Strategies Adopted by Addiction Facilities during the Coronavirus Pandemic to Support Treatment for Individuals in Recovery or Struggling with a Substance Use Disorder: A Scoping Review
Abstract
:1. Introduction
2. Materials and Methods
2.1. Search Strategy
2.2. Eligibility Criteria
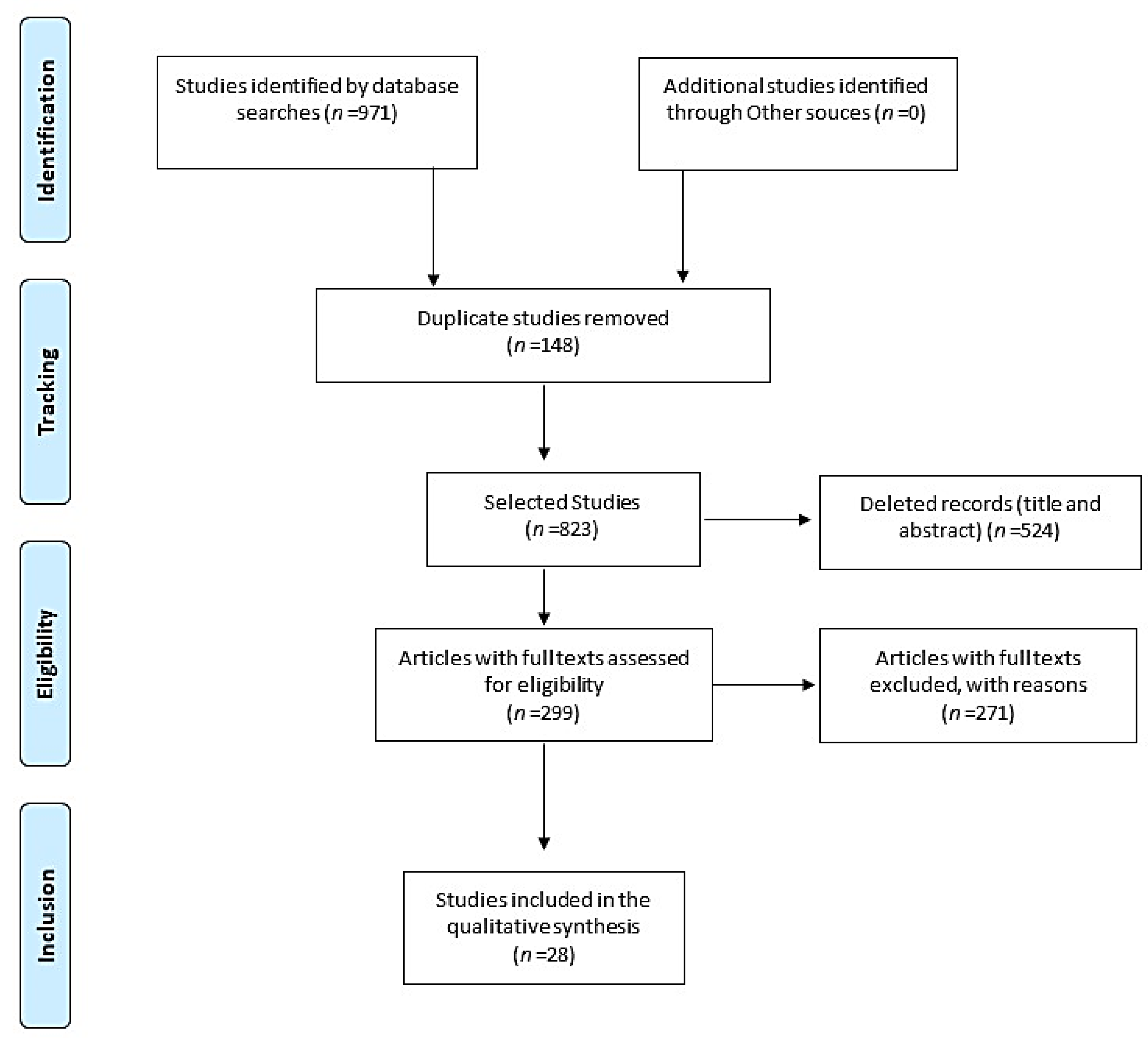
2.3. Selection of Studies
3. Results
4. Discussion
4.1. Strategies to Support the Care Offer Maintenance
4.1.1. Telehealth/Telemedicine Support
4.1.2. Adequacy of Prescription and Distribution of Medications
4.2. Strategies That Limited Care Offer
4.2.1. Reorganization in the Face-to-Face Assistance of Specialized Services
4.2.2. Care Aimed at Preventing Coronavirus and Harm Reduction
4.3. Limitations
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Conflicts of Interest
References
- World Health Organization (WHO). Timeline: WHO’s COVID-19 Response. 2021. Available online: https://www.who.int/emergencies/diseases/novel-coronavirus-2019/interactive-timeline?gclid=CjwKCAjwyIKJBhBPEiwAu7zll5MLHIC7uevWiLON1zSfTgmtnOJUgnyKNqPK2n78ax0UvxkCChAFZRoCSjsQAvD_BwE#! (accessed on 21 August 2021).
