In Situ Measurement of Airborne Particle Concentration in a Real Dental Office: Implications for Disease Transmission
Abstract
:1. Introduction
2. Materials and Methods
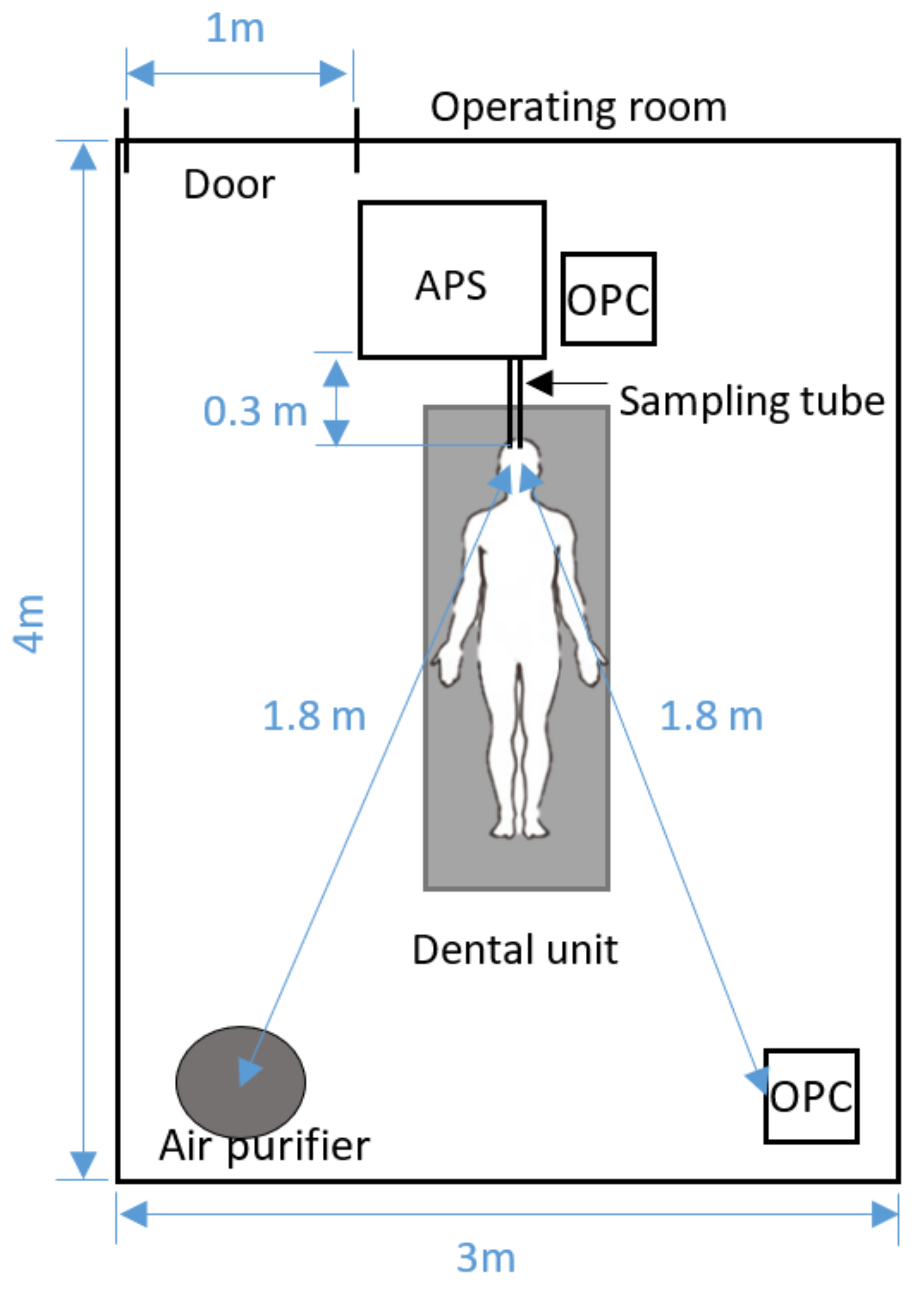
2.1. Measurement Site and Instruments
2.2. Study Design of Dental Operation on Pig Jaw
2.3. Study Design of Real Operation with the Patient
