School Parks as a Community Health Resource: Use of Joint-Use Parks by Children before and during COVID-19 Pandemic
Abstract
:1. Introduction
2. Materials and Methods
2.1. Study Setting
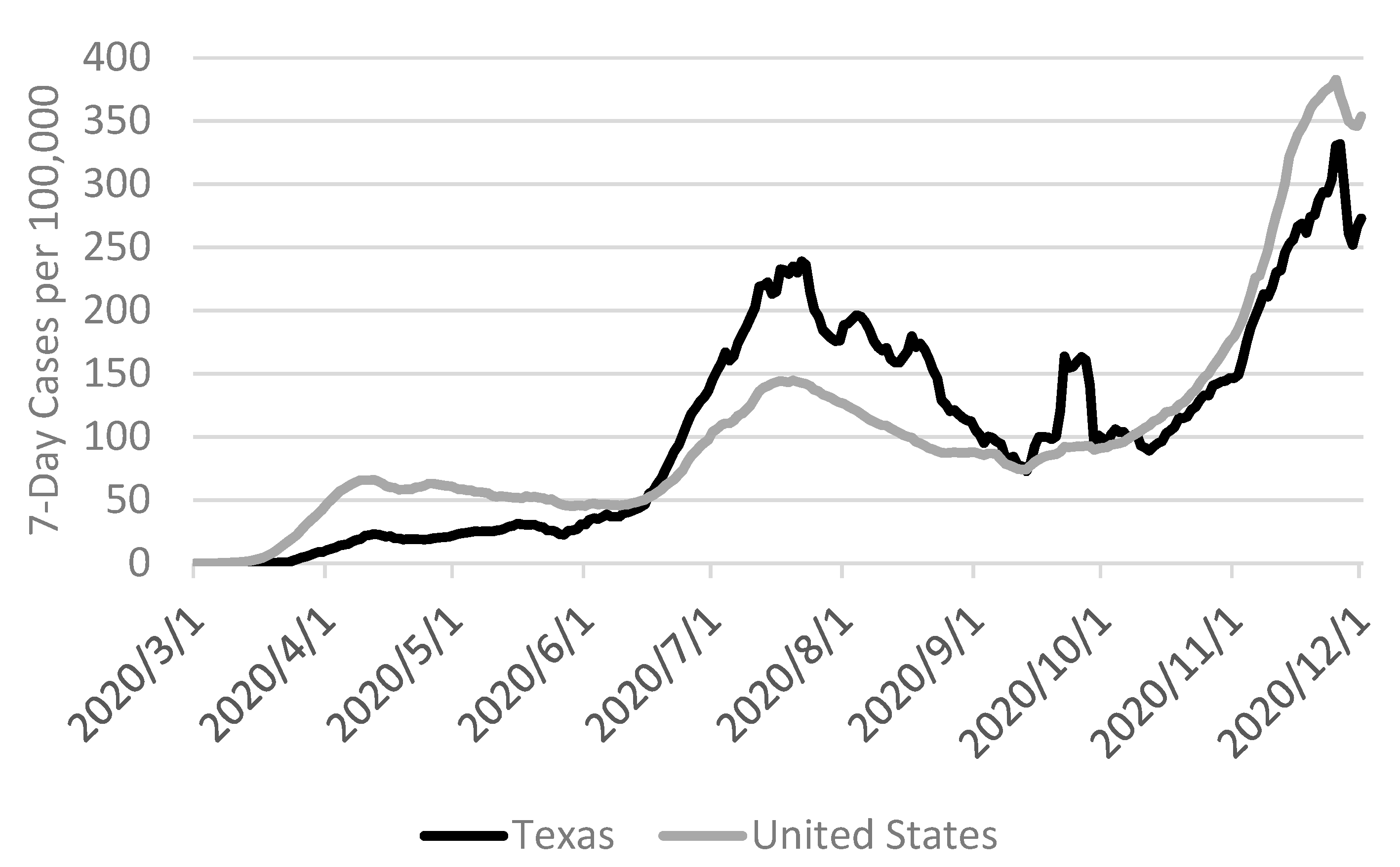
2.2. COVID-19 Pandemic in Texas
2.3. Measurement of Park Use by Children
2.4. Measurement of Variables That May Impact Park Use by Children
2.5. Measurement of COVID-19 Protective Health Behaviors by Children
2.6. Statistical Analyses
3. Results
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
Appendix A

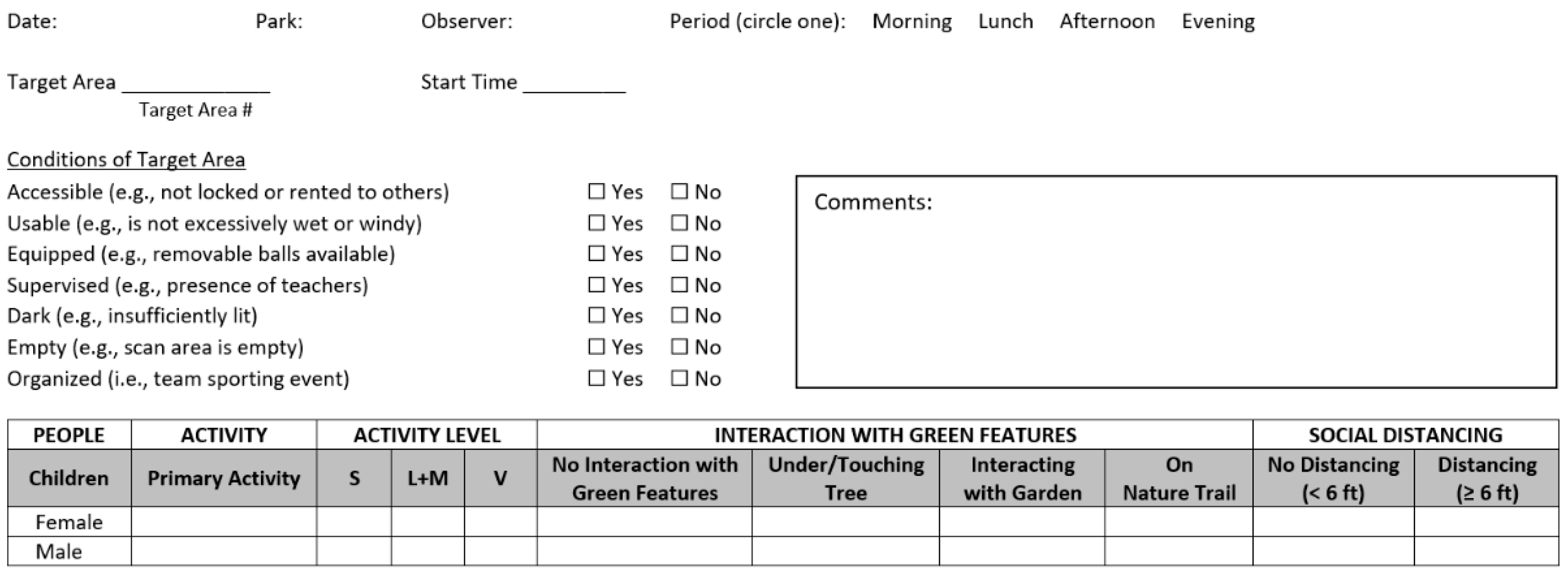
References
- Dattner, I.; Goldberg, Y.; Katriel, G.; Yaari, R.; Gal, N.; Miron, Y.; Ziv, A.; Sheffer, R.; Hamo, Y.; Huppert, A. The role of children in the spread of COVID-19: Using household data from Bnei Brak, Israel, to estimate the relative susceptibility and infectivity of children. PLoS Comput. Biol. 2021, 17, e1008559. [Google Scholar] [CrossRef] [PubMed]
- US Centers for Disease Control and Prevention. Demographic Trends of COVID-19 Cases and Deaths in the US Reported to CDC. Available online: https://covid.cdc.gov/covid-data-tracker/#demographics (accessed on 13 July 2021).
