Lighting in the Home and Health: A Systematic Review
Abstract
1. Introduction
2. Materials and Methods
2.1. Protocol
2.2. Search Strategy
2.3. Eligibility Criteria
2.3.1. Study Type
2.3.2. Population
2.3.3. Exposure
2.3.4. Outcome Measures
2.3.5. Publication Type
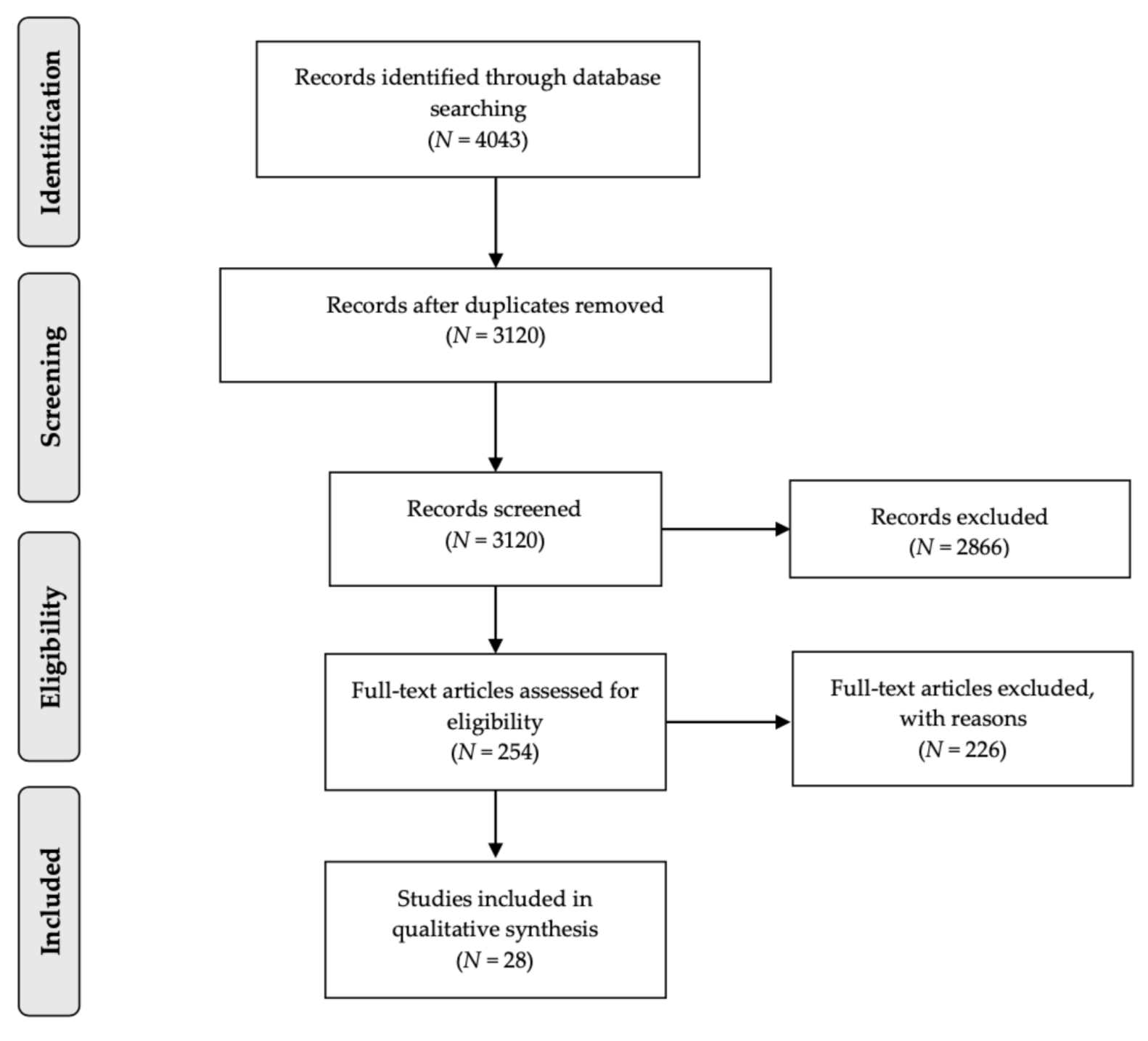
2.4. Study Selection
2.5. Data Extraction
2.6. Study Quality Assessment
2.7. Data Analysis
3. Results
3.1. Study Characteristics
3.2. Methodological Quality Assessment
3.3. Summary of Findings
3.3.1. Natural Light
Physical Health
Mental Health
Sleep Health
3.3.2. Artificial Light
General Health
Physical Health
Mental Health
Sleep Health
3.3.3. Light at Night
Physical Health
Mental Health
Sleep Health
4. Discussion
4.1. Impact of Lighting in the Home on Health
4.1.1. Natural Light
4.1.2. Artificial Light
4.1.3. Light at Night
4.2. Strengths and Limitations
4.3. Future Research
4.4. Wider Policy Implications
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- UN Office of the High Commissioner for Human Rights (OHCHR); The Right to Adequate Housing; UN HABITAT: Geneva, Switzerland, 2009.
