The Importance of Close Follow-Up in Patients with Early-Grade Diabetic Retinopathy: A Taiwan Population-Based Study Grading via Deep Learning Model
Abstract
1. Introduction
2. Materials and Methods
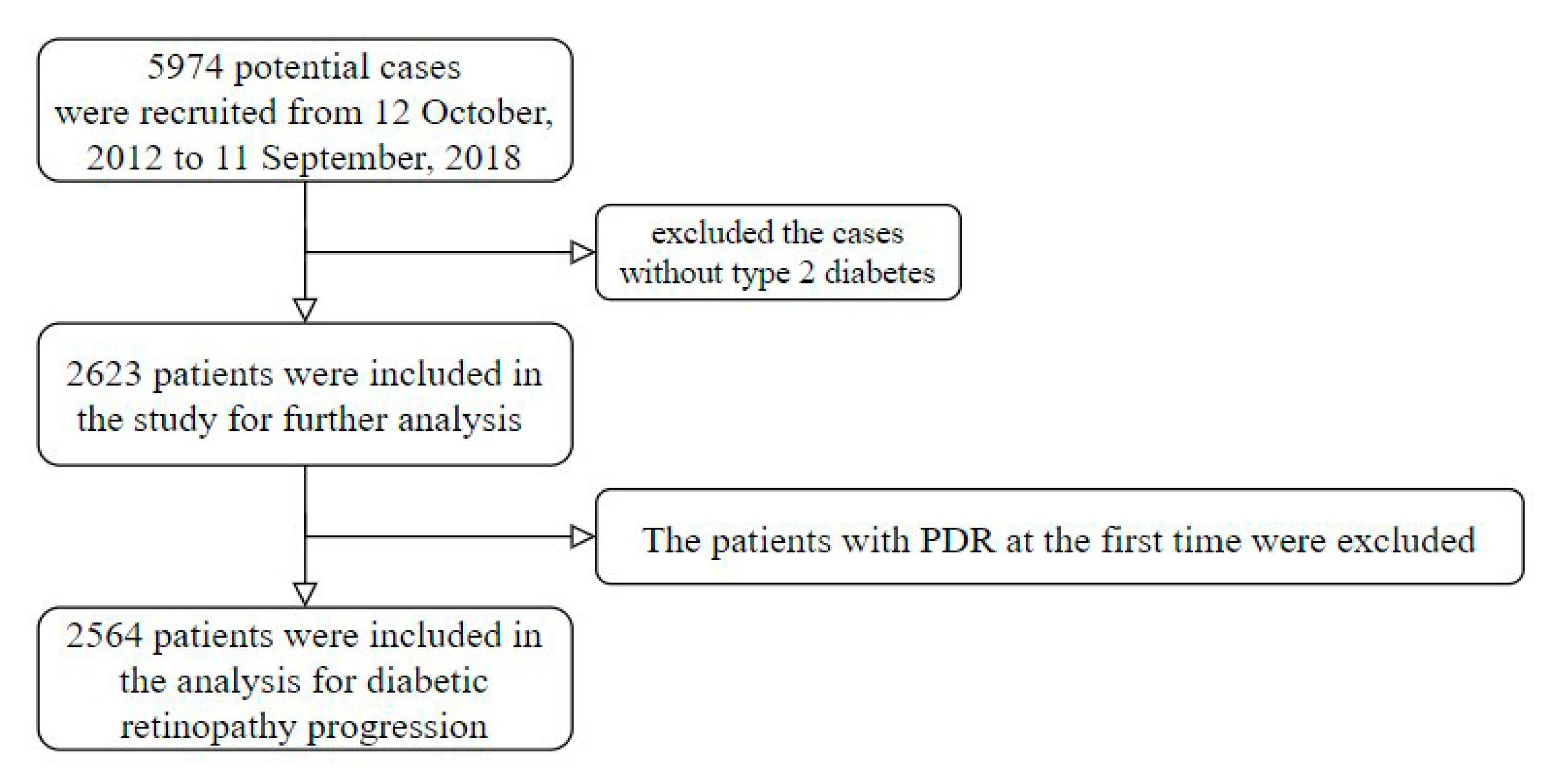
2.1. Population
2.2. DLM for Grading Diabetic Retinopathy
2.3. Statistical Analysis and Model Performance Assessment
3. Results
3.1. Prevalence of Different Grades of DR
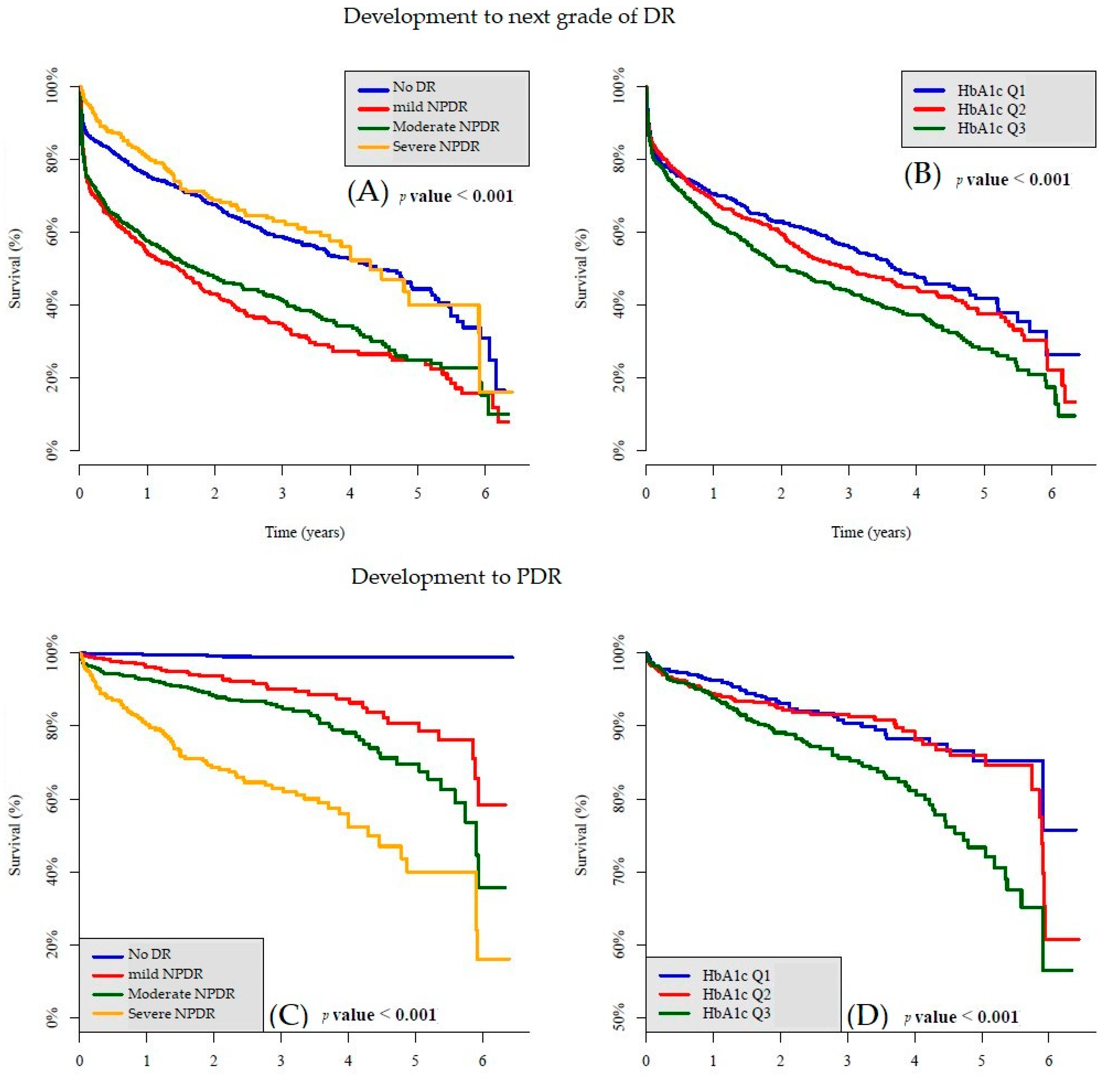
3.2. Effect of HbA1c on DR Progression
3.3. Effect of Initial Grade on DR Progression
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Shaw, J.E.; Sicree, R.A.; Zimmet, P.Z. Global estimates of the prevalence of diabetes for 2010 and 2030. Diabetes Res. Clin. Pract. 2010, 87, 4–14. [Google Scholar] [CrossRef] [PubMed]
- Beulens, J.; Patel, A.; Vingerling, J.; Cruickshank, J.; Hughes, A.; Stanton, A.; Lu, J.; Thom, S.M.; Grobbee, D.; Stolk, R. Effects of blood pressure lowering and intensive glucose control on the incidence and progression of retinopathy in patients with type 2 diabetes mellitus: A randomised controlled trial. Diabetologia 2009, 52, 2027–2036. [Google Scholar] [CrossRef] [PubMed]
- Chen, M.-S.; Kao, C.-S.; Chang, C.-J.; Wu, T.-J.; Fu, C.-C.; Chen, C.-J.; Tai, T.-Y. Prevalence and risk factors of diabetic retinopathy among noninsulin-dependent diabetic subjects. Am. J. Ophthalmol. 1992, 114, 723–730. [Google Scholar] [CrossRef]
- Huang, Y.Y.; Lin, K.D.; Jiang, Y.D.; Chang, C.H.; Chung, C.H.; Chuang, L.M.; Tai, T.Y.; Ho, L.T.; Shin, S.J. Diabetes-related kidney, eye, and foot disease in Taiwan: An analysis of the nationwide data for 2000–2009. J. Formos. Med. Assoc. Taiwan Yi Zhi 2012, 111, 637–644. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Lee, R.; Wong, T.Y.; Sabanayagam, C. Epidemiology of diabetic retinopathy, diabetic macular edema and related vision loss. Eye Vis. 2015, 2, 17. [Google Scholar] [CrossRef] [PubMed]
- Sivaprasad, S.; Prevost, A.T.; Vasconcelos, J.C.; Riddell, A.; Murphy, C.; Kelly, J.; Bainbridge, J.; Tudor-Edwards, R.; Hopkins, D.; Hykin, P. Clinical efficacy of intravitreal aflibercept versus panretinal photocoagulation for best corrected visual acuity in patients with proliferative diabetic retinopathy at 52 weeks (CLARITY): A multicentre, single-blinded, randomised, controlled, phase 2b, non-inferiority trial. Lancet 2017, 389, 2193–2203. [Google Scholar] [CrossRef]