- Deolmi, M.; Pisani, F. Psychological and psychiatric impact of COVID-19 pandemic among children and adolescents. Acta Bio Med. Atenei Parm. 2020, 91, e2020149. [Google Scholar] [CrossRef]
- Nearchou, F.; Flinn, C.; Niland, R.; Subramaniam, S.S.; Hennessy, E. Exploring the impact of CoViD-19 on mental health outcomes in children and adolescents: A systematic review. Int. J. Environ. Res. Public Health 2020, 17, 8479. [Google Scholar] [CrossRef]
- Ravens-Sieberer, U.; Kaman, A.; Otto, C.; Adedeji, A.; Devine, J.; Erhart, M.; Napp, A.-K.; Becker, M.; Blanck-Stellmacher, U.; Löffler, C. Mental health and quality of life in children and adolescents during the COVID-19 pandemic—results of the COPSY study. Dtsch. Ärzteblatt Int. 2020, 117, 828. [Google Scholar] [CrossRef]
- Ravens-Sieberer, U.; Kaman, A.; Erhart, M.; Devine, J.; Schlack, R.; Otto, C. Impact of the COVID-19 pandemic on quality of life and mental health in children and adolescents in Germany. Eur. Child Adolesc. Psychiatry 2021, 30, 1–11. [Google Scholar] [CrossRef]
- Aguilar-Farias, N.; Toledo-Vargas, M.; Miranda-Marquez, S.; Cortinez-O’Ryan, A.; Cristi-Montero, C.; Rodriguez-Rodriguez, F.; Martino-Fuentealba, P.; Okely, A.D.; del Pozo Cruz, B. Sociodemographic Predictors of Changes in Physical Activity, Screen Time, and Sleep among Toddlers and Preschoolers in Chile during the COVID-19 Pandemic. Int. J. Environ. Res. Public Health 2021, 18, 176. [Google Scholar] [CrossRef]
- Bates, L.C.; Zieff, G.; Stanford, K.; Moore, J.B.; Kerr, Z.Y.; Hanson, E.D.; Barone Gibbs, B.; Kline, C.E.; Stoner, L. COVID-19 Impact on behaviors across the 24-hour day in children and adolescents: Physical activity, sedentary behavior, and sleep. Children 2020, 7, 138. [Google Scholar] [CrossRef]
- Dunton, G.F.; Do, B.; Wang, S.D. Early effects of the COVID-19 pandemic on physical activity and sedentary behavior in children living in the US. BMC Public Health 2020, 20, 1351. [Google Scholar] [CrossRef]
- López-Bueno, R.; López-Sánchez, G.F.; Casajús, J.A.; Calatayud, J.; Gil-Salmerón, A.; Grabovac, I.; Tully, M.A.; Smith, L. Health-related behaviors among school-aged children and adolescents during the Spanish Covid-19 confinement. Front. Pediatrics 2020, 8, 573. [Google Scholar] [CrossRef] [PubMed]
- Medrano, M.; Cadenas-Sanchez, C.; Oses, M.; Arenaza, L.; Amasene, M.; Labayen, I. Changes in lifestyle behaviours during the COVID-19 confinement in Spanish children: A longitudinal analysis from the MUGI project. Pediatric Obes. 2021, 16, e12731. [Google Scholar] [CrossRef]
- Mitra, R.; Moore, S.A.; Gillespie, M.; Faulkner, G.; Vanderloo, L.M.; Chulak-Bozzer, T.; Rhodes, R.E.; Brussoni, M.; Tremblay, M.S. Healthy movement behaviours in children and youth during the COVID-19 pandemic: Exploring the role of the neighbourhood environment. Health Place 2020, 65, 102418. [Google Scholar] [CrossRef]
- Moore, S.A.; Faulkner, G.; Rhodes, R.E.; Brussoni, M.; Chulak-Bozzer, T.; Ferguson, L.J.; Mitra, R.; O’Reilly, N.; Spence, J.C.; Vanderloo, L.M. Impact of the COVID-19 virus outbreak on movement and play behaviours of Canadian children and youth: A national survey. Int. J. Behav. Nutr. Phys. Act. 2020, 17, 85. [Google Scholar] [CrossRef] [PubMed]
- Xiang, M.; Zhang, Z.; Kuwahara, K. Impact of COVID-19 pandemic on children and adolescents’ lifestyle behavior larger than expected. Prog. Cardiovasc. Dis. 2020, 63, 531–532. [Google Scholar] [CrossRef]
- Razani, N.; Radhakrishna, R.; Chan, C. Public lands are essential to public health during a pandemic. Pediatrics 2020, 146, e20201271. [Google Scholar] [CrossRef] [PubMed]
- Slater, S.J.; Christiana, R.W.; Gustat, J. Peer Reviewed: Recommendations for keeping parks and green space accessible for mental and physical health during COVID-19 and other pandemics. Prev. Chronic Dis. 2020, 17, E59. [Google Scholar] [CrossRef]
