The Families and Schools for Health Project: A Longitudinal Cluster Randomized Controlled Trial Targeting Children with Overweight and Obesity
Abstract
1. Introduction
1.1. Conceptual Model: Families and Schools as Contexts for Intervention
1.1.1. Family Context
1.1.2. School Context
1.2. Current Study
2. Materials and Methods
2.1. Participants
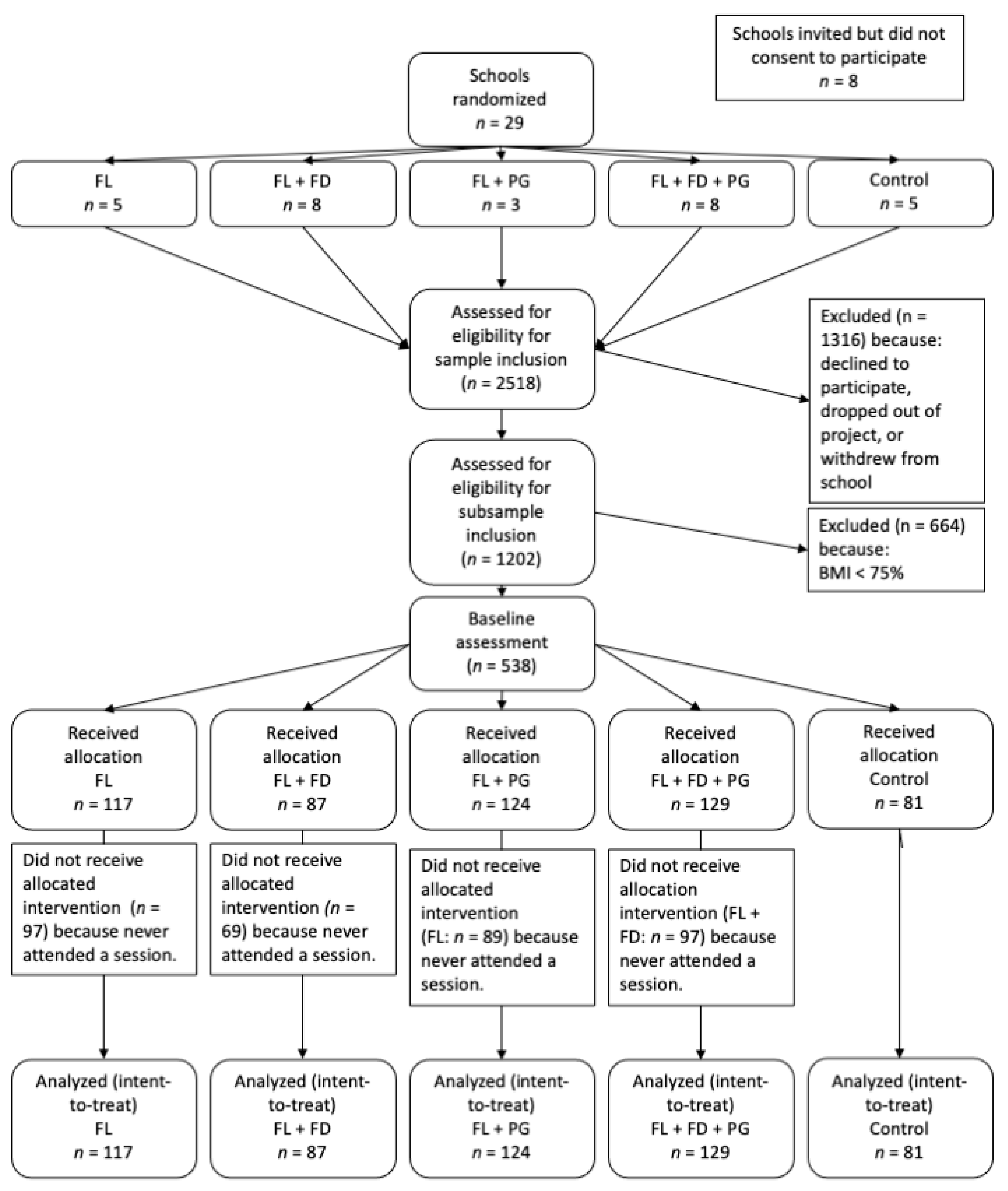
2.1.1. Recruitment and Randomization
2.1.2. Sample Characteristics
2.2. Procedures and Measures
2.3. Interventions
2.3.1. Family Psychoeducational Groups
2.3.2. Peer Group (PG) Intervention
2.3.3. Control Group
2.4. Analytic Plan
3. Results
3.1. Control Group
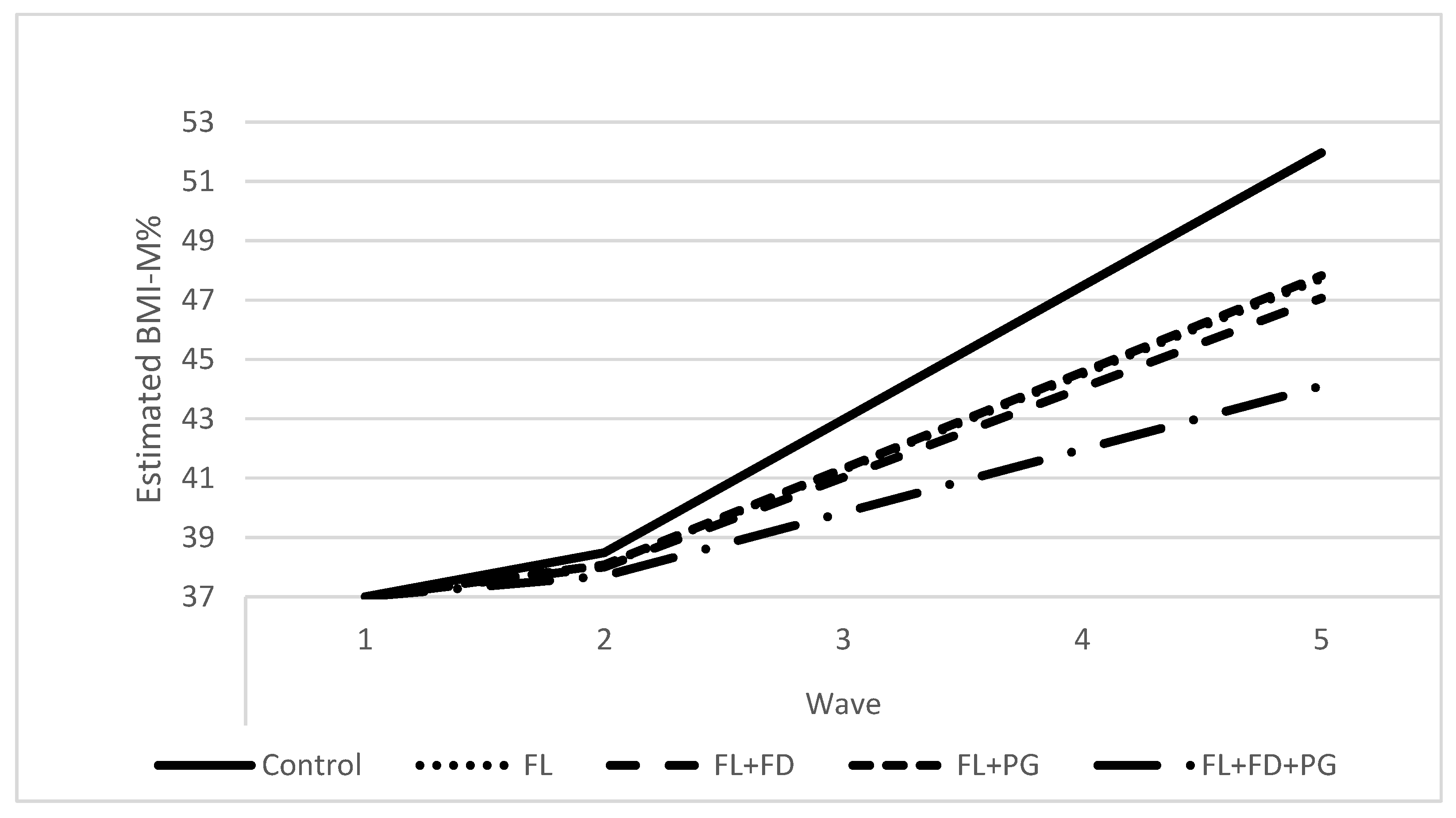
3.2. Intervention Effects
4. Discussion
Limitations
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Ogden, C.L.; Fryar, C.D.; Hales, C.; Hales, C.; Carroll, M.D.; Aoki, Y.; Freedman, D.S. Differences in obesity. JAMA 2018, 319, 2410–2418. [Google Scholar] [CrossRef]
- Skinner, A.C.; Ravanbakht, S.N.; Skelton, J.A.; Perrin, E.M.; Armstrong, S.C. Prevalence of obesity and severe obesity in U.S. children, 1999–2016. Pediatrics 2018, 141, e20173459. [Google Scholar] [CrossRef] [PubMed]
- Smith, J.D.; Egan, K.N.; Montaño, Z.; Dawson-McClure, S.; Jake-Schoffman, D.E.; Larson, M.; St. George, S.M. A developmental cascade perspective of paediatric obesity: A conceptual model and scoping review. Health Psychol. Rev. 2018, 12, 271–293. [Google Scholar] [CrossRef]
