Longitudinal Impact of Depressive Symptoms and Peer Tobacco Use on the Number of Tobacco Products Used by Young Adults
Abstract
1. Introduction
Current Study
2. Materials and Methods
2.1. Participants
2.2. Procedures
2.3. Measures
2.3.1. Dependent Variable
2.3.2. Independent Variable
2.3.3. Moderating Variable
2.4. Data Analysis
2.4.1. Depressive Symptoms Model
2.4.2. Peer Tobacco Use Moderation Model
2.4.3. Attrition Analyses
3. Results
3.1. Depressive Symptoms Model
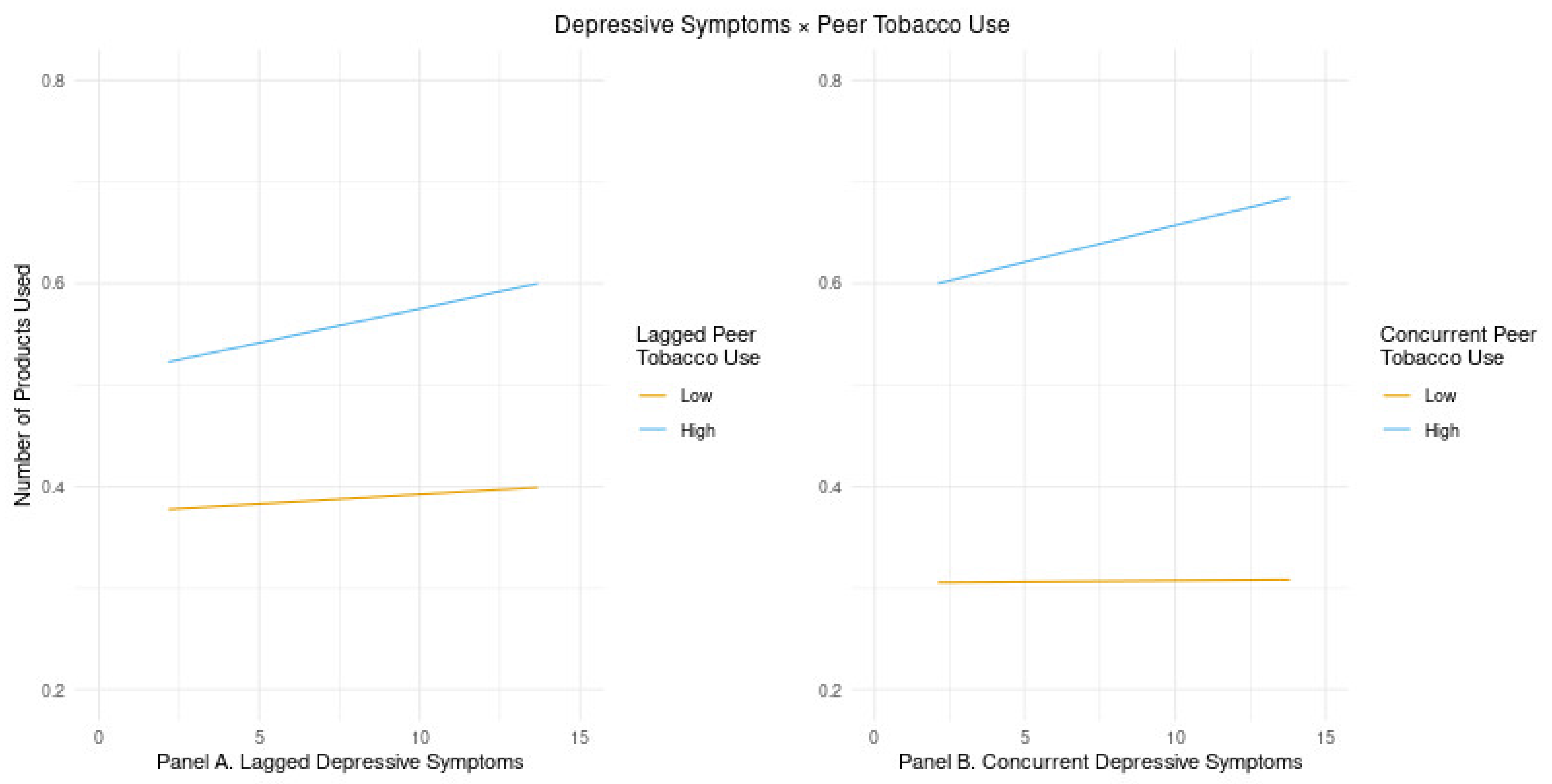
3.2. Peer Tobacco Use Moderation Model
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Kasza, K.A.; Ambrose, B.K.; Conway, K.P.; Borek, N.; Taylor, K.; Goniewicz, M.L.; Cummings, K.M.; Sharma, E.; Pearson, J.L.; Green, V.R.; et al. Tobacco-Product Use by Adults and Youths in the United States in 2013 and 2014. N. Engl. J. Med. 2017, 376, 342–353. [Google Scholar] [CrossRef]
- Osibogun, O.; Jaber, R.; Bahelah, R.; Ben Taleb, Z.; Maziak, W. Poly-Tobacco Use among Young Adults in the United States: Findings from the Population Assessment on Tobacco and Health Study, 2013–2014. Ann. Epidemiol. 2017, 27, 535. [Google Scholar] [CrossRef]
- Osibogun, O.; Taleb, Z.B.; Bahelah, R.; Salloum, R.G.; Maziak, W. Correlates of Poly-Tobacco Use among Youth and Young Adults: Findings from the Population Assessment of Tobacco and Health Study, 2013–2014. Drug Alcohol Depend. 2018, 187, 160–164. [Google Scholar] [CrossRef]
- Perry, C.L.; Pérez, A.; Bluestein, M.; Garza, N.; Obinwa, U.; Jackson, C.; Clendennen, S.L.; Loukas, A.; Harrell, M.B. Youth or Young Adults: Which Group Is at Highest Risk for Tobacco Use Onset? J. Adolesc. Health 2018, 63, 413–420. [Google Scholar] [CrossRef] [PubMed]
- Chassin, L.; Presson, C.C.; Pitts, S.C.; Sherman, S.J. The Natural History of Cigarette Smoking from Adolescence to Adulthood in a Midwestern Community Sample: Multiple Trajectories and Their Psychosocial Correlates. Health Psychol. 2000, 19, 223–231. [Google Scholar] [CrossRef] [PubMed]
- Wetter, D.W.; Kenford, S.L.; Welsch, S.K.; Smith, S.S.; Fouladi, R.T.; Fiore, M.C.; Baker, T.B. Prevalence and Predictors of Transitions in Smoking Behavior Among College Students. Health Psychol. 2004, 23, 168–177. [Google Scholar] [CrossRef] [PubMed]
- Rath, J.M.; Villanti, A.C.; Abrams, D.B.; Vallone, D.M. Patterns of Tobacco Use and Dual Use in US Young Adults: The Missing Link between Youth Prevention and Adult Cessation. J. Environ. Public Health 2012, 2012, 1–9. [Google Scholar] [CrossRef]