- WHO. Housing and Health Guidelines; World Health Organization: Geneva, Switzerland, 2018. [Google Scholar]
- World Health Organisation. Housing and Health Equity. Available online: https://www.who.int/sustainable-development/housing/health-equity/en/ (accessed on 19 April 2020).
- Bonnefoy, X. Inadequate housing and health: An overview. Int. J. Environ. Pollut. 2007, 30. [Google Scholar] [CrossRef]
- Krieger, J.; Higgins, D.L. Housing and health: Time again for public health action. Am. J. Public Health 2002, 92, 758–768. [Google Scholar] [CrossRef] [PubMed]
- Shaw, M. Housing and public health. Annu. Rev. Public Health 2004, 25, 397–418. [Google Scholar] [CrossRef] [PubMed]
- Caillaud, D.; Leynaert, B.; Keirsbulck, M.; Nadif, R. Indoor mould exposure, asthma and rhinitis: Findings from systematic reviews and recent longitudinal studies. Eur. Respir. Rev. 2018, 27. [Google Scholar] [CrossRef]
- Shannon, H.; Allen, C.; Clark, M.; Dávila, D.; Fletcher-Wood, L.; Gupta, S.; Web Annex, A. Report of the systematic review on the effect of household crowding on health. In WHO Housing and Health Guidelines; World Health Organization: Geneva, Switzerland, 2018. [Google Scholar]
- Van Bommel, W.J.M.; Van den Beld, G.J. Lighting for work: A review of visual and biological effects. Lighting Res. Technol. 2016, 36, 255–266. [Google Scholar] [CrossRef]
- Boubekri, M. Daylight, architecture and people’s health. In Environmental Health Risk IV. 11; Brebbia, C.A., Ed.; WIT Press: Southampton, UK, 2007; pp. 53–59. [Google Scholar]
- Christoffersen, J. The importance of light to health and well-being. In Proceedings of the 4th VELUX Daylight Symposium “Daylight in a Human Perspective”, Lausanne, Switzerland, 4–5 May 2011. [Google Scholar]
- Wurtman, R. Biological Implications of Artificial Illumination Illuminating Engineering. In Proceedings of the National Technical Conference of the Illuminating Engineering Society, Phoenix, AZ, USA, 9–12 September 1968; Volume 63, pp. 523–529. [Google Scholar]
- Edwards, L.; Torcellini, P. A Literature Review of the Effects of Natural Light on Building Occupants; Contract No.: NREL/TP-550-30769; National Renewable Energy Laboratory: Golden, CO, USA, 2002. [Google Scholar]
- Perera, S.; Eisen, R.; Bhatt, M.; Bhatnagar, N.; de Souza, R.; Thabane, L.; Samaan, Z. Light therapy for non-seasonal depression: Systematic review and meta-analysis. BJPsych Open 2016, 2, 116–126. [Google Scholar] [CrossRef]
- Wirz-Justice, A.; Graw, P.; Kräuchi, K.; Sarrafzadeh, A.; English, J.; Arendt, J.; Sand, L. ‘Natural’ light treatment of seasonal affective disorder. J. Affect. Disord. 1996, 37, 109–120. [Google Scholar] [CrossRef]
- Pail, G.; Huf, W.; Pjrek, E.; Winkler, D.; Willeit, M.; Praschak-Rieder, N.; Kasper, S. Bright-light therapy in the treatment of mood disorders. Neuropsychobiology 2011, 64, 152–162. [Google Scholar] [CrossRef]
- Golden, R.N.; Gaynes, B.N.; Ekstrom, R.D.; Hamer, R.M.; Jacobsen, F.M.; Suppes, T.; Wisner, K.L.; Nemeroff, C.B. The efficacy of light therapy in the treatment of mood disorders: A review and meta-analysis of the evidence. Am. J. Psychiatry 2005, 162, 656–662. [Google Scholar] [CrossRef]
- Hobday, R.A.; Dancer, S.J. Roles of sunlight and natural ventilation for controlling infection: Historical and current perspectives. J. Hosp. Infect. 2013, 84, 271–282. [Google Scholar] [CrossRef]
- Nightingale, F. Notes on Nursing: What It Is, and What It Is Not; J.B Lippincott Company: Philadelphia, PA, USA, 1960. [Google Scholar]
- Anderson, D.J.; Chen, L.F.; Weber, D.J.; Moehring, R.W.; Lewis, S.S.; Triplett, P.F.; Blocker, M.; Becherer, P.; Schwab, J.C.; Knelson, L.P.; et al. Enhanced terminal room disinfection and acquisition and infection caused by multidrug-resistant organisms and Clostridium difficile (the Benefits of Enhanced Terminal Room Disinfection study): A cluster-randomised, multicentre, crossover study. Lancet 2017, 389, 805–814. [Google Scholar] [CrossRef]
