Telemonitoring of Real-World Health Data in Cardiology: A Systematic Review
Abstract
1. Introduction
2. Materials and Methods
2.1. Search Strategy
2.2. Inclusion and Exclusion Criteria
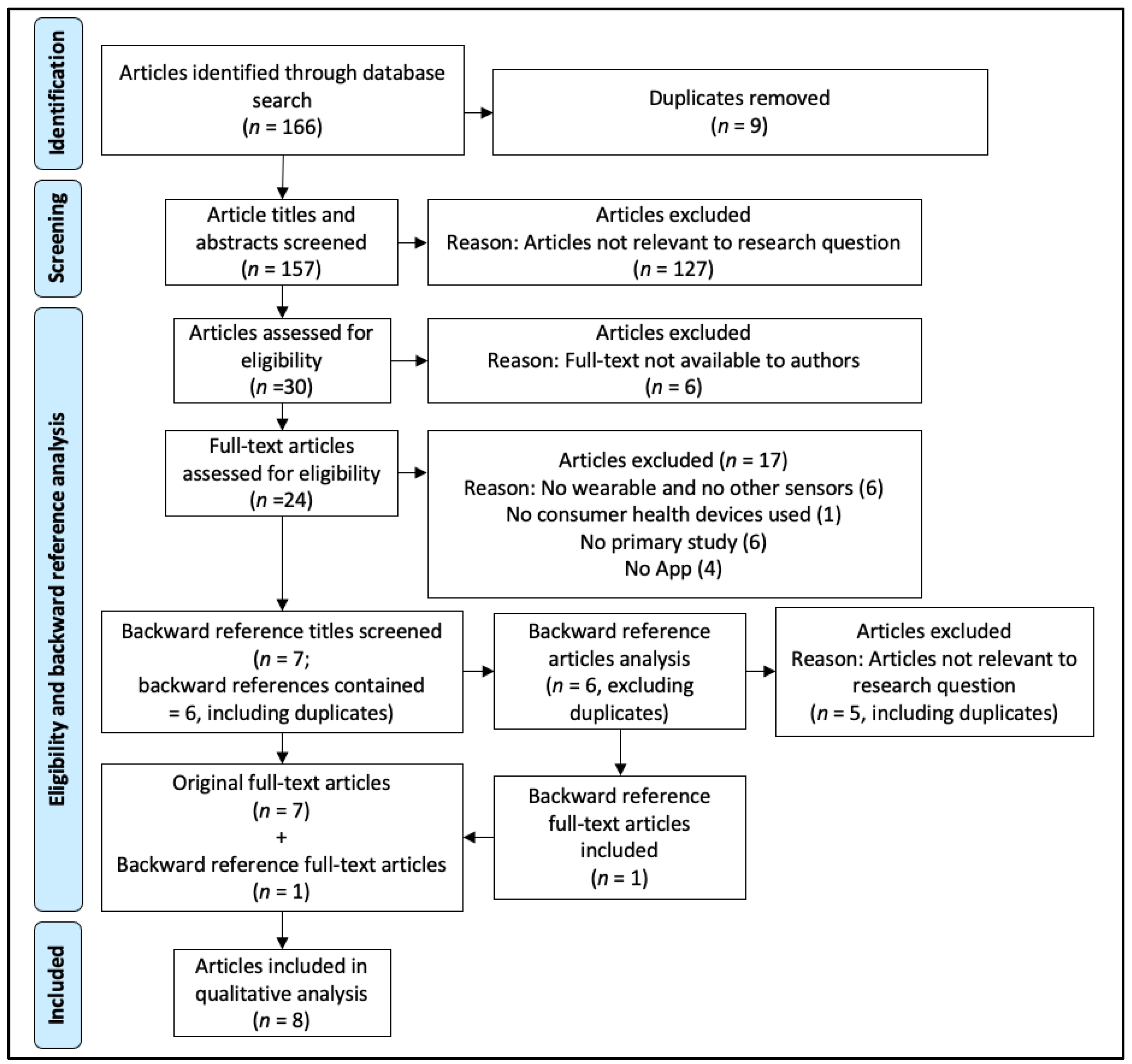
2.3. Selection and Data Extraction
2.4. Comparison Criteria
2.4.1. Study Protocol
2.4.2. Technical Parameters
2.4.3. Qualitative and Quantitative Parameters
3. Results
4. Discussion
4.1. Limitations
4.2. Outlook
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Conflicts of Interest
References
- Lamkin, P. Smart Wearables Market to Double by 2022: $27 Billion Industry Forecast. Available online: https://www.forbes.com/sites/paullamkin/2018/10/23/smart-wearables-market-to-double-by-2022-27-billion-industry-forecast/ (accessed on 14 July 2021).