- Hair, E.C.; Romberg, A.R.; Niaura, R.; Abrams, D.B.; Bennett, M.A.; Xiao, H.; Rath, J.M.; Pitzer, L.; Vallone, D. Longitudinal Tobacco Use Transitions Among Adolescents and Young Adults: 2014–2016. Nicotine Tob. Res. 2019, 21, 458–468. [Google Scholar] [CrossRef] [PubMed]
- Loukas, A.; Marti, C.N.; Perry, C.L. Trajectories of Tobacco and Nicotine Use Across Young Adulthood, Texas, 2014–2017. Am. J. Public Health 2019, 109, 465–471. [Google Scholar] [CrossRef]
- Stanton, C.A.; Sharma, E.; Edwards, K.C.; Halenar, M.J.; Taylor, K.A.; Kasza, K.A.; Day, H.; Anic, G.; Gardner, L.D.; Hammad, H.T.; et al. Longitudinal Transitions of Exclusive and Polytobacco Electronic Nicotine Delivery Systems (ENDS) Use among Youth, Young Adults and Adults in the USA: Findings from the PATH Study Waves 1–3 (2013–2016). Tob. Control 2020, 29, s147–s154. [Google Scholar] [CrossRef]
- Chen, K.; Kandel, D.B. The Natural History of Drug Use from Adolescence to the Mid-Thirties in a General Population Sample. Am. J. Public Health 1995, 85, 41–47. [Google Scholar] [CrossRef]
- Luger, T.M.; Suls, J.; Vander Weg, M.W. How Robust Is the Association between Smoking and Depression in Adults? A Meta-Analysis Using Linear Mixed-Effects Models. Addict. Behav. 2014, 39, 1418–1429. [Google Scholar] [CrossRef]
- Weinberger, A.H.; Kashan, R.S.; Shpigel, D.M.; Esan, H.; Taha, F.; Lee, C.J.; Funk, A.P.; Goodwin, R.D. Depression and Cigarette Smoking Behavior: A Critical Review of Population-Based Studies. Am. J. Drug Alcohol Abus. 2017, 43, 416–431. [Google Scholar] [CrossRef]
- Kessler, R.C.; Chiu, W.T.; Demler, O.; Walters, E.E. Prevalence, Severity, and Comorbidity of 12-Month DSM-IV Disorders in the National Comorbidity Survey Replication. Arch Gen. Psychiatry 2005, 62, 617. [Google Scholar] [CrossRef] [PubMed]
- Kessler, R.C.; Berglund, P.; Demler, O.; Jin, R.; Walters, E.E. Errors in Byline, Author Affiliations, and Acknowledgment in: Lifetime Prevalence and Age-of-Onset Distributions of DSM-IV Disorders in the National Comorbidity Survey Replication. Arch Gen. Psychiatry 2005, 62, 768. [Google Scholar] [CrossRef]
- Hasin, D.S.; Grant, B.F. The National Epidemiologic Survey on Alcohol and Related Conditions (NESARC) Waves 1 and 2: Review and Summary of Findings. Soc. Psychiatry Psychiatr. Epidemiol. 2015, 50, 1609–1640. [Google Scholar] [CrossRef]