- Gross, J.G.; Glassman, A.R.; Liu, D.; Sun, J.K.; Antoszyk, A.N.; Baker, C.W.; Bressler, N.M.; Elman, M.J.; Ferris, F.L., 3rd; Gardner, T.W.; et al. Five-Year Outcomes of Panretinal Photocoagulation vs Intravitreous Ranibizumab for Proliferative Diabetic Retinopathy: A Randomized Clinical Trial. JAMA Ophthalmol. 2018, 136, 1138–1148. [Google Scholar] [CrossRef]
- Wong, T.Y.; Sun, J.; Kawasaki, R.; Ruamviboonsuk, P.; Gupta, N.; Lansingh, V.C.; Maia, M.; Mathenge, W.; Moreker, S.; Muqit, M.M. Guidelines on diabetic eye care: The international council of ophthalmology recommendations for screening, follow-up, referral, and treatment based on resource settings. Ophthalmology 2018, 125, 1608–1622. [Google Scholar] [CrossRef]
- UK Prospective Diabetes Study (UKPDS) Group. Effect of intensive blood-glucose control with metformin on complications in overweight patients with type 2 diabetes (UKPDS 34). Lancet 1998, 352, 854–865. [Google Scholar] [CrossRef]
- Hsing, S.-C.; Lee, C.-C.; Lin, C.; Chen, J.-T.; Chen, Y.-H.; Fang, W.-H. The Severity of Diabetic Retinopathy Is an Independent Factor for the Progression of Diabetic Nephropathy. J. Clin. Med. 2021, 10, 3. [Google Scholar] [CrossRef]
- Hu, J.; Shen, L.; Sun, G. Squeeze-and-excitation networks. In Proceedings of the IEEE Conference on Computer Vision and Pattern Recognition, Salt Lake City, UT, USA, 18–23 June 2018; pp. 7132–7141. [Google Scholar]
- Available online: https://www.kaggle.com/c/diabetic-retinopathy-detection (accessed on 12 June 2020).
- Verma, L.; Prakash, G.; Tewari, H.K.; Gupta, S.K.; Murthy, G.; Sharma, N. Screening for diabetic retinopathy by non-ophthalmologists: An effective public health tool. Acta Ophthalmol. Scand. 2003, 81, 373–377. [Google Scholar] [CrossRef]
- Cheung, N.; Mitchell, P.; Wong, T.Y. Diabetic retinopathy. Lancet 2010, 376, 124–136. [Google Scholar] [CrossRef]
- Bourne, R.R.; Stevens, G.A.; White, R.A.; Smith, J.L.; Flaxman, S.R.; Price, H.; Jonas, J.B.; Keeffe, J.; Leasher, J.; Naidoo, K. Causes of vision loss worldwide, 1990–2010: A systematic analysis. Lancet Glob. Health 2013, 1, e339–e349. [Google Scholar] [CrossRef]
- Yau, J.W.Y.; Rogers, S.L.; Kawasaki, R.; Lamoureux, E.L.; Kowalski, J.W.; Bek, T.; Chen, S.-J.; Dekker, J.M.; Fletcher, A.; Grauslund, J.; et al. Global prevalence and major risk factors of diabetic retinopathy. Diabetes Care 2012, 35, 556–564. [Google Scholar] [CrossRef]
- Smith, J.J.; Wright, D.M.; Scanlon, P.; Lois, N. Risk factors associated with progression to referable retinopathy: A type 2 diabetes mellitus cohort study in the Republic of Ireland. Diabet. Med. 2020, 37, 1000–1007. [Google Scholar] [CrossRef]
