Why Do Public Safety Personnel Seek Tailored Internet-Delivered Cognitive Behavioural Therapy? An Observational Study of Treatment-Seekers
Abstract
:1. Introduction
2. Materials and Methods
2.1. Setting
2.2. Participants and Procedures
2.3. Measures
2.4. Data Analysis
3. Results
3.1. What Demographic and Occupational Groups Do Prospective PSPNET Clients Belong to?
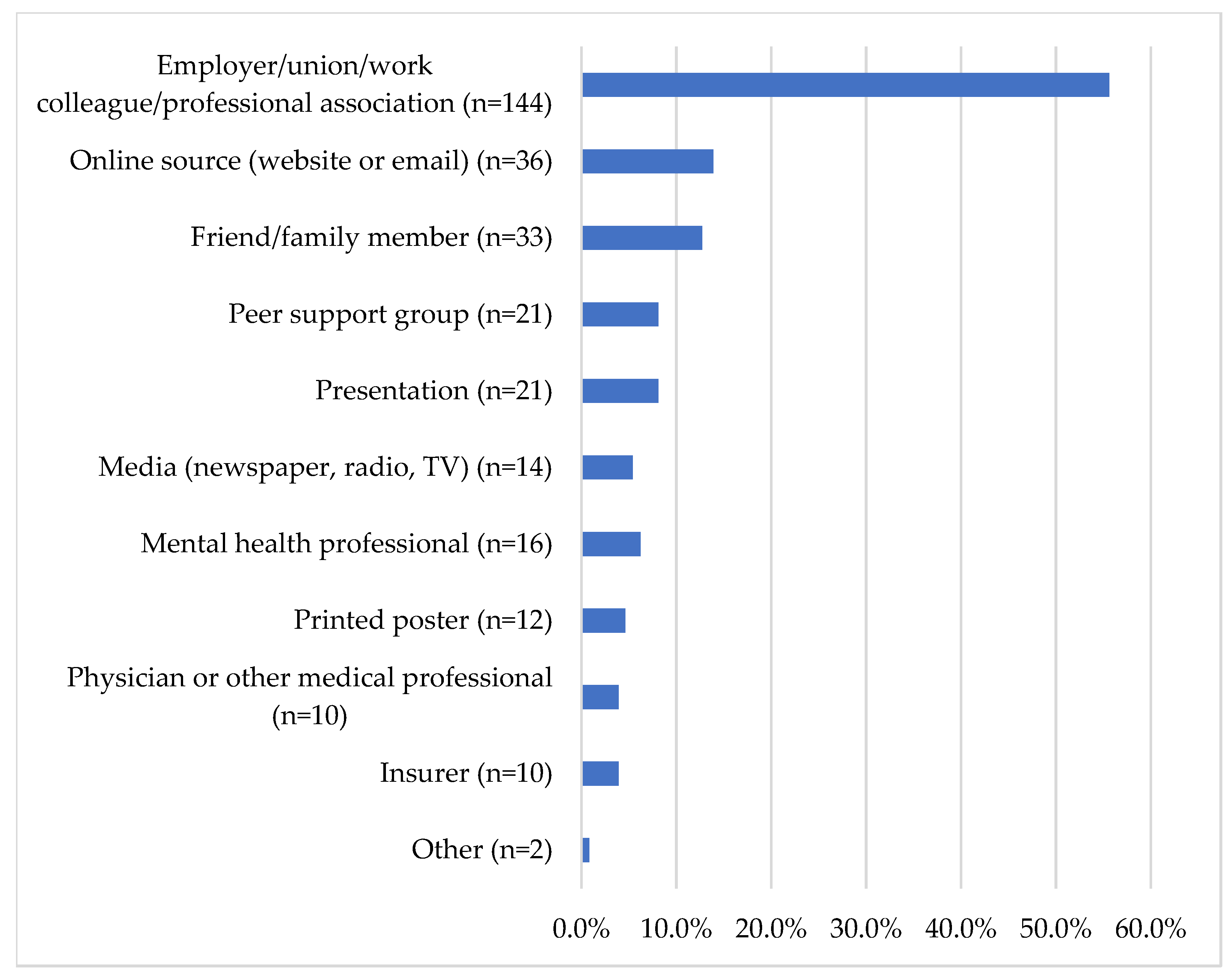
3.2. How Did Prospective Clients First Hear about PSPNET?
3.3. How Do Prospective Clients Perceive ICBT?
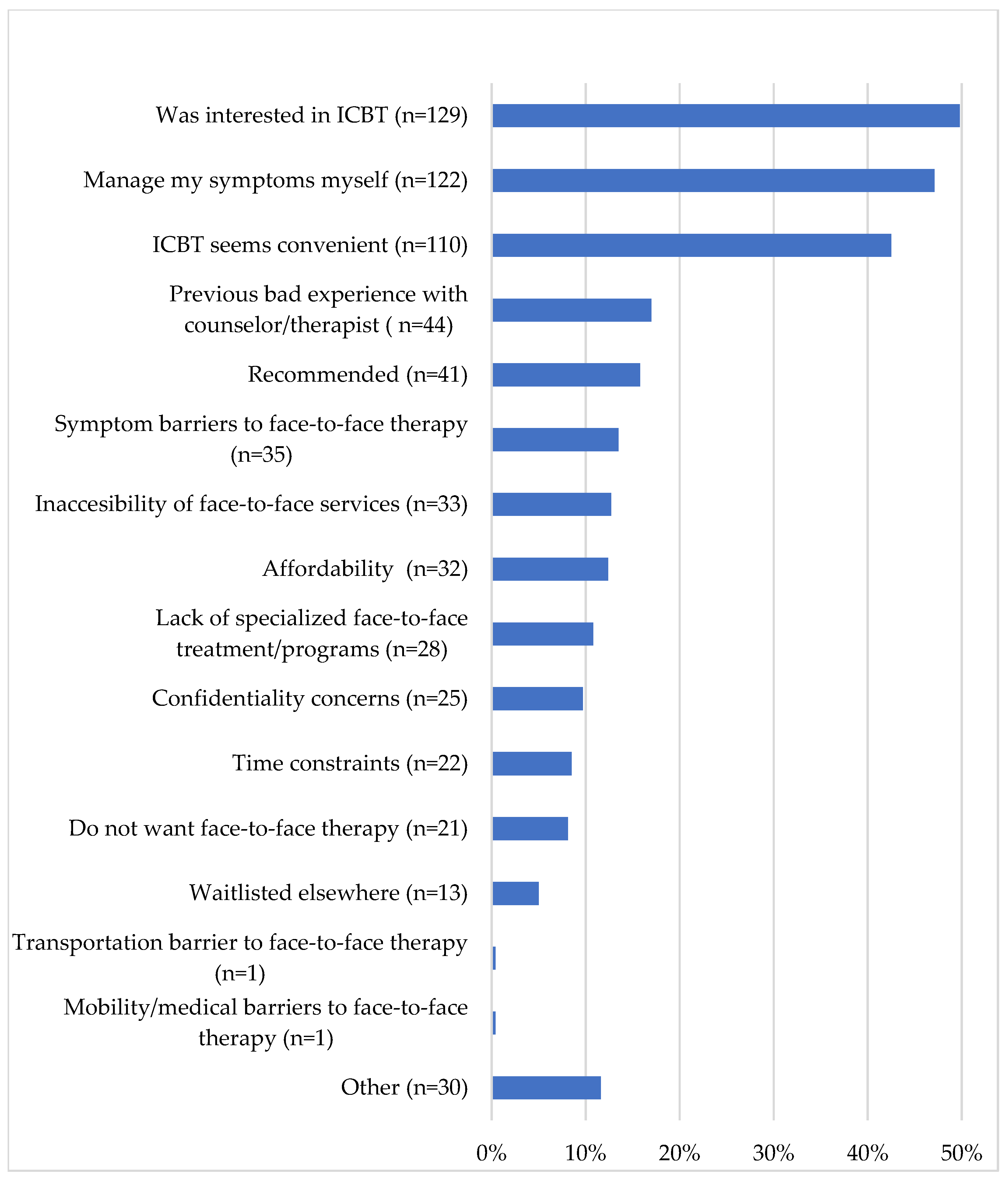
3.4. What Motivations Do Prospective Clients Report for Seeking ICBT?
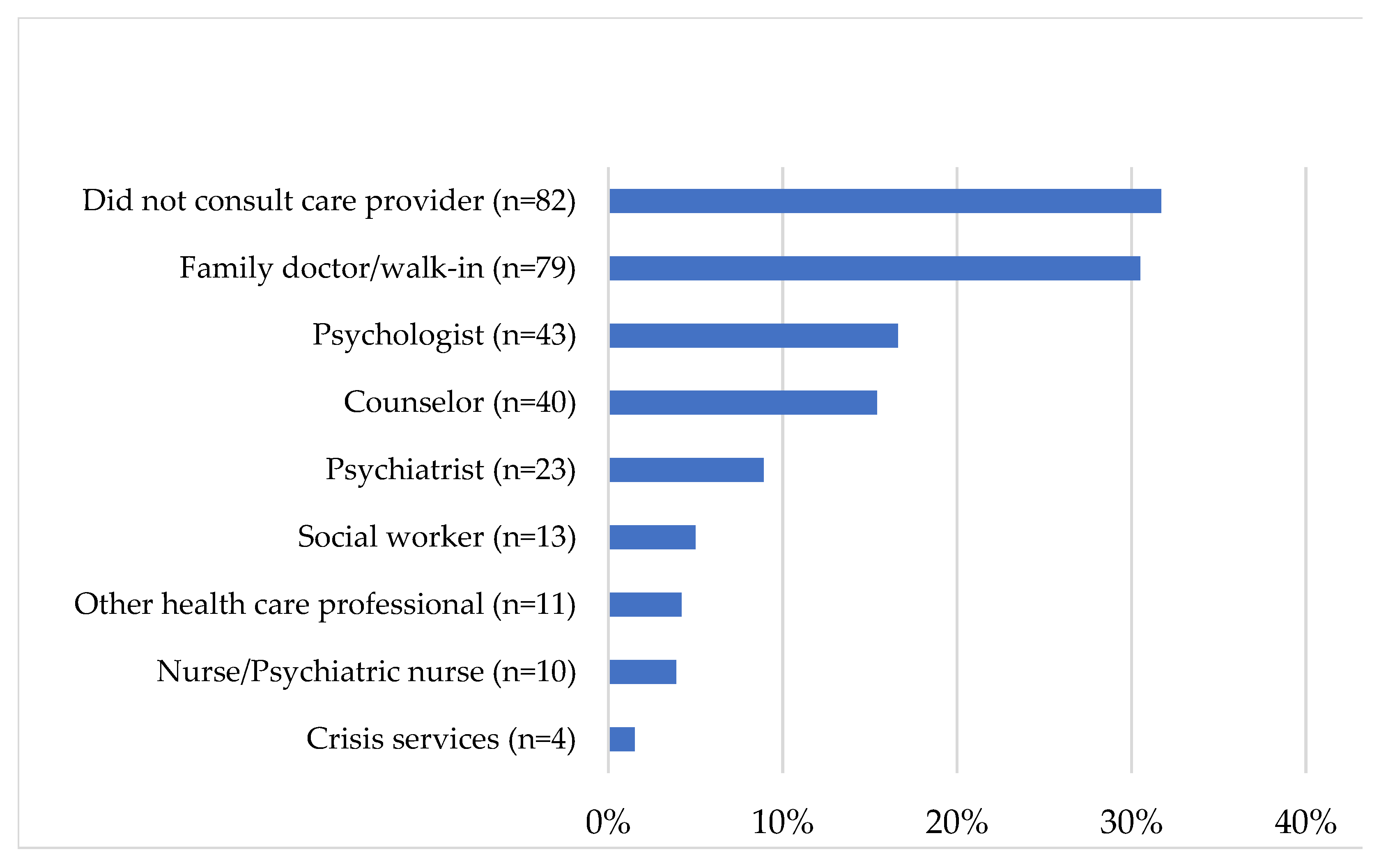
3.5. What Past and Current Mental Health Treatments Do PSP Report Having Tried?
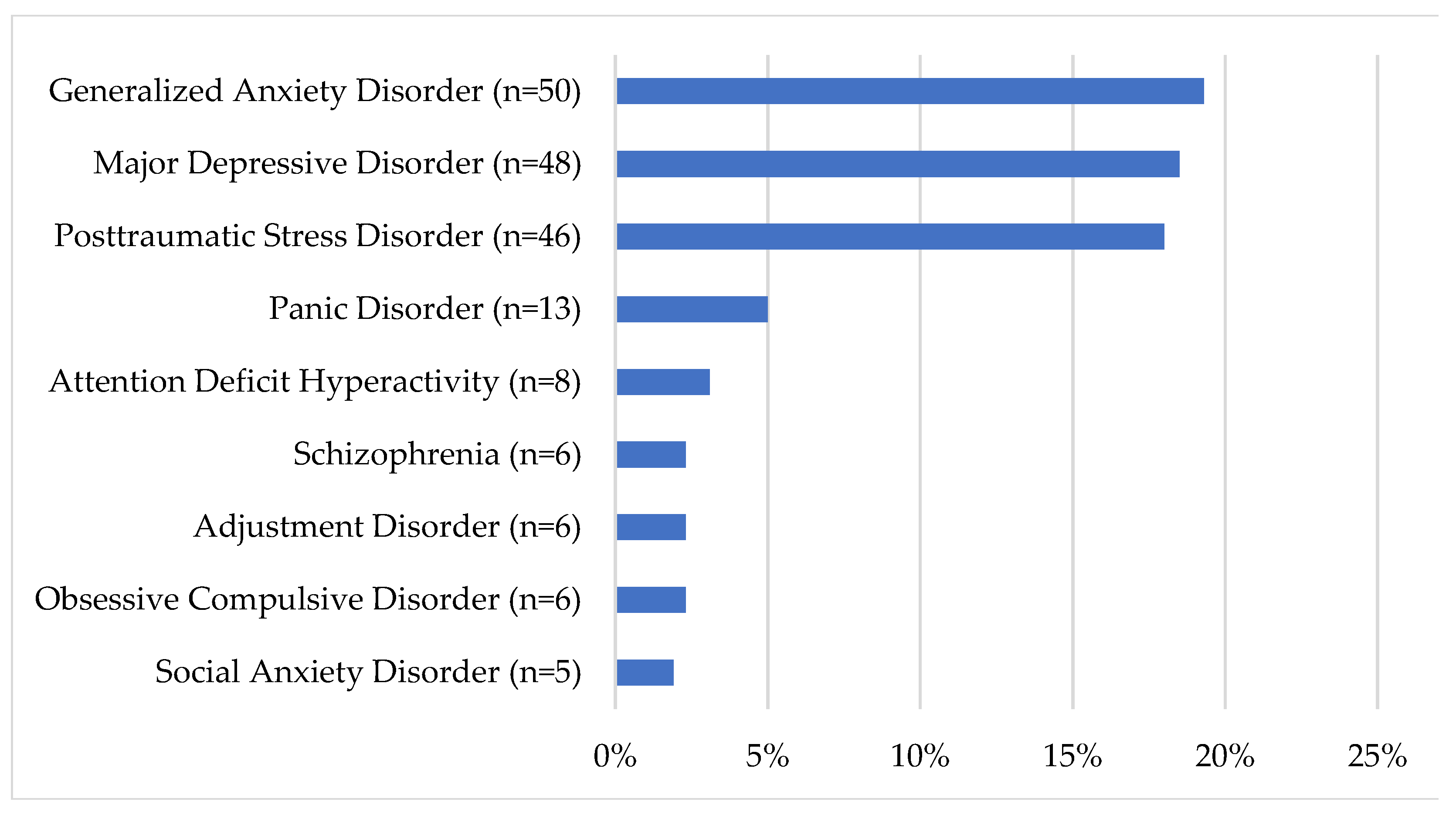
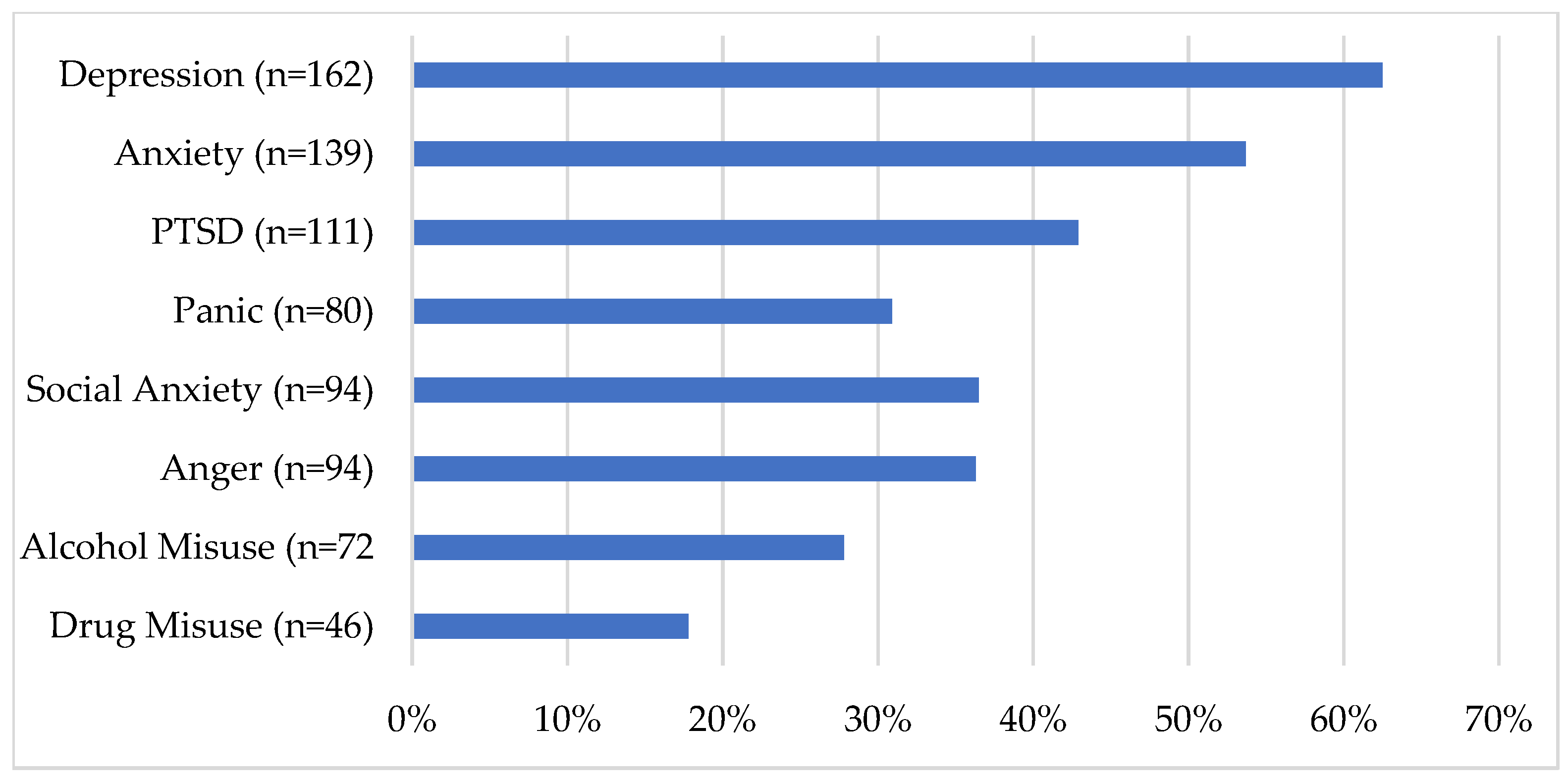
3.6. What Are the Current Clinical Characteristics of Prospective PSPNET Clients?
4. Discussion
4.1. Principal Findings
4.2. Key Implications
4.3. Limitations and Future Directions
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Canadian Institute for Public Safety Research and Treatment Glossary of Terms: A Shared Understanding of the Common Terms Used to Describe Psychological Trauma (Version 2.1). 2019. Available online: https://www.cipsrt-icrtsp.ca/assets/glossary-of-terms-version-21-1.pdf (accessed on 12 November 2021).
- American Psychiatric Association (Ed.) Diagnostic and Statistical Manual of Mental Disorders: DSM-5, 5th ed.; American Psychiatric Association: Washington, DC, USA, 2013; ISBN 978-0-89042-554-1. [Google Scholar]
- Carleton, R.N.; Afifi, T.O.; Taillieu, T.; Turner, S.; Krakauer, R.; Anderson, G.S.; MacPhee, R.S.; Ricciardelli, R.; Cramm, H.A.; Groll, D.; et al. Exposures to Potentially Traumatic Events among Public Safety Personnel in Canada. Can. J. Behav. Sci. Rev. Can. Des Sci. Comport. 2019, 51, 37–52. [Google Scholar] [CrossRef]
- Carleton, R.N.; Afifi, T.O.; Turner, S.; Taillieu, T.; Duranceau, S.; LeBouthillier, D.M.; Sareen, J.; Ricciardelli, R.; MacPhee, R.S.; Groll, D.; et al. Mental Disorder Symptoms among Public Safety Personnel in Canada. Can. J. Psychiatry 2018, 63, 54–64. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Courtney, J.A.; Francis, A.J.P.; Paxton, S.J. Caring for the Country: Fatigue, Sleep and Mental Health in Australian Rural Paramedic Shiftworkers. J. Community Health 2013, 38, 178–186. [Google Scholar] [CrossRef]