- World Health Organization (WHO). Director-Gernal’s Opening Remarks at the Media Briefing on COVID-19. 2020. Available online: https://www.who.int/director-general/speeches/detail/who-director-general-s-opening-remarks-at-the-media-briefing-on-Covid-19---11-march-2020 (accessed on 21 August 2021).
- Damiano, R.F.; Di Santi, T.; Beach, S.; Pan, P.M.; Lucchetti, A.L.; Smith, F.A.; Forlenza, O.V.; Fricchione, G.L.; Miguel, E.C.; Lucchetti, G. Mental health interventions following COVID-19 and other coronavirus infections: A systematic review of current recommendations and meta-analysis of randomized controlled trials. Braz. J. Psychiatry 2021, 1, 14. [Google Scholar] [CrossRef]
- Holmes, E.A.; O’Connor, R.C.; Perry, V.H.; Tracey, I.; Wessely, S.; Arseneault, L.; Ballard, C.; Christensen, H.; Silver, R.C.; Everall, I.; et al. Multidisciplinary research priorities for the COVID-19 pandemic: A call for action for mental health science. Lancet Psychiatry 2020, 7, 547–560. [Google Scholar] [CrossRef]
- Wang, C.; Pan, R.; Wan, X.; Tan, Y.; Xu, L.; McIntyre, R.S.; Choo, F.N.; Tran, B.; Ho, R.; Sharma, V.K.; et al. A longitudinal study on the mental health of general population during the COVID-19 epidemic in China. Brain Behav. Immun. 2020, 87, 40–48. [Google Scholar] [CrossRef]
- Matta, G.C.; Rego, S.; Souto, E.P.; Segata, J. COVID-19 in Brazil and the Various Faces of the Pandemic: Presentation. In COVID-19’s Social Impacts in Brazil: Vulnerable Populations and Responses to the Pandemic; Matta, G.C., Rego, S., Souto, E.P., Segata, J., Eds.; Fiocruz: Rio de Janeiro, Brazil, 2021; pp. 15–24. [Google Scholar] [CrossRef] [Green Version]
- Wei, Y.; Shah, R. Substance Use Disorder in the COVID-19 Pandemic: A Systematic Review of Vulnerabilities and Complications. Pharmaceuticals 2020, 13, 155. [Google Scholar] [CrossRef]
- Karamouzian, M.; Johnson, C.; Kerr, T. Public health messaging and harm reduction in the time of COVID-19. Lancet Psychiatry 2020, 7, 390–391. [Google Scholar] [CrossRef]
- Organização Pan-Americana da Saúde (OPAS). Response to the COVID-19 Pandemic in the Americas: Response Strategy and Call to Donors January-December 2021. 2021. Available online: https://iris.paho.org/bitstream/handle/10665.2/54425/OPASPHEHEOCOVID19210008_por.pdf?sequence=1&isAllowed=y (accessed on 21 August 2021).
- Hirdes, A.; Marcon, G.; Branchi, R.N.; Vivian, A.G. Prevention of Alcohol and Other Drugs Use and Treatment in Primary Health Care in a Southern Brazilian City. Aletheia 2015, 74–89. Available online: http://pepsic.bvsalud.org/scielo.php?script=sci_arttext&pid=S1413-03942015000100007&lng=pt&tlng= (accessed on 19 August 2021).
- Yang, L.H.; Wong, L.Y.; Grivel, M.M.; Hasin, D.S. Stigma and substance use disorders: An international phenomenon. Curr. Opin. Psychiatry 2017, 30, 378–388. [Google Scholar] [CrossRef]
- Melamed, O.C.; Hauck, T.S.; Buckley, L.; Selby, P.; Mulsant, B.H. COVID-19 and persons with substance use disorders: Inequities and mitigation strategies. Subst. Abus. 2020, 41, 286–291. [Google Scholar] [CrossRef]
- Volkow, N.D. Collision of the COVID-19 and Addiction Epidemics. Ann. Intern. Med. 2020, 173, 61–62. [Google Scholar] [CrossRef] [Green Version]
- Arksey, H.; O’Malley, L. Scoping studies: Towards a methodological framework. Int. J. Soc. Res. Methodol. Theory Pract. 2005, 8, 19–32. [Google Scholar] [CrossRef] [Green Version]
- Tricco, A.C.; Lillie, E.; Zarin, W.; O’Brien, K.K.; Colquhoun, H.; Levac, D.; Moher, D.; Peters, M.D.; Horsley, T.; Weeks, L.; et al. PRISMA extension for scoping reviews (PRISMA-ScR): Checklist and explanation. Ann. Int. Med. 2018, 169, 467–473. [Google Scholar] [CrossRef] [Green Version]
- Mericle, A.A.; Sheridan, D.; Howell, J.; Braucht, G.S.; Karriker-Jaffe, K.; Polcin, D.L. Sheltering in place and social distancing when the services provided are housing and social support: The COVID-19 health crisis and recovery housing. J. Subst. Abuse Treat. 2020, 119, 108094. [Google Scholar] [CrossRef]