3. Results and Discussion
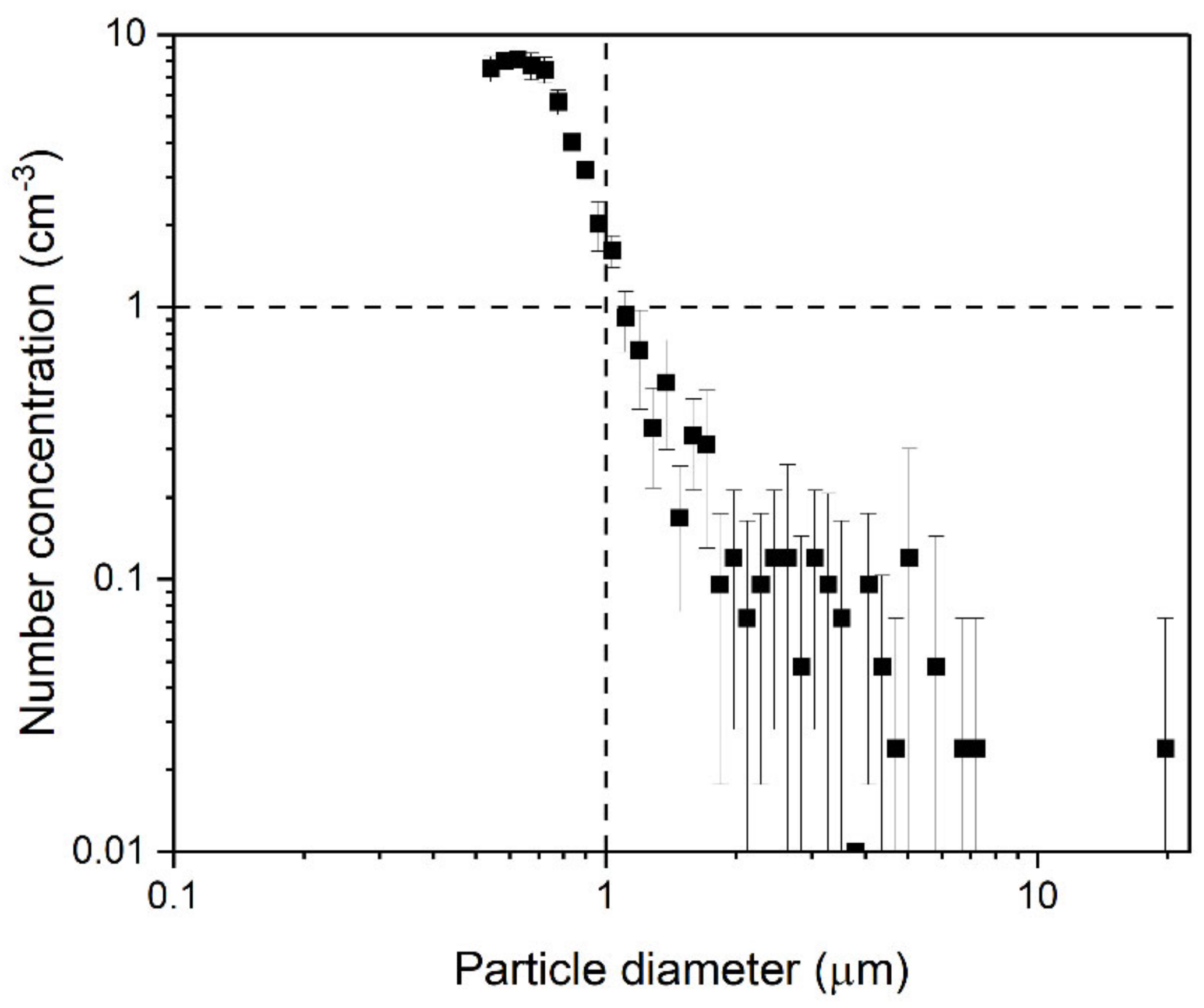
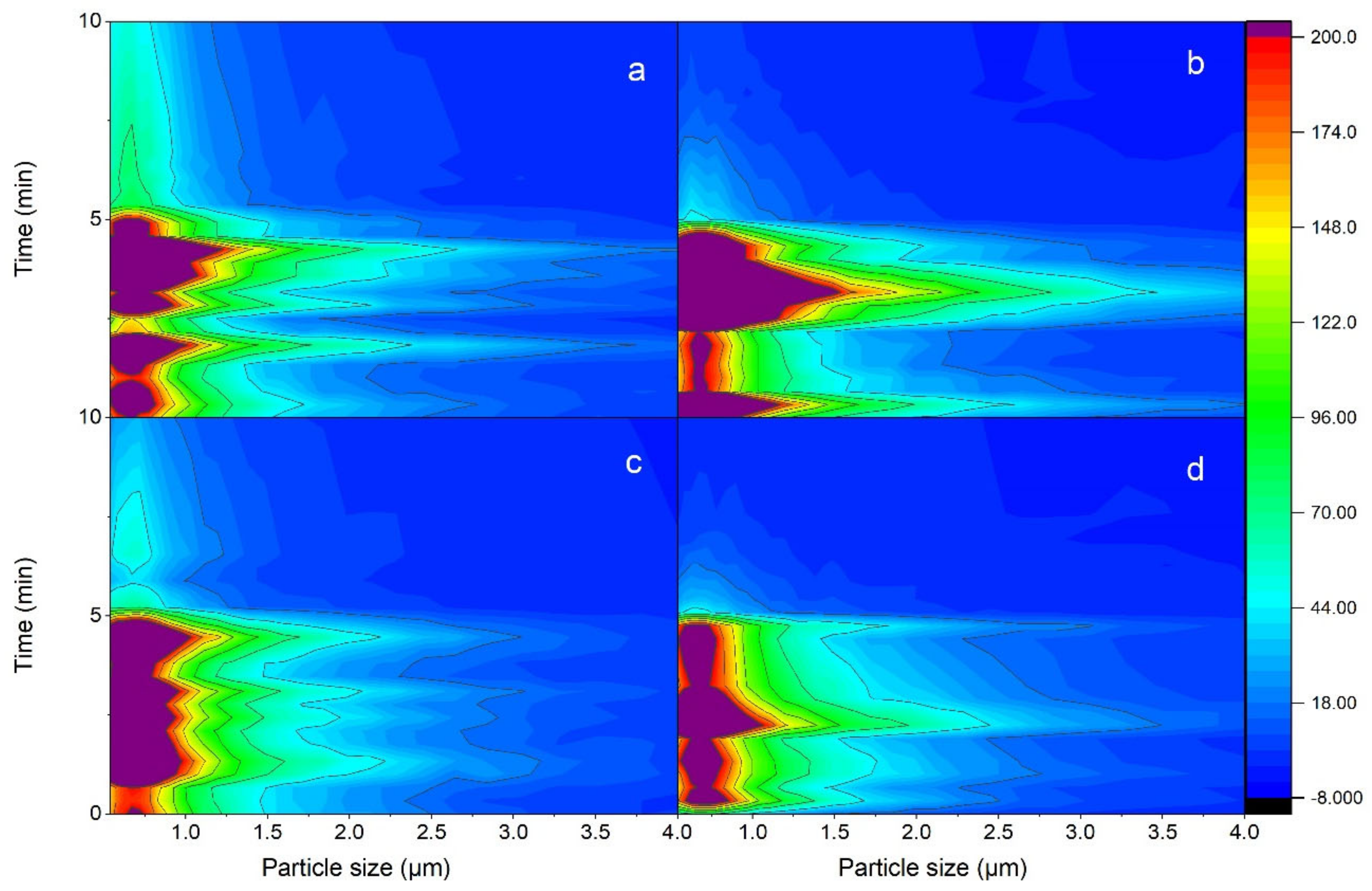
3.1. Particle Generation during Operation for Five Minutes
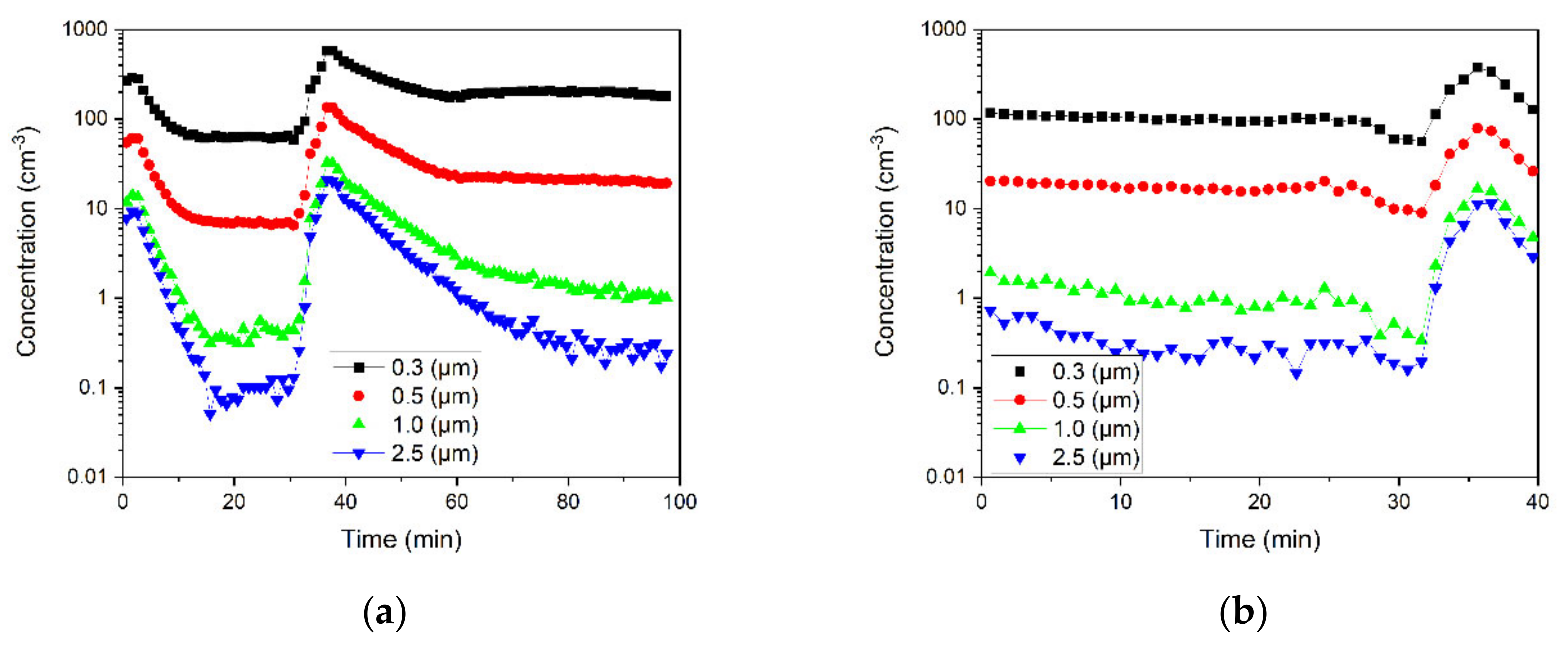
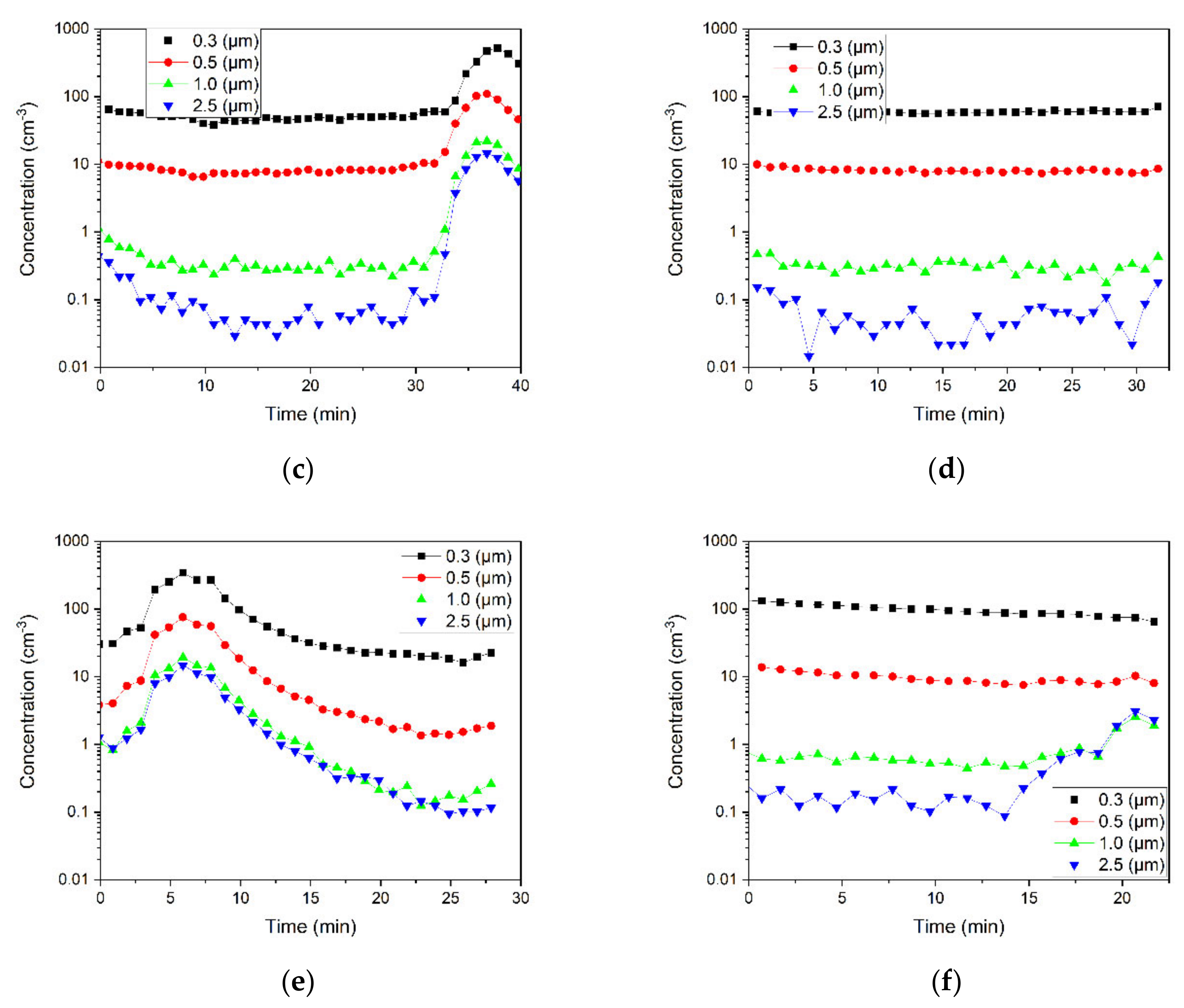
3.2. Temporal Change of Particle Concentrations in the Generated Zone
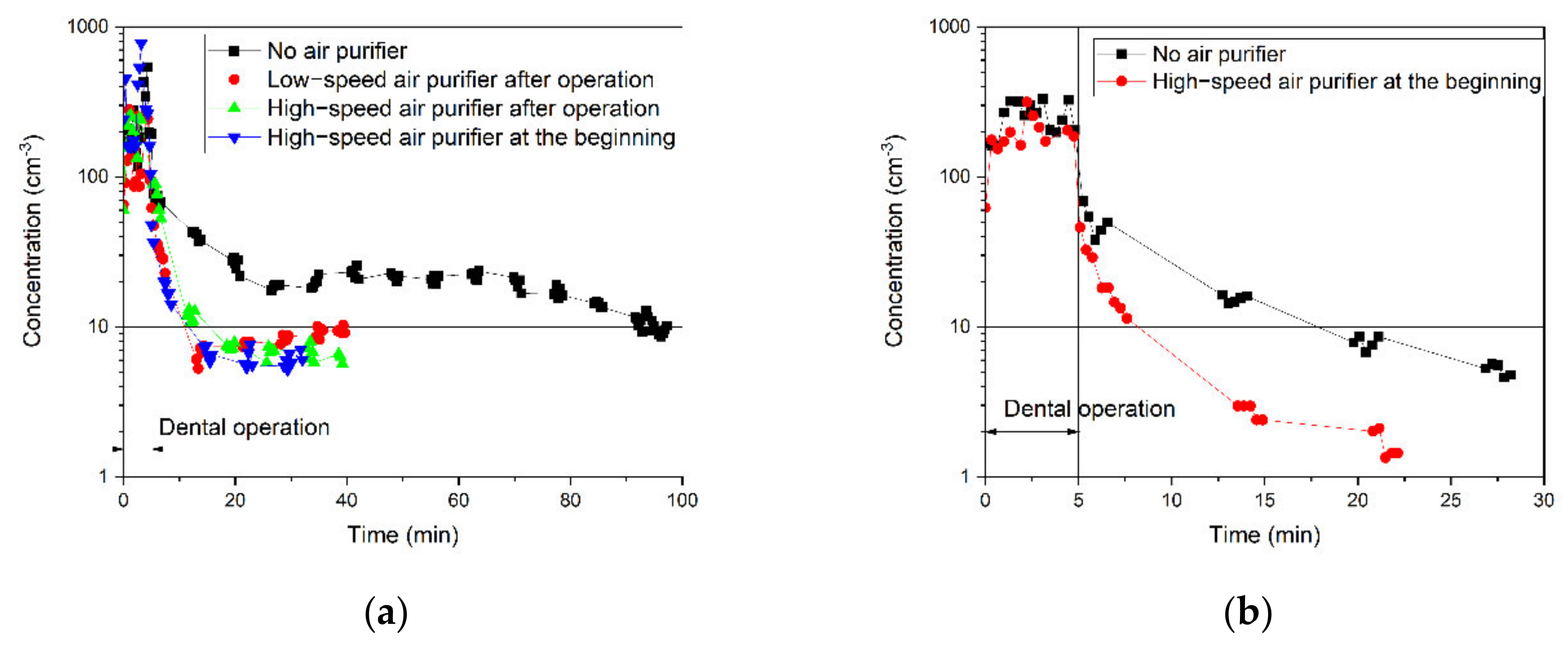