- Chido-Amajuoyi, O.G.; Mantey, D.S.; Omega-Njemnobi, O.; Yu, R.K.; Shete, S. Association of Dual and Poly Tobacco Use with Depressive Symptoms and Use of Antidepressants. Addict. Behav. 2021, 115, 106790. [Google Scholar] [CrossRef] [PubMed]
- Fluharty, M.; Taylor, A.E.; Grabski, M.; Munafo, M.R. The Association of Cigarette Smoking with Depression and Anxiety: A Systematic Review. NICTOB 2017, 19, 3–13. [Google Scholar] [CrossRef]
- Breslau, N.; Johnson, E.O.; Hiripi, E.; Kessler, R. Nicotine Dependence in the United States: Prevalence, Trends, and Smoking Persistence. Arch Gen. Psychiatry 2001, 58, 810. [Google Scholar] [CrossRef]
- Weinberger, A.H.; Mazure, C.M.; Morlett, A.; McKee, S.A. Two Decades of Smoking Cessation Treatment Research on Smokers with Depression: 1990–2010. Nicotine Tob. Res. 2013, 15, 1014–1031. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Hitsman, B.; Papandonatos, G.D.; McChargue, D.E.; DeMott, A.; Herrera, M.J.; Spring, B.; Borrelli, B.; Niaura, R. Past Major Depression and Smoking Cessation Outcome: A Systematic Review and Meta-Analysis Update: Past Major Depression and Smoking Cessation. Addiction 2013, 108, 294–306. [Google Scholar] [CrossRef]
- Conway, K.P.; Green, V.R.; Kasza, K.A.; Silveira, M.L.; Borek, N.; Kimmel, H.L.; Sargent, J.D.; Stanton, C.; Lambert, E.; Hilmi, N.; et al. Co-Occurrence of Tobacco Product Use, Substance Use, and Mental Health Problems among Adults: Findings from Wave 1 (2013-2014) of the Population Assessment of Tobacco and Health (PATH) Study. Drug Alcohol Depend. 2017, 177, 104–111. [Google Scholar] [CrossRef] [PubMed]
- Bandiera, F.C.; Loukas, A.; Wilkinson, A.V.; Perry, C.L. Associations between Tobacco and Nicotine Product Use and Depressive Symptoms among College Students in Texas. Addict. Behav. 2016, 63, 19–22. [Google Scholar] [CrossRef]
- King, J.L.; Reboussin, B.A.; Spangler, J.; Cornacchione Ross, J.; Sutfin, E.L. Tobacco Product Use and Mental Health Status among Young Adults. Addict. Behav. 2018, 77, 67–72. [Google Scholar] [CrossRef] [PubMed]
- Bandiera, F.C.; Loukas, A.; Li, X.; Wilkinson, A.V.; Perry, C.L. Depressive Symptoms Predict Current E-Cigarette Use Among College Students in Texas. Nicotine Tob. Res. 2017, 19, 1102–1106. [Google Scholar] [CrossRef] [PubMed]
- Marsden, D.G.; Loukas, A.; Chen, B.; Perry, C.L.; Wilkinson, A.V. Associations between Frequency of Cigarette and Alternative Tobacco Product Use and Depressive Symptoms: A Longitudinal Study of Young Adults. Addict. Behav. 2019, 99, 106078. [Google Scholar] [CrossRef] [PubMed]