- Maia, D.B.; Marmar, C.R.; Metzler, T.; Nóbrega, A.; Berger, W.; Mendlowicz, M.V.; Coutinho, E.S.F.; Figueira, I. Post-Traumatic Stress Symptoms in an Elite Unit of Brazilian Police Officers: Prevalence and Impact on Psychosocial Functioning and on Physical and Mental Health. J. Affect. Disord. 2007, 97, 241–245. [Google Scholar] [CrossRef] [PubMed]
- Morren, M.; Yzermans, C.J.; Nispen, R.M.A.; Wevers, S.J.M. The Health of Volunteer Firefighters Three Years after a Technological Disaster. J. Occup. Health 2005, 47, 523–532. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Spinhoven, P.; Verschuur, M. Predictors of Fatigue in Rescue Workers and Residents in the Aftermath of an Aviation Disaster: A Longitudinal Study. Psychosom. Med. 2006, 68, 605–612. [Google Scholar] [CrossRef]
- Chang, C.-M.; Davidson, J.R.T. Posttraumatic Distress and Coping Strategies among Rescue Workers after an Earthquake. J. Nerv. Ment. Dis. 2003, 191, 391–398. [Google Scholar] [CrossRef]
- Fullerton, C.S.; Ursano, R.J.; Wang, L. Acute Stress Disorder, Posttraumatic Stress Disorder, and Depression in Disaster or Rescue Workers. Am. J. Psychiatry 2004, 161, 1370–1376. [Google Scholar] [CrossRef]
- Stanley, I.H.; Boffa, J.W.; Hom, M.A.; Kimbrel, N.A.; Joiner, T.E. Differences in Psychiatric Symptoms and Barriers to Mental Health Care between Volunteer and Career Firefighters. Psychiatry Res. 2017, 247, 236–242. [Google Scholar] [CrossRef] [Green Version]
- McCall, H.C.; Beahm, J.D.; Fournier, A.K.; Burnett, J.L.; Carleton, R.N.; Hadjistavropoulos, H.D. Stakeholder Perspectives on Internet-Delivered Cognitive Behavioural Therapy for Public Safety Personnel: A Qualitative Analysis. Can. J. Behav. Sci. Rev. Can. Des Sci. Comport. 2020, 53, 232–242. [Google Scholar] [CrossRef]
- Carleton, R.N.; Afifi, T.O.; Turner, S.; Taillieu, T.; Vaughan, A.D.; Anderson, G.S.; Ricciardelli, R.; MacPhee, R.S.; Cramm, H.A.; Czarnuch, S.; et al. Mental Health Training, Attitudes toward Support, and Screening Positive for Mental Disorders. Cogn. Behav. Ther. 2020, 49, 55–73. [Google Scholar] [CrossRef] [PubMed]