3.2.1. Effects of Air Purifier and the Door Condition on the Removal of 0.5 μm Particles
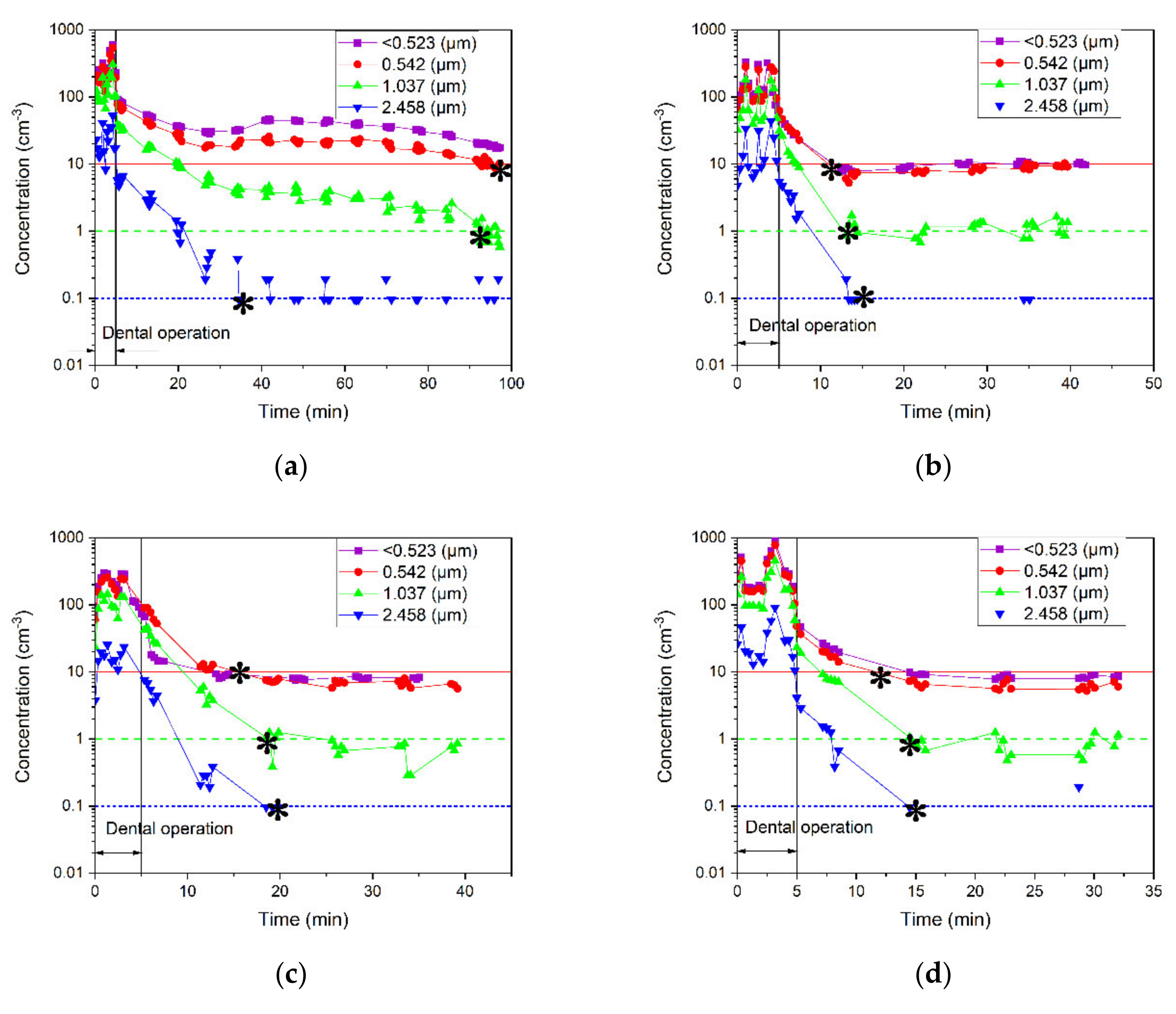
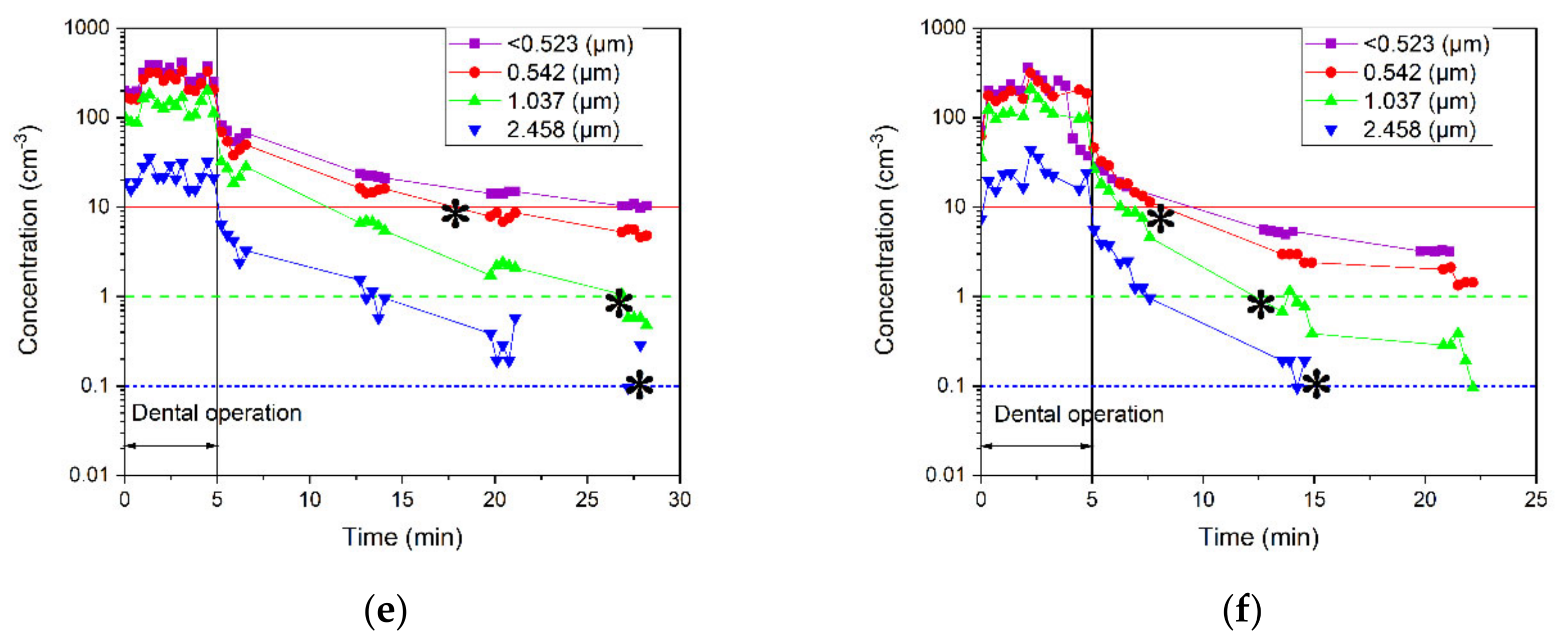
3.2.2. Effects of Particles Size on Particle Removal
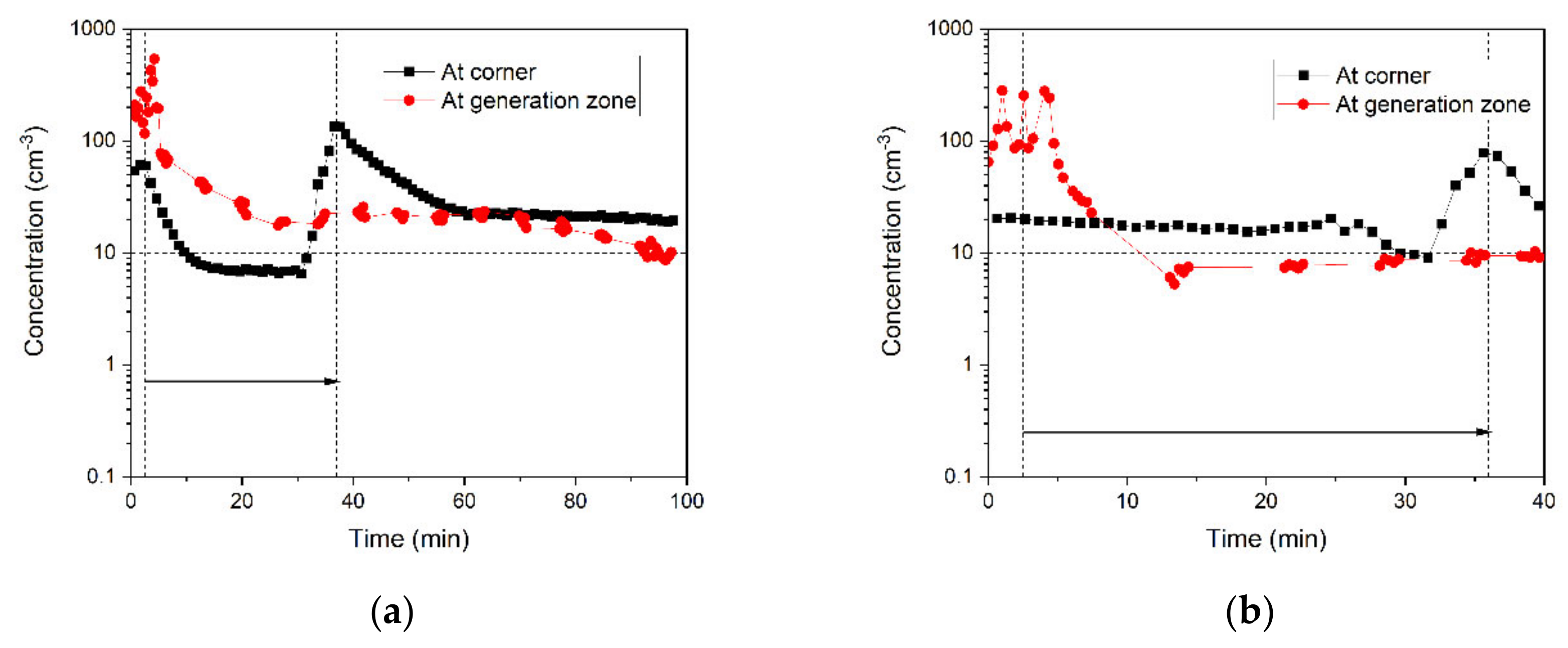
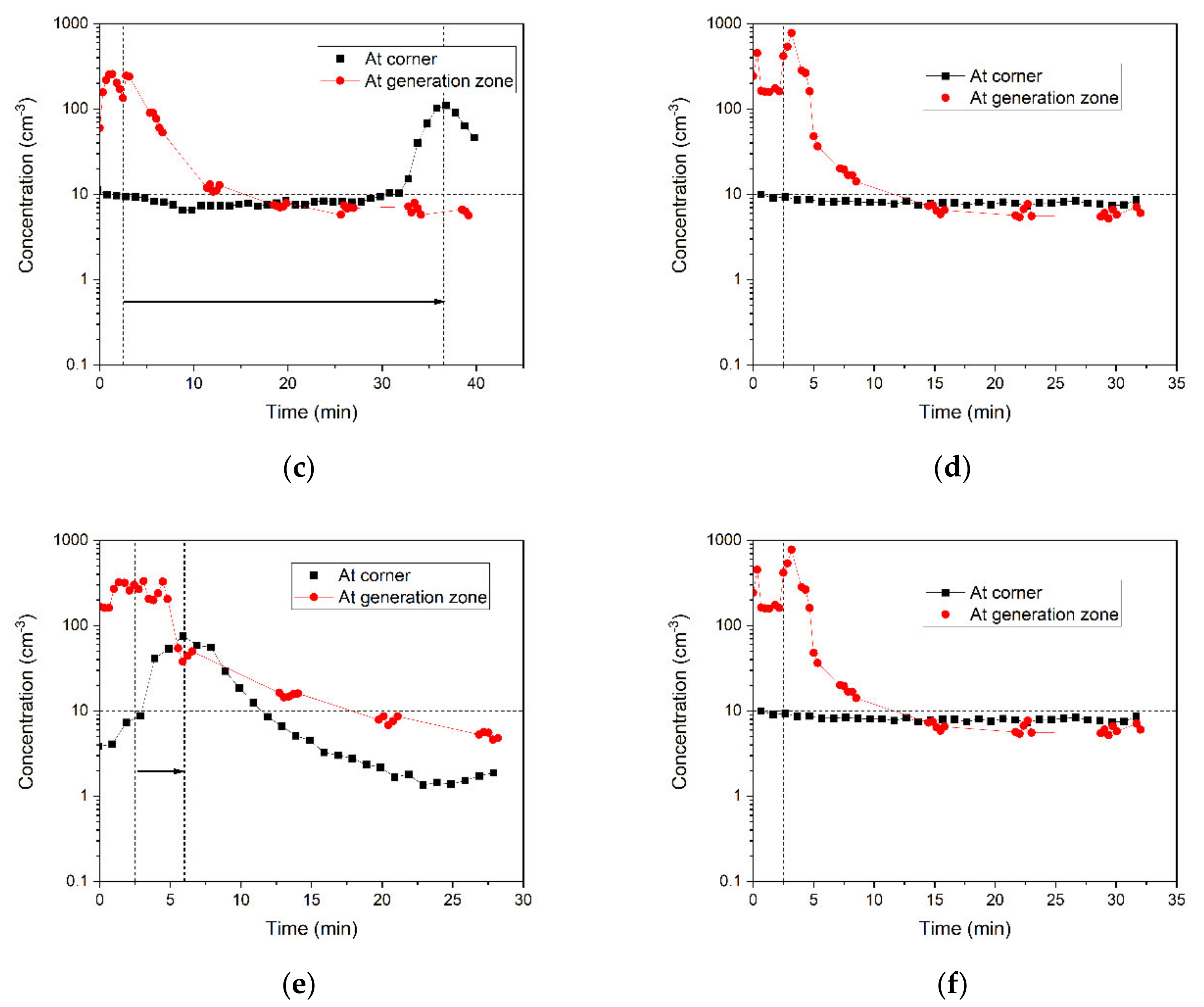
3.3. Spatial and Temporal Change of Particle Concentrations in the Corner of the Dental Office