- Roncero, C.; Vicente-Hernández, B.; Casado-Espada, N.M.; Aguilar, L.; Gamonal-Limcaoco, S.; Garzón, M.A.; Martínez-González, F.; Llanes-Álvarez, C.; Martínez, R.; Franco-Martín, M.; et al. The Impact of COVID-19 Pandemic on the Castile and Leon Addiction Treatment Network: A Real-Word Experience. Front. Psychiatry 2020, 11, 575755. [Google Scholar] [CrossRef]
- Picchio, C.A.; Valencia, J.; Doran, J.; Swan, T.; Pastor, M.; Martró, E. The impact of the COVID-19 pandemic on harm reduction services in Spain. Harm. Reduct. J. 2020, 17, 87. [Google Scholar] [CrossRef]
- Uscher-Pines, L.; Sousa, J.; Raja, P.; Mehrotra, A.; Barnett, M.; Huskamp, H.A. Treatment of opioid use disorder during COVID-19: Experiences of clinicians transitioning to telemedicine. J. Subst. Abuse Treat. 2020, 118, 108124. [Google Scholar] [CrossRef]
- Samuels, E.A.; Clark, S.A.; Wunsch, C.; Keeler, L.A.J.; Reddy, N.; Vanjani, R.; Wightman, R.S. Innovation During COVID-19: Improving Addiction Treatment Access. J. Addict. Med. 2020, 14, e8–e9. [Google Scholar] [CrossRef]
- Kimmel, S.D.; Bazzi, A.R.; Barocas, J.A. Integrating harm reduction and clinical care: Lessons from COVID-19 respite and recuperation facilities. J. Subst. Abuse Treat. 2020, 118, 108103. [Google Scholar] [CrossRef]
- Rosca, P.; Shapira, B.; Neumark, Y. Isolating the isolated: Implications of COVID-19 quarantine measures on in-patient detoxification treatment for substance use disorders. Int. J. Drug Policy 2020, 83, 102830. [Google Scholar] [CrossRef]
- Harris, M.; Johnson, S.; Mackin, S.; Saitz, R.; Walley, A.Y.; Taylor, J.L. Low Barrier Tele-Buprenorphine in the Time of COVID-19: A case report. J. Addict. Med. 2020, 14, e136–e138. [Google Scholar] [CrossRef]
- Khatri, U.G.; Perrone, J. Opioid Use Disorder and COVID-19: Crashing of the Crises. J. Addict. Med. 2020, 14, e6–e7. [Google Scholar] [CrossRef]
- Tringale, R.; Subica, A.M. COVID-19 innovations in medication for addiction treatment at a Skid Row syringe exchange. J. Subst. Abuse Treat. 2021, 121, 108181. [Google Scholar] [CrossRef]
- Vecchio, S.; Ramella, R.; Drago, A.; Carraro, D.; Littlewood, R.; Somaini, L. COVID19 pandemic and people with opioid use disorder: Innovation to reduce risk. Psychiatry Res. 2020, 289, 113047. [Google Scholar] [CrossRef] [PubMed]
- Castillo, M.; Conte, B.; Hinkes, S.; Mathew, M.; Na, C.J.; Norindr, A.; Serota, D.P.; Forrest, D.W.; Deshpade, A.R.; Bartholomew, T.S.; et al. Implementation of a medical student-run telemedicine program for medications for opioid use disorder during the COVID-19 pandemic. Harm Reduct. J. 2020, 17, 88. [Google Scholar] [CrossRef]
- Pajevic, I.; Hasanović, M.; Avdibegović, E.; Džubur-Kulenović, A.; Burgić-Radmanović, M.; Babić, D.; Mehić-Basara, N.; Zivlak-Radulović, N.; Račetović, G. Organization of mental healthcare in Bosnia and Herzegovina during coronavirus disease 2019 pandemic. Indian J. Psychiatry 2020, 62, 479. [Google Scholar] [CrossRef]
- Joseph, G.; Torres-Lockhart, K.; Stein, M.R.; Mund, P.A.; Nahvi, S. Reimagining patient-centered care in opioid treatment programs: Lessons from the Bronx during COVID-19. J. Subst. Abuse Treat. 2021, 122, 108219. [Google Scholar] [CrossRef]
- Crowley, D.; Delargy, I. A national model of remote care for assessing and providing opioid agonist treatment during the COVID-19 pandemic: A report. Harm Reduct. J. 2020, 17, 49. [Google Scholar] [CrossRef]
- Wilson, C.G.; Ramage, M.; Fagan, E.B. A Primary Care Response to COVID-19 for Patients with an Opioid Use Disorder. J. Rural. Health 2020, 37, 169–171. [Google Scholar] [CrossRef] [Green Version]
- MacKinnon, L.; Socías, M.E.; Bardwell, G. COVID-19 and overdose prevention: Challenges and opportunities for clinical practice in housing settings. J. Subst. Abuse Treat. 2020, 108153. [Google Scholar] [CrossRef]
- Figgatt, M.C.; Salazar, Z.; Dia, E.; Vincent, L.; Dasgupta, N. Take-home dosing experiences among persons receiving methadone maintenance treatment during COVID-19. J. Subst. Abuse Treat. 2021, 123, 108276. [Google Scholar] [CrossRef]