- Ricciardelli, R.; Carleton, R.N.; Mooney, T.; Cramm, H. “Playing the System”: Structural Factors Potentiating Mental Health Stigma, Challenging Awareness, and Creating Barriers to Care for Canadian Public Safety Personnel. Health 2020, 24, 259–278. [Google Scholar] [CrossRef] [PubMed]
- Carleton, R.N.; Korol, S.; Mason, J.E.; Hozempa, K.; Anderson, G.S.; Jones, N.A.; Dobson, K.S.; Szeto, A.; Bailey, S. A Longitudinal Assessment of the Road to Mental Readiness Training among Municipal Police. Cogn. Behav. Ther. 2018, 47, 508–528. [Google Scholar] [CrossRef] [Green Version]
- Haugen, P.T.; McCrillis, A.M.; Smid, G.E.; Nijdam, M.J. Mental Health Stigma and Barriers to Mental Health Care for First Responders: A Systematic Review and Meta-Analysis. J. Psychiatr. Res. 2017, 94, 218–229. [Google Scholar] [CrossRef]
- Goffman, E. Stigma and Social Identity. In Understanding Deviance: Connecting Classical and Contemporary Perspectives; Routledge: Abingdon, UK, 1963; Volume 256, p. 265. [Google Scholar]
- Andersson, G.; Carlbring, P.; Titov, N.; Lindefors, N. Internet Interventions for Adults with Anxiety and Mood Disorders: A Narrative Umbrella Review of Recent Meta-Analyses. Can. J. Psychiatry 2019, 64, 465–470. [Google Scholar] [CrossRef] [PubMed]
- Sijbrandij, M.; Kunovski, I.; Cuijpers, P. Effectiveness of Internet-delivered Cognitive Behavioral Therapy for Posttraumatic Stress Disorder: A Systematic Review and Meta-analysis. Depress. Anxiety 2016, 33, 783–791. [Google Scholar] [CrossRef] [PubMed]
- Andersson, G.; Titov, N.; Dear, B.F.; Rozental, A.; Carlbring, P. Internet-delivered Psychological Treatments: From Innovation to Implementation. World Psychiatry 2019, 18, 20–28. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Andrews, G.; Basu, A.; Cuijpers, P.; Craske, M.G.; McEvoy, P.; English, C.L.; Newby, J.M. Computer Therapy for the Anxiety and Depression Disorders Is Effective, Acceptable and Practical Health Care: An Updated Meta-Analysis. J. Anxiety Disord. 2018, 55, 70–78. [Google Scholar] [CrossRef]
