Identification of Novel Simulants for Toxic Industrial Chemicals and Chemical Warfare Agents for Human Decontamination Studies: A Systematic Review and Categorisation of Physicochemical Characteristics
Abstract
1. Introduction
2. Materials and Methods
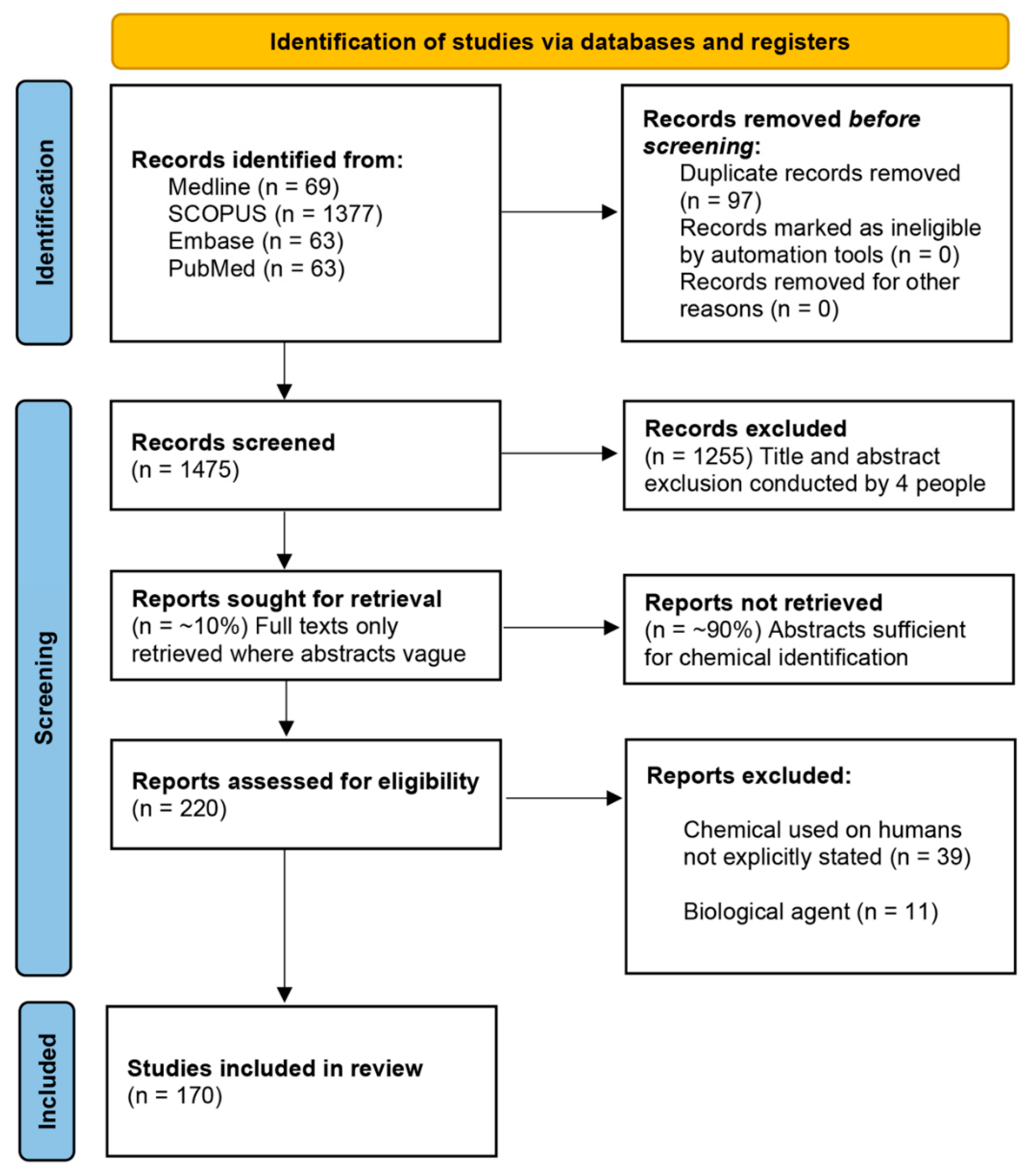
2.1. Literature Search Strategy
2.2. Inclusion Criteria and Literature Screening
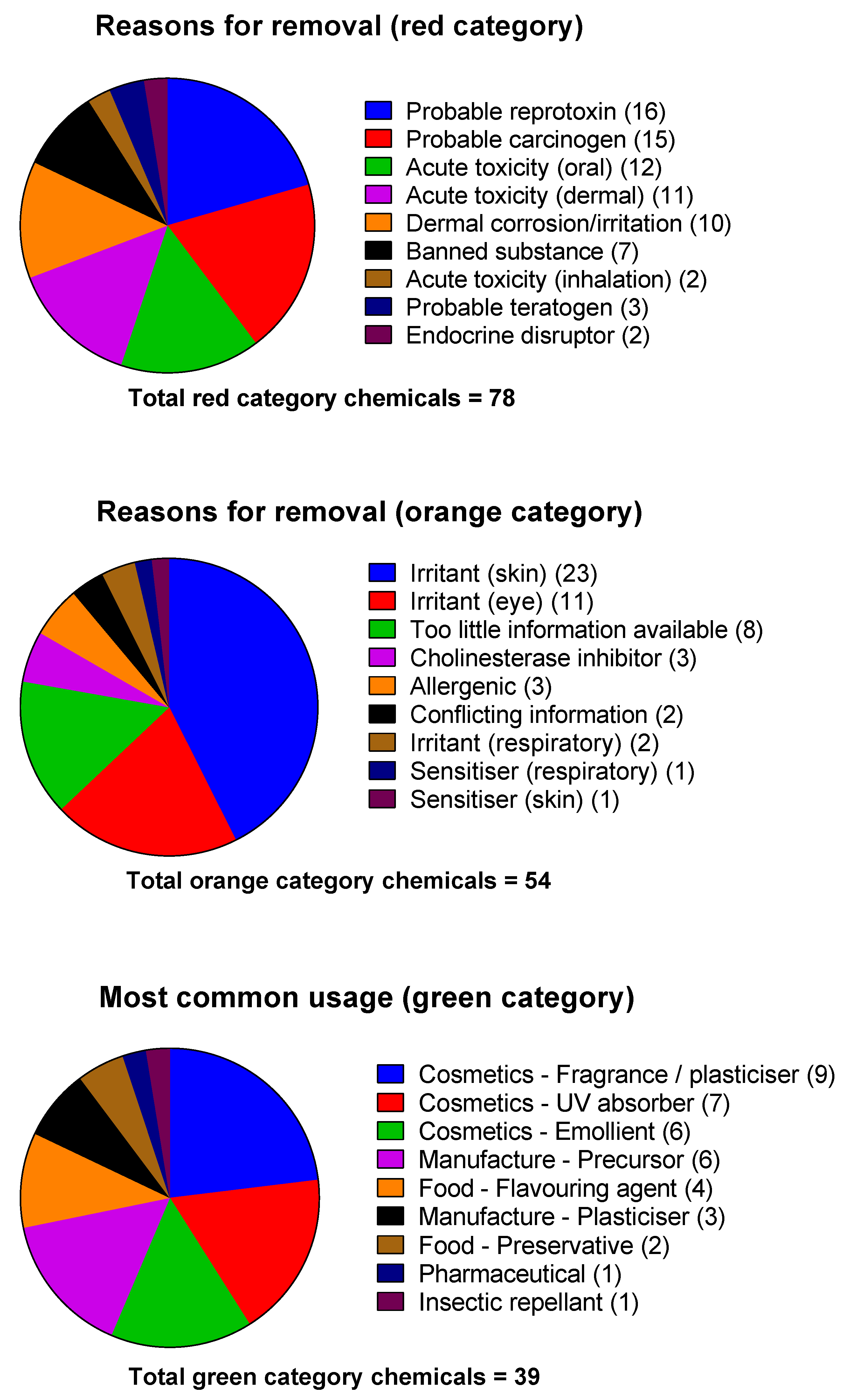
2.3. Chemical Screening
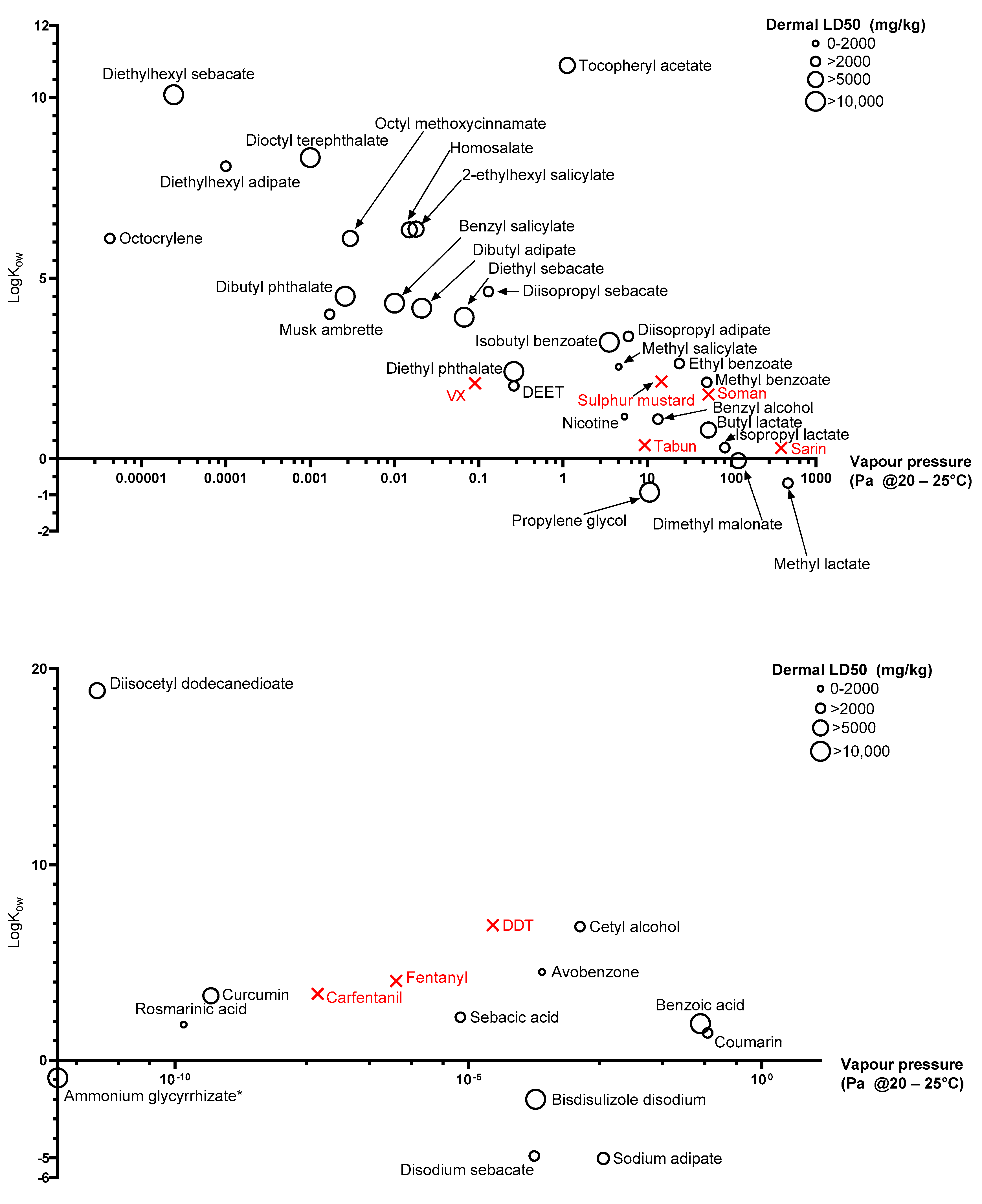
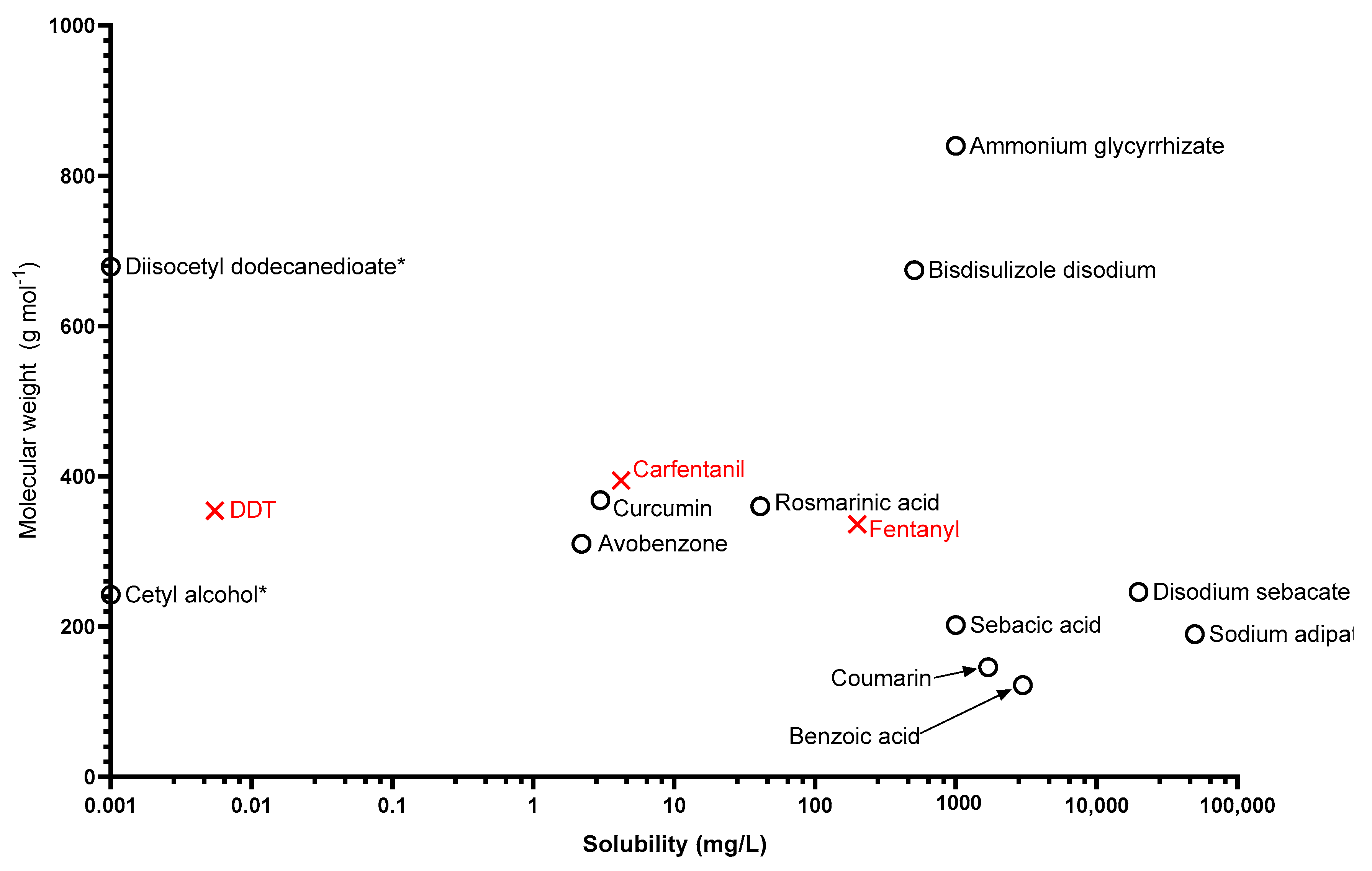
2.4. Physicochemical Property Identification
3. Results
3.1. Chemical Screening
3.2. Physicochemical Property Mapping
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Home Office. Initial Operational Response to a CBRN Incident; Joint Emergency Services Interoperability Programme: Welwyn Garden City, UK, 2015. [Google Scholar]
- James, T.; Wyke, S.; Marczylo, T.; Collins, S.; Gaulton, T.; Foxall, K.; Amlôt, R.; Duarte-Davidson, R. Chemical warfare agent simulants for human volunteer trials of emergency decontamination: A systematic review. J. Appl. Toxicol. 2018, 38, 113–121. [Google Scholar] [CrossRef]
- Collins, S.; James, T.; Carter, H.; Symons, C.; Southworth, F.; Foxall, K.; Marczylo, T.; Amlôt, R. Mass Casualty Decontamination for Chemical Incidents: Research Outcomes and Future Priorities. Int. J. Environ. Res. Public Health 2021, 18, 3079. [Google Scholar] [CrossRef]
- Larner, J.; Hazem, M.; Lorna, R.; Jones, D.R.; Wakefield, J.; Chilcott, R.; Amlôt, R. Human volunteer trial of an optimised decontamination protocol using methyl salicylate as a simulant contaminant. In Evaluation and Optimisation of Emergency Mass Casualty Decontamination (ORCHIDS); Annex, C., Ed.; Technical Report 5 (Deliverable 9); Health Protection Agency (HPA): Porton Down, UK, 2010. [Google Scholar]
- Jenkins, R.A.; Buchanan, M.V.; Merriweather, R.; Ilgner, R.H.; Gayle, T.M.; Watson, A.P. Movement of chemical warfare agent simulants through porous media. J. Hazard. Mater. 1994, 37, 303–325. [Google Scholar] [CrossRef]
- Feldman, R.J. Chemical agent simulant release from clothing following vapor exposure. Acad. Emerg. Med. 2010, 17, 221–224. [Google Scholar] [CrossRef] [PubMed]
- Gazi, E.; Mitchell, S.J. Nuclear magnetic resonance profiling of chemical warfare agent simulant mass-transport through a multilayered polymeric coating. J. Coat. Technol. Res. 2012, 9, 735–743. [Google Scholar] [CrossRef]
- Matar, H.; Guerreiro, A.; Piletsky, S.A.; Price, S.C.; Chilcott, R.P. Preliminary evaluation of military, commercial and novel skin decontamination products against a chemical warfare agent simulant (methyl salicylate). Cutan. Ocul. Toxicol. 2016, 35, 137–144. [Google Scholar] [CrossRef]
- Spiandore, M.; Piram, A.; Lacoste, A.; Prevost, P.; Maloni, P.; Torre, F.; Asia, L.; Josse, D.; Doumenq, P. Efficacy of scalp hair decontamination following exposure to vapours of sulphur mustard simulants 2-chloroethyl ethyl sulphide and methyl salicylate. Chem. Biol. Interact. 2016, 267, 74–79. [Google Scholar] [CrossRef]
- Riviere, J.E.; Smith, C.E.; Budsaba, K.; Brooks, J.D.; Olajos, E.J.; Salem, H.; Monteiro-Riviere, N.A. Use of methyl salicylate as a simulant to predict the percutaneous absorption of sulfur mustard. J. Appl. Toxicol. 2001, 21, 91–99. [Google Scholar] [CrossRef] [PubMed]
- Ribordy, P.; Rockseấn, D.; Dellgar, U.; Persson, S.Å.; Arnoldsson, K.; Ekãlsen, H.; Häggbom, S.; Nerf, O.; Ljungqvist, Å.; Gryth, D.; et al. Mobile decontamination units-room for improvement? Prehosp. Disaster Med. 2012, 27, 425–431. [Google Scholar] [CrossRef] [PubMed]