- Anderson, D.J.; Gergen, M.F.; Smathers, E.; Sexton, D.J.; Chen, L.F.; Weber, D.J. Decontamination of targeted pathogens from patient rooms using an automated ultraviolet-C-emitting device. Infect. Control Hosp. Epidemiol. 2013, 34, 466–471. [Google Scholar] [CrossRef] [PubMed]
- Lu, X.; Park, N.K.; Ahrentzen, S. Lighting Effects on Older Adults’ Visual and Nonvisual Performance: A Systematic Review. J. Hous. Elder. 2019, 33, 298–324. [Google Scholar] [CrossRef]
- Aries, M.B.C.; Aarts, M.P.J.; van Hoof, J. Daylight and health: A review of the evidence and consequences for the built environment. Lighting Res. Technol. 2013, 47, 6–27. [Google Scholar] [CrossRef]
- Cho, Y.; Ryu, S.H.; Lee, B.R.; Kim, K.H.; Lee, E.; Choi, J. Effects of artificial light at night on human health: A literature review of observational and experimental studies applied to exposure assessment. Chronobiol. Int. 2015, 32, 1294–1310. [Google Scholar] [CrossRef] [PubMed]
- Mirick, D.K.; Davis, S. Melatonin as a biomarker of circadian dysregulation. Cancer Epidemiol. Biomark. Prev. 2008, 17, 3306–3313. [Google Scholar] [CrossRef]
- Wells, G.A.; Shea, B.; O’Connell, D.; Peterson, J.; Welch, V.; Losos, M.; Tugwell, P. The Newcastle-Ottawa Scale (NOS) for Assessing the Quality of Nonrandomized Studies in Meta-Analyses. Available online: http://www.ohri.ca/programs/clinical_epidemiology/oxford.asp (accessed on 6 April 2020).
- Patel, S.K.; Patel, S.; Kumar, A. Effects of cooking fuel sources on the respiratory health of children: Evidence from the Annual Health Survey, Uttar Pradesh, India. Public Health 2019, 169, 59–68. [Google Scholar] [CrossRef]
- Rahayu, S.R.; Katsuyama, H.; Demura, M.; Katsuyama, M.; Ota, Y.; Tanii, H.; Higashi, T.; Semadi, N.P.D.; Saijoh, K. Factors associated with tuberculosis cases in Semarang District, Indonesia: Case-control study performed in the area where case detection rate was extremely low. Environ. Health Prev. Med. 2015, 20, 253–261. [Google Scholar] [CrossRef][Green Version]
- Kumar, A.; Girdhar, A.; Yadav, V.S.; Girdhar, B.K. Some epidemiological observations on leprosy in India. Int. J. Lepr. Other Mycobact. Dis. 2001, 69, 234–240. [Google Scholar]
- Brown, M.J.; Jacobs, D.E. Residential light and risk for depression and falls: Results from the LARES study of eight European cities. Public Health Rep. 2011, 126, 131–140. [Google Scholar] [CrossRef]
- Ichimori, A.; Tsukasaki, K.; Koyama, E. Measuring illuminance and investigating methods for its quantification among elderly people living at home in Japan to study the relationship between illuminance and physical and mental health. Geriatr. Gerontol. Int. 2013, 13, 798–806. [Google Scholar] [CrossRef] [PubMed]
- Youngstedt, S.D.; Leung, A.; Kripke, D.F.; Langer, R.D. Association of morning illumination and window covering with mood and sleep among post-menopausal women. Sleep Biol. Rhythm. 2004, 2, 174–183. [Google Scholar] [CrossRef] [PubMed]
- Chen, A.Z.; Fischer, J.; Fraker, A.; Shah, N.B.; Shirrell, S.; Stein, D. Welfare impacts of an entry-level solar home system in Uganda. J. Dev. Eff. 2017, 9, 277–294. [Google Scholar] [CrossRef]
- Brunnstrom, G.; Sorensen, S.; Alsterstad, K.; Sjostrand, J. Quality of light and quality of life--the effect of lighting adaptation among people with low vision. Ophthalmic. Physiol. Opt. 2004, 24, 274–280. [Google Scholar] [CrossRef] [PubMed]
- Falkenberg, H.K.; Kvikstad, T.M.; Eilertsen, G. Improved indoor lighting improved healthy aging at home—An intervention study in 77-year-old Norwegians. J. Multidiscip. Healthc. 2019, 12, 315–324. [Google Scholar] [CrossRef]
- Woldesemayat, E.M.; Datiko, D.G.; Lindtjorn, B. Use of biomass fuel in households is not a risk factor for pulmonary tuberculosis in South Ethiopia. Int. J. Tuberc. Lung Dis. 2014, 18, 67–72. [Google Scholar] [CrossRef][Green Version]