- Langabeer, J.R.; Yatsco, A.; Champagne-Langabeer, T. Telehealth sustains patient engagement in OUD treatment during COVID-19. J. Subst. Abuse Treat. 2020, 122, 108215. [Google Scholar] [CrossRef]
- Hughto, J.M.W.; Peterson, L.; Perry, N.S.; Donoyan, A.; Mimiaga, M.J.; Nelson, K.M.; Pantalone, D.W. The provision of counseling to patients receiving medications for opioid use disorder: Telehealth innovations and challenges in the age of COVID-19. J. Subst. Abuse Treat. 2021, 120, 108163. [Google Scholar] [CrossRef]
- Courser, M.W.; Rifa, H. With crisis comes opportunity: Unanticipated benefits resulting from pivots to take-home naloxone (THN) programs during the COVID-19 pandemic. J. Subst. Abuse Treat. 2020, 122, 108220. [Google Scholar] [CrossRef]
- Ghosh, A.; Mahintamani, T.; Subodh, B.N.; Pillai, R.R.; Mattoo, S.K.; Basu, D. Telemedicine-assisted stepwise approach of service delivery for substance use disorders in India. Asian J. Psychiatr. 2021, 58, 102582. [Google Scholar] [CrossRef]
- Kedia, S.K.; Schmidt, M.; Dillon, P.J.; Arshad, H.; Yu, X. Substance use treatment in Appalachian Tennessee amid COVID-19: Challenges and preparing for the future. J. Subst. Abuse Treat. 2021, 124, 108270. [Google Scholar] [CrossRef]
- Oviedo-Joekes, E.; MacDonald, S.; Boissonneault, C.; Harper, K. Take home injectable opioids for opioid use disorder during and after the COVID-19 Pandemic is in urgent need: A case study. Subst. Abuse Treat. Prev. Policy 2021, 16, 16–22. [Google Scholar] [CrossRef]
- Harris, M.T.H.; Peterkin, A.; Bach, P.; Englander, H.; Lapidus, E.; Rolley, T.; Weimer, M.B.; Weinstein, Z.M. Adapting inpatient addiction medicine consult services during the COVID-19 pandemic. Addict. Sci. Clin. Pract. 2021, 16, 13. [Google Scholar] [CrossRef]
- Hanton, K.; McHugh, D.; Boris, G. A Case Series: Successfully Preventing COVID-19 Outbreak in a Residential Community Setting at a Drug and Alcohol Addiction Treatment Center. Healthcare 2021, 9, 88. [Google Scholar] [CrossRef]
- Noyes, E.; Yeo, E.; Yerton, M.; Plakas, I.; Keyes, S.; Obando, A.; Gaeta, J.M.; Taveras, E.M.; Chatterjee, A. Harm Reduction for Adolescents and Young Adults During the COVID-19 Pandemic: A Case Study of Community Care in Reach. Public Health Rep. 2021, 136, 301–308. [Google Scholar] [CrossRef]
- Pagano, A.; Hosakote, S.; Kapiteni, K.; Straus, E.R.; Wong, J.; Guydish, J.R. Impacts of COVID-19 on residential treatment programs for substance use disorder. J. Subst. Abuse Treat. 2021, 123, 108255. [Google Scholar] [CrossRef]
- Aromataris, E.; Munn, Z. (Eds.) JBI Manual for Evidence Synthesis; JBI: Adelaide, Australia, 2020. [Google Scholar]
- Levesque, J.F.; Harris, M.F.; Russell, G. Patient-centred access to health care: Conceptualising access at the interface of health systems and populations. Int. J. Equity Health 2013, 12, 18. [Google Scholar] [CrossRef] [Green Version]
- Substance Abuse and Mental Health Services Administration. Addressing Diverse Populations in Intensive Outpatient Treatment. In Substance Abuse: Clinical Issues in Intensive Outpatient Treatment; Substance Abuse and Mental Health Services Administration (US): Rockville, MD, USA, 2006. [Google Scholar]
- Marsden, J.; Darke, S.; Hall, W.; Hickman, M.; Holmes, J.; Humphreys, K.; Neale, J.; Tucker, J.; West, R. Mitigating and learning from the impact of COVID-19 infection on addictive disorders. Addiction 2020, 115, 1007–1010. [Google Scholar] [CrossRef] [Green Version]
- Gois-Santos, V.T.; Freire, D.A.; Libório, L.S.; Ferreira, E.C.G.; Santos, V.S. Telehealth actions in times of COVID-19: Information with evidence. Rev. Assoc. Med. Bras. 2020, 66, 1320–1322. [Google Scholar] [CrossRef]
- Uscher-Pines, L.; Sousa, J.; Raja, P.; Mehrotra, A.; Barnett, M.L.; Huskamp, H.A. Suddenly becoming a “virtual doctor”: Experiences of psychiatrists transitioning to telemedicine during the COVID-19 pandemic. Psychiatr. Serv. 2020, 71, 1143–1150. [Google Scholar] [CrossRef]