- American College Health. Association College Health Association-National College Health Assessment II: Reference Group Executive Summary Fall 2017; American College Health Association: Hanover, MD, USA, 2018. [Google Scholar]
- Agarwal, D.; Loukas, A.; Perry, C.L. Examining College Students’ Social Environment, Normative Beliefs, and Attitudes in Subsequent Initiation of Electronic Nicotine Delivery Systems. Health Educ. Behav. 2018, 45, 532–539. [Google Scholar] [CrossRef]
- Coleman, B.N.; Johnson, S.E.; Tessman, G.K.; Tworek, C.; Alexander, J.; Dickinson, D.M.; Rath, J.; Green, K.M. “It’s Not Smoke. It’s Not Tar. It’s Not 4000 Chemicals. Case Closed”: Exploring Attitudes, Beliefs, and Perceived Social Norms of e-Cigarette Use among Adult Users. Drug Alcohol Depend. 2016, 159, 80–85. [Google Scholar] [CrossRef]
- Pokhrel, P.; Herzog, T.A.; Muranaka, N.; Fagan, P. Young Adult E-Cigarette Users’ Reasons for Liking and Not Liking e-Cigarettes: A Qualitative Study. Psychol. Health 2015, 30, 1450–1469. [Google Scholar] [CrossRef]
- Villanti, A.; Boulay, M.; Juon, H.-S. Peer, Parent and Media Influences on Adolescent Smoking by Developmental Stage. Addict. Behav. 2011, 36, 133–136. [Google Scholar] [CrossRef]
- Stice, E.; Ragan, J.; Randall, P. Prospective Relations Between Social Support and Depression: Differential Direction of Effects for Parent and Peer Support? J. Abnorm. Psychol. 2004, 113, 155–159. [Google Scholar] [CrossRef]
- Perry, C.L.; Baranowski, T.; Parcel, G.S. How individuals, environments, and health behavior interact: Social learning theory. In Health Behavior and Health Education: Theory, Research, and Practice; The Jossey-Bass Health Series; Jossey-Bass/Wiley: Hoboken, NJ, USA, 1990; pp. 161–186. ISBN 1-55542-243-8. [Google Scholar]
- Loukas, A.; Chow, S.; Pasch, K.E.; Li, X.; Iii, J.T.H.; Marti, C.N.; Harrell, M.B.; Creamer, M.R.; Perry, C.L.; Hinds, J.T. College Students’ Polytobacco Use, Cigarette Cessation, and Dependence. Am. J. Health Behav. 2016, 40, 514–522. [Google Scholar] [CrossRef] [PubMed]
- Starr, G.; Rogers, T.; Schooley, M.; Porter, S.; Wiesen, E.; Jamison, N. Key Outcome Indicators for Evaluating Comprehensive Tobacco Control Programs; Centers for Disease Control and Prevention: Atlanta, GA, USA, 2005. [Google Scholar]
- National Institutes of Health. Population Assessment of Tobacco and Health. 2015. Available online: https://pathstudyinfo.nih.gov/UI/HomeMobile.aspx (accessed on 1 July 2021).
