of physical activity among parents and youth with physical disabilities. J. Dev. Phys. Disabil. 2005, 17, 395–407. [Google Scholar] [CrossRef]
- Siebert, E.A.; Hamm, J.; Yun, J. Parental influence on physical activity of children with disabilities. Int. J. Disabil. Develop. Educ. 2017, 64, 378–390. [Google Scholar] [CrossRef]
- Bandini, L.; Danielson, M.; Esposito, L.E.; Foley, J.T.; Fox, M.H.; Frey, G.C.; Fleming, R.K.; Krahn, G.; Must, A.; Porretta, D.L.; et al. Obesity in children with developmental and/or physical disabilities. Disabil. Health J. 2015, 8, 309–316. [Google Scholar] [CrossRef] [PubMed]
- Whitney, D.G.; Shapiro, D.N.; Peterson, M.D.; Warschausky, S.A. Factors associated with depression and anxiety in children with intellectual disabilities. J. Intellect. Disabil. Res. 2019, 63, 408–417. [Google Scholar] [CrossRef] [PubMed]
- Santino, N.; Arbour-Nicitopoulos, K.P.; Sharma, R.; Graham, J.D.; Bassett-Gunter, R.L. Physical activity and loneliness among adolescents with disabilities: Examining the quality of physical activity experiences as a possible moderator. Disabil. Health J. 2021, 14, 101060. [Google Scholar] [CrossRef] [PubMed]
- Ottawa Sport Council. Ottawa Return to Play Roadmap: Inclusion and Accessibility. 2021. Available online: https://www.ottawareturntoplayroadmap.ca/inclusion-and-accessibility (accessed on 1 September 2021).
| Parent Demographic Profile | |
| Age (years), M (SD) | 42.42 (5.74) |
| Gender, woman, n (%) | 139 (92.1) |
| Ethnicity, n (%) | |
| European | 114 (75.5) |
| Asian | 24 (15.9) |
| Indigenous | 3 (2.0) |
| Other | 10 (6.6) |
| Marital status, n (%) | |
| Married or common-law | 127 (84.1) |
| Divorced or separated | 9 (6.0) |
| Single | 13 (8.6) |
| Undisclosed | 2 (1.3) |
| Education, n (%) | |
| High school or less | 8 (5.3) |
| College or technical school | 58 (38.4) |
| University | 60 (39.7) |
| Advanced degree | 23 (15.3) |
| Undisclosed | 2 (1.3) |
| Annual household income, n (%) | |
| <$50,000CDN | 35 (23.2) |
| $50,000 to 99,999CDN | 41 (27.1) |
| >$100,000CDN | 60 (39.7) |
| Undisclosed | 15 (10.0) |
| Employment status, n (%) | |
| Full-time | 69 (45.7) |
| Part-time | 29 (19.2) |
| Self-employed | 20 (13.2) |
| Unemployed | 28 (18.6) |
| Other (e.g., student, retired) | 5 (3.3) |
| Child Demographic Profile | |
| Age (years), M (SD) | 10.77 (3.22) |
| Ages 4 to 13 years (years), M (SD) / n (%) | 9.62 (2.45)/121 (80.13) |
| Ages 14 to 17 years (years), M (SD) / n (%) | 15.40 (0.90)/30 (19.87) |
| Gender, girl, n (%) | 38 (25.2) |
| Disability type, n (%) | |
| Developmental | 56 (37.1) |
| Physical | 21 (13.9) |
| Sensory | 6 (4.0) |
| Combination/Other | 68 (45.0) |
| Child’s residence type, n (%) | |
| House (detached or semi-detached) | 124 (82.1) |
| Apartment or townhome | 27 (17.9) |
| Household makeup, M (SD) | |
| Adults | 2.05 (0.64) |
| Children and youth | 2.19 (0.96) |
| Total | Children | Youth | Boys | Girls | |
|---|---|---|---|---|---|
| N = 151 | N = 121 | N = 30 | N = 113 | N = 38 | |
| Current Movement Behaviours of Children and Youth, M (SD) | |||||
| MVPA 1 ≥ 60 min/day (days/week) | 1.60 (2.05) | 1.82 (2.16) | 0.73 (1.20) | 1.56 (2.07) | 1.74 (2.01) |
| Screen time (hours/day) | 5.36 (3.32) | 5.08 (3.22) | 6.49 (3.50) | 5.72 (3.31) | 4.29 (3.12) |