- Li, R.; Zhao, M. Maintaining treatment and prevention programs for opioid use disorders during the coronavirus disease 2019 pandemic. Curr. Opin. Psychiatry 2021, 34, 369–375. [Google Scholar] [CrossRef]
- Mahoney, M.C.; Park, E.; Schlienz, N.J.; Duerr, C.; Hawk, L.W. Transitioning to remote clinic visits in a smoking cessation trial during the SARS coronavirus-2 pandemic: Mixed methods evaluation. JMIR Form. Res. 2021, 5, e25541. [Google Scholar] [CrossRef]
- Oesterle, T.S.; Kolla, B.; Risma, C.J.; Breitinger, S.A.; Rakocevic, D.B.; Loukianova, L.L.; Hall-Flavin, D.K.; Gentry, M.T.; Rummans, T.A.; Chauhan, M.; et al. Substance Use Disorders and Telehealth in the COVID-19 Pandemic Era: A New Outlook. Mayo Clin. Proc. 2020, 95, 2709–2718. [Google Scholar] [CrossRef]
- Leppla, I.E.; Gross, M.S. Optimizing medication treatment of opioid use disorder during COVID-19 (SARS-CoV-2). J. Addict. Med. 2020, 14, e1–e3. [Google Scholar] [CrossRef]
- Tracy, K.; Wallace, S.P. Benefits of peer support groups in the treatment of addiction. Subst. Abuse Rehabil. 2016, 7, 143–154. [Google Scholar] [CrossRef] [Green Version]
- Du Plessis, C.; Whitaker, L.; Hurley, J. Peer support workers in substance abuse treatment services: A systematic review of the literature. J. Subst. Use 2020, 25, 225–230. [Google Scholar] [CrossRef]
- Sampaio, M.; Haro, M.V.N.; De Sousa, B.; Melo, W.V.; Hoffman, H.G. Therapists Make the Switch to Telepsychology to Safely Continue Treating their Patients during the COVID-19 Pandemic. Virtual Reality Telepsychology May Be Next. Front. Virtual Real. 2021, 1, 576421. [Google Scholar] [CrossRef]
- Fawcett, W.J.; Charlesworth, M.; Cook, T.M.; Klein, A.A. Education and scientific dissemination during the COVID-19 pandemic. Anaesthesia 2020, 76, 301–304. [Google Scholar] [CrossRef]
- Ismail, I.I.; Abdelkarim, A.; Al-Hashel, J.Y. Physicians’ attitude towards webinars and online education amid COVID-19 pandemic: When less is more. PLoS ONE 2021, 16, e0250241. [Google Scholar] [CrossRef] [PubMed]
- The American Osteopathic Academ of Addiction Medicine (AOAAM). Webinar Series: Education, Buprenorphine Induction for High Potency Synthetic Opioid Users. Aoaam.Org. 2021. Available online: https://education.aoaam.org/products/buprenorphine-induction-for-high-potency-synthetic-opioid-users (accessed on 18 September 2021).
- Graig, L.; Friedman, K.; Alper, J. Caring for People with Mentl Health and Substance Use Disorders in Primary Care Settings: Proceeding of Workshop; The National Academies Press: Washigton, DC, USA, 2020; pp. 19–21. [Google Scholar] [CrossRef]
- Tebeje, T.H.; Klein, J. Applications of e-Health to support person-centered health care at the time of COVID-19 Pandemic. Telemed. J. E Health 2021, 27, 150–158. [Google Scholar] [CrossRef] [PubMed]
- Esmaeilzadeh, P.; Mirzaei, T. Using Electronic Health Records to Mitigate Workplace Burnout Among Clinicians During the COVID-19 Pandemic: Field Study in Iran. JMIR Med. Inform. 2021, 9, e28497. [Google Scholar] [CrossRef]
- Department of Health and Social Care and Public Health England. COVID-19: Guidance for Commissioners and Providers of Services for People Who Use Drugs or Alcohol. 2020. Available online: https://www.gov.uk/government/publications/Covid-19-guidance-for-commissioners-and-providers-of-services-for-people-who-use-drugs-or-alcohol/Covid-19-guidance-for-commissioners-and-providers-of-services-for-people-who-use-drugs-or-alcohol (accessed on 21 October 2021).
- Substance Abuse and Mental Health Services Administration. FAQs: Provision of Methadone and Buprenorphine for the Treatment of Opioid Use Disorder in the COVID-19 Emergency; Substance Abuse and Mental Health Services Administration: Rockville, MD, USA, 2020.
- Substance Abuse and Mental Health Services Administration. Federal Guidelines for Opioid Treatment Programs Retrieved from Rockville; Substance Abuse and Mental Health Services Administration: Rockville, MD, USA, 2015.