- Torngren, S.; Persson, S.A.; Ljungquist, A.; Berglund, T.; Nordstrand, M.; Hagglund, L.; Rittfeldt, L.; Sandgren, K.; Soderman, E. Personal decontamination after exposure to stimulated liquid phase contaminants: Functional assessment of a new unit. J. Toxicol. Clin. Toxicol. 1998, 36, 567–573. [Google Scholar] [CrossRef] [PubMed]
- Collins, S.; James, T.; Southworth, F.; Davidson, L.; Williams, N.; Orchard, E.; Marczylo, T.; Amlôt, R. Human volunteer study of the decontamination of chemically contaminated hair and the consequences for systemic exposure. Sci. Rep. 2020, 10, 20822. [Google Scholar] [CrossRef] [PubMed]
- Southworth, F.; James, T.; Davidson, L.; Williams, N.; Finnie, T.; Marczylo, T.; Collins, S.; Amlôt, R. A controlled cross-over study to evaluate the efficacy of improvised dry and wet emergency decontamination protocols for chemical incidents. PLoS ONE 2020, 15, e0239845. [Google Scholar] [CrossRef] [PubMed]
- Loke, W.K.; Soo-Hway, U.; Lau, S.K.; Lim, J.S.; Tay, G.S.; Koh, C.H. Wet decontamination-induced stratum corneum hydration—Effects on the skin barrier function to diethylmalonate. J. Appl. Toxicol. 1999, 19, 285–290. [Google Scholar] [CrossRef]
- Reifenrath, W.G.; Mershon, M.M.; Brinkley, F.B.; Miura, G.A.; Broomfield, C.A.; Cranford, H.B. Evaluation of diethyl malonate as a simulant for 1,2,2-trimethylpropyl methylphosphonofluoridate (soman) in shower decontamination of the skin. J. Pharm. Sci. 1984, 73, 1388–1392. [Google Scholar] [CrossRef]
- World Health Organization. Manual for the Public Health Management of Chemical Incidents; WHO Document Production Services: Geneva, Switzerland, 2009. [Google Scholar]
- Hikin, L.; Smith, P.R.; Ringland, E.; Hudson, S.; Morley, S.R. Multiple fatalities in the North of England associated with synthetic fentanyl analogue exposure: Detection and quantitation a case series from early 2017. Forensic Sci. Int. 2018, 282, 179–183. [Google Scholar] [CrossRef]
- Taylor, S.; Annand, F.; Burkinshaw, P.; Greaves, F.; Kelleher, M.; Knight, J.; Perkins, C.; Tran, A.; White, M.; Marsden, J. Dependence and Withdrawal Associated with some Prescribed Medicines: An Evidence Review; Public Health England: London, UK, 2019. [Google Scholar]
- Page, M.J.; McKenzie, J.E.; Bossuyt, P.M.; Boutron, I.; Hoffmann, T.C.; Mulrow, C.D.; Shamseer, L.; Tetzlaff, J.M.; Akl, E.A.; Brennan, S.E.; et al. The PRISMA 2020 statement: An updated guideline for reporting systematic reviews. BMJ 2021, 372, 71. [Google Scholar] [CrossRef]
- U.S. National Library of Medicine. National Center for Biotechnology Information Pubchem Compound Database. 2021. Available online: https://pubchem.ncbi.nlm.nih.gov/ (accessed on 2 May 2021).
- Amlôt, R.; Carter, H.; Riddle, L.; Larner, J.; Chilcott, R.P. Volunteer trials of a novel improvised dry decontamination protocol for use during mass casualty incidents as part of the UK’S Initial Operational Response (IOR). PLoS ONE 2017, 12, e0179309. [Google Scholar] [CrossRef] [PubMed]
- Bury, D.; Bruning, T.; Koch, H.M. Determination of metabolites of the UV filter 2-ethylhexyl salicylate in human urine by online-SPE-LC-MS/MS. J. Chromatogr. B 2019, 1110–1111, 59–66. [Google Scholar] [CrossRef] [PubMed]
- Hiller, J.; Klotz, K.; Meyer, S.; Uter, W.; Hof, K.; Greiner, A.; Göen, T.; Drexler, H. Toxicokinetics of urinary 2-ethylhexyl salicylate and its metabolite 2-ethyl-hydroxyhexyl salicylate in humans after simulating real-life dermal sunscreen exposure. Arch. Toxicol. 2019, 93, 2565–2574. [Google Scholar] [CrossRef] [PubMed]
- Roussel, L.; Gilbert, E.; Salmon, D.; Serre, C.; Gabard, B.; Haftek, M.; Maibach, H.I.; Pirot, F. Measurement, analysis and prediction of topical UV filter bioavailability. Int. J. Pharm. 2015, 478, 804–810. [Google Scholar] [CrossRef] [PubMed]