- East, P.; Delker, E.; Blanco, E.; Burrows, R.; Lozoff, B.; Gahagan, S. Home and family environment related to development of obesity: A 21-year longitudinal study. Child. Obes. 2019, 15, 156–166. [Google Scholar] [CrossRef]
- Sleddens, E.F.C.; Gerards, S.M.P.L.; Thijs, C.; De Vries, N.K.; Kremers, S.P.J. General parenting, childhood overweight and obesity-inducing behaviors: A review. Int. J. Pediatr. Obes. 2011, 6, e12–e27. [Google Scholar] [CrossRef]
- Gray, W.N.; Kahhan, N.A.; Janicke, D.M. Peer victimization and pediatric obesity: A review of the literature. Psychol. Sch. 2009, 46, 720–727. [Google Scholar] [CrossRef]
- Harrist, A.W.; Swindle, T.M.; Hubbs-Tait, L.; Topham, G.L.; Shriver, L.H.; Page, M.C. The social and emotional lives of overweight, obese, and severely obese children. Child. Dev. 2016, 87, 1564–1580. [Google Scholar] [CrossRef]
- Gable, S.; Krull, J.L.; Chang, Y. Implications of overweight onset and persistence for social and behavioral development between kindergarten entry and third grade. Appl. Dev. Sci. 2009, 13, 88–103. [Google Scholar] [CrossRef]
- Harrist, A.W.; Topham, G.L.; Hubbs-Tait, L.; Page, M.C.; Kennedy, T.S.; Shriver, L.H. What developmental science can contribute to a transdisciplinary understanding of childhood obesity: An interpersonal and intrapersonal risk model. Child Dev. Perspect. 2012, 6, 445–455. [Google Scholar] [CrossRef]
- US Preventative Task Force. Screening for obesity in children and adolescents: US Preventive Services Task Force recommendation statement. Clin. Rev. Educ. 2017, 317, 2417–2426. [Google Scholar] [CrossRef]