- Bulfone, T.C.; Malekinejad, M.; Rutherford, G.W.; Razani, N. Outdoor Transmission of SARS-CoV-2 and Other Respiratory Viruses, a Systematic Review. J. Infect. Dis. 2020, 223, 550–561. [Google Scholar] [CrossRef]
- McCormick, R. Does access to green space impact the mental well-being of children: A systematic review. J. Pediatric Nurs. 2017, 37, 3–7. [Google Scholar] [CrossRef] [PubMed]
- Evenson, K.R.; Jones, S.A.; Holliday, K.M.; Cohen, D.A.; McKenzie, T.L. Park characteristics, use, and physical activity: A review of studies using SOPARC (System for Observing Play and Recreation in Communities). Prev. Med. 2016, 86, 153–166. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Lanza, K.; Stone Jr, B.; Haardörfer, R. How race, ethnicity, and income moderate the relationship between urban vegetation and physical activity in the United States. Prev. Med. 2019, 121, 55–61. [Google Scholar] [CrossRef] [PubMed]
- Smith, M.; Hosking, J.; Woodward, A.; Witten, K.; MacMillan, A.; Field, A.; Baas, P.; Mackie, H. Systematic literature review of built environment effects on physical activity and active transport–an update and new findings on health equity. Int. J. Behav. Nutr. Phys. Act. 2017, 14, 158. [Google Scholar] [CrossRef]
- Michael & Susan Dell Center for Healthy Living. SPAN Data Explorer: Meets Recommended Physical Activity Guidelines. Available online: https://span-interactive.sph.uth.edu/ (accessed on 20 August 2021).
- McCormack, G.R.; Doyle-Baker, P.K.; Petersen, J.A.; Ghoneim, D. Parent anxiety and perceptions of their child’s physical activity and sedentary behaviour during the COVID-19 pandemic in Canada. Prev. Med. Rep. 2020, 20, 101275. [Google Scholar] [CrossRef] [PubMed]
- Choi, B.C.; Pak, A.W. Peer reviewed: A catalog of biases in questionnaires. Prev. Chronic Dis. 2005, 2, A13. Available online: https://www.ncbi.nlm.nih.gov/pubmed/15670466 (accessed on 20 June 2021). [PubMed]
- Clark, C.; Davila, A.; Regis, M.; Kraus, S. Predictors of COVID-19 voluntary compliance behaviors: An international investigation. Glob. Transit. 2020, 2, 76–82. [Google Scholar] [CrossRef] [PubMed]
- Hornik, R.; Kikut, A.; Jesch, E.; Woko, C.; Siegel, L.; Kim, K. Association of COVID-19 misinformation with face mask wearing and social distancing in a nationally representative US sample. Health Commun. 2021, 36, 6–14. [Google Scholar] [CrossRef]
- Hutchins, H.J.; Wolff, B.; Leeb, R.; Ko, J.Y.; Odom, E.; Willey, J.; Friedman, A.; Bitsko, R.H. COVID-19 mitigation behaviors by age group—United States, April–June 2020. Morb. Mortal. Wkly. Rep. 2020, 69, 1584. [Google Scholar] [CrossRef]
- Lüdecke, D.; von dem Knesebeck, O. Protective behavior in course of the COVID-19 outbreak—survey results from Germany. Front. Public Health 2020, 8, 567. [Google Scholar] [CrossRef] [PubMed]
- Burford, K.; Dooley, E.; Lanza, K.; Knell, G. Associations of Urbanicity and Sociodemographic Characteristics with Protective Health Behaviors and Reasons for Leaving the Home During COVID-19. Health Psychol. Bull. 2020, 4, 53–63. [Google Scholar] [CrossRef]
- Oosterhoff, B.; Palmer, C.A.; Wilson, J.; Shook, N. Adolescents’ motivations to engage in social distancing during the COVID-19 pandemic: Associations with mental and social health. J. Adolesc. Health 2020, 67, 179–185. [Google Scholar] [CrossRef]
- Dunn, M.R.; DeJonckheere, M.; Schuiteman, S.; Strome, A.; Herbert, K.; Waselewski, M.; Chang, T. “Stay home so this can be over:” a national study of youth perspectives on social distancing during the COVID-19 pandemic. Prev. Med. Rep. 2021, 22, 101355. [Google Scholar] [CrossRef]
- Haischer, M.H.; Beilfuss, R.; Hart, M.R.; Opielinski, L.; Wrucke, D.; Zirgaitis, G.; Uhrich, T.D.; Hunter, S.K. Who is wearing a mask? Gender-, age-, and location-related differences during the COVID-19 pandemic. PLoS ONE 2020, 15, e0240785. [Google Scholar] [CrossRef]
- Newsgd.com. Wearing Masks in Public Compulsory in Guangdong. Available online: http://www.newsgd.com/news/exclusive/content/2020-01/27/content_190144095.htm (accessed on 9 July 2021).