- Mason, M.; Welch, S.B.; Arunkumar, P.; Post, L.A.; Feinglass, J.M. Notes from the Field: Opioid Overdose Deaths before, during, and after an 11-Week COVID-19 Stay-at-Home Order—Cook County, Illinois, January 1 2018–October 6 2020. MMWR Morb. Mortal. Wkly. Rep. 2021, 70, 362–363. [Google Scholar] [CrossRef]
- Moustaqim-Barrette, A.; Papamihali, K.; Mamdani, Z.; Williams, S.; Buxton, J.A. Accessing Take-Home Naloxone in British Columbia and the role of community pharmacies: Results from the analysis of administrative data. PLoS ONE 2020, 15, e0238618. [Google Scholar] [CrossRef]
- Dunn, K.E.; Brooner, R.K.; Stoller, K.B. Technology-assisted methadone take-home dosing for dispensing methadone to persons with opioid use disorder during the COVID-19 pandemic. J. Subst. Abuse Treat. 2021, 121, 108197. [Google Scholar] [CrossRef]
- Fishman, M.; Wenzel, K.; Vo, H.; Wildberger, J.; Burgower, R. A pilot randomized controlled trial of assertive treatment including family involvement and home delivery of medication for young adults with opioid use disorder. Addiction 2021, 116, 548–557. [Google Scholar] [CrossRef]
- Mannelli, P.; Wu, L.T. Primary care for opioid use disorder. Subst. Abuse Rehabil. 2016, 7, 107–109. [Google Scholar] [CrossRef]
- Lagisetty, P.; Klasa, K.; Bush, C.; Heisler, M.; Chopra, V.; Bohnert, A. Primary care models for treating opioid use disorders: What actually works? A systematic review. PLoS ONE 2017, 12, e0186315. [Google Scholar] [CrossRef] [Green Version]
- Kleykamp, B.A.; Guille, C.; Barth, K.S.; McClure, E.A. Substance use disorders and COVID-19: The role of telehealth in treatment and research. J. Soc. Work Pract. Addict. 2020, 20, 248–253. [Google Scholar] [CrossRef]
- McDonnell, A.; MacNeill, C.; Chapman, B.; Gilbertson, N.; Reinhardt, M.; Carreiro, S. Leveraging digital tools to support recovery from substance use disorder during the COVID-19 pandemic response. J. Subst. Abuse Treat. 2021, 124, 108226. [Google Scholar] [CrossRef]
- World Health Organization (WHO). COVID-19 Disrupting Mental Health Services in Most Countries. 2020. Available online: https://www.who.int/news/item/05-10-2020-Covid-19-disrupting-mental-health-services-in-most-countries-who-survey (accessed on 21 October 2021).
- Pettersen, H.; Landheim, A.; Skeie, I.; Biong, S.; Brodahl, M.; Oute, J.; Davidson, L. How social relation-ships influence substance use disorder recovery: A collaborative narrative study. Subst. Abuse 2019, 13, 1178221819833379. [Google Scholar] [CrossRef] [Green Version]
- Reiss, D.R. Institutionalizing the Centers for Disease Control and Prevention’s Independence. ConLawNOW 2020, 12, 107. [Google Scholar] [CrossRef]
- Glynn, M.A. 15 Days to Slow the Spread: COVID-19 and Collective Resilience. J. Manag. Stud. 2021, 58, 265–269. [Google Scholar] [CrossRef]
- Jason, L.A.; Salomon-Amend, M.; Guerrero, M.; Bobak, T.; O’Brien, J.; Soto-Nevarez, A. The Emergence, Role, and Impact of Recovery Support Services. Alcohol Res. 2021, 41, 4. [Google Scholar] [CrossRef]
- Magno, L.; Rossi, T.A.; Mendonça-Lima, F.W.D.; Santos, C.C.D.; Campos, G.B.; Marques, L.M.; Dourado, I. Challenges and proposals for scaling up COVID-19 testing and diagnosis in Brazil. Cien Saude Colet. 2020, 25, 3355–3364. [Google Scholar] [CrossRef] [PubMed]
- Priest, K.C. The COVID-19 pandemic: Practice and policy considerations for patients with opioid use disorder. Health Affairs Blog 2021, 10. [Google Scholar] [CrossRef]
- McCarty, D.; Bougatsos, C.; Chan, B.; Hoffman, K.A.; Priest, K.C.; Grusing, S.; Chou, R. Office-Based Methadone Treatment for Opioid Use Disorder and Pharmacy Dispensing: A Scoping Review. Am. J. Psychiatry 2021, 178, 804–817. [Google Scholar] [CrossRef]
- Cantor, J.; Laurito, A. The new services that opioid treatment programs have adopted in response to COVID-19. J. Subst. Abuse Treat. 2021, 130, 108393. [Google Scholar] [CrossRef]
- Rosen, J.; Harnett, P. Confronting Two Crises: The COVID-19 Pandemic, the Opioid Epidemic, and the Industrial Hygienist. New Solut. 2021, 31, 384–389. [Google Scholar] [CrossRef]