- Kidwell, K.M.; Nelson, T.D.; Nelson, J.M.; Espy, K.A. A longitudinal study of maternal and child internalizing symptoms predicting early adolescent emotional eating. J. Pediatr. Psychol. 2017, 42, 445–456. [Google Scholar] [CrossRef][Green Version]
- Altman, M.; Wilfley, D.E. Evidence update on the treatment of overweight and obesity in children and adolescents. JCCAP 2015, 44, 521–537. [Google Scholar] [CrossRef]
- Weaver, S.P.; Kelley, L.; Griggs, J.; Weems, S.; Meyer, M.R.U. Fit and Healthy Family Camp for engaging families in a child obesity intervention. Fam. Community Health 2014, 37, 31–44. [Google Scholar] [CrossRef] [PubMed]
- Van Der Kruk, J.J.; Kortekaas, F.; Lucas, C.; Jager-Wittenaar, H. Obesity: A systematic review on parental involvement in long-term European childhood weight control interventions with a nutritional focus. Obes. Rev. 2013, 14, 745–760. [Google Scholar] [CrossRef]
- Yavuz, H.M.; Van Ijzendoorn, M.H.; Mesman, J.; Van Der Veek, S. Interventions aimed at reducing obesity in early childhood: A meta-analysis of programs that involve parents. J. Child Psychol. Psychiatry 2015, 56, 677–692. [Google Scholar] [CrossRef] [PubMed]
- Institute of Medicine. IOM Report Identifies Key Obesity-Prevention Strategies to Scale Back ‘Weight of the Nation’. Available online: http://www8.nationalacademies.org/onpinews/newsitem.aspx?RecordID=13275 (accessed on 1 June 2021).