3.3.1. Effects of Air Purifier and the Door Condition on the Spread and Removal of 0.5-μm Particles
3.3.2. Effects of Particle Size on the Spread and Removal
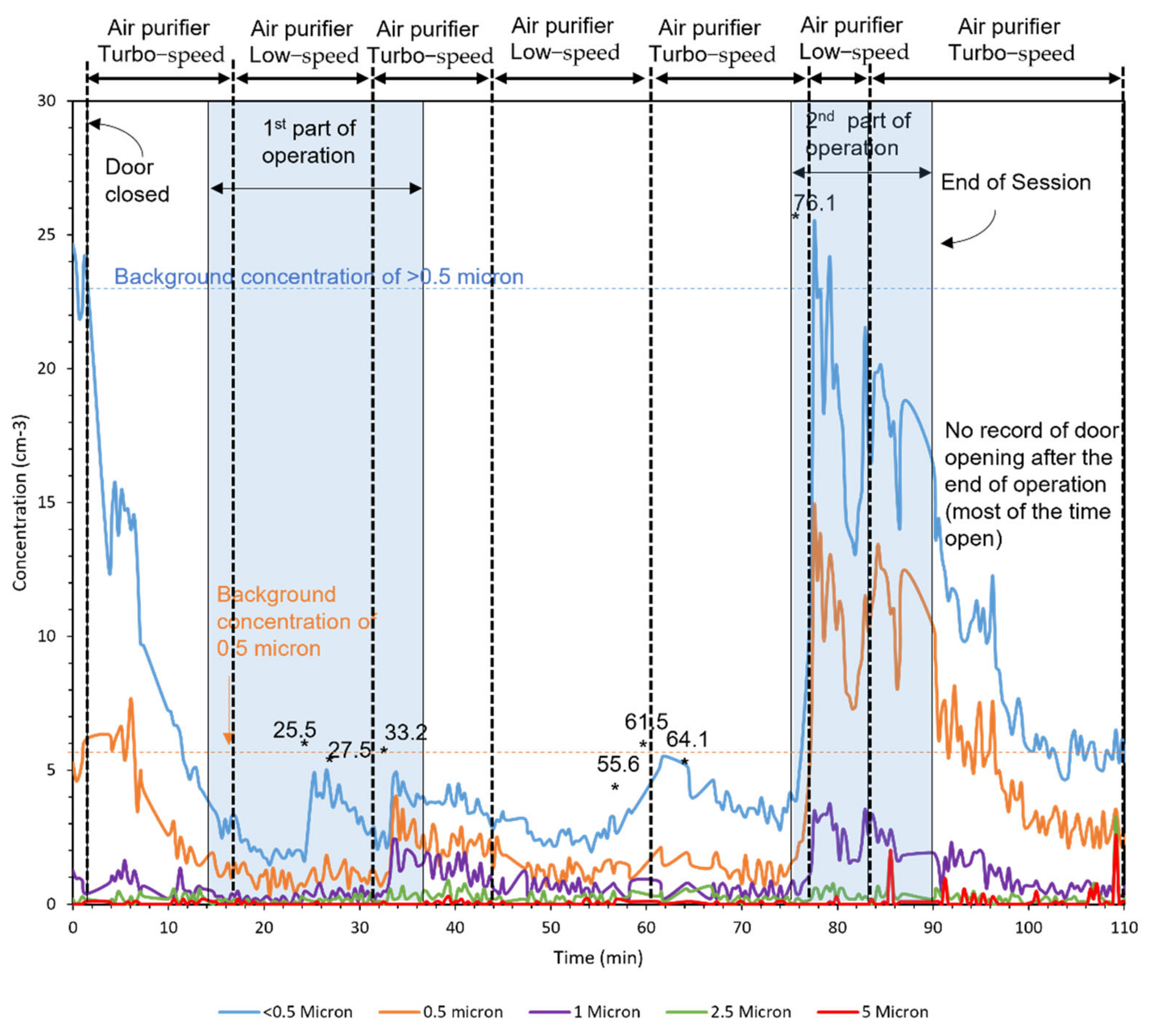
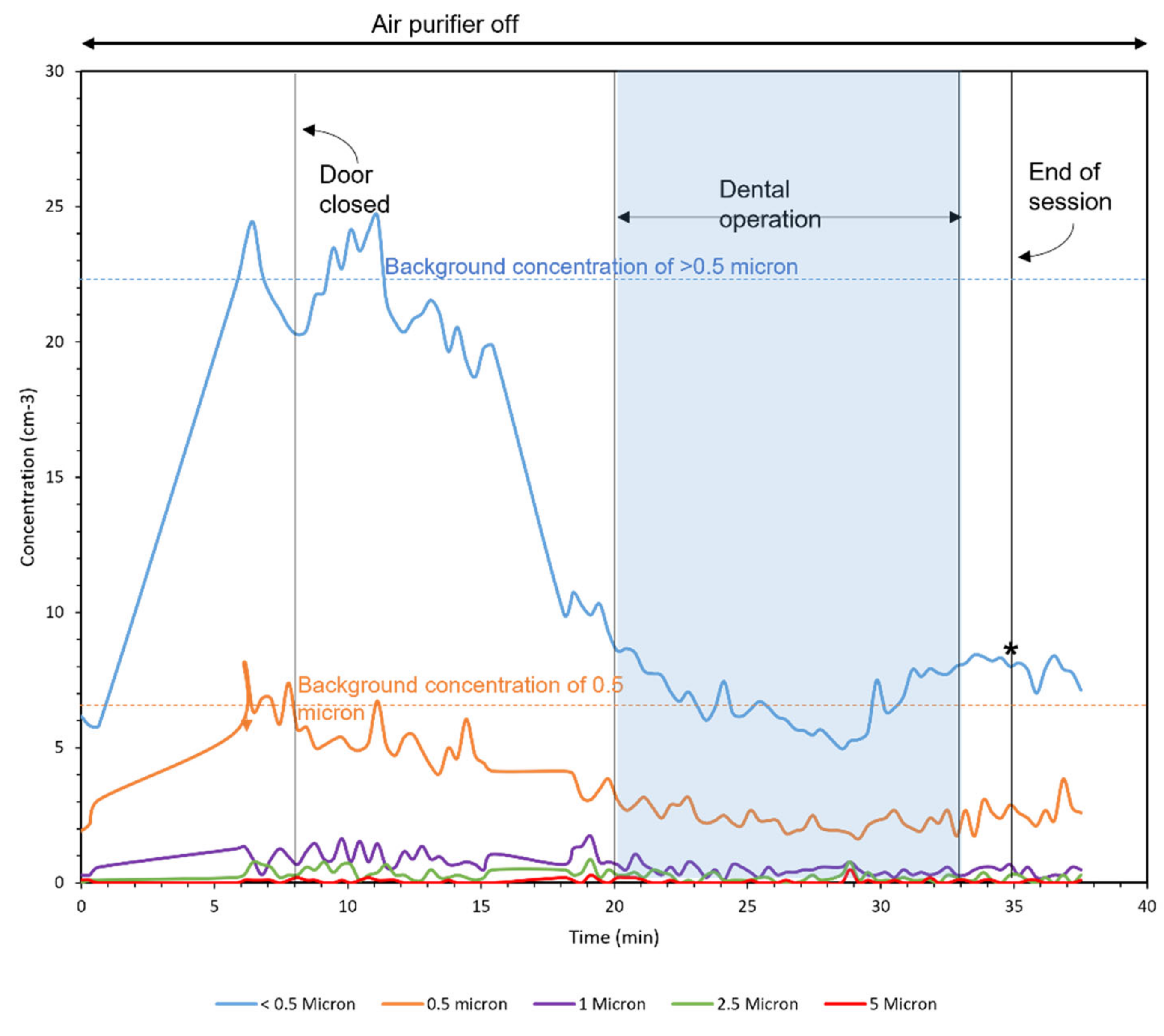
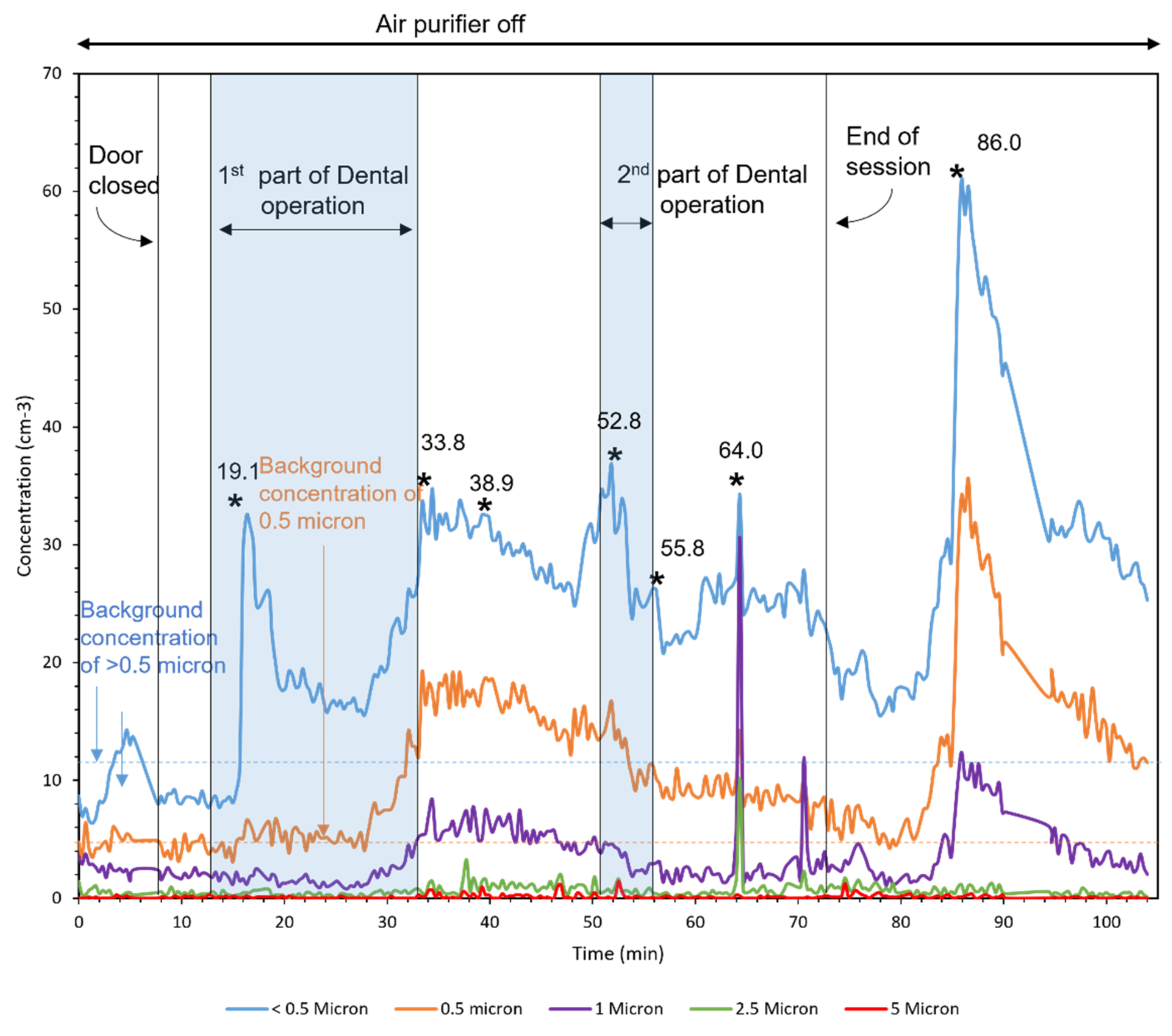
3.4. Field Campaign with REAL Patients
4. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Harrel, S.K.; Molinari, J. Aerosols and splatter in dentistry: A brief review of the literature and infection control implications. J. Am. Dent. Assoc. 2004, 135, 429–437. [Google Scholar] [CrossRef] [PubMed]
- Taira, M.; Sasaki, M.; Kimura, S.; Araki, Y. Characterization of aerosols and fine particles produced in dentistry and their health risk assessments. Nano Biomed. 2009, 1, 9–15. [Google Scholar]
- Gamio, L. The workers who face the greatest coronavirus risk. The New York Times, 15 March 2020. Available online: https://www.nytimes.com/interactive/2020/03/15/business/economy/coronavirus-worker-risk.html(accessed on 24 August 2021).