- Savitha, M.R.; Nandeeshwara, S.B.; Pradeep Kumar, M.J.; Ul-Haque, F.; Raju, C.K. Modifiable risk factors for acute lower respiratory tract infections. Indian J. Pediatr. 2007, 74, 477–482. [Google Scholar] [CrossRef]
- Mashreky, S.R.; Rahman, A.; Khan, T.F.; Svanstrom, L.; Rahman, F. Determinants of childhood burns in rural Bangladesh: A nested case-control study. Health Policy 2010, 96, 226–230. [Google Scholar] [CrossRef]
- Camilloni, L.; Farchi, S.; Rossi, P.G.; Chini, F.; Di Giorgio, M.; Molino, N.; Iannone, A.; Borgia, P.; Guasticchi, G. A case-control study on risk factors of domestic accidents in an elderly population. Int. J. Injury Control Saf. Promot. 2011, 18, 269–276. [Google Scholar] [CrossRef]
- Shi, J.; Zhou, B.Y.; Tao, Y.K.; Yu, P.L.; Zhang, C.F.; Qin, Z.H.; Sun, Z.Q. Incidence and associated factors for single and recurrent falls among the elderly in an urban community of Beijing. Biomed. Environ. Sci. 2014, 27, 939–949. [Google Scholar] [CrossRef]
- Isberner, F.; Ritzel, D.; Sarvela, P.; Brown, K.; Hu, P.; Newbolds, D. Falls of elderly rural home health clients. Home Health Care Serv. Q. 1998, 17, 41–51. [Google Scholar] [CrossRef] [PubMed]
- Czepita, D.; Goslawski, W.; Mojsa, A. Refractive errors among students occupying rooms lighted with incandescent or fluorescent lamps. Ann. Acad. Med. Stetin. 2004, 50, 51–54. [Google Scholar] [PubMed]
- Hopkins, S.; Morgan, P.L.; Schlangen, L.J.M.; Williams, P.; Skene, D.J.; Middleton, B. Blue-Enriched Lighting for Older People Living in Care Homes: Effect on Activity, Actigraphic Sleep, Mood and Alertness. Curr. Alzheimer Res. 2017, 14, 1053–1062. [Google Scholar] [CrossRef] [PubMed]
- Kayaba, M.; Ihara, T.; Kusaka, H.; Iizuka, S.; Miyamoto, K.; Honda, Y. Association between sleep and residential environments in the summertime in Japan. Sleep Med. 2014, 15, 556–564. [Google Scholar] [CrossRef]
- O’Leary, E.S.; Schoenfeld, E.R.; Stevens, R.G.; Kabat, G.C.; Henderson, K.; Grimson, R.; Gammon, M.D.; Leske, M.C. Shift work, light at night, and breast cancer on Long Island, New York. Am. J. Epidemiol. 2006, 164, 358–366. [Google Scholar] [CrossRef]
- Obayashi, K.; Saeki, K.; Kurumatani, N. Light exposure at night is associated with subclinical carotid atherosclerosis in the general elderly population: The HEIJO-KYO cohort. Chronobiol. Int. 2015, 32, 310–317. [Google Scholar] [CrossRef]
- Obayashi, K.; Saeki, K.; Iwamoto, J.; Okamoto, N.; Tomioka, K.; Nezu, S.; Ikada, Y.; Kurumatani, N. Exposure to light at night, nocturnal urinary melatonin excretion, and obesity/dyslipidemia in the elderly: A cross-sectional analysis of the HEIJO-KYO study. J. Clin. Endocrinol. Metab. 2013, 98, 337–344. [Google Scholar] [CrossRef]
- Obayashi, K.; Saeki, K.; Iwamoto, J.; Ikada, Y.; Kurumatani, N. Association between light exposure at night and nighttime blood pressure in the elderly independent of nocturnal urinary melatonin excretion. Chronobiol. Int. 2014, 31, 779–786. [Google Scholar] [CrossRef]
- Obayashi, K.; Saeki, K.; Iwamoto, J.; Ikada, Y.; Kurumatani, N. Independent associations of exposure to evening light and nocturnal urinary melatonin excretion with diabetes in the elderly. Chronobiol. Int. 2014, 31, 394–400. [Google Scholar] [CrossRef]
- Yamauchi, M.; Jacono, F.J.; Fujita, Y.; Kumamoto, M.; Yoshikawa, M.; Campanaro, C.K.; Loparo, K.A.; Strohl, K.P.; Kimura, H. Effects of environment light during sleep on autonomic functions of heart rate and breathing. Sleep Breath. 2014, 18, 829–835. [Google Scholar] [CrossRef]
- Obayashi, K.; Saeki, K.; Iwamoto, J.; Ikada, Y.; Kurumatani, N. Exposure to light at night and risk of depression in the elderly. J. Affect. Disord. 2013, 151, 331–336. [Google Scholar] [CrossRef]
- Obayashi, K.; Saeki, K.; Kurumatani, N. Bedroom Light Exposure at Night and the Incidence of Depressive Symptoms: A Longitudinal Study of the HEIJO-KYO Cohort. Am. J. Epidemiol. 2018, 187, 427–434. [Google Scholar] [CrossRef]