- Mead, E.; Brown, T.; Rees, K.; Azevedo, L.; Whittaker, V.; Jones, D.; Olajide, J.; Mainardi, G.M.; Corpeleijn, E.; O’Malley, C.; et al. Diet, physical activity and behavioural interventions for the treatment of overweight or obese children from the age of 6 to 11 years. Cochrane Database Syst. Rev. 2017, 6, CD012651. [Google Scholar] [CrossRef]
- Kader, M.; Sundblom, E.; Elinder, L.S. Effectiveness of universal parental support interventions addressing children’s dietary habits, physical activity and bodyweight: A systematic review. Prev. Med. 2015, 77, 52–67. [Google Scholar] [CrossRef]
- Nader, P.R.; O’Brien, M.; Houts, R.; Bradley, R.; Belsky, J.; Crosnoe, R.; Friedman, S.; Mei, Z.; Susman, E.J.; For the National Institute of Child Health and Human Development Early Child Care Research Network. Identifying risk for obesity in early childhood. Pediatrics 2006, 118, e594–e601. [Google Scholar] [CrossRef] [PubMed]
- Center for Disease Control and Prevention. Childhood Growth Charts. 2000. Available online: http://www.cdc.gov/growthcharts/ (accessed on 14 January 2021).
- Center for Disease Control and Prevention. Defining Childhood Overweight. 2007. Available online: http://www.cdc.gov/nccdphp/dnpa/obesity/childhood/defining.html (accessed on 1 June 2021).
- Cole, T.J.; Faith, M.S.; Pietrobelli, A.; Heo, M. What is the best measure of adiposity change in growing children: BMI, BMI %, BMI z-score or BMI centile? Eur. J. Clin. Nutr. 2005, 59, 419–425. [Google Scholar] [CrossRef]
- Freedman, D.; Woo, J.; Ogden, C.L.; Xu, J.H.; Cole, T.J. Distance and percentage distance from median BMI as alternatives to BMI z score. Br. J. Nutr. 2019, 124, 493–500. [Google Scholar] [CrossRef]
- Epstein, L.H.; Squires, S. The Stoplight Diet for Children; Little, Brown and Company: Boston, MA, USA, 1988. [Google Scholar]
- Satter, E. How to Get Your Kid to Eat: But Not Too Much; Bull: Boulder, CO, USA, 1987. [Google Scholar]
- Institute of Medicine. Preventing Childhood Obesity; National Academies Press: Washington, DC, USA, 2005. [Google Scholar]
- Wells, M.G.; Law, D.D.; Johnson, J.E. Love, Limits, and Latitude: A Thousand Small Moments of Parenting, 2nd ed.; BYU Academic Publishing: Provo, UT, USA, 2005. [Google Scholar]
- Harrist, A.W.; Bradley, K.D. “You can’t say you can’t play”: Intervening in the process of social exclusion in the kindergarten classroom. Early Child. Res. Q. 2003, 18, 185–205. [Google Scholar] [CrossRef]
- Paley, V.G. You Can’t Say You Can’t Play; Harvard University Press: Cambridge, MA, USA, 1992. [Google Scholar]
- Abraha, I.; Cherubini, A.; Cozzolino, F.; De Florio, R.; Luchetta, M.L.; Rimland, J.; Folletti, I.; Marchesi, M.; Germani, A.; Orso, M.; et al. Deviation from intention to treat analysis in randomised trials and treatment effect estimates: Meta-epidemiological study. BMJ 2015, 350, h2445. [Google Scholar] [CrossRef] [PubMed]
- Feingold, A. Effect sizes for growth-modeling analysis for controlled clinical trials in the same metric as for classical analysis. Psychol. Methods 2009, 14, 43–51. [Google Scholar] [CrossRef] [PubMed]