- UK Prospective Diabetes Study Group. Tight blood pressure control and risk of macrovascular and microvascular complications in type 2 diabetes: UKPDS 38. BMJ 1998, 317, 703–713. [Google Scholar] [CrossRef]
- Ali, M.K.; Bullard, K.M.; Saaddine, J.B.; Cowie, C.C.; Imperatore, G.; Gregg, E.W. Achievement of goals in US diabetes care, 1999–2010. New Engl. J. Med. 2013, 368, 1613–1624. [Google Scholar] [CrossRef] [PubMed]
- American Diabetes Association. 4. Foundations of care: Education, nutrition, physical activity, smoking cessation, psychosocial care, and immunization. Diabetes Care 2015, 38, S20–S30. [Google Scholar] [CrossRef]
- Chrvala, C.A.; Sherr, D.; Lipman, R.D. Diabetes self-management education for adults with type 2 diabetes mellitus: A systematic review of the effect on glycemic control. Patient Educ. Couns. 2016, 99, 926–943. [Google Scholar] [CrossRef]
- Kasznicki, J.; Głowacka, A.; Drzewoski, J. Type 2 diabetic patients compliance with drug therapy and glycaemic control. Diabetol. Doświadczalna Klin. 2007, 7, 198–199. [Google Scholar]
- Jansiraninatarajan, M. Diabetic compliance: A qualitative study from the patient’s perspective in developing countries. IOSR J. Nursing and Health Science 2013, 1, 29–38. [Google Scholar] [CrossRef]
- Regensteiner, J.G.; Golden, S.; Huebschmann, A.G.; Barrett-Connor, E.; Chang, A.Y.; Chyun, D.; Fox, C.S.; Kim, C.; Mehta, N.; Reckelhoff, J.F.; et al. Sex Differences in the Cardiovascular Consequences of Diabetes Mellitus: A Scientific Statement from the American Heart Association. Circulation 2015, 132, 2424–2447. [Google Scholar] [CrossRef]
- Abbate, R.; Mannucci, E.; Cioni, G.; Fatini, C.; Marcucci, R. Diabetes and sex: From pathophysiology to personalized medicine. Intern. Emerg. Med. 2012, 7 (Suppl. 3), S215–S219. [Google Scholar] [CrossRef]
- Seghieri, G.; Policardo, L.; Anichini, R.; Franconi, F.; Campesi, I.; Cherchi, S.; Tonolo, G. The Effect of Sex and Gender on Diabetic Complications. Curr. Diabetes Rev. 2017, 13, 148–160. [Google Scholar] [CrossRef]
- Maric-Bilkan, C. Sex differences in micro- and macro-vascular complications of diabetes mellitus. Clin. Sci. 2017, 131, 833–846. [Google Scholar] [CrossRef]
- Kohner, E.M.; Aldington, S.J.; Stratton, I.M.; Manley, S.E.; Holman, R.R.; Matthews, D.R.; Turner, R.C. United Kingdom Prospective Diabetes Study, 30: Diabetic retinopathy at diagnosis of non-insulin-dependent diabetes mellitus and associated risk factors. Arch. Ophthalmol. 1998, 116, 297–303. [Google Scholar] [CrossRef]