- Strath, S.J.; Rowley, T.W. Wearables for Promoting Physical Activity. Clin. Chem. 2018, 64, 53–63. [Google Scholar] [CrossRef]
- Wright, S.P.; Hall Brown, T.S.; Collier, S.R.; Sandberg, K. How consumer physical activity monitors could transform human physiology research. Am. J. Physiol. Regul. Integr. Comp. Physiol. 2017, 312, R358–R367. [Google Scholar] [CrossRef] [PubMed]
- Lobelo, F.; Kelli, H.M.; Tejedor, S.C.; Pratt, M.; McConnell, M.V.; Martin, S.S.; Welk, G.J. The Wild Wild West: A Framework to Integrate mHealth Software Applications and Wearables to Support Physical Activity Assessment, Counseling and Interventions for Cardiovascular Disease Risk Reduction. Prog. Cardiovasc. Dis. 2016, 58, 584–594. [Google Scholar] [CrossRef] [PubMed]
- Perez, M.V.; Mahaffey, K.W.; Hedlin, H.; Rumsfeld, J.S.; Garcia, A.; Ferris, T.; Balasubramanian, V.; Russo, A.M.; Rajmane, A.; Cheung, L.; et al. Large-Scale Assessment of a Smartwatch to Identify Atrial Fibrillation. N. Engl. J. Med. 2019, 381, 1909–1917. [Google Scholar] [CrossRef] [PubMed]
- Khan, T.V.; Khan, S.S.-S.; Akhondi, A.; Khan, T.W. White coat hypertension: Relevance to clinical and emergency medical services personnel. MedGenMed 2007, 9, 52. [Google Scholar]
- Cohen, J.B.; Lotito, M.J.; Trivedi, U.K.; Denker, M.G.; Cohen, D.L.; Townsend, R.R. Cardiovascular Events and Mortality in White Coat Hypertension: A Systematic Review and Meta-analysis. Ann. Intern. Med. 2019, 170, 853–862. [Google Scholar] [CrossRef]
- Sana, F.; Isselbacher, E.M.; Singh, J.P.; Heist, E.K.; Pathik, B.; Armoundas, A.A. Wearable Devices for Ambulatory Cardiac Monitoring: JACC State-of-the-Art Review. J. Am. Coll. Cardiol. 2020, 75, 1582–1592. [Google Scholar] [CrossRef] [PubMed]
- Savarese, G.; Lund, L.H. Global Public Health Burden of Heart Failure. Card. Fail. Rev. 2017, 3, 7. [Google Scholar] [CrossRef]
- Dharmarajan, K.; Hsieh, A.F.; Lin, Z.; Bueno, H.; Ross, J.S.; Horwitz, L.I.; Barreto-Filho, J.A.; Kim, N.; Bernheim, S.M.; Suter, L.G.; et al. Diagnoses and timing of 30-day readmissions after hospitalization for heart failure, acute myocardial infarction, or pneumonia. JAMA 2013, 309, 355–363. [Google Scholar] [CrossRef]
- Desai, A.S.; Stevenson, L.W. Rehospitalization for heart failure: Predict or prevent? Circulation 2012, 126, 501–506. [Google Scholar] [CrossRef]
- Haarbrandt, B.; Schreiweis, B.; Rey, S.; Sax, U.; Scheithauer, S.; Rienhoff, O.; Knaup-Gregori, P.; Bavendiek, U.; Dieterich, C.; Brors, B.; et al. HiGHmed—An Open Platform Approach to Enhance Care and Research across Institutional Boundaries. Methods Inf. Med. 2018, 57, e66–e81. [Google Scholar] [CrossRef]
- Liberati, A.; Altman, D.G.; Tetzlaff, J.; Mulrow, C.; Gøtzsche, P.C.; Ioannidis, J.P.A.; Clarke, M.; Devereaux, P.J.; Kleijnen, J.; Moher, D. The PRISMA statement for reporting systematic reviews and meta-analyses of studies that evaluate health care interventions: Explanation and elaboration. PLoS Med. 2009, 6, e1000100. [Google Scholar] [CrossRef] [PubMed]
- Weldring, T.; Smith, S.M.S. Patient-Reported Outcomes (PROs) and Patient-Reported Outcome Measures (PROMs). Health Serv. Insights 2013, 6, 61–68. [Google Scholar] [CrossRef]
- Sharpio, M.; Johnston, D.; Wald, J.; Mon, D. Patient-Generated Health Data: White Paper. Available online: https://www.healthit.gov/sites/default/files/rti_pghd_whitepaper_april_2012.pdf (accessed on 12 July 2021).