- Bocca, G.; Kuitert, M.W.B.; Sauer, P.; Sauer, P.; Stolk, R.; Flapper, B.; Corpeleijn, E.; Stolk, R. A multidisciplinary intervention programme has positive effects on quality of life in overweight and obese preschool children. Acta Paediatr. Int. J. Paediatr. 2014, 103, 962–967. [Google Scholar] [CrossRef] [PubMed]
- Brotman, L.M.; Dawson-McClure, S.; Huang, K.-Y.; Theise, R.; Kamboukos, D.; Wang, J.; Petkova, E.; Ogedegbe, G. Early childhood family intervention and long-term obesity prevention among high-risk minority youth. Pediatrics 2012, 129, e621–e628. [Google Scholar] [CrossRef]
- Stark, L.J.; Spear, S.; Boles, R.; Kuhl, E.; Ratcliff, M.; Scharf, C.; Bolling, C.; Rausch, J. A pilot randomized controlled trial of a clinic and home-based behavioral intervention to decrease obesity in preschoolers. Obesity 2011, 19, 134–141. [Google Scholar] [CrossRef]
- Verjans-Janssen, S.R.B.; van de Kolk, I.; Van Kann, D.H.H.; Kremers, S.P.; Gerards, S.M. Effectiveness of school-based physical activity and nutrition interventions with direct parental involvement on children’s BMI and energy balance-related behaviors—A systematic review. PLoS ONE 2018, 13, e0204560. [Google Scholar] [CrossRef]
- Loveman, E.; Al-Khudairy, L.; Johnson, R.E.; Robertson, W.; Colquitt, J.L.; Mead, E.L.; Ells, L.J.; Metzendorf, M.-I.; Rees, K. Parent-only interventions for childhood overweight or obesity in children aged 5 to 11 years. Cochrane Database Syst. Rev. 2015, 12, CD012008. [Google Scholar] [CrossRef]
- Rajjo, T.; Mohammed, K.; Alsawas, M.; Ahmed, A.T.; Farah, W.; Asi, N.; Almasri, J.; Prokop, L.J.; Murad, M.H. Treatment of Pediatric Obesity: An Umbrella Systematic Review. J. Clin. Endocrinol. Metab. 2017, 102, 763–775. [Google Scholar] [CrossRef]
- Bixby, H.; Bentham, J.; Zhou, B.; Di Cesare, M.; Paciorek, C.J.; Bennett, J.E.; Taddei, C.; Stevens, G.A.; Rodriguez-Martinez, A.; NCD Risk Factor Collaboration; et al. Rising rural body-mass index is the main driver of the global obesity epidemic. Nature 2019, 569, 260–264. [Google Scholar] [CrossRef]
- Tomayko, E.J.; Prince, R.J.; Cronin, K.A.; Adams, A.K. The Healthy Children, Strong Families intervention promotes improvements in nutrition, activity and body weight in American Indian families with young children. Public Health Nutr. 2016, 19, 2850–2859. [Google Scholar] [CrossRef] [PubMed]
| Total N | Intervention | Control | Total | ||||
|---|---|---|---|---|---|---|---|
| M | SD | M | SD | Total M | Total SD | ||
| Raw BMI a | 538 | 19.4 | 3.1 | 19.1 | 2.49 | 19.4 | 3.0 |
| N | Percent | N | Percent | Total | Total % | ||
| Sex | 538 | – | – | – | – | – | – |
| Boys | – | 232 | 50.8% | 46 | 56.8% | 278 | 51.7% |
| Girls | – | 225 | 49.2% | 35 | 43.2% | 260 | 48.3% |
| Ethnicity | 529 | – | – | – | – | – | – |
| Euro-American | – | 322 | 71.6% | 59 | 74.7% | 381 | 72.0% |
| American Indian | – | 89 | 19.8% | 9 | 11.4% | 98 | 18.5% |
| Latino | – | 18 | 4.0% | 6 | 7.6% | 24 | 4.5% |