- Andersson, G.; Cuijpers, P.; Carlbring, P.; Riper, H.; Hedman, E. Guided Internet-Based vs. Face-to-Face Cognitive Behavior Therapy for Psychiatric and Somatic Disorders: A Systematic Review and Meta-Analysis. World Psychiatry 2014, 13, 288–295. [Google Scholar] [CrossRef]
- Andersson, G. Internet-Delivered Psychological Treatments. Annu. Rev. Clin. Psychol. 2016, 12, 157–179. [Google Scholar] [CrossRef]
- Donker, T.; Blankers, M.; Hedman, E.; Ljótsson, B.; Petrie, K.; Christensen, H. Economic Evaluations of Internet Interventions for Mental Health: A Systematic Review. Psychol. Med. 2015, 45, 3357–3376. [Google Scholar] [CrossRef]
- Titov, N.; Dear, B.; Nielssen, O.; Staples, L.; Hadjistavropoulos, H.; Nugent, M.; Adlam, K.; Nordgreen, T.; Bruvik, K.H.; Hovland, A.; et al. ICBT in Routine Care: A Descriptive Analysis of Successful Clinics in Five Countries. Internet Interv. 2018, 13, 108–115. [Google Scholar] [CrossRef] [PubMed]
- Firth, J.; Torous, J.; Stubbs, B.; Firth, J.A.; Steiner, G.Z.; Smith, L.; Alvarez-Jimenez, M.; Gleeson, J.; Vancampfort, D.; Armitage, C.J.; et al. The “Online Brain”: How the Internet May Be Changing Our Cognition. World Psychiatry 2019, 18, 119–129. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- McCall, H.C.; Sison, A.P.; Burnett, J.L.; Beahm, J.D.; Hadjistavropoulos, H.D. Exploring Perceptions of Internet-Delivered Cognitive Behaviour Therapy among Public Safety Personnel: Informing Dissemination Efforts. Int. J. Environ. Res. Public Health 2020, 17, 6026. [Google Scholar] [CrossRef] [PubMed]
- Fleming, T.M.; de Beurs, D.; Khazaal, Y.; Gaggioli, A.; Riva, G.; Botella, C.; Baños, R.M.; Aschieri, F.; Bavin, L.M.; Kleiboer, A.; et al. Maximizing the Impact of E-Therapy and Serious Gaming: Time for a Paradigm Shift. Front. Psychiatry 2016, 7. [Google Scholar] [CrossRef] [Green Version]
- Ludden, G.D.; van Rompay, T.J.; Kelders, S.M.; van Gemert-Pijnen, J.E. How to Increase Reach and Adherence of Web-Based Interventions: A Design Research Viewpoint. J. Med. Internet Res. 2015, 17, e172. [Google Scholar] [CrossRef]
- Hadjistavropoulos, H.D.; McCall, H.C.; Thiessen, D.L.; Huang, Z.; Carleton, R.N.; Dear, B.F.; Titov, N. Initial Outcomes of Transdiagnostic Internet-Delivered Cognitive Behavioral Therapy Tailored to Public Safety Personnel: Longitudinal Observational Study. J. Med. Internet Res. 2021, 23, e27610. [Google Scholar] [CrossRef]
