COVID-19 and Unmet Healthcare Needs of Older People: Did Inequity Arise in Europe?
Abstract
:1. Introduction
2. Data and Methods
2.1. Data
2.2. Methods
2.3. Definition of Variables
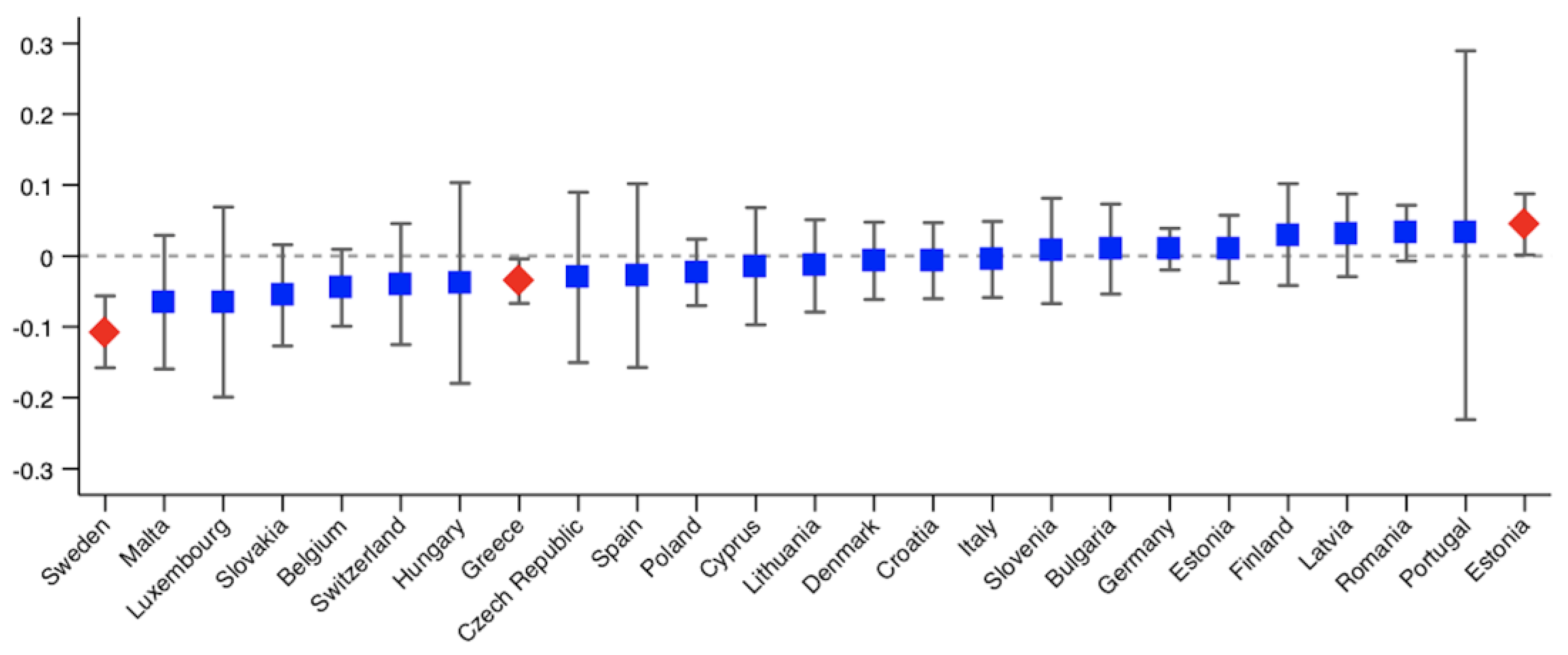
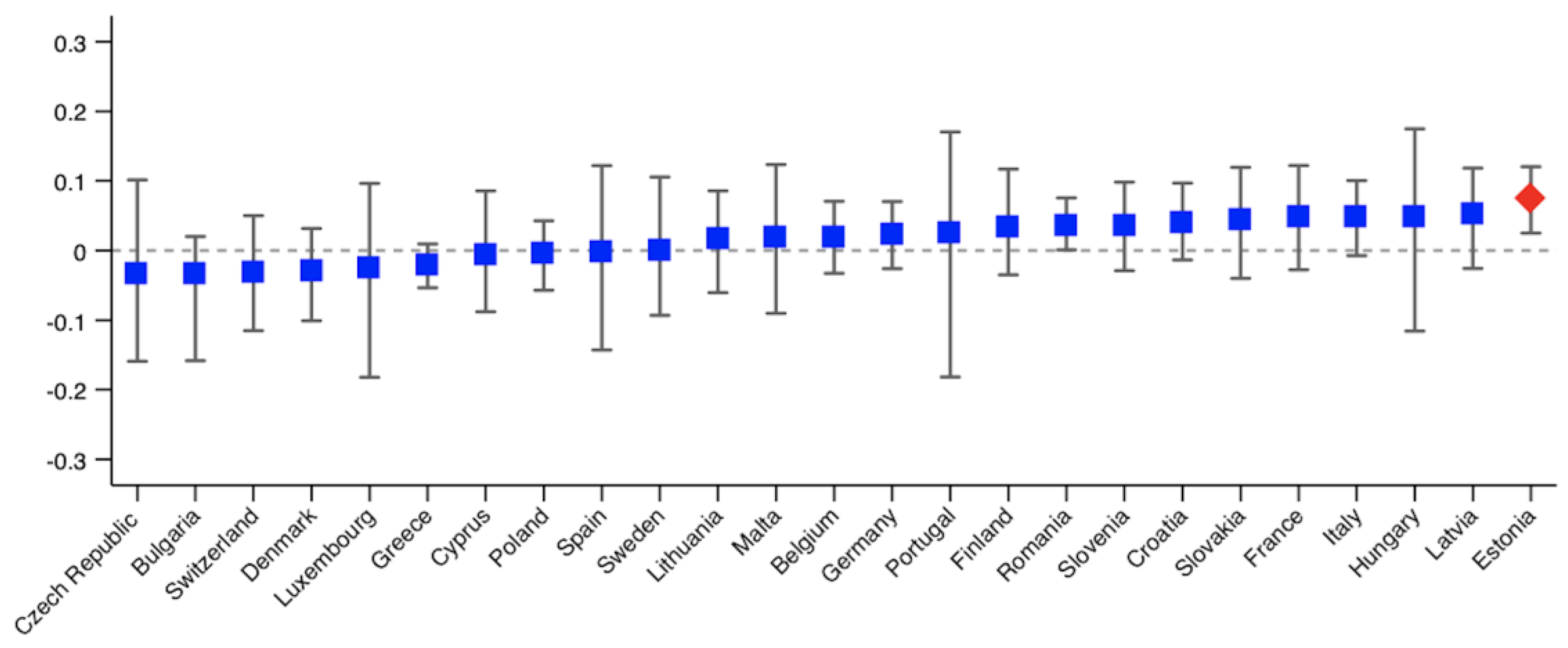
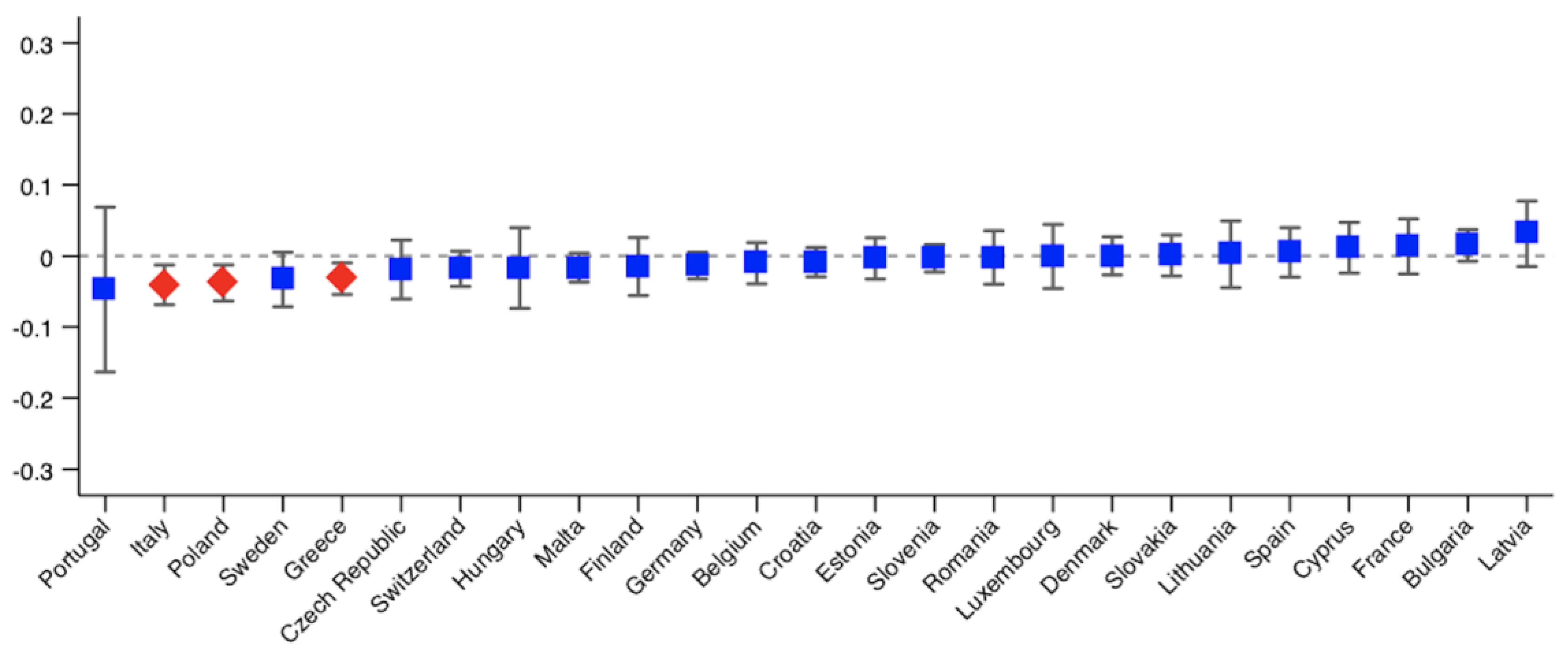
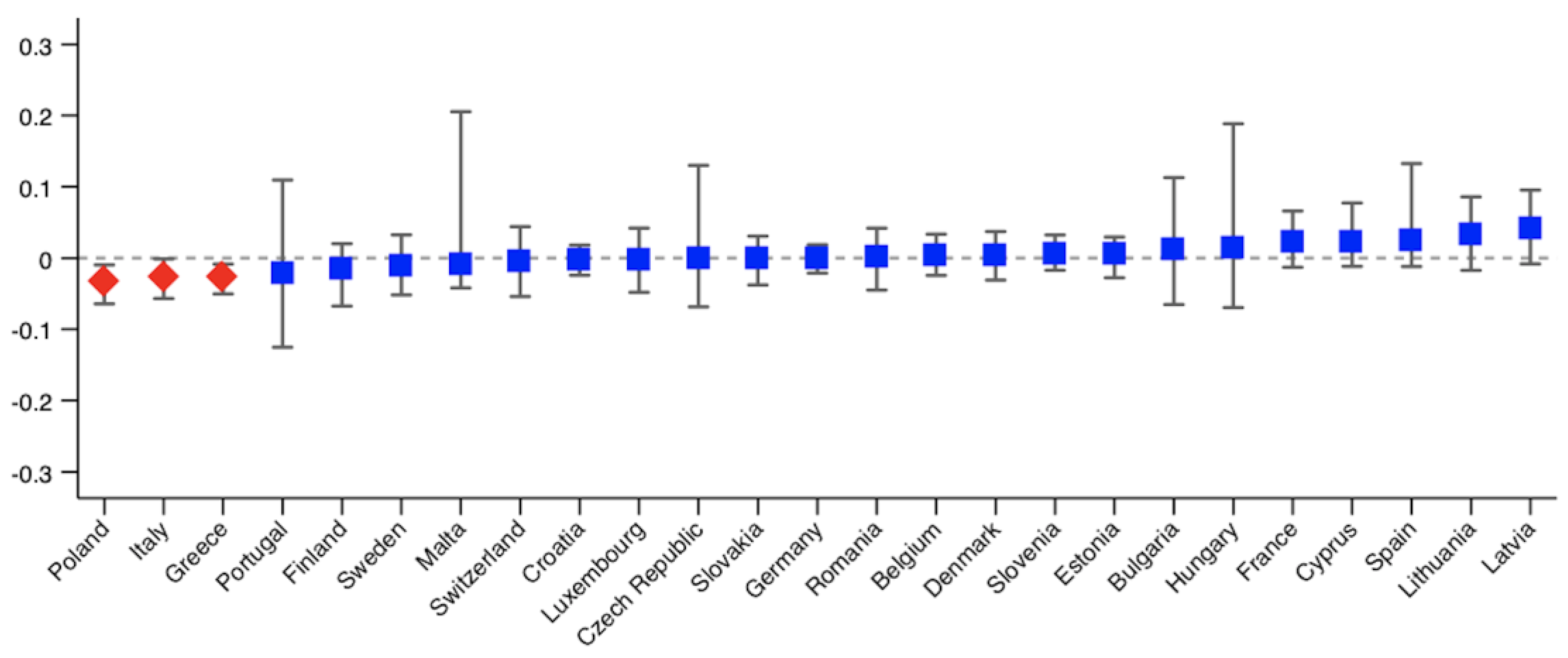
3. Results
4. Discussion
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Commission on Social Determinants of Health. Closing the Gap in a Generation: Health Equity through Action on the Social Determinants of Health. Final Report of the Commission on Social Determinants of Health; World Health Organization: Geneva, Switzerland, 2008. [Google Scholar]
- Van Dorn, A.; Cooney, E.R.; Sabin, M.L. COVID-19 exacerbating inequalities in the US. Lancet 2020, 395, 1243–1244. [Google Scholar] [CrossRef]
- Thomson, S.; Habicht, T.; Evetovits, T. How Are Countries Removing Financial Barriers to Accessing Health Services in the context of COVID-19? COVID-19 Health System Response Monitor (HSRM) 2020. Available online: https://eurohealthobservatory.who.int/monitors/hsrm/analyses/hsrm/how-are-countries-removing-financial-barriers-to-accessing-health-services-in-the-context-of-COVID-19 (accessed on 19 August 2021).