- Cable News Network. Face Masks are Made Mandatory in Wuhan. Available online: https://edition.cnn.com/asia/live-news/wuhan-coronavirus-china-intl-hnk/h_b6ff0d4bd2e53b2ee9e5ca768e231811 (accessed on 9 July 2021).
- Qin, Z.; Shi, L.; Xue, Y.; Lin, H.; Zhang, J.; Liang, P.; Lu, Z.; Wu, M.; Chen, Y.; Zheng, X. Prevalence and Risk Factors Associated with Self-reported Psychological Distress Among Children and Adolescents During the COVID-19 Pandemic in China. JAMA Netw. Open 2021, 4, e2035487. [Google Scholar] [CrossRef]
- Chen, X.; Ran, L.; Liu, Q.; Hu, Q.; Du, X.; Tan, X. Hand hygiene, mask-wearing behaviors and its associated factors during the COVID-19 epidemic: A cross-sectional study among primary school students in Wuhan, China. Int. J. Environ. Res. Public Health 2020, 17, 2893. [Google Scholar] [CrossRef]
- Szeszulski, J.; Lanza, K.; Dooley, E.E.; Johnson, A.M.; Knell, G.; Walker, T.J.; Craig, D.W.; Robertson, M.C.; Salvo, D.; Kohl, H.W. Y-PATHS: A Conceptual Framework for Classifying the Timing, How, and Setting of Youth Physical Activity. J. Phys. Act. Health 2021, 18, 310–317. [Google Scholar] [CrossRef]
- Lanza, K.; Alcazar, M.; Hoelscher, D.M.; Kohl, H.W. Effects of trees, gardens, and nature trails on heat index and child health: Design and methods of the Green Schoolyards Project. BMC Public Health 2021, 21, 98. [Google Scholar] [CrossRef]
- Nowak, D.J.; Maco, S.; Binkley, M. i-Tree: Global tools to assess tree benefits and risks to improve forest management. Arboric. Consultant. 2018, 51, 10–13. [Google Scholar]
- City of Austin. Cities Connecting Children to Nature: GIS Gap Analysis. Available online: https://austin.maps.arcgis.com/apps/MapJournal/index.html?appid=f77ea201c8d04425a1942f5e5f234a6c (accessed on 24 July 2021).
- City of Austin. CCCN_cityofaustinparks. Available online: https://www.arcgis.com/home/item.html?id=3701aa78b77145e68c7207a7832683e7 (accessed on 24 June 2021).
- US Federal Emergency Management Agency. COVID-19 Emergency Declaration. Available online: https://www.fema.gov/press-release/20210318/covid-19-emergency-declaration (accessed on 20 August 2021).
- US Centers for Disease Control and Prevention. Trends in Number of COVID-19 Cases and Deaths in the US Reported to CDC, by State/Territory. Available online: https://covid.cdc.gov/covid-data-tracker/#trends_dailycases (accessed on 20 August 2021).
- City of Austin. Order No. 20200815-019 Stay Home, Mask, and Otherwise Be Safe. Available online: http://austintexas.gov/sites/default/files/files/Health/Order%20No.%2020200814-019%20Stay%20Home%2C%20Mask%2C%20And%20Otherwise%20Be%20Safe.pdf (accessed on 24 June 2021).