- Alavi, N.; Stephenson, C.; Omrani, M.; Gerritsen, C.; Martin, M.S.; Knyahnytskyi, A.; Zhu, Y.; Kumar, A.; Jagayat, J.; Shirazi, A.; et al. Delivering an Online Cognitive Behavioural Therapy Program. Address Mental Health Challenges Faced by Correctional Workers and Other Public Safety Personnel: Protocol for a Mixed Methods Study. JMIR Res. Protoc. 2021, 10, e30845. [Google Scholar] [CrossRef] [PubMed]
- University Health Network, Toronto Further Development and Initial Testing of RESTORE in Frontline Workers: Mental Health Clinical. Available online: https://trialbulletin.com/lib/entry/ct-04873622 (accessed on 15 June 2021).
- Greenberg, R.P.; Constantino, M.J.; Bruce, N. Are Patient Expectations Still Relevant for Psychotherapy Process and Outcome? Clin. Psychol. Rev. 2006, 26, 657–678. [Google Scholar] [CrossRef] [PubMed]
- Joyce, A.S.; Piper, W.E. Expectancy, the Therapeutic Alliance, and Treatment Outcome in Short-Term Individual Psychotherapy. J. Psychother. Pract. Res. 1998, 7, 236–248. [Google Scholar]
- Meyer, B.; Pilkonis, P.A.; Krupnick, J.L.; Egan, M.K.; Simmens, S.J.; Sotsky, S.M. Treatment Expectancies, Patient Alliance and Outcome: Further Analyses from the National Institute of Mental Health Treatment of Depression Collaborative Research Program. J. Consult. Clin. Psychol. 2002, 70, 1051–1055. [Google Scholar] [CrossRef] [PubMed]
- Hadjistavropoulos, H.D.; Peynenburg, V.; Thiessen, D.L.; Nugent, M.; Karin, E.; Staples, L.; Dear, B.F.; Titov, N. Utilization, Patient Characteristics, and Longitudinal Improvements among Patients from a Provincially Funded Transdiagnostic Internet-Delivered Cognitive Behavioural Therapy Program: Observational Study of Trends over 6 Years. Can. J. Psychiatry 2021, 070674372110068. [Google Scholar] [CrossRef] [PubMed]
- Young, C.; Helis, E.; Williams, D. Internet-Delivered Cognitive Behavioural Therapy for Major Depressive Disorder and Anxiety Disorders: An Environmental Scan. 2018. Available online: https://cadth.ca/internet-delivered-cognitive-behavioural-therapy-major-depressive-disorder-and-anxiety-disorders-1 (accessed on 12 November 2021).