- Rothe, C.; Schunk, M.; Sothmann, P.; Bretzel, G.; Froeschl, G.; Wallrauch, C.; Zimmer, T.; Thiel, V.; Janke, C.; Guggemos, W. Transmission of 2019-nCoV infection from an asymptomatic contact in Germany. N. Engl. J. Med. 2020, 382, 970–971. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Peng, X.; Xu, X.; Li, Y.; Cheng, L.; Zhou, X.; Ren, B. Transmission routes of 2019-nCoV and controls in dental practice. Int. J. Oral Sci. 2020, 12, 1–6. [Google Scholar] [CrossRef]
- Kadaifciler, D.G.; Ökten, S.; Sen, B. Mycological contamination in dental unit waterlines in Istanbul, Turkey. Braz. J. Microbiol. 2013, 44, 977–981. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Tellier, R.; Li, Y.; Cowling, B.J.; Tang, J.W. Recognition of aerosol transmission of infectious agents: A commentary. BMC Infect. Dis. 2019, 19, 101. [Google Scholar] [CrossRef]
- World Health Organization. Modes of Transmission of Virus Causing COVID-19: Implications for IPC Precaution Recommendations: Scientific Brief, 27 March 2020. Licencia: CC BY-NC-SA 3.0 IGO. Available online: https://apps.who.int/iris/handle/10665/331616 (accessed on 24 August 2021).
- Rupf, S.; Berger, H.; Buchter, A.; Harth, V.; Ong, M.F.; Hannig, M. Exposure of patient and dental staff to fine and ultrafine particles from scanning spray. Clin. Oral Investig. 2015, 19, 823–830. [Google Scholar] [CrossRef]
- Žitnik, M.; Kastelic, A.; Rupnik, Z.; Pelicon, P.; Vaupetič, P.; Bučar, K.; Novak, S.; Samardžija, Z.; Matsuyama, S.; Catella, G. Time-resolved measurements of aerosol elemental concentrations in indoor working environments. Atmos. Environ. 2010, 44, 4954–4963. [Google Scholar] [CrossRef]
- Maynard, A.D.; Kuempel, E.D. Airborne nanostructured particles and occupational health. J. Nanoparticle Res. 2005, 7, 587–614. [Google Scholar] [CrossRef]
- Day, C.J.; Price, R.; Sandy, J.R.; Ireland, A.J. Inhalation of aerosols produced during the removal of fixed orthodontic appliances: A comparison of 4 enamel cleanup methods. Am. J. Orthod. Dentofac. Orthop. 2008, 133, 11–17. [Google Scholar] [CrossRef] [PubMed]
- Burnett, R.T.; Pope, C.A., III; Ezzati, M.; Olives, C.; Lim, S.S.; Mehta, S.; Shin, H.H.; Singh, G.; Hubbell, B.; Brauer, M. An integrated risk function for estimating the global burden of disease attributable to ambient fine particulate matter exposure. Environ. Health Perspect. 2014, 122, 397–403. [Google Scholar] [CrossRef]
- Lelieveld, J.; Evans, J.S.; Fnais, M.; Giannadaki, D.; Pozzer, A. The contribution of outdoor air pollution sources to premature mortality on a global scale. Nature 2015, 525, 367. [Google Scholar] [CrossRef]
- Affairs, A.C.O.S.; Practice, A.C.O.D. Infection control recommendations for the dental office and the dental laboratory. J. Am. Dent. Assoc. 1996, 127, 672–680. [Google Scholar]
- Safety, O.; Administration, H. Occupational exposure to bloodborne pathogens: Final rule. Fed. Regist. 1991, 56, 64004–64182. [Google Scholar]
- Morawska, L.; Milton, D.K. It is time to address airborne transmission of COVID-19. Clin. Infect. Dis. 2020, 7, ciaa939. [Google Scholar] [CrossRef]
- Mahmud, P.K.; Ali, S.M.; Sabir, D.K. Impacts of Novel Pandemic Coronavirus (COVID-19) Outbreak on Dental Practice: A Review of the Current Literature. Edorium J. Dent. 2020, 8, 100040D01PM2020. [Google Scholar] [CrossRef]
- Izzetti, R.; Nisi, M.; Gabriele, M.; Graziani, F. COVID-19 transmission in dental practice: Brief review of preventive measures in Italy. J. Dent. Res. 2020, 99, 1030–1038. [Google Scholar] [CrossRef]
- World Health Organization. Considerations for the Provision of Essential Oral Health Services in the Context of COVID-19: Interim Guidance, 3 August 2020. Available online: https://apps.who.int/iris/handle/10665/333625 (accessed on 24 August 2021).
- RCDSO. COVID-19: Managing Infection Risks During In-Person Dental Care; Royal College of Dental Surgeons of Ontario: Toronto, ON, Canada, 2020. [Google Scholar]
- Pippin, D.J.; Verderame, R.A.; Weber, K.K. Efficacy of face masks in preventing inhalation of airborne contaminants. J. Oral Maxillofac. Surg. 1987, 45, 319–323. [Google Scholar] [CrossRef]
- Timmerman, M.; Menso, L.; Steinfort, J.; Van Winkelhoff, A.; Van Der Weijden, G. Atmospheric contamination during ultrasonic scaling. J. Clin. Periodontol. 2004, 31, 458–462. [Google Scholar] [CrossRef] [PubMed]
- Avasth, A. High Volume Evacuator (HVE) in reducing aerosol-an exploration worth by clinicians. J. Dent. Health Oral Disord. 2018, 9, 165–166. [Google Scholar] [CrossRef] [Green Version]
- Zhao, B.; Liu, Y.; Chen, C. Air purifiers: A supplementary measure to remove airborne SARS-CoV-2. Build. Environ. 2020, 177, 106918. [Google Scholar] [CrossRef]
- Chen, C.; Zhao, B.; Cui, W.; Dong, L.; An, N.; Ouyang, X. The effectiveness of an air cleaner in controlling droplet/aerosol particle dispersion emitted from a patient’s mouth in the indoor environment of dental clinics. J. R. Soc. Interface 2010, 7, 1105–1118. [Google Scholar] [CrossRef] [PubMed]
- Zhao, B.; An, N.; Chen, C. Using air purifier as a supplementary protective measure in dental clinics during the COVID-19 pandemic. Infect. Control. Hosp. Epidemiol. 2021, 42, 493. [Google Scholar] [CrossRef] [PubMed]
- Polednik, B. Aerosol and bioaerosol particles in a dental office. Environ. Res. 2014, 134, 405–409. [Google Scholar] [CrossRef] [PubMed]
- Sotiriou, M.; Ferguson, S.F.; Davey, M.; Wolfson, J.M.; Demokritou, P.; Lawrence, J.; Sax, S.N.; Koutrakis, P. Measurement of particle concentrations in a dental office. Environ. Monit. Assess. 2008, 137, 351. [Google Scholar] [CrossRef] [PubMed]
- Raynor, P.C.; Cebula, J.I.; Spangenberger, J.S.; Olson, B.A.; Dasch, J.M.; D’Arcy, J.B. Assessing potential nanoparticle release during nanocomposite shredding using direct-reading instruments. J. Occup. Environ. Hyg. 2012, 9, 1–13. [Google Scholar] [CrossRef]
- Van Landuyt, K.L.; Hellack, B.; Van Meerbeek, B.; Peumans, M.; Hoet, P.; Wiemann, M.; Kuhlbusch, T.; Asbach, C. Nanoparticle release from dental composites. Acta Biomater. 2014, 10, 365–374. [Google Scholar] [CrossRef]