| African American | – | 10 | 2.2% | 3 | 3.8% | 13 | 2.5% |
| Multiethnic | – | 9 | 2.0% | 2 | 2.5% | 11 | 2.1 |
| Other | – | 1 | 0.2% | 0 | 0% | 1 | 0.2% |
| Maternal Education | 187 | – | – | – | – | – | – |
| College Degree | – | 55 | 34.8% | 8 | 27.6% | 63 | 33.7% |
| Marital Status | 212 | – | – | – | – | – | – |
| Married/Remarried | – | 141 | 79.2% | 22 | 64.7% | 163 | 76.9% |
| FL | FL + FD | FL + PG | FL + FD + PG | Control | Total | |
|---|---|---|---|---|---|---|
| At-Risk | 28.21% | 27.59% | 25.00% | 27.13% | 29.63% | 27.32% |
| Overweight | 41.88% | 44.83% | 29.84% | 35.66% | 39.51% | 37.73% |
| Obese | 29.91% | 27.59% | 45.16% | 37.21% | 30.86% | 34.94% |
| Total | 100.00% | 100.00% | 100.00% | 100.00% | 100.00% | 100.00% |
| Risk Factors Targeted by Intervention Component a | Intervention Curriculum | |||
|---|---|---|---|---|
| Family Food and Lifestyle (FL) Intervention (12 Weekly Sessions) | ||||
| Factors Addressed by FL Content: Interpersonal Context Poor Family Nutritional Intake Low Family Activity Parental Misperception of Child Weight Parent Pressure, Over-Monitoring of Child Eating Intrapersonal Child Mediators Child Emotional and External Eating Dysregulated eating | First 45 min | Second 45 min | ||
Parent Group
| Child Group
| Parent Group
| Child Group
| |
| Parents and Children Together 3–12: Make and eat a healthy snack | ||||
| Family Food and Lifestyle + Family Dynamics (FL + FD) Intervention (12 Weekly Sessions) | ||||
| Factors Addressed by FD Content: Interpersonal Context Poor Parent-Child Communication Discomfort with Negative Emotion Parent Over-Control or Permissiveness Intrapersonal Child Mediators Poor emotional awareness and regulation Poor behavioral self-control Poor Self-Esteem Poor Body-Esteem Loneliness, Depression Anxiety Eating as coping | Parent Group | Child Group | ||
FL Content (45 min)
| FD Content (45 min)
| FL Content (45 min)
| FD Content (45 min)
| |
| Peer Group (PG) Intervention | ||||
| Factors Addressed by PG Content: Interpersonal Context Negative Peer Dynamics Peer Exclusion and Dislike Peer Teasing Peer Bullying Intrapersonal Child Mediators Child Negative Affect Poor Self-Esteem Poor Body-Esteem Loneliness, Depression Anxiety Social Avoidance | Weekly Session Topics (Presented to class at school, 12 weeks) A. Introduction to the YCSYCP Principles & Rule b
| |||
| Raw BMI a | BMI-M% b | |||||
|---|---|---|---|---|---|---|
| B | SE | p | B | SE | p | |
| Baseline for at-risk | 1.60 | 0.05 | 0.00 | 9.21 | 1.90 | 0.00 |
| Difference in Baseline: At-risk vs. Overweight | 0.25 | 0.06 | 0.00 | 7.90 | 2.48 | 0.00 |
| Difference in Baseline: At-risk vs. Obese | 0.70 | 0.06 | 0.00 | 26.36 | 2.64 | 0.00 |
| Difference in Baseline: Overweight vs. Obese | 0.46 | 0.06 | 0.00 | 18.46 | 2.46 | 0.00 |
| Change for at-risk | 0.14 | 0.02 | 0.00 | 2.22 | 0.56 | 0.00 |
| Difference in Change: At-risk vs. Overweight | 0.00 | 0.02 | 0.99 | 1.03 | 0.74 | 0.17 |
| Difference in Change: At-risk vs. Obese | −0.01 | 0.03 | 0.82 | 2.27 | 0.86 | 0.01 |