- Health at a Glance: Europe 2020: State of Health in the EU Cycle; OECD: Paris, France, 2020. Available online: https://www.oecd-ilibrary.org/social-issues-migration-health/health-at-a-glance-europe-2020_82129230-en (accessed on 31 May 2021).
- Moynihan, R.; Sanders, S.; Michaleff, A.Z.; Scott, A.M.; Clark, J.; To, E.J.; Jones, M.; Kitchener, E.; Fox, M.; Johansson, M.; et al. Impact of COVID-19 pandemic on utilisation of healthcare services: A systematic review. BMJ Open 2021, 11, e045343. [Google Scholar] [CrossRef]
- Rosenbaum, L. The Untold Toll—The Pandemic’s Effects on Patients without COVID-19. N. Engl. J. Med. 2020, 382, 2368–2371. [Google Scholar] [CrossRef]
- Verhoeven, V.; Tsakitzidis, G.; Philips, H.; Van Royen, P. Impact of the COVID-19 pandemic on the core functions of primary care: Will the cure be worse than the disease? A qualitative interview study in Flemish GPs. BMJ Open 2020, 10, e039674. [Google Scholar] [CrossRef]
- Chudasama, Y.V.; Gillies, C.L.; Zaccardi, F.; Coles, B.; Davies, M.; Seidu, S.; Khunti, K. Impact of COVID-19 on routine care for chronic diseases: A global survey of views from healthcare professionals. Diabetes Metab. Syndr. Clin. Res. Rev. 2020, 14, 965–967. [Google Scholar] [CrossRef]
- Maringe, C.; Spicer, J.; Morris, M.; Purushotham, A.; Nolte, E.; Sullivan, R.; Rachet, B.; Aggarwal, A. The impact of the COVID-19 pandemic on cancer deaths due to delays in diagnosis in England, UK: A national, population-based, modelling study. Lancet Oncol. 2020, 21, 1023–1034. [Google Scholar] [CrossRef]
- Clark, J.J.; Dwyer, D.; Pinwill, N.; Clark, P.; Johnson, P.; Hackshaw, A. The effect of clinical decision making for initiation of systemic anticancer treatments in response to the COVID-19 pandemic in England: A retrospective analysis. Lancet Oncol. 2021, 22, 66–73. [Google Scholar] [CrossRef]
- Mansfield, E.K.; Mathur, R.; Tazare, J.; Henderson, A.D.; Mulick, A.R.; Carreira, H.; Matthews, A.A.; Bidulka, P.; Gayle, A.; Forbes, H.; et al. Indirect acute effects of the COVID-19 pandemic on physical and mental health in the UK: A population-based study. Lancet Digit. Health 2021, 3, e217–e230. [Google Scholar] [CrossRef]
- Patt, D.; Gordan, L.; Diaz, M.; Okon, T.; Grady, L.; Harmison, M.; Markward, N.; Sullivan, M.; Peng, J.; Zhou, A. Impact of COVID-19 on Cancer Care: How the Pandemic Is Delaying Cancer Diagnosis and Treatment for American Seniors. JCO Clin. Cancer Inform. 2020, 4, 1059–1071. [Google Scholar] [CrossRef]
- Michalowsky, B.; Hoffmann, W.; Bohlken, J.; Kostev, K. Effect of the COVID-19 lockdown on disease recognition and utilisation of healthcare services in the older population in Germany: A cross-sectional study. Age Ageing 2021, 50, 317–325. [Google Scholar] [CrossRef] [PubMed]
- Lindström, C.; Rosvall, M.; Lindström, M. Unmet health-care needs and mortality: A prospective cohort study from southern Sweden. Scand. J. Public Health 2019, 48, 267–274. [Google Scholar] [CrossRef] [PubMed]
- Palmer, K.; Monaco, A.; Kivipelto, M.; Onder, G.; Maggi, S.; Michel, J.-P.; Prieto, R.; Sykara, G.; Donde, S. The potential long-term impact of the COVID-19 outbreak on patients with non-communicable diseases in Europe: Consequences for healthy ageing. Aging Clin. Exp. Res. 2020, 32, 1189–1194. [Google Scholar] [CrossRef] [PubMed]
- Blundell, R.; Costa Dias, M.; Joyce, R.; Xu, X. COVID-19 and Inequalities. Fisc. Stud. 2020, 41, 291–319. [Google Scholar] [CrossRef]
- Eurostat. Ageing Europe—Statistics on Population Developments. Available online: https://ec.europa.eu/eurostat/statistics-explained/index.php?title=Ageing_Europe_-_statistics_on_population_developments#Older_people_.E2.80.94_population_overview (accessed on 13 July 2021).