- Stratton, I.M.; Kohner, E.M.; Aldington, S.J.; Turner, R.C.; Holman, R.R.; Manley, S.E.; Matthews, D.R. UKPDS 50: Risk factors for incidence and progression of retinopathy in Type II diabetes over 6 years from diagnosis. Diabetologia 2001, 44, 156–163. [Google Scholar] [CrossRef] [PubMed]
- Ozawa, G.Y.; Bearse, M.A., Jr.; Adams, A.J. Male-female differences in diabetic retinopathy? Curr. Eye Res. 2015, 40, 234–246. [Google Scholar] [CrossRef] [PubMed]
- Pardue, M.-L.; Wizemann, T.M. Exploring the biological contributions to human health: Does sex matter? J. Women’s Health Gend. Based Med. 2001, 10, 433–439. [Google Scholar] [CrossRef]
- Fujisawa, T.; Ikegami, H.; Yamato, E.; Kawaguchi, Y.; Ueda, H.; Shintani, M.; Nojima, K.; Kawabata, Y.; Ono, M.; Nishino, T.; et al. Association of plasma fibrinogen level and blood pressure with diabetic retinopathy, and renal complications associated with proliferative diabetic retinopathy, in Type 2 diabetes mellitus. Diabet. Med. 1999, 16, 522–526. [Google Scholar] [CrossRef]
- Mouton, D.P.; Gill, A.J. Prevalence of diabetic retinopathy and evaluation of risk factors. A review of 1005 diabetic clinic patients. South Afr. Med. J. 1988, 74, 399–402. [Google Scholar]
- Segato, T.; Midena, E.; Grigoletto, F.; Zucchetto, M.; Fedele, D.; Piermarocchi, S.; Crepaldi, G. The epidemiology and prevalence of diabetic retinopathy in the Veneto region of north east Italy. Veneto Group for Diabetic Retinopathy. Diabet. Med. 1991, 8, S11–S16. [Google Scholar] [CrossRef]
- Zhou, J.-B.; Song, Z.-H.; Bai, L.; Zhu, X.-R.; Li, H.-B.; Yang, J.-K. Could intensive blood pressure control really reduce diabetic retinopathy outcomes? Evidence from meta-analysis and trial sequential analysis from randomized controlled trials. Diabetes Ther. 2018, 9, 2015–2027. [Google Scholar] [CrossRef] [PubMed]
- Yamamoto, M.; Fujihara, K.; Ishizawa, M.; Osawa, T.; Kaneko, M.; Ishiguro, H.; Matsubayashi, Y.; Seida, H.; Yamanaka, N.; Tanaka, S. Pulse Pressure is a Stronger Predictor Than Systolic Blood Pressure for Severe Eye Diseases in Diabetes Mellitus. J. Am. Heart Assoc. 2019, 8, e010627. [Google Scholar] [CrossRef]
- Steppan, J.; Barodka, V.; Berkowitz, D.E.; Nyhan, D. Vascular stiffness and increased pulse pressure in the aging cardiovascular system. Cardiol. Res. Pract. 2011, 2011, 263585. [Google Scholar] [CrossRef] [PubMed]