- Guo, Y.; Lane, D.A.; Wang, L.; Chen, Y.; Lip, G.Y.H. The mAF-App II Trial Investigators. Mobile Health (mHealth) technology for improved screening, patient involvement and optimising integrated care in atrial fibrillation: The mAFA (mAF-App) II randomised trial. Int. J. Clin. Pract. 2019, 73, e13352. [Google Scholar] [CrossRef]
- Guo, Y.; Wang, H.; Zhang, H.; Liu, T.; Liang, Z.; Xia, Y.; Yan, L.; Xing, Y.; Shi, H.; Li, S.; et al. Mobile Photoplethysmographic Technology to Detect Atrial Fibrillation. J. Am. Coll. Cardiol. 2019, 74, 2365–2375. [Google Scholar] [CrossRef] [PubMed]
- McManus, D.D.; Trinquart, L.; Benjamin, E.J.; Manders, E.S.; Fusco, K.; Jung, L.S.; Spartano, N.L.; Kheterpal, V.; Nowak, C.; Sardana, M.; et al. Design and Preliminary Findings from a New Electronic Cohort Embedded in the Framingham Heart Study. J. Med. Internet Res. 2019, 21, e12143. [Google Scholar] [CrossRef]
- Modena, B.D.; Bellahsen, O.; Nikzad, N.; Chieh, A.; Parikh, N.; Dufek, D.M.; Ebner, G.; Topol, E.J.; Steinhubl, S. Advanced and Accurate Mobile Health Tracking Devices Record New Cardiac Vital Signs. Hypertension 2018, 72, 503–510. [Google Scholar] [CrossRef] [PubMed]
- Seto, E.; Ross, H.; Tibbles, A.; Wong, S.; Ware, P.; Etchells, E.; Kobulnik, J.; Chibber, T.; Poon, S. A Mobile Phone-Based Telemonitoring Program for Heart Failure Patients After an Incidence of Acute Decompensation (Medly-AID): Protocol for a Randomized Controlled Trial. JMIR Res. Protoc. 2020, 9, e15753. [Google Scholar] [CrossRef] [PubMed]
- Wenger, N.K.; Williams, O.O.; Parashar, S. SMARTWOMAN™: Feasibility assessment of a smartphone app to control cardiovascular risk factors in vulnerable diabetic women. Clin. Cardiol. 2019, 42, 217–221. [Google Scholar] [CrossRef]
- Werhahn, S.M.; Dathe, H.; Rottmann, T.; Franke, T.; Vahdat, D.; Hasenfuß, G.; Seidler, T. Designing meaningful outcome parameters using mobile technology: A new mobile application for telemonitoring of patients with heart failure. ESC Heart Fail. 2019, 6, 516–525. [Google Scholar] [CrossRef]
- Koehler, F.; Koehler, K.; Deckwart, O.; Prescher, S.; Wegscheider, K.; Kirwan, B.-A.; Winkler, S.; Vettorazzi, E.; Bruch, L.; Oeff, M.; et al. Efficacy of telemedical interventional management in patients with heart failure (TIM-HF2): A randomised, controlled, parallel-group, unmasked trial. Lancet 2018, 392, 1047–1057. [Google Scholar] [CrossRef]
- Guo, Y.; Lane, D.A.; Wang, L.; Zhang, H.; Wang, H.; Zhang, W.; Wen, J.; Xing, Y.; Wu, F.; Xia, Y.; et al. Mobile Health Technology to Improve Care for Patients with Atrial Fibrillation. J. Am. Coll. Cardiol. 2020, 75, 1523–1534. [Google Scholar] [CrossRef] [PubMed]
- Shcherbina, A.; Mattsson, C.M.; Waggott, D.; Salisbury, H.; Christle, J.W.; Hastie, T.; Wheeler, M.T.; Ashley, E.A. Accuracy in Wrist-Worn, Sensor-Based Measurements of Heart Rate and Energy Expenditure in a Diverse Cohort. J. Pers. Med. 2017, 7, 3. [Google Scholar] [CrossRef]
- O’Connell, S.; ÓLaighin, G.; Quinlan, L.R. When a Step Is Not a Step! Specificity Analysis of Five Physical Activity Monitors. PLoS ONE 2017, 12, e0169616. [Google Scholar] [CrossRef]