- Börsch-Supan, A.; Brandt, M.; Hunkler, C.; Kneip, T.; Korbmacher, J.; Malter, F.; Schaan, B.; Stuck, S.; Zuber, S. Data Resource Profile: The Survey of Health, Ageing and Retirement in Europe (SHARE). Int. J. Epidemiol. 2013, 42, 992–1001. [Google Scholar] [CrossRef] [PubMed]
- Börsch-Supan, A. Survey of Health, Ageing and Retirement in Europe (SHARE) Wave 8. COVID-19 Survey 1. Release Version: 1.0.0; SHARE-ERIC: Munich, Germany, 2020. [Google Scholar] [CrossRef]
- Rodrigues, R.; Ilinca, S.; Schmidt, A.E. Income-rich and wealth-poor? The impact of measures of socio-economic status in the analysis of the distribution of long-term care use among older people. Health Econ. 2018, 27, 637–646. [Google Scholar] [CrossRef]
- Ilinca, S.; Rodrigues, R.; Schmidt, A.E. Fairness and Eligibility to Long-Term Care: An Analysis of the Factors Driving Inequality and Inequity in the Use of Home Care for Older Europeans. Int. J. Environ. Res. Public Health 2017, 14, 1224. [Google Scholar] [CrossRef] [PubMed]
- García-Gómez, P.; Hernández-Quevedo, C.; Jiménez-Rubio, D.; Oliva-Moreno, J. Inequity in long-term care use and unmet need: Two sides of the same coin. J. Health Econ. 2015, 39, 147–158. [Google Scholar] [CrossRef] [PubMed]
- Lera, J.; Pascual-Sáez, M.; Cantarero-Prieto, D. Socioeconomic Inequality in the Use of Long-Term Care among European Older Adults: An Empirical Approach Using the SHARE Survey. Int. J. Environ. Res. Public Health 2020, 18, 20. [Google Scholar] [CrossRef]
- Tavares, L.P.; Zantomio, F. Inequity in healthcare use among older people after 2008: The case of southern European countries. Health Policy 2017, 121, 1063–1071. [Google Scholar] [CrossRef] [Green Version]
- Davillas, A.; Jones, A.M. Unmet health care need and income-Related horizontal equity in use of health care during the COVID-19 pandemic. Health Econ. 2021, 30, 1711–1716. [Google Scholar] [CrossRef]
- Smolić, Š.; Čipin, I.; Međimurec, P. Access to healthcare for people aged 50+ in Europe during the COVID-19 outbreak. Eur. J. Ageing 2021, 1–17. [Google Scholar] [CrossRef]
- Arnault, L.; Jusot, F.; Renaud, T. Social Inequalities in Access to Healthcare among the Population Aged 50+ Years during the COVID-19 Pandemic in Europe. SHARE Working Paper Series 58-2021, 742363. Available online: https://pure.mpg.de/pubman/item/item_3289765 (accessed on 27 April 2021).
- Scherpenzeel, A.; Axt, K.; Bergmann, M.; Douhou, S.; Oepen, A.; Sand, G.; Schuller, K.; Stucj, S.; Wagner, M.; Börsch-Supan, A. Collecting survey data among the 50+ population during the COVID-19 outbreak: The Survey of Health, Ageing and Retirement in Europe (SHARE). Surv. Res. Methods 2020, 14, 217–221. [Google Scholar] [CrossRef]
- Börsch-Supan, A. Survey of Health, Ageing and Retirement in Europe (SHARE) Wave 7. Release Version: 7.1.1; SHARE-ERIC: Munich, Germany, 2020. [Google Scholar] [CrossRef]
- De Luca, G. SHARE Release Guide 7.0.0. Chapter 15.3. 2019. Available online: http://www.share-project.org/fileadmin/pdf_documentation/SHARE_release_guide_7-0-0.pdf (accessed on 22 April 2021).
- De Luca, G.; Celidoni, M.; Trevisan, E. Item Nonresponse and Imputation Strategies in SHARE Wave 5. In SHARE Wave 5: Innovations & Methodology; Malter, F., Börsch-Supan, A., Eds.; MEA Max Planck Institute for Social Law and Social Policy: Munich, Germany, 2015; pp. 85–102. [Google Scholar]
- Wagstaff, A.; Van Doorslaer, E.; Paci, P. Equity in the Finance and Delivery of Health Care: Some Tentative Cross-Country Comparisons. Oxf. Rev. Econ. Policy 1989, 5, 89–112. [Google Scholar] [CrossRef] [Green Version]
- Wagstaff, A.; Van Doorslaer, E. Measuring and Testing for Inequity in the Delivery of Health Care. J. Hum. Resour. 2000, 35, 716. [Google Scholar] [CrossRef]
- Wagstaff, A.; van Doorslaer, E.; Paci, P. On the measurement of horizontal inequity in the delivery of health care. J. Health Econ. 1991, 10, 169–205. [Google Scholar] [CrossRef] [Green Version]
- Van Doorslaer, E.; Koolman, X.; Jones, A.M. Explaining income-related inequalities in doctor utilisation in Europe. Health Econ. 2004, 13, 629–647. [Google Scholar] [CrossRef] [PubMed]
- Wagstaff, A.; van Doorslaer, E.; Watanabe, N. On decomposing the causes of health sector inequalities with an application to malnutrition inequalities in Vietnam. J. Econ. 2003, 112, 207–223. [Google Scholar] [CrossRef] [Green Version]
- O’Donnell, O.; Van Doorslaer, E.; Wagstaff, A.; Lindelow, M. Analyzing Health Equity Using Household Survey Data. In Analyzing Health Equity Using Household Survey Data; The World Bank: Washington, DC, USA, 2007. [Google Scholar]
- Erreygers, G. Correcting the Concentration Index. J. Health Econ. 2009, 28, 504–515. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- D’Uva, T.B.; Jones, A.; van Doorslaer, E. Measurement of horizontal inequity in health care utilisation using European panel data. J. Health Econ. 2009, 28, 280–289. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Van De Poel, E.; Van Doorslaer, E.; O’Donnell, O. Measurement of inequity in health care with heterogeneous response of use to need. J. Health Econ. 2012, 31, 676–689. [Google Scholar] [CrossRef] [Green Version]
- Panteli, D. How Are Countries Reorganizing Non-COVID-19 Health Care Services Delivery? COVID-19 Health System Response Monitor (HSRM) 2020. Available online: https://eurohealthobservatory.who.int/monitors/hsrm/analyses/hsrm/how-are-countries-reorganizing-non-COVID-19-health-care-service-delivery (accessed on 21 July 2021).