- Sarveiya, V.; Risk, S.; Benson, H.A. Liquid chromatographic assay for common sunscreen agents: Application to in vivo assessment of skin penetration and systemic absorption in human volunteers. J. Chromatogr. B 2004, 803, 225–231. [Google Scholar] [CrossRef] [PubMed]
- Andersen, F.A. Final report on the safety assessment of glycyrrhetinic acid, potassium glycyrrhetinate, disodium succinoyl glycyrrhetinate, glyceryl glycyrrhetinate, glycyrrhetinyl stearate, stearyl glycyrrhetinate, glycyrrhizic acid, ammonium glycyrrhizate, dipotassium glycyrrhizate, disodium glycyrrhizate, trisodium glycyrrhizate, methyl glycyrrhizate, and potassium glycyrrhizinate. Int. J. Toxicol. 2007, 26 (Suppl. 2), 79–112. [Google Scholar]
- James, T.; Collins, S.; Amlôt, R.; Marczylo, T. Analysis of Chemical Simulants in Urine: A Useful Tool for Assessing Emergency Decontamination Efficacy in Human Volunteer Studies. Prehosp. Disaster. Med. 2020, 35, 482–487. [Google Scholar] [CrossRef] [PubMed]
- James, T.; Collins, S.; Amlôt, R.; Marczylo, T. GC-MS/MS quantification of benzyl salicylate on skin and hair: A novel chemical simulant for human decontamination studies. J. Chromatogr. B 2019, 1129, 121818. [Google Scholar] [CrossRef]
- Andersen, D.F.A. Final report on the safety assessment of glycolic acid, ammonium, calcium, potassium, and sodium glycolates, methyl, ethyl, propyl, and butyl glycolates, and lactic acid, ammonium, calcium, potassium, sodium, and tea-lactates, methyl, ethyl, isopropyl, and butyl lactates, and lauryl, myristyl, and cetyl lactates. Int. J. Toxicol. 1998, 17 (Suppl. 1), 1–241. [Google Scholar]
- Roy, M.J.; Kraus, P.L.; Cooper, J.A.; Cherstniakova, S.; Coll, R.; Seegers, C.A.; Deuster, P.A.; Koslowe, P.; Law, W.A.; Krantz, D.S.; et al. Initial evaluation of N,N-diethyl-m-toluamide and permethrin absorption in human volunteers under stress conditions. Mil. Med. 2006, 171, 122–127. [Google Scholar] [CrossRef]
- Selim, S.; Preiss, F.J.; Jonkman, J.H.G.; Gabriel, K.L. Dermal absorption and mass balance of MGK 326 and reformulated MGK 326 in human volunteers. Cutan. Ocul. Toxicol. 1994, 13, 83–96. [Google Scholar] [CrossRef]
- Selim, S.; Gabriel, K.L.; Jonkman, J.H.G.; Preiss, F.J. Absorption and mass balance of MGK R11 and MGK R11 formulated with DEET, MGK 264, and MGK 326 following an 8 h dermal exposure in human volunteers. Cutan. Ocul. Toxicol. 1995, 14, 151–167. [Google Scholar] [CrossRef]
- Selim, S.; Hartnagel Jr, R.E.; Osimitz, T.G.; Gabriel, K.L.; Schoenig, G.P. Absorption, metabolism, and excretion of N,N-diethyl-m-toluamide following dermal application to human volunteers. Fundam. Appl. Toxicol. 1995, 25, 95–100. [Google Scholar] [CrossRef]
- Selim, S.; Gabriel, K.L.; Jonkman, J.H.G.; Preiss, F.J. Absorption and mass balance of MGK 264 alone and MGK 264 formulated with N,N-diethyl-m-toluamide (DEET) and MGK 326 following an 8 h dermal exposure in human volunteers. Cutan. Ocul. Toxicol. 1999, 18, 325–340. [Google Scholar] [CrossRef]
- Fradin, M.S.; Day, J.F. Comparative efficacy of insect repellents against mosquito bites. N. Engl. J. Med. 2002, 347, 13–18. [Google Scholar] [CrossRef]
- Golenda, C.F.; Solberg, V.B.; Burge, R.; Gambel, J.M.; Wirtz, R.A. Gender-related efficacy difference to an extended duration formulation of topical N,N-diethyl-M-toluamide (DEET). Am. J. Trop. Med. Hyg. 1999, 60, 654–657. [Google Scholar] [CrossRef]
- Yiin, L.M.; Tian, J.N.; Hung, C.C. Assessment of dermal absorption of DEET-containing insect repellent and oxybenzone-containing sunscreen using human urinary metabolites. Environ. Sci. Pollut. Res. 2015, 22, 7062–7070. [Google Scholar] [CrossRef] [PubMed]
- Fiume, M.M.; Eldreth, H.; Bergfeld, W.F.; Belsito, D.V.; Hill, R.A.; Klaassen, C.D.; Liebler, D.; Marks, J.G., Jr.; Shank, R.C.; Slaga, T.J.; et al. Final Report of the Cosmetic Ingredient Review Expert Panel on the Safety Assessment of Dicarboxylic Acids, Salts, and Esters. Int. J. Toxicol. 2012, 31, 5S–76S. [Google Scholar] [CrossRef]