- Ferguson, T.; Rowlands, A.V.; Olds, T.; Maher, C. The validity of consumer-level, activity monitors in healthy adults worn in free-living conditions: A cross-sectional study. Int. J. Behav. Nutr. Phys. Act. 2015, 12, 42. [Google Scholar] [CrossRef] [PubMed]
- Muehlhausen, W.; Doll, H.; Quadri, N.; Fordham, B.; O’Donohoe, P.; Dogar, N.; Wild, D.J. Equivalence of electronic and paper administration of patient-reported outcome measures: A systematic review and meta-analysis of studies conducted between 2007 and 2013. Health Qual. Life Outcomes 2015, 13, 167. [Google Scholar] [CrossRef]
- Eremenco, S.; Coons, S.J.; Paty, J.; Coyne, K.; Bennett, A.V.; McEntegart, D. PRO data collection in clinical trials using mixed modes: Report of the ISPOR PRO mixed modes good research practices task force. Value Health 2014, 17, 501–516. [Google Scholar] [CrossRef]
- Corral, L.; Janes, A.; Remencius, T. Potential Advantages and Disadvantages of Multiplatform Development Frameworks—A Vision on Mobile Environments. Procedia Comput. Sci. 2012, 10, 1202–1207. [Google Scholar] [CrossRef][Green Version]
- Turakhia, M.P.; Desai, M.; Hedlin, H.; Rajmane, A.; Talati, N.; Ferris, T.; Desai, S.; Nag, D.; Patel, M.; Kowey, P.; et al. Rationale and design of a large-scale, app-based study to identify cardiac arrhythmias using a smartwatch: The Apple Heart Study. Am. Heart J. 2019, 207, 66–75. [Google Scholar] [CrossRef] [PubMed]
| Database | Query |
|---|---|
| PubMed | ((telemedicine OR telecardiology [Title/Abstract]) AND (cardiology OR “cardiovascular disease” [Title/Abstract]) AND (app OR mobile application [Title/Abstract])) AND ((“2001/01/01” [Date—Publication]: “2021/03/31” [Date—Publication])) |
| CINAHL | ((telemedicine OR telecardiology [Title/Abstract]) AND (cardiology OR “cardiovascular disease” [Title/Abstract]) AND (app OR mobile application [Title/Abstract])) AND ((“2001/01/01” [Date—Publication]: “2021/03/31” [Date—Publication])) |
| Cochrane | (telemedicine OR telecardiology):ti,ab AND (cardiology OR “cardiovascular disease”):ti,ab AND (app OR mobile application):ti,ab” with Cochrane Library publication date between Jan 2001 and Mar 2021 |
| Web of Science | (AB = ((telemedicine OR telecardiology) AND (cardiology OR “cardiovascular disease”) AND (app OR mobile application))) OR (TI = ((telemedicine OR telecardiology) AND (cardiology OR “cardiovascular disease”) AND (app OR mobile application))) (Search period was set via the UI of Web of Science.) |
| SCOPUS | ((ABS (telemedicine OR telecardiology) AND ABS (cardiology OR “cardiovascular disease”) AND ABS (app OR mobile AND application))) OR ((TITLE (telemedicine OR telecardiology) AND TITLE (cardiology OR “cardiovascular disease”) AND TITLE (app OR mobile AND application))) AND (LIMIT-TO (SRCTYPE, “j”) OR LIMIT-TO (SRCTYPE, “p”)) (Search period was set via the UI of SCOPUS.) |
| Ref. | Country | Application Area | Study Type | Disease | Sample Size (Population Size) | Participation Duration |
|---|---|---|---|---|---|---|
| Werhahn et al., 2019 [22] | Germany | Local | Proof-of-concept study | Heart failure | 10 (10) | 2 months |
| Wenger et al., 2019 [21] | USA | Local | Pilot Study | Cardiovascular disease | 14 (14) | 6 months |
| Seto et al., 2020 [20] | Canada | Local | RCT 1 | Heart failure | 74 (144) | 3 months |