- Jiskrova, G.K.; Bobák, M.; Pikhart, H.; Ksinan, A.J. Job loss and lower healthcare utilisation due to COVID-19 among older adults across 27 European countries. J. Epidemiol. Community Health 2021. [Google Scholar] [CrossRef]
- The Health Systems and Policy Monitor. Available online: https://www.hspm.org/searchandcompare.aspx (accessed on 22 August 2021).
- Sustainable Development Indicators. Eurostat. Available online: https://ec.europa.eu/eurostat/data/database (accessed on 20 December 2020).
- van Doorslaer, E.; Masseria, C.; Koolman, X. Inequalities in access to medical care by income in developed countries. Can. Med Assoc. J. 2006, 174, 177–183. [Google Scholar] [CrossRef] [Green Version]
- Masseria, C.; Giannoni, M. Equity in access to health care in Italy: A disease-based approach. Eur. J. Public Health 2010, 20, 504–510. [Google Scholar] [CrossRef] [PubMed]
- Devaux, M. Income-related inequalities and inequities in health care services utilisation in 18 selected OECD countries. Eur. J. Health Econ. 2015, 16, 21–33. [Google Scholar] [CrossRef]
- Lam, K.; Lu, A.D.; Shi, Y.; Covinsky, K.E. Assessing Telemedicine Unreadiness Among Older Adults in the United States During the COVID-19 Pandemic. JAMA Intern. Med. 2020, 180, 1389. [Google Scholar] [CrossRef]
- Vergouw, J.W.; Smits-Pelser, H.; Kars, M.C.; van Houwelingen, T.; van Os-Medendorp, H.; Kort, H.; Bleijenberg, N. Needs, barriers and facilitators of older adults towards eHealth in general practice: A qualitative study. Prim. Health Care Res. Dev. 2020, 21, e54. [Google Scholar] [CrossRef] [PubMed]
- Kempf, A.M.; Remington, P.L. New Challenges for Telephone Survey Research in the Twenty-First Century. Annu. Rev. Public Health 2007, 28, 113–126. [Google Scholar] [CrossRef] [PubMed]
- Schokkaert, E.; Dhaene, G.; Van de Voorde, C. Risk adjustment and the trade-off between efficiency and risk selection: An application of the theory of fair compensation. Health Econ. 1998, 7, 465–480. [Google Scholar] [CrossRef]
| Variable | Definition | Mean */Percentage | SD |
|---|---|---|---|
| Health care | |||
| Postponed care | Postponed medical appointment since the COVID-19 outbreak (Yes/No) | 0.2533 | 0.4349 |
| Denied appointment | Denied medical appointment since the COVID-19 outbreak (Yes/No) | 0.0540 | 0.2259 |
| Need variables | |||
| Female | Gender of respondent (1 female; 0 male) | 0.5462 | 0.4979 |
| Age | Age of respondent (years) | 67.75 | 10.07 |
| Age groups | |||
| 50–64 years old | 0.4728 | 0.4993 | |
| 65–69 years old | 0.1363 | 0.3431 | |
| 70–74 years old | 0.1323 | 0.3389 | |
| 75–79 years old | 0.0964 | 0.2952 | |
| 80–84 years old | 0.0890 | 0.2846 | |
| 85 and over years old | 0.0732 | 0.2605 | |
| SAH | Respondent’s self-assessed health status | ||
| Excellent or very good | 0.2481 | 0.4319 | |
| Good | 0.4653 | 0.4988 | |
| Fair | 0.2251 | 0.4177 | |
| Poor | 0.0615 | 0.2402 | |
| Worsened health | Respondent’s health status has worsened since the COVID-19 outbreak (Yes/No) | 0.0925 | 0.2898 |
| Chronic | Number of chronic conditions that the respondent has been diagnosed with (excluding cancer) | 1.83 | 1.75 |