- Kroenke, K.; Spitzer, R.L.; Williams, J.B.W. The PHQ-9: Validity of a Brief Depression Severity Measure. J. Gen. Intern. Med. 2001, 16, 606–613. [Google Scholar] [CrossRef]
- Spitzer, R.L.; Kroenke, K.; Williams, J.B.W.; Löwe, B. A Brief Measure for Assessing Generalized Anxiety Disorder: The GAD-7. Arch. Intern. Med. 2006, 166, 1092–1097. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Blevins, C.A.; Weathers, F.W.; Davis, M.T.; Witte, T.K.; Domino, J.L. The Posttraumatic Stress Disorder Checklist for DSM-5 (PCL-5): Development and Initial Psychometric Evaluation: Posttraumatic Stress Disorder Checklist for DSM-5. J. Trauma Stress 2015, 28, 489–498. [Google Scholar] [CrossRef]
- Houck, P.R.; Spiegel, D.A.; Shear, M.K.; Rucci, P. Reliability of the Self-Report Version of the Panic Disorder Severity Scale. Depress. Anxiety 2002, 15, 183–185. [Google Scholar] [CrossRef] [PubMed]
- Peters, L.; Sunderland, M.; Andrews, G.; Rapee, R.M.; Mattick, R.P. Development of a Short Form Social Interaction Anxiety (SIAS) and Social Phobia Scale (SPS) Using Nonparametric Item Response Theory: The SIAS-6 and the SPS-6. Psychol. Assess. 2012, 24, 66–76. [Google Scholar] [CrossRef] [PubMed]
- Duranceau, S.; Peluso, D.L.; Collimore, K.C.; Asmundson, G.J.G.; Carleton, R.N. La Social Interaction Phobia Scale: Propriétés Psychométriques de La Version Française. Can. J. Behav. Sci. Rev. Can. Des Sci. Comport. 2014, 46, 406–413. [Google Scholar] [CrossRef]
- Carleton, R.N.; Collimore, K.C.; Asmundson, G.J.G.; McCabe, R.E.; Rowa, K.; Antony, M.M. Refining and Validating the Social Interaction Anxiety Scale and the Social Phobia Scale. Depress. Anxiety 2009, 26, E71–E81. [Google Scholar] [CrossRef] [PubMed]
- Menatti, A.R.; Weeks, J.W.; Carleton, R.N.; Morrison, A.S.; Heimberg, R.G.; Hope, D.A.; Blanco, C.; Schneier, F.R.; Liebowitz, M.R. The Social Interaction Phobia Scale: Continued Support for the Psychometric Validity of the SIPS Using Clinical and Non-Clinical Samples. J. Anxiety Disord. 2015, 32, 46–55. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Forbes, D.; Alkemade, N.; Mitchell, D.; Elhai, J.D.; McHugh, T.; Bates, G.; Novaco, R.W.; Bryant, R.; Lewis, V. Utility of The Dimensions of Anger Reactions-5 (Dar-5) Scale As A Brief Anger Measure: Research Article: Utility of DAR-5. Depress. Anxiety 2014, 31, 166–173. [Google Scholar] [CrossRef]
- Saunders, J.B.; Aasland, O.G.; Babor, T.F.; De La Fuente, J.R.; Grant, M. Development of the Alcohol Use Disorders Identification Test (AUDIT): WHO Collaborative Project on Early Detection of Persons with Harmful Alcohol Consumption-II. Addiction 1993, 88, 791–804. [Google Scholar] [CrossRef]
- Berman, A.H.; Bergman, H.; Palmstierna, T.; Schlyter, F. Evaluation of the Drug Use Disorders Identification Test (DUDIT) in Criminal Justice and Detoxification Settings and in a Swedish Population Sample. Eur. Addict. Res. 2005, 11, 22–31. [Google Scholar] [CrossRef] [PubMed]
- Sheehan, D.V. The Sheehan Disability Scales. The Anxiety Disease and How to Overcome It; Charles Scribner and Sons: New York, NY, USA, 1983; Volume 151. [Google Scholar]
- Devilly, G.J.; Borkovec, T.D. Psychometric Properties of the Credibility/Expectancy Questionnaire. J. Behav. Ther. Exp. Psychiatry 2000, 31, 73–86. [Google Scholar] [CrossRef]
- Bouwmans, C.; De Jong, K.; Timman, R.; Zijlstra-Vlasveld, M.; Van der Feltz-Cornelis, C.; Tan, S.S.; Hakkaart-van Roijen, L. Feasibility, Reliability and Validity of a Questionnaire on Healthcare Consumption and Productivity Loss in Patients with a Psychiatric Disorder (TiC-P). BMC Health Serv. Res. 2013, 13, 217. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Braun, V.; Clarke, V. One Size Fits All? What Counts as Quality Practice in (Reflexive) Thematic Analysis? Qual. Res. Psychol. 2021, 18, 328–352. [Google Scholar] [CrossRef]
- Elo, S.; Kyngäs, H. The Qualitative Content Analysis Process. J. Adv. Nurs. 2008, 62, 107–115. [Google Scholar] [CrossRef]
- Braun, V.; Clarke, V. What Can “Thematic Analysis” Offer Health and Wellbeing Researchers? Int. J. Qual. Stud. Health Well-Being 2014, 9, 26152. [Google Scholar] [CrossRef] [Green Version]
- QSR International NVivo 12 Qualitative Data Analysis Software. Available online: https://www.qsrinternational.com/nvivo-qualitative-data-analysis-software/home (accessed on 27 October 2020).