- Janjua, N.R.; Mortensen, G.K.; Andersson, A.M.; Kongshoj, B.; Skakkebæk, N.E.; Wulf, H.C. Systemic uptake of diethyl phthalate, dibutyl phthalate, and butyl paraben following whole-body topical application and reproductive and thyroid hormone levels in humans. Environ. Sci. Technol. 2007, 41, 5564–5570. [Google Scholar] [CrossRef]
- Lorber, M.; Weschler, C.J.; Morrison, G.; Bekö, G.; Gong, M.; Koch, H.M.; Salthammer, T.; Schripp, T.; Toftum, J.; Clausen, G. Linking a dermal permeation and an inhalation model to a simple pharmacokinetic model to study airborne exposure to di(n-butyl) phthalate. J. Expos. Sci. Environ. Epidemiol. 2017, 27, 601–609. [Google Scholar] [CrossRef] [PubMed]
- Morrison, G.C.; Weschler, C.J.; Bekö, G.; Koch, H.M.; Salthammer, T.; Schripp, T.; Toftum, J.; Clausen, G. Role of clothing in both accelerating and impeding dermal absorption of airborne SVOCs. J. Expos. Sci. Environ. Epidemiol. 2016, 26, 113–118. [Google Scholar] [CrossRef] [PubMed]
- Weschler, C.J.; Bekö, G.; Koch, H.M.; Salthammer, T.; Schripp, T.; Toftum, J.; Clausen, G. Transdermal uptake of diethyl phthalate and di(n-butyl) phthalate directly from air: Experimental verification. Environ. Health Perspect. 2015, 123, 928–934. [Google Scholar] [CrossRef]
- David, R.M.; Lockhart, L.K.; Ruble, K.M. Lack of sensitization for trimellitate, phthalate, terephthalate and isobutyrate plasticizers in a human repeated insult patch test. Food Chem. Toxicol. 2003, 41, 589–593. [Google Scholar] [CrossRef]
- ’Becker, L.C.; Bergfeld, W.F.; Belsito, D.V.; Hill, R.A.; Klaassen, C.D.; Liebler, D.; Marks, J.G.; Shank, R.C.; Slaga, T.J.; Snyder, P.W.; et al. Safety Assessment of Alkyl Benzoates as Used in Cosmetics. Int. J. Toxicol. 2012, 31, 342S–372S. [Google Scholar] [CrossRef]
- James, T.; Collins, S.; Amlôt, R.; Marczylo, T. Optimisation and validation of a GC–MS/MS method for the analysis of methyl salicylate in hair and skin samples for use in human-volunteer decontamination studies. J. Chromatogr. B 2019, 1109, 84–89. [Google Scholar] [CrossRef]
- Hawkins, D.R.; Elsom, L.F.; Kirkpatrick, D.; Ford, R.A.; Api, A.M. Dermal absorption and disposition of musk ambrette, musk ketone and musk xylene in human subjects. Toxicol. Lett. 2002, 131, 147–151. [Google Scholar] [CrossRef]
- Bury, D.; Modick-Biermann, H.; Leibold, E.; Brüning, T.; Koch, H.M. Urinary metabolites of the UV filter octocrylene in humans as biomarkers of exposure. Arch. Toxicol. 2019, 93, 1227–1238. [Google Scholar] [CrossRef]
- Janjua, N.R.; Kongshoj, B.; Andersson, A.M.; Wulf, H.C. Sunscreens in human plasma and urine after repeated whole-body topical application. J. Eur. Acad. Dermatol. Venereol. 2008, 22, 456–461. [Google Scholar]
- Scalia, S.; Mezzena, M.; Ramaccini, D. Encapsulation of the UV filters ethylhexyl methoxycinnamate and butyl methoxydibenzoylmethane in lipid microparticles: Effect on in vivo human skin permeation. Skin Pharmacol. Physiol. 2011, 24, 182–189. [Google Scholar] [CrossRef]
- Asche, H.; Botta, L.; Rettig, H.; Weirich, E.G. Influence of formulation factors on the availability of drugs from topical preparations. Pharm. Acta Helv. 1985, 60, 232–237. [Google Scholar]
- Fiume, M.M.; Bergfeld, W.F.; Belsito, D.V.; Hill, R.A.; Klaassen, C.D.; Liebler, D.C.; Marks, J.G., Jr.; Shank, R.C.; Slaga, T.J.; Snyder, P.W.; et al. Safety Assessment of Tocopherols and Tocotrienols as Used in Cosmetics. Int. J. Toxicol. 2018, 37 (Suppl. 2), 61S–94S. [Google Scholar] [CrossRef]
- Andersen, F.A. Final report on the safety assessment of Benzyl Alcohol, Benzoic Acid, and Sodium Benzoate. Int. J. Toxicol. 2001, 20 (Suppl. 3), 23–50. [Google Scholar]