- Obayashi, K.; Saeki, K.; Kurumatani, N. Association between light exposure at night and insomnia in the general elderly population: The HEIJO-KYO cohort. Chronobiol. Int. 2014, 31, 976–982. [Google Scholar] [CrossRef]
- Obayashi, K.; Saeki, K.; Iwamoto, J.; Okamoto, N.; Tomioka, K.; Nezu, S.; Ikada, Y.; Kurumatani, N. Effect of exposure to evening light on sleep initiation in the elderly: A longitudinal analysis for repeated measurements in home settings. Chronobiol. Int. 2014, 31, 461–467. [Google Scholar] [CrossRef] [PubMed]
- Schiefer, U.; Kraus, C.; Baumbach, P.; Ungewiß, J.; Michels, R. Refractive errors. Dtsch. Arztebl. Int. 2016, 113, 693–702. [Google Scholar] [CrossRef]
- Boubekri, M.; Cheung, I.N.; Reid, K.J.; Wang, C.H.; Zee, P.C. Impact of windows and daylight exposure on overall health and sleep quality of office workers: A case-control pilot study. J. Clin. Sleep Med. 2014, 10, 603–611. [Google Scholar] [CrossRef] [PubMed]
- Figueiro, M.G.; Steverson, B.; Heerwagen, J.; Kampschroer, K.; Hunter, C.M.; Gonzales, K.; Plitnick, B.; Rea, M.S. The impact of daytime light exposures on sleep and mood in office workers. Sleep Health 2017, 3, 204–215. [Google Scholar] [CrossRef] [PubMed]
- Pennings, E. Hospital Lighting and Patient’s Health; Wageningen University: Wageningen, The Netherlands, 2018. [Google Scholar]
- Strong DTG. Daylight Benefits in Healthcare Buildings. 2014. Available online: http://www.designingbuildings.co.uk/wiki/Daylight_benefits_in_healthcare_buildings (accessed on 13 May 2020).
- Joseph, A. Impact of Light on Outcomes in Healthcare Settings; The Center for Health Design: Concord, MA, USA, 2006. [Google Scholar]
- Hockberger, P.E. The discovery of the damaging effect of sunlight on bacteria. J. Photochem. Photobiol. B 2000, 58, 185–191. [Google Scholar] [CrossRef]
- Doudney, C.O.; Young, C.S. Ultraviolet Light Induced Mutation and Deoxyribonucleic Acid Replication in Bacteria. Genetics 1962, 47, 1125–1138. [Google Scholar]
- Broadhurst, J.; Hausmann, T.W. Bacterial Destruction through Glass. Am. J. Nurs. 1930, 30. [Google Scholar] [CrossRef]
- Fahimipour, A.K.; Hartmann, E.M.; Siemens, A.; Kline, J.; Levin, D.A.; Wilson, H.; Betancourt-Román, C.M.; Brown, G.Z.; Fretz, M.; Northcutt, D.; et al. Daylight exposure modulates bacterial communities associated with household dust. Microbiome 2018, 6, 175. [Google Scholar] [CrossRef] [PubMed]
- IEA. SDG7: Data and Projections; Internation Energy Agency: Paris, France, 2019. [Google Scholar]
- Mills, E. Identifying and reducing the health and safety impacts of fuel-based lighting. Energy Sustain. Dev. 2016, 30, 39–50. [Google Scholar] [CrossRef]
- Mills, E. Health Impacts of Fuel-Based Lighting; The Lumina Project: Berkeley, CA, USA, 2012. [Google Scholar]
- Muyanja, D.; Allen, J.G.; Vallarino, J.; Valeri, L.; Kakuhikire, B.; Bangsberg, D.R.; Christiani, D.C.; Tsai, A.C.; Lai, P.S. Kerosene lighting contributes to household air pollution in rural Uganda. Indoor Air 2017, 27, 1022–1029. [Google Scholar] [CrossRef] [PubMed]
- Smith, K.R.; Samet, J.M.; Romieu, I.; Bruce, N. Indoor air pollution in developing countries and acute lower respiratory infections in children. Thorax 2000, 55, 518–532. [Google Scholar] [CrossRef]
- Household Air Pollution and Health Geneva: World Health Organization. 2018. Available online: https://www.who.int/news-room/fact-sheets/detail/household-air-pollution-and-health (accessed on 22 April 2020).
- Tran, V.V.; Park, D.; Lee, Y.C. Indoor Air Pollution, Related Human Diseases, and Recent Trends in the Control and Improvement of Indoor Air Quality. Int. J. Environ. Res. Public Health 2020, 17, 2927. [Google Scholar] [CrossRef]
- Burns: WHO. 2018. Available online: https://www.who.int/news-room/fact-sheets/detail/burns (accessed on 8 September 2020).
- Ahlström, K.; Ahlström, M.; Plummer, A. Jisho.org: Japanese Dictionary. 2020. Available online: https://jisho.org/word/電球 (accessed on 13 May 2020).