- McCall, H.C.; Beahm, J.; Landry, C.; Huang, Z.; Carleton, R.N.; Hadjistavropoulos, H. How Have Public Safety Personnel Seeking Digital Mental Healthcare Been Affected by the COVID-19 Pandemic? An Exploratory Mixed Methods Study. Int. J. Environ. Res. Public Health 2020, 17, 9319. [Google Scholar] [CrossRef]
- D’Alfonso, S. AI in Mental Health. Curr. Opin. Psychol. 2020, 36, 112–117. [Google Scholar] [CrossRef]
- Duradoni, M.; Colombini, G.; Russo, P.A.; Guazzini, A. Robotic Psychology: A PRISMA Systematic Review on Social-Robot-Based Interventions in Psychological Domains. J 2021, 4, 664–709. [Google Scholar] [CrossRef]
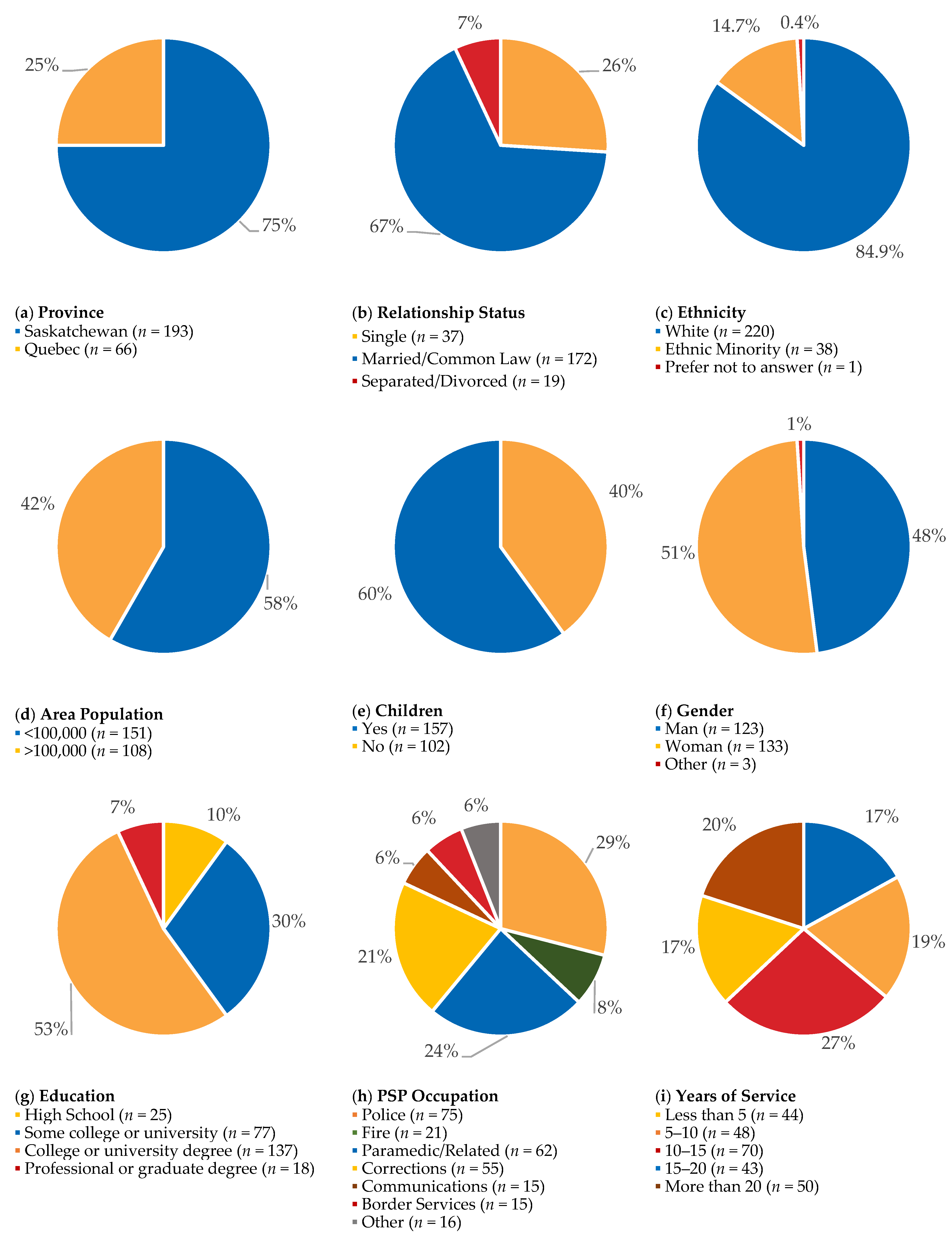
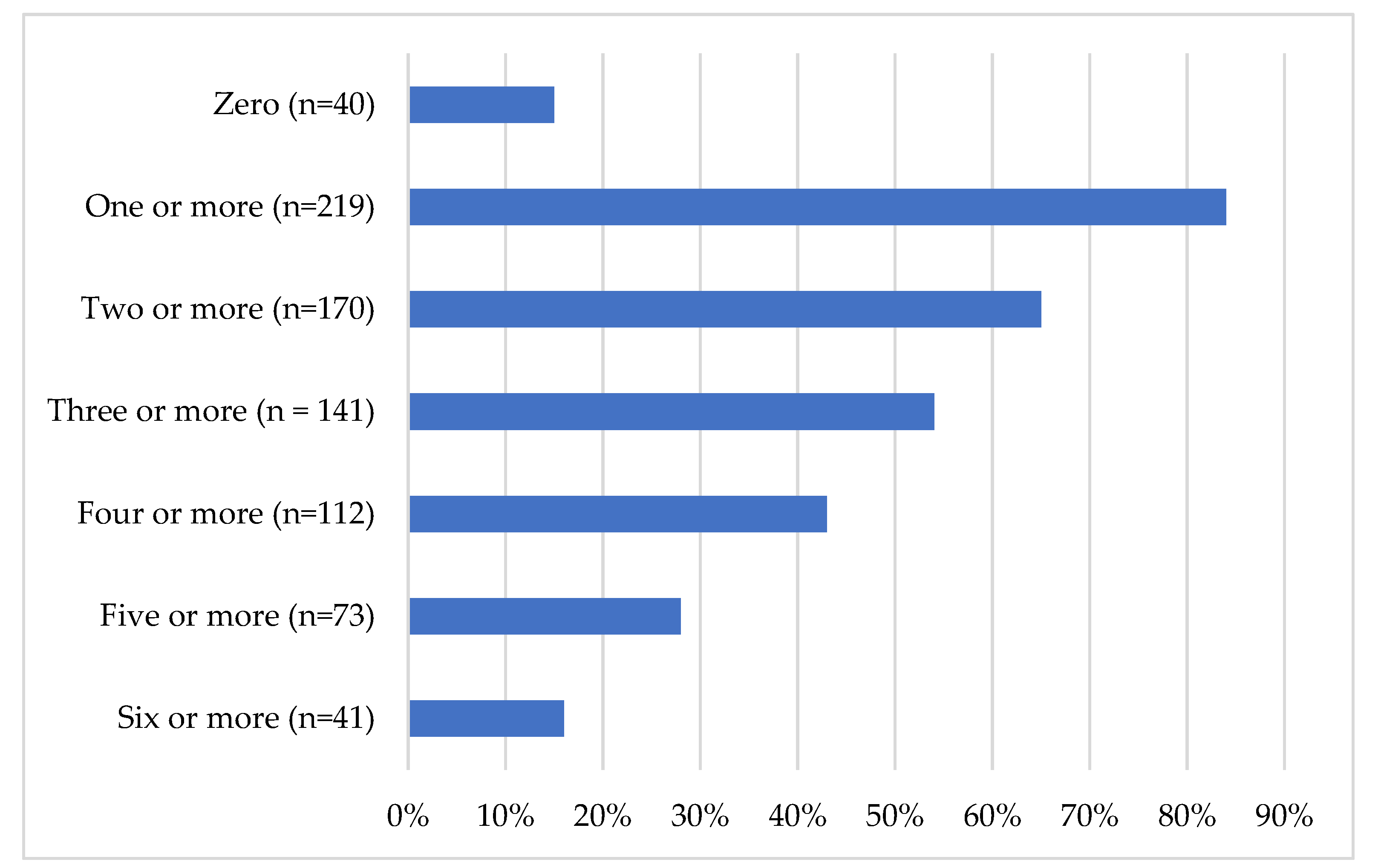
| Measure | Construct Measured | Number of Items | Item Score Range | Clinical Significance Cut-Off Score | Cronbach’s Alpha |
|---|---|---|---|---|---|
| PHQ-9 [38] | MDD | 9 | 0–3 | 10 | 0.87 |
| GAD-7 [39] | GAD | 7 | 0–3 | 10 | 0.89 |
| PCL-5 [40] | PTSD | 20 | 0–4 | 33 | 0.95 |
| PDSS-SR [41] | Panic Disorder | 7 | 0–4 | 8 | 0.92 |
| SIAS-6/SPS-6 [42] | Social Anxiety | 12 | 0–4 | 7 and 2 1 | 0.93 |
| SIPS (French) [43,44,45] | Social Anxiety | 14 | 0–4 | 12 | 0.94 |
| DAR-5 [46] | Anger | 5 | 1–5 | 12 | 0.85 |
| SDS [49] | Disability | 3 | 0–10 | n/a 2 | 0.87 |
| AUDIT [47] | Alcohol Use | 10 | 0–4 | 6/8 3 | 0.85 |
| DUDIT [48] | Drug Use | 11 | 0–4 | 2/6 3 | 0.89 |
| CEQ [50] | Treatment Credibility | 4 | 1–9, 0–100 | n/a 2 | n/a 4 |
| Adapted Tic-P [51] | Health Service Use | 18–83 5 | Not a scored measure | n/a 2 | n/a 4 |
| Description of Theme | Example Quotes | Frequency of Theme, n (%) |
|---|---|---|
| Dealing with perceived symptoms | “Learning how to manage anxiety.” | 126 (52) |
| Multiple reasons | “Improve my quality of life and self-view. Be better in my relationship and increase intimacy. Increase ability to focus and process.” | 18 (7) |
| Desire to improve wellbeing | “Improve my life and mental health.” | 16 (7) |
| Coping tools and stress management | “Adding additional coping skills and resources to my skill set.” | 14 (6) |
| Convenience | “Ease of treatment working around shift work.” | 10 (4) |
| Increasing knowledge to help myself | “Wanting to learn”; “Better myself.” | 9 (4) |