| Cancer | Respondent has been ever diagnosed or currently having cancer (Yes/No) | 0.0372 | 0.1894 |
| ADL | Number of limitations with activities of daily living | 0.1784 | 0.7150 |
| IADL | Number of limitations with instrumental activities of daily living | 0.3358 | 1.1702 |
| Non-need variables | |||
| Living alone | Respondent living alone (Yes/No) | 0.2721 | 0.4451 |
| Household income | Equivalent household net income (euros) | 18,694.16 € | 16,886.41 € |
| Education | Respondent’s highest level of education | ||
| Primary education | 0.3578 | 0.4794 | |
| Secondary education | 0.4211 | 0.4937 | |
| Higher education | 0.2211 | 0.4150 | |
| Current job situation | |||
| Inactive (retired, permanently sick or homemaker) | 0.5729 | 0.4947 | |
| Employed or self-employed | 0.3341 | 0.4717 | |
| Unemployed | 0.0930 | 0.2905 | |
| Urban | Respondent’s living area (1 Urban area; 0 Rural area) | 0.6192 | 0.4856 |
| Country | Number of Observations | Postponed Care | Denied Care | Equivalent Household Net Income (Euros) |
|---|---|---|---|---|
| Germany | 2446 | 0.1866 (0.3897) | 0.0289 (0.1647) | 24,780 (11,978) |
| Sweden | 1107 | 0.1578 (0.3647) | 0.0395 (0.1948) | 30,124 (11,566) |
| Spain | 1585 | 0.2775 (0.4479) | 0.0384 (0.1922) | 13,249 (7720) |
| Italy | 3008 | 0.2507 (0.4335) | 0.0595 (0.2366) | 19,143 (18,864) |
| France | 1772 | 0.3593 (0.4799) | 0.1005 (0.3008) | 25,518 (16,502) |
| Denmark | 1823 | 0.3050 (0.4605) | 0.0422 (0.2011) | 41,494 (37,022) |
| Greece | 2341 | 0.1043 (0.3057) | 0.0324 (0.1770) | 13,056 (17,022) |
| Switzerland | 1637 | 0.2740 (0.4462) | 0.0294 (0.1690) | 47,818 (35,662) |
| Belgium | 3297 | 0.3378 (0.4730) | 0.0710 (0.2569) | 24,258 (9322) |
| Czech Republic | 2228 | 0.3720 (0.4834) | 0.0332 (0.1792) | 8296 (2770) |
| Poland | 2706 | 0.2775 (0.4479) | 0.0682 (0.2522) | 6380 (3470) |
| Luxembourg | 719 | 0.5368 (0.4990) | 0.0598 (0.2372) | 43,708 (22,753) |
| Hungary | 719 | 0.2310 (0.4218) | 0.0425 (0.2020) | 5893 (2449) |
| Portugal | 849 | 0.5586 (0.4968) | 0.0905 (0.2870) | 9865 (6030) |
| Slovenia | 2621 | 0.3128 (0.4637) | 0.0300 (0.1705) | 10,808 (4870) |
| Estonia | 3514 | 0.2476 (0.4317) | 0.0747 (0.2629) | 8296 (4688) |
| Croatia | 1770 | 0.2195 (0.4140) | 0.0293 (0. 1687) | 6239 (3442) |
| Lithuania | 1119 | 0.2757 (0.4471) | 0.1100 (0.3130) | 5527 (3094) |
| Bulgaria | 773 | 0.0162 (0.1261) | 0.0110 (0.1045) | 3215 (1748) |
| Cyprus | 672 | 0.1839 (0.3877) | 0.0419 (0.2004) | 32,298 (45,758) |
| Finland | 1192 | 0.1809 (0.3851) | 0.0502 (0.2184) | 26,302 (13,524) |
| Latvia | 877 | 0.1432 (0.3505) | 0.0752 (0.2639) | 5069 (2707) |
| Malta | 730 | 0.3495 (0.4771) | 0.0219 (0.1466) | 11,433 (8215) |
| Romania | 1289 | 0.0720 (0.2587) | 0.0496 (0.2172) | 2791 (1693) |
| Slovakia | 812 | 0.2085 (0.4065) | 0.0438 (0.2047) | 9631 (8532) |
| Europe | 41,606 | 0.2533 (0.4349) | 0.0540 (0.2259) | 18,694 (16,886) |
| Country | Postponed Care | Denied Care | ||
|---|---|---|---|---|
| Erreygers CI a | HI b | Erreygers CI a | HI b | |
| Germany | 0.0096 (0.0243) | 0.0227 (0.0242) | −0.0136 (0.0096) | −0.0007 (0.0099) |
| Sweden | −0.1085 *** (0.0258) | 0.0003 (0.0525) | −0.0325 * (0.0195) | −0.0116 (0.0214) |