- Austin Independent School District. Twitter @AustinISD. Available online: https://twitter.com/austinisd/status/1254899918319300610 (accessed on 23 June 2021).
- McKenzie, T.L.; Cohen, D.A.; Sehgal, A.; Williamson, S.; Golinelli, D. System for Observing Play and Recreation in Communities (SOPARC): Reliability and feasibility measures. J. Phys. Act. Health 2006, 3, S208–S222. [Google Scholar] [CrossRef] [PubMed]
- Huang, J.-H.; Hipp, J.A.; Marquet, O.; Alberico, C.; Fry, D.; Mazak, E.; Lovasi, G.S.; Robinson, W.R.; Floyd, M.F. Neighborhood characteristics associated with park use and park-based physical activity among children in low-income diverse neighborhoods in New York City. Prev. Med. 2020, 131, 105948. [Google Scholar] [CrossRef] [PubMed]
- Edwards, N.M.; Myer, G.D.; Kalkwarf, H.J.; Woo, J.G.; Khoury, P.R.; Hewett, T.E.; Daniels, S.R. Outdoor temperature, precipitation, and wind speed affect physical activity levels in children: A longitudinal cohort study. J. Phys. Act. Health 2015, 12, 1074–1081. [Google Scholar] [CrossRef] [Green Version]
- Kabisch, N.; Kraemer, R. Physical activity patterns in two differently characterised urban parks under conditions of summer heat. Environ. Sci. Policy 2020, 107, 56–65. [Google Scholar] [CrossRef]
- Nasir, R.A.; Ahmad, S.S.; Ahmed, A.Z. Physical activity and human comfort correlation in an urban park in hot and humid conditions. Procedia-Soc. Behav. Sci. 2013, 105, 598–609. [Google Scholar] [CrossRef] [Green Version]
- Matias, M.; Lopes, A. Surface Radiation Balance of Urban Materials and Their Impact on Air Temperature of an Urban Canyon in Lisbon, Portugal. Appl. Sci. 2020, 10, 2193. [Google Scholar] [CrossRef] [Green Version]
- Mallen, E.; Bakin, J.; Stone, B.; Sivakumar, R.; Lanza, K. Thermal impacts of built and vegetated environments on local microclimates in an Urban University campus. Urban Clim. 2020, 32, 100640. [Google Scholar] [CrossRef]
- US National Weather Service. The Heat Index Equation. Available online: https://www.wpc.ncep.noaa.gov/html/heatindex_equation.shtml (accessed on 20 June 2021).
- Austin Independent School District. Open for Learning Plans for the 2020–21 School Year (1 September 2020—Version Three). Available online: https://www.austinisd.org/sites/default/files/dept/openforlearning/docs/V3_ENGLISH_Open%20for%20Learning_090120_final.pdf (accessed on 20 June 2021).
- Austin Independent School District. Open for Learning Plans for the 2020–21 School Year (11 November 2020—Version 4.2). Available online: https://www.austinisd.org/sites/default/files/dept/communications/Open%20for%20Learning/3_V%204.2%20Open%20for%20Learning_Revised%20111120.pdf (accessed on 20 June 2021).
- Hilbe, J.M. Negative Binomial Regression; Cambridge University Press: Cambridge, UK, 2011. [Google Scholar]
- McHugh, M.L. Interrater reliability: The kappa statistic. Biochem. Med. 2012, 22, 276–282. [Google Scholar] [CrossRef]
- Hamidi, S.; Zandiatashbar, A. Compact development and adherence to stay-at-home order during the COVID-19 pandemic: A longitudinal investigation in the United States. Landsc. Urban Plan. 2021, 205, 103952. [Google Scholar] [CrossRef] [PubMed]
- Riazi, N.A.; Wunderlich, K.; Gierc, M.; Brussoni, M.; Moore, S.A.; Tremblay, M.S.; Faulkner, G. “You Can’t Go to the Park, You Can’t Go Here, You Can’t Go There”: Exploring Parental Experiences of COVID-19 and Its Impact on Their Children’s Movement Behaviours. Children 2021, 8, 219. [Google Scholar] [CrossRef]
- KXAN. Park Usage Skyrockets During Pandemic, New Art Installation Encourages Social Distancing. Available online: https://www.kxan.com/news/local/austin/park-usage-skyrockets-during-pandemic-new-art-installation-encourages-social-distancing/ (accessed on 22 August 2021).