- Paudyal, V.; Cadogan, C.; Fialová, D.; Henman, M.C.; Hazen, A.; Okuyan, B.; Lutters, M.; Stewart, D. Provision of clinical pharmacy services during the COVID-19 pandemic: Experiences of pharmacists from 16 European countries. Res. Soc. Adm. Pharm. 2021, 17, 1507–1517. [Google Scholar] [CrossRef]
- Olding, M.; Barker, A.; McNeil, R.; Boyd, J. Essential work, precarious labour: The need for safer and equitable harm reduction work in the era of COVID-19. Int. J. Drug Policy 2021, 90, 103076. [Google Scholar] [CrossRef]
- Polcin, D.L.; Mahoney, E.; Wittman, F.; Sheridan, D.; Mericle, A.A. Understanding challenges for recovery homes during COVID-19. Int. J. Drug Policy 2021, 93, 102986. [Google Scholar] [CrossRef]
- Spagnolo, P.A.; Montemitro, C.; Leggio, L. New Challenges in Addiction Medicine: COVID-19 Infection in Patients With Alcohol and Substance Use Disorders-The Perfect Storm. Am. J. Psychiatry 2020, 177, 805–807. [Google Scholar] [CrossRef] [PubMed]
- Avena, N.M.; Simkus, J.; Lewandowski, A.; Gold, M.S.; Potenza, M.N. Substance Use Disorders and Behavioral Addictions During the COVID-19 Pandemic and COVID-19-Related Restrictions. Front. Psychiatry 2021, 12, 653674. [Google Scholar] [CrossRef] [PubMed]
- Aquino, E.M.L.; Silveira, I.H.; Pescarini, J.M.; Aquino, R.; Souza-Filho, J.A.; Rocha, A.S.; Ferreira, A.; Victor, A.; Teixeira, C.; Machado, D.B. Social distancing measures to control the COVID-19 pandemic: Potential impacts and challenges in Brazil. Cien Saude Colet. 2020, 25, 2423–2446. [Google Scholar] [CrossRef]
- Oliveira, A.C.D.; Lucas, T.C.; Iquiapaza, R.A. What has the Covid-19 pandemic taught us about adopting preventive measures? Texto Contexto-Enferm. 2020, 29, e20200106. [Google Scholar] [CrossRef]
- Bardwell, G.; Boyd, J.; Tupper, K.W.; Kerr, T. “We don’t got that kind of time, man. We’re trying to get high!”: Exploring potential use of drug checking technologies among structurally vulnerable people who use drugs. Int. J. Drug Policy 2019, 71, 125–132. [Google Scholar] [CrossRef] [PubMed]
- Bourgois, P.; Holmes, S.M.; Sue, K.; Quesada, J. Structural Vulnerability: Operationalizing the Concept to Address Health Disparities in Clinical Care. Acad. Med. 2017, 92, 299–307. [Google Scholar] [CrossRef]
- Vallecillo, G.; Perelló, R.; Güerri, R.; Fonseca, F.; Torrens, M. Clinical impact of COVID-19 on people with substance use disorders. J. Public Health 2021, 43, 9–12. [Google Scholar] [CrossRef]
- Babor, T.F. Treatment systems for population management of substance use disorders: Requirements and priorities from a public health perspective. In Textbook of Addiction Treatment; Springer: Berlin/Heidelberg, Germany, 2021; pp. 553–567. [Google Scholar] [CrossRef]
- Barbosa, D.J.; Gomes, M.P.; Gomes, A.M.T.; Souza, F.B.A. Relationship between Psychoactive Drug Consumption and COVID-19: Synthesis of evidence. J. Manag. Prim. Health Care 2020, 12, 1. [Google Scholar] [CrossRef]
- Orio, L.; Antón, M.; Rodríguez-Rojo, I.C.; Correas, Á.; García-Bueno, B.; Corral, M.; Fonseca, F.R.; García-Moreno, L.M.; Maestú, F.; Cadaveira, F.; et al. Young alcohol binge drinkers have elevated blood endotoxin, peripheral inflammation and low cortisol levels: Neuropsychological correlations in women. Addict. Biol. 2018, 23, 1130–1144. [Google Scholar] [CrossRef]
- Arcavi, L.; Benowitz, N.L. Cigarette Smoking and Infection. Arch. Intern. Med. 2004, 164, 2206–2216. [Google Scholar] [CrossRef]
- Underner, M.; Peiffer, G.; Perriot, J.; Jaafari, N. Pulmonary complications in cocaine users. Rev. Mal. Respir. 2020, 37, 45–59. [Google Scholar] [CrossRef] [PubMed]
- Gupta, N.M.; Lindenauer, P.K.; Yu, P.C.; Imrey, P.B.; Haessler, S.; Deshpande, A.; Higgins, T.L.; Rothberg, M.B. Association Between Alcohol Use Disorders and Outcomes of Patients Hospitalized With Community-Acquired Pneumonia. JAMA Netw. Open 2019, 2, e195172. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- World Drug Report 2020. Drug Use and Health Consequences; United Nations Publication: Vienna, Austria, 2020; Volume 2, p. E.20.XI.6.