- Lucas, R.J.; Peirson, S.N.; Berson, D.M.; Brown, T.M.; Cooper, H.M.; Czeisler, C.A.; Figueiro, M.G.; Gamlin, P.D.; Lockley, S.W.; O’Hagan, J.B.; et al. Measuring and using light in the melanopsin age. Trends Neurosci. 2014, 37, 1–9. [Google Scholar] [CrossRef]
- Sliney, D.H. What is light? The visible spectrum and beyond. Eye 2016, 30, 222–229. [Google Scholar] [CrossRef]
- Aulsebrook, A.E.; Jones, T.M.; Mulder, R.A.; Lesku, J.A. Impacts of artificial light at night on sleep: A review and prospectus. J. Exp. Zool. Ecol. Integr. Physiol. 2018, 329, 409–418. [Google Scholar] [CrossRef]
- Effects on Human Health and the Environment (Fauna and Flora) of Systems Using Light-Emitting Diodes (LEDs); ANSES: Maisons-Alfort, France, 2019.
- Rea, M.S.; Brons, J.A.; Figueiro, M.G. Measurements of light at night (LAN) for a sample of female school teachers. Chronobiol. Int. 2011, 28, 673–680. [Google Scholar] [CrossRef]
- Huss, A.; van Wel, L.; Bogaards, L.; Vrijkotte, T.; Wolf, L.; Hoek, G.; Vermeulen, R. Shedding Some Light in the Dark-A Comparison of Personal Measurements with Satellite-Based Estimates of Exposure to Light at Night among Children in the Netherlands. Environ. Health Perspect. 2019, 127, 67001. [Google Scholar] [CrossRef]
- Dautovich, N.D.; Schreiber, D.R.; Imel, J.L.; Tighe, C.A.; Shoji, K.D.; Cyrus, J.; Bryant, N.; Lisech, A.; O’Brien, C.; Dzierzewski, J.M. A systematic review of the amount and timing of light in association with objective and subjective sleep outcomes in community-dwelling adults. Sleep Health 2019, 5, 31–48. [Google Scholar] [CrossRef] [PubMed]
- Caddick, Z.A.; Gregory, K.; Arsintescu, L.; Flynn-Evans, E.E. A review of the environmental parameters necessary for an optimal sleep environment. Build. Environ. 2018, 132, 11–20. [Google Scholar] [CrossRef]
- Gooley, J.J.; Chamberlain, K.; Smith, K.A.; Khalsa, S.B.; Rajaratnam, S.M.; Van Reen, E.; Zeitzer, J.M.; Czeisler, C.A.; Lockley, S.W. Exposure to room light before bedtime suppresses melatonin onset and shortens melatonin duration in humans. J. Clin. Endocrinol. Metab. 2011, 96, E463–E472. [Google Scholar] [CrossRef] [PubMed]
- The Right Light: Selecting Low Energy Lighting—Introduction for Designers and House Builders; Energy Saving Trust: London, UK, 2016.
- Residential Lighting Design Guide; Contech Lighting: Chicago, IL, USA, 2018.
- National Healthy Housing Standard; National Center for Healthy Housing: Columbia, MD, USA, 2018.
- Housing Health and Safety Rating System; Ministry of Housing, Government DfCaL: London, UK, 2006.
| First Author, Year Reference | Study Design | Country | Sample Size | Age (Years) | Lighting Exposure | Health Domain | Health Outcome | Main Finding | Quality Score |
|---|---|---|---|---|---|---|---|---|---|
| NATURAL LIGHT | |||||||||
| Rahayu, 2015 [28] | Case-control | Indonesia | 212 | Adults | Subjective: Presence of sunlight | PH | OM: Tuberculosis | ↑ Presence of sunlight in the house protective against tuberculosis (OR 0.06, 95% CI 0.00–0.67) * | Fair |
| Kumar, 2001 [29] | Cross-sectional | India | 13,320 | All | Subjective: Insufficient household light exposure | PH | OM: Leprosy | ↑ Persons living in houses with insufficient sunlight exposure observed to be more afflicted by leprosy (OR 1.57, 95% CI 0.84–2.88) | Fair |
| Brown, 2011 [30] | Cross-sectional | Lithuania, Switzerland, Italy, Germany, Portugal, Hungary, Slovakia and France | 6017 | ≥18 | Subjective: Inadequate residential light | PH MH | SR: Falls and depression | ↑ Participants reporting inadequate natural light in dwelling more likely to report falls (OR 1.5, 95% CI 1.2–1.9) * and depression (OR 1.4, 95% CI 1.2–1.7) * | Fair |
| Ichimori, 2013 [31] | Cross-sectional | Japan | 24 | 76–90 | Objective: Daytime illuminance | PH MH | SR: Physical health and depression | - No relationship between illuminance and physical health ↑ Time exposed to light over 400 lx and depression scores * | Fair |
| Youngstedt, 2004 [32] | Cross-sectional | USA | 459 | 50–81 | Objective: Morning illuminance | PH SH | SR: Mood SR and OM: Sleep | ↑ Morning illumination moderately associated with improved mood * and sleep | Fair |
| ARTIFICIAL LIGHT | |||||||||
| Chen, 2017 [33] | Case-control | Uganda | 934 | NR | Treatment: Solar home lighting system Comparison: Low quality sources | PH GH | SR: Burns, cough and personal health | ↑ Burns by lighting source 6.5 p.p. less; cough 9.3 p.p. less; and self-reported health 35.2 p.p. higher among households with solar home lighting system | Fair |