- Amplify Austin. The Trail Foundation. Available online: https://www.amplifyatx.org/organizations/ttf (accessed on 22 August 2021).
- Smart, N.R.; Horwell, C.J.; Smart, T.S.; Galea, K.S. Assessment of the wearability of facemasks against air pollution in primary school-aged children in London. Int. J. Environ. Res. Public Health 2020, 17, 3935. [Google Scholar] [CrossRef]
- World Health Organization. Coronavirus Disease (COVID-19): Children and Masks. Available online: https://www.who.int/emergencies/diseases/novel-coronavirus-2019/question-and-answers-hub/q-a-detail/q-a-children-and-masks-related-to-covid-19 (accessed on 22 August 2021).
- Huggins, J.C. A cartographic perspective on the correlation between redlining and public health in Austin, Texas–1951. Cityscape 2017, 19, 267–280. [Google Scholar]
- Hoffman, J.S.; Shandas, V.; Pendleton, N. The Effects of Historical Housing Policies on Resident Exposure to Intra-Urban Heat: A Study of 108 US Urban Areas. Climate 2020, 8, 12. [Google Scholar] [CrossRef] [Green Version]
- Mathiarasan, S.; Hüls, A. Impact of Environmental Injustice on Children’s Health—Interaction between Air Pollution and Socioeconomic Status. Int. J. Environ. Res. Public Health 2021, 18, 795. [Google Scholar] [CrossRef]
- Benfer, E.A.; Mohapatra, S.; Wiley, L.F.; Yearby, R. Health justice strategies to combat the pandemic: Eliminating discrimination, poverty, and health inequity during and after COVID-19. Yale J. Health Pol’y L. & Ethics 2020, 19, 122–171. [Google Scholar] [CrossRef]
- US Centers for Disease Control and Prevention. Considerations for Youth Sports. Available online: https://search.bvsalud.org/global-literature-on-novel-coronavirus-2019-ncov/resource/en/ppcovidwho-2595 (accessed on 22 July 2021).
- Shoari, N.; Ezzati, M.; Baumgartner, J.; Malacarne, D.; Fecht, D. Accessibility and allocation of public parks and gardens in England and Wales: A COVID-19 social distancing perspective. PLoS ONE 2020, 15, e0241102. [Google Scholar] [CrossRef] [PubMed]
- Mckenzie, T.L.; Cohen, D.A. SOPARC (System for Observing Play and Recreation in Communities) Description and Procedures Manual. Active Living Research. Available online: https://activelivingresearch.org/sites/activelivingresearch.org/files/SOPARC_Protocols.pdf (accessed on 22 July 2021).
- Marquet, O.; Hipp, J.A.; Alberico, C.; Huang, J.-H.; Fry, D.; Mazak, E.; Lovasi, G.S.; Floyd, M.F. Use of SOPARC to assess physical activity in parks: Do race/ethnicity, contextual conditions, and settings of the target area, affect reliability? BMC Public Health 2019, 19, 1730. [Google Scholar] [CrossRef] [PubMed] [Green Version]

| Before COVID-19 | During COVID-19 | |||
|---|---|---|---|---|
| Variables 1 | Mean (Std. Dev.) | % of Total (Count) | Mean (Std. Dev.) | % of Total (Count) |
| Female children (#) | 5.76 (4.77) | 36.6% (311) | 3.02 (3.17) | 45.2% (163) |
| Male children (#) | 9.96 (15.44) | 63.4% (538) | 3.67 (3.59) | 54.8% (198) |
| Female children—sedentary (#) | 1.81 (2.53) | 31.5% (98) | 0.83 (1.49) | 27.6% (45) |
| Female children—light-to-moderate physical activity (#) | 3.15 (2.85) | 54.7% (170) | 1.44 (1.81) | 47.9% (78) |
| Female children—vigorous physical activity (#) | 0.80 (1.63) | 13.8% (43) | 0.74 (1.42) | 24.5% (40) |