| Spain | −0.0290 (0.0661) | −0.0019 (0.0677) | 0.0052 (0.0177) | 0.0233 (0.0365) |
| Italy | −0.0046 (0.0274) | 0.0485 * (0.0275) | −0.0409 ** (0.0143) | −0.0277 ** (0.0139) |
| France | 0.0066 (0.0379) | 0.0469 (0.0389) | 0.0128 (0.0197) | 0.0223 (0.0198) |
| Denmark | −0.0071 (0.0278) | −0.0307 (0.0338) | 0.0000 (0.0136) | 0.0040 (0.0175) |
| Greece | −0.0355 ** (0.0160) | −0.0206 (0.0163) | −0.0321 ** (0.0113) | −0.0263 ** (0.0106) |
| Switzerland | −0.0414 (0.0435) | −0.0311 (0.0425) | −0.0182 (0.0127) | −0.0054 (0.0243) |
| Belgium | −0.0449 (0.0277) | 0.0186 (0.0266) | −0.0099 (0.0148) | 0.0034 (0.0153) |
| Czech Republic | −0.0309 (0.0613) | −0.0333 (0.0673) | −0.0191 (0.0211) | −0.0017 (0.0681) |
| Poland | −0.0231 (0.0239) | −0.0055 (0.0242) | −0.0381 ** (0.0130) | −0.0343 ** (0.0135) |
| Luxembourg | −0.0653 (0.0683) | −0.0255 (0.0691) | −0.0006 (0.0229) | −0.0032 (0.0225) |
| Hungary | −0.0378 (0.0721) | 0.0487 (0.0724) | −0.0169 (0.0289) | 0.0128 (0.0728) |
| Portugal | 0.0330 (0.1325) | 0.0240 (0.0934) | −0.0468 (0.0591) | −0.0221 (0.0595) |
| Slovenia | 0.0093 (0.0324) | 0.0353 (0.0313) | −0.0032 (0.0099) | 0.0044 (0.0124) |
| Estonia | 0.0445 ** (0.0220) | 0.0739 *** (0.0247) | −0.0034 (0.0148) | 0.0045 (0.0144) |
| Croatia | −0.0062 (0.0274) | 0.0399 (0.0278) | −0.0088 (0.0106) | −0.0035 (0.0125) |
| Lithuania | −0.0142 (0.0332) | 0.0171 (0.0373) | 0.0030 (0.0239) | 0.0321 (0.0263) |
| Bulgaria | 0.0094 (0.0150) | −0.0333 (0.0421) | 0.0149 (0.0114) | 0.0117 (0.0475) |
| Cyprus | −0.0164 (0.0421) | −0.0066 (0.0437) | 0.0112 (0.0182) | 0.0229 (0.2060) |
| Finland | 0.0287 (0.0366) | 0.0337 (0.0381) | −0.0148 (0.0208) | −0.0155 (0.0210) |
| Latvia | 0.0296 (0.0298) | 0.0513 (0.0360) | 0.0317 (0.0235) | 0.0405 (0.0262) |
| Malta | −0.0658 (0.0480) | 0.0183 (0.0549) | −0.0168 (0.0104) | −0.0097 (0.1025) |
| Romania | 0.0318 (0.0201) | 0.0352 * (0.0190) | −0.0024 (0.0192) | 0.0013 (0.0218) |
| Slovakia | −0.0557 (0.0364) | 0.0429 (0.0430) | 0.0007 (0.0148) | −0.0010 (0.0171) |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
González-Touya, M.; Stoyanova, A.; Urbanos-Garrido, R.M. COVID-19 and Unmet Healthcare Needs of Older People: Did Inequity Arise in Europe? Int. J. Environ. Res. Public Health 2021, 18, 9177. https://doi.org/10.3390/ijerph18179177
González-Touya M, Stoyanova A, Urbanos-Garrido RM. COVID-19 and Unmet Healthcare Needs of Older People: Did Inequity Arise in Europe? International Journal of Environmental Research and Public Health. 2021; 18(17):9177. https://doi.org/10.3390/ijerph18179177
Chicago/Turabian StyleGonzález-Touya, Marta, Alexandrina Stoyanova, and Rosa M. Urbanos-Garrido. 2021. "COVID-19 and Unmet Healthcare Needs of Older People: Did Inequity Arise in Europe?" International Journal of Environmental Research and Public Health 18, no. 17: 9177. https://doi.org/10.3390/ijerph18179177
APA StyleGonzález-Touya, M., Stoyanova, A., & Urbanos-Garrido, R. M. (2021). COVID-19 and Unmet Healthcare Needs of Older People: Did Inequity Arise in Europe? International Journal of Environmental Research and Public Health, 18(17), 9177. https://doi.org/10.3390/ijerph18179177