| Taking course for family and relationships | “To be healthy for my children.” | 7(3) |
| Complementing existing treatment | “My psychologist felt it would be appropriate and would assist or compliment the treatment outline he sees for me.” | 6 (2) |
| Curious about ICBT | “I am open to try new things.” | 6 (2) |
| Benefit others | “I’m trying the material out to provide support to other members of my [profession].” | 4 (2) |
| Alternative to face-to-face therapy | “I would like help fixing my issues without having to go to regimented face to face therapy.” | 3 (1) |
| Using ICBT to diagnose perceived symptoms | “To see if I have any issues or if what I am feeling is just normal.” | 3 (1) |
| Other | “Simplicity.” | 10 (4) |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
McCall, H.C.; Landry, C.A.; Ogunade, A.; Carleton, R.N.; Hadjistavropoulos, H.D. Why Do Public Safety Personnel Seek Tailored Internet-Delivered Cognitive Behavioural Therapy? An Observational Study of Treatment-Seekers. Int. J. Environ. Res. Public Health 2021, 18, 11972. https://doi.org/10.3390/ijerph182211972
McCall HC, Landry CA, Ogunade A, Carleton RN, Hadjistavropoulos HD. Why Do Public Safety Personnel Seek Tailored Internet-Delivered Cognitive Behavioural Therapy? An Observational Study of Treatment-Seekers. International Journal of Environmental Research and Public Health. 2021; 18(22):11972. https://doi.org/10.3390/ijerph182211972
Chicago/Turabian StyleMcCall, Hugh C., Caeleigh A. Landry, Adeyemi Ogunade, R. Nicholas Carleton, and Heather D. Hadjistavropoulos. 2021. "Why Do Public Safety Personnel Seek Tailored Internet-Delivered Cognitive Behavioural Therapy? An Observational Study of Treatment-Seekers" International Journal of Environmental Research and Public Health 18, no. 22: 11972. https://doi.org/10.3390/ijerph182211972
APA StyleMcCall, H. C., Landry, C. A., Ogunade, A., Carleton, R. N., & Hadjistavropoulos, H. D. (2021). Why Do Public Safety Personnel Seek Tailored Internet-Delivered Cognitive Behavioural Therapy? An Observational Study of Treatment-Seekers. International Journal of Environmental Research and Public Health, 18(22), 11972. https://doi.org/10.3390/ijerph182211972