| Male children—sedentary (#) | 2.44 (4.31) | 24.5% (132) | 0.93 (1.30) | 25.3% (50) |
| Male children—light-to-moderate physical activity (#) | 5.54 (9.97) | 55.6% (299) | 1.59 (1.79) | 43.4% (86) |
| Male children—vigorous physical activity (#) | 1.98 (4.28) | 19.9% (107) | 1.15 (2.10) | 31.3% (62) |
| Weekend (1 = weekend day) | 0.17 (0.38) | 16.7%(3) | 0.17 (0.38) | 16.7% (3) |
| Rain during observation (1 = rain) | 0.02 (0.14) | 1.90% (1) | 0.06 (0.23) | 5.60% (3) |
| Average heat index 16:00–18:30 (°C) | 30.46 (8.15) | – | 26.72 (5.34) | – |
| Variables | (1) Female Users | (2) Male Users | (3) Female PA | (4) Male PA |
|---|---|---|---|---|
| Pandemic (1 = during pandemic) 1 | 0.54 ** (0.37–0.80) | 0.38 *** (0.24–0.61) | 0.58 ** (0.41–0.84) | 0.40 *** (0.25–0.64) |
| Weekend (1 = weekend day) 1 | 1.15 (0.70–1.90) | 0.76 (0.40–1.46) | 1.00 (0.63–1.61) | 0.82 (0.42–1.57) |
| Rain during observation (1 = rain) 1 | 0.06 * (0.01–0.54) | 0.20 * (0.05–0.81) | 0.00 (0.00–0.00) 2 | 0.16 * (0.03–0.79) |
| Average heat index 16:00–18:30 (°C) 1 | 1.00 (0.99–1.02) | 0.99 (0.97–1.01) | 1.00 (0.98–1.01) | 0.99 (0.97–1.01) |
| Intervention park (1 = intervention) | 0.79 (0.50–1.26) | 0.86 (0.47–1.58) | 0.83 (0.53–1.29) | 0.82 (0.45–1.51) |
| Low-green park (1 = low-green) | 1.21 (0.77–1.89) | 1.38 (0.76–2.50) | 1.70 * (1.12–2.57) | 1.90 * (1.06–3.40) |
| Lnalpha | 0.68 (0.41–1.02) | 1.20 (0.87–1.66) | 0.47 ** (0.28–0.79) | 1.13 (0.80–1.59) |
| Constant | 5.35 * (1.35–21.23) | 17.98 *** (3.72–86.97) | 3.68 * (1.01–13.36) | 14.23 *** (2.96–68.44) |
| N | 108 | 108 | 108 | 108 |
| Variables | % of Total (Count) |
|---|---|
| Female children who maintained social distance (≥ six feet) | 39.4% (61) |
| Male children who maintained social distance (≥ six feet) | 26.4% (47) |
| Observations where all children wore face coverings | 6.0% (14) |
| Observations where some children wore face coverings | 2.2% (5) |
| Observations where no children wore face coverings | 91.8% (213) |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Lanza, K.; Durand, C.P.; Alcazar, M.; Ehlers, S.; Zhang, K.; Kohl, H.W., III. School Parks as a Community Health Resource: Use of Joint-Use Parks by Children before and during COVID-19 Pandemic. Int. J. Environ. Res. Public Health 2021, 18, 9237. https://doi.org/10.3390/ijerph18179237
Lanza K, Durand CP, Alcazar M, Ehlers S, Zhang K, Kohl HW III. School Parks as a Community Health Resource: Use of Joint-Use Parks by Children before and during COVID-19 Pandemic. International Journal of Environmental Research and Public Health. 2021; 18(17):9237. https://doi.org/10.3390/ijerph18179237
Chicago/Turabian StyleLanza, Kevin, Casey P. Durand, Melody Alcazar, Sierra Ehlers, Kai Zhang, and Harold W. Kohl, III. 2021. "School Parks as a Community Health Resource: Use of Joint-Use Parks by Children before and during COVID-19 Pandemic" International Journal of Environmental Research and Public Health 18, no. 17: 9237. https://doi.org/10.3390/ijerph18179237
APA StyleLanza, K., Durand, C. P., Alcazar, M., Ehlers, S., Zhang, K., & Kohl, H. W., III. (2021). School Parks as a Community Health Resource: Use of Joint-Use Parks by Children before and during COVID-19 Pandemic. International Journal of Environmental Research and Public Health, 18(17), 9237. https://doi.org/10.3390/ijerph18179237