| No DR (n = 1046) | Mild NPDR (n = 480) | Moderate NPDR (n = 756) | Severe NPDR (n = 282) | PDR (n = 59) | p-Value | |
|---|---|---|---|---|---|---|
| Basic characteristics | ||||||
| Gender | 0.176 | |||||
| Female | 506 (48.4%) | 215 (44.8%) | 328 (43.4%) | 129 (45.7%) | 32 (54.2%) | |
| Male | 540 (51.6%) | 265 (55.2%) | 428 (56.6%) | 153 (54.3%) | 27 (45.8%) | |
| Age | 63.85 ± 13.22 | 63.24 ± 12.45 | 59.65 ± 11.35 | 57.93 ± 11.81 | 56.66 ± 12.49 | <0.001 |
| Height (cm) | 162.40 ± 8.59 | 162.21 ± 8.97 | 162.47 ± 8.73 | 162.56 ± 9.15 | 161.92 ± 9.08 | 0.968 |
| Weight (kg) | 67.77 ± 13.85 | 67.82 ± 14.02 | 67.81 ± 13.72 | 68.83 ± 15.08 | 68.79 ± 12.96 | 0.806 |
| Body mass index | 25.59 ± 4.27 | 25.74 ± 4.94 | 25.59 ± 4.27 | 25.91 ± 4.66 | 26.14 ± 3.92 | 0.697 |
| SBP (mmHg) | 139.02 ± 20.33 | 140.19 ± 21.56 | 141.31 ± 22.37 | 140.05 ± 22.93 | 144.76 ± 26.41 | 0.102 |
| DBP (mmHg) | 79.32 ± 12.15 | 78.20 ± 11.54 | 79.80 ± 12.75 | 80.09 ± 12.63 | 81.64 ± 15.08 | 0.084 |
| Comorbidity | ||||||
| Hypertension | 376 (35.9%) | 194 (40.4%) | 290 (38.3%) | 112 (39.7%) | 25 (42.4%) | 0.416 |
| Ischemic heart disease | 234 (22.4%) | 119 (24.8%) | 170 (22.5%) | 70 (24.8%) | 7 (11.9%) | 0.208 |
| Stroke | 139 (13.3%) | 64 (13.3%) | 109 (14.4%) | 30 (10.6%) | 8 (13.6%) | 0.641 |
| Diabetic neuropathy | 65 (6.2%) | 47 (9.8%) | 73 (9.6%) | 19 (6.7%) | 11 (18.6%) | 0.001 |
| Laboratory test | ||||||
| HbA1c (%) | 7.65 ± 1.87 | 7.96 ± 1.85 | 8.30 ± 2.05 | 8.40 ± 2.20 | 8.01 ± 2.05 | <0.001 |
| Fasting glucose (mg/dL) | 142.11 ± 54.96 | 144.54 ± 52.14 | 154.47 ± 62.63 | 153.02 ± 62.83 | 148.37 ± 64.99 | <0.001 |
| Triglyceride (mg/dL) | 150.33 ± 102.70 | 160.32 ± 130.04 | 161.75 ± 129.51 | 160.62 ± 138.91 | 158.69 ± 99.36 | 0.284 |
| Total cholesterol (mg/dL) | 170.36 ± 41.25 | 168.40 ± 46.84 | 171.55 ± 44.40 | 172.40 ± 46.86 | 179.27 ± 62.02 | 0.375 |
| LDL (mg/dL) | 99.43 ± 33.94 | 98.50 ± 36.38 | 99.94 ± 35.95 | 101.51 ± 36.32 | 107.46 ± 49.14 | 0.388 |
| HDL (mg/dL) | 46.90 ± 12.95 | 45.62 ± 12.23 | 45.57 ± 12.46 | 45.01 ± 12.68 | 48.32 ± 13.49 | 0.039 |
| Creatinine (mg/dL) | 1.31 ± 1.60 | 1.59 ± 1.95 | 1.68 ± 2.02 | 1.59 ± 1.72 | 1.93 ± 2.37 | <0.001 |
| ALT (U/L) | 23.37 ± 20.28 | 23.62 ± 25.94 | 23.84 ± 39.17 | 22.32 ± 21.39 | 20.64 ± 12.46 | 0.877 |
| Hemoglobin (g/dL) | 13.02 ± 1.87 | 12.58 ± 2.00 | 12.36 ± 2.10 | 12.38 ± 2.04 | 11.62 ± 2.04 | <0.001 |
| White blood cell (103/uL) | 7.32 ± 2.77 | 7.54 ± 2.95 | 7.83 ± 6.40 | 7.54 ± 2.48 | 7.24 ± 2.45 | 0.138 |