| Sleep (hours/day) | 9.33 (1.53) | 9.39 (1.52) | 9.13 (1.59) | 9.26 (1.50) | 9.58 (1.64) |
| Proportion of Children and Youth Meeting Movement Guideline, % | |||||
| MVPA | 5.3 | 6.6 | 0.0 | 5.3 | 5.3 |
| Screen time | 11.3 | 14.0 a | 0.0 | 7.1 | 23.7 g |
| Sleep | 66.2 | 66.9 | 63.3 | 69.0 | 57.9 |
| 24-h movement behaviours 2 | 1.3 | 1.7 | 0.0 | 1.0 | 2.6 |
| Total | Children | Youth | Boys | Girls | |
|---|---|---|---|---|---|
| N = 151 | N = 121 | N = 30 | N = 113 | N = 38 | |
| Change in Child Movement and Play Behaviours During COVID-19 Outbreak, M (SD) 1 | |||||
| Outdoor Physical Activity | |||||
| Outdoor physical activity or sport | 2.24 (1.39) | 2.24 (1.41) | 2.23 (1.33) | 2.18 (1.35) | 2.42 (1.54) |
| Outdoor play | 2.70 (1.34) | 2.68 (1.38) | 2.80 (1.16) | 2.68 (1.32) | 2.76 (1.38) |
| Walk, wheel, or bike in the neighbourhood | 2.74 (1.49) | 2.74 (1.50) | 2.73 (1.46) | 2.68 (1.47) | 2.92 (1.53) |
| Indoor Physical Activity | |||||
| Indoor physical activity or sport | 2.45 (1.23) | 2.45 (1.22) | 2.45 (1.30) | 2.38 (1.19) | 2.63 (1.36) |
| Indoor play | 3.51 (1.13) | 3.56 (1.10) | 3.28 (1.22) | 3.48 (1.13) | 3.59 (1.12) |
| Household chores | 3.40 (0.90) | 3.32 (0.93) | 3.70 a (0.70) | 3.43 (0.91) | 3.29 (0.87) |
| Sedentary Behaviours | |||||
| Television (TV) or other screens | 4.30 (0.98) | 4.28 (0.99) | 4.37 (0.96) | 4.36 (0.97) | 4.11 (0.98) |
| Social media | 3.25 (1.06) | 3.22 (1.09) | 3.40 (0.93) | 3.24 (1.07) | 3.29 (1.04) |
| Non-screen-based leisure activities | 3.60 (0.99) | 3.60 (1.01) | 3.63 (0.89) | 3.57 (0.99) | 3.74 (0.98) |
| Sleep | |||||
| Sleep quantity | 3.20 (0.87) | 3.09 (0.86) | 3.60 a (0.81) | 3.12 (0.77) | 3.43 (1.09) |
| Sleep quality | 3.02 (0.90) | 3.00 (0.90) | 3.10 (0.92) | 3.02 (0.86) | 3.03 (1.03) |
| Family-Based Activity | |||||
| Physical activity | 2.87 (1.24) | 2.86 (1.25) | 2.90 (1.24) | 2.79 (1.27) | 3.08 (1.12) |
| Sedentary behaviours | 3.83 (0.98) | 3.81 (1.01) | 3.90 (0.88) | 3.85 (0.97) | 3.76 (1.05) |
| Overall Healthy Movement Behaviours | 2.49 (1.03) | 2.47 (1.02) | 2.57 (1.10) | 2.45 (1.04) | 2.61 (1.03) |
| Outdoor Physical Activity and Sport | Outdoor play | Walking, Wheeling, and Cycling | Indoor Physical Activity and Sport | Indoor Play | Household Chores | Television and Other Screens | Social Media | Non-Screen-Based Sedentary Activity | Sleep Quantity | Sleep Quality | Family-Based Physical Activity | Family-Based Sedentary Behaviour | Overall Healthy Movement Behaviours | |
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| Parent Age | −0.02 | −0.03 | −0.02 | −0.10 | −0.10 | −0.04 | 0.13 | 0.15 | −0.08 | 0.14 | −0.03 | 0.06 | 0.10 | −0.10 |
| Parent Gender 1 | 0.16 | 0.21 ** | 0.08 | −0.07 | <0.01 | 0.10 | −0.04 | −0.05 | −0.02 | 0.01 | −0.19 * | 0.11 | 0.05 | −0.05 |
| Marital Status 2 | 0.27 ** | 0.26 ** | 0.21 * | 0.09 | −0.06 | 0.19 * | −0.11 | −0.11 | −0.08 | −0.03 | 0.09 | 0.26 ** | −0.15 | 0.13 |
| Parent’s Education | 0.03 | 0.04 | 0.07 | 0.02 | 0.21 * | 0.15 | 0.05 | 0.08 | −0.01 | 0.01 | 0.07 | 0.08 | 0.05 | 0.07 |
| Parent Work Status 3 | −0.11 | 0.04 | 0.04 | 0.05 | −0.08 | 0.12 | −0.01 | 0.03 | −0.04 | 0.09 | 0.13 | 0.03 | 0.02 | −0.08 |