- Balaguer, A.; Chisvert, A.; Salvador, A. Sequential-injection determination of traces of disodium phenyl dibenzimidazole tetrasulphonate in urine from users of sunscreens by on-line solid-phase extraction coupled with a fluorimetric detector. J. Pharm. Biomed. Anal. 2006, 40, 922–927. [Google Scholar] [CrossRef]
- Ford, R.A.; Api, A.M.; Hawkins, D.R.; Mayo, B.C. The in vivo dermal absorption and metabolism of 14C coumarin by rats and by human volunteers under simulated conditions of use in fragrances. Food Chem. Toxicol. 2001, 39, 153–162. [Google Scholar] [CrossRef]
- Abraham, K.; Pfister, M.; Wöhrlin, F.; Lampen, A. Relative bioavailability of coumarin from cinnamon and cinnamon-containing foods compared to isolated coumarin: A four-way crossover study in human volunteers. Mol. Nutr. Food Res. 2011, 55, 644–653. [Google Scholar] [CrossRef]
- Anand, P.; Kunnumakkara, A.B.; Newman, R.A.; Aggarwal, B.B. Bioavailability of curcumin: Problems and promises. Mol. Pharm. 2007, 4, 807–818. [Google Scholar] [CrossRef]
- Baba, S.; Osakabe, N.; Natsume, M.; Yasuda, A.; Muto, Y.; Hiyoshi, K.; Takano, H.; Yoshikawa, T.; Terao, J. Absorption, metabolism, degradation and urinary excretion of rosmarinic acid after intake of Perilla frutescens extract in humans. Eur. J. Nutr. 2005, 44, 1–9. [Google Scholar] [CrossRef]
- Feldmann, R.J.; Maibach, H.I. Percutaneous penetration of some pesticides and herbicides in man. Toxicol. Appl. Pharmacol. 1974, 28, 126–132. [Google Scholar] [CrossRef]
- European Union. Commission Regulation (EU) 2017/238 of 10 February 2017 amending Annex VI to Regulation (EC) No 1223/2009 of the European Parliament and of the Council on cosmetic products. Document 32017R0238 2017. Available online: http://data.europa.eu/eli/reg/2017/238/oj (accessed on 4 May 2021).
- Mueller, J.; Oliveira, J.S.L.; Barker, R.; Trapp, M.; Schroeter, A.; Brezesinski, G.; Neubert, R.H.H. The effect of urea and taurine as hydrophilic penetration enhancers on stratum corneum lipid models. Biochim. Biophys. Acta 2016, 1858, 2006–2018. [Google Scholar] [CrossRef]
- Moody, R.P.; Akram, M.; Dickson, E.; Chu, I. In vitro dermal absorption of methyl salicylate, ethyl parathion, and malathion: First responder safety. J. Toxicol. Environ. 2007, 70, 985–999. [Google Scholar] [CrossRef]
- United States Environmental Protection Agency. Reregistration Eligibility Decision (RED) for Malathion; Case No. 0248; 2009. Available online: https://archive.epa.gov/pesticides/reregistration/web/pdf/malathion-red-revised.pdf (accessed on 16 August 2021).
- Yourick, J.J.; Koenig, M.L.; Yourick, D.L.; Bronaugh, R.L. Fate of chemicals in skin after dermal application: Does the in vitro skin reservoir affect the estimate of systemic absorption? Toxicol. Appl. Pharmacol. 2004, 195, 309–320. [Google Scholar] [CrossRef]
- Roberts, M.S.; Cross, S.E.; Anissimov, Y.G. Factors affecting the formation of a skin reservoir for topically applied solutes. Skin Pharmacol. Physiol. 2004, 17, 3–16. [Google Scholar] [CrossRef]
- Wyke, S.; Brooke, N.; Dobney, A.; Baker, D.; Murray, V. UK Recovery Handbook for Chemical Incidents; Version 1.1; Public Health England: Oxford, UK, 2020. [Google Scholar]
- Amlôt, R.; Larner, J.; Matar, H.; Jones, D.R.; Carter, H.; Turner, E.A.; Price, S.C.; Chilcott, R.P. Comparative analysis of showering protocols for mass-casualty decontamination. Prehosp. Disaster Med. 2010, 25, 435–439. [Google Scholar] [CrossRef]
- Spiandore, M.; Piram, A.; Lacoste, A.; Josse, D.; Doumenq, P. Hair analysis as a useful procedure for detection of vapour exposure to chemical warfare agents: Simulation of sulphur mustard with methyl salicylate. Drug Test. Anal. 2014, 6 (Suppl. 1), 67–73. [Google Scholar] [CrossRef]