- Andresen, E.M.; Malmgren, J.A.; Carter, W.B.; Patrick, D.L. Screening for Depression in Well Older Adults: Evaluation of a Short Form of the CES-D. Am. J. Prev. Med. 1994, 10, 77–84. [Google Scholar] [CrossRef]
- Bates, D.; Mächler, M.; Bolker, B.; Walker, S. Fitting Linear Mixed-Effects Models Using Lme4. J. Stat. Soft. 2015, 67, 1–48. [Google Scholar] [CrossRef]
- Singer, J.; Willett, J. Applied Longitudinal Data Analysis: Modeling Change and Event Occurrence; Oxford University Press: New York, NY, USA, 2003. [Google Scholar]
- Raftery, A.E. Bayesian Model Selection in Social Research. Sociol. Methodol. 1995, 25, 111. [Google Scholar] [CrossRef]
- Lenth, R. Emmeans: Estimated Marginal Means, aka Least-Squares Means. 2019. Available online: https://CRAN.R-project.org/package=emmeans (accessed on 1 August 2021).
- Twenge, J.M.; Cooper, A.B.; Joiner, T.E.; Duffy, M.E.; Binau, S.G. Age, Period, and Cohort Trends in Mood Disorder Indicators and Suicide-Related Outcomes in a Nationally Representative Dataset, 2005–2017. J. Abnorm. Psychol. 2019, 128, 185–199. [Google Scholar] [CrossRef] [PubMed]
- Varela, A.; Pritchard, M.E. Peer Influence: Use of Alcohol, Tobacco, and Prescription Medications. J. Am. Coll. Health 2011, 59, 751–756. [Google Scholar] [CrossRef]
- Windle, M.; Haardörfer, R.; Lloyd, S.A.; Foster, B.; Berg, C.J. Social Influences on College Student Use of Tobacco Products, Alcohol, and Marijuana. Subst. Use Misuse 2017, 52, 1111–1119. [Google Scholar] [CrossRef] [PubMed]
- Horwath, E. Depressive Symptoms as Relative and Attributable Risk Factors for First-Onset Major Depression. Arch. Gen. Psychiatry 1992, 49, 817. [Google Scholar] [CrossRef]
- Kessler, R.C.; Wang, P.S. Epidemiology of depression. In Handbook of Depression, 2nd ed.; The Guilford Press: New York, NY, USA, 2009; pp. 5–22. ISBN 978-1-59385-450-8. [Google Scholar]
- Lewinsohn, P.M.; Seeley, J.R.; Roberts, R.E.; Allen, N.B. Center for Epidemiologic Studies Depression Scale (CES-D) as a Screening Instrument for Depression among Community-Residing Older Adults. Psychol. Aging 1997, 12, 277–287. [Google Scholar] [CrossRef]
- Mason, M.; Benotsch, E.G.; Way, T.; Kim, H.; Snipes, D. Text Messaging to Increase Readiness to Change Alcohol Use in College Students. J. Prim. Prev. 2014, 35, 47–52. [Google Scholar] [CrossRef] [PubMed]
- Morrison, S.D.; Talbott, L.L. TRUCE for Advocacy and Peer Education in Tobacco Prevention. J. Am. Coll. Health 2005, 54, 193–195. [Google Scholar] [CrossRef] [PubMed]
| Variable Name | Study Waves | |||||||
|---|---|---|---|---|---|---|---|---|
| Fall, 2014 | Spring, 2015 | Fall, 2015 | Spring, 2016 | Fall, 2016 | Spring, 2017 | Spring, 2018 | Spring, 2019 | |
| Number of tobacco products used | * | 0.53 (0.94) | 0.47 (0.88) | 0.45 (0.81) | 0.41 (0.81) | 0.41 (0.80) | 0.41 (0.80) | 0.38 (0.77) |