| Household Income | 0.12 | 0.20 * | 0.14 | −0.01 | −0.04 | 0.18 * | 0.04 | −0.04 | −0.13 | 0.06 | 0.13 | 0.18 * | −0.09 | 0.02 |
| Household (Dwelling) Type 4 | 0.11 | 0.28 ** | 0.09 | 0.01 | −0.12 | 0.10 | < 0.01 | −0.07 | −0.16 * | −0.13 | 0.12 | 0.19 * | −0.08 | 0.04 |
| Family Distress | −0.18 * | −0.16 * | −0.21 * | 0.02 | 0.04 | −0.10 | 0.10 | −0.03 | 0.06 | 0.02 | −0.14 | −0.21 * | 0.03 | −0.01 |
| Total | Children | Youth | Boys | Girls | |
|---|---|---|---|---|---|
| N = 151 | N = 121 | N = 30 | N = 113 | N = 38 | |
| Changes in parent-perceived ability to encourage and provide support for their child’s healthy movement behaviours, M (SD) 1 | |||||
| Encouraged child to participate in PA | 3.49 (1.13) | 3.52 (1.12) | 3.40 (1.22) | 3.46 (1.14) | 3.58 (1.13) |
| Played outside or did PA with child | 3.35 (1.08) | 3.37 (1.12) | 3.27 (0.91) | 3.31 (1.07) | 3.47 (1.11) |
| Drove or provided transportation for child to do PA | 1.68 (1.14) | 1.64 (1.09) | 1.87 (1.31) | 1.74 (1.19) | 1.51 (0.96) |
| Encouraged child to do chores | 3.73 (0.82) | 3.72 (0.85) | 3.77 (0.73) | 3.79 (0.76) | 3.55 (0.98) |
| Encouraged child to stop sitting/watching screens | 3.72 (1.12) | 3.73 (1.14) | 3.67 (1.03) | 3.77 (1.08) | 3.54 (1.24) |
| Encouraged child to sleep | 3.43 (0.76) | 3.44 (0.78) | 3.40 (0.67) | 3.43 (0.73) | 3.42 (0.83) |
| Changes in parent-perceived capability and opportunity to support their child’s healthy movement behaviours, M (SD) | |||||
| Capable of supporting child’s physical activity | 3.51 (1.03) | 3.50 (1.00) | 3.53 (1.14) | 3.41 (1.04) | 3.79 (0.93) |
| Opportunity to support child’s physical activity | 3.54 (1.03) | 3.50 (1.02) | 3.70 (1.09) | 3.42 (1.05) | 3.89 (0.92) |
| Capable of restricting child’s screen time (e.g., screen breaks) | 2.74 (1.31) | 2.78 (1.33) | 2.60 (1.22) | 2.67 (1.29) | 2.95 (1.35) |
| Opportunity to restrict child’s screen time (e.g., screen breaks) | 2.64 (1.25) | 2.64 (1.24) | 2.62 (1.30) | 2.61 (1.23) | 2.71 (1.31) |
| Capable of supporting child’s sleep | 3.90 (0.91) | 3.90 (0.90) | 3.90 (0.96) | 3.95 (0.92) | 3.76 (0.88) |
| Opportunity to support child’s sleep | 3.89 (0.91) | 3.89 (0.90) | 3.90 (0.98) | 3.95 (0.91) | 3.74 (0.89) |
| Outdoor PA and Sport | Outdoor Play | Walking, Wheeling, and Cycling | Indoor PA and Sport | Indoor Play | Household Chores | Television and Other Screens | Social Media | Non-screen-BasedSedentary Activity | Sleep Quantity | Sleep Quality | Family-Based PA | Family-BasedSedentary Behaviour | Overall HealthyMovement Behaviours | |
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| Parents Encouragement and Support of Healthy Movement Behaviours | ||||||||||||||
| Encouraged PA 1 | 0.23 ** | 0.26 ** | 0.19 * | 0.16 * | 0.06 | 0.19 * | −0.07 | −0.09 | .05 | 0.09 | 0.06 | 0.26 ** | 0.17 * | 0.17 * |
| Participated in PA | 0.26 ** | 0.34 ** | 0.39 ** | 0.14 | 0.11 | 0.08 | −0.03 | −0.18* | −0.02 | −0.01 | 0.04 | 0.41 ** | 0.21 * | 0.06 |
| Provided transport to PA | 0.05 | −0.06 | −0.04 | 0.09 | −0.21* | −0.25 ** | −0.14 | −0.02 | −0.15 | 0.08 | <0.01 | −0.12 | −0.11 | 0.11 |
| Encouraged chores | 0.04 | 0.07 | 0.02 | −0.04 | 0.12 | 0.61 ** | 0.07 | 0.07 | 0.05 | 0.10 | −0.07 | 0.02 | 0.17 * | −0.01 |
| Encouraged reduced screens | −0.10 | −0.13 | 0.04 | −0.03 | −0.13 | 0.10 | 0.19 * | 0.06 | 0.05 | 0.20 * | 0.13 | −0.04 | 0.11 | −0.08 |