- Josse, D.; Wartelle, J.; Cruz, C. Showering effectiveness for human hair decontamination of the nerve agent VX. Chem. Biol. Interact. 2015, 232, 94–100. [Google Scholar] [CrossRef]
- Bos, J.D.; Meinardi, M.M. The 500 Dalton rule for the skin penetration of chemical compounds and drugs. Exp. Dermatol. 2000, 9, 165–169. [Google Scholar] [CrossRef]
- Trebilcock, K.L.; Heylings, J.R.; Wilks, M.F. In vitro tape stripping as a model for in vivo skin stripping. Toxicol. Vitr. 1994, 8, 665–667. [Google Scholar] [CrossRef]
- Chilcott, R.P.; Larner, J.; Durrant, A.; Hughes, P.; Mahalingam, D.; Rivers, S.; Thomas, E.; Amer, N.; Barrett, M.; Matar, H.; et al. Evaluation of US Federal Guidelines (Primary Response Incident Scene Management [PRISM]) for Mass Decontamination of Casualties During the Initial Operational Response to a Chemical Incident. Ann. Emerg. Med. 2019, 73, 671–684. [Google Scholar] [CrossRef]
- Moody, R.P.; Maibach, H.I. Skin decontamination: Importance of the wash-in effect. Food Chem. Toxicol. 2006, 44, 1783–1788. [Google Scholar] [CrossRef]
| OVID—Medline (69 Results) | ||
|---|---|---|
| No. | Search | Results |
| 1 | “Human volunt *”.tw. | 9372 |
| 2 | “Human test *”.tw. | 3835 |
| 3 | 1 OR 2 | 13,183 |
| 4 | Skin Absorption/ | 11,729 |
| 5 | Skin penetra *.tw. | 2250 |
| 6 | Dermal penetra *.tw. | 296 |
| 7 | Percutaneous absor *.tw. | 2109 |
| 8 | Skin absor *.tw. | 731 |
| 9 | Dermal absor *.tw. | 1002 |
| 10 | Skin diffus *.tw. | 130 |
| 11 | Dermal diffus *.tw. | 24 |
| 12 | Skin applica *.tw. | 546 |
| 13 | Dermal applica *.tw. | 712 |
| 14 | 4 OR 5 OR 6 OR 7 OR 8 OR 9 OR 10 OR 11 OR 12 OR 13 | 15,375 |
| 15 | Urin *.tw. | 496,262 |
| 16 | Biomonit *.tw. | 7693 |
| 17 | Excret *.tw. | 178,618 |
| 18 | 15 OR 16 OR 17 | 584,621 |
| 19 | 3 AND 14 AND 18 | 69 |
| SCOPUS (1377 Results) | ||
| (ALL (Human) W/1 ALL (Volunt * OR test *)) AND (ALL(skin OR dermal OR percutan *) W/2 ALL (penetra * OR absor * OR diffus * OR applica *)) AND (All(urin * OR biomonit * OR excret *)) | ||
| HDAS—Embase (63 Results) and PubMed (63 Results) | ||
| (((Human ADJ1 (Volunt * OR test *)) AND ((skin OR dermal OR percutan *) ADJ2 (penetra * OR absor * OR diffus * OR applica *))) AND (urin * OR biomonit * OR excret *)).ti,ab | ||
| Physicochemical Property | Reason for Interest |
|---|---|
| Molecular weight | Molecules larger than 500 Da are unlikely to penetrate through skin |
| State (at room temperature) | Ability to separate liquid and solid simulants and to reject any gaseous chemicals |
| logKow | Hydrophilicity/lipophilicity is a key parameter in skin and tissue penetration/sequestration and partitioning into water is key for wet decontamination |
| Vapour pressure (at 20/25 °C) | An indicator of persistence and possible inhalational risk |
| Dermal toxicity (LD50) | A measure of safety for human application; where not available, toxicity via other routes will be captured |
| Water solubility | To indicate the likelihood of dissolving in water during wet decontamination |
| Reason for Removal (Red Category) | ||||||||
| Probable Reprotoxin | Probable Carcinogen | Acute Toxicity (Oral) | Acute Toxicity (Dermal) | Dermal Corrosion/Irritation | Banned Substance | Probable Teratogen | Acute Toxicity (Inhalation) | Endocrine Disruptor |