| Brunnstrom, 2004 [34] | Randomised trial | Sweden | 46 | 20–90 | Intervention: Living room adjustment-50 Watts halogen, 12 Volt standard floor lamp | GH | SR: General health and depressed mood | ↑ Improvement in general health p < 0.01 and depressed mood p < 0.04 after the adaptation was found for the intervention group | Fair |
| First Author, Year | Study Design | Country | Sample Size | Age (Years) | Lighting Exposure | Health Domain | Health Outcome | Main Finding | Quality Score |
| Falkenberg, 2019 [35] | Randomised trial | Norway | 60 | 77 | Intervention: Providing lamps to achieve recommended living room lighting levels (200 lux) | GH | SR: Visual health and general health | - Self-reported visual problems and health unchanged in both groups during the intervention | Good |
| Woldesemayat, 2014 [36] | Case-control | Ethiopia | 1154 | Adult | Kerosene lamps, electricity, others | PH | OM: Pulmonary tuberculosis | - Kerosene lamps used for lighting by 73% cases and 71.5% controls, electric lighting used by 24.5% cases and 26.6% controls. The remaining participants used other kerosene-based or other light sources | Fair |
| Savitha, 2007 [37] | Case-control | India | 208 | 0–5 | Kerosene lamps, electricity | PH | OM: Acute lower respiratory infection (ALRI) | ↑ 36.54% of ALRI cases used kerosene lamps for lighting compared to 2.88% of controls, which used electric lighting | Fair |
| Patel, 2019 [27] | Cross-sectional | India | 932,341 | 0–59 months | Electricity and solar, kerosene and other oils, others | PH | SR: Acute respiratory infection (ARI) | ↑ Kerosene and other sources for lighting have higher (OR 1.07, 95% CI 1.05–1.10) * for ARI compared to electric and solar lighting | Fair |
| Mashreky, 2010 [38] | Case–control | Bangladesh | 840 | <10 | Use of traditional kerosene lamp (kupi bati) | PH | OM: Burn | ↑ Using a kupi bati increased risk of burn (OR 3.16, 95% CI 1.58–6.35) * with attributable risk of 68.38% | Fair |
| Camilloni, 2011 [39] | Case-control | Italy | 74 | 65–85 | Subjective: Poor lighting | PH | SR: Home injuries | ↑ Poor household illumination associated with home injuries (OR 3.00, 95% CI 1.41–6.38) * | Fair |
| Shi, 2014 [40] | Cross-sectional | China | 472 | Adults | Subjective: Sufficient lighting for stairway | PH | SR: Falls | ↑ Sufficient lighting for stairway can lower the risk for a single fall (OR 0.45, 95% CI 0.21–0.96) * | Good |
| Isberner, 1998 [41] | Case-control | USA | 90 | ≥60 | Subjective: Poor lighting at stairs | PH | SR: Falls | ↑ Participants with poor lighting at stairs had a higher chance of falling (OR 3.31, 95% CI 0.63–17.36) | Fair |
| First Author, Year | Study Design | Country | Sample Size | Age (Years) | Lighting Exposure | Health Domain | Health Outcome | Main Finding | Quality Score |
| Czepita, 2004 [42] | Cross-sectional | Poland | 3636 | 6–18 | Type of lighting: Fluorescent or incandescent in living room, dining room, child’s room, parent’s room, kitchen and bathroom. | PH | OM: Refractive error: emmetropia, myopia, hyperopia, astigmatism and anisometropia | ↑ Higher prevalence of hyperopia with fluorescent lamp in kitchen (p < 0.01) * - No statistically significant findings for other exposure-outcome combinations | Fair |
| Hopkins, 2017 [43] | Crossover | UK | 80 | >60 | Blue-enriched white lighting (17,000 K ≃ 900 lux), white lighting (4000 K ≃200 lux) | MH SH | SR: Mood SR and OM: Sleep | ↑ Blue-enriched lighting reduced anxiety, sleep efficiency and quality * ↑ Blue-enriched light increased night-time activity * | Fair |
| Kayaba, 2014 [44] | Cross-sectional | Japan | 351 | 20–70 | Light-emitting diode (LED), light bulb, fluorescent light | SH | SR: Sleep quality | Compared with LED lighting: ↑ Light bulbs (OR: 3.7, 95% CI 1.1–12.6) * were risk factors for variable sleep quality - Fluorescent lighting produced no significant results (OR 2.1, 95% CI 0.8–5.7) | Fair |
| LIGHT AT NIGHT | |||||||||
| Czepita, 2004 [42] | Cross-sectional | Poland | 3636 | 6–18 | Lighting habit: Sleeping in darkness or with the light on | PH | OM: Refractive error (emmetropia, myopia, hyperopia, astigmatism and anisometropia) | - No relationship between prevalence of refractive error and sleeping with the light turned on or off at night | Fair |