| Peer tobacco use | 1.85 (0.65) | 1.79 (0.65) | 1.73 (0.58) | 1.69 (0.57) | 1.66 (0.57) | 1.62 (0.56) | 1.65 (0.57) | 1.63 (0.55) |
| Depressive symptoms | 7.82 (5.38) | 6.92 (5.17) | 8.42 (5.78) | 8.37 (5.92) | 8.12 (6.03) | 8.09 (6.04) | 7.96 (5.94) | 8.07 (5.90) |
| Depressive Symptoms Model | Peer Tobacco Use Moderation Model | |||||||||
|---|---|---|---|---|---|---|---|---|---|---|
| Parameter | Coefficient | SE | df | t | p | Coefficient | SE | df | t | p |
| Intercept | 0.49 | 0.05 | 121 | 9.03 | <0.001 | 0.40 | 0.05 | 175 | 8.78 | <0.001 |
| Age | −0.02 | 0.00 | 25,220 | −9.27 | <0.001 | −0.01 | 0.00 | 24,091 | −3.50 | <0.001 |
| Depressive symptoms | 0.01 | 0.00 | 25,761 | 6.86 | <0.001 | 0.00 | 0.00 | 25,068 | 4.50 | <0.001 |
| Depressive symptoms (lagged) | 0.01 | 0.00 | 24,709 | 6.75 | <0.001 | 0.00 | 0.00 | 25,024 | 5.12 | <0.001 |
| Peer tobacco use | 0.29 | 0.01 | 25,097 | 33.19 | <0.001 | |||||
| Peer tobacco use (lagged) | 0.14 | 0.01 | 25,128 | 17.08 | <0.001 | |||||
| Male sex | 0.27 | 0.02 | 4360 | 12.53 | <0.001 | 0.23 | 0.02 | 4141 | 12.04 | <0.001 |
| Hispanic/Latino | −0.03 | 0.03 | 3888 | −0.97 | 0.332 | −0.01 | 0.02 | 3470 | −0.49 | 0.621 |
| African/Black | −0.05 | 0.04 | 3383 | −1.17 | 0.242 | 0.00 | 0.04 | 2962 | −0.06 | 0.950 |
| Asian | −0.10 | 0.03 | 4234 | −3.38 | 0.001 | −0.06 | 0.03 | 3937 | −2.10 | 0.036 |
| Other race/ethnicity | 0.05 | 0.04 | 4364 | 1.16 | 0.246 | 0.04 | 0.04 | 4121 | 1.09 | 0.275 |
| 4-year institution | 0.03 | 0.06 | 46 | 0.45 | 0.657 | 0.03 | 0.05 | 58 | 0.67 | 0.508 |
| Depressive symptoms × Peer tobacco use | 0.01 | 0.00 | 24,233 | 5.11 | <0.001 | |||||
| Dep symptoms (lagged) × Peer Tobacco use (lagged) | 0.00 | 0.00 | 24,035 | 3.48 | <0.001 | |||||
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
North, C.; Marti, C.N.; Loukas, A. Longitudinal Impact of Depressive Symptoms and Peer Tobacco Use on the Number of Tobacco Products Used by Young Adults. Int. J. Environ. Res. Public Health 2021, 18, 11077. https://doi.org/10.3390/ijerph182111077
North C, Marti CN, Loukas A. Longitudinal Impact of Depressive Symptoms and Peer Tobacco Use on the Number of Tobacco Products Used by Young Adults. International Journal of Environmental Research and Public Health. 2021; 18(21):11077. https://doi.org/10.3390/ijerph182111077
Chicago/Turabian StyleNorth, Caroline, C. Nathan Marti, and Alexandra Loukas. 2021. "Longitudinal Impact of Depressive Symptoms and Peer Tobacco Use on the Number of Tobacco Products Used by Young Adults" International Journal of Environmental Research and Public Health 18, no. 21: 11077. https://doi.org/10.3390/ijerph182111077
APA StyleNorth, C., Marti, C. N., & Loukas, A. (2021). Longitudinal Impact of Depressive Symptoms and Peer Tobacco Use on the Number of Tobacco Products Used by Young Adults. International Journal of Environmental Research and Public Health, 18(21), 11077. https://doi.org/10.3390/ijerph182111077