| Beclomethasone dipropionate Budesonide Diflorasone diacetate Dimethylacetamide Dimethylformamide Ethylhexyl benzoate Fluazifop-butyl Methotrexate N-Methyl-2-pyrrolidone Penconazole Retinyl palmitate Styrene Tebuconazole Titanium dioxide Toluene Tris(2-ethylhexyl)trimellitate | 1,1,1-trichloroethane 2,4,5-Trichlorophenoxyacetic acid Bromodichloromethane Carbaryl Chromium Dichloromethane Epoxiconazol Halometasone Hydroquinone Musk Ketone Musk Xylene Pirimicarb Propoxur Tetrachloroethene Trichloroethene | Cyfluthrin Deltamethrin Diclofenac sodium Ethion Flurbiprofen Indomethacin Ketoprofen Lindane Methyl formate Nonane Selenium Triclopyr | Cyanamide 1,3-dichloropropene (cis) Iloprost Laurocapram m-xylene N-Octyl bicycloheptene dicarboximide Nicotine p-phenylenediamine Promestriene Propetamphos Pyrethrin (unspecificed) | Ethyl glycolate Glycolic acid Lactic acid Lauryldimethylamine oxide Mercury (II) chloride N,N-Dimethylethylamine Sodium metasilicate Sodium silicate Stearamine oxide Tripropylene glycol diacrylate | Aldrin Dieldrin Diquat Guthion MGK 11 Monocrotophos Parathion | Dipyrithione Furosemide Trimethyl pentanyl diisobutyrate | 3-Carene Methyldibromo glutaronitrile | Dihydrotestosterone Estradiol |
| Reason for Removal (Orange Category) | ||||||||
| Irritant (Skin) | Irritant (Eye) | Not enough Available Information | May Cause Allergic Reaction | Cholinesterase Inhibitor | Conflicting Information | Irritant (Respiratory) | ||
| 2-butoxyethanol 2-methyl 1,3-propanediol 2-phenylphenol 4-aminobenzoic acid Borax Boric acid Butyl acetate Butyl benzoate Butyl paraben Capsaicin Captan Hydroxycitronellal Isopropyl alcohol Isostearyl alcohol Methyl glycolate Methyl tert-butyl ether Oxybenzone Permethrin Pyrene Pyroglutamic Acid Sodium lactate Stearyl benzoate Undecanedioic acid | Azelaic acid Benzaldehyde Butyl glycolate Dodecanedioic acid Dodecanol Ethyl acetate Ethyl butylacetylaminopropionate Ethyl lactate Methylparaben Salicylic acid Sodium benzoate | 2-hexanone Dioctyldodecyl dodecanedioate Disodium octaborate tetrahydrate DMPS Isostearyl benzoate Piperonyl butoxide | 2,4-D 2,4-D amine 2,4-D isooctyl ester Diisostearyl adipate Ethyl paraben Propranolol hydrochloride | Chlorpyrifos Diazinon Malathion | Enzacamene Glycyrrhizic acid MGK 326 | Cypermethrin Propylene glycol methyl ether | ||
| Chemical | CAS-Number | References | Molecular Weight | logKow | Vapour Pressure (Pa at 20–25 °C) | Acute Toxicity | Solubility at 20/25 °C (mg/L) | |
|---|---|---|---|---|---|---|---|---|
| Liquids | 2-ethylhexyl salicylate | 118-60-5 | [23,24,25,26] | 250.3 | 6.36 | 0.018 | >5000 mg/kg—Dermal—Rat | <0.5 |
| Benzyl alcohol | 100-51-6 | [27] | 108.1 | 1.1 | 13.3 | 2000 mg/kg—Dermal—Rabbit | 40,000 | |
| Benzyl salicylate | 118-58-1 | [28,29] | 228.2 | 4.31 | 0.01 | 14,150 mg/kg—Dermal—Rabbit | 8.8 | |
| Butyl lactate | 138-22-7 | [30] | 146.2 | 0.8 | 53 | >5000 mg/kg—Dermal—Rabbit | 40 | |
| DEET | 134-62-3 | [31,32,33,34,35,36,37,38] | 191.3 | 2.02 | 0.26 | 4280 mg/kg—Dermal—Rabbit | <1000 | |
| Dibutyl adipate | 105-99-7 | [39] | 258.4 | 4.17 | 0.021 | 19,000 mg/kg—Dermal—Rabbit | 35 | |
| Dibutyl phthalate | 84-74-2 | [40,41,42,43] | 278.3 | 4.5 | 0.0026 | 20,000 mg/kg—Dermal—Rabbit | 11.4 | |
| Diethyl phthalate | 84-66-2 | [40,41,42,43,44] | 222.2 | 2.42 | 0.26 | >22,400 mg/kg—Dermal—Rat | 932 | |
| Diethyl sebacate | 110-40-7 | [39] | 258.4 | 3.92 | 0.067 | 14,470 mg/kg—Oral—Rat | 16 | |
| Diethylhexyl adipate | 103-23-1 | [39,45] | 370.6 | 8.1 | 0.0001 | >2000 mg/kg—Dermal—Rat | 0.0032 | |
| Diethylhexyl sebacate | 122-62-3 | [39] | 426.7 | 10.08 | 0.000024 | >15,029 mg/kg—Dermal—Rabbit | <1 | |
| Diisopropyl adipate | 6938-94-9 | [39] | 230.3 | 3.39 | 5.946 | >2000 mg/kg—Dermal—Rat | 500 | |
| Diisopropyl sebacate | 7491-02-3 | [39] | 286.4 | 4.63 | 0.13 | >2000 mg/kg—Oral—Mouse | 2 | |
| Dimethyl malonate | 108-59-8 | [39] | 132.1 | −0.05 | 120 | >5000 mg/kg—Dermal—Rabbit | 99,000 | |
| Dioctyl terephthalate | 4654-26-6 | [44] | 390.6 | 8.34 | 0.001 | >19,680 mg/kg—Dermal—Guinea pig | 0.0002 | |
| Ethyl benzoate | 93-89-0 | [45] | 150.2 | 2.64 | 24 | >2000 mg/kg—Dermal—Rabbit | 720 | |
| Homosalate | 118-56-9 | [26] | 262.3 | 6.34 | 0.015 | >5000 mg/kg—Dermal—Rabbit | 0.4 | |