| Difference in Change: Overweight vs. Obese | −0.01 | 0.02 | 0.82 | 1.25 | 0.82 | 0.13 |
| Raw BMI a | BMI-M% b | ||||||||
|---|---|---|---|---|---|---|---|---|---|
| Intervention Condition Effects | |||||||||
| Baseline BMI%tile Group | B | SE | p | ES | B | SE | p | ES | |
| At-risk | FL vs. Control | −0.03 | 0.02 | 0.18 | −0.20 | −0.75 | 0.71 | 0.29 | −0.12 |
| FL + FD vs. Control | −0.04 | 0.02 | 0.09 | −0.28 | −0.87 | 0.78 | 0.26 | −0.14 | |
| FL + PG vs. Control | 0.00 | 0.02 | 0.97 | −0.01 | 0.05 | 0.72 | 0.95 | 0.01 | |
| FL + FD + PG vs. Control | 0.01 | 0.02 | 0.66 | 0.07 | 0.66 | 0.71 | 0.35 | 0.10 | |
| Overweight | FL vs. Control | 0.01 | 0.02 | 0.59 | 0.07 | 0.18 | 0.63 | 0.77 | 0.03 |
| FL + FD vs. Control | 0.03 | 0.02 | 0.15 | 0.19 | 1.04 | 0.62 | 0.10 | 0.16 | |
| FL + PG vs. Control | 0.02 | 0.02 | 0.25 | 0.16 | 0.80 | 0.67 | 0.23 | 0.13 | |
| FL + FD + PG vs. Control | −0.01 | 0.02 | 0.58 | −0.07 | −0.55 | 0.60 | 0.36 | −0.09 | |
| Obese | FL vs. Control | −0.05 | 0.02 | 0.03 | −0.36 | −1.27 | 0.78 | 0.10 | −0.20 |
| FL + FD vs. Control | −0.02 | 0.02 | 0.37 | −0.17 | −1.47 | 0.85 | 0.08 | −0.23 | |
| FL + PG vs. Control | −0.02 | 0.02 | 0.44 | −0.12 | −1.24 | 0.75 | 0.10 | −0.20 | |
| FL + FD + PG vs. Control | −0.05 | 0.02 | 0.04 | −0.34 | −2.36 | 0.75 | 0.00 | −0.37 | |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Topham, G.L.; Washburn, I.J.; Hubbs-Tait, L.; Kennedy, T.S.; Rutledge, J.M.; Page, M.C.; Swindle, T.; Shriver, L.H.; Harrist, A.W. The Families and Schools for Health Project: A Longitudinal Cluster Randomized Controlled Trial Targeting Children with Overweight and Obesity. Int. J. Environ. Res. Public Health 2021, 18, 8744. https://doi.org/10.3390/ijerph18168744
Topham GL, Washburn IJ, Hubbs-Tait L, Kennedy TS, Rutledge JM, Page MC, Swindle T, Shriver LH, Harrist AW. The Families and Schools for Health Project: A Longitudinal Cluster Randomized Controlled Trial Targeting Children with Overweight and Obesity. International Journal of Environmental Research and Public Health. 2021; 18(16):8744. https://doi.org/10.3390/ijerph18168744
Chicago/Turabian StyleTopham, Glade L., Isaac J. Washburn, Laura Hubbs-Tait, Tay S. Kennedy, Julie M. Rutledge, Melanie C. Page, Taren Swindle, Lenka H. Shriver, and Amanda W. Harrist. 2021. "The Families and Schools for Health Project: A Longitudinal Cluster Randomized Controlled Trial Targeting Children with Overweight and Obesity" International Journal of Environmental Research and Public Health 18, no. 16: 8744. https://doi.org/10.3390/ijerph18168744
APA StyleTopham, G. L., Washburn, I. J., Hubbs-Tait, L., Kennedy, T. S., Rutledge, J. M., Page, M. C., Swindle, T., Shriver, L. H., & Harrist, A. W. (2021). The Families and Schools for Health Project: A Longitudinal Cluster Randomized Controlled Trial Targeting Children with Overweight and Obesity. International Journal of Environmental Research and Public Health, 18(16), 8744. https://doi.org/10.3390/ijerph18168744