| Platelets (103/uL) | 212.06 ± 73.80 | 213.44 ± 72.56 | 221.54 ± 78.57 | 224.32 ± 66.05 | 220.17 ± 79.28 | 0.024 |
| HbA1c ≤ 6.7% (n = 799) | 6.7% < HbA1c ≤ 8.2% (n = 891) | 8.2% < HbA1c (n = 933) | p-Value | |
|---|---|---|---|---|
| Basic characteristics | ||||
| Gender | 0.309 | |||
| Female | 358 (44.8%) | 403 (45.2%) | 449 (48.1%) | |
| Male | 441 (55.2%) | 488 (54.8%) | 484 (51.9%) | |
| Age | 62.08 ± 12.80 | 64.26 ± 11.38 | 59.01 ± 13.03 | <0.001 |
| Height (cm) | 162.33 ± 9.00 | 162.56 ± 8.28 | 162.29 ± 9.02 | 0.786 |
| Weight (kg) | 66.84 ± 13.47 | 68.07 ± 13.78 | 68.71 ± 14.48 | 0.020 |
| Body mass index | 25.26 ± 4.07 | 25.67 ± 4.39 | 26.01 ± 4.74 | 0.002 |
| SBP (mmHg) | 138.39 ± 21.07 | 140.41 ± 20.78 | 141.36 ± 22.73 | 0.016 |
| DBP (mmHg) | 78.59 ± 12.01 | 78.80 ± 11.89 | 80.64 ± 12.97 | 0.001 |
| Comorbidity | ||||
| Hypertension | 311 (38.9%) | 341 (38.3%) | 345 (36.9%) | 0.682 |
| Ischemic heart disease | 187 (23.4%) | 236 (26.5%) | 177 (19.0%) | 0.001 |
| Stroke | 101 (12.6%) | 117 (13.1%) | 132 (14.1%) | 0.644 |
| Diabetic neuropathy | 61 (7.6%) | 63 (7.1%) | 91 (9.7%) | 0.090 |
| Laboratory test | ||||
| HbA1c (%) | 6.12 ± 0.43 | 7.41 ± 0.42 | 10.12 ± 1.69 | <0.001 |
| Fasting glucose (mg/dL) | 124.15 ± 33.53 | 138.02 ± 41.28 | 176.33 ± 74.30 | <0.001 |
| Triglyceride (mg/dL) | 134.53 ± 106.32 | 145.88 ± 86.40 | 186.12 ± 149.67 | <0.001 |
| Total cholesterol (mg/dL) | 164.57 ± 39.09 | 166.30 ± 41.32 | 180.32 ± 49.60 | <0.001 |
| LDL (mg/dL) | 96.19 ± 33.29 | 96.09 ± 32.47 | 106.46 ± 39.34 | <0.001 |
| HDL (mg/dL) | 46.54 ± 12.86 | 46.45 ± 12.65 | 45.42 ± 12.53 | 0.117 |
| Creatinine (mg/dL) | 1.62 ± 2.08 | 1.47 ± 1.70 | 1.45 ± 1.74 | 0.107 |
| ALT (U/L) | 22.53 ± 20.98 | 23.07 ± 18.91 | 24.39 ± 38.45 | 0.355 |
| Hemoglobin (g/dL) | 12.42 ± 2.06 | 12.64 ± 1.96 | 12.86 ± 2.00 | <0.001 |
| White blood cell (103/uL) | 7.26 ± 4.73 | 7.47 ± 4.66 | 7.82 ± 2.93 | 0.018 |
| Platelets (103/uL) | 203.70 ± 70.38 | 212.64 ± 69.60 | 231.26 ± 79.68 | <0.001 |
| Crude-HR (95% CI) | p-Value | Adjusted-HR (95% CI) | p-Value | |
|---|---|---|---|---|
| Initial grade | <0.001 | <0.001 | ||
| No DR | 1.00 | 1.00 | ||
| Mild NPDR | 2.00 (1.72–2.32) | <0.001 | 1.95 (1.68–2.27) | <0.001 |
| Moderate NPDR | 1.82 (1.58–2.09) | <0.001 | 1.73 (1.50–1.99) | <0.001 |
| Severe NPDR | 0.87 (0.69–1.09) | 0.223 | 0.82 (0.65–1.03) | 0.082 |
| Basic characteristics | ||||
| Gender | 0.019 | 0.042 | ||
| Female | 1.00 | 1.00 | ||
| Male | 1.15 (1.02–1.29) | 0.019 | 1.13 (1.00–1.27) | 0.042 |
| Age | 0.95 (0.90–1.01) | 0.076 | 0.97 (0.91–1.03) | 0.275 |