| Modena et al., 2018 [19] | USA | National | Proof-of-concept study | Cardiovascular disease | 250 (250) | 17 weeks |
| McManus et al., 2019 [18] | USA | Local | Longitudinal cohort study | Cardiovascular disease | 790 (4095) | ≥3 months |
| Guo et al., 2019a [17] | China | National | Screening study | Atrial fibrillation | 187,912 (246,541) | ≥14 days |
| Guo et al., 2019 [16] [24] | China | National | CRT 2 | Atrial fibrillation | 32,259 (32,259) | ≥14 days |
| Koehler et al., 2018 [23] | Germany | National | RCT 1 | Heart failure | 796 (1571) | 365–393 days |
| Ref. | Monitoring (Interventional/Observing) | Operating System/ Platform | Wearable | Other Consumer Health Devices |
|---|---|---|---|---|
| Werhahn et al., 2019 [22] | Interventional | iOS versions 10.2.1–11.2.1 | (1) Apple Watch 1st Gen. | / |
| Wenger et al., 2019 [21] | Interventional | Unknown | (1) Fitbit | (1) Weight-scale (2) Glucometer (3) Sphygmomanometer |
| Seto et al., 2020 [20] | Interventional | Unknown | / | (1) A&D Medical Bluetooth weight scales (2) A&D Medical Bluetooth BP 1 monitors |
| Modena et al., 2018 [19] | Observing | Android/iOS | (1) Withings fitness tracker (2) Withings Watch | (1) mHealth BP 1 monitor (2) Smart weight scale (3) Sleep-tracking system |
| McManus et al., 2019 [18] | Observing | iOS versions 9 or higher | (1) Apple Watch | (1) Nokia Withings Digital BP 1 cuff |
| Guo et al., 2019a [17] | Interventional | Android 5.0 or higher | (1) Honor Band 4 (2) Honor Watch (3) Huawei Watch GT | / |
| Guo et al., 2019 [16] | Interventional | Unknown | (1) Honor Band 4 (2) Honor Watch (3) Huawei Watch GT | / |
| Koehler et al., 2018 [23] | Interventional | Unknown | / | (1) Three-channel ECG device: PhysioMem PM 1000, GETEMED (2) A&D BP 1 measuring device (UA767PBT) (3) Seca 861 Weighing scales (4) SpO2 2 Signal Masimo Extraction Technology |
| Ref. | PROM | PGHD | Clinical Parameters and Scales | Self-Tracked Follow-Up Parameters | Frequency |
|---|---|---|---|---|---|
| Werhahn et al., 2019 [22] | (1) Minnesota Living with Heart Failure Questionnaire (MLHFQ) (2) Kansas City Cardiomyopathy Questionnaire (KCCQ) (3) Patient Health Questionnaire Depression Scale (PHQ-9) (4) Cardiac Anxiety Questionnaire (CAQ) (5) eHealth literacy (questionnaire similar to the eHealth Literacy Scale) | (1) Self-measured blood pressure (2) Self-measured body weight (before breakfast) (3) Confirmation of medication intake | (1) Holter electrocardiograms (ECGs) with 4 days of records (2) Six-minute walk test (6MWT) | (1) Mean daily step count (MDSC) (2) Heart rate (3) Six-minute walk test (6MWT) | (1), (2) Daily (3) Three times at site visits |
| Wenger et al., 2019 [21] | (1) Individualized questionnaires (e.g., for medication adherence in case of missing BP measurements) | (1) Taking insulin or oral diabetes medication (2) Cholesterol medication (3) Following a diabetic healthful diet (4) Smoking cessation | / | (1) Blood glucose (2) Blood pressure (3) Weight (4) Daily steps | (1) Daily (every morning) (2) (3) Weekly (on the same day) (4) Daily |