| O’Leary, 2006 [45] | Case-control | USA | 1161 | <75 | Lighting habit during sleep hours | PH | OM: Breast cancer | ↑ Increased risk of breast cancer for women who frequently turned on lights at home during sleep hours (OR 1.65, 95% CI 1.02–2.69) * | Fair |
| First Author, Year | Study Design | Country | Sample Size | Age (Years) | Lighting Exposure | Health Domain | Health Outcome | Main Finding | Quality Score |
| Obayashi, 2015 [46] | Cross-sectional | Japan | 700 | ≥60 | Objective: Indoor illumination level | PH | OM: Carotid atherosclerosis | ↑ With each quartile increase in light exposure, mean carotid intima-media thickness increased (ptrend = 0.002) * | Good |
| Obayashi, 2013 [47] | Cross-sectional | Japan | 528 | ≥60 | Objective: Indoor illumination level | PH | SR and OM: Obesity and dyslipidaemia | ↑ Light intensity and Body Mass Index (OR 1.89, 95% CI 1.02–2.57) *; abdominal obesity (OR 1.62, 95% CI 1.02–2.57) *; and dyslipidaemia (OR 1.72, 95% CI 1.11–2.68) * | Good |
| Obayashi, 2014 [48] | Cross-sectional | Japan | 528 | ≥60 | Objective: Indoor illumination level | PH | OM: Night-time blood pressure | ↑ Light intensity (≥5 lux) higher night-time systolic BP (adjusted mean: 120.8 vs. 116.5 mmHg) and diastolic BP (70.1 vs. 67.1 mmHg) compared with group <5lux | Good |
| Obayashi, 2014 [49] | Cross-sectional | Japan | 513 | ≥60 | Objective: Indoor illumination level | PH | OM: Diabetes | ↑ Brighter evening light amounts and increase in diabetes prevalence (OR 1.72, 95% CI 1.12–2.64) * | Good |
| Yamauchi, 2014 [50] | Crossover | Japan | 17 | Adult | Light environment: 1000 lux, Dark: 0 lux | PH SH | SR and OM: Sleep (efficacy, latency and apnea) and heart rate variability | ↑ Higher low-frequency power divided by high-frequency ratio power in the analysis of heart rate variability and apnea-hypopnea index in the light environment * - No other differences in sleep in the different light environments | Fair |
| Obayashi, 2013 [51] | Cross-sectional | Japan | 516 | ≥60 | Objective: Indoor illumination level | MH | SR: Depression | ↑ Higher prevalence of light intensity ≥5lux in the depressed group compared with that in the nondepressed group (OR 1.89, 95% CI 1.10–3.25) * ↑ Light at night 10 lux ≥30 min is a risk for depressive symptoms (OR 1.71, 95% CI 1.01–2.89) * | Good |
| Obayashi, 2018 [52] | Longitudinal | Japan | 863 | ≥60 | Objective: Indoor illumination level | MH | SR: Depression | ↑ Light intensity (≥5 Lux) and higher depression risk (HR 1.78, 95% CI 1.07–2.96) * | Good |
| Obayashi, 2014 [53] | Cross-sectional | Japan | 857 | ≥60 | Objective: Indoor illumination level | SH | SR and OM: Sleep quality | ↑ Highest quartile of light intensity showed higher odds for insomnia (OR 1.61, 95% CI 1.05–2.45) *; higher OR for insomnia with each quartile increase in light exposure (ptrend = 0.043) * | Good |
| Obayashi, 2014 [54] | Longitudinal | Japan | 192 | ≥60 | Objective: Indoor illumination level | SH | OM: Sleep onset latency | ↑ Brighter evening light amounts and longer sleep onset latency (regression co-efficient 0.133, 95% CI 0.020–0.247) * | Good |
| Physical Health | Mental Health | Sleep Health |
|---|---|---|
| Injury (including falls and burns) Leprosy Tuberculosis Acute respiratory infections Cough Breast cancer Visual health (including refractive errors) Atherosclerosis Obesity Dyslipidaemia Diabetes Blood pressure Heart function | Depression Anxiety Mood | Sleep quality Sleep latency Sleep efficacy Sleep time Sleep percentage Sleep apnoea |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Osibona, O.; Solomon, B.D.; Fecht, D. Lighting in the Home and Health: A Systematic Review. Int. J. Environ. Res. Public Health 2021, 18, 609. https://doi.org/10.3390/ijerph18020609
Osibona O, Solomon BD, Fecht D. Lighting in the Home and Health: A Systematic Review. International Journal of Environmental Research and Public Health. 2021; 18(2):609. https://doi.org/10.3390/ijerph18020609
Chicago/Turabian StyleOsibona, Oluwapelumi, Bethlehem D. Solomon, and Daniela Fecht. 2021. "Lighting in the Home and Health: A Systematic Review" International Journal of Environmental Research and Public Health 18, no. 2: 609. https://doi.org/10.3390/ijerph18020609
APA StyleOsibona, O., Solomon, B. D., & Fecht, D. (2021). Lighting in the Home and Health: A Systematic Review. International Journal of Environmental Research and Public Health, 18(2), 609. https://doi.org/10.3390/ijerph18020609