| Encouraged sleep | −0.04 | < 0.01 | −0.10 | 0.02 | −0.04 | <0.01 | 0.08 | −0.12 | −0.09 | −0.03 | −0.02 | −0.07 | <−0.01 | −0.07 |
| Parent-Perceived Capability and Opportunity to Support Healthy Movement Behaviours | ||||||||||||||
| Capable of supporting PA | 0.29 ** | 0.23 ** | 0.23 ** | 0.09 | 0.07 | −0.04 | −0.05 | 0.01 | 0.07 | 0.04 | 0.13 | 0.39 ** | 0.06 | 0.23 ** |
| Opportunity to support PA | 0.29 ** | 0.31 ** | 0.18 ** | 0.20* | 0.16 | 0.01 | −0.13 | 0.02 | 0.11 | 0.06 | 0.20* | 0.35 ** | 0.08 | 0.37 ** |
| Capable of restricting screens | 0.42 ** | 0.33 ** | 0.28 ** | 0.13 | 0.17 * | 0.17 * | −0.30 ** | −0.20 * | 0.08 | −0.10 | 0.13 | 0.22 ** | −0.05 | 0.20 * |
| Opportunity to restrict screens | 0.35 ** | 0.29 ** | 0.22 ** | 0.02 | 0.10 | 0.11 | −0.27 ** | −0.07 | 0.08 | −0.01 | 0.14 | 0.18 ** | −0.02 | 0.21 * |
| Capable of supporting sleep | 0.04 | 0.10 | 0.07 | −0.18 * | 0.05 | 0.19 * | −0.05 | −0.07 | −0.04 | 0.16 | 0.39 ** | 0.20 ** | −0.04 | 0.12 |
| Opportunity to support sleep | 0.08 | 0.14 | 0.06 | −0.16 * | 0.10 | 0.21 * | −0.02 | −0.10 | 0.02 | 0.19 * | 0.41 ** | 0.21 ** | −0.01 | 0.18 * |
| Overall Parental Encouragement and Support and Parent-Perceived Capability and Opportunity to Support Healthy Movement Behaviours | ||||||||||||||
| Encouragement and support | 0.14 | 0.15 | 0.17 * | 0.12 | −0.04 | 0.18 * | 0.01 | −0.08 | −0.03 | 0.14 | 0.05 | 0.16 | 0.16 * | 0.06 |
| Capability and opportunity | 0.38 ** | 0.35 ** | 0.26 ** | 0.04 | 0.16 | 0.16 * | −0.22 ** | −0.11 | 0.07 | 0.06 | 0.31 ** | 0.37 ** | 0.01 | 0.31 ** |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Moore, S.A.; Sharma, R.; Martin Ginis, K.A.; Arbour-Nicitopoulos, K.P. Adverse Effects of the COVID-19 Pandemic on Movement and Play Behaviours of Children and Youth Living with Disabilities: Findings from the National Physical Activity Measurement (NPAM) Study. Int. J. Environ. Res. Public Health 2021, 18, 12950. https://doi.org/10.3390/ijerph182412950
Moore SA, Sharma R, Martin Ginis KA, Arbour-Nicitopoulos KP. Adverse Effects of the COVID-19 Pandemic on Movement and Play Behaviours of Children and Youth Living with Disabilities: Findings from the National Physical Activity Measurement (NPAM) Study. International Journal of Environmental Research and Public Health. 2021; 18(24):12950. https://doi.org/10.3390/ijerph182412950
Chicago/Turabian StyleMoore, Sarah A., Ritu Sharma, Kathleen A. Martin Ginis, and Kelly P. Arbour-Nicitopoulos. 2021. "Adverse Effects of the COVID-19 Pandemic on Movement and Play Behaviours of Children and Youth Living with Disabilities: Findings from the National Physical Activity Measurement (NPAM) Study" International Journal of Environmental Research and Public Health 18, no. 24: 12950. https://doi.org/10.3390/ijerph182412950
APA StyleMoore, S. A., Sharma, R., Martin Ginis, K. A., & Arbour-Nicitopoulos, K. P. (2021). Adverse Effects of the COVID-19 Pandemic on Movement and Play Behaviours of Children and Youth Living with Disabilities: Findings from the National Physical Activity Measurement (NPAM) Study. International Journal of Environmental Research and Public Health, 18(24), 12950. https://doi.org/10.3390/ijerph182412950