| Seto et al., 2020 [20] | (1) Self-Care of Heart Failure Index (SCHFI) (2) Kansas City Cardiomyopathy Questionnaire-12 (KCCQ-12) (3) 5-level EQ-5D (EQ-5D-5L) (4) Shortness of Breath Scale | / | (1) Routine blood test (creatinine, sodium and potassium levels) (2) Brain natriuretic peptide (BNP) | (1) Weight (2) Blood pressure (3) Heart rate | (1), (2), (3) Daily |
| Modena et al., 2018 [19] | (1) Perceived Stress Scale Survey | / | / | (1) Pulse wave velocity (PWV) (2) Physical activity level (3) Blood pressure (4) Heart rate (5) Sleep duration (6) Weight (BMI) | (1), (3), (4), (6) ≥2 days per week (2) Tracked using built-in activity trackers on the participants’ smartphone (5) Daily |
| McManus et al., 2019 [18] | (1) Center for Epidemiologic Studies Depression Scale, (CES-D) (2) Physical activity index (FHS) | (1) Socio-demographics (2) Medication use (3) Self-reported risk factors (4) Smoking (5) Alcohol use (6) Health survey (7) CVD history/non-CVD medical history | / | (1) Blood pressure (2) Heart rate | (1) 1 day per week at the same day (2) Daily |
| Guo et al., 2019a [17] | / | (1) Medicine usage (2) Visits for AF-related adverse outcomes (3) Hospitalizations | (1) HAS-BLED score 1 (2) Congestive heart failure, hypertension, age > 75, diabetes, stroke, vascular disease, age 65–74 years, and sex category (CHA2DS2-VASc) (3) Female sex, age, medical history, treatment, tobacco use, race score (SAMe-T2T2R) | (1) Heart rate | (1) Every 10 min |
| Guo et al., 2019 [16] | (1) Patient-reported thromboembolism or bleeding events (2) Atrial Fibrillation (AF) symptom assessment scale from the European Heart Rhythm Association (EHRA) | (1) Drug adherence (dose and drug use) (2) Patient-specific cost diary | (1) Hemoglobin, liver, renal function (2) HAS-BLED score 1 | (1) Blood pressure (2) Heart rate | Unknown |
| Koehler et al., 2018 [23] | (1) Minnesota Living with Heart Failure Questionnaire (MLHFQ) (2) Self-rated health status (scale range 1–5) | / | (1) Follow Up Visit Biomarker (2) N-terminal prohormone brain natriuretic peptide (NT-proBNP) (3) Mid-regional proadrenomedullin (MR-proADM) | (1) Weight (2) Blood pressure (3) Heart rate (4) Heart rhythm peripheral capillary oxygen saturation (SpO2) | (1), (2), (3), (4) Daily |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Kinast, B.; Lutz, M.; Schreiweis, B. Telemonitoring of Real-World Health Data in Cardiology: A Systematic Review. Int. J. Environ. Res. Public Health 2021, 18, 9070. https://doi.org/10.3390/ijerph18179070
Kinast B, Lutz M, Schreiweis B. Telemonitoring of Real-World Health Data in Cardiology: A Systematic Review. International Journal of Environmental Research and Public Health. 2021; 18(17):9070. https://doi.org/10.3390/ijerph18179070
Chicago/Turabian StyleKinast, Benjamin, Matthias Lutz, and Björn Schreiweis. 2021. "Telemonitoring of Real-World Health Data in Cardiology: A Systematic Review" International Journal of Environmental Research and Public Health 18, no. 17: 9070. https://doi.org/10.3390/ijerph18179070
APA StyleKinast, B., Lutz, M., & Schreiweis, B. (2021). Telemonitoring of Real-World Health Data in Cardiology: A Systematic Review. International Journal of Environmental Research and Public Health, 18(17), 9070. https://doi.org/10.3390/ijerph18179070