- Lang, A.; Ovsenik, M.; Verdenik, I.; Remškar, M.; Oblak, Č. Nanoparticle concentrations and composition in a dental office and dental laboratory: A pilot study on the influence of working procedures. J. Occup. Environ. Hyg. 2018, 15, 441–447. [Google Scholar] [CrossRef]
- Simu, M.; Borzan, C.; Mesaros, M.; Chiriac, M.; Radu, T. Complex characterization of dental office aerosols reveals important loads of risk elements for the human health. Dig. J. Nanomater. Biostructures 2014, 9, 1429–1438. [Google Scholar]
- Lipinski, T.; Ahmad, D.; Serey, N.; Jouhara, H. Review of ventilation strategies to reduce the risk of disease transmission in high occupancy buildings. Int. J. Thermofluids 2020, 7–8, 100045. [Google Scholar] [CrossRef]
- Juraeva, M.; Park, B.H.; Ryu, K.J.; Song, D.J. Designing high-speed dental air-turbine handpiece by using a computational approach. Int. J. Precis. Eng. Manuf. 2017, 18, 1403–1407. [Google Scholar] [CrossRef]
- Popowics, T.; Rensberger, J.; Herring, S. Enamel microstructure and microstrain in the fracture of human and pig molar cusps. Arch. oral Biol. 2004, 49, 595–605. [Google Scholar] [CrossRef]
- Lopes, F.M.; Markarian, R.A.; Sendyk, C.L.; Duarte, C.P.; Arana-Chavez, V.E. Swine teeth as potential substitutes for in vitro studies in tooth adhesion: A SEM observation. Arch. oral Biol. 2006, 51, 548–551. [Google Scholar] [CrossRef] [PubMed]
- Marshall, J.S.; Li, S. Adhesive Particle Flow; Cambridge University Press: Cambridge, UK, 2014. [Google Scholar]
- Tan, Z. Air Pollution and Greenhouse Gases: From Basic Concepts to Engineering Applications for Air Emission Control; Springer: Berlin/Heidelberg, Germany, 2014. [Google Scholar]
- Zemouri, C.; Volgenant, C.; Buijs, M.; Crielaard, W.; Rosema, N.; Brandt, B.; Laheij, A.; De Soet, J. Dental aerosols: Microbial composition and spatial distribution. J. Oral Microbiol. 2020, 12, 1762040. [Google Scholar] [CrossRef] [PubMed]
- Tsuda, A.; Henry, F.S.; Butler, J.P. Particle transport and deposition: Basic physics of particle kinetics. Compr. Physiol. 2011, 3, 1437–1471. [Google Scholar]
| Case No. | Dental Operation Duration | Door (Open/Close) | Air Purifier | ||
|---|---|---|---|---|---|
| On/Off | Fan Speed | Air Cleaning Starting Time | |||
| 1 | 5 min | Close | Off | - | - |
| 2 | 5 min | Close | On | Low (153 CFM) | After 5 min of operation |
| 3 | 5 min | Close | On | High (312 CFM) | After 5 min of operation |
| 4 | 5 min | Close | On | High (312 CFM) | At the beginning of the operation |
| 5 | 5 min | Open | Off | - | - |
| 6 | 5 min | Open | On | High (312 CFM) | At the beginning of the operation |
| Operation No. | Dental Operation | Room Size | Air Purifier | Room Condition before the Operation | Room Condition after Operation | |||
|---|---|---|---|---|---|---|---|---|
| Type of Operation | Duration | Temperature (°C) | Humidity (%) | Temperature (°C) | Humidity (%) | |||
| 1 | Filling with 1 root canal High/low-speed handpieces | 88 min | Large (Room A) | On | 21.9 | 60 | 23.6 | 58 |
| 2 | Filling with 1 root canal High/low-speed handpieces | 33 min | Large (Room A) | Off | 24.7 | 54 | 24.9 | 49 |
| 3 | Crown insertion High/low-speed handpieces | 73 min | Small (Room B) | Off | 23.3 | 51 | 24.3 | 51 |
| Case No. | Concentration >200 (1/cm3) | Concentration 200–70 (1/cm3) | Concentration 70–18 (1/cm3) |
|---|---|---|---|
| 1 | 0.5–1.3 | 1.3–2 | 2–3.7 |
| 4 | 0.5–1.5 | 1.5–2.8 | 2.8–4 |
| 5 | 0.5–1 | 1–1.5 | 1.5–3 |
| 6 | 0.5–1.4 | 1.4–2 | 2–3.5 |
| No. | Door | Air Purifier | Removal Time at Generation Zone (min) | ||||
|---|---|---|---|---|---|---|---|
| On/Off | Fan Mode (Flow Rate) | Air Cleaning Starting Time | 0.5 μm | 1 μm | 2.5 μm | ||
| 1 | Close | Off | - | - | 95 | 92 | 35 |
| 2 | Close | On | Low (153 CFM) | After dental operation | 11 | 13 | 15 |
| 3 | Close | On | High (312 CFM) | After dental operation | 15 | 18.5 | 20 |
| 4 | Close | On | High (312 CFM) | At the beginning of the dental operation | 12 | 14.5 | 15 |
| 5 | Open | Off | - | - | 18 | 26.5 | 28 |
| 6 | Open | On | High (312 CFM) | At the beginning of the dental operation | 8 | 12.5 | 15 |
| No. | Door | Air Purifier | Travel Time (min) | Concentration Ratio | ||||||
|---|---|---|---|---|---|---|---|---|---|---|
| On/Off | Fan Mode (Flow Rate) | Air Cleaning Starting Time | 0.5 μm | 1 μm | 2.5 μm | 0.5 μm | 1 μm | 2.5 μm | ||
| 1 | Close | Off | - | - | 37 | 37 | 37 | 0.5 | 0.16 | 0.66 |
| 2 | Close | On | Low (153 CFM) | After dental operation | 36 | 36 | 36 | 0.33 | 0.1 | 0.4 |
| 3 | Close | On | High (312 CFM) | After dental operation | 36.5 | 36.5 | 36.5 | 0.33 | 0.11 | 0.5 |
| 4 | Close | On | High (312 CFM) | At the beginning of the dental operation | - | - | - | - | - | - |
| 5 | Open | Off | - | - | 6 | 6 | 6 | 0.26 | 0.11 | 0.5 |
| 6 | Open | On | High (312 CFM) | At the beginning of the dental operation | - | 21 | 21 | - | 0.016 | 0.06 |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Razavi, M.; Butt, Z.A.; Chen, H.; Tan, Z. In Situ Measurement of Airborne Particle Concentration in a Real Dental Office: Implications for Disease Transmission. Int. J. Environ. Res. Public Health 2021, 18, 8955. https://doi.org/10.3390/ijerph18178955
Razavi M, Butt ZA, Chen H, Tan Z. In Situ Measurement of Airborne Particle Concentration in a Real Dental Office: Implications for Disease Transmission. International Journal of Environmental Research and Public Health. 2021; 18(17):8955. https://doi.org/10.3390/ijerph18178955
Chicago/Turabian StyleRazavi, Maryam, Zahid Ahmad Butt, Helen Chen, and Zhongchao Tan. 2021. "In Situ Measurement of Airborne Particle Concentration in a Real Dental Office: Implications for Disease Transmission" International Journal of Environmental Research and Public Health 18, no. 17: 8955. https://doi.org/10.3390/ijerph18178955
APA StyleRazavi, M., Butt, Z. A., Chen, H., & Tan, Z. (2021). In Situ Measurement of Airborne Particle Concentration in a Real Dental Office: Implications for Disease Transmission. International Journal of Environmental Research and Public Health, 18(17), 8955. https://doi.org/10.3390/ijerph18178955