| Height | 1.06 (1.00–1.12) | 0.057 | 1.05 (0.99–1.12) | 0.095 |
| Weight | 1.02 (0.96–1.08) | 0.474 | 1.08 (0.97–1.22) | 0.169 |
| Body mass index | 1.00 (0.94–1.06) | 0.876 | 0.99 (0.94–1.05) | 0.802 |
| SBP | 1.03 (0.97–1.09) | 0.309 | 1.02 (0.96–1.08) | 0.542 |
| DBP | 1.04 (0.98–1.10) | 0.201 | 1.03 (0.97–1.10) | 0.287 |
| Comorbidity | ||||
| Hypertension | 1.11 (0.99–1.25) | 0.087 | 1.08 (0.96–1.22) | 0.197 |
| Ischemic heart disease | 1.06 (0.92–1.21) | 0.417 | 1.07 (0.94–1.23) | 0.319 |
| Stroke | 1.15 (0.97–1.35) | 0.104 | 1.11 (0.94–1.31) | 0.203 |
| Diabetic neuropathy | 1.23 (1.01–1.50) | 0.043 | 1.11 (0.91–1.36) | 0.311 |
| Laboratory test | ||||
| HbA1c | 1.13 (1.08–1.20) | <0.001 | 1.11 (1.05–1.17) | <0.001 |
| Fasting glucose | 1.04 (0.98–1.10) | 0.173 | 0.97 (0.91–1.03) | 0.302 |
| Triglyceride | 1.01 (0.95–1.06) | 0.784 | 0.97 (0.91–1.03) | 0.343 |
| Total cholesterol | 1.00 (0.94–1.06) | 0.966 | 0.98 (0.92–1.04) | 0.537 |
| LDL cholesterol | 1.01 (0.95–1.08) | 0.682 | 0.99 (0.93–1.06) | 0.821 |
| HDL cholesterol | 0.95 (0.90–1.01) | 0.101 | 0.98 (0.92–1.04) | 0.458 |
| Creatinine | 1.05 (1.00–1.11) | 0.061 | 1.02 (0.96–1.07) | 0.568 |
| ALT | 0.87 (0.79–0.96) | 0.005 | 0.86 (0.79–0.95) | 0.003 |
| Hemoglobin | 0.89 (0.84–0.94) | <0.001 | 0.91 (0.86–0.96) | 0.001 |
| White blood cell | 1.06 (1.01–1.11) | 0.022 | 1.04 (0.99–1.09) | 0.159 |
| Platelets | 1.06 (1.00–1.12) | 0.037 | 1.04 (0.98–1.10) | 0.199 |
| Crude-HR (95% CI) | p-Value | Adjusted-HR (95% CI) | p-Value | |
|---|---|---|---|---|
| Initial grade | <0.001 | <0.001 | ||
| No DR | 1.00 | 1.00 | ||
| Mild NPDR | 13.83 (6.19–30.93) | <0.001 | 13.58 (6.07–30.39) | <0.001 |
| Moderate NPDR | 25.06 (11.61–54.08) | <0.001 | 23.09 (10.68–49.91) | <0.001 |
| Severe NPDR | 62.29 (28.87–134.40) | <0.001 | 55.24 (25.54–119.46) | <0.001 |
| Basic characteristics | ||||
| Gender | 0.422 | 0.750 | ||
| Female | 1.00 | 1.00 | ||
| Male | 1.11 (0.86–1.44) | 0.422 | 0.96 (0.74–1.25) | 0.750 |
| Age | 0.67 (0.60–0.76) | <0.001 | 0.73 (0.63–0.84) | <0.001 |
| Height | 1.04 (0.92–1.19) | 0.522 | 0.97 (0.84–1.12) | 0.671 |
| Weight | 0.98 (0.86–1.12) | 0.789 | 0.93 (0.71–1.20) | 0.569 |
| Body mass index | 0.95 (0.83–1.09) | 0.470 | 0.91 (0.79–1.03) | 0.146 |
| SBP | 1.10 (0.97–1.25) | 0.137 | 1.11 (0.98–1.25) | 0.111 |
| DBP | 1.23 (1.08–1.40) | 0.001 | 1.15 (1.01–1.31) | 0.038 |
| Comorbidity | ||||
| Hypertension | 1.18 (0.91–1.54) | 0.210 | 1.11 (0.86–1.45) | 0.421 |