| Isobutyl benzoate | 120-50-3 | [45] | 178.2 | 3.23 | 3.54 | 20,000 mg/kg—Dermal—Rabbit | 98.3 | |
| Isopropyl lactate | 617-51-6 | [30] | 132.2 | 0.31 | 82.93 | 2500 mg/kg—Intramuscular—Guinea pig | 183,000 | |
| Methyl benzoate | 93-58-3 | [45] | 136.2 | 2.12 | 50.66 | >2000 mg/kg—Dermal—Rat | 2100 | |
| Methyl lactate | 547-64-8 | [30] | 104.1 | −0.67 | 466.6 | >2000 mg/kg—Oral—Rat | Miscible | |
| Methyl salicylate | 119-36-8 | [11,12,14,22,46] | 152.2 | 2.55 | 4.57 | 700 mg/kg—Dermal—Guinea Pig | 625 | |
| Musk ambrette | 83-66-9 | [47] | 268.3 | 4 | 0.0017 | >2000 mg/kg—Dermal—Rabbit | 2.41 | |
| Octocrylene | 6197-30-4 | [48] | 361.5 | 6.1 | 0.0000042 | >2000 mg/kg—Dermal—Rat | 0.04 | |
| Octyl methoxycinnamate | 5466-77-3 | [25,26,49,50] | 290.4 | 6.1 | 0.003 | >5000 mg/kg—Dermal—Rat | <1 | |
| Propylene glycol | 57-55-6 | [51] | 76.1 | −0.92 | 10.6 | 20,800 mg/kg—Dermal—Rabbit | Miscible | |
| Tocopheryl acetate | 58-95-7 | [52] | 472.7 | 10.89 | 1.12 | >3000 mg/kg—Dermal—Rat | <1000 | |
| Solids | Ammonium glycyrrhizate | 53956-04-0 | [27] | 840 | −0.9 | Presumed 0 | 12,700 mg/kg—Oral—Mouse | 1000 |
| Avobenzone | 70356-09-1 | [50] | 310.4 | 4.51 | 0.00018 | >1000 mg/kg—Dermal—Rat | 2.2 | |
| Benzoic acid | 65-85-0 | [45,53] | 122.1 | 1.87 | 0.09 | 10,000 mg/kg—Dermal—Rabbit | 3000 | |
| Bisdisulizole disodium | 180898-37-7 | [54] | 674.6 | −2 | 0.00014 | >20 000 mg/kg—Dermal—Rat | 509 | |
| Cetyl alcohol | 36653-82-4 | [45] | 242.4 | 6.83 | 0.0008 | >2600 mg/kg—Dermal—Rabbit | 0 | |
| Coumarin | 91-64-5 | [55,56] | 146.1 | 1.39 | 0.12 | >2000 mg/kg—Dermal—Rat | 1700 | |
| Curcumin | 458-37-7 | [57] | 368.4 | 3.29 | 4.1 × 10−10 | >5000 mg/kg—Dermal—Rabbit | 3 | |
| Diisocetyl dodecanedioate | 131252-83-0 | [39] | 679.1 | 18.9 | 4.7 × 10−12 | >5000 mg/kg—Oral—Rat | 0 | |
| Disodium sebacate | 17265-14-4 | [39] | 246.2 | −4.9 | 0.000133322 | >2000 mg/kg—Dermal—Rat | 19,880 | |
| Rosmarinic acid | 20283-92-5 | [58] | 360.3 | 1.82 | 1.4 × 10−10 | 561 mg/kg—Intravenous—Mouse | 41 | |
| Sebacic acid | 111-20-6 | [39] | 202.3 | 2.2 | 0.0000073 | >2000 mg/kg—Dermal—Rat | 1000 | |
| Sodium adipate | 7486-38-6 | [39] | 190.1 | −5.03 | 0.002 | >7940 mg/kg—Dermal—Rabbit | 50,000 |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
James, T.; Collins, S.; Marczylo, T. Identification of Novel Simulants for Toxic Industrial Chemicals and Chemical Warfare Agents for Human Decontamination Studies: A Systematic Review and Categorisation of Physicochemical Characteristics. Int. J. Environ. Res. Public Health 2021, 18, 8681. https://doi.org/10.3390/ijerph18168681
James T, Collins S, Marczylo T. Identification of Novel Simulants for Toxic Industrial Chemicals and Chemical Warfare Agents for Human Decontamination Studies: A Systematic Review and Categorisation of Physicochemical Characteristics. International Journal of Environmental Research and Public Health. 2021; 18(16):8681. https://doi.org/10.3390/ijerph18168681
Chicago/Turabian StyleJames, Thomas, Samuel Collins, and Tim Marczylo. 2021. "Identification of Novel Simulants for Toxic Industrial Chemicals and Chemical Warfare Agents for Human Decontamination Studies: A Systematic Review and Categorisation of Physicochemical Characteristics" International Journal of Environmental Research and Public Health 18, no. 16: 8681. https://doi.org/10.3390/ijerph18168681
APA StyleJames, T., Collins, S., & Marczylo, T. (2021). Identification of Novel Simulants for Toxic Industrial Chemicals and Chemical Warfare Agents for Human Decontamination Studies: A Systematic Review and Categorisation of Physicochemical Characteristics. International Journal of Environmental Research and Public Health, 18(16), 8681. https://doi.org/10.3390/ijerph18168681