- Wang, Q.Q.; Kaelber, D.C.; Xu, R.; Volkow, N.D. COVID-19 risk and outcomes in patients with substance use disorders: Analyses from electronic health records in the United States. Mol. Psychiatry 2021, 26, 30–39. [Google Scholar] [CrossRef] [PubMed]
- Hesse, M.; Thylstrup, B.; Seid, A.K.; Skogen, J.C. Suicide among people treated for drug use disorders: A Danish national record-linkage study. BMC Public Health 2020, 20, 1–9. [Google Scholar] [CrossRef] [Green Version]
- Lopes, L.L.T.; Silva, M.R.S.; Santos, A.M.; Oliveira, J.F. Multidisciplinary team actions of a Brazilian Psychosocial Care Center for Alcohol and Drugs. Rev. Bras. Enferm. 2019, 72, 1702–1709. [Google Scholar] [CrossRef] [Green Version]
- Armstrong, M.; Shulman, C.; Hudson, B.; Stone, P.; Hewett, N. Barriers and facilitators to accessing health and social care services for people living in homeless hostels: A qualitative study of the experiences of hostel staff and residents in UK hostels. BMJ Open 2021, 11, e053185. [Google Scholar] [CrossRef]
- World Health Organization (WHO). Global Status Report on Alcohol and Health 2018. 2018. Available online: https://apps.who.int/iris/handle/10665/274603 (accessed on 27 October 2021).
| Number of Articles (%) | |
|---|---|
| Year of Publication | |
| 2020 [16,17,18,19,20,21,22,23,24,25,26,27,28,29,30,31,32] | 17 (61) |
| 2021 [33,34,35,36,37,38,39,40,41,42,43] | 11 (39) |
| Type of Study/Article | |
| Opinion articles [16,20,21,22,25,26,30,31,32,35,36,38] | 12 (42) |
| Cross-sectional study [17,19,28,34] | 4 (14) |
| Experience report [27,29,40,41] | 4 (14) |
| Case study [23,24,39] | 3 (11) |
| Qualitative study [19,43] | 2 (7) |
| Analytical study before and after [33] | 1 (4) |
| Retrospective study and post hoc analysis [37] | 1 (4) |
| Mixed study (quanti/quali) [42] | 1 (4) |
| Country of Corresponding Author | |
| U.S.A. [16,19,20,21,23,24,25,27,29,31,32,33,34,35,36,38,40,41,42,43] | 19 (68) |
| Canada [32,39] | 2 (6) |
| Spain [17,18] | 2 (6) |
| Ireland [30] | 1 (4) |
| India [37] | 1 (4) |
| Italy [26] | 1 (4) |
| Bosnia and Herzegovina [28] | 1 (4) |
| Israel [22] | 1 (4) |
| Categories | Strategies Adopted in Specialized Health Services |
|---|---|
| Strategies to Support the Care Offer Maintenance | |
| Telehealth/telemedicine support (n = 19) [16,17,19,20,22,23,24,27,28,30,31,32,34,35,37,38,40,41,43] | |
| Adequacy of prescription and distribution of medications (n = 13) [17,20,25,26,27,28,29,31,33,36,38,39] | |
| Strategies that Limited Care Offer | |
| Reorganization of face-to-face healthcare services (n = 11) [16,18,22,26,28,29,30,31,41,42,43] |
|
| Care aimed at preventing COVID-19 and harm reduction (n = 12) [16,17,21,23,25,27,31,33,39,40,42,43] | |
| Living Characteristic | Categories |
|---|---|
| Living not specified (n = 19) [17,18,19,20,21,22,24,26,27,28,29,30,32,33,34,35,37,40,42] | |
| People who live in residential facilities/residential community (n = 5) [16,17,38,41,43] | |
| Homeless people/room occupancy (n = 5) [17,19,23,25,39] |
|
| Rural population (n = 5) [31,36,37,38,41] |
|
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
de Vargas, D.; Pereira, C.F.; Volpato, R.J.; Lima, A.V.C.; da Silva Ferreira, R.; de Oliveira, S.R.; Aguilar, T.F. Strategies Adopted by Addiction Facilities during the Coronavirus Pandemic to Support Treatment for Individuals in Recovery or Struggling with a Substance Use Disorder: A Scoping Review. Int. J. Environ. Res. Public Health 2021, 18, 12094. https://doi.org/10.3390/ijerph182212094
de Vargas D, Pereira CF, Volpato RJ, Lima AVC, da Silva Ferreira R, de Oliveira SR, Aguilar TF. Strategies Adopted by Addiction Facilities during the Coronavirus Pandemic to Support Treatment for Individuals in Recovery or Struggling with a Substance Use Disorder: A Scoping Review. International Journal of Environmental Research and Public Health. 2021; 18(22):12094. https://doi.org/10.3390/ijerph182212094
Chicago/Turabian Stylede Vargas, Divane, Caroline Figueira Pereira, Rosa Jacinto Volpato, Ana Vitória Corrêa Lima, Rogério da Silva Ferreira, Sheila Ramos de Oliveira, and Thiago Faustino Aguilar. 2021. "Strategies Adopted by Addiction Facilities during the Coronavirus Pandemic to Support Treatment for Individuals in Recovery or Struggling with a Substance Use Disorder: A Scoping Review" International Journal of Environmental Research and Public Health 18, no. 22: 12094. https://doi.org/10.3390/ijerph182212094
APA Stylede Vargas, D., Pereira, C. F., Volpato, R. J., Lima, A. V. C., da Silva Ferreira, R., de Oliveira, S. R., & Aguilar, T. F. (2021). Strategies Adopted by Addiction Facilities during the Coronavirus Pandemic to Support Treatment for Individuals in Recovery or Struggling with a Substance Use Disorder: A Scoping Review. International Journal of Environmental Research and Public Health, 18(22), 12094. https://doi.org/10.3390/ijerph182212094