| Ischemic heart disease | 1.13 (0.84–1.52) | 0.414 | 1.11 (0.82–1.50) | 0.498 |
| Stroke | 1.61 (1.16–2.25) | 0.005 | 1.72 (1.23–2.40) | 0.001 |
| Diabetic neuropathy | 1.45 (0.95–2.21) | 0.087 | 1.15 (0.75–1.78) | 0.519 |
| Laboratory test | ||||
| HbA1c | 1.30 (1.16–1.46) | <0.001 | 1.09 (0.97–1.22) | 0.164 |
| Fasting glucose | 1.13 (1.01–1.26) | 0.032 | 0.93 (0.82–1.06) | 0.263 |
| Triglyceride | 1.05 (0.94–1.17) | 0.397 | 1.01 (0.91–1.12) | 0.878 |
| Total cholesterol | 1.01 (0.88–1.16) | 0.916 | 0.93 (0.81–1.07) | 0.305 |
| LDL | 1.00 (0.87–1.14) | 0.963 | 0.89 (0.78–1.03) | 0.120 |
| HDL | 0.84 (0.74–0.97) | 0.017 | 0.88 (0.76–1.01) | 0.069 |
| Creatinine | 1.17 (1.05–1.29) | 0.003 | 1.11 (0.99–1.23) | 0.062 |
| ALT | 0.89 (0.72–1.10) | 0.285 | 0.92 (0.76–1.12) | 0.425 |
| Hemoglobin | 0.74 (0.65–0.84) | <0.001 | 0.84 (0.74–0.96) | 0.008 |
| White blood cell | 1.08 (0.97–1.21) | 0.148 | 1.03 (0.89–1.19) | 0.686 |
| Platelets | 1.14 (1.01–1.28) | 0.033 | 1.05 (0.92–1.20) | 0.493 |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Lee, C.-C.; Hsing, S.-C.; Lin, Y.-T.; Lin, C.; Chen, J.-T.; Chen, Y.-H.; Fang, W.-H. The Importance of Close Follow-Up in Patients with Early-Grade Diabetic Retinopathy: A Taiwan Population-Based Study Grading via Deep Learning Model. Int. J. Environ. Res. Public Health 2021, 18, 9768. https://doi.org/10.3390/ijerph18189768
Lee C-C, Hsing S-C, Lin Y-T, Lin C, Chen J-T, Chen Y-H, Fang W-H. The Importance of Close Follow-Up in Patients with Early-Grade Diabetic Retinopathy: A Taiwan Population-Based Study Grading via Deep Learning Model. International Journal of Environmental Research and Public Health. 2021; 18(18):9768. https://doi.org/10.3390/ijerph18189768
Chicago/Turabian StyleLee, Chia-Cheng, Shi-Chue Hsing, Yu-Ting Lin, Chin Lin, Jiann-Torng Chen, Yi-Hao Chen, and Wen-Hui Fang. 2021. "The Importance of Close Follow-Up in Patients with Early-Grade Diabetic Retinopathy: A Taiwan Population-Based Study Grading via Deep Learning Model" International Journal of Environmental Research and Public Health 18, no. 18: 9768. https://doi.org/10.3390/ijerph18189768
APA StyleLee, C.-C., Hsing, S.-C., Lin, Y.-T., Lin, C., Chen, J.-T., Chen, Y.-H., & Fang, W.-H. (2021). The Importance of Close Follow-Up in Patients with Early-Grade Diabetic Retinopathy: A Taiwan Population-Based Study Grading via Deep Learning Model. International Journal of Environmental Research and Public Health, 18(18), 9768. https://doi.org/10.3390/ijerph18189768









